Abstract
The present study was aimed to explore the potential of an antidepressant drug lithium (Li) in reducing aluminium (Al) induced neurotoxicity. To carry out the investigations, Al was administered orally (100 mg AlCl3/Kg b wt/day) whereas, Li was administered through diet (1.1 g Li2CO3/Kg diet, daily) for a total duration of 2 months. Al treatment resulted in a significant increase in the activity of enzyme nitric oxide synthase and the levels of l-citrulline which, however, were decreased appreciably following lithium supplementation. Al treatment also revealed an increase in DNA fragmentation as evidenced by an increase in number of comets. Interestingly, Li supplementation to Al treated rats reduced the damage inflicted on DNA by Al. Ultrastructural studies revealed an increase in chromatin condensation with discontinuity in nuclear membrane in both the cerebrum and cerebellum of Al treated rats which showed improvement following Li supplementation. Alterations in the structure of synapse and mitochondrial swelling were also seen. The present study shows the potential of Li in containing the damage inflicted by Al on rat brain.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Aluminium (Al) is one of the most abundant elements in the biosphere and causes adverse effects on various organs (Suwalsky et al. 2001; Reinke et al. 2003). Human population is constantly exposed to Al through various sources such as Al cooking utensils, certain beverages and drinking water (Gupta et al. 2005; Ochmanski and Barabasz 2000). High levels of Al have been linked with an increased risk of a number of pathogenic disorders such as microcytic anemia, osteomalacia as well as neurodegenerative disorders (Becaria et al. 2002; Solfrizzi et al. 2006; Santibáñez et al. 2007). Al-induced neurotoxicity is caused by various factors which include induction of nitric oxide, free radical-induced damage and neurotransmission alterations (Cordeiro et al. 2003; Kaizer et al. 2005). Both apoptosis and necrosis are suggested to be the mechanisms involved in cellular death resulting from Al toxicity (Brenner 2002). Suárez-Fernández et al. (1999) have reported DNA fragmentation and changes in nuclear morphology after Al exposure. Further, mutagenic effects of Al toxicity have also been observed by various researchers (Synzynys et al. 2004; Varella et al. 2004). Al-induced free radicals load may be responsible for initiating the process of apoptosis. Nitric oxide is one such free radical (Schmidt and Walter 1994) which apart from playing vital physiological functions (Garthwaite 1991; Lipton et al. 1993) also causes cytotoxic effects by reacting with superoxide anions (Estévez et al. 1995).
Various drugs/compounds have been examined for their role against aluminium-induced neurotoxicity in rat and mice models (Gong et al. 2005; Jyoti et al. 2007; Luo et al. 2007; Pan et al. 2008). In the recent studies, lithium has been shown to exert neuroprotective effects against various stimuli both in vitro and in vivo (Li et al. 2002; Yuan et al. 2004; Aghdam et al. 2007). Further, lithium has also been shown to inhibit cell death, DNA fragmentation and lipid peroxidation (Tandon et al. 1998; Shao et al. 2005). The present study was designed to explore further the potential of lithium in reducing cytotoxic effects induced by Al in rat brain.
Materials and methods
Animals
Sprague-dawley rats in the weight range of 130–150 g were obtained from the central animal house of Panjab University and were housed in polypropylene cages under hygiene conditions. The animals had free access to food and water throughout the treatment schedule. All the procedures were carried out in accordance with the ethical guidelines for care and use of laboratory animals, and protocols were approved by the institute’s ethical committee.
Treatments
Forty animals were randomly and equally segregated into four main groups.
Animals in group I-served as normal controls and were provided free access to water and diet.
Animals in group II were administered Al, in the form of aluminium chloride, everyday at a dose of 100 mg/kg b wt in drinking water through oral gavage (Nehru et al. 2007).
Animals in group III received Li in the form of lithium carbonate daily at a dose of 1.1 g/Kg in diet (Tandon et al. 2006).
Animals in group IV were given combined Al and Li treatments as were given to group II and group III animals, respectively.
