Abstract
Purpose of Review
A growing body of epidemiological and experimental data indicate that nutritional or environmental stressors during early development can induce long-term adaptations that increase risk of obesity, diabetes, cardiovascular disease, and other chronic conditions—a phenomenon termed “developmental programming.” A common phenotype in humans and animal models is altered body composition, with reduced muscle and bone mass, and increased fat mass. In this review, we summarize the recent literature linking prenatal factors to future body composition and explore contributing mechanisms.
Recent Findings
Many prenatal exposures, including intrauterine growth restriction, extremes of birth weight, maternal obesity, and maternal diabetes, are associated with increased fat mass, reduced muscle mass, and decreased bone density, with effects reported throughout infancy and childhood, and persisting into middle age. Mechanisms and mediators include maternal diet, breastmilk composition, metabolites, appetite regulation, genetic and epigenetic influences, stem cell commitment and function, and mitochondrial metabolism.
Summary
Differences in body composition are a common phenotype following disruptions to the prenatal environment, and may contribute to developmental programming of obesity and diabetes risk.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Environmental and nutritional exposures during prenatal and early postnatal development can result in increased risk for chronic diseases, a phenomenon known as “developmental programming.” Thus, optimizing maternal and child health during the “first 1000 days,” i.e., the critical period between conception and age 2, has become a key focus of public health efforts [1, 2]. With obesity, metabolic syndrome, and type 2 diabetes (T2D) reaching unprecedented levels in both Western and developing societies [3,4,5], it is crucial to understand the mechanisms by which suboptimal prenatal or early postnatal environments contribute to future disease vulnerability.
Identifying mechanisms and mediators of developmental programming has been an area of active research for the past two decades. A number of experimental models have been used, including rodents, large mammals, and primates, with a variety of dietary paradigms (e.g., high-fat diet, Western diets, low-protein diets, global caloric restriction, micronutrient restriction, etc.), surgical paradigms (e.g., uterine artery ligation), chemical exposures, psychological stress, transgenic models, and other systems [6,7,8,9,10,11]. Based on these experimental data, developmental programming may be caused by a number of overlapping and interacting factors, including epigenetic signals, mitochondrial inheritance, milk composition, the intestinal microbiome, and features of the maternal metabolic environment, such as insulin resistance, fatty acids, and inflammation. In many cases, the effects of the prenatal perturbations are exacerbated by postnatal exposure to a high-calorie diet, accelerated postnatal growth, stress, or other factors. While numerous markers and mediators have been implicated (and are reviewed elsewhere [12,13,14,15]), a common phenotype is altered body composition, with reduced lean mass and increased fat mass. This review summarizes recent publications on the prenatal determinants of abnormal body composition, with an emphasis on recent data in human populations published between 2012 and 2019. We will discuss evidence addressing mechanisms by which diet and appetite regulation, epigenetic regulation, differences in stem cell commitment and function, and impaired mitochondrial metabolism may contribute to obesity and diabetes risk.
Historical Observations
Early evidence for developmental programming came from studying historical cohorts. Studies of individuals exposed to the Dutch Famine during World War 2, in which a German blockade of the Western Netherlands caused a severe famine in a previously prosperous society, demonstrated that maternal exposure to undernutrition during pregnancy led to multiple adverse health outcomes for offspring, including fetal growth restriction [16, 17], and increased risk of visceral obesity, metabolic syndrome, T2D and other chronic diseases [18,19,20]. Subsequent work by David Barker, who discovered an association between low weight at birth and future cardiometabolic disease [21], further underscored the importance of early nutritional exposures as determinants of adult chronic disease risk. Barker hypothesized that stress experienced in utero—or during other critical developmental windows—induces compensatory responses in tissue structure and function that may persist permanently. Such developmental programming may allow the organism to withstand the stressor initially, but may create disease vulnerability in the future. Initial observations in the field focused on the deleterious effects of low birth weight and undernutrition during key developmental windows on future diabetes and obesity risk. A strong effect of prenatal exposure to undernutrition and low birth weight on T2D has been observed among ethnically diverse populations, in both historical and contemporary cohorts, including survivors of the Chinese Famine (1959–1961), the U.S. Nurses’ Health Study, a French cohort of women born between 1925 and 1950, the Shanghai Men’s and Women’s Health Studies, the Japanese Nurses’ Health Study, and other international cohorts [22,23,24,25,26].
Subsequent work demonstrated that over-nutrition or nutrient excess during critical developmental windows may also contribute to long-term chronic disease risk. For example, in utero exposure to maternal obesity can significantly increase risk of obesity, metabolic syndrome, and T2D in offspring [27,28,29]. Studies among siblings born before versus after maternal weight loss surgery (where the comparison of sibling pairs reduces the influence of genetics) indicate that risk of childhood obesity is increased by prenatal exposure to maternal obesity [30]. Similarly, studies of siblings discordant for in utero diabetes exposure (i.e., comparing siblings born before vs. after maternal T2D diagnosis) demonstrate that prenatal exposure to diabetes results in higher risk of obesity, hyperglycemia, dyslipidemia, and hypertension [31,32,33]. These effects are not limited to maternal T2D: type 1 diabetes, monogenic diabetes, gestational diabetes (GDM), and subclinical hyperglycemia not reaching the threshold for GDM are also linked to adiposity and glucose intolerance in offspring [34, 35]. More recently, there has been growing evidence for pollutants and chemical exposures, including vehicle emissions, cigarette smoke, endocrine-disrupting chemicals, and pesticides, as inducers of developmental programming [36,37,38,39,40,41,42,43,44,45]. Thus, a diverse range of prenatal exposures has been linked to obesity and metabolic diseases in the offspring.
Developmental Programming of Adiposity
Birth Weight and Future Adiposity
Prenatal exposure to a suboptimal in utero environment is associated with increased BMI, increased fat mass, and central/abdominal fat distribution—body composition patterns linked to T2D risk. Since prenatal growth is influenced by a wide range of factors (e.g., maternal nutrition, placental insufficiency, hypoxia, smoking, etc.), birth weight can be considered a biomarker for disruptions in the prenatal environment. Many population-based studies indicate that both low and high birth weight are associated with excess adiposity throughout the lifespan; these studies are summarized in Table 1. Several groups have documented associations between small for gestational age (SGA) birth weight and future risk of central or visceral adiposity [85,86,87], but the literature has not been entirely consistent, with several large studies failing to document such associations [54, 62]. At the other end of the spectrum, large for gestational age (LGA) infants are at increased risk for increased fat mass and high BMI [86], so that the association between birth weight and future adiposity has been described as a “U-shaped” distribution [88]. Although the studies vary in methodology and sample size, the effect of birth weight on future BMI seems most reproducible for infants with high birth weight, whereas increases in central adiposity (assessed by MRI, DXA, or skinfold thickness) appear more reproducible among those born SGA.
Some of the discordance in the literature may stem from differences in statistical adjustment for confounders. A recent analysis in the Danish National Birth Cohort indicated that socioeconomic confounders including low maternal education and household income were associated with both low birth weight and high childhood BMI [89]; careful adjustment for these factors is therefore essential. Adjusting for offspring BMI may also introduce variability in study outcomes. For example, Kramer et al. applied two statistical approaches to the same dataset and showed that the association between SGA and childhood body fat had the opposite directionality depending on how the statistical models dealt with BMI. Adjustment for the child’s current BMI indicated increased percent body fat with SGA, but decreased body fat with SGA in an unadjusted analysis. Notably, the association between SGA and increased subscapular/triceps skinfold thickness was significant using both statistical approaches [58•].
Genetic factors, too, can influence the relationship between birth weight and future adiposity. For example, genetic variation at many SNPs linked to obesity and/or diabetes are also linked to birth weight [90, 91]. However, a recent pooled analysis of 27 twin cohorts confirmed a strong influence of birth weight on BMI, in both fraternal and monozygotic twin pairs, suggesting that these effects are not fully explained by genetic factors [92].
Maternal Obesity and Future Adiposity
Maternal pre-pregnancy BMI is among the strongest risk factors for childhood obesity and is estimated to account for 10–20% of the population attributable risk of childhood obesity [93,94,95]. Effects of maternal obesity on offspring adiposity emerge early: higher maternal BMI is linked to higher birth weight and greater newborn skinfold thickness, with differences in body weight detectable by 32 weeks’ gestation [96,97,98]. Maternal obesity has been reproducibly associated with offspring adiposity throughout the lifespan, as summarized in Table 1. Maternal pre-pregnancy BMI is associated with higher childhood BMI and with increased adiposity (percent body fat and skinfold thicknesses) [71, 72]. Based on a meta-analysis of data from 162,129 mothers and their children from 37 pregnancy and birth cohort studies from Europe, North America, and Australia, maternal BMI has the strongest effect in late childhood (age 10–18 years) [95], but effects remained detectable into late adulthood [74]. Moreover, maternal obesity has also been linked to accelerated weight gain throughout early and mid-adulthood [29].
While the association between maternal pre-pregnancy BMI and offspring adiposity is strong and reproducible across ethnically diverse populations, it is unclear whether the effect is due to programming by the in utero environment, or by confounders such as shared genetic, nutritional, or socioeconomic risk factors. Studies of siblings born before versus after maternal weight loss (e.g., following obesity surgery) show increased childhood obesity risk for the sibling born before maternal weight loss, supporting the concept that in utero exposure to maternal obesity plays a pathogenic role [30, 99]. Moreover, recent studies using Mendelian randomization have indicated that genetic variants linked to maternal BMI (e.g., rs3736485 in DMXL2) are associated with higher offspring birth weight and childhood BMI, independent of offspring genotype [100, 101], although a similar analysis in the ALSPAC and Generation R cohorts found no effect of maternal BMI on childhood BMI after adjusting for shared genetics [102]. Taken together, these data support an important effect of prenatal exposure to maternal obesity on offspring adiposity, although the relative role of genetic versus epigenetic and environmental factors remains unclear.
Maternal Hyperglycemia or Diabetes and Future Adiposity
Prenatal exposure to maternal diabetes, or to hyperglycemia not reaching diagnostic cut-offs for GDM, is associated with increased adiposity in offspring. Some of the most compelling evidence for this effect has come from the Hyperglycemia and Adverse Pregnancy Outcome (HAPO) Follow-up Study, a large international cohort study designed to examine associations of glucose levels during pregnancy with multiple adverse perinatal outcomes, in order to establish diagnostic cut-offs for GDM [103]. In the HAPO Follow-up Study, maternal glucose levels at 28 weeks’ gestation were found to be positively associated with birth weight and newborn adiposity, and with childhood BMI, skinfold thicknesses, waist circumference, and percent body fat between 10 and 14 years of age [78, 104]. Similarly, associations between higher maternal glucose during gestation and childhood adiposity were reported in the Danish National Birth Cohort, the US-based EPOCH Study, and other cohort studies (Table 1) [79, 81].
A longstanding controversy centers around whether maternal hyperglycemia per se contributes to offspring obesity, independent of maternal BMI, given that women with GDM are more likely to be obese. However, in HAPO and many recent studies, the effects of maternal GDM or hyperglycemia persisted after adjustment for maternal pre-pregnancy BMI [75••, 78, 79, 81, 82••]. Moreover, the EPOCH Study demonstrated that effects of maternal GDM on offspring adiposity were not explained by the child’s genetic risk score for obesity [105]. Prenatal exposure to maternal type 1 diabetes has similarly been linked to increased total body fat in offspring [83]. Together, these data support a strong effect of maternal hyperglycemia and diabetes on offspring adiposity, and raise the possibility that interventions to detect and treat gestational hyperglycemia might be a promising strategy for preventing childhood obesity.
Developmental Programming of Muscle Mass
Decreased muscle mass has been reported across several types of in utero disruptions, spanning undernutrition, maternal diabetes, and prenatal stress. Paucity of muscle mass may be an important contributor to diabetes risk: muscle is a crucial insulin target tissue, and decreased muscle mass is linked to insulin resistance due to reduced whole-body glucose uptake, independent of BMI [106].
Effects of Birth Weight on Muscle Mass
Low birth weight infants have been reported to have reduced muscle mass throughout childhood, adolescence, and young adulthood (reviewed in [65, 107]), and reduced muscle strength both in later childhood [108] and in adulthood [109, 110]. These effects have been reported among infants born low birth weight due to intrauterine growth restriction, as well as those born premature. Among the latter group, low birth weight is strongly correlated with reduced lean mass in childhood [111]. Based on one of the earliest cohorts of extremely low birth weight (ELBW, < 1000 g, typically < 27 weeks’ gestation) infants born between 1977 and 1982, ELBW infants have detectable reductions in lean body mass into their fourth decade as compared to normal birth weight infants [64]. Conversely, infants born LGA have higher lean mass in later life [69, 70]. Recent studies linking birth weight to lean mass are summarized in Table 2.
