Abstract
Twenty-six strains of Vibrio parahaemolyticus and 14 strains of V. vulnificus isolated from selected beaches in Lagos State, Nigeria, were examined for virulence and antimicrobial resistance genes. The V. parahaemolyticus isolates were further serotyped and subjected to pulsed field gel electrophoresis (PFGE). Five strains of V. vulnificus and one of V. parahaemolyticus carried the New Delhi-metallo-beta-lactamase gene blaNDM-1, seven strains carried blaTEM, and four strains of V. vulnificus and one of V. parahaemolyticus carried blaCMY. Real-time PCR assay for detection of virulence genes tdh and trh in the V. parahaemolyticus isolates showed that five isolates were positive for tdh, two for trh, and one isolate carried both genes. Ten V. parahaemolyticus serogroups and 23 pulsotypes were identified from 26 isolates based on O and K antigens typing and PFGE. Five of the isolates belong to the pandemic strains O1:Kut and O3:K6, and three belonged to the highly virulent O4:Kut serotype. Nineteen of the isolates showed distinct PFGE banding patterns. These results highlighted the importance of Nigerian recreational beaches as reservoirs of antimicrobial resistance genes of global public health interest, such as blaNDM-1.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Antimicrobial resistance in bacteria has become a serious public health problem worldwide (WHO 2015). Initially, concerns about the problem of resistance focused on hospitals, but recently, the presence of clinically relevant antimicrobial resistance genes in the natural environment has become a source of worry to the scientific community (Pruden et al. 2013; Berendonk et al. 2015). Routes of exposure to antimicrobial resistance outside the hospital setting include contact with human and animal carriers, and contaminated food and water (Valverde et al. 2008; Kennedy and Collignon 2010; Coleman et al. 2012). Exposure through the water route can occur by drinking contaminated water or by contact with recreational water at freshwater and marine beaches.
Beach tourism has evolved to be an important and rapidly growing activity in the world due to its suitability for recreation and sporting activities (Orams 2003) leading to a concomitant increase in the incidence of infections associated with recreational waters over the past decade (Halliday and Gast 2011). Thus, the current challenge posed by the presence of antimicrobial-resistant bacteria in the environment is an important public health issue for beach goers and those living in coastal areas. This problem is more acute in the developing world where the aquatic ecosystem serves as a sink for untreated wastewater from domestic, industrial, hospital, agricultural, and aquaculture sources. Through this practice, residual antimicrobial agents, antimicrobial-resistant bacteria, and antimicrobial resistance genes enter the aquatic environment (Taylor et al. 2011). In addition, the usual flow of human traffic to coastal areas in search of jobs and recreation with the attendant anthropogenic impact, and the corresponding lack of surface water quality monitoring in many developing countries, make recreational beaches in these countries an area of special interest for the development and spread of antimicrobial resistance (Overbey et al. 2015). Unfortunately, very little is known about the health status of beaches in Nigeria, especially as it relates to the presence of bacteria carrying clinically relevant antimicrobial resistance genes.
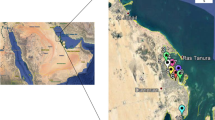
Lagos State, located in the south-western part of Nigeria on the narrow coastal floodplain of the Bight of Benin, consists of a long coastline of about 255 km long stretching from Epe in the east to Cotonu in the Republic of Benin to the west. This long coastline is home to a number of marine recreational beaches who by virtue of their location in the tropical ecosystem makes them potential breeding ground for the proliferation of pathogenic or potentially pathogenic bacteria such as Vibrio species whose presence in the aquatic ecosystem has been known to be positively correlated with mean water temperature (Blackwell and Oliver 2008; Rosec et al. 2009; Johnson et al. 2010; Urquhart et al. 2016).
Potentially, human pathogenic species of Vibrio such as V. parahaemolyticus, V. vulnificus, and non-O1/non-O39 V. cholera are common inhabitants of marine and brackish water environments worldwide (Fabbro et al. 2010; Johnson et al. 2012; Oliver et al. 2013; Ceccarelli et al. 2013; Wu et al. 2014). These organisms are important causal agent of septicemia, and gastrointestinal and wound infections, especially in immunocompromised patients (Daniels and Shafaie 2000; Drake et al. 2007). V. parahaemolyticus and V. vulnificus in particular are leading causes of human intestinal and wound infections after consumption of raw and undercooked seafood or contact with seawater during beach activities (Letchumanan et al. 2014). However, despite the growing importance of environmental Vibrio species as agents of opportunistic infections and reservoir of antimicrobial resistance genes (García-Aljaro et al. 2014), most studies of antimicrobial resistance in Vibrio species have focused on clinical and aquaculture isolates (Okoh and Igbinosa 2010). Only few studies have investigated the resistance of environmental isolates of Vibrio to antimicrobial agents (Baker-Austin et al. 2008; Okoh and Igbinosa 2010; Mudryk et al. 2013; Shaw et al. 2014; Baron et al. 2016; De Menezes et al. 2017; Ghenem and Elhadi 2018); fewer still among these studies focused on recreational beaches and none of these studies emanated from Nigeria, the most populous nation in Africa where little is known of antimicrobial resistance in environmental reservoirs.
In this study, we investigated the prevalence of resistance to selected antimicrobials, and the presence of virulence and antimicrobial resistance genes in V. parahaemolyticus and V. vulnificus isolated from public beaches along the shoreline of Lagos in southwestern Nigeria. We also used pulse field gel electrophoresis (PFGE) to detect clonal relationship among V. parahaemolyticus isolates. Our aim is to generate important baseline information on the health status of Nigerian recreational beaches and their role as reservoir of antimicrobial resistance that can pose a threat to the health of beach goers.
