Abstract
Diabetes mellitus (DM) commonly leads to progressive chronic kidney disease despite current best medical practice. The pathogenesis of diabetic kidney disease (DKD) involves a complex network of primary and secondary mechanisms with both intra-renal and systemic components. Apart from inhibition of the renin angiotensin aldosterone system, targeting individual pathogenic mediators with drug therapy has not, thus far, been proven to have high clinical value. Stem or progenitor cell therapies offer an alternative strategy for modulating complex disease processes through suppressing multiple pathogenic pathways and promoting pro-regenerative mechanisms. Mesenchymal stem cells (MSCs) have shown particular promise based on their accessibility from adult tissues and their diverse mechanisms of action including secretion of paracrine anti-inflammatory and cyto-protective factors. In this review, the progress toward clinical translation of MSC therapy for DKD is critically evaluated. Results from animal models suggest distinct potential for systemic MSC infusion to favourably modulate DKD progression. However, only a few early phase clinical trials have been initiated and efficacy in humans remains to be proven. Key knowledge gaps and research opportunities exist in this field. These include the need to gain greater understanding of in vivo mechanism of action, to identify quantifiable biomarkers of response to therapy and to define the optimal source, dose and timing of MSC administration. Given the rising prevalence of DM and DKD worldwide, continued progress toward harnessing the inherent regenerative functions of MSCs and other progenitor cells for even a subset of those affected has potential for profound societal benefits.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction: Diabetic Kidney Disease and Its Pathogenesis
Diabetes mellitus (DM) is a global pandemic [1]. An estimated 171 million people worldwide had a confirmed diagnosis of DM in 2000 [2], doubling to 346 million in 2012—the majority having type 2 DM [3]. By 2030, this number is expected to increase to over 430 million people [4]. Key contributory factors include population ageing, increasing levels of obesity and declining physical activity coupled with improved life expectancy due to advances in medical care [1].
Consequent to this global pandemic, there has been an increase in the macro- and micro-vascular complications associated with DM, particularly diabetic nephropathy and other forms of chronic kidney disease (CKD), referred to in this review under the umbrella term of diabetic kidney disease (DKD) [5, 6]. Currently, DM is the commonest cause of CKD and end-stage renal disease (ESRD) worldwide [7]. The reported prevalence of CKD amongst those with DM varies from 8.6 to 17.7 % [5, 8, 9] with higher prevalence among people of African American, Asian and Native American ethnicity compared to Caucasians [7, 10]. The widespread adaptation of the Modification of Diet in Renal Disease (MDRD) equation for estimating glomerular filtration rate (eGFR) may also have contributed to the reporting of increased DKD prevalence [11]. Importantly, DKD is associated with greatly increased risk for cardiovascular [12–14] and all-cause mortality [15, 16, 17••, 18•]. Individuals with ESRD secondary to DKD have an annual mortality rate of approximately 20 % [19•]. In the USA, the cost of treating a person with DM and CKD has increased more than 11-fold in the last decade [20].
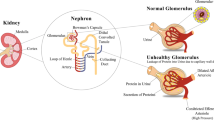
The most consistent pathological features of DKD are capillary basement membrane thickening and diffuse and nodular glomerulosclerosis. In the early stages of DKD, these glomerular lesions manifest as hyper-filtration and increased albumin excretion followed, as the disease advances, by progressively increasing proteinuria and declining eGFR. Importantly, DKD is also associated with primary and secondary pathological changes to the vascular and tubulo-interstitial compartments, the severity of which exert a strong influence on the rate of loss of renal function. Furthermore, in a proportion of individuals with clinical features of DKD, additional primary renal conditions (e.g. IgA nephropathy, renal arterial disease) may be superimposed upon DM-driven pathological changes.
The pathophysiology of DKD (Fig. 1a) is primarily driven by elevated blood glucose but extends to a broad network of local and systemic processes [21••]. These processes remain only partially understood but key details have been revealed through experimental studies in cell culture, animal models, tissue samples and human subjects. For example, hyperglycaemia induces abnormal activation of protein kinase C (PKC) in renal parenchymal cells which is associated with up-regulation of the pro-fibrotic cytokine transforming growth factor-β (TGF-β) along with the matrix proteins fibronectin and collagen type IV, nitric oxide dysregulation, endothelial dysfunction and activation of the mitogen-activated protein kinase (MAPK) and nuclear factor kappa B (NF-κB) signalling pathways [22, 23]. Hyperglycaemia is also associated with high levels of advanced glycation end-products (AGE) which further stimulate the production of TGF-β.
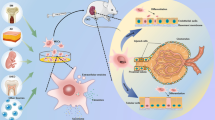
a A schematic representation of known elements of the pathophysiological networks involved in the development and progression of diabetic kidney disease (DKD) is shown. Abbreviations for a: Mon = monocyte; ICAM-1 = intracellular adhesion molecule 1; Mac = macrophages; RAAS = renin-angiotensin aldosterone system; AGE = advanced glycation end-products; NADPH = nicotinamide adenine dinucleotide phosphate; GLUT-1 = glucose transporter 1; ROS = reactive oxygen species; VEGF = vascular endothelial growth factor; TGF = transforming growth factor; IL = interleukin; TNF = tumour necrosis factor; PKC = protein kinase C; MAPK = mitogen-activated protein kinases; CSF-1 = colony-stimulating factor 1; MCP-1 = monocyte chemotactic protein 1; MIF = macrophage migration inhibitory factor; CTGF = connective tissue growth factor; ECM = extracellular matrix; eGFR = estimated glomerular filtration rate; ESRD = end-stage renal disease; RTA = renal tubular acidosis. b A conceptual model is shown of the mechanisms whereby paracrine properties of systemically administered MSCs may exert reno-protective effects in the setting of DKD based on insights from published animal model studies. Abbreviations for b: SOD = superoxide dismutase; MDA = malondialdehyde; GLUT 1 = glucose transporter 1; ECM, = extracellular matrix; Hsp 47 = heat shock protein 47; TGFβ1 = transforming growth factor β1; EMT = epithelial mesenchymal transition; Th1 = T helper 1 lymphocytes; IL-1β = interleukin-1β; IL-6 = interleukin-6; TNFα = tumour necrosis factor α; IL-10 = interleukin-10; MCP-1 = monocyte chemotactic protein 1; MAPK = mitogen-activated protein kinase; p-ERK = phosphorylated extracellular signal-regulated kinase; p-JNK = phosphorylated jun n-terminal kinase; p38 = phosphorylated p38 kinase; HGF = hepatocyte growth factor; EGF = epidermal growth factor; GDNF = glial cell line-derived neurotrophic factor; VEGF = vascular endothelial growth factor; IGF-1 = insulin-like growth factor 1; IGFBP-1 = insulin-like growth factor-binding protein-1; PlGF = placental growth factor; BMP-7 = bone morphogenetic protein; WT1 = Wilms tumour 1 protein; BAX = Bcl-2-associated X protein; Bcl-2 = B cell lymphoma-2 protein
Activation of the renin-angiotensin aldosterone system (RAAS) has been linked to hyperglycaemia-associated increased formation of succinate [24, 25]. This causes elevated levels of angiotensin II leading to pro-inflammatory signals, hypertrophy of mesangial and tubular epithelial cells, increases in TGF-β [26, 27] and monocyte chemoattractant protein-1 (MCP-1) [28, 29], and the generation of reactive oxygen species (ROS) [30]. Induction of MCP-1 results in increased trafficking of monocytes into the kidney. Infiltrating monocytes are then converted to macrophages which release pro-inflammatory factors including interleukin-6 (IL-6), tumour necrosis factor α (TNF-α) and ROS [31•]. During this inflammatory process, additional angiotensin II is also generated at tissue level by macrophages and lymphocytes [32].
Growth factors also contribute to the development of glomerular structural alterations. For example, elevated glucose levels induce an early activation of platelet-derived growth factor-β (PDGF-β) which causes an increase in TGF-β1 expression [33]. Systemic arterial hypertension and localised haemodynamic dysfunction may further exacerbate intra-renal inflammation and the production of growth factors and extracellular matrix (ECM) proteins.
Based on these and other pathogenic mechanisms, DKD is now understood to occur in the setting of a pro-inflammatory milieu that is driven by metabolic dysregulation [19•] and mediated by humoral factors that cause pathogenic structural and functional alterations to the kidney [34]. In addition to the primary parenchymal cells of the kidney, specific immune cells also act as an important source of pathogenic mediators in DKD. For example, the severity of glomerulosclerosis is associated with the extent of macrophage accumulation in the kidney [35, 36]. While the role of lymphocytes has yet to be clearly defined [37], early DKD is associated with an increase in activated T cells [38]. A counter-balancing role for regulatory T cells (T-reg) has also been demonstrated in animal models of DKD. It has been shown that the anti-inflammatory effects of T-reg ameliorate metabolic abnormalities and insulin resistance [39], while depletion of T-reg exacerbates albuminuria and hyperfiltration [40].
