Abstract
Previous studies have demonstrated that the red nucleus (RN) is involved in the regulation of neuropathic pain and plays both facilitated and inhibitory roles through different cytokines. Here, we aim to investigate the expression changes and roles of interleukin-6 (IL-6), a pleiotropic cytokine, as well as its receptor (IL-6R) in the RN of rats with neuropathic pain induced by spared nerve injury (SNI). Immunohistochemistry indicated that IL-6 and IL-6R were weakly expressed in the RN of normal rats, and were mainly co-localized with neurons and oligodendrocytes. Following SNI, the expression levels of IL-6 and IL-6R in the RN did not show obvious changes at 1 week and 2 weeks postinjury. However, both of them were significantly increased in the RN contralateral (but not ipsilateral) to the nerve ligation side at 3 weeks postinjury, and co-localized not only with neurons and oligodendrocytes, but also with numerous astrocytes. Injection of different doses of anti-IL-6 antibody (100, 250, 500 ng) into the RN contralateral to the nerve ligation side at 3 weeks postinjury dose-dependently increased the paw withdrawal threshold (PWT) of rats and alleviated SNI-induced mechanical allodynia. Conversely, injection of different doses of recombinant rat IL-6 (5.0, 10, 20 ng) into the unilateral RN of normal rats dose-dependently decreased the PWT of contralateral (but not ipsilateral) hind paw and evoked significant mechanical allodynia, which was similar to SNI-induced neuropathic allodynia. These results further support the conclusion that the RN is involved in the modulation of neuropathic pain, and suggest that IL-6 and IL-6R in the RN play a facilitated role in the later maintenance of SNI-induced neuropathic pain.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The red nucleus (RN), an important nucleus of the extrapyramidal tract, plays an important role in motor control. It is involved in modulating muscle tension, motor learning, triggering conditioned motor responses, postural corrections, and the recovery of movement after spinal injury [1–5]. The RN neurons in the intact and decerebrate cat show phasic discharge in the swing phase of locomotion, during which they influence the activity of flexor muscles [4]. Unilateral lesions of the RN in rats produce a characteristic asymmetry in which abnormal braking and propulsive forces are induced during locomotion [1]. Furthermore, chemical or electrical stimulation of the RN promotes the low-threshold afferent-evoked jaw-opening reflex (JOR), but inhibits the high-threshold afferent-evoked JOR, implying the important role of the RN in the control of jaw movements [6].
In recent years, accumulating evidence has shown that the RN is also involved in nociceptive processing and the modulation of pathological pain. Spontaneous discharges have been recorded in RN neurons in normal rats, and the discharge frequency in most neurons is altered by nociceptive stimulation of the peripheral nerve or limbs [7, 8]. Injection of glutamic acid into the RN can increase the tail flick latency of normal rats, and this effect is blocked by lidocaine injected into the nucleus raphe magnus [9]. Our recent studies indicate that the expression levels of pro-inflammatory cytokines, including interleukin-1β (IL-1β) and tumor necrosis factor-alpha (TNF-α), are significantly increased in the RN of rats with spared nerve injury (SNI), and blockade with corresponding antibodies could alleviate SNI-induced mechanical allodynia [10, 11]. Repeated injection of recombinant rat TNF-α into the RN of normal rats evokes a significant mechanical allodynia [12]. Further studies demonstrate that IL-10, an anti-inflammatory cytokine, is also increased in the RN of rats with SNI, and injection of recombinant rat IL-10 into the RN alleviates SNI-induced mechanical allodynia [13]. On the contrary, transforming growth factor-β (TGF-β), another anti-inflammatory cytokine, is significantly decreased after SNI although it is highly expressed in the RN of normal rats and has antinociceptive effects [14]. These findings indicate that the RN takes part in the modulation of pain and plays both facilitated and inhibitory roles by different neurotransmitters and cytokines.
IL-6, a pleiotropic cytokine, plays multiple roles in the central nervous system including neuronal differentiation, neuronal survival and neuroprotection [15, 16]. The biological effects of IL-6 are transmitted through a combination with specific membrane-anchored IL-6R that associates with gp130, a transmembrane subunit necessary to activate IL-6 intracellular signaling. IL-6 can act via soluble IL-6R that is produced by the limited proteolysis of the membrane-anchored IL-6R or by the alternative splicing of IL-6R mRNA [17]. Recent studies imply that IL-6 is also involved in nociceptive processing and the regulation of pathological pain [18–28]. However, the expressions and roles of IL-6 in the RN under normal and neuropathic pain conditions are still unknown. Thus, the aim of this study was to explore the expression patterns of IL-6 and its receptor (IL-6R) in the RN and also their biological roles in the development of SNI-induced neuropathic pain.
Materials and Methods
Animals
A total of 74 adult male Sprague–Dawley rats (200–230 g) were used for the study, all of which were provided by the Experimental Animal Center of Shaanxi Province, China. All animals were housed with ad libitum access to food and water and maintained on a 12 /12 h light/dark cycle (lights on at 07:00 h). The experiments were approved by the institutional Animal Care Committee of Xi’an Jiaotong University and carried out in accordance with the ethical guidelines of the International Association for the Study of Pain [29].
