Abstract
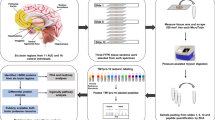
We report on changes in neurotransmitter metabolome and protein expression in the striatum of humans exposed to heavy long-term consumption of alcohol. Extracts from post mortem striatal tissue (dorsal striatum; DS comprising caudate nucleus; CN and putamen; P and ventral striatum; VS constituted by nucleus accumbens; NAc) were analysed by high performance liquid chromatography coupled with tandem mass spectrometry. Proteomics was studied in CN by two-dimensional gel electrophoresis followed by mass-spectrometry. Proteomics identified 25 unique molecules expressed differently by the alcohol-affected tissue. Two were dopamine-related proteins and one a GABA-synthesizing enzyme GAD65. Two proteins that are related to apoptosis and/or neuronal loss (BiD and amyloid-β A4 precursor protein-binding family B member 3) were increased. There were no differences in the levels of dopamine (DA), 3,4-dihydrophenylacetic acid (DOPAC), serotonin (5HT), homovanillic acid (HVA), 5-hydroxyindoleacetic acid (HIAA), histamine, l-glutamate (Glu), γ-aminobutyric acid (GABA), tyrosine (Tyr) and tryptophan (Tryp) between the DS (CN and P) and VS (NAc) in control brains. Choline (Ch) and acetylcholine (Ach) were higher and norepinephrine (NE) lower, in the VS. Alcoholic striata had lower levels of neurotransmitters except for Glu (30 % higher in the alcoholic ventral striatum). Ratios of DOPAC/DA and HIAA/5HT were higher in alcoholic striatum indicating an increase in the DA and 5HT turnover. Glutathione was significantly reduced in all three regions of alcohol-affected striatum. We conclude that neurotransmitter systems in both the DS (CN and P) and the VS (NAc) were significantly influenced by long-term heavy alcohol intake associated with alcoholism .
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
As dopamine (DA) has been considered a key neurotransmitter in mechanisms leading to addiction, it seems natural that DA systems in brain have been studied in relationship to alcoholism for some time. The most powerful associations between alcohol dependence and genes involved in dopamine metabolism has been reported for genes DRD2 (TaqI A polymorphism of ANKK1 gene) and DRD4 encoding corresponding dopamine receptors D2 and D4 [1–3]. Significant associations between alcoholism and polymorphisms in genes for enzymes monoamine oxidase [4], catechol-O-methyl transferase (COMT) [5–7], dopamine-β-hydroxylase (DBH) [8], and a serotonin transporter (SLC6A4); [3] have also been found; however, despite many studies in the literature, no satisfactory understanding of neurochemical mechanisms underlying alcoholism has been achieved to date.
Our previous studies of more than 7000 proteins expressed in various regions of alcoholic post-mortem human or rat brains identified 238 proteins as being associated with alcoholism; these have been categorized into cytoskeletal (28 %), metabolic (42 %), oxidative stress (15 %), signalling-related (22 %) and apoptosis-related (5 %) proteins [9–14]. The functional profiles of the altered proteins (enzymes in particular) have indicated that alcohol could interfere with glucose metabolism, tricarboxylic acid cycle, and other crucial metabolic pathways associated with thiamine, lactate, glutathione, fatty acid/lipase as well as the metabolism of signalling compounds such as dopamine, serotonin and glutamate [10–12]. In order to follow up in more detail how the changes in expression of the functional proteins that we have already identified may translate into specific changes in neurochemistry of neurotransmitters and related metabolites we are now expanding this approach by adding metabolomic techniques to our investigations. Given that biochemical and physiological changes underlying development of drug addiction have often been traced to the striatum, we selected this part of brain as the main region of interest in the present study.
The striatum has been conventionally divided into caudate nucleus (CN) and putamen (P) but, more recently, a third sub-region has been recognized [15] comprising mainly nucleus accumbens (NAc) at the ventral confluence of CN and P. Striatum receives two major inputs: axons of excitatory pyramidal glutamatergic neurons from the cerebral cortex and an array of mainly dopaminergic, serotoninergic and cholinergic fibres from the brain stem. While the dorsal striatum (DS: CN and P) receives most of its direct cortical input from sensorimotor (P) or association (CN) cortex [16], ventral striatum (VS: NAc) is targeted mainly by the areas of the cerebral cortex concerned with motivational or emotional activities and include insula, temporal lobe, anterior cingulate gyrus, parts of prefrontal cortex (PFC) and hippocampus [17]. Dopaminergic innervation of the VS originates mainly in the ventral tegmental area (VTA) of the brainstem and, to a lesser extent, in the medial substantia nigra [18, 19]. DS receives its dopaminergic input from substantia nigra, pars compacta. Interestingly, the VTA dopaminergic fibres also release glutamate [20, 21]. Functional differences between the dorsal and ventral striatum could be reflected in neurochemical differences; this would agree with our previous proteomic studies of human brain [22].
In terms of cytoarchitecture, medium-sized densely-spiny GABAergic neurons constitute the principal neuronal population and the only projection neurons in both dorsal and ventral striatum accounting for 75–80 % of all striatal neurons in human brain [23]. The remainder is formed by local interneurons, the majority of which are also GABAergic [23, 24]. There is a small but functionally significant indigenous population of cholinergic interneurons throughout the striatum.
While no sharp boundary between the dorsal and ventral striata can be established on the basis of cytoarchitecture, myeloarchitecture or chemoarchitecture [15, 25], accumulated evidence indicates that there exists a functional heterogeneity within the structures [25]. The VS appears to regulate the overall level of locomotor activity, aggressive behaviour and reward/aversion-related learning [27] while DS is more intimately involved in motor coordination and procedural learning [28, 29]. The circuitry involving the dopaminergic input from VTA to NAc seems crucial for processing of incentive-motivational properties of drugs and drug-related cues while other regions such as the amygdala and the hippocampus (HP) are more likely to contribute to the habitual learning behavior which could also be a part of the addiction-forming mechanism [30]. A model of neuronal networking regulating human addiction process as proposed by Volkow et al. [31] includes the following: (a) reward and drug seeking circuits mediated by the NAc, (b) motivation/drive located in the orbitofrontal cortex and the subcallosal cortex, (c) memory and learning mediated by DS, the amygdala and the HP and (d) the cortical control executed from the PFC and the anterior cingulate gyrus.
The overall evidence therefore suggests that, even though the VS is anatomically and/or cytoarchitecturally similar to DS, the functional activities related to addiction could be very different and this may be reflected in the regional neurochemical make up, as we have noted in our previous study using proteomics in otherwise apparently homogenous sub-regions of the corpus callosum [22]. Here we look for such differential neurochemical changes; particularly for those associated with neurotransmitters and cellular signalling.