It is clear from this brief synopsis of DKD pathophysiology that the driving factors, primary cell responses and secondary, exacerbating factors represent a complex network of damaging mechanisms that are unlikely to be reversed by targeting a single mediator or intracellular pathway. Cellular therapies, particularly stem or progenitor cells, offer the potential for modifying multiple pathogenic mechanisms simultaneously and for actively promoting inherent capacity for tissue repair and regeneration [41•]. In this review, we summarise and critically evaluate the evidence for mesenchymal stem cells (MSCs)—a progenitor cell population that can be culture-expanded to large numbers from samples of bone marrow, fat, umbilical cord and other human tissues—as a cellular therapy for DKD.
Animal Models Used to Evaluate MSCs in DKD
Rodents have served as the primary animal model of DKD due to their widespread availability, well defined genotypes, large repertoire of associated experimental reagents and amenability to genetic modification [42]. Almost all in vivo studies of MSCs in models of DKD have been carried out in mice or rats. Recently, however, Pan et al. reported results of a study evaluating the effects of MSC administration on DKD in tree shrews—a species having greater genome homology with primates which may also develop spontaneous dysglycaemia [43–47]
The characteristics of a given model of DKD reflect both the method(s) used to induce DM and the species/strain susceptibility to the development of DKD [48]. A range of methods has been developed for inducing type 1- or type 2-like DM in mice, including dietary, pharmacologic and genetic interventions [49]. Pharmacologic induction of DM with streptozotocin (STZ), with or without accelerating factors such as high-fat diet [43], uni-nephrectomy [50•] or use of the non-obese diabetic (NOD) strain [51], has been the predominant rodent DKD model used in the evaluation of MSCs. Experimental results in the db/db mouse model of obese, type 2 DM with uni-nephrectomy have also been reported in abstract form [52]. Some concerns related to the renal disease observed in STZ-induced type 1 DM are of relevance. Non-specific renal cytotoxicity of STZ itself can lead to acute tubular injury raising the concern that some of the observed beneficial effects of MSC administration may be due to their well-documented capacity to reduce the severity of acute kidney injury (AKI) [41•, 53–55]. While all but one reported study used a low-dose STZ regimen [56], a residual risk of STZ-induced AKI has been described even at low doses [57]. Furthermore, STZ-induced diabetes rarely progresses to histologically advanced DKD and renal failure [58]. The recent development of murine models which more readily recapitulate the more advanced features of DKD may be of value for testing the pre-clinical efficacy of MSCs across the spectrum of DKD severity [59–61].
Efficacy and Mechanism of Action of MSCs in Pre-clinical Models of DKD
Over the past decade, several groups have reported results of experiments in which therapeutic benefits of MSCs were evaluated in the small animal models of DKD described above. These pre-clinical studies have involved administration of autologous/syngeneic [56, 62, 63], allogeneic [43, 64, 65, 66•, 67, 68] and xenogeneic (human) [50•, 51, 69•, 70, 71] MSCs. Most studies employed MSCs of bone marrow origin but umbilical cord- [70, 71] and adipose-derived MSCs [50•, 62, 69•] have also been used. Systemic administration of MSCs via the intravenous route has been utilised in the majority of studies. Two studies employed intra-cardiac administration via the left ventricle [51, 68] while another reported local delivery via the left renal artery [67].
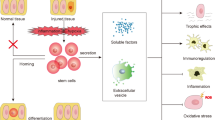
These published studies have generally provided evidence that MSCs ameliorate clinically relevant indicators of DKD severity including albuminuria; serum creatinine/urea; glomerular hypertrophy, mesangial expansion and sclerosis; podoctye number and foot process effacement; and tubular injury and interstitial fibrosis. Taken together, the results to date indicate that systemic administration of one or more doses of MSCs exerts beneficial effects on proteinuric DKD in small animal models regardless of tissue source and genetic/species compatibility. In keeping with MSC anti-inflammatory properties, a consistent observation in rodent models of DKD has been reduction in the intra-renal expression of key inflammatory mediators such as TNFα, IL-6 and IL-1β and reduced infiltration by macrophages [51, 62, 64, 66•]. These studies also provide insights into other key issues related to the clinical translation of MSC therapy to human subjects with DKD including impact on glycaemic control, bio-distribution and persistence of administered cells and mechanism(s) of action.
The potential for MSCs to improve blood glucose control after systemic administration may delay the progression of DKD independently of direct reno-protective effects [72]. Of 14 studies assessing the in vivo effect of MSCs in animal models of DKD, 8 reported a concomitant significant reduction in blood glucose [43, 51, 62–65, 66•, 73]. One study reported a reduction in blood glucose only when allogeneic MSCs (allo-MSCs) were administered in combination with cyclosporine [68], suggesting that immunologic rejection could hinder the propensity of allo-MSCs to lower blood glucose. Three of these nine studies reported concomitant islet cell regeneration despite low levels of MSC engraftment in the pancreas [51, 63, 73], suggesting that paracrine mechanisms underpin the anti-hyperglycaemic benefit of MSCs. This is in keeping with evidence from the wider literature regarding the beneficial effects of MSCs in models of DM [74–76]. For studies in which no significant reduction in blood glucose occurred [50•, 56, 67, 70, 71], various explanations have been proposed. Factors such as MSC tissue origin, administration route and dosage may influence their potency [72]. Additionally, variations in DKD model characteristics such as the mechanism and degree of pancreatic β cell injury at the time of administration may dictate whether rescue is possible [56]. Clarification of these factors will be paramount for maximising the efficacy of MSC therapy when applied to human DKD.
Regarding MSC bio-distribution in models of DKD, all studies have demonstrated tracking of MSCs to the kidneys after systemic administration, albeit of a degree and duration that is unlikely to fully explain their beneficial effects on renal function and structure [77]. Although Lee et al. reported direct differentiation of some human bone marrow-derived MSCs into intra-renal CD31+ endothelial cells in diabetic NOD/scid mice [51], it is generally accepted that such trans-differentiation events are rare at best and insufficient to represent a major mechanism of tissue repair. However, Wang et al. also reported that 10 % of glomeruli contained adipocytes arising from administered MSCs in rats with type 1 DM [67], a finding which should be closely monitored in human studies.
It remains unclear whether trafficking of systemically administered MSCs to the kidney in DKD is essential for maximising the beneficial effects of their paracrine activities. Nonetheless, two recent studies have reported results for the application of ultrasound-targeted micro-bubble destruction (UTMD) to enhance MSC homing to diabetic kidneys. Zhang et al. demonstrated that UTMD increased MSC localisation to the kidneys by increasing interstitial capillary permeability and endothelial VCAM-1 expression. In this study, UTMD-enhanced renal trafficking was associated with reduced urinary albumin excretion without a concomitant reduction in blood glucose compared with MSC administration alone [73]. Subsequently, Wu et al. exploited the interaction between stromal cell-derived factor-1 (SDF-1) and the CXCR4 receptor, which is of central importance to MSC migration [78], by loading micro-bubbles with covalently attached SDF-1. The resultant increase in SDF-1 in the renal interstitium after application of ultrasound greatly enhanced MSC homing at 24 h compared to conventional UTMD [79•]. No studies have yet assessed the ability of UTMD to increase MSC homing to the pancreas [80].
A large body of literature has accumulated related to the mediators and pathways involved in MSC paracrine functions in diseases involving maladaptive inflammation and tissue degeneration [41•]. Figure 1b summarises the paracrine reno-protective effects of MSCs which have been elucidated in animal models of DKD to date. As shown, experimental evidence supports modulatory effects of MSC-derived factors on mechanisms of fibrosis, oxidative stress, immune/inflammatory activity, cellular de-differentiation pathways and growth factor responses. Rather than viewing them independently, it is important to recognise that most of these mechanisms interact at one or more levels within the complex molecular milieu of DKD. For example, Lv et al. demonstrated that hepatocyte growth factor (HGF) elaboration from MSCs significantly reduced hyperglycaemia-induced TGFβ1 expression in mesangial cells, which in turn was responsible for the reduced GLUT1 expression and consequent reduction in glucose-mediated intracellular oxidative stress observed with allo-MSC administration [65]. Despite this, the consequences of trophic factor secretion by MSCs in the setting of DKD remains under-evaluated, with the reno-protective effect of only three of these factors being rigorously examined using neutralising antibodies and/or small interfering RNA in vitro. Along with HGF, epidermal growth factor (EGF) has been shown to prevent podocyte apoptosis and hyperglycaemia-induced down-regulation of synaptopodin and nephrin expression [69•]. Glial cell line-derived neurotrophic factor (GDNF) prevents hyperglycaemia-induced down-regulation of podocyte synaptopodin and Wilms tumour 1 protein [50•]. Clearly, continued investigation of MSCs mechanism of action in animal models of DKD is needed to optimise clinical translation.
