Abstract
Although aluminum chronic neurotoxicity is well documented, there are no well-established experimental protocols of Al exposure. In the current study, toxic effects of sub-chronic Al exposure have been evaluated in outbreed male rats (gastrointestinal administration). Forty animals were used: 10 were administered with AlCl3 water solution (2 mg/kg Al per day) for 1 month, 10 received the same concentration of AlCl3 for 3 month, and 20 (10 per observation period) saline as control. After 30 and 90 days, the animals underwent behavioral tests: open field, passive avoidance, extrapolation escape task, and grip strength. At the end of the study, the blood, liver, kidney, and brain were excised for analytical and morphological studies. The Al content was measured by inductively coupled plasma mass-spectrometry. Essential trace elements—Co, Cr, Cu, Fe, Mg, Mn, Mo, Se, and Zn—were measured in whole blood samples. Although no morphological changes were observed in the brain, liver, or kidney for both exposure terms, dose-dependent Al accumulation and behavioral differences (increased locomotor activity after 30 days) between treatment and control groups were indicated. Moreover, for 30 days exposure, strong positive correlation between Al content in the brain and blood for individual animals was established, which surprisingly disappeared by the third month. This may indicate neural barrier adaptation to the Al exposure or the saturation of Al transport into the brain. Notably, we could not see a clear neurodegeneration process after rather prolonged sub-chronic Al exposure, so probably longer exposure periods are required.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Aluminum (Al) is one of the most abundant elements on Earth [1]. However, its health impacts and role in the human body have drawn research interest relatively recently. The first described cases of Al chronic intoxications were associated with dialysis encephalopathy [2,3,4]. This state leads to severe damage and mortality of a significant fraction of hemodialysis patients [5]. The ability of Al to penetrate the blood-brain barrier leads to the progression of neurodegenerative effects, resembling senile dementia [6]. In this regard, Al as a toxicant has received increased attention in both clinical [7, 8] and experimental medicine [9,10,11]. Nevertheless, although a large quantity of data on the relationship between Al exposure and neurodegenerative effects was documented [12] and there are serious epidemiological data, relating Al exposure to the Alzheimer’s disease morbidity [13], the underlying cause and mechanism of the development is not yet clear [14].
To assess the effects of Al on human beings, experimental modeling approaches are required. Soluble Al salts are widely used for modeling neurodegenerative effects in laboratory animals [15,16,17], in particular, Alzheimer’s disease [18]. Nevertheless, there are no generally accepted protocols for the purpose. In case of in vitro studies [19] and observation of individual biochemical systems of model organisms [20], the interpretation of the results is unambiguous. However, for long-term exposure, the effect of study duration and other confounding factors hampers the analysis of the data obtained. Additionally, the use of Al-containing food additives [21] causes a multilateral impact on humans of excessive amounts of Al.
In our previous studies, we investigated the susceptibility of people to the accumulation of metals, including Al, in both occupationally exposed workers [22, 23] and in general population living in industrialized areas [24]. The aim of this study was to model sub-chronic Al toxicity in rats, to investigate Al effect on the activity and functional state of the central nervous system at various observation periods, to evaluate the effect of Al on the metabolism of essential elements (cobalt—Co, chromium—Cr, copper—Cu, iron—Fe, magnesium—Mg, manganese—Mn, molybdenum—Mo, selenium—Se, and zinc—Zn), and to characterize Al distribution in target organs and tissue.
Material and Methods
Animals
The study was conducted in 40 male outbreed rats, derived from Wistar line (age 12 weeks, body weight 180–200 g at the beginning of the study), and supplied by the Rappolovo animal husbandry (Leningradskaya oblast’, Russia). The animals were kept in the polycarbonate cages (five per cage), covered with a stainless steel lattice. The cage floor was covered with sawdust. In the vivarium, an artificial 12/12 light-dark cycle, the temperature of 18–26 °С and relative humidity of 30–70% were maintained. The animals had access to tap drinking water and standard rodent chow (Assortiment-Agro Ltd., Turakovo, Moscow region, Russia) ad libitum. The study was approved by the local Bioethics Committee of the Institute of Toxicology (protocol No. 8/16, dated 16.05.2016) and was conducted in accordance with the ethical regulations.
A solution of aluminum chloride (AlCl3) was prepared from aluminum chloride hexahydrate (Biochem Chemopharma, Cosne-Cours-sur-Loire, France). The per oral administration of the AlCl3·6H2O solution (2 g/L of hexahydrate, corresponding to 224 mg Al per liter) was performed through a stainless steel probe daily. A volume of 0.9 mL per 100 g of the body weight was administered, which is equivalent to a dose of 2 mg/kg Al per day. Weight dose adjustment was performed weekly after the regular weighing. The weight of the animals at the end of the study was 280–310 g.
Experimental Design
The design of the experiment is summarized in Table 1. The animals were randomly assigned to four groups. The following parameters were evaluated: Al concentration in the blood and tissue; essential elements (Co, Cu, Cr, Fe, Mg, Mn, Mo, Se, and Zn) in whole blood; open field test; grip strength, conditioned reaction of passive avoidance; extrapolation escape test; and morphological study of tissue samples of the liver, kidney, hippocampus, cerebral cortex, and white matter of the brain.
