Abstract
Purpose of Review
The objective of this review is to shed light on the transformative potential of machine learning (ML) in coronary angiography. We aim to understand existing developments in using ML for coronary angiography and discuss broader implications for the future of coronary angiography and cardiovascular medicine.
Recent Findings
The developments in invasive and noninvasive imaging have revolutionized diagnosis and treatment of coronary artery disease (CAD). However, CAD remains underdiagnosed and undertreated. ML has emerged as a powerful tool to further improve image analysis, hemodynamic assessment, lesion detection, and predictive modeling. These advancements have enabled more accurate identification of CAD, streamlined workflows, reduced the need for invasive diagnostic procedures, and improved the diagnostic value of invasive procedures when they are needed. Further integration of ML with coronary angiography will advance the prevention, diagnosis, and treatment of CAD.
Summary
The integration of ML with coronary angiography is ushering in a new era in cardiovascular medicine. We highlight five use cases to leverage ML in coronary angiography: (1) improvement of quality and efficacy, (2) characterization of plaque, (3) hemodynamic assessment, (4) prediction of future outcomes, and (5) diagnosis of non-atherosclerotic coronary disease.
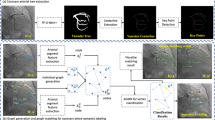
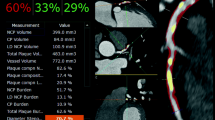
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Coronary artery disease (CAD) remains a leading cause of morbidity and mortality despite remarkable advances in invasive and noninvasive diagnostic modalities [1]. A comprehensive evaluation of CAD involves assessing the severity, burden, and characteristics of coronary atherosclerosis, with (i) noninvasive modalities such as computed coronary tomography angiography (CCTA) and/or (ii) catheterization with invasive coronary angiography (ICA) and sometimes intravascular imaging. A comprehensive understanding of CAD requires not only an identification of its presence but also an assessment of the coronary burden which represents the extent and severity of coronary atherosclerosis. Furthermore, the specific characteristics of plaques, such as their composition, vulnerability to rupture, and location, play crucial roles in translating to different clinical outcomes. Characterization of plaque burden and features might lead to potential therapeutic nuances and variability in prognostication [2]. In addition to this anatomic evaluation of CAD, a physiologic evaluation of the flow-limiting effects of a stenosis in a coronary artery is often necessary and constitutes the main driver for revascularization decisions. Physiologic evaluations can also be performed (i) noninvasively such as with myocardial perfusion stress testing and fractional flow reserve-computed tomography (FFR-CT) or (ii) invasively using pressure-wire indices such as fractional flow reserve (FFR) or non-hyperemic pressure wave ratios (iFR, DFR, RFR, etc.) [3,4,5].
Although CCTA and ICA lie on different ends of the invasiveness spectrum, they are the two most important modalities for anatomic evaluation of CAD. As a noninvasive option, CCTA offers visualization of coronary tree and atherosclerotic plaques but also can accurately quantify plaque volumes and identify high-risk plaque features such as low attenuation plaque and napkin-ring sign that have been associated with future cardiovascular events [6, 7]. On the other hand, ICA not only can assess coronary anatomy and plaque and identify plaque characteristics with intraluminal imaging, but also can facilitate real-time therapeutic interventions [6].
The proliferation of artificial intelligence (AI)-enabled medical technologies in recent years has led to new capabilities of diagnostic and therapeutic modalities. Historically, medical procedures and diagnostics relied on a blend of practitioner expertise and available technological tools. However, AI has bridged the gap between massive datasets and actionable insights, processing and analyzing intricate data at unprecedented scales [8]. Unsurprisingly, this progress was also represented in the realm of cardiology. The diagnostic nuances and treatment intricacies required in cardiology often mandate processing vast arrays of data, from electrocardiograms to imaging modalities. Therefore, AI found many potential use cases to improve diagnostics and therapeutics by identifying patterns and anomalies that might otherwise escape the human eye [8].
The Need to Improve CCTA and ICA
The developments in noninvasive imaging, particularly CCTA, as well as advancements in invasive intraluminal imaging have ushered in a revolutionary era for visualizing coronary anatomy and plaques but most importantly identifying plaque characteristics [9]. However, despite these advancements, coronary disease remains underdiagnosed and undertreated leading to significant morbidity and mortality in the world [10].
There are several issues with the current diagnostic tools including inter-reader variability, insufficient accuracy, and high costs (Table 1) [11•, 12]. One of the primary concerns is the subjectivity that comes with interpreting CCTA and ICA. As the interpretations of the images largely depend on the expertise and experience of the radiologist or cardiologist, there is an inherent variability in readings [11•]. Two clinicians may perceive the severity of a stenosis differently or might miss a subtle lesion altogether. This lack of standardization can potentially lead to misdiagnosis, unnecessary interventions, or overlooked therapeutic opportunities [12].
