Abstract
Purpose
Heart failure is a global health concern and associated with poor health-related quality of life and increased mortality. There is a disproportionate burden on patients and health systems in low- and middle-income countries. This systematic review and meta-analysis estimates the health-related quality of life of people with heart failure in low- and middle-income countries.
Methods
A systematic literature search was conducted to identify relevant studies from January 2012 to November 2022 using the following databases: MEDLINE, EMBASE, PsycINFO, CINAHL, Web of Science, Scopus and JBI EBP database. Study screening, quality appraisal and data extraction were conducted using JBI methodology. A random-effects model was used to perform the meta-analysis. Heterogeneity was assessed using the I2 statistic. All statistical analyses were done in STATA version 17.
Results
A total of 33 studies with 5612 participants were included in this review. The Minnesota Living with Heart Failure Questionnaire (MLHFQ) and the Short-Form-36 questionnaire (SF-36) were the most used instruments across 19 and 8 studies, respectively. The pooled mean MLHFQ and SF-36 scores using the random-effects model were 46.08 (95% CI 35.06, 57.10) and 41.23 (95% CI 36.63, 45.83), respectively. In a subgroup analysis using both instruments, the highest health-related quality-of-life scores occurred in studies with inpatient participants.
Conclusion
The overall health-related quality of life of people with heart failure in low- and middle-income countries is poor. Strategies should be strategically developed to improve the health-related quality of life of people with heart failure in these countries.
Systematic review registration
PROSPERO CRD42022377781.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Background
Heart failure (HF) is a global health problem characterised by a variety of devastating symptoms, whose severity is measured by changes in symptoms with exercise [1, 2]. It is one of the major causes of morbidity, mortality and rehospitalisations internationally. In 2019, more than 64 million people were living with HF globally [3], a number predicted to increase despite advances in medical therapy [4]. Heart failure is a significant health concern and economic burden with a growing prevalence in low- and middle-income countries (LMICs) [5]. Although there are little data on the prevalence of HF in these settings, one population-based study from Northern China reported a prevalence of 3.5% (N = 2230) [6].
Health-related quality of life (HRQoL) is defined as an individual’s perception of their physical, mental, emotional and social health functioning [7]. People with HF are more likely to experience variety of symptoms such as shortness of breathing, fatigue, pain and oedema and develop emotional conditions like depression compared to the general population [8, 9]. These symptoms affect activities of daily living and can adversely affect HRQoL [10]. In LMICs, HF is associated with poorer outcomes, including longer hospital stays, lower HRQoL and significant in-hospital mortality [11]. People with HF and associated poor HRQoL are at further risk of the deleterious effects of rehospitalisation and increased healthcare costs. Consequently, there is an imperative to evaluate the level of HRQoL in these populations [12, 13].
To date, there is a paucity of systematic reviews or meta-analyses estimating the HRQoL of people with HF in LMICs. A recently published systematic review determined the global level of HRQoL in people with HF [14]. However, this estimate was mainly based on data from developed countries with little data from developing countries, which limits generalisability to populations in LMICs. Additionally, this review only used three international databases (PubMed, Scopus and Web of Science) which was inconsistent with data collection and reporting standards for systematic reviews [15]. Consequently, this paper reports a systematic review and meta-analysis which estimated the HRQoL among people with HF in LMICs. The findings will indicate a need to develop strategies to improve management, care and HRQoL in these populations.
Review question
What is the HRQoL of people with heart failure in low- and middle-income countries?
Inclusion criteria
Participants
Studies including adult participants with a confirmed diagnosis of HF were included in this review.
Condition
This review included studies that reported the HRQoL of people with HF measured using a psychometrically validated instrument. HRQoL was defined as an individual’s perceived physical and mental health functioning over time [16].
Context
This review included studies from LMICs. For the purposes of this review, low- to middle-income countries were defined using the World Bank atlas method based on the stratification of economies based on gross national income (GNI) per capita. Low-income countries were those with a GNI per capita of $1,045 or less; lower and upper middle-income economies were those with a GNI per capita between $1,046 and $4,095 and $4,096 and $12,695, respectively [17].
Types of studies
Observational (cross-sectional, cohort, case–control) studies that reported the HRQoL of people with HF published in English from January 2012 to November 2022 were included in this review.
Methods
The Joanna Briggs Institute (JBI) methodology for Systematic Reviews [15] was used to inform the processed for this review, and the protocol was registered with the PROSPERO database (registration number CRD42022377781).