While the association between birth weight and lean mass is strong and reproducible, it is unclear whether it is driven by prenatal versus postnatal factors. For example, decreased prenatal growth velocity (calculated as the change in fetal weight percentiles between 22 weeks’ gestational age and birth) is a strong predictor of reduced lean mass at birth, independent of birth weight [65]. Moreover, low birth weight is often associated with postnatal catch-up growth, a growth pattern characterized by upward crossing of weight for age percentiles, and with “catch-up fat,” or accelerated adipose tissue growth outstripping the growth of lean mass [116]. Catch-up weight gain following intrauterine growth restriction is associated with higher fat mass and lower lean mass in later life, independent of birth weight [117, 118]. Conversely, LGA infants have been reported to have accelerated growth of lean mass during the early postnatal period [119]. Thus the role of prenatal versus postnatal factors in developmental programming of lean mass remains an important question.
In utero exposure to hyperglycemia is also linked to reductions in lean body mass, similar to prenatal undernutrition and low birth weight, which is paradoxical given that maternal hyperglycemia tends to increase birth weight. Effects of maternal GDM on lean mass have been reported in early childhood and in adolescence [80, 81]. Prenatal exposure to nutrient excess has been linked to impaired myogenesis in offspring rodents and pigs [120], but it is unclear whether similar mechanisms are at play in humans.
Developmental Programming of Bone Mass
Bone density is known to influence osteoporosis and fracture risk, and is linked to healthy aging. Recent studies have highlighted connections between bone density, marrow adipocytes, and systemic metabolism, leading some to propose that osteoporosis should be viewed as “obesity of bone” [121]. Loss of bone density is usually accompanied by increases in bone marrow adipocyte populations. Osteocytes and marrow adipocytes are derived from common precursors, mesenchymal stem cells. Although they were historically viewed as “filler,” bone marrow adipocytes are increasingly recognized as playing an important role in bone health and metabolic disease. For example, leptin and other adipokines can stimulate osteocyte development [122], and marrow adipocytes can influence bone metabolism and hematopoiesis [123]. Thus, effects of prenatal exposures on bone density may have broad implications for healthy aging and metabolism.
Birth Weight and Future Bone Mass
Nutritional exposures during early development can significantly impact future skeletal health, bone mineral density, and osteoporosis risk. Bone mineral density accrues fastest during the third trimester of pregnancy, but continues to increase postnatally and peaks in young adulthood [124]. Thus, periods of suboptimal nutrition, or other stressors (e.g., inflammation, chronic disease, glucocorticoid treatment, etc.) during early life can impair peak bone mass, increase osteoporosis risk, and “program” future bone health (available data summarized in Table 3). For example, birth weight is predictive of childhood bone mineral density: individuals with lower birth weight (< 10th percentile) had lower forearm cortical bone mineral density [127], whereas whole-body bone mineral density and content are positively associated with birth weight [134]. Intrauterine growth indices, too, may be predictive of childhood bone density, with increases in fetal abdominal circumference between 19 and 34 weeks’ gestation positively associated with greater bone mineral density at age 4 years [135]. Meta-analyses and systematic literature reviews support a role for prenatal growth on future skeletal health: higher birth weight has been reproducibly associated with higher bone mineral content in childhood and adulthood [136, 137]. However, there is some heterogeneity between studies: some groups have demonstrated only sex-specific effects or have only noted effects on certain bone indices (e.g., bone mineral content vs. density) [112]; moreover, effects of birth weight on bone mass may be stronger in childhood and adolescence than in later life [126, 137, 138]. These effects are recapitulated in animal models: Wallace et al. reported that prenatal growth restricted lambs had lower bone mineral density (as compared to normal birth weight lambs) throughout the lifespan [139], whereas Devlin et al. reported increased trabecular bone volume in female offspring of high-fat diet fed mouse dams [140].
Maternal Diabetes and Offspring Bone Mass
Despite positive associations between LGA and higher bone mass, some reports have suggested that infants of mothers with GDM have decreased bone strength [132] and bone mineral density, with more severe defects in offspring of mothers with uncontrolled diabetes (reviewed in [141]). However, other studies have found no effect, or a higher bone density, in offspring of mothers with diabetes [84, 130, 133]. Thus, further analyses are needed to better define the net effect of maternal hyperglycemia and diabetes on offspring bone health.
Mechanisms
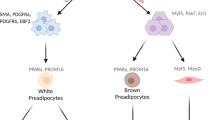
From a mechanistic standpoint, developmentally programmed differences in body composition may be caused by numerous factors, including: diet or lifestyle, reduced numbers and/or function of muscle progenitors, increased numbers and/or function of adipose progenitors, adipocyte hypertrophy and lipogenesis, altered nutrient uptake by lean versus adipose tissues, altered signaling through pathways regulating muscle growth (e.g., GH, IGF1, myostatin [119]), genetics, and/or by persistent changes in epigenetic marks. Based on recent data in experimental models and in translational studies of human tissues, each of these potential pathways has been implicated in developmental programming of body composition (Fig. 1). We review the evidence supporting each of these possibilities in this section, with an emphasis on mechanistic studies in humans.
Maternal Diet and Metabolites
Maternal diet is a key potential mediator of the association between prenatal exposures and postnatal body composition. Maternal intake of macronutrients or micronutrients may create a metabolic milieu that modulates infant growth. For example, higher maternal carbohydrate intake during pregnancy is associated with higher fat mass in childhood [142]; conversely, high-protein/low-carbohydrate intake during pregnancy is associated with lower abdominal adiposity in the newborn period [143]. Associations have also been reported between offspring waist circumference and maternal adherence to the Mediterranean diet during pregnancy [144], and between neonatal adiposity and maternal intake of pro-inflammatory foods (positively correlated) [145] and maternal diet quality (inversely correlated) [146].
Maternal intake of micronutrients has also been linked to offspring obesity and altered body composition. For example, lower maternal intake of vitamin D has been linked to reduced adiposity at birth, but higher fat mass at ages 1, 4, and 6 years [147, 148]. Although the association was not detected in a population with a low prevalence of vitamin D deficiency [149], a large meta-analysis (35,032 mother–infant pairs) confirmed associations between low prenatal maternal vitamin D and low birth weight, and with increased infant weight at 9 months (unadjusted for birth weight) [150].
Maternal diabetes and obesity may influence levels of specific metabolites that influence fetal growth or metabolism. For example, a metabolomic analysis in women with GDM identified increased levels of the furan fatty acid metabolite CMPF (derived from the diet/microbiome), which, when administered to mice, induced beta cell dysfunction and impaired mitochondrial metabolism [151]. Moreover, higher maternal intake and cord blood concentrations of the long-chain fatty acids DHA and EPA, and a higher ratio of cord plasma n-6:n-3 PUFAs, were associated with higher infant skinfold thicknesses and increased odds of obesity [152]. In this same cohort, cord blood levels of metabolites related to tryptophan and the one-carbon methyl donor pathway were associated with more rapid infancy weight gain and higher childhood BMI [153]. Moreover, higher maternal levels of the choline metabolite and methyl donor betaine have been associated with lower infant birth weight and abdominal fat [154].
Although maternal diet is a modifiable risk factor and an attractive target for interventions to prevent childhood obesity, dietary interventions during pregnancy among obese women have largely been unsuccessful. For example, a randomized controlled intervention to reduce the omega-6 to omega-3 PUFA ratio throughout pregnancy and lactation yielded no detectable effects on childhood body composition, assessed by MRI at age 5–6 years [155], nor did a trial of maternal DHA supplementation result in any differences in adiposity measures in offspring [156]. Further studies will be essential to identify effective nutritional strategies during gestation to prevent childhood obesity and adiposity.
Breast Feeding and Milk Composition
The mode of infant feeding and milk composition are important contributors to childhood obesity and body composition. Formula feeding is associated with more rapid postnatal weight gain, higher childhood BMI, and greater acquisition of lean mass, as compared to breast feeding [157, 158]. However, obesity risk is increased by maternal obesity even in exclusively breastfed infants [159], raising the possibility that differences in human milk composition could contribute to mother–child transmission of obesity risk. Consistent with this, several groups have identified differences in bioactive compounds in milk from obese versus lean mothers, including increased insulin, leptin, adiponectin, ghrelin, IL-6, TNF-alpha, and lower omega-3 fatty acids (reviewed in [160] and [161]). However, for many of these compounds, there is a positive association with maternal BMI and a negative association with infant adiposity (notably insulin, adiponectin and IL-6), or no association, so that it is unclear whether milk composition differences play a pathogenic role in infant adiposity.
Recent data suggest that milk content of fructose and human milk oligosaccharides are linked to body composition in exclusively breastfed infants [162, 163]; however, these were not significantly associated with maternal BMI. A recent metabolomics analysis of human milk in obese versus lean mothers found associations between the abundance of several milk metabolites and infant fat mass, assessed by DXA. Although there was only minimal overlap between metabolites associated with maternal and infant adiposity, some intermediates of nucleotide metabolism were linked to both maternal BMI and infant fat mass, raising the possibility that these metabolites might play a mechanistic role in mother–child transmission of obesity [164]. Further evidence for milk composition as contributor to childhood obesity has come from experimental studies. For example, in mice, cross-fostering experiments indicate that lactational exposure to maternal obesity confers obesity in the offspring [165]. Moreover, in a rat model, maternal HFD was associated with reduced prolactin receptor expression and prolactin content in milk, and normalizing milk prolactin levels reduced visceral adiposity and normalized insulin sensitivity [166]. Together, these data provide strong support for the role of milk in shaping childhood body composition.
Postnatal Diet and Appetite Regulation
Postnatal diet is another potential mechanism for developmentally programmed effects on body composition. For example, the nutritional environment that may have contributed to suboptimal (or excessive) prenatal growth could also affect postnatal phenotypes. Consistent with this, in a study from rural Southern India, LBW individuals had lower average daily protein intake at age 20 years, in association with significantly reduced lean mass and trends for reduced bone mineral content [167]. Moreover, in Western societies, dietary patterns associated with higher maternal BMI are also associated with childhood obesity, e.g., sugar-sweetened beverages, highly processed snack foods, food insecurity, etc. Thus, it can be challenging to disentangle effects of prenatal nutrition versus postnatal diet on offspring body composition.
Prenatal perturbations may also affect appetite regulation and eating behaviors. For example, children with higher birth weight had differences in eating behavior survey measures, such as Satiety Responsiveness (lower), Food Responsiveness (higher), and Enjoyment of Food (higher) in early childhood [168]. Similarly, prenatal exposure to hyperglycemia or GDM was associated with altered eating behavior; adolescent offspring were more likely to score highly on the Eating in the Absence of Hunger in Children and Adolescents questionnaire [169, 170]. Mechanistic studies of appetite regulation are challenging in humans. However, based on experimental animal models, maternal HFD may alter the formation of satiety regulating hypothalamic neuronal projections in offspring, via insulin signaling and endoplasmic reticulum (ER) stress pathways [171, 172]. The satiety hormone leptin also may shape appetite pathways during the perinatal period, based on experimental studies in which postnatal leptin administration reversed developmental programming by prenatal undernutrition [173, 174].
Postnatal Lifestyle
Body composition can be influenced by physical activity and exercise, and these too may be associated with prenatal exposures. For example, reductions in lean mass in individuals with a history of LBW may be due in part to differences in postnatal exercise patterns. Several studies have reported that a history of very low birth weight (birth weight < 1500 g) was associated with reduced levels of leisure time physical activity in young adulthood [175, 176]. Postnatal physical activity and fitness may also mediate the association between maternal BMI and childhood adiposity: for example, higher maternal BMI was associated with lower physical fitness measures in preschool-aged children [177]. These data suggest that postnatal exercise interventions might mitigate the effects of prenatal exposures on postnatal body composition. Consistent with this, data from two observational studies indicate that physical activity may reverse the adverse effects of LBW on body composition and insulin resistance [178].
Endocrine Factors
Several endocrine factors and signaling pathways have been implicated in developmental programming of body composition. For example, maternal adipokines including leptin and adiponectin have been linked to offspring adiposity in infancy [179, 180], while cytokines including IL4, IL5, and IL13 have been linked to decreased risk of early childhood adiposity [181]. Differences in growth hormone and its effectors have been reported in several human studies and experimental paradigms of prenatal perturbation. In a longitudinal study of VLBW and SGA infants over the first 2 years of life, IGF1 levels at 1 week and 3 months post partum were positively correlated with lean mass at 24 months [182]. Children with a history of SGA birth weight are sometimes treated with recombinant human growth hormone (GH) for short stature; GH treatment is associated with a reduction in fat mass and an increase in lean mass [183, 184]. However, it is not clear that such changes persist into adulthood [185, 186]. Recent studies have also implicated myostatin (an inhibitor of myogenesis) and the fibroblast growth factor family members FGF19 and FGF21 in differences in body composition between SGA and LGA offspring [119, 187].
