Abstract
Purpose of Review
For more than 20 years there has been considerable interest in the development of pharmacological inhibitors of cholesteryl ester transfer protein (CETP) by virtue of their ability to raise levels of high-density lipoprotein cholesterol. This review endeavors to integrate existing data from prior clinical trials with emerging data to understand whether there is a pathway forward to develop CETP inhibitors to prevent cardiovascular disease.
Recent Findings
Large clinical trials have proved disappointing with successive reports of a failure to reduce cardiovascular events. The one clinical development program that did demonstrate a reduction in cardiovascular risk found adipose tissue accumulation and did not proceed for regulatory approval. More recent observations suggest that less CETP activity may prevent cardiovascular events, but due to lipid lowering rather than raising high-density lipoprotein cholesterol. In addition, treatment with CETP inhibitors appears to have a beneficial impact on glycemic control in the setting of diabetes.
Summary
Advances in the field of CETP inhibition suggest a potentially protective effect on the risk of both cardiovascular disease and diabetes. This has implications for how to best design future clinical development programs and leaves the door open to potentially bring CETP inhibitors to the preventive cardiology clinic.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Consistent findings of cardiovascular benefit with agents that lower levels of low-density lipoprotein cholesterol (LDL-C) support their cornerstone role in treatment guidelines for the prevention of cardiovascular disease [1]. However, many patients continue to experience cardiovascular events, despite the use of LDL-C lowering agents [2]. This is likely to result from the inability to achieve optimal LDL-C lowering in all patients[3] and from the concept that other factors are likely to underscore the residual risk observed in these patients[2]. On the basis of these findings, there continues to be a robust search for new pharmacological targets in order to achieve more effective reduction in cardiovascular risk.
Cholesteryl Ester Transfer Protein
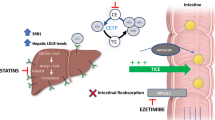
Cholesteryl ester transfer protein (CETP) plays an important role in the regulation of lipoprotein metabolism, facilitating the transfer of esterified cholesterol from high-density lipoproteins (HDL) to LDL and very-low-density lipoprotein (VLDL) in exchange for triglyceride [4]. (Fig. 1) Early cohort studies demonstrated that lower levels of CETP and genetic polymorphisms associated with lower levels of CETP associated with higher levels of HDL cholesterol and lower rates of coronary heart disease [4,5,6,7,8,9,10]. The development of pharmacological inhibitors provided early signs of benefit in animal models. When reductions in CETP were achieved in response to administration with oligosense nucleotide, vaccine or small molecule inhibitors, reductions in atheroma burden were observed in rabbit models [11,12,13,14]. Transition of small molecule CETP inhibitors (Fig. 2) to clinical development demonstrated dose-dependent increases in HDL-C and variable reductions in levels of LDL-C and lipoprotein (a) [Lp(a)] [15, 16]. This experience presented considerable hope that CETP inhibitors might establish themselves as the next generation strategy for reducing cardiovascular risk in the statin-treated patient.
CETP and lipid metabolism. Role of cholesteryl ester transfer protein (CETP) promoting movement of cholesteryl ester (CE) from high-density lipoproteins (HDL) to very low-density lipoproteins (VLDL) and low-density lipoproteins (LDL) in exchange for triglyceride (TG) (upper panel). Impact of CETP inhibition leads to generation of larger HDL particles with associated increases in HDL cholesterol and decreases in levels of LDL cholesterol (lower panel)
Torcetrapib
Torcetrapib was the first CETP inhibitor to reach an advanced phase of clinical development. Early studies demonstrated that torcetrapib produced dose-dependent increases in HDL-C by up to 70%, in addition to lowering LDL-C by 20% and Lp(a) by 11% [15]. However, a large clinical outcomes trial was terminated early due to evidence of an increase in cardiovascular events. The ILLUMINATE trial of more than 15,000 patients with cardiovascular disease was terminated due to demonstration that torcetrapib administration was associated with a 25% increase in cardiovascular events and 58% in all-cause mortality [17]. The excess in death rate with torcetrapib was due to a combination of both cardiovascular and non-cardiovascular (sepsis, cancer) causes. In parallel, three serial vascular imaging studies demonstrated that administration of torcetrapib did not have a favorable impact on progression of either coronary atherosclerosis[18] or carotid intima-medial thickness[19, 20].
