Abstract
Background
Advanced hepatocellular carcinoma (HCC) responds poorly to conventional systemic therapies. Therefore, new effective therapy strategies are urgently needed. Molecular targeted therapies have entered the field of anti-neoplastic treatment and are being used on their own and in combination with other drugs. Sorafenib inhibits proliferation and angiogenesis of HCC by suppressing the Raf serine/threonine kinases and the receptor tyrosine kinases. The proteasome inhibitor bortezomib has shown activity in a variety of solid tumors, including HCC. However, the precise anti-proliferative mechanisms of these agents remain unclear.
Methods
We treated human hepatoma cell lines (Huh7 and Hep3B) and immortalized human hepatocyte (OUMS29) with sorafenib and/or proteasome inhibitors, including epoxomicin and acetyl-leucyl-leucyl-norleucinal. Cytotoxic effects were examined by morphometric analyses of apoptosis and necrosis. Apoptosis was also evaluated by Western blotting of keratin18, PARP and caspase3. The activity of Akt and stress-activated protein kinases was examined by Western blotting.
Results
Both sorafenib and proteasome inhibitors induced apoptosis in Huh7 and OUMS29. However, sorafenib attenuated proteasome inhibitor-induced apoptosis. Sorafenib induced necrosis, especially in combination with proteasome inhibitors. Sorafenib induced down-regulation of Akt synergistically in combination with proteasome inhibitors in Huh7. Sorafenib inhibited both the JNK and p38 pathways in a time- and dose-dependent manner. In addition, sorafenib also inhibited proteasome inhibitor-mediated JNK and p38 activation in both Huh7 and OUMS29.
Conclusions
Sorafenib enhances the anti-proliferative effect of proteasome inhibitors in part by inactivating the Akt signaling pathway and modulating stress-activated protein kinases. The combination of these agents could be an ideal molecular targeted therapy for HCC.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Hepatocellular carcinoma (HCC) is currently the sixth most prevalent cancer and the third most frequent cause of cancer-related death [1]. Curative treatments for early stage HCC include surgery, percutaneous ablation and liver transplantation, but they are only feasible in a minority of patients [2]. For those patients who have advanced stage or recurrent tumors after local treatments, systemic pharmacologic treatment is the main therapy. Unfortunately, the response rate to conventional chemotherapies for HCC patients is quite low and the outcome is poor [3, 4]. Therefore, new effective and well-tolerated therapeutic strategies are urgently needed.
Two randomized placebo-controlled trials of molecular targeted therapy for advanced HCC have offered hope for improving the median survival of advanced HCC [5, 6]. The Raf/mitogen-activated protein kinase (MAPK)/extracellular signal-regulated protein kinase (ERK) signaling pathway has been shown to play a significant role in tumor cell proliferation in HCC. Sorafenib is a multi-kinase inhibitor which inhibits proliferation and angiogenesis in HCC. Sorafenib targets the Raf serine/threonine kinases, including Raf-1 and B-Raf, which are members of the Raf/MEK/ERK signaling pathway, and tyrosine kinases such as vascular endothelial growth factor receptor (VEGFR) 2, VEGFR 3, platelet-derived growth factor receptor (PDGFR) β, Flt3 and c-Kit [7].
Bortezomib (also called Velcade or PS-341) is a proteasome inhibitor (PI) which has been clinically used for the treatment of multiple myeloma and evaluated for treating other malignancies [8]. Although success of bortezomib in the treatment of hematological malignancies has been reported, the efficacy of bortezomib in solid tumors, including HCC, has been less promising than in hematological malignancies [9]. PIs have been reported to induce anti-tumor effects owing to their ability to down-regulate the nuclear factor-kappa B (NFκB), induce the accumulation of proapoptotic Bcl-2 family members, and inhibit the degradation of p53 and p27 [10]. In addition, down-regulation of Akt activity plays an important role in the anti-tumor effect of bortezomib in hepatoma cells [11]. Thus, PIs are a new class of chemotherapeutic drugs with great therapeutic potential [12]. But the precise mechanisms of their anti-tumor effects are not fully understood. A recent study demonstrated that the combination of sorafenib and bortezomib induced anti-tumor effects via inactivation of Akt in malignant cells [13, 14]. The combination of sorafenib and bortezomib is being investigated in phase I trials in patients with advanced renal cell carcinoma [15].
