Abstract
Inflammatory bowel disease (IBD) is a chronic inflammatory disease of the gastrointestinal tract (GI) with a high incidence rate globally, and IBD patients are often accompanied by zinc deficiency. This review aims to summarize the potential therapeutic value of zinc supplementation in IBD clinical patients and animal models. Zinc supplementation can relieve the severity of IBD especially in patients with zinc deficiency. The clinical severity of IBD were mainly evaluated through some scoring methods involving clinical performance, endoscopic observation, blood biochemistry, and pathologic biopsy. Through conducting animal experiments, it has been found that zinc plays an important role in alleviating clinical symptoms and improving pathological lesions. In both clinical observation and animal experiment of IBD, the therapeutic mechanisms of zinc interventions have been found to be related to immunomodulation, intestinal epithelial repair, and gut microbiota’s balance. Furthermore, the antioxidant activity of zinc was clarified in animal experiment. Appropriate zinc supplementation is beneficial for IBD therapy, and the present evidence highlights that alleviating zinc-deficient status can effectively improve the severity of clinical symptoms in IBD patients and animal models.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Inflammatory bowel disease (IBD) is a chronic and life-threatening inflammatory disease of the gastrointestinal tract [1, 2] with increasingly prevalent especially in newly industrialized countries [3, 4]. Ulcerative colitis (UC) and Crohn’s disease (CD) represent the two main types of IBD [5, 6], which result from multiple factors including abnormal gut microbiota, immune response disorders, environmental disturbance, and genetic susceptibility [7, 8]. IBD, as the paradigm of auto-immune disease, is often firstly initiated by poorly understood dietary factors and then in turn presents an imbalanced internal gut environment, a first local innate, and then, chronic latent systemic immune response in patients [9]. This complex and individualized disease procedure involves variable environmental factors and damages multiple tissues [9], so the diagnosis, monitoring, and treatment of this disease has many challenges. At present, the treatment for IBD is mainly through controlling disease progression and treating specific complications by using immune-suppressants, monoclonal antibodies, and nutritional manipulation [10,11,12,13]. Considering nutritional factors, trace elements, especially zinc and selenium, have attracted much attention in IBD study [7]. As one of the most importance essential trace element, zinc participates in the formation of about 3000 proteins, which involve DNA synthesis [14], gene expression [15], anti-inflammatory, antioxidant, and wound healing [14, 15]. Due to its important biological function, zinc deficiency is associated with some clinical disorders such as dermatitis, loss of appetite, impaired wound healing, increased blood ammonia, and hypogonadism, and zinc excessive have toxic effects [16]. Multiple intestinal diseases are associated with zinc levels in the body, including IBD, irritable bowel syndrome (IBS), and colorectal cancer (CRC) [17].
Zinc deficiency is common in patients with CD and UC [18,19,20] and is associated with an increased risk of subsequent hospitalizations, surgeries, and adverse disease-specific outcomes [21, 22]. It seems that monitoring and maintaining normal levels of zinc in IBD patients are necessary [23] based on its ability to keep immune balance, redox balance, and maintain normal proliferation and structure of cell [18, 24,25,26,27,28,29,30]. And clinical symptoms often are relieved after zinc supplementing with different zinc sources in IBD patients. Animal experiments are suitable for studying intervention effects and related mechanisms. In this review, we describe the relationship of zinc and IBD in clinical practice and give a summary on zinc’s therapeutic efficacy in animal models.
Clinical Studies Related to Zinc and IBD
According to the epidemiological analysis carried out by the affiliated hospitals or institutions, the IBD patients often suffer from zinc deficiency. The prevalence of disease and the association between zinc exposure and outcomes were evaluated in IBD populations [31]. The results indicated that IBD patients often suffer from zinc deficiency (serum zinc content < 70 μg/dL [32]) companied by the decrease of other trace elements including selenium (Se), magnesium (Mn), and copper (Cu) [19, 21, 32,33,34,35]. Exposure to plumbum (Pb), arson (As), Cu, and ferrum (Fe) in drinking water would induce the deterioration of IBD [33]. Fortunately, the zinc-deficiency-related adverse effects could be improved by zinc addition [21, 36]. Follow-up survey found that dietary zinc levels were negatively associated with the prevalence of IBD [37]. In addition, nickel (Ni) concentrations in the intestinal biopsies [33] and exposure periods to fluorine (F) [38] were also negative related to the risk of IBD. The above-mentioned studies indicate that zinc deficiency is associated with the high incidence of IBD, and zinc supplementation has a protective effect on IBD.
In some clinical trials, zinc and placebo have been used to observe the therapeutic effects on IBD. In these studies, the patients suffered from UC or CD were between 18 and 69 years old, and the zinc sources were variation, in which zinc gluconate was mainly used [39,40,41]; meanwhile, zinc sulfate [42], zinc acetate hydrate [43], zinc-rich foods [44], and zinc carnosine [45] were also applied (listed in Table 1). Except that zinc-carnosine chelate compound was treated by enema with a suspension, all other zinc sources were orally taken in tablets or capsules with a dose of 30–35 mg/day for 30–60 days.
The therapeutic effects of zinc supplementation on IBD could be determined through clinical examination, histopathological score, and biochemical examination [45,46,47,48,49,50]. The clinical severity of IBD were mainly evaluated through some scoring methods including the Mayo score, Ulcerative Colitis Endoscopic Severity Index (UCEIS) score, Matts endoscopic score, and the Clinical Activity Index (CAI) (listed in Table 2). The clinic performances of IBD patients include apparent bleeding, erosion, and ulcers observed under endoscopy, as well as pathological changes such as crypt expansion, mucosal layer detachment, goblet cell depletion, glandular reduction, and inflammatory cell infiltration in the biopsy intestinal tissue [45]. These situations became relived by zinc supplementation, which have been confirmed by Matts endoscopic score and Geboes histopathological score (GHS), Matts endoscopic score, and GHS et al. [40, 44, 45]. In addition, some studies showed that zinc supplementation could obviously increase the concentration of plasma and erythrocyte zinc in UC and CD patients [35, 39, 41].
