Abstract
Inflammasome, a cytosolic multi-protein complex, assembly is a response to sensing intracellular pathogenic and endogenic danger signals followed by caspase-1 activation, which maturates precursor cytokines such as interleukin (IL)-1β. Most inflammasome research has been undertaken in humans and rodents, and inflammasomes in veterinary species have not been well-characterized. In this study, we observed the effects of well-known inflammasome activators on equine peripheral blood monocytes (PBMCs). The NLRP3 inflammasome triggers include ATP, nigericin, aluminum crystals, and monosodium urate crystals, and NLRP3 activation induces IL-1β secretion in a dose-dependent manner. Activators of NLRC4 and AIM2 inflammasomes include cytosolic flagellin and dsDNA, and their activation induces IL-1β secretion. The bacterial inflammasome triggers Salmonella Typhimurium and Listeria monocytogenes also induce IL-β releases. To elucidate the role of potassium efflux as an upstream signal of NLRP3 inflammasome activation, equine PBMCs were treated with blockers of potassium efflux in the presence of NLRP3 triggers. As a result, the IL-1β secretion stemming from equine NLRP3 inflammasome activation was not completely attenuated by the inhibition of potassium efflux. Taken together, the results indicate that equine PBMCs normally secrete IL-1β in response to well-known inflammasome activators, although equine NLRP3 inflammasome activation might not be dependent on potassium efflux.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
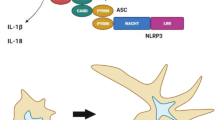
Cytosolic pathogen- and damage-associated molecular pattern molecules (PAMPs and DAMPs) lead to the assembly of inflammasomes, multi-protein complexes in myeloid and epithelial cells, which activate caspase-1 to maturate interleukin (IL)-1β and IL-18. Inflammasomes have been implicated in the pathogenesis of a wide range of diseases in humans and mice, and they have been investigated as potential therapeutic targets in attempts to cure those diseases (Swanson et al. 2019). Initially inflammasomes were simply known as regulators of the secretion of IL-1β and IL-18 through caspase-1 activation in innate immune cells, but it has been recently reported that they are active in governing between innate and adaptive immunities in host immune homeostasis (Ciraci et al. 2012; Evavold and Kagan 2018; Swanson et al. 2019). An inflammasome consists of a sensor, an adaptor protein (ASC [apoptosis-associated speck-like protein containing a caspase recruitment domain]), and an effector (caspase-1) and is named according to the identity of the sensor. The most well-known sensors are NLRP3 (nucleotide-binding oligomerization domain [NOD]-like receptor [NLR] pyrin domain-containing protein 3), NLRC4 (NLR caspase activation and recruitment domain [CARD]-containing protein 4), and AIM2 (absent in melanoma 2). NLRP3 senses several signals including those related to potassium efflux, calcium flux, lysosomal disruption, mitochondrial dysfunction, and metabolic changes (Swanson et al. 2019). The NLRC4 complex with NAIPs (NLR family, apoptosis inhibitory proteins) interacts with bacterial ligands such as flagellin and the type 3 secretion system (T3SS) (Duncan and Canna 2018), whereas AIM2 detects dsDNA derived from host, bacteria, or virus (Lugrin and Martinon 2018). NLRP3 has three domains, PYD (pyrin domain), NACHT (neuronal apoptosis inhibitor protein [NAIP] class 2 transcription activator [C2TA] of the heterokaryon incompatibility [HET-E] and telomerase-associated protein 1 [TP1]), and LRR (leucine-rich repeat). Upon stimulation, NLRP3 induces self-oligomerization via NACHT–NACHT interaction, and recruits ASC and caspase-1 through PYD–PYD and CARD–CARD binding (Swanson et al. 2019). Caspase-1 is activated by proximity-induced self-cleavage and matures cytokines of the IL-1 family (Swanson et al. 2019).
In past decades, inflammasomes have been studied in humans and rodents; recently, however, the inflammasomes of veterinary species have received research attention. Among livestock, porcine inflammasomes have been relatively well-characterized because pigs are an animal model used in the study of human diseases and xenotransplantation. Inflammasome-related genes such as NLRP3, ASC, and caspase-1 are expressed in the lymph nodes of pigs, and the inflammasome triggers observed in humans and rodents are reported to provoke IL-1β secretion in porcine peripheral blood monocytes (Dawson et al. 2017; Kim et al. 2014b; Tohno et al. 2011). Porcine inflammasomes are activated by PAMPs, such as porcine reproductive and respiratory syndrome virus (PRRSV) and the swine fever virus, and by DAMPs, including hypoxia and atherosclerosis, and such activations are similar to the inflammasome responses in humans and rodents (Angelis et al. 2014; Islam et al. 2016; Li et al. 2013; Vrentas et al. 2018). In cattle, viral and bacterial pathogens do not only lead to inflammasome activation resulting in IL-1β secretion, but human- and rodent-identified NLRP3 triggers also result in activation (Di Virgilio et al. 2017; Vrentas et al. 2018). Moreover, gene expressions of NLRP3, ASC, and caspase-1 have been detected in sheep and goats, although the mechanisms of IL-1β secretion and inflammasome activation have not been elucidated (Zhang et al. 2017). As well, it has been reported that canine NLRP3 inflammasomes are activated by pathogens, and IL-1β secretion has been observed in dogs suffering from myocardial ischemia and inflammatory bowel diseases (Hu et al. 2015; Jalilian et al. 2012; Vrentas et al. 2018). Based on recent results, inflammasome activation in veterinary species is, for the most part, similar to that of humans and mice, but there are some exceptions or differences (Vrentas et al. 2018). For example, although pigs do not possess the NLRC4 and AIM2 genes in their chromosomes, the NLRC4 and AIM2 triggers, flagellin and dsDNA transfection, successfully lead to the secretion of IL-1β in porcine peripheral blood monocytes (Ahn et al. 2018c; Dawson et al. 2017).