Material and methods
Strains of V. parahaemolyticus and V. vulnificus used in this study
Eighty-five strains of V. parahaemolyticus and V. vulnificus were isolated from Eleko (ELK), Lekki (LEK), Takwa Bay (TAK), and Badagry (BDG) beaches, Lagos, Nigeria, as previously described (Oyelade et al. 2018). Typical V. parahaemolyticus and V. vulnificus colonies were selected from CHROMagar™ Vibrio plates (CHROMagar, Paris, France) after enrichment in alkaline peptone water. Presumptive V. vulnificus colonies were further subcultured onto mCPC agar and TCBS agar before the identities of both V. parahaemolyticus and V. vulnificus were confirmed using API20E (API system, France) (Dumontet et al. 2000) and qPCR detection of tlh genes (V. prahaemolyticus) and vvhA genes (V. vulnificus) as previously described (Nordstrom et al. 2007; Campbell and Wright 2003). The isolated organisms were screened for resistance to ceftazidime (16 μg/ml) and meropenem (4 μg/ml) as indicators of extended spectrum beta-lactamase (ESBL) and carbapenemase production based on CLSI breakpoints listed in Table 20 of CLSI document M45-A3 (CLSI 2016). Forty isolates (26 V. parahaemolyticus and 14 V. vulnificus) that showed resistance to ceftazidime and meropenem were selected for further analysis. The origins, sources, and dates of isolation of the strains are listed in Table 1.
DNA extraction
Genomic DNA was extracted from the isolates by boiling lysis as described by Blackstone et al. (2003) and used as template in the qPCR detection of virulence and antimicrobial resistance genes as described below.
Real-Time qPCR amplification of tlh, tdh, trh, and vvha
Real-time qPCR was used for the multiplex detection and quantification of the tlh, tdh, trh (V. parahaemolyticus), and vvha (V. vulnificus) genes with primers (Table 2) and conditions previously described (Campbell and Wright 2003; Nordstrom et al. 2007) using an ABI 7500 instrument (Applied Biosystems Carlsbad, CA, USA). The reaction mixture (25 μl) contains the following: 1× PCR buffer (Invitrogen, Carlsbad, CA, USA), 5.0 mM MgCl2 (Invitrogen), 300 nM of each of the dNTPs (Roche, Indianapolis, USA), 300 nM each of the trh and vvhA primers, 200 nM tlh primers, 100 nM of tdh primers, 75 nM of tlh and vvha IAC primers, 25 nM of tdh and trh IAC primers, 150 nM tlh probe and IAC, 75 nM tdh and trh probes, 200 nM vvha probe, and 1.50 U, 1.12 U, 2.25 U platinum Taq polymerase (Invitrogen) for tlh, vvha, and tdh/trh respectively. All primers, IACs, tlh, and vvha probes were obtained from Integrated DNA Technologies (Coralville, IA, USA) while the tdh and trh probes were obtained from Life Technologies (Carlsbad, CA, USA). The rest of the reaction mixture volume consisted of a previously quantified IAC DNA (2 μl), nuclease-free water and DNA templates (2 μl of boiled cell lysates). V. parahaemolyticus ATCC 17802 carrying tlh, tdh, and trh, and V. vulnificus ATCC 27562 possessing vvha gene were used as positive controls while nuclease-free water served as negative control.
Serotyping of V. parahaemolyticus
Serotyping of the V. parahaemolyticus isolates was performed using a commercially available V. parahaemolyticus antiserum test kit (Denka Seiken, Tokyo, Japan) according to the manufacturer’s instructions. For O antigen typing, a heavy cell suspension was prepared in a normal saline solution and was then autoclaved at 121 °C for 2 h. A 1-μl loopful of the autoclaved suspension was added to one drop of each O antiserum which was observed for agglutination. For K antigen typing, a 1-μl loopful of isolate colony was mixed with one drop of each pool of K antisera and was observed for agglutination. If an isolate agglutinated in any K pool, the individual antisera of that pool were tested.
Antimicrobial resistance analysis
Antimicrobial resistance analysis was carried out using MicroScan Dried Gram Negative antibiotic panel (Beckman Coulter, Inc., Brea, CA, USA) containing 30 antimicrobial agents. The list of antimicrobial agents used, breakpoints, and references are listed in Table S3. The production of extended spectrum beta-lactamase (ESBL) in isolates showing phenotypic resistance to third-generation cephalosporins was confirmed using MicroScan ESBL plus panel. Inoculum preparation was performed in 2% NaCl solution according to the manufacturer’s instruction based on CLSI document M07-A10 (CLSI 2015a). Test panels were incubated for 16–20 h at 35 °C and results interpreted using the CLSI breakpoints described for Enterobacteriaceae in Table 2A of document M100-S25 for the following antimicrobial agents: aztreonam, cefotetan, ceftriaxone, cephalothin, ertapenem, nitrofurantoin, ticarcillin/K clavulanate, and tobramycin (CLSI 2015b). Breakpoints specific for Vibrio spp. in Table 20 of document M45-A3 was used for interpretation of the following antimicrobial agents: amikacin, ampicillin, ampicillin/sulbactam, cefazolin, cefepime, cefotaxime, cefoxitin, ceftazidime, cefuroxime, chloramphenicol, ciprofloxacin, gentamicin, imipenem, levofloxacin, meropenem, piperacillin, piperacillin/tazobactam, tetracycline, and trimethoprim/sulfamethoxazole (CLSI 2016). Cefotaxime/K clavulanate and ceftazidime/K clavulanate do not have interpretive breakpoint criteria, a ≥ 3-fold MIC decrease between CAZ and CAZ/CA; CTX and CTX/CA are considered positive for ESBL production according to the manufacturer’s manual. For tigecycline, the manufacturer’s breakpoint was used.