The protective mechanisms of zinc on IBD have been preliminarily explored in clinical study, which mainly involve the immunomodulation, intestinal epithelial repair, and microbiota’s balance. In terms of the immunomodulation, some research suggests that zinc plays an important role in maintenance of balanced intestinal mucosal immune, which mainly involved the regulation of T cells. It has been found that zinc deficiency can lead to an imbalance of T cell subsets and promote inflammatory reactions, which can then exacerbate the pathological severity of IBD [51,52,53]. Increased Th17 cells and decreased Tregs were observed in IBD patients [54,55,56], while physiological zinc supplementation could ameliorate human IBD through inhibiting Th17-induced cytokines [57] or increasing the number of Tregs [58]. Other researches focused on the changes of some frequently used immune parameters, which is not closely related to certain immune cells. Significantly elevated fecal calprotectin and serum CRP were determined in IBD patients with zinc deficiency [19, 34]. However, zinc supplementation could increase serum interleukin 10 (IL-10) [39], decrease interleukin 2 (IL-2) [40], and tumor necrosis factor-alpha (TNF-α) [39]. There are almost no clinical trials systematically studying the effects of zinc on intestinal epithelial barrier. There is only one paper which demonstrated that zinc supplementation could significantly reduce the intestinal permeability by lactulose/mannitol ratio (L/M) test [59]. The composition of gut microbiota in IBD patients is distinct from that of healthy individuals, and disruption of the microbiota’s balance can lead to inflammation and intestinal damage [60]. Furtherly, gut microbiota-based therapeutic approaches might be used for the treatment of IBD [61]. However, it is a need to be explored whether zinc is involved in regulating intestinal flora in IBD patients.
Taken together, adequate zinc supplementation can help alleviate the clinical symptoms of IBD patients to some extent. However, it is worth noting that excessive zinc intake will cause obvious toxic symptoms (nausea, vomiting, epigastric pain, lethargy, and fatigue) [62] and impair immune response [63]. Although present published researches never used toxic doses to treat IBD, the toxicity of excessive zinc remains a high concern (Fig. 1).
The left part marked light blue shows that IBD patients suffer from deficiency of some trace elements including zinc, Mn, Se, and Cu, and exposure to Pb, As, Cu, and Fe in drinking water would induce the deterioration of IBD. IBD patients often have high hospitalization rate and surgical risk. The right part indicates that the serum zinc, erythrocyte zinc, serum IL 10, and Tregs are increased, and the scores of Mayo, UCEIS, CAI, and Matts, and the contents of Th17, MT1G, and IL-2 are decreased
Animal Experiments Related to Zinc and IBD
Although the relationship between appropriate zinc intake and remission of IBD severity has been determined based on clinical studies, the relevant mechanisms are still blurry. Animal experiment, as the most rigorous research method under controlled conditions, is suitable for studying intervention effects and mechanisms [64]. In the animal experiment focusing on the relationship of zinc levels and IBD, tablets, capsules, or dietary therapies are mostly used. In recent years, zinc nanoparticles (NPs) have been brought into focus due to its faster and better performance compared to traditional zinc sources [65, 66]. NPs possess higher physical activity and chemical neutrality, and their bioavailability can be enhanced because of the increased surface area of respective minerals [67]. Researchers have developed several nanomedicines to specifically treat IBD, and the therapeutic mechanisms of zinc NPs are similar to traditional zinc, which include eliminating reactive oxygen species (ROS), inhibiting inflammation, repairing the mucosal barrier, and eradicating pathogens [68,69,70,71,72,73]. In this review, we focus on the effects of zinc on the clinical results, inflammatory response, intestinal barrier, and gut microbiota in IBD animals, rather than the intervention differences of different zinc sources.
Clinical Evaluation and Pathological Observation
Similar to human clinical examinations, clinical detections in experimental IBD animals include clinical observation, disease activity index (DAI), colonoscopy, and serum zinc content detection. In animals suffered from colitis, food intake and body weight were obviously reduced [74,75,76,77], and DAI was significantly increased [74, 78]. Interestingly, zinc supplementation could significantly increase the average daily gain, feed intake [79,80,81], body weight [77, 82, 83], and serum zinc concentration [30] and markedly reduce DAI scores in IBD animals [75, 83].
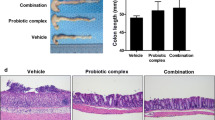
Pathological examination includes gross and histopathological observation on colon. Colitis animals had shortened colon [74, 78, 84] and increased wet weight [76, 85]. The intestinal mucosa showed congestion, edema, thickening, and obvious ulcers formation [76, 86]. Intriguingly, zinc supplementation could increase the colon length [65], mitigate the colonic injury, and decrease the macroscopic colon mucosa damage index (CMDI) [75]. Microscopically, the loss of mucosal epithelia and crypts and infiltration of inflammatory cells were observed in colon [87], while zinc supplementation is able to restore the damaged histological structure [83], increase the thickness and width of intestinal mucosa [88], and increase the ratio of jejunal mucosal villus height to crypt depth [79].
These results indicate that zinc supplementation can alleviate the severity of colitis showing as improving the clinical, anatomical, and histological status of experimental animals.
Zinc and Intestinal Barrier
Intestinal barrier, which is consisted of mucous layer, epithelial tight junction, immune cells, and intestinal flora, is important for protecting body from damages caused by virus, pathogen, and toxins. Zinc plays a pivotal role in modulating the secretion of mucus, the structure of tight junction, and the balance of intestinal flora.
The mucous layer is made from lamina propria and epithelial, including differentiated cells and undifferentiated cells. Differentiated cells include absorption epithelial, goblet cells, and Pan’s cell [89, 90]. Mucus secreted by goblet cells which cover overall inner surface of gut-intestine tract (GIT) is a physical barrier to protect from chemical, physical injuries and pathogens [91]. It has been reported that goblet cells became decreased in experimental colitis, while goblet cells and secreted mucus were increased with the zinc supplementation [75, 85, 92,93,94]. Regulation of goblet cell function may be related to Zinc Transporter (ZnT) [95]. Zinc Transporter 7(ZnT7) is responsible for the accumulation of zinc in the Golgi apparatus of cells [96, 97] and mucus secretion of goblet cells. If ZnT7 is knocked out, C57BL/6 mice become zinc deficiency [95].