Thus, further characterization of inflammasomes in veterinary species can provide the information needed to elucidate veterinary diseases and develop potential veterinary therapeutics that target inflammasome-mediated veterinary diseases (Swanson et al. 2019; Vrentas et al. 2018). To date, however, equine inflammasomes have not been widely studied. In the present study, we characterize equine inflammasome activation by using NLRP3, NLRC4, and AIM2 inflammasome triggers that are well-established in humans and rodents. In addition, presence of an upstream signaling event, potassium efflux, associated with equine NLRP3 inflammasome activation was confirmed by using blockers, and the results were compared with those from human and murine inflammasomes.
Materials and Methods
Cell preparation
Equine peripheral blood monocytes (PBMCs) were isolated from blood freshly drawn from a Manchurian horse (Equus ferus caballus; 2-year-old male) by using lymphocyte separation medium (LSM; Thermo Fisher Scientific, Waltham, MA, USA). Briefly, blood was drained into anticoagulant EDTA-containing tubes (1.5 mg/mL of blood) and moved to the laboratory. The blood was then mixed with the same volume of phosphate-buffered saline (PBS) in 50 mL centrifuge tubes (SPL Life Science Co., Gyeonggi-do, Republic of Korea), and the same volume of LSM was carefully added into the bottom of the tube (blood: PBS: LSM = 1: 1: 1). After centrifuging at 500 × g at room temperature (RT) for 30 min, the blood-LSM interphase containing mononuclear cells was harvested, placed in a new tube, and washed with PBS to eliminate residual LSM. Cell pellets, mixed with red blood cells lysis buffer (iNtRON Biotech., Sengnam-si, Republic of Korea), were collected by centrifuging at 500 × g at RT. The obtained PBMCs were maintained in DMEM (Dulbecco’s modified Eagle’s medium; Capricorn Scientific, Ebsdorfergrund, Germany) containing 10% fetal bovine serum (FBS; Capricorn Scientific) and antibiotics (100 U/mL of penicillin and 100 μg/mL of streptomycin; Capricorn Scientific) at 37 °C in a 5% CO2 atmosphere. Further experiments were conducted within one day from when the PBMCs were isolated.
To obtain murine bone marrow-derived macrophages (BMDMs), marrow progenitor cells were collected from the tibias and femurs of C57BL/6 mice (Narabio Co., Seoul, Republic of Korea) and differentiated into macrophages in DMEM with 30% L929 cell-conditioned media that contained granulocyte/macrophage colony-stimulating factor, 10% FBS, and antibiotics for 7 days at 37 °C in a 5% CO2 atmosphere (Ahn et al. 2019, 2014, 2015; Kim et al. 2014a). Human monocyte-like cells (THP-1) were obtained from the Korea Cell Line Bank (Seoul, Republic of Korea) and cultured in RPMI (Roswell Park Memorial Institute 1640; Capricorn Scientific) media containing 10% FBS and antibiotics (Ahn et al. 2018b). The THP-1 cells were differentiated into macrophage-like phenotypes by treating with 12-myristate 13-acetate (PMA, 200 nM; InvivoGen, San Diego, CA. USA) overnight (Kim et al. 2019). Animal experiments were conducted in accordance with the National Institutes of Health Guide for the Care and Use of Laboratory Animals and were approved by the Institutional Animal Care and Use Committee of Kangwon National University (IACUC; approval KW-190319-3 for mice and KW-191028-1 for horses).