Materials and Methods
Chemicals
Dopamine hydrochloride (DA), serotonin hydrochloride (5HT), tyrosine (Tyr), tryptophan (Tryp), homovanillic acid (HVA), 3,4-dihydroxyphenylacetic acid (DOPAC), 5-hydroxyindole-3-acetic acid (5-HIAA), norepinephrine (NE), γ-aminobutyric acid (GABA), l-glutamic acid (Glu), histamine (His), choline (Ch), acetylcholine (Ach), glutathione (GSH), heptafluorobutyric acid (HFBA) and internal standard 3,4-dihydroxybenzylamine (DHB) were purchased from Sigma-Aldrich (St. Louis, MO, USA). HPLC grade methanol and formic acid were also supplied by Sigma-Aldrich and ultrapure water was obtained from a Milli-Q Gradient water system (Millipore, Bedford, MA, USA). All consumables for gel electrophoresis were obtained from Proteome Systems Ltd (Australia) and IPG (immobilized pH gradient) strips were from Biorad Lab Pty Ltd (Australia).
Human Brain Tissue
In our study, we have been using post-mortem brains from 12 males. The samples came from 6 control brains (CB) and 6 alcoholic brains (AB). Mean age in groups, alcoholics and controls was 59 years (cf. Table 1 for further details). All post-mortem human brains were obtained from the NSW Brain Bank (University of Sydney). The tissue samples were taken from the caudate nucleus (CN), the putamen (P) and the nucleus accumbens (NAc). The groups were, as far as possible, matched for age and pH (except for the post-mortem interval; PMI, of 3 alcoholic samples). Post-mortem examination of the alcoholic brains revealed that there were no complications from Wernicke–Korsakoff Syndrome (WKS) in any of the alcoholic brains used in the present study. Clinical history of the patients indicated that patients did not suffer from any additional psychiatric or neurological diseases unrelated to their alcoholic condition. Death of the patients was not directly caused by any known dysfunction of the central or peripheral nervous system. Alcoholic cases fulfilled the criteria of the Diagnostic and Statistical Manual of Mental Disorders IV (DSM-IV) for alcohol dependence [32]. Alcohol consumption data were obtained from medical records or from reports by the next of kin. Ethics approval for human tissue use was obtained from the Sydney South West Area Health Service.
Preparation of Standards and Calibration curves for Liquid Chromatography/Tandem Mass Spectrometry (LC-MS/MS)
Standard stock solutions were prepared in a 0.1 M formic acid solution to assist dissolution and minimize oxidation of labile samples [33]. These solutions were stored at −20 °C until use. Standard curves were prepared by adding analytes (Tyr, Tryp, DA, DOPAC, NE, 5HT, GABA, Ch, Ach, His, 5HIAA, HVA, Glu, GSH and internal standard DHB to a 0.1 % formic acid solution. A constant amount (500 pg/μL) of internal standard was added to all standard solutions to produce a fixed concentration.
Sample Preparation for LC-MS/MS
The brain samples were weighed and homogenized at 1 mg per 50 μL of 0.1 M formic acid [33, 34]. The internal standard (DHB) was then added to 500 pg/μL final concentration. The suspension was sonicated and centrifuged at 16,000×g for 20 min at 4 °C. The supernatant was filtered and diluted within the range of calibration curve.
Analysis of Metabolites
Chromatographic analyses have been performed in an Acquity UPLC™ system (Waters, Milford, MA, USA), using a BEH C18 column (150 mm × 2.1 mm; Waters), with 1.7 μm particle size [33, 35]. The mobile phase for elution was a gradient established between solvent A (0.05 % formic acid in water + 1 mM HFBA) and solvent B (methanol) at a flow rate of 200 μL/min. Gradient conditions were: 0.0–1.0 min, 5–50 % B; 1.0–2.0 min, 50–95 % B; 2.0–3.0 min, 95 % B; and back to 5 % B in 1.0 min. Flow rate was 0.2 mL min−1, injection volume 5 μL (in partial loop mode), the column temperature was maintained at 25–27 °C and the sample temperature was at 4 °C.
Mass spectrometric detection was carried out using a Waters Acquity TQD tandem quadrupled mass spectrometer (Waters, Manchester, UK) [33]. The tandem mass spectrometer was operated in multiple reactions monitoring (MRM) mode and Q1 and Q3 quadruples were set at unit mass resolution. The instrument was operated using electro spray ionization (ESI) source in positive mode. ESI parameters were capillary voltage 3.0 kV, extractor voltage 3 V, source temperature 120 °C, desolvation temperature 350 °C, cone gas flow 80 L/h and desolvation flow 600 L/h (both gases were nitrogen). Collision-induced dissociation was performed using argon as the collision gas at the pressure of 4 × 10−3 mbar in the collision cell. The MRM transitions as well as the cone voltages and collision energies are shown in Table 2. Data acquisition was performed using MassLynx 4.0 software with QuanLynx program (Waters).
Protein assay was performed by the Bradford method using bovine serum albumin as a standard [36].
Preparation of Tissue Extracts for Proteomics and Two-Dimensional Gel Electrophoresis (2-DE)
Protein extraction and gel analysis were done as previously described in detail [11, 19, 22]. Briefly, 100 mg of tissue was homogenised, sonicated (3×) and centrifuged at 16,000g for 20 min at 15 °C. The supernatant was reduced and alkylated in 5 mM tributyl phosphine and 10 mM acrylamide monomer at room temperature for 2 h. The reaction was quenched using 10 mM DTT (dithiothreitol). Acetone (five times of extract volume) and citric acid (20 mg) and the resulting precipitate centrifuged at 2500g × 15 min at 15 °C. The pellet was air dried, resuspended and stored at −80 °C before isoelectric focusing.
Following protein estimation [36], 2-DE was conducted as previously described using SDS-PAGE (sodium dodecyl sulphate—polyacrylamide gel electrophoresis); [9–12, 22].
Image Analysis, Matrix-Assisted Laser Desorption/Ionization (MALDI)-Mass Spectroscopy and Protein Identification
A total of 24 gels (duplicate runs for each sample) were scanned using a flatbed scanner (UMAX, USA). The images were analysed by Phoretix 2D Expression software (Nonlinear Dynamics Ltd, UK) and quantified (spot area x optical density, background subtracted). Following log transformation and normalization, one-way analysis of variance (ANOVA, P < 0.05) was performed to identify significant differences (spot volume) between alcoholic and control brains.
