Abstract
The neurofibromatoses (NF) are incurable genetic disorders that can cause nerve sheath tumors, chronic pain, and disfiguration. Patients with NF report lower quality of life and greater distress, and may benefit from programs that promote resiliency. To test effects of an 8-week mind–body program (Relaxation Response Resiliency Program for NF [3RP-NF]) on resiliency, using data derived from a larger randomized controlled trial of the 3RP-NF versus attention placebo control (Vranceanu et al. in Neurology 87:806–814, 2016). Participants (N = 63; 46 female; 52 White) were randomized to 3RP-NF (n = 32, M age = 42.86) or control (n = 31, M age = 39.90), completed intervention sessions via group videoconferencing, and provided self-report measures of resiliency (i.e., perceived coping abilities, perceived social support, gratitude, optimism, spiritual well-being, mindfulness) at baseline, post-intervention, and 6-month follow-up. All participants attended at least 6/8 sessions and 83% (N = 52) provided 6-month follow-up data. The 3RP-NF (vs. control) produced greater improvements from pre- to post-intervention in perceived coping abilities (M difference = 6.68; p = .008), perceived social support (M difference = 9.16; p = .032), and mindfulness (M difference = 2.23; p = .035), which were maintained at 6-month follow up. We did not observe group differences in spiritual well-being, optimism, or gratitude. The 3RP-NF produced sustained increases in multiple dimensions of resiliency (perceived coping abilities, perceived social support, and mindfulness). Promoting resiliency may be particularly important for a population that is underserved and living with a chronic, incurable illness.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The neurofibromatoses (NF) are a group of heterogeneous genetic disorders (NF1, NF2, and schwannomatosis) that predispose patients to develop nerve sheath tumors, which can occur anywhere in the body and cause disfiguring cutaneous tumors (NF1); hearing loss, facial weakness, and poor gait (NF2); and chronic pain (schwannomatosis). NF1 is the most common of the neurofibromatoses, occurring approximately 1:2700 live births [1], and NF2 and schwannomatosis each have estimated birth incidences of 1:25,000–33,000 [2,3,4]. There is no cure for NF, and surgery and palliative measures are the primary means of treatment.
Patients with NF have lower quality of life [5], greater symptoms of depression and anxiety, higher levels of stress, more pain, and lower self-esteem, relative to population norms [6,7,8,9]. The level of emotional distress in patients with NF is comparable to that of patients with other medical conditions (e.g., cancer) [6]. Disturbances in emotional functioning appear to be independent of NF severity [6, 10], suggesting that psychosocial factors play an important role in determining patients’ experiences of NF. Despite differential biological mechanisms of disease, the psychosocial profile is similar among patients with NF1, NF2 and schwannomatosis [5, 6]. Similar to patients with other chronic illnesses [11], patients with NF who self-report more difficulty coping and depression symptoms also undergo more medical visits [12].
Resiliency—the process of adaptation or ‘bouncing back’ in the face of adversity [13,14,15]—is a multidimensional construct that has positive associations with numerous health outcomes [16]. Several modifiable psychosocial factors that have been shown to promote successful adaptation include: coping skills (i.e., the ability to utilize multiple coping strategies effectively) [17, 18]; mindfulness (i.e., the ability to remain attentive without making judgment) [19, 20]; social support (i.e., the ability to meet needs through interpersonal interactions) [21, 22]; gratitude (i.e., the ability to appreciate what one has) [23]; optimism (i.e., holding “generalized favorable expectancies”) [24]; and spiritual well-being (i.e. a sense of meaning, peace, and the role of faith) [25].
Promoting resiliency is particularly relevant to patients with NF who live with a progressive, incurable disease. Vranceanu et al. recently adapted a Relaxation Response Resiliency Program to address needs of the NF population (i.e., 3RP-NF) [26], including intervention delivery via secure videoconferencing to reduce barriers to care (e.g., travel) [27]. Although components of the 3RP-NF were designed to address a complex interplay of psychosocial resiliency factors [28], Vranceanu and colleagues’ pilot randomized controlled trial was designed as a feasibility and acceptability trial, and primary outcomes were quality of life and mental health symptoms. Relative to the attention placebo control, the 3RP-NF produced sustained increases in Physical, Psychological, Environmental, and Social Quality of Life and anxiety symptoms [26].