The finding that torcetrapib not only failed to reduce cardiovascular risk, but actually produced an increase in adverse clinical events, stimulated considerable debate in the field. Critics of the concept of CETP inhibition argued that impairment of reverse cholesterol transport may have contributed to the findings [21]. However, a number of subsequent findings pointed to potential off target effects of torcetrapib. Plasma isolated from individuals with genetic low CETP activity or treated with torcetrapib demonstrated intact, in fact enhanced, cholesterol efflux capacity, and administration of torcetrapib did not impair reverse cholesterol transport in mouse models [21]. A progressively greater increase in blood pressure was observed with clinical studies of torcetrapib [15, 17]. Post hoc analyses of ILLUMINATE revealed electrolyte abnormalities consistent with activation of the renin angiotensin aldosterone system and preclinical studies demonstrated that torcetrapib promoted secretion of aldosterone and cortisol by the adrenal and upregulated endothelin expression within the aortic wall [17, 22, 23]. The findings of these effects in murine models supported an off target phenomenon, given that these animals do not express CETP. Additional analyses of the clinical trials demonstrated that torcetrapib-treated patients achieving the highest HDL cholesterol levels demonstrated plaque regression and lower cardiovascular event rates [22, 24]. These observations were important as they suggested that if other CETP inhibitors lacked such effects then they still had the potential for development as agents to lower cardiovascular risk.
Dalcetrapib
Dalcetrapib is a relatively modest CETP inhibitor, with evidence of raising HDL cholesterol by up to 30% and no evidence of LDL cholesterol lowering [25]. In the light of the findings of clinical toxicity with torcetrapib, additional studies were performed to establish a lack of deleterious effects on the vasculature in early clinical studies. These trials demonstrated that administration of dalcetrapib had no adverse impact on either endothelial function, measured by flow mediated dilatation, and arterial wall inflammation on positron emission tomography imaging [26, 27]. These findings permitted advancing dalcetrapib to a large clinical outcomes trial. The dal_OUTCOMES trial compared the impact of dalcetrapib and placebo on cardiovascular events in patients with a recent acute coronary syndrome. This study was terminated prematurely due to the finding of clinical futility with no difference in clinical event rates in the two groups [28].
Evacetrapib
Evacetrapib is a more potent CETP inhibitor, with early clinical trials demonstrating increases in HDL cholesterol by more than 120% and decreases in LDL cholesterol by more than 25% and Lp(a) by 30–40% [29, 30]. These early studies also demonstrated no adverse impact on blood pressure or adrenocortical hormone levels, suggesting a lack of torcetrapib like toxicity [29]. The ACCELERATE trial evaluated the impact of evacetrapib on cardiovascular events in high risk patients, but was similarly terminated due to the finding of clinical futility [31]. Subsequent analyses have attempted to understand why this agent did not produce cardiovascular benefit. Given the larger increase in HDL cholesterol levels with evacetrapib than observed with previous CETP inhibitors and contemporary trials of niacin, this suggested that HDL cholesterol raising alone is not a viable strategy for cardiovascular protection. This is supported by observations from genomic studies that fail to demonstrate a relationship between polymorphisms underscoring increases in HDL cholesterol with a reduction in cardiovascular events [32]. Some critics of CETP inhibition have suggested that generation of larger, cholesterol rich HDL particles might impair their functionality [21]. While the increase in HDL cholesterol was accompanied by an increase in levels of apolipoprotein C-III, there is no evidence of a deleterious impact on cholesterol efflux capacity with evacetrapib [16]. Given the difficulty measuring LDL cholesterol with conventional assays in the setting of CETP inhibition, it is likely that real reduction was likely to be less robust, given that apoB levels decreased by only 10–15% with evacetrapib. This is an important point as the median duration of treatment in ACCELERATE was only 26 months, and it is possible that the trial was not long enough to demonstrate clinical benefit with that degree of difference in levels of apoB and LDL cholesterol between the two treatment groups. It was therefore possible that a potent CETP inhibitor might still reduce cardiovascular risk in a sufficiently large enough trial with a long duration of clinical follow-up.