The spots so identified were de-stained using 25 mM NH4HCO3/50 % (v/v) acetonitrile (ACN) for 3 × 15 min at 37 °C. The gel portions were then dehydrated using 100 % ACN and digested with 12.5-ng/ml trypsin (Roche, sequencing grade, Germany) buffer [25 mM NH4HCO3/0.1 % TFA (trifluoroacetic acid)] for 45 min at 4 °C and incubated a further 3 h at 37 °C. The peptide mixtures were purified using C-18 purification tips (Eppendorf, Germany), eluted onto a MALDI sample plate with 3 µL of matrix solution [5 mg/mL solution of α-cyano-4-hydroxycinnamic acid in 70 % (v/v) ACN/0.1 %(v/v) TFA] and allowed to air dry. The samples were analyzed using Qstar XL Excell Hybride MS system (AB Applied Biosystems, Foster City, CA, USA) in positive reflector mode, with delayed extraction. The data from mass spectra were matched to the Swiss-Prot database (http://www.matrixscience.com/) using criteria based on a MOWSE (Molecular Weight Search) score (>64, human database) with matched isoelectric pH (pI), molecular weight values (estimated from 2D gels) and sequence coverage.
Statistical Analyses
Each sample was measured twice and each group contained 12 data points. All data were statistically analysed using single factor ANOVA. Accordingly, the mean of the two groups is considered to be statistically significant only if P < 0.05. Pearson correlation was performed on the estimates of metabolite levels and on the values of agonal factors.
Results
General
Control brains (CB) and alcoholic brains (AB) were matched for age, brain pH and post-mortem interval time (PMI) (Table 1). The only significant difference between AB and CB was in PMI but, even there, the overlap between the two groups was quite large. Available evidence suggest that PMI has no significant effect on GABA, amino acid and biogenic amine contents of brain tissue [37, 38], and, additionally, our own previously published data indicated that agonal factors had no effect on the expression of proteins, including those acting as enzymes in neurotransmitter metabolism, in several regions of post-mortem human brain [10–12]. As Pearson correlation statistical test showed no significant difference between agonal factors and metabolite expression we assumed that the data in this study are free from the effects of agonal factors.
Regional Variations in Metabolite Levels
Analyses of the metabolites in sub-regions (CN, P and NAc) of striatum in CB showed no significant differences in the levels of metabolites from one sub-region of striatum to another except for NE, Ch and Ach contents (Table 3). In the CB striatum, Ch and Ach were, resp. 58 and 70 % higher, and NE 40 % lower, in the NAc relative to the DS (represented as mean of the values in CN and P, resp.; Table 3).
Changes in Neurotransmitter and Metabolite Levels in Alcoholic Striatum: Catecholamines
The levels of DA, NE, DOPAC, HVA and their precursor amino acid Tyr were significantly decreased in all subregions of AB striatum compared to CB (Table 4). DA reduction was similar in all sub-regions (~60 %). The decline rates of other catecholamine metabolites appeared somewhat variable but the regional variability was not statistically significant (Table 4).
The increase in the ratio of DOPAC/DA observed in AB was significantly higher in the VS (76 %) than in the DS (~18 %);(Table 4). Similarly, the increase in HIAA/5HT ratio was higher in the NAc (34 %) than in the DS (Table 4).
Preliminary estimation using Western blotting (WB) suggested that the expression of dopamine biosynthesis enzyme tyrosine hydroxylase (TH) was lower (Fig. 1) but the decreases in other three enzymes of the catecholamine metabolic pathway : DOPA decarboxylase (DDC), catechol-O-methyltransferase (COMT) and dopamine-β-hydroxylase (DBH), were variable and the apparent differences did not reach statistical significance (Fig. 1; see also the section on proteomics in CN below).
Total protein was extracted from the caudate nucleus of both control and alcoholic tissues and western blotting (top) was performed using antibodies as specified in “Materials and Methods” section. Bands were digitized and quantified; the controls were normalized as 100 (bottom). Columns represent the mean ± SE (n = 3 per group; asterisk significantly different from control at P < 0.05)
Expressions of two other proteins potentially linked to dopamine and/or addiction mechanisms, namely DARPP-32 (dopamine- and cAMP-regulated phosphoprotein of 32 kDa) and CREB (cAMP response element-binding protein) were significantly decreased (Fig. 1) in AB relative to CB (cf. also [9, 39]).
Changes in Neurotransmitter and Metabolite Levels in Alcoholic Striatum: Indolamines
Serotonin (5HT), HIAA and Tryp contents in AB striatum were significantly decreased compared to the CB striatum (Table 4; cf. also [9, 40]. The HIAA depletion in the alcoholic CN was higher (57 %) relative to other regions (~38 %; Table 4). Additionally, the expression of tryptophan hydroxylase (TPH), the key enzyme of serotonin biosynthesis, was decreased (44 %) in the CN of AB (Fig. 1, cf. also [40, 41]. The increase in HIAA/5HT ratio was higher in the NAc (34 %) than in the DS (Table 4).
Changes in Neurotransmitter and Metabolite Levels in Alcoholic Striatum: Acetylcholine
Choline and acetylcholine contents were significantly decreased in AB striatum (Table 4) and the degree of depletion appeared variable from one subregion to another but these variations did not reach statistical significance (Table 4).
Changes in Neurotransmitter and Metabolite Levels in Alcoholic Striatum: Amino Acids
No significant changes in GABA levels were observed between striata of AB and CB (Table 4). Glu content was significantly higher in the VS (30 %) relative to the DS (5 %) (Table 4). Glutamate decarboxylase (GAD), the enzyme of GABA synthesis, was lower in the CN of AB (Fig. 1; Table 5, see below).
Changes in Neurotransmitter and Metabolite Levels in Alcoholic Striatum: Histamine
Histamine (His) content was significantly lower in AB and the rates of depletion were similar in all regions (Table 4). Preliminary estimations of histidine decarboxylase (HDC), an enzyme that synthesizes histamine, have indicated that its expression was not significantly decreased in AB (Fig. 1).
Glutathione (GSH)
Free radical scavenging molecule GSH content was lower in AB. The reduction was highest in CN (67 %) followed by the NAc (58 %) and P (34 %) (Table 4). The only enzyme related to GSH that was found to be significantly decreased in the CN of AB was glutathion-S-transferase Mu 3 (cf. the next section on proteomics and Table 5).
