Abstract
Background
Metabolic/bariatric surgery is a highly effective treatment for obesity and metabolic diseases. Serum glucagon, bile acids, and FGF-19 are key effectors of various metabolic processes and may play central roles in bariatric surgical outcomes. It is unclear whether these factors behave similarly after Roux-en-Y gastric bypass (RYGB) vs vertical sleeve gastrectomy (VSG).
Methods
Serum glucagon, bile acids (cholic acid [CA], chenodeoxycholic acid [CDCA], deoxycholic acid [DCA]), and FGF-19 were analyzed in samples of fasting blood collected before bariatric surgery, on postoperative days 2 and 10, and at 3- and 6-month follow-up.
Results
From September 2016 to July 2017, patients with obesity underwent RYGB or VSG; 42 patients (RYGB n = 21; VSG n = 21) were included in the analysis. In the RYGB group, glucagon, CA, and CDCA increased continuously after surgery (p = 0.0003, p = 0.0009, p = 0.0001, respectively); after an initial decrease (p = 0.04), DCA increased significantly (p = 0.0386). Serum FGF-19 was unchanged. In the VSG group, glucagon increased on day 2 (p = 0.0080), but decreased over the 6-month study course (p = 0.0025). Primary BAs (CA and CDCA) decreased immediately after surgery (p = 0.0016, p = 0.0091) and then rose (p = 0.0350, p = 0.0350); DCA followed the curve of the primary BAs until it fell off at 6 months (p = 0.0005). VSG group serum FGF-19 trended upward.
Conclusion
RYGB and VSG involve different surgical techniques and final anatomical configurations. Between postoperative day 2 and 6-month follow-up, RYGB and VSG resulted in divergent patterns of change in serum glucagon, bile acids, and FGF-19.
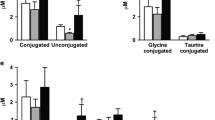
Graphical abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Metabolic/bariatric surgery has been proven to be the most effective and durable therapy for obesity [1]: surgical treatment can achieve permanent weight loss and thus sustained improvement in comorbidities [2, 3]. For example, the metabolic improvement regarding glucose homeostasis and insulin sensitivity can be observed within days after surgery, before substantial weight loss occurs [4, 5].
Hormonal or other metabolic mediators are likely responsible for these early effects. The “hindgut theory” postulates that the rapid transit of nutrients to the distal intestine causes intense stimulation of intestinal L-cells and GLP-1 secretion [6, 7]. Previous studies have described a marked increase in postprandial GLP-1 levels immediately following RYGB that is sustained [8,9,10] and that coincides with a significant increase in bile acids (BAs) [11]. Bile acids are synthesized primarily in the liver through the classic and alternate pathways. The classic pathway is responsible for 75% of BA pool size and is regulated by the rate-limiting enzyme, cholesterol 7α-hydroxylase (CYP7A1) [12, 13]. Cholic acid (CA) and chenodeoxycholic acid (CDCA) are the most abundant primary BAs and are secreted into the gastrointestinal tract for digestion and absorption of dietary fats. The majority of the BAs are reabsorbed by the enterohepatic circulation in the distal intestine [14]. BAs that escape the enterohepatic circulation are transformed into secondary BAs (e.g., CA is converted to deoxycholic acid [DCA] by gut bacteria) [15]. Fibroblast growth factor 19 (FGF-19) inhibits the expression of CYP7A1 in hepatocytes and, thus, in BA synthesis. In addition, the nuclear BA receptor FXR regulates the expression of FGF-19 in the ileum [16]. Increased levels of BA after RYGB have been shown to affect FGF-19 concentrations, reduce insulin resistance, initiate better glucose metabolism control, and influence weight loss [17].
Another key hormone suspected to be affected by RYGB is glucagon, since hyperglucagonemia is etiologically related to hyperglycemia in patients with diabetes [18, 19]. However, the findings reported in the literature on postoperative glucagon changes are inconsistent, depending on the assays used [20,21,22].
Results for RYGB and VSG weight loss, comorbidity resolution, and metabolic improvement are comparable and cannot be explained by restriction alone after surgery. In rodents, after VSG, changes have been detected in circulating BA concentrations [23,24,25]. Also in VSG, another important mechanism seems to be modulation of the abundance and composition of gut microbial communities, with direct or indirect interaction with BAs [26]. Almost all rodent studies unanimously describe an increase of total BAs following VSG that is congruent with the results after RYGB [27, 28]. The limited data in humans remain highly contradictory and often show no significant changes in BA concentrations after VSG [29,30,31,32,33].
