Abstract
Purpose of Review
This review summarizes the current management of patients with newly diagnosed aortic stenosis.
Recent Findings
Recent developments include detection of early myocardial dysfunction using serum B-type natriuretic peptide levels and global longitudinal strain, as well as ongoing trials of transcatheter aortic valve replacement in asymptomatic patients and patients with moderate aortic stenosis complicated by symptoms or left ventricular systolic dysfunction.
Summary
Given the high mortality associated with severe symptomatic aortic stenosis, all symptomatic patients should be referred for aortic valve replacement. Asymptomatic patients with left ventricular systolic dysfunction, abnormal exercise stress test, high degree of stenosis, rapid disease progression, or elevated serum B-type natriuretic peptide level may also have an indication for valve replacement, based on established criteria. The progress in management of severe aortic stenosis has been in the direction of earlier detection and earlier valve replacement.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Once symptomatic, severe aortic stenosis (AS) is a lethal disease. The chances of dying from severe symptomatic AS are approximately 50% within 1 year and 75% within 3 years without valve replacement [1, 2]. Early diagnosis and prompt aortic valve replacement (AVR) are the main priorities for the treating physician. Echocardiography is the most important diagnostic tool in AS with invasive hemodynamics and cardiac computed tomography (CT) standing by as important adjuncts. Hemodynamic markers of severe AS on echo include peak aortic valve velocity (Vmax) ≥ 4 m/s, mean transvalvular pressure gradient ≥ 40 mmHg, and calculated aortic valve area (AVA) ≤ 1.0 cm2. The first 2 parameters are measured directly and are usually reliable. In contrast, Doppler-derived AVA is less reliable and is not an absolute requirement for the diagnosis of severe AS [3••, 4]. In conditions of low flow, such as left ventricular (LV) failure or otherwise reduced forward cardiac output, standard high-gradient criteria are frequently not met, despite small calculated AVA. These patients are said to have low-flow, low-gradient severe aortic stenosis. For patients with reduced LVEF low-dose dobutamine stress testing can increase contractility and forward flow which can help differentiate true aortic stenosis (no change in AVA with flow augmentation) from pseudo-stenosis (increase in AVA with flow augmentation) due to insufficient opening forces. Patients with low-flow, low-gradient severe AS and normal LVEF are said to have a “paradoxical” low-flow, low-gradient severe AS. In such cases the confirmation of severe AS relies on careful analysis of multiple clinical and hemodynamic factors. A detailed discussion of workup of low-flow low-gradient aortic stenosis can be found in current clinical guidelines [3••, 4].
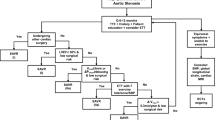
The current review is focused on patients who already have an established diagnosis of severe AS, regardless of flow state. Given the life-threatening nature of the disease, these patients should undergo rapid triage to determine the timing of valve replacement. The current risk-stratification is based on the presence of AS-related symptoms, LV dysfunction, and other high-risk factors [3••] (Fig. 1). The only effective treatment today remains aortic valve replacement (AVR) by surgical (SAVR) or transcatheter (TAVR) means.
Risk stratification and timing of valve replacement after the diagnosis of severe AS. AS, aortic stenosis; LV, left ventricle; LVEF, LV ejection fraction; Vmax, peak aortic valve velocity; BNP, brain natriuretic peptide. *Roman numerals/letters in parentheses denote the class (strength) of current guideline recommendations. (Adapted from: Otto et al. J Am Coll Cardiol. 2021 Feb, 77 4 e25–e197, with permission from Elsevier) [3••]
Symptoms
Before AS becomes symptomatic, there is a prolonged asymptomatic period during which the LV attempts to compensate for the increased afterload of the stenotic valve by variable degrees of concentric hypertrophy [5]. Occurrence of symptoms represents a pivotal moment in clinical course of severe AS. Ross and Braunwald mapped this natural history of AS in a relatively young AS population with rheumatic disease and with bicuspid valves [6] (Fig. 2A). While the demographics of severe AS have now changed to the majority being older with calcific disease, the precipitation of symptoms remains an ominous sign of decompensated severe AS (Fig. 2B). To date, only AVR, surgical or transcatheter, can prevent these patients from imminent and rapid decline (Fig. 3). Classic AS-related symptoms, in order of worsening prognosis, are heart failure, syncope, and angina [6] (Fig. 2A). Described in 1968, these symptoms are thought to reflect end-stage disease. Currently, largely due to earlier detection with widespread clinical use of echocardiography, the most common first presenting symptoms of AS are exertional — dyspnea on exertion or decreased exercise tolerance. Exertional dizziness (presyncope) or syncope and exertional angina are seen as well. Once symptomatic with severe AS, the risk of death begins to increase by approximately 2% per month [7, 8]. Prompt SAVR or TAVR, depending on individual circumstances, should be facilitated at this point (Fig. 1) [3••].