An important next step in this line of research is to understand the effects of the 3RP-NF on its proximal treatment targets, including resiliency. These additional analyses are necessary, because understanding which targets were most robustly impacted will inform future iterations of treatment development. The purpose of this secondary analysis is to examine effects of the 3RP-NF on multiple dimensions of resiliency. We hypothesized that participants randomized to 3RP-NF (vs. control) would demonstrate improvements in perceived coping abilities, perceived social support, mindfulness, gratitude, optimism, and spiritual well-being at post-intervention, which would be maintained at 6-month follow-up.
Methods
Patient population and data source
Participants included 63 patients with NF who enrolled in a pilot feasibility and acceptability trial of the 3RP-NF (NCT# 02298270). Details regarding recruitment and study design have been published previously [26]. All study procedures were approved by our Institutional Review Board. We recruited a geographically diverse sample via an email to the NF registry (http://www.ctf.org/understanding-nf/nf-registry), which advertised groups for patients with difficulty coping with NF. Potential participants were screened in an interview via Skype for inclusion (NF diagnosis; age ≥ 18; ability to read English, provide informed consent and comply with study procedures; self-reported difficulty coping with NF) and exclusion criteria (severe psychopathology; unwilling or unable to use Skype). Informed consent was obtained from all individual participants included in the study. After providing informed consent, participants completed baseline questionnaires via a secure web portal (REDCap) [29] and were randomized to intervention condition. Post-treatment questionnaires were completed via REDCap within 1 week after the final session and at 6-month follow-up.
Active and control intervention conditions
A detailed description of active and control conditions has been published previously [26]. Both interventions were conducted across eight 90-min group sessions Vranceanu et al. who have prior experience working with the NF population [26]. All sessions were conducted via Skype videoconferencing, and followed fidelity guides and participant manuals. Sessions were conducted during weekends to accommodate heterogenous time zones and maximize participation.
Active intervention
The 3RP-NF was adapted from the Relaxation Response Resiliency Program [28] based on qualitative data collected via in-person focus groups and exit interviews with NF patients following an open-label pilot [30]. The 3RP-NF is aimed at increasing resiliency through integration of three interrelated components: (1) Relaxation Response-Elicitation, (2) Appraisal and Coping, and (3) Growth Enhancement. The Relaxation Response-Elicitation includes techniques that are designed to elicit a state of calm and awareness, and a primary target is mindfulness (see Fig. 1). Components of Appraisal and Coping are designed to facilitate adaptive thinking in the face of NF-related stressors, and a primary target is perceived coping ability. Growth enhancement addresses connectedness to self and others, and primary targets include perceived social support, spiritual well-being, optimism, and gratitude.
Control intervention
The Health Enhancement Program for NF (HEP-NF) [26] provides psychoeducation to enhance general health (e.g., exercise, nutrition, patient-provider communication). NF-specific adaptations were made utilizing educational materials from the Children’s Tumor Foundation and the Center for Disease Control. All sessions followed the same format as the 3RP-NF (e.g., each session began with review).
Measures
Perceived coping abilities
The Measure of Current Status-A (MOCS-A) [31] uses 13-items to assess perceived ability in using relaxation, recognizing tension and stress-inducing situations, assertiveness, and ability to restructure thoughts and choose appropriate coping responses. Items are rated on a scale from 0 (I cannot do this at all) to 4 (I can do this extremely well) and summed to create a total score with higher scores representing greater perceived coping ability (range: 0–52).
Perceived social support
The Medical Outcomes Study Social Support Survey (MOS) [32] is a 19-item measure that assesses perceived availability of social support across four domains: emotional, tangible, affectionate, and positive social interaction. Items are rated on a scale from 1 (none of the time) to 5 (all of the time) and summed to create a total score with higher scores representing greater perceived social support (range: 19–95).
