Abstract
Nitric oxide (NO) regulates numerous physiological process and is the main source of reactive nitrogen species (RNS). NO promotes cell survival, but it also induces apoptotic death having been involved in the pathogenesis of several neurodegenerative diseases. NO and superoxide anion react to form peroxynitrite, which accounts for most of the deleterious effects of NO. The mechanisms by which these molecules regulate the apoptotic process are not well understood. In this study, we evaluated the role of NO and peroxynitrite in the apoptotic death of cultured cerebellar granule neurons (CGN), which are known to experience apoptosis by staurosporine (St) or potassium deprivation (K5). We found that CGN treated with the peroxynitrite catalyst, FeTTPs were completely rescued from St-induced death, but not from K5-induced death. On the other hand, the inhibition of the inducible nitric oxide synthase partially protected cell viability in CGN treated with K5, but not with St, while the inhibitor L-NAME further reduced the cell viability in St, but it did not affect K5. Finally, an inhibitor of the soluble guanylate cyclase (sGC) diminished the cell viability in K5, but not in St. Altogether, these results shows that NO promotes cell survival in K5 through sGC-cGMP and promotes cell death by other mechanisms, while in St NO promotes cell survival independently of cGMP and peroxynitrite results critical for St-induced death. Our results suggest that RNS are differentially handled by CGN during cell death depending on the death-inducing conditions.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Apoptosis is a type of programmed cell death that participates in the modelling of structures during development, the elimination of activated immune cells and transformed cells, among other processes. This is a fundamental and dynamic biological phenomenon characterized by DNA fragmentation, chromatin condensation, activation of caspases, translocation of phosphatidylserine and formation of apoptotic bodies [1–6]. It has been suggested that the production of reactive oxygen species (ROS) is critical for the initial phase of the apoptotic process. There are several reports showing that ROS are required for the progression of apoptotic death in neurons and glial cells [7–11].
On the other hand, reactive nitrogen species (RNS) have also been associated with the molecular mechanisms involved in the apoptotic cell death process [12, 13]. RNS are generated by nitric oxide synthases (NOS), which produce nitric oxide from l-arginine and oxygen. NO is a free radical and it is the main source for other RNS [14]. It is present in all tissues including the nervous system, where it serves major physiological roles such as synaptic plasticity, regulation of cerebral blood flow, modulation of neuroendocrine functions, among others [15].
Both, ROS and RNS are intimately related and may interact to induce the formation of reactive species that result critical for the apoptotic cell death. The imbalance of ROS levels increase the number of reactions between ROS and RNS, leading to nitrosative stress. The main reaction is the formation of peroxynitrite, which is produced by the reaction between nitric oxide and superoxide anion [14]. Peroxynitrite is a highly reactive molecule that may induce alterations of macromolecules [16, 17] and induce apoptosis in a variety of cell types including neurons [12, 18]. In fact, some of the deleterious actions of nitric oxide in neurons can be attributed to the formation of peroxynitrite [19]. Furthermore, this molecule has been described to be critical for the mechanisms of neuronal injury in a variety of neurodegenerative diseases, such as Alzheimer’s disease, Parkinson’s disease and amyotrophic lateral sclerosis [14, 20].
The actions of peroxynitrite are not limited to cell damage, low levels of peroxynitrite lead to the activation of Akt and by this way it may influence cell survival [21]. Both, nitric oxide and peroxynitrite are able to induce cell survival or cell death depending on the cell type and the cell context [22–25]. However, in contrast to ROS, there is little and controversial information about the possible role of RNS in the apoptotic cell death process and the mechanisms by which peroxynitrite induces apoptosis in neurons are unclear. For these reasons, in the present study, we assessed the participation of RNS during the apoptotic death of cerebellar granule neurons (CGN). These cells undergo apoptosis when they are treated with staurosporine (St), an inhibitor of protein kinases, or when they are transferred from a 25 mM [K+]-containing medium (K25) to a medium containing 5 mM [K+] (K5) [1–3, 26, 27]. The apoptotic process induced by these conditions is accompanied by the early production of ROS, suggesting that ROS could be critical in this process and raises the possibility that they could constitute an early signal in the apoptotic death of CGN [9, 28]. This possibility has been further strengthened by the observation that antioxidant treatment prevents cell death and that ROS can directly induce apoptotic death [10, 28–30].
In these model of apoptotic death, there is no substantial information about the role of nitric oxide, neither the possible involvement of peroxynitrite. To assess this, we induced apoptosis in CGN by St treatment and potassium deprivation and we examined the cell survival, apoptotic parameters and the levels of tyrosine nitration in the presence of a peroxynitrite decomposition catalyst 5,10,15,20-tetrakis(4-sulfonatophenyl)porphyrinato iron III chloride (FeTPPS) and NOS inhibitors.
Materials and Methods
Materials
Fetal calf serum and penicillin/streptomycin were from GIBCO (Grand Island, NY, USA). Calcein-AM was from Invitrogen, Molecular Probes (Eugene, OR, USA). Poly-l-lysine (molecular weight_300,000), 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide (MTT), propidium iodide (PI), cytosine-d-arabino-furoanoside and staurosporine (St) were from Sigma (St Louis, MO, USA). FeTTPs was from Calbiochem, Merck. Others chemicals were of the purest grade available from regular commercial sources.
Cerebellar Granule Neurons Cultures
All animal used for the experimentation described in the present study were treated in accordance with the accepted standards of animals care and with the procedures approved by the local Committee of Research and Ethics of the Instituto de Fisiología Celular, Universidad Nacional Autónoma de México. The protocol used followed the Guidelines for the Care and Use of Mammals in Neuroscience as well as guidelines released by the Mexican Institutes of Health Research and the National Institutes of Health guide for the care and use of Laboratory animals. All efforts were made to minimize animal suffering, and to reduce the number of animals used.