Spared Nerve Injury
After rats were anesthetized with sodium pentobarbital (50 mg/kg, i.p.), three terminal branches of the right sciatic nerve were isolated. The common peroneal and tibial nerves were tightly ligated with 5–0 silk sutures and sectioned distal to the ligation, removing 2–4 mm of the distal nerve stump [30]. In the sham-operated rats, three terminal branches of sciatic nerve were exposed but not lesioned. Utmost care was taken to avoid damaging the sural nerve in the process of establishing SNI rats since any stretching or injury of sural nerve would decrease the sensory sensitivity of SNI rats [30]. To exclude rats with damage of the sural nerve, only rats with a 50 % withdrawal threshold lower than 4.0 g (≈80 %) in the right hind paw were used in these studies.
Immunohistochemistry
Following SNI, rats in different groups (four rats/group) were anesthetized with sodium pentobarbital (50 mg/kg, i.p.) and transcardially perfused with saline followed by Bouin’s fixation fluid [14]. The brain tissues containing the RN were harvested and postfixed in the same fixative for 1 day, and then dehydrated by 30 % sucrose. Each brain tissue was embedded in optimal cutting temperature (OCT) compound, and cut into 10 µm-thick coronal sections using a freezing microtome. Three sections (one section from 100 µm) were picked from each rat and used for the following experiment.
After treatments with ice acetone, 3 % H2O2 and goat serum blocking solution, all of the sections were incubated with rabbit anti-rat IL-6 antibody (1:800; Abcam) or anti-rat IL-6R antibody (1:250; Beijing Biosynthesis Biotechnology Co., Ltd., China) overnight at 4 °C. Sections were then incubated for 30 min with horseradish peroxidase (HRP)-labeled goat anti-rabbit immunoglobulin G (IgG), and subsequently reacted with DAB for color development. Negative controls in which the primary antibody was omitted or preadsorbed with soluble IL-6 (200 ng/μl; Sigma) were performed to confirm immunospecificity. Olympus BX51 microscope and DP71 camera were used to view histological sections and capture the images. Using Image J software (National Institute of Health, Bethesda, MA, USA), IL-6 and IL-6R immunoreactivity (IR) were quantified by an experimenter blinded to the treatment group. Briefly, digital images from each rat were opened using Image J and converted to eight-bit grayscale, allowing the computer to distinguish between areas of immunoreactivity and background. Following a standardized elimination of background through adjusting the threshold, the RN area was selected and the mean optical density (MOD) and area ratio of IL-6- and IL-6R-positive cells (area of positive signal/area of region of interest) were measured to reflect the intensity of IR and the number of positive cells, respectively (http://rsb.info.nih.gov/ij/).
Immunofluorescence Staining
Three weeks after SNI, rats in different groups (three rats/group) were deeply anesthetized with a lethal dose of sodium pentobarbital (70 mg/kg, i.p.) followed by heart bloodletting. The brain tissues containing the RN were rapidly removed and freshly freezed at −80 °C after embedded in OCT. Each brain tissue was cut into 10 µm-thick coronal sections using a freezing microtome.
After treatments with acetone and goat serum blocking solution, all of the sections were incubated with the primary antibodies of rabbit anti-rat IL-6 antibody (1:400; Abcam) or anti-rat IL-6R antibody (1:200; Beijing Biosynthesis Biotechnology Co., Ltd., China) mixed with mouse anti-rat NeuN (1:1000; Abcam; marker of neuron), mouse anti-rat O4 (1:250; Abcam; marker of oligodendrocyte), mouse anti-rat glial fibrillary acidic protein (GFAP) (1:250; Sigma; marker of astrocyte), or mouse anti-rat OX42 (1:100; Millipore, USA.; marker of microglia) overnight at 4 °C, then followed by 1 h incubation with secondary antibodies, including FITC-conjugated goat anti-mouse IgG antibody (1:250; Abcam; green fluorescence) and Cy3-conjugated goat anti-rabbit IgG antibody (1:2500; Abcam; red fluorescence) at room temperature. The cell nucleus was counterstained with 4′,6-diamidino-2-phenylindole (DAPI).
Catheterization and Drug Administration
After rats were anesthetized with sodium pentobarbital (50 mg/kg, i.p.), the rat skull was exposed, and a stainless steel guide cannula (0.8 mm in diameter) was implanted at a position 2.0 mm dorsal to the left RN at the following coordinates: 5.2–6.7 mm from the bregma, 0.6–1.4 mm lateral, 4.4–5.4 mm below the cortical surface [14]. The guide cannula was fixed on the skull with four microscrews and dental cement. A stainless steel plug was inserted into the guide cannula, and kept in place until intracerebral injection. After catheterization, each rat was injected intraperitoneally with 0.2 million units penicillin per day for three consecutive days.