Adipose Tissue Growth
Growth of adipose tissue depots occurs through two main processes: adipogenesis, i.e., commitment of precursor stem cells toward the adipocyte lineage, and hypertrophy, i.e., growth of existing adipocytes through lipid uptake and lipogenesis. Both processes have been implicated in the developmental programming of adiposity. For example, expression of Pref-1, a key inhibitor of adipogenesis, was reduced in placenta from SGA versus AGA infants and inversely correlated with total fat mass at 4 and 12 months post partum [188]. Adipose expression of Pref-1 was also reduced in a mouse model of prenatal calorie restriction and low birth weight [189]. In a rat model of maternal gestational obesity, offspring developed visceral adiposity with adipocyte hypertrophy and upregulation of lipogenesis genes (Srebp1, Fas), together with decreased expression and epigenetic silencing of adipogenesis genes [190]. Other groups have reported that gestational exposure to maternal obesity is associated with increased adipocyte commitment and differentiation [191].
Epigenetic Mechanisms
The dominant mechanistic model for developmental programming of body composition (and other phenotypes) is that exposure to an adverse prenatal environment induces lasting changes in epigenetic regulation; such changes may include hyper- or hypomethylation of DNA, changes in chromatin marks, and/or expression of large and small noncoding RNA [13]. There is now a robust body of data supporting such epigenetic mechanisms in human obesity. Based on epigenome-wide association studies in a consortium of cohort studies, adult BMI is associated with widespread changes in DNA methylation, with enrichment of loci near genes involved in lipid and lipoprotein metabolism and inflammation. However, analysis of genetic variants suggested that the changes in DNA methylation were largely the consequence of BMI rather than the cause [192]. In another adult population, DNA methylation within or near genes related to ER function was associated with BMI and percent fat mass, which is intriguing in light of evidence linking nutrient-mediated ER stress to the pathogenesis of insulin resistance and obesity [193]. Epigenome-wide studies have also identified associations between DNA methylation and lean muscle mass [194].
In contrast to studies in adult populations, where epigenetic changes may occur as a consequence of obesity, studies in early childhood indicate that changes in DNA methylation precede and predict childhood body composition. For example, analysis of DNA methylation patterns in dried blood spots in neonates identified associations between methylation at 69 genomic regions and BMI z-score at age 5, and 27 genomic regions were associated with percent body fat at age 5 [195]. Moreover, DNA methylation at retinoid X receptor alpha (RXRA) in umbilical cord tissue was associated with total and percent fat mass at age 9 years [196], as well as with childhood bone mineral content [197, 198]. Additional epigenome-wide association studies in European and US-based populations have similarly uncovered associations between DNA methylation in whole blood in early childhood, and body composition [199, 200].
Birth Weight and Body Composition: Epigenetic Mediators
Recent studies have suggested that DNA methylation changes in placenta and cord blood may mediate the association between birth weight and body composition. In a small study of term infants born appropriate-for-gestational-age (AGA) or small-for-gestational-age (SGA), hypermethylation near ATG2B, NKX6.1, and SLC13A5, and hypomethylation of GPR120, in placenta and cord blood from SGA newborns was linked to changes in gene expression levels (opposite to methylation status), and total and abdominal fat at age 2 weeks [201]. Moreover, in a prospective pregnancy cohort, umbilical cord DNA methylation at six loci was linked to birth weight, offspring size, and adiposity in early childhood [202].
Maternal Obesity and Offspring Body Composition: Epigenetic Mediators
In the ALSPAC study (N = 1018), offspring epigenome-wide DNA methylation was analyzed in relation to maternal and offspring adiposity. In total, 28 and 1621 CpG sites were differentially methylated in offspring of obese and underweight mothers, respectively, compared with offspring of normal weight mothers [203]. Lower methylation at the SLC6A4 locus in umbilical cord was associated with higher maternal gestational weight gain and with higher adiposity in early childhood (total fat mass and % fat mass between 4 and 7 years); moreover, adipose tissue methylation and expression of SLC6A4 was lower in obese compared with lean individuals [204]. SLC6A4 encodes a serotonin transporter which may play a role in energy balance.
Maternal Diabetes and Offspring Body Composition: Epigenetic Mediators
In the setting of maternal diabetes, analysis of genome-wide DNA methylation patterns has identified strong effects on the epigenome of placenta [205], cord blood, and peripheral leukocytes throughout childhood and early adulthood [206]. Mechanistically, DNA methylation differences in placenta may affect nutrient transfer: for example, GDM is associated with increased methylation at CpG2 of placental lipoprotein lipase, decreased mRNA expression, and abundance of lipids in the neonatal circulation [207]. Interestingly, a subset of genomic loci for which cord blood DNA methylation levels have been linked to maternal glucose exposure (Hyperglycemia and Adverse Pregnancy Outcome (HAPO) study) overlaps with loci linked to birth weight in the Cambridge Baby Growth Study and to maternal prenatal undernutrition in a Gambian population; these loci (TERF2IP, SUSD1, C6orf96, and ACYP2) may be especially sensitive to nutritional status during development [208].
Taken together, these data provide strong support for the concept that epigenetic regulation mediates the association between prenatal exposures and offspring body composition. However, it remains uncertain whether epigenetic marks play a causal role or alternatively reflect alterations in transcriptional activity at these loci, in turn mediated by additional pathway-specific or generalized chromatin modulating mechanisms. While more experimentally challenging than methylation analyses, these studies will be critical to determine causal relationships.
Stem Cells as Mediators of Developmentally Programmed Phenotypes
Stem cell populations are established in utero and may carry an “epigenetic memory” of nutritional or other insults during development. Thus, they have been proposed as potential mediators of developmental programming of obesity and body composition [209, 210]. Consistent with this, our group has described reductions in the number and regenerative capacity of skeletal muscle stem cells in a mouse model of late gestation undernutrition and low birth weight [211]. A leading hypothesis posits that developmental exposures may alter commitment of mesenchymal cells toward the adipocyte lineage. Adipose-derived stem cells (ADSCs) from a small study of young adults born either LBW or normal weight showed significant differences in gene expression and in genome-wide DNA methylation patterns. Interestingly, such differences were more pronounced in ADSC than in mature differentiated adipocytes, suggesting that stem cells may carry an epigenetic memory of prenatal disruptions [212].
In the past, studying stem cell function in human infants was complicated by the unavailability of relevant cells for analysis. However, the discovery of fetal mesenchymal stem cells—a precursor cell able to differentiate into adipocytes, myocytes, cartilage, and bone—in perinatal tissues such as amniotic membranes and in umbilical cord Wharton’s jelly has allowed new insights into stem cell biology and developmental programming [213,214,215]. How closely such perinatal stem cells recapitulate the biology of adipose tissue-derived precursor cells is unclear. Still, data from such translational model systems support an effect of prenatal exposures on infant stem cell fate and function. For example, umbilical Wharton’s jelly mesenchymal stem cells from SGA infants exhibit increased proliferation capacity, impaired oxidative metabolism, and increased expression of the lipid synthesis gene fatty acid elongase ELOVL2 [216, 217]. Adipocytes derived from MSC of SGA infants showed increased expression of acyl-coenzyme A synthetase 1 (ACSL1), which in turn was noted to regulate cellular lipid uptake and adipogenesis [218].
Maternal obesity, too, has been reported to alter mesenchymal stem cell function. For example, one human study reported increased adipogenic capacity in amniotic membrane stem cells from offspring of obese women [219]. Another group has reported that prenatal exposure to maternal obesity results in increased adipogenic capacity and reduced myogenesis in infant mesenchymal stem cells isolated from umbilical cord, and that in vitro adipogenic capacity of such MSC was correlated with postnatal weight gain and accelerated adipose tissue growth from birth to 5 months [220••, 221,222,223]. Higher adiposity at age 5 months was associated with higher acylcarnitine levels, higher expression of genes involved in lipid metabolism, and markers of oxidative stress in MSC [221]. Together, these data suggest that mesenchymal stem cells from infants exposed to abnormal prenatal environments can be used to model developmentally programmed changes in body composition and may shed new insights into pathophysiology and treatment.
Mitochondrial Metabolism
Multiple lines of evidence suggest that disruptions to the prenatal environment—both undernutrition and overnutrition—can result in impaired mitochondrial function in offspring tissue. For example, umbilical mesenchymal stem cells from SGA infants have decreased mitochondrial oxygen consumption rates [217]. Similar impairments in mitochondrial metabolism in skeletal muscle [224], cardiac muscle [225], adipose tissue [226], and liver have also been described in rodent models of intrauterine growth restriction and LBW. Moreover, such mitochondrial perturbations can be exacerbated by postnatal diet. For example, in a study of LBW versus normal birth weight (NBW) young men, overfeeding via high-fat diet increased adipose tissue DNA methylation of PPARGC1A, a critical regulator of mitochondrial biogenesis and oxidative metabolism, in LBW, but not NBW, young men, suggesting that prenatal factors may alter the postnatal adipose response to nutrient excess [227]. However, the data are not homogeneous: some groups have reported normal mitochondrial function in skeletal muscle of LBW young men [228] or increased skeletal muscle mitochondrial content and function following prenatal undernutrition in rodents [229, 230].
By contrast, prenatal overnutrition and maternal obesity have been more consistently associated with impaired offspring mitochondrial metabolism. Both mitochondrial biogenesis and function are reduced in placenta of obese women [231]. Similarly, transcriptomic analysis in human umbilical vein endothelial cells, umbilical mesenchymal stem cells, and skin fibroblasts showed reductions in OXPHOS gene expression and altered mitochondrial function in infants of obese mothers [219, 232, 233]. In animal models, maternal high-fat diet has been linked to reduced mitochondrial biogenesis and impaired mitochondrial metabolism in oocytes (both F0 mothers’ and F1 daughters’) [234,235,236,237], placenta [238], and in offspring skeletal muscle [239, 240], cardiac muscle [241], adipose tissue, liver [242], and hypothalamus [243].
Resting Energy Expenditure and Thermogenesis
Reductions in resting energy expenditure can contribute to weight gain and adiposity, and energy expenditure in turn is strongly influenced by body composition. The main contributor to resting energy expenditure is muscle, which expends energy through physical activity and shivering, but mitochondria-rich brown and beige adipose tissue may also contribute through thermogenesis, or heat production. Brown adipose tissue (BAT) was once thought to be present only in small mammals and babies, but BAT depots have recently been discovered in adult humans, and their size and activity have been linked to obesity and metabolic outcomes. Emerging data suggest that prenatal growth restriction is linked to altered BAT function. In a study of BAT activation in prepubertal SGA versus AGA children, Malpique et al. reported that BAT activity was associated with smaller visceral fat mass and improved metabolism [244]. Prenatal growth restriction may be associated with long-term changes in resting energy expenditure. For example, birth weight was positively associated with lean mass and resting metabolic rate in adult women [245]. However, these effects have not been consistently reported, perhaps due to differences in how energy expenditure was normalized. In studies in which resting energy expenditure was normalized to lean mass, adults with history of prematurity and very low birth weight may even have higher resting energy expenditure per unit lean body mass [246]. Moreover, diet may cause differences in energy expenditure: when challenged with a 5-day high-fat overfeeding challenge, energy expenditure and fat oxidation were significantly higher among young men with a history of LBW as compared with NBW controls [247]. These data highlight the interaction of prenatal stress with postnatal nutrition.
Cellular Aging/Senescence
In an interesting translational study, De Zegher et al. recently reported that birth weight was directly correlated with leukocyte telomere length at birth, and that telomere length in turn predicted lean mass at age 12 months [248]. Similarly, prenatal exposure to GDM has also been linked to reduced telomere length in childhood (age 9–16 years) [249]. These data raise the possibility that prenatal stressors may activate cellular aging and senescence pathways.
Conclusion
With advances in “-omics” techniques and increased interest in the prenatal environment as a determinant of chronic health and disease, the last decade has brought a greater understanding of the developmental programming of offspring body composition. Birth weight (which can be viewed as a biomarker for the adequacy of the prenatal environment), maternal obesity, and gestational diabetes are each linked to increased adiposity in childhood and later life. Birth weight is also robustly linked to muscle mass and bone density later life. On the other hand, associations between prenatal exposure to diabetes and offspring lean mass and bone density differ between populations. Mechanistically, programming of body composition may arise via differences in nutrients or metabolites, postnatal lifestyle factors, epigenetic regulation, impaired mitochondrial metabolism, and/or increased mesenchymal stem cell commitment to the adipose lineage. The hope is that an improved mechanistic understanding will allow the development of early markers of future risk, to facilitate targeted nutritional, metabolite-based, or other therapeutic interventions that might curb the ongoing epidemics of obesity and diabetes.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Hanson M, Gluckman P. Developmental origins of noncommunicable disease: population and public health implications. Am J Clin Nutr. 2011;94(6 Suppl):1754S–8S.
