Abstract
Glioblastoma (GBM) is the most aggressive malignant brain tumor in adults. Improvements in the treatment of GBM have remained static since the advent of the standard therapy which includes radiation with concurrent and adjuvant temozolomide treatment. Developing treatment and diagnostic or companion biomarker combinations is transforming the way we treat numerous cancers. However, can this emerging paradigm be also effective for GBM? Can GBM be treated the same way as other cancers? Here we review the challenges for a personalized molecular targeted therapeutic approach in GBM. The specific challenges for establishing a personalized molecular targeted medicine program for GBM patients include overcoming the blood brain barrier, unravelling the intra- and inter-heterogeneity that exists and the importance of developing more relevant animal models that recapitulate a patient’s GBM tumor.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The survival trends for patients diagnosed with glioblastoma (GBM) have remained largely static, reflecting a lack of improvement in the therapeutic options for patients. Prognosis is poor for most patients diagnosed with GBM and less than 5 % of newly diagnosed GBM survive more than 5 years. GBM are highly refractory to treatment with local tumor recurrence occurring 2–3 cm from the original resection cavity (the area exposed to radiation treatment) frequently observed. Relapsed GBMs are difficult to manage with a median survival of only a few months after recurrence [1]. Increasingly, the development of novel therapies involve defining drug-diagnostic combinations where the presence of a molecular target or marker identifies patients who are most likely to respond to a specific therapy. This model of developing treatment and diagnostic/companion biomarker combinations is the emerging paradigm for novel drug and diagnostic development [2–4] with a recent example being the use of BRAF inhibitors, which target a specific activating mutation of BRAF (V600E) in melanoma [5]. GBM is characterized by inter- and intra-patient genomic and histopathological diversity, arising from the complex dynamics that underpin its development. Given this, a single “bullet” approach is unrealistic.
Temozolomide (TMZ) chemotherapy improves the survival of patients with GBM by a few months when used in combination with radiation therapy [6, 7]. However, GBMs with methylation and suppression of the O-6-Methylguanine DNA methyltransferase (MGMT) promoter region of the gene are more sensitive to TMZ [7, 8]. Rindopepimut (Rintega®) received Breakthrough Therapy Designation from the FDA to treat epidermal growth factor receptor variant III deletion mutation (EGFRvIII) positive GBM [9]. Results from the ACT III study showed a median overall survival of 21.8 months, and 36-month overall survival was 26 % [9]. In the future, as more chemotherapeutic agents with similar efficacy are developed based on molecular alterations, it may be possible to design clinical trials assessing the differential sensitivities of patients with different molecular signatures and alterations to chemotherapy.
The aim of this paper is to discuss the challenges that are possibly faced in the practical application of an individualized medicine approach for GBM patients, from molecular challenges to translating the results to the bedside.
Molecular subtypes of GBM
Breakthroughs in human genomics have led to exciting prospects in the field of cancer therapy. The profiling of the human genome has given scientists and researchers an insight into the possibilities of the DNA being the root source of a person’s susceptibility to a certain disease or condition. This discovery has led to an era of—omics technology, where treatment is focused on molecular targets specific to a patient’s genomic data. GBM was the first malignancy to be studied by The Cancer Genome Atlas (TCGA) Research Network [10]. The key aims of TCGA are “to identify the changes in each cancer’s genome and understand how these changes interact to drive the disease, thereby laying the foundation for improved cancer prevention, early detection and treatment”, with priority afforded to cancers associated with the highest disease burden. TCGA GBM project, conducted in two phases, has provided a comprehensive genome-wide map of the genetic, epigenetic and transcriptomic changes, as well as proteomic changes, in over 500 GBM samples [10, 11]. This led to the identification of four distinct molecular subtypes of GBM on the basis of signatory gene expression profiles, namely classical, mesenchymal, neural, and proneural. These have also been associated with particular genetic alterations [12]. The Classical subtype is associated with an astrocytic expression profile, with frequent EGFR amplification, concomitant chromosome 7 amplification and chromosome 10 loss, and focal deletions of 9p encompassing CDKN2A. Although TP53 mutations are common in GBM, the Classical subtype lacks these. The mesenchymal subtype is typified by the expression of mesenchymal markers, with frequent deletions or mutations of the NF1 and PTEN genes. The neural subtype exhibits expression of neuronal markers and displays various mutations and copy number alterations including amplification of EGFR and deletion of PTEN. The proneural subtype exhibits an oligodendrocytic expression signature and is characterized by focal amplifications of the chromosome 4q12 region containing the oligodendrocytic development gene PDGFRA, or mutations of the isocitrate dehydrogenase 1 gene, IDH1.