Natural history of aortic stenosis. A Natural course of aortic stenosis in the original (1968) description based largely on patients with rheumatic and bicuspid aortic valve disease. The onset of symptoms correlates with the sharp inflection point on the survival curve. B Natural history of aortic stenosis based on contemporary population with predominantly calcific (senile) AS and later symptom onset. (Reprinted from: Carabello. Circ Res. 2013; 113:179–185, with permission from Wolters Kluwer Health, Inc.) [5]
Effect of aortic valve replacement on survival. Survival with (black dots) and without (white dots) aortic valve replacement over the course of 5 years in patients with aortic stenosis. Numbers on the bottom indicate the number of patients in each cohort alive at the beginning of each follow up interval. (Reprinted from: Schwarz et al. Circ. 1982; 66:1105–1110, with permission from Wolters Kluwer Health, Inc.) [2]
LV Dysfunction
Although, in most cases, symptoms precede overt LV systolic dysfunction, in some patients, the LVEF begins to decline even while AS is still moderate [9]. When compensation by hypertrophy for high wall stress is no longer a match for the excess afterload from AS, the LVEF begins to decline [9, 10]. Akin to the occurrence of symptoms, this represents a sharp downward turn in clinical course [3••, 9] (Fig. 4). The occurrence of the decline in LV systolic function while AS is still moderate suggests that an otherwise unexpected LVEF < 60% in the setting of moderate AS may represent failure of hypertrophic compensation [9]. The current guidelines take a conservative approach in recommending AVR for asymptomatic severe AS and LVEF < 50%. In addition, progressive decline in LVEF on 3 serial studies to < 60% may be considered a trigger for AVR [3••]. Recent data suggest that asymptomatic patients may gain benefit from early AVR independent from their LVEF [11, 12]. Echocardiographic strain imaging, measuring shortening of myocardium by speckle tracking, allows earlier detection of myocardial dysfunction — before the LVEF decline. A recent meta-analysis of strain data from over a thousand asymptomatic patients with severe AS and LVEF > 50% revealed that impaired global longitudinal strain (cutoff at − 14.7%) is associated with 2.6 times higher chances of dying [13], (Fig. 5). These findings raise concern that using LVEF < = 50% as the trigger for intervention does not capture patients with lesser degree of myocardial dysfunction who may still benefit from AVR.