Search strategy
A three-step search strategy was undertaken on 9 November 2022 using several databases including MEDLINE (Ovid), EMBASE (Ovid), PsycINFO (EBSCOhost), CINAHL(EBSCOhost), Web of Science (direct access), Scopus (direct access) and JBI EBP database (Ovid) to identify relevant research from the January 2012 to November 2022. The CoCoPop (Co = Condition, Co = Context, Pop = Population) framework was used to develop the search strategy using a combination of subject headings (index terms) and text words including “quality of life”, “health-related quality of life”, QoL, HRQoL, “heart diseases”, “heart failure”, “cardiac failure” and all LMICs [17]. Boolean operators were used to combine search terms. The search strategy and results are reported in Appendix I.
Study selection
All identified records were imported into EndNote V20 (Clarivate Analytics, PA, USA). After the removal of duplicates, all identified articles were exported into Microsoft Excel (Redmond, Washington, USA) for screening. Blinded screening was done by two independent reviewers, starting with a title and abstract screening, followed by a full-text screening. First, all titles and abstracts were screened by two authors (HM and PS) in accordance with the predetermined inclusion criteria and a preliminary list of articles for full-text screening was generated. Then, the two reviewers (HM and PS) screened the full-text articles against the inclusion criteria. The per cent agreement between the two reviewers was calculated by dividing the number of agreements by total number of studies reviewed. The authors reported a per cent agreement of 88%, indicating a high level of agreement between the two reviewers in their screening decision. Any disagreements between the reviewers were resolved through discussion. References of included studies and related articles were hand searched to identify any additional relevant studies. The search for unpublished studies and grey literature was conducted by using Google scholar, Mednar, ProQuest and dissertation databases.
Quality assessment
The methodological quality of eligible articles was appraised independently by two reviewers (HM and PS) using the standardised JBI critical appraisal instrument for studies reporting prevalence data [18] which provides a numerical quality score out of 9 points. A threshold cut-off criterion was set so that studies with quality score of six or less would be excluded. This cut-off was consistent with other published systematic reviews in this area. Disagreements between the reviewers were resolved through discussion. The Preferred Reporting Items for Systematic Reviews and Meta-analyses (PRISMA) guidelines [19] were followed in the reporting of the review.
Data extraction
Two authors (HM and AW) independently conducted the primary data extraction from the included studies using the JBI data extraction tool for prevalence data studies [20] and PS cross-checked for accuracy. Any disagreements and discrepancies between the reviewers were resolved by discussion. The following data from each included study were extracted: authors, year of publication, country, region, study design, population, sample size, sampling methods, outcome measuring tool, mean HRQoL score and quality appraisal score.
Data analysis
The meta-analysis to estimate the pooled mean HRQoL score was performed using the DerSimonian and Laird random-effects model [21]. Heterogeneity was assessed using standard Chi-squared and I-squared tests. Sources of heterogeneity were analysed using subgroup analysis and meta-regression. Publication bias was assessed visually by funnel plot and statistically using Egger test. A leave-one-out sensitivity analysis was also conducted for assessing the influence of each study on the overall effect size estimate. The pooled effect size was presented using a forest plot. All statistical analysis was performed using STATA Version 17.0 (StataCorp, College Station, TX, USA).
Results
Search results
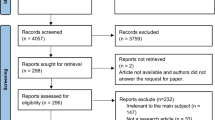
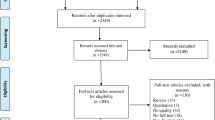
A total of 4249 initial records (4126 from databases and 123 from the grey literature) were retrieved. Of these, 1562 duplicate articles were removed. Then, 2622 articles were excluded after screening titles and abstracts. From the remaining 65 articles, 32 were removed after full-text review and quality appraisal leaving a total of 33 articles that met the inclusion criteria and were subsequently included in this review and meta-analysis (Fig. 1).
Assessment of methodological quality
The methodological quality of included studies was appraised using the JBI critical appraisal checklist. Of the 33 studies, 2 [22, 23] scored the maximum 9 points and 14 [24,25,26,27,28,29,30,31,32,33,34,35,36,37] scored 8 points. The remaining 17 articles [38,39,40,41,42,43,44,45,46,47,48,49,50,51,52,53,54,55] scored 7 points in the checklist (Table 1).