In the present study, we examined the effect of sorafenib on phosphorylation of the Akt signaling pathway and stress-activated protein kinases. Our results indicate that sorafenib enhances PI-mediated cytotoxicity via inactivation of the Akt signaling pathway and of stress-activated protein kinases.
Materials and methods
Cells culture and reagents
We used human hepatoma cell lines established from hepatocellular carcinoma cell lines (Huh7 and Hep3B cells) and a highly differentiated immortalized human hepatocyte cell line (OUMS29 cells) [16]. Cells were cultured in Dulbecco’s modified Eagle’s medium supplemented with 10 % fetal bovine serum and antibiotics. Cell cultures were maintained in a 37 °C incubator with 5 % CO2.
Antibodies to the following antigens were used: keratin 18 (K18) (Santa Cruz Biotechnology; Santa Cruz, CA, USA); poly-ADP-ribose-polymerase (PARP), cleaved caspase3, c-Jun N-terminal kinase (JNK), phospho JNK (Thr183/Tyr185), phospho c-Jun (Ser73), p38, phospho p38 (Thr180/Tyr182), phospho CREB (Ser133), Akt, phospho Akt (Ser473), p70 S6 kinase, phospho p70 S6 kinase (Thr389) (Cell Signaling Technology, Danvers, MA, USA); and actin (Sigma-Aldrich, St. Louis, MO, USA). We used the primary and secondary antibodies at 1:1000 dilutions.
The following materials were used: sorafenib (LKT Laboratories, St. Paul, MN, USA); acetyl-leucyl-leucyl-norleucinal (ALLN) and epoxomicin as PIs (Calbiochem, La Jolla, CA, USA); human recombinant insulin and insulin-like growth factor-1 (IGF-1) (Wako Pure Chemical Industries, Osaka, Japan).
Because we previously reported that the above-mentioned concentration of PIs induce apoptosis, but not induced too much cell death, in Huh7 cells [17], we treated cells with the indicated concentration of PIs, ALLN (30 μM) and epoxomicin (1 μM), respectively. ALLN is one of the first proteasome inhibitors discovered and has been widely used to study the proteasome function. On the other hand, epoxomicin binds specifically to the proteasome hydrolases [18]. To exclude the possibility that the effects of ALLN or epoxomicin may be indigenous, we used two kinds of PIs.
To activate the Akt signaling pathway, cells were treated with IGF-1 [19] and insulin [20] at the concentration indicated in serum-deprived medium, respectively.
Morphometric analyses of apoptosis and necrosis
Apoptotic cells were detected by propidium iodide (Wako Pure Chemical Industries, Osaka, Japan) staining (permeabilization with 0.1 % Triton X-100 in PBS for 15 min was performed before staining), which allows identification of apoptotic nuclear changes as described previously [13]. Necrotic cells were detected by propidium iodide staining, without permeabilization with Triton X-100, which allows identification of cell nuclei that have lost their plasma membrane integrity (i.e., necrotic cells). Images were acquired using a confocal laser (Zeiss 510 Meta with Lasersharp software, Carl Zeiss MicroImaging Inc; Jena, Germany). The percentage of apoptotic nuclear positive cells and necrotic cells were calculated in 10 visual fields (40×) in one experiment and data were derived from 3 independent experiments. All data are expressed as mean ± SD. Differences between two groups were analyzed using the Mann–Whitney U test. P value <0.05 were considered significant.