Biomarkers of DKD Progression and Their Role in Clinical Translation of MSCs
A significant unmet need for successful translation of MSCs, and other cellular therapies for DM and its complications, in human subjects is the identification of measurable factors (“biomarkers”) that can serve as predictors or early indicators of favourable therapeutic response. This is particularly important for DKD as impact on the relevant “hard outcomes” such as rate of decline of GFR, development of ESRD, cardiovascular events or death may not be evident for years following intervention. Increased urine albumin excretion is an important marker of risk for development of progressive DKD [81–83] but, in recent years, it has been shown to fluctuate over time in many individuals with DM [83–86]. Thus, although albuminuria combined with eGFR continues to be a guideline-endorsed biomarker of CKD [87], its value as a surrogate for future risk of progressive CKD/ESRD in the context of clinical trials in DKD is open to question. It is against this backdrop that the evaluation of alternative biomarkers or panels of biomarkers linked to a growing understanding of the pathophysiology of DKD has become an important research topic [88–90]. Although the majority of novel DKD biomarkers are currently in the early stages of validation, several have biological plausibility and have been the subject of promising studies in cohorts of subjects with diabetes. In some cases, such emerging biomarkers may be linked to the putative mechanisms of action of MSCs in animal models of DKD discussed above (see Table 1). Thus, the design of experimental systems and clinical trials of MSCs as a therapeutic intervention for DKD may be enhanced by careful consideration of the growing literature on measurable biomarkers in blood and urine. For the purpose of this review, we will focus on a selection of such novel biomarkers which we believe may have specific potential for predicting the effects of MSC therapy in DKD.
Pro-inflammatory cytokines may represent important indicators of DKD risk and severity. For example, serum and urine concentrations of TNF-α are elevated in people with DM compared to healthy controls [91–93]. Navarro et al. demonstrated that urinary TNF-α is raised in type 2 DM and independently correlates with albuminuria status and renal function [93]. In vivo models of the role of MSCs on renal function in rats with DKD have demonstrated a decrease in TNF-α following MSC therapy [64]. The receptors for TNF-α, TNF receptor-1 (TNFR1) or TNF receptor-2 (TNFR2), may also serve as indicators of DKD severity in their soluble forms (sTNFR1 and sTNFR2). Niewczas et al. in a cross-sectional study of type 1 diabetic subjects identified that serum TNF-α and the sTNFRs were associated with cystatin-C-based eGFR (cC-eGFR) in univariate analyses. However, on multivariate analysis, only the association with sTNFRs remained significant [94]. Further work by this group demonstrated that circulating TNFRs are predictive of stage 3 CKD in type 1 DM [95] and of ESRD in type 2 DM [96••]. Serum and/or urine concentrations of other pro-inflammatory mediators such as IL-6, IL-1β and MCP-1 have also been shown to be associated with DKD in patient cohorts. Although their value as clinical predictors of DKD progression and complications has not been robustly proven, they may also be considered as putative biomarkers of the anti-inflammatory effects of MSCs.
Type 2 DM is associated with down-regulation of the adipokine adiponectin in association with obesity and insulin resistance [97]. Adiponectin is reported to have a reno-protective effect in rodent experiments [98–100]. Consistent with this, serum adiponectin levels have been observed to be negatively correlated with urinary albumin excretion in subjects with DM, normo-albuminuria and preserved GFR. However, this correlation is less consistent in subjects with micro-albuminuria [98, 101–104]. Furthermore, in subjects with overt DKD, serum and urine adiponectin levels have been shown to have positive correlations with albuminuria and negative correlations with GFR [105–112]. Saraheimo et al., in a prospective study of subjects with type 1 DM, observed that increased serum adiponectin predicted progression from macro- but not micro- or normo-albuminuria to ESRD [113]. Similarly, Panduru et al. identified an association between urinary adiponectin and progression to ESRD in type 1 DM [114•]. The authors concluded that urinary adiponectin was a better predictor than albumin excretion rate. Thus, serum or urine adiponectin may be of specific value as a predictor of DKD progression in the setting of overt proteinuria and reduced eGFR—perhaps the most likely target group for MSC therapy.
Other novel biomarkers of interest include neutrophil gelatinase-associated lipocalin (NGAL), fibroblast growth factor 23 (FGF-23) and fibroblast growth factor 21 (FGF-21). NGAL is a small molecule belonging to the lipocalin superfamily which plays a role in apoptosis, immune regulation and transportation of small hydrophobic molecules [88, 115]. In a cohort of subjects with type 2 DM, Yang et al. demonstrated that urine NGAL correlated positively with cystatin C, urea nitrogen and serum creatinine and inversely with eGFR [116]. Nielsen et al. demonstrated that urine NGAL was elevated in type 1 DM with and without albuminuria suggesting a tubular source [117]. They showed that urine NGAL increases significantly with increasing albuminuria. In a study by Bolignano et al., urine and serum NGAL were higher in subjects with DM compared to controls and the rate of increase of NGAL was associated with increasing albuminuria [118]. However, controversy exists regarding the utility of this marker as other authors have suggested that there may not be an association following adjustment for clinical predictors [119–121]. FGF-23 is an osteocyte-produced hormone involved in the regulation of phosphate excretion and vitamin D activation [122]. Titan et al. demonstrated that serum FGF-23 concentration is an independent predictor of renal outcome in patients with type 2 DM and macro-albuminuria [123]. A related factor, FGF-21, is secreted by the liver and has been shown to regulate various metabolic conditions [124]. In a large cohort of subjects with type 2 DM, higher serum FGF-21 concentration at baseline was associated with eGFR decline during a median 4-year follow-up. In subjects with eGFR ≥60 mL/min/1.73m2 and normo-albuminuria, serum FGF-21 was an independent predictor of eGFR decline. Other biomarkers such as kidney injury molecule-1 (KIM-1) [31•, 121, 125–129, 130••], vascular endothelial growth factor (VEGF) [131–135] and α-1 microglobulin [130••, 136–140] may also be relevant in trials of stem cell therapies.
As an alternative to measurement of individual biomarkers, assays involving quantification of biomarker panels may eventually allow for more precise prediction of adverse renal outcomes or responses to novel therapies. Recently, Looker et al. evaluated a large number of candidate biomarkers for their predictive value for rapid progression from CKD stage 3 in a longitudinally followed cohort of subjects with DKD [130••]. This study identified a minimal panel of 14 biomarkers which provided significant predictive value when added to clinical information. The panel included the above-mentioned KIM-1, FGF-21 and α-1 microglobulin along with other proteins and small molecules/metabolites. Building on rapid advances in mass spectrometry, urinary proteomics has been extensively applied as a technology for non-biased discovery of biomarkers panels for CKD/DKD progression [141–143]. Notably, Goode et al. identified a 273-peptide urine signature (CKD 273) with a sensitivity of 85.5 % and specificity of 100 % in classifying CKD among subjects from a multicentre prospective study [144]. Subsequently, the CKD 273 panel was shown to have predictive value for loss of renal function and death in a prospectively followed CKD cohort [145]. It was also validated as accurately identifying DKD [146•] and for predicting transition to micro- or macro-albuminuria in a cohort of subjects with type 2 DM [147]. In a longitudinal study of normo-albuminuric subjects with type 1 and type 2 DM, the CKD 273 panel significantly enhanced the predictive value of urinary albumin alone for development of macro-albuminuria up to 5 years later [148]. Sharma et al. quantified 94 urine metabolites using gas-chromatography-mass spectrometry and found that 13 metabolites were significantly reduced in subjects with DKD [21••]. The metabolic signature was specifically linked to mitochondrial metabolism and the authors concluded that global suppression of intra-renal mitochondrial function may be a measurable indicator of DKD severity. As MSCs and their products have been demonstrated to have direct cytoprotective effects on renal epithelial cells [149], it is interesting to speculate that changes in urine metabolites could serve as an early indicator of response to cellular therapy in DKD.
Human Clinical Trials of MSCs in DKD
Clinical trial activity in the area of MSC therapy for DKD, or for other causes of CKD, has only recently been initiated and remains at an early stage worldwide. A search of the major clinical trial registries [WHO International Clinical Trials Registry (www.who.int/ictrp/en/); EU Clinical Trials Register (www.clinicaltrialsregister.eu/) and the U.S. National Institutes of Health ClinicalTrials.gov (www.clinicaltrials.gov)] yielded only three clinical trials of MSC therapy in DKD as well as four additional trials in non-diabetic CKD. The details of these trials are summarised in Table 2. As is clear from the table, these clinical trials involve small numbers of subjects with DKD/CKD and represent either exploratory studies (Phase 0) or studies with safety as the primary end-point and potential signals of efficacy as secondary end-points (Phase I/II). Two clinical trials in DKD/CKD involve allo-MSC administration while the remainder focus on autologous MSCs from bone marrow or adipose tissue. With the exception of an ongoing trial of autologous MSCs delivered intra-arterially in subjects with reno-vascular disease, all trials involve intra-venous administration of various doses of MSCs.
