Abstract
Sirtuins (SIRTs) are master metabolic regulators with protective roles against obesity and obesity-associated metabolic disorders, including non-alcoholic fatty liver disease (NAFLD) and type-2 diabetes. We aimed to ascertain whether there is a relationship between serum SIRT1 and liver steatosis severity in obese patients. Seventy-two obese patients (BMI ≥ 30 kg/m2), 18 males and 54 females, mean age 39.66 ± 12.34 years, with ultrasonographic evidence of NAFLD, were studied. BMI, transaminases, insulin, HOMA-index, HbA1c, body composition (DXA), plasma SIRT1 levels (ELISA) and representative measures of metabolic syndrome (waist circumference, fasting plasma glucose, blood pressure, HDL-cholesterol, triglycerides) and inflammation (ESR, CRP, fibrinogen) were evaluated. Thirty healthy lean patients were included as controls. SIRT1 was significantly lower in severe liver steatosis obese group compared to the mild steatosis group, both had lower SIRT1 plasma values compared to control lean patients (P = 0.0001). SIRT1 showed an inverse correlation with liver steatosis and HbA1c in univariate analysis (ρ = −0.386; P = 0.001; ρ = −0.300; P = 0.01, respectively). Multiple linear regression analysis showed that liver steatosis was the independent correlate of SIRT1 even after adjustment for potentially relevant variables (β = −0.442; P = 0.003). Serum SIRT1 might be a novel clinical/biochemical parameter associated with fat liver infiltration. Further studies in larger cohorts are warranted.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Sirtuins (SIRTs) are a family of highly conserved NAD(+)-dependent protein deacetylases acting as cellular sensors to detect energy availability and modulate metabolic processes (1). SIRT1, the most studied member of this family, is recognized as a metabolic modulator in different tissues, central to the control of several homeostatic circuits as well development, inflammation, cell cycle and reproduction. Defects in SIRT1 pathways result in metabolic disorders such as diabetes and non-alcoholic fatty liver disease (NAFLD), cardiovascular disease and neurodegeneration [1–3]. Furthermore, SIRT1 shows a tumor suppression activity in metabolic syndrome-associated cancer [4, 5].
A profound involvement of SIRT1 in several functions of the adipose tissue has been reported. The up-regulation of SIRT1 leads to decreased fat storage and increased lipolysis in differentiated adipose cells. Accordingly, an increased adipogenic potential in SIRT1-deficient cell has been observed [6]. The in vivo reduction of SIRT1 stimulates macrophage recruitment toward adipose tissue, whereas its over-expression prevents adipose tissue macrophage accumulation during chronic high-fat feeding [7]. SIRT1 inhibits adipocyte differentiation and suppresses pro-inflammatory transcription in adipocytes and macrophages, functioning as a suppressor of adipose tissue inflammation [7, 8]. Moreover, coordinately with Pparγ, SIRT1 leads to selective induction of brown adipose tissue genes and repression of visceral white adipose tissue genes associated with insulin resistance [9]. Finally, SIRT1 mRNA levels in visceral and subcutaneous adipose tissues are suppressed in obese women compared to normal-weight [10, 11]. Collectively, SIRT1 is protective from obesity-induced inflammation and insulin resistance.
Studies in humans and animal models have suggested obesity as the predisposing soil for NAFLD [12]. There are close relationships between SIRT1 and liver pathophysiology. Transgenic SIRT1 mice under a high-fat diet are almost entirely protected from hepatic steatosis and show lower lipid-induced inflammation along with better glucose tolerance [13]. On the contrary, the lack of SIRT1 activity leads to liver steatosis in the SIRT1+/− mice [14], and hepatocyte-specific deletion of SIRT1 alters fatty acid metabolism and results in fatty liver disease and inflammation [15].
Altogether, the above mentioned data suggest a decisive involvement of SIRT1 against metabolic derangements in obese. To date, there are no data on serum SIRT1 concentrations in obese individuals affected by hepatic steatosis. The objective of this study was to evaluate the relationship between SIRT1 plasma values and different degrees of fat liver infiltration in obese patients.