Gratitude
The Gratitude Questionnaire (GQ-6) [33] is a 6-item measure that assesses experience of gratitude in daily life. Items are rated on a scale from 1 (strongly disagree) to 7 (strongly agree) and summed to create a total score with higher scores representing a greater disposition towards gratitude (range: 6–42).
Optimism
Life Orientation Test Optimism Scale (LOT) [34] is an 8-item measure that assesses the tendency towards optimism vs. pessimism. Items are rated on a scale from 0 (I disagree a lot) to 4 (I agree a lot), reverse coded as appropriate, and summed to generate a total score (range: 0–32) with higher scores representing greater optimism (i.e., holding “generalized favorable expectancies for the future”) [24].
Spiritual well-being
Functional Assessment of Chronic Illness Therapy-Spiritual Well-Being Scale (FACIT-Sp) [25] is a 12-item measure that assesses a sense of meaning, peace, and faith, during the past 7 days. Items are rated on a scale from 0 (not at all) to 4 (very much) and summed to create a total score and three facet scores (meaning, peace and faith) with higher scores representing greater spiritual well-being (total score range: 0–48; facet score ranges:0–16).
Mindfulness
The Cognitive and Affective Mindfulness Scale (CAMS) [35] is a 12-item measure that assesses the degree to which individuals are mindful of and experience their thoughts and feelings in the present moment. Items are rated on a scale from 1 (rarely/not at all) to 4 (almost always) and summed to create a total score with higher scores representing greater mindfulness (range: 12–48).
Data analytic strategy
We conducted secondary data analysis of a randomized controlled trial [26] to test the hypothesis that participating in the 3RP-NF increased resiliency factors. We utilized mixed-model repeated-measures ANOVA to test the effects of treatment condition across time. Linear contrasts were used to compare the effect of the intervention on changes from baseline to post-intervention and from the post-intervention to 6-month follow-up. To reduce the threat of bias, analyses followed the intent-to-treat principles. Use of a mixed model permitted inclusion of participants lost to follow-up and yields unbiased estimates assuming that data were missing at random conditional on the observed trajectories. All analyses were conducted using the statistical program SPSS Version 24 (IBM Corp, 2016).
Power analyses
The target sample size of 30 completers per condition was based on recommendations for sample sizes for pilot RCTs and was considered to yield stable estimates of means and variance components based on recommendations for psychosocial clinical trials [26, 36,37,38,39]. A priori power analyses also indicated that a sample size of 30 completers per condition would provide sufficient power (≥ 0.80) to detect mean differences between groups that would be considered large in magnitude (d = 0.8) [40].
Results
Sample characteristics and attrition
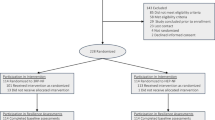
The sample demographics and attrition have been previously described [26]. All eligible participants (N = 63; 46 female, 52 White) attended at least 6/8 sessions, provided posttest assessments (100%), and 83% completed the six-month follow-up assessment (N = 52; 33% attrition in the HEP-NF group). No differences in demographics or study variables were observed between completers and non-completers. The sample was geographically diverse, with participants from Canada (n = 6), Australia (n = 1), England (n = 3) and 22 states within the United States (n = 53). No differences in demographic characteristics were observed across treatment condition. Sociodemographics are presented in Table 1, participant flow is presented in Fig. 2 and Table 2 presents unadjusted means for the outcome variable at each time point.