To date, only one Phase I/II trial has been completed with results reported in abstract form at the 2015 American Diabetes Association national meeting [150••]. In this trial, two doses of a cell product manufactured by the Australian company Mesoblast Ltd. consisting of allogeneic bone marrow-derived Stro3+ mesenchymal precursor cells (MPCs) were compared with placebo infusion in a cohort of 30 subjects with type 2 DM and eGFR of 20–50 mL/min/1.73/m2 on stable medical therapy. Preliminary results from 12 and 24 weeks follow-up indicated an acceptable safety profile for MPCs in the setting of relatively advanced DKD. In addition, trends for change in renal function provided an “efficacy signal” in that subjects receiving placebo had greater decline in eGFR during follow-up compared to those receiving cell infusion—particularly for those with higher baseline eGFR (>30 mL/min/1.73/m2) and higher serum IL-6 concentration (>3.5 pg/dL). A Phase 0 trial of autologous bone marrow MSCs in 20 subjects with type 1 DM and nephropathy has completed enrolment in Iran. To our knowledge, results for this study have not yet been reported. Finally, the authors of this review, along with partner institutes from five other European countries (UK, Belgium, the Netherlands, Germany and Italy) have recently initiated a project (www.nephstrom.eu) which will conduct a multi-site, placebo-controlled, dose-escalating Phase I/II clinical trial of a prospectively isolated bone marrow-derived allo-MSC therapy in subjects with progressive, proteinuric DKD (eGFR 30–50 mL/min/1.73/m2) despite optimal medical therapy (see Table 2). Thus, while it has been almost 10 years since the first promising animal model study [51], the clinical translation of MSC therapies for DKD is in its infancy and further development of the field may well be dependent on encouraging results from such early phase trials.
Conclusion: What Are the Key Challenges and Unanswered Questions?
Of the many diseases for which MSCs are considered to be of potential benefit, progressive DKD represents one of the most significant worldwide health challenges. As described in this review, the therapeutic model which has been evaluated in pre-clinical models to date consists of a single, timed intervention by which multiple elements of disease pathogenesis are favourably modulated. The efficacy of this model rests predominantly upon MSC-associated paracrine mechanisms which result in alterations to the systemic and intra-renal milieu with consequent slowing or reversal of key pathogenic pathways including glomerular barrier dysfunction, pro-inflammatory cellular infiltration, tubular epithelial cell stress and progressive interstitial fibrosis. Thus, the clinical niche for MSC administration in DKD could be viewed as a broad re-programming of chronic nephrotoxic processes occurring in DM which may “reset the clock” of progression toward ESRD in responsive individuals. Of additional significance, MSC administration has also been demonstrated to improve glycaemic control as well as the advancement of other diabetic end-organ complications in some experimental settings. Furthermore, MSC therapy is conceptually compatible with established pharmacological and lifestyle-based treatments for DKD and with a model of intermittent administration that has proven to be highly effective for other “biological agents”. However, as we make clear here, small animal models of DM and DKD provide, at best, only a partial reproduction of human disease pathogenesis and progression. Therefore, the design and outcome of early phase clinical trials in this area represent a critical juncture in the evolution of cellular therapies for diabetic complications. Confirmation of the safety of autologous and allogeneic progenitor cell therapy is paramount. However, the identification and interpretation of “efficacy signals” from these studies may well determine whether the necessary investment of funding, resources and expertise can be secured to proceed with trials of sufficient scope to robustly prove therapeutic value.
To conclude this review, we highlight the following areas for which ongoing and new research efforts will be needed to maximise the likelihood of widespread future clinical application of MSCs and other stem/progenitor cell therapies to DKD: (a) Further efficacy and mechanism of action studies in emerging animal models of DKD. (b) Development of in vitro systems and potency assays to optimise MSC production and patient selection for cell therapy intervention. (c) Identification of biomarkers linked to DKD progression and to in vivo MSC mechanism of action for application to Phase II/III clinical trials. (d) Economic analysis and modelling of the delivery, reimbursement and cost-effectiveness of MSC administration in DKD at varying stages of severity.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance, •• Of major importance
van Dieren S, Beulens JW, van der Schouw YT, Grobbee DE, Neal B. The global burden of diabetes and its complications: an emerging pandemic. Eur J Cardiovasc Prev Rehabil. 2010;17 Suppl 1:S3–8.
Wild S, Roglic G, Green A, Sicree R, King H. Global prevalence of diabetes: estimates for the year 2000 and projections for 2030. Diabetes Care. 2004;27:1047–53.
World Health Organization: Diabetes Fact Sheet, 2012. Available at: http://www.whoint/mediacentre/factsheets/fs312/en/indexhtml
Shaw JE, Sicree RA, Zimmet PZ. Global estimates of the prevalence of diabetes for 2010 and 2030. Diabetes Res Clin Pract. 2010;87:4–14.
de Boer IH, Rue TC, Hall YN, Heagerty PJ, Weiss NS, Himmelfarb J. Temporal trends in the prevalence of diabetic kidney disease in the United States. JAMA. 2011;305:2532–9.
Gross JL, de Azevedo MJ, Silveiro SP, Canani LH, Caramori ML, Zelmanovitz T. Diabetic nephropathy: diagnosis, prevention, and treatment. Diabetes Care. 2005;28:164–76.
USRDS: the United States Renal Data System. Am J Kidney Dis. 2003;42(6 Suppl 5):1–230.
Chen W, Chen W, Wang H, Dong X, Liu Q, Mao H, et al. Prevalence and risk factors associated with chronic kidney disease in an adult population from southern China. Nephrol Dial Transplant. 2009;24:1205–12.
Yokoyama H, Sone H, Oishi M, Kawai K, Fukumoto Y, Kobayashi M, et al. Prevalence of albuminuria and renal insufficiency and associated clinical factors in type 2 diabetes: the Japan Diabetes Clinical Data Management study (JDDM15). Nephrol Dial Transplant. 2009;24:1212–9.
Young BA, Maynard C, Boyko EJ. Racial differences in diabetic nephropathy, cardiovascular disease, and mortality in a national population of veterans. Diabetes Care. 2003;26(8):2392–9.
Yang CW, Park JT, Kim YS, Kim YL, Lee YS, Oh YS, et al. Prevalence of diabetic nephropathy in primary care type 2 diabetic patients with hypertension: data from the Korean Epidemiology Study on Hypertension III (KEY III study). Nephrol Dial Transplant. 2011;26:3249–55.
de Boer IH, Katz R, Cao JJ, Fried LF, Kestenbaum B, Mukamal K, et al. Cystatin C, albuminuria, and mortality among older adults with diabetes. Diabetes Care. 2009;32:1833–8.
Ninomiya T, Perkovic V, de Galan BE, Zoungas S, Pillai A, Jardine M, et al. Albuminuria and kidney function independently predict cardiovascular and renal outcomes in diabetes. J Am Soc Nephrol. 2009;20:1813–21.
Emerging Risk Factors Collaboration, Seshasai SR, Kaptoge S, Thompson A, Di Angelantonio E, Gao P, et al. Diabetes mellitus, fasting glucose, and risk of cause-specific death. N Engl J Med. 2011;364:829–41.
Groop PH, Thomas MC, Moran JL, Waden J, Thorn LM, Makinen VP, et al. The presence and severity of chronic kidney disease predicts all-cause mortality in type 1 diabetes. Diabetes. 2009;58:1651–8.
Orchard TJ, Secrest AM, Miller RG, Costacou T. In the absence of renal disease, 20 year mortality risk in type 1 diabetes is comparable to that of the general population: a report from the Pittsburgh Epidemiology of Diabetes Complications Study. Diabetologia. 2010;53:2312–9.
Afkarian M, Sachs MC, Kestenbaum B, Hirsch IB, Tuttle KR, Himmelfarb J, et al. Kidney disease and increased mortality risk in type 2 diabetes. J Am Soc Nephrol. 2013;24:302–8. This epidemiological study, based on the NHANES cohort from the USA, underscores the fact that the excess cardiovascular morbidity and mortality associated with type 2 DM is predominantly manifest among those with CKD.
Tancredi M, Rosengren A, Svensson AM, Kosiborod M, Pivodic A, Gudbjörnsdottir S, et al. Excess mortality among persons with type 2 diabetes. New Engl J Med. 2015;373:1720–32. This epidemiological study from Sweden demonstrated that the excess risk of all-cause and cardiovascular death in type 2 DM increased with greater severity of renal complications as well as with younger age and worse glycaemic control.
