Abstract
Patients diagnosed with stage I non-seminomatous germ cell tumor (NSGCT) face the task of selecting a management strategy. Whereas these options all offer excellent survival, unfortunately, each has drawbacks. Retroperitoneal lymph node dissection (RPLND) is a major operation with low, but significant risks of bleeding, chylous ascites, and retrograde ejaculation. Platinum-based chemotherapy is associated with a number of long-term side effects, not all of which are quantified, but include secondary malignancy and early cardiovascular disease. While surveillance minimizes the chances of exposure to unnecessary treatment, it is not infrequently salvaged with chemotherapy and requires a compliant patient willing to undergo serial imaging often with ionizing radiation. Although fewer than one-third of patients will relapse without intervention, the current guidelines propose treatment for stage I patients with high-risk features. New developments in minimally invasive techniques may mitigate the harms of RPLND and avoid the side effects of chemotherapy, making it an ideal option for this cohort of patients. Unlike laparoscopic RPLND, which was introduced as a staging procedure and heavily criticized for the advanced skill set required to achieve oncologic equivalence, robotic RPLND may offer the benefits of a minimally invasive technique without a steep learning curve and a true therapeutic operation in experienced hands.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Germ cell tumors (GCTs) comprise 95 % of malignant neoplasms arising in the testicle and are the most common solid tumor found in men aged 20 to 34 years [1, 2]. In fact, the incidence of testicular GCTs is increasing [3–6]. Fortunately, only 10–30 % of men will present with distant disease [7]. GCTs can be further classified as seminoma or nonseminoma, which differ in terms of histology, serum tumor markers, metastatic potential, and management options [1]. For instance, non-seminomatous GCTs (NSGCTs) are believed to be more aggressive and are often treated with chemotherapy or surgery, while seminomas are often effectively treated with chemo- or radiotherapy [1]. For patients with clinical stage I NSCGTs, there are three main treatment options to consider: surveillance, platinum-based chemotherapy, and retroperitoneal lymph node dissection (RPLND) [1, 8].
Today, laparoscopic and robotic RPLND (L-RPLND, R-RPLND) are both options for minimally invasive management of stage I NSCGTs and are offered primarily in high-volume academic centers. While proponents hope to distinguish robotic RPLND as superior to laparoscopy, even if only in terms of the requisite learning curve, limited data exist to support this claim. In the following review, we describe the available published outcomes of R-RPLND that exist to date.
RPLND Versus Surveillance
For those considering surveillance as a management option, the risk of recurrence is a major concern. A contemporary surveillance cohort revealed a 5-year relapse rate of 30.6 % [9•]. Further, for patients without known high-risk features such as lymphovascular invasion (LVI), the recurrence rate was only 12 % [9•, 10]. Based on these outcomes, the authors promote surveillance to avoid overtreatment for the majority of patients. Yet, others interpret the numbers differently and recommend primary treatment with RPLND to provide definitive pathology and avoid salvage chemotherapy (see below for discussion on chemotherapy).
There are a number of benefits to primary RPLND in the management of clinical stage I NSGCT. These include local control of the retroperitoneum, complete staging, and removal of any chemo-resistant tumor elements. Traditionally, primary RPLND is performed through an open, midline approach. The risk of abdominopelvic recurrence after primary RPLND is extremely low (2 %) when done at an experienced center, and while recurrent cancer is effectively salvaged with chemotherapy, cure rates are high for patients with N1 disease without chemotherapy [11]. Downsides include peri- and post-operative complications and ejaculatory dysfunction due to injury to the sympathetic nerves as they course around the great vessels. In centers of excellence, the risks of excessive blood loss, bowel obstruction (1 %), chylous ascites (0.4 %), other visceral injuries, and long-term convalescence can be minimized [11, 12, 13•, 14–17]. In addition, template-based and nerve-sparing techniques preserve antegrade ejaculation in approximately 75 and 90 % of men, respectively [11, 12]. This involves active identification of the sympathetic chain and hypogastric plexus and avoiding electrocautery in these areas [18].