Anacetrapib
Anacetrapib is another potent CETP inhibitor, raising HDL cholesterol by more than 130% and decreasing LDL cholesterol by more than 25% and Lp(a) by 35% [33]. Additional studies have demonstrated similarly favorable reductions in LDL cholesterol in patients with familial hypercholesterolemia [34]. A large safety study demonstrated no adverse effect of anacetrapib administration on blood pressure or adrenocortical stimulation, with a subsequent Bayesian analysis revealing a 94% confidence of excluding a 25% increase in cardiovascular event as observed with torcetrapib [33]. This study of more 1600 patients demonstrated less cardiovascular events, largely due to coronary revascularization, in patients treated with anacetrapib [33]. This paved the way for a large clinical outcomes trial (REVEAL) of more than 30,000 patients at high cardiovascular risk. This study, of mean treatment duration of 4.1 years, demonstrated a statistically significant 9% reduction in cardiovascular events with anacetrapib, with evidence that the event curves did not begin to separate for 2 years [35]. Longer term follow-up of patients in the REVEAL study demonstrated ongoing event curve separation with evidence of a greater clinical benefit of anacetrapib [36•]. Subsequent analyses demonstrated a direct association between reductions in non-HDL cholesterol and cardiovascular risk, suggesting that the potential benefit of CETP inhibition might be derived exclusively from reductions in atherogenic lipoproteins and not raising HDL cholesterol [35]. While the same considerations exist for the reported degree of LDL cholesterol lowering with anacetrapib as applied to evacetrapib, REVEAL suggests that patients needed to be treated for a greater duration to produce the cardiovascular benefit that a modest reduction in apoB and LDL cholesterol should promote. However, the finding of prolonged lipid effects of anacetrapib, after cessation of administration, led to the demonstration of adipose tissue accumulation [37]. As a result of these findings, anacetrapib did not progress to regulatory approval and is not used in clinical practice.
Impact of CETP Inhibition on Risk of Developing Diabetes
While the large clinical outcomes trials of CETP inhibitors have proven to be disappointing, a positive finding of each of these trials has been the finding of a potentially favorable impact of CETP inhibitors on diabetes. ILLUMINATE demonstrated that torcetrapib-treated patients had lower levels of glucose, insulin, glycated hemoglobin and homeostasis model assessment of insulin resistance compared with placebo in patients with and without diabetes at baseline [38]. ACCELERATE demonstrated lower levels of glycated hemoglobin with evacetrapib treatment in patients with diabetes[39], while REVEAL demonstrated that anacetrapib-treated patients were less likely to be diagnosed with diabetes during the study[40]. A formal analysis of the dal_OUTCOMES study, of patients without established diabetes at baseline, demonstrated that dalcetrapib treatment associated with a lower rate of progression from normoglycemia to prediabetes, new diagnoses of diabetes in patients with prediabetes at baseline and a greater rate of regression of diabetes during the trial. It was estimated that treatment of 40 patients with dalcetrapib for 3 years would be required to prevent one new case of diabetes [41]. A meta-analysis of these trials demonstrated that treatment with a CETP inhibitor is associated with a 16% reduction in the risk of being diagnosed with diabetes during the relatively short follow-up of these studies [42•]. Mendelian randomization suggests a causal role of CETP inhibition in reducing the risk of diabetes, with HDL being the likely mediator [43].
The potential mechanism underscoring the association between CETP inhibitors and a lower risk of diabetes in the clinical trials remains uncertain. Given a similar degree of protection with all CETP inhibitors and no LDL cholesterol effect of dalcetrapib, it is unlikely to relate to reductions in atherogenic lipoproteins. It may, however, reflect the impact of CETP inhibitors on HDL, although their variable effects on HDL cholesterol suggest this relationship would not be linear. Favorable effects of HDL on pancreatic beta-cell apoptosis, inflammation and functionality appear to result in greater insulin secretion[44,45,46], while more peripherally HDL improves skeletal muscle insulin sensitivity and increases insulin dependent glucose uptake[45,46,47]. It is also possible that CETP inhibitors may exert a direct effect on pancreatic beta-cells. Further studies are required to understand this relationship, but it also points to potential clinical benefits of CETP inhibitors which require further exploration.
Insights from Genomic Studies of CETP
Additional investigations using genomic data have provided insights that may identify alternative approaches to use of these agents. While the dal_OUTCOMES trial was terminated due to clinical futility, a subsequent pharmacogenomic analysis suggested that patients harboring the AA polymorphism at rs1967309 of the adenylate cyclase 9 (ADCY9) gene on chromosome demonstrated less cardiovascular events with dalcetrapib compared with placebo [48]. Mechanistic studies demonstrated that the presence of the AA polymorphism associated with greater increases in cholesterol efflux capacity and an attenuated increase in hsCRP with dalcetrapib [49]. These findings led to the conduct of a large, prospective clinical trial comparing the impact of dalcetrapib and placebo on cardiovascular events in high risk patients identified at baseline to possess the AA polymorphism [50]. This finding was not replicated upon analysis of the ACCELERATE[51] and REVEAL[52] studies, suggesting that if it were to prove to be validated it is more likely to reflect a dalcetrapib specific effect.