Despite the high-resolution imaging provided by CCTA and ICA, there are three major limitations when it comes to their accuracy. First, the presence of heavy calcifications can pose challenges in determining the exact extent of luminal narrowing, leading to either overestimation or underestimation of stenosis [9]. Second, while invasive angiograms provide a two-dimensional view, they might not capture the complexities of certain lesions, particularly in tortuous coronary segments unless intraluminal imaging is utilized. Third, these advanced imaging modalities can be costly and might not be readily available in all healthcare settings, especially in low-resource areas [13].Considering these challenges, there is an impending need to refine current diagnostic strategies. The integration of machine learning (ML) could offer solutions by providing a more standardized, accurate, and comprehensive analysis of coronary artery disease and lower associated costs. However, despite advancements in medicine, cardiology, and imaging, ML has not yet well penetrated the coronary angiography space.
ML has already made significant strides in medical imaging across various specialties. In pathology, ML has been employed to analyze digital pathology slides, aiding in the detection and classification of diseases such as malignancies [14]. Stroke detection has been revolutionized with algorithms that rapidly identify signs in CT scans, specifically targeting large vessel occlusions [15, 16]. In dermatology and ophthalmology, ML-enabled tools can assist in diagnosing conditions such as skin cancers [17] and diabetic retinopathy [18]. Similarly, ML has the potential to significantly enhance coronary angiography. It can improve image interpretation by detecting subtle atherosclerotic disease and provide more information on plaque morphology and hemodynamic significance, reduce radiation exposure through optimized parameters, and offer predictive insights by analyzing angiographic data alongside patient history. Furthermore, ML can automate intricate measurements, ensuring consistency and reducing variability, while also integrating angiographic data with other diagnostic modalities for a holistic view of cardiovascular health.
We have identified five key areas of opportunity to leverage ML in coronary angiography to advance the prevention, diagnosis, and treatment of CAD (Fig. 1).
Five key areas of opportunity to leverage ML in coronary angiography. ML offers significant potential in coronary angiography, particularly in five key areas to enhance the prevention, diagnosis, and treatment of CAD: (1) improvement of quality and efficacy; (2) characterization of plaque; (3) hemodynamic assessment; (4) prediction of future outcomes; and (5) diagnosis of non-atherosclerotic coronary disease
Improvement in Quality and Efficacy of Coronary Evaluation
ML algorithms, especially those based on deep learning architectures, have shown remarkable proficiency in image recognition tasks [19]. When trained on vast datasets of angiograms, these algorithms have the potential to achieve a level of precision that might rival or even surpass, medical experts. There are three primary advantages of ML in this context. First, ML can identify and quantify features such as stenoses, plaques, and vessel diameters with high accuracy [20, 21••]. Conventional manual analysis is often subjective and prone to variability between different observers [12]. ML on the other hand might offer a consistent and objective analysis, significantly reducing human error [20, 21••], similar to prior studies on echocardiograms [22]. Second, the subtleties in angiographic images, which might be missed during manual inspection, can be detected by ML algorithms. These subtle findings, though they might appear insignificant, can often be clinically relevant and indicative of early disease stages or potential complications. By ensuring that such findings are not overlooked, ML can aid in enhancing the overall diagnostic quality. Third, automated image analysis can streamline diagnostic workflows. Manual analysis of angiograms can be time-consuming, especially in complex cases. ML-enabled tools can rapidly process these images, providing insights in a fraction of the time. This acceleration in the diagnostic process allows for faster patient management decisions, potentially leading to timely interventions and improved patient outcomes [23].
The clarity and quality of angiographic images are paramount for accurate diagnosis. With the advent of ML, there is an opportunity to significantly refine these images. In other cardiovascular imaging modalities, ML algorithms, particularly those based on convolutional neural networks, have demonstrated the ability to filter out noise and artifacts, enhancing the overall clarity of the images [21••, 24]. Additionally, these algorithms can enhance contrast, making it easier to differentiate between various structures and abnormalities in the coronary arteries. As a result, even miniscule changes or abnormalities, which might be overlooked in conventional image interpretation, become discernible [25].
Enhanced images are especially beneficial in challenging cases, where traditional imaging might fall short due to factors like patient movement, suboptimal contrast injection, or anatomical complexities. In such scenarios, the capabilities of ML can be harnessed to improve image quality, ensuring that the diagnosis is based on the best possible visualization of the coronary anatomy. Although this remains to be studied, ML-enhanced imaging and improved image quality could potentially result in more accurate diagnoses, timely interventions, and ultimately, better patient outcomes. In a recent example from multi-modal magnetic resonance imaging, using a cascade of convolutional neural networks for brain tumor segmentation led to an improvement of segmentation accuracy [26].
