Abstract
A number of studies have assessed the association between serum magnesium (Mg) and premenstrual syndrome (PMS) in different population, but the findings have been inconclusive. Herein, we systematically reviewed available observational studies to elucidate the overall relationship between Mg and PMS. PubMed, Cochrane’s library, ScienceDirect, Scopus, Google Scholar, and ISI web of science databases were searched for all available literature until January 2019 for studies evaluating the association between Mg and PMS. The Newcastle-Ottawa Quality Assessment Scale was used to assess the quality of observational studies. A total of 13 studies out of 196 met our inclusion criteria and were included in our systematic review and meta-analysis. There were no associations between serum magnesium and PMS (WMD − 0.04; 95% CI, − 0.14 to 0.06; P = 0.46) during follicular or serum/erythrocyte magnesium (WMD − 0.37; 95% CI, − 1.01 to 0.27; P = 0.25)/(WMD − 0.04; 95% CI, − 0.10 to 0.03; P = 0.26) and during luteal phase except for the sub-group of studies done outside of the US in which recent association became significant and means that serum Mg is lower in PMS subjects. According to what have been discussed, although our study did not show any significant association between serum/erythrocyte Mg and PMS except for serum Mg in luteal phase in the sub-group of studies done outside of the USA, heterogeneity between studies should be taken into accounts when interpreting these results. Additional well-designed clinical trials should be considered in future research to develop firm conclusions on the efficacy of magnesium on PMS.
Registration number: CRD42018114473.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Premenstrual syndrome (PMS) is defined as a cyclic disorder with predictable psychological and physical symptoms that occur in the late luteal phase of menstrual cycle. The main symptoms are dizziness, palpitations, headache, edema, mastalgia, abdominal pains, anxiety, depressive mood, agitation, and aggression [1]. Generally, symptoms are mild, but 5–8% of women experience severe PMS, which is called premenstrual dysphoric disorder (PMDD) [2].
There are different hypotheses contributed to PMS etiology, including endocrine factors such as hypoglycemia, hyperprolactinemia, and fluctuations in the levels of circulating estradiol and progesterone. The other etiology of PMS might be excessive amounts of aldosterone or antidiuretic hormone or lower nocturnal melatonin concentrations, neurotransmitter involvement, including serotonin and gama-aminobutyric acid. None of these hypotheses have been scientifically supported [1], and, so far, the main etiology of PMS as same as the PMDD remains unclear [3]. The symptoms of PMS may be serious enough to disturb women’s regular living, quality of life, and social relationships and lead to amplified rates of suicides, accidents, joblessness, work and school absenteeism, and poor scholastic execution. Besides, reproductive health issues such as child abuse and domestic violence have also been documented in families with individuals experiencing PMS. This syndrome not only impacts the individual herself, but also has consequences for the family and even the society [4]; therefore, sufficient attention is needed to decrease its undesirable effects.
Based on current literature, many different pharmacological treatments, including hormone therapy have been recommended as possible options for women with PMS [5]. These therapies may be applicable to resolving PMS in many women, but they are also associated with significant unfavorable effects and can be expensive. Alternatives to hormone therapy, such as dietary supplementation, are being evaluated [6]. Non-pharmacologic management with some evidence for efficacy includes cognitive-behavioral relaxation therapy, aerobic exercise, as well as calcium, magnesium, vitamin B6 or L-tryptophan supplementation or intake of complex carbohydrate [7].
Magnesium (Mg) is a cofactor of more than 300 enzymes systems, which were contributed to diverse biochemical reaction regulations such as protein synthesis, muscle and nerve function, blood-glucose control, and blood pressure regulation [8]. Abnormal Mg metabolism has been reported in several neuropsychiatric disorders with prominent mood and physical symptoms, including migraine, epilepsy, and chronic pain [9,10,11,12]. Because PMS is associated with symptoms such as mood instability, fatigue, and fluid changes and share some similar characteristics with Mg deficiency symptoms, it has been hypothesized that there is a relationship between Mg and PMS [3].
Not all studies, however, have established either differences in Mg levels among women with PMS and control subjects or improvement in PMS symptoms in response to the administration of Mg [13,14,15]. Thus, the importance of Mg in the pathophysiology, diagnosis, and treatment of PMS remains unclear. Therefore, the aim of the current study was to carry out a systematic review and meta-analysis on the observational studies investigating the association between serum/erythrocyte Mg levels and PMS in general populations to reach a conclusion in this regard.