Inflammasome activation and inhibition
Equine PBMCs (2 × 106 cells / well), murine BMDMs (1 × 106 cells / well) and THP-1 (1 × 106 cells / well) were plated in 12-well plates (SPL Life Science), and then primed with lipopolysaccharide (LPS, 1 μg/mL; #L4130, Sigma-Aldrich, St. Louis, MI, USA) in RPMI media containing 10% of FBS and antibiotics. After 3 h of LPS priming, cells were treated with adenosine triphosphate (ATP; InvivoGen) for 1 h, nigericin (NG; Tocris Bioscience, Bristol, UK) for 1 h, aluminum potassium sulfate (Alum; Daejeung Chemicals & Materials Co., Gyeonggi-do, Republic of Korea) for 3 h, monosodium urate crystals (MSU; U2875, Sigma-Aldrich), prepared as described previously (Martinon et al. 2006), for 6 h, Salmonella enterica serovar Typhimurium (Salmonella, optical density at 600 nm [OD600] = 1.2) for 1 h, flagellin (InvivoGen) with Lipofectamine 2000 (10 μL/mL; Invitrogen, Carlsbad, CA, USA) for 1 h, Listeria monocytogenes (Listeria, OD600 = 1.2) for 6 h, or double-stranded DNA (dsDNA) with jetPRIME™ (2 μL/mL; Polyplus-transfection Inc., Illkirch, France) for 1 h (Ahn et al. 2017a, b; Lee et al. 2016). For inflammasome inhibition assessment, LPS-primed cells were treated with glibenclamide (Glibe, 150 μM; Santa Cruz Biotech., Santa Cruz, CA, USA), extracellular high potassium solution (KCl, 50 mM; Biosesang, Seoul, Republic of Korea), or Z-VAD-FMK (10 μg/mL; R&D System, Minneapolis, MN, USA) in the presence of ATP (5 mM) or NG (40 μM) for 1 h (Ahn et al. 2018a). Cellular supernatant (Sup) and lysate (Lys) were prepared for use in further analyses.
Immunoblotting
Sup and Lys samples were analyzed by performing SDS-PAGE (10% or 16%) in a gel running system (Mini-PROTEAN® TETRA Handcast system; BIO-RAD, Hercules, CA, USA). The obtained gels were transferred onto a polyvinylidene difluoride membrane (Thermo Fisher Scientific), and the membranes were then blocked with 3% skim milk and probed with anti-human IL-1β sera (AF-201-NA, R&D Systems) or anti-mouse IL-1β sera (AF-401-NA, R&D Systems) overnight at 4 °C (Ahn and Lee 2017; Han et al. 2017). In addition, the membrane was probed with horseradish peroxidase (HRP) secondary antibody (#sc-2020, Santa Cruz Biotechnology) for 1 h and then visualized by applying a chemiluminescence solution (WESTSAVE STAR™, Abfrontier, Seoul, Republic of Korea) and a chemiluminescence imaging system (EZ-Capture II, ATTO Technology, Tokyo, Japan). The membranes were stripped and re-probed with anti-actin sera (#sc-1615, Santa Cruz Biotechnology). Band intensity was determined by using image analyzing software (CS analyzer version 3, ATTO Technology).
Statistical analysis
Statistical analyses were conducted by applying one-way ANOVA (Tukey’s multiple comparisons test) for multiple groups and nonparametric t-tests (Mann-Whitney test) for two groups by using GraphPad software (version 6, GraphPad Software, San Diego, CA, USA). The obtained p values are included in the figures.
Results
Detection of IL-1β secretion in derived equine PBMCs
Activation of inflammasomes finally leads to the secretion of IL-1β p17, referred to as the active form of IL-1β, following by activation of caspase-1 (Ahn et al. 2018d). Thus secretion of the active form of IL-1β is a well-known indication of inflammasome activation and its presence should be detected by immunoblot analysis rather than via ELISA because anti-IL-1β cannot distinguish between the cleavage form (p17) and the pro-form (p36) of IL-1β (Kim et al. 2014b). Initially, we tested which anti-sera against human and mouse IL-1β were appropriate for the detection of equine IL-1β (Fig. 1A). Macrophages or monocytes of mouse, human, porcine, and equine were treated with LPS to induce pro-IL-1β expression and the cellular lysates were then subjected to immunoblotting. Although equine IL-1β was well detected by each antiserum, anti-human IL-1β sera showed a stronger band intensity than that of anti-mouse IL-1β. We also analyzed the sequence similarity of the amino acids of human, mouse, porcine, and equine IL-1β. The sequences of equine IL-1β were 66.67%, 64.15%, and 62.78% similar to those of human, mouse, and porcine IL-1β, respectively (Fig. 1B). Based on those results, human anti-IL-1β serum was selected for use in further studies.
Detection of IL-1β expression in equine PBMCs. A, Mouse BMDMs, human PBMCs, porcine PBMCs, and equine PBMCs were primed with LPS (1 μg/mL) for 3 h, and the cellular lysates were immunoblotted with the indicated anti-IL-1β sera. The lysate samples for human and porcine PBMCs were obtained from those in a previous study (Kim et al. 2014b). B, Amino acid alignment of equine (GenBank ID: NP_001075995), human (NP_000567), murine (NP_032387), and porcine (NP_999220) IL-1β precursors was analyzed by using the EMBL-EBI web-tool (http://www.ebi.ac.uk/Tools). The numbers presented indicate the amino acid positions. Gray indicates the same sequence as that of the equine, and dark gray reflects sequences with the same amino acids between the four species
Equine NLRP3 inflammasomes
NLRP3 is a well-characterized inflammasome because it is involved in a variety genetic, infectious, and metabolic diseases; however, the equine NLRP3 inflammasome has not yet been characterized (Ahn et al. 2018d; Guo et al. 2015; Vrentas et al. 2018). In this study, we characterized NLRP3 inflammasome activation in equine PBMCs by applying several well-known NLRP3 activation triggers: ATP, NG, Alum, and MSU (Hornung et al. 2008; Mariathasan et al. 2006; Martinon et al. 2006). Equine PBMCs were primed with LPS to induce the expression of inflammasome components and then treated with increasing dosages of each NLRP3 activation trigger, as indicated in Fig. 2A. The results reveal that the LPS-primed PBMCs showed up-regulation of pro-IL-1β expression in the cellular lysates. In addition, all NLRP3 activation triggers dose-dependently induced IL-1β secretion in the cellular supernatant (Fig. 2B). Based on Fig. 2B bar graphs, the band intensities of IL-1β p17 secretion were significantly increased by treatment with the NLRP3 activation triggers. Thus, common NLRP3 activation triggers (ATP, NG, Alum, and MSU) elicit equine IL-1β secretion, thereby implying that equine NLRP3 inflammasomes are similar to those in other species.
