Abstract
Hepatocellular carcinoma (HCC) is among the most frequently occurring cancers and the leading causes of cancer mortality worldwide. Identification of the signaling pathways regulating liver carcinogenesis is critical for developing novel chemoprevention and targeted therapies. C-Jun N-terminal kinase (JNK) is a member of a larger group of serine/threonine (Ser/Thr) protein kinases known as the mitogen-activated protein kinase (MAPK) family. JNK is an important signaling component that converts external stimuli into a wide range of cellular responses, including cell proliferation, differentiation, survival, migration, invasion, and apoptosis, as well as the development of inflammation, fibrosis, cancer growth, and metabolic diseases. Because of the essential roles of JNK in these cellular functions, deregulated JNK is often found to contribute to the development of HCC. Recently, the functions and molecular mechanisms of JNK in HCC development have been addressed using mouse models and human HCC cell lines. Furthermore, recent studies demonstrate that the activation of JNK by oncogenes can promote the development of cancers by regulating the transforming growth factor (TGF)-β/Smad pathway, which makes the oncogenes/JNK/Smad signaling pathway an attractive target for cancer therapy. Additionally, JNK-targeted therapy has a broad potential for clinical applications. In summary, we are convinced that promising new avenues for the treatment of HCC by targeting JNK are on the horizon, which will undoubtedly lead to better, more effective, and faster therapies in the years to come.

Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
Hepatocellular carcinoma (HCC) is the fifth most common cancer and the third leading cause of cancer-related death [1]. The most prominent factors associated with HCC include chronic hepatitis B viral (HBV) and hepatitis C viral (HCV) infection, chronic alcohol consumption, aflatoxin-B1-contaminated food, and virtually all cirrhosis-inducing conditions [2–4]. Other etiological factors with lower frequencies have also been proposed for HCC, including long-term oral contraceptive use in women, certain metabolic disorders, diabetes, and non-alcoholic fatty liver disease (NAFLD) [5, 6]. In addition, gender can also influence the risk and behavior of HCC, because men account for a larger fraction of cases [2]. HBV or HCV infection-induced hepatitis is the most important risk factor for HCC development. In the mainland of China, more than 90 % of HCC patients are diagnosed with an HBV infection.
The molecular analysis of human HCC has identified many genetic and epigenetic alterations that result in the deregulation of key oncogenes and tumor-suppressor genes, including transforming growth factor (TGF)-β, tumor protein P53 (TP53), β-cadherin-associated protein (β-catenin), ErbB receptor family members, Met and its ligand hepatocyte growth factor (HGF), p16 (INK4a), E-cadherin, and cyclooxygenase 2 (COX2) [2, 7]. Notably, many of these deregulated genes have been reported to be associated with an important signaling pathway, the c-Jun N-terminal kinase (JNK) pathway. In the present review, the roles of JNK in HCC development and the potential of targeting JNK for the treatment of HCC are discussed.
2 JNK Family Kinases
JNK is a member of a larger group of serine/threonine (Ser/Thr) protein kinases known as the mitogen-activated protein kinase (MAPK) family [8]. The JNK proteins are also known as stress-activated protein kinases (SAPKs), and their enzymatic activity is induced in response to diverse stimuli, such as cytokines (tumor necrosis factor [TNF], interleukin-1[IL-1], TGF-β, platelet-derived growth factor [PDGF], epidermal growth factor [EGF]), intra- and extracellular pathogens (lipopolysaccharide [LPS], peptidoglycan, and bacterial unmethylated CpG-DNA that activates Toll-like receptors [TLRs]), reactive oxygen species (ROS), pathological and environmental stress (ischemia, hypoxia, and ultraviolet and ionizing radiation), toxins, drugs, endoplasmic reticulum (ER) stress, and metabolic changes, including obesity and hyperlipidemia [Reviewed in 9].
A host of MAP kinase kinase kinases (MAP3Ks), such as members of the MEKK family, the mixed-lineage kinase family, the apoptosis signal-regulating kinase family, transforming growth factor β-activated kinase 1 (TAK1) and tumor progression locus 2 (TPL2), serve as proximal conduits for the diverse signals that activate the JNK pathway. These kinases phosphorylate and activate two distinct MAP kinase kinases (MAP2Ks), MKK4 and MKK7, which directly phosphorylate JNKs on threonine 183 (Thr183) and tyrosine (Tyr185) residues in a conserved tripeptide motif (Thr-Pro-Tyr) within their activation loop [10]. Moreover, the kinase activity of JNKs is regulated by interaction with scaffold proteins [11], as well as dual-specificity phosphatases [12] and nuclear factor-kB (NF-kB) transcription factors [13].
There are three isoforms of JNK in mammals: JNK1, JNK2, and JNK3 (encoded by MAPK8, MAPK9, and MAPK10, respectively). The JNK proteins, including splicing variants, range from 46 kDa to 55 kDa in size. Alternative splicing of these genes results in at least 10 different transcriptional isoforms [14]. Specifically, four splice forms (JNK1α1, JNK1β1, JNK1α2, JNK1β2) arise from the JNK1 gene, four (JNK2α1, JNK2β1, JNK2α2, JNK2β2) arise from the JNK2 gene, and two (JNK3α1, JNK3α2) arise from the JNK3 gene [15].
Upon activation by upstream MKK4/7, JNKs phosphorylate and activate a number of nuclear and non-nuclear proteins. To date, at least 50 proteins have been identified as JNK substrates. Phosphorylation can modulate the substrate protein activity in a positive (c-Jun, JunB, JunD, activating transcription factor 2 [ATF2], ets-like protein 1 [ElK1], c-Myc, p53, nuclear factor of activated T-cells, cytoplasmic, calcineurin-dependent [NFATc]2, forkhead box O4 [FOXO4], signal transducer and activator of transcription 3 [STAT]3, STAT1, paired box 2 [Pax2], T-cell factor [TCF]-β1 and heterogeneous nuclear ribonucleoprotein K [hnRNP-K]), negative (Net, heat shock transcription factor 1 [HSF1], NFATc3, NFATc1α, peroxisome proliferator-activated receptor gamma 1 [PPARγ1], Glucocorticoid R, retinoic acid receptor alpha [RARα], Androgen R, nuclear receptor 77 [Nur77], transcription initiation factor IA [TIFIA], insulin receptor substrate 1 [IRS-1], B-cell cll/lymphoma 2 [Bcl-2], myeloid cell leukemia 1 [Mcl-1], Bcl-2-like 1 [Bcl-XL], Bcl-2-associated agonist of cell death [Bad], superior cervical ganglion-10 protein [SCG10], Tau and Kinesin), or modulating (retinoid x receptor α [RXRα], JNK-interacting protein 1 [JIP1], pol delta C subunit [p66] and 14-3-3) fashion. JNK binding can even modulate the activity of some target proteins in a phosphorylation-independent manner (e.g., degradation of c-Jun, ATF2, p53, and c-Myc) [Reviewed in 9, 15, 16]. Previous studies revealed that TGF-β and Ras differentially activated TGF-β type I receptor (TβRI) and JNK, which converted the common mediator Smad2/3 into two distinctive phospho-isoforms: C-terminally phosphorylated Smad2/3 (pSmad2/3C) and linker-phosphorylated Smad2/3 (pSmad2/3L). JNK is also responsible for the phosphorylation of Smad2/3L [17]. In some cases, the consequences of phosphorylation by JNK have not yet been defined (Jun dimerization protein 2 [JDP2], JNK-interacting protein 3 [JIP3], SH3BP5 [Sab], microtubule-associated protein 1B [MAP-1B], Keratin 8, and amyloid β-precursor) [Reviewed in 15] (Table 1). These proteins control multiple cellular processes, such as cell proliferation, apoptosis and survival, differentiation, acting as transcription factors, controlling protein degradation, localization, and signaling. Furthermore, recent studies using genetically engineered mice showed that the loss or hyper-activation of the JNK pathway contributes to the development of inflammation, fibrosis, cancer growth, and metabolic diseases that include obesity, hepatic steatosis, and insulin resistance [9] (Fig. 1).
Activation of JNK signaling pathways is involved in HCC tumorigenesis and tumor progression. Diverse stimuli can activate JNK through the upstream molecules, and the phosphorylated JNK activates a number of downstream nuclear and non-nuclear proteins involved in HCC cellular activities, including cell proliferation, differentiation, apoptosis, survival, migration, invasion, fibrosis, and inflammation. Abbreviations: JNK, c-Jun N-terminal kinase; HCC, Hepatocellular carcinoma; TNF, tumor necrosis factor; IL-1, interleukin-1; TGF-β, transforming growth factor β; PDGF, platelet-derived growth factor; EGF, epidermal growth factor; LPS, lipopolysaccharide; ROS, reactive oxygen species; ER, endoplasmic reticulum; MLKs, mixed lineage kinases; TAK1, transforming growth factor β-activated kinase 1; MAP3Ks, MAP kinase kinase kinases; ASK1, apoptosis signal‑regulating kinase 1; ATF2, activating transcription factor 2; ElK1, ets-like protein 1; Smad3L, linker region of Smad3; NFATc1, nuclear factor of activated T-cells, cytoplasmic, calcineurin-dependent 1; NFAT4, nuclear factor of activated T-cells 4; TCF-β1, T-cell factor β1; PPARγ1, peroxisome proliferator-activated receptor gamma 1; RARα, retinoic acid receptor α; RXRα, retinoid x receptor α; Nur77, nuclear receptor 77; TIFIA; transcription initiation factor IA; IRS-1, insulin receptor substrate 1; MAP-1B, microtubule-associated protein 1B; Pax2, paired box 2; SCG10, superior cervical ganglion-10 protein; Smad2L, linker region of Smad2; Bcl-2, B-cell cll/lymphoma 2; Bcl-XL, Bcl-2-like 1; Mcl-1, myeloid cell leukemia 1; Bad, Bcl-2-associated agonist of cell death; FOXO4, forkhead box O4; p66, pol delta C subunit; Sab, SH3BP5; hnRNP-K, heterogeneous nuclear ribonucleoprotein K
3 The Roles of JNK Pathway in Cancer Development
The transforming actions of several oncogenes such as Ras, c-fos, Met, Bcr-Abl, and mutant HER2 also could be JNK dependent [18–22], which suggests that JNK signaling contributes to the cellular transformation that supports the development of various cancers. A substantial body of evidence indicates that JNK activation is required for transformation induced by Ras, an oncogene that is activated by mutation in almost 30 % of human cancers, and N-Ras mutations were found in HCC, melanoma, and hematologic malignancies [23]. Ras induces phosphorylation of c-Jun on the same serine residues phosphorylated by JNK [18, 24], and acts cooperatively with c-Jun to enhance cellular transformation [25]. Moreover, fibroblasts from mice harboring a mutated c-Jun allele that lacks the JNK phosphorylation sites (JunAA) were resistant to transformation induced by activated Ras and Fos [21]. c-Fos induced osteosarcomas and skin tumors induced by chronic activation of the Ras pathway were reduced in JunAA mice [22]. In 1997, Rodrigues et al. found that the activation of the JNK pathway is essential for transformation by the Met oncogene [20]. Bcr-Abl, a leukemia oncogene, preferentially activated JNK, and also enhanced the activity of Jun-responsive promoters through a Ras- and JNK-dependent pathway, and dominant-negative mutants of Jun inhibit the transforming activity of Bcr-Abl [19]. Oncogenic HER2 and H-Ras could induce TGF-β secretion through the JNK/activator protein (AP)-1 pathway in mammary epithelial cells, which suggests that oncogenic HER2 and H-Ras promote the development of breast cancer by activating the JNK signaling pathway [26]. Differentiation and apoptosis mediated by the tumor-suppressive pSmad3C pathway are blocked by the oncogenic Ras/JNK/pSmad3L pathway [27]. This blockage is a frequent theme in the development of gastrointestinal malignancies [17]. Phospho-Smad3 signaling confers a selective advantage upon tumor cells by shifting from the tumor-suppressive TβRI/pSmad3C pathway to the oncogenic JNK/pSmad3L pathway during sporadic human colorectal carcinogenesis [28]. This observation has been extended to hepatic carcinogenesis [29, 30]. The phenotypes of benign tumors are dictated by genotype, and tumorigenic growth is essentially a cell-autonomous phenomenon that involves the constitutive shift induced by alterations in the Ras oncogene. Collectively, all these data indicate that JNK activity is necessary for efficient transformation and tumorigenesis by these oncogenes.