Methods and Materials
This study was performed according to the Preferred Reporting Items for Systematic Reviews and Meta-analysis (PRISMA) statement and was registered on Prospero database (CRD42018114473) [16].
Data Source and Search Strategy
We searched databases, including PubMed, Scopus, Cochrane Library, ScienceDirect, and ISI web of sciences up to December 2018 to identify relevant studies. The reference lists of the included papers were also reviewed to discover additional eligible studies. The following search strategy was run in PubMed and tailored to each database when necessary: ((((Magnesium [MeSH Terms]) OR Mg [Title/Abstract]) AND premenstrual syndrome [MeSH Terms]) OR premenstrual tension[Title/Abstract]) OR PMS[Title/Abstract].
Inclusion Criteria
To be included in the study, publications investigating the association between serum Mg and PMS or its symptoms had to meet the following criteria: (1) original articles; (2) human studies with no restrictions on study parameters (study duration, design or sample size); (3) adequate data to calculate a relevant measure of association (mean, range or interquartile range); (4) articles published in English. Articles were excluded if they were of non-human studies, review articles, case reports, editorials, and poster abstracts.
Data Extraction
Pairs of independent reviewers (A.A and H.H) screened the titles and the abstracts of each study prior to full-text screening of nominee studies. Any divergences in terms of the decision on a given study were dealt with via discussion and if necessary, arbitration by a third reviewer. For all included studies, two reviewers independently extracted information, including first author’s name, year of publication, country, sample size, participants’ age, gender, study design, dietary and PMS assessment method, and statistical adjustment.
Study Quality
The Newcastle-Ottawa Quality Assessment Scale (NOS) was used to assess the quality of each study [17]. The scale consists of assessment of three domains: selection (5 points), comparability (2 points), and outcome (3 points) for a total score of 10 points. Studies scoring 7–10, 3–6, and 0–3 points were identified as high, moderate, and low quality, respectively [18].
Statistical Analysis
Meta-analysis was performed using weighted mean difference (WMD) with 95% confidence intervals (CIs) for assessing the association between serum Mg level and PMS. If heterogeneity is presented between studies, the random effects model was used, otherwise, the fixed effects model was used. The sensitivity analyses were also performed to assess the influence of each individual study on the stability of the meta-analysis results. Each time, one study was excluded to show the study’s impact on the combined effect estimate.
Assessment of Heterogeneity
Heterogeneity of the study results was estimated by the chi-squared (χ2) test and quantified using the I2 statistic, which represents the percentage of the total variation across studies that is attributable to heterogeneity rather than to chance. I2 was calculated using the formula: I2 = 100% × (Q − df)/Q (where Q is the chi-squared statistic, and df is the degrees of freedom), and an I2 value of 75% or greater was deemed to indicate a high level of inconsistency. Significant heterogeneity was defined with a P value of < 0.05 [18].
Assessment of Publication Bias
Publication bias as was assessed by visual inspection of funnel plots and Egger’s and Begg’s tests was conducted to determine the degree of funnel plot asymmetry with P < 0.05 representing significant publication bias [18].
Results
Search Results
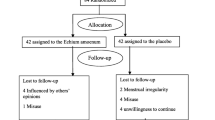
Our initial search through databases identified a total of 361 articles. Removing duplicates yielded 134 articles, which were reviewed based on the title and abstract by two independent reviewers. Seventy-nine papers retrieved and reviewed based on full text which 13 articles met inclusion criteria and were included in our systematic review and meta-analysis. The PRISMA flow diagram summarizes the results of the study selection process for this systematic review and meta-analysis (Fig. 1).