Element Quantification
To determine the content of aluminum (27Al) and essential elements (24Mg, 52Cr, 55Mn, 56Fe, 59Co, 63Cu, 66Zn, 95Mo, and 77Se), a double focusing sector field mass spectrometer Thermo Element 2 (Thermo Scientific, Bremen, Germany) with nickel cones, a cyclone spray chamber, and a polytetrafluoroethylene concentric nebulizer was employed. The main operating parameters of the device were as follows: RF power 1050 W; auxiliary flow 16.0, cooling flow 1.55, and nebulizing flow 1.015 L/min; and peristaltic pump speed 6 rpm. Deionized water was prepared using a Milli-Q® Advantage A10 system (Millipore, Molsheim, France). High purity argon (99.997%, Lentekhgaz, St. Petersburg, Russia) was used to maintain the inductively coupled plasma. Calibration solutions were prepared from a multielement IV-ICPMS-71A standard (Inorganic Ventures, Christiansburg, VA, USA). The internal standard was prepared from a rhodium CGRHN1-1 standard (Inorganic Ventures, Christiansburg, VA, USA).
For sample preparation, the UltraClave™ microwave system (Milestone, Sorisole, Italy) with 20 mL polytetrafluoroethylene liners was used. For the digestion, approximately 0.25 g of a homogenized tissue or 0.5 mL of whole blood was placed in a liner and 3 mL of concentrated nitric acid (65%, Suprapur®, Merck, Darmstadt, Germany) was added. The samples were digested for 45 min (pressure 90 bar, maximum temperature 220 °C). The resulting digestates were transferred into the 50 mL volumetric flasks (class A), and internal standard (Rh) was added to a final concentration of 1 μg/L. For more details on digestion protocol used, please, see our previous studies [23, 24].
The detection limits (3σ, μg/L) for the elements of interest were as follows: Al—0.010, Co—0.001, Cr—0.008, Cu—0.017, Fe—0.015, Mg—0.180, Mn—0.003, Mo—0.015, Zn—0.030, and Se—0.070. Quantification was performed using a calibration with internal standard correction (Rh, 1 μg/L). After every 10 sample sets, a blank and a standard control solution of the elements (concentration 1 μg/L) were measured to check for possible contamination or calibration slope change. A within-day reproducibility was 1–3% for Al, Co, Cr, Cu, Fe, Mg, Mn, Mo, and Zn, respectively, and 3–5% for Se. For the validation purpose, whole blood reference materials Seronorm™ Trace Elements Whole Blood L-1 and L-3 (Sero AS, Billingstad, Norway) were analyzed. The results are shown in Table 2.
Behavioral Tests
All behavioral tests were conducted on the next day after the last administration of AlCl3 solution (except the passive avoidance test, which was performed 24 h after a training).
Open Field Test
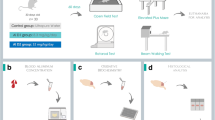
The assessment of behavior and motor activity was performed using a complex open field system for small laboratory animals TSE Acti MoTil (TSE, Bad Homburg, Germany), with three dimension infrared sensors (Open Field Phenomaster Activity regulators, TSE, Bad Homburg, Germany), 100 Lux light source, and automated recording device (Process Control MoTil 302,020 Series, TSE, Bad Homburg, Germany). Field dimensions were 50 × 50 × 50 cm. The animals had been acclimatized in the testing room for at least 30 min before the test commenced. Observation periods were 2 min, and eight parameters were recorded: horizontal and vertical movement (number of movement acts and stands), mean movement velocity, average distance, time spent at the periphery part /center of the open field cell, number of grooming acts, and general motor activity (sum of movement, grooming, and standing acts).
Grip Strength
A BIO-GS3 device (Bioseb, Vitrolles, France) with an automated Grip strength meter 303500 (TSE, Bad Homburg, Germany) was employed. Animals were allowed to grip the metal grid by forelimb, while being held near the tail base. A grid was pulled until the animal let go of it. Each measurement was repeated in triplicate and an average was taken as a result.
Extrapolation Escape Task
Extrapolation escape task is a test, which allows for estimating of the cognitive functions and emotional reactivity under acute stress conditions [25]. In this study, emotional behavioral reactivity was assessed using the Extrapolation Escape Task device (Open Science, Moscow, Russia). The device consists of vertically installed transparent plastic cylinder (7.2 cm diameter, 23 cm height), partially (2.5 cm) submerged into water (room temperature) of the external vessel (31 cm diameter, 32.5 cm height). For more details on the test and experimental setup, please, see e.g. [26]. In brief, an animal is pulled down into the inner cylinder held by the upper body part. After placing into the water, at first, the animal attempts to hop up to escape. However, the inner cylinder is high enough to prevent jumping away. After a certain time, which is a test result, the animal may realize to dive out from the cylinder, thus escaping. In our study, time of observation was limited to 2 min; otherwise, the animal was considered to fail the task. A trained observer manually recorded an amount of hops and the time before the escape.
Passive Avoidance Test
A conditional reflex of avoidance with negative pain reinforcement was evaluated by the PACS-30 Expansion device (Columbus Instruments, Columbus, OH, US) with automated infrared recorders. Compartments dimensions were 23 × 24 × 24 cm; the illuminated compartment was equipped with a 10-Lux light source. Compartments were connected by a 8 × 6.5-cm automated door. For training, an animal was placed in illuminated chamber; when it moved to the dark compartment, the door was automatically closed and the animal received electrical stimulation (1 mA) for 3 s. The animals, which did not move to the dark compartment after 2 min of the training session, were excluded from the experiment. After the training, the following indicators were assessed: latent period of entering the cell, time spent in the light compartment, and time spent in the dark compartment. The indicators were evaluated after 2 and 24 h post training. Each animal passed the test once after 2 and 24 h.