Detection of beta-lactams resistance genes
qPCR was carried out to detect β-lactams resistance genes from ESBL-producing V. parahaemolyticus) and V. vulnificus isolates with primers targeting the following beta-lactam resistance genes: blaKPC, blaNDM-1, blaTEM, blaSHV, blaCTX-M-1 and -M-9 (Cluster A), and blaCMY (Table S1). Total genomic DNA for antimicrobial resistance gene detection was extracted from each isolate according to the Center for Disease Control and Prevention (CDC) protocol for Multiplex Real-Time PCR Detection of blaKPC and blaNDM-1 (CDC 2011). The reaction mixture (25 μl) contains 1× PCR buffer (Invitrogen, Carlsbad, CA, USA), 5.0 mM MgCl2 (Invitrogen), 300 nM of each of the dNTPs (Roche, Indianapolis, USA), 200 nM forward and reverse primers (Integrated DNA Technologies), 75 nM for IAC forward and reverse primers (Integrated DNA Technologies), 150 nM probes (Integrated DNA Technologies), and 1.50 U, platinum Taq polymerase (Invitrogen). The rest of the reaction mixture volume consisted of a previously quantified IAC DNA (2 μl), nuclease-free water, and a DNA template (2 μl cell lysates). The cycling parameters consisted of a 95 °C hold for 3 min for the initial denaturation and activation of the hot-start Taq polymerase, followed by 35 cycles of amplification, with each cycle consisting of denaturation at 95 °C for 3 s and a combined annealing/extension step at 60 °C for 30 s. Klebsiella pneumoniae ATCC BAA-1705 strain possessing blaKPC (as described by ATCC) and K. pneumoniae ATCC BAA-2146 carrying the blaNDM-1 (as described by ATCC), blaTEM, blaSHV, blaCTX-M-15, and blaCMY (Leski et al. 2012) were used as positive controls while the negative control was nuclease-free water added to the PCR mix as a template.
Pulse field gel electrophoresis analysis of V. parahaemolyticus
Pulse field gel electrophoresis (PFGE) was performed according to the CDC PulseNet protocol for V. parahaemolyticus (CDC 2013) using Sfi I (40 U/sample) (Roche Diagnostics, Indianapolis, IN, USA) for restriction digestion. The restricted fragments were resolved in 1% seakem gold agarose gel in 0.5% Tris-boric acid-EDTA buffer using CHEF Mapper system (Bio-Rad Laboratories, Richmond, CA, USA). The following electrophoresis conditions were used: Auto Algorithm of 78 kb and 396 kb for low and high molecular weight, initial and final switch time of 10 s and 35.03 s, and run time of 16.5 h at 14 °C. Voltage density and included angle were 6.0 V/cm and 120° respectively, while linear ramping and pump speed was 1 l/min. Xba I digested DNA from Salmonella enterica serovar Braenderup strain H9812 was used as a molecular size marker. Stained gels were visualized using Gel Doc XR+ (Bio-Rad Laboratories, Richmond, CA, USA). The PFGE patterns were analyzed using BioNumerics software version 7.6 (Applied Maths, Austin, TX, USA). Clustering was performed using the unweighted pair group method and the Dice correlation coefficient with position tolerance of 1.5%. Clusters were defined on the basis of an 80% similarity cutoff (CDC 2013).
Results and discussion
In Nigeria, studies of Vibrio species are mostly focused on the detection of these organisms in seafoods (Oramadike and Ogunbanwo 2015; Adebayo-Tayo et al. 2011) with few studies focusing on environmental isolates (Eyisi et al. 2013). In this study, we isolated V. parahaemolyticus and V. vulnificus from recreational beaches along the shoreline of Lagos, Nigeria. V. parahaemolyticus was isolated from all the beaches sampled and occurred more frequently in beach sand compared to seawater samples (Table 1). V. vulnificus was, however, only detected from water samples of ELK, LEK, and TAK, and sand from ELK and LEK.
Detection of tlh and tdh/trh genes and serotyping of V. parahaemolyticus
The results of real-time PCR assay showed that all the tested V. parahaemolyticus were positive for thermolabile hemolysin (tlh) gene (Table 2) confirming the identity of these isolates as V. parahaemolyticus (Brasher et al. 1998; Bej et al. 1999; Rojas et al. 2011). Similarly, all V. vulnificus isolates were positive for the cytotoxin hemolysin protein encoded by vvha. Further, results of real-time PCR assay for detection of virulence genes tdh and trh showed that five isolates were positive for tdh and two isolates for trh while one isolate (LEK 108) carried both tdh and trh (Table 2). tdh and trh are the most predictive indicators of potential virulence in V. parahaemolyticus (Baker-Austin et al. 2008) and are responsible for hemolytic activity in many clinical strains (Ceccarelli et al. 2013). Similar to our results, previous studies (Cook et al. 2002; Hara-Kudo et al. 2003; Robert-Pillot et al. 2004; Baker-Austin et al. 2008; Li et al. 2015; He et al. 2016; Ghenem and Elhadi 2018) have reported a low prevalence of these virulence factors in food and environmental V. parahaemolyticus strains, confirming that non-clinical isolates of this bacteria rarely possess virulence factors. However, the prevalence of virulence factors reported in our study is higher than those reported in the studies cited above. Additionally, we also detected the co-occurrence of tdh and trh genes in an isolate from one of our study sites.