Decreased survival in severe AS patients with reduced LVEF. Survival of patients with severe AS during 6 years after initial diagnosis, stratified by LVEF. Patients with LVEF < 50% had significant higher mortality compared to those with preserved LVEF. (Reprinted from: Ito et al. J Am Coll Cardiol 2018; 71:1313–21, with permission from Elsevier) [9]
Decreased survival in severe AS patients with reduced global longitudinal strain. Kaplan–Meier survival curves illustrating higher mortality in severe AS patients with reduced global longitudinal strain in the population with LVEF > 50% (A) and a subset with LVEF > 60% (B). Survival rates at 2- and 4-year follow-up are indicated as percentages along the curves. (Reprinted from: Magne et al. J Am Coll Cardiol Img 2019; 12:84–92, with permission from Elsevier) [13]
Role of Stress Testing
Whether or not there are symptoms is a key question in timing aortic valve replacement in patients with severe AS. About half of these patients do not reveal symptoms on presentation and some may unconsciously scale down their activity level to below the symptomatic threshold. Clinical history is not always reliable, which becomes particularly clear when missed information can result in premature death. Therefore, confirming the asymptomatic state often requires objective assessment of symptoms with exercise tolerance testing (ETT). A positive ETT in patients with isolated severe AS has been associated with 7 times higher risk of appearance of symptoms or sudden death [14] (Fig. 6). On average, almost 50% of initially asymptomatic severe AS patients referred for ETT will reveal symptoms during the test [14–16]. These patients are considered symptomatic and should be referred for AVR. Realizing that not all symptoms with exercise may be due to AS, the following are considered specific: exertional dyspnea, heart failure, angina, syncope, or presyncope. In addition, decreased exercise tolerance adjusted for age and sex or a drop in systolic blood pressure by > = 10 mmHg from baseline to peak exercise are reasonable signs of symptomatic severe AS in need of intervention [3••]. Given the concern for serious hemodynamic complications, ETT of severe AS patients requires careful monitoring by an experienced clinician [3••]. Stress echocardiography may help uncover exertional LV systolic dysfunction. Encouragingly, a meta-analysis of 491 stress tests revealed no complications that required treatment during or after the stress test for severe AS [17].
Decreased survival in asymptomatic severe AS patients with abnormal exercise stress test. Probability of event-free survival during 5-year follow-up in patients with asymptomatic severe AS based on exercise stress test results. (Reprinted from: Amato et al. Heart. 2001; 86:381–386, with permission from BMJ Publishing Group Ltd.) [14]
Other High-Risk Markers
Other high-risk markers have been identified as reasonable triggers for AVR for asymptomatic severe AS patients who are at low risk of surgical complications. Currently, these include very severe AS reflected in AV Vmax ≥ 5 m/s; serum B-type natriuretic peptide (BNP) level elevated more than 3 times normal, and rapidly increasing AV Vmax by ≥ 0.3 m/s per year [3••].
Previously, Vmax ≥ 4.5 m/s was associated with increased risk of experiencing symptoms, cardiac surgery, or death [18]. Separately, Vmax > 5.5 m/s was associated with lower survival and higher chance of developing severe symptoms (NYHA class III or IV) than those with lower Vmax [19]. However, more recent outcome data from a larger population identified Vmax ≥ 5 m/s as the best indicator of high mortality risk [20] (Fig. 7A).
Other high-risk markers in asymptomatic severe AS. A Kaplan–Meier survival curves stratifying asymptomatic AS patients by their peak aortic velocity (AV Vmax). Patients with very severe AS (Vmax ≥ 5 m/s) had a higher mortality compared to those with Vmax < 5 m/s. (Reprinted from: Bohbot et al. Circ Cardiovasc Imaging. 2017;10(10), with permission from Wolters Kluwer Health, Inc.) [20]. B Composite incidence of AV-related death or heart failure hospitalizations in asymptomatic severe AS patients stratified by serum B-type natriuretic peptide (BNP) levels demonstrating worse outcomes in those with higher serum BNP. (Reprinted from: Nakatsuma et al. Heart 2019;105:384–390, with permission from BMJ Publishing Group Ltd.) [22]
Elevated BNP is one of the early signs of the LV’s inability to cope with the afterload imposed by severe AS. BNP levels parallel symptom severity and predict symptom onset as well as surgical outcomes [21]. Recent registry data on asymptomatic severe AS patients revealed that isolated increased BNP identified patients at high risk for AS-related death or hospitalization due to heart failure [22] (Fig. 7B). The current ACC/AHA guidelines recommend using BNP levels (> 3 times normal) as a reasonable trigger for AVR in asymptomatic AS patients [3].
There is significant individual variability in the rate of hemodynamic progression of aortic stenosis. Rapidly worsening hemodynamics of severe AS have been associated with higher risk of AS-related complications. Along with AV Vmax and functional status, the rate of AS progression independently predicts outcomes in asymptomatic patients [23]. Retrospective data stratified by how rapidly AV Vmax increased revealed significantly higher incidence of AS-related death or referral for AVR/balloon valvuloplasty in patients who progressed faster (increase in AV Vmax ≥ 0.22 m/s per year) [24]. Currently, AV Vmax increase at ≥ 0.3 m/s per year is a reasonable indication for AVR in asymptomatic severe AS patients with low surgical risk [3••].