Morphological Studies
For a morphological study, samples of the liver tissue, kidneys, and brain were excised using sterile surgical tools the next day after the behavioral tests (2 days after the last AlCl3 administration). For the brain, hippocampus, white matter, and cerebral cortex were studied. After the decapitation, a whole rat brain was frozen under − 80 °C. One half of the total brain was provided for morphological studies, whereas the second part was homogenized for elemental analysis. Morphological studies were performed by a pathologist blind to the treatment of the animals according to the standardized protocol [27]. In brief, immediately after the sampling, 7-mm-thick samples were defatted in water-ethanol mixture of increasing alcohol concentration, treated with chloroform using Tissue-Tek VIP 6 device (Sakura Finetek Europe, Alphen an den Rijn, Netherlands) and paraffinized. After slicing into 5–7 μm sections with a microtome Leica RM2235 (Leica Biosystems, Wetzlar, Germany) and de-paraffinization, the samples were stained with hematoxylin and eosin (both from Sigma-Aldrich, St. Louis, MO, USA) using a Tissue-Tek device Prisma (Sakura Finetek Europe, Alphen aan den Rijn, the Netherlands). The stained sections were studied using Leica DM 1000 light microscope (Leica Microsystems, Wetzlar, Germany).
Statistics
To process the data on trace elements blood and tissue accumulation and to assess the variance between the treatment and control groups, standard parametric statistics were employed. The normality of the distributions was checked using the Shapiro-Wilk test. For behavioral tests, the differences were assessed using one-way ANOVA. Linear correlations were calculated in accordance with the Pearson’s formula. For the calculations, Microsoft Excel 2010 (Microsoft, Redmond, WA, USA) and Statistica 10 (Dell Software, Tulsa, OK, USA) software packages were used. Confidence level below 0.05 was considered as statistically significant.
Results
Condition of the Animals
Throughout the experiment, there was no significant difference between the groups in the dynamics of body weight gain, consumption of food and water and visually monitored behavior. The results of the weekly veterinary examination did not reveal any serious disorders—diarrhea, seizures, excessive psychomotor agitation, etc. for all experimental groups.
Morphological Study
Figure 1 shows hematoxylin and eosin stained samples of the white matter (Fig. 1a, b), cerebral cortex (Fig. 1c, d), and hippocampus (Fig. 1e, f). The corresponding images of the liver (Fig. S1a, b) and kidney (Fig. S1c, d) tissue are showed in the supplementary information (Fig. S1). The choice of the brain structure was made owing to their functions and reported alterations in senile dementia.
Histology samples (hematoxylin-eosin staining) of rat brain tissue after 30 days of per oral Al exposure. a, c, e White matter, cerebral cortex, and hippocampus of the treatment group, respectively. b, d, f White matter, cerebral cortex, and hippocampus of control group, respectively. Observed minute changes: commercial at—light expansion of perivascular space; number sign—a group of single dark neurons; percent—neurons under functional stress
Behavioral Tests
Among the conducted behavioral tests (open field, grip strength, extrapolation escape, and conditional reaction of passive avoidance), the differences between the treatment and control groups were significant only for the open field test. The results of the open field test are presented in Table 3. Interestingly, the significant increase of the locomotor activity compared to the control was observed after 30 days only; at a longer period of 90 days, the difference became insignificant. The results of grip strength assessment, extrapolation escape, and the passive avoidance test are presented in the supplementary information, Tables S1, S2, and S3, respectively.
Aluminum and Essential Element Quantification in the Blood and Tissues
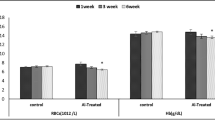
The results of Al and trace elements quantification in whole blood are presented in Table 4. Notably, the increase in blood and tissue Al did not affect the trace element status of the animals for both observation periods. Since no difference was observed for the essential trace elements in the blood, only Al was later quantified in the organs and tissue. The results are shown in Table 5.
Significant increase in Al concentration in the organs and tissues for the treatment group was clearly observed after 30 days of exposure and continued to steadily increase by the third month. As for the control group, Al content of the organs remained unchanged, in spite of a noticeable weight gain in the animals. Also, to evaluate the effect of Al exposure on the metal homeostasis, Pearson’s linear correlation coefficients between individual blood Al level and the concentrations of essential trace elements have been calculated (Table 6). Figure 2 represents the correlations between Al level in the blood and in the brain of individual animals for 30-day (Fig. 2a) and 90-day (Fig. 2b) treatment groups.
Discussion
Aluminum accumulation in the brain during the 3-month exposure period showed direct dose-dependent trend. Similar trends were observed for other studied compartments—liver, kidney, and whole blood. Thus, Al transport into the brain seems to be associated with a non-facilitated diffusion through the blood-brain barrier, mainly [28]. In comparison with heavy metals (thallium, mercury, lead, cadmium, etc.) and metalloids (arsenic and selenium), Al does not tend to form strong bonds with proteins [29,30,31]. However, it exhibits its toxic effect via the substitution of calcium at specific binding sites in proteins such as calmodulin and protein kinase C [32]. Aluminum has relatively high background level in the body, and its toxicity profile is really distinct amongst inorganic substances with virtual absence of acute toxicity [1]. Therefore, the studies of Al biochemical pathways and health outcomes are somewhat complicated. The absence of acute toxic effect may be partially reflected in our findings. The sub-chronic Al exposure had practically no effect on transport and metabolism of trace elements (Table 4). Additionally, the neurodegenerative effects, modeled by Al, were already shown not to affect selenium content in the body [33, 34]. This is also consistent with the data obtained.
