Abstract
Improvements in the outcomes of surgical and catheter-based interventions and medical therapy have led to a growing population of adult patients with congenital heart disease. Adult patients with previously undiagnosed congenital heart disease or those previously palliated or repaired may have challenging echocardiographic examinations. Understanding the distinct anatomic and hemodynamic features of the congenital anomaly and quantifying ventricular function and valvular dysfunction plays an important role in the management of these patients. Rapid advances in imaging technology with magnetic resonance imaging (MRI) and computed tomography angiography (CTA) allow for improved visualization of complex cardiac anatomy in the evaluation of this unique patient population. Although echocardiography remains the most widely used imaging tool to evaluate congenital heart disease, alternative and, at times, complimentary imaging modalities should be considered. When caring for adults with congenital heart disease, it is important to choose the proper imaging study that can answer the clinical question with the highest quality images, lowest risk to the patient, and in a cost-efficient manner.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Imaging plays a very important role in the diagnosis and management of the adult patient with congenital heart disease. Echocardiography has traditionally been the workhorse of cardiac imaging in these patients and continues to be the modality used most frequently. The ability to answer all clinical questions with echocardiography can be challenging in the adult patient due to poor acoustic windows related to patient size, prior operations, or lung disease. These patients will often require additional imaging to answer the clinical question. Rapid advances in the fields of cardiac magnetic resonance imaging (MRI) and computed tomography angiography (CTA) have made these modalities a clinically useful adjunct, and sometimes alternative, to echocardiography. These modalities are used in the evaluation of patients with congenital heart disease with increasing frequency [1–3]. As these modalities become more widely available, understanding when to choose a particular modality can sometimes be confusing for the providers and patients. This article seeks to describe the basics regarding the use of MRI and CTA in the adult with congenital heart disease, including advantages of each modality, contraindications, and technical considerations.
Basic Concepts
Magnetic Resonance Imaging
MRI uses the signal from hydrogen ions (protons) in various tissues to generate an image [4]. When a patient is placed in the MRI scanner, all hydrogen ions in the body align with and precess (spin) along the axis of that strong magnetic field. Radiofrequency pulses are applied to move the protons out of phase and the rate of relaxation back to baseline is measured. These differences are processed to form images. Different tissues have variable rates of relaxation and these differences allow MRI to provide tissue characterization and detect the presence of edema, fluid, fibrosis, or fat. By taking advantage of differences in tissues, MRI imaging can obtain high-resolution images for evaluation of cardiac morphology and function without the use of contrast.
There are many advantages to cardiac MRI. There is no need for ionizing radiation and high-resolution cine images can be obtained for accurate quantitation of ventricular volumes and ejection fraction without the use of a contrast agent [5, 6]. Images can be obtained in any selected plane without limitations from acoustic windows or overlapping structures. Phase contrast imaging can quantify flow, which is used to quantitate valvular regurgitation, shunt fraction, and differential pulmonary perfusion [7]. The use of gadolinium-based contrast agents allows for assessment of myocardial perfusion and delayed-enhancement sequences allow for assessment of viability and fibrosis [8, 9]. Gadolinium can also be used to perform magnetic resonance angiography (MRA), which allows for visualization of vascular structures such as the aorta, pulmonary arteries, and systemic and pulmonary veins [10–13]. Myocardial tagging can be used for strain analysis [14]. New technology with the use of 4D flow mapping holds promise for evaluation of many congenital lesions [15]. A detailed description of the various sequences used in cardiac MRI is beyond the scope of this article.
Limitations to the use of MRI may be due to the lack of availability or contraindications to MRI. It is critically important that individuals with both knowledge in image acquisition and interpretation and an understanding of congenital heart disease perform cardiac MRI [1–3]. Unlike CTA, where images are obtained in an axial stack and then reconstructed in various planes, MRI is very operator dependent and requires an understanding of the anatomy and physiology to appropriately setup and obtain the proper imaging planes. Patient-specific limitations include the presence of implanted devices such as pacemakers or defibrillators or metallic coils, clips, or wires. The majority of implanted cardiac devices such as stents, valves, coils, and surgical clips are safe for use in MRI but may cause significant artifact that precludes assessment of some cardiac structures. Specific MRI sequences can be employed to try to reduce this artifact [16]. MRI-conditional pacemakers are commercially available but are approved only for use with 1.5 Tesla magnets and have not been approved for use in cardiac MRI. MRI can safely be performed in patients with conventional pacemakers and defibrillators, as long as they are not pacemaker-dependent, exhibit normal device function, and have been in place for more than 90 days [17]. The presence of leads in the heart can cause artifact and may limit the evaluation. The use of gadolinium contrast should be avoided in the setting of renal dysfunction with a creatinine clearance <30 mL/min/1.73 m2 or with acute kidney injury to avoid the risk of development of nephrogenic systemic fibrosis, a systemic disorder resembling scleroderma in which fibrosis occurs in the skin and connective tissues thought to be due to the inability to clear gadolinium chelates [18]. Cardiac MRI requires ECG gating and irregular rhythms such as atrial fibrillation can make image acquisition challenging. The patient must also be able to lie flat, still, and perform breath holds in order to reduce motion artifact. MRI examinations are time-consuming, and sequences should be tailored to obtain the necessary imaging to answer the clinical question.