Subjects and methods
Subjects
Seventy-two obese patients (BMI ≥ 30 kg/m2) of both sexes (18 males, 54 females), aged 18–65 year, with ultrasound evidence of NAFLD were recruited for the study. The subjects met the following inclusion criteria: no history of current or past excessive alcohol drinking (a threshold of <20 g/d for women and <30 g/d for men); negative tests for the presence of hepatitis B surface antigen and antibody to hepatitis C virus; absence of history and findings consistent with cirrhosis and other chronic liver diseases. The patients underwent complete medical examination, anthropometric measurements (body weight, height, waist circumference), determination of fasting glycemia and insulin, homeostasis model assessment of insulin resistance (HOMA-IR) calculated from Matthews et al. [16], HbA1c, total cholesterol, HDL-cholesterol, triglycerides, erythrocyte sedimentation rate (ESR), C-reactive protein (CRP), fibrinogen, aspartate aminotransferase (AST), alanine aminotransferase (ALT), serum SIRT1, systolic and diastolic blood pressure (mmHg) and Dual energy X-ray absorptiometry (DXA) body composition. Thirty adult healthy lean individuals (range 18–65 year, mean age 37.58 ± 10.18 year, 15 males and 15 females, average BMI 22.36 ± 2.74 kg/m2), without ultrasound evidence of NAFLD, were used as controls; all the controls had the same parameters considered for the obese population of patients within the normal range (data not shown).
The study was approved by the ethical committee of the Sapienza University of Rome, Policlinico Umberto I, and was concordant with Helsinki Declaration. Each patient gave a written informed consent before admission to the study.
SIRT1 assay
The plasma SIRT1 was determined by a monoclonal antibody-based ELISA method using a commercially available human SIRT1 ELISA kit (MyBioSource, Cod. GDMBS705558). Microtiter plates were coated with equal amount of primary mouse anti-human SIRT1 monoclonal IgG. 100 µL standard and serum samples were pipetted in each well and the protocol was followed by using secondary avidin conjugated horseradish peroxidase. The formation of horseradish peroxidase was measured at 405 nm using ELISA reader (Quanta Biotech, UK). Seven different concentrations of purified SIRT1 (0.15, 0.312, 0.625, 1.25, 2.5, 5.0, and 10 ng/mL) were used to plot a standard curve. The inter- and intra-assay coefficient of variation were 4 and 6 % respectively, with a detection limit of 0.1 ng/mL.
Determination of liver adiposity
The determination of NAFLD was based on liver-kidney contrast measured with ultrasonography [17] by one single trained radiologist with extensive experience in abdominal ultrasound examinations. The analysis was carried out using a Esaote Medica apparatus equipped with a convex 3.5 MHz probe (Esaote MyLab40, Esaote Europe B.V., The Netherlands). The severity of liver adiposity was based according to the brightness of the liver estimated as a numerical value (1 = mild lipid accumulation; and 2 = severe lipid accumulation).
DXA analysis
DXA was performed by one single experienced technician using a DXA scan (Hologic Inc., Bedford, MA, USA, QDR 4500 W). Coefficient of variation for fat mass (FM) was <1.5 %. Body composition was measured in the whole body and in specific body regions. Delimiters for regional analysis were determined by a standard software (Hologic Inc., S/N 47168 VER. 11.2). With the use of specific anatomic landmarks, regions of the trunk and legs were distinguished. Whole-body FM and trunk to leg FM (trunk/leg) ratio, calculated as trunk FM divided by legs FM (an index of FM distribution that closely associates with cardiometabolic risk factors) were recorded [18]. Scans were performed according to the manufacturer’s instructions.
Statistical analysis
Data were analyzed with the use of STATISTICA software, version 6.1 (Stat Soft, Inc., Tulsa, Oklahoma). Results were expressed as mean ± SD. Differences between groups of steatosis were analyzed using ANOVA for continuous variables. Spearman correlation coefficient test was used to analyze the relationship between variables. Sex, age, liver steatosis, BMI, WC, total FM, trunk/legs FM ratio, ALT, AST, HOMA-IR, HbA1c and CRP in relation to SIRT1 were tested by the use of multivariate analyses. All P values presented are two-tailed, and values less than 0.05 are considered to indicate statistical significance.