Characterization of Coronary Plaque
CCTA is a powerful noninvasive tool to visualize coronary anatomy and most importantly, coronary plaque morphology [9]. Its ability to provide high-resolution images of the coronary arteries noninvasively makes it invaluable for detecting and characterizing coronary artery disease. In contrast, ICA primarily offers an anatomical assessment of the coronary arteries. It visualizes the lumen of the arteries and the extent of the coronary disease highlighting areas of potential significant flow restriction, which can be indicative of clinically significant stenoses [27]. However, it also allows for intravascular coronary imaging which provides excellent detail and a granular morphological understanding of plaques. Techniques such as optical coherence tomography (OCT) and intravascular ultrasound (IVUS) provide high-resolution images of plaque composition, size, and location. These modalities delve deeper into the vessel wall, revealing details that are often invisible to other imaging techniques, thus providing invaluable information for planning interventional strategies [28]. This information offers insights into plaque composition, stability, and potential for rupture [29]. With the integration of ML algorithms, these imaging techniques can be further enhanced by analyzing the vast amount of data generated by these modalities, offering predictive insights that can help clinicians anticipate potential complications like plaque rupture or thrombosis [30]. By understanding the biological characteristics of plaques, clinicians can tailor treatment strategies. This personalized approach, ranging from medication adjustments to specific interventional procedures, ensures that patients receive optimal care based on their unique plaque biology [31]. Furthermore, these algorithms can integrate data from multiple sources, such as patient history, blood tests, and other diagnostic tests, to provide a comprehensive risk profile for individual patients [32]. With this knowledge, one can devise more personalized treatment strategies. For some patients, this might lead to medication adjustments and optimization, while for others, it can involve percutaneous coronary interventions such as stenting or balloon angioplasty [33]. This personalized approach might ensure that patients receive optimal care tailored to their unique plaque biology and overall cardiovascular risk, leading to better outcomes [34].
Hemodynamic Assessment of Coronary Stenosis
Both CCTA and ICA can provide information on lesion location, severity, and extent. However, ICA provides an additional advantage by allowing hemodynamic evaluation of potentially clinically significant lesions. Hemodynamic evaluation can be done using FFR, a measure that compares the pressure before and after the stenosis under maximal hyperemia [35] or instantaneous wave-free ratio (IFR) that achieves the same by evaluating wave-free period of cardiac cycle without the need for drug-induced hyperemia [3]. Recently, noninvasive methods like CT-derived FFR have emerged as reliable alternatives to invasive FFR measurements [5]. CT-derived FFR, which utilizes computational fluid dynamics on CCTA data, offers the advantage of assessing both anatomical and functional significance of coronary lesions without the need for invasive catheterization [4]. HeartFlow, a specific CT-derived FFR analysis tool, has been shown to improve diagnostic accuracy and patient outcomes while potentially reducing healthcare costs [36].
Despite the advancements in CT-derived FFR technology, ICA still offers a benefit by allowing for interventions during the same procedure if the lesion of interest is deemed to be hemodynamically significant. However, invasive hemodynamic assessment requires passing a coronary wire through the lesion in the coronary artery which is a further invasive method that increases time and potential risks associated with the procedure [3]. Deep learning models trained with datasets with hemodynamic measurements and high-quality angiograms have the potential to provide the same hemodynamic information without the need for coronary wiring [37, 38]. This technology could enhance the evaluation of flow characteristics in lesions that were not initially identified as intermediate through visual assessment. This advancement offers an additional avenue to reduce oversight by standardizing measurements.
Prediction of Future Outcomes
Despite our growing knowledge and advanced diagnostic tools, recurrent cardiovascular events remain a significant concern [2]. This underscores the need for risk stratification based on improved prediction models and personalized preventative interventions. The coronary artery calcium (CAC) score, derived from non-contrast CT scans, has been a cornerstone in predicting future cardiovascular events [39]. It quantifies the amount of calcium in coronary arteries, providing insights into the extent of atherosclerotic plaque burden. While the CAC score has proven to be highly beneficial, it can only identify calcified plaques and cannot predict future events based on plaques morphology. This especially poses a potential issue for the younger population with higher likelihood of having noncalcified coronary plaques [40]. Therefore, advanced modalities like CCTA and ICA combined with ML could offer insights beyond calcification, such as plaque morphology, and inflammation. It holds promise in enhancing our predictive capabilities and reducing recurrent events by analyzing the vast patient data outside of a given imaging modality and identify subtle patterns [19]. Furthermore, ML can also be used to enhance existing predictive tools such as CAC score by incorporating clinical features and improving quantification of CAC scoring [41•].
Diagnosing Non-atherosclerotic Coronary Disease
While atherosclerosis remains at the forefront of concerns in coronary artery disease, there are non-atherosclerotic conditions that demand equal attention and understanding. Spontaneous coronary artery dissection (SCAD), cardiac allograft vasculopathy (CAV), and microvascular disease are among these conditions, each presenting its own set of challenges and complexities (Table 2).