Taveras EM, Perkins M, Woo Baidal JA, et al. The impact of the first 1000 days on childhood obesity. Durham, NC: Robert Wood Johnson Foundation, Healthy Eating Research; 2016.
Dabelea D, Mayer-Davis EJ, Saydah S, Imperatore G, Linder B, Divers J, et al. Prevalence of type 1 and type 2 diabetes among children and adolescents from 2001 to 2009. JAMA. 2014;311(17):1778–86.
Ogden CL, Carroll MD, Lawman HG, Fryar CD, Kruszon-Moran D, Kit BK, et al. Trends in obesity prevalence among children and adolescents in the United States, 1988–1994 through 2013–2014. JAMA. 2016;315(21):2292–9.
Ogden CL, Carroll MD, Kit BK, Flegal KM. Prevalence of childhood and adult obesity in the United States, 2011–2012. JAMA. 2014;311(8):806–14.
Shepherd PR, Crowther NJ, Desai M, Hales CN, Ozanne SE. Altered adipocyte properties in the offspring of protein malnourished rats. Br J Nutr. 1997;78(1):121–9.
Park JH, Stoffers DA, Nicholls RD, Simmons RA. Development of type 2 diabetes following intrauterine growth retardation in rats is associated with progressive epigenetic silencing of Pdx1. J Clin Invest. 2008;118(6):2316–24.
Woodall SM, Breier BH, Johnston BM, Gluckman PD. A model of intrauterine growth retardation caused by chronic maternal undernutrition in the rat: effects on the somatotrophic axis and postnatal growth. J Endocrinol. 1996;150(2):231–42.
Isganaitis E, Woo M, Ma H, Chen M, Kong W, Lytras A, et al. Developmental programming by maternal insulin resistance: hyperinsulinemia, glucose intolerance, and dysregulated lipid metabolism in male offspring of insulin-resistant mice. Diabetes. 2014;63(2):688–700.
Jimenez-Chillaron JC, Hernandez-Valencia M, Reamer C, Fisher S, Joszi A, Hirshman M, et al. Beta-cell secretory dysfunction in the pathogenesis of low birth weight-associated diabetes: a murine model. Diabetes. 2005;54(3):702–11.
Owens JA, Falconer J, Robinson JS. Glucose metabolism in pregnant sheep when placental growth is restricted. Am J Phys. 1989;257(2 Pt 2):R350–7.
Fleming TP, Watkins AJ, Velazquez MA, Mathers JC, Prentice AM, Stephenson J, et al. Origins of lifetime health around the time of conception: causes and consequences. Lancet. 2018;391(10132):1842–52.
Sales VM, Ferguson-Smith AC, Patti ME. Epigenetic mechanisms of transmission of metabolic disease across generations. Cell Metab. 2017;25(3):559–71.
Woo M, Patti ME. Diabetes risk begins in utero. Cell Metab. 2008;8(1):5–7.
Gingras V, Hivert MF, Oken E. Early-life exposures and risk of diabetes mellitus and obesity. Curr Diab Rep. 2018;18(10):89.
Stein Z, Susser M. The Dutch famine, 1944–1945, and the reproductive process. I. Effects on six indices at birth. Pediatr Res. 1975;9(2):70–6.
Lumey LH, Stein AD. In utero exposure to famine and subsequent fertility: the Dutch famine birth cohort study. Am J Public Health. 1997;87(12):1962–6.
Ravelli AC, van der Meulen JH, Michels RP, Osmond C, Barker DJ, Hales CN, et al. Glucose tolerance in adults after prenatal exposure to famine. Lancet. 1998;351(9097):173–7.
de Rooij SR, Painter RC, Roseboom TJ, Phillips DI, Osmond C, Barker DJ, et al. Glucose tolerance at age 58 and the decline of glucose tolerance in comparison with age 50 in people prenatally exposed to the Dutch famine. Diabetologia. 2006;49(4):637–43.
Stein AD, Kahn HS, Rundle A, Zybert PA, Van der Pal-de Bruin K, Lumey LH. Anthropometric measures in middle age after exposure to famine during gestation: evidence from the Dutch famine. Am J Clin Nutr. 2007;85(3):869–76.
Barker DJ, Gluckman PD, Godfrey KM, Harding JE, Owens JA, Robinson JS. Fetal nutrition and cardiovascular disease in adult life. Lancet. 1993;341(8850):938–41.
Zimmet P, Shi Z, El-Osta A, Ji L. Epidemic T2DM, early development and epigenetics: implications of the Chinese famine. Nat Rev Endocrinol. 2018;14(12):738–46.
Rich-Edwards JW, Colditz GA, Stampfer MJ, Willett WC, Gillman MW, Hennekens CH, et al. Birthweight and the risk for type 2 diabetes mellitus in adult women. Ann Intern Med. 1999;130(4 Pt 1):278–84.
Xia Q, Cai H, Xiang YB, Zhou P, Li H, Yang G, et al. Prospective cohort studies of birth weight and risk of obesity, diabetes, and hypertension in adulthood among the Chinese population. J Diabetes. 2019;11(1):55–64.
de Lauzon-Guillain B, Balkau B, Charles MA, Romieu I, Boutron-Ruault MC, Clavel-Chapelon F. Birth weight, body silhouette over the life course, and incident diabetes in 91,453 middle-aged women from the French etude Epidemiologique de femmes de la Mutuelle Generale de l'Education Nationale (E3N) cohort. Diabetes Care. 2010;33(2):298–303.
Katanoda K, Noda M, Goto A, Mizunuma H, Lee JS, Hayashi K. Impact of birth weight on adult-onset diabetes mellitus in relation to current body mass index: The Japan Nurses’ Health Study. J Epidemiol. 2017;27(9):428–34.
Yu Z, Han S, Zhu J, Sun X, Ji C, Guo X. Pre-pregnancy body mass index in relation to infant birth weight and offspring overweight/obesity: a systematic review and meta-analysis. PLoS One. 2013;8(4):e61627.
Eriksson JG, Sandboge S, Salonen MK, Kajantie E, Osmond C. Long-term consequences of maternal overweight in pregnancy on offspring later health: findings from the Helsinki birth cohort study. Ann Med. 2014;46(6):434–8.
Schoppa I, Lyass A, Heard-Costa N, de Ferranti SD, Fox C, Gillman MW, et al. Association of maternal prepregnancy weight with offspring adiposity throughout adulthood over 37 years of follow-up. Obesity (Silver Spring). 2019;27(1):137–44.
Kral JG, Biron S, Simard S, Hould FS, Lebel S, Marceau S, et al. Large maternal weight loss from obesity surgery prevents transmission of obesity to children who were followed for 2 to 18 years. Pediatrics. 2006;118(6):e1644–9.
Bunt JC, Tataranni PA, Salbe AD. Intrauterine exposure to diabetes is a determinant of hemoglobin A(1)c and systolic blood pressure in pima Indian children. J Clin Endocrinol Metab. 2005;90(6):3225–9.
Wright CS, Rifas-Shiman SL, Rich-Edwards JW, Taveras EM, Gillman MW, Oken E. Intrauterine exposure to gestational diabetes, child adiposity, and blood pressure. Am J Hypertens. 2009;22(2):215–20.
Pettitt DJ, Lawrence JM, Beyer J, Hillier TA, Liese AD, Mayer-Davis B, et al. Association between maternal diabetes in utero and age at offspring’s diagnosis of type 2 diabetes. Diabetes Care. 2008;31(11):2126–30.
Regnault N, Gillman MW, Rifas-Shiman SL, Eggleston E, Oken E. Sex-specific associations of gestational glucose tolerance with childhood body composition. Diabetes Care. 2013;36(10):3045–53.
Kawasaki M, Arata N, Miyazaki C, Mori R, Kikuchi T, Ogawa Y, et al. Obesity and abnormal glucose tolerance in offspring of diabetic mothers: a systematic review and meta-analysis. PLoS One. 2018;13(1):e0190676.
Fleisch AF, Luttmann-Gibson H, Perng W, Rifas-Shiman SL, Coull BA, Kloog I, et al. Prenatal and early life exposure to traffic pollution and cardiometabolic health in childhood. Pediatr Obes. 2017;12(1):48–57.
Fleisch AF, Rifas-Shiman SL, Koutrakis P, Schwartz JD, Kloog I, Melly S, et al. Prenatal exposure to traffic pollution: associations with reduced fetal growth and rapid infant weight gain. Epidemiology. 2015;26(1):43–50.
Chiu YM, Hsu HL, Wilson A, Coull BA, Pendo MP, Baccarelli A, et al. Prenatal particulate air pollution exposure and body composition in urban preschool children: examining sensitive windows and sex-specific associations. Environ Res. 2017;158:798–805.
Albers L, Sobotzki C, Kuss O, Ajslev T, Batista RF, Bettiol H, et al. Maternal smoking during pregnancy and offspring overweight: is there a dose–response relationship? An individual patient data meta-analysis. Int J Obes. 2018;42(7):1249–64.
Vafeiadi M, Roumeliotaki T, Myridakis A, Chalkiadaki G, Fthenou E, Dermitzaki E, et al. Association of early life exposure to bisphenol A with obesity and cardiometabolic traits in childhood. Environ Res. 2016;146:379–87.
Hoepner LA, Whyatt RM, Widen EM, Hassoun A, Oberfield SE, Mueller NT, et al. Bisphenol A and adiposity in an inner-city birth cohort. Environ Health Perspect. 2016;124(10):1644–50.
Harley KG, Berger K, Rauch S, Kogut K, Claus Henn B, Calafat AM, et al. Association of prenatal urinary phthalate metabolite concentrations and childhood BMI and obesity. Pediatr Res. 2017;82(3):405–15.
Vafeiadi M, Georgiou V, Chalkiadaki G, Rantakokko P, Kiviranta H, Karachaliou M, et al. Association of prenatal exposure to persistent organic pollutants with obesity and cardiometabolic traits in early childhood: the Rhea mother–child cohort (Crete, Greece). Environ Health Perspect. 2015;123(10):1015–21.
Warner M, Ye M, Harley K, Kogut K, Bradman A, Eskenazi B. Prenatal DDT exposure and child adiposity at age 12: the CHAMACOS study. Environ Res. 2017;159:606–12.
Coker E, Chevrier J, Rauch S, Bradman A, Obida M, Crause M, et al. Association between prenatal exposure to multiple insecticides and child body weight and body composition in the VHEMBE south African birth cohort. Environ Int. 2018;113:122–32.
Saenz de Pipaon M, Dorronsoro I, Alvarez-Cuervo L, Butte NF, Madero R, Barrios V, et al. The impact of intrauterine and extrauterine weight gain in premature infants on later body composition. Pediatr Res. 2017;82(4):658–64.
Wang X, Zhu J, Guo C, Shi H, Wu D, Sun F, et al. Growth of infants and young children born small for gestational age: growth restriction accompanied by overweight. J Int Med Res. 2018;46(9):3765–77.
Jabakhanji SB, Boland F, Ward M, Biesma R. Body mass index changes in early childhood. J Pediatr. 2018;202:106–14.
Ibanez L, Suarez L, Lopez-Bermejo A, Diaz M, Valls C, de Zegher F. Early development of visceral fat excess after spontaneous catch-up growth in children with low birth weight. J Clin Endocrinol Metab. 2008;93(3):925–8.
Sebastiani G, Diaz M, Bassols J, Aragones G, Lopez-Bermejo A, de Zegher F, et al. The sequence of prenatal growth restraint and post-natal catch-up growth leads to a thicker intima–media and more pre-peritoneal and hepatic fat by age 3–6 years. Pediatr Obes. 2016;11(4):251–7.
Han DY, Murphy R, Morgan AR, Lam WJ, Thompson JM, Wall CR, et al. Reduced genetic influence on childhood obesity in small for gestational age children. BMC Med Genet. 2013;14:10.
Lindberg J, Norman M, Westrup B, Ohrman T, Domellof M, Berglund SK. Overweight, obesity, and body composition in 3.5- and 7-year-old Swedish children born with marginally low birth weight. J Pediatr. 2015;167(6):1246–52 e3.
Kapral N, Miller SE, Scharf RJ, Gurka MJ, DeBoer MD. Associations between birthweight and overweight and obesity in school-age children. Pediatr Obes. 2018;13(6):333–41.