Tight junction (TJ) is composed of cytoplasmic attachment proteins including occludin, claudins, and scaffold protein, which plays pivotal physiological roles in preventing abnormal immune function caused by intestine flora and active inflammation cause by bacteria and excessively infiltrated antigen in the mucous [98]. In IBD, colonic permeability is increased, which has been determined by the increasing of the flux of isothiocyanate glucan fluorescein isothiocyanate-dextran 4 kDa (FD4), the decreasing of colonic transepithelial electrical resistance (TEER), and ratio of lactose to mannitol [80, 81, 99]. The mechanisms of high colonic permeability are related to the reduced expression of tight junction proteins, including occludin and claudin-3 [100]. When dietary zinc was supplemented, increased colonic permeability was suppressed because of the increased expression of claudin-1, occludin, and tight junction protein 1(ZO-1) [80, 81, 99, 101].
It was well known that the most gut microbiota growing in the mucus layer serves as the first line of defense against harmful microbial invasion. In colitis models, the diversity and stability of gut microbiota are disturbed, showing as an increase in actinobacteria and decrease of bacteroidetes and facultative anaerobic bacteria [102, 103]. Zinc supplementation could increase the stability and diversity of the microbiota [88] and decrease pH values for maintaining acid–base balance of intestinal contents [93]. In addition, the internal balance of zinc affects the interaction between intestinal microbiota and mucosal immune function [18].
Zinc and Intestinal Mucosal Immunity
In terms of non-specific immunity, the functions of polymorphonuclear leukocytes, macrophages, and dendritic cells (DCs) in IBD model animals are all inhibited. In the body with zinc deficiency, the function of polymorphonuclear leucocytes (PMN) is impaired, showing decreased activity, phagocytosis, and decreased host defense [104,105,106]. Neutrophil infiltration is a common feature in the pathogenesis of IBD [105, 107, 108]. In IBD, mucosal myeloperoxidase (MPO) activity, mucosal prostaglandin E2 (PGE2), and Leukotriene B4 (LTB4) levels were significantly increased, all of which were improved after supplementing with zinc [109]. It has been reported that DCs in the inflamed colonic lamina propria were increased in number with colitis development [110, 111]. However, little is known about the effect of zinc levels on macrophages and DCs in IBD, which need to be further researched. It seems that researchers have overlooked the study of zinc intervention on the specific immune function of IBD animals, although many studies found that zinc deficiency or IBD decreased the production of thymulin and induced the decrease and subset-unbalance of T cells [51, 58, 86, 112, 113].
Furthermore, there are many studies about the relationship between zinc deficiency and cytokine network in IBD animal models. Zinc deficiency in IBD promotes inflammatory reactions through increasing the secretion of IL-1β and TNF-α [65, 66, 114]. After zinc supplementation, it can significantly increase the levels of Foxp3, IL-10, and TGF-1β, reduce IL-8,IL-1 β, TNF-α, prostaglandin-endoperoxide synthase 2 (Cox-2) levels in intestinal tissue [65, 66, 83, 115]. As for related mechanism, there are a few studies on signaling pathways and zinc finger proteins. Zinc enriched diet fed to piglets decreased colonic toll-like receptor 4 (TLR4) expression and reduces nuclear factor-kappa B (NF-κB) signaling and autophagy, which reduced colonic inflammation [116]. Zinc finger protein A20, induced by TNF-α, is an anti-inflammatory protein that regulates the activation of transcription factor NF-κB [117]. Mice with specific A20 deficiency will spontaneously developed lymphocytic dependent colitis and serum negative ankylosing arthritis [112], and zinc supplementation can promote upregulation of A20 mRNA and finally lead to the decreased expression of TNF-α, IL-1β, and IL-8 [118,119,120]. Meredith et al. found that the zinc finger transcription factor zDC (also known as Zbtb46 or Btbd4) is a negative regulatory factor that inhibits the activation of classical DCs [121], which proved a clue for further researching the relationship between zinc and DCs.
Zinc and Antioxidant
Zinc participates in antioxidant activity by inhibiting oxidase activity, promoting antioxidant activity, inducing metallothionein (MT) gene expression, and competing with copper and iron ions.
Zinc is an inhibitor of nicotinamide adenine dinucleotide phosphate (NADPH) oxidase, which acts as an electron donor and catalyzes the generation of oxygen (O2) and generates superoxide (O2−). Zinc is also a cofactor of superoxide dismutase (SOD), which catalyzes the dismutation of O2 to H2O2 [119, 122, 123]. During the pathogenesis of IBD, it has been found that reactive oxygen species (ROS) and malondialdehyde (MDA) levels were significantly increased, while glutathione (GSH) levels were significantly decreased [65, 66]. Interestingly, supplementary of zinc alone or in combination with other drugs can reduce MDA and nitric oxide (NO) levels and significantly increase SOD and GSH levels, indicating that zinc has antioxidant effects on experimental colitis [75, 124].
MT is a small molecule protein containing homocysteine [125], which is an effective electrophilic scavenger and anti-oxidant [126]. MT can capture various ROS, including O2−, H2O2, OH−, and NO [127]. MT can regulate zinc homeostasis by binding with 20% intracellular zinc [125]. Under oxidative stress conditions, micronutrients are released from their complexes with MT and redistributed within cells to exert antioxidant effects [120]. The expression of endogenous MTs can be stimulated by moderate dietary zinc supplementation. By transcriptomics analysis, it was demonstrated that high-dose dietary zinc can induce the expression of MT-encoding genes in the colon of healthy mice and has a significant protective effect on colitis in mice [128]. Using wild-type (MT + / +) and MT-null (MT − / −) mice as the research object, zinc treatment suppressed DSS-induced colitis particularly in MT + / + mice [92]. In the DSS-induced mouse colitis model, MTs exert a protective effect on colonic mucosal inflammation through their anti-inflammatory effect on macrophages, while MT deficiency can exacerbate the disease [87].
In addition, Fe2+ and Cu2+ can catalyze H2O2 to generate OH−, while Zn2+ can replace these redox active metals and reduces OH− generation through competing with Fe2+ and Cu2+ ions and binding to cell membranes and proteins [119, 122]. It is worth noting that zinc supplementation is helpful for the recovery of IBD, but its dosage should be well controlled, as excessive zinc can lead to side effects which is related to the antagonized levels of Cu and Fe [129].
The overview of the relationship between zinc and IBD animals is shown in the Fig. 2, and the therapeutic mechanisms are listed in Table 3.