Most studies have confirmed that BA concentrations are increased following RYGB, while the effect of VSG on bile acids was inconsistent: Some studies showed a similar tendency [30, 33], while others detected no change [31, 34]. At 6-month follow-up after both RYGB [35, 36] and VSG [37], FGF-19 levels have been reported to increase.
To gain deeper insight into the roles of glucagon, BAs, and FGF-19 in obesity, this study aimed to evaluate their postoperative course in serum after RYGB and VSG.
Methods
Study Design
The study was designed as a prospective, single-center analysis comparing the effects of two bariatric procedures (RYGB, VSG) on the modulation of molecules centrally involved in weight and metabolism. The study was approved by the university faculty ethics committee and institutional review board (#EK 416092015) and was conducted at a university hospital.
Inclusion
Participants were patients with poorly managed obesity (body mass index [BMI] ≥ 35 kg/m2 with one or more comorbidities [e.g., diabetes, arterial hypertension, sleep apnea] or BMI ≥ 40 kg/m2) who presented for bariatric surgery in the outpatient clinic. Patients were completely informed about the procedure options and the study and engaged in discussion with the surgeon.
Generally, RYGB was recommended if gastroesophageal reflux disease (GERD) was diagnosed previously. VSG was recommended particularly to patients with a BMI > 50 kg/m2 or young female patients who desired to have children in the future. After consultation with the surgeon and depending on the patients’ wishes, RYGB or VSG was elected. Participation for all patients was predicated on their written informed consent.
Surgical Technique
The RYGB technique included a small gastric pouch of 30 ml with a 30-mm pouch-jejunostomy. A 150-cm antecolic Roux limb and an exclusion of 60 cm of the biliopancreatic limb were measured. The VSG procedure was performed along the length of a 42-F bougie from the angle of His to approximately 4–5 cm from the pylorus.
Fasting blood samples were collected before surgery, on days 2 and 10 after the surgery, as well as at 3 to 6 months postoperatively. Perioperative care was the same for all patients in the study regardless of operative group.
Assays
Serum glucagon, BAs, and FGF-19 were assayed. In the normal course of our center’s bariatric surgery workup, we do not measure BA concentrations; BA measurements taken were especially performed for this prospective study. Every blood sample was frozen and later underwent enzyme-linked immunosorbent assay (ELISA) and chromatography for this trial.
Glucagon levels were assayed using the Quantikine Glucagon Immunoassay (R&D Systems Europe Ltd, Abingdon, UK). CA, DCA, and CDCA were analyzed using high-performance liquid chromatography (JASCO, Portland, OR, USA) and tandem mass spectrometry (Applied Biosystems, Cheshire, UK). An ELISA Quantikine Human FGF-19 Immunoassay (R&D Systems Europe Ltd, Abingdon, UK) was used to assess FGF-19.
Statistical Analysis
All statistical calculations were performed with the SAS statistical program, release 9.4 (SAS Institute Inc., Cary, NC, USA). For quantitative variables, mean and standard deviations were assessed. For qualitative factors, absolute and relative frequencies were given. For comparing the two treatment groups regarding baseline values, Fisher’s exact test or the two-sample t test was applied, as appropriate. In order to investigate if there are changes over time regarding glucagon, BAs, and FGF-19, a Friedman rank sum test was performed. In the case of a significant test result, pairwise comparisons were performed using Wilcoxon tests for paired samples. In general, the result of a statistical test was considered statistically significant for a p value < 0.05.
Results
The study was conducted at our university hospital between September 2016 and July 2017. All operations were performed laparoscopically by two of the co-authors (MO, GV).
Demographics
Patients who presented for bariatric surgery who wished to participate in the study were included. Fifty-seven patients were enrolled, with an average age of 40 years old. Postoperatively, 15 patients were excluded for incomplete blood tests or test failures. The final analysis included 21 patients who underwent RYGB and 21 patients, VSG.
Baseline characteristics are shown in Table 1. Average preoperative weight and BMI were lower in the RYGB group (124.1 ± 16.0 kg; 46.4 ± 4.7 kg/m2) than in the VSG group (160.0 ± 26.0 kg; 56.3 ± 7.7 kg/m2). Diabetes mellitus, dyslipidemia, and their treatments did not differ between groups. The weight loss was more pronounced in the RYGB group (p = 0.014). However, no correlation was found between the bile acids and weight loss. Serious complication (> grade 2 in the Clavien-Dindo classification) did not occur in all patients.