All the treatments were continued for a total duration of 2 months. Lithium levels in the serum were also estimated by flame photometer and were found to be in the range of 0.6–0.8 mEq/l. At the end of treatment schedules, all the animals were sacrificed by decapitation immediately after anesthetization by diethyl ether. Brains were immediately removed, placed in ice-cold isotonic saline and dissected into two regions viz cerebrum and cerebellum. Tissue homogenates (10% w/v) were prepared in ice-cold 10 mM PBS (phosphate-buffered saline, 0.15 M NaCl), pH 7.4. The homogenates were centrifuged at 2,000g for 10 min at 4°C to remove the cell debris and nuclear pellets. The supernatants so obtained were again homogenized at 10,000g for 30 min. at 4°C to obtain post-mitochondrial supernatants (PMS). In the present study, PMS’ were used to carry out the estimations of nitric oxide synthase enzyme activity and l-citrulline levels.
Nitric oxide synthase
Nitric oxide synthase (NOS) activity was determined in terms of nitric oxide (NO) production by using the method described by Raddassi et al. (1994). NOS converts l-arginine to l-citrulline and NO which then reacts with oxygen to yield nitrite. Nitrite, thus formed reacts with the Griess reagent which produces color. To carry out the experiment, 0.1 ml of tissue homogenates, 0.1 ml of Griess reagent [(a) 0.1% solution of n-Napthyl ethylenediamine dihydrochloride prepared freshly in double distilled water (b) 1% Sulphanilamide prepared in 2.5% o-phosphoric acid solution, Mixed solution a and b in equal volume] were added into the wells of ELISA plate. The ELISA plate was then incubated in dark at 37°C for 30 min. The pink color so obtained was read at 540 nm on ELISA plate reader.
l-Citrulline
Estimation of l-citrulline was carried out by using the method of Boyde and Rahmatullah (1980). Determination of l-citrulline in proteins and peptides utilizes the reaction of ureido groups with doacetylmonoxime to give pink color after acid hydrolysis of proteins. To 0.1 ml of homogenates, 0.05 ml of zinc sulphate (30%) was added and the contents were mixed well to precipitate proteins. The tubes were then subjected to centrifugation at 10,000×g for 10 min. About 0.1 ml of supernatants were taken and 0.4 ml of 0.1N HCl were added followed by an addition of 1.5 ml of chromogenic solution [(a) 85% H3PO4 (b) 0.5% (w/v) diacetylmonoxime + 0.1% (w/v) thiosimocarbazide. Subsequently both a and b were mixed in the ratio 2:1]. After through mixing, the tubes were put in boiling water bath for 10 min. The tubes were then cooled at room temperature and the absorbance was measured against a reagent blank at 530 nm.
Protein estimation
The protein contents in the samples were measured by following the method of Lowry et al. (1951). For the assay of protein, 0.01 ml of sample, BSA standard (10–200 μg) and buffer (blank) were taken in respective tubes and the final volume was made to 0.5 ml with distilled water. About 5 ml of reagent (prepared by mixing 48 ml of 2% sodium carbonate, 1 ml of 1% copper sulphate and 1 ml of 2% potassium sodium tartarate) was then added. It was thoroughly mixed and allowed to stand for 10 min at room temperature. About 0.25 ml of 1N Folin’s reagent was added followed by immediate mixing. The contents were vigorously shaken and allowed to stand for 30 min at room temperature and the absorbance was measured at 680 nm.
Alkaline comet assay
Comet assay was performed according to the method of Singh et al. (1988). The assay works upon the principle that strand breakage of the supercoiled duplex DNA leads to the reduction of the size of the large molecule and these strands can be stretched out by electrophoresis. Briefly, 130 mg of brain tissue was homogenized in PBS (phosphate buffer saline with pH 7.4) using a tip homogenizer. The homogenate (80 μl) was then mixed with 100 μl of 1% low melting temperature agarose at 37°C and then placed on a slide pre-coated with thin layer of 1% regular melting agarose. It was immediately covered with coverslips and the slides were kept at 4°C for 45 min to allow solidification of the agarose. After removing the coverslips, the cells were lysed in a lysing solution (2.5 mM NaCl, 100 mM EDTA, 10 mM Tris base, 1% Triton-X-100 and 10% DMSO) for 1 h. After washing in double distilled water, the slides were placed in a horizontal gel electrophoresis chamber. The chamber was filled with cold alkaline buffer (300 mM NaOH, 1 mM EDTA with pH >13.0) and the slides were kept at 4°C for 20 min to allow the DNA to unwind. Electrophoresis was performed for 30 min (25 V/cm, 300 mA). After electrophoresis, the slides were washed three times with neutralization buffer (0.4 M Tris buffer with pH 7.5) for 5 min. All preparative steps were conducted in dark to prevent additional DNA damage. The slides were stained with ethidium bromide for 10 min and analyzed under a fluorescence microscope at 450× for comet assay using 550–560 nm excitations and 590 nm barrier filters.