As it was already mentioned, we chose the brain structures, which may be primarily affected by Al. The hippocampus is responsible for consolidating the memory, but in our case, it stays intact under 30-day treatment (Fig. 1e, f). Also the axons, which constitute the white matter, are being damaged in dementia [35] and, in our case, they also remain clear after Al administration (Fig. 1a, b). Under the development of Al-induced dementia, the gray matter was shown to accumulate a considerably larger amount of Al than the white matter [36]. Although the gray matter contained a large number of demyelinated axons, the main compartments of aluminum accumulation were the vascular-epithelial (choroid) plexus and auxiliary contractures of the blood-brain barrier, as well as the oligodendrocytes [37]. Nevertheless, the morphological studies also did not detect any significant changes in the cerebral cortex tissues of the animals (Fig. 1c, d). Thus, we cannot state that Al exposure under the doses and exposure periods employed caused a clear neurodegeneration process, causing, however, certain behavioral alterations.
Previously, the accumulation of Al was shown to cause a wide range of morphological changes and functional disorders in the brain, related to disturbances in the membrane structure and enzymatic activity. For example, for intragastric administration of 100 mg/kg per day of AlCl3 (equivalent to 20 mg/kg per day of Al) for 2 months, a spectrum of various morphological changes was reported in the brain of rats: a disruption of the homogeneity of nuclear membranes in the cortex, impaired structure of cerebellar dendrites and synaptic bends, and altered dopamine, acetylcholine, and serotonin neurotransmission in cerebrum and cerebellum [38]. Under intraperitoneal administration of a similar dose, a strong disruption of the neuronal structure and nuclear membranes was observed in the hippocampus [18]. Also, similar impairments were observed in rats after the 6 month exposure to lower doses of Al (5–20 mg/kg per day), supplied via drinking water [39]. The deleterious effect was the most pronounced in the hippocampus, where spongiform lesions of a pyramidal neuron layer were observed. In addition to the damage in the pyramidal system, the formation of neurofibrillary tangles (NFT) of the tau-protein, similarly to these under the dementia of Alzheimer’s type, was also reported [40]. Interestingly, no NFT formation was observed under the exposure to higher doses of Al over shorter periods [37, 41]. So, accounting for the low bioavailability of Al in the gastrointestinal tract, it may be assumed that Al absorption in the brain is limited by its transport via the blood-brain barrier. Nevertheless, in the current study, optical microscopy did not reveal any significant morphological changes between the treatment and control groups (Fig. 1). So, in further studies, longer exposure terms and the use of electron microscopy seem necessary.
In the first month, linear increase of Al content in the brain relative to the Al blood level was observed. Notably, by the third month, this trend has disappeared. The open field test demonstrated similar dynamics: an increase in locomotor activity of animals after 30 days of experiment disappeared for a longer period. It is tempting to assume that these observations may be interconnected. Although more insight is required to support this notion, similar findings were reported for the intragastric daily administration of Al (10 mg/kg per day) with an addition of 0.2 g/kg per day of ethanol [42]. After 4 weeks, there were differences between the experimental and control groups in reducing the motor and exploration activity of the animals receiving Al.
From the available published data, it is quite obvious that the form of Al intake drastically changes the effects induced [28, 43, 44]. For instance, a single intramuscular injection of aluminum oxyhydroxide, a widely distributed vaccine adjuvant, at a dose 0.2 mg/kg Al, led to the accumulation of Al in the brain and neurotoxic effects were observed even after 180 days [45]. Interestingly, the authors reported that under higher doses (0.4 and 0.8 mg/kg), there were no changes in animal activity or cognitive deficits. Similarly to our study, the difference was found only for the open field test, whereas for elevated O-maze, novel object recognition test, wire-mesh hang test, accelerating rotarod, hot plate test, and tail suspension test, no changes between treatment and control groups were observed. Also, as in our case, the open field test changes were expressed in increased motor activity. Therefore, similar trends in the development of Al neurotoxicity may be assumed. Considering that Al is increasing the permeability of the neural barrier [46], the causation of the differences for lower and higher Al doses may be related to the rate of Al delivery to the blood-brain barrier. Also, for aluminum oxyhydroxide, the data on long-term excretion kinetics in rabbits were reported [47]. Three maxima of Al concentration in the blood after a single intramuscular injection were indicated: after 10 h, 4 days, and 17 days. Also, the authors studied the excretion of Al in urine, demonstrating a linear increase in Al urine concentration even 30 days after the exposure [47].
On the other hand, there was an evidence of a significant decrease in the activity of animals under intraperitoneal administration of higher doses of AlCl3 (50–200 mg/kg per day) [18]. Since significantly higher doses and another route of administration were used, these data are quite complicated to be compared with other studies; however, it may be assumed that for lower doses, like in our study, such outcomes would be observed under longer observation period.