In terms of prognosis, no difference was found between the classical, mesenchymal and neural subtypes. However, the Proneural subtype was associated with younger age and prolonged survival time [12]. This has since been attributed to the fraction of cases that have somatic IDH1 mutations. IDH1 wild-type tumors within the Proneural subtype did not show this survival advantage [13]. IDH1 mutations have consistently been associated with improved overall survival in patients with glioma [14], primarily because IDH1 mutations occur most frequently in grade II-III gliomas and secondary glioblastoma and are associated with younger age [15]. Examinations of response to radiation or chemotherapy in randomized trials of high-grade astrocytoma have not found a therapeutic interaction between adjuvant treatment and IDH1 genotype [16]. However, IDH1 mutation status has been associated with therapeutic benefit from maximal surgical resection [17].
Targeted therapy
Targeted therapy has shown successful results in other cancer groups including breast cancer, non-small cell lung carcinoma (NSCLC), bowel cancer and melanoma. In breast cancer, the discovery of trastuzumab as an adjuvant therapy revealed promising results in human epidermal growth factor 2 (HER2) positive patients. The addition of trastuzumab in the treatment program proved a substantial increase in the survival of HER2 positive breast cancer patients [18, 19]. NSCLC patients with EGFR mutations are known to respond better with EGFR tyrosine kinase inhibitors (TKIs) such as gefitinib and erlotinib. However, EGFR TKIs are avoided in NSCLC patients with KRAS mutations, which cause innate or acquired resistance to EGFR TKIs [20, 21]. Similarly, patients diagnosed with colorectal cancer with KRAS mutations are not given EGFR TKIs for the same reason. Other inhibitors are given instead to these patients to target different molecules such as sorafenib of which inhibit the RAF kinase family (ARAF, BRAF, CRAF) and are downstream molecules of RAS [22]. Mutations in the BRAF gene are used as markers for patients with metastatic malignant melanoma. BRAF positive metastatic malignant melanoma benefit from BRAF inhibitors such as vemurafenib [23].
There is significant progress in our understanding of the molecular biology of GBM, which has resulted in new advancements in targeted therapy. Two of the most prominently studied antigens are EGFR and its tumor specific genetic deletion variant III (EGFRvIII). EGFR is amplified and/or mutated in up to 60 % of GBM. Tumor growth and survival are promoted by EGFR through consistent activation of signaling networks and metabolic reprogramming [24]. As mentioned earlier, the injectable peptide vaccine, rindopepimut has shown significant efficacy in tumors positive for EGFRvIII. The seminal study by Sampson and colleagues showed significantly increased survival when compared with a patient history matched group of patients and that this survival gain was associated to increased titer of anti-EGFRvIII antibodies in the serum [25]. In addition, tissue collection of 9 of 11 patients undergoing second surgery showed loss of EGFRvIII expression after treatment, suggesting that the immune cells remove EGFRvIII positive cells [25]. The survival benefits of rindopepimut treatment have been confirmed in the ACT III phase II study, however this was not a randomized study [9]. The clinical benefit of rindopepimut will be clarified with the ongoing randomized phase III study, ACTIV.
A monoclonal antibody drug conjugate (ADC), ABT-414, has shown significant efficacy against tumors expressing amplified EGFR. The results of the Phase I trial were reported at the Society of Neuro-oncology (SNO) meeting in 2014. Four of 12 patients (33 %) achieved an objective response, including two who achieved complete responses. A randomized phase II trial of ABT-414 has been initiated.
Erlotinib has gained regulatory approval to treat EGFR mutant lung cancer, however the results for the treatment of EGFR mutant GBM have been disappointing. Several clinical trials have tested erlotinib in combination with radiotherapy and TMZ, with sirolimus and with bevacizumab [26–29]. However, all trials showed negative results. The specific location of the mutations is important. The majority of the mutations in EGFR in GBM occur in the extracellular domain (ED) in contrast to mutations in lung cancer, which occur in the kinase domain (KD) [30]. Inhibitors like erlotinib target the active kinase conformation. Second-generation EGFR inhibitors such as dacomitinib are beginning to show promise, however much of this data is limited to pre-clinical models.