Western blotting
We homogenized cells in a lysis buffer composed of 0.187 M trishydroxymethylaminomethane-HCl (pH 6.8), 10 % sodium dodecyl sulfate and 5 mM ethylene diamine tetra-acetic acid. Equal amounts of protein were separated by polyacrylamide gel electrophoresis (Bio-Rad Laboratories, Hercules, CA, USA). Proteins were transferred to polyvinylidene fluoride microporous membrane (Millipore Corporation, Billerica, MA, USA). The blots were blocked with 0.2 % skim milk in Tris-buffered saline containing 0.1 % Triton X-100 followed by incubation with the primary antibodies then secondary antibodies (horseradish peroxidase-linked sheep anti-mouse antibody and donkey anti-rabbit antibody; GE Healthcare, Buckinghamshire, UK). The blots were visualized using enhanced chemiluminescence (ECL Plus Western Blotting Detection Reagents; GE Healthcare, Buckinghamshire, UK). The expression of each protein was measured by Light capture (ATTO Corporation, Tokyo, Japan). All blotting data were derived from at least two independent experiments.
Results
Sorafenib and PIs synergistically induce cell death
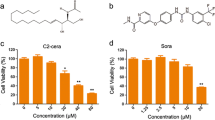
To examine the effect of sorafenib and PIs, including epoxomicin and ALLN, on cell survival, we treated Huh7, Hep3B and OUMS29 with these agents individually or in combination. We assessed apoptosis by propidium iodide staining of permeabilized cells. Apoptotic nuclear changes were evidenced by the typical fragmented nuclear morphology (Fig. 1a). Sorafenib and ALLN induced apoptosis at the concentrations tested in Huh7 and OUMS29 (Fig. 1a, b). The apoptotic changes were clearer in ALLN-treated cells than in sorafenib-treated cells (Fig. 1b).
Effect of sorafenib and PIs on apoptosis. a Phase contrast images (upper) and confocal images of Huh7 cells cultured ± sorafenib (10 μM for 24 h) and/or ALLN (30 μM for 24 h), then permeabilized with 0.1 % Triton X-100 and stained using propidium iodide (bottom) to visualize the nuclei. Sorafenib and/or ALLN treatment induced nucleus fragmentation consistent with apoptosis (arrows). b Morphometric analysis of fragmentation of nucleus. Huh7 (black column) and OUMS29 (white column) cells were treated with sorafenib (10 μM for 24 h) and/or ALLN (30 μM for 24 h). Columns mean (n = 3), bars SD. *P < 0.05. c, d Immunoblotting with indicated antibodies of apoptotic surrogate markers of lysates from cells treated with sorafenib (5 and 10 μM for 24 h) and PIs (ALLN 30 μM for 24 h or epoxomicin 1 μM for 24 h)
To confirm the induction of apoptosis by sorafenib and PIs, we further performed immunoblotting for K18, and cleavage of PARP and caspase3 as surrogate markers. Treatment with epoxomicin and ALLN resulted in K18 fragmentation and cleavage of PARP and caspase3 in hepatoma cells (Fig. 1c) and OUMS29 (Fig. 1d). Formation of the K18 29-kDa caspase-generated fragment is a marker of apoptosis [21, 22]. Sorafenib alone induced apoptosis in both hepatoma cell lines and OUMS29, represented by cleavage of PARP. Induction of K18 fragmentation was clear in hepatoma cell lines, but almost not in OUMS29. Sorafenib induced apoptosis synergistically in combination with PIs in Hep3B (Fig. 1c). However, sorafenib reduced PI-mediated K18 fragmentation and cleavage of PARP and caspase3 in Huh7 (Fig. 1c) and OUMS29 (Fig. 1d).
We also analyzed necrosis by propidium iodide staining (without permeabilization of cells before staining). Interestingly, sorafenib alone induced necrosis as shown by propidium iodide positive nuclei (Fig. 2A, B panels b, f). In control cells (Fig. 2A, panels a, e) and ALLN-treated cells (Fig. 2A, panels c, g), there were few propidium iodide positive nuclei (Fig. 2B). Notably, the combination of sorafenib and ALLN resulted in a marked increase in induction of necrosis in both Huh7 and OUMS29 (Fig. 2A, B, panels d, h).