Characteristics of included studies
A total of 33 studies consisting of 5612 participants with HF in LMICs were included in this review. Eight studies [22, 27,28,29,30,31, 45, 55] were conducted in Middle East and North Africa, five studies [37,38,39,40, 42] were conducted in Latin America and the Caribbean, nine studies [23,24,25,26, 32, 33, 41, 51, 54] were conducted in East Asia and Pacific, four studies [34, 35, 43, 47] were conducted in Sub-Saharan Africa, six studies [44, 46, 48, 49, 52, 53] were conducted in Europe and central Asia, and one study [36] was conducted in South Asia. A cross-sectional study design was used in most of the studies (n = 31). The remaining two studies used a prospective cohort study design. Twenty-two studies recruited participants from outpatient departments and eleven recruited participants, while they were inpatients. Sample sizes ranged from 59 to 500 participants, and the majority of studies (n = 21) used consecutive sampling technique. Five different psychometrically validated instruments were used to measure HRQoL: 19 used the Minnesota Living with Heart Failure Questionnaire (MLHFQ), eight used the Short-Form-36 Questionnaire (SF-36), three studies used the WHO Quality of Life-BREF (WHOQOL-BREEF), two used the Kansas City Cardiomyopathy Questionnaire (KCCQ), and one used the Left Ventricular Dysfunction Questionnaire-36 (LVD-36). Mean scores of HRQoL ranged from 13 to 94 (Table 2).
HRQoL of people with HF in LMICs
The overall meta-analysis for the HRQoL score was performed as a subgroup analysis using the QoL measuring instruments across the included studies. The disease-specific tools included MLHFQ, KCCQ and LVD-36, whereas the general tools included SF-36 and WHOQOL-BREF. The overall pooled HRQoL score is presented in Fig. 2.
Health-related quality of life based on MLHFQ
Nineteen (n = 3197) of the 33 studies used the Minnesota Living with Heart Failure Questionnaire (MLHFQ) which is a psychometrically validated disease-specific instrument used to assess HRQoL. The pooled mean MLHFQ score using the random-effects model was 46.08 (95% CI 35.06, 57.10). The meta-analysis found significant heterogeneity across studies (I2 = 98.01%, P < 0.001) (Fig. 3).
Subgroup analysis
The subgroup analysis demonstrated that higher MLHFQ scores were observed among studies with inpatient participants (58.15, 95% CI 39.77, 76.53) and one study from South Asia (94.16, 95% CI 90.30, 98.02) (Fig. 4).
Assessment of heterogeneity and publication bias
The heterogeneity test showed significant (P ≤ 0.001) variation across the MLHFQ -based studies. The meta-regression analysis using publication year, sample size and quality score found none of the three covariates were significantly associated with the presence of heterogeneity (Table 3). The Egger’s test demonstrated no statistically significant publication bias (P = 0.41).
Sensitivity analysis
The leave-one-out sensitivity analysis using a random-effects model revealed that the omission of study 1 (Costa LL, et al., 2020) had a relatively larger influence on the pooled estimate of MLHFQ score compared to other studies. The omission of study 1 caused the overall MLHFQ score to decrease by 2.76, which would make the overall level of HRQoL moderate. This suggests that the results of the meta-analysis may be sensitive to the inclusion or exclusion of this particular study. The effect size displayed for each study corresponds to an overall effect size computed from a meta-analysis excluding that study (Fig. 5).
Health-related quality of life based on SF-36
Of the 33 included studies, eight studies (n = 1250) evaluated the HRQoL using SF-36. The Short-Form-36 (SF-36) Questionnaire is a general, psychometrically validated instrument used to assess HRQoL. In this study, we have used the overall mean SF-36 score as reported in the included paper, whenever available. In cases where the overall score was not provided, we computed the mean SF-36 score by using the Physical Component Summary (PCS) and Mental Component Summary (MCS) scores. To calculate the overall mean QoL score of SF-36 from PCS and MCS, the following formula was used: overall SF-36 score = PCS score + MCS score. Subsequently, the mean SF-36 QoL score was computed as the overall score divided by 2. The pooled mean SF-36 score using the random-effects model was 41.23 (95% CI 36.63, 45.83). The meta-analysis found significant heterogeneity across the SF-36-based studies (I2 = 61.20%, P = 0.01) (Fig. 6).
Subgroup analysis
The subgroup analysis found the highest SF-36 score was in one study (40] from Latin America and Caribbean region (53.10, 95% CI 40.37, 65.83) and studies with inpatient participants (45.20, 95% CI 34.04, 56.35) (Fig. 7).
Assessment of heterogeneity and publication bias
The heterogeneity test showed significant variation (P = 0.01) across SF-36-based studies. Meta-regression analysis using publication year, sample size and quality score found none of the three covariates were significantly associated with the presence of heterogeneity (Table 3). No statistically significant publication bias was detected on Egger’s test (P = 0.99).