There are many other target-therapeutic combinations in GBM that warrant further exploration. Approximately 2–3 % of all GBM harbour mutations or activating gene rearrangements in BRAF. It would be interesting to determine the response of these mutants to sorafenib. At the recent SNO meeting at San Antonio, 2015, the Adaptive Global Innovative Learning Environment (AGILE) trial was announced. Starting in 2016, this adaptive trial design will test patient tissue for biomarkers and assign treatment based on molecular biology.
Challenges in GBM
Targeting specific molecular aberrations seem to be the most logical and efficient approach for cancer treatment for GBM patients. However, challenges can be observed that may hinder a GBM patient’s way to recovery. The most significant challenges include: inter- and intra-tumor heterogeneity and the blood brain barrier (BBB). Both of these factors may possibly contribute to chemotherapy resistance in GBM patients and complicate treatment response and prognosis [31, 32]. Other factors that should be considered include tumor sampling times, limited therapeutic armamentarium, and low availability of pre-clinical models to be used for testing novel and repurposed drugs prior to giving these to the patient.
Blood brain barrier
Overcoming the blood brain barrier (BBB) has been a long-standing challenge in the treatment of GBM. The BBB is formed by a neurovascular unit comprising endothelial cells enforced by astrocytes and pericytes. This forms an extensive network of capillaries that prevent various substances from the blood stream from entering into the brain [33, 34]. The major factors affecting penetration have been discussed in several reviews and include the substance’s molecular weight, lipid solubility, and polarity [33–37]. Additionally, the presence of multiple transport proteins in the endothelial lining of the BBB’s vascular component is another major factor considered that inhibits the drug from reaching the target tumor tissue [33, 34, 38]. A few examples of drugs that were shown to have limited efficacy for GBM include pazopanib, paclitaxel and doxorubicin. Pazopanib, an oral VEGF inhibitor that has been observed to be effective in renal cell carcinoma, breast and lung cancer cannot be given to GBM patients due to this barrier and efflux mechanism [39, 40]. Similar to pazopanib, paclitaxel and doxorubicin are other chemotherapeutic drugs more commonly used in other cancer groups that has been investigated for efficacy in the treatment of GBM but had poor results due to the presence of multi drug resistant proteins such as the p-glycoprotein [41, 42].
Different drug delivery methods are being investigated to bypass the BBB. Osmotic BBB disruption (BBBD) makes use of chemicals such as mannitol or bradykinin to disrupt the integrity of the tight junctions in the BBB. Two retrospective studies demonstrated survival benefit in patients receiving chemotherapy with BBB modification by intracarotid and intravertebral artery infusion of mannitol [43, 44]. This disruption increases the spaces in between the tight junction thereby increasing drug permeability [33, 34, 45]. Unfortunately, this method has limited usefulness due to toxicity and complexity of the procedure. Another method that result in opening of the tight junctions between the endothelial cells is the transcranial delivery of low frequency ultrasound waves (focused ultrasound [FUS]). Pre-clinically, enhanced brain penetration of carmustine (BCNU) was observed in rat models using a combination of microbubbles (MBs) and focused ultrasound (FUS) [46]. There have been no reports of this method used in patients. Convection-enhanced delivery (CED) is a localized delivery strategy involving continuous positive-pressure infusion of a solute containing a therapeutic agent [47]. This method has been used for the delivery of therapeutic proteins, oligonucleotides, liposomes and viral mediated therapies [48]. CED has feasibility issues including technical expertise and the characteristics of the drug used. Catheter placement effects drug distribution and can also influence adverse effects such as chemical meningitis. Osmolarity, pH, ionic composition and drug solubility can also influence drug distribution by CED. In addition, the effect of CED on infiltrating glioma cells is questionable. The value of CED remains to be validated by a successful clinical trial.
A major mechanism by which the BBB limits drug delivery to the brain is the active efflux transport of molecules from the capillary endothelial cells. There are numerous active efflux transporters, including P-glycoprotein (P-gp), multidrug resistance proteins (e.g. MRP4) and breast cancer resistance protein (BCRP). Some methods take advantage of the presence of multi-drug efflux transporters at the BBB. Drugs, such as elacridar and tariquidar, have been developed to inhibit the function of multi-drug efflux transporters to increase drug influx through the BBB [33, 34]. In a very recent mouse study examining the efficacy of the CDK4/6 inhibitor, palbociclib, significantly higher levels of the drug were detected in the brain tumor when palbociclib was combined with elacridar [49].