4 JNK1 Rather than JNK2 Is more Critical for the Development of HCC
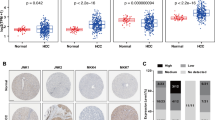
In 2002, Tsutsumi et al. revealed that the development of HCV-associated HCC occurred through the activation of JNK and its downstream effector, AP-1 [31]. There were only a few scattered reports suggesting the potential involvement of JNK in HCC during the subsequent decade. Since that study, numerous studies have confirmed that JNK plays a key role in the progression and tumorigenesis of HCC by regulating various biological functions in cells. JNK1 and JNK2 are expressed in most tissues, whereas JNK3 is mainly expressed in the brain, heart, and testes [10, 16]. This tissue-specific distribution, particularly for JNK3 expression, has led to the idea that different isoforms may perform different cellular roles. There are two isoforms of JNK expressed in HCC tissues: JNK1 and JNK2. Several biochemical experiments have revealed that JNK1, rather than JNK2, is the primary kinase in stress-induced phosphorylation of c-Jun, and several other studies also demonstrated JNK1 is more important than JNK2. In 2006, Sakurai et al. showed that in mice with DEN-induced HCC, NF-kB attenuates liver carcinogenesis by repressing JNK1 activation and that JNK1−/− mice exhibit reduced liver cancers [32]. A single injection of DEN to young mice induces HCC at the age of 8–10 months, while JNK1 deficiency protects mice from DEN-induced hepatocyte death, which resulted in reduced proliferation and HCC formation [32]. Later, in 2008, Hui et al. showed that activation of JNK1, but not JNK2, was increased in human primary HCC [33]. In both of the studies that used the DEN phenobarbital protocol, JNK1−/− mice developed fewer and smaller liver tumors than wildtype or JNK2−/− mice [32, 33]. Therefore, JNK1 was required for human HCC cell proliferation in vitro and tumorigenesis after xenotransplantation. In addition, in mouse models of liver carcinogenesis or regeneration, mice lacking JNK1 displayed decreased tumor cell proliferation [32, 33]. Consistent with the results of Hui et al., in 2009, Chang and colleagues found that enhanced JNK1 activation occurred in 17 out of 31 HCC samples (55 %) relative to the corresponding adjacent non-cancerous tissues, whereas JNK2 activation was roughly equal between HCC and adjacent non-cancerous tissues [34]. The authors also showed that the activation of JNK1 led to an elevated expression of genes regulating cell growth and a decreased expression of the genes for cell differentiation in HCC [34]. The above data reveal a clear correlation between HCC and JNK1. Therefore, targeting JNK1 should be viewed as a new avenue for HCC therapy.
The progressive role of JNK in HCC has been confirmed by pharmacological inhibition of JNK and studies of human HCC cells. However, Davis and coworkers showed contradictory results. They reported an analysis of mice with tissue-specific deficiency of JNK and mice with a compound deficiency of both JNK1 and JNK2, and these analyses indicated that another mechanism must account for the protumorigenic effects of JNK in HCC development. Their results showed that compound JNK deficiency in hepatocytes did not reduce DEN-induced HCC, but compound JNK deficiency in hepatocytes, as well as nonparenchymal cells did reduce DEN-induced HCC. Their work provided important insight into the mechanism of JNK-promoted HCC development [35]. Additional studies by this group revealed that JNK in nonparenchymal cells promotes HCC development by providing an inflammatory environment that supports HCC, including the expression of the protumorigenic cytokines interleukin 6 (IL-6) and TNF-α that contribute to compensatory hepatocyte proliferation [35]. However, JNK in hepatocytes reduces HCC development by promoting hepatocyte survival, which decreases IL-1α release by necrotic hepatocytes and the activation of hepatic innate immune cells, including Kupffer cells, which express the protumorgenic cytokine IL-6 [35]. The study by Davis and coworkers demonstrates that JNK plays a complex role in the development of HCC. It is likely that previous studies using mice with a whole-body knockout of JNK1 or JNK2 reflected a composite phenotype derived from the cell type-specific functions of JNK in hepatocytes and nonparenchymal cells. In summary, all the studies have implications for a more general role for JNK in cancer. Both tumor promotion and inhibition by JNK may contribute to cancer development [10, 36]. These different outcomes complicate the analysis of JNK pathway mutations that have been identified in human cancers [37, 38]. Additionally, this dual role of JNK should be considered in the context of the potential uses for JNK as a therapeutic target for drug development and the treatment of human cancer.
5 Various Molecules Regulate HCC Development through JNK Signaling Pathways
As HBV or HCV infection, non-alcoholic steatohepatitis (NASH), or cirrhosis can develop into HCC, a number of reports suggested that the gene products of HBV and HCV, and NASH were involved in the activation of JNK. In 2005, Guo et al. used immunohistochemical and in situ hybridization techniques to study the role of JNK in HCC with or without HBV infection, and demonstrated positive staining in nuclei for the phosphorylation of JNK in 70 % of HCC tissues, but not in adjacent non-tumor tissues, which indicated that JNK activation may play an important role in the pathogenesis of HBV-associated HCC [39]. P21-activated protein kinase (Pak1), a main downstream effector of the small Rho GTPases Rac1 and cell division cycle 42 (Cdc42), plays an important role in the regulation of cell morphogenesis, motility, mitosis, and angiogenesis. A previous study documented that Pak1 was overexpressed in HCC and played an important role in the metastasis of HCC. Most importantly, the mechanism by which Pak1 induced cancer metastasis involved the activation of JNK [40]. In addition to HBV and Pak1, studies have shown that many factors such as HCV, acetaldehyde, alcohol, CD147, KITENIN, inhibit cytokine-dependent inducible nitric oxide synthase (iNOS), LPS, CYLD, and platelets could promote the proliferation, migration, invasion, or metastasis of HCC through the activation of JNK [41–47]. Furthermore, some other molecules, such as the aqueous extract of butea monosperma flowers, lipocalin 2 (Lcn2), isomalto oligosaccharide (IMOS), heat shock protein 20 (HSP20), Sorafenib, LK-A, and salinomycin, could reduce the development of HCC by inhibiting of JNK [48–54]. These studies suggest that the JNK pathway can regulate different cellular activities involved in HCC. LPS, one of the promoters of JNK activation, was well studied recently. While previous studies have shown that TLR4 is involved in hepatocarcinogenesis, the role of TLR4 in cancer cell survival and proliferation in HCC remains unclear. In 2013, Wang et al. revealed that LPS-induced activation of TLR4-JNK signaling pathway promoted the proliferation of HCC cells [45]. Furthermore, Li et al. and Dong et al. found that TLR4-JNK signaling was required for LPS-induced epithelial-mesenchymal transition (EMT), tumor cell invasion or metastasis, which ultimately provided molecular insights into LPS-related pathogenesis and a basis for developing new strategies against metastasis in HCC [55, 56].
