Abstract
Objective
The aim of this study is to determine the prevalence of diabetes mellitus (DM) in patients with intraductal papillary mucinous neoplasm of the pancreas (IPMN) and compare rates of new/progressive DM between IPMN patients undergoing pancreatectomy versus observation.
Methods
Patients diagnosed with IPMN were identified from institutional databases, divided into two groups based on treatment type, pancreatectomy versus clinical observation, and subsequently evaluated. Standard demographic and clinicopathologic variables, fasting glucose, diabetic status, and pancreatic volume data, were obtained and compared between groups.
Results
One hundred thirty-four IPMN patients were identified; 103 (77 %) underwent pancreatectomy and 31 (23 %) were observed. Baseline DM rate was 18 % (24/134). This was not different between groups [17 % (17/103) resected vs. 23 % (7/31) observed, p = 0.51]. Median follow-up was 53 months and new/progressive DM occurred in 37 (28 %) patients with no difference between groups [29 (28 %) resected vs. 8 (26 %) observed, p = 0.74]. Among resected patients, degree of dysplasia was associated with increase risk of new/progressive DM [moderate dysplasia OR 5.76 (1.24–26.79) and severe dysplasia OR 9.43 (1.54–57.74), p = 0.04], while procedure type and remnant volume were not.
Conclusions
The incidence and prevalence of DM among patients with IPMN was high and did not differ between resected and observed groups. Degree of dysplasia, not the amount of resected pancreas, was associated with increased risk of DM, suggesting that the presence or development of DM may be a marker of malignant progression. Confirmatory studies are required.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Intraductal papillary mucinous neoplasms of the pancreas (IPMN) display differing degrees of dysplasia and vary in terms of their malignant potential.1 IPMN are noninvasive precursor lesions reflective of an underlying field defect and genetic instability, placing the entire gland at increase risk for cancer development.2 Since being formally classified, the diagnosis of IPMN has increased substantially and over the last decade the increasing use of cross-sectional imaging has also resulted in a trend toward detection of smaller, asymptomatic lesions.3 The diagnosis of clinically silent lesions, with varying malignant potential, can make decisions regarding management of patients with IPMN difficult. Appropriate treatment plans require a balanced assessment of malignant potential, operative risk, as well as potential long term complications of pancreatectomy, such as diabetes mellitus (DM).4
The reported risk of malignancy in main duct IPMN (mean 61.3 %, range 35–100 %) is presumed to outweigh the potential short- and long-term complications of pancreatectomy and resection is considered the standard of care. However, in the setting of branch duct (BD) IPMN, the risk of malignancy is lower (mean 24.4 %, range 6–51 %) and indications for resection are much less clear.5 Even when suggested clinical and imaging criteria are employed to risk stratify BD IPMN, prediction of malignancy is suboptimal.6,7 Furthermore, despite many advances, postoperative morbidity associated with pancreatectomy is high (20–30 %) and mortality rates are not insignificant (2–4 %).8
The vast majority of studies evaluating pancreatic endocrine function and IPMN focus solely on the impact of resection8–12 on the development of impaired glucose metabolism. Pancreatic remnant volume has been hypothesized to be associated with the development of DM. Techniques such as parenchymal sparing pancreatectomy (PSP) have been reported to reduce the risk of postpancreatectomy DM from 14 to 18 % with classic resections to 3–4 % with PSP.8,11 Furthermore, natural history studies of IPMN primarily focus on characterizing malignant degeneration over time rather than DM. As such, the incidence and prevalence of DM among patients with IPMN remains poorly characterized.13–15
Our understanding of IPMN as a disease entity has increased exponentially since initial classification in 1996.16 Knowledge of the malignant potential and surgical morbidity/mortality has been evaluated extensively and aids clinical decision-making. However, questions remain as to the long-term implications of IPMN and surgical resection on the development of pancreatic endocrine dysfunction. The primary objective of the current study was to define the prevalence of DM among a cohort of patients with IPMN and to compare rates of new or progressive DM between patients undergoing pancreatectomy versus observation. Risk factors associated with the development of postoperative DM were also assessed.