Spontaneous coronary artery dissection is characterized by a spontaneous tear in the coronary artery wall leading to a false lumen, which can lead to myocardial ischemia and infarction. SCAD is an uncommon yet critical cause of acute coronary syndrome, particularly among younger individuals and women [42]. The exact etiology of SCAD remains to be fully elucidated, but it has been associated with a variety of conditions that affect hormonal, shear stress, and vascular structural factors [43]. CCTA and ICA with intravascular ultrasound are commonly employed tools for its identification [44] but diagnosis can be challenging due to its atypical presentation and variable imaging findings [44]. ML-enhanced imaging interpretation has the potential to improve diagnosis of SCAD by increasing accuracy of reads and reducing missingness.
Cardiac allograft vasculopathy (CAV) is a unique and progressive form of coronary artery disease that affects heart transplant recipients [45]. It is characterized by diffuse intimal thickening and fibroproliferation, leading to stenosis of the coronary arteries. CAV is one of the leading causes of late graft failure and mortality post-heart transplantation. Traditional diagnostic methods, such as coronary angiography, may not be sensitive enough to detect early changes of CAV, given its diffuse nature [46]. Similar to CAV, microvascular disease pertains to the dysfunction of the coronary microvasculature and affects the microcirculation due to factors that are traditionally associated with coronary disease such as hypertension, hyperlipidemia, and diabetes or endothelial dysfunction [47]. It can potentially lead to symptoms such as angina despite the absence of significant epicardial coronary artery stenosis [48]. The intricate nature of these conditions, combined with their diverse presentations, means that they often elude conventional diagnostic tools and strategies, leading to underdiagnosis or misdiagnosis. A variety of invasive and noninvasive imaging modalities are used to assess microvascular dysfunction that utilizes indices such as coronary flow reserves (CFR) and index of microcirculatory resistance (IMR) [49]. However, each noninvasive imaging modality has specific challenges and various sensitivity and specificity levels for detecting microvascular dysfunction [49]. Invasive measurements are the gold standard to diagnose microvascular disease; however, they require advancing pressure wires through coronary arteries which increase procedural risks and time spent during the procedure [49, 50]. Similar to the technologies developed to measure FFR and IFR based on invasive and noninvasive coronary angiograms using flow dynamics, ML algorithms can help with the assessment of coronary microvasculature without the need for pressure wires.
Challenges with Using ML in Coronary Angiograms and Potential Solutions
ML applications in coronary angiograms present both opportunities and challenges. The most important considerations and challenges when using ML applications in coronary angiograms are (i) variability of findings between patients, (ii) ethical considerations, (iii) data privacy, and (iv) interpretability. First, the nature of coronary artery lesions, combined with the variability in patient anatomy and the subtle distinctions between pathological and normal findings, can make automated analysis complex. However, advancements in ML algorithms and the increasing availability of labeled datasets are addressing these complexities [51]. For instance, the variability in coronary angiogram images, stemming from differences in equipment, techniques, and patient anatomy, can be mitigated by training ML models on diverse and representative datasets. Additionally, advanced preprocessing techniques and data augmentation can help filter out noise and artifacts, ensuring that ML models are trained on high-quality data [24].
Second, ethical considerations are paramount when integrating ML into medical imaging. Ensuring patient privacy is crucial, and data used for training ML models must be anonymized, removing any personally identifiable information [52]. Moreover, the potential for algorithmic bias, where models might perform differently for various patient subgroups, is a concern that needs proactive addressing to ensure equitable care. Transparency in communicating to patients about how their data will be used and obtaining informed consent is also important. Furthermore, ML models should be regularly evaluated and updated to ensure they are free from biases and provide consistent results across diverse patient groups.
Third, data sharing is another challenge that needs close attention. While ML models require vast amounts of data to achieve high accuracy, sharing patient data across institutions raises concerns about data privacy and security. Innovative solutions like federated learning, where the model is trained across multiple sites without sharing raw data, are emerging [53]. Ensuring data encryption and implementing differential privacy techniques can further safeguard patient information.
Finally, a significant criticism of ML, especially deep learning models, is their “black box” nature [54]. The challenge lies in understanding how these models arrive at their decisions, a crucial aspect in medical applications where interpretability is essential. Emphasis should be placed on developing or using ML models that offer insights into their decision-making processes. Interpretation and data visualization methods such as saliency maps [55], gradient-weighted class-activation maps [56], backward optimization [57], and novelty detection [58, 59] can help visualize which parts of angiograms were most influential in the model’s decision, adding a layer of transparency.
