Abstract
Objective
To evaluate the feasibility of using gadopentetate dimeglumine (Gd-DTPA) for dual-energy computed tomography pulmonary angiography (CTPA).
Methods
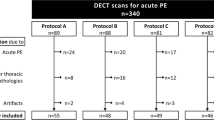
Sixty-six patients were randomly divided into three groups and underwent CTPA. Group A had a turbo flash scan using an iohexol injection, Group B had a turbo flash scan using Gd-DTPA, and Group C had a dual-energy scan using Gd-DTPA. The original images of Group C were linearly blended with a blending factor of 0.5 or reconstructed at 40, 50, 60, 70, 80, 90, 100, and 110 keV, respectively. The groups were compared in terms of pulmonary artery CT value, image quality, and radiation dose.
Results
The pulmonary artery CT values were significantly higher in Group C40keV than in Groups B and C, but lower than in Group A. There was no significant difference in the image noise of Groups C40keV, B, and C. Moreover, Group A had the largest beam hardening artifacts of the superior vena cava (SVC), followed by Groups B and C. Group C40keV showed better vascular branching than the other three groups, among which Group B was superior to Group A. The subjective score of the image quality of Groups A, B, and C showed no significant difference, but the score was significantly higher in Group C40keV than in Groups A and B. The radiation dose was significantly lower in Group B than in Groups A and C.
Conclusion
Gd-CTPA is recommended to patients who are unsuitable for receiving an iodine-based CTPA. Furthermore, a turbo flash scan could surpass a dual-energy scan without consideration for virtual monoenergetic imaging.
Article PDF
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
References
Essien EO, Rali P, Mathai SC. Pulmonary Embolism. Med Clin North Am, 2019,103(3):549–564
Mansella G, Keil C, Nickel CH, et al. Delayed Diagnosis in Pulmonary Embolism: Frequency, Patient Characteristics, and Outcome. Respiration, 2020,99(7):589–597
Di Nisio M, van Es N, Buller HR. Deep vein thrombosis and pulmonary embolism. Lancet, 2016,388(10063):3060–3073
Grabherr S, Heinemann A, Vogel H, et al. Postmortem CT Angiography Compared with Autopsy: A Forensic Multicenter Study. Radiology, 2018,288(1):270–276
Moore AJE, Wachsmann J, Chamarthy MR, et al. Imaging of acute pulmonary embolism: an update. Cardiovasc Diagn Ther, 2018,8(3):225–243
Lakhal K, Ehrmann S, Robert-Edan V. Iodinated contrast medium: Is there a re(n)al problem? A clinical vignette-based review. Crit Care, 2020,24(1):641
Bonelli N, Rossetto R, Castagno D, et al. Hyperthyroidism in patients with ischaemic heart disease after iodine load induced by coronary angiography: Long-term follow-up and influence of baseline thyroid functional status. Clin Endocrinol (Oxf), 2018,88(2):272–278
Davenport MS, Perazella MA, Yee J, et al. Use of Intravenous Iodinated Contrast Media in Patients with Kidney Disease: Consensus Statements from the American College of Radiology and the National Kidney Foundation. Radiology, 2020,294(3):660–668
Dona I, Bogas G, Salas M, et al. Hypersensitivity Reactions to Multiple Iodinated Contrast Media. Front Pharmacol, 2020,11:575437
Stacul F, Bertolotto M, Thomsen HS, et al. Iodine-based contrast media, multiple myeloma and monoclonal gammopathies: literature review and ESUR Contrast Media Safety Committee guidelines. Eur Radiol, 2018,28(2):683–691
Xiao YD, Paudel R, Liu J, et al. MRI contrast agents: Classification and application (Review). Int J Mol Med, 2016,38(5):1319–1326
Kane GC, Stanson AW, Kalnicka D, et al. Comparison between gadolinium and iodine contrast for percutaneous intervention in atherosclerotic renal artery stenosis: clinical outcomes. Nephrol Dial Transplant, 2008,23(4):1233–1240
Remy-Jardin M, Bahepar J, Lafitte JJ, et al. Multi-detector row CT angiography of pulmonary circulation with gadolinium-based contrast agents: prospective evaluation in 60 patients. Radiology, 2006,238(3):1022–1035
Patino M, Parakh A, Lo GC, et al. Virtual Monochromatic Dual-Energy Aortoiliac CT Angiography With Reduced Iodine Dose: A Prospective Randomized Study. AJR Am J Roentgenol, 2019,212(2):467–474
De Santis D, Eid M, De Cecco CN, et al. Dual-Energy Computed Tomography in Cardiothoracic Vascular Imaging. Radiol Clin North Am, 2018,56(4):521–534
