Abstract
The purposes of this study were to determine the influence of kinematic model parameter variability on scapulothoracic angle estimates, and to define which parameters of the kinematic model have the largest effect on scapulothoracic angle estimates. Nominal subject-specific kinematic models of nine participants were implemented. Fifteen parameters of the nominal models relative to the clavicle length, ellipsoid, sternoclavicular and acromioclavicular joint centers, and contact point location were altered from − 1 to 1 cm. Then, scapulothoracic angles were computed during four movements using multibody kinematic optimizations for nominal and altered models. The percentage of scapulothoracic angle variance explained by each parameter of the kinematic model was computed using Effective Algorithm for Computing Global Sensitivity Indices. When altering simultaneously the 15 parameters of the kinematic model, scapulothoracic angles varied up to 50°. For all movements and degrees of freedom, the clavicle length significantly explained the largest part of scapulothoracic angle variance (up to 25%, p < 0.01). In conclusion, kinematic model parameters need to be estimated accurately to avoid any bias in scapulothoracic angle estimates especially in a clinical context. The present sensitivity analysis may also be used as a benchmark for future works focusing on improving shoulder kinematic models.
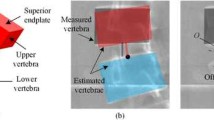
Graphical abstract
The curves represent mean scapulothoracic angles computed with the nominal model and their variability when kinematic model parameters are altered. The colormap graphs represent the percentage of scapulothoracic angle variance explained by each parameter of the kinematic model.

Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
Scapular positioning and motion are of great interest in patients suffering from shoulder problems. Indeed, an alteration in the normal position or motion of the scapula relative to the thorax, named scapular dyskinesis [1], may be the cause or consequence of shoulder troubles [2]. In this context, scapular motions have to be assessed and quantified by clinicians [3]. However, the accuracy of such clinical assessment is limited by soft tissue artifacts, due to the bones sliding underneath the skin [4]. Improvement of procedures to estimate accurately scapulothoracic joint motion therefore remains crucial to help clinicians in their diagnosis.
Among procedures depicted to quantify scapulothoracic joint angles, the multibody kinematic optimization (MKO) would be the most promising approach [5]. The latter consists of optimizing joint angles by minimizing the distance between the positions of the measured markers and the virtual markers attached to the kinematic model. For the scapulothoracic joint, the MKO has been improved, on one hand, by enforcing the scapula to stay in contact with the surface of an ellipsoid representing the sliding plane between the scapula and the thorax, and on the other hand, by ensuring a constant clavicle length to avoid non-physiological joint dislocation [6,7,8]. These kinematic models are thus defined by several parameters, namely, the clavicle length, the location of the sternoclavicular and acromioclavicular joints, the ellipsoid’s dimension and location, and the location of the scapulothoracic contact point. To ensure accurate estimation of scapulothoracic joint angles, these parameters demand also subject-specific calibration. Although several studies proposed methods to calibrate the kinematic model [8, 9], subject- or patient-specific configuration of all the model parameters may be time-consuming [10] or irradiant [11] when based on imagery and therefore sometimes hard-to-use in a clinical context. In consequence, screening and quantifying the kinematic model parameters presenting the greatest influence on the scapulothoracic angle estimates may be useful to find the best trade-off between accuracy and efficiency in a clinical context.
To the best of our knowledge, few studies [12, 13] assessed the sensitivity of the scapulothoracic angle estimates to the kinematic model parameters. When altering the radii and the location of the ellipsoid center by more or less 20% of a nominal model, scapulothoracic joint angles varied about 15° during wheelchair propulsion [12]. During arm elevation in the frontal plane, scapulothoracic angles were the most sensitive to the clavicle length followed by the scapulothoracic contact point location and the center of the ellipsoid [13]. Although these two studies help to determine in what extend scapulothoracic angle estimates are sensitive to kinematic model parameters, some concerns may be raised. First, only one participant and one movement were investigated while the sensitivity analysis may also depend on individual and movement variability. Second, no study has investigated the sensitivity of the scapulothoracic angles to the location of the sterno- and acromioclavicular joints.
The purpose of this study was twofold: (1) to determine the influence of the kinematic model parameters variability on scapulothoracic angle estimates (uncertainty analysis) and (2) to define which parameters of the kinematic model have the largest effect on scapulothoracic angle estimates (sensitivity analysis). It was hypothesized that scapulothoracic angles were affected by alterations of the kinematic model parameters, especially when the clavicle length changed.
