Abstract
Microglia is the resident innate immune cells that sense pathogens and tissue injury in the central nervous system. Microglia becomes activated in response to injury, infection, and other stimuli that threaten neuronal survival. Microglia activation plays an important role in neurodegenerative diseases. Neochlorogenic acid (NCA) is a natural polyphenolic compound found in dried fruits and other plants. Although previous studies have shown that phenolic acids including NCA have outstanding antioxidant, antibacterial, antiviral, and antipyretic activities, there has not yet been investigated for anti-inflammatory effects. Therefore, for the first time we have examined the potential of NCA to inhibit microglial activation and pro-inflammatory responses in the brain. We found that lipopolysaccharide-induced inducible nitric oxide synthase, and cyclooxygenase-2 expression, and nitric oxide formation was suppressed by NCA in a dose-dependent manner in BV2 microglia. NCA also inhibited the production of pro-inflammatory mediators, tumor necrosis factor-α and interleukin-1 beta. Furthermore, phosphorylated nuclear factor-kappa B p65 and p38 mitogen-activated protein kinase activation were blocked by NCA. Taken together, these results suggest that NCA exerts neuroprotective effects through the inhibition of pro-inflammatory pathways in activated microglia.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Microglia is the resident macrophages of the central nervous system (CNS). They play a major role in the defense against neuronal injury and contribute to homeostasis in the brain [1–3]. However, activation of microglia can cause chronic neuroinflammation due to inflammatory and pathophysiological stimuli such as lipopolysaccharide (LPS). LPS is a bacterial endotoxin and is widely used to create inflammation in the brain [4]. Activated microglia releases pro-inflammatory mediators and cytokines, including nitric oxide (NO), cyclooxygenase-2 (COX-2), tumor necrosis factor-α (TNF-α), and interleukin-1 beta (IL-1β), eventually leading to neuronal dysfunction and cell death [5–7]. Clinical evidence has shown that microglial activation and neuroinflammation are implicated in the pathogenesis of neurodegenerative diseases including Alzheimer’s disease, Parkinson’s disease, brain ischemia, and Huntington’s disease [8–10]. Thus, regulating microglial activation and pro-inflammatory responses may help patients with neurodegenerative diseases by reducing brain damage or neuronal cell death.
Neochlorogenic acid (NCA) (Fig. 1), an isomer of chlorogenic acid, is a natural polyphenolic compound found in some types of dried fruits and a variety of other plant sources such as peaches [11]. Previous studies have shown that phenolic acids have outstanding antioxidant, antibacterial, antiviral, and antipyretic activities [12–14]. In addition, geniposide, another phenolic acid, has shown analgesic and anti-inflammatory effects [12, 15]. However, the effects of NCA on inflammation have not yet been investigated. Therefore, for the first time we examined the potential of NCA to inhibit microglial activation and pro-inflammatory responses in the brain.
Materials and Methods
Materials
Murine microglial BV2 cells were provided to us by Dr. Myungsook Oh from Kyunghee University (Seoul, Korea). LPS, NCA, dexamethasone, Griess reagent, 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide (MTT) reagent and dimethyl sulfoxide (DMSO) were purchased from Sigma Aldrich (St. Louis, MO, USA). Cell culture media [Dulbecco’s modified Eagle’s minimal essential medium (DMEM)], antibiotic–antimycotic solution, fetal bovine serum (FBS) and other ingredients required to culture BV2 cells were purchased from Life Technologies (Grand Island, NY, USA). Protease and phosphatase inhibitor cocktail tablets were supplied by Thermo Scientific (Rockford, IL, USA). Primary and secondary antibodies used for western blot analysis were purchased from Santa Cruz Biotechnology (Santa Cruz, CA, USA), Cell Signaling Technology (Danvers, MA, USA), and BD Biosciences (San Jose, CA, USA). ELISA kits were obtained from Enzo Life Sciences (Farmingdale, NY, USA).
