Abstract
Assessing left ventricular function is an essential part of the cardiovascular evaluation as it plays an important role in managing the patient and predicting prognosis. Recent advances in the imaging modalities currently allow a non-invasive comprehensive assessment of cardiac mechanics and precise estimation of cardiovascular hemodynamics. In this review, we will discuss and compare the currently available techniques and novel approaches utilized by echocardiography, cardiac magnetic resonance, and computed tomography for the assessment of global left ventricular performance.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Left ventricular (LV) size and function have a significant role in the evaluation, management, and prognosis of patients with arrhythmias, cardiomyopathies, coronary artery disease, congenital heart disease, systolic or diastolic heart failure, and valvular heart disease [1••, 2]. Therefore, an accurate assessment of LV function is essential in clinical cardiology and often plays a pivotal role in patient management [3,4,5]. Transthoracic echocardiography (echo) has been the most commonly used non-invasive modality for assessing LV size and function because of its portability, availability, and widely validated measurements. However, echo, cardiac magnetic resonance (CMR) imaging, and multidetector computed tomography (MDCT) acquisition and post-processing techniques have continued to evolve. The goal of this review is to outline the assessment of global myocardial function using these modalities.
Assessment of Global Left Ventricular Function:
LV performance is determined by preload (the initial sarcomere length, clinically determined by LV end-diastolic pressure (LVEDP) or end-diastolic volume (EDV)), afterload (the impedance of the vascular system against which the LV contracts, mainly determined by arterial elastance on the pressure-volume loop), contractility (inotropy), and diastolic function (lusitropy and chamber compliance) [6].
Non-invasively, various LV parameters have been suggested as surrogates for different aspects of overall global LV function—such as dimensions, volumes, ejection fraction (EF), contractility and deformation parameters, relaxation parameters, filling parameters, and end-diastolic pressure [7]. Global LV systolic function is most frequently assessed by measuring the difference in end-diastolic and end-systolic values in one dimension, two dimensions (2D), or three dimensions (3D) divided by the corresponding end-diastolic value [1••]. End-diastole is usually defined as the largest LV dimension or volume or that measured immediately after the closure of the mitral valve. End-systole is usually defined as the smallest LV dimension or volume or that measured immediately after the closure of the aortic valve.
Fractional Shortening
Dimensional fractional shortening is a measurement of the percent change in LV cavity dimension during systolic contraction and is calculated as the difference in the LV end-diastolic and LV end-systolic diameter divided by the LV end-diastolic diameter [1••]. This measurement can be obtained from 2D echo, 2D-targeted M-mode, CMR, or MDCT; however, this technique is no longer routinely used because of more advanced techniques based on 2D or 3D measurements. In addition, reference values depend on the technique used (e.g., −M-mode and 2D echo have different reference values) and whether measurements were made at the level of the mitral valve leaflet tips or mid ventricle.
Volumes and Ejection Fraction
Global LV volume estimates or measurements can be obtained from 2D or 3D methods, respectively. EF is calculated using the following formula: EF = (End diastolic volume (EDV) − End systolic volume (ESV)) / End diastolic volume (EDV). The accuracy of calculating these parameters is dependent on the precision in visualizing and delineating endocardial borders and having sufficient frame rate or temporal resolution to determine the exact frames that correspond to end-diastole and end-systole, respectively.
Acquisition Methods
Echocardiography
Echo is the most widely used technique for the evaluation of LV volume and EF due to its availability, relatively inexpensive, and lacking radiation exposure [8]. Traditionally, LV volumes can be calculated from linear or 2D measurements using formulae that are based on geometric assumptions of LV shape [9]. These formulae, especially the ones for the linear measurements, are more accurate in symmetric ventricles. Therefore, the current cardiac chamber quantification document of the American Society Echocardiography (ASE) and the European Association of Cardiovascular Imaging (EACVI) recommends against the use of the Teichholz and Quinones methods of calculating LV volumes [1••].
The most widely used 2D echo method for LV volumetric assessment and EF calculation is the biplane disk summation approach, i.e., the “modified Simpson’s rule.” In this method, it is important to trace the interface between the compacted myocardium and the LV cavity, with the inclusion of papillary muscles as part of the LV cavity, at end-diastole and end-systole in the apical four- and two-chamber views [1••]. The contour is then closed at the base by connecting the opposite edges of the mitral annular ring by a straight line. The LV length is defined by the longest distance between the midpoint of the transannular line to the apex obtained from either the two- or four-chamber apical view (Fig. 1). In this method, caution should be taken to avoid foreshortening the LV, which can result in underestimation of the LV volumes and potential error in the estimated EF. Alternatively, the current ASE guidelines suggest the use of the area-length method when the endocardial borders in one of the apical views are not well defined rather than the use of a single plane-modified ellipsoid model for the LV EF calculation. Here, the area is obtained from the parasternal short axis at the mid-papillary level and the LV length is obtained from the apical four-chamber view similar to the modified Simpson’s method. This method, which presumes a bullet shape for the LV, is not accurate when there is asymmetry of the LV cavity [1••].