DNA fragmentation studies
Tissue slices were placed in the digestion buffer (10 mM Tris–Cl with pH 8.0; 0.1 M EDTA with pH 8.0; 1% SDS and proteinase K with concentration of 1 mg/10 ml) and were incubated (14–18 h, 55°C) in a shaking water bath. The DNA contents were extracted, precipitated, and stored as described below for the analysis by agarose gel electrophoresis. After digestion, samples were extracted three times with 10% saturated phenol/chloroform/isoamyl alcohol (24:24:1) and were precipitated using ethanol. The precipitates were rinsed two times with 70% ethanol, air dried, and resuspended in Tris EDTA buffer. DNA contents were measured using a spectrophotometer (A260/A280), and only samples with 1.8 ratios were used. Agarose gel electrophoresis was then carried out to analyze the fragmentation.
Electron microscopic studies
Electron microscopic studies were also carried out to assess the effects of various treatments at the subcellular level. A very small portion of brain was incised out and immersion fixed in the fixative having formaldehyde and glutaraldehyde made in 0.2 M sodium cacodylate buffer (pH 7.2) for 4–5 h at 4°C. The specimens were then thoroughly washed thrice in 0.1 M cacodylate buffer and post fixed for 1 h in 1% osmium tetraoxide prepared in the same buffer. The specimens were then washed, dehydrated (in the ascending series of acetone), infiltered and subsequently embedded in resin. Specimen blocks were made out by polymerization of the pure embedding resin at 60°C for 48–72 h. Ultra thin sections were prepared using ultramicrotome. Initially, semi-thin sections of thickness about 1 μm were cut using very sharp glass knives to locate the area of interest in samples belonging to different treatment groups. These semi-thin sections were then stained with 0.5% toludine blue prepared in 1% borax solution. Ultrathin sections of interference colors from golden to silver were cut and loaded on fine copper grids of 100–300 mesh size. Sections were double stained with uranyl acetate and lead citrate. These ultrathin sections were finally viewed under transmission electron microscope at AIIMS, New Delhi.
Aluminium estimation
Al levels were also determined in cerebrum and cerebellum by wet acid digestion method of Zumkley et al. (1979) using the Atomic Absorption Spectrophotometer (Perkin Elmer, India).
Statistical analysis
The statistical significance of the data has been determined using one-way analysis of variance (ANOVA) followed by multiple post-hoc test (Student–Newman–Keuls).
Chemicals
Aluminium chloride and lithium carbonate were procured from CDH (Central Drug House) Chemicals Ltd, New Delhi, India. All other chemicals were of high analytical grade.
Results
Table 1 show the body and brain weights of the normal control and treated animals. A significant decrease (P ≤ 0.001) in the body and brain weights was observed after Al treatment as compared to normal control animals. Lithium treatment alone did not cause any significant change in the body and brain weights of the animals when compared with normal control animals. Whereas, lithium co-administration with Al was able to check the weight loss and both the body and brain weights were found to be significantly improved (P ≤ 0.01) when compared to Al treated group.
The diet consumption in normal and rats subjected to different treatments varied between 5 and 8 g per day per rat throughout the period of study.
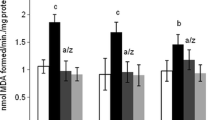
The nitric oxide synthase enzyme activity was measured by estimating the levels of nitric oxide and was found to be significantly increased (P ≤ 0.001) in both the regions after Al treatment in comparison to normal control animals (Table 2). Similarly, an increase in the levels of l-citrulline levels was also seen in both the cerebrum (P ≤ 0.001) and cerebellum (P ≤ 0.01) when compared to normal controls (Table 3). Lithium supplementation to Al treated animals significantly decreased the enzyme activity as well as the levels of l-citrulline when compared to Al treated animals, however, the enzyme activity was significantly high in both the cerebrum (P ≤ 0.05) and cerebellum (P ≤ 0.01) in comparison to normal controls. No significant change in the enzyme activity as well as in l-citrulline levels were observed in animals given only lithium treatment.