Post-intervention outcomes
Participation in 3RP-NF resulted in greater improvement in perceived coping abilities (M difference = 6.68; 95% CI 1.78–11.58; p = .008; d = 1.17), perceived social support (M difference = 9.16; 95% CI 0.82–17.50; p = .032; d = 0.63), and mindfulness (M difference = 2.23; 95% CI 0.16–4.29; p = .035; d = 1.19), relative to HEP-NF. Specifically, for perceived coping abilities, participants in 3RP-NF improved by 8.96 points on average (95% CI 5.51–12.43; p < .001), while those in the HEP-NF improved on average by 2.29 points (95% CI − 1.18–5.77; p = .19). On average, participants in 3RP-NF reported a 5.03 point increase in perceived social support (95% CI − 0.75–10.82; p = .087), whereas participants in HEP-NF reported a 4.13 point decrease in perceived social support (95% CI− 10.13–1.88, p = .174). Finally, participants in 3RP-NF reported a 2.97 point increase in mindfulness (95% CI 1.52–4.42; p < .001), on average, while participants in HEP-NF reported an average increase of 0.74 points (95% CI − 0.73–2.22; p = .318).
We did not observe group differences on spiritual well-being scores for neither the total score (M difference = 1.64; 95% CI − 1.66–4.93; p = .325), nor the Meaning (M difference = 0.72; 95% CI − 0.48–1.93; p = .233), Peace (M difference = 0.82; 95% CI − 0.28–1.94; p = .142), or Faith (M difference = 0.51; 95% CI − 0.60–1.58; p = .345) facets. No differences as a function of intervention condition were observed with regard to gratitude (M difference = 2.04; 95% CI − 0.57–4.65; p = .123) or optimism (M difference = 1.55; 95% CI − 0.75–3.86; p = .182).
Six-month follow-up outcomes
Participants in the 3RP-NF maintained their posttest improvement in perceived coping abilities, perceived social support, and mindfulness. Analyses showed no difference between groups in change between posttest and 6-month follow-up for perceived coping abilities (M difference = − 2.72; 95% CI − 7.73–2.29, p = .281), perceived social support (M difference = − 2.62, 95% CI − 11.49–6.25; p = .555), and mindfulness (M difference = − 1.30; 95% CI − 3.44–0.84; p = .228), suggesting no additional differential group response during the follow-up period. Improvements in resiliency throughout the study period are presented in Fig. 3.
Average improvements in resiliency factors, as a function of group assignment, at baseline, post-treatment, and 6-month follow-up. Participants were randomized to either the active (3RP-NF) or control (HEP-NF) intervention. Separate graphs are depicted with group mean scores for a perceived coping abilities, b perceived social support, and c mindfulness, respectively. HEP-NF Health Enhancement Program for neurofibromatosis; 3RP-NF Relaxation Response Resiliency Program for neurofibromatosis. Significant differences at post-test are depicted with *p < .05; **p < .01. Linear contrasts revealed that differences remained stable from post-test to 6-month follow-up
Discussion
Although previous work has demonstrated that the 3RP-NF improves quality of life among patients with NF [26], this is the first study to examine its effects on multiple dimensions of resiliency. Patients who received 3RP-NF (vs. HEP-NF) reported greater improvements in perceived coping abilities, perceived social support, and mindfulness, which were sustained during the 6-month follow-up period. No differences between treatment conditions were observed for spiritual wellbeing, gratitude, or optimism.
Patients with NF encounter multiple disease-related stressors, including uncertainty about prognosis, disfigurement, and pain. Current medical treatments are limited to surgical interventions and palliative care, and there is an increasing interest in factors associated with successful adaptation to NF. The ability to cope with disease-related stressors, access social support, and attend to symptoms and stress non-judgmentally have been shown to improve health outcomes in other populations [41,42,43] and identified as important targets for psychosocial interventions for medical illness [43, 44]. Thus, it is encouraging to observe that the 3RP-NF (vs. HEP-NF) produced sustainable increases in perceived coping abilities, perceived social support, and mindfulness, which were targeted individually by each of the three respective treatment components (appraisal and coping, growth enhancement, relaxation methods).