Although the brain and blood Al concentrations showed a linear growth between the controls, D30, and D90 groups, the observed significant increase in animal activity (Table 3) seems consistent with the results of elemental analysis (Table 4), if the correlations between the blood and brain Al levels are taken into account (Fig. 2). Correlation analysis is commonly used tool for elemental analysis data interpretation [24, 48, 49]. Since transporting and metabolic pathways of trace elements in the body are quite complicated, in some cases, correlation analysis allows for revealing additional information, concerning trace element metabolism and exposure biomarkers. For the blood and brain Al level (Fig. 2), clear change in relation of Al content for D30 (Fig. 2a) and D90 (Fig. 2b) treatment groups could be seen (correlation change from highly positive values to slightly negative ones). At the same time, immediate Al content showed only continuous time-dependent relation. This might indicate the change in Al transport via the neural barrier, probably, related to the adaptation of the animals to constant Al exposure by the third month or to the saturation of Al transport into the brain. Certainly, more insight is required to support these hypotheses. As for essential trace element status of the animals, although any alterations in the elemental concentrations were absent throughout the experiment, the correlations between Al concentration and concentration of the trace elements in blood, as well as the correlations between Al content in the tissues, were observed at both observation periods (Table 6). In particular, an increase of Al level in the blood altered the nature of the correlations between Al concentration and these of other metals such as zinc and cobalt. Cobalt is known to act as a potent pro-oxidant, actively generating reactive oxygen species (ROS) [50] and also affecting the transport structures responsible for the influx of calcium ions [51]. Additionally, cobalt was considered to participate in the Alzheimer’s disease pathology [34]. Accordingly, the increase in the blood cobalt level, accompanying the increase in Al, might be one of the reasons for the development of oxidative stress under Al exposure. A noticeable manifestation of this trend in case of cobalt is probably associated with its significantly lower content in the body, compared with the main redox-active metals—iron, copper, and manganese [52, 53]. Accordingly, it may be assumed that for iron, copper, and manganese, the effect of Al, at the dosages and observation periods employed, could not be visible, owing to their high background levels in the body. As for zinc, a change in its homeostasis may also contribute to the pro-oxidation, owing to the well-known antagonism between zinc and copper [54].
Interestingly, the difference in the correlations between Al and trace elements was observed not only for the corresponding “treatment-control” pairs, but also for the pair “treatment D30-treatment D90” (Fig. 2). This observation was consistent with the theories, linking age-related changes with alterations in trace element homeostasis [55]. When considering neurodegenerative diseases, aging seems to be not a causation for the development itself, rather than a necessary time factor for their manifestation [56]. Noteworthy, with the flow of time, the absorption of Al increases [57]. In our case, with the administration of relatively high doses of Al, the time factor probably affects, first of all, the delayed excretion of Al [40]. Under longer periods of exposure to Al, other mechanisms of neurodegeneration may manifest themselves. For instance, neurofibrillary plaques, characteristic for Al-induced dementia, contain a nucleus, enriched with aluminum and silicon [58]. That distinguishes those lesions from the plaques in Alzheimer’s disease, which may not contain Al [59].
Finally, it should be stressed that the main limitation of this study is associated with rather short observation period (90 days) and a use of outbreed stock. This does not allow for assessing the pathology of longer-term changes in the body and brain of the animals, associated with the exposure to Al. Additionally, young animals were used in the study, owing to the complexity to evaluate the behavior patterns of older rodents, which are often prone to obesity, especially if kept under ad libitum access to laboratory chow. Finally, the absence of the data on aluminum distribution in different brain regions may also be considered as a limitation. However, this is planned to be studied further as well as aluminum protein binding and its influence on the gene expression in the brain. Thus, the current results cannot be directly connected with the potential role of Al in the etiology of senile dementia of the Alzheimer’s type in humans. Nevertheless, we consider that our results may be helpful for future studies on Al neurotoxicity and for designing more optimal neurodegeneration models using Al. This study demonstrated the importance of Al accumulation and distribution into biological tissues, rather than only total Al level.
Conclusion
Although the amount of data, obtained in this study, is rather limited, it may be concluded that the use of Al for the modeling of neurodegenerative disorders should be accompanied with the study of the kinetic parameters of a chosen administration route. The presence of local extrema in the behavioral impairment was not that much consistent with the Al concentration itself rather than with the trends of Al accumulation and distribution into biological tissues. Thus, experimental outcomes on Al toxicity seem very sensitive to factors such as dosage, route of exposure, chemical speciation, and observation period. In certain cases, even direct dose-dependency cannot be traced. So, the data from different studies should be treated with extreme care. The effect of long-term absorption and excretion kinetics of Al on the ion transport, enzymatic systems, and blood-brain barrier permeability requires evaluating the rate of Al transport into the brain rather than its total concentration in the body compartments. Correspondingly, to ensure study representativeness, the use of Al toxicity as models for neurodegenerative disorders requires exposure terms and sampling protocol optimization.