The DNA damage caused in the cell as a result of Al treatment was examined by single cell gel electrophoresis (comet assay) (Table 4). The results indicated that the DNA of Al treated cell showed a comet tail indicating the DNA damage arising from the genotoxicity in the Al treated cell as compared to DNA of normal cell. The average % of DNA damage in the Al treated group was 70% as compared to normal control (28%). In the combined treatment group, damage to DNA was appreciably less (42%) as compared to Al treated rats.
As shown in Fig. 1, fragments of DNA were observed in Al treated animals (Lane 2) as compared to normal control animals (Lane 1). However, no significant fragmentation could be observed in Al treatment animals which were simultaneously subjected to lithium treatment (Lane 4).
A significant increase in the levels of Al was observed in both the regions after Al treatment in comparison to normal controls. In the combined treatment group, Al levels were significantly decreased when compared with Al treated animals. However, the Al levels were significantly high in cerebrum (P ≤ 0.01) when compared to normal animals (Table 5).
Figure 2a shows the rat cerebrum from the normal rat with a well defined nucleus and nucleolus. Myelin sheath as well as the nuclear membrane can also be clearly seen. Figure 3a shows the effect of Al treatment at the subcellular level. An increase in the chromatin condensation was observed along with the discontinuity of nuclear membrane. Vacuoles and mitochondrial swelling can also be seen. No change at the cellular level was visible after treatment with lithium (Fig. 4a). However, in the combined treatment group, a decrease in the chromatin condensation was observed and the continuity of nuclear membrane was also seen (Fig. 5a).
a Electron micrograph from control rat showing a portion of cerebrum from frontal part with a well defined nucleus (1) and nucleolus (2) and mylinated nerve fibers (3). b Electron micrograph from control rat showing a portion of cerebellum dendrite (1), sine and synapse (2) as well as mitochondria (3)
Figure 2b shows the portions of cerebellum from normal control animal with a nucleus, dendrites, synapse point and a number of mitochondria. Chromatin condensation along with the disruption of synapse structure was observed in cerebellum after Al treatment (Fig. 3b). A curvature could be observed at synapse. No change at the cellular level was visible in cerebellum after lithium treatment (Fig. 4b). Lithium co-treatment with Al significantly decreased the chromatin condensation in cerebellum also, as compared to Al treated animals (Fig. 5b).
Discussion
Exposure to heavy metals cast a shadow of great concern as heavy metals are associated with the etiology of various diseases. Amongst the list of metals, adverse effects caused by Al exposure are a matter of great concern and investigations are warranted so as to contain them. Thus, in the present study, the effects of Al alone or in combination with lithium at a cellular level in brain were examined. Al exposure resulted in a significant decrease in the body and brain weights. Similar results were also observed by earlier researchers (Ondreicka et al. 1996; Baydar et al. 2003; Azzaoui et al. 2008). Baydar et al. (2003) have attributed the decrease in body weights to the interference of Al with the hormonal status and/or protein synthesis. In our study, as we did not observe any appreciable change in the diet consumption of the rats subjected to Al treatment so it can be anticipated that this effect could possibly be due to increased peroxidation of lipids as a consequence of oxidative stress in the animals following Al treatment, which has also been pointed out in our earlier studies (Bhalla and Dhawan 2009). Further, inhibition in the glycolytic pathway would also result in decreased body weights as in such toxic conditions there is an enhanced synthesis of glucose from non-exhausted carbohydrate sources thereby leading to mobilization of fat deposits resulting in decreased body weights. Lithium co-administration was, however, able to restore the body weight loss and a recovery in the weights could be seen. Lithium administration has been shown to cause increase in body weights (Canolty and Johnson 1987; Geoffroy et al. 1991) and moreover lithium therapy has been shown to decrease lipid peroxidation which may result in an improvement in body weights.