Computed Tomography Angiography
To perform imaging with CTA, iodinated contrast agents are injected and the scan is timed to opacify the structure(s) of interest. Rapidly rotating x-ray beams and detectors are used to create images and ECG gating is used to reduce motion artifact and allow for cine reconstructions in various phases to measure ventricular volumes and ejection fraction [19, 20]. Postprocessing is used to perform multiplanar reformats to view structures in any plane, perform measurements of vascular structures, and understand spatial relationships and connections.
CTA has excellent spatial resolution and is very good for evaluation of small vascular structures, such as coronary arteries. Advances in technology with the use of dual-source scanners and multidetector rows have allowed for shorter scan times, better temporal resolution, and lower radiation doses [21, 22, 23•]. CTA is a very useful alternative for patients with implanted devices that are contraindicated or would result in significant artifact with MRI. CTA has a very short scan time with all images being acquired in a single breath hold.
The major disadvantage to CTA is the use of ionizing radiation. Although technologic advances have decreased the radiation exposure, for young patients that will require serial imaging, the cumulative radiation dose still remains a concern. CTA always requires the use of iodinated contrast, which can be an issue for patients with chronic renal disease or contrast allergies. As with MRI, technical expertise is incredibly important, as the timing of the scan must be optimized for maximum contrast enhancement of the structure of interest. Knowledge of congenital heart disease is essential; as timing of the scan will be vastly different for a patient with a Fontan circulation than it would be for a patient with a normal four-chamber heart; and the location of the intravenous injection will impact the ability to visualize the intended structures. Failure to properly address these issues may lead to unnecessary risk to the patient from radiation and contrast exposure with a low likelihood of answering the clinical question. CTA also requires ECG gating and, as with MRI, irregular rhythms can make for challenging images.
Choosing an Imaging Modality
Basic Principles
In many adult patients with congenital heart disease, it is often challenging to answer all relevant clinical questions with a single imaging study. It is critical for the provider to understand the strengths and weaknesses of each modality and to outline all clinical questions that need to be addressed. The goal should be to choose a modality that will answer the clinical question(s) in the most cost-effective manner and with the least amount of risk and discomfort to the patient. If there are multiple clinical queries to answer, which is often the case, the modality best proven to answer them all should be chosen, keeping in mind that this may not be possible or may not be the least expensive modality. In selecting the most appropriate imaging technique, it is equally important to have the right expertise in performing and interpreting those studies. Therefore, all patients with complex congenital heart disease should have imaging performed in regional adult congenital heart disease centers by providers with expertise in both advanced cardiac imaging and congenital heart disease [3]. For many clinical questions, either MRI or CTA can provide similar information. The choice of one over the other often is determined by individual patient characteristics (kidney function, implanted devices), patient preference (claustrophobia with MRI), need for serial imaging and a desire to avoid radiation exposure (right ventricular volumes or aortic dimensions), or plans for upcoming surgery (may choose CTA to be able to exclude coronary artery disease without the need for invasive coronary angiography).
Shunt Lesions
Atrial septal defects (ASDs), ventricular septal defects (VSDs), and atrioventricular septal defects (AVSDs) are typically evaluated with echocardiography, and additional imaging is usually not needed. However, in a patient with a known cardiac shunt, flow measurements obtained with MRI can quantitate the severity of the shunt when the latter is in doubt [24, 25]. MRI or CTA should be performed in the patient with unexplained dilation of right ventricle or concern for anomalous pulmonary venous connections when an obvious shunt is not detected by echocardiography. Similarly, MRI or CTA needs to be considered if device closure of a secundum atrial septal defect is planned and normal pulmonary venous connections could not be established with echocardiography. MRI or CTA can be used to quantitate right ventricular volumes in a patient with a suspected shunt and can clearly delineate a sinus venosus defect (Fig. 1) or anomalous pulmonary venous connections [26].
Pulmonary Venous Anomalies
Anomalous pulmonary venous connection can be a single defect or more commonly associated with an atrial septal defect. Either MRI or CTA can be used to evaluate normal and anomalous pulmonary venous connections (Fig. 2) [27–30]. The ability to visualize the location and number of anomalous connections is vital in planning a surgical approach. In the adult patient requiring surgical intervention, such as in sinus venosus ASD with partial anomalous pulmonary venous return, CTA may be a better imaging choice, because it allows for excellent visualization of the location of the anomalous veins (often the right upper lobe vein) and also allows the ability to look for coronary artery disease, thus obviating the need for invasive coronary angiography. The entry point of the anomalous vein in relation to the superior vena cava-right atrium junction is an important determinant of the surgical approach needed to baffle the anomalous vein(s) into the left atrium. In the patient with previous repair of anomalous pulmonary veins, MRI or CTA provide excellent delineation of the postoperative anatomy and should be performed when there are concerns about baffle stenosis or leaks.
Aortopathies and Disorders of the Aorta
MRI and CTA are ideal imaging techniques in evaluation of patients with aortic disease, whether it is an aortopathy due to abnormalities of connective tissue such as Marfan syndrome, or a structural abnormality of the aorta, such as coarctation of the aorta or a vascular ring [31, 32]. Both modalities provide a three-dimensional evaluation of the aorta and branch vessels and allow for accurate measurement of dimensions. For the patient with an aortopathy requiring serial surveillance studies, MRI is preferable because it does not expose the patient to radiation. However, in a patient with a newly diagnosed large aortic aneurysm by echo, CTA may be the best choice to evaluate the size, location, and extent of the aneurysm because it also allows for a non-invasive evaluation of the coronary arteries prior to surgery. For newly diagnosed thoracic aortic aneurysm, imaging of the abdomen and pelvis is recommended to look for other aneurysmal diseases that can at times assist in identifying the underlying genetic mutation. Similarly, for the patient who has undergone surgical repair of thoracic ascending aortic aneurysm, follow-up imaging of the aorta is needed to assess result of the repair and to look for potential complication such as pseudoaneurysm, or to assess the size of the rest of the aorta that could later be involved in the disease, such as the descending aorta.