Cell Culture and Treatment
Mouse BV2 microglial cells were maintained in DMEM, supplemented with 5 % FBS and 1 % antibiotic–antimycotic in a humidified incubator with 5 % CO2 at 37 °C. NCA and dexamethasone as positive control were dissolved in DMSO to a final concentration of 10 mM for the stock solution. Treatments with LPS and/or NCA were carried out under serum-free conditions.
NO Production Assay
NO production of LPS-activated BV2 cells was measured by the Griess test. BV2 cells were plated into 96-well plates at a density of 3 × 105 and treated with LPS (4 μg/ml), Dexamethasone (10 μM) and NCA (0, 10, 50, and 100 μM) for 24 h. The culture supernatant from each sample (50 μl) was mixed with the same volume of the Griess reagent (1 % sulfanilamide, 0.1 % N-1-naphthylethylenediamine dihydrochloride in 5 % phosphoric acid) and then incubated for 10 min at room temperature. The absorbance values were measured at 540 nm using a microplate reader, and NaNO2 was used as the standard to determine NO2 concentrations.
MTT Cell Viability Assay
Cell viability was confirmed by the MTT assay. The medium was removed from the wells, MTT was added, and the samples were then incubated for 3 h at 37 °C. The formazan crystals were dissolved by adding DMSO, and the absorbance values were measured at 540 nm using a microplate reader.
Enzyme Immunoassay
The inhibitory effects of NCA on the production of the proinflammatory cytokines TNF-α and IL-1β were determined by an enzyme-linked immunosorbent assay (ELISA). Conditioned media were analyzed as per the manufacturer’s instructions with a mouse enzyme immunoassay (EIA) kit (Enzo Life Sciences).
Western Blot Analysis
BV2 cells were seeded in 6-well plates. The cells were lysed with Protein Extraction Solution (Elpis biotech, Daejeon, Korea) and cell lysates were separated into the nuclear and cytosol fractions using a nuclear/cytosol fraction kit (Biovision Inc., Milpitas, CA, USA). The protein concentration was measured using a protein assay dye reagent with bovine serum albumin as the standard. The same amount of protein from each sample was separated by 10 % sodium dodecyl sulfate–polyacrylamide gel electrophoresis and transferred onto a nitrocellulose membrane. The membranes were blocked with 5 % skimmed milk and incubated with different primary antibodies inducible nitric oxide synthase (iNOS), COX-2, β-actin, p38 mitogen-activated protein kinase (p38 MAPK), phospho-p38 MAPK, nuclear factor kappa B p65 (NF-κB p65), and phospho-NF-κB p65 overnight at 4 °C. Then, the horseradish peroxidase-conjugated secondary antibodies were incubated for 1 h. Antibody detection was carried out using ECL reagent (Thermo Scientific, USA) and visualized by ChemiDoc (Bio-Rad Laboratories, Hercules, CA, USA). The intensities of the bands were normalized to the β-actin band using Image Lab Software (Bio-Rad).
Statistics Analysis
All statistical parameters were calculated using GraphPad Prism 3.0 software (GraphPad Software Inc., San Diego, CA, USA). Values were expressed as the mean ± standard error of the mean (SEM). The results were analyzed by one-way analysis of variance (ANOVA) followed by Tukey’s post hoc test. Differences with a P value less than 0.05 were considered statistically significant.
Results
Inhibitory Effects of NCA on NO Production in LPS-Induced BV2 Microglia Cells
To determine the effects of NCA on the LPS-induced production of the inflammatory mediator NO in microglia, the NO levels in the cell culture medium were measured using the Griess assay (Fig. 2a). NCA or dexamethasone treated alone was not any affected to NO production. LPS-treated BV2 cells showed a marked increase of cellular nitrite levels compared to the control group. In the presence of NCA, NO production by LPS-induced BV2 cells was inhibited in a dose-dependent manner, with levels significantly inhibited after treatment with 50 and 100 μM NCA. Especially 100 μM NCA had similar inhibitory effects to dexamethasone. Dexamethasone is widely used as a positive control to anti-inflammatory effect and used 10 μM, which had a marked effective dose in previous studies [16].