Overview of Included Studies
A total of 13 studies, including 11 case-control [3, 14, 19,20,21,22,23,24,25,26,27,28] and 1 cross-sectional [29] which involved 813 participants were included in our systematic review and meta-analysis. The included studies were conducted between 1981 and 2017. Among included studies, 7 were from USA [3, 20, 21, 23, 25, 27, 29], 2 Iran [19, 26], and the others were established from Italy [22], Australia [14], UK [28], and Turkey [24]. Five studies [3, 20, 22, 25, 28] measure Mg levels in both serum and erythrocyte, 7 in serum [14, 19, 21, 23, 24, 26, 29], and only 1 in erythrocyte [27]. Only 5 studies [3, 21, 23, 26, 29] assessed the dietary intake of participants, and the others did not mention anything [14, 19, 20, 22, 24, 25, 27, 28]. Among included studies, 12 studies [3, 14, 20,21,22,23,24,25,26,27,28,29] identified as moderate and 1 as low quality [19], respectively. Characteristics of included studies are illustrated in Table 1.
The Association Between Serum Mg and PMS During Follicular Phase
Five studies with 215 participants examined the association between serum Mg and PMS among subjects with and without PMS during follicular phase [14, 21, 22, 24, 25]. There was no significant association between serum Mg and PMS (WMD − 0.04; 95% CI, − 0.14 to 0.06; P = 0.46). There was evidence of heterogeneity between the effect sizes of included studies (I2 = 63.9% P = 0.02). No evidence of publication bias was found (Begg’s test; P = 0.32, Egger’s test; P = 0.36) (Fig. 2).
The Association Between Serum Mg and PMS During Luteal Phase
Thirteen studies with 813 participants examined the association between serum Mg and PMS among subjects with and without PMS during luteal phase [3, 14, 19,20,21,22,23,24,25,26,27,28,29]. There was no significant association between serum Mg and PMS (WMD − 0.04; 95% CI, − 0.10 to 0.03; P = 0.26). There was evidence of heterogeneity between the effect sizes of included studies (I2 = 80.8% P < 0.001) so we have done sub-group analysis based on the studies’ location (USA vs outside of the USA). The heterogeneity decreased significantly in a sub-group of studies done in the USA (I2 = 22.4% P = 0.25), but there was no significant result (WMD − 0.04; 95% CI, − 0.01 to 0.09; P = 0.12) in this subgroup too. On the other hand, in the sub-group of studies done outside of the USA, the recent association became significant which means that serum Mg is lower in PMS subjects, but there is still evidence of heterogeneity in this sub-group. No evidence of publication bias was found (Begg’s test; P = 0.62, Egger’s test; P = 0.85) (Fig. 3).
The Association Between Erythrocyte Magnesium and PMS During Luteal Phase
Five studies with 295 participants examined the association between erythrocyte Mg and PMS among subjects with and without PMS during luteal phase [3, 14, 19,20,21,22,23,24,25,26,27,28,29]. There was no significant association between erythrocyte Mg and PMS (WMD − 0.37; 95% CI, − 1.01 to 0.27; P = 0.25). There was evidence of heterogeneity between the effect sizes of included studies (I2 = 91.5% P < 0.001). No evidence of publication bias was found (Begg’s test; P = 0.32, Egger’s test; P = 0.36) (Fig. 4).
Discussion
To the best of our knowledge, no systematic review and meta-analysis has been published to evaluate the association between serum/erythrocyte Mg and PMS in general populations. Therefore, we gathered all the observational studies which examined recent relationship. In our analysis, we did not find any significant association between serum/erythrocyte Mg and PMS either in luteal or follicular phase except for serum Mg in luteal phase in the sub-group of studies done outside of the USA. Some points should be taken into accounts when interpreting these findings.
In the analysis of erythrocyte Mg during luteal phase, the difference between PMS and healthy subjects is not significant, which is in line with previous reports [3, 22, 25]. It should be mentioned that all the included studies in this category are rated as moderate quality based on NOS. One of the probable explanations for this discrepancy is that red cell Mg is not a good indicator of Mg nutritional status [22]. On the other hand, none of these studies assessed or adjusted nutritional intake of participants which could affect the overall result.