Results
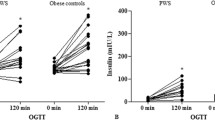
Mean obese patient age was 39.58 ± 12.27 year, 25.0 % of the participants were male (n = 18) and 75.0 % were female (n = 54). Their average BMI was 41.86 ± 7.89 kg/m2, the mean WC was 127.42 ± 15.83 cm, 11 were diabetics. All patients had fat liver infiltration. Based on liver brightness, two different subgroups emerged: 38 patients (52.77 %) presented mild liver lipid accumulation, 34 patients presented intensely bright liver, with severe lipid accumulation (47.22 %). The main features of the obese population, stratified according to the ultrasound degree of fat liver infiltration, are summarized in Table 1. There was no significant difference in age, fasting plasma glucose and insulin, HOMA-IR, inflammation markers, systo/diastolic blood pressure, total FM, HDL-C and triglycerides between groups. Instead, weight, BMI, trunk/legs FM ratio, WC, AST, ALT and HbA1c were all significantly higher in the group with severe liver fat accumulation. SIRT1 was detected in all individuals and the SIRT1 measured values were significantly lower (P = 0.0001) in obese subjects with severe steatosis compared to those with mild fatty liver infiltration (Fig. 1). The group of lean healthy controls with no ultrasound evidence of fat liver accumulation, had significantly higher levels of SIRT1 compared with both severe and mild liver steatosis patients (Fig. 1).
SIRT1 plasma levels in obese subjects with mild and severe fat liver infiltration and lean healthy controls. Obese patients were stratified according to the ultrasound degree of liver brightness. Solid circles represent the patients individual values. Means are indicated by the horizontal lines; SIRT1 was significantly higher (P = 0.0001) in subjects with mild steatosis compared with those with severe steatosis; the mean value of SIRT1 in lean healthy controls was significantly higher than the mean values measured in both mild steatosis (P < 0.001) and severe steatosis (P < 0.001) groups
The correlation between SIRT1 and the other variables in the obese patients was analyzed using the Spearman correlation coefficient test. The analysis showed that SIRT1 was inversely correlated with liver steatosis (ρ = −0.386; P = 0.001) and HbA1c (ρ = −0.300; P = 0.01), and that SIRT1 did not correlate with BMI, total FM, trunk/legs FM ratio, WC, BP, ALT, AST, HDL-cholesterol, triglycerides, ESR, CRP, fibrinogen, fasting plasma glucose, insulin and HOMA-IR.
Sex and age adjusted multivariate regression analyses for the associations between SIRT1 and selected covariates for the obese study group are shown in Table 2. We performed a multivariable regression analysis to examine the predictive relationship of SIRT1 with liver steatosis and others potentially relevant variables (BMI, WC, total FM, trunk/legs FM ratio, ALT, AST, HOMA-IR, HbA1c and CRP). Liver steatosis was the best independent correlate of SIRT1 (β = −0.442; R = 0.564; P = 0.003), even after the adjustment for the others variables (Table 2).
Discussion
Fat liver accumulation of metabolic origin is one of the most common liver disease [19], with an estimated prevalence between 57.5 and 74 % in obese subjects [20, 21]. Together, obesity and NAFLD reach alarming proportion and represent independent risk factors for cardiometabolic events [19, 22]. Fat liver infiltration, in fact, is a component of the metabolic syndrome [23] and patients with steatosis, analogously to the patients with altered body fat distribution, are at increased risk of diabetes and cardiovascular disease [18, 19, 24–27].
There are no specific functional indicators of steatosis severity. Recently, important roles in energy homeostasis, liver function and protective effects on obesity and metabolic disorders have been ascribed to SIRTs. Mammalian SIRT1, the ortholog of yeast gene sir 2 (silent information regulator 2) intervenes in maintaining energy balance. By deacetylating a variety of proteins that regulate anabolic and catabolic processes, SIRT1 coordinately increases cellular energy stores and maintains cellular energy homeostasis. Furthermore, several studies indicate that SIRT1 is closely linked to the extension of lifespan [1].