Materials and Methods
Study Design
This study was deemed exempt from full institutional review, and ethics approval was obtained via waiver of the Health Insurance Portability and Accountability Act. From January 2000 to September 2013, patients with a primary diagnosis of IPMN, undergoing resection or radiographic surveillance at the study institution, were identified from prospectively maintained databases and retrospectively reviewed. Diagnosis of IPMN among resected patients was histopathologically confirmed. Observed patients were defined as having IPMN based on characteristic radiographic findings and a cyst fluid CEA level >200 ng/mL. Patients in whom DM status was unknown/not ascertainable and patients with type 1 DM were excluded from evaluation.
Data Collection
Standard demographic and clinicopathologic characteristics were obtained from the database and supplemented with information from the electronic medical record where necessary. Date of IPMN diagnosis was defined as the date of initial radiographic imaging consistent with, or concerning for, IPMN. Radiology reports were used to determine cyst size (mm) and anatomic location within the pancreas (head, neck, body, tail). Patients were categorized as “obese” if the calculated BMI at the time of diagnosis was ≥30 kg/m2. Baseline (preoperative or prediagnosis) diabetic status was determined based on review of the electronic medical record as well as the initial referral and consultation notes. If following this review, patient status was still unknown, home medication profiles were evaluated for use of oral hypoglycemic medications and/or insulin prior to the date of diagnosis. If present, this was considered evidence of preexisting DM. DM was also considered preexisting if it was diagnosed in conjunction with the workup of the pancreatic lesion. Progression of DM was defined as an increase in the frequency or dose of oral hypoglycemic medications and/or insulin following the date of IPMN diagnosis in the observed group or the date of surgery in the resected group. Likewise, new DM was considered if diagnosis was made after IPMN was detected in the observed group or after resection in the surgical group. Multiple mechanisms were employed to determine new or progressive DM status including review of updated clinics notes and medication profiles. In addition, all patients with available baseline DM status information were mailed a survey, explaining the study aims and inquiring as to the current disease (IPMN) and DM status. A waiver for exemption of IRB/peer review for collection of prospective data in the form of a survey was completed and approved by the institution. Approval was in direct accordance with the “Code of Federal Regulation-Title 45, Section 46-101b” and the institutional requirements for collection of prospective data in form of a survey. After an interval of 4 weeks, patients who failed to respond to the survey were contacted by telephone and DM status ascertained. However, if both survey and telephone attempts were unsuccessful patients were excluded from evaluation. Fasting plasma glucose measurements were obtained at two time points for all patients, baseline and at last clinical follow-up.
Among patients who underwent pancreatectomy, operative characteristics, including procedure type, operative time (min), and estimated blood loss (EBL, mL) were determined. Pathology reports were reviewed and data regarding degree of dysplasia (mild, moderate, severe) and lesion histology (gastric, intestinal, mixed, pancreatobiliary) were obtained. Surgical complications were noted and morbidity was graded according to the Memorial Sloan Kettering Secondary Events Program database.17 This severity scoring ranges from 0 (no complication) to (5 complication) resulting in death and is consistent with “Common Terminology Criteria for Adverse Events Version 4.0,” endorsed by the National Institutes of Health and the National Cancer Institute. Major complications were those with a grade ≥3. Follow-up time for the entire cohort was taken as the interval from the date of IPMN diagnosis to last clinical contact or death.
Pancreatic Volume Measurement
In a subset of patients with adequate CT imaging at both diagnosis and follow-up three-dimensional (3D) pancreas volume was measured using Scout Liver (Pathfinder Technologies, Nashville, TN). This is a commercially available software that allows the user to pull CT scans from institutional databases, segment anatomic areas of interest from surrounding structures, generate a 3D model, and subsequently calculate the model volume. The software was designed for liver segmentation prior to surgery; however, any anatomic area of interest that is distinguishable on CT scan can be segmented and volume calculated.18 In the current study, both the pancreas and cyst were segmented manually and volumes were obtained at diagnosis and either postoperatively (resected group) or at 12-month follow-up (observed group). In the observed group, pancreatic volume at diagnosis and at 12-month follow-up was calculated as absolute pancreas volume minus pancreatic cyst volume. Among resected patients, pancreatic remnant volume was measured postoperatively and relative change in pancreas volume from baseline to postoperative (∆PV) was calculated. All pancreatic volume data were normalized to BMI and presented as mL m2/kg.