6 MUC1 Promotes the Development of HCC by Activating the JNK/Smad Pathway
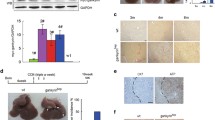
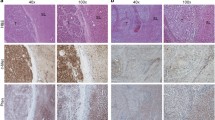
A recent study found that JNK was activated by oncoprotein Mucin 1 (MUC1), and could mediate autocrine TGF-β signaling in HCC cells [7]. MUC1 is a transmembrane glycoprotein that is expressed on the apical surface of epithelial cells and is aberrantly overexpressed in most epithelial malignant tumors and some hematological malignant tumors. MUC1 promotes the progression and tumorigenesis of many human adenocarcinomas [57–61]. Various studies have shown that MUC1 is overexpressed in HCC cells and tissues [62, 63]. Previous results revealed that MUC1 gene silencing inhibited the growth of the SMMC-7721 HCC cell line in vivo and in vitro, which suggests that MUC1 plays a key role in HCC tumorigenesis. MUC1 is involved in many signaling pathways other than JNK [64], including Wnt/β-catenin [65], c-terminal Src kinase (c-Src) [66], growth factor receptor-bound protein 2 (Grb2)/son of sevenless (Sos) [67], PI3K/AKT [58], p53 [68], glycogen synthase kinase 3β (GSK3β) [69], epidermal growth factor receptor (EGFR) [70, 71], and NF-kB [72], to regulate the processes of cell survival, proliferation, and apoptosis. However, the downstream pathway by which activated JNK could regulate the biological function of HCC is still unclear. A series of studies has shown that JNK signaling communicates closely with TGF-β signaling to regulate hepatic carcinogenesis [29, 30, 73]. Reports showed that MUC1 overexpression in HCC cells reduced TGF-β-dependent tumor-suppressive activity by TβRI/pSmad3C/p21(WAF1), while promoted the proliferation of HCC cells by directly activated JNK/pSmad3L/c-Myc. Conversely, MUC1 gene silencing in MUC1 expressing HCC cells resulted in preserved tumor-suppressive functions via pSmad3C, while eliminated pSmad3L-mediated oncogenic activity both in vitro and in vivo. A high correlation between MUC1 and JNK/pSmad3L/c-Myc, but not TβRI/pSmad3C/p21(WAF1) expression was observed in HCC tissues from patients. Collectively, these results indicate that the activated JNK by MUC1 shifts Smad3 signaling from a tumor-suppressive pSmad3C/p21(WAF1) to an oncogenic pSmad3L/c-Myc pathway in HCC cells [74] (Fig. 2). Consistent with these studies, Nagata et al. also found that the JNK inhibitor SP600125 significantly prolonged the median survival time in rat model of DEN-induced HCC [73]. As JNK/pSmad3L/c-Myc was enhanced in the rat hepatocytes exposed to DEN, while TβRI/pSmad3C/p21(WAF1) was impaired as DEN-induced HCC developed and progressed, the specific inhibition of JNK activity by SP600125 suppressed pSmad3L/c-Myc in the damaged hepatocytes and enhanced pSmad3C/p21(WAF1) by acting as a tumor suppressor in normal hepatocytes [73]. Further investigation demonstrated that MUC1-mediated JNK activation not only enhanced the phosphorylation of Smad2 at C-terminal (Smad2C) through TGF-β/TβRI, but also directly enhanced the phosphorylation of Smad2 at linker region (Smad2L), and then both of them collaborate to upregulate matrix metalloproteinase (MMP)-9-mediated cell migration and invasion of HCC [75] (Fig. 2). Together, these results uncovered a new signaling pathway in which oncogenes are upstream of JNK and the TGF-β/Smad pathway is downstream of JNK, and oncogenes are the upstream switch of JNK activity in tumor cells. In summary, all of these recent studies demonstrate that oncogenic transformation by MUC1 is mediated by the activation of JNK in HCC. The findings from all these studies have led to the hypothesis that oncogenes could promote the development of various cancers by activating JNK signaling pathways, which makes JNK just as an attractive target as oncogenes for cancer therapy.
MUC1 promotes the progression and tumorigenesis of HCC through the activation of JNK. MUC1 enhances the expression of the autocrine TGF-β1 by directly activating the JNK/AP-1 pathway in HCC cells, and MUC1-mediated JNK activation not only enhances the phosphorylation of Smad2C through TGF-β/TβRI, but also directly enhances the phosphorylation of Smad2L, and then pSmad2L/C collaborates to upregulate matrix metalloproteinase (MMP)-9-mediated cell migration and invasion of HCC. Furthermore, MUC1 directly activates JNK/pSmad3L/c-Myc, while suppressing TβRI/pSmad3C/p21(WAF1), which indicates that MUC1 can shift Smad3 signaling from a tumor-suppressive pSmad3C/p21(WAF1) to an oncogenic pSmad3L/c-Myc pathway by directly activating JNK in HCC cells. Abbreviations: MUC1, mucin 1; MUC1-CT, the cytoplasmic tail of MUC1; HCC, hepatocellular carcinoma; JNK, c-Jun N-terminal kinase; TGF-β1, transforming growth factor β1; AP-1, activator protein-1; TβRI, TGF-β type I receptor; Smad2C, the C-terminal of Smad2; Smad2L, the linker region of Smad2; pSmad2C, C-terminally phosphorylated Smad2; pSmad2L, linker-phosphorylated Smad2; MMP-9, matrix metalloproteinase-9; pSmad3L, linker-phosphorylated Smad3; pSmad3C, C-terminally phosphorylated Smad3
Clinical analyses of pSmad3L and pSmad3C in human tumor development have provided substantial insight into relevant mechanisms. For example, human livers infected by HCV progress from chronic hepatitis C through cirrhosis to HCC several decades later. Specimens from patients with chronic hepatitis C who develop HCC show abundant Smad3L but limited Smad3C phosphorylation in hepatocytic nuclei, while other patients with abundant hepatocytic pSmad3C but limited pSmad3L do not develop HCC [29]. The same relationships were observed in human HBV-related hepatocarcinogenesis [30]. These clinical observations point to roles for pSmad3C as a tumor suppressor and pSmad3L as a promoter during carcinogenesis. Therefore, pSmad3L and pSmad3C could function as biomarkers for the prediction of cancer risk in humans.
An improved understanding of Smad phospho-isoform signaling during human carcinogenesis suggests better ways to prevent human cancer development, exemplifying laboratory-driven translational research. A key question concerning the effectiveness of therapy for preventing liver HCC development is whether such a therapy still has value once pre-neoplastic hepatocytes have appeared. Molecular analyses of paired liver biopsy specimens enabled us to predict HCC risk after HCV clearance. Specimens from HCV-related chronic liver diseases can be divided into two subgroups based on phospho-Smad3 profiles [76]. One group carried a risk of HCC after HCV clearance, while another carried a lower risk of HCC occurrence. This grouping explains the observation that some patients with HCV-related liver disease respond effectively to antiviral therapy in terms of reversal from carcinogenic pSmad3L to tumor-suppressive pSmad3C signaling, while others do not. Irrespective of HCV clearance, patients with cirrhosis who maintain strong pSmad3L signaling in hepatocytic nuclei require continued close follow-up because the HCC risk is likely to persist. Deng et al. recently demonstrated reversibility of phospho-Smad3 signaling in stepwise human HBV-related carcinogenesis after anti-HBV therapy [77]. All the findings suggest that pSmad3L and pSmad3C are useful biomarkers for assessing the effectiveness of interventions aimed at reducing cancer risk in humans.
7 The Role of JNK Activation in HCC Apoptosis: A Double-Edged Sword
Apoptosis represents a physiological way to eliminate excess cells during both liver development and regeneration [78]. Apoptotic signaling within the cell is transduced mainly via two molecular pathways: the death receptor pathway and the mitochondrial pathway. Apoptotic events in hepatocytes can be regulated by different stimuli that bind to death receptors in the cell membrane, such as Fas ligand (FasL), TNF-α, or TNF-related apoptosis-inducing ligand (TRAIL) [79]. Furthermore, other factors, such as TGF-β, HGF, fibroblast growth factors (FGFs), EGF, heparin-binding EGF-like growth factor (HB-EGF), TNF-α, amphiregulin and others, do not bind to death receptors, but intracellular signals do couple to the apoptotic machinery through activation of the mitochondrial pathway [80]. Many pathways are involved in apoptosis, including p53, PI3K (phosphoinositide 3-kinase)/protein kinase B (AKT), extracellular regulated protein kinase (ERK), P38 MAPK, NF-kB, and TGF-β/Smad, among others [80]. Previous studies showed that both Aplidin and celastrol, which have anti-cancer activities, could induce apoptosis of human breast cancer and multiple myeloma cells through activation of the JNK signaling pathway [81, 82], which indicates that the JNK pathway is also involved in apoptosis. JNK phosphorylates and activates the BH3-only proteins Bim and Bad as well as the proapoptotic Bcl-2 protein Bax, which directly triggers the mitochondrial apoptotic pathway [83–85]. Finally, research has shown that JNK induces Fas and DR5 expression by sensitizing steatotic hepatocytes to circulating Fas or TRAIL-mediated toxicity [86, 87]. Indeed, insufficient apoptosis has been associated with the development and progression of HCC [80]. In 2003, Qi et al. showed that the activation of p53 and JNK signalings by Notch1 inhibited the growth of HCC through induction of the cell cycle arrest and apoptosis [88]. Since that study, JNK signaling-associated apoptosis in HCC was well studied. Sorafenib, as the first molecular targeted agent that showed survival benefit for patients with advanced HCC, could induce apoptosis of HCC cells through the activation of JNK signaling [89]. In addition, Adiponectin treatment resulted in increased apoptosis of HCC cells via the activation of caspase-3 and JNK, and inhibition of JNK-phosphorylation inhibited adiponectin-induced apoptosis and caspase-3 activation [90]. As ROS can induce the activation of JNK, several studies showed that activating the ROS/JNK signaling pathways could promote apoptosis in HCC induced by different factors, such as 8-Bromo-7-methoxychrysin, Longikaurin A (LK-A), and Wentilactone B, and the applying of ROS and JNK inhibitors could markedly reverse the apoptosis [48, 91, 92]. Furthermore, TRAIL induces apoptosis in a wide range of malignant cells. However, several cancers, including HCC, exhibit a major resistance to TRAIL-induced cell death. Wang et al. found that in the presence of melittin, TRAIL-induced apoptosis is significantly increased in TRAIL-resistant HCC cells, which may be attributed to melittin-induced TAK1-JNK/p38 activation and melittin-mediated inhibition of IkappaBalpha kinase-NfkappaB [93]. Consistent with these results, Song et al. also found that inhibition of MKK7-JNK by the TOR signaling pathway regulator-like protein contributed to the resistance of HCC cells to TRAIL-induced apoptosis [94]. All these results reveal that the activation of JNK can promote apoptosis of HCC cells.