Modified Simpson’s rule (the biplane disk summation approach) for estimating LV volumes, ejection fraction, and mass. The four panels depict tracing of the interface between the compacted myocardium and the LV cavity and designation of the LV long axis at end-diastole (LV EDD) and end-systole (LV ESD) in the apical four- (A4C) and two-chamber (A2C) views (reproduced from [9] with permission from Elsevier)
The introduction of 3D Echo has allowed assessing LV volumes and EF independent of LV geometry and without any assumption about LV shape [10, 11••]. The advent of the 3D matrix array transducer has allowed real-time 3D imaging of the entire heart using an electrocardiogram (EKG)-gated full-volume, wide-angled acquisition in less than 10 s [11••]. Additionally, the semiautomated border detection, after identifying the LV apex and mitral annulus landmarks, has made 3D Echo a relatively fast and simple diagnostic tool [12].
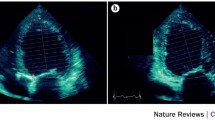
For 3D Echo-derived LV volume assessment, the acquisition should be made during a single breath-hold and from the least possible number of beats to reduce the risk of “stitch artifact.” The current ASE guidelines for image acquisition proposed the use of apical windows for real-time 3D full-volume acquisition of the LV. The acquisition can be guided by simultaneous multiplane mode which permits the display of two orthogonal planes or triplane with a 60° angle between each plane (Fig. 2) [11••]. Furthermore, global and regional LV function can be quantified using a surface rendering technique by either manual or semiautomatic LV cavity tracing (Fig. 3) [11••]. During tracing, the papillary muscles and trabecular myocardium should be included as part of the LV cavity [11••, 13].
Image acquisition using a 3D matrix array transducer from the apical window that produces simultaneous triplane (60° angle apart) images in the apical four-chamber (4C), two-chamber (2C), and three-chamber (3C) views. The simultaneous multiplane mode can guide the acquisition of 3D full-volume data (reproduced [11••] with permission from Elsevier)
Global and regional LV function can be quantified using a surface rendering technique by either manual or semiautomatic LV cavity tracing (reproduced from [11••] with permission from Elsevier)
The use of an ultrasound contrast agent (UCA) has the advantage of improving the delineation of the myocardial tissue-blood interface and thus provides more accurate LV volume and EF assessment [14]. The ASE recommends the use of UCA when two or more contiguous segments are not well visualized in any three of the apical views. It is also recommended, whenever available, to use a very low mechanical index (<0.2) with the vendor-specific tissue cancelation technique when performing ultrasound contrast imaging [15•].
Lastly, in an attempt to improve reproducibility and to reduce the time needed for obtaining EF, different automated methods of EF assessment have been suggested. Biplane speckle tracking-based auto-2D Echo EF assessment (AutoEF; GE Vingmed Ultrasound AS, Horten, Norway) has correlated well with CMR data (r = 0.7, slightly worse than r = 0.79 for the biplane Simpson’s 2D Echo method). AutoEF was also found to be twice as fast as the time needed to perform the biplane Simpson’s method and has significantly better reproducibility (interobserver correlation coefficient (r) = 0.8 versus 0.52 for Simpson’s method) [16]. Similarly, AutoEF (Version 0.9, Siemens) utilizing machine-learned pattern recognition, an algorithm that applies the artificial intelligence theory to mimic an expert manual tracing of the LV cavity, has been investigated for the EF assessment. The artificial intelligence-learned algorithm starts by searching the whole Digital Imaging and Communications in Medicine (DICOM) grayscale for a pattern consistent with LV cavity, and then the LV borders are tracked throughout the cardiac cycle to calculate LV volumes and EF (Fig. 4) [17]. This automated EF assessment showed good correlation with that obtained by the manual Simpson’s method (r = 0.98; 6% limits of agreement) and CMR (r = 0.95; 12% limits of agreement). Furthermore, AutoEF had lower intra- and interobserver variability in comparison to Simpson’s rule and visual EF assessments [17]. Lastly, recently published data from the FAST-EF Multicenter study has shown that automated LV volume and EF (assessed using AutoLV (TomTec-Arena 1.2) utilizing the artificial intelligence-learned pattern recognition) correlated well (intra-class correlation coefficient of 0.83) with manual Simpson’s rule EF calculations, without any interobserver or intra-observer variability and an average analysis time of only 8 s per patient [18•]. Similarly, for 3D Echo, a fully automated EF assessment has been investigated. Thavendiranathan et al. showed that the use of fully automated contouring of the LV endocardium (using a knowledge-based probabilistic contouring algorithm (eSie LVA, Siemens Ultrasound)) had an excellent correlation with that of CMR for the assessment of LV volume and EF [19•].
Automated left ventricular volume and ejection fraction assessment utilizing the artificial intelligence-learned algorithm (AutoEF; Version 0.9, Siemens). Two patient examples are depicted here: one with normal left ventricular function (a, top two panels) and another with heart failure (b, bottom two panels). The left side of each panel shows auto tracings of the LV in apical four- and two-chamber views, and the right side of each panel shows the corresponding volume curve and ejection fraction (EF) (reproduced from [17] with permission from Elsevier)
Cardiac Magnetic Resonance
CMR is considered to be the gold standard for LV volumetric and EF assessment [20]. The most commonly used quantification technique for LV volumetric assessment is EKG-gated, segmented balanced steady-state free precession (SSFP) imaging, which provides excellent blood-tissue differentiation without the need for intravenous contrast [20]. Most CMR scanners have multichannel coil elements that accelerate the SSFP sequences and enable acquisition of one or multiple short-axis images in a single breath-hold. LV volumes are assessed using Simpson’s rule using a stack of short-axis images acquired with a slice thickness of 6–8 mm; the entire ventricular volume is assessed in 10–15 slices (Fig. 5). A 20–50% gap between slices can be utilized to reduce the number of slices obtained. Tracings of the endocardium can be performed either manually or semiautomatically. It is essential to identify the LV base plane by cross-referencing the short-axis images with long-axis images to identify the exact location of the mitral annulus [20]. Alternatively, similar to echo, a biplane disk summation approach using the modified Simpson’s rule with four- and two-chamber views can be performed.
