Abstract
Purpose
Neurofibromatoses (NF; NF1, NF2, and schwannomatosis) are incurable tumor suppressor syndromes with heterogeneous symptoms. Emotional distress (e.g., depression, anxiety, stress) is common in NF and impairs quality of life (QoL). Several modifiable dimensions of resiliency can contribute to enhanced QoL in medical populations but have been overlooked as treatment mechanisms for NF. Our goal was to determine, using data from an ongoing efficacy RCT testing a mind–body program for NF, if resiliency explains the relationship between emotional distress and QoL.
Methods
We performed structural equation modeling mediation analysis on baseline measures of QoL (physical health, psychological, social relationships, environmental), emotional distress (depression, anxiety, stress), and resiliency (gratitude, optimism, coping, mindfulness, empathy) completed by adults with NF (N = 228). We controlled for variables known to impact psychosocial functioning in NF (age, diagnosis, learning disability, and education).
Results
After adjusting for covariates, resiliency had a significant and large indirect effect on the negative relationship between emotional distress and QoL (CSIE = − 0.31, 95% CI = − 0.59 to − 0.19, p = .001). The direct effect of emotional distress on QoL was smaller but remained significant (β = − 0.23, 95% CI = − 0.44 to − 0.03, p = .03), suggesting partial mediation through resiliency.
Conclusions
Resiliency may buffer the high rates of emotional distress in NF. Mind–body interventions targeting multiple modifiable resiliency factors may be a promising path toward promoting QoL in adults with NF.
Trial registration
Clinical Trials.gov Identifier: NCT03406208.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Neurofibromatoses (NF), including NF1, NF2, and Schwannomatosis (SCHWN), are the most common neurological conditions caused by a single gene (> 100,000 in the U.S.) [1]. Nerve sheath tumors are primary symptoms across NF subtypes, can occur anywhere in the nervous system, and lead to significant morbidity. Other common symptoms include disfiguring cutaneous and subcutaneous tumors in NF [2]; hearing loss, facial weakness, and poor gait in NF2 [3]; and chronic pain in SCHWN [4]. Because there is no cure for NF, treatments (e.g., surgical, pharmacological) typically aim to reduce symptoms [5].
Patients with NF experience emotional distress, including depression, anxiety, and perceived stress, at rates higher than the general population [6] and comparable to other populations with serious illness (e.g., cancer) [7]. Patients with NF also report low quality of life across physical, social, and psychological domains [8]. Emotional distress is associated with lower resiliency [9] and QoL [10,11,12,13] beyond the physical symptoms of NF (e.g., skin and voice-related). Exploring modifiable factors that mitigate this association is a crucial avenue for intervention research.
Resiliency, or adapting and “bouncing back” from adversity [14], is a multidimensional construct that promotes adjustment to illness in neurological populations [15, 16] but is understudied in NF. In addition to static factors (e.g., intellectual ability, medical history), several modifiable dimensions of resiliency may contribute to enhanced QoL in NF [17]. These include coping skills (adaptative strategies for stressors), mindfulness (deliberate attention to the present moment without judgment), gratitude (an appreciation for what one has), and optimism (favorable expectations for the future) [18]. A multidimensional model of resiliency, which has potential to identify modifiable factors of QoL, has not been examined as a potential buffer of emotional distress in NF.
We examined the cross-sectional relationship between emotional distress, resiliency, and QoL in baseline data from an efficacy RCT of a mind–body program for NF (N = 228). Understanding the role of resiliency in key patient-reported outcomes can inform targets for mind–body interventions in NF and identify patients most likely to benefit. We used structural equation modeling (SEM) to comprehensively represent QoL (physical health, psychological, social relationships, environmental), emotional distress (depression, anxiety, stress), and resiliency (gratitude, optimism, mindfulness, coping) as multidimensional constructs that align with our conceptual model [20]. We hypothesized: 1) that resiliency would significantly mediate the relationship between emotional distress and QoL in patients with NF, 2) the indirect effect of resiliency on QoL would be stronger than the variance explained by emotional distress alone (i.e., direct effect), and 3) hold after controlling for variables (age, NF diagnosis, learning disability, and education) known to impact psychosocial functioning in NF [19].
Methods
We pre-registered our trial (ClinicalTrials.gov, NCT03406208) and published full details in our prior work [21]. Here, we outline the methodology pertinent to our mediation analysis in this study.