Effect of sorafenib and PIs on necrosis. a Confocal images of Huh7 and OUMS29 cells cultured ± sorafenib (10 μM for 24 h) and/or ALLN (30 μM for 24 h) then stained using propidium iodide without permeabilization. Propidium iodide staining of nuclei represents necrotic change of the cells. b Morphometric analysis of PI positive of nucleus. Huh7 (black column) and OUMS29 (white column) cells were treated with sorafenib (10 μM for 24 h) and/or ALLN (30 μM for 24 h). Columns mean (n = 3), bars SD. *P < 0.05
Sorafenib enhances PI-mediated cell death via Akt inactivation in hepatoma cells
We next examined the effect of the combination of sorafenib and PIs on activity of the Akt signaling pathway. In the control condition, the Akt activity was higher in hepatoma cell lines (Fig. 3a) than OUMS29 (Fig. 3b). In the present study, PIs alone inhibited phosphorylation of Akt and its downstream p70 S6 kinase in hepatoma cell lines, which is consistent with previous reports (Fig. 3a). However, sorafenib alone increased phosphorylation of Akt and its downstream p70 S6 kinase in both Huh7 (Fig. 3a) and OUMS29 (Fig. 3b). Co-treatment with sorafenib and PIs synergistically inhibited Akt phosphorylation in hepatoma cell lines (Fig. 3a). In contrast, sorafenib blocked the PI-mediated inhibition of Akt phosphorylation in OUMS29 (Fig. 3b).
We also treated Huh7 and OUMS29 with IGF-1 or insulin. IGF-1 or insulin treatment activated Akt phosphorylation in Huh7 (Fig. 4a) and Huh7 and OUMS29 cells-treated with sorafenib and epoxomicin (Fig. 4b, c). Additionally, IGF-1 or insulin treatment suppressed the sorafenib and PI-mediated apoptosis in Huh7 (Fig. 4b) and OUMS29 (Fig. 4c) and necrosis in Huh7 (Fig. 4d, e).
Re-activation of Akt signaling suppresses the sorafenib and PI-mediated cell death. a Immunoblotting with anti-phospho Akt antibody of lysates from Huh7 cells treated with IGF-1 (100 ng/mL for 1, 6 and 12 h) and insulin (100 ng/mL for 1, 6 and 12 h). b, c Immunoblotting with antibodies of apoptotic surrogate markers and phospho Akt of lysates from cells treated with sorafenib (10 μM for 12 h) and epoxomicin (1 μM for 12 h) ± IGF-1 (100 ng/mL for 12 h) or insulin (100 ng/mL for 12 h). d Confocal images of Huh7 cells cultured ± sorafenib (10 μM for 12 h) and ALLN (30 μM for 12 h) plus IGF-1 (100 ng/mL for 12 h) or insulin (100 ng/mL for 12 h) then stained using propidium iodide without permeabilization. e Morphometric analysis of PI positive of nucleus of Huh7 cells. Columns mean (n = 3), bars SD. *P ≤ 0.05
Sorafenib inhibits phosphorylation of stress-activated protein kinases
JNK and p38 are mitogen-activated protein kinases (MAPK) that are activated by various types of stresses, including endoplasmic reticulum (ER) stress. Because PIs induced ER stress via induction of misfolded protein accumulation in the ER lumen, we next examined the effect of sorafenib on JNK and p38 phosphorylation. We treated the hepatoma cells and OUMS29 with sorafenib at concentrations of 5 and 10 μM for 1, 6 and 24 h, respectively. Interestingly, sorafenib inhibited the phosphorylation of JNK and p38 in a time and dose dependent manner in both hepatoma cell lines (Fig. 5a) and in OUMS29 (Fig. 5b). Hep3B cells seemed to be more resistant to this inhibitory effect than Huh7 and OUMS29. Sorafenib also induced down-regulation of the downstream of JNK and p38, phospho c-Jun and phospho cAMP response element-binding protein (CREB). Although the mechanism remains unclear, protein levels of JNK and p38 were also decreased by sorafenib in our study (Fig. 5a, b).