Cardiac magnetic resonance assessment of LV volumes utilizing EKG-gated, segmented balanced steady-state free precession (SSFP) imaging. LV and RV volumes in diastole and systole, ejection fraction, etc., are quantified using Simpson’s rule using a stack of short-axis images acquired with a slice thickness of 6–8 mm
Cardiac Computed Tomography
LV volumes and EF can be assessed using MDCT with retrospective EKG gating to enable imaging of the entire heart throughout the cardiac cycle [2]. MDCT data quality is dependent on both spatial and temporal resolution. Spatial resolution can be divided into axial (x- and y-planes) and longitudinal resolution (z-axis). In general, axial plane resolution is usually adequate but the challenge is to improve z-axis resolution (which is dependent on slice thickness, patient motion, and helical pitch). The temporal resolution on CT is dependent on gantry rotation time. An image can be reconstructed after acquiring 180° of data. Hence, temporal resolution on CT is defined as time taken for 360° gantry rotation [2]. Currently available MDCT and dual-source computed tomography (DSCT) scanners have offered high spatial and temporal resolution with faster gantry rotation along with submillimeter isotropic voxels, allowing for 3D reconstruction of images. Traditionally, LV volume quantification has been performed using Simpson’s method, which requires manual, semiautomated, or automated planimetry of the LV cavity in contiguous short-axis images along the length of the LV long axis. In this method, papillary muscles are generally included as part of the LV cavity [21]. It is important to determine accurately the most basal segment at the mitral annulus level and the LV apical segments. Since this method can be time-consuming, another technique has been utilized based on attenuation differences between contrast in the LV cavity and the myocardium, allowing for 3D “threshold-based segmentation” [21]. In this approach, the mitral annulus is determined manually and the contrast-filled cavity then automatically segmented by summing the adjacent voxels whose attenuation values exceed a predefined threshold (Fig. 6) [21]. This approach has better intra- and interobserver variability in comparison to the Simpson’s method. On the other hand, the threshold-based technique is sensitive to homogeneity of the contrast enhancement and the difference in attenuation between the myocardium and the LV cavity and, additionally, it may require special attention in patients with pacemakers or ventricular septal defects [22].
Multidetector computed tomographic threshold-based segmentation of the left ventricle. In this technique, the contrast-filled cavity is automatically segmented by summing the adjacent voxels whose attenuation values exceed a predefined threshold (reproduced with permission from [21])
Modality Agreement of LV Volume and EF Assessment
Each of the cardiovascular imaging modalities has its advantages and disadvantages (see Table 1). Because of excellent tissue characterization and endocardium definition, CMR is considered the gold standard for the assessment of LV function. CMR showed low interobserver variability for the assessment of EF (ranging from 5.1 to 6.3%) and low intra-observer variability (from 3.7 to 5.7%) [20]. Using 2D Echo, in spite of the available quantification methods, EF is routinely assessed subjectively by visual assessment. In a meta-analysis of 25 studies, McGowan et al. showed that visual assessment of EF had median Bland-Altman limits of agreement with reference methods (contrast ventriculography and radionuclide ventriculography) of ±19% (95% CI of ±16 to ±24%), while that for the 2D Echo Simpson’s method was ±18% (95% CI of ±7 to ±25%) [23]. More recently, using contemporary echo techniques, visual assessment was reported to have an interobserver variability, among 12 experienced readers, of only 5.1% [24].
In a direct comparison of traditional 2D and 3D Echo methods with CMR, 3D Echo showed better agreement with CMR and better interobserver and intra-observer variability. Dorosz et al., in their meta-analysis of 23 studies (1638 Echos) with CMR as the reference technique, showed that 2D Echo-pooled Bland-Altman biases for EDV, ESV, and EF were −48.2 ± 55.9, −27.7 ± 45.7, and 0.1 ± 13.9%, respectively [25•]. They also showed that the pooled Bland-Altman biases for 3D echo-derived EDV, ESV, and EF were −19.1 ± 34.2, −10.1 ± 29.7, and −0.6 ± 11.8%, respectively. The differences in biases between 2D and 3D Echo-derived values were significant for LV volumes, but not for EF. Additionally, interobserver and intra-observer variabilities, reported as mean percent difference ± 2 standard deviations, were 4.8 ± 21.1 and 0.2 ± 19.6, respectively, for 2D Echo while those for 3D Echo were 5.8 ± 12.54 and 3.9 ± 8.5, with the difference in width of the variances between 2D and 3D Echo being statistically significant [25•].