Truly Asymptomatic Aortic Stenosis Without High-Risk Features
Truly asymptomatic patients with severe AS are reported to have low mortality risk of < 1% per year [3••]. These patients may be carefully observed, provided they promptly report onset of symptoms, with clinical and echocardiographic surveillance every 6–12 months. Most, however, will develop symptoms within 5 years [18]. Surgical risks should be taken into consideration, particularly in the asymptomatic elderly patient population with severe AS where their risk of sudden death, at least in some cases, could be lower than their risk of surgical mortality or serious morbidity. TAVR is less invasive, but there are not enough data to compare TAVR to SAVR in this population because asymptomatic patients were excluded from pivotal TAVR trials.
But while management of symptomatic severe aortic stenosis has once been called “one of the most straightforward in medicine” [7], namely valve replacement, management of truly asymptomatic severe AS patients with normal LV function and no high-risk features has been a subject of controversy. Advocates of a “watchful waiting” strategy have argued that the risk of sudden death in these patients is low; that surgical mortality varies widely in part dependent on surgical expertise, and that prosthetic valves are vulnerable to infectious, thrombotic, and degenerative complications [25]. In turn, the proponents of early AVR have argued that the risk of sudden death during “watchful waiting” is still higher than that in normal population, that pressure-induced LV dysfunction continues to occur during “watchful waiting” potentially leading to HF, that patients may not recognize symptoms, and that most will develop symptoms anyway within a few years [7]. Several nonrandomized studies, a meta-analysis of observational studies, and more recently 2 randomized trials of SAVR in asymptomatic severe AS — the RECOVERY trial and the AVATAR trial — demonstrated improved outcomes with early SAVR compared to a “watchful waiting” strategy [26•, 27•]. The EARLY TAVR trial is a currently ongoing randomized clinical trial evaluating TAVR vs. clinical surveillance in patients with truly asymptomatic (confirmed with ETT) severe aortic stenosis. This trial has completed enrollment; its initial results are expected soon and will shed even more light on the problem of timing of intervention for truly asymptomatic aortic stenosis without high-risk features.
Moderate AS
Another direction of research has been early treatment with TAVR of patients with symptomatic moderate AS. The EXPAND TAVR II Pivotal Trial is the first randomized clinical trial of TAVR using a self-expanding prosthesis (Medtronic Evolut PRO +) vs GDMT in patients with moderate, AS with symptoms or evidence of LV dysfunction, or for whom surgery is currently not recommended [28]. This study uses a composite primary safety endpoint of all-cause mortality, all-stroke, life-threatening or fatal bleeding, acute kidney injury, hospitalization due to device or procedure-related complication, or valve dysfunction requiring reintervention at 30 days. The primary effectiveness endpoint is the composite of all-cause mortality, heart failure, AVR or reintervention at 2 years. In parallel, a similar trial using a balloon-expandable TAVR platform (Edwards Sapien 3 Ultra) is underway — the Management of Moderate Aortic Stenosis by Clinical Surveillance or TAVR (PROGRESS) trial — a prospective, randomized, controlled, multicenter study of TAVR vs. clinical surveillance [29]. The results of these and other trials are likely to narrow down the search for optimal time of intervention in aortic stenosis.