One week after catheterization, rats were lightly anesthetized with Enflurane (Baxter Caribe Inc., Guayama, Puerto Rico, USA) and maintained for 2 min, and a 1.0 μl microsyringe with its tip extending 2.0 mm beyond the end of the guide cannula was used for the injection of drugs (0.5 μl). Drugs used during this study, including rabbit anti-rat IL-6 antibody (anti-IL-6-Ab; Abcam) and recombinant rat IL-6 (Sigma), were diluted with normal saline and slowly infused into the RN within 60 s. To prevent the backflow of drug solution, microsyringe was left in place for an additional 30 s. Anti-IL-6-Ab (100, 250, 500 ng) was injected into the RN of SNI rats at 3 weeks postinjury, while recombinant rat IL-6 (5.0, 10, 20 ng) was injected into the RN of normal rats. The same volume of normal saline or normal rabbit IgG was injected as vehicle control. At the end of experiments, the injection sites were histologically verified to be within the RN using toluidine blue (0.1 %) staining.
Behavioral Testing
All of the rats were habituated in the experimental arena for 20 min daily at least 3 days before the formal test. The paw withdrawal threshold (PWT) of rat was measured blindedly by an experimenter before and after drug administration by using the up-down method [31]. Briefly, the rat was put under a transparent plastic chamber (28 × 25 × 21 cm) placed on a metal wire mesh floor, and ten von Frey filaments ranging from 0.4 to 15.0 g (Stoelting Company, USA) were used to stimulate the lateral surface of the hind paw (sural nerve skin area). The pattern of negative and positive responses was converted into a 50 % PWT. In the cases where continuous negative or positive responses were observed all the way to the end of the stimulus range, a value of 15.0 or 0.25 g was appointed, respectively.
Data Analysis
All results were presented as Mean ± SEM. Pearson’s correlation analysis was used to assess the correlation between the effects and doses of drug. One-way analysis of variance (ANOVA) was used to analyze the differences in the MOD and area ratio of positive cells. Two-way repeated measures of ANOVA (two-way RM ANOVA) was used to test the differences in drug effect among groups. Logarithmic transformed values were used for the statistical analysis, enabling ANOVA tests. For all comparisons P < 0.05 was considered significant.
Results
General
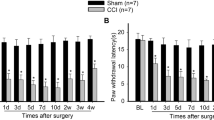
After SNI, the PWT on the nerve ligation side (but not intact side) dropped from a baseline value of 13.35 ± 0.41 g (before surgery, n = 12) to 2.48 ± 0.27 g (1 week postinjury; t = 19.53, P < 0.001). At 2 weeks and 3 weeks postinjury, the PWT were extremely low, respectively reaching 1.96 ± 0.23 g and 1.95 ± 0.19 g (t = 30.26, t = 31.32; P < 0.001). During the whole test period, no significant changes of PWT were observed in sham-operated rats compared with the baseline value (12.62 ± 0.75 g) (P > 0.05), the PWTs were 12.03 ± 0.62 g for 1 week, 12.56 ± 0.53 g for 2 weeks and 12.74 ± 0.38 g for 3 weeks postinjury, respectively.
Expressions of IL-6 and IL-6R in the RN of Normal and SNI Rats
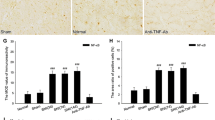
Immunohistochemistry demonstrated a low-level expression of IL-6 in the RN of normal (Fig. 1a) and sham-operated rats (Fig. 1b). Following SNI, IL-6 immunoreactivity (IR) did not show significant differences in the RN of rats at 1 week (Fig. 1c) and 2 weeks postinjury (Fig. 1d), while was markedly up-regulated in the RN contralateral but not ipsilateral to the nerve ligation side at 3 weeks postinjury (Fig. 1e, f) compared with normal and sham-operated rats. Consistent with the expression of IL-6, IL-6R IR was also seen in the RN of normal (Fig. 1g) and sham-operated rats (Fig. 1h), and did not show obvious changes at 1 week (Fig. 1i) and 2 weeks after SNI (Fig. 1j). However, IL-6R IR did increase in the RN contralateral, but not ipsilateral to the nerve ligation side at 3 weeks after SNI (Fig. 1k, l). No immunoreactivity was observed after the primary antibodies were omitted (Fig. 1m, n) or anti-IL-6-Ab was preadsorbed with soluble IL-6 (Fig. 1o), suggesting that the IL-6 IR and IL-6R IR in the RN were specific. Quantitative analysis of immunoreactivity indicated that both the MOD and the area ratio of IL-6- and IL-6R-positive cells were significantly (t = 15.44, P < 0.001; t = 13.30; P < 0.001) enhanced in the RN at 3 weeks (but not 1 and 2 weeks) after SNI compared with sham-operated rats (Fig. 2a, b). Neither IL-6 IR nor IL-6R IR showed difference between normal and sham-operated rats (P = 0.76; P = 0.74). These results imply that IL-6 and IL-6R in the RN perhaps take part in the modulation of pain, and contribute to the later maintenance of SNI-induced neuropathic pain.