Serotyping revealed 10 different serogroups among the 26 isolates based on O and K antigens (Table 2). The most prevalent serogroup is the O5:Kut (K untypeable) with six isolates, followed by O1:Kut (4 isolates), O3:K31 and O4:Kut (3 isolates each), O2:K3, O3:K6, O8:K70, and O11:Kut with two isolates each, and O5:K30 and O10:Kut with one isolate each. Two serotypes of public health importance were isolated in three of the beaches included in this study. The first of such serotype, O3:K6, was detected in V. parahaemolyticus strain isolated from ELK. Serotype O3:K6 has been reported in large outbreaks of V. parahaemolyticus infections worldwide (Raszl et al. 2016) but are rarely detected in food and environmental isolates (Raghunath 2014). Secondly, serotype O4:Kut, known to be more virulent than other pathogenic strains of V. parahaemolyticus and has previously caused large outbreaks in the USA, Europe, and South America (Martinez-Urtaza et al. 2013; Newton et al. 2014; Haendiges et al. 2015), was isolated from ELK, TAK, and BDG. The detection of these serotypes in the Nigerian coastal environment, especially from recreational beaches, is of great public health concern for beach users.
Antimicrobial resistance analysis of V. parahaemolyticus and V. vulnificus
Results of susceptibility testing using 30 antibiotics revealed that all the V. parahaemolyticus and V. vulnificus isolates showed resistance to multiple antibiotics with the least being resistance to seven antibiotics in combination. There was 100% resistance to AMP, CFZ, CEF, and PIP among the isolates; and all V. parahaemolyticus isolates were in addition resistant to CAZ, TIM, AMK, and TOB (Fig. 1, Table S2). In contrast, all isolates were sensitive to CHL, LVX, and TGC while in addition to these three antibiotics, all V. parahaemolyticus were sensitive to CTX, CTX/CA, CRO, CTT, SXT, CIP, NIT, and TET (Fig. 1, Table S2). One V. parahaemolyticus isolate from Takwa Bay (TAK 145) and ten V. vulnificus isolates from ELK (ELK 125, 173, 175), LEK (95B, 164), and TAK (TAK 141, 178, 181B, 184, 196) showed resistance to carbapenems (IMP, MER, and ETP) (Table S2).
Frequency of resistance to antimicrobial agents among V. parahaemolyticus and V. vulnificus isolates from the Nigerian Beaches. AMK amikacin, AMP ampicillin, ATM aztreonam, CAZ Ceftazidime, CAZ/CA ceftazidime/clavulanate, CEF cephalothin, CFZ cefazolin, CHL chloramphenicol, CIP ciprofloxacin, CRO ceftriaxone, CTT cefotetan, CTX cefotaxime, CTX/CA cefotaxime/clavulanate, CXM cefuroxime, ETP ertapenem, FEP cefepime, FOX cefoxitin, GEN gentamicin, IMP imipenem, LVX levofloxacin, MER meropenem, NIT nitrofuratoin, PIP piperacillin, SAM ampicillin/sulbactam, SXT trimethoprim/sulfamethoxazole, TET tetracycline, TGC tigecycline, TIM ticarcillin/clavulanate, TOB tobramycin, TZP piperacillin/taxobactam,
The widespread resistance shown by the isolates of the present study to third (CAZ, CRO, CTX) and fourth-generation (FEP) cephalosporins, which remains rare among Vibrio species (Han et al. 2007; Baker-Austin et al. 2008; Wong et al. 2012; Li et al. 2015), is worrisome. Further, in contrast to previous observations by Baker-Austin et al. (2008), we found no significant difference in the resistance (12.6 antimicrobials per isolate) of V. parahaemolyticus isolates possessing the tdh and trh virulence determinants their counterparts lacking these genes (13.5 antimicrobials per isolate).
Detection of β-lactams resistance genes in ESBL-producing Vibrio isolates
The New Delhi metallo-β-lactamase gene blaNDM-1 was found in five strains of V. vulnificus from ELK (ELK125, ELK175), LEK (LEK164), and TAK (TAK141, TAK196) and one V. parahaemolyticus isolated from TAK (TAK145) (Table 3). All the blaNDM-1-positive isolates except one which carried blaTEM (ELK175) were also positive for blaTEM and blaCMY. None of the tested genes was found in one isolate of V. vulnificus (TAK 178). All the blaNDM-1 producers showed resistance to multiple antibiotics with the least being resistant to 17 antibiotics. One blaNDM-1 producer (ELK175) was resistant to 24 of the 30 antibiotics tested. blaNDM-1 producers are always resistant to several classes of antibiotics (Rolain et al. 2010; Nordmann and Poirel 2014).