2 Methods
2.1 Participants
Nine healthy males (29.2 ± 8.2 years, 1.74 ± 0.08 m, 73.7 ± 9.6 kg) volunteered to participate in this study. All participants declared having no upper-limb and shoulder injury during the year prior to the experiment. The study was approved by the ethical committee Ouest V (2018-A02449-46) according to the statements of ethical principles of the Declaration of Helsinki, and the participants signed an informed consent document.
2.2 Data collection and procedure
Participants were fitted with spherical reflective markers located on the thorax (6 markers), right clavicle (2), and right scapula (8) (Fig. 1). For further calibration of the kinematic model, participants were asked to hold five static poses corresponding to 0%, 25%, 50%, 75%, and 100% of maximal arm elevation in the scapular plane (defined by a goniometer as 40° from the frontal plane [14]). At each pose, a scapula locator was used to identify the location of the acromion posterior edge, trigonum spinae, and scapular inferior angle. Thereafter, participants performed five movements, namely, three unilateral arm elevation/depression (one in the frontal, one in the scapular, and one in sagittal plane), one horizontal unilateral abduction, and one ball throw. The latter consisted of performing an overarm throw, at submaximal preferred speed (5.63 ± 1.96 m.s−1), of a tennis ball into a 1-m side length square located at 3 m in front of the participant. Marker trajectories were recorded using a 10-camera optoelectronic system with a sample frequency of 200 Hz (Qualysis, Sweden).
2.3 Nominal kinematic model
The nominal kinematic model was calibrated to each participant’s anthropometry. The model was composed of three segments (thorax, clavicle, and scapula) for which coordinate systems were implemented regarding the International Society of Biomechanics recommendations [15]. The coordinates of the scapula center recorded with the scapula locator (i.e., barycenter of the acromion posterior edge, trigonum spinae, and scapular inferior angle) were used to calibrate the dimension of the ellipsoid (i.e., three radii), while its center was fixed to the thorax origin reference system (i.e., midpoint between the xiphoid process and the eight’s vertebra) [16]. Sternoclavicular and acromioclavicular joint locations were defined by palpation in line with Michaud, et al. [9] recommendations. Based on Seth et al. [6], the model could be actuated by six degrees of freedom (DoF) between the ground and the thorax, and five DoF between the scapula and the thorax (i.e., two DoF for the translation of the scapula center along the ellipsoid surface and three DoF for scapular rotations) (see the mathematical description in supplementary file for more details).
Model-derived joint angles were computed for each movement using MKO subject to an equality constraint ensuring a constant clavicle length. Scapulothoracic angles were extracted following the sequence upward/downward rotation, internal/external rotation, and anterior/posterior tilt.
2.4 Uncertainty and sensitivity analysis
Both uncertainty and sensitivity analysis were performed regarding Pianosi et al.’s [17] recommendations. The first step consisted of applying a variation from − 1 to 1 cm on fifteen parameters of the nominal kinematic models relative to the ellipsoid (6 parameters), clavicle (7), and the scapulothoracic contact point (2) (Fig. 2). To that end, a Latin-hypercube sampling procedure was used by varying all the parameters at a time to obtain 10 000 different values per parameter. Then for each participant, each movement, and each altered kinematic model, the MKO was run to compute the new scapulothoracic joint angles. If the MKO did not satisfy the equality constraint (tolerance = 10–6 m), the simulation was removed from the analysis.
Parameters of the kinematic model undergoing alterations. 3D coordinates of the ellipsoid center (OE) in the thorax reference system {XT, YT, ZT} (n = 3), ellipsoid radii (n = 3), 3D coordinates of the sternoclavicular joint (OC) in the thorax reference system (n = 3), 3D coordinates of the acromioclavicular joint (OS) in the scapula reference system {XS, YS, ZS} (n = 3), the clavicle length being the Euclidian distance between the sternoclavicular and acromioclavicular joints (n = 1), 2D scapulo-thoracic contact point (STCS) in the scapular plane {XS, ZS} (n = 2)
To assess whether the uncertainty and sensitivity analyses were independent of the input sample size, the convergence of the scapulothoracic angle variance was visually analyzed from 100 to 10 000 simulations. The slope of the scapulothoracic angles variance between the 9 000th and 10 000th simulation was then computed. The linearity of the relationship between the kinematic model parameters and the scapulothoracic angles was graphically controlled.
