Abstract
Purpose
This study evaluated the correlation of anti-β2-glycoprotein I (anti-β2-GPI) antibodies with complement activation in patients with idiopathic membranous nephropathy (IMN).
Methods
Thirty-two IMN patients with positive anti-β2-GPI antibody were enrolled, and 32 age- and sex-matched IMN patients with negative anti-β2-GPI antibody were randomly enrolled as controls. The frozen serum samples of these 64 patients were collected for detection of anti-phospholipase A2 receptor (PLA2R) antibody and the activity of three complement pathways. Paraffin specimens of the kidney tissues of these 64 patients were collected for immunohistochemical staining of C4d.
Results
IMN patients with positive anti-β2-GPI antibody had a significant decline of the residual complement activity of alternative pathway than those with negative anti-β2-GPI antibody (37.4 ± 21.2% vs 65.7 ± 50.5%, P = 0.021). The positive rate of kidney C4d staining in IMN patients with and without anti-β2-GPI was 65.6 and 81.2%, with no significant difference (P = 0.257). Patients with and without anti-β2-GPI had the same positive rate of anti-PLA2R antibody.
Conclusion
Anti-β2-GPI antibody was associated with alternative complement activation in patients with IMN.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Idiopathic membranous nephropathy (IMN) is a non-inflammatory autoimmune disease of the kidney glomerulus, characterized by the formation of immune deposits and complement-mediated proteinuria [1, 2]. The autoimmune nature of MN was clearly delineated in 2009 with the identification of the antigen of phospholipase A2 receptor (PLA2R) [3]. In 2014, a second autoantigen, thrombospondin type-1 domain-containing 7A (THSD7A) was identified [4]. Recently, neural epidermal growth factor-like 1 protein (NELL-1) protein was defined as a third possible antigen in IMN [5]. Anti-PLA2R antibodies and anti-THSD7A antibodies can be detected in approximately 70% or more of IMN patients [6], still up to 30% of IMN patients have no detectable serum antibodies. After the glomerular deposition of autoimmune antibodies, complement activation is involved in the progress of IMN [7]. Although immunostaining for complement C3 is universal in IMN renal biopsy tissue, the serum levels of C3 and C4 are always in normal ranges, and the pathway of complement activation involved is unclear. There are three complement activation pathways, which are classical pathway, mannan-binding lectin (MBL) pathway and alternative pathway. Thus far, most reports showed that the complement activation in IMN was mainly through the alternative pathway, while the classical pathway was not involved, and the involvement of MBL pathway was still uncertain [8, 9].
Antiphospholipid antibodies (aPLs) are a heterogeneous family of antibodies against phospholipids or phospholipid-binding proteins. Among these, the main antibodies are anti-β2-glycoprotein I (anti-β2 GPI) antibodies and anticardiolipin (ACL) antibodies [10, 11]. In vivo immune-deficient mice transfused with peripheral blood lymphocytes from a patient with aPLs and MN developed renal lesions resembling human MN [12]. In a retrospective study, ten antiphospholipid syndrome (APS) patients with renal involvement underwent renal biopsy and four of them had MN [13]. In our previous study [14], we found that the positive rate of anti-β2-GPI antibodies in IMN patients was 11.9%, which was significantly higher than the nephrotic patients with MCD/FSGS (3.7%), and anti-β2-GPI antibody-positive MN patients had significant improvement of serum creatinine compared to anti-β2-GPI antibody-negative MN patients after 24 weeks of treatment [14]. These results revealed that anti-β2-GPI antibody may play a role in the progression of IMN.
In this study, we measured the serum levels of anti-β2GPI antibody, anti-PLA2R antibody and the complement components in the same IMN patients, and tried to find out the association between anti-β2GPI antibody and anti-PLA2R antibody and the correlation of anti-β2GPI antibody with complement activation pathways.