Siegel MJ, Kaza RK, Bolus DN, et al. White Paper of the Society of Computed Body Tomography and Magnetic Resonance on Dual-Energy CT, Part 1: Technology and Terminology. J Comput Assist Tomogr, 2016,40(6):841–845
Deseive S, Pugliese F, Meave A, et al. Image quality and radiation dose of a prospectively electrocardiography-triggered high-pitch data acquisition strategy for coronary CT angiography: The multicenter, randomized PROTECTION IV study. J Cardiovasc Comput Tomogr, 2015,9(4):278–285
Flohr TG, Leng S, Yu L, et al. Dual-source spiral CT with pitch up to 3.2 and 75 ms temporal resolution: image reconstruction and assessment of image quality. Med Phys, 2009,36(12):5641–5653
Thurnher SA, Capelastegui A, Del Olmo FH, et al. Safety and effectiveness of single- versus triple-dose gadodiamide injection-enhanced MR angiography of the abdomen: a phase III double-blind multicenter study. Radiology, 2001,219(1):137–146
Chicoskie C, Tello R. Gadolinium-enhanced MDCT angiography of the abdomen: feasibility and limitations. AJR Am J Roentgenol, 2005,184(6):1821–1828
Nadjiri J, Pfeiffer D, Straeter AS, et al. Spectral Computed Tomography Angiography With a Gadolinium-based Contrast Agent: First Clinical Imaging Results in Cardiovascular Applications. J Thorac Imaging, 2018,33(4):246–253
Flynn MM, Parekh AN, Parikh MR, et al. Renal Safety of Intravenous Gadolinium-enhanced MRI in Patients Following Liver Transplantation. Transplantation, 2019,103(6):e159–e163
Rajiah P, Ciancibello L, Novak R, et al. Ultra-low dose contrast CT pulmonary angiography in oncology patients using a high-pitch helical dual-source technology. Diagn Interv Radiol, 2019,25(3):195–203
Silva M, Milanese G, Cobelli R, et al. CT angiography for pulmonary embolism in the emergency department: investigation of a protocol by 20 ml of high-concentration contrast medium. Radiol Med, 2020,125(2):137–144
Abujudeh HH, Kosaraju VK, Kaewlai R. Acute adverse reactions to gadopentetate dimeglumine and gadobenate dimeglumine: experience with 32,659 injections. AJR Am J Roentgenol, 2010,194(2):430–434
Aran S, Shaqdan KW, Abujudeh HH. Adverse allergic reactions to linear ionic gadolinium-based contrast agents: experience with 194, 400 injections. Clin Radiol, 2015,70(5):466–475
Bleicher AG, Kanal E. Assessment of adverse reaction rates to a newly approved MRI contrast agent: review of 23,553 administrations of gadobenate dimeglumine. AJR Am J Roentgenol, 2008,191(6):W307–311
Bruder O, Schneider S, Pilz G, et al. 2015 Update on Acute Adverse Reactions to Gadolinium based Contrast Agents in Cardiovascular MR. Large Multi-National and Multi-Ethnical Population Experience With 37788 Patients From the EuroCMR Registry. J Cardiovasc Magn Reson, 2015,17(1):58
Hunt CH, Hartman RP, Hesley GK. Frequency and severity of adverse effects of iodinated and gadolinium contrast materials: retrospective review of 456,930 doses. AJR Am J Roentgenol, 2009,193(4):1124–1127
Matsumura T, Hayakawa M, Shimada F, et al. Safety of gadopentetate dimeglumine after 120 million administrations over 25 years of clinical use. Magn Reson Med Sci, 2013,12(4):297–304
Uhlig J, Lucke C, Vliegenthart R, et al. Acute adverse events in cardiac MR imaging with gadolinium-based contrast agents: results from the European Society of Cardiovascular Radiology (ESCR) MRCT Registry in 72,839 patients. Eur Radiol, 2019,29(7):3686–3695
Young LK, Matthew SZ, Houston JG. Absence of potential gadolinium toxicity symptoms following 22,897 gadoteric acid (Dotarem(R)) examinations, including 3,209 performed on renally insufficient individuals. Eur Radiol, 2019,29(4):1922–1930
Haneder S, Kucharczyk W, Schoenberg SO, et al. Safety of magnetic resonance contrast media: a review with special focus on nephrogenic systemic fibrosis. Top Magn Reson Imaging, 2015,24(1):57–65
Murphy KJ, Brunberg JA, Cohan RH. Adverse reactions to gadolinium contrast media: a review of 36 cases. AJR Am J Roentgenol, 1996,167(4):847–849
Runge VM. Safety of approved MR contrast media for intravenous injection. J Magn Reson Imaging, 2000,12(2):205–213