Participants and procedure
The Massachusetts General Hospital Institutional Review Board approved all study procedures (protocol #2017P000143). We recruited adults with NF (NF1, NF2, and SCHWN) from NF-specific U.S. and international foundations (e.g., Children’s Tumor Foundation, Children’s Tumor Trust), U.S. clinics, and on social media groups for patients (May 2017 to February 2021). We screened for eligibility via secure live video (total contacts N = 993).
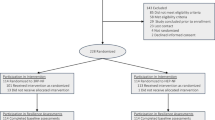
Inclusion required: (1) a diagnosis of NF1, NF2, or SCHWN, (2) ≥ 18 years of age, (3) English speaking, (4) ≥ 6 grade reading level, (5) self-reported stress and difficulties coping with NF symptoms, and (6) Perceived Stress Scale—4 item (PSS-4) score ≥ 6. Exclusion criteria were: (1) serious medical illness unrelated to NF that was a significant stressor and was expected to worsen in the next 12 months (e.g., metastatic cancer), (2) change in antidepressant medication ≤ 3 months, (3) participation in cognitive behavioral or relaxation therapy ≤ 3 months, (4) severe and/or persistent mental illness (e.g., untreated bipolar disorder, psychotic disorder, active substance use) requiring immediate treatment, (5) unable/unwilling to complete assessments online, and (6) unable/unwilling participate in live video interventions. We obtained written informed consent from participants prior to enrollment. For blinding purposes, participants were told that they would complete one of two programs for coping with NF stress and symptoms.
Enrolled participants (N = 228) received a Research Electronic Data Capture (REDCap) survey link for the baseline assessments (< 30 min). Participants had no knowledge of group assignment when completing the baseline measures. We aimed to prevent missing data with reminder emails and phone calls as needed. After completion of baseline assessments, participants were randomized to Relaxation Response Resiliency Program (NF 3RP-NF) or the active education control (Health Enhancement Program for NF, HEP-NF). Table 1 presents the sample demographics and clinical characteristics.
Measures
Quality of life (outcome)
Quality of life (QoL)
The World Health Organization Quality of Life – Brief version (WHOQOL-BREF) [22] is a 26-item self-report of QoL across 4 domains: physical health, psychological, social relationships, and environmental domains using a 5-point Likert scale ranging from 1 (“Not at All”) to 5 (“An Extreme Amount”). Scores for each domain are transformed (range = 0 to 100) and higher scores indicate greater QoL. The WHOQOL – BREF has good to excellent reliaibltiy (internal consistency = 0.68 to 0.82) and validity (four factors explain 50 to 81% of variance in QoL) [22] (Table 2).
Emotional distress (predictor)
Depression
The Patient Health Questionnaire 9-Item version (PHQ-9) [23] is a self-report of depressive symptoms in the past two weeks using a 4-point Likert scale ranging from 0 (“Not at All”) to 3 (“Nearly Every Day”). Higher scores indicate greater frequency and clinical severity of depressive symptoms (range = 0 to 27). The PHQ-9 measure has demonstrated validity for identifying depression in neurologic populations (sensitivity and specificity > 78%) [24].
Anxiety
The Generalized Anxiety Disorder 7-Item version (GAD-7) [25] measures the frequency of anxiety symptoms in the past two weeks using a 4-point Likert scale ranging from 0 (“Not at All”) to 3 (“Nearly Every Day”). Higher scores indicate greater frequency and clinical severity of anxiety (range = 0 to 21). The GAD-7 has demonstrated excellent reliability (internal consistency = 0.83 to 0.93) and validity (convergence with anxiety measures, r = 0.69 to 0.76) in patients with heterogeneous psychiatric conditions [26].
Stress
The Perceived Stress Scale 10-Item version (PSS-10) [27] is a self-report of stress-related thoughts and feelings within the past month using a 5-point Likert scale ranging from 0 (“Never”) to 4 (“Very Often”). Higher scores indicate greater perceived stress (range = 0 to 40). The PSS-10 measure has demonstrated adequate reliability (internal and test–retest > 0.70) and validity (moderate to strong convergence with emotional distress measures) in diverse populations [28].