Conclusion
In this review, substantial evidence highlights the significant role of zinc interventions in mitigating the progression of IBD in clinical patients and animal models. Zinc plays an important role in maintaining intestinal homeostasis including modulating mucosal barrier integrity and immune response and maintaining the balance of redox state and gut microbiota.
Intestinal immune dysfunction is one of the important mechanisms of IBD, but there is limited research on the immune related mechanisms when studying the effect of zinc levels on IBD. In clinical study, zinc supplementation has been found to mainly regulate T cell subsets. However, in the researches of animal models, changes in polymorphonuclear leukocytes are of greater concern. Hence, the identification of disease-specific alterations in the mucosal immune function is of utmost importance to further study the immune-related mechanisms. Consequently, it is imperative to conduct further trials in order to determine appropriate zinc dosage for providing a certain positive outcome of using zinc supplementation as adjunctive therapy for IBD.
Zinc NPs are widely used as an animal feed additive because zinc NPs have higher bioavailability and can effectively improve animal growth performance compared to traditional zinc sources [130, 131]. Meanwhile, NPs have unique physicochemical properties such as targeting to the site of inflammation and altering the pharmacokinetics of other drugs [132]. Therefore, zinc NPs have the prospect of being used in clinical practice in IBD, so designing new NPs and clarifying its effects are worthy of further vigorous exploration.
Data Availability
No datasets were generated or analyzed during the current study.
References
Thoreson R, Cullen JJ (2007) Pathophysiology of inflammatory bowel disease: an overview [J]. 575–85. https://doi.org/10.1016/j.suc.2007.03.001
Campieri M, Gionchetti P (2001) Bacteria as the cause of ulcerative colitis [J]. 132–5. https://doi.org/10.1136/gut.48.1.132
Buie MJ, Quan J, Windsor JW, et al. (2023) Global hospitalization trends for Crohn’s disease and ulcerative colitis in the 21st century: a systematic review with temporal analyses [J]. 2211–2221. https://doi.org/10.1016/j.cgh.2022.06.030
Ng SC, Shi HY, Hamidi N, et al. (2017) Worldwide incidence and prevalence of inflammatory bowel disease in the 21st century: a systematic review of population-based studies [J]. 2769–2778. https://doi.org/10.1016/s0140-6736(17)32448-0
Baumgart DC, Carding SR (2007) Inflammatory bowel disease: cause and immunobiology [J]. 1627–40. https://doi.org/10.1016/s0140-6736(07)60750-8
Xavier RJ, Podolsky DK (2007) Unravelling the pathogenesis of inflammatory bowel disease [J]. 427–34. https://doi.org/10.1038/nature06005
Vaghari-Tabari M, Jafari-Gharabaghlou D, Sadeghsoltani F, et al. (2021) Zinc and selenium in inflammatory bowel disease: trace elements with key roles? [J]. 3190–3204. https://doi.org/10.1007/s12011-020-02444-w
Lee SH, Kwon JE, Cho ML (2018) Immunological pathogenesis of inflammatory bowel disease [J]. 26–42. https://doi.org/10.5217/ir.2018.16.1.26
Rimmer P, Iqbal T (2023) Prognostic modelling in IBD [J]. 101877. https://doi.org/10.1016/j.bpg.2023.101877
Pithadia AB, Jain S (2011) Treatment of inflammatory bowel disease (IBD) [J]. 629–642
Hazlewood GS, Rezaie A, Borman M, et al. (2015) Comparative effectiveness of immunosuppressants and biologics for inducing and maintaining remission in Crohn’s disease: a network meta-analysis [J]. 344–54.e5; quiz e14–5. https://doi.org/10.1053/j.gastro.2014.10.011
Ben-Horin S, Novack L, Mao R, et al. (2022) Efficacy of biologic drugs in short-duration versus long-duration inflammatory bowel disease: a systematic review and an individual-patient data meta-analysis of randomized controlled trials [J]. 482–494. https://doi.org/10.1053/j.gastro.2021.10.037
Zhou Y, Wang D, Yan W (2023) Treatment effects of natural products on inflammatory bowel disease in vivo and their mechanisms: based on animal experiments [J]. https://doi.org/10.3390/nu15041031
MacDonald RS (2000) The role of zinc in growth and cell proliferation [J]. 1500s-8s. https://doi.org/10.1093/jn/130.5.1500S
Wu FY, Wu CW (1987) Zinc in DNA replication and transcription [J]. 251–72. https://doi.org/10.1146/annurev.nu.07.070187.001343
Evans G (1986) Zinc and its deficiency diseases [J]. 94–98
Quaglio AEV, Grillo TG, De Oliveira ECS, et al. (2022) Gut microbiota, inflammatory bowel disease and colorectal cancer [J]. 4053–4060. https://doi.org/10.3748/wjg.v28.i30.4053
Wan Y, Zhang B (2022) The impact of zinc and zinc homeostasis on the intestinal mucosal barrier and intestinal diseases [J]. https://doi.org/10.3390/biom12070900
Schneider T, Caviezel D, Ayata CK, et al. (2020) The copper/zinc ratio correlates with markers of disease activity in patients with inflammatory bowel disease [J]. otaa001. https://doi.org/10.1093/crocol/otaa001
Zupo R, Sila A, Castellana F, et al. (2022) Prevalence of zinc deficiency in inflammatory bowel disease: a systematic review and meta-analysis [J]. https://doi.org/10.3390/nu14194052
Siva S, Rubin DT, Gulotta G, et al. (2017) Zinc deficiency is associated with poor clinical outcomes in patients with inflammatory bowel disease [J]. 152–157. https://doi.org/10.1097/mib.0000000000000989
García-Mateo S, Martínez-Domínguez SJ, Gargallo-Puyuelo CJ, et al. (2023) Lifestyle can exert a significant impact on the development of metabolic complications and quality life in patients with inflammatory bowel disease [J]. https://doi.org/10.3390/nu15183983