In a multicenter study, Hoffman et al. [26•] observed that the use of contrast-enhanced 2D or 3D Echo resulted in increased LV volumes in comparison to non-enhanced imaging and, consequently, a better correlation with CMR-derived LV volumes. Similarly, contrast-enhanced 2D or 3D Echo-derived LV EF demonstrated improved interobserver variabilities of 8.0 and 7.4%, respectively, which were significantly better than the 14.3% for both non-contrast-enhanced 2D and 3D Echo and similar to that for CMR of 7.9% [26•].
MDCT has shown good correlation with CMR for the assessment of LV volumes and EF. Sarwar et al. [27] have compared the LV global assessment of contrast-enhanced 64-slice MDCT, after reperfused ST-elevation myocardial infarction, with CMR. Using reconstructed short-axis images, MDCT scan-derived LV volumes and EF correlated well with CMR data (EDV, r = 0.91; ESV, r = 0.94; LVEF, r = 0.90). Using Bland-Altman analysis, the mean differences between MDCT and CMR-derived values for EDV, ESV, and EF were 3 mL, −0.2 mL, and 1%, respectively [27]. Similarly, the use of DSCT for the quantification of EDV, ESV, and EF (in comparison to CMR) has shown rank correlation rho values of 0.81 (P = 0.0024), 0.79 (P = 0.0031), and 0.64 (P = 0.0168), respectively [28]. Additionally, DSCT-derived EDV was overestimated by 3.7 mL, ESV was underestimated by 2.6 mL, and, consequently, EF was overestimated by 3.8% when compared to CMR [28]. The automated threshold-based 3D LV segmentation technique for DSCT has shown a significantly lower interobserver variability and mean analysis time (172 ± 20 versus 248 ± 29 s; P < 0.05) in comparison to 2D short-axis planimetry [29•].
Finally, Greupner et al. [30•] compared CMR (reference standard), MDCT, and 2D Echo (biplane Simpson’s rule) and 3D Echo for the assessment of LV global function among patients referred for coronary angiography. Bland-Altman analysis showed comparable limits of agreement for both MDCT and 2D Echo in the assessment of EF versus CMR while 3D Echo had higher variability. MDCT also showed significantly better agreement (compared to CMR) for stroke volume than did both 2D Echo and 3D Echo. In comparison with CMR, 2D Echo and 3D Echo significantly underestimated the EDV and ESV, while MDCT did not [30•].
General and Technical Limitations of LV Volume and EF Assessment
A major limitation of LV volume and EF estimation is the fact that they are dependent on preload and afterload conditions, influenced by heart rate, and insensitive to subtle changes in contractile reserve [6, 7, 20]. For Echo, the main limitation is the fact that it is operator- and acoustic window-dependent. In addition, 2D and linear Echo measurements are dependent on geometric assumptions that are inaccurate in the setting of LV asymmetry [1••]. Consequently, Echo has lower reproducibility and accuracy than do MDCT and CMR [2].
Although CMR is considered the reference technique for the assessment of LV volume and EF, the use of CMR is limited because of its high cost, limited availability, lack of portability, length of the procedure, patient claustrophobia, reduced accuracy in the setting of arrhythmias, and inability to image patients with implanted devices that are not MRI compatible—such as some pacemakers or implanted defibrillators [2, 20]. The main limitations of MDCT are the need for contrast administration and the high-radiation exposure associated with an ECG-gated CT study (more so with retrospectively gated exam), which makes it impractical, especially when serial assessments are needed [21].
Contractility Parameters
LV contractility is defined as the increase in LV power or work performed per unit increase in the LV preload [6]. While LV EF evaluation has been well validated as a measure of global LV assessment and it has been correlated with clinical outcomes, it is important to recognize that EF has several limitations as it is affected by afterload conditions and changes in heart rate. In an attempt to provide a less load-dependent parameter for LV global function, different indices have been suggested to estimate the invasive parameters of contractility, which are derived from ventricular pressure-volume data. The most commonly used parameters are slope, end-systolic elastance, and preload recruitable stroke work [7, 31].
LV Systolic Velocity Acceleration
The measurement of LV systolic velocity acceleration through the LV outflow tract (LVOT acc) has been shown to have a linear correlation with invasively measured LV end-systolic elastance (Ees) and was shown to be independent of the loading conditions [32]. Echocardiographically, LVOT acc is calculated by dividing the maximum systolic velocity in the LVOT recorded by pulsed-wave Doppler by the time from onset to peak LVOT flow velocity (Fig. 7) [6].
Left ventricular (LV) acceleration through the LV outflow (LVOT acc) can be calculated by dividing the maximum systolic velocity in the LVOT recorded by pulsed-wave Doppler by the time from onset to peak LVOT flow velocity (right). LVOT acc has a linear correlation with invasively measured LV end-systolic elastance (Ees) (left) (reproduced from [32] with permission from Elsevier)
Left Ventricular dP/dt
Another parameter of LV global systolic function is dP/dt which can be measured invasively using a high-fidelity micrometer catheter to determine the rate of increase in LV pressure during contraction. When it is measured during isovolumetric contraction, if the LA pressure is constant, it represents a relatively load-independent measure of contractility [31].
Non-invasively, dP/dt can be determined using the mitral regurgitation jet spectral display obtained by continuous-wave Doppler. It is measured by calculating the time interval (dt) between the velocities 1 and 3 m/s on the mitral regurgitation velocity profile (dP = 32 mmHg). This parameter can be influenced by dyssynchrony even if the myocardial contractility was constant [6, 31]. Similarly, the ejection intraventricular pressure difference between the LV apex and the LVOT, utilizing Euler’s momentum equation, and measured using color Doppler M-Mode obtained from the apical five-chamber view, has been reported to be a non-invasive load-independent measure of contractility that correlates closely with Ees [33].