Resiliency (mediator)
We administered multiple measures of resiliency for three main reasons. First, single instruments do not capture all domains of resiliency targeted by the 3RP-NF [20] or align with multidimensional conceptualizations of resiliency in neurological populations [16, 18]. Second, single instruments have missing or limited psychometrics [29]. Third, multiple measures were required for the SEM examining relationships between comprehensive resiliency, QoL, emotional distress constructs. Fourth, our prior studies show that the resiliency measures below are appropriate and sensitive to NF samples [17, 30].
Gratitude
The Gratitude Questionnaire 6-Item version (GQ-6) [31] is a self-report of daily experiences of gratitude using a 7-point Likert scale ranging from 1 (“Strongly Disagree”) to 7 (“Strongly Agree”). Higher scores indicate greater levels of gratitude (range = 7 to 49). The GQ-6 measure has evidenced acceptable reliability (internal consistency = 0.73) and validity (e.g., convergence with spiritual well-being = 0.61) for chronic illness populations [32].
Optimism
The 11-item Life Orientation Test Revised (LOT-R) [33] is a self-report on experiences of optimism in daily life using a 5-point Likert scale ranging from 0 (“Strongly Disagree”) to 4 (“Strongly Agree”). Higher scores indicate greater levels of optimism (range = 0 to 44). The LOT-R has demonstrated adequate reliability (internal consistency = 0.80) and validity (e.g., convergence with psychological well-being = 0.34 to 0.65) in healthy adults [34].
Coping
The 13-item Measure of Current Status – Part A (MOCS-A) [35] is a self-report of coping abilities on four subscales: relaxation, awareness of tension, assertiveness, and coping confidence. Participants indicate perceived coping using a 5-point Likert scale ranging from 0 (“I Cannot Do This At All”) to 4 (“I Can Do This Extremely Well”). Higher scores indicate greater perceived coping ability (range = 0 to 52). The MOCS-A has demonstrated construct validity in patients with cancer (e.g., strong model fit for MOCS-A relaxation and coping confidence) [36].
Mindfulness
The 12-item Cognitive and Affective Mindfulness Revised (CAMS-R) [37] is a self-report of mindfulness in everyday life using a 4-point Likert scale ranging from 1 (“Rarely or Not at All”) to 4 (“Almost Always”). Higher scores indicate greater experience of mindfulness (range = 12–48). The CAMS-R measure has demonstrated acceptable reliability (internal consistency = 0.74–0.77) and validity (e.g., convergence with cognitive flexibility = 0.46) in the general population [37].
Statistical methods
We conducted mediation analysis using structural equation modeling (SEM) in R using best-practice guidelines in the following sequence [38]. First, we estimated the effect of emotional distress on the resiliency mediator (path A). Second, we estimated the effect of the resiliency mediator on QoL (path B). Third, we estimated the indirect effect of emotional distress through the resiliency mediator (path A × B). Fourth, we estimated the direct effect of emotional distress on QoL minus the resiliency mediator (path C). Fifth, we estimated the total effect of emotional distress on QoL plus the resiliency mediator (path C). Finally, we re-tested the mediation model by specifying direct paths from covariates (age, NF diagnosis, learning disability, and education) to each latent variable.
We estimated SEM with case-wise maximum likelihood estimation. Criteria for optimal model fit included: Chi-square test of fit (Cmin/df) near 2, a comparative fit index (CFI) ≥ 0.95, and the root-mean-square error approximation (RMSEA) between 0.002 and 0.08. We report standardized effects (β) with bias corrected 95% confidence intervals (CI) bootstrapped for 10,000 samples. For path A x B, we report “completely standardized” indirect effects (CSIE) and the ratio (paths A × B/C).
Results
Depression (PHQ-9), anxiety (GAD-7), and stress (PSS-10) loaded onto the emotional distress latent variable (Bartlett’s test < 0.001, KMO = 0.71, loadings = 0.70 to 0.80, variance explained = 61%). Physical health, psychological, social relationships, and environmental domains (WHOQOL-BREF) loaded onto the QoL latent variable (Bartlett’s test < 0.001, KMO = 0.74, loadings = 0.57 to 0.82, variance explained = 45%). Gratitude (GQ-6), optimism (LOT-R), coping (MOCS-A), and mindfulness (CAMS-R) loaded onto the resiliency latent variable (Bartlett’s test < 0.001, KMO = 0.68, loadings = 0.56 to 0.87, variance explained = 52%).