Furthermore, proponents note that criticisms of open RPLND derive primarily from historical complication data. One contemporary 2014 series of open RPLND reported a complication rate of just 9 % and length of stay (LOS) of only 4 days [19]. What is clear is that if the complications of surgical management could be minimized, this would obviate much of the discussion on the optimal modality for stage I non-seminomas. Laparoscopic RPLND was introduced to accomplish this, citing small incisions, shorter hospital stay, and decreased blood loss, but initially faced heavy criticism as oncologically inferior [20].
Surveillance does offer an excellent survival outcome for clinical stage I NSGCTs, exceeding 95 % [21]. The problem is that many patients on surveillance do go on to progress and then may suffer the side effects of chemotherapy. Recently published 5-year progression-free survival rates were 74.1 % for surveillance, as compared to 92.3 % for chemotherapy, and 100 % for RPLND [10]. In this series, risk factors for progression on multivariable analysis included patient age, cryptorchidism, and LVI. Interestingly, a 2011 SEER population study found the use of RPLND for stage I NSGCTs had decreased over time from 39 % in 1988–1995 to 18 % in 2004–2006 [22]. This may be secondary to the preference for surveillance for stage IA disease based upon the most recent NCCN guidelines [1].
While surveillance avoids overtreatment for many patients, it necessitates a significant radiation burden due to follow-up imaging. The current NCCN guidelines call for a total of nine abdominal (plus minus pelvic) CTs over 4 years of surveillance for stage IB [1]. Looking at this, a 2009 study compared the surveillance protocol to the radiation of a single scan after RPLND [23]. Strikingly, they found that the relative risk of a secondary malignancy is 15.2, with a lifetime cancer risk of 1–2 %. More recently, a study from Columbia University revealed that this is still a problem, finding that in excess of 75 % of testicular cancer patients in surveillance for 5 years exceeded standard safety limits for radiation exposure [24]. Additionally, compliance with frequent follow-up may be an issue in this young and often mobile population of patients.
RPLND Versus Chemotherapy
In general, GCTs are very susceptible to platinum-based chemotherapy, making this a useful management option to have available, especially for patients with advanced disease [25]. However, as previously stated, stage I NSGCTs are associated with excellent survival in excess of 95 % [21]. Chemotherapy has many serious negative consequences, which is the reason why many in the United States feel it is inappropriate for stage I disease and why it is not an option for stage IA disease according to the NCCN guidelines [1]. Specifically, there are associations with secondary malignancies and cardiac risks [23, 26]. In fact, a quarter of patients treated with cisplatin-based chemotherapy will have sub-clinically impaired renal function, and in one study, a statistically significant 2.59 (95 % CI 1.15 to 5.84; P = .022) relative risk of having a cardiac event [26, 27]. Furthermore, patients with the teratoma subtype of NSGCT will receive no benefit from chemotherapy, due to its chemo-resistant nature [28]. Notably, there is some evidence that chemotherapy may be superior to RPLND. One study randomnized clinical stage I NSCGT patients to one cycle of chemotherapy versus RPLND, and they found a statistically significant improvement in 2-year recurrence-free survival from 91.87 % with RPLND to 99.46 % for chemotherapy [29].
Laparoscopic RPLND
At its inception, L-RPLND was very controversial, and in early adaptations, this technique was used simply as a staging procedure [30, 31]. There was no retrocaval or retroaortic dissection, and the case was often aborted if disease was encountered [28, 30–32]. Over time, this changed, and the goal of L-RPLND was to perform an oncologically equivalent dissection to its open counterpart [28, 33, 34]. There have been no randomized controlled trials of open versus L-RPLND, yet in many retrospective series, the minimally invasive method has been shown to offer a shorter hospital stay, less blood loss, and shorter convalescence [16, 20, 28, 35–38] Table 1.
One systematic review of L-RPLND included more than 800 patients from 34 series spanning 1992–2008, with 63-month follow-up. The complication rate was 15.6 %, with 2 % retrograde ejaculation. In fact, OR time was longer than open RPLND, at 204 min (versus 186 min, P < 0.05). They found no difference in oncologic outcomes compared to open surgery, with local relapse of 1.4 % and distant relapse rate 3.3 % [14]. Yet, critics say that contemporary open series have similar outcomes, with one group demonstrating a 7 % complication rate for primary RPLND, with operative time 188 min [20]. Other comparisons investigated in the metaanalysis include length of stay, which was shorter at 3.3 days for laparoscopic vs 6.6 days for open surgery, and on sub-analysis of the most contemporary series, laparoscopic patients required 33–50 % less analgesic than their open surgery counterparts [14].