The adult patient with a new diagnosis of coarctation of the aorta requires cross-sectional imaging of the aorta to evaluate the location and severity of the coarctation, as well as the presence of any associated aortic dilatation, hypoplastic arch, or collateral formation. CTA is ideal in this situation as it provides additional information needed to determine the best treatment approach and, if surgery is indicated, allows for assessment of the coronary arteries. MRI would provide all of the same information but without assessment for obstructive coronary artery disease (Fig. 3). MRI-based computational fluid dynamics may offer additional hemodynamic information which could obviate the need for cardiac catheterization in some patients when the coarctation severity is in question, although additional study is necessary[33]. In a patient with prior surgical coarctation repair, serial imaging of the coarctation site, to assess for restenosis, aneurysm, or pseudoaneurysm, is often performed with MRI to reduce the cumulative radiation exposure. In patients with prior stenting of coarctation, significant artifacts may be present with MRI and CTA may be a better way to evaluate the stented segment [34].
Tetralogy of Fallot
Almost all adult patients with Tetralogy of Fallot (TOF) will have undergone repair in childhood and many will have important hemodynamic sequelae, and less so residua, as a result of that repair. Until recently, relief of right ventricular outflow tract obstruction, commonly accompanied by transannular patch, has resulted in significant, often free, pulmonary regurgitation in the majority of patients. Chronic pulmonary valve regurgitation leads to right ventricular volume overload and subsequently right ventricular dysfunction, tricuspid annular dilatation, tricuspid regurgitation, and ventricular arrhythmias. Cardiac MRI has become a powerful tool in the assessment of right ventricular volume and function to help determine optimal timing of pulmonary valve replacement (PVR). Cardiac MRI is also important in determining candidacy for percutaneous PVR. Multiple studies have determined that PVR should be performed before the right ventricular end diastolic volume index exceeds 150–170 ml/m2 in order to achieve normalization of right ventricular volumes after surgery [35–41]. Quantification of right ventricular volume and ejection fraction is highly reproducible, especially if performed on axial datasets [42]. Left ventricular systolic dysfunction occurs in up to 20 % of patients with repaired TOF and is associated with poorer prognosis and increased risk of sudden death [43, 44]. Ventricular-ventricular interaction related to right ventricular dysfunction is one proposed mechanism for the development of left ventricular dysfunction [45]. Left ventricular function can be accurately evaluated with MRI. MRI can also be used to assess for fibrosis, which has been associated with other adverse clinical markers and arrhythmias in patients with repaired TOF [46].
MRI can also quantitate pulmonary valve regurgitation with phase contrast imaging and the same sequences can be used to quantitate flow in each of the branch pulmonary arteries [47–50]. MRA of the pulmonary arteries can be used to evaluate pulmonary arterial stenosis, often occurring at the site of prior palliative shunts, or pulmonary artery aneurysms. Aortic root dilatation occurs in conotruncal defects and can lead to aortic valve regurgitation. The aortic dimensions can be measured with MRA and aortic regurgitation can be quantitated [51].
Transposition of the Great Arteries
Adult patients with d-TGA will have undergone palliative interventions in childhood, including the atrial switch (Mustard or Senning), Rastelli, or arterial switch operation. Each of these repairs is associated with both anatomic and hemodynamic sequelae [52].
Patients with prior atrial switch procedure often develop systemic right ventricular dysfunction and secondary tricuspid regurgitation and heart failure. MRI has been used to accurately quantitate the volumes and function of the systemic right ventricle, and the presence of fibrosis as detected by late gadolinium enhancement has been associated with poor outcomes [53–55]. In addition, systemic or pulmonary venous baffle obstruction can be challenging and often suboptimally evaluated with echo [56]. Both MRI and CTA provide great spatial resolution, enabling accurate assessment of the baffles to look for stenosis (Fig. 4). The high prevalence of sinus node dysfunction requiring pacemakers may make MRI less useful in this situation, as the presence of leads in the superior vena cava baffle may result in artifact.
a Steady-state free precession imaging in a patient with transposition of the great arteries status post atrial switch with a Mustard procedure demonstrates obstruction of the inferior vena cava baffle (arrow). b Oblique coronal reformat from CTA in the same patient after stent was placed in IVC baffle (arrow). SVC = superior vena cava, IVC = inferior vena cava, LV = subpulmonary morphologic left ventricle, PA = pulmonary artery, Ao = aorta
In patients with prior Rastelli repair, progressive right ventricular to pulmonary artery (RV–PA) conduit dysfunction is expected 10 to 15 years after repair [57]. The Rastelli procedure is an operation to treat d-transposition of the great arteries with pulmonary or subpulmonary stenosis and VSD. This operation involves direction of the outflow from the left ventricle to the aorta using a patch, which also closes the VSD, and surgical closure of the pulmonary valve with creation of a conduit to direct blood from the right ventricle to the pulmonary arteries. Although echocardiography will provide very useful information such as right ventricular function and pressure, the conduit itself can be challenging to evaluate due to its retrosternal location. MRI and CTA both provide excellent visualization of the conduit and can localize obstruction, while MRI can be used to quantitate regurgitation.