NAFLD is a group of syndromes ranging from hepatic steatosis to more severe forms, including NASH and cirrhosis, which may further progress to HCC [95]. NAFLD is strongly associated with an increased level of serum free fatty acids (FFAs), and report shows that the FFAs levels are increased in patients with NASH and correlate with disease severity [96]. Apoptosis or programmed cell death is a morphologic and pathogenic hallmark of NASH [97, 98], which in the context of NAFLD, and secondary to its association with excess lipid deposition, is referred to as lipoapoptosis. Lipoapoptosis is a key pathogenic process in NAFLD, and the severity of NAFLD correlates with the degree of hepatocyte lipoapoptosis [97]. Multiple studies suggest that an elevated concentration of FFAs in the circulation plays a key role in stimulating lipoapoptosis in liver cells [83, 99, 100]. Of the three mammalian JNK genes, only JNK1 and JNK2 are expressed in the liver [101]. JNK activity was increased in experimental murine dietary and genetic models of NASH [102–104] as well as in patients with NASH, and JNK activity correlates with the degree of apoptosis [105]. Activation of the JNK signaling pathway has been implicated as a central mediator of FFA-induced hepatocyte lipoapoptosis in both rodents and human steatohepatitis [103–105]. Alternatively, JNK can post-transcriptionally activate the pro-apoptotic members of the Bcl-2 family Bim, Bad, and Bax [84, 106, 107], or inactivate the anti-apoptotic members of this family Bcl-2 and Bcl-XL [108]. In addition, both JNK1 and JNK2 have been implicated in insulin resistance, although JNK1 is more strongly associated with steatohepatitis [103, 104]. Genetic deletion of JNK1 prevents FFA-mediated c-Jun activation and p53-upregulated modulator of apoptosis (PUMA) induction by FFA [109]. A study showed that SP600125, a JNK inhibitor, decreased lipoapoptosis in vitro [109, 110] by attenuating saturated FFA induced PUMA induction [109]. In summary, because lipoapoptosis is a key player in the progression of NAFLD, which is a high-risk factor for HCC, targeting the JNK signaling pathway would be useful to halt disease progression.
Nevertheless, the results from Mucha et al. were the opposite. They showed that inhibited JNK by SP600125 caused cell cycle arrest, enhanced caspase recruitment, and greatly sensitized HCC cells, but not normal hepatocytes, to TRAIL [111]. In 2008, Aderca et al. also showed that the JNK inhibitor SP600129 enhances apoptosis of HCC cells induced by the tumor suppressor WW domain containing oxidoreductase (WWOX) [112]. All these results indicate that the function of JNK in apoptosis is complex, and JNK may have a proapoptotic, antiapoptotic, or no role in the process. It is most likely that JNK activation modulates the apoptotic process in a cell type- and stimulus-dependent manner, and this work highlights the importance of understanding fully both the roles of JNK and the molecular basis for the distinct functions of JNK.
8 JNK Targeting for Potential Clinical Applications
The contributions of JNK in HCC pathogenesis strongly suggest that JNK signaling could be a promising target for developing novel chemoprevention and targeted therapies for HCC. To date, many small molecule inhibitors that might modulate specific components of JNK signaling have been developed. These inhibitors can be broadly classified into two categories: ATP-competitive inhibitors and ATP-non-competitive inhibitors (Tables 2 and 3).
8.1 ATP-Competitive Inhibitors
SP600125, one of the earliest and most commonly used ATP-competitive JNK inhibitors, is an anthrapyrazolone derivative that exhibited high efficacy in blocking the kinase activity of JNK1, JNK2, and JNK3 [157]. It was developed by Celgene for the treatment of auto-immune, inflammatory, and neurodegenerative diseases, and intriguing anticancer properties were recently described [157, 158]. SP600125 can inhibit the inflammatory response in vivo and showed promise as a potential therapeutic agent for rheumatoid arthritis and asthma in humans [113, 114]. Reports showed that SP600125 modified cell cycle progression induced cell apoptosis and cell cycle arrest and increased cell sensitivity to various anti-proliferative drugs [48, 115–123]. When SP600125 was combined with some chemotherapy drugs, such as TRAIL and gartanin, cell apoptosis was increased in human HCC cultures [111, 124]. Furthermore, in a rat DEN-induced HCC model, the administration of SP600125 reduced the number and size of HCC tumors [73]. All the reported mechanisms of action make SP600125 an ideal candidate for developing new therapies against HCC. However, additional data showed that SP600125 binds to a range of kinases in phage interaction screening assays [159], which suggests there may be many additional kinase targets of SP600125. Despite concerns about the specificity of SP600125, it has good potential as an anti-cancer therapeutic agent and will be further investigated because of its continued usefulness for in vivo studies with minimal toxicity or few undesirable side effects.
CC-401, a second generation of ATP-competitive anthrapyrazolone JNK inhibitor targeting JNK1/2/3, was developed by Celgene based on the chemistry of SP600125. Uehara et al. showed that CC-401 decreased hepatic necrosis and apoptosis after orthotopic liver transplantation, while Vasilevskaya et al. showed that CC-401 treatment resulted in greater DNA damage and delayed tumor growth when combined with bevacizumab and oxaliplatin in mouse xenografts [125, 126]. In addition, CC-401 has been used in models of liver injury and significantly improved rat survival rates from 40 % (vehicle) to 80 % (CC-401, 10 mg/kg) and 100 % (CC-401, 20 mg/kg) [160]. Celgene carried out a Phase I study to evaluate the safety, pharmacokinetics, and pharmacodynamics of CC-401 in subjects with refractory acute myelogenous leukemia, but the study was terminated [127]. Nevertheless, there are no reports yet of CC-401 being used in the therapy of HCC in humans. To confirm the benefits associated with CC-401 treatment in HCC, additional interventions directed towards JNK activity in vivo are needed. CC-930, which targets JNK1/2 as well as ERK1 and p38, is a JNK inhibitor discovered by and in clinical development with Celgene [128]. CC-930 is mainly being investigated for the prevention and treatment of fibrosis, including idiopathic pulmonary fibrosis and skin fibrosis [128, 129]. Two Phase II research studies to assess if CC-930 was safe for treating subjects with discoid lupus erythematosus, as well as to characterize the safety, PK, and biological activity of CC-930 in idiopathic pulmonary fibrosis have been terminated [130]. AS601245, which belongs to a new class of benzothiazole acetonitrile derivatives, proved to be a structurally unique JNK inhibitor. This inhibitor provided neuroprotective effects in rats with transient focal cerebral ischaemia and gerbils with transient global ischemia [131] and was effective in myocardial ischemia-reperfusion injury [132]. Moreover, Cerbone et al. showed that combined treatment of AS601245 with clofibrate synergistically reduced cell proliferation, cyclin D1 and proliferating cell nuclear antigen (PCNA) expression [133]. The combination also induced apoptosis and differentiation in human colon cancer cells [133].
These inhibitors have poor kinase specificity because they target the highly conserved ATP-binding site. To overcome the specificity problem, Zhang et al. developed and characterized an inhibitor of all three JNK proteins, JNK-IN-8 [134]. JNK-IN-8 is a selective JNK inhibitor that inhibits phosphorylation of c-Jun in cells exposed to sub-micromolar drugs in a manner that depends on covalent modification of the conserved cysteine residue. Extensive biochemical, cellular, and pathway-based profiling established the selectivity of JNK-IN-8 for JNK and suggested that the compound will be broadly useful as a pharmacological probe for JNK-dependent signal transduction [134]. In 2013, Li et al. showed that JNK-IN-8 rescued head and neck squamous cell carcinoma cells from AZD8055-induced cytotoxicity by inhibiting JNK signals [161]. In summary, there has been significant progress in developing selective ATP-competitive inhibitors, and many of them have shown useful pharmacological effects in a variety of tumor cells, including HCC cells. However, the high homology of the ATP site for JNK isoforms has impeded the development of potent isoform selective JNK inhibitors. As a consequence, many JNK peptide and small molecule ATP-non-competitive inhibitors have also been developed.
8.2 ATP-Non-Competitive Inhibitors
The discovery of the JNK inhibitory properties of the JNK scaffold protein JIP1, followed by the identification of its minimum inhibitory sequence, has opened a new avenue in the use of JIP1-derived JNK inhibitory peptides. JIP1 is a scaffolding protein that enhances JNK signaling by creating a proximity effect between JNK and upstream kinases. D-JNKI-1 (also named as XG-102/AM-111) is a protease-resistant JNK-inhibiting peptide that is produced by linking the 20 amino acid terminal JNK-inhibitory sequence (JNK binding domain) of JIP1/IB1 to a 10-amino-acid TAT sequence of the HIV-TAT protein, which allows intracellular translocation [162]. D-JNKI-1 inhibits phosphorylation of the JNK substrate c-Jun and is more potent than the small-molecule inhibitor SP600125 [163]. A recent study showed that D-JNKI-1 crosses cellular membranes with fast kinetics through an active and passive mechanism. After acute intraperitoneal (ip) administration of D-JNKI-1 in mice, the peptide was found in the main organs, especially the liver and kidney, and could cross the blood brain barrier and reach the brain [164]. Peptidergic JNK inhibition using D-JNKI-1 has previously demonstrated benefits without undesirable side effects in various diseases, such as traumatic hearing loss, colitis, uveitis, diabetes, myocardial ischemia, acute inflammatory insult, Alzheimer’s disease, antigen-induced arthritis, adult hemorrhage, and hepatic injury [Reviewed in 165]. Recently, the application of D-JNKI-1 in vivo achieved numerous new progresses in the therapy of those diseases [139–152]. Especially, the Phase III clinical trials to evaluate the efficacy and safety of XG-102 in the reduction of post-cataract surgery intraocular inflammation and pain have been completed [135, 136]. In addition, the Phase II clinical trial to evaluate the efficacy of AM-111 in patients with acute sensorineural hearing loss has been completed with good results, and the Phase III clinical trial of AM-111 in the treatment of acute inner ear hearing loss is currently recruiting participants [137, 138]. The range of therapeutic applications of D-JNKI-1 continues to expand, and it will be broadly applied in the treatment of cancers. In a mouse skin cancer pain model, repeated systemic injections of D-JNKI-1 not only produced accumulative inhibition of mechanical allodynia and heat hyperalgesia, but also suppressed tumor growth in vivo and melanoma cell proliferation in vitro [153]. In addition, D-JNKI-1 significantly reduced the development of chemical-induced mouse HCC or xenografted human HCC cells, which suggested there is great promise for this type of JNK inhibitor in HCC therapy [33]. Unlike D-JNKI-1, there have only been a few studies on other cell permeable JIP1-derived peptides, such as L-JNKI-1, TIJIP, or TAT-TIJIP (TAT-linked JIP-based Peptide), and the in vivo effect of these compounds in liver tumor suppression remains unknown [Reviewed in 165]. However, the efficacy of TAT-mediated drug delivery is still controversial. This controversy combined with poor cell permeability, peptide instability, and a short half-life in vivo has served to hinder the development of peptide-based inhibitors. Increased attention has been directed towards the discovery of small molecules that also could act in an analogous fashion, i.e., as ATP-noncompetitive inhibitors of JNK [166]. In 2008, Stebbins et al. reported a series of small molecule JIP1 mimics that function as substrate competitive inhibitors of JNK [156]. One such compound, BI-78D3 can inhibit human prostate smooth muscle contractions and increase apoptosis in vitro [154, 155]. In animal studies, BI-78D3 not only blocked JNK-dependent Con A-induced liver damage, but also restored insulin sensitivity in mouse models of type 2 diabetes [156]. It will be interesting to see how these inhibitors of JNK activity are broadly applied in the treatment of JNK-associated HCC and whether desired therapeutic outcomes would be achieved without unwanted side effects.