Effects of neochlorogenic acid (NCA) on nitric oxide (NO) production and cell viability in lipopolysaccharide (LPS)-stimulated BV2 microglial cells. The cells were treated with or without LPS (4 μg/ml) and NCA (10, 50, and 100 μM) for 24 h. Dexamethasone (10 μM) was used for positive control. Then, a nitrite concentrations in the medium were determined using the Griess reagent. b Cell viability was confirmed by the MTT assay. Each value indicates the mean ± SEM and represents results obtained from three independent experiments. ### P < 0.001 indicates that the mean value was significantly different from the control group receiving no treatment. *P < 0.05 and ***P < 0.001 indicate that the mean value was significantly different from the group receiving LPS alone
No Effect of NCA on Cell Viability
The potential cytotoxicity of NCA on LPS-induced BV2 cells was evaluated using the MTT assay. Our results showed that cell viability was not affected at any concentration used (Fig. 2b), confirming that the inhibition of NO production in LPS-induced BV2 cells was not due to cytotoxic effects of NCA. Moreover, NCA was dissolved in DMSO to less than 0.01 % and it was not affected to cell death (data not shown).
Inhibitory Effects of NCA on iNOS and COX-2 Protein Expression in LPS-Induced BV2 Microglia Cells
In order to determine whether the inhibitory effect of NCA on NO production was associated with a downstream modulation of iNOS and COX-2 expression, we measured the protein levels using western blotting. The protein levels of these enzymes were analyzed in the whole cell lysates 24 h after treatment with LPS. As shown in Fig. 3, iNOS and COX-2 levels were increased in LPS-induced BV2 cells, but this increase was significantly inhibited after treatment with 50 and 100 μM NCA.
Inhibitory effects of neochlorogenic acid (NCA) on inducible nitric oxide synthase (iNOS) and cyclooxygenase-2 (COX-2) protein induction in lipopolysaccharide (LPS)-stimulated BV2 microglial cells. After treating with LPS (4 μg/ml) and NCA (10, 50, and 100 μM) for 24 h, the cell lysates were prepared and western blot analysis was performed using anti-iNOS and anti-COX-2 antibodies. Protein levels of iNOS (b) and COX-2 (d) were normalized to β-actin. Representative band images from individual experiments are shown in a and c. Each value indicates the mean ± SEM and represents results obtained from three independent experiments. ### P < 0.001 indicates that the mean value was significantly different from the control group receiving no treatment. *P < 0.05 and ***P < 0.001 indicate that the mean value was significantly different from the group receiving LPS alone
Effects of NCA on the LPS-Induced Release of Pro-inflammatory Cytokines in BV2 Microglia Cells
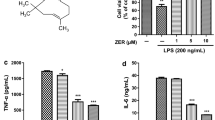
The effects of NCA on the secretion of pro-inflammatory cytokines such as TNF-α and IL-1β were investigated by ELISA in LPS-induced BV2 microglial cells (Fig. 4). The results showed that the expression of TNF-α and IL-1β increased in LPS-induced BV2 cells, but these increases were blocked in the NCA-treated group. Specifically, treatments with 50 and 100 μM NCA significantly inhibited the increase in TNF-α and IL-1β expression relative to treatment with LPS alone.
Inhibitory effects of NCA on tumor necrosis factor-α (TNF-α) and interleukin-1 beta (IL-1β) production in lipopolysaccharide (LPS)-stimulated BV2 microglial cells. The cells were treated with LPS (4 μg/ml) and NCA (10, 50, and 100 μM) for 24 h. The levels of a TNF-α and b IL-1β present in the supernatants were measured by ELISA. Results indicate the mean ± SEM and represent results obtained from three independent experiments. # P < 0.05 indicates that mean value was significantly different from the control group receiving no treatment. *P < 0.05 and **P < 0.01 indicate that mean value was significantly different from the group receiving LPS alone
Degradation Effects of NCA on Activation of p38 MAPK and Nuclear Translocation of NF-κB p65 in LPS-Induced BV2 Microglia Cells
To clarify that the inhibition of the increases of iNOS and COX-2 expression was mediated by an NCA-induced blockade of LPS-induced microglial activation, the effects of NCA on activation of phosphorylated p38 MAPK and NF-κB p65 were examined. Figure 5a shows that NCA at 100 μM, the most effective concentration in other assays, also attenuated the LPS-induced increase of p38 MAPK phosphorylation compared with the group treated with LPS alone. NCA also markedly attenuated the LPS-induced increase of NF-κB p65 phosphorylation compared with the group treated with LPS alone (Fig. 5b).