There are increasing reports of the carriage of cephalosporinase-encoding genes among Vibrio species in other parts of the world. These include blaCMY-2 located on IncA/C plasmids in V. parahaemolyticus (Li et al. 2015) and V. alginolyticus (Ye et al. 2016), blaVEB-2 in V. parahaemolyticus (Li et al. 2016), and blaPER-1 located on an IncN plasmid in V. parahaemolyticus, all isolated from seafood in China. Further complicating this disturbing observation is the increasing report of carbapenemases, which in some cases are novel (Bier et al. 2015; Mangat et al. 2016) in members of the genus Vibrionaceae. Previous studies have detected blaNDM-1 in V. parahaemolyticus isolated from shrimps (Briet et al. 2018) and other Vibrio species such as environmental V. cholera in India (Walsh et al. 2011), clinical V. cholera O1 E1 Tor in india (Mandal et al. 2012), environmental non O1/non O39 V. cholera in Vietnam (Diep et al. 2015); clinical non O1/non O39 V. cholera in the UK (Darley et al. 2012), and V. fluvialis of clinical origin in India (Chowdhury et al. 2016). However, reports of blaNDM-1 in V. parahaemolyticus and V. vulnificus are not very common. The presence of these genes in bacteria of public health importance such as V. parahaemolyticus and V. vulnificus portend great danger for beach goers as they not only limit treatment options in case of infection, but they can also transmit their resistance elements to other pathogenic and potentially pathogenic bacteria in the beach ecosystem.
Pulse field gel electrophoresis analysis of V. parahaemolyticus strains
The PFGE profiles of the SfiI-digested DNA of V. parahaemolyticus are presented in Fig. 2. A total of 23 pulsotypes were recognized among 26 V. parahaemolyticus strains with 19 isolates showing distinct banding patterns; the remaining four banding patterns included at least two isolates. This suggested a large degree of genomic variation among the isolates even within the same sampling sites. It also suggested that the isolates included in this study are not just clonal replicates. The isolates sharing the same banding patterns are TAK 145 and BDG 151B both belonging to serotype O3:K31, ELK 169 and ELK 170 both with serotype O11:Kut, TAK 139 and TAK 142 both with serotype O8:K70, and ELK 124 and ELK 127 with serotype O3:K6 respectively. It is interesting to note that the only clade found among this organism is between isolate TAK 145 from wet sand sample collected from Takwa Bay beach and BDG 151B from dry sand sample collected from Badagry beach.
In conclusion, we isolated V. parahaemolyticus and V. vulnificus showing resistance to multiple antimicrobial agents from four recreational beaches in Lagos, southwestern Nigeria. The virulence gene tdh and trh was detected in six isolates of V. parahaemolyticus with one isolate positive for both genes, confirming the presence of potentially pathogenic strains of V. parahaemolyticus in Nigerian recreational waters. Five V. vulnificus and one V. parahaemolyticus tested positive for the metallo-β-lactamase gene blaNDM-1which occurred together with blaTEM and blaCMY in five isolates. The detection of these genes in public beaches visited by beach goers is of great public health concern and highlights the need for urgent mitigation efforts to protect beach goers and curbs further dissemination of these resistance genes to other bacterial population through horizontal gene transfer.
References
Adebayo-Tayo BC, Okonko IO, John MO, Odu NN, Nwanze JC, Ezediokpu MN (2011) Occurrence of potentially pathogenic Vibrio species in sea foods obtained from Oron Creek. Adv Biol Res 5:356–365
Baker-Austin C, McArthur JV, Tuckfield RC et al (2008) Antibiotic resistance in the shellfish pathogen Vibrio parahaemolyticus isolated from the coastal water and sediment of Georgia and South Carolina, USA. J Food Prot 71:2552–2558
Baron S, Lesne J, Jouy E, Larvor E, Kempf I, Boncy J, Rebaudet S, Piarroux R (2016) Antimicrobial susceptibility of autochthonous aquatic Vibrio cholerae in Haiti. Front Microbiol 7:1671. https://doi.org/10.3389/fmicb.2016.01671
Bej AK, Patterson DP, Brasher CW, Vickery MCL, Jones DD, Kaysner CA (1999) Detection of total and hemolysin-producing Vibrio parahaemolyticus in shellfish using multiplex PCR amplification of tlh, tdh and trh. J Microbiol Methods 36(3):215–225. https://doi.org/10.1016/S0167-7012(99)00037-8
Berendonk TU, Manaia CM, Merlin C, Fatta-Kassinos D, Cytryn E, Walsh F, Bürgmann H, Sørum H, Norström M, Pons MN, Kreuzinger N, Huovinen P, Stefani S, Schwartz T, Kisand V, Baquero F, Martinez JL (2015) Tackling antibiotic resistance: the environmental framework. Nat Rev Microbiol 13(5):310–317
Bier N, Schwartz K, Guerra B, Strauch E (2015) Survey on antimicrobial resistance patterns in Vibrio vulnificus and Vibrio cholerae non-O1/non-O139 in Germany reveals carbapenemase-producing Vibrio cholerae in coastal waters. Front Microbiol 6:1179. https://doi.org/10.3389/fmicb.2015.01179