An additional contribution made by genomic investigation of CETP has been provided by Mendelian randomization analysis. Investigation of genomic data from large cohorts has established that polymorphisms that associate with low CETP also associate with lower rates of cardiovascular disease [53••]. This relationship appears to be driven by lower levels of apoB, suggesting that it lowers atherogenic lipids and does not raise HDL cholesterol that may underscore any potential for CETP inhibition to lower cardiovascular risk [53••]. These studies have also established the relationship to be stronger in the presence of greater amounts of HMG CoA reductase[53••], suggesting potentially greater clinical benefit in patients treated with lower doses of statins. The findings from these genomic analyses do provide a pathway forward for ongoing development of CETP inhibitors. These programs would need to involve agents that were effective in lowering apoB and LDL cholesterol, were well tolerated by patients and were evaluated in clinical outcomes trials that were designed to test the impact of lipid lowering and not HDL raising. Obicetrapib is a potent CETP inhibitor with early evidence of lowering LDL cholesterol by 45.3% as monotherapy and by more than 60% when administered in combination with statin therapy [54•]. Additional analyses demonstrated HDL cholesterol raising by 124.3% and commensurate increases in cholesterol efflux capacity [54•]. More recent studies performed in patients treated with background high-intensity statin therapy demonstrated LDL cholesterol lowering by 51%, with no difference in effect when using different analytical assays (preparative ultracentrifugation, Friedewald) [55]. These findings provide a pathway for a cardiovascular outcomes trial of obicetrapib in addition to statin therapy in high cardiovascular risk patients with suboptimal control of LDL cholesterol.
More recent genetic analyses using a CETP allele score suggested a potential increase in the rate of age-related macular degeneration accompanying the cardiovascular protection with low CETP [56]. This appeared to associate with rising levels of HDL cholesterol. However, considerable ongoing work will be required to understand whether this finding proves to be clinically correct. A number of concerns regarding this analysis have been raised including potentially limited biological plausibility and the inability of large HDL particles with CETP inhibition to penetrate Bruch’s membrane and the lack of certainty whether HDL cholesterol represents a viable intermediate factor on a causal pathway to macular degeneration [57]. Any ongoing clinical trial will need to evaluate safety and tolerability in addition to cardiovascular efficacy.
Conclusions
For more than 20 years there has been interest in targeting CETP as a potential novel approach to the prevention of cardiovascular disease. However, early optimism has been challenged by disappointing results of large clinical trials (Table 1). Subsequent analyses of these studies and genomic cohorts have provided important information with regard to potential clinical benefits and tolerability of CETP inhibitors. The ability to lower LDL cholesterol and have potentially protective effects on the risk of diabetes both demonstrate an ongoing hope that CETP inhibitors may prove to be useful therapeutics in the clinic. However, the results of larger clinical trials will ultimately be required to provide the evidence base to translate the hope of CETP inhibition to the clinic.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Baigent C, Blackwell L, Emberson J, Holland LE, Reith C, Bhala N, et al. Efficacy and safety of more intensive lowering of LDL cholesterol: a meta-analysis of data from 170,000 participants in 26 randomised trials. Lancet. 2010;376(9753):1670–81. https://doi.org/10.1016/S0140-6736(10)61350-5.
Libby P. The forgotten majority: unfinished business in cardiovascular risk reduction. J Am Coll Cardiol. 2005;46(7):1225–8.
Ray KK, Molemans B, Schoonen WM, Giovas P, Bray S, Kiru G, et al. EU-wide cross-sectional observational study of lipid-modifying therapy use in secondary and primary care: the DA VINCI study. Eur J Prev Cardiol. 2021;28(11):1279–89. https://doi.org/10.1093/eurjpc/zwaa047.
Barter PJ, Chapman MJ, Hennekens CH, Rader DJ, Tall AR. Cholesteryl ester transfer protein. A novel target for raising HDL and inhibiting atherosclerosis. Arterioscler Thromb Vasc Biol. 2003;23:160–7.
Vasan RS, Pencina MJ, Robins SJ, Zachariah JP, Kaur G, D’Agostino RB, et al. Association of circulating cholesteryl ester transfer protein activity with incidence of cardiovascular disease in the community. Circulation. 2009;120(24):2414–20. https://doi.org/10.1161/CIRCULATIONAHA.109.872705.