Nitric oxide is a known signaling molecule and its actions are the result of its influence on a variety of protein functions (Jaffrey et al. 2001; Lane et al. 2001). Nitric oxide along with l-citrulline are the principal products of nitric oxide synthase (NOS) enzyme activity (Griffith and Stuehr 1995; Chinje and Startford 1997). In the present study, an increase in the levels of nitrite and l-citrulline were observed following Al exposure in both cerebrum and cerebellum (Tables 2, 3). Increase in nitrite levels signifies an increase in nitric oxide production. Similar increase was also observed in an earlier study by Satoh et al. (2007). Acute and chronic exposure to Al stimulates nitric-oxide synthase activity mostly present in glial cells whose contribution to the total activity is around 70% under resting conditions (Bondy et al. 1998). NOS is found to coexist with neurofibrillary tangle bearing neurons (Smith et al. 1997, 1998) and thus signifies the importance of nitric oxide in Alzheimer’s disease where Al-induced neurotoxicity is also one of the causative factor. Nitric oxide is a well known free radical (Schmidt and Walter 1994) and after reacting with superoxide anion radials forms peroxynitrite (Estévez et al. 1995) which then adversely acts on various macromolecules. Further, an important regulator of NOS activity is free Ca2+ which via calmodulin can activate the NOS enzyme activity and thus leads to the increased amount of NO (Esplugues 2002). Al toxicity has been reported to cause an increase in calcium levels (Kaur and Gill 2005). The increased amount of Ca2+ will bind to calmodulin, which further gets associated with NOS and activates the enzyme thus leading to the increased production of NO in brain regions. Co-administration of lithium was able to decrease the levels of nitric oxide and l-citrulline in both the regions. Studies have shown that antidepressant activity of lithium is mediated through the regulation of nitric oxide levels. Thus, lithium treatment is able to regulate the nitro stress induced by Al toxicity in brain.
Effects of Al toxicity on DNA were also investigated. Al treatment caused an increased DNA damage as indicated by the increased fragmentation of DNA and the number of comets observed. DNA fragmentation and increase in the appearance of comets have also been reported in other studies as a consequence of Al exposure (Lima et al. 2007). Al is known to increase the levels of reactive oxygen species (Bondy and Kirstein 1996; Bondy et al. 1998) as well as nitrogen species as seen in the present study also, which are known to cause damage to various macromolecules and also to DNA. An increase in the Al levels was also observed, which may result in more production of free radicals and thus contribute to the cytogenetic effects resulting from Al toxicity. Damage to DNA is one of the markers and typical characteristic of apoptosis (Wyllie 1993) and the present study shows that Al toxicity can lead to faster apoptosis as seen in the electron micrographs which clearly revealed disruption of cells. Lithium, on the other hand revealed neuroprotective effects as evidenced by decreased DNA damage in the combined treatment group. A similar inhibition of DNA fragmentation was observed in primary cultured rat cerebral cortical cells (Shao et al. 2005) after lithium treatment. Studies have shown that lithium significantly reduces cytochrome c release, which is a key initial event in apoptosis (Lai et al. 2006) and also inhibits DNA fragmentation (Ghribi et al. 2002) thus showing anti-apoptotic properties, which is further strengthened by the present study. Further, lithium has been shown to possess antioxidative properties (Tandon et al. 1998; Schafer et al. 2004) and hence may decrease the levels of free radicals and ultimately the damage to DNA.
In microscopic observations, disruption at the cellular level was seen after Al treatment thus indicating its adverse effects at the histoarchitecture level. Chromatin condensation (Fig. 3a, b) in both the cerebrum and cerebellum can be seen. Jyoti et al. (2007) have also observed similar changes at the cellular level after Al treatment. Changes in the structure of synapse was also seen after Al treatment, which may affect neurotransmission and hence learning and memory processes in rats and the same is also observed in a number of studies (Rifat et al. 1990; Hänninen et al. 1994; Amador et al. 2001). Al has been shown to alter the cholesterol, phospholipids, total lipids contents of the membranes and thus may be responsible for the membrane damage as seen in an earlier study from our lab (Bhalla et al. 2009). Lithium co-administration proved beneficial and is supported by the fact that in combined treatment group an appreciable improvement was seen in structure of both the regions (Fig. 5a, b). Lithium significantly reduced the levels of ROS thereby preventing lipid peroxidation, composition and fluidity of the membranes which may account for the structural improvement as seen in the present study.