Woolen SA, Shankar PR, Gagnier JJ, et al. Risk of Nephrogenic Systemic Fibrosis in Patients With Stage 4 or 5 Chronic Kidney Disease Receiving a Group II Gadolinium-Based Contrast Agent: A Systematic Review and Meta-analysis. JAMA Intern Med, 2020,180(2):223–230
Kanda T, Fukusato T, Matsuda M, et al. Gadolinium-based Contrast Agent Accumulates in the Brain Even in Subjects without Severe Renal Dysfunction: Evaluation of Autopsy Brain Specimens with Inductively Coupled Plasma Mass Spectroscopy. Radiology, 2015,276(1):228–232
Maximova N, Gregori M, Zennaro F, et al. Hepatic Gadolinium Deposition and Reversibility after Contrast Agent-enhanced MR Imaging of Pediatric Hematopoietic Stem Cell Transplant Recipients. Radiology, 2016,281(2):418–426
McDonald RJ, McDonald JS, Kallmes DF, et al. Gadolinium Deposition in Human Brain Tissues after Contrast-enhanced MR Imaging in Adult Patients without Intracranial Abnormalities. Radiology, 2017,285(2):546–554
Murata N, Gonzalez-Cuyar LF, Murata K, et al. Macrocyclic and Other Non-Group 1 Gadolinium Contrast Agents Deposit Low Levels of Gadolinium in Brain and Bone Tissue: Preliminary Results From 9 Patients With Normal Renal Function. Invest Radiol, 2016,51(7):447–453
McDonald RJ, McDonald JS, Kallmes DF, et al. Intracranial Gadolinium Deposition after Contrast-enhanced MR Imaging. Radiology, 2015,275(3):772–782
Layne KA, Dargan PI, Archer JRH, et al. Gadolinium deposition and the potential for toxicological sequelae — A literature review of issues surrounding gadolinium-based contrast agents. Br J Clin Pharmacol, 2018,84(11):2522–2534
Kanda T, Nakai Y, Oba H, et al. Gadolinium deposition in the brain. Magn Reson Imaging, 2016,34(10):1346–1350
Iliff JJ, Wang M, Liao Y, et al. A paravascular pathway facilitates CSF flow through the brain parenchyma and the clearance of interstitial solutes, including amyloid beta. Sci Transl Med, 2012,4(147):147ra111
Malikova H. Nephrogenic systemic fibrosis: the end of the story? Quant Imaging Med Surg, 2019,9(8):1470–1474
Taoka T, Naganawa S. Gadolinium-based Contrast Media, Cerebrospinal Fluid and the Glymphatic System: Possible Mechanisms for the Deposition of Gadolinium in the Brain. Magn Reson Med Sci, 2018,17(2):111–119
Esteban JM, Alonso A, Cervera V, et al. One-molar gadolinium chelate (gadobutrol) as a contrast agent for CT angiography of the thoracic and abdominal aorta. Eur Radiol, 2007,17(9):2394–2400
Becker CR, Hong C, Knez A, et al. Optimal contrast application for cardiac 4-detector-row computed tomography. Invest Radiol, 2003,38(11):690–694
Kalisz K, Buethe J, Saboo SS, et al. Artifacts at Cardiac CT: Physics and Solutions. Radiographics, 2016,36(7):2064–2083
Holmes DR, 3rd, Fletcher JG, Apel A, et al. Evaluation of non-linear blending in dual-energy computed tomography. Eur J Radiol, 2008,68(3):409–413
Silva AC, Morse BG, Hara AK, et al. Dual-energy (spectral) CT: applications in abdominal imaging. Radiographics, 2011,31(4):1031–1046, discussion 1047–1050
Behrendt FF, Schmidt B, Plumhans C, et al. Image fusion in dual energy computed tomography: effect on contrast enhancement, signal-to-noise ratio and image quality in computed tomography angiography. Invest Radiol, 2009,44(1):1–6
Grant KL, Flohr TG, Krauss B, et al. Assessment of an advanced image-based technique to calculate virtual monoenergetic computed tomographic images from a dual-energy examination to improve contrast-to-noise ratio in examinations using iodinated contrast media. Invest Radiol, 2014,49(9):586–592
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
The authors declare that there is no conflict of interest with any financial organization or corporation or individual that can inappropriately influence this work.
Additional information
This study was supported by grants from the Scientific Research Project of Hunan Health Commission in 2019 (No. B2019071) and the Scientific Research Project of Hunan Health Commission in 2020 (No. B20200059).
Rights and permissions
About this article
Cite this article
Xie, A., Sun, Wj., Zeng, Yf. et al. Gadolinium Enhances Dual-energy Computed Tomography Scan of Pulmonary Artery. CURR MED SCI 42, 1310–1318 (2022). https://doi.org/10.1007/s11596-022-2621-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11596-022-2621-5