Conclusion
Diagnosis of CAD requires assessing the severity and characteristics of coronary atherosclerosis, with both CCTA and ICA playing pivotal roles in diagnosing and offering insights into plaque characteristics. Following the growth of AI-enabled technologies in other areas of medicine, ML can similarly be leveraged to enhance both invasive and noninvasive coronary angiography for better diagnosis and management of CAD. We highlighted five potential use cases in which ML for coronary angiography holds significant promise: (1) improvement of quality and efficacy, (2) characterization of plaque, (3) hemodynamic assessment, (4) prediction of future outcomes, and (5) diagnosis of non-atherosclerotic coronary disease. While ML offers transformative potential in the realm of coronary angiograms, careful consideration of challenges, ethical implications, data sharing protocols, and model interpretability is essential to harness its full potential and ensure optimal patient care.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Roth GA, Mensah GA, Johnson CO, Addolorato G, Ammirati E, Baddour LM, et al. Global burden of cardiovascular diseases and risk factors, 1990–2019: Update From the GBD 2019 Study. J Am Coll Cardiol. 2020;76(25):2982–3021. https://doi.org/10.1016/j.jacc.2020.11.010.
Stone GW, Maehara A, Lansky AJ, de Bruyne B, Cristea E, Mintz GS, et al. A prospective natural-history study of coronary atherosclerosis. N Engl J Med. 2011;364(3):226–35. https://doi.org/10.1056/NEJMoa1002358.
Davies JE, Sen S, Dehbi HM, Al-Lamee R, Petraco R, Nijjer SS, et al. Use of the instantaneous wave-free ratio or fractional flow reserve in PCI. N Engl J Med. 2017;376(19):1824–34. https://doi.org/10.1056/NEJMoa1700445.
Nørgaard BL, Leipsic J, Gaur S, Seneviratne S, Ko BS, Ito H, et al. Diagnostic performance of noninvasive fractional flow reserve derived from coronary computed tomography angiography in suspected coronary artery disease: the NXT trial (Analysis of Coronary Blood Flow Using CT Angiography: Next Steps). J Am Coll Cardiol. 2014;63(12):1145–55. https://doi.org/10.1016/j.jacc.2013.11.043.
Taylor CA, Fonte TA, Min JK. Computational fluid dynamics applied to cardiac computed tomography for noninvasive quantification of fractional flow reserve: scientific basis. J Am Coll Cardiol. 2013;61(22):2233–41. https://doi.org/10.1016/j.jacc.2012.11.083.
Miller JM, Rochitte CE, Dewey M, Arbab-Zadeh A, Niinuma H, Gottlieb I, et al. Diagnostic performance of coronary angiography by 64-row CT. N Engl J Med. 2008;359(22):2324–36. https://doi.org/10.1056/NEJMoa0806576.
Williams MC, Moss AJ, Dweck M, Adamson PD, Alam S, Hunter A, et al. Coronary artery plaque characteristics associated with adverse outcomes in the SCOT-HEART study. J Am Coll Cardiol. 2019;73(3):291–301. https://doi.org/10.1016/j.jacc.2018.10.066.
Johnson KW, Torres Soto J, Glicksberg BS, Shameer K, Miotto R, Ali M, et al. Artificial intelligence in cardiology. J Am Coll Cardiol. 2018;71(23):2668–79. https://doi.org/10.1016/j.jacc.2018.03.521.
Budoff MJ, Dowe D, Jollis JG, Gitter M, Sutherland J, Halamert E, et al. Diagnostic performance of 64-multidetector row coronary computed tomographic angiography for evaluation of coronary artery stenosis in individuals without known coronary artery disease: results from the prospective multicenter ACCURACY (Assessment by Coronary Computed Tomographic Angiography of Individuals Undergoing Invasive Coronary Angiography) trial. J Am Coll Cardiol. 2008;52(21):1724–32. https://doi.org/10.1016/j.jacc.2008.07.031.
Benjamin EJ, Muntner P, Alonso A, Bittencourt MS, Callaway CW, Carson AP, et al. Heart disease and stroke statistics-2019 update: a report from the American Heart Association. Circulation. 2019;139(10):e56–528. https://doi.org/10.1161/cir.0000000000000659.
Jonas RA, Weerakoon S, Fisher R, Griffin WF, Kumar V, Rahban H, et al. Interobserver variability among expert readers quantifying plaque volume and plaque characteristics on coronary CT angiography: a CLARIFY trial sub-study. Clin Imaging. 2022;91:19–25. https://doi.org/10.1016/j.clinimag.2022.08.005. Findings from this study highlights the subjectivity and inherent variability of coronary computer tomography angiography evaluations.
Zhang H, Mu L, Hu S, Nallamothu BK, Lansky AJ, Xu B, et al. Comparison of physician visual assessment with quantitative coronary angiography in assessment of stenosis severity in China. JAMA Intern Med. 2018;178(2):239–47. https://doi.org/10.1001/jamainternmed.2017.7821.
Priest VL, Scuffham PA, Hachamovitch R, Marwick TH. Cost-effectiveness of coronary computed tomography and cardiac stress imaging in the emergency department: a decision analytic model comparing diagnostic strategies for chest pain in patients at low risk of acute coronary syndromes. JACC Cardiovasc Imaging. 2011;4(5):549–56. https://doi.org/10.1016/j.jcmg.2011.03.008.