The arterial switch operation is associated with neoaortic root dilatation and neoaortic valve regurgitation, branch pulmonary artery stenosis, and coronary artery obstruction [58]. CTA is superior for evaluation of the coronary artery anatomy, while MRI provides the ability to quantitate valvular regurgitation. Both allow for assessment of anatomic abnormalities such as root dilatation or branch pulmonary stenosis (Fig. 5).
Volume-rendered image from CTA in a patient with transposition of the great arteries status post arterial switch with LeCompte maneuver (bringing the main and branch pulmonary arteries anterior to the ascending aorta) demonstrates the typical anatomy with the main pulmonary artery pulled anterior to the aorta and the branch pulmonary arteries draped over the ascending aorta. The coronary arteries were also noted to be widely patent on this study (not completely visualized on this image). MPA = main pulmonary artery, Ao = aorta, LAD = left anterior descending coronary artery, RCA = right coronary artery
Ebstein Anomaly
Right ventricular dysplasia is a very common finding in Ebstein anomaly. In addition, chronic severe tricuspid regurgitation leads to further right ventricular volume overload and dysfunction and is a major determinant of outcome. Although echo has been the modality of choice in the evaluation of patients with Ebstein anomaly, at times, assessment of RV size and function is suboptimal. MRI has increasingly been used to complement echo, allowing quantitation of RV volumes and function prior to consideration for surgical intervention, especially when there are concerns about the severity of the dysfunction and its associated increased postoperative mortality [59–61]. Left ventricular dysfunction is also a risk factor for poor outcomes after surgical repair, and ventricular function can be quantitated with MRI. In patients with severe RV dysfunction, a 1.5 ventricle repair can be used to offload the RV. This operation includes repair of the tricuspid valve and a bidirectional cavopulmonary anastomosis, which directs blood from the SVC directly to the pulmonary arteries, hence reducing the preload to the dysfunctional RV. MRI can be used to assess patency of the bidirectional cavopulmonary anastomosis following this repair (Fig. 6) [62].
Single Ventricle Physiology
Evaluation of the adult patients with single ventricle physiology following Fontan palliation can be extremely challenging and almost always requires repeated cardiac imaging to assess for its known sequelae, such as Fontan obstruction, ventricular dysfunction, atrioventricular valve regurgitation, venovenous collaterals, and intracardiac or intrapulmonary thrombus formation. Accurate quantitation of single ventricular function with echocardiography can be suboptimal, and adequate visualization of the whole Fontan pathway can be very difficult in the adult. Complications such as focal narrowing of the pathway, thrombus formation, or branch pulmonary artery stenosis can be easily evaluated with MRI or CTA [63–65]. Assessment of flow dynamics can be performed with MRI and research in this area is ongoing to better understand how the physiology differs in the different types of Fontan connections [66–68]. Liver dysfunction is now recognized as a major contributor to morbidity and mortality in patients after Fontan palliation, including the development of cirrhosis and hepatocellular carcinoma [69•, 70, 71]. Routine imaging of the liver should be performed in these patients to detect the presence of cirrhosis or masses. Our institution has adopted a practice of performing combined imaging of the heart and liver with MRI, utilizing a limited evaluation of the liver for masses and evaluation of liver stiffness with magnetic resonance elastography (MRE). MRE is a non-invasive way to evaluate liver stiffness and may obviate the need for liver biopsy [72]. MRE evaluation of patients with prior Fontan palliation has been shown to be feasible and increased levels of stiffness correlate with fibrosis as detected by biopsy [73–75].
Evaluation of Fontan pathways with MRI or CTA requires an understanding of the often complex anatomy and physiology in order to adequately visualize the pathways. Injecting contrast into an upper extremity intravenous site will only opacify venous return from the upper extremities and the mixing of non-contrast opacified blood from the inferior vena cava (IVC) can create artificial filling defects in the pulmonary arteries, often misinterpreted as thrombi. In order to adequately visualize the pathways, simultaneous injection of contrast in both the upper and lower extremities must be performed and timing this can be challenging.
Coronary Artery Anomalies
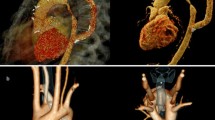
Both CTA and MRI can be used to evaluate the anomalous coronary artery [76]. CTA has superior spatial resolution and recent advances in technology have led to improved temporal resolution. In a patient with anomalous aortic origin of the coronary artery from the opposite sinus of Valsalva, CTA allows for identification of the origin and course of the coronary artery, as well as the presence of high-risk features such as an acute angle of takeoff, slit-like orifice, and proximal intramural course (Fig. 7) [77–79]. It is important to remember that CTA allows for excellent delineation of the anatomy but does not provide additional information about the physiology [80]. CTA also allows for evaluation of the entire extent of the coronary arteries, to exclude atherosclerotic plaque [81]. Other congenital coronary artery anomalies can be adequately evaluated by CTA such as coronary fistulae and myocardial bridging. The origin, course, and termination of coronary fistulae are important in planning an approach to treatment, and CTA allows for excellent evaluation of the anatomy, making it the procedure of choice [82, 83]. MRI can also be used to evaluate the location of the origins of the coronary arteries, but imaging is challenging due to small vessel size and both cardiac and respiratory motion, requiring special expertise to obtain high quality images [84].