Another approach plays on receptor-mediated transport mechanism where a ‘shuttling factor’ is coupled with the drug and goes through the BBB by targeting specific receptors such as insulin or transferrin [33, 50]. Alternatively, nanoparticles has likewise been used as drug vehicles to increase the chances of drug molecules, such as doxorubicin and paclitaxel, by-passing this barrier [51]. Circumvention of the BBB by directly administering the drug into the brain or tumor parenchyma through the use of intraventricular/intracavitary systems or polymer wafers has also been clinically investigated. An example of this approach is the use of carmustine (Gliadel) wafers. Gliadel wafers permit a slow release of carmustine (BCNU) after placement in the surgical cavity of high grade glioma. Despite significant survival benefits reported in Phase III studies, uptake to use gliadel wafers has been poor [52]. This may be due to the lack of phase III evidence that gliadel adds benefit to the current standard treatment; high infection rates, high cost of treatment and the fact that gliadel wafer placement frequently represents an exclusion criterion for recruitment of patients into further clinical trials.
Overcoming the physiological barriers with novel drug and diet options
Although numerous studies have been conducted to find treatment for GBM, only a handful of drugs have been FDA-approved. The development of new drugs could involve very lengthy processes and massive costs. On an average, a single drug takes 15 years and approximately US$800 million before a single drug is approved for marketing [53–55]. Repurposing drugs is being explored to compensate for the limited availability of drugs used for treatment of, not only, GBM but in other cancer groups as well [54]. Such in the case of the use of anti-fungal drugs as treatment for breast cancer and prostate cancer. Clotrimazole is being investigated in vitro for its effect on cell proliferation, viability and glycolysis in human-derived breast cancer cell lines [56]. Itraconazole, on the other hand, was recently investigated in a phase 2 clinical trial for castration-resistant prostate cancer (CRPC) [53]. Additionally, ibudilast, a drug that has been previously marketed for the treatment of asthma, is being investigated for its effects in combination with TMZ for the treatment of MGMT-unmethylated GBM [57]. Metformin is an oral anti-diabetic drug gaining much interest in the treatment of GBM. Metformin potentiates the pro-apoptotic effect of TMZ via the activation of 5′-adenosine monophosphate (AMPK). This enzyme plays a role in cellular energy homoeostasis, acting as a metabolic master switch and hence regulating several intracellular systems, including the inhibition of the mTOR pathway [58]. Hydroxychloroquine (HCQ), an autophagy inhibitor, has been shown to potentiate the effects of DNA damaging agents such as radiotherapy. Rosenfeld and colleagues tested the effect of HCQ in combination with RT and TMZ in a phase I trial design followed by a non-comparative phase II trial design [59]. No significant improvement in overall survival was observed.
Other non-conservative treatment options include the use of devices and diet. Recent Phase III data presented by Stupp and colleagues at the ASCO meeting in June 2015 have shown a significant survival benefit for the use of the Novo-TTF-100A (Optune™) device. The Optune device generates tumor treating fields directly to the patient’s scalp and acts as an anti-mitotic therapy for GBM. The device gained FDA approval for its use however it is unavailable in many countries, including Australia and the cost of treatment is extremely high. Dietary options such as a restrictive ketogenic diet (KD) to result in glucose deprivation have been explored. A recent study developed a supplemented high-fat low-carbohydrate (sHFLC) diet and showed that this diet was able to reduce glucose in vitro and inhibited proliferation and tumor stem cell expansion [60]. Survival was extended in an orthotopic xenograft model.
Tumor heterogeneity
A critical problem with large cohort studies such as TCGA, is that single-tumor sampling leads to significant sampling biases. Fluorescence in situ hybridizaton (FISH) analyses of sections of GBM revealed cells with mutations to EGFR and PDGFR co-existing within the same GBM [61]. Therefore, a single agent targeting the EGFR mutation may show limited efficacy in these tumor types because it fails to target the PDGFR gene aberration [62]. The discovery of cells with different driver mutations side by side within a single tumor suggests that targeting a single mutation may be an ineffective strategy in GBMs. In a study by Watts and colleagues, 38 fragments from 9 patients with GBM were sampled and genome-wide somatic copy number levels were measured [63]. Although the fragments from the same patient shared a common gene profile, indicating the clonal origin of the tumor, they displayed a striking variety of copy number alterations that were present in only a subset of fragments, indicating clonal evolution [63]. In addition using gene expression arrays, they found that in 6 out of 10 cases the fragments from the same tumor mass were classified into at least 2 different GBM subgroups (mesenchymal, neural, classical or proneural) [63]. This indicates that tumor clones with different phenotypic profiles coexist within the same malignancy. Yachida et al. demonstrated heterogeneity in pancreatic cancer using whole exome sequencing and copy number analysis of samples obtained from different anatomical regions of a pancreatic cancer [64]. This study showed that clonal tumor populations present in the primary tumor give rise to metastatic disease in a branched evolutionary pattern, with progressor mutations common to metastatic sites and within regionally separated subclones of the primary lesion [64].