Conclusion
Severe aortic stenosis tends to progress to its malignant form such that approximately 75% of symptomatic patients will die within 3 years of symptom onset without AVR. AVR (SAVR or TAVR, depending on clinical scenario) remains the only effective life-extending option and is recommended for all symptomatic patients with severe AS. Stress testing has an important role in identifying truly asymptomatic patients. Evidence of LV dysfunction is another important trigger for intervention. In addition, AVR is a reasonable route for patients with very severe AS, rapidly progressing disease, or elevated BNP levels. For those who reveal no symptoms or other high-risk features, increasing evidence suggests an early AVR strategy could be beneficial. The relatively new TAVR technology provides a less invasive valve replacement option to many patients who would not otherwise be candidates for AVR. In addition, there are ongoing randomized trials of TAVR vs. standard therapy in moderate symptomatic aortic stenosis as well as trials of early AVR in truly asymptomatic patients with severe AS. These data are likely to have a significant impact on future recommendations for these patient populations. Progress in the treatment of severe aortic stenosis to date has been in the direction of earlier detection and earlier intervention.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Leon MB, Smith CR, Mack M, Miller DC, Moses JW, Svensson LG, et al. Transcatheter aortic-valve implantation for aortic stenosis in patients who cannot undergo surgery. N Engl J Med. 2010;363(17):1597–607.
Schwarz F, Baumann P, Manthey J, Hoffmann M, Schuler G, Mehmel HC, et al. The effect of aortic valve replacement on survival. Circulation. 1982;66(5):1105–10.
•• Otto CM, Nishimura RA, Bonow RO, Carabello BA, Erwin JP 3rd, Gentile F, et al. 2020 ACC/AHA guideline for the management of patients with valvular heart disease: a report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation. 2021;77(4):e25–e197. https://doi.org/10.1016/j.jacc.2020.11.018. Latest American College of Cardiology/American Heart Association guidelines on diagnosis and management of valvular heart disease incorporating latest indications for transcathter aortic valve replacement.
Baumgartner H, Hung J, Bermejo J, Chambers JB, Evangelista A, Griffin BP, et al. Echocardiographic assessment of valve stenosis: EAE/ASE recommendations for clinical practice. J Am Soc Echocardiogr. 2009;22(1):1–23; quiz 101–2.
Carabello BA. Introduction to aortic stenosis. Circ Res. 2013;113(2):179–85.
Ross J Jr, Braunwald E. Aortic stenosis. Circulation. 1968;38(1 Suppl):61–7.
Carabello BA. Should severe aortic stenosis be operated on before symptom onset? Aortic valve replacement should be operated on before symptom onset. Circulation. 2012;126(1):112–7.
Kelly TA, Rothbart RM, Cooper CM, Kaiser DL, Smucker ML, Gibson RS. Comparison of outcome of asymptomatic to symptomatic patients older than 20 years of age with valvular aortic stenosis. Am J Cardiol. 1988;61(1):123–30.
Ito S, Miranda WR, Nkomo VT, Connolly HM, Pislaru SV, Greason KL, et al. Reduced left ventricular ejection fraction in patients with aortic stenosis. J Am Coll Cardiol. 2018;71(12):1313–21.
Koide M, Nagatsu M, Zile MR, Hamawaki M, Swindle MM, Keech G, et al. Premorbid determinants of left ventricular dysfunction in a novel model of gradually induced pressure overload in the adult canine. Circulation. 1997;95(6):1601–10.
Bohbot Y, de Meester de Ravenstein C, Chadha G, Rusinaru D, Belkhir K, Trouillet C, et al. Relationship between left ventricular ejection fraction and mortality in asymptomatic and minimally symptomatic patients with severe aortic stenosis. JACC Cardiovasc Imaging. 2019;12(1):38–48.
Perry AS, Li S. Optimal threshold of left ventricular ejection fraction for aortic valve replacement in asymptomatic severe aortic stenosis: a systematic review and meta-analysis. J Am Heart Assoc. 2021;10(7): e020252.
Magne J, Cosyns B, Popescu BA, Carstensen HG, Dahl J, Desai MY, et al. Distribution and prognostic significance of left ventricular global longitudinal strain in asymptomatic significant aortic stenosis: an individual participant data meta-analysis. JACC Cardiovasc Imaging. 2019;12(1):84–92.
Amato MC, Moffa PJ, Werner KE, Ramires JA. Treatment decision in asymptomatic aortic valve stenosis: role of exercise testing. Heart. 2001;86(4):381–6.
Saeed S, Rajani R, Seifert R, Parkin D, Chambers JB. Exercise testing in patients with asymptomatic moderate or severe aortic stenosis. Heart. 2018;104(22):1836–42.