Sensitivity analysis
The result of leave-one-out sensitivity analysis using a random-effects model showed that no single study unduly influenced the pooled SF-36 score. For each study, the displayed effect size corresponds to an overall effect size computed from a meta-analysis excluding that study (Fig. 8).
Discussion
Heart failure is a chronic condition with poor prognosis [56]. Health-related quality of life (HRQoL) is an important predictor of poor HF outcomes such as hospitalisation and death [57, 58]. To the best of our knowledge, this is the first systematic review on HRQoL of people with HF in LMICs. This review identified 33 relevant studies that reported the HRQoL of people with HF. Study characteristics such as study area, study participants and outcome measuring instruments varied considerably across the included studies.
Instruments used to quantify the HRQoL varied significantly among the included studies. The MLHFQ, KCCQ and LVD-36 (disease-specific instruments) and SF-36 and WHOQOL-BREEF (generic instruments) were used across the included studies. The most frequently used disease-specific and generic measures were the MLHFQ and the SF-36, respectively. The MLHFQ has 21 questions about how participants feel HF has affected their life over the previous month using a six-point Likert-type scale that ranges from 0 (no effect) to 5 (very much effect). The score ranges from 0 to 105 with the higher scores representing a poorer quality of life [59, 60]. The SF-36 Questionnaire consists of 36 items and eight dimensions that are summarised into the PCS and MCS scores. The scores on all subscales are transformed linearly to a possible range of 0–100 with higher scores represent better HRQoL. The cut-off points for poor HRQoL were: MLHFQ score ≥ 45 and SF-36 score < 60 [61]. It is important to note that these new cut-off points are specific to heart failure patients and may not be applicable to other health condition.
In this review, the pooled mean HRQoL score based on the MLHFQ was 46.08 (95% CI 35.06, 57.10) showing poor HRQoL in people with HF in LMICs. This conclusion differs from a recently published meta-analysis by Moradi M. et al. on a global MLHFQ-based pooled HRQoL score [42] which found a moderate HRQoL [14]. The higher MLHFQ score in the current review could be due to difference in sociodemographic characteristics of the study participants or because the majority of the studies in Moradi M. et al.’s study were conducted in upper-income countries. People with HF in LMICs are generally diagnosed at a later stage and have poor health literacy, less access to HF healthcare services and poorer prognosis than those in upper-income countries [62,63,64]. The pooled mean SF-36 score in this review was 41.23 (95% CI 36.63, 45.83) which suggests that participants in the cohorts had a poor HRQoL. This finding is consistent with previous systematic reviews of the SF-36 tool on other chronic diseases (hypertension and tuberculosis) which revealed poor HRQoL [65, 66]. Based on the result of this review, inpatient participants had higher HRQoL scores than outpatient participants. This is likely due to inpatient participants generally being more acutely unwell than outpatient participants.
This review has several implications for clinical practice. Heart failure has a negative impact on outcomes such as morbidity, mortality and QoL. The key finding in this review was people with HF in LMICs had poor HRQoL, highlighting the greater impact of HF on overall HRQoL scores. This evidence helps health professionals in these countries to consider changing HF care practice and develop strategies to improve the HRQoL of these populations. The finding of a recent systematic review provides evidence that better HRQoL was associated with lower mortality risk [67]. Therefore, healthcare professionals should give clinical priority for assessment of the HRQoL of people with HF during their routine follow-up care to reduce the risk of poor outcomes such as death.
This systematic review involved a systematic search of seven large databases and identified a larger number of studies conducted in LMICs than previous reviews. However, there are some limitations that should be considered. The cut-off date of 2012 was selected arbitrarily to estimate the most recent evidence relevant to current clinical practice today; there may be previous important studies which were not included. The included articles were restricted to the English language, which may have excluded important studies published in other languages. The results of this meta-analysis should be interpreted with caution as it had statistically significant heterogeneity across the included studies which can affect the quality of the evidence and the conclusion of the review. Additionally, several factors that were not examined in this review may confound the HRQoL of these populations.
Conclusion
This systematic review and meta-analysis revealed that people with HF in LMICs had poor HRQoL. These findings provide evidence-based data about the need of improving HRQoL to reduce the risk of morbidity and mortality in these populations. Therefore, early interventions should focus on improving HRQoL to achieve a better prognosis and to enhance the overall experience of living with HF. Large-scale prospective studies are needed to verify these findings and to investigate factors influencing the HRQoL of people with HF.
Availability of data and materials
All the data are available from the corresponding author up on request.