Analysis of serum Mg during luteal and follicular phase did not show any significant difference in PMS and healthy controls except for sub-group of studies done outside of the USA. These findings are consistent with previous reports [3, 21,22,23, 25, 27]. Additionally, the included studies in this category are rated as moderate quality. A probable explanation for this finding could be described by “vulnerability hypothesis” mentioned that women with PMS have the vulnerability to luteal phase mood state destabilization, and Mg deficiency may act as one of a number of potential factors contributing to that vulnerability. This hypothesis also explained why some PMS patients have normal Mg concentration, and some other Mg-deficient subjects did not show any symptoms of PMS [25, 30, 31]. Moreover, Shamberger et al. suggested that the interaction of the two elements may be more consequential to PMS than either element alone. It means that, for example, Ca/Mg ratio is more important in PMS subjects than dietary amounts of either elements [27]. Furthermore, it should be noticed that vitamin and mineral levels in blood do not parallel those in the central nervous system. It means that bioavailability of Mg in the central nervous system which is linked to the activities of several neurotransmitters could change during the luteal phase of some patients with PMS, but these changes in central nervous system may not be reflected in the blood level [21, 32].
In addition to Mg roles in brain dopamine depletion and increasing insulin sensitivity, its deficiency could promote an increased pituitary and adrenal response to environmental stimuli with increased aldosterone secretion [33,34,35]. Mg is known to increase the threshold for stressful stimuli and decrease the secretion of aldosterone, which is responsible for water retention in PMS [36]. Mg deficiency has led to aldosterone elevation, which could increase the urinary excretion of Mg and resulting in its further deficiency [37]. Mg deficiency in PMS patients may be due to decreased intake/absorption or increased renal excretion [20]. PMS subjects often complain of nervous tension which these stress, stimulated secretion of mineralocorticoids and glucocorticoids. Glucocorticoids decrease intestinal absorption, and mineralocorticoids increase renal excretion of Mg. Combined with poor eating habits, Mg depletion can occur rapidly among patients with PMS. Although PMS could have led to Mg depletion, many of the PMS symptoms could be explained by Mg deficiency [20, 26, 38]. Furthermore, it has been reported that Mg deficiency could deplete brain dopamine, possibly leading to mood disturbance, and hypertrophy of adrenal cortex leading to fluid retention [39, 40]. Mg is known as the endogenous antagonist of calcium, and the presence of selective Mg channels inside the plasma membranes is linked with membrane stabilizing properties of this cation. Reproductive hormones, progesterone and estrogen, seems to play a regulatory role on Mg balance [22]. Progesterone displays an Mg-retentive action, but estrogen has the opposite effects. The levels of recent hormones were similar in patients with PMS and healthy controls, which suggested that the ovarian function was not the primary cause for reduced Mg in PMS patients [22].
The present study has some limitations that warrant consideration. First, significant heterogeneity was present in our analysis that would limit the generalization of our findings. Heterogeneity between studies may be explained by the number of participants, participant’s different serum Mg levels, different methods for assessment of PMS and Mg, and different population and adjusted models. Moreover, designs of included studies were case-control, which were prone to selection bias. Third, small sample size of included studies. Furthermore, most of the included studies did not assess dietary intake of participants, and the others which done this measurement did not adjust the effects of dietary intake of Mg. Also genetic characteristics of participants may impact on Mg concentration and overall results which this point did not mention in included studies.
There is no previous systematic review, and meta-analysis assessed the association between serum/erythrocyte Mg and PMS in observational studies which this point is our study strength.
Conclusion
According to what have been discussed, although our study did not show any significant association between serum/erythrocyte Mg and PMS except for serum Mg in luteal phase in the sub-group of studies done outside of the USA, heterogeneity between studies should be taken into accounts when interpreting these results. Additional well-designed clinical trials should be considered in future research to develop firm conclusions on the efficacy of magnesium on PMS.