Reidy K, Kang HM, Hostetter T, Susztak K. Molecular mechanisms of diabetic kidney disease. J Clin Invest. 2014;124:2333–40. This review by leading researchers summarises recent insights into the pathophysiology of renal damage in DM.
United States Renal Data System, 2014 Annual Data Report. Epidemiology of Kidney Disease in the United States. Bethesda, MD: National Institutes of Health, National Institute of Diabetes and Digestive and Kidney Disease; 2014. [cited 2015 16 June]. Available from: http://www.usrds.org/adr.aspx.
Sharma K, Karl B, Mathew AV, Gangoiti JA, Wassel CL, Saito R, et al. Metabolomics reveals signature of mitochondrial dysfunction in diabetic kidney disease. J Am Soc Nephrol. 2013;24:1901–12. Using metabolomics screening of urine, the authors identified a 14-metabolite signature that was altered in DKD and that provided evidence for intra-renal mitochondrial dysfunction as an important pathophysiological abnormality.
Noh H, King GL. The role of protein kinase C activation in diabetic nephropathy. Kidney Int Suppl. 2007;106:S49–53.
Derubertis FR, Craven PA. Activation of protein kinase C in glomerular cells in diabetes. Mechanisms and potential links to the pathogenesis of diabetic glomerulopathy. Diabetes. 1994;43:1–8.
Hayashi T, Takai S, Yamashita C. Impact of the renin-angiotensin-aldosterone-system on cardiovascular and renal complications in diabetes mellitus. Curr Vasc Pharmacol. 2010;8:189–97.
Vargas SL, Toma I, Kang JJ, Meer EJ, Peti-Peterdi J. Activation of the succinate receptor GPR91 in macula densa cells causes renin release. J Am Soc Nephrol. 2009;20:1002–11.
Wolf G, Mueller E, Stahl RA, Ziyadeh FN. Angiotensin II-induced hypertrophy of cultured murine proximal tubular cells is mediated by endogenous transforming growth factor-beta. J Clin Invest. 1993;92:1366–72.
Kalinyak JE, Sechi LA, Griffin CA, Don BR, Tavangar K, Kraemer FB, et al. The renin-angiotensin system in streptozotocin-induced diabetes mellitus in the rat. J Am Soc Nephrol. 1993;4:1337–45.
Tesch GH. MCP-1/CCL2: a new diagnostic marker and therapeutic target for progressive renal injury in diabetic nephropathy. Am J Physiol Renal Physiol. 2008;294:F697–701.
Wada T, Yokoyama H, Matsushima K, Kobayashi K. Monocyte chemoattractant protein-1: does it play a role in diabetic nephropathy? Nephrol Dial Transplant. 2003;18:457–9.
Yadav A, Vallabu S, Arora S, Tandon P, Slahan D, Teichberg S, et al. ANG II promotes autophagy in podocytes. Am J Physiol Cell Physiol. 2010;299:C488–96.
Sun L, Kanwar YS. Relevance of TNF-alpha in the context of other inflammatory cytokines in the progression of diabetic nephropathy. Kidney Int. 2015;88:662–5. This recent review focusses on clinical and experimental evidence for the role of TNF-α in the pathogenesis of DKD.
Rodriguez-Iturbe B, Pons H, Herrera-Acosta J, Johnson RJ. Role of immunocompetent cells in nonimmune renal diseases. Kidney Int. 2001;59:1626–40.
Di Paolo S, Gesualdo L, Ranieri E, Grandaliano G, Schena FP. High glucose concentration induces the overexpression of transforming growth factor-beta through the activation of a platelet-derived growth factor loop in human mesangial cells. Am J Pathol. 1996;149:2095–106.
Schena FP, Gesualdo L. Pathogenetic mechanisms of diabetic nephropathy. J Am Soc Nephrol. 2005;16 Suppl 1:S30–3.
Furuta T, Saito T, Ootaka T, Soma J, Obara K, Abe K, et al. The role of macrophages in diabetic glomerulosclerosis. Am J Kidney Dis. 1993;21:480–5.
Nguyen D, Ping F, Mu W, Hill P, Atkins RC, Chadban SJ. Macrophage accumulation in human progressive diabetic nephropathy. Nephrol (Carlton). 2006;11:226–31.
Lim A. Diabetic nephropathy—complications and treatment. Int J Nephrol Renovasc Dis. 2014;7:361–81.
Bending JJ, Lobo-Yeo A, Vergani D, Viberti GC. Proteinuria and activated T-lymphocytes in diabetic nephropathy. Diabetes. 1988;37:507–11.
Ilan Y, Maron R, Tukpah AM, Maioli TU, Murugaiyan G, Yang K, et al. Induction of regulatory T cells decreases adipose inflammation and alleviates insulin resistance in ob/ob mice. Proc Natl Acad Sci U S A. 2010;107:9765–70.
Eller K, Kirsch A, Wolf AM, Sopper S, Tagwerker A, Stanzl U, et al. Potential role of regulatory T cells in reversing obesity-linked insulin resistance and diabetic nephropathy. Diabetes. 2011;60:2954–62.
Griffin MD, Elliman SJ, Cahill E, English K, Ceredig R, Ritter T. Concise review: adult mesenchymal stromal cell therapy for inflammatory diseases: how well are we joining the dots? Stem Cells. 2013;31:2033–41. This recent review provides a critical evaluation of current progress in understanding the anti-inflammatory properties of MSCs and in developing successful MSC therapies for human inflammatory diseases with emphasis on key challenges in the translational process.
Alpers CE, Hudkins KL. Mouse models of diabetic nephropathy. Curr Opin Nephrol Hypertens. 2011;20:278–84.
Pan XH, Yang XY, Yao X, Sun XM, Zhu L, Wang JX, et al. Bone-marrow mesenchymal stem cell transplantation to treat diabetic nephropathy in tree shrews. Cell Biochem Funct. 2014;32:453–63.
Fan Y, Huang ZY, Cao CC, Chen CS, Chen YX, Fan DD, et al. Genome of the Chinese tree shrew. Nat Commun. 2013;4:1426.
Xu L, Chen SY, Nie WH, Jiang XL, Yao YG. Evaluating the phylogenetic position of Chinese tree shrew (Tupaia belangeri chinensis) based on complete mitochondrial genome: implication for using tree shrew as an alternative experimental animal to primates in biomedical research. J Genet Genomics. 2012;39:131–7.
Rabb GB, Getty RE, Williamson WM, Lombard LS. Spontaneous diabetes mellitus in tree shrews, Urogale everetti. Diabetes. 1966;15:327–30.
Wu X, Chang Q, Zhang Y, Zou X, Chen L, Zhang L, et al. Relationships between body weight, fasting blood glucose concentration, sex and age in tree shrews (Tupaia belangeri chinensis). J Anim Physiol Anim Nutr (Berl). 2013;97:1179–88.
Gurley SB, Clare SE, Snow KP, Hu A, Meyer TW, Coffman TM. Impact of genetic background on nephropathy in diabetic mice. Am J Physiol Renal Physiol. 2006;290:F214–22.
Kong LL, Wu H, Cui WP, Zhou WH, Luo P, Sun J, et al. Advances in murine models of diabetic nephropathy. J Diabetes Res. 2013;2013:797548.
Zhang L, Li K, Liu X, Li D, Luo C, Fu B, et al. Repeated systemic administration of human adipose-derived stem cells attenuates overt diabetic nephropathy in rats. Stem Cell Dev. 2013;22:3074–86. In this pre-clinical study, repeated intravenous administration of human adipose-derived MSCs resulted in improvements to albuminuria and structural features of renal damage in an accelerated model of DKD in rat.
Lee RH, Seo MJ, Reger RL, Spees JL, Pulin AA, Olson SD, et al. Multipotent stromal cells from human marrow home to and promote repair of pancreatic islets and renal glomeruli in diabetic NOD/scid mice. Proc Natl Acad Sci U S A. 2006;103:17438–43.
Devarapu SK, Junhui X, Darisipudi M, Rocanin Arjo A, Anders HJ. CD362+ mesenchymal stem cell treatment of kidney disease in type 2 diabetic Lepr db/db mice. Nephrol Dial Transplant. 2015;30 suppl 3:iii223–4.
Tay YC, Wang Y, Kairaitis L, Rangan GK, Zhang C, Harris DC. Can murine diabetic nephropathy be separated from superimposed acute renal failure? Kidney Int. 2005;68:391–8.
Bruno S, Grange C, Deregibus MC, Calogero RA, Saviozzi S, Collino F, et al. Mesenchymal stem cell-derived microvesicles protect against acute tubular injury. J Am Soc Nephrol. 2009;20:1053–67.
Herrera MB, Bussolati B, Bruno S, Fonsato V, Romanazzi GM, Camussi G. Mesenchymal stem cells contribute to the renal repair of acute tubular epithelial injury. Int J Mol Med. 2004;14:1035–41.