Concerning the uncertainty analysis, the overall effect of kinematic model parameters on scapulothoracic angles was represented through two standard deviations to the mean computed from all the simulations of each participant and each movement.
For the first-order sensitivity analysis, the percentage of scapulothoracic angle variance explained by each parameter of the kinematic model was computed using Effective Algorithm for Computing Global Sensitivity Indices [18]. For each DoF, the proportion of scapulothoracic angle variance explained by each kinematic model parameter was averaged over the time. Then, the influence of the kinematic model parameter variability on the variance explained was assessed using linear mixed models with logit correction. When a main effect was revealed by the linear mixed-model, post hoc pairwise comparisons were performed using Tukey’s honestly significant difference procedure (R core Team, lme4 package). In addition, SPM random effect analyses [19] were used to compute alpha parameters, quantifying the slope of the linear relationships between each kinematic model parameter and scapulothoracic angles variation over the time.
3 Results
Convergence analysis of scapulothoracic angle variance showed that 10 000 simulations were adequate since the slope of the variance between the last 1 000 simulations was inferior to 0.001 (see figure S1 and Table T1 in the supplementary file for more details).
3.1 Uncertainty
When altering simultaneously the 15 parameters of the kinematic model from − 1 to 1 cm, mean scapulothoracic angles variation over the time ranged from 9.8 to 32.6°, 8.9 to 33.1°, 9.7 to 43.6°, 18.9 to 44.6°, and 9.5 to 49.5° for arm elevation/depression in the frontal, scapular, and sagittal plane, for horizontal abduction and for ball throw respectively (Figs. 3, 4 and 5, and table T2 and Fig.S2-S3 in the supplementary file). Furthermore, scapulothoracic angle variations changed regarding the phase of the movement and the DoF, with the highest variabilities observed at the middle or at the end of the movement for arm elevations/depressions and throwing respectively.
Nominal (thick black line), mean (dashed line), and ± 2 standard deviations from the mean (gray lines) scapulothoracic angles (ST) as a function of the normalized time (from 0 to 100%) computed during arm elevation/depression in the scapular plane for the 10 000 simulations and the nine participants. The color bars represent the average proportion of scapulothoracic angle variance explained by each of the 15 parameters of the kinematic model. EllR for ellipsoid radii, EllC for ellipsoid center, ClavLength for clavicle length, AC for acromioclavicular joint location, SC for sternoclavicular joint location, ScapCon for scapulothoracic contact point location
Nominal (thick black line), mean (dashed line), and ± 2 standard deviations from the mean (gray lines) scapulothoracic angles (ST) as a function of the normalized time (from 0 to 100%) computed during horizontal abduction for the 10 000 simulations and the nine participants. The color bars represent the average proportion of scapulothoracic angle variance explained by each of the 15 parameters of the kinematic model. EllR for ellipsoid radii, EllC for ellipsoid center, ClavLength for clavicle length, AC for acromioclavicular joint location, SC for sternoclavicular joint location, ScapCon for scapulothoracic contact point location
Nominal (thick black line), mean (dashed line), and ± 2 standard deviations from the mean (gray lines) scapulothoracic angles (ST) as a function of the normalized time (from 0 to 100%) computed during ball throwing for the 10 000 simulations and the nine participants. The color bars represent the average proportion of scapulothoracic angle variance explained by each of the 15 parameters of the kinematic model. EllR for ellipsoid radii, EllC for ellipsoid center, ClavLength for clavicle length, AC for acromioclavicular joint location, SC for sternoclavicular joint location, ScapCon for scapulothoracic contact point location
3.2 Sensitivity
For all movements and DoF, the clavicle length is the parameter that most explained the scapulothoracic angle variance (from 14 to 25% on average, p < 0.01), followed by the acromioclavicular joint location in the antero-posterior direction (from 9 to 18% on average, p < 0.01) and the sternoclavicular joint location in the medio-lateral direction (from 5 to 15% on average, p < 0.01) (Figs. 3, 4 and 5, and table T2 and Fig.S2-S3 in the supplementary file). Discrepancies between movements and DoF were observed concerning the influence of both the sternoclavicular joint location in the antero-posterior direction and the center of the ellipsoid in the medio-lateral and antero-posterior directions on scapulothoracic angle variance (from 3 to 9%, from 3 to 11%, and from 2 to 13% respectively). For all movements and DoF, the location of the scapulothoracic contact point, the ellipsoid vertical radius, and the ellipsoid center location in the vertical direction presented the least influence on scapulothoracic angle variance (from 0.1 to 1.6% on average, p < 0.01). The scapulothoracic angle variance was not fully explained by the 15 kinematic model parameters. The proportion of variance explained by the interaction effects between the kinematic model parameters ranged on average from 30 to 34%, 12 to 26%, 10 to 27%, 14 to 20%, and 7 to 11% for arm elevation/depression in the scapular plane, horizontal abduction, ball throw, and elevation/depression in the frontal and sagittal planes respectively.
