Abstract
Objective
To validate and use the Chinese Version of the M. D. Anderson Symptom Inventory (MDASI-C) to assess the symptom burden of breast cancer patients in China.
Methods
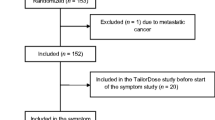
A total of 342 breast cancer patients in China participated in this study. Their symptoms were investigated with the MDASI-C from November 2020 to February 2021, and the reliability and validity of this tool were evaluated, respectively. Cluster analysis and correlation analysis were also performed.
Results
The Cronbach’s alpha coefficient values of the symptom and interference items were 0.827 and 0.880, respectively. Construct validity revealed a four-factor structure. The Kaiser—Meyer—Olkin value was 0.760. The Karnofsky Performance Status, treatment phase, and cancer stage of the patients were grouped, and the differences of scores within the groups were significant. In addition, the employment status, education level, and age of the patients were significantly correlated with the symptoms. The correlation analysis of the education level of the patients showed that most of the symptoms and interference items were reduced as the education level was increased. The top three symptoms were disturbed sleep (3.10±2.52), difficulty remembering (2.54±2.30), and fatigue (2.24±2.13). The clinical and biochemical indicators such as body mass index and neutral granulocyte lymphocyte ratio had effects on many symptoms. As the patients’ BMI increased, the patients’ pain, disturbed sleep, and difficulty remembering were aggravated, and numbness was alleviated.
Conclusion
The MDASI-C is a reliable and effective assessment tool to evaluate patients with breast cancer in China. The symptoms are related to many clinical and biochemical indicators.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Siegel RL, Miller KD, Fuchs HE, et al. Cancer Statistics, 2021. CA Cancer J Clin, 2021,71(1):7–33
Azim HA, Ibrahim AS. Breast cancer in Egypt, China and Chinese: statistics and beyond. J Thorac Dis, 2014, 6(7):864–866
Cao W, Chen HD, Yu YW, et al. Changing profiles of cancer burden worldwide and in China: a secondary analysis of the global cancer statistics 2020. Chin Med J (Engl), 2021,134(7):783–791
Kalter J, Verdonck-de Leeuw IM, et al. Effects and moderators of psychosocial interventions on quality of life, and emotional and social function in patients with cancer: An individual patient data meta-analysis of 22 RCTs. Psychooncology, 2018,27(4):1150–1161
Subramaniam S, Kong YC, Chinna K, et al. Health-related quality of life and psychological distress among cancer survivors in a middle-income country. Psychooncology, 2018,27(9):2172–2179
Wen FH, Chen JS, Chou WC, et al. Quality of life and psychological distress are differentially associated with distinct symptom-functional states in terminally ill cancer patients’ last year of life. Psychooncology, 2018,27(9):2111–2118
Pachman DR, Barton DL, Swetz KM, et al. Troublesome symptoms in cancer survivors: fatigue, insomnia, neuropathy, and pain. J Clin Oncol, 2012,30(30):3687–3696
Pandya C, Magnuson A, Dale W, et al. Association of falls with health-related quality of life (HRQOL) in older cancer survivors: A population based study. J Geriatr Oncol, 2016,7(3):201–210
Shapiro CL. Cancer Survivorship. N Engl J Med, 2018,379(25):2438–2450
Hamer J, McDonald R, Zhang L, et al. Quality of life (QOL) and symptom burden (SB) in patients with breast cancer. Support Care Cancer, 2017,25(2):409–419
Admiraal JM, van Nuenen FM, Burgerhof JG, et al. Cancer patients’ referral wish: effects of distress, problems, socio-demographic and illness-related variables and social support sufficiency. Psychooncology, 2016,25(11):1363–1370
Park EM, Deal AM, Check DK, et al. Parenting concerns, quality of life, and psychological distress in patients with advanced cancer. Psychooncology, 2016, 25(8):942–948
Saadatpour L, Hemati S, Habibi F, et al. Linguistic Validation of the M. D. Anderson Symptom Inventory in Persian-Speaking Iranian Cancer Patients. J Pain Symptom Manage, 2015,50(3):387–393.