Statistical Analysis
All statistical analyses were performed using SPSS software version 21 (Chicago, IL, USA). Overall, baseline demographic, clinicopathologic, and operative characteristics are presented as frequency (%) and mean ± standard deviation. Follow-up time is reported as median (range). Patients with IPMN were stratified into resected and observed groups, and clinical and diabetic outcomes were compared. Between groups, comparison of categorical data was completed using chi-squared or Fisher’s exact test depending on the number of observations. Continuous data was compared using the Mann–Whitney U test or independent t test depending on the sample distribution. To identify potential factors associated with the development of new/progressive DM amongst resected patients with IPMN, binary logistic regression analysis was completed. All statistical tests were two-sided, and significance was set at p < 0.05.
Results
IPMN Resected Versus Observed
From January 2000 to September 2013, 154 patients diagnosed with IPMN and possessing adequate data regarding baseline DM status were identified and evaluated. A survey was mailed to all patients to elucidate current disease (IPMN) and DM status. Survey response rate was 77 % (n = 119). Following review, one patient was found to have type 1 DM and was excluded. Of the 35 nonresponders, 16 patients were reached via telephone or in follow-up clinics during the study period and DM status ascertained. The remaining 19 patients were unreachable and excluded from evaluation. Overall, 134 patients with IPMN had up to date, reliable DM data, and were included in the primary analysis. Among the study cohort, 103 (77 %) patients underwent pancreatectomy (resection group) while 31 (23 %) underwent routine radiographic surveillance (observation group). Mean age at the time of diagnosis was 65 ± 17 years and 66 % (n = 89) of the cohort were female. Baseline demographic, radiologic, and pancreatic volumetry characteristics stratified by initial management strategy (resection vs observation) are outlined in Table 1. Overall, the two groups were similar in terms of age, sex, race, BMI, and obesity status; however, hyperlipidemia was more common among the resected group [60 (58 %) resected vs 7 (23 %) observed, p < 0.0001]. Cyst characteristics at diagnosis were significantly different. Among resected patients, cyst size was greater compared to observed patients (26 ± 10 mm resected vs 19 ± 7 mm observed, p = 0.001) and lesions were more commonly of the main duct variety [40 (39 %) resected vs 1 (3 %) observed, p = 0.002]. Pancreatic volume [(total pancreas volume) − (cyst volume) / BMI] at the time of diagnosis was 2.9 ± 0.88 mL m2/kg for the cohort and was not different between resected and observed (2.8 ± 0.91 vs 2.9 ± 0.81, respectively, p = 0.87). Overall, three patients died of unrelated causes (one lung cancer, one B cell lymphoma, and one unknown cause) during a median follow-up of 53 months (154).
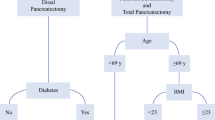
Fasting plasma glucose at diagnosis was 115 ± 43 mg/dL and was not different between resected and observed groups (114 ± 44 mg/dL resected vs 118 ± 37 mg/dL observed, p = 0.69). Likewise, glucose at follow-up was 123 ± 37 and 103 ± 26 mg/dL in resected and observed groups, respectively, and was not statistically different (p = 0.11). The prevalence of DM at the time of diagnosis was 18 % (n = 24) for the entire cohort and development of new (n = 24), or progressive (n = 13) DM, occurred in 28 % of patients. The baseline rate of DM, as well as incidence of new or progressive DM during follow-up for resected and observed groups, is illustrated in Fig. 1. No significant differences in terms of DM status (baseline, new, progressive, new + progressive) were observed between patients undergoing pancreatectomy versus those being managed with observation alone.