Alpha parameters computed with SPM random effect analyses revealed that for arm elevation/depression in the sagittal and scapular planes, and ball throwing, lengthening the clavicle by 1 cm increased scapular downward rotation and posterior tilt on average from 4.1 to 7.1° and from 4.0 to 4.4° respectively. Lengthening the clavicle by 1 cm also increased scapular internal rotation from 3.6 to 4.1° on average during arm elevation/depression in the sagittal plane and horizontal abduction (Fig. 6, 7 and 8 and Fig. S4-S5 in the supplementary file). In addition, for all movements but the horizontal abduction, when moving anteriorly the acromioclavicular joint center or when moving laterally or posteriorly the sternoclavicular joint center by 1 cm, scapular downward rotation increased on average from 3.1 to 5.9°, from 2.9 to 5.6°, and from 1.9 to 3.2°, respectively, while the scapular posterior tilt increased from 3.1 to 3.7°, from 2.1 to 3.1°, and from 1.8 to 2.7° respectively. The linear relationship between the abovementioned parameters and the scapular internal rotation was only significant for the midpart of the movements. Concerning the horizontal abduction, moving anteriorly the acromioclavicular joint center or moving laterally or posteriorly the sternoclavicular joint center by 1 cm led to increased scapular internal rotation by on average 3.7°, 2.8°, and 1.9° respectively (Fig. 6, 7 and 8 and Fig. S4-S5 in the supplementary file). Finally, moving laterally the ellipsoid center by 1 cm mainly increased the scapular upward rotation and internal rotation for all movements up to 3.0° and 1.8° respectively. When moving anteriorly the ellipsoid center by 1 cm, upward and internal rotations were significantly increased only for arm elevation/depression in the scapular and frontal planes and during horizontal abduction (Fig. 6, 7 and 8 and Fig. S4-S5 in the supplementary file).
Mean (line) and standard error of the mean (shadow) of the alpha parameter, representing the slope of the linear relationship between kinematic model parameters and scapulothoracic angle variation, with respect to the normalized time (from 0 to 100%) during arm elevation/depression in the scapular plane. Horizontal lines represent, for each degree of freedom, the part of the curve for which a significant relationship is revealed (p < 0.05)
Mean (line) and standard error of the mean (shadow) of the alpha parameter, representing the slope of the linear relationship between kinematic model parameters and scapulothoracic angle variation, with respect to the normalized time (from 0 to 100%) during horizontal abduction. Horizontal lines represent, for each degree of freedom, the part of the curve for which a significant relationship is revealed (p < 0.05)
Mean (line) and standard error of the mean (shadow) of the alpha parameter, representing the slope of the linear relationship between kinematic model parameters and scapulothoracic angle variation, with respect to the normalized time (from 0 to 100%) during ball throwing. Horizontal lines represent, for each degree of freedom, the part of the curve for which a significant relationship is revealed (p < 0.05)
4 Discussion
The purposes of this study were first to determine the influence of the kinematic model parameters variability on scapulothoracic angle estimates, and second to define which kinematic model parameters have the largest effect on scapulothoracic angle estimates. The main findings were that altering kinematic model parameters from − 1 to 1 cm resulted in scapulothoracic angle estimate variations up to 50° depending on the movement studied, and that scapulothoracic angles were the most sensitive to the clavicle length.