Effect of NLRP3 activation triggers on equine PBMCs. A, Schematic diagram of the experimental procedure. Briefly, equine PBMCs were primed with LPS (1 μg/mL) for 3 h and then treated with NLRP3 triggers for the indicated time. Cellular supernatants (Sup) and lysates (Lys) were then analyzed by immunoblotting. B, LPS-primed equine PBMCs treated with the indicated concentration of the NLRP3 triggers ATP, NG, Alum, or MSU. Sup and Lys were immunoblotted with anti-IL-1β sera. The lower bar graphs present the mean ± SD intensities of IL-1β p17 normalized to that of actin in Lys. Immunoblotting images are representative of two independent experiments
Equine NLRC4 and AIM2 inflammasomes
Two other inflammasomes, NLRC4 and AIM2, are mainly activated by pathogens and regarded as gatekeepers for intracellular infection. Based on previous study, Salmonella Typhimurium induces assembly of the NLRC4 inflammasome and Listeria monocytogenes triggers activation of the AIM2 inflammasome (Diamond et al. 2017; Guo et al. 2015; Tsuchiya et al. 2010; Zhao et al. 2011). In this study, equine PBMCs were primed with LPS and then inoculated with Salmonella or Listeria to activate the NLRC4 or AIM2 inflammasomes (Fig. 3A). As expected, both bacterial treatments lead to the secretion of IL-1β in the supernatant. Moreover, the IL-1β p17 band intensities in the bacteria-inoculated samples were significantly greater than those of the non-inoculated samples. In addition, flagellin or dsDNA were intracellularly introduced into LPS-primed equine PBMCs to activate NLRC4 or AIM2 inflammasome (Fig. 3B). Similar to the bacteria treatment results, flagellin and dsDNA provoked IL-β secretion in dose-dependent manners. Thus, various well-known NLRC4 and AIM2 activation triggers induced IL-1β secretion.
Effect of NLRC4 or AIM2 activation triggers on equine PBMCs. A, LPS-primed equine PBMCs were inoculated with Salmonella (Salmonella enterica serovar Typhimurium) or Listeria (Listeria monocytogenes) as indicated. IL-1β secretion was analyzed by immunoblotting. The band intensities of the active form of IL-1β p17 are presented in the lower bar graphs (mean ± SD). B, Equine PBMCs were primed with LPS and then flagellin or dsDNA was introduced into the cytoplasm. IL-1β secretion was analyzed by immunoblotting. Immunoblotting images are representative of two independent experiments
Mechanistic study of equine NLRP3 inflammasome activation
NLRP3 inflammasomes are activated by several intracellular signaling molecules and proteins. In particular, potassium efflux has been reported to be a key mediator of NLRP3 inflammasome activation (Munoz-Planillo et al. 2013). To characterize equine NLRP3 inflammasome activation, we applied the potassium efflux inhibitors, glibenclamide (Glibe) and an extracellular high potassium solution (KCl) (Di et al. 2018; Fernandes-Alnemri et al. 2010; Lamkanfi et al. 2009). As shown in Fig. 4A and Supplementary Figure 1, equine PBMCs primed with LPS were treated with Glibe or KCl in the presence of ATP, an NLRP3 trigger. As expected, ATP led to the secretion of equine IL-1β and the pan-caspase inhibitor (Z-VAD-FMK) completely blocked that IL-1β secretion. The KCl treatment inhibited the ATP-mediated IL-1β secretion but not completely. We undertook the same experiments in mouse BMDMs and the human THP-1 cells. In mouse macrophages (Fig. 4B), ATP mediated the secretion of IL-1β, and treatment with Glibe or KCl blocked the ATP-induced IL-1β secretion. In addition, Z-VAD-FMK blocked the ATP-mediated IL-1β secretion. As shown in Fig. 4C, human THP-1 cells produced the active form of IL-1β in response to treatment with NG, an NLRP3 activation trigger. Moreover, Glibe, KCl, and Z-VAD-FMK treatments inhibited IL-1β secretion in THP-1 cells. Based on those results, compared to human and mouse cell responses, the equine NLRP3 inflammasome activation response might be less dependent on potassium efflux stimulation.