Resected IPMN With and Without New/Progressive DM
Operative characteristics of patients undergoing pancreatectomy for IPMN (n = 103) are outlined in Table 2. Classic pancreaticoduodenectomy (n = 51, 50 %) and distal pancreatectomy (n = 31, 30 %) were the two most commonly performed operations and branch duct IPMN accounted for just over half of all resections (n = 57, 55 %). Overall and major complication rates were 48 % (n = 49) and 18 % (n = 18), respectively. Among the resected group, 29 (28 %) patients developed new or progressive DM (DM+) while 74 (72 %, DM−) did not. Demographic, clinicopathologic, operative, and volumetric characteristics of the groups (DM− vs DM+) are outlined in Table 3. At baseline, BMI was significantly higher in the DM+ group (29 ± 6 kg/m2) compared to the DM− group (26 ± 4 kg/m2), p = 0.003. Similarly, the number of patients defined as obese was higher among the DM+ group [16 (56 %) DM+ vs 11 (16 %) DM−, p < 0.0001]. Among resected patients, 44 (42 %) had evaluable pancreatic volume measurements: 31 (42 %) in the DM− group and 12 (40 %) in DM+ group. Overall, from baseline to postoperative follow-up, the ∆PV was 48 ± 17 % among all resected patients. No differences were observed in volume at diagnosis, remnant volume, or ∆PV, between patients who did and did not develop new or progressive DM.
Univariate analyses of risk factors for new/progressive DM are outlined in Table 3. Obesity (OR 7.81, 95 % CI 3.19–19.15, p < 0.0001) and plasma glucose at diagnosis [OR 1.17 (per 10 mg/dL increase), 95 % CI 1.05–1.31, p = 0.006] and at last follow-up [OR 1.26 (per 10 mg/dL increase), 95 % CI 1.09–1.45, p = 0.002] were associated with new/progressive DM. Furthermore, degree of dysplasia (moderate dysplasia, OR 5.37, 95 % CI 1.15–25.03, and severe dysplasia, OR 9.43, 95 % CI 1.54–57.74, p = 0.04) was also significantly associated with new or progressive DM. The small sample size and low event rate (28 %, n = 29) precluded multivariate analysis and further identification of potential independent predictors.
Discussion
Clinical decision making regarding treatment of IPMN can be difficult. The risks of malignancy must be balanced against operative risk and potential long-term complications such as endocrine dysfunction. In the current study, we evaluated the prevalence of DM among a cohort of patients with IPMN and compared the incidence of new or progressive DM between patients undergoing pancreatectomy to those subjected to observation. Among the entire cohort of patients with IPMN, the prevalence of DM was high. Furthermore, the development of new or progressive DM was not different between patients with IPMN undergoing pancreatectomy versus those subject to routine radiographic surveillance. Among resected patients, variables associated with an increased risk of postpancreatectomy DM included; obesity (BMI ≥30 kg/m2), higher plasma glucose (baseline and follow-up), and degree of dysplasia within the resected pancreas.
It is unclear whether IPMN may in and of itself predispose patients to higher risks of impaired glucose metabolism and DM.19 Prevalence of DM at baseline among patients with IPMN (18 %) in the current study was nearly double that reported in a 2014 Center for Disease Control diabetes report, estimating the overall prevalence of DM among adult Americans to be 9.3 %.20 Similarly, in a study from the Italian Association for the Study of the Pancreas (AISP) comparing 390 patients with IPMN to matched healthy controls, DM at baseline was 13.9 % in the IPMN group and was significantly higher than controls (7.5 %, p < 0.01).19 Elucidation of possible mechanisms by which IPMN imposes an increase risk of DM is beyond the scope of this observational study. Previous studies, however, have hypothesized that IPMN may lead to obstruction of the pancreatic ductal system and may induce low-grade pancreatitis distal to the lesion with subsequent parenchymal atrophy and endocrine dysfunction.11
Studies comparing the impact of extent of pancreatectomy on subsequent endocrine function suggest that larger volume resections are associated with increased risk of DM.8–12 However, the heterogeneity of the included pathologies in these studies, as well as the lack of observational arms, fails to account for the inherent risk of new or progressive DM associated with the underlying disease process. To our knowledge, this is the first study to evaluate the incidence of DM among a cohort of patients with IPMN subjected to pancreatectomy or observation. The overall incidence of new or progressive DM in our study cohort was 28 % during a moderate follow-up period of 53 months, and no differences were observed between resected and observed groups (28 vs 26 %, respectively) with similar follow-up periods. Based on current literature, the incidence of DM following pancreatectomy varies widely and has been reported to range anywhere from 1 to 18 %.8,11,21 In our cohort of patients, even among the observation arm, rates were much higher. This discrepancy may simply reflect differences in follow-up time, means of determining DM status and/or rigor of DM surveillance between studies. However, the lack of difference noted between resected and observed groups in our study suggests that among patients with IPMN, the extent of resection and/or the size of the remnant pancreas does not dictate progression of endocrine dysfunction. Rather, it may be that the underlying field defect of the entire pancreatic gland associated with IPMN increases the inherent risk of DM. Clinically, this suggests that decisions to treat IPMN with resection should hinge more on malignant risk and surgical morbidity rather than long-term risk of DM. Moreover, these findings challenge the utility of parenchymal sparing pancreatectomy (PSP) where the presumed benefit is a reduction in long-term endocrine dysfunction. In patients with IPMN, where partial pancreatectomy is indicated, PSP may simply impose greater risks of early morbidity8,22,23 without any alteration of the risk of developing DM.