Patients and methods
Patients
According to our reported study [14], there were 267 IMN patients hospitalized in the First Affiliated Hospital of Zhejiang University between June 2015 and June 2017. Among them, 32 patients were anti-β2-GPI antibody-positive, the other 32 age- and sex-matched patients with negative anti-β2-GPI antibody were randomly enrolled as controls. Briefly, patients with negative anti-β2-GPI antibody were matched to patients with positive anti-β2-GPI antibody according to age ± 2 years and same gender, then the “Case Control Matching” procedure was used to choose the controls by SPSS 22.0. The frozen serum samples of these 64 patients were collected from the biological sample bank of our hospital (stored in the refrigerator at – 80 ℃) for detection of anti-PLA2R antibody and the activity of three complement pathways. Paraffin specimens of the kidney tissues of these 64 patients were collected from the kidney pathological specimen library of our hospital for immunohistochemical staining of C4d. This study was approved by the Ethics Committee of First Affiliated Hospital, Zhejiang University, approval number 2018503.
Data collection
Clinical data were collected before renal biopsy, including anti-β2-GPI antibodies, ACL antibodies, sex, age, duration, serum albumin, serum creatinine, estimated glomerular filtration rate (eGFR), serum complement C3 and C4, and urine protein/creatinine ratio; renal biopsy data were including C3, C1q and IgG subtypes (IgG1and IgG4) deposits in the kidney.
Measurement of anti-PLA2R antibodies
The serum samples were stored at – 80 ℃ and thawed at room temperature, the levels of anti-PLA2R antibody were measured using ELISA kits (EUROIMMUN®, German). The concentration ≥ 14RU/ml was considered positive for anti-PLA2R antibody.
Activations of the three complement pathways
We measured the activity of the complement pathways using a commercial kit (WIESLAB®, Sweden) according to the manufacture’s recommendations. This enzyme immunoassay is used for the measurement of a functionally active classical pathway, MBL pathway, and alternative pathway in human serum. The wells of the microtiter plate were coated with specific activators of each pathway. Patient sera used in the classical and MBL pathway assays were applied to the wells at 1:100 dilution; for the alternative pathway assay, a 1:18 dilution with the diluent provided in the kit was used. The quantity of complement activation correlates with the color intensity and the absorbance was measured at OD405. All measured values were expressed as percentage complement activity, determined as follows: (sample value − negative control value)/(positive control value − negative control value) × 100.
Immunohistochemical staining of C4d
Expression of C4d was performed by immunohistochemistry using the immunoperoxidase technique. The sections were deparaffinized and hydrated, and antigen retrieval was performed by high-temperature and high-pressure method. After incubation with anti-C4d primary antibody (Biomedica®, Austria), the sections were developed using Kit-9901 (Sangon Biotech, China) as a secondary antibody, and diaminobenzidine (Sangon Biotech, China). Immunostaining for C4d was considered positive in cases with more than 50% of immune-stained glomeruli [15].
Statistical analysis
Variables are described as mean and standard deviation or proportion. Chi-square analysis or t-tests were used to compare differences between MN patients with and without anti-β2-GPI antibody. A P value of < 0.05 was considered statistically significant. All statistical analyses were performed using SPSS 22 (IBM, Cary, NC, USA).
Results
The general clinical characteristics of these 64 patients with IMN were summarized in Table 1, there were no significant differences in disease duration, the levels of serum albumin, serum creatinine, eGFR and urine protein/creatinine ratio between patients with and without anti-β2-GPI antibody.
As shown in Table 2, the average positive rate of anti-PLA2R antibody was 64.1%, including 20 cases (62.5%) in the anti-β2-GPI positive group and 21 cases (65.6%) in the anti-β2-GPI negative group (P > 0.05). The median titer of anti-PLA2R was 58.1 (0–290.5) RU/ml in the anti-β2-GPI positive group and 88.2 (0–612.9) RU/ml for the anti-β2-GPI negative group (P = 0.324).
IMN patients with positive anti-β2-GPI antibody had a significant decline of the residual complement activity of alternative pathway than those with negative anti-β2-GPI antibody (37.4 ± 21.2% vs 65.7 ± 50.5%, P = 0.021), indicating that the complement alternative pathway was significantly activated in IMN patients with positive anti-β2-GPI antibody. There were no significant differences in the residual complement activity of classical pathway and the MBL pathway between the two groups. The positive rate of kidney C4d staining in IMN patients with and without anti-β2-GPI antibody was 65.6 and 81.2% (P = 0.257). Figure 1a, b showed C4d-positive and C4d-negative glomerulus of typical IMN kidney. There were no significant differences of serum levels of C3 and C4, and glomerular deposits of C3, C1q, IgG1, and IgG4 between the two groups (Table 3).