Brown ML, Inazu A, Hesler CB, Agellon LB, Mann C, Whitlock ME, et al. Molecular basis of lipid transfer protein deficiency in a family with increased high-density lipoproteins. Nature. 1989;342(6248):448–51.
Inazu A, Brown ML, Hesler CB, Agellon LB, Koizumi J, Takata K, et al. Increased high-density lipoprotein levels caused by a common cholesteryl-ester transfer protein gene mutation. N Engl J Med. 1990;323(18):1234–8.
Ritsch A, Scharnagl H, Eller P, Tancevski I, Duwensee K, Demetz E, et al. Cholesteryl ester transfer protein and mortality in patients undergoing coronary angiography: the Ludwigshafen Risk and Cardiovascular Health study. Circulation. 2010;121(3):366–74. https://doi.org/10.1161/CIRCULATIONAHA.109.875013.
Thompson A, Di Angelantonio E, Sarwar N, Erqou S, Saleheen D, Dullaart RP, et al. Association of cholesteryl ester transfer protein genotypes with CETP mass and activity, lipid levels, and coronary risk. JAMA. 2008;299(23):2777–88.
Johannsen TH, Frikke-Schmidt R, Schou J, Nordestgaard BG, Tybjaerg-Hansen A. Genetic inhibition of CETP, ischemic vascular disease and mortality, and possible adverse effects. J Am Coll Cardiol. 2012;60(20):2041–8. https://doi.org/10.1016/j.jacc.2012.07.045.
Rittershaus CW, Miller DP, Thomas LJ, Picard MD, Honan CM, Emmett CD, et al. Vaccine-induced antibodies inhibit CETP activity in vivo and reduce aortic lesions in a rabbit model of atherosclerosis. Arterioscler Thromb Vasc Biol. 2000;20(9):2106–12.
Sugano M, Makino N, Sawada S, Otsuka S, Watanabe M, Okamoto H, et al. Effect of antisense oligonucleotides against cholesteryl ester transfer protein on the development of atherosclerosis in cholesterol-fed rabbits. J Biol Chem. 1998;273(9):5033–6.
Okamoto H, Yonemori F, Wakitani K, Minowa T, Maeda K, Shinkai H. A cholesteryl ester transfer protein inhibitor attenuates atherosclerosis in rabbits. Nature. 2000;406(6792):203–7.
Morehouse LA, Sugarman ED, Bourassa PA, Sand TM, Zimetti F, Gao F, et al. Inhibition of CETP activity by torcetrapib reduces susceptibility to diet-induced atherosclerosis in New Zealand White rabbits. J Lipid Res. 2007;48(6):1263–72. https://doi.org/10.1194/jlr.M600332-JLR200.
Brousseau ME, Schaefer EJ, Wolfe ML, Bloedon LT, Digenio AG, Clark RW, et al. Effects of an inhibitor of cholesteryl ester transfer protein on HDL cholesterol. N Engl J Med. 2004;350(15):1505–15.
Nicholls SJ, Ray KK, Ballantyne CM, Beacham LA, Miller DL, Ruotolo G, et al. Comparative effects of cholesteryl ester transfer protein inhibition, statin or ezetimibe on lipid factors: the ACCENTUATE trial. Atherosclerosis. 2017;261:12–8. https://doi.org/10.1016/j.atherosclerosis.2017.04.008.
Barter PJ, Caulfield M, Eriksson M, Grundy SM, Kastelein JJ, Komajda M, et al. Effects of torcetrapib in patients at high risk for coronary events. N Engl J Med. 2007;357(21):2109–22.
Nissen SE, Tardif JC, Nicholls SJ, Revkin JH, Shear CL, Duggan WT, et al. Effect of torcetrapib on the progression of coronary atherosclerosis. N Engl J Med. 2007;356(13):1304–16.
Bots ML, Visseren FL, Evans GW, Riley WA, Revkin JH, Tegeler CH, et al. Torcetrapib and carotid intima-media thickness in mixed dyslipidaemia (RADIANCE 2 study): a randomised, double-blind trial. Lancet. 2007;370(9582):153–60.
Kastelein JJ, van Leuven SI, Burgess L, Evans GW, Kuivenhoven JA, Barter PJ, et al. Effect of torcetrapib on carotid atherosclerosis in familial hypercholesterolemia. N Engl J Med. 2007;356(16):1620–30.
Tall AR, Yvan-Charvet L, Wang N. The failure of torcetrapib: was it the molecule or the mechanism? Arterioscler Thromb Vasc Biol. 2007;27(2):257–60.