Kuhle S, Maguire B, Ata N, MacInnis N, Dodds L. Birth weight for gestational age, anthropometric measures, and cardiovascular disease markers in children. J Pediatr. 2017;182:99–106.
Beukers F, Rotteveel J, van Weissenbruch MM, Ganzevoort W, van Goudoever JB, van Wassenaer-Leemhuis AG. Growth throughout childhood of children born growth restricted. Arch Dis Child. 2017;102(8):735–41.
Li P, Yang F, Xiong F, Huo T, Tong Y, Yang S, et al. Nutritional status and risk factors of overweight and obesity for children aged 9–15 years in Chengdu, Southwest China. BMC Public Health. 2012;12:636.
Mullett MD, Cottrell L, Lilly C, Gadikota K, Dong L, Hobbs G, et al. Association between birth characteristics and coronary disease risk factors among fifth graders. J Pediatr. 2014;164(1):78–82.
• Kramer MS, Zhang X, Dahhou M, Yang S, Martin RM, Oken E, et al. Does fetal growth restriction cause later obesity? Pitfalls in analyzing causal mediators as confounders. Am J Epidemiol. 2017;185(7):585–90. The authors apply different statistical approaches to adjusting for childhood BMI to the same dataset, and show that adjustment for current BMI can alter the observed effect of prenatal growth on childhood obesity.
Kramer MS, Martin RM, Bogdanovich N, Vilchuk K, Dahhou M, Oken E. Is restricted fetal growth associated with later adiposity? Observational analysis of a randomized trial. Am J Clin Nutr. 2014;100(1):176–81.
Geserick M, Vogel M, Gausche R, Lipek T, Spielau U, Keller E, et al. Acceleration of BMI in early childhood and risk of sustained obesity. N Engl J Med. 2018;379(14):1303–12.
Meas T, Deghmoun S, Armoogum P, Alberti C, Levy-Marchal C. Consequences of being born small for gestational age on body composition: an 8-year follow-up study. J Clin Endocrinol Metab. 2008;93(10):3804–9.
Melo AS, Bettiol H, Silva AA, Rosa-e-Silva AC, Cardoso VC, Reis RM, et al. Small for gestational age babies are not related to changes in markers of adipose tissue dysfunction during reproductive age. Early Hum Dev. 2014;90(5):231–5.
Crane JD, Yellin SA, Ong FJ, Singh NP, Konyer N, Noseworthy MD, et al. ELBW survivors in early adulthood have higher hepatic, pancreatic and subcutaneous fat. Sci Rep. 2016;6:31560.
Morrison KM, Ramsingh L, Gunn E, Streiner D, Van Lieshout R, Boyle M, et al. Cardiometabolic health in adults Born premature with extremely low birth weight. Pediatrics. 2016;138(4):e20160515.
Beltrand J, Verkauskiene R, Nicolescu R, Sibony O, Gaucherand P, Chevenne D, et al. Adaptive changes in neonatal hormonal and metabolic profiles induced by fetal growth restriction. J Clin Endocrinol Metab. 2008;93(10):4027–32.
Carlsen EM, Renault KM, Norgaard K, Nilas L, Jensen JE, Hyldstrup L, et al. Newborn regional body composition is influenced by maternal obesity, gestational weight gain and the birthweight standard score. Acta Paediatr. 2014;103(9):939–45.
Thurber KA, Dobbins T, Kirk M, Dance P, Banwell C. Early life predictors of increased body mass index among indigenous Australian children. PLoS One. 2015;10(6):e0130039.
Boscaini C, Pellanda LC. Birth weight, current anthropometric markers, and high sensitivity C-reactive protein in Brazilian school children. J Obes. 2015;2015:846376.
Prioreschi A, Munthali RJ, Kagura J, Said-Mohamed R, De Lucia Rolfe E, Micklesfield LK, et al. The associations between adult body composition and abdominal adiposity outcomes, and relative weight gain and linear growth from birth to age 22 in the birth to twenty plus cohort, South Africa. PLoS One. 2018;13(1):e0190483.
Rillamas-Sun E, Sowers MR, Harlow SD, Randolph JF Jr. The relationship of birth weight with longitudinal changes in body composition in adult women. Obesity (Silver Spring). 2012;20(2):463–5.
West J, Santorelli G, Whincup PH, Smith L, Sattar NA, Cameron N, et al. Association of maternal exposures with adiposity at age 4/5 years in white British and Pakistani children: findings from the Born in Bradford study. Diabetologia. 2018;61(1):242–52.
Gademan MG, Vermeulen M, Oostvogels AJ, Roseboom TJ, Visscher TL, van Eijsden M, et al. Maternal prepregancy BMI and lipid profile during early pregnancy are independently associated with offspring’s body composition at age 5–6 years: the ABCD study. PLoS One. 2014;9(4):e94594.
Pirkola J, Pouta A, Bloigu A, Hartikainen AL, Laitinen J, Jarvelin MR, et al. Risks of overweight and abdominal obesity at age 16 years associated with prenatal exposures to maternal prepregnancy overweight and gestational diabetes mellitus. Diabetes Care. 2010;33(5):1115–21.
Eriksson JG, Sandboge S, Salonen M, Kajantie E, Osmond C. Maternal weight in pregnancy and offspring body composition in late adulthood: findings from the Helsinki Birth Cohort Study (HBCS). Ann Med. 2015;47(2):94–9.
Zhu Y, Olsen SF, Mendola P, Yeung EH, Vaag A, Bowers K, et al. Growth and obesity through the first 7 y of life in association with levels of maternal glycemia during pregnancy: a prospective cohort study. Am J Clin Nutr. 2016;103(3):794–800.
Aris IM, Soh SE, Tint MT, Saw SM, Rajadurai VS, Godfrey KM, et al. Associations of gestational glycemia and prepregnancy adiposity with offspring growth and adiposity in an Asian population. Am J Clin Nutr. 2015;102(5):1104–12.
Thaware PK, McKenna S, Patterson CC, Hadden DR, Pettitt DJ, McCance DR. Untreated mild hyperglycemia during pregnancy and anthropometric measures of obesity in offspring at age 5–7 years. Diabetes Care. 2015;38(9):1701–6.
Lowe WL Jr, Lowe LP, Kuang A, Catalano PM, Nodzenski M, Talbot O, et al. Maternal glucose levels during pregnancy and childhood adiposity in the hyperglycemia and adverse pregnancy outcome follow-up study. Diabetologia. 2019;62(4):598–610.
Carlsen EM, Renault KM, Norgaard K, Nilas L, Jensen JE, Hitz MF, et al. Glucose tolerance in obese pregnant women determines newborn fat mass. Acta Obstet Gynecol Scand. 2016;95(4):429–35.
Kearney M, Perron J, Marc I, Weisnagel SJ, Tchernof A, Robitaille J. Association of prenatal exposure to gestational diabetes with offspring body composition and regional body fat distribution. Clin Obes. 2018;8(2):81–7.
Grunnet LG, Hansen S, Hjort L, Madsen CM, Kampmann FB, Thuesen ACB, et al. Adiposity, dysmetabolic traits, and earlier onset of female puberty in adolescent offspring of women with gestational diabetes mellitus: a clinical study within the Danish National Birth Cohort. Diabetes Care. 2017;40(12):1746–55.
•• Lowe WL Jr, Scholtens DM, Lowe LP, Kuang A, Nodzenski M, Talbot O, et al. Association of gestational diabetes with maternal disorders of glucose metabolism and childhood adiposity. JAMA. 2018;320(10):1005–16. This large multi-national cohort study shows a strong effect of maternal hyperglycemia on childhood adiposity. Strengths include the large and diverse study sample, and adjustment for numerous potential confounders.
Lohse Z, Knorr S, Bytoft B, Clausen TD, Jensen RB, Oturai P, et al. Differential effects of age and sex on insulin sensitivity and body composition in adolescent offspring of women with type 1 diabetes: results from the EPICOM study. Diabetologia. 2018;61(1):210–9.
Mughal MZ, Eelloo J, Roberts SA, Maresh M, Ward KA, Ashby R, et al. Body composition and bone status of children born to mothers with type 1 diabetes mellitus. Arch Dis Child. 2010;95(4):281–5.
Biosca M, Rodriguez G, Ventura P, Samper MP, Labayen I, Collado MP, et al. Central adiposity in children born small and large for gestational age. Nutr Hosp. 2011;26(5):971–6.
Rockenbach G, Luft VC, Mueller NT, Duncan BB, Stein MC, Vigo A, et al. Sex-specific associations of birth weight with measures of adiposity in mid-to-late adulthood: the Brazilian longitudinal study of adult health (ELSA-Brasil). Int J Obes. 2016;40(8):1286–91.
Araujo de Franca GV, De Lucia Rolfe E, Horta BL, Gigante DP, Yudkin JS, Ong KK, et al. Associations of birth weight, linear growth and relative weight gain throughout life with abdominal fat depots in adulthood: the 1982 Pelotas (Brazil) birth cohort study. Int J Obes. 2016;40(1):14–21.
Stansfield BK, Fain ME, Bhatia J, Gutin B, Nguyen JT, Pollock NK. Nonlinear relationship between birth weight and visceral fat in adolescents. J Pediatr. 2016;174:185–92.
Morgen CS, Andersen PK, Mortensen LH, Howe LD, Rasmussen M, Due P, et al. Socioeconomic disparities in birth weight and body mass index during infancy through age 7 years: a study within the Danish National Birth Cohort. BMJ Open. 2017;7(1):e011781.
Morgan AR, Thompson JM, Murphy R, Black PN, Lam WJ, Ferguson LR, et al. Obesity and diabetes genes are associated with being born small for gestational age: results from the Auckland Birthweight Collaborative study. BMC Med Genet. 2010;11:125.
Horikoshi M, Beaumont RN, Day FR, Warrington NM, Kooijman MN, Fernandez-Tajes J, et al. Genome-wide associations for birth weight and correlations with adult disease. Nature. 2016;538(7624):248–52.
Jelenkovic A, Yokoyama Y, Sund R, Pietilainen KH, Hur YM, Willemsen G, et al. Association between birthweight and later body mass index: an individual-based pooled analysis of 27 twin cohorts participating in the CODATwins project. Int J Epidemiol. 2017;46(5):1488–98.
Kuhle S, Allen AC, Veugelers PJ. Prevention potential of risk factors for childhood overweight. Can J Public Health. 2010;101(5):365–8.
Patro Golab B, Santos S, Voerman E, Lawlor DA, Jaddoe VWV, Gaillard R, et al. Influence of maternal obesity on the association between common pregnancy complications and risk of childhood obesity: an individual participant data meta-analysis. Lancet Child Adolesc Health. 2018;2(11):812–21.
Voerman E, Santos S, Patro Golab B, Amiano P, Ballester F, Barros H, et al. Maternal body mass index, gestational weight gain, and the risk of overweight and obesity across childhood: an individual participant data meta-analysis. PLoS Med. 2019;16(2):e1002744.
McCloskey K, Ponsonby AL, Collier F, Allen K, Tang MLK, Carlin JB, et al. The association between higher maternal pre-pregnancy body mass index and increased birth weight, adiposity and inflammation in the newborn. Pediatr Obes. 2018;13(1):46–53.
Zhang C, Hediger ML, Albert PS, Grewal J, Sciscione A, Grobman WA, et al. Association of maternal obesity with longitudinal ultrasonographic measures of fetal growth: findings from the NICHD fetal growth studies—singletons. JAMA Pediatr. 2018;172(1):24–31.
Sewell MF, Huston-Presley L, Super DM, Catalano P. Increased neonatal fat mass, not lean body mass, is associated with maternal obesity. Am J Obstet Gynecol. 2006;195(4):1100–3.
Guenard F, Deshaies Y, Cianflone K, Kral JG, Marceau P, Vohl MC. Differential methylation in glucoregulatory genes of offspring born before vs. after maternal gastrointestinal bypass surgery. Proc Natl Acad Sci U S A. 2013;110(28):11439–44.
Tyrrell J, Richmond RC, Palmer TM, Feenstra B, Rangarajan J, Metrustry S, et al. Genetic evidence for causal relationships between maternal obesity-related traits and birth weight. JAMA. 2016;315(11):1129–40.
Li A, Robiou-du-Pont S, Anand SS, Morrison KM, McDonald SD, Atkinson SA, et al. Parental and child genetic contributions to obesity traits in early life based on 83 loci validated in adults: the FAMILY study. Pediatr Obes. 2018;13(3):133–40.
Richmond RC, Timpson NJ, Felix JF, Palmer T, Gaillard R, McMahon G, et al. Using genetic variation to explore the causal effect of maternal pregnancy adiposity on future offspring adiposity: a Mendelian randomisation study. PLoS Med. 2017;14(1):e1002221.