Single-Beat Determination of Left Ventricular End-Systolic Elastance
LV Ees estimation can be calculated non-invasively using a modified single-beat method by measuring systolic (Ps) and diastolic (Pd) blood pressure, echo-derived stroke volume (SV) and LVEF, and an estimated normalized ventricular elastance at arterial end-diastole (ENd). The LV Ees (single beat) can be calculated using the following formula: [P d − (E Nd * P s * 0.9)] / (E Nd * SV) [34]. Similar parameters can be calculated utilizing CMR-derived volumes and LV pressures measured either invasively [35] or non-invasively using optical sensors [36].
Myocardial Performance Index
Myocardial performance index (MPI) or Tei index has been proposed as a measure of global LV function. This parameter reflects the combined systolic and diastolic function of the LV, and it has been shown to correlate with clinical outcome [37, 38]. MPI is calculated by dividing the LV isovolumetric times (isovolumetric relaxation plus isovolumetric contraction) by the LV ejection time (Fig. 8). These times can be obtained from either conventional Doppler or tissue Doppler imaging (TDI). Although MPI is independent of heart rate, it is influenced by preload and afterload conditions [31].
Schematic presentation of the Doppler-derived myocardial performance index (MPI). MPI is calculated by (a − b) / b, where a is the interval between the end and onset of mitral inflow, (a − b) is the left ventricular (LV) isovolumetric times (isovolumetric relaxation (IRT), isovolumetric contraction (ICT)), and b is the LV ejection time (ET) (reproduced from [38] with permission from Elsevier)
Global Strain
2D Global Longitudinal Strain
Strain is a marker of deformation and is defined as the change in the shape and dimensions of an object expressed as a percentage. The most common reference frame is the original length of the object (Lagrangian strain). Global longitudinal strain (GLS) is calculated by dividing the change in LV myocardial length between end-diastole and end-systole in relation to the original end-diastolic length. GLS is expressed as negative percentage [1••]. GLS has emerged as a promising and sensitive parameter for LV global function which has shown good correlations with clinical outcomes [39,40,41].
Echocardiographically, GLS can be measured by either TDI or speckle tracking; the latter is more widely used as it has the advantage of being angle-independent.
Using CMR, multiple techniques can be used for assessment of GLS including balanced steady-state free precession (SSFP), myocardial tagging, tissue phase mapping, displacement encoding with stimulated echoes, strain-encoded imaging, and feature-tracking imaging [20]. In a recent study, Onishi et al. showed that GLS measured by feature-tracking CMR and speckle-tracking echo was significantly correlated (r = −0.8, P < 0.0001) as were GLS (measured by either modality) and CMR-derived EF (r = −0.85, P < 0.001) [42•]. In the EACVI/ASE Inter-Vendor Comparison study, GLS measured by speckle-tracking Echo showed trivial, but statistically significant variability [3.7% (P < 0.001)] among nine vendors, but demonstrated excellent reproducibility in comparison to conventional Echo measurements [43•].
GLS has the limitations of intervendor and intersoftware variability and being load- and age-dependent. Therefore, it is recommended to perform serial GLS measurements using the same vendor and software. The current ASE/EACI Chamber Quantification document suggests that a peak GLS value of around −20% is to be expected in healthy individuals, regardless of the vendor used; lower absolute values of strain are more likely to be associated with abnormal global LV function [1••]. Because GLS is also dependent on the quality of the images, it has also been suggested to use DTI-derived mitral annular peak systolic velocity (s′) as an alternative to GLS to gain insight into the longitudinal function of the LV when two or more of the myocardial segments are suboptimal in one imaging plane.
3D Global Strain
The technical advances in the matrix array transducer allow the acquisition of 3D pyramidal datasets of the LV and subsequently has led to the development of off-line software capable of global speckle tracking homogenously in any of the standard three dimensions over time (longitudinal, radial, and circumferential) and, in addition, can perform global area strain [44, 45]. In one study of 38 newly diagnosed untreated hypertensive patients, global area strain, 3D global longitudinal strain, and global radial strain were significantly lower among hypertensive patients in comparison to healthy controls [44]. Moreover, in a meta-analysis of 375 patients with congestive heart failure, Ma et al. [46] showed that 3D-derived speckle tracking global longitudinal, circumferential, and radial strains was significantly reduced in comparison to the controls.
Conclusions
Global assessment of the LV function is an essential part of the evaluation of LV performance. Accurate determination of the LV volumes and EF plays a pivotal role not only in influencing the clinical decision in the patients’ management but also in providing an important prognostic value. In spite of the limitation related to being operator- and acoustic window-dependent, 2D Echo continues to be the most ubiquitous modality used for the assessment of the LV global function. The advances in technology have allowed more accurate evaluation of LV volumes and EF using 3D Echo, CMR, and MDCT. Non-invasively different parameters (most prominently are the 2D and 3D global strains) have emerged as potential better markers of global LV performance, in comparison to EF, as being less dependent on load conditions and more sensitive in identifying subclinical diseases. In Part 2 of this review, we will discuss and compare Echo, CMR, and MDCT for the assessment of diastolic and regional left ventricular function [47].