9 Conclusions and Perspectives
HCC is the third leading cause of cancer-related death worldwide. To date, numerous data have indicated that the JNK signaling pathway plays a key role in the progression and tumorigenesis of HCC, and JNK has increasingly been recognized as an attractive molecular target for HCC therapy. As we have reviewed in this article, molecular inhibitors that target JNK have been widely developed, and a new generation of JNK inhibitors, such as small molecule ATP-non-competitive and peptide-based inhibitors, promise improved efficacy with the possibility of fewer off-target effects. In particular, the targeting of protein substrate docking domains provides a higher degree of specificity than previously achieved with ATP-competitive inhibitors. However, it is quite frustrating that many investigations have been discontinued or are still currently being clinically tested. To date, no clinical use of these molecules has been reported in the literature. Still, as the field of JNK inhibitors is rapidly moving, it is anticipated that several JNK targeted therapies with new drugs will be successfully developed and used in clinical settings in the near future. All in all, we are convinced that promising new avenues for the treatment of HCC are on the horizon, which will undoubtedly lead to better, more effective, and faster therapies in the years to come.
References
Torre LA, Bray F, Siegel RL, Ferlay J, Lortet-Tieulent J, Jemal A. Global cancer statistics, 2012. CA Cancer J Clin. 2015;65:87–108.
Farazi PA, Depinho RA. Hepatocellular carcinoma pathogenesis: from genes to environment. Nat Rev Cancer. 2006;6:674–87.
Levrero M, Zucman-Rossi J. Mechanisms of HBV-induced hepatocellular carcinoma. J Hepatol. 2016;64:S84–101.
de Martel C, Ferlay J, Franceschi S, Vignat J, Bray F, Forman D, et al. Global burden of cancers attributable to infections in 2008: a review and synthetic analysis. Lancet Oncol. 2012;13:607–15.
El-Serag HB. Hepatocellular carcinoma. N Engl J Med. 2011;365:1118–27.
Mittal S, El-Serag HB. Epidemiology of hepatocellular carcinoma: consider the population. J Clin Gastroenterol. 2013;47:S2–6.
Li QS, Liu GM, Shao D, Wang J, Yuan HY, Chen TX, et al. Mucin1 mediates autocrine transforming growth factor beta signaling through activating the c-Jun N-terminal kinase/activator protein 1 pathway in human hepatocellular carcinoma cells. Int J Biochem Cell Biol. 2015;59:116–25.
Weston CR, Davis RJ. The JNK signal transduction pathway. Curr Opin Genet Dev. 2002;12:14–21.
Ekihiro S, Brenner DA, Michael K. A liver full of JNK: signaling in regulation of cell function and disease pathogenesis, and clinical approaches. Gastroenterology. 2012;143:307–20.
Davis RJ. Signal transduction by the JNK group of MAP kinases. Cell. 2000;103:239–52.
Whitmarsh AJ, Kuan CY, Kennedy NJ, Kelkar N, Haydar TF, Mordes JP, et al. Requirement of the JIP1 scaffold protein forstress-induced JNK activation. Genes Dev. 2001;15:2421–32.
Owens DM, Keyse SM. Differential regulation of MAP kinasesignalling by dual-specificity protein phosphatases. Oncogene. 2007;26:3203–13.
Papa S, Bubici C, Zazzeroni F, Pham CG, Kuntzen C, Knabb JR, et al. The NF-kappaB-mediated control of the JNK cascade in theantagonism of programmed cell death in health and disease. Cell Death Differ. 2006;13:712–29.
Gupta S, Barrett T, Whitmarsh AJ, Cavanagh J, Sluss HK, Dérijard B, et al. Selective interaction of JNK protein kinase isoforms with transcription factors. EMBO J. 1996;15:2760–70.
Bogoyevitch MA, Kobe B. Uses for JNK: the many and varied substrates of the c-Jun N-terminal kinases. Microbiol Mol Biol Rev. 2006;70:1061–95.
Wagner EF, Nebreda AR. Signal integration by JNK and p38 MAPK pathways in cancer development. Nat Rev Cancer. 2009;9:537–49.
Matsuzaki K. Smad phospho-isoforms direct context-dependent TGF-β signaling. Cytokine Growth Factor Rev. 2013;24:385–99.
Smeal T, Binetruy B, Mercola DA, Birrer M, Karin M. Oncogenic and transcriptional cooperation with Ha-Ras requires phosphorylation of c-Jun on serines 63 and 73. Nature. 1991;354:494–6.
Raitano AB, Halpern JR, Hambuch TM, Sawyers CL. The Bcr-Abl leukemia oncogene activates Jun kinase and requires Jun for transformation. Proc Natl Acad Sci U S A. 1995;92:11746–50.
Rodrigues GA, Park M, Schlessinger J. Activation of the JNK pathway is essential for transformation by the Met oncogene. EMBO J. 1997;16:2634–45.
Behrens A, Jochum W, Sibilia M, Wagner EF. Oncogenic transformation by ras and fos is mediated by c-Jun N-terminal phosphorylation. Oncogene. 2000;19:2657–63.
Manning AM, Davis RJ. Targeting JNK for therapeutic benefit: from junk to gold? Nat Rev Drug Discov. 2003;2:554–65.
Adjei AA. Blocking oncogenic Ras signaling for cancer therapy. J Natl Cancer Inst. 2001;93:1062–74.
Dérijard B, Hibi M, Wu IH, Barrett T, Su B, Deng T, et al. JNK1: a protein kinase stimulated by UV light and Ha-Ras that binds and phosphorylates the c-Jun activation domain. Cell. 1994;76:1025–37.
Schutte J, Minna JD, Birrer MJ. Deregulated expression of human c-Jun transforms primary rat embryo cells in cooperation with an activated c-Ha-ras gene and transforms rat-1a cells as a single gene. Proc Natl Acad Sci U S A. 1989;86:2257–61.
Wang SE, Yu Y, Criswell TL, Debusk LM, Lin PC, Zent R, et al. Oncogenic mutations regulate tumor microenvironment through induction of growth factors and angiogenic mediators. Oncogene. 2010;29:3335–48.
Sekimoto G, Matsuzaki K, Yoshida K, Mori S, Murata M, Seki T, et al. Reversible Smad-dependent signaling between tumor suppression and oncogenesis. Cancer Res. 2007;67:5090–6.
Yamagata H, Matsuzaki K, Mori S, Yoshida K, Tahashi Y, Furukawa F, et al. Acceleration of Smad2 and Smad3 phosphorylation via c-Jun NH(2)-terminal kinase during human colorectal carcinogenesis. Cancer Res. 2005;65:157–65.
Matsuzaki K, Murata M, Yoshida K, Sekimoto G, Uemura Y, Sakaida N, et al. Chronic inflammation associated with hepatitis C virus infection perturbs hepatic transforming growth factor beta signaling, promoting cirrhosis and hepatocellular carcinoma. Hepatology. 2007;46:48–57.
Murata M, Matsuzaki K, Yoshida K, Sekimoto G, Tahashi Y, Mori S, et al. Hepatitis Bvirus X protein shifts human hepatic TGF-beta signaling from tumor-suppression to oncogenesis in early chronichepatitis B. Hepatology. 2009;49:1203–17.
Tsutsumi T, Suzuki T, Moriya K, Yotsuyanagi H, Shintani Y, Fujie H, et al. Alteration of intrahepatic cytokine expression and AP-1 activation in transgenic mice expressing hepatitis C virus core protein. Virology. 2002;304:415–24.
Sakurai T, Maeda S, Chang L, Karin M. Loss of hepatic NF-kappa B activity enhances chemical hepatocarcinogenesis through sustained c-Jun N-terminal kinase 1 activation. Proc Natl Acad Sci U S A. 2006;103:10544–51.
Hui L, Zatloukal K, Scheuch H, Stepniak E, Wagner EF. Proliferation of human HCC cells and chemically induced mouse liver cancers requires JNK1-dependent p21 downregulation. J Clin Invest. 2008;118:3943–53.
Chang Q, Zhang Y, Beezhold KJ, Bhatia D, Zhao H, Chen J, et al. Sustained JNK1 activation is associated with altered histone H3 methylations in human liver cancer. J Hepatol. 2009;50:323–33.
Das M, Garlick DS, Greiner DL, Davis RJ. The role of JNK in the development of hepatocellular carcinoma. Genes Dev. 2011;25:634–45.
Whitmarsh AJ, Davis RJ. Role of mitogen-activated protein kinase kinase 4 in cancer. Oncogene. 2007;26:3172–84.
Greenman C, Stephens P, Smith R, Dalgliesh GL, Hunter C, Bignell G, et al. Patterns of somatic mutation in human cancer genomes. Nature. 2007;446:153–8.
Kan Z, Jaiswal BS, Stinson J, Janakiraman V, Bhatt D, Stern HM, et al. Diverse somatic mutation patterns and pathway alterations in human cancers. Nature. 2010;466:869–73.
Guo L, Guo Y, Xiao S, Shi X. Protein kinase p-JNK is correlated with the activation of AP-1 and its associated Jun family proteins in hepatocellular carcinoma. Life Sci. 2005;77:1869–78.
Ching YP, Leong VY, Lee MF, Xu HT, Jin DY, Ng IO. P21-activated protein kinase is overexpressed in hepatocellular carcinoma and enhances cancer metastasis involving c-Jun NH2-terminal kinase activation and paxillin phosphorylation. Cancer Res. 2007;67:3601–8.
Hsiang CY, Wu SL, Chen JC, Lo HY, Li CC, Chiang SY, et al. Acetaldehyde induces matrix metalloproteinase-9 gene expression via nuclear factor-kappaB and activator protein 1 signaling pathways in human hepatocellular carcinoma cells: association with the invasive potential. Toxicol Lett. 2007;171:78–86.