Robotic RPLND
Robotic RPLND was first described in a case report from 2006 [39]. Since, the body of literature encompasses several small case-series (Table 1). An early three-patient series published in 2011 by Williams et al. reported a 2-day length of stay, zero perioperative complications, and lymph node count of 25 [19]. As was the case for laparoscopic RPLND, the first major hurdle to overcome for the robotic modality is demonstrating equivalence. In 2015, Harris et al. published the first comparative analysis of robotic and laparoscopic RPLND to evaluate perioperative outcomes and safety [40••]. In this single-surgeon series of 16 R-RPLND and 21 L-RPLND, equivalence was found in terms of operative time, blood loss, lymph node yield, and ejaculatory status [24]. Still, it remains to be demonstrated that R-RPLND offers a specific benefit over L-RPLND.
Most notably, a recent multi-institutional experience combining data from four centers was presented, with a total of 56 patients [41••]. Estimated blood loss was only 50 mL, and median length of stay was just one day. There was one open conversion (2 %) and a 9 % perioperative complication rate. Antegrade ejaculation was preserved in 96 % of patients. Importantly, this series also contains oncologic outcomes: With 15-month median follow-up, the recurrence-free rate was 98 %.
While direct comparative evidence across modalities is limited, proponents of R-RPLND would put forth that it offers the benefits of minimally invasive surgery without demanding an advanced skill set. In the first report of R-RPLND by Davol et al. in 2006, the authors justified their novel approach by citing the advanced skill set necessary to adequately perform an L-RPLND, and need for alternatives [39]. In general, it is accepted that robotic surgery has a faster learning curve than laparoscopic surgery [42]. Still, any RPLND represents a challenging operation that should be performed in high-volume centers of excellence for optimal results. In addition to primary RPLND, post-chemotherapy RPLND is another arena where robotic RPLND is emerging. Though expected to be technically more difficult, post-chemotherapy R-RPLND is feasible. From the Mayo Clinic, a series of 18 patients had zero major complications, and 15 of 18 were able to be completed robotically [13•].
With increasing scrutiny of health care spending, a cost comparison of surgical modalities is prudent. While information specific to RPLND is limited, this topic has recently been addressed in the setting of robotic nephrectomy. One group performed model-based cost analysis, assuming 55 % higher costs for patients who suffered surgical complications related to open surgery [43]. With this assertion, robot-assisted partial nephrectomy was cost-effective by virtue of its ability to prevent additional complications. Separately, a more concrete analysis was performed based on the Maryland Health Services Cost Review Commission total hospital charge to patients [44]. Interestingly, robotic partial nephrectomy was less expensive than laparoscopic partial, while robotic radical was more costly than laparoscopic partial. Granularly, savings for robotic partial nephrectomy were due to decreased room and board charges. More study is needed specifically for RPLND, but clearly length of stay and complication rate are important drivers of cost, which may offset the price tag of newer surgical technologies.
Robotic RPLND Technique
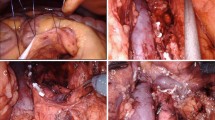
At our institution, a transperitoneal approach is performed, and nerve-sparing is based upon surgeon preference. A modified node dissection template is used as previously described [12, 45–47]. Ports include a 12-mm camera port, three robotic ports, and additional ports for liver retraction and the assistant. Two positioning methods are used, dorsal lithotomy and flank position with a slightly flexed bed. For dorsal lithotomy, the patient is placed in Trendelenburg, and the robot is docked over the left shoulder. First, the colon is mobilized, and a two hitch stitches are used to tack the peritoneum to the anterior abdominal wall, exposing the retroperitoneum. For the nodal dissection, the superior border is the renal hilum and laterally, the ureter. The gonadal vein is also removed. For left templates, separate nodal packets removed include the left common iliac, pre-aortic, para-aortic, and retroaortic. Occasionally, interaortocaval nodes are removed. For right templates, right common iliac, paracaval, precaval, retrocaval, interaortocaval, and pre-aortic nodes are sent separately.