Inhibitory effects of neochlorogenic acid (NCA) on activation of p38 mitogen-activated protein kinase (p38 MAPK) and nuclear translocation of NF-κB p65 in liposaccharide (LPS)- stimulated BV2 microglia cells. The cells were treated with LPS (4 μg/ml) and NCA (0 and 100 μM) for 30 min. The effects of NCA on phosphorylation of p38 MAPK and NF-κB p65 were investigated using western blotting analysis. For p38 MAPK detection, antibodies directed against phosphorylated p38 MAPK (p-p38) and total p38 MAPK were used in whole protein lysate. For NF-κB p65 detection, antibodies directed against phosphorylated NF-κB p65 (p-p65) and total NF-κB p65 were used in the nuclear fraction. Levels of p-p38 (b) and p-p65 (d) were normalized to total p38 MAPK and total NF-κB p65. Representative band images from each experiment are shown in a and c. Each value indicates the mean ± SEM and represents results obtained from three independent experiments. # P < 0.05 and ## P < 0.01 indicate that mean value was significantly different from the control group receiving no treatment. *P < 0.05 indicates that mean value was significantly different from the group receiving LPS alone
Discussion
NCA is reported to be a major bioactive component of dried fruits and other plants, and has been demonstrated to have various beneficial effects [12–14]. However, the effects of NCA on inflammatory processes are still unclear. Our present results provide, for the first time, evidence for the anti-inflammatory effects of NCA. In this study, NCA showed a reduction of LPS-induced NO production by suppressing iNOS and COX-2 protein expression and production of pro-inflammatory cytokines, such as TNF-α and IL-1β, in BV2 microglia cells. In addition, phosphorylated p38 MAPK and NF-κB p65 were also inhibited by NCA in activated microglia. These results suggest that NCA exhibited anti-inflammatory effects in BV2 microglial cells.
Microglia is sensitive to changes in their microenvironment and is activated in response to infection or injury. Microglia-mediated neuroinflammation is a major component enhancing neurodegeneration. Overactivation and dysregulation of microglia cause neuronal death and brain injury, most likely due to the production of high levels of cytotoxic and pro-inflammatory factors [17–19]. Microglial activation is pivotal in the initiation of neuroinflammation and prolonged activation of microglial cells leads to excessive release of NO by iNOS in the brain [20]. NO plays an important role in cell survival and NO can induce neuronal cell death [21]. COX-2 is upregulated in response to various inflammatory stimuli and NO functions to enhance its expression and activity [22]. A number of studies have shown that the expression of iNOS and COX-2, key enzymes for NO, is upregulated in activated glial cells. Pro-inflammatory cytokines such as TNF-α and IL-1β are also initiators of the inflammatory response and mediators in the pathogenesis of neurodegenerative disorders [23, 24]. Previous evidence has demonstrated the damaging and inflammatory effects of these cytokines in neuropathology [25]. Thus, downregulation of these inflammatory molecules could be beneficial for alleviating the progression of neurodegeneration caused by microglial activation. In the present study, treating LPS-stimulated BV2 cells with NCA effectively decreased iNOS, COX-2, TNF-α, and IL-1β levels and the release of their respective end-products, including NO. Further, the MTT assay results demonstrated that this effect was not due to any cytotoxicity of NCA.