CGN cultures were prepared as previously described [31]. Briefly, cell suspensions dissociated from 7-day-old rat cerebellum were plated at a density of 265 × 103 cells/cm2 in plastic dishes or coverslips coated with poly-l-lysine (5 µg/ml) and were maintained for 7 days in vitro (DIV). Culture medium contained basal Eagle’s medium supplemented with 10 % (v/v) heat-inactivated fetal calf serum, 2 mM glutamine, 25 mM KCl, 50 U/ml penicillin and 50 mg/ml streptomycin. This medium is referred in text as K25 and is the control condition. The culture dishes were incubated at 37 °C in a humidified 5 % CO2/95 % air atmosphere. To avoid non-neuronal cells, cytosine arabinoside (10 mM) was added 24 h after seeding. Cell death was induced by treating cells with staurosporine (St) (0.5 μM) or by transferring cells to a medium containing 5 mM KCl (K5). In some experiments, FeTTPs or NOS inhibitors were added simultaneously with K5 or St, and they were present until the end of the experiment.
Cell Viability
Cell viability was estimated by calcein and propidium iodide staining and by MTT transformation. Calcein enters to viable cells and emits green fluorescence when it is cleaved by esterases and cannot be longer permeable to cell membranes. Propidium iodide is not permeable to cell membranes and only death cells are stained. CGN were incubated with 2.5 µM calcein-AM and 2 µM and propidium iodide for 10 min at 37 °C, and then cells were photographed in a fluorescence microscope using filters with the following characteristics: excitation filter wavelength/dichromatic mirror cut-on wavelength/barrier filter wavelengths of 450–490/500/515 and 510–560/565/590 nm for calcein and propidium iodide, respectively. Subsequent analysis involved the determination of calcein-positive cells from at least two different images for each condition. Results are expressed as the percentage of viable cells (calcein-positive cells) from the total number of cells (calcein-positive cells + propidium iodide-positive cells) evaluated per field.
CGN were incubated with MTT (0.5 mg/ml) for15 min in the culture medium at 37 °C. After incubation, the formazan crystals formed from MTT transformation were extracted with DMSO (100 %) and quantified spectroscopically at 560 nm. There was a good correspondence between MTT and calcein incorporation assays.
Nuclear Condensation
Cells were plated on coverslips and cultured for 7 days in vitro (DIV) and then treated to induce apoptosis. After 24 h of treatment, cells were fixed in 4 % paraformaldehyde for 20 min, and then incubated with Hoechst 332558 (0.01 %) in PBS for 5 min. Cells were examined with an epifluorescence microscope using a filter with following characteristics: excitation filter wavelength/dichromatic mirror cut-on wavelength/barrier filter wavelengths of 340/400/460 nm. Three different photographs taken at random were analyzed for each condition.
Caspase 3 Activity
After St treatment, CGN were washed with cold PBS and homogenized in lysis buffer [Tris–HCl (10 mM), NaH2PO4 (10 mM), NaCl (130 mM) and triton (1 %)]. Caspase 3 activity was determined by adding Ac-DEVD-MCA (Peptide Institute, Japan) diluted in an equal volume of reaction buffer [HEPES (40 mM), DTT (2 mM) and Ac-DEVD-MCA (20 µM)]. Fluorescence recording and the injection of the reaction buffer were performed with the microplate reader Synergy HT (BioTek Instruments, USA). Data were adjusted with protein concentration and normalized with respect to control.
Nitrosylation of Tyrosine Residues by Dot Blot Analysis
After 4, 8, 12 and 24 h of K5 or staurosporine (0.5 μM) treatment, CGN were washed with 37 °C PBS and homogenized in lysis buffer [25 mM Tris–HCl, 50 mM NaCl, 1 % (v/v) NP-40, 0.2 % (w/v) SDS, complete protease inhibitor cocktail], and the homogenates (30 μg of protein per lane) were spotted through circular templates directly onto the nitrocellulose membrane (BIO-RAD, Trans-Blot) using dot camera during 30 min. Then, the membranes were dry and blocked 1 h with 5 % nonfat dry milk in TBS buffer, and then incubated overnight at 4 °C with the primary antibody against Nitro-Tyrosine proteins and peptides containing nitro-tyrosine (Cell Signalling, Technology, USA, #9691).
Statistical Analysis
Statistical analysis was done by using SigmaPlot 12.1 software. Data are expressed as mean ± SEM. Pairwise comparison within multiples groups was done by analysis of variance (ANOVA) followed by the Tukey post hoc test; p values <0.05 were considered statistically significant.
Results
Peroxynitrite Mediates CGN Death Induced by St but not by Potassium Deprivation
In order to determine the role of RNS in the apoptotic death of CGN, firstly we assayed two apoptotic cell death models, St treatment and potassium deprivation. These conditions, induce in CGN the acquisition of different apoptotic characteristics such as caspase activation, DNA fragmentation, nuclear condensation and cytochrome c release, among others [27, 32]. These characteristics are accompanied by the early production of ROS, which is determinant for the completion of the apoptotic cell death process [9, 28]. Figure 1a, b show that the cell viability of CGN diminished in a time dependent manner under St treatment or when cells were transferred from depolarizing concentrations of potassium chloride (25 mM, referred as K25) to non-depolarizing concentrations of potassium chloride (5 mM, referred as K5). Under these conditions, the cell viability, seen by MTT transformation, diminished around 30–40 % at 12 h and 40–50 % at 24 h. After 24 and 48 h, the cell viability diminished around 10–20 %. Similar results were observed when the cell viability was evaluated by calcein staining (Fig. 1c) by showing that the cell viability diminished around 30–50 % at 24 h, corroborating that by 24 h, an important percentage of CGN had already died. The cell viability reduction could be observed by the morphological changes that CGN experienced during the apoptotic process. In control conditions, CGN had rounded cell bodies that tended to aggregate and from these aggregates numerous bundled processes were extended. When CGN are transferred to K5 or they are treated with St for 24 h, approximately half of the cell bodies shrank and the processes began to degenerate, which was more evident in St treated cells. After 48 h, almost all the cell bodies were shrunken and the processes were completely damaged (Fig. 1a).