Ezquer F, Ezquer M, Simon V, Pardo F, Yanez A, Carpio D, et al. Endovenous administration of bone-marrow-derived multipotent mesenchymal stromal cells prevents renal failure in diabetic mice. Biol Blood Marrow Transplant. 2009;15:1354–65.
Kraynak AR, Storer RD, Jensen RD, Kloss MW, Soper KA, Clair JH, et al. Extent and persistence of streptozotocin-induced DNA damage and cell proliferation in rat kidney as determined by in vivo alkaline elution and BrdUrd labeling assays. Toxicol Appl Pharmacol. 1995;135:279–86.
Tesch GH, Allen TJ. Rodent models of streptozotocin-induced diabetic nephropathy. Nephrol (Carlton). 2007;12:261–6.
Hudkins KL, Pichaiwong W, Wietecha T, Kowalewska J, Banas MC, Spencer MW, et al. BTBR Ob/Ob mutant mice model progressive diabetic nephropathy. J Am Soc Nephrol. 2010;21:1533–42.
Xu J, Huang Y, Li F, Zheng S, Epstein PN. FVB mouse genotype confers susceptibility to OVE26 diabetic albuminuria. Am J Physiol Renal Physiol. 2010;299:F487–94.
Zhao HJ, Wang S, Cheng H, Zhang MZ, Takahashi T, Fogo AB, et al. Endothelial nitric oxide synthase deficiency produces accelerated nephropathy in diabetic mice. J Am Soc Nephrol. 2006;17:2664–9.
Fang Y, Tian X, Bai S, Fan J, Hou W, Tong H, et al. Autologous transplantation of adipose-derived mesenchymal stem cells ameliorates streptozotocin-induced diabetic nephropathy in rats by inhibiting oxidative stress, pro-inflammatory cytokines and the p38 MAPK signaling pathway. Int J Mol Med. 2012;30:85–92.
Ezquer FE, Ezquer ME, Parrau DB, Carpio D, Yanez AJ, Conget PA. Systemic administration of multipotent mesenchymal stromal cells reverts hyperglycemia and prevents nephropathy in type 1 diabetic mice. Biol Blood Marrow Transplant. 2008;14:631–40.
Abdel Aziz MT, Wassef MA, Ahmed HH, Rashed L, Mahfouz S, Aly MI, et al. The role of bone marrow derived-mesenchymal stem cells in attenuation of kidney function in rats with diabetic nephropathy. Diabetol Metab Syndr. 2014;6:34.
Lv S, Cheng J, Sun A, Li J, Wang W, Guan G, et al. Mesenchymal stem cells transplantation ameliorates glomerular injury in streptozotocin-induced diabetic nephropathy in rats via inhibiting oxidative stress. Diabetes Res Clin Pract. 2014;104:143–54.
Lv SS, Liu G, Wang JP, Wang WW, Cheng J, Sun AL, et al. Mesenchymal stem cells transplantation ameliorates glomerular injury in streptozotocin-induced diabetic nephropathy in rats via inhibiting macrophage infiltration. Int Immunopharmacol. 2013;17:275–82. In this study, administration of autologous bone marrow-derived MSCs to rats with streptozotocin-induced DM resulted in improvements in the severity of DKD with reduced intra-renal expression of MCP-1 and pro-inflammatory cytokines as well as reduced renal macrophage infiltration.
Wang S, Li Y, Zhao J, Zhang J, Huang Y. Mesenchymal stem cells ameliorate podocyte injury and proteinuria in a type 1 diabetic nephropathy rat model. Biol Blood Marrow Transplant. 2013;19:538–46.
Zhou H, Tian HM, Long Y, Zhang XX, Zhong L, Deng L, et al. Mesenchymal stem cells transplantation mildly ameliorates experimental diabetic nephropathy in rats. Chin Med J. 2009;122:2573–9.
Li D, Wang N, Zhang L, Hanyu Z, Xueyuan B, Fu B, et al. Mesenchymal stem cells protect podocytes from apoptosis induced by high glucose via secretion of epithelial growth factor. Stem Cell Res Ther. 2013;4:103. This mechanistic study provided evidence that epithelial growth factor secreted by human adipose-derived MSCs protect podocytes from hyperglycaemia-induced apoptosis.
Park JH, Hwang I, Hwang SH, Han H, Ha H. Human umbilical cord blood-derived mesenchymal stem cells prevent diabetic renal injury through paracrine action. Diabetes Res Clin Pract. 2012;98:465–73.
Park JH, Park J, Hwang SH, Han H, Ha H. Delayed treatment with human umbilical cord blood-derived stem cells attenuates diabetic renal injury. Transplant Proc. 2012;44:1123–6.
Davey GC, Patil SB, O'Loughlin A, O'Brien T. Mesenchymal stem cell-based treatment for microvascular and secondary complications of diabetes mellitus. Front Endocrinol. 2014;5:86.
Zhang Y, Ye C, Wang G, Gao Y, Tan K, Zhuo Z, et al. Kidney-targeted transplantation of mesenchymal stem cells by ultrasound-targeted microbubble destruction promotes kidney repair in diabetic nephropathy rats. BioMed Res Int. 2013;2013:526367.
Ezquer F, Ezquer M, Contador D, Ricca M, Simon V, Conget P. The anti-diabetic effect of mesenchymal stem cells is unrelated to their transdifferentiation potential but to their capability to restore Th1/Th2 balance and to modify the pancreatic microenvironment. Stem Cells. 2012;30:1664–74.
Hess D, Li L, Martin M, Sakano S, Hill D, Strutt B, et al. Bone marrow-derived stem cells initiate pancreatic regeneration. Nat Biotechnol. 2003;21:763–70.
Madec AM, Mallone R, Afonso G, Abou Mrad E, Mesnier A, Eljaafari A, et al. Mesenchymal stem cells protect NOD mice from diabetes by inducing regulatory T cells. Diabetologia. 2009;52:1391–9.
Ezquer ME, Ezquer FE, Arango-Rodriguez ML, Conget PA. MSC transplantation: a promising therapeutic strategy to manage the onset and progression of diabetic nephropathy. Biol Res. 2012;45:289–96.
Marquez-Curtis LA, Janowska-Wieczorek A. Enhancing the migration ability of mesenchymal stromal cells by targeting the SDF-1/CXCR4 axis. Biomed Res Int. 2013;2013:561098.
Wu S, Li L, Wang G, Shen W, Xu Y, Liu Z, et al. Ultrasound-targeted stromal cell-derived factor-1-loaded microbubble destruction promotes mesenchymal stem cell homing to kidneys in diabetic nephropathy rats. Int J Nanomedicine. 2014;9:5639–51. The authors of this innovative study demonstrated that release of SDF-1 in the kidney by USTMD resulted in increased homing of intravenously administered MSCs and improved MSC efficacy in a rat model of DKD.
Chen S, Ding JH, Bekeredjian R, Yang BZ, Shohet RV, Johnston SA, et al. Efficient gene delivery to pancreatic islets with ultrasonic microbubble destruction technology. Proc Natl Acad Sci U S A. 2006;103:8469–74.
Viberti GC, Hill RD, Jarrett RJ, Argyropoulos A, Mahmud U, Keen H. Microalbuminuria as a predictor of clinical nephropathy in insulin-dependent diabetes mellitus. Lancet. 1982;1:1430–2.
Parving HH, Oxenboll B, Svendsen PA, Christiansen JS, Andersen AR. Early detection of patients at risk of developing diabetic nephropathy. A longitudinal study of urinary albumin excretion. Acta Endocrinol (Copenh). 1982;100:550–5.
Mogensen CE, Christensen CK. Predicting diabetic nephropathy in insulin-dependent patients. N Engl J Med. 1984;311:89–93.
Garrahy A, Tormey WP. Pitfalls of the urinary albumin creatinine ratio in detection of early diabetic kidney disease. Ir Med J. 2015;108:102–3.
Ismail N, Becker B, Strzelczyk P, Ritz E. Renal disease and hypertension in non-insulin-dependent diabetes mellitus. Kidney Int. 1999;55:1–28.
Caramori ML, Fioretto P, Mauer M. The need for early predictors of diabetic nephropathy risk: is albumin excretion rate sufficient? Diabetes. 2000;49:1399–408.
Stevens PE, Levin A, Kidney Disease: Improving Global Outcomes Chronic Kidney Disease Guideline Development Work Group Members. Evaluation and management of chronic kidney disease: synopsis of the kidney disease: improving global outcomes 2012 clinical practice guideline. Ann Intern Med. 2013;158:825–30.
Currie G, McKay G, Delles C. Biomarkers in diabetic nephropathy: present and future. World J Diabetes. 2014;5:763–76.
Fassett RG, Venuthurupalli SK, Gobe GC, Coombes JS, Cooper MA, Hoy WE. Biomarkers in chronic kidney disease: a review. Kidney Int. 2011;80:806–21.