Sorafenib treatment inhibits phosphorylation of stress-activated protein kinases in hepatoma cell lines and OUMS29. a, b Time and dose dependent analysis of Western blotting using indicated antibodies of lysates from cells treated with DMSO for 24 h as a control and sorafenib (5 and 10 μM for 1, 6 and 24 h). c Western blotting using indicated antibodies of Huh7 and OUMS29 treated with ± sorafenib (10 μM) and ALLN (30 μM) for 12 h
Next, we treated Huh7 and OUMS29 with sorafenib and ALLN individually or in combination for 12 h. Proteasome inhibition by ALLN induced phosphorylation of JNK and p38 in Huh7 and OUMS29 (Fig. 5c). Notably, sorafenib also inhibited ALLN-mediated phosphorylation of JNK and p38 in both tested cells (Fig. 5c).
Discussion
As previously reported, both sorafenib and PIs have pleiotropic anti-tumor effects. Sorafenib can inhibit tumor growth and angiogenesis through either Raf/MEK/ERK dependent or independent pathways [23]. However, the precise mechanism of these anti-tumor effects on hepatocytes remains unclear. The present study demonstrated the anti-proliferative effects of sorafenib with relation to phosphorylation of Akt and stress-activated protein kinases.
We demonstrated that sorafenib induced apoptotic and necrotic cell death in hepatoma cell lines and OUMS29 cells (Figs. 1, 2). From the results of morphometry (Fig. 1b) and Western blotting (Fig. 1c, d), the sorafenib-induced apoptosis was clearer in hepatoma cell lines than OUMS29. Because the differentiation of Huh7 is better than Hep3B [24], sorafenib-induced apoptosis was stronger in Hep3B than in Huh7 (Fig. 1c) represented that the cytotoxic effects of sorafenib might be dependent on the difference of differentiation of hematoma cells. Interestingly, the sorafenib-induced necrosis was increased when used in combination with PIs (Fig. 2A, B). Thus, we considered that the combination of sorafenib and PIs induces cell death synergistically, and examined the detailed mechanisms of the synergistic effect of these agents. We also showed the effect of these agents on apoptosis by cleavage of PARP and caspase3 and K18 apoptotic fragmentation. Our results demonstrated that sorafenib alone failed to activate caspase3 in Huh7 (Fig. 1c). In contrast, sorafenib activated caspase3 in OUMS29 (Fig. 1c, d). Other apoptotic markers, including PARP cleavage and K18 apoptotic fragmentation, were also induced by sorafenib, especially in Hep3B (Fig. 1c). Surprisingly, sorafenib down-regulated the PI-induced apoptotic surrogate markers in Huh7 and OUMS29 (Fig. 1c, d). In contrast, sorafenib induced apoptosis synergistically in combination with PIs in Hep3B (Fig. 1c). The sorafenib and PI-induced cell death was clearer in hepatoma cell lines than OUMS29 (Figs. 1b, 2B). Thus, we consider that the effect of sorafenib on cell death, including apoptosis and necrosis differs among cell types.
Several reports have shown that down-regulation of Akt signaling is a major molecular determinant in PI-induced apoptosis in hepatoma cells [11]. Similarly, PIs induced down-regulation of Akt signaling in hepatoma cell lines and OUMS29 in our study (Fig. 3a, b). On the other hand, sorafenib has been reported to induce Akt phosphorylation at threonine 308 and serine 473 in hepatoma cells [25]. The phosphorylation at threonine 308 suggests the activation of phosphoinositide 3-kinase (PI3K), an upstream molecule of Akt, and phosphorylation at serine 473 suggests the activation of mammalian target of rapamycin complex2 (mTORC2) [26]. In the present study, sorafenib alone induced up-regulation of Akt phosphorylation at serine 473 in Huh7 and OUMS29 (Fig. 3a, b).