Genereux P, Stone GW, O’Gara PT, Marquis-Gravel G, Redfors B, Giustino G, et al. Natural history, diagnostic approaches, and therapeutic strategies for patients with asymptomatic severe aortic stenosis. J Am Coll Cardiol. 2016;67(19):2263–88.
Rafique AM, Biner S, Ray I, Forrester JS, Tolstrup K, Siegel RJ. Meta-analysis of prognostic value of stress testing in patients with asymptomatic severe aortic stenosis. Am J Cardiol. 2009;104(7):972–7.
Pellikka PA, Sarano ME, Nishimura RA, Malouf JF, Bailey KR, Scott CG, et al. Outcome of 622 adults with asymptomatic, hemodynamically significant aortic stenosis during prolonged follow-up. Circulation. 2005;111(24):3290–5.
Rosenhek R, Zilberszac R, Schemper M, Czerny M, Mundigler G, Graf S, et al. Natural history of very severe aortic stenosis. Circulation. 2010;121(1):151–6.
Bohbot Y, Rusinaru D, Delpierre Q, Marechaux S, Tribouilloy C. Risk stratification of severe aortic stenosis with preserved left ventricular ejection fraction using peak aortic jet velocity: an outcome study. Circ Cardiovasc Imaging. 2017;10(10).
Bergler-Klein J, Klaar U, Heger M, Rosenhek R, Mundigler G, Gabriel H, et al. Natriuretic peptides predict symptom-free survival and postoperative outcome in severe aortic stenosis. Circulation. 2004;109(19):2302–8.
Nakatsuma K, Taniguchi T, Morimoto T, Shiomi H, Ando K, Kanamori N, et al. B-type natriuretic peptide in patients with asymptomatic severe aortic stenosis. Heart. 2019;105(5):384–90.
Otto CM, Burwash IG, Legget ME, Munt BI, Fujioka M, Healy NL, et al. Prospective study of asymptomatic valvular aortic stenosis. Clinical, echocardiographic, and exercise predictors of outcome. Circulation. 1997;95(9):2262–70.
Nishimura S, Izumi C, Nishiga M, Amano M, Imamura S, Onishi N, et al. Predictors of rapid progression and clinical outcome of asymptomatic severe aortic stenosis. Circ J. 2016;80(8):1863–9.
Shah PK. Should severe aortic stenosis be operated on before symptom onset? Severe aortic stenosis should not be operated on before symptom onset. Circulation. 2012;126(1):118–25.
• Kang DH, Park SW. Early surgery or conservative care for asymptomatic aortic stenosis. Reply N Engl J Med. 2020;382(2):111-119. This a randomized trial of early surgery vs. conservative care for asymptomatic patients with severe aortic stenosis. Early surgery was associated with less operative mortality or death from cardiovascular cause at 8-year follow up.
• Banovic M, Putnik S, Penicka M, Doros G, Deja MA, Kockova R, et al. Aortic valve replacement versus conservative treatment in asymptomatic severe aortic stenosis: the AVATAR trial. Circulation. 2022;145(9):648–58.This is a recent randomized trial of early surgery vs. conservative care for asymptomatic patients with severe aortic stenosis. Patients who underwent early surgery were less likely to experience death from any cause, acute myocardial infarction, stroke, or unplanned hospitalization for heart failure.
ClinicalTrials.gov. EXPAND TAVR II Pivotal Trial evaluating the Evolut™ TAVR platform 2021. [Available from: https://clinicaltrials.gov/ct2/show/NCT05149755.
ClinicalTrials.gov. PROGRESS: management of moderate aortic stenosis by clinical surveillance or TAVR (PROGRESS) 2021. [Available from: https://clinicaltrials.gov/ct2/show/NCT04889872.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Echocardiography
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Marcoff, L., Gillam, L.D. Aortic Stenosis: Risk Stratification and Timing of Surgery. Curr Cardiol Rep 25, 89–95 (2023). https://doi.org/10.1007/s11886-022-01835-w
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11886-022-01835-w