Abbreviations
- ASE:
-
American Society of Echocardiography
- CMR:
-
Cardiac magnetic resonance imaging
- DSCT:
-
Dual-source computed tomography
- EACVI:
-
European Association of Cardiovascular Imaging
- Echo:
-
Echocardiography
- EDV:
-
End-diastolic volume
- Ees:
-
End-systolic elastance
- EF:
-
Ejection fraction
- EKG:
-
Electrocardiogram
- ESV:
-
End-systolic volume
- GLS:
-
Global longitudinal strain
- LV:
-
Left ventricular
- LVEDP:
-
Left ventricular end-diastolic pressure
- MDCT:
-
Multidetector computed tomography
- MPI:
-
Myocardial performance index
- SSFP:
-
Balanced steady-state free precession
- TDI:
-
Tissue Doppler imaging
- UCA:
-
Ultrasound contrast agent
- 2D:
-
Two-dimensional
- 3D:
-
Three-dimensional
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
•• Lang RM, Badano LP, Mor-Avi V, et al. Recommendations for cardiac chamber quantification by echocardiography in adults: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. Journal of the American Society of Echocardiography: official publication of the American Society of Echocardiography. 2015;28:1–39.e14. This document provides comprehensive guidelines for the echocardiographic chamber quantification as recommended by the ASE/EACVI .
Sayyed SH, Cassidy MM, Hadi MA. Use of multidetector computed tomography for evaluation of global and regional left ventricular function. Journal of cardiovascular computed tomography. 2009;3:S23–34.
Herlitz J, Karlson BW, Sjoland H, et al. Long term prognosis after CABG in relation to preoperative left ventricular ejection fraction. Int J Cardiol. 2000;72:163–71. discussion 173–4
Russo AM, Stainback RF, Bailey SR, et al. ACCF/HRS/AHA/ASE/HFSA/SCAI/SCCT/SCMR 2013 appropriate use criteria for implantable cardioverter-defibrillators and cardiac resynchronization therapy: a report of the American College of Cardiology Foundation appropriate use criteria task force, Heart Rhythm Society, American Heart Association, American Society of Echocardiography, Heart Failure Society of America, Society for Cardiovascular Angiography and Interventions, Society of Cardiovascular Computed Tomography, and Society for Cardiovascular Magnetic Resonance. J Am Coll Cardiol. 2013;61:1318–68.
Yancy CW, Jessup M, Bozkurt B, et al. 2013 ACCF/AHA guideline for the management of heart failure: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol. 2013;62:e147–239.
Lang RM, Goldstein SA, Kronzon I, Khandheria BK, Mor-Avi V. ASE's comprehensive echocardiography. Second ed. Philadelphia, PA 19103–2899: Elsevier Saunders; 2016.
Thomas JD, Popovic ZB. Assessment of left ventricular function by cardiac ultrasound. J Am Coll Cardiol. 2006;48:2012–25.
Wong M, Johnson G, Shabetai R, et al. Echocardiographic variables as prognostic indicators and therapeutic monitors in chronic congestive heart failure. Veterans Affairs cooperative studies V-HeFT I and II. V-HeFT VA Cooperative Studies Group. Circulation. 1993;87:Vi65–70.
Lang RM, Bierig M, Devereux RB, et al. Recommendations for chamber quantification: a report from the American Society of Echocardiography’s Guidelines and Standards Committee and the Chamber Quantification Writing Group, developed in conjunction with the European Association of Echocardiography, a branch of the European Society of Cardiology. Journal of the American Society of Echocardiography: official publication of the American Society of Echocardiography. 2005;18:1440–63.
Lang RM, Mor-Avi V, Sugeng L, Nieman PS, Sahn DJ. Three-dimensional echocardiography: the benefits of the additional dimension. J Am Coll Cardiol. 2006;48:2053–69.
•• Lang RM, Badano LP, Tsang W, et al. EAE/ASE recommendations for image acquisition and display using three-dimensional echocardiography. Journal of the American Society of Echocardiography : official publication of the American Society of Echocardiography. 2012;25:3–46. This document provides a comprehensive approach for acquiring 3D Echo, clinical applications, and weaknesses and strength of 3D Echo.
Kleijn SA, Aly MF, Terwee CB, van Rossum AC, Kamp O. Three-dimensional speckle tracking echocardiography for automatic assessment of global and regional left ventricular function based on area strain. Journal of the American Society of Echocardiography: official publication of the American Society of Echocardiography. 2011;24:314–21.
Macron L, Lim P, Bensaid A, et al. Single-beat versus multibeat real-time 3D echocardiography for assessing left ventricular volumes and ejection fraction: a comparison study with cardiac magnetic resonance. Circulation Cardiovascular imaging. 2010;3:450–5.
Mulvagh SL, Rakowski H, Vannan MA, et al. American Society of Echocardiography consensus statement on the clinical applications of ultrasonic contrast agents in echocardiography. Journal of the American Society of Echocardiography : official publication of the American Society of Echocardiography. 2008;21:1179–201. quiz 1281
• Porter TR, Abdelmoneim S, Belcik JT, et al. Guidelines for the cardiac sonographer in the performance of contrast echocardiography: a focused update from the American Society of Echocardiography. Journal of the American Society of Echocardiography : official publication of the American Society of Echocardiography. 2014;27:797–810. This document provides an updated recommendation from the ASE for the optimization of images obtained with UCA and the safety and indications of the contrast media in echocardiography.