Conclusion
Patients with clinical stage I NSGCT have a number of excellent management options, each with benefits and side effects. Robotic RPLND offers patients the opportunity to avoid the long-term side effects of chemotherapy, and for patients undergoing surveillance, it obviates the need for serial imaging with ionizing radiation and the anxieties related to surveillance. With promising early oncologic outcomes and improved perioperative outcomes, robotic RPLND may offer a truly effective management strategy for men with early stage NSGCT.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Motzer RJ, Jonasch E, Agarwal N, Beard C, Bhayani S, Bolger GB, et al. Testicular cancer, version 2 2015. J Natl Compr Cancer Netw. 2015;13(6):772–99.
Howlader N, Noone AM, Krapcho M, Garshell J, Miller D, Altekruse SF et al. SEER cancer statistics review, 1975–2012, National Cancer Institute. Bethesda, http://seer.cancer.gov/csr/1975_2012/, based on November 2014 SEER data submission, posted to the SEER web site, April 2015.
Huyghe E, Matsuda T, Thonneau P. Increasing incidence of testicular cancer worldwide: a review. J Urol. 2003;170:5–11.
Shanmugalingam T, Soultati A, Chowdhury S, et al. Global incidence and outcome of testicular cancer. Clin Epidemiol. 2013;5:417–27.
Verhoeven RH, Gondos A, Janssen-Heijnen ML, et al. Testicular cancer in Europe and the USA: survival still rising among older patients. Ann Oncol. 2013;24:508–13.
Chia VM, Quraishi SM, Devesa SS, et al. International trends in the incidence of testicular cancer, 1973–2002. Cancer Epidemiol Biomarkers Prev. 2010;19:1151–9.
McGlynn KA, Devesa SS, Graubard BI, Castle PE. Increasing incidence of testicular germ cell tumors among black men in the United States. J Clin Oncol. 2005;23(24):5757–61.
Albers P, Albrecht W, Algaba F, Bokemeyer C, Cohn-Cedermark G, Fizazi K, et al. Guidelines on testicular cancer: 2015 update. Eur Urol. 2015;68(6):1054–68. doi:10.1016/j.eururo.2015.07.044.
De Wit R. Optimal management of clinical stage I nonseminoma: new data for patients to consider. J Clin Oncol. 2014;32:3792–3. This article nicely summarizes the surveillance option for stage I NSCGT, and found a 30.6% 5-year relapse rate.
Dong P, Liu ZW, Li XD, Li YH, Yao K, Wu S, et al. Risk factors for relapse in patients with clinical stage I testicular nonseminomatous germ cell tumors. Med Oncol. 2013;30(1):494.
Kovac E, Stephenson AJ. Management of stage I nonseminomatous germ cell tumors. Urol Clin N Am. 2015;42(3):299–310. doi:10.1016/j.ucl.2015.04.004. Review.
Sheinfeld J, Herr HW. Role of surgery in management of germ cell tumor. Semin Oncol. 1998;25:203–9.
Cheney SM, Andrews PE, Leibovich BC, et al. Robot assisted retroperitoneal lymph node dissection: technique and initial case series of 18 patients. BJU Int. 2014;115:114–20. This series demonstrates the feasibility of post-chemotherapy RPLND.
Rassweiler JJ, Scheitlin W, Heidenreich A, Laguna MP, Janetschek G. Laparoscopic retroperitoneal lymph node dissection: does it still have a role in the management of clinical stage I nonseminomatous testis cancer? A European perspective. Eur Urol. 2008;54:1004–15.
Kenney PA, Tuerk IA. Complications of laparoscopic retroperitoneal lymph node dissection in testicular cancer. World J Urol. 2008;26:561–9.
Albqami N, Janetschek G. Laparoscopic retroperitoneal lymph-node dissection in the management of clinical stage I and II testicular cancer. J Endourol. 2005;19(6):683–92. discussion 692.
Neyer M, Peschel R, Akkad T, Springer-Stöhr B, Berger A, Bartsch G, et al. Long-term results of laparoscopic retroperitoneal lymph-node dissection for clinical stage I nonseminomatous germ-cell testicular cancer. J Endourol. 2007;21(2):180–3.