Litjens G, Sánchez CI, Timofeeva N, Hermsen M, Nagtegaal I, Kovacs I, et al. Deep learning as a tool for increased accuracy and efficiency of histopathological diagnosis. Sci Rep. 2016;6:26286. https://doi.org/10.1038/srep26286.
Chilamkurthy S, Ghosh R, Tanamala S, Biviji M, Campeau NG, Venugopal VK, et al. Deep learning algorithms for detection of critical findings in head CT scans: a retrospective study. Lancet. 2018;392(10162):2388–96. https://doi.org/10.1016/s0140-6736(18)31645-3.
Lansberg MG, Christensen S, Kemp S, Mlynash M, Mishra N, Federau C, et al. Computed tomographic perfusion to predict response to recanalization in ischemic stroke. Ann Neurol. 2017;81(6):849–56. https://doi.org/10.1002/ana.24953.
Esteva A, Kuprel B, Novoa RA, Ko J, Swetter SM, Blau HM, et al. Dermatologist-level classification of skin cancer with deep neural networks. Nature. 2017;542(7639):115–8. https://doi.org/10.1038/nature21056.
Gulshan V, Peng L, Coram M, Stumpe MC, Wu D, Narayanaswamy A, et al. Development and validation of a deep learning algorithm for detection of diabetic retinopathy in retinal fundus photographs. JAMA. 2016;316(22):2402–10. https://doi.org/10.1001/jama.2016.17216.
Al’Aref SJ, Anchouche K, Singh G, Slomka PJ, Kolli KK, Kumar A, et al. Clinical applications of machine learning in cardiovascular disease and its relevance to cardiac imaging. Eur Heart J. 2019;40(24):1975–86. https://doi.org/10.1093/eurheartj/ehy404.
Kang D, Dey D, Slomka PJ, Arsanjani R, Nakazato R, Ko H, et al. Structured learning algorithm for detection of nonobstructive and obstructive coronary plaque lesions from computed tomography angiography. J Med Imaging (Bellingham). 2015;2(1):014003. https://doi.org/10.1117/1.Jmi.2.1.014003.
Lin A, Manral N, McElhinney P, Killekar A, Matsumoto H, Kwiecinski J, et al. Deep learning-enabled coronary CT angiography for plaque and stenosis quantification and cardiac risk prediction: an international multicentre study. Lancet Digit Health. 2022;4(4):e256–65. https://doi.org/10.1016/s2589-7500(22)00022-x. In this international, multicenter study, a comprehensive and externally validated machine learning model was developed for rapid measurements of plaque volume and stenosis. It demonstrated that the model agreed closely with the expert readers but was more consistent and significantly faster.
Madani A, Arnaout R, Mofrad M, Arnaout R. Fast and accurate view classification of echocardiograms using deep learning. NPJ Digit Med. 2018;1. https://doi.org/10.1038/s41746-017-0013-1
van Rosendael AR, Maliakal G, Kolli KK, Beecy A, Al’Aref SJ, Dwivedi A, et al. Maximization of the usage of coronary CTA derived plaque information using a machine learning based algorithm to improve risk stratification; insights from the CONFIRM registry. J Cardiovasc Comput Tomogr. 2018;12(3):204–9. https://doi.org/10.1016/j.jcct.2018.04.011.
Shen D, Wu G, Suk HI. Deep learning in medical image analysis. Annu Rev Biomed Eng. 2017;19:221–48. https://doi.org/10.1146/annurev-bioeng-071516-044442.
Liu F, Jang H, Kijowski R, Bradshaw T, McMillan AB. Deep learning MR imaging-based attenuation correction for PET/MR imaging. Radiology. 2018;286(2):676–84. https://doi.org/10.1148/radiol.2017170700.
Wang G, Li W, Ourselin S, Vercauteren T. Automatic brain tumor segmentation based on cascaded convolutional neural networks with uncertainty estimation. Front Comput Neurosci. 2019;13:56. https://doi.org/10.3389/fncom.2019.00056.
Douglas PS, Hoffmann U, Patel MR, Mark DB, Al-Khalidi HR, Cavanaugh B, et al. Outcomes of anatomical versus functional testing for coronary artery disease. N Engl J Med. 2015;372(14):1291–300. https://doi.org/10.1056/NEJMoa1415516.
De la Garza-Salazar F, Lankenau-Vela DL, Cadena-Nuñez B, González-Cantú A, Romero-Ibarguengoitia ME. The effect of functional and intra-coronary imaging techniques on fluoroscopy time, radiation dose and contrast volume during coronary angiography. Sci Rep. 2020;10(1):6950. https://doi.org/10.1038/s41598-020-63791-1.