Expression of Proteins in the Caudate Nucleus Studied by Proteomics
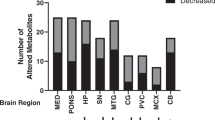
The average 2D-gels showed 570 spots in the samples from control brains and 550 spots in the samples of alcoholic brains. Subsequent analysis identified 25 unique proteins which were differentially expressed in the CN of AB and CB (Table 5). The proteins directly linked to DA included TH and COMT, an enzyme of catecholamine metabolism. One other protein linked to neurotransmitter metabolism, a GABA-synthesizing enzyme GAD65, was also decreased in the alcohol affected tissue. The decrease in TPH indicated by WB studies was not, however, supported by the proteomics.
Changes in some of the proteins found to be differentially expressed in the CN of AB and CB could be related to oxidative stress, tissue damage and/or neurodegenerations (e.g., glutathione-S-transferase Mu 3, synaptosomal-assocaciated protein 25, amyloid-β-precursor protein-binding family B member 3, BH3-interacting domain death agonist BiD; Table 5).
Discussion
General
To the best of our knowledge, this is the first study using the LC-MS/MS technique to obtain information on the effects of long-term heavy alcohol intake on the levels of neurotransmitters and related metabolites in striatal regions of human brain. The major findings in this study are the following: First, lower contents of Tyr, Tryp, His, Ch, Ach, DA, 5HT, HVA, HIAA and GSH in AB compared to CB. Second, variation, in some cases, of the depletion rates from one part of striatum to another, suggesting that neurotransmitter metabolism in the striatum does not have the same sensitivity to chronic alcohol in all subregions (Table 4). Third, the ratios of DOPAC/DA and HIAA/5HT were, in AB, higher in the VS relative to the DS. Thus it appears that both VS and DS are sensitive to the effects of heavy long-term alcohol exposure. The susceptibility of DS to the chronic excessive alcohol intake is also in accordance with the observation of differences between AB and CB in terms of expression of several important proteins in the CN (a part of DS), as revealed by proteomics (Table 5) and WB (Fig. 1).
Regional Variations in the Striatum of CB: Differential Sensitivity of DS and VS to Alcohol?
In CB, Ch and Ach levels were higher and the NE level was lower in the NAc relative to the dorsal striatum suggesting that either the density of noradrenergic and cholinergic innervations, their synaptic activities or, simply the metabolic rates of Ch, Ach and NE in the VS differ from those in the DS. The above findings are compatible with other published data; for example a comparative study of cholinergic neurons in sub-regions of the striatum revealed that NAc has at least 30 % more cholinergic neurons than the dorsal striatum [42]. The cholinergic interneurons of the VS have large dendritic arbors that connect many cell bodies including the core and shell subdivisions of the NAc. Cholinergic neurons have been shown to play an important role in the modulation of both food and drug intake including aversive responses to foods or drug-related addictive behaviours [43]. The stress-related neurotransmitter norepinephrine (NE) [44] is lower in the VS relative to DS (Table 3).
The levels of catabolic products of DA and 5HT and their ratios in the DS did not differ significantly from those in NAc. This is consistent with the morphological similarities of DS and the VS. Region-specific variable metabolite levels in the rat striatum have, however, been previously reported [45, 46]; it is, therefore, possible that more subtle differences will be revealed by future studies using larger numbers of human brains.
In our earlier proteomic study we noted that free radical scavenging (GSH metabolism) and pentose phosphate pathways were dominantly expressed in the splenium of corpus callosum (CC) relative to the genu of CC and, the higher activities of these two pathways might have been linked to the region-specific sensitivity to the alcohol. Considering the present results in the context of the previous evidence and in analogy with previous conclusions, we propose that the neurochemistry of the NAc is different from that of DS in terms of alcohol-sensitivity of metabolic pathways associated with noradrenergic, dopaminergic and cholinergic neurotransmission and these differences may contribute to the pathophysiology of alcoholism and alcohol addiction [47, 48].
Alcoholism-Associated Region-Specific Changes in Neurotransmitter Metabolism
Previous studies have preferred NAc as the striatal region most important for the mechanisms of addictive behaviour, however there are indications that the DS may also be involved in addiction-related mechanisms [31, 49, 50] even if this may involve its connections to VS [51]. Specifically, alleviation of alcohol and nicotine addiction after a cerebrovascular incident in the human DS has been reported [52]. In the present study we have noted that the contents of most of the neurometabolites in DS and VS are similar (Table 3) but alcohol-induced expression pattern, in particular the relative changes (Table 4), in alcoholic regions (CN, P and NAc) are more variable. These results are reminiscent of those of Tran-Nguyen et al. [26] who found that the administration of the dopamine-depleting toxin 6-hydroxydopamine into DS and VS produced a heterogeneous response in terms of changes in monoamine content in the regions.
Thus DA in the DS might be involved in the addiction-related process analogous to that which exists in NAc and it is possible that both parts of the striatum contribute to drug craving/relapse and/or habitual learning involved in substance abuse [53–55]. This suggestion is strongly supported by the differences between AB and CB identified by proteomics in the CN (a part of DS), particularly the reduced expression of DA-related proteins (Table 5).
Glu content in AB compared to CB was significantly increased in NAc (30 %) relative to DS (Table 4). This is in contrast to the other signalling molecules but similar findings have been made before; Glu level has been reported as increased in the prefrontal cortex of alcoholic patients relative to control and glutamate/glutamine ratio has been proposed as a biomarker for alcohol-dependence [56, 57]. l-Glutamate is the principal excitatory neurotransmitter in the mammalian CNS and, as such, would be expected to play the central role in a whole spectrum of brain functions [58, 59]. While short term exposure to alcohol decreases glu activity, long term exposure has the opposite effect [57, 60].
Alcohol and Oxidative Stress
Alcohol has been shown to induce oxidative stress and result in low levels of GSH in the brain cells; in fact, oxidative stress may be one of the most important mechanisms mediating alcohol-induced brain damage. It is, therefore, quite significant that, in this study, we observed that glutathione, the free radical scavenging molecule, was reduced by up to 60 % in alcoholic tissues (Table 4). This is similar to the reductions in GSH reported by others [61]. The depletion of glutathione (GSH) would seem to correlate with alcohol-induced reduction in glutathione biosynthesis enzymes as detected previously in our proteome studies in alcoholic post-mortem human and rat brain [10–12]; cf. decrease in glutathione S-transferase Mu 3 in the alcoholic CN in the present study (Table 5). In the context, the decreases in synaptosomal-associated protein 25 and β-synuclein (Table 5) may indicate loss of synaptic contacts and the increase in apoptosis-associated protein BiD (Table 5) might indicate apoptotic loss of neurons caused by oxidative stress. The apparent regional variation in the effect of alcohol on GSH levels (Table 4) merits additional study.