Peschel R, Gettman MT, Neururer R, Hobisch A, Bartsch G. Laparoscopic retroperitoneal lymph node dissection: description of the nerve-sparing technique. Urology. 2002;60(2):339–43. discussion 343.
Williams SB, Lau CS, Josephson DY. Initial series of robot-assisted laparoscopic retroperitoneal lymph node dissection for clinical stage I nonseminomatous germ cell testicular cancer. Eur Urol. 2011;60:1299–302.
Poulakis V, Skriapas K, De Vries R, et al. Quality of life after laparoscopic and open retroperitoneal lymph node dissection in clinical stage I nonseminomatous germ cell tumor: a comparison study. Urology. 2006;68:154–60.
Stephenson AJ, Bosl GJ, Motzer RJ, Kattan MW, Stasi J, Bajorin DF, et al. Retroperitoneal lymph node dissection for nonseminomatous germ cell testicular cancer: impact of patient selection factors on outcome. J Clin Oncol. 2005;23(12):2781–8.
Sun M, Abdollah F, Budaüs L, Liberman D, Tian Z, Morgan M, et al. Trends of retroperitoneal lymphadenectomy use in patients with nonseminomatous germ cell tumor of the testis: a population-based study. Ann Surg Oncol. 2011;18(10):2997–3004. doi:10.1245/s10434-011-1722-3.
Tarin TV, Sonn G, Shinghal R. Estimating the risk of cancer associated with imaging related radiation during surveillance for stage I testicular cancer using computerized tomography. J Urol. 2009;181(2):627–32. discussion 632–3.
Silva MV, Motamedinia P, Badalato GM, Hruby G, McKiernan JM. Diagnostic radiation exposure risk in a contemporary cohort of male patients with germ cell tumor. J Urol. 2012;187(2):482–6. doi: 10.1016/j.juro.2011.10.028. Erratum in: J Urol. 2012;188(1):334.
McCaffrey JA, Mazumdar M, Bajorin DF, Bosl GJ, Vlamis V, Motzer RJ. Ifosfamide- and cisplatin-containing chemotherapy as first-line salvage therapy in germ cell tumors: response and survival. J Clin Oncol. 1997;15(7):2559–63.
Huddart RA, Norman A, Shahidi M, et al. Cardiovascular disease as a long-term complication of treatment for testicular cancer. J Clin Oncol. 2003;21:1513–23.
Fosså SD, Aass N, Winderen M, Börmer OP, Olsen DR. Long-term renal function after treatment for malignant germ-cell tumours. Ann Oncol. 2002;13:222–8.
Wein AJ, In Kavoussi LR, Campbell MF, Walsh PC. Campbell-Walsh urology. 2012
Albers P, Siener R, Krege S et al. Randomized phase III trial comparing retroperitoneal lymph node dissection with one course of bleomycin and etoposide plus cisplatin chemotherapy in the adjuvant treatment of clinical stage I nonseminomatous testicular germ cell tumors: AUO trial AH 01/94 by the German Testicular Cancer Study Group. J Clin Oncol. 2008;26(18):2966–72. doi: 10.1200/JCO.2007.12.0899. Erratum in: J Clin Oncol. 2010;28(8):1439.
Bianchi G, Beltrami P, Giusti G, Tallarigo C, Mobilio G. Unilateral laparoscopic retroperitoneal lymph node dissection for clinical stage I nonseminomatous germ cell testicular neoplasm. Eur Urol. 1998;33(2):190–4.
Janetschek G, Hobisch A, Peschel R, Hittmair A, Bartsch G. Laparoscopic retroperitoneal lymph node dissection for clinical stage I nonseminomatous testicular carcinoma: long-term outcome. J Urol. 2000;163(6):1793–6.
Nelson JB, Chen RN, Bishoff JT, Oh WK, Kantoff PW, Donehower RC, et al. Laparoscopic retroperitoneal lymph node dissection for clinical stage I nonseminomatous germ cell testicular tumors. Urology. 1999;54(6):1064–7.
Allaf ME, Bhayani SB, Link RE, Schaeffer EM, Varkarakis JM, Shadpour P, et al. Laparoscopic retroperitoneal lymph node dissection: duplication of open technique. Urology. 2005;65(3):575–7.