Figure 1 presents the SEM (Cmin/df = 6.08, CFI = 0.84, RMSEA = 0.15). Emotional distress and resiliency were inversely related (path A; β = − 0.77, 95% CI = − 0.98 to − 0.58, p < 0.001). Higher resiliency was associated with higher QoL (path B; β = 0.41, 95% CI = 0.24 to 0.65, p < 0.001). The overall model explained 54% of the variance in QoL for this sample of adults with NF (path C; β = − 0.54, 95% CI = − 0.69 to − 0.41, p < 0.001). The indirect effect of resiliency accounted for over half of the relationship between emotional distress and QoL (path A × B; CSIE = − 0.31, 95% CI = − 0.59 to − 0.19, ratio = − 0.57, p = 0.001). The direct effect of emotional distress on QoL was smaller but remained significant (path C’; β = − 0.23, 95% CI = − 0.44 to − 0.03, p = 0.03), after accounting for the indirect effect of resiliency, indicating that the mediation was partial. Adjusting for covariates did not influence the indirect effect of resiliency (path A × B; CSIE = − 0.31, 95% CI = − 0.57 to − 0.17, ratio = − 0.57, p < 0.001) or direct effect of emotional distress on QoL (path C’; β = − 0.24, 95% CI = − 0.48 to − 0.003, p = 0.002).
Emotional distress (ED) and quality of life (QoL) is mediated by resiliency (RSL) in patients with NF (path A × B; CSIE = − 0.31, 95% CI = − 0.59 to − 0.19, ratio = − 0.57, p = .001). Emotional distress (ED) measures include the Patient Health Questionnaire – 9 item (PHQ) for depression, Generalized Anxiety Disorder 7-Item Version (GAD) for anxiety, and the Perceived Stress Scale 10-Item version (PSS) for stress. Quality of life (QoL) measures include the physical health (PhQOL) psychological (PsQoL), social relationships (SQO), and environmental (EQO) domains from the World Health Organization Quality of Life – Brief version (WHOQOL-BREF). Resiliency (RSL) measures include the Gratitude Questionnaire 6-Item version (GQ6) for gratitude, 11-item Life Orientation Test Revised (LOT) for optimism, 13-item Measure of Current Status Part A (MOCS) for coping, and the 12-item Cognitive and Affective Mindfulness Revised (CAMS) for mindfulness
Discussion
QoL is a critical outcome in NF given its impact on daily functioning, physical, and mental health [8, 10,11,12,13]. We explored multiple domains of resiliency as a buffer against the high rates of emotional distress in NF that negatively impact QoL. Our SEM-based mediation analysis found support for all three study hypotheses with implications for enhancing QoL in NF. First, resiliency had a significant indirect effect on the negative association between emotional distress and QoL. Second, the variance explained by the indirect effect of resiliency was large and greater than the moderate direct effect of emotional distress on QoL alone. Third, we observed these effects after controlling for age, NF diagnosis, learning disability, and education. Our model with emotional distress and resiliency explained over half of the variance in patients’ QoL. This underscores the importance of psychosocial factors in the QoL of this population, which have been traditionally overlooked in treatments compared to physical symptoms.
Clinical implications
Resiliency may buffer the high rates of emotional distress in NF, suggesting that enhancing multiple dimensions of resiliency is a promising path toward promoting QoL. Gratitude, optimism, mindfulness, and adaptive coping skills, may help patients with NF adjust to disease-related challenges, including pain, physical disfigurement, and uncertain prognosis. The positive associations between these resiliency domains and improved health outcomes, as well as their importance as mechanisms in psychosocial interventions, is supported in other medical populations [15,16,17]. The 3RP-NF is designed to enhance resiliency by targeting three inter-related components: relaxation methods (elicit calm and awareness with mindfulness), stress appraisal and coping (facilitate adaptive thinking through perceived coping ability), and growth enhancement (foster connectedness to self and others through optimism and gratitude) [17]. Prior research in NF has shown that these treatment components are associated with sustainable improvements in resilience factors of coping, social support, and mindfulness [17]. These findings are consistent with interventions that promote resilience in other high-need medical populations [16, 39].