Our study is the first to report the measurement of serum SIRT1 in obese patients and to find that SIRT1 might be a predictor of the severity of liver steatosis.
The majority of our obese patients showed serum SIRT1 concentrations in the low normal range and their mean plasma values were significantly lower compared with the average value found in the lean controls. This finding is in line with the evidence that obese patients have lower SIRT1 expression in visceral and subcutaneous adipose tissue compared to lean patients [10, 11], and that SIRT1 mRNA and protein expression in mice adipose tissue are suppressed in diet-induced obesity [28]. Furthermore, a negative association between visceral adiposity and SIRT1 expression in peripheral blood mononuclear cells has been recently reported in humans [29].
Interestingly, we did not find any correlation between SIRT1 and BMI, FM, weight or WC, neither between SIRT1 and trunk/legs FM ratio in obese patients. However, we found that SIRT1 values were significantly lower in severe fat liver infiltration compared to mild steatosis. Although we have no definitive explanation for this pattern of expression, some hypothesis can be argued. SIRT1 controls key aspects of hepatic lipid and glucose metabolism through interaction with several transcription factors. Transgenic SIRT1 mice under a high-fat diet are almost entirely protected from hepatic steatosis [13]. On the contrary, the lack of SIRT1 activity leads to liver steatosis in the SIRT1+/− mice [14]. Thus, the healthy liver strongly contributes to the circulating levels of SIRT1.
Liver steatosis is a key determinant to the ontogeny of metabolic inflammation, being a more relevant source of serum inflammatory markers than omental adipose tissue [30]. SIRT1 has a protective effect on tissue inflammation suppressing some proinflammatory transcriptions [7, 8]. Transgenic SIRT1 mice show lower lipid-induced inflammation [13] and SIRT1 overexpression prevents adipose tissue macrophage accumulation during chronic high-fat feeding [7]. Accordingly, the in vivo reduction of SIRT1 stimulates macrophage recruitment to adipose tissue. We did not find any correlation between SIRT1 and major inflammatory markers like CRP, ESR and fibrinogen. However, it is well known that SIRT1 inhibits the transcriptional activity of NF-kappaB [31] and that SIRT1+/− mice show increased expression of proinflammatory cytokines [14]. Thus, cytokines involved in steatosis or targeted by SIRT1, should be analyzed. In particular, since NAFLD could be a relevant source of inflammatory markers [30] the measurement of classical inflammatory serum markers such as TNF-α or IL-6 is warranted.
SIRT1 participates in the control of glucose homeostasis modulating diverse biological processes [32], including insulin secretion, pancreatic β-cells protection [33] and improvement of insulin resistance [34]. Our data show that SIRT1 is inversely correlated with HbA1c while no correlation was found with HOMA-IR. This finding is partially in line with that of others [10], who demonstrated that adipose SIRT1 expression inversely correlates with HOMA-IR and other insulin resistance-related parameters, including fasting glucose in women with obesity and type 2 diabetes. We found higher HbA1c values in individuals with severe fat liver infiltration. Nevertheless, in multivariate analysis the correlation between SIRT1 and HbA1c was lost, and only liver steatosis kept significant inverse association, indicating that fat liver infiltration correlates with SIRT1 better than fat distribution and classical indices of glucose metabolism. Whether these discrepancies depend on the source of protein expression, tissutal versus plasmatic, or is due to the differences in the population of patients it is not clear and deserves further investigation. Furthermore, SIRT1 regulates multiple hormones, adipokines and growth factors implicated in energy balance, including glucose and lipid metabolism [35, 36]. Thus, the relevant role of SIRT1 as a mediator of the function of hormones and adipokines suggests that future studies should elucidate the precise effects of this interaction.
Collectively, our findings are supportive of the value of SIRT1 in estimating adiposity-related steatosis burden. Obese patients with severe fatty liver infiltration had lower amount of circulating SIRT1 compared with mild fat liver infiltration and both had lower SIRT1 compared with lean no NAFLD affected individuals. Indirectly, these results may indicate a protective potential of SIRT1 against the metabolic consequences of obesity.