Sampling times
Targeted therapy is typically utilized as a salvage therapy for glioblastoma patients when they relapse. Not all patients are suitable candidates for a second round of surgery. When it comes to biomarker analysis, the only tissue available for testing is typically the specimen used for the primary diagnosis. The genomic road leading to recurrence in GBM is not well understood. Most likely, after therapy, the surviving population may not be a single resistant cancer clone, but rather a heterogeneous population of malignant cells with genetic aberrations that allow them to survive the initial treatment. Shah et al., described the genome of a metastatic obular breast cancer with 19 non-synonymous mutations present in the metastatic lesion that were not present in the primary cancer diagnosed 9 years previously, illustrating the temporal dynamics of intra-tumor heterogeneity [65]. Clonal evolution, driven by genomic instability, underlies the development of metastatic pancreatic cancer [66]. A recent study by Verhaak examined the genomic events in pre- and post-treatment GBM pairs [67]. Through longitudinal comparisons of tumor samples before and after treatment, TP53-mutated tumors showed a further increase in clonal complexity at the time of relapse, whereas TP53 wildtype recurrences appeared to have gone through a bottleneck, which resulted in relatively monoclonal recurrent tumors [67]. TP53 mutations have been associated with an increased frequency of double-strand breaks and chromothripsis in medulloblastoma [68]. The apoptosis negating properties of TP53 DNA binding domain mutations may result in an increased tolerance for acquiring and sustaining single nucleotide polymorphisms (SNPs) [67].
A potential strategy to overcome this issue of tumor sampling would be to re-biopsy the tumor at the time of progression and perform the molecular profiling on the recurrent sample. This approach may not be feasible for all patients, particularly when the tumor is located in eloquent areas of the brain. Measuring circulating tumor cell DNA (ctDNA) may be another viable and minimally invasive clinical option for GBM patients allowing clinicians to identify potentially druggable molecular alterations driving recurrence. These “liquid biopsies” can be collected from several sources including blood, urine and the CSF. As a result of cell death or active secretion, tumor cells can release small pieces of their DNA and/or RNA into the bloodstream or CSF and are relatively stable. Multiple molecular alterations including loss of heterozygosity of 1p and 19q, IDH1 and EGFRvIII as well as the methylation status of promoters of MGMT, PTEN and CDKN2A have been detected [69–71].
Pre-clinical models
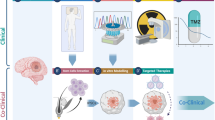
Solid and robust pre-clinical data is required to advance clinical trials for GBM patients. In this era of ‘omics’, there is a unique opportunity to use genomic profiling to identify biomarkers to treatments. Dynamic biobanking is becoming more frequent at large Neurosurgical centres. That is, at the time of patient surgery, the tumor is collected. Rather than just storing the piece of tissue in paraffin or cryopreservation, cells are dissociated from the tumor and grown in culture and/or immediately surgically implanted into the brains of immune-compromised mice. We appreciate now that more traditional, serum-based cell lines do not allow for recapitulation of patient tumor physiology and many of these cell lines cannot form tumor in vivo [72]. Cells grown as neurospheres or monolayers on a laminin-coated surface in a serum free environment with growth factors closely mirror the genotype and gene expression patterns of patient tumors [73, 74]. These “patient-derived cell lines (PDCLs)” are becoming more common in laboratory practices and are now being used in high-throughput drug screens [75]. Another area of significant development is the in vivo models used to test drug efficacy. In the past, subcutaneous models of GBM were commonly used and tumor growth could be measured with calipers. This model does not address whether the agent can reach the tumor target, and cross the blood brain barrier. Frequently, orthotopic GBM mouse models in NOD-SCID gamma mice are being used to determine drug efficacy. Recent advances in the use of animal models for cancer research has been reported in a review written by Malaney and colleagues. The concept of “mouse avatars” and co-clinical trials is a valuable attempt to test novel or repurposed drugs on xenograft models that has the characteristics of a patient’s tumor biology. This approach could revolutionize drug development and individualized therapy [76]. There are important caveats to this approach that still need to be addressed. Firstly, the mice do not have an immune system. Inflammatory cells may be a critical component to the biology of the tumor and its response to certain drugs, particularly immunotherapy. Secondly, the surrounding stroma and microenvironment is of mouse origin, not human and may interfere with drug response. Thirdly, metabolism of the drug may be different in mice and again may skew drug response.