Qian AR, Zhang W, Cao JP, Yang PF, Gao X, Wang Z, et al. Downregulation of CD147 expression alters cytoskeleton architecture and inhibits gelatinase production and SAPK pathway in human hepatocellular carcinoma cells. J Exp Clin Cancer Res. 2008;27:50.
Cho SB, Park YL, Park SJ, Park SY, Lee WS, Park CH, et al. KITENIN is associated with activation of AP-1 target genes via MAPK cascades signaling in human hepatocellular carcinoma progression. Oncol Res. 2011;19:115–23.
Park YH, Shin HJ, Kim SU, Kim JM, Kim JH, Bang DH, et al. iNOS promotes HBx-induced hepatocellular carcinoma via upregulation of JNK activation. Biochem Biophys Res Commun. 2013;435:244–9.
Wang L, Zhu R, Huang Z, Li H, Zhu H. Lipopolysaccharide-induced toll-like receptor 4 signaling in cancer cells promotes cell survival and proliferation in hepatocellular carcinoma. Dig Dis Sci. 2013;58:2223–6.
Pannem RR, Dorn C, Ahlqvist K, Bosserhoff AK, Hellerbrand C, Massoumi R. CYLD controls c-MYC expression through the JNK-dependent signaling pathway in hepatocellular carcinoma. Carcinogenesis. 2014;35:461–8.
Carr BI, Cavallini A, D’Alessandro R, Refolo MG, Lippolis C, Mazzocca A, et al. Platelet extracts induce growth, migration and invasion in human hepatocellular carcinoma in vitro. BMC Cancer. 2014;14:43.
Yang XH, Zheng X, Cao JG, Xiang HL, Liu F, Lv Y. 8-Bromo-7-methoxychrysin-induced apoptosis of hepatocellular carcinoma cells involves ROS and JNK. World J Gastroenterol. 2010;16:3385–93.
Choedon T, Shukla SK, Kumar V. Chemopreventive and anti-cancer properties of the aqueous extract of flowers of Butea monosperma. J Ethnopharmacol. 2010;129:208–13.
Lee EK, Kim HJ, Lee KJ, Lee HJ, Lee JS, Kim DG, et al. Inhibition of the proliferation and invasion of hepatocellular carcinoma cells by lipocalin 2 through blockade of JNK and PI3K/Akt signaling. Int J Oncol. 2011;38:325–33.
Xiao CL, Tao ZH, Guo L, Li WW, Wan JL, Sun HC, et al. Isomalto oligosaccharide sulfate inhibits tumor growth and metastasis of hepatocellular carcinoma in nude mice. BMC Cancer. 2011;11:150.
Matsushima-Nishiwaki R, Adachi S, Yoshioka T, Yasuda E, Yamagishi Y, Matsuura J, et al. Suppression by heat shock protein 20 of hepatocellular carcinoma cell proliferation via inhibition of the mitogen-activated protein kinases and AKT pathways. J Cell Biochem. 2011;112:3430–9.
Honma Y, Shimizu S, Takehara T, Harada M. Sorafenib enhances proteasome inhibitor-induced cell death via inactivation of Akt and stress-activated protein kinases. J Gastroenterol. 2014;49:517–26.
Xu L, Wang T, Meng WY, Wei J, Ma JL, Shi M, et al. Salinomycin inhibits hepatocellular carcinoma cell invasion and migration through JNK/JunD pathway-mediated MMP9 expression. Oncol Rep. 2015;33:1057–63.
Li H, Li Y, Liu D, Liu J. LPS promotes epithelial-mesenchymal transition and activation of TLR4/JNK signaling. Tumour Biol. 2014;35:10429–35.
Dong YQ, Lu CW, Zhang L, Yang J, Hameed W, Chen W. Toll-like receptor 4 signaling promotes invasion of hepatocellular carcinoma cells through MKK4/JNK pathway. Mol Immunol. 2015;68:671–83.
Kufe DW. Mucins in cancer: function, prognosis and therapy. Nat Rev Cancer. 2009;9:874–85.
Nath S, Mukherjee P. MUC1: a multifaceted oncoprotein with a key role in cancer progression. Trends Mol Med. 2014;20:332–42.
Chou CH, Huang MJ, Chen CH, Shyu MK, Huang J, Hung JS, et al. Up-regulation of C1GALT1 promotes breast cancer cell growth through MUC1-C signaling pathway. Oncotarget. 2015;6:6123–35.
Joshi S, Kumar S, Choudhury A, Ponnusamy MP, Batra SK. Altered Mucins (MUC) trafficking in benign and malignant conditions. Oncotarget. 2014;5:7272–84.
Alam M, Rajabi H, Ahmad R, Jin C, Kufe D. Targeting the MUC1-C oncoprotein inhibits self-renewal capacity of breast cancer cells. Oncotarget. 2014;5:2622–34.
Horm TM, Schroeder JA. MUC1 and metastatic cancer: expression, function and therapeutic targeting. Cell Adhes Migr. 2013;7:187–98.
Li QS, Wang FL, Liu GM, Yuan HY, Chen TX, Wang J, et al. Impact of Mucin1 knockdown on the phenotypic characteristics of the human hepatocellular carcinoma cell line SMMC-7721. Oncol Rep. 2014;31:2811–9.
Chen Q, Li D, Ren J, Li C, Xiao ZX. MUC1 activates JNK1 and inhibits apoptosis under genotoxic stress. Biochem Biophys Res Commun. 2013;440:179–83.
Huang L, Chen D, Liu D, Yin L, Kharbanda S, Kufe DW. MUC1 oncoprotein blocks glycogen synthase kinase 3beta-mediated phosphorylation and degradation of beta-catenin. Cancer Res. 2005;65:10413–22.
Li YQ, Kuwahara H, Ren J, Wen GY, Kufe DW. The c-Src tyrosine kinase regulates signaling of the human DF3/MUC1 carcinoma-associated antigen with GSK3 beta and beta-catenin. J Biol Chem. 2001;276:6061–4.
Pandey P, Kharbanda S, Kufe DW. Association of the DF3/MUC1 breast cancer antigen with Grb2 and the Sos/Ras exchange protein. Cancer Res. 1995;55:4000–3.
Wei XL, Xu H, Kufe DW. Human mucin 1 oncoprotein represses transcription of the p53 tumor suppressor gene. Cancer Res. 2007;67:1853–8.
Kufe DW. MUC1-C oncoprotein as a target in breast cancer: activation of signaling pathways and therapeutic approaches. Oncogene. 2013;32:1073–81.
Schroeder JA, Thompson MC, Gardner MM, Gendler SJ. Transgenic MUC1 interacts with epidermal growth factor receptor and correlates with mitogen-activated protein kinase activation in the mouse mammary gland. J Biol Chem. 2001;276:13057–64.
Merlin J, Stechly L, de Beaucé S, Monté D, Leteurtre E, van Seuningen I, et al. Galectin-3 regulates MUC1 and EGFR cellular distribution and EGFR downstream pathways in pancreatic cancer cells. Oncogene. 2011;30:2514–25.
Ahmad R, Raina D, Trivedi V, Ren J, Rajabi H, Kharbanda S, et al. MUC1 oncoprotein activates the IkappaB kinase beta complex and constitutive NF-kappaB signaling. Nat Cell Biol. 2007;9:1419–27.
Nagata H, Hatano E, Tada M, Murata M, Kitamura K, Asechi H, et al. Inhibition of c-Jun NH2-terminal kinase switches Smad3 signaling from oncogenesis to tumor-suppression in rat hepatocellular carcinoma. Hepatology. 2009;49:1944–53.
Li QS, Liu GM, Yuan HY, Wang J, Guo YY, Chen TX, et al. Mucin1 shifts Smad3 signaling from the tumor-suppressive pSmad3C/p21(WAF1) pathway to the oncogenic pSmad3L/c-Myc pathway by activating JNK in human hepatocellular carcinoma cells. Oncotarget. 2015;6:4253–65.
Wang J, Liu GM, Li QS, Wang F, Xie F, Zhai RP, et al. Mucin1 promotes the migration and invasion of hepatocellular carcinoma cells via JNK-mediated phosphorylation of Smad2 at the C-terminal and linker regions. Oncotarget. 2015;6:19264–78.
Yamaguchi T, Matsuzaki K, Inokuchi R, Kawamura R, Yoshida K, Murata M, et al. Phosphorylated Smad2 and Smad3 signaling: shifting between tumor suppression and fibro-carcinogenesis in chronic hepatitis C. Hepatol Res. 2013;43:1327–42.
Deng YR, Yoshida K, Jin QL, Murata M, Yamaguchi T, Tsuneyama K, et al. Reversible phospho-Smad3 signalling between tumour suppression and fibrocarcinogenesis in chronic hepatitis B infection. Clin Exp Immunol. 2014;176:102–11.
Guicciardi ME, Gores GJ. Apoptosis: a mechanism of acute and chronic liver injury. Gut. 2005;54:1024–33.
Fabregat I. Dysregulation of apoptosis in hepatocellular carcinoma cells. World J Gastroenterol. 2009;15:513–20.
Fabregat I, Roncero C, Fernandez M. Survival and apoptosis: a dysregulated balance in liver cancer. Liver Int. 2007;27:155–62.
Cuadrado A, Gonzalez L, Suarez Y, Martinez T, Munoz A. JNK activation is critical for Aplidin-induced apoptosis. Oncogene. 2004;23:4673–80.
Kannaiyan R, Manu KA, Chen L, Li F, Rajendran P, Subramaniam A, et al. Celastrol inhibits tumor cell proliferation and promotes apoptosis through the activation of c-Jun N-terminal kinase and suppression of PI3K/Akt signaling pathways. Apoptosis. 2011;16:1028–41.
Malhi H, Bronk SF, Werneburg NW, Gores GJ. Free fatty acids induce JNK-dependent hepatocyte lipoapoptosis. J Biol Chem. 2006;281:12093–101.
Kim BJ, Ryu SW, Song BJ. JNK- and p38 kinase-mediated phosphorylation of Bax leads to its activation and mitochondrial translocation and to apoptosis of human hepatoma HepG2 cells. J Biol Chem. 2006;281:21256–65.
Dhanasekaran DN, Reddy EP. JNK signaling in apoptosis. Oncogene. 2008;27:6245–51.
Malhi H, Gores GJ. Molecular mechanisms of lipotoxicity in nonalcoholic fatty liver disease. Semin Liver Dis. 2008;28:360–9.