Blackstone GM, Nordstrom JL, Vickery MC, Bowen MD, Meyer RF, DePaola A (2003) Detection of pathogenic Vibrio parahaemolyticus in oyster enrichments by real time PCR. J Microbiol Methods 53(2):149–155
Blackwell KD, Oliver JD (2008) The ecology of Vibrio vulnificus, Vibrio cholerae, and Vibrio parahaemolyticus in North Carolina estuaries. J Microbiol 46(2):146–153. https://doi.org/10.1007/s12275-007-0216-2
Brasher CW, Depaola A, Jones DD, Bej AK (1998) Detection of microbial pathogens in shellfish with multiplex PCR. Curr Microbiol 37(2):101–107
Briet A, Helsens N, Delannoy S, Debuiche S, Brisabois S, Midelet G, Granier SA (2018) NDM-1-producing Vibrio parahaemolyticus isolated from imported seafood. J Antimicrob Chemother. https://doi.org/10.1093/jac/dky200
Campbell SM, Wright AC (2003) Real-time PCR analysis of Vibrio vulnificus from oysters. Appl Environ Microbiol 77(17):7137–7144
CDC (2011) Multiplex real-time PCR detection of Klebsiella pneumoniae Carbapenemase (KPC) and New Delhi metallo-β-lactamase (NDM-1). https://www.cdc.gov/hai/settings/lab/kpc-ndm1-lab-protocol.html. Accessed 16 Nov 2017
CDC (2013) Standard operating procedure for PulseNet PFGE of Vibrio cholera and Vibrio parahaemolyticus. Centers for Disease Control and Prevention, Atlanta, GA, USA. https://www.cdc.gov/pulsenet/PDF/vibrio_pfge_protocol-508c.pdf. Accessed 4 Dec 2017
Ceccarelli D, Hasan NA, Hug A, Colwell RR (2013) Distribution and dynamics of epidemic and pandemic Vibrio parahaemolyticus virulence factors. Front Cell Infect Microbiol 3:97
Chowdhury G, Pazhani PP, Sarkar A et al (2016) Carbapenem resistance in clonally distinct clinical strains of Vibrio fluvialis isolated from diarrheal samples. Emerg Infect Dis 22:1754–1761
CLSI (2015a) Methods for dilution antimicrobial susceptibility tests for bacteria that grow aerobically. Approved standard-Tenth edition. CLSI document M07-10. Clinical and Laboratory Standards Institute, Wayne
CLSI (2015b) Performance standards for antimicrobial susceptibility testing: Twenty-fifth informational supplement. CLSI document M100-S25. Clinical and Laboratory Standards Institute, Wayne
CLSI (2016) Methods for antimicrobial dilution and disk susceptibility testing of infrequently isolated or fastidious bacteria. CLSI document M45-A3. Clinical and Laboratory Standards Institute, Wayne
Coleman BL, Salvadori MI, McGeer AJ et al (2012) The role of drinking water in the transmission of antimicrobial-resistant E. coli. Epidemiol Infect 140:633–642
Cook DW, O’Leary P, Hunsucker JC, Sloan EM, Bowers JC, Blodgett RJ, DePaola A (2002) Vibrio vulnificus and Vibrio parahaemolyticus in U.S. retail shell oysters: a national survey June 1998 to July 1999. J Food Prot 65:79–87
Daniels NA, Shafaie A (2000) A review of pathogenic Vibrio infections for clinicians. Infect Med 17:665–685
Darley E, Weeks J, Jones L, Daniels V, Wootton M, MacGowan A, Walsh T (2012) NDM-1 polymicrobial infections including Vibrio cholerae. Lancet 380:1358
De Menezes FGR, Rodriguez MTT, De Carvalho FCT et al (2017) Pathogenic Vibrio species isolated from estuarine environments (Ceará, Brazil)-antimicrobial resistance and virulence potential profiles. An Acad Bras Cienc 89(2):1175–1188
Diep TT, Nguyen NT, Nguyen TN, An HK, Nguyen TQ, Nguyen VH, Nguyen TV, Nguyen TNA, Izumiya H, Ohnishi M, Yamashiro T, Nguyen LTP (2015) Isolation of New Delhi metallo-β-lactamase 1-producing Vibrio cholerae non-O1, non-O139 strain carrying ctxA, st and hly genes in southern Vietnam. Microbiol Immunol 59:262–267
Drake SL, DePaola A, Jaykus LA (2007) An overview of Vibrio vulnificus and Vibrio parahaemolyticus. Compr Rev Food Sci Food Saf 6:120–144
Dumontet S, Krovacek K, Svenson V, Baloda S, Figliulo G (2000) Prevalence and diversity of Aeromonas and Vibrio spp in coastal waters in Southern Italy. Comp Immun Microbial Infect Dis 23:53–72
Eyisi OAL, Nwodo UU, Iroegbu CU (2013) Distribution of Vibrio species in shellfish and water samples collected from the Atlantic coastline of south-east Nigeria. J Health Popul Nutr 31(3):314–320
Fabbro C, Cataletto B, Del Negro P (2010) Detection of pathogenic Vibrio parahaemolyticus through biochemical and molecular-based methodologies in coastal waters of the Gulf of Trieste (North Adriatic Sea). FEMS Microbiol Lett 307:158–164. https://doi.org/10.1111/j.1574-6968.2010.01969.x
García-Aljaro C, Riera-Heredia J, Blanch AR (2014) Antimicrobial resistance and presence of the SXT mobile element in Vibrio spp. isolated from aquaculture facilities. New Microbiol 37:339–346
Ghenem L, Elhadi N (2018) Isolation, molecular characterization, and antibiotic resistance patterns of Vibrio parahaemolyticus isolated from coastal water in the Eastern Province of Saudi Arabia. J Water Health 16(1):57–69. https://doi.org/10.2166/wh.2017.361