References
Linert W, Kozlowski H (2012) Metal ions in neurological systems. Springer-Verlag Wien, Vienna. https://doi.org/10.1007/978-3-7091-1001-0
Arieff AI, Cooper JD, Armstrong D, Lazarowitz VC (1979) Dementia, renal failure, and brain aluminum. Ann Intern Med 90(5):741–747. https://doi.org/10.7326/0003-4819-90-5-741
Lederman RJ, Henry CE (1978) Progressive dialysis encephalopathy. Ann Neurol 4(3):199–204. https://doi.org/10.1002/ana.410040302
Etteldorf JN, Dobbins WT, Sweeney MJ, Smith JD, Whittington GL, Sheffield JA, Meadows RW (1962) Intermittent peritoneal dialysis in the management of acute renal failure in children. J Pediatr 60(3):327–339. https://doi.org/10.1016/S0022-3476(62)80057-2
Alfrey AC, LeGendre GR, Kaehny D (1976) The dialysis encephalopathy syndrome. Possible aluminium intoxication. New Engl J Med 294(4):184–188. https://doi.org/10.1056/NEJM197601222940402
Exley C (2001) Aluminium and Alzheimer’s disease. The science that describes the link. Elsevier, Amsterdam
Berend K, Van Der Voet G, Boer WH (2001) Acute aluminum encephalopathy in a dialysis center caused by a cement mortar water distribution pipe. Kidney Int 59(2):746–753. https://doi.org/10.1046/j.1523-1755.2001.059002746.x
de la Torre MLR, de la Lopez García SH, Martí del Moral L, Palomares Bayo M, Navarro-Alarcón M (2017) Increased serum Al levels in hemodialysis patients kept enhanced during a 2-year prospective study. Biol Trace Elem Res 178(1):7–13. https://doi.org/10.1007/s12011-016-0902-1
Fulgenzi A, De Giuseppe R, Bamonti F, Vietti D, Ferrero ME (2015) Efficacy of chelation therapy to remove aluminium intoxication. J Inorg Biochem 152:214–218. https://doi.org/10.1016/j.jinorgbio.2015.09.007
Bhalla P, Garg ML, Dhawan DK (2010) Protective role of lithium during aluminium-induced neurotoxicity. Neurochem Int 56(2):256–262. https://doi.org/10.1016/j.neuint.2009.10.009
Chen C-L, Chang K-Y, Pan T-M (2016) Monascus purpureus NTU 568 fermented product improves memory and learning ability in rats with aluminium-induced Alzheimer’s disease. J Funct Foods 21:167–177. https://doi.org/10.1016/j.jff.2015.12.017
Sideman S, Manor D (1982) The dialysis dementia syndrome and aluminum intoxication. Nephron 31(1):1–10. https://doi.org/10.1159/000182595
Killin LO, Starr JM, Shiue IJ, Russ TC (2016) Environmental risk factors for dementia: a systematic review. BMC Geriatr 16(1):175. https://doi.org/10.1186/s12877-016-0342-y
Mirza A, King A, Troakes C, Exley C (2017) Aluminium in brain tissue in familial Alzheimer’s disease. J Trace Elem Med Biol 40:30–36. https://doi.org/10.1016/j.jtemb.2016.12.001
Walton JR (2012) Cognitive deterioration and associated pathology induced by chronic low-level aluminum ingestion in a translational rat model provides an explanation of Alzheimer's disease, tests for susceptibility and avenues for treatment. Int J Alzheimer’s Dis 2012:914947. https://doi.org/10.1155/2012/914947
Fernandez-Davila ML, Razo-Estrada AC, Garcia-Medina S, Gomez-Olivan LM, Pinon-Lopez MJ, Ibarra RG, Galar-Martinez M (2012) Aluminum-induced oxidative stress and neurotoxicity in grass carp (Cyprinidae-Ctenopharingodon idella). Ecotoxicol Environ Saf 76(2):87–92. https://doi.org/10.1016/j.ecoenv.2011.09.012
Lecanu L, Papadopoulos V (2013) Modeling Alzheimer’s disease with non-transgenic rat models. Alzheimers Res Ther 5(3):17–17. https://doi.org/10.1186/alzrt171
Thenmozhi AJ, Raja TRW, Janakiraman U, Manivasagam T (2015) Neuroprotective effect of hesperidin on aluminium chloride induced Alzheimer’s disease in Wistar rats. Neurochem Res 40(4):767–776. https://doi.org/10.1007/s11064-015-1525-1
Korchazhkina OV, Ashcroft AE, Croom J, Exley C (2003) Does either the gastrointestinal peptide PYY or the neuropeptide NPY bind aluminium? J Inorg Biochem 94(4):372–380. https://doi.org/10.1016/s0162-0134(03)00031-x
Shati AA, Elsaid FG, Hafez EE (2011) Biochemical and molecular aspects of aluminium chloride-induced neurotoxicity in mice and the protective role of Crocus sativus L. extraction and honey syrup. Neuroscience 175:66–74. https://doi.org/10.1016/j.neuroscience.2010.11.043
Saiyed SM, Yokel RA (2005) Aluminium content of some foods and food products in the USA, with aluminium food additives. Food Addit Contam 22(3):234–244. https://doi.org/10.1080/02652030500073584
Ivanenko NB, Solovyev ND, Ivanenko AA, Ganeev AA (2012) Application of Zeeman graphite furnace atomic absorption spectrometry with high-frequency modulation polarization for the direct determination of aluminum, beryllium, cadmium, chromium, mercury, manganese, nickel, lead, and thallium in human blood. Arch Environ Contam Toxicol 63(3):299–308. https://doi.org/10.1007/s00244-012-9784-1