Steiner H, Zangerl F, Stöhr B, Granig T, Ho H, Bartsch G, et al. Results of bilateral nerve sparing laparoscopic retroperitoneal lymph node dissection for testicular cancer. J Urol. 2008;180(4):1348–52.
Janetschek G, Hobisch A, Höltl L, Bartsch G. Retroperitoneal lymphadenectomy for clinical stage I nonseminomatous testicular tumor: laparoscopy versus open surgery and impact of learning curve. J Urol. 1996;156(1):89–93. discussion 94.
Abdel-Aziz KF, Anderson JK, Svatek R, Margulis V, Sagalowsky AI, Cadeddu JA. Laparoscopic and open retroperitoneal lymph-node dissection for clinical stage I nonseminomatous germ-cell testis tumors. J Endourol. 2006;20(9):627–31.
Gardner MW, Roytman TM, Chen C, et al. Laparoscopic retroperitoneal lymph node dissection for low-stage cancer: a Washington University update. J Endourol Endourol Soc. 2011;25:1753–7.
Hyams ES, Pierorazio P, Proteek O, Sroka M, Kavoussi LR, Allaf ME. Laparoscopic retroperitoneal lymph node dissection for clinical stage I nonseminomatous germ cell tumor: a large single institution experience. J Urol. 2012;187(2):487–92.
Davol P, Sumfest J, Rukstalis D. Robotic-assisted laparoscopic retroperitoneal lymph node dissection. Urology. 2006;67:199.
Harris KT, Gorin MA, Ball MW, Pierorazio PM, Allaf ME. A comparative analysis of robotic vs laparoscopic retroperitoneal lymph node dissection for testicular cancer. BJU Int. 2015;116(6):920–3. doi:10.1111/bju.13121. This is the first comparative analysis of robotic and laparoscopic RPLND to evaluate perioperative outcomes and safety.
Pearce SM, Gorin MA et al. Multicenter evaluation of primary robot-assisted laparoscopic RPLND in low-stage non-seminomatous testicular cancer. SUO 2015 abstract, manuscript in preparation. This is a multicenter report on robotic RPLND outcomes.
Moore LJ, Wilson MR, Waine E, Masters RS, McGrath JS, Vine SJ. Robotic technology results in faster and more robust surgical skill acquisition than traditional laparoscopy. J Robot Surg. 2015;9(1):67–73. doi:10.1007/s11701-014-0493-9.
Buse S, Hach CE, Klumpen P, Alexandrov A, Mager R, Mottrie A, et al. Cost-effectiveness of robot-assisted partial nephrectomy for the prevention of perioperative complications. World J Urol. 2015.
Kates M, Ball MW, Patel HD, Gorin MA, Pierorazio PM, Allaf ME. The financial impact of robotic technology for partial and radical nephrectomy. J Endourol. 2015;29(3):317–22. doi:10.1089/end.2014.0559.
Donohue JP, Thornhill JA, Foster RS, et al. Retroperitoneal lymphadenectomy for clinical stage A testis cancer (1965 to 1989): modifications of technique and impact on ejaculation. J Urol. 1993;149:237–43.
Weissbach L, Boedefeld EA. Localization of solitary and multiple metastases in stage II nonseminomatous testis tumor as basis for a modified staging lymph node dissection in stage I. J Urol. 1987;138:77–82.
Janetschek G, Reissigl A, Peschel R, et al. Laparoscopic retroperitoneal lymph node dissection for clinical stage I nonseminomatous testicular tumor. Urology. 1994;44:382ction.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Heather J. Chalfin, Wesley Ludwig, Phillip M. Pierorazio, and Mohamad E. Allaf each declare no potential conflicts of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Minimally Invasive Surgery
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
(MP4 352791 kb)
Rights and permissions
About this article
Cite this article
Chalfin, H.J., Ludwig, W., Pierorazio, P.M. et al. Robotic Primary RPLND for Stage I Testicular Cancer: a Review of Indications and Outcomes. Curr Urol Rep 17, 41 (2016). https://doi.org/10.1007/s11934-016-0597-z
Published:
DOI: https://doi.org/10.1007/s11934-016-0597-z