Effect of K5 and staurosporine on the cell viability of CGN. a Representative micrographs of CGN of 7 DIV grown in depolarizing conditions (K25, Control) and transferred to non-depolarizing conditions (K5), or treated with St (0.5 µM) for the indicated times. b Cells were cultured for 7 DIV in (K25) and then transferred to K5 or treated with St (0.5 µM), and cell viability was evaluated by MTT transformation after 6, 12, 24 and 48 h or c after 24 h by calcein staining. Data are presented as mean ± SEM of 6 independent experiments (b) and 3 independent experiments (c). *Significantly different from control (p < 0.05, ANOVA)
One of the most oxidative molecules produced by the reaction between RNS and ROS is peroxynitrite [33], which is known to induce apoptosis [12, 18]. For this reason, we studied whether this molecule was implicated in the apoptotic process induced by St and potassium deprivation. Figure 2a shows the normal morphology of CGN in phase contrast microcopy and the viable cells stained with calcein and non-viable cells labeled with propidium iodide staining. Under St treatment, the number of calcein-positive cells diminished and the correspondingly member of propidium iodide-positive cells increased. This effect was completely reverted by FeTTPs co-treatment. FeTTPs catalyzes the isomerization of peroxynitrite to nitrate [34]. Figure 2b shows that when CGN were treated with St for 24 h, the cell viability diminished around 45 %, which was completely rescued by FeTTPs. We tested different concentrations of FeTTPs, ranging from 1 to 100 µM, and only 100 µM FeTTPs completely rescued from cell death (not shown). Interestingly, when we added FeTTPs 12 h after the St treatment, we found that FeTTPs was still able to protect CGN from cell death, indicating that the effect of FeTTPs occurs after initiated the apoptotic process induced by St (Fig. 2c). In contrast, in the potassium deprivation model, FeTTPs (100 µM) induced the complete death of CGN and lower concentrations of FeTTPs, ranged from 0.1 to 10 µM, had no effect on cell viability (only FeTTPs 1 µM is shown), suggesting that peroxynitrite have little or no effect in the apoptotic process and showing a protective effect (Fig. 3a, b). This can be observed in the calcein staining assays where almost no calcein-positive cells were present under potassium deprivation and FeTTPs (100 µM) treatment (Fig. 3a).
Effect of FeTTPs on the CGN death induced by St. a Representative micrographs of CGN labelled with calcein and propidium iodide as detailed in Methods. CGN of 7 DIV grown in depolarizing conditions (K25, Control) treated with St (0.5 µM) for 24 h or St (0.5 µM) plus FeTTPs (100 µM) for 24 h. Panels are phase contrast images, calcein stained cells and propidium iodide stained cells. b Quantification of the cell viability of the CGN shown in (a). Data are presented as mean ± SEM of 3 independent experiments. *Significantly different from St (p < 0.05, ANOVA). c Quantification of the cell viability of CGN treated with St (0.05 µM) for 24 h plus FeTTPs (100 µM) for 12 h. Data are presented as mean ± SEM of 3 independent experiments. *Significantly different from St (p < 0.05, ANOVA)
Effect of FeTTPs on the CGN death induced by K5. a Representative micrographs of CGN labelled with calcein and propidium iodide as detailed in methods. CGN of 7 DIV were grown in depolarizing conditions (K25, Control) and transferred to non-depolarizing conditions (K5) for 24 h with or without FeTTPs (100 µM) for 24 h. Panels are phase contrast images, calcein stained cells and propidium iodide stained cells. b Quantification of the cell viability of CGN grown in K25 and transferred to K5 with or without different concentrations of FeTTPs (11 and 100 µM). Data are presented as mean ± SEM of 4 independent experiments. No significant differences were found between K5 and FeTTPs treatments (ANOVA)
Peroxynitrite Inhibits Caspase 3 Activity and Nuclear Condensation Under St Treatment
Two hallmark characteristics of the apoptotic process are nuclear condensation and the activation of the executioner caspase 3. Figure 4a shows that both, St treatment and potassium deprivation induced nuclear condensation of CGN after 24 h. Correspondently with the cell viability assays, FTTPs (100 µM) prevented the nuclear condensation only in St treatment and it reduced the total number of nuclei in potassium deprivation, but not the condensed nuclei. St increased by 60 % the number of condensed nuclei and FeTTPs significantly diminished this number (Fig. 4b). We also explored the possibility that the effect of FeTTPs in the apoptotic death induced by St occurs through the regulation of the caspase 3 activation. Figure 4c shows that St induced the activation of caspase 3 at early stages of the apoptotic process. After 2 h of treatment, the activity increased around threefold and continued increasing gradually, reaching a peak at 10 h. Caspase 3 activity was markedly reduced by FeTTPs, even when this compound were incubated after 2-4 h of St treatment, suggesting that the effect of FeTTPs is upstream of caspase 3 activation.