Notably, sorafenib induced down-regulation of Akt synergistically in combination with PIs in hepatoma cell lines (Fig. 3a). Because Akt activation is implicated in the pathogenesis and development of HCC [27], we consider that the combination of sorafenib and PIs induces a synergistic anti-proliferative effect via Akt down-regulation in hepatoma cells. Actually, the Akt activity was higher in hepatoma cell lines than OUMS29 in control condition. In contrast, sorafenib inhibited the PI-mediated down-regulation of Akt in OUMS29 (Fig. 3b). Thus, the effect of combined sorafenib and PIs on Akt phosphorylation differs between cell types. This difference between hepatoma and hepatocyte cells seems to be attractive in terms of sorafenib and/or PI-mediated anti-tumor effect and liver injury. To examine the contribution of inactivation of Akt in synergistic anti-tumor effect of the combination of sorafenib and PI, we also examined the effect of Akt re-activation. Interestingly, re-activation of Akt by IGF-1 or insulin treatment suppressed the sorafenib and PI-mediated cell death (Fig. 4b, c, d, e).
The MAPK pathway regulates various cellular functions, such as proliferation, differentiation, and apoptosis [28]. The JNK pathway is implicated in regulating liver carcinogenesis and activation of this pathway contributes to hepatocyte proliferation. Recently, an association was shown between the therapeutic response to sorafenib and JNK activation in HCC cells [29]. On the other hand, among MAPKs, JNK and p38 respond to various types of stress, including reactive oxygen species (ROS), tumor necrosis factor-α (TNF-α) and ER stress, and regulate apoptosis through the phosphorylation of various target molecules [30]. Though sorafenib has been reported to inhibit phosphorylation of p38 [31], the exact effect of sorafenib on JNK and p38 activity is still unknown. In the present study, sorafenib inhibited the phosphorylation of JNK and p38 in a time and dose dependent manner in both hepatoma cell lines and OUMS29 (Fig. 5a, b). PIs activated the JNK and p38 pathways via induction of cell stresses (Fig. 5c). Sorafenib also inhibited the PI-mediated JNK and p38 activation (Fig. 5c). Because of the essential roles of JNK and p38 in cellular functions, deregulation of JNK and p38 are often found to contribute to the development of many cancers, including HCC. In addition to participating in cell transformation and carcinogenesis, p38 activation has an association with the invasive or metastatic potential in some human cancers. Thus, our results indicate that sorafenib may suppress HCC progression, in part, via inactivation of JNK and p38 signaling.
In conclusion, our study demonstrated that there are additive or synergistic cytotoxic effects between sorafenib and PIs in HCC. Our results indicate that these synergistic effects have the potential to substantially enhance the clinical efficacy of sorafenib and PIs. The mechanism of synergism involves inhibition of Akt inactivation and perhaps modulation of the JNK and p38 signaling pathways. Further clinical studies to investigate these combinations are clearly warranted.
Abbreviations
- Ab:
-
Antibody
- ALLN:
-
Acetyl-leucyl-leucyl-norleucinal
- CREB:
-
cAMP response element-binding protein
- DAPI:
-
4′6-diamidino-2-phenylindole
- ER:
-
Endoplasmic reticulum
- ERK:
-
Extracellular signal-regulated protein kinase
- HCC:
-
Hepatocellular carcinoma
- IGF-1:
-
Insulin-like growth factor-1
- JNK:
-
c-Jun N-terminal kinase
- K:
-
Keratin
- MAPK:
-
Mitogen-activated protein kinase
- MEK:
-
MAPK/ERK kinase
- mTOR:
-
Mammalian target of rapamycin
- mTORC:
-
Mammalian target of rapamycin complex
- NFκB:
-
Nuclear factor-kappa B
- PARP:
-
Poly-ADP-ribose-polymerase
- PDGFR:
-
Platelet-derived growth factor receptor
- PI:
-
Proteasome inhibitor
- PI3K:
-
Phosphoinositide 3-kinase
- ROS:
-
Reactive oxygen species
- TNF-α:
-
Tumor necrosis factor-α
- TRAF2:
-
Tumor necrosis factor receptor-associated factor-2
- VEGFR:
-
Vascular endothelial growth factor receptor
References
Forner A, Llovet JM, Bruix J. Hepatocellular carcinoma. Lancet. 2012;379:1245–55.