Conclusions
Imaging plays a central role in the management of the adult patient with congenital heart disease. Understanding the strengths, weaknesses, and risks of each imaging modality is important in order to choose the study that will answer the clinical question with the lowest risk to the patient and in a cost-effective manner, especially given that repeated imaging is often required over the lifespan of the patient. As technology continues to improve, this field will continue to evolve and offer improved visualization of the anatomy and physiology in patients with congenital heart disease.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Baumgartner H, Bonhoeffer P, De Groot NM, et al. ESC Guidelines for the management of grown-up congenital heart disease (new version 2010). Eur Heart J. 2010;31(23):2915–57.
Kilner PJ, Geva T, Kaemmerer H, Trindade PT, Schwitter J, Webb GD. Recommendations for cardiovascular magnetic resonance in adults with congenital heart disease from the respective working groups of the European Society of Cardiology. Eur Heart J. 2010;31(7):794–805.
Warnes CA, Williams RG, Bashore TM, et al. ACC/AHA 2008 guidelines for the management of adults with congenital heart disease: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to Develop Guidelines on the Management of Adults With Congenital Heart Disease). Developed in collaboration with the American Society of Echocardiography, Heart Rhythm Society, International Society for Adult Congenital Heart Disease, Society for Cardiovascular Angiography and Interventions, and Society of Thoracic Surgeons. J Am Coll Cardiol. 2008;52(23):e143–263.
Bitar R, Leung G, Perng R, et al. MR pulse sequences: what every radiologist wants to know but is afraid to ask. Radiographics. 2006;26(2):513–37.
Maceira AM, Prasad SK, Khan M, Pennell DJ. Reference right ventricular systolic and diastolic function normalized to age, gender and body surface area from steady-state free precession cardiovascular magnetic resonance. Eur Heart J. 2006;27(23):2879–88.
Maceira AM, Prasad SK, Khan M, Pennell DJ. Normalized left ventricular systolic and diastolic function by steady state free precession cardiovascular magnetic resonance. J Cardiovasc Magn Reson. 2006;8(3):417–26.
Srichai MB, Lim RP, Wong S, Lee VS. Cardiovascular applications of phase-contrast MRI. AJR Am J Roentgenol. 2009;192(3):662–75.
Saraste A, Nekolla S, Schwaiger M. Contrast-enhanced magnetic resonance imaging in the assessment of myocardial infarction and viability. J Nucl Cardiol. 2008;15(1):105–17.
Broberg CS, Chugh SS, Conklin C, Sahn DJ, Jerosch-Herold M. Quantification of diffuse myocardial fibrosis and its association with myocardial dysfunction in congenital heart disease. Circ Cardiovasc Imaging. 2010;3(6):727–34.
Febbo JA, Galizia MS, Murphy IG, et al. Congenital heart disease in adults: quantitative and qualitative evaluation of IR FLASH and IR SSFP MRA techniques using a blood pool contrast agent in the steady state and comparison to first pass MRA. Eur J Radiol. 2015;84(10):1921–9.
Fenchel M, Saleh R, Dinh H, et al. Juvenile and adult congenital heart disease: time-resolved 3D contrast-enhanced MR angiography. Radiology. 2007;244(2):399–410.
Naehle CP, Kaestner M, Muller A, et al. First-pass and steady-state MR angiography of thoracic vasculature in children and adolescents. J Am Coll Cardiol Img. 2010;3(5):504–13.
Potthast S, Mitsumori L, Stanescu LA, et al. Measuring aortic diameter with different MR techniques: comparison of three-dimensional (3D) navigated steady-state free-precession (SSFP), 3D contrast-enhanced magnetic resonance angiography (CE-MRA), 2D T2 black blood, and 2D cine SSFP. J Magn Reson Imaging. 2010;31(1):177–84.
Jeung MY, Germain P, Croisille P. El ghannudi S, Roy C, Gangi A. Myocardial tagging with MR imaging: overview of normal and pathologic findings. Radiographics. 2012;32(5):1381–98.
Vasanawala SS, Hanneman K, Alley MT, Hsiao A. Congenital heart disease assessment with 4D flow MRI. J Magn Reson Imaging. 2015;42(4):870–86.
Saremi F, Grizzard JD, Kim RJ. Optimizing cardiac MR imaging: practical remedies for artifacts. Radiographics. 2008;28(4):1161–87.
Boilson BA, Wokhlu A, Acker NG, et al. Safety of magnetic resonance imaging in patients with permanent pacemakers: a collaborative clinical approach. J Interv Card Electrophysiol. 2012;33(1):59–67.
Agarwal R, Brunelli SM, Williams K, Mitchell MD, Feldman HI, Umscheid CA. Gadolinium-based contrast agents and nephrogenic systemic fibrosis: a systematic review and meta-analysis. Nephrol Dial Transplant. 2009;24(3):856–63.
Bardo DM, Brown P. Cardiac multidetector computed tomography: basic physics of image acquisition and clinical applications. Curr Cardiol Rev. 2008;4(3):231–43.
Bardo DM, Kachenoura N, Newby B, Lang RM, Mor-Avi V. Multidetector computed tomography evaluation of left ventricular volumes: sources of error and guidelines for their minimization. J Cardiovasc Comput Tomogr. 2008;2(4):222–30.