Discussion
In this study, we found that serum activity of complement alternative pathway was significant higher in IMN patients with positive anti-β2-GPI antibody compared with those with negative anti-β2-GPI antibody, and there were no significant differences in C1q and C4d deposits between the two groups, showing the presence of anti-β2-GPI antibody was associated with higher activity of complement alternative pathway but not classical pathway or MBL pathway. There were evidences of alternative complement activation in MN. Studies have shown that C1q deposition in glomerulus was negative in IMN patients, but C3c, MAC and factor P were positive [16, 17]. The Borza group [18] used a model of MN induced by immunization with the noncollagenous domain of the α-3 chain of collagen in complement factor B-deficient mice, which lack a functional alternative pathway. Unlike wild-type mice, those lacking factor B did not develop albuminuria or exhibit glomerular deposition of C5b-9, despite similar amounts of deposited IgG. Thus, this model provided direct evidence that alternative pathway was necessary for complement activation by subepithelial immune complexes.
β2 GPI has a weak binding capacity with negatively charged phospholipids and therefore does not inhibit phospholipid-dependent clotting, but in the presence of aPLs, such as anti-β2-GPI antibody or ACL, it can mediate the binding of aPLs to the membrane/phospholipid membrane, causing damage to endothelial cells, leading to hypercoagulability and thrombus formation [10, 11]. Studies also showed a strong association between complement activation and aPLs in patients with primary or secondly APS [19, 20]. Oku et al. investigated the significance of complement activation in patients with primary APS and found that low serum concentrations of complement were common in patients with primary APS, suggesting that aPLs may activate monocytes and macrophages via an aphylatoxins produced during complement activation [21]. In a study of the correlation between anti-β2-GPI antibodies and B factor in patients with lupus nephritis (LN) and glomerular microthrombosis, Zhou et al. found that the serum B factor was significantly correlated with anti-β2GPI antibody, which indicated the process of alternative complement activation mediated by anti-β2GPI antibody [22].
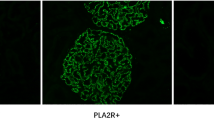
In our study, the positive rate of anti-PLA2R antibody was 62.5% in anti-β2-GPI positive group and 65.6% in anti-β2-GPI negative group, which was similar to previous studies about the positive rate of anti-PLA2R antibody in IMN (50–80%) [7, 8]. Also, in our results, there was no significant difference of the positive rate of kidney PLA2R staining between MN patients with and without anti-β2-GPI antibody (84.3% vs 90.6%, P = 0.708, not shown in the results part). The above results indicated that there was no correlation between anti-PLA2R antibody and anti-β2-GPI antibody, and did supported that patients in anti-β2-GPI positive group were not secondary MN.
It is generally believed that that MN patients are more likely to develop deep vein and renal vein thrombosis comparing with other pathological types of nephrotic syndrome [23, 24]. However, whether antiphospholipid antibodies play a role is still unknown. In the present study, we did not analyze the results of coagulation function indicators and thrombosis events, so the correlation between anti-β2-GPI antibody positivity and thrombosis in MN needs further research to confirm.
However, our study has several limitations. Firstly, the small sample size may affect the efficacy of the test. Second, due to the complexity of the complement system, we measured the residual activities of the complement pathways, but did not measure the levels of some important regulatory factors, such as B factor and P factor, which may help to further prove the role of anti-β2GPI antibody-correlated complement pathway in IMN.
In conclusion, we showed here that anti-β2-GPI antibody was associated with alternative complement activation in patients with IMN.