Gîlcă-Blanariu GE, Diaconescu S, Ciocoiu M, et al. (2018) New insights into the role of trace elements in IBD [J]. 1813047. https://doi.org/10.1155/2018/1813047
Hojyo S, Fukada T (2016) Roles of zinc signaling in the immune system [J]. 6762343. https://doi.org/10.1155/2016/6762343
Fraker PJ (2005) Roles for cell death in zinc deficiency [J]. 359–62. https://doi.org/10.1093/jn/135.3.359
Cai C, Lin P, Zhu H, et al. (2015) Zinc binding to MG53 protein facilitates repair of injury to cell membranes [J]. 13830–9. https://doi.org/10.1074/jbc.M114.620690
Zhong W, McClain CJ, Cave M, et al. (2010) The role of zinc deficiency in alcohol-induced intestinal barrier dysfunction [J]. G625–33. https://doi.org/10.1152/ajpgi.00350.2009
Wang X, Valenzano MC, Mercado JM, et al. (2013) Zinc supplementation modifies tight junctions and alters barrier function of CACO-2 human intestinal epithelial layers [J]. 77–87. https://doi.org/10.1007/s10620-012-2328-8
Wen M, Zhao H, Liu G, et al. (2018) Effect of zinc supplementation on growth performance, intestinal development, and intestinal barrier-related gene expression in Pekin ducks [J]. 351–360. https://doi.org/10.1007/s12011-017-1143-7
Wen C, Wang J, Sun Z, et al. (2023) Dietary zinc ameliorates TNBS-induced colitis in mice associated with regulation of Th1/Th2/Th17 balance and NF-κB/NLRP3 signaling pathway [J]. https://doi.org/10.1007/s12011-023-03715-y
Setia MS (2016) Methodology series module 3: cross-sectional studies [J]. 261–4. https://doi.org/10.4103/0019-5154.182410
Ishihara J, Arai K, Kudo T, et al. (2022) Serum zinc and selenium in children with inflammatory bowel disease: a multicenter study in Japan [J]. 2485–2491. https://doi.org/10.1007/s10620-021-07078-z
Bagherzadeh F, Karami Horestani M, Sadeghi M et al (2022) Influence of metal ions concentration in drinking water in the development of ulcerative colitis [J]. 3539–3546. https://doi.org/10.1007/s13762-021-03498-6
Hussien A, El-Moniem SA, Tawhid Z et al (2022) Micronutrient deficiency among patients with ulcerative colitis [J] 83. https://doi.org/10.1186/s43162-022-00171-3
Soltani Z, Rafiei F, A EB, et al. The prevalence of zinc deficiency in Crohn’s disease patients [J]. 2021. p. 29–33.DOI: https://doi.org/10.26574/maedica.2020.16.1.29.
Kobayashi Y, Ohfuji S, Kondo K, et al. (2019) Association between dietary iron and zinc intake and development of ulcerative colitis: a case-control study in Japan [J]. 1703–1710. https://doi.org/10.1111/jgh.14642
Ananthakrishnan AN, Khalili H, Song M, et al. (2015) Zinc intake and risk of Crohn’s disease and ulcerative colitis: a prospective cohort study [J]. 1995–2005. https://doi.org/10.1093/ije/dyv301
Zhou S, Chai P, Dong X, et al. (2023) Drinking water quality and inflammatory bowel disease: a prospective cohort study [J]. 71171–71183. https://doi.org/10.1007/s11356-023-27460-w
Soares NRM, de Moura MSB, de Pinho FA et al (2018) Zinc supplementation reduces inflammation in ulcerative colitis patients by downregulating gene expression of Zn metalloproteins [J] 119–124. https://doi.org/10.1016/j.phanu.2018.06.004
de Moura MSB, Soares NRM, Barros SÉ L, et al. (2020) Zinc gluconate supplementation impacts the clinical improvement in patients with ulcerative colitis [J]. 15–27. https://doi.org/10.1007/s10534-019-00225-0
Paz Matias J, Costa e Silva DM, Clímaco Cruz KJ, et al. (2014) Effect of zinc supplementation on superoxide dismutase activity in patients with ulcerative rectocolitis [J]. 1434–7. https://doi.org/10.3305/nh.2015.31.3.8402
Sturniolo GC, Di Leo V, Ferronato A, et al. (2001) Zinc supplementation tightens “leaky gut” in Crohn’s disease [J]. 94–8. https://doi.org/10.1097/00054725-200105000-00003
Sakurai K, Furukawa S, Katsurada T, et al. (2022) Effectiveness of administering zinc acetate hydrate to patients with inflammatory bowel disease and zinc deficiency: a retrospective observational two-center study [J]. 78–89. https://doi.org/10.5217/ir.2020.00124
Miyaguchi K, Tsuzuki Y, Ichikawa Y, et al. (2023) Positive zinc intake and a Japanese diet rich in n-3 fatty acids induces clinical remission in patients with mild active ulcerative colitis: a randomized interventional pilot study [J]. 82–88. https://doi.org/10.3164/jcbn.22-72
Itagaki M, Saruta M, Saijo H, et al. (2014) Efficacy of zinc-carnosine chelate compound, Polaprezinc, enemas in patients with ulcerative colitis [J]. 164–72. https://doi.org/10.3109/00365521.2013.863963
Schroeder KW, Tremaine WJ, Ilstrup DM (1987) Coated oral 5-aminosalicylic acid therapy for mildly to moderately active ulcerative colitis. A randomized study [J]. 1625–9. https://doi.org/10.1056/nejm198712243172603
Travis SP, Schnell D, Krzeski P, et al. (2012) Developing an instrument to assess the endoscopic severity of ulcerative colitis: the Ulcerative Colitis Endoscopic Index of Severity (UCEIS) [J]. 535–42. https://doi.org/10.1136/gutjnl-2011-300486
Rachmilewitz D (1989) Coated mesalazine (5-aminosalicylic acid) versus sulphasalazine in the treatment of active ulcerative colitis: a randomised trial [J]. 82–6. https://doi.org/10.1136/bmj.298.6666.82
Flavell Matts S (1961) The value of rectal biopsy in the diagnosis of ulcerative colitis1 [J]. 393–407
Geboes K, Riddell R, Ost A, et al. (2000) A reproducible grading scale for histological assessment of inflammation in ulcerative colitis [J]. 404–9. https://doi.org/10.1136/gut.47.3.404
Prasad AS (2009) Zinc: role in immunity, oxidative stress and chronic inflammation [J]. 646–52. https://doi.org/10.1097/MCO.0b013e3283312956