Ivanenko NB, Ivanenko AA, Solovyev ND, Zeimal AE, Navolotskii DV, Drobyshev EJ (2013) Biomonitoring of 20 trace elements in blood and urine of occupationally exposed workers by sector field inductively coupled plasma mass spectrometry. Talanta 116:764–769. https://doi.org/10.1016/j.talanta.2013.07.079
Drobyshev EJ, Solovyev ND, Ivanenko NB, Kombarova MY, Ganeev AA (2017) Trace element biomonitoring in hair of school children from a polluted area by sector field inductively coupled plasma mass spectrometry. J Trace Elem Med Biol 39:14–20. https://doi.org/10.1016/j.jtemb.2016.07.004
Valdman AV, Bondarenko NA, Kozlovskaya MM (1986) Psychotropic effect of Tuftsin, a natural phagocytosis-stimulating peptide, and some of its analogs. In: Valdman VA (ed) Drug dependence and emotional behavior: neurophysiological and neurochemical approaches. Springer, New York, pp 175–202. https://doi.org/10.1007/978-1-4684-1656-5_7
Grabovska S, Salyha Y (2015) ADHD-like behaviour in the offspring of female rats exposed to low chlorpyrifos doses before pregnancy. Arh Hig Rada Toksikol 66(2):121–127. https://doi.org/10.1515/aiht-2015-66-2624
Gu J (1997) Analytical morphology. Theory, applications and protocols. Birkhäuser Basel, Basel
Michalke B, Willkommen D, Drobyshev E, Solovyev N (2017) The importance of speciation analysis in neurodegeneration research. TrAC Trends Anal Chem:in Press. https://doi.org/10.1016/j.trac.2017.08.008
Solovyev ND, Ivanenko NB, Ivanenko AA (2011) Whole blood thallium determination by GFAAS with high-frequency modulation polarization Zeeman effect background correction. Biol Trace Elem Res 143(1):591–599. https://doi.org/10.1007/s12011-010-8865-0
Ivanenko NB, Solovyev ND, Ivanenko AA, Navolotskii DV (2014) Biological monitoring of arsenic pollution based on whole blood arsenic atomic absorption assessment with in situ hydride trapping. J Anal Atom Spectrom 29(10):1850–1857. https://doi.org/10.1039/c4ja00130c
Zubakina EA, Solovyev ND, Savinkova ES, Slesar NI (2016) Sample preparation for cadmium quantification in sunflower (Heliánthus ánnuus) seeds using anodic stripping voltammetry. Anal Methods 8(2):326–332. https://doi.org/10.1039/c5ay02275d
Cochran M, Coates JH, Elliott DC (1990) Aluminium interaction with macromolecules and membranes. In: de Broe ME, Coburn JW (eds) Aluminum and renal failure. Springer Netherlands, Dordrecht, pp 139–153. https://doi.org/10.1007/978-94-009-1868-9_10
Solovyev ND (2015) Importance of selenium and selenoprotein for brain function: from antioxidant protection to neuronal signalling. J Inorg Biochem 153:1–12. https://doi.org/10.1016/j.jinorgbio.2015.09.003
González-Domínguez R, García-Barrera T, Gómez-Ariza JL (2014) Characterization of metal profiles in serum during the progression of Alzheimer’s disease. Metallomics 6(2):292–300. https://doi.org/10.1039/c3mt00301a
Haroutunian V, Katsel P, Roussos P, Davis KL, Altshuler LL, Bartzokis G (2014) Myelination, oligodendrocytes, and serious mental illness. Glia 62(11):1856–1877. https://doi.org/10.1002/glia.22716
Exley C, House ER (2011) Aluminium in the human brain. Monatsh Chem 142(4):357–363. https://doi.org/10.1007/s00706-010-0417-y
Shirabe T, Irie K, Uchida M (2002) Autopsy case of aluminum encephalopathy. Neuropathology 22(3):5–210. https://doi.org/10.1046/j.1440-1789.2002.00432.x
Bhalla P, Singla N, Dhawan DK (2010) Potential of lithium to reduce aluminium-induced cytotoxic effects in rat brain. Biometals 23(2):197–206. https://doi.org/10.1007/s10534-009-9278-4
Somova LI, Missankov A, Khan MS (1997) Chronic aluminum intoxication in rats: dose-dependent morphological changes. Method Find Exp Clin 19(9):599–604
Yokel RA (2000) The toxicology of aluminum in the brain: a review. Neurotoxicology 21(5):813–828
Mizoroki T, Meshitsuka S, Maeda S, Murayama M, Sahara N, Takashima A (2007) Aluminum induces tau aggregation in vitro but not in vivo. J Alzheimers Dis 11(4):419–427. https://doi.org/10.3233/JAD-2007-11401
Nayak P, Chowdary NVS, Sharma SB (2015) Influence of prooxidant exposure on aluminum-induced alterations in open-field behavioral study in rats. Indian J Physiol Pharmacol 59(3):10
Mirshafa A, Nazari M, Jahani D et al (2017) Size-dependent neurotoxicity of aluminum oxide particles: a comparison between nano- and micrometer size on the basis of mitochondrial oxidative damage. Biol Trace Elem Res. https://doi.org/10.1007/s12011-017-1142-8
Wu X, Li J, Hu JN, Deng ZY (2012) The effects of glutamate and citrate on absorption and distribution of aluminum in rats. Biol Trace Elem Res 148(1):83–90. https://doi.org/10.1007/s12011-012-9345-5