The present study thus shows the protective effects of lithium by containing the cytotoxic effects inflicted by Al.
References
Aghdam Y, Barger S, Steven W (2007) Glycogen synthase kinase-3 in neurodegeneration and neuroprotection: lessons from lithium. Curr Alzheimer Res 4(1):21–31 (11)
Amador FC, Santos MS, Oliveira CR (2001) Lipid peroxidation and aluminium effects on the cholinergic system in nerve terminals. Neurotox Res 3(3):223–233
Azzaoui FZ, Ahami AO, Khadmaoui A (2008) Impact of aluminum sub-chronic toxicity on body weight and recognition memory of wistar rat. Pak J Biol Sci 11(14):1830–1834
Baydar T, Papp A, Aydin A, Nagymajtenyi L, Schulz H, Isimer A, Sahin G (2003) Accumulation of aluminum in rat brain: does it lead to behavioral and electrophysiological changes? Biol Trace Elem Res 92(3):231–244
Becaria A, Campbell A, Bondy SC (2002) Aluminum as a toxicant. Toxicol Ind Health 18(7):309–320
Bhalla P, Dhawan DK (2009) Protective role of lithium in ameliorating the aluminium-induced oxidative stress and histological changes in rat brain. Cell Mol Neurobiol 29(4):513–521
Bhalla P, Nair P, Garg ML, Dhawan DK (2009) Effects of lithium on membrane fluidity and lipid profile in brain membranes of aluminium treated rats. Toxicol Environ Chem 1029-0486 91(4):723–733
Bondy SC, Kirstein S (1996) The promotion of iron-induced generation of reactive oxygen species in nerve tissue by aluminium. Mol Chem Neuropathol 27:185–194
Bondy SC, Liu D, Guo-Ross S (1998) Aluminum treatment induces nitric oxide synthase in the rat brain. Neurochem Int 33:51–54
Boyde TRC, Rahmatullah M (1980) Optimization of conditions for the colorimetric determination of citrulline, using diacetyl monoxime. Analytical Biochem J 107:424–431
Brenner S (2002) Aluminum neurotoxicity is reduced by dantrolene and dimethyl sulfoxide in cultured rat hippocampal neurons. Biol Trace Elem Res 86(1):85–89
Canolty NL, Johnson MA (1987) Effects of increasing dietary lithium carbonate on weight and mineral contents of tissues from weanling rats. Fed Proc 46:906
Chinje EC, Startford IJ (1997) Role of nitric oxide in growth of solid tumors: a balancing act. Essays Biochem 32:61–72
Cordeiro JM, Silva VS, Oliveira CR, Gonçalves PP (2003) Aluminium-induced impairment of Ca2+ modulatory action on GABA transport in brain cortex nerve terminals. J Inorg Biochem 15, 97(1):132–142
Esplugues JV (2002) NO as a signalling molecule in the nervous system. Br J Pharmacol 135(5):1079–1095
Estévez AG, Radi R, Barbeito L, Shin JT, Thompson JA, Beckman JS (1995) Peroxynitrite-induced cytotoxicity in PC12 cells: evidence for an apoptotic mechanism differentially modulated by neurotrophic factors. J Neurochem 65(4):1543–1550
Garthwaite J (1991) Glutamate, nitric oxide and cell-cell signalling in the nervous system. Trends Neurosci 14(2):60–67
Geoffroy M, Tvede K, Christensen AV, Schou JS (1991) The effect of impramine and lithium on “learned helplessness and acetylcholinestsrase in rat brain”. Pharmacol Biochem Behav 38(1):93–97
Ghribi O, Herman MM, Spaulding NK, Savory J (2002) Lithium inhibits aluminum-induced apoptosis in rabbit hippocampus, by preventing cytochrome c translocation, Bcl-2 decrease, Bax elevation and caspase-3 activation. J Neurochem 82(1):137–145
Gong QH, Wu Q, Huang XN, Sun AS, Shi JS (2005) Protective effects of Ginkgo biloba leaf extract on aluminum-induced brain dysfunction in rats. Life Sci 77(2):140–148
Griffith OW, Stuehr DJ (1995) Nitric oxide synthetase: Properties and catalytic mechanism. Ann Rev Physiol 57:707–736