Kim B, Kim HY, Yoon BR, et al. (2020) Cytoplasmic zinc promotes IL-1β production by monocytes and macrophages through mTORC1-induced glycolysis in rheumatoid arthritis [J]. eabi7400. https://doi.org/10.1126/scisignal.abi7400
Rink L, Haase H (2007) Zinc homeostasis and immunity [J] 1–4. https://doi.org/10.1016/j.it.2006.11.005
Jiang P, Zheng C, Xiang Y, et al. (2023) The involvement of TH17 cells in the pathogenesis of IBD [J]. 28–42. https://doi.org/10.1016/j.cytogfr.2022.07.005
Chen L, Ruan G, Cheng Y, et al. (2022) The role of Th17 cells in inflammatory bowel disease and the research progress [J]. 1055914. https://doi.org/10.3389/fimmu.2022.1055914
Fujino S, Andoh A, Bamba S, et al. (2003) Increased expression of interleukin 17 in inflammatory bowel disease [J]. 65–70. https://doi.org/10.1136/gut.52.1.65
Herrlinger KR, Diculescu M, Fellermann K, et al. (2013) Efficacy, safety and tolerability of vidofludimus in patients with inflammatory bowel disease: the entrance study [J]. 636–43. https://doi.org/10.1016/j.crohns.2012.09.016
Dünkelberg S, Maywald M, Schmitt AK, et al. (2020) The interaction of sodium and zinc in the priming of T cell subpopulations regarding Th17 and Treg cells [J]. e1900245. https://doi.org/10.1002/mnfr.201900245
Sturniolo GC, Di Leo V, Ferronato A et al (2001) Zinc supplementation tightens “leaky gut” in Crohn’s disease [J] 94–98. https://doi.org/10.1097/00054725-200105000-00003
Foppa C, Rizkala T, Repici A, et al. (2023) Microbiota and IBD: current knowledge and future perspectives [J]. https://doi.org/10.1016/j.dld.2023.11.015
Khan I, Ullah N, Zha L, et al. (2019) Alteration of gut microbiota in inflammatory bowel disease (IBD): cause or consequence? IBD treatment targeting the gut microbiome [J]. https://doi.org/10.3390/pathogens8030126
Fosmire GJ (1990) Zinc toxicity [J]. 225–7. https://doi.org/10.1093/ajcn/51.2.225
Chandra RK (1984) Excessive intake of zinc impairs immune responses [J] 1443–6. https://doi.org/10.1001/jama.1984.03350110043027
Bhide A, Shah PS, Acharya G (2018) A simplified guide to randomized controlled trials [J]. 380–387. https://doi.org/10.1111/aogs.13309
Li J, Chen H, Wang B, et al. (2017) ZnO nanoparticles act as supportive therapy in DSS-induced ulcerative colitis in mice by maintaining gut homeostasis and activating Nrf2 signaling [J]. 43126. https://doi.org/10.1038/srep43126
Abou Zaid OA, El-sonbaty SM, Heba M (2017) Evaluation of therapeutic role of zinc oxide nanoparticles on dextran sulfate sodium salt-induced ulcerative colitis in rats via modulation of COX-2, IL-6 TNF-α, oxidant and antioxidant defense system on colon [J]. 554–559
Hassan S, Hassan FU, Rehman MS (2020) Nano-particles of trace minerals in poultry nutrition: potential applications and future prospects [J]. 591–612. https://doi.org/10.1007/s12011-019-01862-9
Jin T, Lu H, Zhou Q, et al. (2024) H(2) S-releasing versatile montmorillonite nanoformulation trilogically renovates the gut microenvironment for inflammatory bowel disease modulation [J]. e2308092. https://doi.org/10.1002/advs.202308092
Zeng Y, Fan M, Zhou Q, et al. (2023) Reactive oxygen species‐activated CO versatile nanomedicine with innate gut immune and microbiome remodeling effects for treating inflammatory bowel disease [J] 2304381. https://doi.org/10.1002/adfm.202304381
Zhang C, Li Q, Shan J, et al. (2023) Multifunctional two-dimensional Bi(2)Se(3) nanodiscs for anti-inflammatory therapy of inflammatory bowel diseases. [J]. 252–264. https://doi.org/10.1016/j.actbio.2023.02.016
Zhang C, Li Q, Xing J, et al. (2024) Tannic acid and zinc ion coordination of nanase for the treatment of inflammatory bowel disease by promoting mucosal repair and removing reactive oxygen and nitrogen species [J]. 347–360. https://doi.org/10.1016/j.actbio.2024.02.015
Cao F, Gui S-Y, Gao X et al (2022) Research progress of natural product-based nanomaterials for the treatment of inflammation-related diseases [J] 110686. https://doi.org/10.1016/j.matdes.2022.110686
Li Q, Lin L, Zhang C, et al. (2024) The progression of inorganic nanoparticles and natural products for inflammatory bowel disease [J]. 17. https://doi.org/10.1186/s12951-023-02246-x
Suwendi E, Iwaya H, Lee JS, et al. (2012) Zinc deficiency induces dysregulation of cytokine productions in an experimental colitis of rats [J]. 329–36. https://doi.org/10.2220/biomedres.33.329
Sonkar A, Sachdeva P (2022) Evaluation of protective effect of atorvastatin in combination with zinc sulphate on acetic acid induced ulcerative colitis in rats [J]
Di Leo V, D’Incà R, Barollo M, et al. (2001) Effect of zinc supplementation on trace elements and intestinal metallothionein concentrations in experimental colitis in the rat. [J]. 135–9. https://doi.org/10.1016/s1590-8658(01)80068-2
Sturniolo GC, Fries W, Mazzon E, et al. (2002) Effect of zinc supplementation on intestinal permeability in experimental colitis. [J]. 311–5. https://doi.org/10.1067/mlc.2002.123624
Iwaya H, Kashiwaya M, Shinoki A, et al. (2011) Marginal zinc deficiency exacerbates experimental colitis induced by dextran sulfate sodium in rats [J]. 1077–82. https://doi.org/10.3945/jn.111.138180
Ou D, Li D, Cao Y, et al. (2007) Dietary supplementation with zinc oxide decreases expression of the stem cell factor in the small intestine of weanling pigs [J]. 820–6. https://doi.org/10.1016/j.jnutbio.2006.12.022
Zhang B, Guo Y (2009) Supplemental zinc reduced intestinal permeability by enhancing occludin and zonula occludens protein-1 (ZO-1) expression in weaning piglets [J]. 687–93. https://doi.org/10.1017/s0007114509289033