Group HSCR, Metzger BE, Lowe LP, Dyer AR, Trimble ER, Chaovarindr U, et al. Hyperglycemia and adverse pregnancy outcomes. N Engl J Med. 2008;358(19):1991–2002.
Group HSCR. Hyperglycemia and Adverse Pregnancy Outcome (HAPO) study: associations with neonatal anthropometrics. Diabetes. 2009;58(2):453–9.
Raghavan S, Zhang W, Yang IV, Lange LA, Lange EM, Fingerlin TE, et al. Association between gestational diabetes mellitus exposure and childhood adiposity is not substantially explained by offspring genetic risk of obesity. Diabet Med. 2017;34(12):1696–700.
Burrows R, Correa-Burrows P, Reyes M, Blanco E, Albala C, Gahagan S. Low muscle mass is associated with cardiometabolic risk regardless of nutritional status in adolescents: a cross-sectional study in a Chilean birth cohort. Pediatr Diabetes. 2017;18(8):895–902.
Wells JC, Chomtho S, Fewtrell MS. Programming of body composition by early growth and nutrition. Proc Nutr Soc. 2007;66(3):423–34.
Barr JG, Veena SR, Kiran KN, Wills AK, Winder NR, Kehoe S, et al. The relationship of birthweight, muscle size at birth and post-natal growth to grip strength in 9-year-old Indian children: findings from the Mysore Parthenon study. J Dev Orig Health Dis. 2010;1(5):329–37.
Sayer AA, Syddall HE, Gilbody HJ, Dennison EM, Cooper C. Does sarcopenia originate in early life? Findings from the Hertfordshire cohort study. J Gerontol A Biol Sci Med Sci. 2004;59(9):M930–4.
Bielemann RM, Gigante DP, Horta BL. Birth weight, intrauterine growth restriction and nutritional status in childhood in relation to grip strength in adults: from the 1982 Pelotas (Brazil) birth cohort. Nutrition. 2016;32(2):228–35.
Stutte S, Gohlke B, Peiler A, Schreiner F, Born M, Bartmann P, et al. Impact of early nutrition on body composition in children aged 9.5 years born with extremely low birth weight. Nutrients. 2017;9(2):E124.
Callreus M, McGuigan F, Akesson K. Birth weight is more important for peak bone mineral content than for bone density: the PEAK-25 study of 1,061 young adult women. Osteoporos Int. 2013;24(4):1347–55.
Kitazawa S, Itabashi K, Umeda Y, Inoue M, Nishioka T. Growth and bone mineralization in small-for-gestational-age preterm infants. Pediatr Int. 2014;56(1):67–71.
Sepulveda C, Urquidi C, Pittaluga E, Iniguez G, Avila A, Carrasco F, et al. Differences in body composition and resting energy expenditure in childhood in preterm children born with very low birth weight. Horm Res Paediatr. 2013;79(6):347–55.
Bann D, Wills A, Cooper R, Hardy R, Aihie Sayer A, Adams J, et al. Birth weight and growth from infancy to late adolescence in relation to fat and lean mass in early old age: findings from the MRC National Survey of health and development. Int J Obes. 2014;38(1):69–75.
Dulloo AG, Jacquet J, Seydoux J, Montani JP. The thrifty ‘catch-up fat’ phenotype: its impact on insulin sensitivity during growth trajectories to obesity and metabolic syndrome. Int J Obes. 2006;30(Suppl 4):S23–35.
Beltrand J, Nicolescu R, Kaguelidou F, Verkauskiene R, Sibony O, Chevenne D, et al. Catch-up growth following fetal growth restriction promotes rapid restoration of fat mass but without metabolic consequences at one year of age. PLoS One. 2009;4(4):e5343.
Leunissen RW, Stijnen T, Hokken-Koelega AC. Influence of birth size on body composition in early adulthood: the programming factors for growth and metabolism (PROGRAM)-study. Clin Endocrinol. 2009;70(2):245–51.
de Zegher F, Perez-Cruz M, Diaz M, Gomez-Roig MD, Lopez-Bermejo A, Ibanez L. Less myostatin and more lean mass in large-born infants from nondiabetic mothers. J Clin Endocrinol Metab. 2014;99(11):E2367–71.
Zou T, He D, Yu B, Yu J, Mao X, Zheng P, et al. Moderately increased maternal dietary energy intake delays foetal skeletal muscle differentiation and maturity in pigs. Eur J Nutr. 2016;55(4):1777–87.
Horowitz MC, Berry R, Holtrup B, Sebo Z, Nelson T, Fretz JA, et al. Bone marrow adipocytes. Adipocyte. 2017;6(3):193–204.
Zhou BO, Yue R, Murphy MM, Peyer JG, Morrison SJ. Leptin-receptor-expressing mesenchymal stromal cells represent the main source of bone formed by adult bone marrow. Cell Stem Cell. 2014;15(2):154–68.
Ambrosi TH, Scialdone A, Graja A, Gohlke S, Jank AM, Bocian C, et al. Adipocyte accumulation in the bone marrow during obesity and aging impairs stem cell-based hematopoietic and bone regeneration. Cell Stem Cell. 2017;20(6):771–84 e6.
Wood CL, Stenson C, Embleton N. The developmental origins of osteoporosis. Curr Genomics. 2015;16(6):411–8.
Christoffersen T, Ahmed LA, Daltveit AK, Dennison EM, Evensen EK, Furberg AS, et al. The influence of birth weight and length on bone mineral density and content in adolescence: the Tromso study, fit futures. Arch Osteoporos. 2017;12(1):54.
Balasuriya CND, Evensen KAI, Mosti MP, Brubakk AM, Jacobsen GW, Indredavik MS, et al. Peak bone mass and bone microarchitecture in adults born with low birth weight preterm or at term: a cohort study. J Clin Endocrinol Metab. 2017;102(7):2491–500.
Fricke O, Semler O, Stabrey A, Tutlewski B, Remer T, Herkenrath P, et al. High and low birth weight and its implication for growth and bone development in childhood and adolescence. J Pediatr Endocrinol Metab. 2009;22(1):19–30.
Heppe DH, Medina-Gomez C, de Jongste JC, Raat H, Steegers EA, Hofman A, et al. Fetal and childhood growth patterns associated with bone mass in school-age children: the generation R study. J Bone Miner Res. 2014;29(12):2584–93.
Longhi S, Mercolini F, Carloni L, Nguyen L, Fanolla A, Radetti G. Prematurity and low birth weight lead to altered bone geometry, strength, and quality in children. J Endocrinol Investig. 2015;38(5):563–8.
Schushan-Eisen I, Cohen M, Leibovitch L, Maayan-Metzger A, Strauss T. Bone density among infants of gestational diabetic mothers and macrosomic neonates. Matern Child Health J. 2015;19(3):578–82.
Macdonald-Wallis C, Tobias JH, Smith GD, Lawlor DA. Relation of maternal prepregnancy body mass index with offspring bone mass in childhood: is there evidence for an intrauterine effect? Am J Clin Nutr. 2010;92(4):872–80.
Regev RH, Dolfin T, Eliakim A, Arnon S, Bauer S, Nemet D, et al. Bone speed of sound in infants of mothers with gestational diabetes mellitus. J Pediatr Endocrinol Metab. 2004;17(8):1083–8.
Lapillonne A, Guerin S, Braillon P, Claris O, Delmas PD, Salle BL. Diabetes during pregnancy does not alter whole body bone mineral content in infants. J Clin Endocrinol Metab. 1997;82(12):3993–7.
Akcakus M, Koklu E, Kurtoglu S, Kula M, Koklu SS. The relationship among intrauterine growth, insulinlike growth factor I (IGF-I), IGF-binding protein-3, and bone mineral status in newborn infants. Am J Perinatol. 2006;23(8):473–80.
Harvey NC, Mahon PA, Robinson SM, Nisbet CE, Javaid MK, Crozier SR, et al. Different indices of fetal growth predict bone size and volumetric density at 4 years of age. J Bone Miner Res. 2010;25(4):920–7.
Devlin MJ, Bouxsein ML. Influence of pre- and peri-natal nutrition on skeletal acquisition and maintenance. Bone. 2012;50(2):444–51.
Martinez-Mesa J, Restrepo-Mendez MC, Gonzalez DA, Wehrmeister FC, Horta BL, Domingues MR, et al. Life-course evidence of birth weight effects on bone mass: systematic review and meta-analysis. Osteoporos Int. 2013;24(1):7–18.
Hovi P, Andersson S, Jarvenpaa AL, Eriksson JG, Strang-Karlsson S, Kajantie E, et al. Decreased bone mineral density in adults born with very low birth weight: a cohort study. PLoS Med. 2009;6(8):e1000135.
Wallace JM, Milne JS, Aitken RP, Horgan GW, Adam CL. Ovine prenatal growth restriction impacts glucose metabolism and body composition throughout life in both sexes. Reproduction. 2018;156(2):103–19.
Devlin MJ, Grasemann C, Cloutier AM, Louis L, Alm C, Palmert MR, et al. Maternal perinatal diet induces developmental programming of bone architecture. J Endocrinol. 2013;217(1):69–81.
Namgung R, Tsang RC. Factors affecting newborn bone mineral content: in utero effects on newborn bone mineralization. Proc Nutr Soc. 2000;59(1):55–63.
Renault KM, Carlsen EM, Norgaard K, Nilas L, Pryds O, Secher NJ, et al. Intake of carbohydrates during pregnancy in obese women is associated with fat mass in the newborn offspring. Am J Clin Nutr. 2015;102(6):1475–81.
Chen LW, Tint MT, Fortier MV, Aris IM, Bernard JY, Colega M, et al. Maternal macronutrient intake during pregnancy is associated with neonatal abdominal adiposity: the Growing Up in Singapore Towards healthy Outcomes (GUSTO) study. J Nutr. 2016;146(8):1571–9.
Fernandez-Barres S, Romaguera D, Valvi D, Martinez D, Vioque J, Navarrete-Munoz EM, et al. Mediterranean dietary pattern in pregnant women and offspring risk of overweight and abdominal obesity in early childhood: the INMA birth cohort study. Pediatr Obes. 2016;11(6):491–9.
Moore BF, Sauder KA, Starling AP, Hebert JR, Shivappa N, Ringham BM, et al. Proinflammatory diets during pregnancy and neonatal adiposity in the Healthy Start Study. J Pediatr. 2018;195:121–7 e2.
Shapiro AL, Kaar JL, Crume TL, Starling AP, Siega-Riz AM, Ringham BM, et al. Maternal diet quality in pregnancy and neonatal adiposity: the Healthy Start Study. Int J Obes. 2016;40(7):1056–62.
Crozier SR, Harvey NC, Inskip HM, Godfrey KM, Cooper C, Robinson SM, et al. Maternal vitamin D status in pregnancy is associated with adiposity in the offspring: findings from the Southampton Women’s Survey. Am J Clin Nutr. 2012;96(1):57–63.
Morales E, Rodriguez A, Valvi D, Iniguez C, Esplugues A, Vioque J, et al. Deficit of vitamin D in pregnancy and growth and overweight in the offspring. Int J Obes. 2015;39(1):61–8.
Ong YL, Quah PL, Tint MT, Aris IM, Chen LW, van Dam RM, et al. The association of maternal vitamin D status with infant birth outcomes, postnatal growth and adiposity in the first 2 years of life in a multi-ethnic Asian population: the Growing Up in Singapore Towards healthy Outcomes (GUSTO) cohort study. Br J Nutr. 2016;116(4):621–31.
Santamaria C, Bi WG, Leduc L, Tabatabaei N, Jantchou P, Luo ZC, et al. Prenatal vitamin D status and offspring’s growth, adiposity and metabolic health: a systematic review and meta-analysis. Br J Nutr. 2018;119(3):310–9.
Prentice KJ, Luu L, Allister EM, Liu Y, Jun LS, Sloop KW, et al. The furan fatty acid metabolite CMPF is elevated in diabetes and induces beta cell dysfunction. Cell Metab. 2014;19(4):653–66.
Donahue SM, Rifas-Shiman SL, Gold DR, Jouni ZE, Gillman MW, Oken E. Prenatal fatty acid status and child adiposity at age 3 y: results from a US pregnancy cohort. Am J Clin Nutr. 2011;93(4):780–8.
Isganaitis E, Rifas-Shiman SL, Oken E, Dreyfuss JM, Gall W, Gillman MW, et al. Associations of cord blood metabolites with early childhood obesity risk. Int J Obes. 2015;39(7):1041–8.
van Lee L, Tint MT, Aris IM, Quah PL, Fortier MV, Lee YS, et al. Prospective associations of maternal betaine status with offspring weight and body composition at birth: the Growing Up in Singapore Towards healthy Outcomes (GUSTO) cohort study. Am J Clin Nutr. 2016;104(5):1327–33.