Finn RS. Development of molecularly targeted therapies in hepatocellular carcinoma: where do we go now? Clin Cancer Res. 2010;16:390–7.
Schwartz M, Roayaie S, Konstadoulakis M. Strategies for the management of hepatocellular carcinoma. Nat Clin Pract Oncol. 2007;4:424–32.
Zhu AX. Development of sorafenib and other molecularly targeted agents in hepatocellular carcinoma. Cancer. 2008;112:250–9.
Llovet JM, Ricci S, Mazzaferro V, Hilgard P, Gane E, Blanc JF, SHARP Investigation Study Group, et al. Sorafenib in advanced hepatocellular carcinoma. N Engl J Med. 2008;359:378–90.
Cheng AL, Kang YK, Chen Z, Tsao CJ, Qin S, Kim JS, et al. Efficacy and safety of sorafenib in patients in the Asia-Pacific region with advanced hepatocellular carcinoma: a phase III randomized, double-blind, placebo-controlled trial. Lancet Oncol. 2009;10:25–34.
Wilhelm SM, Carter C, Tang L, Wilkie D, McNabola A, Rong H, et al. BAY 43–9006 exhibits broad spectrum oral autitumor activity and targets the RAF/MEK/ERK pathway and receptor tyrosine kinases involved in tumor progression and angiogenesis. Cancer Res. 2004;64:7099–109.
Adams J. The proteasome: a suitable antineoplastic target. Nat Rev Cancer. 2004;4:349–60.
Kim GP, Mahoney MR, Szydlo D, Mok TS, Marshke R, Holen K, et al. An international, multicenter phase II trial of bortezomib in patients with hepatocellular carcinoma. Invest New Drugs. 2012;30:387–94.
Voorhees PM, Orlowski RZ. The proteasome and proteasome inhibitors in cancer therapy. Annu Rev Pharmacol Toxicol. 2006;46:189–213.
Chen KF, Yeh PY, Yeh KH, Lu YS, Huang SY, Cheng AL. Down-regulation of phosphor-Akt is a major molecular determinant of bortezomib-induced apoptosis in hepatocellular carcinoma cells. Cancer Res. 2008;68:6698–707.
Ganten TM, Koschny R, Haas TL, Sykora J, Li-Weber M, Herzer K, et al. Proteasome inhibition sensitizes hepatocellular carcinoma cells, but not human hepatocytes, to TRAIL. Hepatology. 2005;42:588–97.
Yu C, Friday BB, Lai JP, Yang L, Sarkaria J, Kay NE, et al. Cytotoxic synergy between the multikinase inhibitor sorafenib and the proteasome inhibitor bortezomib in vitro: induction of apoptosis through Akt and c-Jun NH2-terminal kinase pathways. Mol Cancer Ther. 2006;5:2378–87.
Chen KF, Yu HC, Liu TH, Lee SS, Chen PJ, Cheng AL. Synergistic interactions between sorafenib and bortezomib in hepatocellular carcinoma involve PP2A-dependent Akt inactivation. J Hepatol. 2010;52:88–95.
Wright JJ. Combination therapy of bortezomib with novel targeted agents: an emerging treatment strategy. Clin Cancer Res. 2010;16:4094–104.
Kobayashi N, Miyazaki M, Fukaya K, Inoue Y, Sakaguchi M, Uemura T, et al. Transplantation of highly differentiated immortalized human hepatocytes to treat acute liver failure. Transplantation. 2000;69:202–7.