Otero HJ, Steigner ML, Rybicki FJ. The "post-64" era of coronary CT angiography: understanding new technology from physical principles. Radiol Clin N Am. 2009;47(1):79–90.
Cook SC, Raman SV. Multidetector computed tomography in the adolescent and young adult with congenital heart disease. J Cardiovasc Comput Tomogr. 2008;2(1):36–49.
Ghoshhajra BB, Sidhu MS, El-Sherief A, et al. Adult congenital heart disease imaging with second-generation dual-source computed tomography: initial experiences and findings. Congenit Heart Dis. 2012;7(6):516–25. This paper highlights the utility of dual-source CTA in patients with congenital heart disease. This modality allows for superior spatial resolution with lower radiation doses and shorter scan times than MRI.
Powell AJ, Maier SE, Chung T, Geva T. Phase-velocity cine magnetic resonance imaging measurement of pulsatile blood flow in children and young adults: in vitro and in vivo validation. Pediatr Cardiol. 2000;21(2):104–10.
Powell AJ, Tsai-Goodman B, Prakash A, Greil GF, Geva T. Comparison between phase-velocity cine magnetic resonance imaging and invasive oximetry for quantification of atrial shunts. Am J Cardiol. 2003;91(12):1523–5. A1529.
Kafka H, Mohiaddin RH. Cardiac MRI and pulmonary MR angiography of sinus venosus defect and partial anomalous pulmonary venous connection in cause of right undiagnosed ventricular enlargement. AJR Am J Roentgenol. 2009;192(1):259–66.
Ferrari VA, Scott CH, Holland GA, Axel L, Sutton MS. Ultrafast three-dimensional contrast-enhanced magnetic resonance angiography and imaging in the diagnosis of partial anomalous pulmonary venous drainage. J Am Coll Cardiol. 2001;37(4):1120–8.
Festa P, Ait-Ali L, Cerillo AG, De Marchi D, Murzi B. Magnetic resonance imaging is the diagnostic tool of choice in the preoperative evaluation of patients with partial anomalous pulmonary venous return. Int J Cardiovasc Imaging. 2006;22(5):685–93.
Prompona M, Muehling O, Naebauer M, Schoenberg SO, Reiser M, Huber A. MRI for detection of anomalous pulmonary venous drainage in patients with sinus venosus atrial septal defects. Int J Cardiovasc Imaging. 2011;27(3):403–12.
Dyer KT, Hlavacek AM, Meinel FG, et al. Imaging in congenital pulmonary vein anomalies: the role of computed tomography. Pediatr Radiol. 2014;44(9):1158–68. quiz 1155–1157.
Meyersohn NM, Ghemigian K, Shapiro MD, Shah SV, Ghoshhajra BB, Ferencik M. Role of computed tomography in assessment of the thoracic aorta. Curr Treat Options Cardiovasc Med. 2015;17(8):395.
Karaosmanoglu AD, Khawaja RD, Onur MR, Kalra MK. CT and MRI of aortic coarctation: pre- and postsurgical findings. AJR Am J Roentgenol. 2015;204(3):W224–33.
Goubergrits L, Riesenkampff E, Yevtushenko P, et al. MRI-based computational fluid dynamics for diagnosis and treatment prediction: clinical validation study in patients with coarctation of aorta. J Magn Reson Imaging. 2015;41(4):909–16.
Kenny D, Hamilton MC, Martin RP. Stainless steel stents and magnetic resonance imaging looking into a black hole. J Am Coll Cardiol. 2009;54(23):2202–3. author reply 2203.
Buechel ER, Dave HH, Kellenberger CJ, et al. Remodelling of the right ventricle after early pulmonary valve replacement in children with repaired tetralogy of Fallot: assessment by cardiovascular magnetic resonance. Eur Heart J. 2005;26(24):2721–7.
Dave HH, Buechel ER, Dodge-Khatami A, et al. Early insertion of a pulmonary valve for chronic regurgitation helps restoration of ventricular dimensions. Ann Thorac Surg. 2005;80(5):1615–20. discussion 1620–1611.
Frigiola A, Tsang V, Bull C, et al. Biventricular response after pulmonary valve replacement for right ventricular outflow tract dysfunction: is age a predictor of outcome? Circulation. 2008;118(14 Suppl):S182–90.
Geva T, Gauvreau K, Powell AJ, et al. Randomized trial of pulmonary valve replacement with and without right ventricular remodeling surgery. Circulation. 2010;122(11 Suppl):S201–8.
Lee C, Kim YM, Lee CH, et al. Outcomes of pulmonary valve replacement in 170 patients with chronic pulmonary regurgitation after relief of right ventricular outflow tract obstruction: implications for optimal timing of pulmonary valve replacement. J Am Coll Cardiol. 2012;60(11):1005–14.
Oosterhof T, van Straten A, Vliegen HW, et al. Preoperative thresholds for pulmonary valve replacement in patients with corrected tetralogy of Fallot using cardiovascular magnetic resonance. Circulation. 2007;116(5):545–51.
Therrien J, Provost Y, Merchant N, Williams W, Colman J, Webb G. Optimal timing for pulmonary valve replacement in adults after tetralogy of Fallot repair. Am J Cardiol. 2005;95(6):779–82.
Clarke CJ, Gurka MJ, Norton PT, Kramer CM, Hoyer AW. Assessment of the accuracy and reproducibility of RV volume measurements by CMR in congenital heart disease. JACC Cardiovasc Imaging. 2012;5(1):28–37.