Szulik M, Pappas CJ, Jurcut R, et al. Clinical validation of a novel speckle-tracking-based ejection fraction assessment method. Journal of the American Society of Echocardiography : official publication of the American Society of Echocardiography. 2011;24:1092–100.
Cannesson M, Tanabe M, Suffoletto MS, et al. A novel two-dimensional echocardiographic image analysis system using artificial intelligence-learned pattern recognition for rapid automated ejection fraction. J Am Coll Cardiol. 2007;49:217–26.
• Knackstedt C, Bekkers SC, Schummers G, et al. Fully automated versus standard tracking of left ventricular ejection fraction and longitudinal strain: the FAST-EFs Multicenter Study. J Am Coll Cardiol. 2015;66:1456–66. This study showed that the utilization of fully automated software using machine learning-enabled image analysis was feasible and it can provide a rapid and reproducible assessment of the LVEF and longitudinal strain.
• Thavendiranathan P, Liu S, Verhaert D, et al. Feasibility, accuracy, and reproducibility of real-time full-volume 3D transthoracic echocardiography to measure LV volumes and systolic function: a fully automated endocardial contouring algorithm in sinus rhythm and atrial fibrillation. JACC Cardiovascular imaging. 2012;5:239–51. This study demonstrated the feasibility and accuracy of an automated (using trabecular edge contouring algorithm) 3D Echo assessment of the LV volumes and EF in both patients with atrial fibrillation and normal sinus rhythm.
Collins JD. Global and regional functional assessment of ischemic heart disease with cardiac MR imaging. Radiol Clin N Am. 2015;53:369–95.
van Ooijen PM, de Jonge GJ, Oudkerk M. Informatics in radiology: postprocessing pitfalls in using CT for automatic and semiautomatic determination of global left ventricular function. Radiographics : a review publication of the Radiological Society of North America, Inc. 2012;32:589–99.
Krishnam MS, Tomasian A, Iv M, et al. Left ventricular ejection fraction using 64-slice CT coronary angiography and new evaluation software: initial experience. Br J Radiol. 2008;81:450–5.
McGowan JH, Cleland JG. Reliability of reporting left ventricular systolic function by echocardiography: a systematic review of 3 methods. Am Heart J. 2003;146:388–97.
Blondheim DS, Beeri R, Feinberg MS, et al. Reliability of visual assessment of global and segmental left ventricular function: a multicenter study by the Israeli Echocardiography Research Group. Journal of the American Society of Echocardiography : official publication of the American Society of Echocardiography. 2010;23:258–64.
• Dorosz JL, Lezotte DC, Weitzenkamp DA, Allen LA, Salcedo EE. Performance of 3-dimensional echocardiography in measuring left ventricular volumes and ejection fraction: a systematic review and meta-analysis. J Am Coll Cardiol. 2012;59:1799–808. In a meta-analysis of 23 studies, this study showed that 3D Echo is more accurate and precise in the assessment of LV volumes and EF.
• Hoffmann R, Barletta G, von Bardeleben S, et al. Analysis of left ventricular volumes and function: a multicenter comparison of cardiac magnetic resonance imaging, cine ventriculography, and unenhanced and contrast-enhanced two-dimensional and three-dimensional echocardiography. Journal of the American Society of Echocardiography: official publication of the American Society of Echocardiography. 2014;27:292–301. This study provides evidence that the use of UCA in both 2D and 3D Echo improved the estimation of LV volumes (when compared to CMR-derived measurements) and reduced the interobserver variability.
Sarwar A, Shapiro MD, Nasir K, et al. Evaluating global and regional left ventricular function in patients with reperfused acute myocardial infarction by 64-slice multidetector CT: a comparison to magnetic resonance imaging. Journal of cardiovascular computed tomography. 2009;3:170–7.
Busch S, Johnson TR, Wintersperger BJ, et al. Quantitative assessment of left ventricular function with dual-source CT in comparison to cardiac magnetic resonance imaging: initial findings. Eur Radiol. 2008;18:570–5.
• Juergens KU, Seifarth H, Range F, et al. Automated threshold-based 3D segmentation versus short-axis planimetry for assessment of global left ventricular function with dual-source MDCT. AJR Am J Roentgenol. 2008;190:308–14. This study showed that the use of automated threshold-based 3D segmentation was a reproducible method for the assessment of LV volumes and function using DSCT.
• Greupner J, Zimmermann E, Grohmann A, et al. Head-to-head comparison of left ventricular function assessment with 64-row computed tomography, biplane left cineventriculography, and both 2- and 3-dimensional transthoracic echocardiography: comparison with magnetic resonance imaging as the reference standard. J Am Coll Cardiol. 2012;59:1897–907. This study directly compared 64-row MDCT, invasive cine-ventriculography, 2D Echo), and 3D Echo for the assessment of LV function with CMR. It provided evidence of MDCT. It provided data that showed MDCT can be more accurate than the other imaging modalities.
Armstrong WF, Ryan T. Feigenbaum’s echocardiography. Seventh ed. Philadelphia, PA 190106 USA: Lippincott Williams & Wilkins, a Wolters Kluwer business; 2010.