It is possible that we were unable to detect significant differences in spiritual well-being, optimism, and gratitude due to the small sample size and pilot nature of the current study. Within-group analyses revealed increases in optimism and spiritual well-being within the 3RP-NF group, suggesting that optimism and spiritual well-being should be studied in larger trials. Additionally, spiritual well-being, optimism, and gratitude were resiliency dimensions targeted by the growth enhancement treatment component. Given that we did observe significant increases in perceived social support, which was also identified as a target of the growth enhancement component, future research should examine whether additional treatment components are needed to facilitate growth enhancement.
Strengths of the current study include a multidimensional assessment of resiliency, limited attrition, 6-month follow-up period, and use of videoconferencing. Telemedicine can remove barriers to care including lack of access (e.g., in rural areas) and the time and cost associated with travel [27]. Our team [26] examined the acceptability of delivering the 3RP-NF intervention via videoconferencing and concluded that patients with NF were particularly amenable to learning psychosocial skills via teleconferencing and that telemedicine may be an optimal means of reducing barriers to treatment among patients with NF.
Despite these strengths, several limitations should be discussed. First, the clinical trial was primarily designed to address acceptability and feasibility, and was powered to detect only large effect sizes. As such, we may have been unable to detect small to medium effects of the 3RP-NF on our outcome variables. Second, resiliency is a multidimensional construct that can be difficult to operationalize [45]. Although we utilized multiple reliable and valid measures of factors related to resiliency, future research should also examine additional factors (e.g., emotion regulation, distress tolerance, intolerance of uncertainty) that may be related to resiliency. Future studies should also assess biological factors associated with resiliency. For example, researchers have proposed that improvements in resiliency constructs (e.g., perceived social support, perceived coping abilities) could have protective effects on physiological stress-responses in both the hypothalamic pituitary adrenal (HPA) axis and the sympathetic nervous system [46]. We were also unable to collect a thorough medical history or conduct neuropsychological assessments, and it is not clear to what extent resiliency and improvements over the course of the study may be associated with prior medical history or comorbidities (e.g., surgical treatments, comorbid chronic pain syndromes, neuropsychological deficits). Third, our assessments at post-intervention and 6-month follow-up did not allow us to examine changes in resiliency through the course of treatment. Additional research should examine the trajectory of changes in resiliency in order to determine whether such also lead to improved disease outcomes and long-term quality of life, or whether improved resiliency may serve as a factor that enhances treatment engagement. We also observed a 33% attrition in the HEP-NF group at 6-month follow up. It is unknown whether attrition in the control condition could have been affected by either a delayed improvement in resiliency (i.e., participants who improved later may have dropped out when feeling better) or a decrement in resiliency (i.e., participants may have dropped out if they were experiencing more difficulty in multiple resiliency domains) from post-intervention to 6-month follow-up. Fourth, all intervention sessions were delivered by Vranceanu et al. [26]. Although we took steps to promote treatment fidelity via the use of fidelity guides and patient manuals, fidelity was not assessed by independent raters. Finally, our sample was predominantly white, female, employed, and well educated. Baseline scores on resiliency factors (e.g., coping, mindfulness) were similar to scores previously observed among patients with NF and other neurological conditions [26, 30], however, norms for the resiliency measures are not available in NF patients, and it is not known the extent to which participants’ baseline scores on the resiliency measures are representative of the greater NF population. Therefore, although we sought increase generalizability via recruitment of a geographically diverse sample (i.e., patients from 4 countries and 22 US states), future research is needed to determine how well results generalize to a larger NF sample.
The 3RP-NF intervention has previously been shown to improve short-term quality of life among NF patients [26], and our results indicate that 3RP-NF also increases multiple factors related to resiliency. The intervention produced increases in perceived coping abilities, perceived social support, and mindfulness, which were sustained at 6-month follow-up. Taken together, our results indicate that psychosocial interventions can promote resilience among patients with NF and that 3RP-NF may be efficacious in targeting multiple dimensions of resiliency. Results also have the potential to inform future treatment development for patients with NF. For example, given known positive associations between resiliency and mental and physical health outcomes [47,48,49], interventions that promote resiliency, such as the 3RP-NF, may be investigated for the treatment of multiple concerns (e.g., depression, anxiety, disease-related symptoms).