Alcohol Induced Alteration of Neurotransmitter Biosynthesis Pathways
The regionally-variable elevations of Glu content (but no clear change in the content of GABA) as observed in AB relative to the CB are of potential interest, given that a significant component of the ethanol effect on brain metabolism is exerted through a subtype of GABA(A) receptor [62] or by NMDA receptors (for a review see [63]). GABA is synthesized from glutamate via pyridoxal 5′-phosphate dependent glutamic acid decarboxylase (l-glutamate-carboxy-1-lyase, EC 4.1.1.15; GAD). The deficiency of GABA would be consistent with low level of GAD [65] and/or deficit of its cofactor ([9] and Kashem, unpublished data). In fact, even when the data in Table 4 were analysed by ANOVA over six independent data groups i.e. including three regions of control striatum and three regions of alcohol-affected striatum, the decreases were not statistically significant at P = 0.05 (not shown). GABA/Glu ratio in AB relative to CB might appear regionally variable; it is 39 % in VS compared to ~19 % in DS (Table 4) but, again, these variations were not statistically significant. Proteomics data show reduced expression of GAD65 in the alcoholic CN (a part of DS) compared to the control but this may not be enough to cause a significant deficiency in GABAergic inhibitory system (no significant difference detected by WB; Fig. 1).
Alcohol and histamine are metabolized through a common enzymatic pathway (aldehyde reductase) and administration of ethanol has been shown to decrease His concentration in mice [64]; the present findings could be a result of reduced expression of His biosynthesis enzymes HDC (Fig. 1).
Serotonin precursor amino acid Tyr, serotonin, 5HIAA and serotonin metabolic key enzymes tryptophan hydroxylase (TPH) and DDC have all been reported as decreased in alcoholic tissues [65, 66] indicating that long-term alcohol intake could suppress serotonin biosynthesis. Transgenic mice (TPH–2 deficient) displayed 60–80 % lower 5HT and increased capacity of ethanol consumption [67]. Other studies have shown that reduced levels of brain 5HT are associated with increased ethanol intake in both rodents and primates [68–70]. It has been proposed that 5HT deficiency (e.g., reduced levels of the 5HT metabolite, 5-HIAA) be used as a biomarker of alcoholism [68, 71].
Dysregulation of catecholaminergic system has been reported in alcoholism [72]. In the present study we observed that DA and its precursor amino acid Tyr and catabolic products, NE, DOPAC and HVA content were all decreased in regions of alcoholic brains relative to their respective controls [9, 40, 73]; these results suggested that alcohol either disturbed and/or damaged DA innervations leading to reduced biosynthesis. If the lower content of DA is caused by higher catabolism, then the alcoholic tissues might be expected to show higher levels of DOPAC, NE and HVA but this has turned out not to be the case in the present study, their contents were actually lower in the alcoholic regions. Moreover, the preliminary data have not shown any statistically significant changes in the two most important catecholamine catabolising enzymes: catechol-O-methyltransferase and dopamine-β-hydroxylase (DBH);(Fig. 1), while more comprehensive 2D-gel proteomic actually indicated reduced expression of COMT in AB, at least in the CN (Table 5) Genetic studies of human populations indicated that both high- and low- activity COMT alleles could be associated with alcoholism and the enzyme could also be regulated epigenetically [5–7]. Thus, the reasons for the decreases in the content of NE, DOPAC and HVA in alcoholic tissues could be caused by lower availability of the precursor molecule DA or it might be a result of deficient of biosynthesis.
Expressions of DA biosynthesising enzymes and proteins associated with DA signalling [TH, pyrophosphate phosphatase (PPP), DARPP-32] have been found altered in the striatum of a beer-drinking rat model of alcoholism [9, 74] and this seems consistent with the decreased expressions of DARPP-32 indicated by the present study [8, 75].
It is interesting to note that the preliminary WB quantification also indicated a decrease in the expression of CREB in the AB tissue. CREB regulates expression of many proteins in brain including TH, TPH, GAD, choline acetyl transferase, DBH, adenylyl cyclase and glutamine synthase (GS) [76, 77]. Given that CREB activity is regulated by multiple phosphorylations and its immunological estimations may require special care [78], the present finding would seem to be worth of a more thorough study using a larger sample.
Concluding Remarks
The present study has identified significant changes in neurotransmitter levels in all regions of striatum in alcoholic brains. There are significant decreases in the levels of several neurotransmitters (dopamine, noradrenaline and acetylcholine) and related metabolites. This is accompanied by similar changes in enzymes (at least in the caudate nucelus) involved in the neurotransmitter metabolism. Additionally, there is a significant decrease in the levels of antioxidant agent glutathione in all parts of striatum in alcoholic brains. This may further exacerbate the harmful effects of chronic heavy alcohol intake on brain tissue. We have also identified changes to several proteins not directly related to the function and metabolism of neurotransmitters; these may reflect more general aspects of the damage caused by long-term heavy drinking and should be investigated in greater detail in more extensive studies. Despite a small number of brains used in the present study (and the protein data limited to the dorsal striatum only), the findings may add to a more comprehensive model of how alcohol and alcoholism affect neurotransmitter signalling in striatum and lay more solid foundation for the understanding of the relationship between alcohol addiction and alcohol-related disorders.