In some patients with IPMN, observation is not an option for management. Among this group, varying reports of the risks and predictors of postpancreatectomy endocrine dysfunction/DM exist. The resected group in this study consisted of 103 patients, 29 of whom went on to developed new or progressive DM following surgery. In addition to traditional risk factors, increasing degrees of dysplasia were significantly associated with increased risk of new or progressive DM. The basis for this association is likely multifactorial and definitive explanation is outside the bounds of this retrospective study. However; given the genetic instability of the entire pancreatic gland, it is possible that the degree of dysplasia in the resected specimen is a marker of change within the remnant gland potentially associated with pancreatic endocrine dysfunction. The mechanism by which this occurs is unknown but may be related to direct effects on pancreatic islet cells or, similar to some truly malignant diseases, this may represent a paraneoplastic phenomenon.24These observations are novel and lend further credence to a hypothesis that the development of DM in patients with IPMN may be a marker increasing dysplasia and malignant progression.
This study represents a retrospective, single-center study and is subject to all the inherent limitations associated with this design. Additionally, only patients with IPMN who responded to mailed questionnaires/telephone evaluation were included, potentially leading to selection bias. Furthermore, among the observed group, patients who continued follow-up at the study center may have been innately different from those who were initially seen and subsequently followed elsewhere. These may represent a higher risk group and may overestimate the incidence and prevalence of DM in patients with IPMN managed with observation. Furthermore, it is possible that the diagnosis of IPMN alone resulted in heightened awareness and assessment of pancreatic function, leading to increased DM diagnosis, more fastidious monitoring of glucose levels and subsequent change in diabetic medications. Although this may hold true for some resected patients: standard surgical follow-up of observed patients at the study center typically includes annual radiographic surveillance with little focus on diabetic assessment and/or management. As such, the high rates of DM observed in both groups cannot be fully explained by this phenomenon. Finally, the median follow-up time for the entire cohort was moderate [53 months (range 154)] and may underestimate the long-term risk of new or progressive DM among patient with IPMN.
Conclusion
In this study, the prevalence of DM among patients with IPMN was higher than what is typically reported in the general population and development of new or progressive DM was not different between patients who underwent resection versus observation. The degree of dysplasia was associated with increased risk of DM in resected patients while the extent of pancreatectomy was not, suggesting that it is the natural history of the “at risk” gland that dictates DM risk. Larger confirmatory studies are ongoing.
References
D’Angelica, M., et al., Intraductal papillary mucinous neoplasms of the pancreas: an analysis of clinicopathologic features and outcome. Ann Surg, 2004. 239(3): p. 400–8.
Hruban, R.H., et al., Clinical importance of precursor lesions in the pancreas. J Hepatobiliary Pancreat Surg, 2007. 14(3): p. 255–63.
Gaujoux, S., et al., Cystic lesions of the pancreas: changes in the presentation and management of 1,424 patients at a single institution over a 15-year time period. J Am Coll Surg, 2011. 212(4): p. 590–600; discussion 600–3.
Maker, A.V., et al., Cyst Fluid Biomarkers for Intraductal Papillary Mucinous Neoplasms of the Pancreas: A Critical Review from the International Expert Meeting on Pancreatic Branch-Duct-Intraductal Papillary Mucinous Neoplasms. Journal of the American College of Surgeons, 2015. 220(2): p. 243–253.