Some limitations of this study need to be considered. This was a cross-sectional study, so we could not assess the causal relationship between the covariates evaluated and SIRT1. To clarify this point, a prospective study involving clinical intervention will be needed. The relatively small sample size remain a weak point, and we think that our results should be confirmed in larger cohorts. Liver ultrasound, although accurate in identifying all degrees of steatosis [37], offers semi-quantitative results. Magnetic resonance spectroscopy [38] or liver biopsy [39] are deemed to be the best options to quantitative measure liver fat content. A correlation between the plasma SIRT1 and liver tissue SIRT1 protein or gene expression was not assessed.
Interestingly, genetic variations in SIRT1 correlate with different visceral obesity parameters in obese men [40]. This finding, together with the evidence that the beneficial cellular effects of calorie restriction are largely mediated by the induction of SIRT1 [41], that SIRT1 promotes white adipocytes fat mobilization and browning of white adipose tissue [9] and that, with Pparγ, ameliorates insulin resistance [9, 10], suggests that the activation of SIRT1 by genetic or pharmacological means has the potential to elicit multiple metabolic benefits including the improvement of nonalcoholic fatty liver disease.
In conclusion, our data suggest that SIRT1 concentrations are independently associated with fatty liver disease in obese patients; its measurement could be an additional tool for the stratification of the risks associated to visceral fat in obese subjects.
References
D. Herranz, M. Serrano, SIRT1: recent lessons from mouse models. Nat. Rev. Cancer 10, 819–823 (2010)
Y. Yang, W. Duan, Y. Li, Z. Jin, J. Yan, S. Yu, D. Yi, Novel role of silent information regulator 1 in myocardial ischemia. Circulation 128, 2232–2240 (2013)
A.Z. Herskovits, L. Guarente, SIRT1 in Neurodevelopment and Brain Senescence. Neuron 81, 471–483 (2014)
D. Herranz, M. Munoz-Martin, M. Canamero, F. Mulero, B. Martinez-Pastor, O. Fernandez-Capetillo, M. Serrano, Sirt1 improves healthy ageing and protects from metabolic syndrome-associated cancer. Nat. Commun. 1, 3–17 (2010)
L.R. Saunders, E. Verdin, Sirtuins: critical regulators at the crossroads between cancer and aging. Oncogene 26, 5489–5504 (2007)
F. Xu, D. Burk, Z. Gao, J. Yin, X. Zhang, J. Weng, J. Ye, Angiogenic deficiency and adipose tissue dysfunction are associated with macrophage malfunction in SIRT1−/− mice. Endocrinology 153, 1706–1716 (2012)
M.P. Gillum, M.E. Kotas, D.M. Erion, R. Kursawe, P. Chatterjee, K.T. Nead, E.S. Muise, J.J. Hsiao, D.W. Frederick, S. Yonemitsu, A.S. Banks, L. Qiang, S. Bhanot, J.M. Olefsky, D.D. Sears, S. Caprio, I. Shulman, SIRT1 regulates adipose tissue inflammation. Diabetes 60, 3235–3245 (2011)
K.W. Cho, C.N. Lumeng, SIRT1: a guardian at the gates of adipose tissue inflammation. Diabetes 60, 3100–3102 (2011)
L. Qiang, L. Wang, N. Kon, W. Zhao, S. Lee, Y. Zhang, W. Gu, S.R. Farmer, D. Accili, Brown remodeling of white adipose tissue by SirT1-dependent deacetylation of Pparγ. Cell 150, 620–632 (2012)