Abbreviations
- AB:
-
Alcoholic brains
- Ach:
-
Acetylcholine
- ACN:
-
Acetonitrile
- CB:
-
Control brains
- CC:
-
Corpus callosum
- Ch:
-
Choline
- CN:
-
Caudate nucleus
- COMT:
-
Catechol-O-methyl transferase
- CREB:
-
cAMP response element-binding protein
- DA:
-
Dopamine
- DBH:
-
Dopamine-β-hydroxylase
- DDC:
-
Dopa decarboxylase
- DHB:
-
3,4-Dihydroxybenzylamine
- DOPAC:
-
3,4-Dihydrophenylacetic acid
- DS:
-
Dorsal striatum
- DTT:
-
Dithiothreitol
- ESI:
-
Electro spray ionization
- GAD:
-
Glutamate decarboxylase, l-glutamate-1-carboxylyase
- Glu:
-
l-Glutamate
- GS:
-
Glutamine synthase
- GSH:
-
Glutathione
- HDC:
-
Histidine decarboxylase
- HFBA:
-
Heptafluorobutyric acid
- His:
-
Histamine
- HVA:
-
Homovanilic acid
- 5HT:
-
5-Hydroxytryptamine, serotonin
- IPG:
-
Immobilized pH gradient
- LC-MS/MS:
-
Liquid chromatography/tandem mass spectroscopy
- MALDI:
-
Matrix-assisted laser desorption/ionization
- MOWSE:
-
Molecular weight search
- MRM:
-
Multiple reactions monitoring
- NAc:
-
Nucleus accumbens
- NE:
-
Norepinephrine, noradrenaline
- P:
-
Putamen
- PFC:
-
Prefrontal cortex
- PMI:
-
Post-mortem interval
- PPPase:
-
Pyridoxal phosphate phosphatase
- SDS-PAGE:
-
Sodium dodecyl sulphate-polyacrylamides gel electrophoresis
- TFA:
-
Trifluoroacetic acid
- TH:
-
Tyrosine hydroxylase/tyrosine 3-monooxygenase
- TPH:
-
Tryptophan hydroxylase
- Tryp:
-
Tryptophan
- Tyr:
-
Tyrosine
- VS:
-
Ventral striatum
- VTA:
-
Ventral tegmental area
- WB:
-
Western blotting
- WKS:
-
Wernicke–Korsakoff Syndrome
References
Mota NR, Araujo-Jnr EV, Paixao-Cortes VR, Bortolini MC, Bau CHD (2012) Linking dopamine neurotransmission and neurogenesis: the evolutionary history of the NTAD (NCAM1-TTC12-ANKK1-DRD2) gene cluster. Gen Mol Biol 35:912–918
Creemers HE, Harakeh Z, Dick DM, Meyers J, Vollebergh WA, Ormel J, Verhulst FC, Huizink AC (2011) DRD2 and DRD4 in relation to regular alcohol and cannabis use among adolescents: does parenting modify the impact of genetic vulnerability? The TRAILS study. Drug Alcohol Depend 115:35–42. doi:10.1016/j.drugalcdep.2010.10.008
Zwaluw VDCS, Kuntsche E, Engels RC (2011) Risky alcohol use in adolescence: the role of genetic (DRD2, SLC6A4) and coping motives. Alcohol Clin Exp Res 35:756–764
Whitfield JB, Pang D, Bucholz KK, Madden PA, Heath AC, Statham DJ, Martin NG (2000) Monoamine oxidase: associations with alcohol dependence, smoking and other measures of psychopathology. Psychol Med 30:443–454
Šerý O, Didden W, Mikeš V, Pitelová R, Znojil V, Zvolský P (2006) The association between high-activity COMT allele and alcoholism. Neuro Endocrinol Lett 27:231–235
Voisey J, Swagell CD, Hughes IP, Lawford BR, Young RMD, Morris CP (2011) A novel SNP in COMT is associated with alcohol dependence but not opiate or nicotine dependence: a case control study. Behav Brain Funct 7:51
Wang T, Franke P, Neidt H, Cichon S, Knapp M, Lichtermann D, Maier W, Propping P, Nothen MM (2001) Association study of the low-activity allele of catechol-O-methyltransferase and alcoholism using a family-based approach. Mol Psychiatry 6:109–111
Weinshenker D, Rust NC, Miller NS, Palmiter RD (2000) Ethanol-associated behaviors of mice lacking norepinephrine. J Neurosci 20:3157–3164
Kashem MA, Ahmed S, Sarker R, Ahmed EU, Hargreaves GA, McGregor IS (2012) Long-term daily access to alcohol alters dopamine-related synthesis and signaling proteins in the rat striatum. Neurochem Int 6:1280–1288
Kashem MA, Etages HD, Kopitar-Jerala N, McGregor IS, Matsumoto I (2009) Differential protein expression in the corpus callosum (body) of human alcoholic brain. J Neurochem 110:486–495
Kashem MA, Harper C, Matsumoto I (2008) Differential protein expression in the corpus callosum (genu) of human alcoholics. Neurochem Int 53:1–11
Kashem MA, James G, Harper C, Wilce P, Matsumoto I (2007) Differential protein expression in the corpus callosum (splenium) of human alcoholics: a proteomics study. Neurochem Int 50:450–459
Matsuda-Matsumoto H, Iwazaki T, Kashem MA, Harper C, Matsumoto I (2007) Differential protein expression profiles in the hippocampus of human alcoholics. Neurochem Int 51:370–376
Matsumoto I, Alexander-Kaufman K, Iwazaki T, Kashem MA, Matsuda-Matsumoto H (2007) CNS proteomes in alcohol and drug abuse and dependence. Expert Rev Proteomics 4:539–552
Heimer L (2000) Basal forebrain in the context of schizophrenia. Brain Res (Brain Res Rev) 31:205–235
Russo SJ, Nestler EJ (2013) The brain reward circuitry in mood disorders. Nat Rev Neurosci 14:609–625
Dichter GS, Richey JA, Rittenberg AM, Sabatino A, Bodfishet JW (2012) Reward circuitry function in autism during face anticipation and outcomes. J Autism Dev Dis 42:147–160
Andrisani OM (1999) CREB-mediated transcriptional control. Crit Rev Eeukaryot Gene Exp 9:19–32
Hjelmstad GO, Xia Y, Margolis EB, Fields HL (2013) Opioid modulation of ventral pallidal afferents to ventral tegmental area neurons. J Neurosci 33:6454–6459
Chuhma N, Choi WY, Mingote S, Rayport S (2009) Dopamine neuron glutamate cotransmission: frequency-dependent modulation in the mesoventromedial projection. Neuroscience 164:1068–1083. doi:10.1016/j.neuroscience.2009.08.057
Trudeau LE, Hnasko TS, Wallen-Mackenzie A, Morales M, Rayport S, Sulzer D (2014) The multilingual nature of dopamine neurons. Prog Brain Res 211:141–164
Kashem MA, King N, Rita M, McGregor IS, Sarker R, Des Etages H, Matsumoto I (2009) Comparative proteomics in the corpus callosal sub-regions of postmortem human brain. Neurochem Int 55:483–490
Tepper JM, Koos T, Wilson CJ (2004) GABAergic microcircuits in the neostriatum. Trends Neurosci 27:662–669
Kreitzer AC (2009) Physiology and pharmacology of striatal neurons. Ann Rev Neurosci 32:127–147
Prensa L, Richard S, Parent A (2003) Chemical anatomy of the human ventral striatum and adjacent basal forebrain structures. J Comp Neurol 460:345–367