Our study has several methodological strengths. First, we followed our live video protocol [21] to recruit a large and geographically diverse sample of adults with NF across the three subtypes—an underrepresented population in clinical research. Second, we administered reliable and valid measures that strongly loaded on to QoL, emotional distress, and resiliency in the SEM. Third, our mediation analysis was informed by our conceptual model for the 3RP-NF [20]. Fourth, we controlled for variables known to impact psychosocial functioning in NF [19].
Study limitations
Study limitations also warrant consideration. First, we recruited adults with NF reporting elevated stress and excluded adults with NF2 who are deaf. We also had difficulty enrolling ethnically and racially diverse patients. The combination of these factors limits the generalizability of our findings, which may not be representative of the NF population as a whole. Future trials will make efforts to recruit demographics underrepresented in this sample through attendance of NF forums and collaborations with national organizations (Children’s Tumor Foundation). Second, the latent variables were strongly correlated and loadings for several measures were high, which likely reduced model fit. This is consistent with the conceptual overlap commonly observed for self-reports of psychosocial functioning [40]. Third, the causal role of resiliency in the relationship between QoL and emotional distress in NF cannot be determined from this cross-sectional analysis. Fourth, we did not collect data on secondary diagnosis (e.g., schwannoma, ependymoma), age of diagnosis, and therapies. While prior research has revealed similar psychosocial profiles regardless of differences in NF pathophysiology [6], future studies are needed to confirm whether these clinical characteristics influence QoL outcomes.
Conclusion
Growing evidence that psychosocial factors, in addition to physical symptoms, influence QoL among NF patients, suggests a strong need for biopsychosocial models of care for NF. Emotional distress significantly interferes with QoL among this population and our results identified multiple resiliency factors that can buffer this association. To build on our partial mediation finding, we recommend that future research examines additional domains of resiliency (e.g., executive skills) that may explain the remaining variance in QoL for NF. Using the efficacy outcomes data from the completed RCT, we will prospectively explore resiliency as a mediator of pre-post improvements in QoL and emotional distress following the 3RP-NF. We also encourage research on mind–body and resiliency skills for promoting QoL in high-stress populations not represented in our sample, such as adolescents and adults with NF2 who are deaf.
Data availability
The authors have full control of all primary data and that they agree to allow the journal to review their data if requested.
Code availability
Not applicable.
References
Friedman JM (1999) Epidemiology of neurofibromatosis type 1. Am J Med Genet 89(1):1–6
Jouhilahti E-M, Peltonen S, Heape AM, Peltonen J (2011) The pathoetiology of neurofibromatosis 1. Am J Pathol 178(5):1932–1939. https://doi.org/10.1016/j.ajpath.2010.12.056
Evans D (1993) Neurofibromatosis 2. In: Adam M, Ardinger H, Pagon R, et al. (eds) Genereviews. https://scholar.google.com/scholar_lookup?title=GeneReviews&author=DG+Evans&publication_year=1993&
Hilton DA, Hanemann CO (2014) Schwannomas and their pathogenesis: schwannomas and their pathogenesis. Brain Pathol 24(3):205–220. https://doi.org/10.1111/bpa.12125
Lin AL, Gutmann DH (2013) Advances in the treatment of neurofibromatosis-associated tumours. Nat Rev Clin Oncol 10(11):616–624. https://doi.org/10.1038/nrclinonc.2013.144
Vranceanu A-M, Merker VL, Park E, Plotkin SR (2013) Quality of life among adult patients with neurofibromatosis 1, neurofibromatosis 2 and schwannomatosis: a systematic review of the literature. J Neurooncol 114(3):257–262. https://doi.org/10.1007/s11060-013-1195-2
Wang DL, Smith KB, Esparza S et al (2012) Emotional functioning of patients with neurofibromatosis tumor suppressor syndrome. Genet Med 14(12):977–982. https://doi.org/10.1038/gim.2012.85
Sanagoo A, Jouybari L, Koohi F, Sayehmiri F (2019) Evaluation of QoL in neurofibromatosis patients: a systematic review and meta-analysis study. BMC Neurol 19(1):123. https://doi.org/10.1186/s12883-019-1338-y
Rietman AB, van Helden H, Both PH et al (2018) Worries and needs of adults and parents of adults with neurofibromatosis type 1. Am J Med Genet A 176(5):1150–1160. https://doi.org/10.1002/ajmg.a.38680
Cosetti MK, Golfinos JG, Roland JT (2015) Quality of life (QoL) assessment in patients with neurofibromatosis type 2 (NF2). Otolaryngol Neck Surg 153(4):599–605. https://doi.org/10.1177/0194599815573002
Graf A, Landolt MA, Mori AC, Boltshauser E (2006) Quality of life and psychological adjustment in children and adolescents with neurofibromatosis type 1. J Pediatr 149(3):348–353. https://doi.org/10.1016/j.jpeds.2006.04.025
Hamoy-Jimenez G, Kim R, Suppiah S, Zadeh G, Bril V, Barnett C (2020) Quality of life in patients with neurofibromatosis type 1 and 2 in Canada. Neuro-Oncol Adv 2(Supplement_1):i141-i149. https://doi.org/10.1093/noajnl/vdaa003
Simon MK (2005) Meaning, coping and life satisfaction among individuals with neurofibromatosis type-1 (NF1).