Very little attention has been paid so far to the uncertainty analysis of shoulder kinematic model parameters on scapulothoracic angles, since to the best of our knowledge only one study focused on this topic [12]. We observed a variability of scapulothoracic angles about twice greater than the one described during wheelchair propulsion. However, we have explored movements with higher range of motion and only ellipsoid parameters were altered in Hybois’s study [12], while other parameters relative to the clavicle and scapulothoracic contact point were also altered in our study. In a clinical context, the results of our uncertainty analysis suggest that clinicians should take caution when a kinematic model is used to assess the evolution of scapular positioning over the time. Indeed, slight differences in the calibration of the kinematic model may lead to drastic changes in scapulothoracic angles, which may be a non-negligible confounding factor when assessing scapular dyskinesis for instance [3]. Therefore, calibrating the kinematic model demands caution when assessment of scapular positioning is performed.
Cadaveric and in vivo studies showed that changing the clavicle length significantly affects scapulothoracic angles [20, 21]. A previous sensitivity analysis also depicts that clavicle length is the kinematic model parameter that most influences scapulothoracic angles during arm abduction [13]. Such outcomes are reinforced by our study since we observed that the clavicle length was also the most influential parameter for all investigated movements. In consequence, when scapulothoracic angles are estimated with MKO, the clavicle length of the patient must be estimated accurately. To that end, computed tomography [22] and conventional radiograph [23] are the favored option for clinicians but expose the patient to radiations and may be time consuming. Low-dose biplane X-rays [11] can be also considered as an alternative solution. In addition, a procedure based on navigation ultrasound has been suggested as a non-invasive method to assess clavicle length [22]. Although this approach seems promising, it might be also time consuming in a clinical context. Finally, a palpation method has also been proposed to measure clavicle length [24]; nevertheless, further study should explore the accuracy of such procedure.
Noninvasive palpation methods used to determine sternoclavicular and acromioclavicular joint center location are subject to errors ranging from 1.5 to 3 cm on average [9]. Besides, we observed that altering the location of these joint centers may lead to variations up to 6°/cm. Consequently, determining sternoclavicular and acromioclavicular joint locations with noninvasive methods, such as palpation, may not be satisfying to accurately estimate scapulothoracic angles. In a clinical context, imagery procedures based on low-dose radiation should be preferred [25]. Although time consuming, the use of ultrasonography coupled with a motion capture system seems to be interesting since it avoids any radiation exposure [22]. However, further studies demand also to be conducted to assess the accuracy of such a method.
When assessing scapulothoracic angles, most of shoulder kinematic models enforce the scapula to stay in contact with an ellipsoid representing the scapulothoracic sliding plane to avoid any non-physiological scapular winging [5]. Several procedures have been suggested to calibrate the ellipsoid (i.e., radii and center location) [7, 8, 26]. Our results led us to suggest that efforts should focus on the ellipsoid center location especially in the anteroposterior and mediolateral directions. In addition, the vertical position of the ellipsoid center or its vertical radii may not deserve too much attention during the calibration procedure since they barely influence scapulothoracic angle estimates. Although previous studies depicted promising approaches to calibrate the ellipsoid [8, 16], further researches should be conducted to calibrate subject- and movement-specific ellipsoid when scapulothoracic angle estimates are of interest. To that end, MKO including model parameters in the optimization process may be explored [27, 28].
A previous study highlighted the relevancy of performing the sensitivity analysis throughout the movement instead of considering time averages since variations may occur over the movement [29]. Although the main findings are discussed above, we also observed that the most influential parameters may vary over the time, meaning that ranking the kinematic model parameters that should be calibrated in priority is not always a straightforward process. In addition, only first-order effects have been analyzed, while interactions between parameters may have a non-negligible influence on scapulothoracic angles estimates. The fact that the sensitivity analysis revealed major interaction effects is logical as the kinematic chain represents a close loop between scapula and thorax. Therefore, further investigations focusing on screening approach could be conducted to assess these interaction effects.
This study presents some limitations warranting discussion. First, our results can only be applied in the domain of variation investigated (i.e., ± 1 cm of alteration of the kinematic model parameters). Nevertheless, in a preliminary study, we attempt to make varied kinematic model parameters from − 2 to 2 cm, but the optimization procedure did not converge in many simulations. Second, the scapulothoracic contact point location barely influenced scapulothoracic angle estimates. However, this result should be taken with caution since different conclusions may have been drawn when more than one contact point is defined or when the contact point is initially located at the medial border of the scapula [7].