Glucagon
In the RYGB group, glucagon increased continuously and significantly after surgery: Median increasing percentages were 73% (p < 0.0001), 98% (p = 0.0004), and 60% (p = 0.0003) after 2 days, 10 days, and 6 months relative to preoperative values (Fig. 1). In the VSG group, glucagon increased by 52% from preoperative status by the second day after surgery (p = 0.0080). However, at 6 months, glucagon had decreased by 47% compared to the second postoperative day (p = 0.0025).
Bile Acids
CA
After RYGB, serum CA increased continuously (Table 2). The difference became significant between 3 and 6 months (4.3-fold compared to preoperative values, p = 0.0132, and 2-fold compared to postoperative day 2, p = 0.0009). In the VSG group, CA decreased by 54% shortly after surgery (p = 0.0016 on day 2) and increased by 49% between day 2 and day 10 (p = 0.0350) (Fig. 2).
Serum cholic acid (CA) in Roux-en-Y gastric bypass (RYGB) group and in vertical sleeve gastrectomy (VSG) group. Pre = preoperatively, 2D post = 2 days postoperatively, 10D post = 10 days postoperatively, 3–6 Mon post = 3–6 months postoperatively. Significant p values between time points are indicated
DCA
In both groups, the level of serum DCA dropped until the day 2 (p = 0.0400 RYGB, p = 0.0005 VSG) and rose again afterwards (Table 2). The difference became significant after 6 months in the RYGB group (p = 0.0009, p < 0.0001, and p = 0.0386 compared to preoperative values and those on day 2 and 10, respectively). In the VSG group, DCA increased significantly from day 2 to day 10 (p = 0.0001) and then decreased through the 6-month study course (p = 0.0005, compared to day 2) (Fig. 3).
Serum deoxycholic acid (DCA) in Roux-en-Y gastric bypass (RYGB) group and in vertical sleeve gastrectomy (VSG) group. Pre = preoperatively, 2D post = 2 days postoperatively, 10D post = 10 days postoperatively, 3–6 Mon post = 3–6 months postoperatively. Significant p values between time points are indicated
CDCA
A continuous increase of CDCA levels was observed in the RYGB group, reaching its peak after 6 months (Table 2). This was a 4.3-fold increase relative to preoperative CDCA levels (p =0 .0030), a 2.8-fold increase compared to day 2 (p = 0.0001), and a 1.2-fold increase compared to day 10 (p = 0.0317). In the VSG group, the CDCA level dropped immediately after surgery (p = 0.0091) and then rose until it reached its original level at 6 months (p = 0.0425 on day 10, and p = 0.0350 at 6 months compared to day 2) (Fig. 4).
Serum chenodeoxycholic acid (CDCA) in Roux-en-Y gastric bypass (RYGB) group and in vertical sleeve gastrectomy (VSG) group. Pre = preoperatively, 2D post = 2 days postoperatively, 10D post = 10 days postoperatively, 3–6 Mon post = 3–6 months postoperatively. Significant p values between time points are indicated
FGF-19
In RYGB and VSG group, the serum level of FGF 19 stayed unchanged after the surgeries (p = 0.5936 and p = 0.6652 using Friedman test, respectively).
Discussion
As the metabolic effects of BAs have been increasingly recognized, a number of clinical studies have investigated their changes after bariatric surgery to identify the causal connection between BAs and metabolic improvements [38]. Most published studies show that fasting total BA concentrations increased following RYGB [11, 30, 33, 35, 39]. However, only a few studies differentiated individual BAs and their postoperative course, as was done in the current study. Also, early changes in BAs have not been observed since most studies did not begin to track postoperative changes until 1 month after surgery, even though metabolic improvements can be observed within days after surgery. For this reason, the current study was designed to detect longitudinal changes in primary and secondary BAs from as early as 2 days after bariatric surgery.
After RYGB, both primary BAs (CA and CDCA) increased continuously and reached their highest levels at the last points of examination (3–6 months after surgery). The secondary BA (DCA) decreased initially but showed a significant increase after 3–6 months. This observation is in line with findings in the existing literature [11, 17, 30, 35, 36, 39]. After RYGB, the rapid delivery of nutrients to the distal intestine causes stimulation of intestinal L-cells and GLP-1 secretion [6, 20]. Prior studies describe a large increase in postprandial GLP-1 immediately after RYGB that is sustained in the long term [8, 9]. This GLP-1 rise coincided with a significant increase of BAs in the current study.