Haendiges J, Timme R, Allard MW, Myers RA, Brown EW, Gonzalez-Escalona N (2015) Characterization of Vibrio parahaemolyticus clinical strains from Maryland (2012-2013) and comparisons to a locally and globally diverse V. parahaemolyticus strains by whole-genome sequence analysis. Front Microbiol 6:1–11
Halliday E, Gast RJ (2011) Bacteria in beach sands: an emerging challenge in protecting coastal water quality and bather health. Environ Sci Technol 45(2):370–379
Han F, Walker RD, Janes ME, Prinyawiwatkul W, Ge B (2007) Antimicrobial susceptibilities of Vibrio parahaemolyticus and Vibrio vulnificus isolates from Louisiana Gulf and retail raw oysters. Appl Environ Microbiol 73:7096–7098
Hara-Kudo Y, Sugiyama K, Nishibuchi M, Chowdhury A, Yatsuyanagi J, Ohtomo Y, Saito A, Nagano H, Nishina T, Nakagawa H, Konuma H, Miyahara M, Kumagai S (2003) Prevalence of pandemic thermostable direct hemolysin-producing Vibrio parahaemolyticus O3:K6 in seafood and the coastal environment in Japan. Appl Environ Microbiol 69:3883–3891
He Y, Jin L, Sun F, Hu Q, Chen L (2016) Antibiotic and heavy-metal resistance of Vibrio parahaemolyticus isolated from fresh shrimps in Shanghai fish markets, China. Environ Sci Pollut Res 23(15):15033–15040. https://doi.org/10.1007/s11356-016-6614-4
Johnson CN, Flowers AR, Noriea NF, Zimmerman AM, Bowers JC, DePaola A, Grimes DJ (2010) Relationships between environmental factors and pathogenic vibrios in the northern Gulf of Mexico. Appl Environ Microbiol 76:7076–7084. https://doi.org/10.1128/AEM.00697-10
Johnson CN, Bowers JC, Griffitt KJ, Molina V, Clostio RW, Pei S, Laws E, Paranjpye RN, Strom MS, Chen A, Hasan NA, Huq A, Noriea NF III, Grimes DJ, Colwell RR (2012) Ecology of Vibrio parahaemolyticus and Vibrio vulnificus in the coastal and estuarine waters of Louisiana, Maryland, Mississippi, and Washington (United States). Appl Environ Microbiol 78:7249–7257
Kennedy K, Collignon P (2010) Colonization with Escherichia coli resistant to “critically important” antibiotics: a high risk for international travellers. Eur J Clin Microbiol Infect Dis 29:1501–1506
Leski T, Vora GJ, Taitt CR (2012) Multidrug resistance determinants from NDM-1-producing Klebsiella pneumoniae in the USA. Int J Antimicrob Agents 40(3):282–284
Letchumanan V, Chan KG, Lee LH (2014) Vibrio parahaemolyticus: a review on the pathogenesis, prevalence, and advance molecular identification techniques. Front Microbiol 5:705
Li R, Lin D, Chen K, Wong MH, Chen S (2015) First detection of AmpC β-lactamase bla(CMY-2) on a conjugative IncA/C plasmid in Vibrio parahaemolyticus of food origin. Antimicrob Agents Chemother 59:4106–4111. https://doi.org/10.1128/AAC.05008-14
Li R, Ye L, Zheng Z, Chan EWC, Chen S (2016) Genetic characterization of a blaVEB-2-carrying plasmid in Vibrio parahaemolyticus. Antimicrob Agents Chemother 60:6965–6968. https://doi.org/10.1128/AAC.01749-16
Mandal J, Sangeetha V, Ganesan V, Parveen M, Preethi V, Harish BN, Srinivasan S, Parija SC (2012) Third-generation cephalosporin-resistant Vibrio cholerae, India. Emerg Infect Dis 18:1326–1328
Mangat CS, Boyd D, Janecko N, Martz S-L, Desruisseau A, Carpenter M, Reid-Smith RJ, Mulvey MR (2016) Characterization of VCC-1, a novel Ambler class A carbapenemase from Vibrio cholerae isolated from imported retail shrimp sold in Canada. Antimicrob Agents Chemother 60:1819–1825. https://doi.org/10.1128/AAC.02812-15
Martinez-Urtaza J, Baker-Austin C, Jones JL, Newton AE, Gonzalez-Aviles GD, DePaola A (2013) Spread of Pacific Northwest Vibrio parahaemolyticus strain. N Engl J Med 369:1573–1574
Mudryk ZJ, Kosiorek A, Perliński P (2013) In-vitro antibiotic resistance of Vibrio-like organisms isolated from seawater and sand of marine recreation beach in the southern Baltic Sea. Hydrobiol 702:141–150
Newton AE, Garret N, Stroika SG, Halpin JL, Turnsek M, Mody RK (2014) Notes from the field: increase in Vibrio parahaemolyticus infections associated with consumption of Atlantic coast shellfish. Morb Mortal Wkly Rep 63:335–336
Nordmann P, Poirel L (2014) The difficult-to-control spread of carbapenemase producers among Enterobacteriaceae worldwide. Clin Microbiol Infect 20:821–830. https://doi.org/10.1111/1469-0691.12719
Nordstrom JL, Vickery MCL, Blackstone GM, Murray SL, DePaola A (2007) Development of a multiplex real-time PCR assay with an internal amplification control for the detection of total and pathogenic Vibrio parahaemolyticus bacteria in oysters. Appl Environ Microbiol 73(18):5840–5847
Okoh AI, Igbinosa EO (2010) Antibiotic susceptibility profiles of some Vibrio strains isolated from wastewater final effluents in a rural community of the Eastern Cape Province of South Africa. BMC Microbiol 10:143. https://doi.org/10.1186/1471-2180-10-143
Oliver JD, Pruzzo C, Vezzulli L, Kaper JB (2013) Vibrio species. In Doyle MP, Buchanam RL (ed) Food Microbiology: Fundamentals and Frontiers. ASM Press, Washington DC. pp 401–440