Y.S. Song, S.K. Lee, Y.J. Jang, H.S. Park, J.H. Kim, Y.J. Lee, Y.S. Heo, Association between low SIRT1 expression in visceral and subcutaneous adipose tissues and metabolic abnormalities in women with obesity and type 2 diabetes. Diabetes Res. Clin. Pract. 101, 341–348 (2013)
S.B. Pedersen, J. Olholm, S.K. Paulsen, M.F. Bennetzen, B. Richelsen, Low Sirt1 expression, which is upregulated by fasting, in human adipose tissue from obese women. Int. J. Obes. 32, 1250–1255 (2008)
E. Hui, A. Xu, H. Bo Yang, K.S. Lam, Obesity as the common soil of non-alcoholic fatty liver disease and diabetes: role of adipokines. J. Diabetes Investig. 4, 413–425 (2013)
P.T. Pfluger, D. Herranz, S. Velasco-Miguel, M. Serrano, M.H. Tschöp, Sirt1 protects against high-fat diet-induced metabolic damage. Proc. Natl. Acad. Sci. USA 105, 9793–9798 (2008)
F. Xu, Z. Gao, J. Zhang, C.A. Rivera, J. Yin, J. Weng, J. Ye, Lack of SIRT1 (mammalian sirtuin 1) activity leads to liver steatosis in the SIRT1 ± mice: a role of lipid mobilization and inflammation. Endocrinology 151, 2504–2514 (2010)
A. Purushotham, T.T. Schug, Q. Xu, S. Surapureddi, X. Guo, X. Li, Hepatocyte-specific deletion of SIRT1 alters fatty acid metabolism and results in hepatic steatosis and inflammation. Cell Metab. 9, 327–338 (2009)
D.R. Matthews, J.P. Hosker, Homeostasis model assessment: insulin resistance and b-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 28, 412–419 (1985)
G. Iacobellis, G. Barbarini, C. Letizia, G. Barbaro, Epicardial fat thickness and nonalcoholic fatty liver disease in obese subjects. Obesity (Silver Spring) 22, 332–336 (2014)
T.L.I. Kelly, K.E. Wilson, S.B. Heymsfield, Dual energy X-Ray absorptiometry body composition reference values from NHANES. PLoS ONE 4, e7038 (2009)
J.M. Pappachan, A.A. Farrah, M. Edavalath, A. Mukherjee, Non-alcoholic fatty liver disease: a diabetologist’s perspective. Endocrine 45, 344–353 (2014)
P. Angulo, Nonalcoholic fatty liver disease. N. Engl. J. Med. 346, 1221–1231 (2002)
G. Marchesini, S. Moscatiello, S. Di Domizio, G. Forlani, Obesity-associated liver disease. J. Clin. Endocrinol. Metab. 93 (11 Suppl 1), S74–S80 (2008)
G. Targher, C.P. Day, E. Bonora, Risk of cardiovascular disease in patients with nonalcoholic fatty liver disease. N. Engl. J. Med. 363, 1341–1350 (2010)
A. Kotronen, H. Yki-Jarvinen, Fatty liver: a novel component of the metabolic syndrome. Arterioscler. Thromb. Vasc. Biol. 28, 27–38 (2008)
S. Sookoian, T.F. Gianotti, M.S. Rosselli, A.L. Burgueño, G.O. Castaño, C.J. Pirola, Liver transcriptional profile of atherosclerosis-related genes in human nonalcoholic fatty liver disease. Atherosclerosis 218, 378–385 (2011)
S.A. Mirbagheri, A. Rashidi, S. Abdi, D. Saedi, M. Abouzari, Liver: an alarm for the heart? Liver Int. 27, 891–894 (2007)
P. Pisto, M. Santaniemi, R. Bloigu, O. Ukkola, Y.A. Kesäniemi, Fatty liver predicts the risk for cardiovascular events in middle-aged population: a population-based cohort study. BMJ Open 4, e004973 (2014). doi:10.1136/bmjopen-2014-004973
S. Mariani, D. Fiore, G. Barbaro, S. Basciani, M. Saponara, E. D’Arcangelo, S. Ulisse, C. Moretti, A. Fabbri, L. Gnessi, Association of epicardial fat thickness with the severity of obstructive sleep apnea in obese patients. Int. J. Cardiol. 167, 2244–2249 (2013)
M.E. Kotas, M.C. Gorecki, M.P. Gillum, Sirtuin-1 is a nutrient-dependent modulator of inflammation. Adipocyte 2, 113–118 (2013)