Effect of FeTTPs on the nuclear condensation induced by K5 and St and in the caspase 3 activity induced by St. a Representative micrographs of CGN stained with Hoechst 33258 as detailed in Methods. CGN of 7 DIV were grown in depolarizing conditions (K25) and transferred to non-depolarizing conditions (K5) or treated with St for 24 h with or without FeTTPs (100 µM). b Quantification of the St treatment shown in (a). Data are presented as mean ± SEM of 3 independent experiments. *Significantly different from St (p < 0.05, ANOVA). c Caspase 3 activity was evaluated as detailed in methods. CGN of 7 DIV were treated with St (0.5 µM) for 2, 4, 6, 8, 10 and 12 h and St (0.5 µM) for 12 h plus FeTTPs (100 µM) for 10 and 8 h and caspase 3 was evaluated. Date are presented as mean ± SEM of 4 independent experiments. *Significantly different from St 12 h (p < 0.05, ANOVA)
Tyrosine Nitration Induced by St and Potassium Deprivation is Reduced by FeTTPs
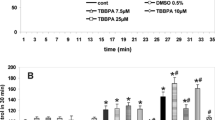
RNS induce different posttranslational modifications that includes S-nitrosylation, glutathionylation and tyrosine nitration, among which, tyrosine nitration is mainly mediated by peroxynitrite [14]. Here we found that both. St and potassium deprivation induced an increase of tyrosine nitration after 8 h, which was sustained until 24 h. After 4 h, the levels of tyrosine nitration in K5 and St were similar to control. Interestingly, under both conditions, FeTTPs (100 µM) markedly reduced the levels of tyrosine nitration (Fig. 5). These results demonstrated the production of peroxynitrite under these apoptotic conditions.
Effect of FeTTPs on tyrosine nitration induced by K5 and St. Representative blot of tyrosine nitrated proteins extracted from CGN of 7 DIV grown in depolarizing conditions (K25), or transferred to non-depolarizing conditions (K5) or treated with St (0.5 µM) for the indicated times. Cells were cultured for 7 DIV in (K25) and then transferred to K5 or treated with St (0.5 µM) for 4, 8 and 24 h with or without FeTTPs (100 µM) for 24 h. Cell lysates (30 µg of protein per line) were directly transferred to a nitrocellulose membrane by using a dot camera. Three independent experiments were performed
Nitric Oxide Inhibition Shows Differential Effects on the Death Induced by St and Potassium Deprivation
Finally, we tested the role of nitric oxide in the apoptotic death process, since this molecule might play a dual role in cell survival, On one hand, nitric oxide is the precursor of peroxynitrite and it is known that nitric oxide can cause neuronal death [35], which could be independent of peroxynitrite formation [36]. On the other hand, nitric oxide may have a neuroprotective effect through cGMP production in different models [37, 38]. In order to understand the role of nitric oxide in the apoptotic process induced by St and K5, we tested different NOS inhibitors and an inhibitor of the soluble guanylate cyclase in CGN survival under control and apoptotic conditions. Different concentrations of L-NAME (100, 200 and 500 µM) did not alter the overall appearance of the cell culture (Fig. 6a), or reduced the cell viability of cells (Fig. 6b) or protected against the cell death induced by potassium deprivation or St (Fig. 6c (only l-NAME 500 µM is shown). Even higher concentrations of L-NAME (1–10 mM) did not protect against the cell death induced by potassium deprivation and St (Table 1). Only 10 mM L-NAME reduced cell viability in control conditions and with St treatment (Table 1). L-NAME is a competitive inhibitor of endothelial NOS (IC50 10 µM), neuronal NOS (IC50 60 µM) and inducible NOS (IC50 11.5 µM), once this molecule is hydrolyzed by esterases inside the cells, it is converted into L-NNA and interact non-covanlently with all NOS. The union of this molecule with endothelial NOS (eNOS) and neuronal NOS (nNOS) is more stable than the union with the inducible NOS (iNOS) [39], conferring certain selectivity of eNOS and nNOS over iNOS, thereby the observed effects seen in St and K5 are probably are related to the activation of the iNOS.
Effect of L-NAME on the cell death induced by K5 and St. a Representative micrographs of CGN labelled with calcein and propidium iodide as detailed in Methods. CGN of 7 DIV were grown in depolarizing conditions (K25) and transferred to non-depolarizing conditions (K5) for 24 h or treated with St (100 µM) plus L-NAME (500 µM) for 24 h. b CGN of 7 DIV were grown in K25 and treated with DMSO (0.8 % v/v) for 24 h, or L-NAME (500 µM). Data are presented as mean ± SEM of 5 independent experiments. No significant differences were found between the treatments (ANOVA). c Cell viability was measured by calcein staining in CGN of 7 DIV grown in depolarizing conditions (K25) and transferred to non-depolarizing conditions (K5) for 24 h and treated with L-NAME (500 µM) for 24 h or d treated with St (0.5 µM) for 24 h and L-NAME (500 µM) for 24 h. Data are presented as mean ± SEM of 5 (c) and 4 (d) independent experiments. No significant differences were found between the treatments (ANOVA)
To evaluate this possibility, we tested two non-selective NOS inhibitors, 2-ethyl-2-thiopseudourea hydrobromide (EPTU, IC50 values for eNOS, nNOS and iNOS of 0.37, 0.25 and 0.13 µM, respectively) and 7-nitroindazole (7-NI, IC50 values for eNOS, nNOS and iNOS of 0.78, 0.71 and 5.8 µM, respectively). Table 1 shows that the cell viability measured by MTT was slightly reduced by EPTU and 7-NI in control cells at the higher concentrations used. In K5 treated cells, EPTU, but not 7-NI, increased the cell viability. No significant changes were observed in the group treated with St and EPTU or 7-NI. These results suggest that nitric oxide is required for cell survival in control conditions and probably under St treatment. On the other hand, nitric oxide might be necessary for the process of cell death induced by K5. We found a tendency of the inhibitors EPTU and L-NAME (10 mM) to reduce the cell viability in St treatment, which suggest that nitric oxide might have a pro-survival effect under this condition.