Effects of potassium efflux on NLRP3 inflammasome activation. A, Equine PBMCs were primed with LPS and then treated with ATP (5 mM) in the presence of glibenclamide (Glibe, 150 μM), high KCl solution (KCl, 50 mM), or Z-VAD (Z-VAD-FMK, 10 μg/mL). B, Mouse BMDMs were primed with LPS for 3 h followed by ATP (5 mM) and Glibe, KCl, or Z-VAD treatment. C, THP-1 cells were pre-treated with PMA to induce differentiation into macrophage-like cells. PMA-treated THP-1 cells were then primed with LPS and treated with NG (40 μM) in the presence of Glibe, KCl, or Z-VAD. The lower bar graphs indicate the relative equine IL-1β p17 band intensities or IL-1β secretion of human and mice (mean ± SD). Immunoblotting images are representative of two independent experiments.
Discussion
In this study, we characterized equine inflammasome activation and its upstream mechanism. Inflammasome activation can be divided into two distinct steps: priming and activation (Ahn et al. 2018d; Lee 2013). During the priming step, equine monocytes were up-regulated to the p36 pro-form of IL-1β by LPS treatment. The LPS-primed equine monocytes secreted the p17 active form of IL-1β in response to exposure to inflammasome activators (ATP, NG, Alum, MSU, Salmonella, Listeria, flagellin, and dsDNA) at the activation step. To characterize the intracellular mechanism, a common pathway, potassium efflux, in the activation of NLRP3 inflammasomes was blocked by glibenclamide or high KCl solution at the activation step. The results indicated that equine PBMCs showed a lower response level to the pathway blockage than those of human THP-1 cells and mouse BMDMs. Taken together, the results show that the NLRP3, NLRC4, and AIM2 equine inflammasomes are activated by activation triggers well-established in other species including human and mouse. However, the lower response of the potassium efflux pathway indicates that it may not be a key pathway in the activation of equine inflammasomes.
Before establishment of the inflammasome concept, it was reported that ATP and NG elicited IL-1β maturation and secretion (Perregaux and Gabel 1994). It was subsequently revealed that ATP activated the NLRP3 inflammasome through potassium efflux (Mariathasan et al. 2006). NG, a bacterial toxin derived from Streptomyces hygroscopicus, acts as a potassium ionophore and decreases intracellular potassium levels resulting in NLRP3 inflammasome activation similar to that of ATP (Mariathasan et al. 2006). To date, several NLRP3 activation triggers have been reported. Among them, Alum can activate NLRP3 inflammasomes and is currently used as a vaccine adjuvant (Hornung et al. 2008). As well, MSU crystals, which can induce acute gout inflammation, can induce the secretion IL-1β via NLRP3 inflammasome activation (Martinon et al. 2006). Although NLRP3 inflammasomes are involved in genetic, metabolic, and infectious diseases, NLRC4 and AIM2 inflammasomes have been mainly associated with reactions to pathogens (Guo et al. 2015). Salmonella enterica serovar Typhimurium, a Gram-negative bacteria related to food- and water-borne diseases, activates both NLRP3 and NLRC4 inflammasomes (Diamond et al. 2017). Intracellular flagellin and T3SS derived from Salmonella Typhimurium activate NLRC4 inflammasomes through the recognition of NAIP5 (Diamond et al. 2017). Extracellular flagellin interacts with toll-like receptor 5, whereas cytosolic flagellin is recognized by NLRC4/NAIP5 following inflammasome activation (Zhao et al. 2011). Listeria monocytogenes, a Gram-negative bacteria associated with listeriosis and lethal food-borne infections, contains components that can activate NLRP3, NLRC4, and AIM2 inflammasomes (Tsuchiya et al. 2010). Among various inflammasomes, Listeria-mediated inflammasome activation is strongly dependent on AIM2 (Tsuchiya et al. 2010). AIM2 also recognizes dsDNA derived from infected bacteria and/or damaged cells or mitochondria (Man et al. 2016). Various previously well-characterized activation triggers of NLRP3, NLRC4, and AIM2 inflammasomes were shown in the present study to successfully elicit IL-1β maturation and secretion in equine PBMCs. We also obtained similar results in porcine PBMCs (Ahn et al. 2018c; Kim et al. 2014b). Taken together, equine inflammasome activation might be identical with that in humans, mice, and pigs.
Although equine inflammasome activation has not been widely reported, there are several reports on the role of equine IL-1β, one of the final substrates of inflammasome activation, in arthritis (Colbath et al. 2018; Lasarzik et al. 2016; Ross et al. 2012). Recombinant IL-1β has been injected into the joints of horse to induce a model of arthritis (Colbath et al. 2018; Ross et al. 2012). In addition, synovial levels of IL-1β have been monitored as a biomarker of arthritis (Lasarzik et al. 2016). Based on these reports, inflammasome activation triggers might be replaced by recombinant IL-1β in efforts to induce arthritis, and synovial levels of inflammasome components could be useful as biomarkers of arthritis.