In comparison, postoperative BA changes in the VSG cohort were less pronounced and did not mirror BA behavior after RYGB. Shortly after VSG, BAs decreased significantly. However, no significant changes were detected after 10 days or at 3–6 months. These findings are consistent with most previous findings [31,32,33,34, 40]. VSG accelerates intestinal motility, enabling the transportation of a greater amount of primary BA to the distal ileum and the large intestine [41, 42]. Following the elevated resorption of primary BAs and, thus, reduction of BAs entering the large intestine, it was not surprising that DCA dropped immediately after surgery. Similarly, in rodents following VSG, increased primary BAs were seen in the jejunum and decreased secondary BAs in the ileum [23]. The different alterations in bile acid levels following RYGB and VSG were confirmed by a recent meta-analysis, in which the existence of a bile loop and different gut microbiota profiles were considered to be potential causes of the divergent effects of the bariatric procedures [43].
To date, very few publications have addressed the behavior of glucagon after bariatric surgical procedures. In our study, fasting glucagon levels continuously increased following RYGB at every point of measurement (2 days, 10 days, and 6 months) compared to preoperative concentrations. These findings have been reported rarely in the prior literature, for example, by Holst et al., as a paradoxical behavior of glucagon in hyperglycemia and an exaggerated GLP-1 response after RYGB [44]. It seems that glucagon concentrations after surgery do not follow the expected pattern of inhibition by GLP-1 and hyperglycemia. Alexiadou et al. described the different effects on glucagon after RYGB in 19 patients, measuring fasting and postprandial concentrations after a mixed meal. In their study, fasting glucagon showed a significant decrease, but non-fasting glucagon was not altered [18]. Our study showed a similar pattern of fasting glucagon levels in VSG patients. These changes were also noted by Yang et al. [45] and might explain the significant improvement in glucose homeostasis in the early VSG postoperative stage.
Throughout the first months after surgery, hepatic bile acid production and enterohepatic circulation increased. These changes were commensurate with increased FGF-19 and GLP-1 production and improved hepatic insulin sensitivity [38]. Based on the current known mechanisms controlling BA homeostasis, the observed increases in circulating BAs following bariatric procedures should negatively regulate synthetic mechanisms through direct (FXR transcriptional control) and/or indirect BA mediation (FGF-19) [15, 46, 47]. In our study, as in some previous studies, fasting levels of FGF-19 did not increase after RYGB. Neither was a significant decrease detected.
On the other hand, the VSG group showed a weak trend toward increasing levels of fasting FGF-19, although it did not reach statistical significance. This tendency is confirmed by the findings of Escalona et al. [31] and Haluzíková et al. [37], who also described increased FGF-19 after VSG, finding that reduction of BA synthesis may be partially secondary to the inhibitory effect of FGF-19.
Limitations
Fasting blood samples were collected; however, the period of fasting time was not controlled. Owing to different indications for both procedures, the BMI of the RYGB group was lower than the VSG group. Overall, there are more female than male participants in our study. To minimize the bias, patients indicated for bariatric surgery should be randomized into RYGB or VSG groups in further trials.
Conclusions
RYGB and VSG involve different surgical approaches and final anatomical configurations. Between postoperative day 2 and 6-month follow-up, RYGB and VSG resulted in divergent patterns of change in serum glucagon, bile acids, and FGF-19.
References
Wadden TA, Bantle JP, Blackburn GL, Bolin P, Brancati FL, Bray GA, et al. Eight-year weight losses with an intensive lifestyle intervention: The look AHEAD study. Obesity. Hoboken: Wiley. 2014;22:5–13.
Sjostrom L, Narbro K, Sjostrom D, Karason K, Larsson B, Wedel H, et al. Effects of bariatric surgery on mortality in Swedish obese subjects. N Engl J Med Waltham: Massachusetts Medical Soc. 2007;357:741–52.
Pories WJ. Bariatric surgery: risks and rewards. J Clin Endocrinol Metab Washington: Endocrine Soc. 2008;93:S89–96.
Schauer PR, Bhatt DL, Kirwan JP, Wolski K, Aminian A, Brethauer SA, et al. Bariatric surgery versus intensive medical therapy for diabetes-5-year outcomes. N Engl J Med Waltham: Massachusetts Medical Soc. 2017;376:641–51.