References
Evans DG, Howard E, Giblin C et al (2010) Birth incidence and prevalence of tumor-prone syndromes: estimates from a UK family genetic register service. Am J Med Genet A 152A:327–332. https://doi.org/10.1002/ajmg.a.33139
Antinheimo J, Sankila R, Carpén O, Pukkala E, Sainio M, Jääskeläinen J (2000) Population-based analysis of sporadic and type 2 neurofibromatosis-associated meningiomas and schwannomas. Neurology 54:71–76
Asthagiri AR, Parry DM, Butman JA et al (2009) Neurofibromatosis type 2. Lancet Lond Engl 373:1974–1986. https://doi.org/10.1016/S0140-6736(09)60259-2
Lu-Emerson C, Plotkin SR (2009) The neurofibromatoses. Part 2: NF2 and schwannomatosis. Rev Neurol Dis 6:E81–E86
Vranceanu A-M, Merker VL, Park E, Plotkin SR (2013) Quality of life among adult patients with neurofibromatosis 1, neurofibromatosis 2 and schwannomatosis: a systematic review of the literature. J Neurooncol 114:257–262. https://doi.org/10.1007/s11060-013-1195-2
Wang DL, Smith KB, Esparza S et al (2012) Emotional functioning of patients with neurofibromatosis tumor suppressor syndrome. Genet Med 14:977. https://doi.org/10.1038/gim.2012.85
Wolkenstein P, Zeller J, Revuz J, Ecosse E, Leplège A (2001) Quality-of-life impairment in neurofibromatosis type 1: a cross-sectional study of 128 cases. Arch Dermatol 137:1421–1425
Page PZ, Page GP, Ecosse E, Korf BR, Leplege A, Wolkenstein P (2006) Impact of neurofibromatosis 1 on quality of life: a cross-sectional study of 176 American cases. Am J Med Genet A 140A:1893–1898. https://doi.org/10.1002/ajmg.a.31422
Kodra Y, Giustini S, Divona L et al (2009) Health-related quality of life in patients with neurofibromatosis type 1. A survey of 129 Italian patients. Dermatol Basel Switz 218:215–220. https://doi.org/10.1159/000187594
Rumsey N, Harcourt D (2004) Body image and disfigurement: issues and interventions. Body Image 1:83–97. https://doi.org/10.1016/S1740-1445(03)00005-6
Brantley PJ, Dutton GR, Grothe KB, Bodenlos JS, Howe J, Jones GN (2005) Minor life events as predictors of medical utilization in low income African American family practice patients. J Behav Med 28:395–401. https://doi.org/10.1007/s10865-005-9001-z
Carlson LE, Bultz BD (2003) Benefits of psychosocial oncology care: improved quality of life and medical cost offset. Health Qual Life Outcomes 1:8. https://doi.org/10.1186/1477-7525-1-8
Bonanno GA, Galea S, Bucciarelli A, Vlahov D (2007) What predicts psychological resilience after disaster? The role of demographics, resources, and life stress. J Consult Clin Psychol 75:671–682. https://doi.org/10.1037/0022-006X.75.5.671
Shaffer KM, Riklin E, Jacobs JM, Rosand J, Vranceanu A-M (2016) Psychosocial resiliency is associated with lower emotional distress among dyads of patients and their informal caregivers in the neuroscience intensive care unit. J Crit Care 36:154–159. https://doi.org/10.1016/j.jcrc.2016.07.010
Windle G (2011) What is resilience? A review and concept analysis. Rev Clin Gerontol 21:152–169. https://doi.org/10.1017/S0959259810000420
Tugade MM, Fredrickson BL, Feldman Barrett L (2004) Psychological resilience and positive emotional granularity: examining the benefits of positive emotions on coping and health. J Pers 72:1161–1190. https://doi.org/10.1111/j.1467-6494.2004.00294.x
Steinhardt M, Dolbier C (2008) Evaluation of a resilience intervention to enhance coping strategies and protective factors and decrease symptomatology. J Am Coll Health 56:445–453. https://doi.org/10.3200/JACH.56.44.445-454