The intracellular mechanistic pathways of the NLRC4 and AIM2 inflammasomes are relatively well-established when compared with that of the NLRP3 inflammasome (Munoz-Planillo et al. 2013; Swanson et al. 2019). NLRC4 and NAIPs, which directly interact with cytosolic flagellin and/or T3SS, recruit ASC and caspase-1 to activate inflammasomes (Duncan and Canna 2018). The hematopoietic interferon-inducible nuclear (HIN) domain of AIM2 binds with cytosolic dsDNA and starts to assemble other inflammasome components such as ASC and caspase-1 (Jin et al. 2012). Otherwise, a direct binding pattern of NLRP3 has not been fully reported because a variety of NLRP3 activation triggers, from metabolic products to pathogens, activate NLRP3 inflammasomes (Munoz-Planillo et al. 2013). Thus, it has been suggested that common cytosolic signals, such as cytosolic ions changes, lysosomal disruption, mitochondrial dysregulation, and metabolic changes, can act as upstream signals in the activation of NLRP3 inflammasomes (Swanson et al. 2019). Among these, the potassium efflux pathway is the most fully characterized because cytosolic potassium depletion has been observed when macrophages are treated with a variety of NLRP3 activation triggers (Di et al. 2018; Munoz-Planillo et al. 2013). In this study, we tested the effect of potassium efflux on the activation of equine NLRP3 inflammasomes (Fig. 4). Glibenclamide (or glyburide), used as a type 2 diabetes drug, is an inhibitor of the ATP-sensitive potassium channel and inhibits IL-1β secretion resulting from NLRP3 inflammasome activation (Lamkanfi et al. 2009). Administration of an extracellular high potassium solution is reported to block the secretion of IL-1β by inhibiting potassium efflux (Di et al. 2018; Fernandes-Alnemri et al. 2010). Unexpectedly, the disruption of potassium efflux did not inhibit IL-1β secretion following equine NLRP3 inflammasome activation as fully as that of human and mouse NLRP3 inflammasomes. As well, we previously tested the effect of glibenclamide and high KCl solution on porcine NLRP3 inflammasome activation (Kim et al. 2014b) and observed that IL-1β secretion of swine PBMCs treated with NLRP3 triggers was significantly attenuated by the interruption of potassium efflux, similar to the effects on human and rodent cells (Kim et al. 2014b). Based on these findings, the potassium efflux pathway is not as tightly involved in the activation of equine NLRP3 inflammasome as it is in other species.
References
Ahn H et al (2017) Lentinan from shiitake selectively attenuates AIM2 and non-canonical inflammasome activation while inducing pro-inflammatory cytokine production. Sci Rep 7:1314. https://doi.org/10.1038/s41598-017-01462-4
Ahn H et al (2017) Methylene blue inhibits NLRP3, NLRC4, AIM2, and non-canonical inflammasome activation. Sci Rep 7:12409. https://doi.org/10.1038/s41598-017-12635-6
Ahn H et al (2018) Mercury and arsenic attenuate canonical and non-canonical NLRP3 inflammasome activation. Sci Rep 8:13659. https://doi.org/10.1038/s41598-018-31717-7
Ahn H et al (2019) Nonsaponin fraction of Korean Red Ginseng attenuates cytokine production via inhibition of TLR4 expression. J Ginseng Res 43:291–299. https://doi.org/10.1016/j.jgr.2018.03.003
Ahn H, Lee GS (2017) Isorhamnetin and hyperoside derived from water dropwort inhibits inflammasome activation Phytomedicine. Int J Phytother Phytopharmacol 24:77–86. https://doi.org/10.1016/j.phymed.2016.11.019
Ahn H, Kim J, Jeung EB, Lee GS (2014) Dimethyl sulfoxide inhibits NLRP3 inflammasome activation. Immunobiology 219:315–322. https://doi.org/10.1016/j.imbio.2013.11.003
Ahn H, Kim J, Lee MJ, Kim YJ, Cho YW, Lee GS (2015) Methylsulfonylmethane inhibits NLRP3 inflammasome activation. Cytokine 71:223–231. https://doi.org/10.1016/j.cyto.2014.11.001
Ahn H, Kang SG, Yoon SI, Kim PH, Kim D, Lee GS (2018) Poly-gamma-glutamic acid from Bacillus subtilis upregulates pro-inflammatory cytokines while inhibiting NLRP3, NLRC4 and AIM2 inflammasome activation. Cell Mol Immunol 15:111–119. https://doi.org/10.1038/cmi.2016.13
Ahn H, Kim J, Kwon S, Kim PH, Kwon HM, Lee E, Lee GS (2018) Triggers of NLRC4 and AIM2 inflammasomes induce porcine IL-1beta secretion . Vet Res Commun 42:265–273. https://doi.org/10.1007/s11259-018-9729-x
Ahn H, Kwon HM, Lee E, Kim PH, Jeung EB, Lee GS (2018) Role of inflammasome regulation on immune modulators. J Biomed Res 32:401–410. https://doi.org/10.7555/JBR.32.20170120