Barter P. Lessons learned from the Investigation of Lipid Level Management to Understand its Impact in Atherosclerotic Events (ILLUMINATE) trial. Am J Cardiol. 2009;104(10 Suppl):10E-E15. https://doi.org/10.1016/j.amjcard.2009.09.014.
Vergeer M, Stroes ES. The pharmacology and off-target effects of some cholesterol ester transfer protein inhibitors. Am J Cardiol. 2009;104(10 Suppl):32E-E38. https://doi.org/10.1016/j.amjcard.2009.09.017.
Nicholls SJ, Tuzcu EM, Brennan DM, Tardif JC, Nissen SE. Cholesteryl ester transfer protein inhibition, high-density lipoprotein raising, and progression of coronary atherosclerosis: insights from ILLUSTRATE (Investigation of Lipid Level Management Using Coronary Ultrasound to Assess Reduction of Atherosclerosis by CETP Inhibition and HDL Elevation). Circulation. 2008;118(24):2506–14.
Ray KK, Ditmarsch M, Kallend D, Niesor EJ, Suchankova G, Upmanyu R, et al. The effect of cholesteryl ester transfer protein inhibition on lipids, lipoproteins, and markers of HDL function after an acute coronary syndrome: the dal-ACUTE randomized trial. Eur Heart J. 2014;35(27):1792–800. https://doi.org/10.1093/eurheartj/ehu105.
Luscher TF, Taddei S, Kaski JC, Jukema JW, Kallend D, Munzel T, et al. Vascular effects and safety of dalcetrapib in patients with or at risk of coronary heart disease: the dal-VESSEL randomized clinical trial. Eur Heart J. 2012;33(7):857–65. https://doi.org/10.1093/eurheartj/ehs019.
Fayad ZA, Mani V, Woodward M, Kallend D, Abt M, Burgess T, et al. Safety and efficacy of dalcetrapib on atherosclerotic disease using novel non-invasive multimodality imaging (dal-PLAQUE): a randomised clinical trial. Lancet. 2011;378(9802):1547–59. https://doi.org/10.1016/S0140-6736(11)61383-4.
Schwartz GG, Olsson AG, Abt M, Ballantyne CM, Barter PJ, Brumm J, et al. Effects of dalcetrapib in patients with a recent acute coronary syndrome. N Engl J Med. 2012;367(22):2089–99. https://doi.org/10.1056/NEJMoa1206797.
Nicholls SJ, Brewer HB, Kastelein JJ, Krueger KA, Wang MD, Shao M, et al. Effects of the CETP inhibitor evacetrapib administered as monotherapy or in combination with statins on HDL and LDL cholesterol: a randomized controlled trial. JAMA. 2011;306(19):2099–109. https://doi.org/10.1001/jama.2011.1649.
Nicholls SJ, Ruotolo G, Brewer HB, Kane JP, Wang MD, Krueger KA, et al. Cholesterol efflux capacity and pre-beta-1 HDL concentrations are increased in dyslipidemic patients treated with evacetrapib. J Am Coll Cardiol. 2015;66(20):2201–10. https://doi.org/10.1016/j.jacc.2015.09.013.
Nicholls SJ, Lincoff AM, Barter PJ, Brewer HB, Fox KA, Gibson CM, et al. Assessment of the clinical effects of cholesteryl ester transfer protein inhibition with evacetrapib in patients at high-risk for vascular outcomes: rationale and design of the ACCELERATE trial. Am Heart J. 2015;170(6):1061–9. https://doi.org/10.1016/j.ahj.2015.09.007.
Voight BF, Peloso GM, Orho-Melander M, Frikke-Schmidt R, Barbalic M, Jensen MK, et al. Plasma HDL cholesterol and risk of myocardial infarction: a mendelian randomisation study. Lancet. 2012;380(9841):572–80. https://doi.org/10.1016/S0140-6736(12)60312-2.
Cannon CP, Shah S, Dansky HM, Davidson M, Brinton EA, Gotto AM, et al. Safety of anacetrapib in patients with or at high risk for coronary heart disease. N Engl J Med. 2010;363(25):2406–15. https://doi.org/10.1056/NEJMoa1009744.
Kastelein JJ, Besseling J, Shah S, Bergeron J, Langslet G, Hovingh GK, et al. Anacetrapib as lipid-modifying therapy in patients with heterozygous familial hypercholesterolaemia (REALIZE): a randomised, double-blind, placebo-controlled, phase 3 study. Lancet. 2015;385(9983):2153–61. https://doi.org/10.1016/S0140-6736(14)62115-2.