The main signaling pathway activated by nitric oxide involves soluble guanylate cyclases (sGC) that seems to be involved in the neuroprotective effects exerted by nitric oxide [37, 38]. To clarify the possibility that some of the above described actions of NO are mediated by sGC, we tested the effect of ODQ, a specific inhibitor of sGC, on the cell viability measured as MTT transformation. Table 1 shows that ODQ treatment reduced the cell viability only under K5 conditions, suggesting a possible protective action of the nitric oxide-cGMP pathway in the K5-induced cell. Similar results were obtained when viability was evaluated with calcein and propidium iodide staining (data not shown).
Discussion
In the present study we found that the neuronal apoptotic death may show different molecular mechanisms depending on the initial mechanism for the induction of apoptotic cell death. Particularly, we showed that reactive species play a differential role when cells are treated with two different apoptotic conditions in the same cell type. In previous studies we and others showed that ROS play a critical role acting as signals in apoptotic death of CGN induced by both K5 and St [7, 9, 30, 40]. Here, we further suggest that peroxynitrite is necessary for the progression of apoptosis induced by St, and that in the case of K5-induced death it might act as an anti-apoptotic molecule.
These results are in line with some of our previous studies in which we found differences in the signaling pathways involved in the apoptotic process induced by these two conditions. For example, we demonstrated that JNK and p38 pathways mediate the apoptotic death of CGN induced by K5, but cell death induced by St is mediated only by p38 [7, 8]. Also, in contrast to K5-induced cell death, the ROS generation in St-induced death is downstream of p38 activation. Our present results showed a marked neuroprotective action of the peroxynitrite decomposition catalysts FeTTPs in CGN treated with St. These results are in agreement with the observed effect of FeTTPs on the apoptotic parameters evaluated, nuclear condensation and caspase 3 activity.
In contrast to St, FeTTPs did not modify any of the evaluated apoptotic parameters under K5 conditions. Moreover, this compound markedly increased the cell death induced by K5 suggesting a possible protective action of peroxynitrite under these conditions. The idea that peroxynitrite may be beneficial has previously been proposed in other models of brain injury induced by NMDA [41] and excitotoxicity mediated by glutamate [42], as well as in a model of myocardial ischemic postconditioning followed by episodes of ischemia–reperfusion injury [25].
An interesting result from our study was the observed protective effect of FeTTPs when it was administered to CGN after long periods of St treatment, which corresponds with a time when caspase 3 is already active. A similar delayed neuroprotective action of FeTTPs has been shown in a model of cerebral ischemia [43]. One possibility to explain this delayed action is that peroxynitrite could be acting upstream or directly on active caspase 3 and therefore reducing the effects of the apoptotic process. It is well established that S-nitrosylation and denitrosylation of proteins can be an important mechanism to modify the function of several proteins [44, 45]. Caspase 3 activity can be regulated by nitrosylation [46], tyrosine nitration and glutathionylation [47], which are events mediated by RNS [14]. It is known that thioredoxin induces transnitrosylation of Cys163 of caspase 3 and by this way it inhibits caspase activity [48]. Peroxynitrite can also regulate caspase 3 activity in a different way. For example, peroxynitrite induces caspase 3 activation in a model of spinal cord injury [49] and in a model of cerebral ischemia [50], but it also induces its inactivation by tyrosine nitration of caspase 3 in a model of traumatic brain injury [51]. These studies show that peroxynitrite may exert different actions on caspase 3 activation through posttranslational modifications.
In support of this idea, it has been shown in skeletal muscle that low exogenous levels of peroxynitrite (0.1 mM) inactivate the sarco/endoplasmic reticulum calcium (Ca2+) ATPase (SERCA) by inducing nitrosylation of the Cys349, probably mediated by a direct interaction of peroxynitrite on the molecule or by transnitrosylation through the initial modification of other cysteine residues [52]. In contrast, physiological levels of peroxynitrite in smooth muscle increase the activity of SERCA by reversible glutathionylation of this protein [53]. These results demonstrate that peroxynitrite may mediate tyrosine nitration, as well as nitrosylation and glutathionylation of cysteine residues in a variety of proteins, but more importantly, these studies show that the levels of peroxynitrite may determine its role in the activity/inactivity state of the protein. Based on these evidences and due to the fact that FeTTPs reduced the caspase 3 activity at a time when caspase 3 was highly active and that peroxynitrite catalysis exacerbates the cell death induced by K5, we speculate that peroxynitrite could regulate caspase 3 in these models.
It is interesting that both, K5 and St induced a clear increase in the levels of tyrosine nitrated proteins, which was markedly reduced by FeTTPs in both cases. As discussed above, FeTTPs only inhibited the apoptotic process induced by St, but not by K5. These results firstly suggest that both St and K5 induce peroxynitrite formation; and secondly that peroxynitrite may have differential roles. In the case of St, it is possible that peroxynitrite could induce apoptotic death through the tyrosine nitration, nitrosylation or glutathionylation of proteins. In fact, peroxynitrite induce tyrosine nitration of cytochrome c [54], cytochrome c release [55] and the activation of caspases 8 and 9 [55], which probably mediates caspase 3 activation. In the case of K5, peroxynitrite may induce tyrosine nitration or cysteine nitrosylation of caspase 3, therefore promoting an anti-apoptotic effect. Further experiments will be required to elucidate these possibilities.