Angelis D, Fontanez-Nieves TD, Delivoria-Papadopoulos M (2014) The role of SRC kinase in the caspase-1 pathway after hypoxia in the brain of newborn piglets. Neurochem Res 39:2118–2126. https://doi.org/10.1007/s11064-014-1404-1
Ciraci C, Janczy JR, Sutterwala FS, Cassel SL (2012) Control of innate and adaptive immunity by the inflammasome. Microbes infect 14:1263–1270. https://doi.org/10.1016/j.micinf.2012.07.007
Colbath AC, Dow SW, Hopkins LS, Phillips JN, McIlwraith CW, Goodrich LR (2018) Induction of synovitis using Interleukin-1 Beta: Are there differences in the response of middle carpal joint compared to the tibiotarsal joint? Front Vet Sci 5:208. https://doi.org/10.3389/fvets.2018.00208
Dawson HD, Smith AD, Chen C, Urban JF Jr (2017) An in-depth comparison of the porcine, murine and human inflammasomes; lessons from the porcine genome and transcriptome. Vet Microbiol 202:2–15. https://doi.org/10.1016/j.vetmic.2016.05.013
Di A et al (2018) The TWIK2 potassium efflux channel in macrophages mediates NLRP3 inflammasome-induced inflammation. Immunity 49:56-65 e54. https://doi.org/10.1016/j.immuni.2018.04.032
Di Virgilio F, Dal Ben D, Sarti AC, Giuliani AL, Falzoni S (2017) The P2 × 7 Receptor in infection and inflammation . Immunity 47:15–31. https://doi.org/10.1016/j.immuni.2017.06.020
Diamond CE, Leong KWK, Vacca M, Rivers-Auty J, Brough D, Mortellaro A (2017) Salmonella typhimurium-induced IL-1 release from primary human monocytes requires NLRP3 and can occur in the absence of pyroptosis. Sci Rep 7:6861. https://doi.org/10.1038/s41598-017-07081-3
Duncan JA, Canna SW (2018) The NLRC4 inflammasome . Immunol Rev 281:115–123. https://doi.org/10.1111/imr.12607
Evavold CL, Kagan JC (2018) How inflammasomes inform adaptive immunity. J Mol Biol 430:217–237. https://doi.org/10.1016/j.jmb.2017.09.019
Fernandes-Alnemri T et al (2010) The AIM2 inflammasome is critical for innate immunity to Francisella tularensis. Nat Immunol 11:385–393. https://doi.org/10.1038/ni.1859
Guo H, Callaway JB, Ting JP (2015) Inflammasomes: mechanism of action, role in disease, and therapeutics. Nat Med 21:677–687. https://doi.org/10.1038/nm.3893
Han BC et al (2017) Nonsaponin fractions of Korean Red Ginseng extracts prime activation of NLRP3 inflammasome. J Ginseng Res 41:513–523. https://doi.org/10.1016/j.jgr.2016.10.001
Hornung V et al (2008) Silica crystals and aluminum salts activate the NALP3 inflammasome through phagosomal destabilization. Nat Immunol 9:847–856. https://doi.org/10.1038/ni.1631
Hu Q, Wei B, Wei L, Hua K, Yu X, Li H, Ji H (2015) Sodium tanshinone IIA sulfonate ameliorates ischemia-induced myocardial inflammation and lipid accumulation in Beagle dogs through NLRP3 inflammasome. Int J Cardiol 196:183–192. https://doi.org/10.1016/j.ijcard.2015.05.152
Islam MA et al (2016) Deciphering transcriptome profiles of peripheral blood mononuclear cells in response to PRRSV vaccination in pigs. BMC Genomics 17:641. https://doi.org/10.1186/s12864-016-2849-1
Jalilian I, Peranec M, Curtis BL, Seavers A, Spildrejorde M, Sluyter V, Sluyter R (2012) Activation of the damage-associated molecular pattern receptor P2 × 7 induces interleukin-1beta release from canine monocytes. Vet Immunol Immunopathol 149:86–91. https://doi.org/10.1016/j.vetimm.2012.05.004
Jin T et al (2012) Structures of the HIN domain:DNA complexes reveal ligand binding and activation mechanisms of the AIM2 inflammasome and IFI16 receptor. Immunity 36:561–571. https://doi.org/10.1016/j.immuni.2012.02.014
Kim J et al (2014) Korean red ginseng extracts inhibit NLRP3 and AIM2 inflammasome activation. Immunol Lett 158:143–150. https://doi.org/10.1016/j.imlet.2013.12.017
Kim J et al (2019) Obovatol inhibits NLRP3, AIM2, and non-canonical inflammasome activation. Phytomedicine 63:153019. https://doi.org/10.1016/j.phymed.2019.153019
Kim J, Ahn H, Woo HM, Lee E, Lee GS (2014b) Characterization of porcine NLRP3 inflammasome activation and its upstream mechanism. Vet Res Commun 38:193–200. https://doi.org/10.1007/s11259-014-9602-5
Lamkanfi M et al (2009) Glyburide inhibits the Cryopyrin/Nalp3 inflammasome. J Cell Biol 187:61–70. https://doi.org/10.1083/jcb.200903124
Lasarzik J et al (2016) Interleukin-1 receptor antagonist and Interleukin-1 Beta levels in equine synovial fluid of normal and osteoarthritic joints: Influence of anatomic joint location and repeated arthrocentesis. J Equine Vet Sci 42:67–72. https://doi.org/10.1016/j.jevs.2016.03.017