Tait L, Birchwood M, Trower P (2004) Adapting to the challenge of psychosis: personal resilience and the use of sealing-over (avoidant) coping strategies. Br J Psychiatry 185:410–415. https://doi.org/10.1192/bjp.185.5.410
Fiol CM, O’Connor EJ (2003) Waking up! Mindfulness in the face of bandwagons. Acad Manage Rev 28:54–70. https://doi.org/10.2307/30040689
Thompson RW, Arnkoff DB, Glass CR (2011) Conceptualizing mindfulness and acceptance as components of psychological resilience to trauma. Trauma Violence Abuse 12:220–235. https://doi.org/10.1177/1524838011416375
Horton TV, Wallander JL (2001) Hope and social support as resilience factors against psychological distress of mothers who care for children with chronic physical conditions. Rehabil Psychol 46:382–399. https://doi.org/10.1037/0090-5550.46.4.382
Tsai J, Harpaz-Rotem I, Pietrzak RH, Southwick SM (2012) The role of coping, resilience, and social support in mediating the relation between PTSD and social functioning in veterans returning from Iraq and Afghanistan. Psychiatry 75:135–149. https://doi.org/10.1521/psyc.2012.75.2.135
Pentz M (2005) Resilience among older adults with cancer and the importance of social support and spirituality-faith. J Gerontol Soc Work 44:3–22. https://doi.org/10.1300/J083v44n03_02
Carver CS, Scheier MF, Segerstrom SC (2010) Optimism. Clin Psychol Rev 30:879–889. https://doi.org/10.1016/j.cpr.2010.01.006
Peterman AH, Fitchett G, Brady MJ, Hernandez L, Cella D (2002) Measuring spiritual well-being in people with cancer: the functional assessment of chronic illness therapy-spiritual well-being scale (FACIT-Sp). Ann Behav Med 24:49–58
Vranceanu A-M, Riklin E, Merker VL, Macklin EA, Park ER, Plotkin SR (2016) Mind-body therapy via videoconferencing in patients with neurofibromatosis: an RCT. Neurology 87:806–814. https://doi.org/10.1212/WNL.0000000000003005
Vockley M (2015) The rise of telehealth: “Triple Aim,” innovative technology, and popular demand are spearheading new models of health and wellness care. Biomed Instrum Technol Assoc Adv Med Instrum 49:306–320. https://doi.org/10.2345/0899-8205-49.5.306
Park ER, Traeger L, Vranceanu A-M et al (2013) The development of a patient-centered program based on the relaxation response: the relaxation response resiliency program (3RP). Psychosomatics 54:165–174. https://doi.org/10.1016/j.psym.2012.09.001
Harris PA (2012) Research electronic data capture (REDCap): planning, collecting and managing data for clinical and translational research. BMC Bioinform 13:1–1. https://doi.org/10.1186/1471-2105-13-S12-A15
Vranceanu A-M, Merker VL, Plotkin SR, Park ER (2014) The relaxation response resiliency program (3RP) in patients with neurofibromatosis 1, neurofibromatosis 2, and schwannomatosis: results from a pilot study. J Neurooncol 120:103–109. https://doi.org/10.1007/s11060-014-1522-2
Carver C (2006) Measaure of current status. http://www.psy.miami.edu/faculty/ccarver/sclMOCS.html
Sherbourne CD, Stewart AL (1991) The MOS social support survey. Soc Sci Med 1982 32:705–714
Mccullough ME, Emmons RA, Tsang J-A (2002) The grateful disposition: a conceptual and empirical topography. J Pers Soc Psychol 82:112–127. https://doi.org/10.1037/0022-3514.82.1.112
Scheier MF, Carver CS (1985) Optimism, coping, and health: assessment and implications of generalized outcome expectancies. Health Psychol Off J Div Health Psychol Am Psychol Assoc 4:219–247
Feldman G, Hayes A, Kumar S, Greeson J, Laurenceau J-P (2007) Mindfulness and emotion regulation: the development and initial validation of the cognitive and affective mindfulness scale-revised (CAMS-R). J Psychopathol Behav Assess 29:177–190. https://doi.org/10.1007/s10862-006-9035-8