Abbreviations
- HF:
-
Heart failure
- HRQoL:
-
Health-related quality of life
- JBI:
-
Joanna Briggs Institute
- KCCQ:
-
Kansas City Cardiomyopathy Questionnaire
- LMICs:
-
Low- and middle-income countries
- LVD-36:
-
Left Ventricular Dysfunction Questionnaire-36
- MLHFQ:
-
Minnesota Living with Heart Failure Questionnaire
- PRISMA:
-
Preferred Reporting Items for Systematic Reviews and Meta-analyses
- SF-36:
-
Short-Form-36 Questionnaire
- WHOQOL-BREEF:
-
WHO Quality of Life-BREF
References
Bragazzi, N. L., Zhong, W., Shu, J., Abu Much, A., Lotan, D., Grupper, A., et al. (2021). Burden of heart failure and underlying causes in 195 countries and territories from 1990 to 2017. European Journal of Preventive Cardiology, 28(15), 1682–1690.
Reddy, Y. N., Rikhi, A., Obokata, M., Shah, S. J., Lewis, G. D., AbouEzzedine, O. F., et al. (2020). Quality of life in heart failure with preserved ejection fraction: Importance of obesity, functional capacity, and physical inactivity. European Journal of Heart Failure, 22(6), 1009–1018.
Groenewegen, A., Rutten, F. H., Mosterd, A., & Hoes, A. W. (2020). Epidemiology of heart failure. European Journal of Heart Failure, 22(8), 1342–1356.
Lippi, G., & Sanchis-Gomar, F. (2020). Global epidemiology and future trends of heart failure. AME Medical Journal, 5(15), 1–6.
Ruan, Y., Guo, Y., Zheng, Y., Huang, Z., Sun, S., Kowal, P., et al. (2018). Cardiovascular disease (CVD) and associated risk factors among older adults in six low-and middle-income countries: Results from SAGE wave 1. BMC Public Health, 18(1), 1–13.
Guo, L., Guo, X., Chang, Y., Yang, J., Zhang, L., Li, T., et al. (2016). Prevalence and risk factors of heart failure with preserved ejection fraction: A population-based study in Northeast China. International Journal of Environmental Research and Public Health, 13(8), 770.
Karimi, M., & Brazier, J. (2016). Health, health-related quality of life, and quality of life: What is the difference? Pharmacoeconomics, 34(7), 645–649.
Lee, K. S., Lennie, T. A., & Moser, D. K. (2020). Prospective evaluation of association between negative emotions and heart failure symptom severity. Psychology Research and Behavior Management, 13, 1299.
Alpert, C. M., Smith, M. A., Hummel, S. L., & Hummel, E. K. (2017). Symptom burden in heart failure: Assessment, impact on outcomes, and management. Heart Failure Reviews, 22(1), 25–39.
Audi, G., Korologou, A., Koutelekos, I., Vasilopoulos, G., Karakostas, K., Makrygianaki, K., et al. (2017). Factors affecting health related quality of life in hospitalized patients with heart failure. Cardiology Research and Practice, 2017, 4690458.
Agbor, V. N., Ntusi, N. A., & Noubiap, J. J. (2020). An overview of heart failure in low-and middle-income countries. Cardiovascular Diagnosis and Therapy, 10(2), 244.
Long, L., Mordi, I. R., Bridges, C., Sagar, V. A., Davies, E. J., Coats, A. J., et al. (2019). Exercise-based cardiac rehabilitation for adults with heart failure. Cochrane Database of Systematic Reviews. https://doi.org/10.1002/14651858.CD003331
Erceg, P., Despotovic, N., Milosevic, D. P., Soldatovic, I., Mihajlovic, G., Vukcevic, V., et al. (2019). Prognostic value of health-related quality of life in elderly patients hospitalized with heart failure. Clinical Interventions in Aging, 14, 935.
Moradi, M., Daneshi, F., Behzadmehr, R., Rafiemanesh, H., Bouya, S., & Raeisi, M. (2020). Quality of life of chronic heart failure patients: A systematic review and meta-analysis. Heart Failure Reviews, 25(6), 993–1006.
Aromataris, E., Munn, Z. (2020). JBI manual for evidence synthesis. JBI: Adelaide, Australia.
Malik, M., Dawood, Z. S., Janjua, M., Chauhan, S. S. B., & Ladak, L. A. (2021). Health-related quality of life in adults with tetralogy of fallot repair: A systematic review and meta-analysis. Quality of Life Research, 30(10), 2715–2725.
The World Bank. (2022). World development indicators/the world by income and region. https://datatopics.worldbank.org/world-development-indicators/the-world-by-income-and-region.html.