Lee GS (2013) Inflammasomes, multi-cellular protein complex in myeloid cells, induce several metabolic diseases via interleukin-1β maturation. J Biomed Res 14:195–200. https://doi.org/10.12729/jbr.2013.14.4.195
Lee J, Ahn H, Hong EJ, An BS, Jeung EB, Lee GS (2016) Sulforaphane attenuates activation of NLRP3 and NLRC4 inflammasomes but not AIM2 inflammasome. Cell Immunol 306–307:53–60. https://doi.org/10.1016/j.cellimm.2016.07.007
Li Y, Xu S, Jiang B, Cohen RA, Zang M (2013) Activation of sterol regulatory element binding protein and NLRP3 inflammasome in atherosclerotic lesion development in diabetic pigs. PloS One 8:e67532. https://doi.org/10.1371/journal.pone.0067532
Lugrin J, Martinon F (2018) The AIM2 inflammasome: Sensor of pathogens and cellular perturbations. Immunol Rev 281:99–114. https://doi.org/10.1111/imr.12618
Man SM, Karki R, Kanneganti TD (2016) AIM2 inflammasome in infection, cancer, and autoimmunity: Role in DNA sensing, inflammation, and innate immunity European. J Immunol 46:269–280. https://doi.org/10.1002/eji.201545839
Mariathasan S et al (2006) Cryopyrin activates the inflammasome in response to toxins and. ATP Nat 440:228–232. https://doi.org/10.1038/nature04515
Martinon F, Petrilli V, Mayor A, Tardivel A, Tschopp J (2006) Gout-associated uric acid crystals activate the NALP3 inflammasome. Nature 440:237–241. https://doi.org/10.1038/nature04516
Munoz-Planillo R, Kuffa P, Martinez-Colon G, Smith BL, Rajendiran TM, Nunez G (2013) K(+) efflux is the common trigger of NLRP3 inflammasome activation by bacterial toxins and particulate matter. Immunity 38:1142–1153. https://doi.org/10.1016/j.immuni.2013.05.016
Perregaux D, Gabel CA (1994) Interleukin-1 beta maturation and release in response to ATP and nigericin. Evidence that potassium depletion mediated by these agents is a necessary and common feature of their activity. J Biol Chem 269:15195–15203
Ross TN, Kisiday JD, Hess T, McIlwraith CW (2012) Evaluation of the inflammatory response in experimentally induced synovitis in the horse: a comparison of recombinant equine interleukin 1 beta and lipopolysaccharide . Osteoarthr Cartil 20:1583–1590. https://doi.org/10.1016/j.joca.2012.08.008
Swanson KV, Deng M, Ting JP (2019) The NLRP3 inflammasome: molecular activation and regulation to therapeutics. Nat Rev Immunol 19:477–489. https://doi.org/10.1038/s41577-019-0165-0
Tohno M, Shimosato T, Aso H, Kitazawa H (2011) Immunobiotic Lactobacillus strains augment NLRP3 expression in newborn and adult porcine gut-associated lymphoid tissues . Vet Immunol Immunopathol 144:410–416. https://doi.org/10.1016/j.vetimm.2011.09.010
Tsuchiya K et al (2010) Involvement of absent in melanoma 2 in inflammasome activation in macrophages infected with Listeria monocytogenes. J Immunol 185:1186–1195. https://doi.org/10.4049/jimmunol.1001058
Vrentas CE, Schaut RG, Boggiatto PM, Olsen SC, Sutterwala FS, Moayeri M (2018) Inflammasomes in livestock and wildlife: Insights into the intersection of pathogens and natural host species . Vet Immunol Immunopathol 201:49–56. https://doi.org/10.1016/j.vetimm.2018.05.008
Zhang K, Tao P, Liu J, Wang Q, Ge S, Ning Z (2017) Distinct expression profile and histological distribution of NLRP3 inflammasome components in the tissues of Hainan black goat suggest a site-specific role in the inflammatory response. Acta Vet Hung 65:402–416. https://doi.org/10.1556/004.2017.038
Zhao Y et al (2011) The NLRC4 inflammasome receptors for bacterial flagellin and type III secretion apparatus. Nature 477:596–600. https://doi.org/10.1038/nature10510
Acknowledgments
This study was supported by the Basic Science Research Program through the National Research Foundation of Korea (NRF) funded by the Ministry of Education, Science and Technology (NRF-2018R1A2B2004097 and NRF-2018R1D1A1B07048337). We thank Prof. Yeonsu Oh (Kangwon National University) for supporting the blood collection.
Author information
Authors and Affiliations
Contributions
Ahn, H., Kim, J., and Lee, G.-S. designed the research; Ahn, H., Kim, J., and Lee, H., performed the experiments; Ahn, H., Lee, E., and Lee, G.-S. analyzed the results; Ahn, H. and Lee, G.-S. wrote the paper; Lee, E. edited and commented on the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 371 kb)
Rights and permissions
About this article
Cite this article
Ahn, H., Kim, J., Lee, H. et al. Characterization of equine inflammasomes and their regulation. Vet Res Commun 44, 51–59 (2020). https://doi.org/10.1007/s11259-020-09772-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11259-020-09772-1