Bauer F, Jones M, Shiota T, et al. Left ventricular outflow tract mean systolic acceleration as a surrogate for the slope of the left ventricular end-systolic pressure-volume relationship. J Am Coll Cardiol. 2002;40:1320–7.
Yotti R, Bermejo J, Desco MM, et al. Doppler-derived ejection intraventricular pressure gradients provide a reliable assessment of left ventricular systolic chamber function. Circulation. 2005;112:1771–9.
Chen CH, Fetics B, Nevo E, et al. Noninvasive single-beat determination of left ventricular end-systolic elastance in humans. J Am Coll Cardiol. 2001;38:2028–34.
Schmitt B, Steendijk P, Lunze K, et al. Integrated assessment of diastolic and systolic ventricular function using diagnostic cardiac magnetic resonance catheterization: validation in pigs and application in a clinical pilot study. JACC Cardiovascular imaging. 2009;2:1271–81.
Abi-Abdallah Rodriguez D, Durand E, de Rochefort L, Boudjemline Y, Mousseaux E. Simultaneous pressure-volume measurements using optical sensors and MRI for left ventricle function assessment during animal experiment. Med Eng Phys. 2015;37:100–8.
Tei C, Ling LH, Hodge DO, et al. New index of combined systolic and diastolic myocardial performance: a simple and reproducible measure of cardiac function—a study in normals and dilated cardiomyopathy. J Cardiol. 1995;26:357–66.
Tei C, Dujardin KS, Hodge DO, Kyle RA, Tajik AJ, Seward JB. Doppler index combining systolic and diastolic myocardial performance: clinical value in cardiac amyloidosis. J Am Coll Cardiol. 1996;28:658–64.
Kalam K, Otahal P, Marwick TH. Prognostic implications of global LV dysfunction: a systematic review and meta-analysis of global longitudinal strain and ejection fraction. Heart. 2014;100:1673–80.
Cimino S, Canali E, Petronilli V, et al. Global and regional longitudinal strain assessed by two-dimensional speckle tracking echocardiography identifies early myocardial dysfunction and transmural extent of myocardial scar in patients with acute ST elevation myocardial infarction and relatively preserved LV function. European heart journal cardiovascular Imaging. 2013;14:805–11.
Kraigher-Krainer E, Shah AM, Gupta DK, et al. Impaired systolic function by strain imaging in heart failure with preserved ejection fraction. J Am Coll Cardiol. 2014;63:447–56.
• Onishi T, Saha SK, Delgado-Montero A, et al. Global longitudinal strain and global circumferential strain by speckle-tracking echocardiography and feature-tracking cardiac magnetic resonance imaging: comparison with left ventricular ejection fraction. Journal of the American Society of Echocardiography : official publication of the American Society of Echocardiography. 2015;28:587–96. This study provides evidence that the use of feature-tracking CMR analysis for the assessment of GLS was feasible and it was comparable to the GLS obtained by speckle-tracking Echo.
• Farsalinos KE, Daraban AM, Unlu S, Thomas JD, Badano LP, Voigt JU. Head-to-head comparison of global longitudinal strain measurements among nine different vendors: the EACVI/ASE Inter-Vendor Comparison Study. Journal of the American Society of Echocardiography : official publication of the American Society of Echocardiography. 2015;28:1171–1181, e2. This study compared the GLS measurement using nine different vendors. It provided evidence that GLS has good reproducibility. It also showed that the differences between intervendor GLS is small but it was statistically significant.
Galderisi M, Esposito R, Schiano-Lomoriello V, et al. Correlates of global area strain in native hypertensive patients: a three-dimensional speckle-tracking echocardiography study. European heart journal cardiovascular Imaging. 2012;13:730–8.
Luis SA, Yamada A, Khandheria BK, et al. Use of three-dimensional speckle-tracking echocardiography for quantitative assessment of global left ventricular function: a comparative study to three-dimensional echocardiography. Journal of the American Society of Echocardiography: official publication of the American Society of Echocardiography. 2014;27:285–91.
Ma C, Chen J, Yang J, et al. Quantitative assessment of left ventricular function by 3-dimensional speckle-tracking echocardiography in patients with chronic heart failure: a meta-analysis. Journal of ultrasound in medicine : official journal of the American Institute of Ultrasound in Medicine. 2014;33:287–95.
Kinno M, Nagpal P, Horgan S, Waller AH. Comparison of Echocardiography, Cardiac Magnetic Resonance, and Computed Tomographic Imaging for the Evaluation of Left Ventricular Myocardial Function: Part 2 (Diastolic and Regional Assessment). Curr Cardiol Rep. 2017;19:6.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Menhel Kinno, Prashant Nagpal, Stephen Horgan, and Alfonso H. Waller declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Echocardiography
Rights and permissions
About this article
Cite this article
Kinno, M., Nagpal, P., Horgan, S. et al. Comparison of Echocardiography, Cardiac Magnetic Resonance, and Computed Tomographic Imaging for the Evaluation of Left Ventricular Myocardial Function: Part 1 (Global Assessment). Curr Cardiol Rep 19, 9 (2017). https://doi.org/10.1007/s11886-017-0815-4
Published:
DOI: https://doi.org/10.1007/s11886-017-0815-4