Song ZH, Ke YL, Xiao K, et al. (2015) Diosmectite-zinc oxide composite improves intestinal barrier restoration and modulates TGF-β1, ERK1/2, and Akt in piglets after acetic acid challenge. [J]. 1599–607. https://doi.org/10.2527/jas.2014-8580
Jensen-Waern M, Melin L, Lindberg R, et al. (1998) Dietary zinc oxide in weaned pigs--effects on performance, tissue concentrations, morphology, neutrophil functions and faecal microflora [J]. 225–31. https://doi.org/10.1016/s0034-5288(98)90130-8
Park JS, Choi J, Kwon JY, et al. (2018) A probiotic complex, rosavin, zinc, and prebiotics ameliorate intestinal inflammation in an acute colitis mouse model [J]. 37. https://doi.org/10.1186/s12967-018-1410-1
Gao H, Dai W, Zhao L, et al. (2018) The role of zinc and zinc homeostasis in macrophage function [J]. 6872621. https://doi.org/10.1155/2018/6872621
McGourty K, Vijayakumar R, Wu T, et al. (2022) ZnT2 is critical for TLR4-mediated cytokine expression in colonocytes and modulates mucosal inflammation in mice [J]. https://doi.org/10.3390/ijms231911467
Higashimura Y, Takagi T, Naito Y, et al. (2020) Zinc deficiency activates the IL-23/Th17 axis to aggravate experimental colitis in mice [J]. 856–866. https://doi.org/10.1093/ecco-jcc/jjz193
Tsuji T, Naito Y, Takagi T, et al. (2013) Role of metallothionein in murine experimental colitis [J]. 1037–46. https://doi.org/10.3892/ijmm.2013.1294
Li B, Van Kessel A, Caine W, et al. (2001) Small intestinal morphology and bacterial populations in ileal digesta and feces of newly weaned pigs receiving a high dietary level of zinc oxide [J] 511–516. https://doi.org/10.4141/A01-043
Knoop KA, Newberry RD (2018) Goblet cells: multifaceted players in immunity at mucosal surfaces [J]. 1551–1557. https://doi.org/10.1038/s41385-018-0039-y
Read SA, Obeid S, Ahlenstiel C, et al. (2019) The role of zinc in antiviral immunity [J]. 696–710. https://doi.org/10.1093/advances/nmz013
Maares M, Keil C, Straubing S, et al. (2020) Zinc deficiency disturbs mucin expression, O-glycosylation and secretion by intestinal goblet cells. [J]. https://doi.org/10.3390/ijms21176149
Tran CD, Ball JM, Sundar S, et al. (2007) The role of zinc and metallothionein in the dextran sulfate sodium-induced colitis mouse model. [J]. 2113–21. https://doi.org/10.1007/s10620-007-9765-9
Kwon CH, Lee CY, Han SJ, et al. (2014) Effects of dietary supplementation of lipid-encapsulated zinc oxide on colibacillosis, growth and intestinal morphology in weaned piglets challenged with enterotoxigenic Escherichia coli. [J]. 805–13. https://doi.org/10.1111/asj.12215
Liu P, Pieper R, Rieger J, et al. (2014) Effect of dietary zinc oxide on morphological characteristics, mucin composition and gene expression in the colon of weaned piglets. [J]. e91091. https://doi.org/10.1371/journal.pone.0091091
Kable ME, Riazati N, Kirschke CP, et al. (2020) The Znt7-null mutation has sex dependent effects on the gut microbiota and goblet cell population in the mouse colon [J]. e0239681. https://doi.org/10.1371/journal.pone.0239681
Kirschke CP, Huang L (2003) ZnT7, a novel mammalian zinc transporter, accumulates zinc in the Golgi apparatus [J]. 4096–102. https://doi.org/10.1074/jbc.M207644200
Chi ZH, Wang X, Wang ZY, et al. (2006) Zinc transporter 7 is located in the cis-Golgi apparatus of mouse choroid epithelial cellz [J]. 1807–11. https://doi.org/10.1097/01.wnr.0000239968.06438.c5
Martel J, Chang SH, Ko YF, et al. (2022) Gut barrier disruption and chronic disease [J]. 247–265. https://doi.org/10.1016/j.tem.2022.01.002
Zhang J, Li Z, Yu C et al (2022) Efficacy of using zinc oxide nanoparticle as a substitute to antibiotic growth promoter and zinc sulphate for growth performance, antioxidant capacity, immunity and intestinal barrier function in broilers [J] 562–576. https://doi.org/10.1080/1828051X.2022.2041494
Miyoshi Y, Tanabe S, Suzuki T (2016) Cellular zinc is required for intestinal epithelial barrier maintenance via the regulation of claudin-3 and occludin expression [J]. G105–16 https://doi.org/10.1152/ajpgi.00405.2015
Shao Y, Wolf PG, Guo S, et al. (2017) Zinc enhances intestinal epithelial barrier function through the PI3K/AKT/mTOR signaling pathway in Caco-2 cells [J]. 18–26. https://doi.org/10.1016/j.jnutbio.2017.01.013
Hansen J, Gulati A, Sartor RB (2010) The role of mucosal immunity and host genetics in defining intestinal commensal bacteria [J]. 564–71. https://doi.org/10.1097/MOG.0b013e32833f1195
Wu R, Xiong R, Li Y, et al. (2023) Gut microbiome, metabolome, host immunity associated with inflammatory bowel disease and intervention of fecal microbiota transplantation [J]. 103062. https://doi.org/10.1016/j.jaut.2023.103062
Chen S, Saeed A, Liu Q, et al. (2023) Macrophages in immunoregulation and therapeutics [J]. 207. https://doi.org/10.1038/s41392-023-01452-1
Guan Q (2019) A comprehensive review and update on the pathogenesis of inflammatory bowel disease [J]. 7247238. https://doi.org/10.1155/2019/7247238
Hassan A, Sada KK, Ketheeswaran S, et al. (2020) Role of zinc in mucosal health and disease: a review of physiological, biochemical, and molecular processes [J]. e8197. https://doi.org/10.7759/cureus.8197
Luk HH, Ko JK, Fung HS, et al. (2002) Delineation of the protective action of zinc sulfate on ulcerative colitis in rats [J]. 197–204. https://doi.org/10.1016/s0014-2999(02)01592-3
Zhang Z, Zheng M, Bindas J, et al. (2006) Critical role of IL-17 receptor signaling in acute TNBS-induced colitis [J]. 382–8. https://doi.org/10.1097/01.Mib.0000218764.06959.91