Mendoza TR, Zhao F, Cleeland CS, et al. The validity and utility of the M. D. Anderson Symptom Inventory in patients with breast cancer: evidence from the symptom outcomes and practice patterns data from the eastern cooperative oncology group. Clin Breast Cancer, 2013, 13(5):325–334
Wang XS, Wang Y, Guo H, et al. Chinese version of the M. D. Anderson Symptom Inventory: validation and application of symptom measurement in cancer patients. Cancer, 2004,101(8):1890–1901
Wang XS, Cleeland CS, Mendoza TR, et al. Impact of cultural and linguistic factors on symptom reporting by patients with cancer. J Natl Cancer Inst, 2010,102(10): 732–738
Anshabo AT, Migbaru S, Mulu A, et al. Validation of the Amharic Version of the M. D. Anderson Symptom Inventory and Assessment of Symptoms in Ethiopian Cancer Patients. J Pain Symptom Manage, 2016,51(5):947–953
Guirimand F, Buyck JF, Lauwers-Allot E, et al. Cancer-related symptom assessment in France: validation of the French M. D. Anderson Symptom Inventory. J Pain Symptom Manage, 2010,39(4):721–733
Mystakidou K, Cleeland C, Tsilika E, et al. Greek M.D. Anderson Symptom Inventory: validation and utility in cancer patients. Oncology, 2004,67(3–4):203–210
Chen RW, Yang SL, Xu ZY, et al. Validation and Application of the Chinese Version of the M. D. Anderson Symptom Inventory Gastrointestinal Cancer Module (MDASI-GI-C). J Pain Symptom Manage, 2019,57(4):820–827
Lin CC, Chang AP, Cleeland CS, et al. Taiwanese version of the M. D. Anderson symptom inventory: symptom assessment in cancer patients. J Pain Symptom Manage, 2007,33(2):180–188
Aktas A, Walsh D, Kirkova J. The psychometric properties of cancer multisymptom assessment instruments: a clinical review. Support Care Cancer, 2015,23(7):2189–2202
Carvalho CS, Souza DS, Lopes JR, et al. Relationship between patient-generated subjective global assessment and survival in patients in palliative care. Ann Palliat Med, 2017,6(Suppl 1):S4–S12
Gulati RR. The Challenge of Cancer Pain Assessment. Ulster Med J, 2021,90(1):37–40
Lesley A, Henson M, Matthew Maddocks P, et al. Palliative care and the management of common distressing symptoms in advanced cancer: Pain, breathlessness, nausea and vomiting, and fatigue. J Clin Oncol, 2020,38(9):905–914
Cheung WY, Le LW, Gagliese L, et al. Age and gender differences in symptom intensity and symptom clusters among patients with metastatic cancer. Support Care Cancer, 2011,19(3):417–423
Nipp RD, Greer JA, El-Jawahri A, et al. Age and Gender Moderate the Impact of Early Palliative Care in Metastatic Non-Small Cell Lung Cancer. Oncologist, 2016,21(1):119–126
Chow E, Abdolell M, Panzarella T, et al. Predictive model for survival in patients with advanced cancer. J Clin Oncol, 2008,26(36):5863–5869
Chow S, Wan BA, Pidduck W, et al. Symptom clusters in patients with breast cancer receiving radiation therapy. Eur J Oncol Nurs, 2019,42:14–20
Sullivan CW, Leutwyler H, Dunn LB, et al. Stability of Symptom Clusters in Patients With Breast Cancer Receiving Chemotherapy. J Pain Symptom Manage, 2018,55(1):39–55
Rhondali W, Chisholm GB, Daneshmand M, et al. Association between body image dissatisfaction and weight loss among patients with advanced cancer and their caregivers: a preliminary report. J Pain Symptom Manage, 2013,45(6):1039–1049
Hwang SS, Chang VT, Rue M, et al. Multidimensional independent predictors of cancer-related fatigue. J Pain Symptom Manage, 2003,26(1):604–614
Strasser F, Blum D, von Moos R, et al. The effect of real-time electronic monitoring of patient-reported symptoms and clinical syndromes in outpatient workflow of medical oncologists: E-MOSAIC, a multicenter cluster-randomized phase III study (SAKK 95/06). Ann Oncol, 2016,27(2):324–332
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The authors declare that they have no conflicts of interest.
Additional information
This work was supported by the National Natural Science Foundation of China (No. 81672977).
Rights and permissions
About this article
Cite this article
Chen, Rw., Wang, Q., Hu, T. et al. Validation and Application of the Chinese Version of the M. D. Anderson Symptom Inventory in Breast Cancer Patients. CURR MED SCI 42, 426–433 (2022). https://doi.org/10.1007/s11596-022-2544-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11596-022-2544-1