Koskinas KC, Nakamura M, Räber L, Colleran R, Kadota K, Capodanno D, et al. Current use of intracoronary imaging in interventional practice - results of a European Association of Percutaneous Cardiovascular Interventions (EAPCI) and Japanese Association of Cardiovascular Interventions and Therapeutics (CVIT) Clinical Practice Survey. EuroIntervention. 2018;14(4):e475–84. https://doi.org/10.4244/eijy18m03_01.
Dey D, Gaur S, Ovrehus KA, Slomka PJ, Betancur J, Goeller M, et al. Integrated prediction of lesion-specific ischaemia from quantitative coronary CT angiography using machine learning: a multicentre study. Eur Radiol. 2018;28(6):2655–64. https://doi.org/10.1007/s00330-017-5223-z.
Jia H, Dai J, Hou J, Xing L, Ma L, Liu H, et al. Effective anti-thrombotic therapy without stenting: intravascular optical coherence tomography-based management in plaque erosion (the EROSION study). Eur Heart J. 2017;38(11):792–800. https://doi.org/10.1093/eurheartj/ehw381.
Krittanawong C, Zhang H, Wang Z, Aydar M, Kitai T. Artificial intelligence in precision cardiovascular medicine. J Am Coll Cardiol. 2017;69(21):2657–64. https://doi.org/10.1016/j.jacc.2017.03.571.
Fahed AC, Jang IK. Plaque erosion and acute coronary syndromes: phenotype, molecular characteristics and future directions. Nat Rev Cardiol. 2021;18(10):724–34. https://doi.org/10.1038/s41569-021-00542-3.
Motwani M, Dey D, Berman DS, Germano G, Achenbach S, Al-Mallah MH, et al. Machine learning for prediction of all-cause mortality in patients with suspected coronary artery disease: a 5-year multicentre prospective registry analysis. Eur Heart J. 2017;38(7):500–7. https://doi.org/10.1093/eurheartj/ehw188.
Tonino PA, De Bruyne B, Pijls NH, Siebert U, Ikeno F, van’t Veer M, et al. Fractional flow reserve versus angiography for guiding percutaneous coronary intervention. N Engl J Med. 2009;360(3):213–24. https://doi.org/10.1056/NEJMoa0807611.
Douglas PS, De Bruyne B, Pontone G, Patel MR, Norgaard BL, Byrne RA, et al. 1-year outcomes of FFRCT-guided care in patients with suspected coronary disease: the PLATFORM study. J Am Coll Cardiol. 2016;68(5):435–45. https://doi.org/10.1016/j.jacc.2016.05.057.
Cho H, Lee JG, Kang SJ, Kim WJ, Choi SY, Ko J, et al. Angiography-based machine learning for predicting fractional flow reserve in intermediate coronary artery lesions. J Am Heart Assoc. 2019;8(4):e011685. https://doi.org/10.1161/jaha.118.011685.
Kogame N, Ono M, Kawashima H, Tomaniak M, Hara H, Leipsic J, et al. The impact of coronary physiology on contemporary clinical decision making. JACC Cardiovasc Interv. 2020;13(14):1617–38. https://doi.org/10.1016/j.jcin.2020.04.040.
Detrano R, Guerci AD, Carr JJ, Bild DE, Burke G, Folsom AR, et al. Coronary calcium as a predictor of coronary events in four racial or ethnic groups. N Engl J Med. 2008;358(13):1336–45. https://doi.org/10.1056/NEJMoa072100.
Kral BG, Becker LC, Vaidya D, Yanek LR, Qayyum R, Zimmerman SL, et al. Noncalcified coronary plaque volumes in healthy people with a family history of early onset coronary artery disease. Circ Cardiovasc Imaging. 2014;7(3):446–53. https://doi.org/10.1161/circimaging.113.000980.
Nakanishi R, Slomka PJ, Rios R, Betancur J, Blaha MJ, Nasir K, et al. Machine learning adds to clinical and CAC assessments in predicting 10-year CHD and CVD deaths. JACC Cardiovasc Imaging. 2021;14(3):615–25. https://doi.org/10.1016/j.jcmg.2020.08.024. This study demonstrated that a machine learning model was superior in predicting cardiovascular disease and coronary heart disease related mortality compared to existing prediction tools including atherosclerotic cardiovascular disease risk calculators and coronary artery calcium score.
Hayes SN, Kim ESH, Saw J, Adlam D, Arslanian-Engoren C, Economy KE, et al. Spontaneous coronary artery dissection: current state of the science: a scientific statement from the American Heart Association. Circulation. 2018;137(19):e523–57. https://doi.org/10.1161/cir.0000000000000564.
Tweet MS, Hayes SN, Pitta SR, Simari RD, Lerman A, Lennon RJ, et al. Clinical features, management, and prognosis of spontaneous coronary artery dissection. Circulation. 2012;126(5):579–88. https://doi.org/10.1161/circulationaha.112.105718.