Tanaka, M., et al., International consensus guidelines 2012 for the management of IPMN and MCN of the pancreas. Pancreatology, 2012. 12(3): p. 183–97.
Nguyen, A.H., et al., Current recommendations for surveillance and surgery of intraductal papillary mucinous neoplasms may overlook some patients with cancer. J Gastrointest Surg, 2015. 19(2): p. 258–65.
Goh, B.K., et al., Utility of the sendai consensus guidelines for branch-duct intraductal papillary mucinous neoplasms: a systematic review. J Gastrointest Surg, 2014. 18(7): p. 1350–7.
Sauvanet, A., et al., Parenchyma-sparing pancreatectomy for presumed noninvasive intraductal papillary mucinous neoplasms of the pancreas. Ann Surg, 2014. 260(2): p. 364–71.
Schnelldorfer, T., et al., Experience with 208 resections for intraductal papillary mucinous neoplasm of the pancreas. Arch Surg, 2008. 143(7): p. 639–46; discussion 646.
You, D., et al., Long term effects ofpancreaticoduodenectomy on glucose metabolism. ANZ journal of surgery, 2012: p. 447–451.
Falconi, M., et al., Pancreatic insufficiency after different resections for benign tumours. Br J Surg, 2008. 95(1): p. 85–91.
Crippa, S., et al., Middle pancreatectomy: indications, short- and long-term operative outcomes. Ann Surg, 2007. 246(1): p. 69–76.
Bassi, C., et al., Natural history of intraductal papillary mucinous neoplasms (IPMN): current evidence and implications for management. J Gastrointest Surg, 2008. 12(4): p. 645–50.
Allen, P.J., The management of intraductal papillary mucinous neoplasms of the pancreas. Surg Oncol Clin N Am, 2010. 19(2): p. 297–310.
Lafemina, J., et al., Malignant progression in IPMN: a cohort analysis of patients initially selected for resection or observation. Ann Surg Oncol, 2013. 20(2): p. 440–7.
Kloppel G S.E., Longnecker D.S, Capella C, Sobin L.H, World Health Organization International Histologic Typing of Tumors of the Exocrine Pancreas. 2nd ed. 1996, Berlin: Springer-Verlag.
Grobmyer, S.R., et al., Defining morbidity after pancreaticoduodenectomy: use of a prospective complication grading system. J Am Coll Surg, 2007. 204(3): p. 356–64.
Simpson, A.L., et al., Chemotherapy-induced splenic volume increase is independently associated with major complications after hepatic resection for metastatic colorectal cancer. J Am Coll Surg, 2015. 220(3): p. 271–80.
Capurso, G., et al., Risk factors for intraductal papillary mucinous neoplasm (IPMN) of the pancreas: a multicentre case–control study. Am J Gastroenterol, 2013. 108(6): p. 1003–9.
National Diabetes Statistic Report 2014. Available at http://www.cdc.gov/diabetes/data/statistics/2014statisticsreport.html . Accessed March 23, 2015.
Park, J.W., et al., Effects of pancreatectomy on nutritional state, pancreatic function and quality of life. Br J Surg, 2013. 100(8): p. 1064–70.
Shikano, T., et al., Middle pancreatectomy: safety and long-term results. Surgery, 2010. 147(1): p. 21–9.
Crippa, S., et al., Parenchyma-sparing resections for pancreatic neoplasms. J Hepatobiliary Pancreat Sci, 2010. 17(6): p. 782–7.
Burt, M.E., et al., Peripheral tissue metabolism in cancer-bearing man. Ann Surg, 1983. 198(6): p. 685–91.
Conflict of Interest
The authors declare that they have no competing interests.
Author information
Authors and Affiliations
Corresponding author
Additional information
This manuscript is based on submission to the Society for Surgery of the Alimentary Tract/ Digestive Disease Week annual meeting.
Rights and permissions
About this article
Cite this article
Leal, J.N., Kingham, T.P., D’Angelica, M.I. et al. Intraductal Papillary Mucinous Neoplasms and the Risk of Diabetes Mellitus in Patients Undergoing Resection Versus Observation. J Gastrointest Surg 19, 1974–1981 (2015). https://doi.org/10.1007/s11605-015-2885-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-015-2885-1