Malhi H, Barreyro FJ, Isomoto H, Bronk SF, Gores GJ. Free fatty acids sensitise hepatocytes to TRAIL mediated cytotoxicity. Gut. 2007;56:1124–31.
Qi R, An H, Yu Y, Zhang M, Liu S, Xu H, et al. Notch1 signaling inhibits growth of human hepatocellular carcinoma through induction of cell cycle arrest and apoptosis. Cancer Res. 2003;63:8323–9.
Ou DL, Shen YC, Yu SL, Chen KF, Yeh PY, Fan HH, et al. Induction of DNA damage-inducible gene GADD45beta contributes to sorafenib-induced apoptosis in hepatocellular carcinoma cells. Cancer Res. 2010;70:9309–18.
Saxena NK, Fu PP, Nagalingam A, Wang J, Handy J, Cohen C, et al. Adiponectin modulates C-jun N-terminal kinase and mammalian target of rapamycin and inhibits hepatocellular carcinoma. Gastroenterology. 2010;139:1762–73. 1773 e1–5.
Liao YJ, Bai HY, Li ZH, Zou J, Chen JW, Zheng F, et al. Longikaurin A, a natural ent-kaurane, induces G2/M phase arrest via downregulation of Skp2 and apoptosis induction through ROS/JNK/c-Jun pathway in hepatocellular carcinoma cells. Cell Death Dis. 2014;5:e1137.
Zhang Z, Miao L, Lv C, Sun H, Wei S, Wang B, et al. Wentilactone B induces G2/M phase arrest and apoptosis via the Ras/Raf/MAPK signaling pathway in human hepatoma SMMC-7721 cells. Cell Death Dis. 2013;4:e657.
Wang C, Chen T, Zhang N, Yang M, Li B, Lü X, et al. Melittin, a major component of bee venom, sensitizes human hepatocellular carcinoma cells to tumor necrosis factor-related apoptosis-inducing ligand (TRAIL)-induced apoptosis by activating CaMKII-TAK1-JNK/p38 and inhibiting IkappaBalpha kinase-NFkappaB. J Biol Chem. 2009;284:3804–13.
Song IS, Jun SY, Na HJ, Kim HT, Jung SY, Ha GH, et al. Inhibition of MKK7-JNK by the TOR signaling pathway regulator-like protein contributes to resistance of HCC cells to TRAIL-induced apoptosis. Gastroenterology. 2012;143:1341–51.
Bugianesi E, McCullough AJ, Marchesini G. Insulin resistance: a metabolic pathway to chronic liver disease. Hepatology. 2005;42:987–1000.
Nehra V, Angulo P, Buchman AL, Lindor KD. Nutritional and metabolic considerations in the etiology of nonalcoholic steatohepatitis. Dig Dis Sci. 2001;46:2347–52.
Feldstein AE, Canbay A, Angulo P, Taniai M, Burgart LJ, Lindor KD, et al. Hepatocyte apoptosis and fas expression are prominent features of human nonalcoholic steatohepatitis. Gastroenterology. 2003;125:437–43.
Ribeiro PS, Cortez-Pinto H, Solá S, Castro RE, Ramalho RM, Baptista A, et al. Hepatocyte apoptosis, expression of death receptors, and activation of NFkappaB in the liver of nonalcoholic and alcoholic steatohepatitis patients. Am J Gastroenterol. 2004;99:1708–17.
de Almeida IT, Cortez-Pinto H, Fidalgo G, Rodrigues D, Camilo ME. Plasma total and free fatty acids composition in human non-alcoholic steatohepatitis. Clin Nutr. 2002;21:219–23.
Wei Y, Wang D, Topczewski F, Pagliassotti MJ. Saturated fatty acids induce endoplasmic reticulum stress and apoptosis independently of ceramide in liver cells. Am J Physiol Endocrinol Metab. 2006;291:E275–81.
Czaja MJ. Cell signaling in oxidative stress-induced liver injury. Semin Liver Dis. 2007;27:378–89.
Hirosumi J, Tuncman G, Chang L, Görgün CZ, Uysal KT, Maeda K, et al. A central role for JNK in obesity and insulin resistance. Nature. 2002;420:333–6.
Schattenberg JM, Singh R, Wang Y, Lefkowitch JH, Rigoli RM, Scherer PE, et al. JNK1 but not JNK2 promotes the development of steatohepatitis in mice. Hepatology. 2006;43:163–72.
Singh R, Wang Y, Xiang Y, Tanaka KE, Gaarde WA, Czaja MJ. Differential effects of JNK1 and JNK2 inhibition on murine steatohepatitis and insulin resistance. Hepatology. 2009;49:87–96.
Puri P, Mirshahi F, Cheung O, Natarajan R, Maher JW, Kellum JM, et al. Activation and dysregulation of the unfolded protein response in nonalcoholic fatty liver disease. Gastroenterology. 2008;134:568–76.
Lei K, Davis RJ. JNK phosphorylation of Bim-related members of the Bcl2 family induces Bax-dependent apoptosis. Proc Natl Acad Sci U S A. 2003;100:2432–7.
Donovan N, Becker EB, Konishi Y, Bonni A. JNK phosphorylation and activation of BAD couples the stress-activated signaling pathway to the cell death machinery. J Biol Chem. 2002;277:40944–9.
Yamamoto K, Ichijo H, Korsmeyer SJ. BCL-2 is phosphorylated and inactivated by an ASK1/Jun N-terminal protein kinase pathway normally activated at G(2)/M. Mol Cell Biol. 1999;19:8469–78.
Cazanave SC, Mott JL, Elmi NA, Bronk SF, Werneburg NW, Akazawa Y, et al. JNK1-dependent PUMA expression contributes to hepatocyte lipoapoptosis. J Biol Chem. 2009;284:26591–602.
Pagliassotti MJ, Wei Y, Wang D. Insulin protects liver cells from saturated fatty acid-induced apoptosis via inhibition of c-Jun NH2 terminal kinase activity. Endocrinology. 2007;148:3338–45.
Mucha SR, Rizzani A, Gerbes AL, Camaj P, Thasler WE, Bruns CJ, et al. JNK inhibition sensitises hepatocellular carcinoma cells but not normal hepatocytes to the TNF-related apoptosis-inducing ligand. Gut. 2009;58:688–98.
Aderca I, Moser CD, Veerasamy M, Bani-Hani AH, Bonilla-Guerrero R, Ahmed K, et al. The JNK inhibitor SP600129 enhances apoptosis of HCC cells induced by the tumor suppressor WWOX. J Hepatol. 2008;49:373–83.
Han Z, Boyle DL, Chang L, Bennett B, Karin M, Yang L, et al. c-Jun N-terminal kinase is required for metalloproteinase expression and joint destruction in inflammatory arthritis. J Clin Invest. 2001;108:73–81.
Eynott PR, Xu L, Bennett BL, Noble A, Leung SY, Nath P, et al. Effect of an inhibitor of Jun N-terminal protein kinase, SP600125, in single allergen challenge in sensitized rats. Immunology. 2004;112:446–53.
Miyamoto-Yamasaki Y, Yamasaki M, Tachibana H, Yamada K. Induction of endoreduplication by a JNK inhibitor SP600125 in human lung carcinoma A 549 cells. Cell Biol Int. 2007;31:1501–6.
Kim JA, Lee J, Margolis RL, Fotedar R. SP600125 suppresses Cdk1 and induces endoreplication directly from G2 phase, independent of JNK inhibition. Oncogene. 2010;29:1702–16.
Jemaà M, Vitale I, Kepp O, Berardinelli F, Galluzzi L, Senovilla L, et al. Selective killing of p53-deficient cancer cells by SP600125. EMBO Mol Med. 2012;4:500–14.
Mingo-Sion AM, Marietta PM, Koller E, Wolf DM, Van Den Berg CL. Inhibition of JNK reduces G2/M transit independent of p53, leading to endoreduplication, decreased proliferation, and apoptosis in breast cancer cells. Oncogene. 2004;23:596–604.
Kuntzen C, Sonuc N, De Toni EN, Opelz C, Mucha SR, Gerbes AL, et al. Inhibition of c-Jun-N-terminal-kinase sensitizes tumor cells to CD95-induced apoptosis and induces G2/M cell cycle arrest. Cancer Res. 2005;65:6780–8.
Lu YY, Chen TS, Wang XP, Qu JL, Chen M. The JNK inhibitor SP600125 enhances dihydroartemisinin-induced apoptosis by accelerating Bax translocation into mitochondria in human lung adenocarcinoma cells. FEBS Lett. 2010;584:4019–26.
Kim JH, Chae M, Choi AR, Sik Kim H, Yoon S. SP600125 overcomes antimitotic drug-resistance in cancer cells by increasing apoptosis with independence of P-gp inhibition. Eur J Pharmacol. 2014;723:141–7.
Zhang C, Zhang J, Li X, Sun N, Yu R, Zhao B, et al. Huaier aqueous extract induces hepatocellular carcinoma cells arrest in S phase via JNK signaling pathway. Evid Based Complement Alternat Med. 2015;2015:171356.
Wu JR, Hu CT, You RI, Pan SM, Cheng CC, Lee MC, et al. Hydrogen peroxide inducible clone-5 mediates reactive oxygen species signaling for hepatocellular carcinoma progression. Oncotarget. 2015;6:32526–44.
Kim MO, Lee HS, Chin YW, Moon DO, Ahn JS. Gartanin induces autophagy through JNK activation which extenuates caspase-dependent apoptosis. Oncol Rep. 2015;34:139–46.
Uehara T, Xi Peng X, Bennett B, Satoh Y, Friedman G, Currin R, et al. c-Jun N-terminal kinase mediates hepatic injury after rat liver transplantation. Transplantation. 2004;78:324–32.
Vasilevskaya IA, Selvakumaran M, Hierro LC, Goldstein SR, Winkler JD, O’Dwyer PJ. Inhibition of jnk sensitizes hypoxic colon cancer cells to dna-damaging agents. Clin Cancer Res. 2015;21:4143–52.
www.Clinicaltrials.gov; Trial Identifier NCT00126893.
Plantevin Krenitsky V, Nadolny L, Delgado M, Ayala L, Clareen SS, Hilgraf R, et al. Discovery of CC-930, an orally active anti-fibrotic JNK inhibitor. Bioorg Med Chem Lett. 2012;22:1433–8.