Gotto AM Jr, Cannon CP, Li XS, Vaidya S, Kher U, Brinton EA, et al. Evaluation of lipids, drug concentration, and safety parameters following cessation of treatment with the cholesteryl ester transfer protein inhibitor anacetrapib in patients with or at high risk for coronary heart disease. Am J Cardiol. 2014;113(1):76–83. https://doi.org/10.1016/j.amjcard.2013.08.041.
• Group HTRC, Writing C, Sammons E, Hopewell JC, Chen F, Stevens W et al. Long-term safety and efficacy of anacetrapib in patients with atherosclerotic vascular disease. Eur Heart J. 2022;43(14):1416-24.https://doi.org/10.1093/eurheartj/ehab863.longer term cardiovascular benefits of anacetrapib.
Krishna R, Gheyas F, Liu Y, Hagen DR, Walker B, Chawla A, et al. Chronic administration of anacetrapib is associated with accumulation in adipose and slow elimination. Clin Pharmacol Ther. 2017;102(5):832–40. https://doi.org/10.1002/cpt.700.
Barter PJ, Rye KA, Tardif JC, Waters DD, Boekholdt SM, Breazna A, et al. Effect of torcetrapib on glucose, insulin, and hemoglobin A1c in subjects in the Investigation of Lipid Level Management to Understand its Impact in Atherosclerotic Events (ILLUMINATE) trial. Circulation. 2011;124(5):555–62. https://doi.org/10.1161/CIRCULATIONAHA.111.018259.
Menon V, Kumar A, Patel DR, St John J, Riesmeyer J, Weerakkody G et al. Effect of CETP inhibition with evacetrapib in patients with diabetes mellitus enrolled in the ACCELERATE trial. BMJ Open Diabetes Res Care. 2020;8(1). https://doi.org/10.1136/bmjdrc-2019-000943.
https://www.revealtrial.org/REVEAL_AHA_DM_2017-11-13.pdf. 2017. https://www.revealtrial.org/REVEAL_AHA_DM_2017-11-13.pdf. Accessed December 30, 2020 2020.
Schwartz GG, Leiter LA, Ballantyne CM, Barter PJ, Black DM, Kallend D, et al. Dalcetrapib reduces risk of new-onset diabetes in patients with coronary heart disease. Diabetes Care. 2020;43(5):1077–84. https://doi.org/10.2337/dc19-2204.
• Dangas K, Navar AM, Kastelein JJP. The effect of CETP inhibitors on new-onset diabetes: a systematic review and meta-analysis. Eur Heart J Cardiovasc Pharmacother. 2022.https://doi.org/10.1093/ehjcvp/pvac025. meta-analysis demonstrating favorable effect of CETP inhibitors on diabetes.
Schmidt AF, Hunt NB, Gordillo-Maranon M, Charoen P, Drenos F, Kivimaki M, et al. Cholesteryl ester transfer protein (CETP) as a drug target for cardiovascular disease. Nat Commun. 2021;12(1):5640. https://doi.org/10.1038/s41467-021-25703-3.
Fryirs MA, Barter PJ, Appavoo M, Tuch BE, Tabet F, Heather AK, et al. Effects of high-density lipoproteins on pancreatic beta-cell insulin secretion. Arterioscler Thromb Vasc Biol. 2010;30(8):1642–8. https://doi.org/10.1161/ATVBAHA.110.207373.
Siebel AL, Heywood SE, Kingwell BA. HDL and glucose metabolism: current evidence and therapeutic potential. Front Pharmacol. 2015;6:258. https://doi.org/10.3389/fphar.2015.00258.
Drew BG, Rye KA, Duffy SJ, Barter P, Kingwell BA. The emerging role of HDL in glucose metabolism. Nat Rev Endocrinol. 2012;8(4):237–45. https://doi.org/10.1038/nrendo.2011.235.
Vaisar T, Pennathur S, Green PS, Gharib SA, Hoofnagle AN, Cheung MC, et al. Shotgun proteomics implicates protease inhibition and complement activation in the antiinflammatory properties of HDL. J Clin Invest. 2007;117(3):746–56.
Tardif JC, Rheaume E, Lemieux Perreault LP, Gregoire JC, Feroz Zada Y, Asselin G, et al. Pharmacogenomic determinants of the cardiovascular effects of dalcetrapib. Circ Cardiovasc Genet. 2015. https://doi.org/10.1161/CIRCGENETICS.114.000663.