References
Couser WG (2017) Primary membranous nephropathy. Clin J Am Soc Nephrol 12:983–997
Cattran DC, Brenchley PE (2017) Membranous nephropathy: integrating basic science into improved clinical management. Kidney Int 91:566–574
Beck LH, Bonegio RG, Lambeau G et al (2009) M-type phospholipase A2 receptor as target antigen in idiopathic membranous nephropathy. N Engl J Med 361:11–21
Tomas NM, Beck LH, Meyer-Schwesinger C et al (2014) Thrombospondin type-1 domain-containing 7A in idiopathic membranous nephropathy. N Engl J Med 371:2277–2287
Sethi S, Debiec H, Madden B et al (2020) Neural epidermal growth factor-like 1 protein (NELL-1) associated membranous nephropathy. Kidney Int 97:163–174
Pozdzik A, Brochériou I, David C et al (2018) Membranous nephropathy and anti-podocytes antibodies: implications for the diagnostic workup and disease management. Biomed Res Int 2018:6281054
Ma H, Sandor DG, Beck LH Jr (2013) The role of complement in membranous nephropathy. Semin Nephrol 33:531–542
Francis JM, Beck LH Jr, Salant DJ (2016) Membranous nephropathy: a journey from bench to bedside. Am J Kidney Dis 68:138–147
Salant DJ (2019) Unmet challenges in membranous nephropathy. Curr Opin Nephrol Hypertens 28:70–76
Sciascia S, Radin M (2018) Thrombotic antiphospholipid syndrome. Lupus 27:21–27
Levine JS, Branch DW, Rauch J (2002) The antiphospholipid syndrome. N Engl J Med 346:752–763
Levy Y, Ziporen L, Gilburd B et al (1996) Membranous nephropathy in primary antiphospholipid syndrome: description of a case and induction of renal injury in SCID mice. Hum Antibodies Hybridomas 7:91–96
Sinico RA, Cavazzana I, Nuzzo M et al (2010) Renal involvement in primary antiphospholipid syndrome: retrospective analysis of 160 patients. Clin J Am Soc Nephrol 5:1211–1217
Zhang Q, Wang Y, Xu Y et al (2019) Antiphospholipid antibodies in patients with membranous nephropathy. Nephron 143:228–233
Val-Bernal JF, Garijo MF, Val D et al (2011) C4d immunohistochemical staining is a sensitive method to confirm immunoreactant deposition in formalin-fixed paraffin-embedded tissue in membranous glomerulonephritis. Histol Histopathol 26:1391–1397
Borza DB, Zhang JJ, Beck LH Jr et al (2013) Mouse models of membranous nephropathy: the road less travelled by. Am J Clin Exp Immunol 2:135–145
Jelezarova E, Lutz HU (2005) IgG naturally occurring antibodies stabilize and promote the generation of the alternative complement pathway C3 convertase. Mol Immunol 42:1393–1403
Luo W, Olaru F, Miner JH et al (2018) Alternative pathway is essential for glomerular complement activation and proteinuria in a mouse model of membranous nephropathy. Front Immunol 9:1433
Pierangeli SS, Vega-Ostertag M, Liu X et al (2005) Complement activation: a novel pathogenic mechanism in the antiphospholipid syndrome. Ann N Y Acad Sci 1051:413–420
Ruiz-Irastorza G, Crowther M, Branch W et al (2010) Antiphospholipid syndrome. Lancet 376:1498–1509
Oku K, Atsumi T, Bohgaki M et al (2009) Complement activation in patients with primary antiphospholipid syndrome. Ann Rheum Dis 68:1030–1035
Zhou Y, Chen P, Li Y (2019) Association between antiphospholipid antibodies and factor Bb in lupus nephritis patients with glomerular microthrombosis. Int J Rheum Dis 22:2185–2190
Lionaki S, Derebail VK, Hogan SL et al (2012) Venous thromboembolism in patients with membranous nephropathy. Clin J Am Soc Nephrol 7:43–51
Barbour SJ, Greenwald A, Djurdjev O et al (2012) Disease-specific risk of venous thromboembolic events is increased in idiopathic glomerulonephritis. Kidney Int 81:190–195
Acknowledgement
This study was supported by the funds from Primary Research & Development plan of Zhejiang Province (2020C03034) to Fei Han, Zhejiang Medical and Health Science and Technology Project (2019RC036) to Lan Lan and Project of Natural Science Foundation of Zhejiang Province (Q19H050030) to Pingping Ren.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zhang, Q., Wang, Y., Ma, Y. et al. The correlation of anti-β2-glycoprotein I antibody with complement activation in patients with idiopathic membranous nephropathy. Int Urol Nephrol 53, 955–959 (2021). https://doi.org/10.1007/s11255-020-02698-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-020-02698-2