Expressions of IL-6 and IL-6R in the RN of normal and SNI rats. a, b IL-6 IR in the RN of normal rats (a) and sham-operated rats (b). c–e IL-6 IR in the RN contralateral to the nerve ligation side at 1 week (c), 2 weeks (d) and 3 weeks (e) after SNI. f IL-6 IR in the RN contralateral and ipsilateral to the nerve ligation side at 3 weeks after SNI. g, h IL-6R IR in the RN of normal rats (g) and sham-operated rats (h). i–k IL-6R IR in the RN contralateral to the nerve ligation side at 1 week (i), 2 weeks (j) and 3 weeks (k) after SNI. l IL-6R IR in the RN contralateral and ipsilateral to the nerve ligation side at 3 weeks after SNI. m–o Negative controls in which the primary antibodies were omitted (m and n) or anti-IL-6-Ab was preadsorbed with soluble IL-6 (o). Scale bars 100 µm
Distributions of IL-6 and IL-6R in the RN of Normal and SNI Rats
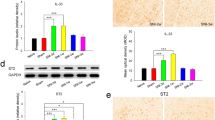
Immunofluorescence staining demonstrated that IL-6 IR and IL-6R IR in the RN of normal rats were mainly co-localized with neurons (Fig. 3a, i) and oligodendrocytes (Fig. 3b, j), while were hardly observed in astrocytes (Fig. 3c, k) and microglia (Fig. 3d, l). At 3 weeks after SNI, both IL-6 IR and IL-6R IR in the RN contralateral to the nerve ligation side were obviously up-regulated in neurons and glia, and co-localized not only with neurons (Fig. 3e, m) and oligodendrocytes (Fig. 3f, n), but also with numerous astrocytes (Fig. 3g, o). Neither IL-6 nor IL-6R was detected in the RN microglia under neuropathic pain condition (Fig. 3h, p). The percentages of IL-6- and IL-6R-positive neurons and glial cells in the RN of normal and SNI rats were shown in Table 1. These results imply that RN neurons, oligodendrocytes and astrocytes maybe contribute to the later maintenance of SNI-induced neuropathic pain through expressing IL-6 and IL-6R.
Co-localization of cell specific markers (green) and IL-6 or IL-6R (red) in the RN of normal and SNI rats. a–d IL-6 IR in the RN of normal rats was co-localized with neurons (a) and oligodendrocytes (b) (yellow), while was hardly observed in astrocytes (c) and microglia (d). e–h At 3 weeks after SNI, increased IL-6 IR was co-localized with the RN neurons (e), oligodendrocytes (f) and astrocytes (g) but not microglia (h). i–l IL-6R IR in the RN of normal rats was co-localized with neurons (i) and oligodendrocytes (j) (yellow), while was hardly observed in astrocytes (k) and microglia (l). m–p At 3 weeks after SNI, increased IL-6R IR was co-localized with the RN neurons (m), oligodendrocytes (n) and astrocytes (o) but not microglia (p). NeuN, marker of neuron; O4, marker of oligodendrocyte; GFAP, marker of astrocyte; OX42, marker of microglia. Scale bars 50 µm (Color figure online)
IL-6 in the RN Facilitated the Neuropathic Pain Induced by SNI
To further investigate the roles of the RN IL-6 in the maintenance of SNI-induced neuropathic pain, different doses (100, 250, 500 ng) of anti-IL-6-Ab were injected into the RN contralateral to the nerve ligation side at 3 weeks after SNI, and the mechanical PWT were dynamically measured. As shown in Fig. 4c, injection of different doses of anti-IL-6-Ab into the RN dose-dependently (Pearson’s analysis; r = 0.988, P = 0.01) increased the PWT of hind paw ipsilateral to the nerve ligation side and alleviated SNI-induced mechanical allodynia. The mean PWTs during the 120 min (15–135 min) observation period were 1.83 ± 0.07 g (n = 6) for vehicle control, 2.13 ± 0.14 g (n = 6) for 100 ng of anti-IL-6-Ab, 3.85 ± 0.24 g (n = 6) for 250 ng of anti-IL-6-Ab, and 5.21 ± 0.39 g (n = 6) for 500 ng of anti-IL-6-Ab, respectively. Further analysis indicated that 250 and 500 ng of anti-IL-6-Ab injected into the RN both significantly increased the mechanical PWT of SNI rats (t = 6.04, P < 0.001; t = 10.10, P < 0.001), the peak analgesic effects appeared at 75 min and thereafter gradually reduced to the baseline at 135 min. However, 100 ng of anti-IL-6-Ab did not show significant anti-allodynic effect (t = 1.16, P = 1.00) compared with vehicle group although a short anti-allodynic effect was observed at 45 min. In contrast, injection of different doses (5.0, 10, 20 ng) of recombinant rat IL-6 into the RN of normal rats dose-dependently (Pearson’s analysis; r = −0.955, P = 0.04) decreased the PWT of contralateral hind paw and induced a unilateral mechanical allodynia (Fig. 4d). The mean PWTs during the 75 min (15–90 min) observation period were 12.61 ± 0.17 g (n = 6) for vehicle control, 12.37 ± 0.23 g (n = 6) for 5.0 ng of IL-6, 10.50 ± 0.35 g (n = 6) for 10 ng of IL-6, and 9.54 ± 0.55 g (n = 6) for 20 ng of IL-6, respectively. Further analysis indicated that 10 and 20 ng of IL-6 injected into the RN both significantly decreased the PWT of normal rats (t = 3.47, P = 0.02; t = 5.04, P < 0.001), the peak algesic effect appeared at 45 min and then gradually recovered to the baseline at 90 min. Whereas, 5.0 ng of IL-6 did not show any effect compared with vehicle control (t = 0.38, P = 1.00). Injection of vehicle controls into the RN did not change the PWTs of normal and SNI rats (t = 0.32, P = 1.00; t = 0.61; P = 1.00). During the whole test period, no obvious changes were observed in motor behaviors after injection of anti-IL-6-Ab into the RN of SNI rats or IL-6 into the RN of normal rats. These results demonstrate that IL-6 in the RN is involved in nociceptive processing and plays a facilitated role in the maintenance of SNI-induced neuropathic pain.