Gupta VB, Anitha S, Hegde ML, Zecca L, Garruto RM, Ravid R, Shankar SK, Stein R, Shanmugavelu P, Jagannatha Rao KS (2005) Aluminium in Alzheimer’s disease: are we still at a crossroad? Cell Mol Life Sci 62(2):143–158
Hänninen H, Matikainen E, Kovala T, Valkonen S, Riihimäki V (1994) Internal load of aluminum and the central nervous system function of aluminum welders. Scand J Work Environ Health 20(4):279–285
Jaffrey SR, Erdjument-Bromage H, Ferris CD, Tempst P, Snyder SH (2001) Protein S-nitrosylation: a physiological signal for neuronal nitric oxide. Nat Cell Biol 3:193–197
Jyoti A, Sethi P, Sharma D (2007) Bacopa monniera prevents from aluminium neurotoxicity in the cerebral cortex of rat brain. J Ethnopharmacol 111(1):56–62
Kaizer RR, Corrêa MC, Spanevello RM, Morsch VM, Mazzanti CM, Gonçalves JF, Schetinger MR (2005) Acetylcholinesterase activation and enhanced lipid peroxidation after long-term exposure to low levels of aluminum on different mouse brain regions J. Inorg Biochem 99(9):1865–1870
Kaur A, Gill KD (2005) Disruption of neuronal calcium homeostasis after chronic aluminium toxicity in rats. Basic Clin Pharmacol Toxicol 96(2):118–122
Lai JS, Zhao C, Warsh JJ, Li PP ( 2006) Cytoprotection by lithium and valproate varies between cell types and cellular stresses. Eur J Pharmacol 539 (1–2):18–26
Lane P, Hao G, Gross SS (2001) S-nitrosylation is emerging as a specic and fundamental posttranslational protein modication: head to head comparison with O-phosphorylation. Sci SKTE 86:1–9
Li X, Bijur GN, Jope RS (2002) Glycogen synthase kinase-3β, mood stabilizers, and neuroprotection. Bipolar Disord 4:137–144
Lima PDL, Leite DS, Vasconcellos MC, Cavalcanti BC, Santos RA, Costa-Lotufo LA, Pessoa C, Moraes MO, Burbano RR (2007) Genotoxic effects of aluminum chloride in cultured human lymphocytes treated in different phases of cell cycle. Food Chem Toxicol 45:1154–1159
Lipton SA, Choi YB, Pan ZH, Lei SZ, Chen HS, Sucher NJ, Loscalzo J, Singel DJ, Stamler JS (1993) A redox-based mechanism for the neuroprotective and neurodestructive effects of nitric oxide and related nitroso-compounds. Nature 364(6438):626–632
Lowry OH, Rosebrough NJ, Farr AL, Ranell RJ (1951) Protein measurements with the Follin’s phenol reagent. J Biol Chem 193:265–275
Luo Y, Nie J, Gong QH, Lu YF, Wu Q, Shi JS (2007) Protective effects of icariin against learning and memory deficits induced by aluminium in rats. Clin Exp Pharmacol Physiol 34(8):792–795
Nehru B, Bhalla P, Garg A (2007) Further evidence of centrophenoxine mediated protection in aluminium exposed rats by biochemical and light microscopy analysis. Food Chem Toxicol 45(12):2499–2505
Ochmanski W, Barabasz W (2000) Aluminium-occurance and toxicity for organisms. Przegl Lek 57:665–668
Ondreicka R, Ginter E, Kortus J (1996) Chronic toxicity of aluminium in rats and mice and its effects on phosphorous metabolism. Br J Ind Med 23:305–312
Pan R, Qiu S, Lu DX, Dong J (2008) Curcumin improves learning and memory ability and its neuroprotective mechanism in mice. Chin Med J (Engl) 121(9):832–839
Raddassi K, Berthon B, Petit JF, Lemaire G (1994) Role of calcium in the activation of mouse peritoneal macrophages: induction of NO synthase by calcium ionophores and thapsigargin. Cell Immunol 53:443–455
Reinke CM, Breitkreutz J, Leuenberger H (2003) Aluminium in over-the-counter drugs: risks outweigh benefits? Drug Saf 26(14):1011–1025