Brei C, Stecher L, Much D, Karla MT, Amann-Gassner U, Shen J, et al. Reduction of the n-6:n-3 long-chain PUFA ratio during pregnancy and lactation on offspring body composition: follow-up results from a randomized controlled trial up to 5 y of age. Am J Clin Nutr. 2016;103(6):1472–81.
Foster BA, Escaname E, Powell TL, Larsen B, Siddiqui SK, Menchaca J, et al. Randomized controlled trial of DHA supplementation during pregnancy: child adiposity outcomes. Nutrients. 2017;9(6):E566.
Temples HS, Willoughby D, Holaday B, Rogers CR, Wueste D, Bridges W, et al. Breastfeeding and growth of children in the peri/postnatal epigenetic twins study (PETS): theoretical epigenetic mechanisms. J Hum Lact. 2016;32(3):481–8.
Bell KA, Wagner CL, Feldman HA, Shypailo RJ, Belfort MB. Associations of infant feeding with trajectories of body composition and growth. Am J Clin Nutr. 2017;106(2):491–8.
Li C, Kaur H, Choi WS, Huang TT, Lee RE, Ahluwalia JS. Additive interactions of maternal prepregnancy BMI and breast-feeding on childhood overweight. Obes Res. 2005;13(2):362–71.
Fields DA, Schneider CR, Pavela G. A narrative review of the associations between six bioactive components in breast milk and infant adiposity. Obesity (Silver Spring). 2016;24(6):1213–21.
Andreas NJ, Hyde MJ, Gale C, Parkinson JR, Jeffries S, Holmes E, et al. Effect of maternal body mass index on hormones in breast milk: a systematic review. PLoS One. 2014;9(12):e115043.
Goran MI, Martin AA, Alderete TL, Fujiwara H, Fields DA. Fructose in breast milk is positively associated with infant body composition at 6 months of age. Nutrients. 2017;9(2):E146.
Alderete TL, Autran C, Brekke BE, Knight R, Bode L, Goran MI, et al. Associations between human milk oligosaccharides and infant body composition in the first 6 mo of life. Am J Clin Nutr. 2015;102(6):1381–8.
Isganaitis E, Venditti S, Matthews TJ, Lerin C, Demerath EW, Fields DA. Maternal obesity and the human milk metabolome: associations with infant body composition and postnatal weight gain. Am J Clin Nutr. 2019.
Oben JA, Mouralidarane A, Samuelsson AM, Matthews PJ, Morgan ML, McKee C, et al. Maternal obesity during pregnancy and lactation programs the development of offspring non-alcoholic fatty liver disease in mice. J Hepatol. 2010;52(6):913–20.
de Los Rios EA, Ruiz-Herrera X, Tinoco-Pantoja V, Lopez-Barrera F, de la Martinez Escalera G, Clapp C, et al. Impaired prolactin actions mediate altered offspring metabolism induced by maternal high-fat feeding during lactation. FASEB J. 2018;32(6):3457–70.
Thomas N, Grunnet LG, Poulsen P, Christopher S, Spurgeon R, Inbakumari M, et al. Born with low birth weight in rural southern India: what are the metabolic consequences 20 years later? Eur J Endocrinol. 2012;166(4):647–55.
Ester WA, Jansen PW, Hoek HW, Verhulst FC, Jaddoe VW, Marques AH, et al. Fetal size and eating behaviour in childhood: a prospective cohort study. Int J Epidemiol. 2018;48:124–33.
Derks IPM, Hivert MF, Rifas-Shiman SL, Gingras V, Young JG, Jansen PW, et al. Associations of prenatal exposure to impaired glucose tolerance with eating in the absence of hunger in early adolescence. Int J Obes 2019.
Shapiro ALB, Sauder KA, Tregellas JR, Legget KT, Gravitz SL, Ringham BM, et al. Exposure to maternal diabetes in utero and offspring eating behavior: the EPOCH study. Appetite. 2017;116:610–5.
Vogt MC, Paeger L, Hess S, Steculorum SM, Awazawa M, Hampel B, et al. Neonatal insulin action impairs hypothalamic neurocircuit formation in response to maternal high-fat feeding. Cell. 2014;156(3):495–509.
Melo AM, Benatti RO, Ignacio-Souza LM, Okino C, Torsoni AS, Milanski M, et al. Hypothalamic endoplasmic reticulum stress and insulin resistance in offspring of mice dams fed high-fat diet during pregnancy and lactation. Metabolism. 2014;63(5):682–92.
Vickers MH, Gluckman PD, Coveny AH, Hofman PL, Cutfield WS, Gertler A, et al. Neonatal leptin treatment reverses developmental programming. Endocrinology. 2005;146(10):4211–6.
Bouret SG, Draper SJ, Simerly RB. Trophic action of leptin on hypothalamic neurons that regulate feeding. Science. 2004;304(5667):108–10.
Kajantie E, Strang-Karlsson S, Hovi P, Raikkonen K, Pesonen AK, Heinonen K, et al. Adults born at very low birth weight exercise less than their peers born at term. J Pediatr. 2010;157(4):610–6, 6 e1.
Kaseva N, Wehkalampi K, Strang-Karlsson S, Salonen M, Pesonen AK, Raikkonen K, et al. Lower conditioning leisure-time physical activity in young adults born preterm at very low birth weight. PLoS One. 2012;7(2):e32430.
Cadenas-Sanchez C, Henriksson P, Henriksson H, Delisle Nystrom C, Pomeroy J, Ruiz JR, et al. Parental body mass index and its association with body composition, physical fitness and lifestyle factors in their 4-year-old children: results from the MINISTOP trial. Eur J Clin Nutr. 2017;71(10):1200–5.
Ortega FB, Ruiz JR, Hurtig-Wennlof A, Meirhaeghe A, Gonzalez-Gross M, Moreno LA, et al. Physical activity attenuates the effect of low birth weight on insulin resistance in adolescents: findings from two observational studies. Diabetes. 2011;60(9):2295–9.
Li LJ, Rifas-Shiman SL, Aris IM, Young JG, Mantzoros C, Hivert MF, et al. Associations of maternal and cord blood adipokines with offspring adiposity in Project Viva: is there an interaction with child age? Int J Obes. 2018;42(4):608–17.
Castro NP, Euclydes VV, Simoes FA, Vaz-de-Lima LR, De Brito CA, Luzia LA, et al. The relationship between maternal plasma leptin and adiponectin concentrations and newborn adiposity. Nutrients. 2017;9(3):E182.
Englich B, Herberth G, Rolle-Kampczyk U, Trump S, Roder S, Borte M, et al. Maternal cytokine status may prime the metabolic profile and increase risk of obesity in children. Int J Obes. 2017;41(9):1440–6.
Hernandez MI, Rossel K, Pena V, Cavada G, Avila A, Iniguez G, et al. Leptin and IGF-I/II during the first weeks of life determine body composition at 2 years in infants born with very low birth weight. J Pediatr Endocrinol Metab. 2012;25(9–10):951–5.
de Kort SW, Willemsen RH, van der Kaay DC, Hokken-Koelega AC. The effect of growth hormone treatment on metabolic and cardiovascular risk factors is similar in preterm and term short, small for gestational age children. Clin Endocrinol. 2009;71(1):65–73.
Ibanez L, Lopez-Bermejo A, Diaz M, Jaramillo A, Marin S, de Zegher F. Growth hormone therapy in short children born small for gestational age: effects on abdominal fat partitioning and circulating follistatin and high-molecular-weight adiponectin. J Clin Endocrinol Metab. 2010;95(5):2234–9.
Lem AJ, van der Kaay DC, Hokken-Koelega AC. Bone mineral density and body composition in short children born SGA during growth hormone and gonadotropin releasing hormone analog treatment. J Clin Endocrinol Metab. 2013;98(1):77–86.
Breukhoven PE, Kerkhof GF, van Dijk M, Hokken-Koelega AC. Long-term impact of GH treatment during childhood on body composition and fat distribution in young adults born SGA. J Clin Endocrinol Metab. 2011;96(12):3710–6.
Sanchez-Infantes D, Gallego-Escuredo JM, Diaz M, Aragones G, Sebastiani G, Lopez-Bermejo A, et al. Circulating FGF19 and FGF21 surge in early infancy from infra- to supra-adult concentrations. Int J Obes. 2015;39(5):742–6.
Diaz M, Bassols J, Aragones G, Mazarico E, Lopez-Bermejo A, Ibanez L. Decreased placental expression of pre-adipocyte factor-1 in children born small-for-gestational-age: association to early postnatal weight gain. Placenta. 2013;34(4):331–4.
Jimenez-Chillaron JC, Isganaitis E, Charalambous M, Gesta S, Pentinat-Pelegrin T, Faucette RR, et al. Intergenerational transmission of glucose intolerance and obesity by in utero undernutrition in mice. Diabetes. 2009;58(2):460–8.
Lecoutre S, Deracinois B, Laborie C, Eberle D, Guinez C, Panchenko PE, et al. Depot- and sex-specific effects of maternal obesity in offspring’s adipose tissue. J Endocrinol. 2016;230(1):39–53.
Borengasser SJ, Zhong Y, Kang P, Lindsey F, Ronis MJ, Badger TM, et al. Maternal obesity enhances white adipose tissue differentiation and alters genome-scale DNA methylation in male rat offspring. Endocrinology. 2013;154(11):4113–25.
Wahl S, Drong A, Lehne B, Loh M, Scott WR, Kunze S, et al. Epigenome-wide association study of body mass index, and the adverse outcomes of adiposity. Nature. 2017;541(7635):81–6.
Ramos-Lopez O, Riezu-Boj JI, Milagro FI, Martinez JA, Project M. DNA methylation signatures at endoplasmic reticulum stress genes are associated with adiposity and insulin resistance. Mol Genet Metab. 2018;123(1):50–8.
Livshits G, Gao F, Malkin I, Needhamsen M, Xia Y, Yuan W, et al. Contribution of heritability and epigenetic factors to skeletal muscle mass variation in United Kingdom twins. J Clin Endocrinol Metab. 2016;101(6):2450–9.
van Dijk SJ, Peters TJ, Buckley M, Zhou J, Jones PA, Gibson RA, et al. DNA methylation in blood from neonatal screening cards and the association with BMI and insulin sensitivity in early childhood. Int J Obes. 2018;42(1):28–35.
Godfrey KM, Sheppard A, Gluckman PD, Lillycrop KA, Burdge GC, McLean C, et al. Epigenetic gene promoter methylation at birth is associated with child’s later adiposity. Diabetes. 2011;60(5):1528–34.
Harvey NC, Lillycrop KA, Garratt E, Sheppard A, McLean C, Burdge G, et al. Evaluation of methylation status of the eNOS promoter at birth in relation to childhood bone mineral content. Calcif Tissue Int. 2012;90(2):120–7.
Harvey NC, Sheppard A, Godfrey KM, McLean C, Garratt E, Ntani G, et al. Childhood bone mineral content is associated with methylation status of the RXRA promoter at birth. J Bone Miner Res. 2014;29(3):600–7.
Rzehak P, Covic M, Saffery R, Reischl E, Wahl S, Grote V, et al. DNA-methylation and body composition in preschool children: epigenome-wide-analysis in the European Childhood Obesity Project (CHOP)-Study. Sci Rep. 2017;7(1):14349.
Kresovich JK, Zheng Y, Cardenas A, Joyce BT, Rifas-Shiman SL, Oken E, et al. Cord blood DNA methylation and adiposity measures in early and mid-childhood. Clin Epigenetics. 2017;9:86.
Diaz M, Garcia C, Sebastiani G, de Zegher F, Lopez-Bermejo A, Ibanez L. Placental and cord blood methylation of genes involved in energy homeostasis: association with fetal growth and neonatal body composition. Diabetes. 2017;66(3):779–84.
Lin X, Lim IY, Wu Y, Teh AL, Chen L, Aris IM, et al. Developmental pathways to adiposity begin before birth and are influenced by genotype, prenatal environment and epigenome. BMC Med. 2017;15(1):50.
Sharp GC, Lawlor DA, Richmond RC, Fraser A, Simpkin A, Suderman M, et al. Maternal pre-pregnancy BMI and gestational weight gain, offspring DNA methylation and later offspring adiposity: findings from the Avon Longitudinal Study of Parents and Children. Int J Epidemiol. 2015;44(4):1288–304.
Lillycrop KA, Garratt ES, Titcombe P, Melton PE, Murray RJS, Barton SJ, et al. Differential SLC6A4 methylation: a predictive epigenetic marker of adiposity from birth to adulthood. Int J Obes. 2019.