Pena MJ, Lambers Heerspink HJ, Hellemons ME, Friedrich T, Dallmann G, Lajer M, et al. Urine and plasma metabolites predict the development of diabetic nephropathy in individuals with type 2 diabetes mellitus. Diabet Med. 2014;31(9):1138–47.
Navarro JF, Mora C, Macıéa M, Garcıéa J. Inflammatory parameters are independently associated with urinary albumin in type 2 diabetes mellitus. Am J Kidney Dis. 2003;42:53–61.
Navarro JF, Mora C, Gomez M, Muros M, Lopez-Aguilar C, Garcia J. Influence of renal involvement on peripheral blood mononuclear cell expression behaviour of tumour necrosis factor- and interleukin-6 in type 2 diabetic patients. Nephrol Dial Transplant. 2007;23:919–26.
Navarro JF, Mora C, Muros M, Garcia J. Urinary tumour necrosis factor- excretion independently correlates with clinical markers of glomerular and tubulointerstitial injury in type 2 diabetic patients. Nephrol Dial Transplant. 2006;21:3428–34.
Niewczas MA, Ficociello LH, Johnson AC, Walker W, Rosolowsky ET, Roshan B, et al. Serum concentrations of markers of TNF and Fas-mediated pathways and renal function in nonproteinuric patients with type 1 diabetes. Clin J Am Soc Nephrol. 2009;4:62–70.
Gohda T, Niewczas MA, Ficociello LH, Walker WH, Skupien J, Rosetti F, et al. Circulating TNF receptors 1 and 2 predict stage 3 CKD in type 1 diabetes. J Am Soc Nephrol. 2012;23:516–24.
Niewczas MA, Gohda T, Skupien J, Smiles AM, Walker WH, Rosetti F, et al. Circulating TNF receptors 1 and 2 predict ESRD in type 2 diabetes. J Am Soc Nephrol. 2012;23:507–15. This biomarker study provides strong evidence that elevated serum sTNFR 1 and 2 concentrations in subjects with type 2 diabetes mellitus predict progression to ESRD.
Christou GA, Kiortsis DN. The role of adiponectin in renal physiology and development of albuminuria. J Endocrinol. 2014;221:R49–61.
Sharma K, Ramachandrarao S, Qiu G, Usui HK, Zhu Y, Dunn SR, et al. Adiponectin regulates albuminuria and podocyte function in mice. J Clin Invest. 2008;118:1645–56.
Ohashi N, Kato A, Misaki T, Sakakima M, Fujigaki Y, Yamamoto T, et al. Association of serum adiponectin levels with all-cause mortality in hemodialysis patients. Intern Med. 2008;47:485–91.
Nakamaki S, Satoh H, Kudoh A, Hayashi Y, Hirai H, Watanabe T. Adiponectin reduces proteinuria in streptozotocin-induced diabetic Wistar rats. Exp Biol Med. 2011;236:614–20.
Tsioufis C, Dimitriadis K, Chatzis D, Vasiliadou C, Tousoulis D, Papademetriou V, et al. Relation of microalbuminuria to adiponectin and augmented C-reactive protein levels in men with essential hypertension. Am J Cardiol. 2005;96:946–51.
Barlovic DP, Zaletel J, Prezelj J. Association between adiponectin and low-grade albuminuria is BMI-dependent in type 2 diabetes. Kidney Blood Press Res. 2010;33:405–10.
Barlovic DP, Zaletel J, Prezelj J. Adipocytokines are associated with renal function in patients with normal range glomerular filtration rate and type 2 diabetes. Cytokine. 2009;46:142–5.
Tamba S, Nakatsuji H, Kishida K, Noguchi M, Ogawa T, Okauchi Y, et al. Relationship between visceral fat accumulation and urinary albumin-creatinine ratio in middle-aged Japanese men. Atherosclerosis. 2010;211:601–5.
Jorsal A, Petersen EH, Tarnow L, Hess G, Zdunek D, Frystyk J, et al. Urinary adiponectin excretion rises with increasing albuminuria in type 1 diabetes. J Diabetes Complications. 2013;27:604–8.
Fujita H, Morii T, Koshimura J, Ishikawa M, Kato M, Miura T, et al. Possible relationship between adiponectin and renal tubular injury in diabetic nephropathy. Endocr J. 2006;53:745–52.
Koshimura J, Fujita H, Narita T, Shimotomai T, Hosoba M, Yoshioka N, et al. Urinary adiponectin excretion is increased in patients with overt diabetic nephropathy. Biochem Biophys Res Commun. 2004;316:165–9.
Looker HC, Krakoff J, Funahashi T, Matsuzawa Y, Tanaka S, Nelson RG, et al. Adiponectin concentrations are influenced by renal function and diabetes duration in Pima Indians with type 2 diabetes. J Clin Endocrinol Metab. 2004;89:4010–7.
Costacou T, Zgibor JC, Evans RW, Otvos J, Lopes-Virella MF, Tracy RP, et al. The prospective association between adiponectin and coronary artery disease among individuals with type 1 diabetes. The Pittsburgh Epidemiology of Diabetes Complications Study. Diabetologia. 2005;48:41–8.
Frystyk J, Tarnow L, Hansen TK, Parving HH, Flyvbjerg A. Increased serum adiponectin levels in type 1 diabetic patients with microvascular complications. Diabetologia. 2005;48:1911–8.
Schalkwijk CG, Chaturvedi N, Schram MT, Fuller JH, Stehouwer CD, Group EPCS. Adiponectin is inversely associated with renal function in type 1 diabetic patients. J Clin Endocrinol Metab. 2006;91:129–35.
Kacso IM, Bondor CI, Kacso G. Plasma adiponectin is related to the progression of kidney disease in type 2 diabetes patients. Scand J Clin Lab Invest. 2012;72:333–9.
Saraheimo M, Forsblom C, Thorn L, Waden J, Rosengard-Barlund M, Heikkila O, et al. Serum adiponectin and progression of diabetic nephropathy in patients with type 1 diabetes. Diabetes Care. 2008;31:1165–9.
Panduru NM, Saraheimo M, Forsblom C, Thorn LM, Gordin D, Waden J, et al. Urinary adiponectin is an independent predictor of progression to end-stage renal disease in patients with type 1 diabetes and diabetic nephropathy. Diabetes Care. 2015;38:883–90. This recent study from the FinnDiane study group demonstrated that urinary adiponectin independently predicts progression from macro-albuminuria to ESRD in type 1 DM.
Fu W-J, Li B-L, Wang S-B, Chen M-L, Deng R-T, Ye C-Q, et al. Changes of the tubular markers in type 2 diabetes mellitus with glomerular hyperfiltration. Diabetes Res Clin Pract. 2012;95:105–9.
Yang Y-H, He X-J, Chen S-R, Wang L, Li E-M, Xu L-Y. Changes of serum and urine neutrophil gelatinase-associated lipocalin in type-2 diabetic patients with nephropathy: one year observational follow-up study. Endocrine. 2009;36:45–51.
Nielsen SE, Sugaya T, Hovind P, Baba T, Parving HH, Rossing P. Urinary liver-type fatty acid-binding protein predicts progression to nephropathy in type 1 diabetic patients. Diabetes Care. 2010;33:1320–4.
Bolignano D, Lacquaniti A, Coppolino G, Donato V, Fazio MR, Nicocia G, et al. Neutrophil gelatinase-associated lipocalin as an early biomarker of nephropathy in diabetic patients. Kidney Blood Press Res. 2009;32:91–8.
Nielsen SE, Reinhard H, Zdunek D, Hess G, Gutiérrez OM, Wolf M, et al. Tubular markers are associated with decline in kidney function in proteinuric type 2 diabetic patients. Diabetes Res Clin Pract. 2012;97:71–6.
Chou K-M, Lee C-C, Chen C-H, Sun C-Y. Clinical value of NGAL, L-FABP and albuminuria in predicting GFR decline in type 2 diabetes mellitus patients. PLoS One. 2013;8:e54863.
Conway BR, Manoharan D, Manoharan D, Jenks S, Dear JW, McLachlan S, et al. Measuring urinary tubular biomarkers in type 2 diabetes does not add prognostic value beyond established risk factors. Kidney Int. 2012;82:812–8.
Lee CH, Lam KS. Biomarkers of progression in diabetic nephropathy: the past, present and future. J Diabetes Investig. 2015;6:247–9.
Titan SM, Zatz R, Graciolli FG, dos Reis LM, Barros RT, Jorgetti V, et al. FGF-23 as a predictor of renal outcome in diabetic nephropathy. Clin J Am Soc Nephrol. 2011;6:241–7.
Lee CH, Hui EY, Woo YC, Yeung CY, Chow WS, Yuen MM, et al. Circulating fibroblast growth factor 21 levels predict progressive kidney disease in subjects with type 2 diabetes and normoalbuminuria. J Clin Endocrinol Metab. 2015;100:1368–75.