It has been reported that nitric oxide may induce cell death by different mechanisms. Nitric oxide can produce damage either by a direct action on proteins or through peroxynitrite. We therefore investigated the possible role of nitric oxide in the process of cell death induced by both, K5 and St. Our results showed that all NOS inhibitors failed to rescue CGN from cell death induced by St, suggesting that nitric oxide does not promote cell death, which could be apparently contradictory to the results on peroxynitrite requirement for St-induced death, since peroxynitrite is a product of nitric oxide [33]. This can be explained by a possible generation of nitric oxide mediated by S-nitrosothiols that can act as nitric oxide reservoirs [56]. On the other hand, L-NAME further increased the cell death induced by St. Interestingly, all NOS inhibitors tested reduced the cell viability of CGN maintained in basal conditions. These results suggest that under these conditions nitric oxide could exert a neuroprotective action. This possibility has been extensively documented in several preparations, including developing CGN [22, 57, 58] and mature CGN [38, 59–61].
In contrast to St, the inhibition of NOS by EPTU, significantly reduced the cell death induced by K5, which support the idea that nitric oxide could be necessary for the apoptotic death induced by this condition. Thus, as previously mentioned, nitric oxide could play a dual action in our preparation. On one side, it may act as a physiological and neuroprotective agent probably by activating the cGMP/PKG cascade [38, 59] or through some other no-cGMP-dependent function of nitric oxide [62, 63]. On the other hand, nitric oxide and its derivative peroxynitrite could directly interact with several proteins, which could lead to alterations in their function, resulting in cell death, as it could be the case for the K5-induced cell death mediated by nitric oxide or the St-induced death mediated by peroxynitrite.
Finally, we explored the possibility that cGMP/PKG cascade could mediate the protective effect of nitric oxide in St-induced death. Our results using ODQ showed no changes in the cell viability, suggesting that the neuroprotective action of nitric oxide in this condition is not mediated by this cascade. However, ODQ treatment diminished the cell viability in K5, suggesting that the cGMP/PKG cascade promotes cell survival in this model. These results show a dual role of nitric oxide in the same model. On one hand, nitric oxide favor K5-induced death in a mechanism independent of the cGMP/PKG cascade. On the other hand, nitric oxide promotes cell survival in K5-induced death, which depends on the cGMP/PKG cascade.
In conclusion, these evidences show a differential regulation of the apoptotic pathway by RNS in the same cell type under two different apoptotic conditions. This suggests that the inductor of apoptotic death determines the initial mechanism involving reactive species. Our results suggest a limited participation of nitric oxide in the apoptotic death induced by St and a partial contribution in the K5-induced death of CGN. In contrast to K5, peroxynitrite seems to play a critical role in the death process induced by staurosporine in cerebellar granule neurons.
References
Moran J, Itoh T, Reddy UR, Chen M, Alnemri ES, Pleasure D (1999) Caspase-3 expression by cerebellar granule neurons is regulated by calcium and cyclic AMP. J Neurochem 73:568–577
Nardi N, Avidan G, Daily D, Zilkha-Falb R, Barzilai A (1997) Biochemical and temporal analysis of events associated with apoptosis induced by lowering the extracellular potassium concentration in mouse cerebellar granule neurons. J Neurochem 68:750–759
D’Mello SR, Galli C, Ciotti T, Calissano P (1993) Induction of apoptosis in cerebellar granule neurons by low potassium: inhibition of death by insulin-like growth factor I and cAMP. Proc Natl Acad Sci USA 90:10989–10993
D’Mello SR, Borodezt K, Soltoff SP (1997) Insulin-like growth factor and potassium depolarization maintain neuronal survival by distinct pathways: possible involvement of PI 3-kinase in IGF-1 signaling. J Neurosci 17:1548–1560
Nicholls DG, Budd SL (2000) Mitochondria and neuronal survival. Physiol Rev 80:315–360
Cohen GM (1997) Caspases: the executioners of apoptosis. Biochem J 326(Pt 1):1–16
Ramiro-Cortes Y, Moran J (2009) Role of oxidative stress and JNK pathway in apoptotic death induced by potassium deprivation and staurosporine in cerebellar granule neurons. Neurochem Int 55:581–592
Ramiro-Cortes Y, Guemez-Gamboa A, Moran J (2011) Reactive oxygen species participate in the p38-mediated apoptosis induced by potassium deprivation and staurosporine in cerebellar granule neurons. Int J Biochem Cell Biol 43:1373–1382
Valencia A, Moran J (2001) Role of oxidative stress in the apoptotic cell death of cultured cerebellar granule neurons. J Neurosci Res 64:284–297
Valencia A, Moran J (2004) Reactive oxygen species induce different cell death mechanisms in cultured neurons. Free Radic Biol Med 36:1112–1125
Olguin-Albuerne M, Dominguez G, Moran J (2014) Effect of staurosporine in the morphology and viability of cerebellar astrocytes: role of reactive oxygen species and NADPH oxidase. Oxid Med Cell Longev 2014:678371