The effects of anti-IL-6 antibody (anti-IL-6-Ab) and recombinant IL-6 injected respectively into the RN of SNI rats and normal rats. a A schematic picture showing the injection site in the RN. b A photograph indicating the actual injection site in the RN (stained with toluidine blue). c Injection of different doses (100, 250, 500 ng) of anti-IL-6-Ab into the RN at 3 weeks after SNI dose-dependently (Pearson’s analysis; r = 0.988, P = 0.01) increased the PWT of hind paw ipsilateral to the nerve ligation side and alleviated mechanical allodynia induced by SNI. d Injection of different doses (5.0, 10, 20 ng) of IL-6 into the RN of normal rats dose-dependently (Pearson’s analysis; r = −0.955, P = 0.04) decreased the PWT of contralateral hind paw and induced a unilateral mechanical allodynia. Aq aqueduct, DpMe deep mesencephalic nucleus, PAG periaqueductal gray, RN red nucleus. *P < 0.05, **P < 0.01 and ***P < 0.001, compared with vehicle group at those time points (two-way RM ANOVA). Scale bars 500 µm (Color figure online)
Discussion
IL-6 is a multifunctional cytokine and plays various roles in different tissue systems, depending on the target cell and cell conditions. Numerous studies have shown that IL-6 and IL-6R are detected in the peripheral nerve, dorsal root ganglia (DRG), spinal cord and various brain areas under physiological condition, and distributed in neurons and also glial cells [18–28, 32, 33]. In the central nervous system, IL-6 is involved in the development, differentiation, survival, regeneration and degeneration of neurons [15, 16]. Recent studies show that IL-6 is also involved in nociceptive processing and the regulation of pathological pain [23]. In patients with chronic pain, an elevated IL-6 has been observed in the cerebrospinal fluid in patients with lumbar radicular pain or complex regional pain syndrome [34, 35]. In animal pain models, an increased level of IL-6 is detected in the injured nerve, DRG, spinal cord and also various brain areas [18–28, 36]. In accordance with these results, we demonstrate that IL-6 and IL-6R are weakly expressed in the RN of normal rats and significantly increased in the RN of rats at 3 weeks after SNI. However, different from our previous reports that TNF-α and IL-1β are significantly increased in the RN at 2 weeks after SNI [10, 11], the rise time of IL-6 is later than those of TNF-α and IL-1β. These results imply that the RN IL-6 and IL-6R maybe participate only in the later maintenance (but not early initiation) of SNI-induced neuropathic pain, and the increase of the RN IL-6 is perhaps not directly caused by SNI, but may be secondary to up-regulation of TNF-α and/or IL-1β. Further experimentation is required to clarify the production mechanisms of IL-6 in the RN of rats with SNI. In addition, our data indicate that IL-6 and IL-6R in the RN are co-localized mainly with neurons and oligodendrocytes in normal rats, while co-localized not only with neurons and oligodendrocytes but also with numerous astrocytes in SNI rats, suggesting that RN neurons, oligodendrocytes and astrocytes maybe contribute to the later maintenance of SNI-induced neuropathic pain through expressing IL-6 and IL-6R.
Further studies suggest that IL-6 is a relevant mediator of nociception. Intraplantar, intrathecal or intracerebroventricular administration of IL-6 induces pain hypersensitivity in normal animals, and increases the pain-related behaviors in rats with nerve injury [37–41]. In contrast, genetic deletion of IL-6 shows a reduced sensitivity to mechanical and thermal stimuli [42, 43]. Intraplantar, perineural or intrathecal administration of neutralizing anti-IL-6 antibody significantly inhibits the development of pain-related behaviors induced by inflammation or nerve injury [24, 37, 41, 44–46]. In the present study, we further investigate the regulatory roles of the RN IL-6 in the development of neuropathic pain through injection of anti-IL-6-Ab into the RN of SNI rats and recombinant rat IL-6 into the RN of normal rats. Consistent with previous reports, our data indicate that different doses of anti-IL-6-Ab injected into the RN of rats with SNI dose-dependently increase the mechanical PWT and significantly alleviate SNI-induced neuropathic allodynia, while different doses of IL-6 injected into the RN of normal rats dose-dependently decrease the mechanical PWT and evoke significant mechanical allodynia, which is similar to SNI-induced neuropathic allodynia. These results strongly suggest that IL-6 in the RN is involved in nociceptive processing and plays a facilitated role in the later maintenance of SNI-induced neuropathic pain. Although the analgesic effect of anti-IL-6-Ab we used in the present study lasts only 90 min, this result still recommends that inhibition of IL-6 will be an effective treatment for neuropathic pain since an anti-IL-6 receptor monoclonal antibody, tocilizumab, has been clinically proved to be effective on sciatica [47]. However, some opposite results have also been reported that intraplantar or intrathecal administration of IL-6 produces an antinociceptive effect in pathological pain models, but has little or no effect in normal animals [48–50]. These discrepancies may result from different drug doses, injection sites, behavioral tests, animal models and species.