Liu J X, Liu XG, Chen BW (2003) The role of zinc sulfate solution enema on trinitrobenzenesulphonic acid-induced colitis in rats [J]. 7–10
Krajina T, Leithäuser F, Möller P, et al. (2003) Colonic lamina propria dendritic cells in mice with CD4+ T cell-induced colitis [J]. 1073–83. https://doi.org/10.1002/eji.200323518
Middel P, Raddatz D, Gunawan B, et al. (2006) Increased number of mature dendritic cells in Crohn’s disease: evidence for a chemokine mediated retention mechanism [J]. 220–7. https://doi.org/10.1136/gut.2004.063008
Hammer GE, Turer EE, Taylor KE, et al. (2011) Expression of A20 by dendritic cells preserves immune homeostasis and prevents colitis and spondyloarthritis [J]. 1184–93. https://doi.org/10.1038/ni.2135
Dardenne M (2002) Zinc and immune function. [J]. S20-S23
Elmadfa I, Meyer AL (2019) The role of the status of selected micronutrients in shaping the immune function [J]. 1100–1115. https://doi.org/10.2174/1871530319666190529101816
Song ZH, Xiao K, Ke YL, et al. (2015) Zinc oxide influences mitogen-activated protein kinase and TGF-β1 signaling pathways, and enhances intestinal barrier integrity in weaned pigs [J]. 341–8. https://doi.org/10.1177/1753425914536450
Hu L, Cheng S, Li Y, et al. (2018) Chitosan-Zn chelate downregulates TLR4-NF-κB signal pathway of inflammatory response and cell death-associated proteins compared to inorganic zinc [J]. 92–98. https://doi.org/10.1007/s12011-017-1174-0
Opipari AW Jr, Boguski MS, Dixit VM (1990) The A20 cDNA induced by tumor necrosis factor alpha encodes a novel type of zinc finger protein. [J] 14705–8. https://doi.org/10.1016/S0021-9258(18)77165-2
Prasad AS (2007) Zinc: mechanisms of host defense. [J]. 1345–9. https://doi.org/10.1093/jn/137.5.1345
Prasad AS (2008) Zinc in human health: effect of zinc on immune cells. [J]. 353–7. https://doi.org/10.2119/2008-00033.Prasad
Marreiro DD, Cruz KJ, Morais JB, et al. (2017) Zinc and oxidative stress: current mechanisms [J]. https://doi.org/10.3390/antiox6020024
Meredith MM, Liu K, Kamphorst AO, et al. (2012) Zinc finger transcription factor zDC is a negative regulator required to prevent activation of classical dendritic cells in the steady state [J]. 1583–93. https://doi.org/10.1084/jem.20121003
Prasad AS (2014) Zinc: an antioxidant and anti-inflammatory agent: role of zinc in degenerative disorders of aging [J]. 364–71. https://doi.org/10.1016/j.jtemb.2014.07.019
Prasad AS (2008) Clinical, immunological, anti-inflammatory and antioxidant roles of zinc [J]. 370–7. https://doi.org/10.1016/j.exger.2007.10.013
Mohammadi E, Qujeq D, Taheri H, et al. (2017) Evaluation of serum trace element levels and superoxide dismutase activity in patients with inflammatory bowel disease: translating basic research into clinical application [J]. 235–240. https://doi.org/10.1007/s12011-016-0891-0
Wessels I, Maywald M, Rink L (2017) Zinc as a gatekeeper of immune function [J]. https://doi.org/10.3390/nu9121286
Kang M, Zhao L, Ren M, et al. (2015) Reduced metallothionein expression induced by zinc deficiency results in apoptosis in hepatic stellate cell line LX-2 [J]. 20603–9
Jarosz M, Olbert M, Wyszogrodzka G, et al. (2017) Antioxidant and anti-inflammatory effects of zinc. Zinc-dependent NF-κB signaling [J]. 11–24. https://doi.org/10.1007/s10787-017-0309-4
Foligné B, George F, Standaert A, et al. (2020) High-dose dietary supplementation with zinc prevents gut inflammation: investigation of the role of metallothioneins and beyond by transcriptomic and metagenomic studies [J]. 12615–12633. https://doi.org/10.1096/fj.202000562RR
Kruis W, Phuong Nguyen G (2016) Iron deficiency, zinc, magnesium, vitamin deficiencies in Crohn’s disease: substitute or not? [J]. 105–11. https://doi.org/10.1159/000443012
Hussan F, Krishna D, Preetam VC, et al. (2022) Dietary supplementation of nano zinc oxide on performance, carcass, serum and meat quality parameters of commercial broilers [J]. 348–353. https://doi.org/10.1007/s12011-021-02635-z
Samy A, Hassan H, Elsherif H (2022) Effect of nano zinc oxide and traditional zinc (oxide and sulphate) sources on performance, bone characteristics and physiological parameters of broiler chicks [J] 486–492. https://doi.org/10.47278/journal.ijvs/2022.129
Yang M, Zhang Y, Ma Y et al (2020) Nanoparticle-based therapeutics of inflammatory bowel diseases: a narrative review of the current state and prospects. [J] 157–173. https://doi.org/10.1097/JBR.0000000000000078
Acknowledgements
The authors wish to express their gratitude to Sichuan Youngster Technology Co., Ltd. for their technical assistance. We also thank my colleagues Bo Zhang and Xiaoqin Wang for their assistance.
Funding
This work was supported by Chengdu University (2081921001), National Natural Science Foundation of China (32370557), Nanchong Key Laboratory of Wildlife Nutrition Ecology and Disease Control (NCKL202201), and Training Program for Innovation and Entrepreneurship of Chengdu University (CDUCX2024759).
Author information
Authors and Affiliations
Contributions
X. Peng determined the title and structure of this review and guided throughout the review writing process. Y. Yang and R. Zhong conducted the initial draft writing. All other authors participated in the improvement and revision of the paper and have given the final approval of the manuscript to be published.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Peng, X., Yang, Y., Zhong, R. et al. Zinc and Inflammatory Bowel Disease: From Clinical Study to Animal Experiment. Biol Trace Elem Res (2024). https://doi.org/10.1007/s12011-024-04193-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12011-024-04193-6