Knop FK, Taylor R. Mechanism of metabolic advantages after bariatric surgery it’s all gastrointestinal factors versus it’s all food restriction. Diabetes Care Alexandria: Amer Diabetes Assoc. 2013;36:S287–91.
Isbell JM, Tamboli RA, Hansen EN, Saliba J, Dunn JP, Phillips SE, et al. The importance of caloric restriction in the early improvements in insulin sensitivity after Roux-en-Y gastric bypass surgery. Diabetes Care. 2010;33:1438–42.
Kashyap SR, Daud S, Kelly KR, Gastaldelli A, Win H, Brethauer S, et al. Acute effects of gastric bypass versus gastric restrictive surgery on beta-cell function and insulinotropic hormones in severely obese patients with type 2 diabetes. Int J Obes. 2005;2010(34):462–71.
Bose M, Teixeira J, Olivan B, Bawa B, Arias S, Machineni S, et al. Weight loss and incretin responsiveness improve glucose control independently after gastric bypass surgery. J Diabetes. 2010;2:47–55.
Morínigo R, Lacy AM, Casamitjana R, Delgado S, Gomis R, Vidal J. GLP-1 and changes in glucose tolerance following gastric bypass surgery in morbidly obese subjects. Obes Surg. 2006;16:1594–601.
Morínigo R, Moizé V, Musri M, Lacy AM, Navarro S, Marín JL, et al. Glucagon-like peptide-1, peptide YY, hunger, and satiety after gastric bypass surgery in morbidly obese subjects. J Clin Endocrinol Metab. 2006;91:1735–40.
Albaugh VL, Flynn CR, Cai S, Xiao Y, Tamboli RA, Abumrad NN. Early Increases in bile acids post roux-en-y gastric bypass are driven by insulin-sensitizing, secondary bile acids. J Clin Endocrinol Metab Oxford Academic. 2015;100:E1225–33.
Hofmann AF, Hagey LR. Bile acids: Chemistry, pathochemistry, biology, pathobiology, and therapeutics. Cell Mol Life Sci Basel: Springer Basel Ag. 2008;65:2461–83.
Thomas C, Pellicciari R, Pruzanski M, Auwerx J, Schoonjans K. Targeting bile-acid signalling for metabolic diseases. Nat Rev Drug Discov London: Nature Publishing Group. 2008;7:678–93.
Chiang JYL. Bile acid metabolism and signaling. Compr Physiol Hoboken: Wiley. 2013;3:1191–212.
Staels B, Fonseca VA. Bile acids and metabolic regulation: mechanisms and clinical responses to bile acid sequestration. Diabetes Care Am Diabetes Assoc. 2009;32:S237–45.
Mueller M, Thorell A, Claudel T, Jha P, Koefeler H, Lackner C, et al. Ursodeoxycholic acid exerts farnesoid X receptor-antagonistic effects on bile acid and lipid metabolism in morbid obesity. J Hepatol Amsterdam: Elsevier. 2015;62:1398–404.
Pournaras DJ, Glicksman C, Vincent RP, Kuganolipava S, Alaghband-Zadeh J, Mahon D, et al. The role of bile after Roux-en-Y gastric bypass in promoting weight loss and improving glycaemic control. Endocrinology. 2012;153:3613–9.
Alexiadou K, Cuenco J, Howard J, Wewer Albrechtsen NJ, Ilesanmi I, Kamocka A, et al. Proglucagon peptide secretion profiles in type 2 diabetes before and after bariatric surgery: 1-year prospective study. BMJ Open Diabetes Res Care. 2020;8
Demant M, Bagger JI, Suppli MP, Lund A, Gyldenløve M, Hansen KB, et al. Determinants of fasting hyperglucagonemia in patients with type 2 diabetes and nondiabetic control subjects. Metab Syndr Relat Disord. 2018;16:530–6.
Laferrère B, Heshka S, Wang K, Khan Y, McGinty J, Teixeira J, et al. Incretin levels and effect are markedly enhanced 1 month after Roux-en-Y gastric bypass surgery in obese patients with type 2 diabetes. Diabetes Care. 2007;30:1709–16.
Purnell JQ, Johnson GS, Wahed AS, Dalla Man C, Piccinini F, Cobelli C, et al. Prospective evaluation of insulin and incretin dynamics in obese adults with and without diabetes for 2 years after Roux-en-Y gastric bypass. Diabetologia. 2018;61:1142–54.