How could IL-6 in the RN contribute to the development of neuropathic pain following SNI? A previous study has reported that IL-6 enhances the excitability of dural afferents through the modulation of sodium channels, which plays a crucial role in the development of neuropathic pain by sequentially leading to the central sensitization [51]. IL-6 can up-regulate the expressions of transient receptor potential vanilloid channel type 1 (TRPV1) in DRG neurons, and contributes to the sensitization of DRG neurons and the development of bone cancer pain [52]. Moreover, a recent study has demonstrated that IL-6 can suppress GABA- and glycine-induced currents, which decreases inhibitory synaptic transmission in superficial dorsal horn neurons, suggesting an opposing increased excitatory synaptic transmission [53]. These results imply that IL-6 in various tissues may be involved in pain regulation through different pathways. However, whether these pathways are involved in the ability of IL-6 to sensitize RN neurons and mediate neuropathic pain needs to be further explored.
Collectively, this study demonstrates that IL-6 and IL-6R are weakly expressed in the RN of normal rats and up-regulated after SNI. RN neurons, oligodendrocytes and astrocytes contribute to the up-regulations of IL-6 and IL-6R under neuropathic pain condition. IL-6 and IL-6R in the RN play a facilitated role in the later maintenance of SNI-induced neuropathic pain. Targeting IL-6 and/or its receptor system may present a new and efficient way to treat neuropathic pain symptoms.
References
Muir GD, Whishaw IQ (2000) Red nucleus lesions impair overground locomotion in rats: a kinetic analysis. Eur J Neurosci 12:1113–1122
Basso DM, Beattie MS, Bresnahan JC (2002) Descending systems contributing to locomotor recovery after mild or moderate spinal cord injury in rats: experimental evidence and a review of literature. Restor Neurol Neurosci 20:189–218
Küchler M, Fouad K, Weinmann O, Schwab ME, Raineteau O (2002) Red nucleus projections to distinct motor neuron pools in the rat spinal cord. J Comp Neurol 448:349–359
Lavoie S, Drew T (2002) Discharge characteristics of neurons in the red nucleus during voluntary gait modifications: a comparison with the motor cortex. J Neurophysiol 88:1791–1814
Zelenin PV, Beloozerova IN, Sirota MG, Orlovsky GN, Deliagina TG (2010) Activity of red nucleus neurons in the cat during postural corrections. J Neurosci 30:14533–14542
Satoh Y, Yajima E, Ishizuka K, Nagamine Y, Iwasaki S (2013) Modulation of two types of jaw-opening reflex by stimulation of the red nucleus. Brain Res Bull 97:24–31
Huang M, Liu M, Li X (1992) The analgesic effect of red nucleus and preliminary research on its mechanism. Zhen Ci Yan Jiu 17:166–170
Steffens H, Rathelot JA, Padel Y (2000) Effects of noxious skin heating on spontaneous cell activity in the magnocellular red nucleus of the cat. Exp Brain Res 131:215–224
Liu M, Liu X, Liu B (1991) The analgesic effect of red nucleus and strengthening effect thereof to the acupuncture analgesia. Zhen Ci Yan Jiu 16:48–53
Li X, Wang J, Wang Z, Dong C, Dong X, Jing Y, Yuan Y, Fan G (2008) Tumor necrosis factor-α of red nucleus involved in the development of neuropathic allodynia. Brain Res Bull 77:233–236
Wang Z, Wang J, Li X, Yuan Y, Fan G (2008) Interleukin-1 beta of red nucleus involved in the development of allodynia in spared nerve injury rats. Exp Brain Res 188:379–384
Zhang Q, Wang J, Duan MT, Han SP, Zeng XY, Wang JY (2013) NF-κB, ERK, p38 MAPK and JNK contribute to the initiation and/or maintenance of mechanical allodynia induced by tumor necrosis factor-alpha in the red nucleus. Brain Res Bull 99:132–139
Wang ZH, Zeng XY, Han SP, Fan GX, Wang JY (2012) Interleukin-10 of red nucleus plays anti-allodynia effect in neuropathic pain rats with spared nerve injury. Neurochem Res 37:1811–1819
Wang J, Yu J, Ding CP, Han SP, Zeng XY, Wang JY (2015) Transforming growth factor-beta in the red nucleus plays antinociceptive effect under physiological and pathological pain conditions. Neuroscience 291:37–45
Gadient RA, Otten UH (1997) Interleukin-6 (IL-6)–a molecule with both beneficial and destructive potentials. Prog Neurobiol 52:379–390