Zhang Y, Wang H, Li J, Jimenez DA, Levitan ES, Aizenman E, Rosenberg PA (2004) Peroxynitrite-induced neuronal apoptosis is mediated by intracellular zinc release and 12-lipoxygenase activation. J Neurosci 24:10616–10627
Shacka JJ, Sahawneh MA, Gonzalez JD, Ye YZ, D’Alessandro TL, Estevez AG (2006) Two distinct signaling pathways regulate peroxynitrite-induced apoptosis in PC12 cells. Cell Death Differ 13:1506–1514
Martinez MC, Andriantsitohaina R (2009) Reactive nitrogen species: molecular mechanisms and potential significance in health and disease. Antioxid Redox Signal 11:669–702
Szabo C (1996) Physiological and pathophysiological roles of nitric oxide in the central nervous system. Brain Res Bull 41:131–141
Szabo C (2006) Poly(ADP-ribose) polymerase activation by reactive nitrogen species–relevance for the pathogenesis of inflammation. Nitric Oxide 14:169–179
Beckman JS (1996) Oxidative damage and tyrosine nitration from peroxynitrite. Chem Res Toxicol 9:836–844
Bonfoco E, Krainc D, Ankarcrona M, Nicotera P, Lipton SA (1995) Apoptosis and necrosis: two distinct events induced, respectively, by mild and intense insults with N-methyl-d-aspartate or nitric oxide/superoxide in cortical cell cultures. Proc Natl Acad Sci USA 92:7162–7166
Beckman JS, Beckman TW, Chen J, Marshall PA, Freeman BA (1990) Apparent hydroxyl radical production by peroxynitrite: implications for endothelial injury from nitric oxide and superoxide. Proc Natl Acad Sci USA 87:1620–1624
Chabrier PE, Demerle-Pallardy C, Auguet M (1999) Nitric oxide synthases: targets for therapeutic strategies in neurological diseases. Cell Mol Life Sci 55:1029–1035
Klotz LO, Schieke SM, Sies H, Holbrook NJ (2000) Peroxynitrite activates the phosphoinositide 3-kinase/Akt pathway in human skin primary fibroblasts. Biochem J 352(Pt 1):219–225
Wang L, Zhu ZA (2014) Nitric oxide show its survival role by NO-PKC pathway through cGMP-dependent or independent on the culture of cerebella granular neurons. Neurosci Lett 583:165–169
Duport S, Garthwaite J (2005) Pathological consequences of inducible nitric oxide synthase expression in hippocampal slice cultures. Neuroscience 135:1155–1166
Erusalimsky JD, Moncada S (2007) Nitric oxide and mitochondrial signaling: from physiology to pathophysiology. Arterioscler Thromb Vasc Biol 27:2524–2531
Li J, Loukili N, Rosenblatt-Velin N, Pacher P, Feihl F, Waeber B, Liaudet L (2013) Peroxynitrite is a key mediator of the cardioprotection afforded by ischemic postconditioning in vivo. PLoS ONE 8:e70331
Gallo V, Kingsbury A, Balazs R, Jorgensen OS (1987) The role of depolarization in the survival and differentiation of cerebellar granule cells in culture. J Neurosci 7:2203–2213
Caballero-Benitez A, Moran J (2003) Caspase activation pathways induced by staurosporine and low potassium: role of caspase-2. J Neurosci Res 71:383–396
Schulz JB, Weller M, Klockgether T (1996) Potassium deprivation-induced apoptosis of cerebellar granule neurons: a sequential requirement for new mRNA and protein synthesis, ICE-like protease activity, and reactive oxygen species. J Neurosci 16:4696–4706
Atlante A, Calissano P, Bobba A, Azzariti A, Marra E, Passarella S (2000) Cytochrome c is released from mitochondria in a reactive oxygen species (ROS)-dependent fashion and can operate as a ROS scavenger and as a respiratory substrate in cerebellar neurons undergoing excitotoxic death. J Biol Chem 275:37159–37166
Sanchez-Carbente MR, Castro-Obregon S, Covarrubias L, Narvaez V (2005) Motoneuronal death during spinal cord development is mediated by oxidative stress. Cell Death Differ 12:279–291
Moran J, Patel AJ (1989) Effect of potassium depolarization on phosphate-activated glutaminase activity in primary cultures of cerebellar granule neurons and astroglial cells during development. Brain Res Dev Brain Res 46:97–105
Guemez-Gamboa A, Moran J (2009) NOX2 mediates apoptotic death induced by staurosporine but not by potassium deprivation in cerebellar granule neurons. J Neurosci Res 87:2531–2540
Valko M, Leibfritz D, Moncol J, Cronin MT, Mazur M, Telser J (2007) Free radicals and antioxidants in normal physiological functions and human disease. Int J Biochem Cell Biol 39:44–84
Jensen MP, Riley DP (2002) Peroxynitrite decomposition activity of iron porphyrin complexes. Inorg Chem 41:4788–4797
Brown GC (2010) Nitric oxide and neuronal death. Nitric Oxide 23:153–165
Fatokun AA, Stone TW, Smith RA (2008) Prolonged exposures of cerebellar granule neurons to S-nitroso-N-acetylpenicillamine (SNAP) induce neuronal damage independently of peroxynitrite. Brain Res 1230:265–272
Estevez AG, Spear N, Thompson JA, Cornwell TL, Radi R, Barbeito L, Beckman JS (1998) Nitric oxide-dependent production of cGMP supports the survival of rat embryonic motor neurons cultured with brain-derived neurotrophic factor. J Neurosci 18:3708–3714
Bonthius DJ, Bonthius NE, Li S, Karacay B (2008) The protective effect of neuronal nitric oxide synthase (nNOS) against alcohol toxicity depends upon the NO-cGMP-PKG pathway and NF-kappaB. Neurotoxicology 29:1080–1091