Sabbisetti VS, Waikar SS, Antoine DJ, Smiles A, Wang C, Ravisankar A, et al. Blood kidney injury molecule-1 is a biomarker of acute and chronic kidney injury and predicts progression to ESRD in type I diabetes. J Am Soc Nephrol. 2014;25:2177–86.
van Timmeren MM, van den Heuvel MC, Bailly V, Bakker SJL, van Goor H, Stegeman CA. Tubular kidney injury molecule-1 (KIM-1) in human renal disease. J Pathol. 2007;212:209–17.
Vaidya VS, Niewczas MA, Ficociello LH, Johnson AC, Collings FB, Warram JH, et al. Regression of microalbuminuria in type 1 diabetes is associated with lower levels of urinary tubular injury biomarkers, kidney injury molecule-1, and N-acetyl-beta-D-glucosaminidase. Kidney Int. 2011;79:464–70.
Nielsen SE, Andersen S, Zdunek D, Hess G, Parving HH, Rossing P. Tubular markers do not predict the decline in glomerular filtration rate in type 1 diabetic patients with overt nephropathy. Kidney Int. 2011;79:1113–8.
Nielsen SE, Rossing K, Hess G, Zdunek D, Jensen BR, Parving H-H, et al. The effect of RAAS blockade on markers of renal tubular damage in diabetic nephropathy: u-NGAL, u-KIM1 and u-LFABP. Scand J Clin Lab Invest. 2012;72:137–42.
Looker HC, Colombo M, Hess S, Brosnan MJ, Farran B, Dalton RN, et al. Biomarkers of rapid chronic kidney disease progression in type 2 diabetes. Kidney Int. 2015;88(4):888–96. In this study the authors screened a large number of putative biomarkers for associations with DKD progression. A panel of 14 biomarkers including FGF-21, symmetric to asymmetric dimethylarginine ratio, β2-microglobulin, C16-acylcarnitine and KIM-1 was identified as improving the prediction of rapidly progressive decline in eGFR when added to clinical predictors.
Hovind P, Tarnow L, Oestergaard PB, Parving H-H. Elevated vascular endothelial growth factor in type 1 diabetic patients with diabetic nephropathy. Kidney Int. 2000;57(s75):56–61.
Kim NH, Kim KB, Kim DL, Kim SG, Choi KM, Baik SH, et al. Plasma and urinary vascular endothelial growth factor and diabetic nephropathy in type 2 diabetes mellitus. Diabet Med. 2004;21:545–51.
Kim NH, Oh JH, Seo JA, Lee KW, Kim SG, Choi KM, et al. Vascular endothelial growth factor (VEGF) and soluble VEGF receptor FLT-1 in diabetic nephropathy. Kidney Int. 2005;67:167–77.
Santilli F, Spagnoli A, Mohn A, Tumini S, Verrotti A, Cipollone F, et al. Increased vascular endothelial growth factor serum concentrations may help to identify patients with onset of type 1 diabetes during childhood at risk for developing persistent microalbuminuria. J Clin Endocrinol Metab. 2001;86:3871–6.
D'Angio CT, Ambati J, Phelps DL. Do urinary levels of vascular endothelial growth factor predict proliferative retinopathy? Curr Eye Res. 2001;22:90–4.
Fiseha T. Urinary biomarkers for early diabetic nephropathy in type 2 diabetic patients. Biomark Res. 2015;3:16.
Robles-Osorio ML, Sabath E. Tubular dysfunction and non-albuminuric renal disease in subjects with type 2 diabetes mellitus. Rev Invest Clin. 2014;66:234–9.
Hong CY, Hughes K, Chia KS, Ng V, Ling SL. Urinary 1-microglobulin as a marker of nephropathy in type 2 diabetic Asian subjects in Singapore. Diabetes Care. 2003;26:338–42.
Petrica L, Vlad A, Gluhovschi G, Gadalean F, Dumitrascu V, Gluhovschi C, et al. Proximal tubule dysfunction is associated with podocyte damage biomarkers nephrin and vascular endothelial growth factor in type 2 diabetes mellitus patients: a cross-sectional study. PLoS One. 2014;9:e112538.
Petrica L, Petrica M, Vlad A, Jianu DC, Gluhovschi G, Ianculescu C, et al. Proximal tubule dysfunction is dissociated from endothelial dysfunction in normoalbuminuric patients with type 2 diabetes mellitus: a cross-sectional study. Nephron Clin Pract. 2011;118:c155–64.
Fliser D, Novak J, Thongboonkerd V, Argiles A, Jankowski V, Girolami MA, et al. Advances in urinary proteome analysis and biomarker discovery. J Am Soc Nephrol. 2007;18:1057–71.
Mischak H, Coon JJ, Novak J, Weissinger EM, Schanstra JP, Dominiczak AF. Capillary electrophoresis-mass spectrometry as a powerful tool in biomarker discovery and clinical diagnosis: an update of recent developments. Mass Spectrom Rev. 2009;28:703–24.
Mischak H, Delles C, Klein J, Schanstra JP. Urinary proteomics based on capillary electrophoresis-coupled mass spectrometry in kidney disease: discovery and validation of biomarkers, and clinical application. Adv Chronic Kidney Dis. 2010;17:493–506.
Good DM, Zurbig P, Argiles A, Bauer HW, Behrens G, Coon JJ, et al. Naturally occurring human urinary peptides for use in diagnosis of chronic kidney disease. Mol Cell Proteomics. 2010;9:2424–37.
Argiles A, Siwy J, Duranton F, Gayrard N, Dakna M, Lundin U, et al. CKD273, a new proteomics classifier assessing CKD and its prognosis. PLoS One. 2013;8:e62837.
Siwy J, Schanstra JP, Argiles A, Bakker SJL, Beige J, Boucek P, et al. Multicentre prospective validation of a urinary peptidome-based classifier for the diagnosis of type 2 diabetic nephropathy. Nephrol Dial Transplant. 2014;29:1563–70. This study provided the first validation of the CKD273 urinary proteome-based classifier of DKD in a multicentre prospective setting involving type 2 diabetic subjects.
Roscioni SS, de Zeeuw D, Hellemons ME, Mischak H, Zürbig P, Bakker SJL, et al. A urinary peptide biomarker set predicts worsening of albuminuria in type 2 diabetes mellitus. Diabetologia. 2012;56:259–67.
Zurbig P, Jerums G, Hovind P, MacIsaac RJ, Mischak H, Nielsen SE, et al. Urinary proteomics for early diagnosis in diabetic nephropathy. Diabetes. 2012;61:3304–13.
Cantaluppi V, Biancone L, Quercia A, Deregibus MC, Segoloni G, Camussi G. Rationale of mesenchymal stem cell therapy in kidney injury. Am J Kidney Dis. 2013;61:300–9.
Packham DK, Fraser I, Kerr PG, Lichliter J, Itescu S, Skerrett D, et al. Mesenchymal stem cell therapy for diabetic nephropathy: a phase 2 randomized controlled trial. Diabetes. 2015;64(Suppl 1A):LB6. Although only reported in abstract form to date, the preliminary results for this completed Phase I/II trial provide key insights into the safety and potential efficacy of MSC therapy for established DKD.
Acknowledgments
The authors are supported by grants from the European Commission [Horizon 2020 Collaborative Health Project NEPHSTROM (grant number 634086; TPG, WPM, NI, TO’B, MDG) and FP7 Collaborative Health Project VISICORT (grant number 602470; MDG)] and from Science Foundation Ireland [REMEDI Strategic Research Cluster (grant number 09/SRC-B1794; TO’B, MDG) and CÚRAM Research Centre (grant number 13/RC/2073; TO’B, MDG)] and by the European Regional Development Fund. TPG is supported by a Hardiman Scholarship from the College of Medicine, Nursing and Health Science of the National University of Ireland, Galway.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Tomás P. Griffin declares that he has no conflict of interest.
William Patrick Martin reports grant support from the European Commission.
Nahidul Islam reports grant support from the European Commission.
Timothy O’Brien reports grants from the European Commission, Science Foundation Ireland, and Medtronic. He reports other from the European Regional Development Fund, Orbsen Therapeutics and Onkimmune. He reports personal fees from Merck Sharp and Dohme, Sanofi Regeneron, Eli Lilly and Novo Nordisk.
Matthew D. Griffin reports grants from the European Commission, Science Foundation Ireland and Randox Teoranta; and other from the European Regional Development Fund,
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Rights and permissions
About this article
Cite this article
Griffin, T.P., Martin, W.P., Islam, N. et al. The Promise of Mesenchymal Stem Cell Therapy for Diabetic Kidney Disease. Curr Diab Rep 16, 42 (2016). https://doi.org/10.1007/s11892-016-0734-6
Published:
DOI: https://doi.org/10.1007/s11892-016-0734-6