References
Verkaik S, Kamperman AM, van Westrhenen R, Schulte PF (2017) The treatment of premenstrual syndrome with preparations of Vitex agnus castus: a systematic review and meta-analysis. Am J Obstet Gynecol 217(2):150–166
Yonkers KA, O'Brien PS, Eriksson E (2008) Premenstrual syndrome. Lancet 371(9619):1200–1210
Khine K, Rosenstein DL, Elin RJ, Niemela JE, Schmidt PJ, Rubinow DR (2006) Magnesium (mg) retention and mood effects after intravenous mg infusion in premenstrual dysphoric disorder. Biol Psychiatry 59(4):327–333. https://doi.org/10.1016/j.biopsych.2005.07.022
Schiola A, Lowin J, Lindemann M, Patel R, Endicott J (2011) The burden of moderate/severe premenstrual syndrome and premenstrual dysphoric disorder in a cohort of Latin American women. Value Health 14(5 Suppl 1):S93–S95. https://doi.org/10.1016/j.jval.2011.05.008
Maleki-Saghooni N, Karimi FZ, Moghadam ZB, Najmabadi KM (2018) The effectiveness and safety of Iranian herbal medicines for treatment of premenstrual syndrome: a systematic review. Avicenna J Phytomed 8(2):96–113
Bertone-Johnson ER, Hankinson SE, Bendich A, Johnson SR, Willett WC, Manson JE (2005) Calcium and vitamin D intake and risk of incident premenstrual syndrome. Arch Intern Med 165(11):1246–1252
Rapkin A (2003) A review of treatment of premenstrual syndrome & premenstrual dysphoric disorder. Psychoneuroendocrinology 28:39–53
Grubbs RD, Maguire ME (1987) Magnesium as a regulatory cation: criteria and evaluation. Magnesium 6(3):113–127
Bolte AC, van Geijn HP, Dekker GA (2001) Management and monitoring of severe preeclampsia. Eur J Obstet Gynecol Reprod Biol 96(1):8–20
Tepper SJ, Rapoport A, Sheftell F (2001) The pathophysiology of migraine. Neurologist 7(5):279–286
Tramèr MR, Glynn CJ (2002) Magnesium Bier’s block for treatment of chronic limb pain: a randomised, double-blind, cross-over study. Pain 99(1–2):235–241
Weisleder P, Tobin JA, Kerrigan JF, Bodensteiner JB (2002) Hypomagnesemic seizures: case report and presumed pathophysiology. J Child Neurol 17(1):59–61
Cerin A, Collins A, And B-ML, Eneroth P (1993) Hormonal and biochemical profiles of premenstrual syndrome: treatment with essential fatty acids. Acta Obstet Gynecol Scand 72(5):337–343
Mira M, Stewart P, Abraham S (1988) Vitamin and trace element status in premenstrual syndrome. Am J Clin Nutr 47(4):636–641. https://doi.org/10.1093/ajcn/47.4.636
Walker A, De Souza M, Marakis G, Robinson P, Morris A, Bolland K (2002) Unexpected benefit of sorbitol placebo in Mg intervention study of premenstrual symptoms: implications for choice of placebo in RCTs. Med Hypotheses 58(3):213–220
Moher D, Shamseer L, Clarke M, Ghersi D, Liberati A, Petticrew M, Shekelle P, Stewart LA (2015) Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Syst Rev 4(1):1
O’connell WG, Losos DPM, Tugwell P (2000) The Newcastle–Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. In: Proc 3rd Symposium on Systematic Reviews, Oxford, UK
Arab A, Rafie N, Mansourian M, Miraghajani M, Hajianfar H (2018) Dietary patterns and semen quality: a systematic review and meta-analysis of observational studies. Andrology 6(1):20–28. https://doi.org/10.1111/andr.12430
Abbasi ST, Abbasi P, Suhag AH, Qureshi MA (2017) Serum magnesium and 25-hydroxy cholecalciferol in premenstrual syndrome during luteal phase. J Liaquat Uni Med Health Sci 16(4):209–212. https://doi.org/10.22442/jlumhs.171640535
Abraham GE, Lubran MM (1981) Serum and red cell magnesium levels in patients with premenstrual tension. Am J Clin Nutr 34(11):2364–2366. https://doi.org/10.1093/ajcn/34.11.2364
Chuong CJ, Dawson EB (1994) Magnesium levels in premenstrual-syndrome. Nutr Res 14(11):1623–1634
Facchinetti F, Borella P, Fioroni L, Pironti T, Genazzani AR (1990) Reduction of monocyte magnesium in patients affected by premenstrual-syndrome. J Psychosom Obstet Gynecol 11(3):221–229. https://doi.org/10.3109/01674829009084417
Gallant MP, Bowering J, Short SH, Turkki PR, Badawy S (1987) Pyridoxine and magnesium status of women with premenstrual-syndrome. Nutr Res 7(3):243–252. https://doi.org/10.1016/s0271-5317(87)80014-3