Tardif JC, Rhainds D, Brodeur M, Feroz Zada Y, Fouodjio R, Provost S, et al. Genotype-dependent effects of dalcetrapib on cholesterol efflux and inflammation: concordance with clinical outcomes. Circ Cardiovasc Genet. 2016. https://doi.org/10.1161/CIRCGENETICS.116.001405.
Tardif JC, Dube MP, Pfeffer MA, Waters DD, Koenig W, Maggioni AP, et al. Study design of Dal-GenE, a pharmacogenetic trial targeting reduction of cardiovascular events with dalcetrapib. Am Heart J. 2020;222:157–65. https://doi.org/10.1016/j.ahj.2020.01.007.
Nissen SE, Pillai SG, Nicholls SJ, Wolski K, Riesmeyer JS, Weerakkody GJ, et al. ADCY9 genetic variants and cardiovascular outcomes with evacetrapib in patients with high-risk vascular disease: a nested case-control study. JAMA Cardiol. 2018;3(5):401–8. https://doi.org/10.1001/jamacardio.2018.0569.
Hopewell JC, Ibrahim M, Hill M, Shaw PM, Braunwald E, Blaustein RO, et al. Impact of ADCY9 genotype on response to anacetrapib. Circulation. 2019. https://doi.org/10.1161/CIRCULATIONAHA.119.041546.
•• Ference BA, Kastelein JJP, Ginsberg HN, Chapman MJ, Nicholls SJ, Ray KK et al. Association of genetic variants related to CETP inhibitors and statins with lipoprotein levels and cardiovascular risk. JAMA. 2017;318(10):947-56.https://doi.org/10.1001/jama.2017.11467Mendealian randomization demonstrating cardioprotection with low CETP associated with lower apoB levels.
• Hovingh GK, Kastelein JJ, van Deventer SJ, Round P, Ford J, Saleheen D et al. Cholesterol ester transfer protein inhibition by TA-8995 in patients with mild dyslipidaemia (TULIP): a randomised, double-blind, placebo-controlled phase 2 trial. Lancet. 2015;386(9992):452-60.https://doi.org/10.1016/S0140-6736(15)60158-1. early lipid effects of obicetrapib.
https://pace-cme.org/2021/11/29/dose-dependent-reduction-of-ldl-c-levels-by-cetp-inhibitor/. 2021. https://pace-cme.org/2021/11/29/dose-dependent-reduction-of-ldl-c-levels-by-cetp-inhibitor/. Accessed June 26 2022.
Nordestgaard LT, Christoffersen M, Lauridsen BK, Afzal S, Nordestgaard BG, Frikke-Schmidt R, et al. Long-term benefits and harms associated with genetic cholesteryl ester transfer protein deficiency in the general population. JAMA Cardiol. 2022;7(1):55–64. https://doi.org/10.1001/jamacardio.2021.3728.
Tall AR, Rader DJ, Kastelein JJP. Macular degeneration and CETP inhibition. JAMA Cardiol. 2022. https://doi.org/10.1001/jamacardio.2022.1276.
https://www.medkoo.com/products/10671. Accessed August 2 2022.
Liu S, Mistry A, Reynolds JM, Lloyd DB, Griffor MC, Perry DA, et al. Crystal structures of cholesteryl ester transfer protein in complex with inhibitors. J Biol Chem. 2012;287(44):37321–9. https://doi.org/10.1074/jbc.M112.380063.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
SJN has received research support from AstraZeneca, Amgen, Anthera, CSL Behring, Cerenis, The Medicines Company, Eli Lilly, Esperion, Resverlogix, New Amsterdam Pharma, Novartis, InfraReDx, Roche, Sanofi-Regeneron and LipoScience. He also reports being a consultant for Amgen, Akcea, Anthera, AstraZeneca, Boehringer Ingelheim, CSL Behring, Eli Lilly, Esperion, Kowa, Omthera, Merck, New Amsterdam Pharma, Takeda, Resverlogix, Pfizer, Sanofi-Regeneron, Vaxxinity and Novo Nordisk. AJN reports grants and personal fees from Amgen and Boehringer Ingelheim, and personal fees from Bayer and Sanofi.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Topical Collection on Nonstatin Drugs
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Nicholls, S.J., Nelson, A.J. CETP Inhibitors: Should We Continue to Pursue This Pathway?. Curr Atheroscler Rep 24, 915–923 (2022). https://doi.org/10.1007/s11883-022-01070-2
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11883-022-01070-2