Vitecek J, Lojek A, Valacchi G, Kubala L (2012) Arginine-based inhibitors of nitric oxide synthase: therapeutic potential and challenges. Mediators Inflamm 2012:318087
Coyoy A, Olguin-Albuerne M, Martinez-Briseno P, Moran J (2013) Role of reactive oxygen species and NADPH-oxidase in the development of rat cerebellum. Neurochem Int 62:998–1011
Kawano T, Kunz A, Abe T, Girouard H, Anrather J, Zhou P, Iadecola C (2007) iNOS-derived NO and nox2-derived superoxide confer tolerance to excitotoxic brain injury through peroxynitrite. J Cereb Blood Flow Metab 27:1453–1462
Li CY, Chin TY, Chueh SH (2004) Rat cerebellar granule cells are protected from glutamate-induced excitotoxicity by S-nitrosoglutathione but not glutathione. Am J Physiol Cell Physiol 286:C893–C904
Thiyagarajan M, Kaul CL, Sharma SS (2004) Neuroprotective efficacy and therapeutic time window of peroxynitrite decomposition catalysts in focal cerebral ischemia in rats. Br J Pharmacol 142:899–911
Lane P, Hao G, Gross SS (2001) S-nitrosylation is emerging as a specific and fundamental posttranslational protein modification: head-to-head comparison with O-phosphorylation. Sci STKE 2001:re1
Patel RP, McAndrew J, Sellak H, White CR, Jo H, Freeman BA, Darley-Usmar VM (1999) Biological aspects of reactive nitrogen species. Biochim Biophys Acta 1411:385–400
Mannick JB (2007) Regulation of apoptosis by protein S-nitrosylation. Amino Acids 32:523–526
Huang Z, Pinto JT, Deng H, Richie JP Jr (2008) Inhibition of caspase-3 activity and activation by protein glutathionylation. Biochem Pharmacol 75:2234–2244
Mitchell DA, Marletta MA (2005) Thioredoxin catalyzes the S-nitrosation of the caspase-3 active site cysteine. Nat Chem Biol 1:154–158
Bao F, Liu D (2003) Peroxynitrite generated in the rat spinal cord induces apoptotic cell death and activates caspase-3. Neuroscience 116:59–70
Dohi K, Ohtaki H, Inn R, Ikeda Y, Shioda HS, Aruga T (2003) Peroxynitrite and caspase-3 expression after ischemia/reperfusion in mouse cardiac arrest model. Acta Neurochir Suppl 86:87–91
Lau A, Arundine M, Sun HS, Jones M, Tymianski M (2006) Inhibition of caspase-mediated apoptosis by peroxynitrite in traumatic brain injury. J Neurosci 26:11540–11553
Viner RI, Williams TD, Schoneich C (1999) Peroxynitrite modification of protein thiols: oxidation, nitrosylation, and S-glutathiolation of functionally important cysteine residue(s) in the sarcoplasmic reticulum Ca-ATPase. Biochemistry 38:12408–12415
Adachi T, Weisbrod RM, Pimentel DR, Ying J, Sharov VS, Schoneich C, Cohen RA (2004) S-Glutathiolation by peroxynitrite activates SERCA during arterial relaxation by nitric oxide. Nat Med 10:1200–1207
Ghafourifar P, Schenk U, Klein SD, Richter C (1999) Mitochondrial nitric-oxide synthase stimulation causes cytochrome c release from isolated mitochondria. Evidence for intramitochondrial peroxynitrite formation. J Biol Chem 274:31185–31188
Borutaite V, Morkuniene R, Brown GC (1999) Release of cytochrome c from heart mitochondria is induced by high Ca2+ and peroxynitrite and is responsible for Ca(2+)-induced inhibition of substrate oxidation. Biochim Biophys Acta 1453:41–48
Al-Ani B, Hewett PW, Ahmed S, Cudmore M, Fujisawa T, Ahmad S, Ahmed A (2006) The release of nitric oxide from S-nitrosothiols promotes angiogenesis. PLoS ONE 1:e25
Virgili M, Monti B, LoRusso A, Bentivogli M, Contestabile A (1999) Developmental effects of in vivo and in vitro inhibition of nitric oxide synthase in neurons. Brain Res 839:164–172
Salykina MA, Sorokina EG, Krasilnikova IA, Reutov VP, Pinelis VG (2013) Effects of selective inhibitors of neuronal and inducible NO-synthase on ATP content and survival of cultured rat cerebellar neurons during hyperstimulation of glutamate receptors. Bull Exp Biol Med 155:40–43
Ciani E, Virgili M, Contestabile A (2002) Akt pathway mediates a cGMP-dependent survival role of nitric oxide in cerebellar granule neurones. J Neurochem 81:218–228
Pantazis NJ, West JR, Dai D (1998) The nitric oxide-cyclic GMP pathway plays an essential role in both promoting cell survival of cerebellar granule cells in culture and protecting the cells against ethanol neurotoxicity. J Neurochem 70:1826–1838
Karacay B, Li G, Pantazis NJ, Bonthius DJ (2007) Stimulation of the cAMP pathway protects cultured cerebellar granule neurons against alcohol-induced cell death by activating the neuronal nitric oxide synthase (nNOS) gene. Brain Res 1143:34–45
Jaffrey SR, Erdjument-Bromage H, Ferris CD, Tempst P, Snyder SH (2001) Protein S-nitrosylation: a physiological signal for neuronal nitric oxide. Nat Cell Biol 3:193–197
Riccio A, Alvania RS, Lonze BE, Ramanan N, Kim T, Huang Y, Dawson TM, Snyder SH, Ginty DD (2006) A nitric oxide signaling pathway controls CREB-mediated gene expression in neurons. Mol Cell 21:283–294
Acknowledgments
This study was supported by DGAPA-UNAM (IN206213) and CONACYT (179234).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Olguín-Albuerne, M., Ramos-Pittol, J.M., Coyoy, A. et al. Peroxynitrite is Involved in the Apoptotic Death of Cultured Cerebellar Granule Neurons Induced by Staurosporine, but not by Potassium Deprivation. Neurochem Res 41, 316–327 (2016). https://doi.org/10.1007/s11064-015-1805-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11064-015-1805-9