5 Conclusion
Uncertainty of shoulder kinematic model parameters may drastically influence scapulothoracic angle estimates either for analytical or sport movement. In addition, scapular kinematics are particularly sensitive to clavicle length, and to a lesser extent to sterno- and acromioclavicular joint locations, and ellipsoid parameters. Therefore, it is necessary to keep on developing numerical tools and procedures both accurate and easy-to-use to calibrate shoulder kinematic models when looking for assessing scapulothoracic angles.
References
Kibler WB, Ludewig PM, McClure PW, Michener LA, Bak K, Sciascia AD (2013) Clinical implications of scapular dyskinesis in shoulder injury: the 2013 consensus statement from the ‘Scapular Summit.’ Br J Sports Med 47:877–885. https://doi.org/10.1136/bjsports-2013-092425
Kibler WB, Sciascia A, Wilkes T (2012) Scapular dyskinesis and its relation to shoulder injury. J Am Acad Orthop Surg 20:364–372. https://doi.org/10.5435/JAAOS-20-06-364
Carbone S, Moroder P, Runer A, Resch H, Gumina S, Hertel R (2016) Scapular dyskinesis after Latarjet procedure. J Shoulder Elbow Surg 25:422–427. https://doi.org/10.1016/j.jse.2015.08.001
Begon M, Andersen MS, Dumas R (2018) Multibody kinematics optimization for the estimation of upper and lower limb human joint kinematics: a systematized methodological review. J Biomech Eng 140. https://doi.org/10.1115/1.4038741
Duprey S, Naaim A, Moissenet F, Begon M, Cheze L (2017) Kinematic models of the upper limb joints for multibody kinematics optimisation: an overview. J Biomech 62:87–94. https://doi.org/10.1016/j.jbiomech.2016.12.005
Seth A, Matias R, Veloso AP, Delp SL (2016) A biomechanical model of the scapulothoracic joint to accurately capture scapular kinematics during shoulder movements. PLoS ONE 11:e0141028. https://doi.org/10.1371/journal.pone.0141028
Prinold JA, Bull AM (2014) Scaling and kinematics optimisation of the scapula and thorax in upper limb musculoskeletal models. J Biomech 47:2813–2819. https://doi.org/10.1016/j.jbiomech.2014.05.015
Michaud B, Duprey S, Begon M (2017) Scapular kinematic reconstruction – segmental optimization, multibody optimization with openloop or closed-loop chains: which one should be preferred? Int Biomech 4:86–94. https://doi.org/10.1080/23335432.2017.1405741
Michaud B, Jackson M, Arndt A, Lundberg A, Begon M (2016) Determining in vivo sternoclavicular, acromioclavicular and glenohumeral joint centre locations from skin markers, CT-scans and intracortical pins: a comparison study. Med Eng Phys 38:290–296. https://doi.org/10.1016/j.medengphy.2015.12.004
Charbonnier C, Chague S, Kolo FC, Chow JC, Ladermann A (2014) A patient-specific measurement technique to model shoulder joint kinematics. Orthop Traumatol Surg Res 100:715–719. https://doi.org/10.1016/j.otsr.2014.06.015
Dumas R, Duprey S (2022) Subject-specific model-derived kinematics of the shoulder based on skin markers during arm abduction up to 180° - assessment of 4 gleno-humeral joint models. J Biomech 136:111061. https://doi.org/10.1016/j.jbiomech.2022.111061
Hybois S, Lombart A, Puchaud P, Bascou J, Lavaste F, Pillet H et al (2017) Effects of ellipsoid parameters on scapula motion during manual wheelchair propulsion based on multibody kinematics optimization. A preliminary study. Comput Methods Biomech Biomed Engin 20:107–108. https://doi.org/10.1080/10255842.2017.1382884
El Habachi A, Duprey S, Cheze L, Dumas R (2013) Global sensitivity analysis of the kinematics obtained with a multi-body optimisation using a parallel mechanism of the shoulder. Comput Methods Biomech Biomed Engin 16(Suppl 1):61–62. https://doi.org/10.1080/10255842.2013.815907
Ludewig PM, Phadke V, Braman JP, Hassett DR, Cieminski CJ, LaPrade RF (2009) Motion of the shoulder complex during multiplanar humeral elevation. J Bone Joint Surg Am 91:378–389. https://doi.org/10.2106/JBJS.G.01483