Jacobsen SH, Olesen SC, Dirksen C, Jørgensen NB, Bojsen-Møller KN, Kielgast U, et al. Changes in gastrointestinal hormone responses, insulin sensitivity, and beta-cell function within 2 weeks after gastric bypass in non-diabetic subjects. Obes Surg. 2012;22:1084–96.
Myronovych A, Kirby M, Ryan KK, Zhang W, Jha P, Setchell KDR, et al. Vertical sleeve gastrectomy reduces hepatic steatosis while increasing serum bile acids in a weight-loss-independent manner. Obesity. Hoboken: Wiley. 2014;22:390–400.
Cummings BP, Bettaieb A, Graham JL, Stanhope KL, Kowala M, Haj FG, et al. Vertical sleeve gastrectomy improves glucose and lipid metabolism and delays diabetes onset in UCD-T2DM rats. Endocrinology. 2012;153:3620–32.
Ding L, Sousa KM, Jin L, Dong B, Kim B-W, Ramirez R, et al. Vertical sleeve gastrectomy activates GPBAR-1/TGR5 to sustain weight loss, improve fatty liver, and remit insulin resistance in mice. Hepatol Baltim Md. 2016;64:760–73.
Ryan KK, Tremaroli V, Clemmensen C, Kovatcheva-Datchary P, Myronovych A, Karns R, et al. FXR is a molecular target for the effects of vertical sleeve gastrectomy. Nature. London: Nature Publishing Group; 2014;509:183-+.
Bhutta HY, Rajpal N, White W, Freudenberg JM, Liu Y, Way J, et al. Effect of Roux-en-Y gastric bypass surgery on bile acid metabolism in normal and obese diabetic rats. PloS One. 2015;10:e0122273.
Spinelli V, Lalloyer F, Baud G, Osto E, Kouach M, Daoudi M, et al. Influence of Roux-en-Y gastric bypass on plasma bile acid profiles: a comparative study between rats, pigs and humans. Int J Obes. 2005;2016(40):1260–7.
Khan FH, Shaw L, Zhang W, Salazar Gonzalez RM, Mowery S, Oehrle M, et al. Fibroblast growth factor 21 correlates with weight loss after vertical sleeve gastrectomy in adolescents. Obes Silver Spring Md. 2016;24:2377–83.
Jahansouz C, Xu H, Hertzel AV, Serrot FJ, Kvalheim N, Cole A, et al. Bile acids increase independently from hypocaloric restriction after bariatric surgery. Ann Surg. 2016;264:1022–8.
Escalona A, Munoz R, Irribarra V, Solari S, Allende F, Francisco MJ. Bile acids synthesis decreases after laparoscopic sleeve gastrectomy. Surg Obes Relat Dis, vol. 12. New York: Elsevier Science Inc; 2016. p. 763–9.
Belgaumkar AP, Vincent RP, Carswell KA, Hughes RD, Alaghband-Zadeh J, Mitry RR, et al. Changes in bile acid profile after laparoscopic sleeve gastrectomy are associated with improvements in metabolic profile and fatty liver disease. Obes Surg. 2016;26:1195–202.
Steinert RE, Peterli R, Keller S, Meyer-Gerspach AC, Drewe J, Peters T, et al. Bile acids and gut peptide secretion after bariatric surgery: a 1-year prospective randomized pilot trial. Obesity. 2013;21:E660–8.
Nakatani H, Kasama K, Oshiro T, Watanabe M, Hirose H, Itoh H. Serum bile acid along with plasma incretins and serum high–molecular weight adiponectin levels are increased after bariatric surgery. Metab - Clin Exp Elsevier. 2009;58:1400–7.
Gerhard GS, Styer AM, Wood GC, Roesch SL, Petrick AT, Gabrielsen J, et al. A Role for Fibroblast growth factor 19 and bile acids in diabetes remission after Roux-en-Y gastric bypass. Diabetes Care Am Diabetes Assoc. 2013;36:1859–64.
Jansen PLM, van Werven J, Aarts E, Berends F, Janssen I, Stoker J, et al. Alterations of hormonally active fibroblast growth factors after Roux-en-Y gastric bypass surgery. Dig Dis Basel Switz. 2011;29:48–51.