Erta M, Quintana A, Hidalgo J (2012) Interleukin-6, a major cytokine in the central nervous system. Int J Biol Sci 8:1254–1266
Hunter CA, Jones SA (2015) IL-6 as a keystone cytokine in health and disease. Nat Immunol 16:448–457
Okamoto K, Martin DP, Schmelzer JD, Mitsui Y, Low PA (2001) Pro- and anti-inflammatory cytokine gene expression in rat sciatic nerve chronic constriction injury model of neuropathic pain. Exp Neurol 169:386–391
Brázda V, Klusáková I, Svíženská I, Veselková Z, Dubový P (2009) Bilateral changes in IL-6 protein, but not in its receptor gp130, in rat dorsal root ganglia following sciatic nerve ligature. Cell Mol Neurobiol 29:1053–1062
Brázda V, Klusáková I, Hradilová Svíženská I, Dubový P (2013) Dynamic response to peripheral nerve injury detected by in situ hybridization of IL-6 and its receptor mRNAs in the dorsal root ganglia is not strictly correlated with signs of neuropathic pain. Mol Pain 9:42
Dubový P, Klusáková I, Svízenská I, Brázda V (2010) Satellite glial cells express IL-6 and corresponding signal-transducing receptors in the dorsal root ganglia of rat neuropathic pain model. Neuron Glia Biol 6:73–83
Dubový P, Brázda V, Klusáková I, Hradilová-Svíženská I (2013) Bilateral elevation of interleukin-6 protein and mRNA in both lumbar and cervical dorsal root ganglia following unilateral chronic compression injury of the sciatic nerve. J Neuroinflammation 10:55
Sacerdote P, Franchi S, Moretti S, Castelli M, Procacci P, Magnaghi V, Panerai AE (2013) Cytokine modulation is necessary for efficacious treatment of experimental neuropathic pain. J Neuroimmune Pharmacol 8:202–211
Wei XH, Na XD, Liao GJ, Chen QY, Cui Y, Chen FY, Li YY, Zang Y, Liu XG (2013) The up-regulation of IL-6 in DRG and spinal dorsal horn contributes to neuropathic pain following L5 ventral root transection. Exp Neurol 241:159–168
del Rey A, Yau HJ, Randolf A, Centeno MV, Wildmann J, Martina M, Besedovsky HO, Apkarian AV (2011) Chronic neuropathic pain-like behavior correlates with IL-1β expression and disrupts cytokine interactions in the hippocampus. Pain 152:2827–2835
Al-Amin H, Sarkis R, Atweh S, Jabbur S, Saadé N (2011) Chronic dizocilpine or apomorphine and development of neuropathy in two animal models II: effects on brain cytokines and neurotrophins. Exp Neurol 228:30–40
Liu J, Feng X, Yu M, Xie W, Zhao X, Li W, Guan R, Xu J (2007) Pentoxifylline attenuates the development of hyperalgesia in a rat model of neuropathic pain. Neurosci Lett 412:268–272
Chu H, Sun J, Xu H, Niu Z, Xu M (2012) Effect of periaqueductal gray melanocortin 4 receptor in pain facilitation and glial activation in rat model of chronic constriction injury. Neurol Res 34:871–888
Zimmermann M (1983) Ethical guidelines for investigations of experimental pain in conscious animals. Pain 16:109–110
Pertin M, Gosselin RD, Decosterd I (2012) The spared nerve injury model of neuropathic pain. Methods Mol Biol 851:205–212
Chaplan SR, Bach FW, Pogrel JW, Chung JM, Yaksh TL (1994) Quantitative assessment of tactile allodynia in the rat paw. J Neurosci Methods 53:55–63
Schöbitz B, Voorhuis DA, De Kloet ER (1992) Localization of interleukin 6 mRNA and interleukin 6 receptor mRNA in rat brain. Neurosci Lett 136:189–192
Schöbitz B, De Kloet ER, Sutanto W, Holsboer F (1993) Cellular localization of interleukin 6 mRNA and interleukin 6 receptor mRNA in rat brain. Eur J Neurosci 5:1426–1435
Alexander GM, van Rijn MA, van Hilten JJ, Perreault MJ, Schwartzman RJ (2005) Changes in cerebrospinal fluid levels of pro-inflammatory cytokines in CRPS. Pain 116:213–219
Ohtori S, Suzuki M, Koshi T, Takaso M, Yamashita M, Inoue G, Yamauchi K, Orita S, Eguchi Y, Kuniyoshi K, Ochiai N, Kishida S, Nakamura J, Aoki Y, Ishikawa T, Arai G, Miyagi M, Kamoda H, Suzuki M, Toyone T, Takahashi K (2011) Proinflammatory cytokines in the cerebrospinal fluid of patients with lumbar radiculopathy. Eur Spine J 20:942–946
Arruda JL, Colburn RW, Rickman AJ, Rutkowski MD, DeLeo JA (1998) Increase of interleukin-6 mRNA in the spinal cord following peripheral nerve injury in the rat: potential role of IL-6 in neuropathic pain. Mol Brain Res 62:228–235