Wu G, van der Helm FC, Veeger HE, Makhsous M, Van Roy P, Anglin C et al (2005) ISB recommendation on definitions of joint coordinate systems of various joints for the reporting of human joint motion–part II: shoulder, elbow, wrist and hand. J Biomech 38:981–992. https://doi.org/10.1016/j.jbiomech.2004.05.042
Blache Y, Degot M, Rogowski I (2022) Does scapulothoracic contact point trajectory follow an ellipsoid surface? Comput Methods Biomech Biomed Engin 24:sup1, S1-S325. https://doi.org/10.1080/10255842.2021.1978758
Pianosi F, Beven K, Freer J, Hall JW, Rougier J, Stephenson DB et al (2016) Sensitivity analysis of environmental models: a systematic review with practical workflow. Environ Model Softw 79:214–232. https://doi.org/10.1016/j.envsoft.2016.02.008
Plischke E (2010) An effective algorithm for computing global sensitivity indices (EASI). Reliab Eng Syst Saf 95:354–360. https://doi.org/10.1016/j.ress.2009.11.005
Pataky TC (2010) Generalized n-dimensional biomechanical field analysis using statistical parametric mapping. J Biomech 43:1976–1982. https://doi.org/10.1016/j.jbiomech.2010.03.008
Hillen RJ, Burger BJ, Poll RG, van Dijk CN, Veeger DH (2012) The effect of experimental shortening of the clavicle on shoulder kinematics. Clin Biomech 27:777–781. https://doi.org/10.1016/j.clinbiomech.2012.05.003
Su WR, Chen WL, Chen RH, Hong CK, Jou IM, Lin CL (2016) Evaluation of three-dimensional scapular kinematics and shoulder function in patients with short malunion of clavicle fractures. J Orthop Sci 21:739–744. https://doi.org/10.1016/j.jos.2016.07.005
Thorsmark Hoj A, Villa C, Christensen OM, Torp-Pedersen S, Overgaard S, Frich LH (2017) Validation of navigation ultrasound for clavicular length measurement. Ultrasound Med Biol 43:1722–1728. https://doi.org/10.1016/j.ultrasmedbio.2017.04.005
Smekal V, Deml C, Irenberger A, Niederwanger C, Lutz M, Blauth M et al (2008) Length determination in midshaft clavicle fractures: validation of measurement. J Orthop Trauma 22:458–462
Stegeman SA, de Witte PB, Boonstra S, de Groot JH, Nagels J, Krijnen P et al (2016) Measurement of clavicular length and shortening after a midshaft clavicular fracture: spatial digitization versus planar roentgen photogrammetry. J Electromyogr Kinesiol 29:74–80. https://doi.org/10.1016/j.jelekin.2015.07.007
Nicholson KF, Richardson RT, Miller F, Richards JG (2017) Determining 3D scapular orientation with scapula models and biplane 2D images. Med Eng Phys 41:103–108. https://doi.org/10.1016/j.medengphy.2017.01.012
Bolsterlee B, Veeger HE, van der Helm FC (2014) Modelling clavicular and scapular kinematics: from measurement to simulation. Med Biol Eng Comput 52:283–291. https://doi.org/10.1007/s11517-013-1065-2
Reinbolt JA, Schutte JF, Fregly BJ, Koh BI, Haftka RT, George AD et al (2005) Determination of patient-specific multi-joint kinematic models through two-level optimization. J Biomech 38:621–626. https://doi.org/10.1016/j.jbiomech.2004.03.031
Andersen MS, Damsgaard M, MacWilliams B, Rasmussen J (2010) A computationally efficient optimisation-based method for parameter identification of kinematically determinate and over-determinate biomechanical systems. Comput Methods Biomech Biomed Engin 13:171–183. https://doi.org/10.1080/10255840903067080
Jacquelin E, Brizard D, Dumas R (2019) A screening method to analyse the sensitivity of a lower limb multibody kinematic model. Comput Methods Biomech Biomed Engin 22:925–935. https://doi.org/10.1080/10255842.2019.1604950
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Informed consent
This research involved human participants who signed an informed consent after the study was approved by the local ethical committee.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Blache, Y., Rogowski, I., Degot, M. et al. Uncertainty analysis and sensitivity of scapulothoracic joint angles to kinematic model parameters. Med Biol Eng Comput 60, 2065–2075 (2022). https://doi.org/10.1007/s11517-022-02593-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11517-022-02593-1