Munn, Z., Moola, S., Lisy, K., Riitano, D., & Tufanaru, C. (2015). Methodological guidance for systematic reviews of observational epidemiological studies reporting prevalence and cumulative incidence data. International Journal of Evidence-Based Healthcare, 13(3), 147–153.
Page, M. J., McKenzie, J. E., Bossuyt, P. M., Boutron, I., Hoffmann, T. C., Mulrow, C. D., et al. (2021). The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. International Journal of Surgery, 88, 105906.
Munn, Z., Moola, S., Lisy, K., Riitano, D., & Tufanaru, C. (2017). Systematic reviews of prevalence and incidence. Joanna Briggs Institute reviewer’s manual Adelaide, South Australia: The Joanna Briggs Institute, 5, 1–5.
Tufanaru, C., Munn, Z., Stephenson, M., & Aromataris, E. (2015). Fixed or random effects meta-analysis? Common methodological issues in systematic reviews of effectiveness. International Journal of Evidence-Based Healthcare, 13(3), 196–207.
Alemoush, R. A., Al-Dweik, G., & AbuRuz, M. E. (2021). The effect of persistent anxiety and depressive symptoms on quality of life among patients with heart failure. Applied Nursing Research, 62, 151503.
Thida, M., Asdornwised, U., Thosingha, O., Dumavibhat, C., & Chansatitporn, N. (2021). Symptom experience, symptom management strategies, and health related quality of life among people with heart failure. Pacific Rim International Journal of Nursing Research, 25(3), 359–374.
Chu, S. H., Lee, W. H., Yoo, J. S., Kim, S. S., Ko, I. S., Oh, E. G., et al. (2014). Factors affecting quality of life in Korean patients with chronic heart failure. Japan Journal of Nursing Science, 11(1), 54–64.
Jeong, Y., Yu, H., & Hwang, B. (2022). Self-care behaviors mediate the impacts of social support and disease knowledge on health-related quality of life in patients with heart failure. Clinical Nursing Research, 31(7), 1308–1315.
Lee, H., Park, G., Lee, K. S., Jin, H., Chun, K.-J., & Kim, J. H. (2020). Knowledge, adherence to lifestyle recommendations, and quality of life among Koreans with heart failure. Journal of Cardiovascular Pharmacology and Therapeutics, 25(4), 324–331.
Alaloul, F., AbuRuz, M. E., Moser, D. K., Hall, L. A., & Al-Sadi, A. (2017). Factors associated with quality of life in Arab patients with heart failure. Scandinavian Journal of Caring Sciences, 31(1), 104–111.
Odeh, Iyad Mahmoud Hassan., Hasan, Tariq Yousef Khaled., & Alhassan, M. A. (2019). Health related quality of life in Jordanian patients with heart failure. Research Journal of Medical Sciences, 13, 53–9.
AbuRuz, M. E. (2018). Anxiety and depression predicted quality of life among patients with heart failure. Journal of Multidisciplinary Healthcare, 11, 367–373.
Asadi, P., Ahmadi, S., Abdi, A., Shareef, O. H., Mohamadyari, T., & Miri, J. (2019). Relationship between self-care behaviors and quality of life in patients with heart failure. Heliyon, 5(9), e02493.
Poorshadan, S., Fallahi, M., Abdi, A., Mahdavikian, S., Miri, J., & Azami, H. (2019). Quality of life and its predictors in hospitalized patients with heart failure at hospitals affiliated to Kermanshah-Iran University of medical sciences. Journal of Cardiovascular Disease Research, 10(1), 16–19.
An, Y., Zhang, Y., Wang, L., Chen, C., & Fan, X. (2022). The relationship between uncertainty in illness and quality of life in patients with heart failure: Multiple mediating effects of perceived stress and coping strategies. Journal of Cardiovascular Nursing, 37(3), 257–265.
Zhang, J., Gilmour, S., Liu, Y., & Ota, E. (2020). Effect of health literacy on quality of life among patients with chronic heart failure in China. Quality of Life Research, 29(2), 453–461.
Molla, S., Yitayal, M., & Amare, G. (2021). Health-related quality of life and associated factors among adult patients with heart failure in Wolaita Zone Governmental Hospitals, Southern Ethiopia. Risk Management and Healthcare Policy, 14, 263.
Tarekegn, G. E., Gezie, L. D., Birhan, T. Y., & Ewnetu, F. (2021). Health-related quality of life among heart failure patients attending an outpatient clinic in the university of Gondar comprehensive specialized hospital Northwest, Ethiopia, 2020: Using structural equation modeling approach. Patient Related Outcome Measures, 12, 279.