Tran-Nguyen LT, Castaneda E, MacBeth T (1996) Changes in behavior and monoamine levels in microdialysate from dorsal striatum after 6-OHDA infusions into ventral striatum. Pharmacol Biochem Behav 55:141–150
Koob GF, Volkow ND (2010) Neurocircuitry of addiction. Neuropsychopharmacology 35:217–238
Beeler JA, Cao ZF, Kheirbek MA, Ding Y, Koranda J, Murakami M, Kang UJ, Zhuang X (2010) Dopamine-dependent motor learning: insight into levodopa’s long-duration response. Ann Neurol 67:639–647
Dang MT, Yokoi F, Yin HH, Lovinger DM, Wang Y, Li Y (2006) Disrupted motor learning and long-term synaptic plasticity in mice lacking NMDAR1 in the striatum. Proc Natl Acad Sci USA 103:15254–15259
O’Brien CP, Gardner EL (2005) Critical assessment of how to study addiction and its treatment: human and non-human animal models. Pharmacol Ther 108:18–58
Volkow ND, Fowler JS, Wang GJ (2003) The addicted human brain: insights from imaging studies. J Clin Investig 111:1444–1451
Annonymous (1994) Diagnostic and Statistical Manual of Mental Disorders, 4th edn. The Association, Washington
Gonzalez RR, Fernandez RF, Vidal JL, Frenich AG, Perex ML (2011) Development and validation of an ultra-high performance liquid chromatography-tandem mass-spectrometry (UHPLC-MS/MS) method for the simultaneous determination of neurotransmitters in rat brain samples. J Neurosci Methods 198:187–194
Xu N, Qiu C, Wang W, Chai C, Yan Y, Zhu D (2011) HPLC/MS/MS for quantification of two types of neurotransmitters in rat brain and application: myocardial ischemia and protection of Sheng-Mai-San. J Pharm Biomed Anal 55:101–108
Wei B, Li Q, Fan R, Su D, Chen X, Jia Y, Bi K (2014) Determination of monoamine and amino acid neurotransmitters and their metabolites in rat brain samples by UFLC-MS/MS for the study of the sedative-hypnotic effects observed during treatment with S. chinensis. J Pharm Biomed Anal 88:416–422
Bradford MM (1976) A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein-dye binding. Anal Biochem 72:248–254
Korpi ER, Kleinman JE, Goodman SI, Wyatt RJ (1987) Neurotransmitter amino acids in post-mortem brains of chronic schizophrenic patients. Psychiatry Res 22:291–301
Spokes EG, Garrett NJ, Rossor MN, Iversen LL (1980) Distribution of GABA in post-mortem brain tissue from control, psychotic and Huntington’s chorea subjects. J Neurosci 48:303–313
Pandey SC, Roy A, Zhang H, Xu T (2004) Partial deletion of the cAMP response element-binding protein gene promotes alcohol-drinking behaviors. J Neurosci 24:5022–5030
Sun HQ, Liu Y, Li P, Bao YP, Sheng LX, Zhang RL, Cao YJ, Di XL, Yang FD, Wang F, Luo YX, Lu L (2012) Effects of acute combined serotonin and dopamine depletion on cue-induced drinking intention/desire and cognitive function in patients with alcohol dependence. Drug Alcohol Depend 124:200–206
Jacobsen JP, Medvedev IO, Caron MG (2012) The 5-HT deficiency theory of depression: perspectives from a naturalistic 5-HT deficiency model, the tryptophan hydroxylase 2Arg439His knockin mouse. Philos Trans R Soc Lond Ser B Biol Sci 367:2444–2459
Meredith GE, Blank B, Groenewegen HJ (1989) The distribution and compartmental organization of the cholinergic neurons in nucleus accumbens of the rat. Neuroscience 31:327–345
Avena NM, Rada PV (2012) Cholinergic modulation of food and drug satiety and withdrawal. Physiol Behav 106:332–336
Morilak DA, Barrera G, Echevarria DJ, Garcia AS, Hernandez A, Ma S, Petre CC (2005) Role of brain norepinephrine in the behavioral response to stress. Prog Neuropsychopharmacol Biol Psychiatry 29:1214–1224
Laplante F, Zhang ZW, Huppe-Gourgues F, Dufresne MM, Vaucher E, Sullivan RM (2012) Cholinergic depletion in nucleus accumbens impairs mesocortical dopamine activation and cognitive function in rats. Neuropharmacology 63:1075–1084
Schilman EA, Klavir O, Winter C, Sohr R, Joel D (2010) The role of the striatum in compulsive behavior in intact and orbitofrontal-cortex-lesioned rats: possible involvement of the serotonergic system. Neuropsychopharmacology 35:1026–1039
Dobbs LK, Mark GP (2012) Acetylcholine from the mesopontine tegmental nuclei differentially affects methamphetamine induced locomotor activity and neurotransmitter levels in the mesolimbic pathway. Behav Brain Res 226:224–234
Mark GP, Shabani S, Dobbs LK, Hansen ST (2011) Cholinergic modulation of mesolimbic dopamine function and reward. Physiol Behav 104:76–81
Porrino LJ, Lyon D, Smith HR, Daunais JB, Nader MA (2004) Cocaine self-administration produces a progressive involvement of limbic, association, and sensorimotor striatal domains. J Neurosci 24:3554–3562
Volkow ND, Fowler JS, Wang GJ, Swanson JM (2004) Dopamine in drug abuse and addiction: results from imaging studies and treatment implications. Mol Psychiatry 9:557–569
Nummenmaa L, Hirvonen J, Hannukainen JC, Immonen H, Lindroos MM, Salminen P, Nuutila P (2012) Dorsal striatum and its limbic connectivity mediate abnormal anticipatory reward processing in obesity. PLoS ONE 7:e31089
Muskens JB, Schellekens AF, de Leeuw FE, Tendolkar I, Hepark S (2012) Damage in the dorsal striatum alleviates addictive behavior. Gen Hosp Psychiatry 34:702 e709–702 e711
Everitt BJ, Robbins TW (2013) From the ventral to the dorsal striatum: devolving views of their roles in drug addiction. Neurosci Biobehav Rev 37:1946–1954
Lee DK, Oh JH, Shim YB, Choe ES (2013) Protein kinase G regulates dopamine release, DeltaFosB expression, and locomotor activity after repeated cocaine administration: involvement of dopamine D2 receptors. Neurochem Res 38:1424–1433
Natori S, Yoshimi K, Takahashi T, Kagohashi M, Oyama G, Shimo Y, Hattori N, Kitazawa S (2009) Subsecond reward-related dopamine release in the mouse dorsal striatum. Neurosci Res 63:267–272