Browne RH (1995) On the use of a pilot sample for sample size determination. Stat Med 14:1933–1940. https://doi.org/10.1002/sim.4780141709
Lancaster GA, Dodd S, Williamson PR (2004) Design and analysis of pilot studies: recommendations for good practice. J Eval Clin Pract 10:307–312. https://doi.org/10.1111/j..2002.384.doc.x
Shih WJ, Ohman-Strickland PA, Lin Y (2004) Analysis of pilot and early phase studies with small sample sizes. Stat Med 23:1827–1842. https://doi.org/10.1002/sim.1807
Whitehead AL, Julious SA, Cooper CL, Campbell MJ (2005) Estimating the sample size for a pilot randomised trial to minimise the overall trial sample size for the external pilot and main trial for a continuous outcome variable. Stat Methods Med Res. https://doi.org/10.1177/0962280215588241
Rounsaville BJ, Carroll KM, Onken LS (2001) A stage model of behavioral therapies research: getting started and moving on from stage I. Clin Psychol Sci Pract 8:133–142. https://doi.org/10.1093/clipsy.8.2.133
Grossman P, Niemann L, Schmidt S, Walach H (2004) Mindfulness-based stress reduction and health benefits. A meta-analysis. J Psychosom Res 57:35–43. https://doi.org/10.1016/S0022-3999(03)00573-7
Penley JA, Tomaka J, Wiebe JS (2002) The association of coping to physical and psychological health outcomes: a meta-analytic review. J Behav Med 25:551–603
Wang H-H, Wu S-Z, Liu Y-Y (2003) Association between social support and health outcomes: a meta-analysis. Kaohsiung J Med Sci 19:345–351. https://doi.org/10.1016/S1607-551X(09)70436-X
Ridder D de, Schreurs K (1996) Coping, social support and chronic disease: a research agenda. Psychol Health Med 1:71–82. https://doi.org/10.1080/13548509608400007
Luthar SS, Cicchetti D, Becker B (2001) The construct of resilience: a critical evaluation and guidelines for future work. Child Dev 71:543–562
Bower JE, Moskowitz JT, Epel E (2009) Is benefit finding good for your health? Pathways linking positive life changes after stress and physical health outcomes. Curr Dir Psychol Sci 18:337–341
Davydov DM, Stewart R, Ritchie K, Chaudieu I (2010) Resilience and mental health. Clin Psychol Rev 30:479–495. https://doi.org/10.1016/j.cpr.2010.03.003
Logan-Greene P, Green S, Nurius PS, Longhi D (2014) Distinct contributions of adverse childhood experiences and resilience resources: a cohort analysis of adult physical and mental health. Soc Work Health Care 53:776–797. https://doi.org/10.1080/00981389.2014.944251
Terrill AL, Molton IR, Ehde DM et al (2016) Resilience, age, and perceived symptoms in persons with long-term physical disabilities. J Health Psychol 21:640–649. https://doi.org/10.1177/1359105314532973
Funding
This study was fully funded by the Children’s Tumor Foundation through a clinical research grant awarded to Ana-Maria Vranceanu.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Emily L. Zale declares that she has no conflict of interest. Catherine Pierre-Louis declares that she has no conflict of interest. Eric A. Macklin declares that he has no conflict of interest. Eric Riklin declares that he has no conflict of interest. Ana-Maria Vranceanu declares that she has no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Zale, E.L., Pierre-Louis, C., Macklin, E.A. et al. The impact of a mind–body program on multiple dimensions of resiliency among geographically diverse patients with neurofibromatosis. J Neurooncol 137, 321–329 (2018). https://doi.org/10.1007/s11060-017-2720-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-017-2720-5