Costa, L. L., Islam, M. S., Anowar, M. N., & Latif, M. A. (2020). Quality of life of chronic heart failure patients. Open Journal of Nursing, 10(9), 831–857.
Sousa, MMd., Oliveira, Jd. S., Soares, M. J. G. O., Bezerra, S. MMd. S., Araújo, AAd., & Oliveira, SHd. S. (2017). Association of social and clinical conditions to the quality of life of patients with heart failure. Revista gaucha de enfermagem. https://doi.org/10.1590/1983-1447.2017.02.65885
Paz, LFd. A., Medeiros, Cd. A., Martins, S. M., Bezerra, S. MMd. S., Oliveira, Wd., & Silva, M. B. A. (2019). Quality of life related to health for heart failure patients. Revista brasileira de enfermagem, 72, 140–6.
de Sousa, M. M., dos Santos, O. J., Soares, M. J. G. O., Maria, S., da Silva, B. M., & dos Santos Oliveira, S. H. (2017). Physical and psychosocial effects of heart failure in perceived quality of life. Cogitare Enferm., 22(2), e49783.
Jorge, A. J. L., Rosa, M. L. G., Correia, DMd. S., Martins, Wd. A., Ceron, D. M. M., Coelho, L. C. F., et al. (2017). Evaluation of quality of life in patients with and without heart failure in primary care. Arquivos Brasileiros de Cardiologia, 109, 248–52.
Wang, G., & Yang, Q. (2020). Factors associated with health-related quality of life in Chinese patients with heart failure: A cross-sectional study. Collegian, 27(5), 512–520.
Afsharipour, Z., Khademiyeh, M., Arab, M., & Soltani-Nezhad, N. (2016). Evaluating the quality of life in hospitalized patients with heart failure at hospitals affiliated to Kerman University of medical sciences, Iran, during 2012. Nursing Practice Today, 3(2), 51–56.
Seid, M. A. (2020). Health-related quality of life and extent of self-care practice among heart failure patients in Ethiopia. Health and Quality of Life Outcomes, 18(1), 1–7.
DeWolfe, A., Gogichaishvili, I., Nozadze, N., Tamariz, L., Quevedo, H. C., Julian, E., et al. (2012). Depression and quality of life among heart failure patients in Georgia, Eastern Europe. Congestive Heart Failure, 18(2), 107–111.
Borumandpour, M., Valizadeh, G., Dehghan, A., Pourmarjani, A., & Ahmadifar, M. (2016). Application of WHOQOL-BREF for the evaluation of the quality of life in elderly patients with heart failure. Bioscience Biotechnology Research Communications, 9(4), 878–883.
Ahmeti, A., Ibrahimi, P., Bytyci, I., Haliti, E., Olloni, R., Elezi, S., et al. (2016). Use of the “Minnesota living with heart failure questionnaire” quality of life questionnaire in Kosovo’s heart failure patients. International Cardiovascular Forum Journal, 9
Mbakwem, A., Aina, F., Amadi, C., Akinbode, A., Mokwunyei, J. (2013). Comparative analysis of the quality of life of heart failure patients in South Western Nigeria
Erceg, P., Despotovic, N., Milosevic, D. P., Soldatovic, I., Zdravkovic, S., Tomic, S., et al. (2013). Health-related quality of life in elderly patients hospitalized with chronic heart failure. Clinical Interventions in Aging, 8, 1539–1546.
Jovanić, M., Zdravković, M., Stanisavljević, D., & Jović, V. A. (2018). Exploring the importance of health literacy for the quality of life in patients with heart failure. International Journal of Environmental Research and Public Health, 15(8), 1761.
Tsabedze, N., Kinsey, J. L. H., Mpanya, D., Mogashoa, V., Klug, E., & Manga, P. (2021). The prevalence of depression, stress and anxiety symptoms in patients with chronic heart failure. International Journal of Mental Health Systems, 15(1), 44.
Son, Y.-J., Song, Y., Nam, S., Shin, W.-Y., Lee, S.-J., & Jin, D.-K. (2012). Factors associated with health-related quality of life in elderly Korean patients with heart failure. Journal of Cardiovascular Nursing, 27(6), 528–538.
Barutcu, C. D., & Mert, H. (2013). The relationship between social support and quality of life in patients with heart failure. JPMA the Journal of the Pakistan Medical Association, 63(4), 463–467.