Finer S, Mathews C, Lowe R, Smart M, Hillman S, Foo L, et al. Maternal gestational diabetes is associated with genome-wide DNA methylation variation in placenta and cord blood of exposed offspring. Hum Mol Genet. 2015;24(11):3021–9.
Yang IV, Zhang W, Davidson EJ, Fingerlin TE, Kechris K, Dabelea D. Epigenetic marks of in utero exposure to gestational diabetes and childhood adiposity outcomes: the EPOCH study. Diabet Med. 2018;35(5):612–20.
Houde AA, St-Pierre J, Hivert MF, Baillargeon JP, Perron P, Gaudet D, et al. Placental lipoprotein lipase DNA methylation levels are associated with gestational diabetes mellitus and maternal and cord blood lipid profiles. J Dev Orig Health Dis. 2014;5(2):132–41.
Quilter CR, Cooper WN, Cliffe KM, Skinner BM, Prentice PM, Nelson L, et al. Impact on offspring methylation patterns of maternal gestational diabetes mellitus and intrauterine growth restraint suggest common genes and pathways linked to subsequent type 2 diabetes risk. FASEB J. 2014;28(11):4868–79.
Cianfarani S. Foetal origins of adult diseases: just a matter of stem cell number? Med Hypotheses. 2003;61(3):401–4.
Hemberger M, Dean W, Reik W. Epigenetic dynamics of stem cells and cell lineage commitment: digging Waddington’s canal. Nat Rev Mol Cell Biol. 2009;10(8):526–37.
Woo M, Isganaitis E, Cerletti M, Fitzpatrick C, Wagers AJ, Jimenez-Chillaron J, et al. Early life nutrition modulates muscle stem cell number: implications for muscle mass and repair. Stem Cells Dev. 2011;20(10):1763–9.
Broholm C, Olsson AH, Perfilyev A, Hansen NS, Schrolkamp M, Strasko KS, et al. Epigenetic programming of adipose-derived stem cells in low birthweight individuals. Diabetologia. 2016;59(12):2664–73.
Bossolasco P, Montemurro T, Cova L, Zangrossi S, Calzarossa C, Buiatiotis S, et al. Molecular and phenotypic characterization of human amniotic fluid cells and their differentiation potential. Cell Res. 2006;16(4):329–36.
Troyer DL, Weiss ML. Wharton’s jelly-derived cells are a primitive stromal cell population. Stem Cells. 2008;26(3):591–9.
Seshareddy K, Troyer D, Weiss ML. Method to isolate mesenchymal-like cells from Wharton’s jelly of umbilical cord. Methods Cell Biol. 2008;86:101–19.
Sukarieh R, Joseph R, Leow SC, Li Y, Loffler M, Aris IM, et al. Molecular pathways reflecting poor intrauterine growth are found in Wharton’s jelly-derived mesenchymal stem cells. Hum Reprod. 2014;29(10):2287–301.
Tan PY, Chang CW, Duan K, Poidinger M, Ng KL, Chong YS, et al. E2F1 orchestrates transcriptomics and oxidative metabolism in Wharton’s jelly-derived mesenchymal stem cells from growth-restricted infants. PLoS One. 2016;11(9):e0163035.
Joseph R, Poschmann J, Sukarieh R, Too PG, Julien SG, Xu F, et al. ACSL1 is associated with fetal programming of insulin sensitivity and cellular lipid content. Mol Endocrinol. 2015;29(6):909–20.
Iaffaldano L, Nardelli C, Raia M, Mariotti E, Ferrigno M, Quaglia F, et al. High aminopeptidase N/CD13 levels characterize human amniotic mesenchymal stem cells and drive their increased adipogenic potential in obese women. Stem Cells Dev. 2013;22(16):2287–97.
•• Baker PR 2nd, Patinkin Z, Shapiro AL, De La Houssaye BA, Woontner M, Boyle KE, et al. Maternal obesity and increased neonatal adiposity correspond with altered infant mesenchymal stem cell metabolism. JCI Insight. 2017;2(21):94200. In this translational study, the authors identify perturbations in mesenchymal stem cell metabolism and function in infants of obese mothers, suggesting a stem-cell dependent mechanism for mother–child transmission of obesity.
Baker PR 2nd, Patinkin ZW, Shapiro ALB, de la Houssaye BA, Janssen RC, Vanderlinden LA, et al. Altered gene expression and metabolism in fetal umbilical cord mesenchymal stem cells correspond with differences in 5-month-old infant adiposity gain. Sci Rep. 2017;7(1):18095.
Boyle KE, Patinkin ZW, Shapiro ALB, Bader C, Vanderlinden L, Kechris K, et al. Maternal obesity alters fatty acid oxidation, AMPK activity, and associated DNA methylation in mesenchymal stem cells from human infants. Mol Metab. 2017;6(11):1503–16.
Shapiro AL, Boyle KE, Dabelea D, Patinkin ZW, De la Houssaye B, Ringham BM, et al. Nicotinamide promotes adipogenesis in umbilical cord-derived mesenchymal stem cells and is associated with neonatal adiposity: the Healthy Start BabyBUMP Project. PLoS One. 2016;11(7):e0159575.
Beauchamp B, Ghosh S, Dysart MW, Kanaan GN, Chu A, Blais A, et al. Low birth weight is associated with adiposity, impaired skeletal muscle energetics and weight loss resistance in mice. Int J Obes. 2015;39(4):702–11.
Beauchamp B, Thrush AB, Quizi J, Antoun G, McIntosh N, Al-Dirbashi OY, et al. Undernutrition during pregnancy in mice leads to dysfunctional cardiac muscle respiration in adult offspring. Biosci Rep. 2015;35(3):e00200.
Isganaitis E, Jimenez-Chillaron J, Woo M, Chow A, DeCoste J, Vokes M, et al. Accelerated postnatal growth increases lipogenic gene expression and adipocyte size in low-birth weight mice. Diabetes. 2009;58(5):1192–200.
Gillberg L, Jacobsen SC, Ronn T, Brons C, Vaag A. PPARGC1A DNA methylation in subcutaneous adipose tissue in low birth weight subjects—impact of 5 days of high-fat overfeeding. Metabolism. 2014;63(2):263–71.
Brons C, Jensen CB, Storgaard H, Alibegovic A, Jacobsen S, Nilsson E, et al. Mitochondrial function in skeletal muscle is normal and unrelated to insulin action in young men born with low birth weight. J Clin Endocrinol Metab. 2008;93(10):3885–92.
Jousse C, Muranishi Y, Parry L, Montaurier C, Even P, Launay JM, et al. Perinatal protein malnutrition affects mitochondrial function in adult and results in a resistance to high fat diet-induced obesity. PLoS One. 2014;9(8):e104896.
Tarry-Adkins JL, Fernandez-Twinn DS, Chen JH, Hargreaves IP, Neergheen V, Aiken CE, et al. Poor maternal nutrition and accelerated postnatal growth induces an accelerated aging phenotype and oxidative stress in skeletal muscle of male rats. Dis Model Mech. 2016;9(10):1221–9.
Mele J, Muralimanoharan S, Maloyan A, Myatt L. Impaired mitochondrial function in human placenta with increased maternal adiposity. Am J Physiol Endocrinol Metab. 2014;307(5):E419–25.
Costa SM, Isganaitis E, Matthews TJ, Hughes K, Daher G, Dreyfuss JM, et al. Maternal obesity programs mitochondrial and lipid metabolism gene expression in infant umbilical vein endothelial cells. Int J Obes. 2016;40(11):1627–34.
Abraham M, Collins CA, Flewelling S, Camazine M, Cahill A, Cade WT, et al. Mitochondrial inefficiency in infants born to overweight African-American mothers. Int J Obes. 2018;42(7):1306–16.
Wu LL, Russell DL, Wong SL, Chen M, Tsai TS, St John JC, et al. Mitochondrial dysfunction in oocytes of obese mothers: transmission to offspring and reversal by pharmacological endoplasmic reticulum stress inhibitors. Development. 2015;142(4):681–91.
Saben JL, Boudoures AL, Asghar Z, Thompson A, Drury A, Zhang W, et al. Maternal metabolic syndrome programs mitochondrial dysfunction via germline changes across three generations. Cell Rep. 2016;16(1):1–8.
Aiken CE, Tarry-Adkins JL, Penfold NC, Dearden L, Ozanne SE. Decreased ovarian reserve, dysregulation of mitochondrial biogenesis, and increased lipid peroxidation in female mouse offspring exposed to an obesogenic maternal diet. FASEB J. 2016;30(4):1548–56.
Boudoures AL, Saben J, Drury A, Scheaffer S, Modi Z, Zhang W, et al. Obesity-exposed oocytes accumulate and transmit damaged mitochondria due to an inability to activate mitophagy. Dev Biol. 2017;426(1):126–38.
Borengasser SJ, Faske J, Kang P, Blackburn ML, Badger TM, Shankar K. In utero exposure to prepregnancy maternal obesity and postweaning high-fat diet impair regulators of mitochondrial dynamics in rat placenta and offspring. Physiol Genomics. 2014;46(23):841–50.
Pileggi CA, Hedges CP, Segovia SA, Markworth JF, Durainayagam BR, Gray C, et al. Maternal high fat diet alters skeletal muscle mitochondrial catalytic activity in adult male rat offspring. Front Physiol. 2016;7:546.
McCurdy CE, Schenk S, Hetrick B, Houck J, Drew BG, Kaye S, et al. Maternal obesity reduces oxidative capacity in fetal skeletal muscle of Japanese macaques. JCI Insight. 2016;1(16):e86612.
Mdaki KS, Larsen TD, Wachal AL, Schimelpfenig MD, Weaver LJ, Dooyema SD, et al. Maternal high-fat diet impairs cardiac function in offspring of diabetic pregnancy through metabolic stress and mitochondrial dysfunction. Am J Physiol Heart Circ Physiol. 2016;310(6):H681–92.
Bruce KD, Cagampang FR, Argenton M, Zhang J, Ethirajan PL, Burdge GC, et al. Maternal high-fat feeding primes steatohepatitis in adult mice offspring, involving mitochondrial dysfunction and altered lipogenesis gene expression. Hepatology. 2009;50(6):1796–808.
Cardenas-Perez RE, Fuentes-Mera L, de la Garza AL, Torre-Villalvazo I, Reyes-Castro LA, Rodriguez-Rocha H, et al. Maternal overnutrition by hypercaloric diets programs hypothalamic mitochondrial fusion and metabolic dysfunction in rat male offspring. Nutr Metab (Lond). 2018;15:38.
Malpique R, Gallego-Escuredo JM, Sebastiani G, Villarroya J, Lopez-Bermejo A, de Zegher F, et al. Brown adipose tissue in prepubertal children: associations with sex, birthweight, and metabolic profile. Int J Obes. 2019;43(2):384–91.
Ortega FB, Ruiz JR, Alkorta MP, Larrarte E, Simon E, Ares R, et al. The effect of birth weight on low-energy diet-induced changes in body composition and substrate-energy metabolism in obese women. J Am Coll Nutr. 2011;30(2):134–40.
Sipola-Leppanen M, Hovi P, Andersson S, Wehkalampi K, Vaarasmaki M, Strang-Karlsson S, et al. Resting energy expenditure in young adults born preterm--the Helsinki study of very low birth weight adults. PLoS One. 2011;6(3):e17700.
Brons C, Lilleore SK, Astrup A, Vaag A. Disproportionately increased 24-h energy expenditure and fat oxidation in young men with low birth weight during a high-fat overfeeding challenge. Eur J Nutr. 2016;55(6):2045–52.
de Zegher F, Diaz M, Lopez-Bermejo A, Ibanez L. Recognition of a sequence: more growth before birth, longer telomeres at birth, more lean mass after birth. Pediatr Obes. 2017;12(4):274–9.
Hjort L, Vryer R, Grunnet LG, Burgner D, Olsen SF, Saffery R, et al. Telomere length is reduced in 9- to 16-year-old girls exposed to gestational diabetes in utero. Diabetologia. 2018;61(4):870–80.
Acknowledgments
Mikayla Kass and Ming Fang contributed to the literature review. The drawing of a human infant in Fig. 1 is by Charlie Aoun.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
E.I. declares that she has no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Pathogenesis of Type 2 Diabetes and Insulin Resistance
Rights and permissions
About this article
Cite this article
Isganaitis, E. Developmental Programming of Body Composition: Update on Evidence and Mechanisms. Curr Diab Rep 19, 60 (2019). https://doi.org/10.1007/s11892-019-1170-1
Published:
DOI: https://doi.org/10.1007/s11892-019-1170-1