The critical transcription factor, NF-κB p65, is part of a well-known signaling cascade that contributes to the production of an array of inflammatory mediators including COX-2, iNOS, and cytokines. Generation and amplification of TNF-α and IL-1β have been reported to be regulated by NF-κB p65 [26–28]. In addition to NF-κB p65 signaling, MAPKs are also important signaling molecules involved in the production of pro-inflammatory mediators and cytokines and the modulation of NF-κB p65 in microglia [29, 30]. One of the MAPK families, p38, is related to LPS signaling in microglial cells, which respond to pro-inflammatory cytokines [31, 32]. In this study, we detected the inhibitory effects of NCA on LPS-induced activation of NF-κB p65 and p38 MAPK. These results suggest that NCA-mediated inhibition of pro-inflammatory mediators and cytokines is associated with the downregulation of the MAPK signaling pathway.
In conclusion, the present study demonstrates that NCA inhibits LPS-induced NO production by iNOS and COX-2 protein expression in BV2 microglial cells. NCA also inhibits the production of the pro-inflammatory cytokines, TNF-α and IL-1β, and inflammation mediated via phosphorylated NF-κB p65 and p38 MAPK. Our findings suggest that NCA may provide a beneficial effect in the treatment of inflammatory brain damage induced by microglial activation, which should be verified through more precise in vivo model experiments. To our best knowledge, in vivo studies on permeability of NCA into brain and anti-inflammatory effect have not performed. We hope that these studies would contribute to the treatment of neurological disorder involved in microglial activation.
References
Aguzzi A, Barres BA, Bennett ML (2013) Microglia: Scapegoat, saboteur, or something else? Science 339:156–161
Block ML, Zecca L, Hong JS (2007) Microglia-mediated neurotoxicity: uncovering the molecular mechanism. Nat Rev Neurosci 8:57–69
Nimmerjahn A, Kirchhoff F, Helmchen F (2005) Resting microglial cells are highly dynamic surveillants of brain parenchyma in vivo. Science 308:1314–1318
Ock J, Han HS, Hong SH, Lee SY, Han YM, Kwon BM, Suk K (2010) Obovatal attenuates microglia-mediated neuroinflammation by modulating redox regulation. Br J Pharmacol 159:1646–1662
Perry VH, Nicoll JA, Holmes C (2010) Microglia in neurodegenerative disease. Nat Rev Neurol 6:193–201
Rivest S (2003) Molecular insights on the cerebral innate immune system. Brain Behav Immun 17:13–19
Das S, Basu A (2008) Inflammation: a new candidate in modulating adult neurogenesis. J Neurosci Res 86:1199–1208
Lue LF, Kuo YM, Beach T, Walker DG (2010) Microglia activation and anti-inflammatory regulation in Alzheimer’s disease. Mol Neurobiol 41:115–128
Long-Smith CM, Sullivan AM, Nolan YM (2009) The influence of microglia on the pathogenesis of Parkinson’s disease. Prog Neurobiol 89:227–287
Glass CK, Saijo K, Winner B, Matchetto MC, Gage FH (2010) Mechanisms underlying inflammation in neurodegeneration. Cell 140:918–934
Infante R, Contador L, Rubil P, Aros D, Pena-Neira Á (2011) Postharvest sensory and phenolic characterization of ‘Elegant Lady’ and ‘Carson’ peaches. Chil J Agric Res 71:445–451
Chen Y, Li SG, Lin XH, Luo HB, Li GG, Yao H (2008) On-line screening and identification of radical scavenging compounds extracted from Flos Lonicerae by LC-DAD-TOF-MS. Chromatographia 68:327–333
Hung XM, Na M, Thuong PT, Su NA, Sok D, Song KS, Seong YH, Bae K (2006) Antioxidant activity of caffeoyl quinic acid derivatives from the roots of Dipsacus asper Wall. J Ethnopharmacol 108:188–192
Mishima S, Yoshida C, Akino S, Sakamoto T (2005) Antihypertensive effects of Brazillian propolis: identification of caffeoylquinic acids as constituents involved in the hypotension in spontaneously hypertensive rats. Biol Pharm Bull 28:1909–1914