Broberg CS, Aboulhosn J, Mongeon FP, et al. Prevalence of left ventricular systolic dysfunction in adults with repaired tetralogy of Fallot. Am J Cardiol. 2011;107(8):1215–20.
Ghai A, Silversides C, Harris L, Webb GD, Siu SC, Therrien J. Left ventricular dysfunction is a risk factor for sudden cardiac death in adults late after repair of tetralogy of Fallot. J Am Coll Cardiol. 2002;40(9):1675–80.
Geva T, Sandweiss BM, Gauvreau K, Lock JE, Powell AJ. Factors associated with impaired clinical status in long-term survivors of tetralogy of Fallot repair evaluated by magnetic resonance imaging. J Am Coll Cardiol. 2004;43(6):1068–74.
Babu-Narayan SV, Kilner PJ, Li W, et al. Ventricular fibrosis suggested by cardiovascular magnetic resonance in adults with repaired tetralogy of fallot and its relationship to adverse markers of clinical outcome. Circulation. 2006;113(3):405–13.
Grothoff M, Spors B, Abdul-Khaliq H, Gutberlet M. Evaluation of postoperative pulmonary regurgitation after surgical repair of tetralogy of Fallot: comparison between Doppler echocardiography and MR velocity mapping. Pediatr Radiol. 2008;38(2):186–91.
Li W, Davlouros PA, Kilner PJ, et al. Doppler-echocardiographic assessment of pulmonary regurgitation in adults with repaired tetralogy of Fallot: comparison with cardiovascular magnetic resonance imaging. Am Heart J. 2004;147(1):165–72.
Mercer-Rosa L, Yang W, Kutty S, Rychik J, Fogel M, Goldmuntz E. Quantifying pulmonary regurgitation and right ventricular function in surgically repaired tetralogy of Fallot: a comparative analysis of echocardiography and magnetic resonance imaging. Circ Cardiovasc Imaging. 2012;5(5):637–43.
Gorter TM, van Melle JP, Freling HG, et al. Pulmonary regurgitant volume is superior to fraction using background-corrected phase contrast MRI in determining the severity of regurgitation in repaired tetralogy of Fallot. Int J Cardiovasc Imaging. 2015;31(6):1169–77.
Cawley PJ, Maki JH, Otto CM. Cardiovascular magnetic resonance imaging for valvular heart disease: technique and validation. Circulation. 2009;119(3):468–78.
Phillips SD, Bonnichsen CR, McLeod CJ, Ammash NM, Burkhart HM, Connolly HM. Adults with congenital heart disease and previous intervention. Curr Probl Cardiol. 2013;38(8):293–357.
Babu-Narayan SV, Goktekin O, Moon JC, et al. Late gadolinium enhancement cardiovascular magnetic resonance of the systemic right ventricle in adults with previous atrial redirection surgery for transposition of the great arteries. Circulation. 2005;111(16):2091–8.
Giardini A, Lovato L, Donti A, et al. Relation between right ventricular structural alterations and markers of adverse clinical outcome in adults with systemic right ventricle and either congenital complete (after Senning operation) or congenitally corrected transposition of the great arteries. Am J Cardiol. 2006;98(9):1277–82.
Winter MM, Bernink FJ, Groenink M, et al. Evaluating the systemic right ventricle by CMR: the importance of consistent and reproducible delineation of the cavity. J Cardiovasc Magn Reson. 2008;10:40.
Patel S, Shah D, Chintala K, Karpawich PP. Atrial baffle problems following the Mustard operation in children and young adults with dextro-transposition of the great arteries: the need for improved clinical detection in the current era. Congenit Heart Dis. 2011;6(5):466–74.
Kreutzer C, De Vive J, Oppido G, et al. Twenty-five-year experience with rastelli repair for transposition of the great arteries. J Thorac Cardiovasc Surg. 2000;120(2):211–23.
Angeli E, Formigari R, Pace Napoleone C, et al. Long-term coronary artery outcome after arterial switch operation for transposition of the great arteries. Eur J Cardiothorac Surg. 2010;38(6):714–20.
Tobler D, Yalonetsky S, Crean AM, et al. Right heart characteristics and exercise parameters in adults with Ebstein anomaly: new perspectives from cardiac magnetic resonance imaging studies. Int J Cardiol. 2013;165(1):146–50.
Yalonetsky S, Tobler D, Greutmann M, et al. Cardiac magnetic resonance imaging and the assessment of ebstein anomaly in adults. Am J Cardiol. 2011;107(5):767–73.
Brown ML, Dearani JA, Danielson GK, et al. The outcomes of operations for 539 patients with Ebstein anomaly. J Thorac Cardiovasc Surg. 2008;135(5):1120–36. 1136 e1121-1127.
Raju V, Dearani JA, Burkhart HM, et al. Right ventricular unloading for heart failure related to Ebstein malformation. Ann Thorac Surg. 2014;98(1):167–73. discussion 173–164.
Varma C, Warr MR, Hendler AL, Paul NS, Webb GD, Therrien J. Prevalence of "silent" pulmonary emboli in adults after the Fontan operation. J Am Coll Cardiol. 2003;41(12):2252–8.
Grewal J, Al Hussein M, Feldstein J, et al. Evaluation of silent thrombus after the Fontan operation. Congenit Heart Dis. 2013;8(1):40–7.