Oramadike C, Ogunbanwo ST (2015) Prevalence and antimicrobial susceptibility of Vibrio parahaemolyticus isolated from seafoods in Lagos Lagoon, Nigeria. Cogent Food Agric 1:1041349. https://doi.org/10.1080/23311932.2015.1041349
Orams M (2003) Sandy beaches as a tourism attraction: a management challenge for the 21 st century. J Coastal Res SI 35:74–84
Overbey KN, Hatcher SM, Stewart JR (2015) Water quality and antibiotic resistance at beaches of the Galápagos Islands. Front Environ Sci 3:64. https://doi.org/10.3389/fenvs.2015.00064
Oyelade A, Fagade O, Sanuth H, Anjolaiya L, Nwadike B (2018) Microbiological quality of some recreational beaches along the shoreline of Lagos state, Nigeria. J Environ Earth Sci 8(2):61–76
Pruden A, Joakim Larsson DG, Amézquita A et al (2013) Management options for reducing the release of antibiotics and antibiotic resistance genes to the environment. Environ Health Perspect 121:878–885. https://doi.org/10.1289/ehp.1206446
Raghunath P (2014) Roles of thermostable direct hemolysin (TDH) and TDH-related hemolysin (TRH) in Vibrio parahaemolyticus. Front Microbiol 5:805
Raszl SM, Froelich BA, Vieira CRW, Blackwood AD, Noble RT (2016) Vibrio parahaemolyticus and Vibrio vulnificus in South America: water, seafood and human infections. J Appl Microbiol 121:1201–1222
Robert-Pillot A, Guenole A, Lesne J, Delesmont R, Fournier JM, Quilici ML (2004) Occurrence of the tdh and trh genes in Vibrio parahaemolyticus isolates from waters and raw shellfish collected in two French coastal areas and from seafood imported into France. Int J Food Microbiol 91:319–325
Rojas MV, Matte MH, Dropa M, Silva ML, Matte GR (2011) Characterization of Vibrio parahaemolyticus isolated from oysters and mussels in Sao Paulo, Brazil. Rev Inst Med Trop Sao Paulo 53:201–205
Rolain JM, Parola P, Cornaglia G (2010) New Delhi metallo-β-lactamase (NDM-1): towards a new pandemia? Clin Microbiol Infect 16:1699–1701. https://doi.org/10.1111/j.1469-0691.2010.03385.x
Rosec JP, Simon M, Causse V, Boudjemaa M (2009) Detection of total and pathogenic Vibrio parahaemolyticus in shellfish: comparison of PCR protocols using pr72h or toxR targets with a culture method. Int J Food Microbiol 129:136–145. https://doi.org/10.1016/j.ijfoodmicro.2008.11.017
Shaw KS, Rosenberg Goldstein RE, He X, Jacobs JM, Crump BC, Sapkota AR (2014) Antimicrobial susceptibility of Vibrio vulnificus and Vibrio parahaemolyticus recovered from recreational and commercial areas of Chesapeake Bay and Maryland Coastal Bays. PLoS One 9:e89616
Taylor NGH, Verner-Jeffreys DW, Baker-Austin C (2011) Aquatic systems: maintaining, mixing and mobilising antimicrobial resistance? Trends Ecol Evol 26:278–284
Urquhart EA, Jones SH, Yu JW, Schuster BM, Marcinkiewicz AL, Whistler CA, Cooper VS (2016) Environmental conditions associated with elevated Vibrio parahaemolyticus concentrations in Great Bay Estuary, New Hampshire. PLoS One 11(5):e0155018. https://doi.org/10.1371/journal.pone.0155018
Valverde A, Grill F, Coque TM, Pintado V, Baquero F, Canton R, Cobo J (2008) High rate of intestinal colonization with extended-spectrum-beta-lactamase-producing organisms in household contacts of infected community patients. J Clin Microbiol 46:2796–2799
Walsh TR, Weeks J, Livermore DM, Toleman MA (2011) Dissemination of NDM-1 positive bacteria in the New Delhi environment and its implications for human health: an environmental point prevalence study. Lancet Infect Dis 11:355–362
WHO (2015) Global action plan on antimicrobial resistance. World Health Organization, Geneva
Wong MHY, Liu M, Wan HY, Chen S (2012) Characterization of extended-spectrum- beta-lactamase-producing Vibrio parahaemolyticus. Antimicrob Agents Chemother 56:4026–4028
Wu Y, Wen J, Ma Y, Ma X, Chen Y (2014) Epidemiology of foodborne disease outbreaks caused by Vibrio parahaemolyticus, China, 2003-2008. Food Control 46:197–202
Ye L, Li R, Lin D, Zhou Y, Fu A, Ding Q, Chan EW, Yao W, Chen S (2016) Characterization of an IncA/C multidrug resistance plasmid in Vibrio alginolyticus. Antimicrob Agents Chemother 146:3232–3235. https://doi.org/10.1128/AAC.00300-16
Acknowledgments
We thank Dr. Hassan Sanuth and Dr. Lukman Anjolaiya of Lagos State Ministry of Environment, State Secretariat, Alausa, Ikeja, Lagos State, Nigeria, for their assistance in sample collection.
Author information
Authors and Affiliations
Corresponding author
Additional information
Responsible editor: Diane Purchase
Electronic supplementary material
ESM 1
(DOCX 25 kb)
Rights and permissions
About this article
Cite this article
Oyelade, A.A., Adelowo, O.O. & Fagade, O.E. blaNDM-1-producing Vibrio parahaemolyticus and V. vulnificus isolated from recreational beaches in Lagos, Nigeria. Environ Sci Pollut Res 25, 33538–33547 (2018). https://doi.org/10.1007/s11356-018-3306-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11356-018-3306-2