Hermann D, Weber-Fahr W, Sartorius A, Hoerst M, Frischknecht U, Tunc-Skarka N, Perreau-Lenz S, Hasson AC, Krumm B, Kiefer F, Spanagel R, Mann K, Ende G, Sommer WH (2012) Translational magnetic resonance spectroscopy reveals excessive central glutamate levels during alcohol withdrawal in humans and rats. Biol Psychiatry 71:1015–1021
Koob GF (2013) Theoretical frameworks and mechanistic aspects of alcohol addiction: alcohol addiction as a reward deficit disorder. Curr Top Behav Neurosci 13:3–30
Bennett MR, Balcar VJ (1999) Forty years of amino acid transmission in the brain. Neurochem Int 35:269–280
Šerý O, Sultana N, Kashem MA, Pow DV, Balcar VJ (2015) GLAST but not least-distribution, function, genetics and epigenetics of l-glutamate transport in brain-focus on GLAST/EAAT1. Neurochem Res 40:2461–2472. doi:10.1007/s11064-015-1605-2
Valenzuela CF (1997) Alcohol and neurotransmitter interactions. Alcohol Health Res World 21:144–148
Lee DW, Nam YK, Kim TK, Kim JH, Kim SY, Min JW, Lee JH, Kim HY, Kim DJ, Choe BY (2014) Dose-dependent influence of short-term intermittent ethanol intoxication on cerebral neurochemical changes in rats detected by ex vivo proton nuclear magnetic resonance spectroscopy. Neuroscience 262:107–117
Rae CD, Davidson JE, Maher AD, Rowlands BD, Kashem MA, Nasrallah FA, Rallapalli SK, Cook JM, Balcar VJ (2014) Ethanol, not detctably metabolized in brain, significantly reduces brain metabolism, probably via action at specific GABA(A) receptors and has measurable metabolic effects at very low concentrations. J Neurochem 129:304–314
Spanagel R (2009) Alcoholism: a system approach from molecular physiology to addictive behaviour. Physiol Rev 89:649–705
Brabant C, Alleva L, Quertemont E, Tirelli E (2010) Involvement of the brain histaminergic system in addiction and addiction-related behaviors: a comprehensive review with emphasis on the potential therapeutic use of histaminergic compounds in drug dependence. Prog Neurobiol 92:421–441
McBride WJ, Murphy JM, Lumeng L, Li TK (1990) Serotonin, dopamine and GABA involvement in alcohol drinking of selectively bred rats. Alcohol 7:199–205
Vilpoux C, Warnault V, Pierrefiche O, Daoust M, Naassila M (2009) Ethanol-sensitive brain regions in rat and mouse: a cartographic review, using immediate early gene expression. Alcohol Clin Exp Res 33:945–969
Jacobsen JP, Siesser WB, Sachs BD, Peterson S, Cools MJ, Setola V, Folgering JH, Flik G, Caron MG (2012) Deficient serotonin neurotransmission and depression-like serotonin biomarker alterations in tryptophan hydroxylase 2 (Tph2) loss-of-function mice. Mol Psychiatry 17:694–704
Sachs BD, Salahi AA, Caron MG (2014) Congenital brain serotonin deficiency leads to reduced ethanol sensitivity and increased ethanol consumption in mice. Neuropharmacol 77:177–184
Higley JD, King ST Jr, Hasert MF, Champoux M, Suomi SJ, Linnoila M (1996) Stability of interindividual differences in serotonin function and its relationship to severe aggression and competent social behavior in rhesus macaque females. Neuropsychopharmacology 14:67–76
Murphy JM, McBride WJ, Lumeng L, Li TK (1982) Regional brain levels of monoamines in alcohol-preferring and -nonpreferring lines of rats. Pharmacol Biochem Behav 16:145–149
Borg S, Kvande H, Liljeberg P, Mossberg D, Valverius P (1985) 5-Hydroxyindoleacetic acid in cerebrospinal fluid in alcoholic patients under different clinical conditions. Alcohol 2:415–418
Kohnke MD, Zabetian CP, Anderson GM, Kolb K, Gaertner I, Buchkremer G, Vonthein R, Schick S, Lutz U, Kohnkee AM, Cubells JF (2002) A genotype-controlled analysis of plasma dopamine beta-hydroxylase in healthy and alcoholic subjects: evidence for alcohol-related differences in noradrenergic function. Biol Psychiatry 52:1151–1158
Rothblat DS, Rubin E, Schneider JS (2001) Effects of chronic alcohol ingestion on the mesostriatal dopamine system in the rat. Neurosci Lett 300:63–66
McBride WJ, Schultz JA, Kimpel MW, McClintick JN, Wang M, You J, Rodd ZA (2009) Differential effects of ethanol in the nucleus accumbens shell of alcohol-preferring (P), alcohol-non-preferring (NP) and Wistar rats: a proteomics study. Pharmacol Biochem Behav 92:304–313
McPherson CS, Lawrence AJ (2007) The nuclear transcription factor CREB: involvement in addiction, deletion models and looking forward. Curr Neuropharmacol 5:202–212
Asanuma M, Nishibayashi S, Iwata E, Kondo Y, Nakanishi T, Vargas MG, Ogawa N (1996) Alterations of cAMP response element-binding activity in the aged rat brain in response to administration of rolipram, a cAMP-specific phosphodiesterase inhibitor. Brain Res Mol Brain Res 41:210–215
Lonze BE, Ginty DD (2002) Function and regulation of CREB family transcription factors in the nervous system. Neuron 35:605–623
Platenik J, Balcar VJ, Yoneda Y, Mioduszewska B, Buchal R, Hynek R, Kuramoto N, Wilczynski G, Ogita K, Nakamura Y, Kaczmarek L (2005) Apparent presence of Ser133-phosphorylated cyclic AMP response element binding protein (pCREB) in brain mitochondria is due to cross-reactivity of pCREB antibodies with pyruvate dehydrogenase. J Neurochem 95:1446–1460
Acknowledgments
This work was supported by NSW Health Drug and Alcohol Research Scheme (MAK) and by NHMRC, Australia (VJB). Tissues were provided NSW brain bank (supported by the University of Sydney, NISAD, NIAAA and NSW Department of Health).
Author information
Authors and Affiliations
Corresponding author
Additional information
Mohammed Abul Kashem and Selina Ahmed have contributed equally to this work.
Rights and permissions
About this article
Cite this article
Kashem, M.A., Ahmed, S., Sultana, N. et al. Metabolomics of Neurotransmitters and Related Metabolites in Post-Mortem Tissue from the Dorsal and Ventral Striatum of Alcoholic Human Brain. Neurochem Res 41, 385–397 (2016). https://doi.org/10.1007/s11064-016-1830-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11064-016-1830-3