Koo HJ, Lim KH, Jung HJ, Park EH (2006) Anti-inflammatory evaluation of gardenia extract, geniposide and genipin. J Ethnopharmacol 103:496–500
Korhnen R, Lahti A, Hämäläinen M, Kankaanranta H, Moilanen E (2002) Dexamethasone inhibits inducible nitric-oxide synthase expression and nitric oxide production by destabilizing mRNA in lipopolysaccharide-treated macrophages. Mol Pharmacol 62:698–704
Liu B, Hong J-s (2003) Role of microglia in inflammation-mediated neurodegenerative diseases: mechanisms and strategies for therapeutic intervention. J Pharmacol 304:1–7
Minghetti L, Levi G (1998) Microglia as effector cells in brain damage and repair: focus on prostanoids and nitric oxide. Prog Neurobiol 54:99–125
Rivest S (2011) The promise of anti-inflammatory therapies for CNS injuries and diseases. Expert Rev Neurother 11:783–786
Murphy S (2000) Production of nitric oxide by glial cells: regulation and potential roles in the CNS. Glia 29:1–13
Brown GC, Borutaite V (2002) Nitric oxide inhibition of mitochondrial respiration and its role in cell death. Free Radic Biol Med 33:1440–1450
Minghetti L (2004) Cyclooxygenase-2 (COX-2) in inflammatory and degenerative brain diseases. J Neuropathol Exp Neurol 63:901–910
Merson TD, Binder MD, Kilpatrik TJ (2010) Role of cytokines as mediators and regulators of microglia activity in inflammatory demylination of the CNS. Neuromol Med 12:99–132
Hoozemans JJ, Veerhuis R, Rozemuller JM, Eikelenboom P (2006) Neuroinflammation and regeneration in the early stages of Alzheimer’s disease pathology. Int J Dev Neurosci 24:157–165
Inoue K (2006) The function of microglia through purinergic receptors: neuropathic pain and cytokines release. Pharmacol Ther 109:210–226
He FQ, Qiu BY, Zhang XH, Li TK, Xie Q, Cui DJ et al (2011) Tetrandrine attenuates spatial memory impairment and hippocampal neuroinflammation via inhibiting NF-κB activation in a rat model of Alzheimer’s disease induced by amyloid-β (1–42). Brain Res 1384:89–96
Yeo SJ, Yoo JG, Yi AK (2003) Myeloid differentiation factor 88-dependent post-necrosis factor-alpha receptor- associated factor 6, a diverging point in the Toll-like receptor 9-signaling. J Biol Chem 278:40590–40600
Vallabhapurapu S, Karin M (2009) Regulation and function of NF-kappaB transcription factors in the immune system. Annu Res Immunol 27:693–733
Kaminska B, Gozdz A, Zawadzka M, Ellert-Miklaszewska A, Lipko M (2009) MAPK signal transduction underlying brain inflammation and gliosis as therapeutic target. Anat Rec 292:1902–1913
Krementsov DN, Thornton TM, Teuscher C, Rincon M (2013) The emerging role of p38 mitogen-activated protein kinase in multiple sclerosis and its models. Mol Cell Biol 33:3728–3734
Branger J, van den Blink B, Weijer S, Madwed J, Bos CL et al (2006) Anti-inflammatory effects of a p38 mitogen-activated protein kinase inhibitor during human endotoxemia. J Immunol 168:4070–4077
Ashwell JD (2006) The many paths to p38 mitogen-activated protein kinase activation in the immune system. Nat Rev Immunol 6:532–540
Acknowledgments
This study was supported by the Korea Food Research Institute.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Human and animal rights
This article does not contain any studies with human participants or animals performed by any of the authors.
Rights and permissions
About this article
Cite this article
Kim, M., Choi, SY., Lee, P. et al. Neochlorogenic Acid Inhibits Lipopolysaccharide-Induced Activation and Pro-inflammatory Responses in BV2 Microglial Cells. Neurochem Res 40, 1792–1798 (2015). https://doi.org/10.1007/s11064-015-1659-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11064-015-1659-1