Bonanno GA, Galea S, Bucciarelli A, Vlahov D (2007) What predicts psychological resilience after disaster? The role of demographics, resources, and life stress. J Consult Clin Psychol 75(5):671–682. https://doi.org/10.1037/0022-006X.75.5.671
Ovaska-Stafford N, Maltby J, Dale M (2021) Literature review: psychological resilience factors in people with neurodegenerative diseases. Arch Clin Neuropsychol 36(2):283–306. https://doi.org/10.1093/arclin/acz063
Zale EL, Heinhuis TJ, Tehan T, Salgueiro D, Rosand J, Vranceanu A-M (2018) Resiliency is independently associated with greater quality of life among informal caregivers to neuroscience intensive care unit patients. Gen Hosp Psychiatry 52:27–33. https://doi.org/10.1016/j.genhosppsych.2018.02.012
Zale EL, Pierre-Louis C, Macklin EA, Riklin E, Vranceanu A-M (2018) The impact of a mind–body program on multiple dimensions of resiliency among geographically diverse patients with neurofibromatosis. J Neurooncol 137(2):321–329. https://doi.org/10.1007/s11060-017-2720-5
Holland JN, Schmidt AT (2015) Static and dynamic factors promoting resilience following traumatic brain injury: a brief review. Neural Plast 2015:1–8. https://doi.org/10.1155/2015/902802
Granström S, Friedrich RE, Langenbruch AK, Augustin M, Mautner V-F (2014) Influence of learning disabilities on the tumour predisposition syndrome NF1–survey from adult patients’ perspective. Anticancer Res 34(7):3675–3681
Park ER, Traeger L, Vranceanu A-M et al (2013) The development of a patient-centered program based on the relaxation response: the relaxation response resiliency program (3RP). Psychosomatics 54(2):165–174. https://doi.org/10.1016/j.psym.2012.09.001
Vranceanu A-M, Zale EL, Funes CJ et al (2018) Mind-body treatment for international english-speaking adults with neurofibromatosis via live videoconferencing: protocol for a single-blind randomized controlled trial. JMIR Res Protoc 7(10):e11008. https://doi.org/10.2196/11008
Skevington SM, Lotfy M, O’Connell KA (2004) The World Health Organization’s WHOQOL-BREF quality of life assessment: psychometric properties and results of the international field trial. A Report from the WHOQOL Group. Qual Life Res 13(2):299–310. https://doi.org/10.1023/B:QURE.0000018486.91360.00
Kroenke K, Spitzer RL, Williams JBW (2001) The PHQ-9: validity of a brief depression severity measure. J Gen Intern Med 16(9):606–613. https://doi.org/10.1046/j.1525-1497.2001.016009606.x
Williams KG, Sanderson M, Jette N, Patten SB (2020) Validity of the patient health questionnaire-9 in neurologic populations. Neurol Clin Pract 10(3):190–198. https://doi.org/10.1212/CPJ.0000000000000748
Spitzer RL, Kroenke K, Williams JBW, Löwe B (2006) A brief measure for assessing generalized anxiety disorder: the GAD-7. Arch Intern Med 166(10):1092. https://doi.org/10.1001/archinte.166.10.1092
Johnson SU, Ulvenes PG, Øktedalen T, Hoffart A (2019) Psychometric properties of the general anxiety disorder 7-item (GAD-7) scale in a heterogeneous psychiatric sample. Front Psychol 10:1713. https://doi.org/10.3389/fpsyg.2019.01713
Cohen S, Kamarck T, Mermelstein R (1983) A global measure of perceived stress. J Health Soc Behav 24(4):385. https://doi.org/10.2307/2136404
Lee E-H (2012) Review of the psychometric evidence of the Perceived Stress Scale. Asian Nurs Res 6(4):121–127. https://doi.org/10.1016/j.anr.2012.08.004
Windle G, Bennett KM, Noyes J (2011) A methodological review of resilience measurement scales. Health Qual Life Outcomes 9:8. https://doi.org/10.1186/1477-7525-9-8