Rifat SL, Eastwood MR, McLachlan DR, Corey PN (1990) Effect of exposure of miners to aluminium powder. Lancet 336(8724):1162–1165
Santibáñez M, Bolumar F, García AM (2007) Occupational risk factors in Alzheimer’s disease: a review assessing the quality of published epidemiological studies. Occup Environ Med 64(11):723–732
Satoh E, Yasuda I, Yamada T, Suzuki Y, Ohyashiki T (2007) Involvement of NO Generation in Aluminum-Induced Cell Death Biol. Pharm Bull 30(8):1390–1394
Schafer M, Goodenough S, Moosmann B, Behl C (2004) Inhibition of glycogen synthase kinase 3 beta is involved in the resistance to oxidative stress in neuronal HT22 cells. Brain Res 1005:84–89
Schmidt HH, Walter U (1994) NO at work. Cell 78:919–925
Shao L, Young LT, Wang JF (2005) Chronic treatment with mood stabilizers lithium and valproate prevents excitotoxicity by inhibiting oxidative stress in rat cerebral cortical cells, Biol. Psychiatry 58:879–884
Singh NP, Mccoy MT, Tice RR, Schneider ELA (1988) Single technique for quantitation of low levels of DNA damage in individual cells. Exp Cell Res 175:184–191
Smith MA, Richey Harris PL, Sayre LM, Beckman JS, Perry G (1997) Widespread peroxynitrite-mediated damage in Alzheimer’s disease. J Neurosci 17(8):2653–2657
Smith MA, Vasák M, Knipp M, Castellani RJ, Perry G (1998) Dimethylargininase, a nitric oxide regulatory protein, in Alzheimer disease. Free Radic Biol Med 25(8):898–902
Solfrizzi V, Colacicco AM, D’Introno A, Capurso C, Parigi AD, Capurso SA, Torres F, Capurso A, Panza F (2006) Macronutrients, aluminium from drinking water and foods, and other metals in cognitive decline and dementia. J Alzheimers Dis. 10(2–3):303–330
Suárez-Fernández MB, Soldado AB, Sanz-Medel A, Vega JA, Novelli A, Fernández-Sánchez MT (1999) Aluminum-induced degeneration of astrocytes occurs via apoptosis and results in neuronal death. Brain Res 835(2):125–136
Suwalsky M, Ungerer B, Villena F, Norris B, Cardenas H, Zatta P (2001) Effects of AlCl3 on toad skin, human erythrocytes, and model cell membranes. Brain Res Bull 55:205–210
Synzynys BI, Sharetskii AN, Kharlamova OV (2004) Immunotoxicity of aluminum chloride. Gig Sanit 4:70–72
Tandon A, Dhawan DK, Nagpaul JP (1998) Effect of lithium on hepatic lipid peroxidation and antioxidative enzymes under different dietary protein regimens. J Appl Toxicol 18:187–190
Tandon A, Bhalla P, Nagpaul JP, Dhawan DK (2006) Effect of lithium on rat cerebrum under different dietary protein regimens. Drug Chem Toxicol 29:333–344
Varella SD, Pozetti GL, Vilegas W, Varanda EA (2004) Mutagenic activity in waste from an aluminum products factory in Salmonella/microsome assay. Toxicol In Vitro 18:895–900
Wyllie AH (1993) Apoptosis (The 1992 Frank Rose memorial lecture). Br J Cancer 67:205–208
Yuan P, Gould TD, Gray NA, Bachmann RF, Schloesser RJ, Lan MJK, Du J, Moore GJ, Manji HK (2004) Neurotrophic signaling cascades are major long-term targets for lithium: clinical implications. Clin Neurosci Res 4:137–153
Zumkley H, Bertram HP, Lison A, Knoll O, Losse H (1979) Al, Zn and Cu concentrations in plasma in chronic renal insufficiency. Clin Nephrol 12:18–21
Acknowledgment
The work was supported by the Department of Biophysics, Panjab University, Chandigarh, India.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bhalla, P., Singla, N. & Dhawan, D.K. Potential of lithium to reduce aluminium-induced cytotoxic effects in rat brain. Biometals 23, 197–206 (2010). https://doi.org/10.1007/s10534-009-9278-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10534-009-9278-4