Crepeaux G, Eidi H, David MO, Baba-Amer Y, Tzavara E, Giros B, Authier FJ, Exley C, Shaw CA, Cadusseau J, Gherardi RK (2017) Non-linear dose-response of aluminium hydroxide adjuvant particles: selective low dose neurotoxicity. Toxicology 375:48–57. https://doi.org/10.1016/j.tox.2016.11.018
Banks WA, Kastin AJ (1989) Aluminum-induced neurotoxicity: alterations in membrane function at the blood-brain barrier. Neurosci Biobehav Rev 13(1):47–53. https://doi.org/10.1016/S0149-7634(89)80051-X
Flarend RE, Hem SL, White JL, Elmore D, Suckow MA, Rudy AC, Dandashli EA (1997) In vivo absorption of aluminium-containing vaccine adjuvants using 26Al. Vaccine 15(12-13):1314–1318. https://doi.org/10.1016/S0264-410X(97)00041-8
Ray JG, Ghosh R, Mallick D, Swain N, Gandhi P, Ram SS, Selvaraj S, Rathore A, Mathummal S, Chakraborty A (2011) Correlation of trace elemental profiles in blood samples of Indian patients with leukoplakia and oral submucous fibrosis. Biol Trace Elem Res 144(1–3):295–305. https://doi.org/10.1007/s12011-011-9091-0
Wu Y, Yang X, Ge J, Zhang J (2011) Blood lead level and its relationship to certain essential elements in the children aged 0 to 14years from Beijing, China. Sci Total Environ 409(16):3016–3020. https://doi.org/10.1016/j.scitotenv.2011.04.050
Tokar EJ, Qu W, Person RJ, Ngalame ON, Waalkes MP (2015) Oxidative stress and the inorganic carcinogens. In: Roberts SM, Kehrer JP, Klotz L-O (eds) Studies on experimental toxicology and pharmacology. Humana Press, Cham, pp 323–334. https://doi.org/10.1007/978-3-319-19096-9
Frandsen A, Jensen JB, Schousboe A (2000) The role of second messengers in neurodegeneration. In: Reith MEA (ed) Cerebral signal transduction: from first to fourth messengers. Humana Press, Totowa, pp 207–220. https://doi.org/10.1007/978-1-59259-019-3_8
Michalke B, Halbach S, Nischwitz V (2009) JEM spotlight: metal speciation related to neurotoxicity in humans. J Environ Monit 11(5):939–954. https://doi.org/10.1039/b817817h
Solovyev N, Vinceti M, Grill P, Mandrioli J, Michalke B (2017) Redox speciation of iron, manganese, and copper in cerebrospinal fluid by strong cation exchange chromatography–sector field inductively coupled plasma mass spectrometry. Anal Chim Acta 973:25–33. https://doi.org/10.1016/j.aca.2017.03.040
Torres-Vega A, Pliego-Rivero BF, Otero-Ojeda GA, Gomez-Olivan LM, Vieyra-Reyes P (2012) Limbic system pathologies associated with deficiencies and excesses of the trace elements iron, zinc, copper, and selenium. Nutr Rev 70(12):679–692. https://doi.org/10.1111/j.1753-4887.2012.00521.x
Montgomery SC, Streit SM, Beebe ML, Maxwell PJ (2014) Micronutrient needs of the elderly. Nutr Clin Pract 29(4):435–444. https://doi.org/10.1177/0884533614537684
Nehls M (2016) Unified theory of Alzheimer’s disease (UTAD): implications for prevention and curative therapy. J Mol Psychiatry 4(1):3. https://doi.org/10.1186/s40303-016-0018-8
Roberts NB, Clough A, Bellia JP, Kim JY (1998) Increased absorption of aluminium from a normal dietary intake in dementia. J Inorg Biochem 69(3):171–176. https://doi.org/10.1016/S0162-0134(97)10015-0
Edwardson JA, Candy JM (1990) Aluminium and the pathogenesis of senile plaques: studies in Alzheimer’s disease and chronic renal failure. Environ Geochem Health 12(1):94–96. https://doi.org/10.1007/bf01734057
Gupta VB, Anitha S, Hegde ML, Zecca L, Garruto RM, Ravid R, Shankar SK, Stein R, Shanmugavelu P, Jagannatha Rao KS (2005) Aluminium in Alzheimer’s disease: are we still at a crossroad? Cell Mol Life Sci 62(2):143–158. https://doi.org/10.1007/s00018-004-4317-3
Acknowledgments
The authors are grateful to Maria A. Zaitseva and co-workers for the help with animal handling and Olga N. Gaikova for providing histological images.
Funding
N.D. Solovyev acknowledges the financial support of the Russian Foundation for Basic Research (grant No. 16-33-60004 mol_a_dk).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The study protocols were approved by Bioethics Committee of the Institute of Toxicology (protocol No. 8/16, dated 16.05.2016) and was conducted in accordance with the European Union law on the care and use of animals for scientific purposes.
Conflict of Interest
The authors declare that they have no conflict of interest.
Electronic Supplementary Material
ESM 1
(DOCX 4591 kb)
Rights and permissions
About this article
Cite this article
Drobyshev, E.J., Solovyev, N.D., Gorokhovskiy, B.M. et al. Accumulation Patterns of Sub-chronic Aluminum Toxicity Model After Gastrointestinal Administration in Rats. Biol Trace Elem Res 185, 384–394 (2018). https://doi.org/10.1007/s12011-018-1247-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12011-018-1247-8