Haluzíková D, Lacinová Z, Kaválková P, Drápalová J, Křížová J, Bártlová M, et al. Laparoscopic sleeve gastrectomy differentially affects serum concentrations of FGF-19 and FGF-21 in morbidly obese subjects. Obes Silver Spring Md. 2013;21:1335–42.
Albaugh VL, Banan B, Ajouz H, Abumrad NN, Flynn CR. Bile acids and bariatric surgery. Mol Aspects Med Amsterdam: Elsevier. 2017;56:75–89.
Ferrannini E, Camastra S, Astiarraga B, Nannipieri M, Castro-Perez J, Xie D, et al. Increased bile acid synthesis and deconjugation after biliopancreatic diversion. diabetes. Alexandria: Amer Diabetes Assoc. 2015;64:3377–85.
De Vuono S, Ricci MA, Nulli Migliola E, Monti MC, Morretta E, Boni M, et al. Serum bile acid levels before and after sleeve gastrectomy and their correlation with obesity-related comorbidities. Obes Surg. 2019;29:2517–26.
Trung VN, Yamamoto H, Furukawa A, Yamaguchi T, Murata S, Yoshimura M, et al. Enhanced intestinal motility during oral glucose tolerance test after laparoscopic sleeve gastrectomy: preliminary results using cine magnetic resonance imaging. Plos One Public Library Sci. 2013;8:e65739.
Einarsson C, Hillebrant CG, Axelson M. Effects of treatment with deoxycholic acid and chenodeoxycholic acid on the hepatic synthesis of cholesterol and bile acids in healthy subjects. Hepatol Baltim Md. 2001;33:1189–93.
Zhang C, Zhang J, Zhou Z. Changes in fasting bile acid profiles after Roux-en-Y gastric bypass and sleeve gastrectomy. Medicine (Baltimore). 2021;100:e23939.
Holst JJ, Madsbad S, Bojsen-Møller KN, Svane MS, Jørgensen NB, Dirksen C, et al. Mechanisms in bariatric surgery: gut hormones, diabetes resolution, and weight loss. Surg Obes Relat Dis Off J Am Soc Bariatr Surg. 2018;14:708–14.
Yang J, Gao Z, Williams DB, Wang C, Lee S, Zhou X, et al. Effect of laparoscopic Roux-en-Y gastric bypass versus laparoscopic sleeve gastrectomy on fasting gastrointestinal and pancreatic peptide hormones: a prospective nonrandomized trial. Surg Obes Relat Dis Off J Am Soc Bariatr Surg. 2018;14:1521–9.
Chiang JYL. Bile acids: regulation of synthesis. J Lipid Res. 2009;50:1955–66.
Li S, Hsu DDF, Li B, Luo X, Alderson N, Qiao L, et al. Cytoplasmic tyrosine phosphatase Shp2 coordinates hepatic regulation of bile acid and FGF15/19 signaling to repress bile acid synthesis. Cell Metab. 2014;20:320–32.
Acknowledgements
We thank TW McGlennon, McGlennon MotiMetrics, Maiden Rock, WI, USA, for statistical analysis review.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics Approval
All procedures of the study are ethically compliant and were approved (EK 416092015) by the Institutional Review Board of University Medicine Mannheim, Germany. The study was performed in accord with the ethical standards of the 1964 Declaration of Helsinki and its subsequent amendments.
Consent to Participate
Written informed consent was obtained from all study participants.
Conflict of Interest
The authors declare that they have no conflicts of interest or financial ties to disclose. JN Buchwald received a small grant for manuscript development.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Key Points
1. In the RYGB group: Glucagon and the primary bile acids CA and CDCA increased continuously after surgery, while the secondary bile acid DCA decreased initially and later significantly increased.
2. In the VSG group: Glucagon increased initially but later decreased. The primary bile acids CA and CDCA, as well as DCA, decreased immediately and showed no significant change thereafter.
3. RYGB and VSG resulted in divergent patterns of change in serum glucagon, bile acids, and FGF-19. The different alterations in bile acid levels following RYGB and VSG have been confirmed by a recent meta-analysis.
Rights and permissions
About this article
Cite this article
Yang, C., Brecht, J., Weiß, C. et al. Serum Glucagon, Bile Acids, and FGF-19: Metabolic Behavior Patterns After Roux-en-Y Gastric Bypass and Vertical Sleeve Gastrectomy. OBES SURG 31, 4939–4946 (2021). https://doi.org/10.1007/s11695-021-05677-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-021-05677-3