Cunha FQ, Poole S, Lorenzetti BB, Ferreira SH (1992) The pivotal role of tumor necrosis factor alpha in the development of inflammatory hyperalgesia. Br J Pharmacol 107:660–664
Oka T, Oka K, Hosoi M, Hori T (1995) Intracerebroventricular injection of interleukin-6 induces thermal hyperalgesia in rats. Brain Res 692:123–128
DeLeo JA, Colburn RW, Nichols M, Malhotra A (1996) Interleukin-6-mediated hyperalgesia/allodynia and increased spinal IL-6 expression in a rat mononeuropathy model. J Interferon Cytokine Res 16:695–700
Vissers KC, De Jongh RF, Hoffmann VL, Meert TF (2005) Exogenous interleukin-6 increases cold allodynia in rats with a mononeuropathy. Cytokine 30:154–159
Lee KM, Jeon SM, Cho HJ (2009) Tumor necrosis factor receptor 1 induces interleukin-6 upregulation through NF-kappaB in a rat neuropathic pain model. Eur J Pain 13:794–806
Xu XJ, Hao JX, Andell-Jonsson S, Poli V, Bartfai T, Wiesenfeld-Hallin Z (1997) Nociceptive responses in interleukin-6-deficient mice to peripheral inflammation and peripheral nerve section. Cytokine 9:1028–1033
Zhong J, Dietzel ID, Wahle P, Kopf M, Heumann R (1999) Sensory impairments and delayed regeneration of sensory axons in interleukin-6-deficient mice. J Neurosci 19:4305–4313
Arruda JL, Sweitzer S, Rutkowski MD, DeLeo JA (2000) Intrathecal anti-IL-6 antibody and IgG attenuates peripheral nerve injury-induced mechanical allodynia in the rat: possible immune modulation in neuropathic pain. Brain Res 879:216–225
Twining CM, Sloane EM, Milligan ED, Chacur M, Martin D, Poole S, Marsh H, Maier SF, Watkins LR (2004) Peri-sciatic proinflammatory cytokines, reactive oxygen species, and complement induce mirror-image neuropathic pain in rats. Pain 110:299–309
Ma W, Quirion R (2006) Increased calcitonin gene-related peptide in neuroma and invading macrophages is involved in the up-regulation of interleukin-6 and thermal hyperalgesia in a rat model of mononeuropathy. J Neurochem 98:180–192
Ohtori S, Miyagi M, Eguchi Y, Inoue G, Orita S, Ochiai N, Kishida S, Kuniyoshi K, Nakamura J, Aoki Y, Ishikawa T, Arai G, Kamoda H, Suzuki M, Takaso M, Furuya T, Kubota G, Sakuma Y, Oikawa Y, Toyone T, Takahashi K (2012) Efficacy of epidural administration of anti-interleukin-6 receptor antibody onto spinal nerve for treatment of sciatica. Eur Spine J 21:2079–2084
Czlonkowski A, Stein C, Herz A (1993) Peripheral mechanisms of opioid antinociception in inflammation: involvement of cytokines. Eur J Pharmacol 242:229–235
Flatters SJL, Fox AJ, Dickenson AH (2003) Spinal interleukin-6 (IL-6) inhibits nociceptive transmission following neuropathy. Brain Res 984:54–62
Flatters SJL, Fox AJ, Dickenson AH (2004) Nerve injury alters the effects of interleukin-6 on nociceptive transmission in peripheral afferents. Eur J Pharmacol 484:183–191
Yan J, Melemedjian OK, Price TJ, Dussor G (2012) Sensitization of dural afferents underlies migraine-related behavior following meningeal application of interleukin-6 (IL-6). Mol Pain 8:6
Fang D, Kong LY, Cai J, Li S, Liu XD, Han JS, Xing GG (2015) Interleukin-6-mediated functional upregulation of TRPV1 receptors in dorsal root ganglion neurons through the activation of JAK/PI3K signaling pathway: roles in the development of bone cancer pain in a rat model. Pain 156:1124–1144
Kawasaki Y, Zhang L, Cheng JK, Ji RR (2008) Cytokine mechanisms of central sensitization: distinct and overlapping role of interleukin-1β, interleukin-6, and tumor necrosis factor-α in regulating synaptic and neuronal activity in the superficial spinal cord. J Neurosci 28:5189–5194
Acknowledgments
The authors wish to thank Dr. Runxia Tian and Xiaoli Li for their expert help in reviewing the manuscript. The project was sponsored by the National Natural Science Foundation of China (No. 31070979) and the Natural Science Foundation of Shaanxi Province, China (No. 2016JM3028).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ding, CP., Xue, YS., Yu, J. et al. The Red Nucleus Interleukin-6 Participates in the Maintenance of Neuropathic Pain Induced by Spared Nerve Injury. Neurochem Res 41, 3042–3051 (2016). https://doi.org/10.1007/s11064-016-2023-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11064-016-2023-9