Mavroudis C, Backer CL, Deal BJ. Late reoperations for Fontan patients: state of the art invited review. Eur J Cardiothorac Surg. 2008;34(5):1034–40.
Be’eri E, Maier SE, Landzberg MJ, Chung T, Geva T. In vivo evaluation of Fontan pathway flow dynamics by multidimensional phase-velocity magnetic resonance imaging. Circulation. 1998;98(25):2873–82.
Sundareswaran KS, Haggerty CM, de Zelicourt D, et al. Visualization of flow structures in Fontan patients using 3-dimensional phase contrast magnetic resonance imaging. J Thorac Cardiovasc Surg. 2012;143(5):1108–16.
de Leval MR, Dubini G, Migliavacca F, et al. Use of computational fluid dynamics in the design of surgical procedures: application to the study of competitive flows in cavo-pulmonary connections. J Thorac Cardiovasc Surg. 1996;111(3):502–13.
Asrani SK, Warnes CA, Kamath PS. Hepatocellular carcinoma after the Fontan procedure. N Engl J Med. 2013;368(18):1756–7. Although not the first case reports of hepatocellular carcinoma in patients with Fontan circulation, this report provided further evidence that longstanding liver congestion and cirrhosis in Fontan patients is a risk factor for hepatocellular carcinoma and routine surveillance is necessary in these patients.
Elder RW, Parekh S, Book WM. More on hepatocellular carcinoma after the Fontan procedure. N Engl J Med. 2013;369(5):490.
Saliba T, Dorkhom S, O’Reilly EM, Ludwig E, Gansukh B, Abou-Alfa GK. Hepatocellular carcinoma in two patients with cardiac cirrhosis. Eur J Gastroenterol Hepatol. 2010;22(7):889–91.
Venkatesh SK, Yin M, Ehman RL. Magnetic resonance elastography of liver: technique, analysis, and clinical applications. J Magn Reson Imaging. 2013;37(3):544–55.
Poterucha JT, Johnson JN, Qureshi MY, et al. Magnetic resonance elastography: a novel technique for the detection of hepatic fibrosis and hepatocellular carcinoma after the Fontan operation. Mayo Clin Proc. 2015;90(7):882–94.
Serai SD, Wallihan DB, Venkatesh SK, et al. Magnetic resonance elastography of the liver in patients status-post Fontan procedure: feasibility and preliminary results. Congenit Heart Dis. 2014;9(1):7–14.
Wallihan DB, Podberesky DJ, Marino BS, Sticka JS, Serai S. Relationship of MR elastography determined liver stiffness with cardiac function after Fontan palliation. J Magn Reson Imaging. 2014;40(6):1328–35.
Bluemke DA, Achenbach S, Budoff M, et al. Noninvasive coronary artery imaging: magnetic resonance angiography and multidetector computed tomography angiography: a scientific statement from the American Heart Association committee on cardiovascular imaging and intervention of the council on cardiovascular radiology and intervention, and the councils on clinical cardiology and cardiovascular disease in the young. Circulation. 2008;118(5):586–606.
Miller JA, Anavekar NS, El Yaman MM, Burkhart HM, Miller AJ, Julsrud PR. Computed tomographic angiography identification of intramural segments in anomalous coronary arteries with interarterial course. Int J Cardiovasc Imaging. 2012;28(6):1525–32.
Torres FS, Nguyen ET, Dennie CJ, et al. Role of MDCT coronary angiography in the evaluation of septal vs interarterial course of anomalous left coronary arteries. J Cardiovasc Comput Tomogr. 2010;4(4):246–54.
Opolski MP, Pregowski J, Kruk M, et al. Prevalence and characteristics of coronary anomalies originating from the opposite sinus of Valsalva in 8,522 patients referred for coronary computed tomography angiography. Am J Cardiol. 2013;111(9):1361–7.
Angelini P, Cheong B. Left coronary artery from the right coronary sinus: what can CT angiography tell us? J Cardiovasc Comput Tomogr. 2010;4(4):255–7.
Budoff MJ, Dowe D, Jollis JG, et al. Diagnostic performance of 64-multidetector row coronary computed tomographic angiography for evaluation of coronary artery stenosis in individuals without known coronary artery disease: results from the prospective multicenter ACCURACY (Assessment by Coronary Computed Tomographic Angiography of Individuals Undergoing Invasive Coronary Angiography) trial. J Am Coll Cardiol. 2008;52(21):1724–32.
Zhou K, Kong L, Wang Y, et al. Coronary artery fistula in adults: evaluation with dual-source CT coronary angiography. Br J Radiol. 2015;88(1049):20140754.
Saboo SS, Juan YH, Khandelwal A, et al. MDCT of congenital coronary artery fistulas. AJR Am J Roentgenol. 2014;203(3):W244–52.
Ishida M, Sakuma H. Coronary MR angiography revealed: how to optimize image quality. Magn Reson Imaging Clin N Am. 2015;23(1):117–25.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Crystal Bonnichsen and Naser Ammash declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Congenital Heart Disease
Rights and permissions
About this article
Cite this article
Bonnichsen, C., Ammash, N. Choosing Between MRI and CT Imaging in the Adult with Congenital Heart Disease. Curr Cardiol Rep 18, 45 (2016). https://doi.org/10.1007/s11886-016-0717-x
Published:
DOI: https://doi.org/10.1007/s11886-016-0717-x