Posaci C, Erten O, Uren A, Acar B (1994) Plasma copper, zinc and magnesium levels in patients with premenstrual tension syndrome. Acta Obstet Gynecol Scand 73(6):452–455
Rosenstein DL, Elin RJ, Hosseini JM, Grover G, Rubinow DR (1994) Magnesium measures across the menstrual cycle in premenstrual syndrome. Biol Psychiatry 35(8):557–561
Saeedian Kia A, Amani R, Cheraghian B (2015) The association between the risk of premenstrual syndrome and vitamin D, calcium, and magnesium status among university students: a case control study. Health Promot Perspect 5(3):225–230. https://doi.org/10.15171/hpp.2015.027
Shamberger RJ (2003) Calcium, magnesium, and other elements in the red blood cells and hair of normals and patients with premenstrual syndrome. Biol Trace Elem Res 94(2):123–129. https://doi.org/10.1385/bter:94:2:123
Sherwood RA, Rocks BF, Stewart A, Saxton RS (1986) Magnesium and the premenstrual syndrome. Ann Clin Biochem 23(Pt 6):667–670. https://doi.org/10.1177/000456328602300607
Thys-Jacobs S, McMahon D, Bilezikian JP (2007) Cyclical changes in calcium metabolism across the menstrual cycle in women with premenstrual dysphoric disorder. J Clin Endocrinol Metab 92(8):2952–2959. https://doi.org/10.1210/jc.2006-2726
Conrad CD (2008) Chronic stress-induced hippocampal vulnerability: the glucocorticoid vulnerability hypothesis. Rev Neurosci 19(6):395–412
Lam RW, Tam EM, Yatham LN, Shiah I-S, Zis AP (2001) Seasonal depression: the dual vulnerability hypothesis revisited. J Affect Disord 63(1–3):123–132
Mousain-Bosc M, Roche M, Rapin J, Bali J-P (2004) Magnesium vitB6 intake reduces central nervous system hyperexcitability in children. J Am Coll Nutr 23(5):545S–548S
Guerrero-Romero F, Tamez-Perez H, González-González GE, Salinas-Martinez A, Montes-Villarreal J, Trevino-Ortiz J, Rodriguez-Moran M (2004) Oral magnesium supplementation improves insulin sensitivity in non-diabetic subjects with insulin resistance. A double-blind placebo-controlled randomized trial. Diabetes Metab 30(3):253–258
Amyard N, Leyris A, Monier C, Frances H, Boulu R, Henrotte J (1995) Brain catecholamines, serotonin and their metabolites in mice selected for low (MGL) and high (MGH) blood magnesium levels. Magnes Res 8(1):5–9
Atarashi K, Matsuoka H, Takagi M, Sugimoto T (1989) Magnesium ion: a possible physiological regulator of aldosterone production. Life Sci 44(20):1483–1489
MacIntyre I, Davidsson D (1958) The production of secondary potassium depletion, sodium retention, nephrocalcinosis and hypercalcaemia by magnesium deficiency. Biochem J 70(3):456–462
Senda M, Hamano T, Kubota K, Oka T, Yonemoto S, Sakaguchi Y, Nakano C, Isaka Y, Moriyama T (2017) Sp092the positive association between serum magnesium levels and plasma aldosterone concentrations in Ckd. Nephrol Dial Transplant 32(suppl_3):iii135
Serefko A, Szopa A, Poleszak E (2016) Magnesium and depression. Magnes Res 29(3):112–119
Hariri M, Azadbakht L (2015) Magnesium, iron, and zinc supplementation for the treatment of attention deficit hyperactivity disorder: a systematic review on the recent literature. Int J Prev Med 6
Phelan D, Molero P, Martínez-González MA, Molendijk M (2018) Magnesium and mood disorders: systematic review and meta-analysis. BJPsych Oopen 4(4):167–179
Author information
Authors and Affiliations
Contributions
H. Hajianfar and A. Arab contributed in conceptualizing the manuscript and editing the draft.
A. Arab, M. Moslehi, and M. Shadnoush contributed in writing and revising the manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflicts of interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This manuscript has not been published elsewhere or submitted for publication elsewhere.
Rights and permissions
About this article
Cite this article
Moslehi, M., Arab, A., Shadnoush, M. et al. The Association Between Serum Magnesium and Premenstrual Syndrome: a Systematic Review and Meta-Analysis of Observational Studies. Biol Trace Elem Res 192, 145–152 (2019). https://doi.org/10.1007/s12011-019-01672-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12011-019-01672-z