Reich N, Tomcik M, Zerr P, Lang V, Dees C, Avouac J, et al. Jun N-terminal kinase as a potential molecular target for prevention and treatment of dermal fibrosis. Ann Rheum Dis. 2012;71:737–45.
www.Clinicaltrials.gov. Trial Identifier NCT01466725 and NCT01203943.
Carboni S, Hiver A, Szyndralewiez C, Gaillard P, Gotteland JP, Vitte PA. AS601245 (1,3-benzothiazol-2-yl (2-[[2-(3-pyridinyl)ethyl] amino]-4 pyrimidinyl) acetonitrile): a c-Jun NH2-terminalprotein kinase inhibitor with neuroprotective properties. J Pharmacol Exp Ther. 2004;310:25–32.
Ferrandi C, Ballerio R, Gaillard P, Giachetti C, Carboni S, Vitte PA, et al. Inhibition of c-Jun N-terminal kinase decreasescardiomyocyte apoptosis and infarct size after myocardial ischemiaand reperfusion in anaesthetized rats. Br J Pharmacol. 2004;142:953–60.
Cerbone A, Toaldo C, Pizzimenti S, Pettazzoni P, Dianzani C, Minelli R, et al. AS601245, an anti-inflammatory JNK inhibitor, and clofibrate have a synergistic effect in inducing cell responses and in affecting the gene expression profile in CaCo-2 colon cancer cells. PPAR Res. 2012;2012:203–10.
Zhang T, Inesta-Vaquera F, Niepel M, Zhang J, Ficarro SB, Machleidt T, et al. Discovery of potent and selective covalent inhibitors of JNK. Chem Biol. 2012;19:140–54.
Beydoun T, Deloche C, Perino J, Kirwan BA, Combette JM, Behar-Cohen F. Subconjunctival injection of XG-102, a JNK inhibitor peptide, in patients with intraocular inflammation: a safety and tolerability study. J Ocul Pharmacol Ther. 2015;31:93–9.
www.clinicaltrials.gov. Trial Identifier NCT02508337 and NCT02235272.
Suckfuell M, Lisowska G, Domka W, Kabacinska A, Morawski K, Bodlaj R, et al. Efficacy and safety of AM-111 in the treatment of acute sensorineural hearing loss: a double-blind, randomized, placebo-controlled phase II study. Otol Neurotol. 2014;35(8):1317–26.
www.clinicaltrials.gov. Trial Identifier NCT00802425 and NCT02561091.
El Zaoui I, Touchard E, Berdugo M, Abadie C, Kowalczuk L, Deloche C, et al. Subconjunctival injection of XG-102, a c-Jun N-terminal kinase inhibitor peptide, in the treatment of endotoxin-induced uveitis in rats. J Ocul Pharmacol Ther. 2015;31:17–24.
Touchard E, Omri S, Naud MC, Berdugo M, Deloche C, Abadie C, et al. A peptide inhibitor of c-Jun N-terminal kinase for the treatment of endotoxin-induced uveitis. Invest Ophthalmol Vis Sci. 2010;51:4683–93.
Sclip A, Tozzi A, Abaza A, Cardinetti D, Colombo I, Calabresi P, et al. c-Jun N-terminal kinase has a key role in Alzheimer disease synaptic dysfunction in vivo. Cell Death Dis. 2014;5:e1019.
Ploia C, Antoniou X, Sclip A, Grande V, Cardinetti D, Colombo A, et al. JNK plays a key role in tau hyperphosphorylation in Alzheimer’s disease models. J Alzheimers Dis. 2011;26:315–29.
Kersting S, Behrendt V, Kersting J, Reinecke K, Hilgert C, Stricker I, et al. The impact of JNK inhibitor D-JNKI-1 in a murine model of chronic colitis induced by dextran sulfate sodium. J Inflamm Res. 2013;6:71–81.
Reinecke K, Eminel S, Dierck F, Roessner W, Kersting S, Chromik AM, et al. The JNK inhibitor XG-102 protects against TNBS-induced colitis. PLoS One. 2012;7:e30985.
Eshraghi AA, Gupta C, Van De Water TR, Bohorquez JE, Garnham C, Bas E, et al. Molecular mechanisms involved in cochlear implantation trauma and the protection of hearing and auditory sensory cells by inhibition of c-Jun-N-terminal kinase signaling. Laryngoscope. 2013;123 Suppl 1:S1–14.
Repici M, Chen X, Morel MP, Doulazmi M, Sclip A, Cannaya V, et al. Specific inhibition of the JNK pathway promotes locomotor recovery and neuroprotection after mouse spinal cord injury. Neurobiol Dis. 2012;46:710–21.
Guma M, Ronacher LM, Firestein GS, Karin M, Corr M. JNK-1 deficiency limits macrophage-mediated antigen-induced arthritis. Arthritis Rheum. 2011;63:1603–12.
Michel-Monigadon D, Bonny C, Hirt L. c-Jun N-terminal kinase pathway inhibition in intracerebral hemorrhage. Cerebrovasc Dis. 2010;29:564–70.
Liu JR, Zhao Y, Patzer A, Staak N, Boehm R, Deuschl G, et al. The c-Jun N-terminal kinase (JNK) inhibitor XG-102 enhances the neuroprotection of hyperbaric oxygen after cerebral ischaemia in adult rats. Neuropathol Appl Neurobiol. 2010;36:211–24.
Omotehara Y, Hakuba N, Hato N, Okada M, Gyo K. Protection against ischemic cochlear damage by intratympanic administration of AM-111. Otol Neurotol. 2011;32:1422–7.
Nijboer CH, Bonestroo HJ, Zijlstra J, Kavelaars A, Heijnen CJ. Mitochondrial JNK phosphorylation as a novel therapeutic target to inhibit neuroinflammation and apoptosis after neonatal ischemic brain damage. Neurobiol Dis. 2013;54:432–44.
Grindal TC, Sampson EM, Antonelli PJ. AM-111 prevents hearing loss from semicircular canal injury in otitis media. Laryngoscope. 2010;120(1):178–82.
Gao YJ, Cheng JK, Zeng Q, Xu ZZ, Decosterd I, Xu X, et al. Selective inhibition of JNK with a peptide inhibitor attenuates pain hypersensitivity and tumor growth in a mouse skin cancer pain model. Exp Neurol. 2009;219:146–55.
Strittmatter F, Walther S, Gratzke C, Göttinger J, Beckmann C, Roosen A, et al. Inhibition of adrenergic human prostate smooth muscle contraction by the inhibitors of c-Jun N-terminal kinase, SP600125 and BI-78D3. Br J Pharmacol. 2012;166:1926–35.
Posthumadeboer J, van Egmond PW, Helder MN, de Menezes RX, Cleton-Jansen AM, Beliën JA, et al. Targeting JNK-interacting-protein-1 (JIP1) sensitises osteosarcoma to doxorubicin. Oncotarget. 2012;3:1169–81.
Stebbins JL, De SK, Machleidt T, Becattini B, Vazquez J, Kuntzen C, et al. Identification of a new JNK inhibitor targeting the JNK-JIP interaction site. Proc Natl Acad Sci U S A. 2008;105:16809–13.
Bennett BL, Sasaki DT, Murray BW, O’Leary EC, Sakata ST, Xu W, et al. SP600125, an anthrapyrazolone inhibitor of Jun N-terminal kinase. Proc Natl Acad Sci U S A. 2001;98:13681–6.
Koch P, Gehringer M, Laufer SA. Inhibitors of c-Jun N-terminal kinases: an update. J Med Chem. 2015;58:72–95.
Fabian MA, Biggs 3rd WH, Treiber DK, Atteridge CE, Azimioara MD, Benedetti MG, et al. A small molecule-kinase interaction map for clinical kinase inhibitors. Nat Biotechnol. 2005;23:329–69.
Uehara T, Bennett B, Sakata ST, Satoh Y, Bilter GK, Westwick JK, et al. JNK mediates hepatic ischemia reperfusion injury. J Hepatol. 2005;42:850–9.
Li Q, Song XM, Ji YY, Jiang H, Xu LG. The dual mTORC1 and mTORC2 inhibitor AZD8055 inhibits head and neck squamous cell carcinoma cell growth in vivo and in vitro. Biochem Biophys Res Commun. 2013;440:701–6.
Wiegler K, Bonny C, Coquoz D, Hirt L. The JNK inhibitor XG-102 protects from ischemic damage with delayed intravenous administration also in the presence of recombinant tissue plasminogen activator. Cerebrovasc Dis. 2008;26:360–6.
Zhuang ZY, Wen YR, Zhang DR, Borsello T, Bonny C, Strichartz GR, et al. A peptide c-Jun N-terminal kinase (JNK) inhibitor blocks mechanical allodynia after spinal nerve ligation: respective roles of JNK activation in primary sensory neurons and spinal astrocytes for neuropathic pain development and maintenance. J Neurosci. 2006;26:3551–60.
Davoli E, Sclip A, Cecchi M, Cimini S, Carrà A, Salmona M, et al. Determination of tissue levels of a neuroprotectant drug: the cell permeable JNK inhibitor peptide. J Pharmacol Toxicol Methods. 2014;70:55–61.
Bogoyevitch MA, Ngoei KR, Zhao TT, Yeap YY, Ng DC. c-Jun N-terminal kinase (JNK) signaling: recent advances and challenges. Biochim Biophys Acta. 2010;1804:463–75.
Barr RK, Boehm I, Attwood PV, Watt PM, Bogoyevitch MA. The criticalfeatures and the mechanism of inhibition of a kinase interaction motif-basedpeptide inhibitor of JNK. J Biol Chem. 2004;279:36327–38.
Acknowledgments
We apologize to the authors whose excellent works could not be cited in this review article because of space restriction.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This manuscript was supported by grants from the Double Tenth Engineering of Major Research Project of Jilin Provincial Science and Technology Department (No. 20140201012YY) and the Major Development Programs for New Drugs of the Chinese Academy of Sciences during the 12th Five-Year Plan Period (No. 2011ZX09102-001-36).
Conflict of Interest
Juan Wang and Guixiang Tai have no conflict of interest to report with respect to this work.
Rights and permissions
About this article
Cite this article
Wang, J., Tai, G. Role of C-Jun N-terminal Kinase in Hepatocellular Carcinoma Development. Targ Oncol 11, 723–738 (2016). https://doi.org/10.1007/s11523-016-0446-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11523-016-0446-5