H. Lee, S.H. Chu, J.Y. Park, H.K. Park, J.A. Im, J.W. Lee, Visceral adiposity is associated with SIRT1 expression in peripheral blood mononuclear cells: a pilot study. Endocr. J. 60, 1269–1273 (2013)
Y. Li, L. Liu, B. Wang, J. Wang, D. Chen, Simple steatosis is a more relevant source of serum inflammatory markers than omental adipose tissue. Clin. Res. Hepatol. Gastroenterol. 38, 46–54 (2014)
F. Yeung, J.E. Hoberg, C.S. Ramsey, M.D. Keller, D.R. Jones, R.A. Frye, M.W. Mayo, Modulation of NF-kappaB-dependent transcription and cell survival by the SIRT1 deacetylase. EMBO J. 23, 2369–2380 (2004)
M. Kitada, D. Koya, SIRT1 in Type 2 diabetes: mechanisms and therapeutic potential. Diabetes. Metab. J. 37, 315–325 (2013)
L. Bordone, M.C. Motta, F. Picard, A. Robinson, U.S. Jhala, J. Apfeld, T. McDonagh, M. Lemieux, M. McBurney, A. Szilvasi, E.J. Easlon, S.J. Lin, L. Guarente, Sirt1 regulates insulin secretion by repressing UCP2 in pancreatic beta cells. PLoS Biol. 4, e31 (2006)
J.H. Lee, M.Y. Song, E.K. Song, E.K. Kim, W.S. Moon, M.K. Han, J.W. Park, K.B. Kwon, B.H. Park, Overexpression of SIRT1 protects pancreatic beta-cells against cytokine toxicity by suppressing the nuclear factor-kappaB signaling pathway. Diabetes 58, 344–351 (2009)
M. Quiñones, O. Al-Massadi, J. Fernø, R. Nogueiras, Cross-talk between SIRT1 and endocrine factors: effects on energy homeostasis. Mol. Cell. Endocrinol. (2014). doi:10.1016/j.mce.2014.08.002
Y. Li, K. Wong, A. Giles, J. Jiang, J.W. Lee, A.C. Adams, A. Kharitonenkov, Q. Yang, B. Gao, L. Guarente, M. Zang, Hepatic SIRT1 attenuates hepatic steatosis and controls energy balance in mice by inducing fibroblast growth factor 21. Gastroenterology 146, 539–549 (2014)
A. Shannon, N. Alkhouri, C. Carter-Kent, L. Monti, R. Devito, R. Lopez, A.E. Feldstein, V. Nobili, Ultrasonographic quantitative estimation of hepatic steatosis in children with NAFLD. J. Pediatr. Gastroenterol. Nutr. 53, 190–195 (2011)
M. Noureddin, J. Lam, M.R. Peterson, M. Middleton, G. Hamilton, T.A. Le, R. Bettencourt, C. Changchien, D.A. Brenner, C. Sirlin, R. Loomba, Utility of magnetic resonance imaging versus histology for quantifying changes in liver fat in nonalcoholic fatty liver disease trials. Hepatology 58, 1930–1940 (2013)
S. Dasarathy, J. Dasarathy, A. Khiyami, R. Joseph, R. Lopez, A.J. Mc-Cullough, Validity of real time ultrasound in the diagnosis of hepatic steatosis: a prospective study. J. Hepatol. 51, 1061–1067 (2009)
A.V. Peeters, S. Beckers, A. Verrijken, I. Mertens, P. Roevens, P.J. Peeters, W. Van Hul, F.L. Van Gaal, Association of SIRT1 gene variation with visceral obesity. Hum. Genet. 124, 431–436 (2008)
S. Imai, F.B. Johnson, R.A. Marciniak, M. McVey, P.U. Park, L. Guarente, Sir2: an NAD-dependent histone deacetylase that connects chromatin silencing, metabolism, and aging. Cold Spring Harb. Symp. Quant. Biol. 65, 297–302 (2000)
Conflict of interest
The authors have no conflict of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mariani, S., Fiore, D., Basciani, S. et al. Plasma levels of SIRT1 associate with non-alcoholic fatty liver disease in obese patients. Endocrine 49, 711–716 (2015). https://doi.org/10.1007/s12020-014-0465-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-014-0465-x