Gok Metin, Z., & Gulbahar, M. (2021). The prevalence of complementary and integrative health approach use and quality of life among patients with heart failure: A cross-sectional, descriptive, and comparative study. Holistic Nursing Practice, 35(3), 123–132.
Silavanich, V., Nathisuwan, S., Phrommintikul, A., & Permsuwan, U. (2019). Relationship of medication adherence and quality of life among heart failure patients. Heart and Lung, 48(2), 105–110.
Molavynejad, S., Babazadeh, M., Zarea, K., & Ataeeara, S. (2019). Anxiety, depression and quality of life among patients with heart failure. Journal of Research in Medical and Dental Science, 7(3), 69–77.
Wu, J.-R., Lennie, T. A., Frazier, S. K., & Moser, D. K. (2016). Health-related quality of life, functional status and cardiac event-free survival in patients with heart failure. The Journal of Cardiovascular Nursing, 31(3), 236.
Ramos, S., Prata, J., Rocha-Gonçalves, F., Bettencourt, P., & Coelho, R. (2017). Quality of life predicts survival and hospitalisation in a heart failure Portuguese population. Applied Research in Quality of Life, 12(1), 35–48.
Johansson, I., Joseph, P., Balasubramanian, K., McMurray, J. J., Lund, L. H., Ezekowitz, J. A., et al. (2021). Health-related quality of life and mortality in heart failure: The global congestive heart failure study of 23,000 patients from 40 countries. Circulation, 143(22), 2129–2142.
Rector, T. S. (2017). FDA medical device development tool (MDDT) qualification package for the Minnesota living with heart failure questionnaire (MLHFQ), 2017
Audi, G., Korologou, A., Koutelekos, I., Vasilopoulos, G., Karakostas, K., Makrygianaki, K., et al. (2017). Factors affecting health related quality of life in hospitalized patients with heart failure. Cardiology Research and Practice, 2017
Hsu, T. W., Chang, H. C., Huang, C. H., Chou, M. C., Yu, Y. T., & Lin, L. Y. (2018). Identifying cut-off scores for interpretation of the heart failure impact questionnaire. Nursing Open, 5(4), 575–582.
Curry, C., Zuhlke, L., Mocumbi, A., & Kennedy, N. (2018). Acquired heart disease in low-income and middle-income countries. Archives of disease in Childhood, 103(1), 73–77.
Nugent, R. (2008). Chronic diseases in developing countries: Health and economic burdens. Annals of the New York Academy of Sciences, 1136(1), 70–79.
Negesa, L. B., Magarey, J., Rasmussen, P., & Hendriks, J. M. (2019). Cardiovascular risk behaviour is an emerging health issue in developing countries: A cross-sectional study. European Journal of Cardiovascular Nursing, 18(8), 679–690.
Trevisol, D. J., Moreira, L. B., Kerkhoff, A., Fuchs, S. C., & Fuchs, F. D. (2011). Health-related quality of life and hypertension: A systematic review and meta-analysis of observational studies. Journal of Hypertension, 29(2), 179–188.
Guo, N., Marra, F., & Marra, C. A. (2009). Measuring health-related quality of life in tuberculosis: A systematic review. Health and Quality of Life Outcomes, 7(1), 14.
Phyo, A. Z. Z., Freak-Poli, R., Craig, H., Gasevic, D., Stocks, N. P., Gonzalez-Chica, D. A., et al. (2020). Quality of life and mortality in the general population: A systematic review and meta-analysis. BMC Public Health, 20(1), 1–20.
Acknowledgements
We would like to thank UTS Faculty of Health librarian and all authors of the included studies in this systematic review and meta-analysis.
Funding
There was no funding for this systematic review. It is part of a PhD thesis by HM. HM is a higher degree research candidate at the University of Technology Sydney (UTS), funded by the International Research Training Program (IRTP). The IRTP is a commonwealth scholarship funded by the Australian government and the Department of Education and Training. The funders had no role in study design, data collection and analysis, decision to publish or preparation of the manuscript.
Author information
Authors and Affiliations
Contributions
HM conceived the study and drafted the protocol. PS and AW provided support and guidance on the search strategy and screening process. All three authors (HM, PS and AW) were involved in data extraction, quality assessment and analysis. All authors have read, edited and approved the final draft of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors report no competing interests.
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mulugeta, H., Sinclair, P.M. & Wilson, A. Health-related quality of life of people with heart failure in low- and middle-income countries: a systematic review and meta-analysis. Qual Life Res 33, 1175–1189 (2024). https://doi.org/10.1007/s11136-023-03563-2
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-023-03563-2