Vranceanu A-M, Riklin E, Merker VL, Macklin EA, Park ER, Plotkin SR (2016) Mind–body therapy via videoconferencing in patients with neurofibromatosis: an RCT. Neurology 87(8):806–814. https://doi.org/10.1212/WNL.0000000000003005
McCullough ME, Emmons RA, Tsang J-A (2002) The grateful disposition: a conceptual and empirical topography. J Pers Soc Psychol 82(1):112–127. https://doi.org/10.1037/0022-3514.82.1.112
Cousin L, Redwine L, Bricker C, Kip K, Buck H (2020) Psychometrics of the gratitude questionnaire-6 in African-Americans at risk for cardiovascular disease. West J Nurs Res 42(12):1148–1154. https://doi.org/10.1177/0193945920922777
Scheier MF, Carver CS (1985) Optimism, coping, and health: assessment and implications of generalized outcome expectancies. Health Psychol 4(3):219–247. https://doi.org/10.1037/0278-6133.4.3.219
Chiesi F, Galli S, Primi C, Innocenti Borgi P, Bonacchi A (2013) The accuracy of the life orientation test-revised (LOT–R) in measuring dispositional optimism: evidence from item response theory analyses. J Pers Assess 95(5):523–529. https://doi.org/10.1080/00223891.2013.781029
Carver C (2006) Measure of current status. http://www.psy.miami.edu/faculty/ccarver/sclMOCS.html
Antoni MH, Lechner SC, Kazi A et al (2006) How stress management improves quality of life after treatment for breast cancer. J Consult Clin Psychol 74(6):1143–1152. https://doi.org/10.1037/0022-006X.74.6.1143
Feldman G, Hayes A, Kumar S, Greeson J, Laurenceau J-P (2007) Mindfulness and emotion regulation: the development and initial validation of the cognitive and affective mindfulness scale-revised (CAMS-R). J Psychopathol Behav Assess 29(3):177–190. https://doi.org/10.1007/s10862-006-9035-8
Hayes AF (2013) Introduction to mediation, moderation, and conditional process analysis: a regression-based approach. The Guilford Press
Ludolph P, Kunzler AM, Stoffers-Winterling J, Helmreich I, Lieb K (2019) Interventions to promote resilience in cancer patients. Dtsch Aerzteblatt. https://doi.org/10.3238/arztebl.2019.0865
Campbell P, Bishop A, Dunn KM, Main CJ, Thomas E, Foster NE (2013) Conceptual overlap of psychological constructs in low back pain. Pain 154(9):1783–1791. https://doi.org/10.1016/j.pain.2013.05.035
Funding
This work was supported by the U.S. Department of Defense (Grant Number: W81XWH-17-1-0121).
Author information
Authors and Affiliations
Contributions
RM conducted the analyses and wrote the manuscript. JD assisted results interpretation and manuscript writing. JB assisted data analysis, results interpretation, and manuscript writing. JC assisted manuscript writing and preparation. AMV conceptualized the study and guided manuscript preparation. All authors reviewed and agreed with the final manuscript prior to submission.
Corresponding author
Ethics declarations
Conflict of interest
The authors report no conflicts of interest.
Ethical approval
Partners Healthcare Human Research Committee has approved the procedures (IRB # 2020P003067 and 2020P004087). The authors certify that the study was performed in accordance with the ethical standards in the 1964 Declaration of Helsinki and its amendments.
Consent to participate
All participants provided written informed consent.
Consent for publication
The authors affirm that human research participants provided informed consent for publication.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Mace, R.A., Doorley, J., Bakhshaie, J. et al. Psychological resiliency explains the relationship between emotional distress and quality of life in neurofibromatosis. J Neurooncol 155, 125–132 (2021). https://doi.org/10.1007/s11060-021-03852-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-021-03852-1