Harada M, Strnad P, Toivola DM, Omary MB. Autophagy modulates keratin-containing inclusion formation and apoptosis in cell culture in a context-dependent fashion. Exp Cell Res. 2008;314:1753–64.
Groll M, Huber R. Inhibitors of the eukaryotic 20S proteasome core particle: a structural approach. Biochim Biophys Acta. 2004;1695:33–44.
Alexia C, Fourmatgeat P, Delautier D, Groyer A. Insulin-like growth factor-I stimulates H4II rat hepatoma cell proliferation: dominant role of PI3′K/Akt signaling. Exp Cell Res. 2006;312:1142–52.
Kawaguchi T, Yoshida T, Harada M, Hisamoto T, Nagao Y, Ide T, et al. Hepatitis C virus down-regulates insulin receptor substrates 1 and 2 through up-regulation of suppressor of cytokine signaling 3. Am J Pathol. 2004;165:1499–508.
Ku NO, Liao J, Omary MB. Apoptosis generates stable fragments of human type I keratins. J Biol Chem. 1997;272:33197–203.
Caulin C, Salvesen GS, Oshima RG. Caspase cleavage of keratin 18 and reorganization of intermediate filaments during epitherial cell apoptosis. J Cell Biol. 1997;138:1379–94.
Liu L, Cao Y, Chen C, Zhang X, McNabola A, Wilkie D, et al. Sorafenib blocks the RAF/MEK/ERK pathway, inhibits tumor angiogenesis, and induces tumor cell apoptosis in hepatocellular carcinoma model PLC/PRF/5. Cancer Res. 2006;66:11851–8.
Bressac B, Galvin KM, Liang TJ, Isselbacher KJ, Wands JR, Ozturk M. Abnormal structure and expression of p53 gene in human hepatocellular carcinoma. Proc Natl Acad Sci USA. 1990;87:1973–7.
Shimizu S, Takehara T, Hikita H, Kodama T, Tsunematsu H, Miyagi T, et al. Inhibition of autophagy potentiates the antitumor effect of the multikinase inhibitor sorafenib in hepatocellular carcinoma. Int J Cancer. 2012;131:548–57.
Foster KG, Fingar DC. Mammalian target of rapamycin (mTOR): conducting the cellular signaling symphony. J Biol Chem. 2010;285:14071–7.
Whittaker S, Marais R, Zhu AX. The role of signaling pathways in the development and treatment of hepatocellular carcinoma. Oncogene. 2010;29:4989–5005.
Krens SF, Spaink HP, Snaar-Jagalska BE. Functions of the MAPK family in vertebrate-development. FEBS Lett. 2006;580:4984–90.
Hagiwara S, Kudo M, Nagai T, Inoue T, Ueshima K, Nishida N, et al. Activation of JNK and high expression level of CD133 predict a poor response to sorafenib in hepatocellular carcinoma. Br J Cancer. 2012;106:1997–2003.
Takeda K, Naguro I, Nishitoh H, Matsuzawa A, Ichijo H. Apoptosis signaling kinases: from stress response to health outcomes. Antioxid Redox Signal. 2011;15:719–61.
Huynh H. Molecularly targeted therapy in hepatocellular carcinoma. Biochem Pharmacol. 2010;80:550–60.
Acknowledgments
Our work is supported by in part by a grant-in-aid (2059798, 23591000) from the Ministry of Education, Culture, Sports, Science and Technology, Japan and UOEH Grant for Advanced Research (H22-1) to M.H. We thank Ms. Y. Katsuki and Ms. H. Mihara for their expert technical assistance.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Honma, Y., Shimizu, S., Takehara, T. et al. Sorafenib enhances proteasome inhibitor-induced cell death via inactivation of Akt and stress-activated protein kinases. J Gastroenterol 49, 517–526 (2014). https://doi.org/10.1007/s00535-013-0796-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00535-013-0796-z