Alfonso F, Paulo M, Lennie V, Dutary J, Bernardo E, Jiménez-Quevedo P, et al. Spontaneous coronary artery dissection: long-term follow-up of a large series of patients prospectively managed with a “conservative” therapeutic strategy. JACC Cardiovasc Interv. 2012;5(10):1062–70. https://doi.org/10.1016/j.jcin.2012.06.014.
Costanzo MR, Dipchand A, Starling R, Anderson A, Chan M, Desai S, et al. The International Society of Heart and Lung Transplantation Guidelines for the care of heart transplant recipients. J Heart Lung Transplant. 2010;29(8):914–56. https://doi.org/10.1016/j.healun.2010.05.034.
Mehra MR, Crespo-Leiro MG, Dipchand A, Ensminger SM, Hiemann NE, Kobashigawa JA, et al. International Society for Heart and Lung Transplantation working formulation of a standardized nomenclature for cardiac allograft vasculopathy-2010. J Heart Lung Transplant. 2010;29(7):717–27. https://doi.org/10.1016/j.healun.2010.05.017.
Del Buono MG, Montone RA, Camilli M, Carbone S, Narula J, Lavie CJ, et al. Coronary microvascular dysfunction across the spectrum of cardiovascular diseases: JACC state-of-the-art review. J Am Coll Cardiol. 2021;78(13):1352–71. https://doi.org/10.1016/j.jacc.2021.07.042.
Marinescu MA, Löffler AI, Ouellette M, Smith L, Kramer CM, Bourque JM. Coronary microvascular dysfunction, microvascular angina, and treatment strategies. JACC Cardiovasc Imaging. 2015;8(2):210–20. https://doi.org/10.1016/j.jcmg.2014.12.008.
Mathew RC, Bourque JM, Salerno M, Kramer CM. Cardiovascular imaging techniques to assess microvascular dysfunction. JACC Cardiovasc Imaging. 2020;13(7):1577–90. https://doi.org/10.1016/j.jcmg.2019.09.006.
Ford TJ, Stanley B, Sidik N, Good R, Rocchiccioli P, McEntegart M, et al. 1-year outcomes of angina management guided by invasive coronary function testing (CorMicA). JACC Cardiovasc Interv. 2020;13(1):33–45. https://doi.org/10.1016/j.jcin.2019.11.001.
Topol EJ. High-performance medicine: the convergence of human and artificial intelligence. Nat Med. 2019;25(1):44–56. https://doi.org/10.1038/s41591-018-0300-7.
Obermeyer Z, Emanuel EJ. Predicting the future - big data, machine learning, and clinical medicine. N Engl J Med. 2016;375(13):1216–9. https://doi.org/10.1056/NEJMp1606181.
Brisimi TS, Chen R, Mela T, Olshevsky A, Paschalidis IC, Shi W. Federated learning of predictive models from federated electronic health records. Int J Med Inform. 2018;112:59–67. https://doi.org/10.1016/j.ijmedinf.2018.01.007.
Castelvecchi D. Can we open the black box of AI? Nature. 2016;538(7623):20–3. https://doi.org/10.1038/538020a.
Simonyan K, Vedaldi A, Zisserman A. Deep inside convolutional networks: visualising image classification models and saliency maps. 2013. https://doi.org/10.48550/arXiv.1312.6034
Zhou B, Khosla A, Lapedriza A, Oliva A, Torralba A. Learning deep features for discriminative localization. 2016 IEEE Conference on Computer Vision and Pattern Recognition (CVPR)2016. p. 2921–9.
Olah C, Mordvintsev A, Schubert L. Feature Visualization. Distill. https://doi.org/10.23915/distill.00007
McGovern A, Lagerquist R, John Gagne D, Jergensen GE, Elmore KL, Homeyer CR, et al. Making the black box more transparent: understanding the physical implications of machine learning. Bull Am Meteor Soc. 2019;100(11):2175–99. https://doi.org/10.1175/BAMS-D-18-0195.1.
Wagstaff KL, Lee J. Interpretable discovery in large image data sets. 2018. https://doi.org/10.48550/arXiv.1806.08340
Funding
Dr. Unlu receives funding from the National Heart Lung and Blood Institute under award number T32HL007604. Dr. Fahed receives funding from the National Heart Lung and Blood Institute under award numbers K08 HL161448 and R01 HL164629.
Author information
Authors and Affiliations
Contributions
O.U. and A.C.F conceptualized and wrote the main manuscript text and prepared tables and figures.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Conflict of Interest
Dr. Fahed reports being co-founder of Goodpath and received a research grant from Abbott Vascular, unrelated to the subject of this manuscript. Dr. Unlu has nothing to disclose.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Unlu, O., Fahed, A.C. Machine Learning in Invasive and Noninvasive Coronary Angiography. Curr Atheroscler Rep 25, 1025–1033 (2023). https://doi.org/10.1007/s11883-023-01178-z
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11883-023-01178-z