Conclusion
GBM is one of the most problematic cancers to treat. Despite being the most common malignant primary brain tumor and the advances in molecular profiling of the disease, information is still lacking especially in the area of treatment. A one-drug fits all strategy poorly applies to GBM. Various clinical and pre-clinical trials are being conducted to investigate the effects of novel and repurposed drugs, as well as novel drug combinations. Access to a patient’s genomic data through whole genome sequencing must be used to our advantage to personalize a patient’s treatment. The need for pre-clinical models to validate the efficacy of these novel/repurposed drugs and drug combinations is critical. The use of patient-derived cell lines to produce orthotopic xenograft models is highly advisable. This approach could possibly give the most accurate prediction of how a drug will affect a patient’s tumor and hopefully bridge the gap observed in the availability of treatments for those patients unresponsive to the current standard therapy. Additionally, a comprehensive drug-gene database would be useful to give basic researchers and clinicians a guide as to which drug-gene interaction would be highly beneficial to the patient. Personalizing treatment is a multidisciplinary approach where basic researchers, biostatisticians and clinicians play a big role in giving the right therapy to a patient.
References
Gilbert MR (2011) Recurrent glioblastoma: a fresh look at current therapies and emerging novel approaches. Semin Oncol 38(Suppl 4):S21–S33. doi:10.1053/j.seminoncol.2011.09.008
Biankin AV, Chanock SJ (2011) The road ahead: less travelled and more arduous than initially envisioned. Hum Genet 130(1):1–2. doi:10.1007/s00439-011-1046-1
Harris T (2010) Gene and drug matrix for personalized cancer therapy. Nat Rev Drug Discov 9(8):660. doi:10.1038/nrd3181-c1
Schilsky RL (2010) Personalized medicine in oncology: the future is now. Nat Rev Drug Discov 9(5):363–366. doi:10.1038/nrd3181
Nathanson KL (2010) Using genetics and genomics strategies to personalize therapy for cancer: focus on melanoma. Biochem Pharmacol 80(5):755–761. doi:10.1016/j.bcp.2010.04.017
Stupp R, Mason WP, van den Bent MJ, Weller M, Fisher B, Taphoorn MJ et al (2005) Radiotherapy plus concomitant and adjuvant temozolomide for glioblastoma. New Engl J Med 352(10):987–996. doi:10.1056/NEJMoa043330
Jue TR, Hovey E, Davis S, Carleton O, McDonald KL (2014) Incorporation of biomarkers in phase II studies of recurrent glioblastoma. Tumor Biol. doi:10.1007/s13277-014-2960-3
Hegi ME, Diserens A-C, Gorlia T, Hamou M-F, de Tribolet N, Weller M et al (2005) MGMT gene silencing and benefit from temozolomide in glioblastoma. N Engl J Med 352(10):997–1003. doi:10.1056/NEJMoa043331
Schuster J, Lai RK, Recht LD, Reardon DA, Paleologos NA, Groves MD et al (2015) A phase II, multicenter trial of rindopepimut (CDX-110) in newly diagnosed glioblastoma: the ACT III study. Neuro Oncology 17(6):854–861. doi:10.1093/neuonc/nou348
McLendon R, Friedman A, Bigner D, Van Meir EG, Brat DJ, Mastrogianakis GM, Olson JJ, Mikkelsen T, Lehman N, Aldape K, Yung WA (2008) Comprehensive genomic characterization defines human glioblastoma genes and core pathways. Nature 455(7216):1061–1068. doi:10.1038/nature07385
Brennan CW, Verhaak RG, McKenna A, Campos B, Noushmehr H, Salama SR et al (2013) The somatic genomic landscape of glioblastoma. Cell 155(2):462–477. doi:10.1016/j.cell.2013.09.034
Verhaak RG, Hoadley KA, Purdom E, Wang V, Qi Y, Wilkerson MD et al (2010) Integrated genomic analysis identifies clinically relevant subtypes of glioblastoma characterized by abnormalities in PDGFRA, IDH1, EGFR, and NF1. Cancer Cell 17(1):98–110. doi:10.1016/j.ccr.2009.12.020
Noushmehr H, Weisenberger DJ, Diefes K, Phillips HS, Pujara K, Berman BP et al (2010) Identification of a CpG island methylator phenotype that defines a distinct subgroup of glioma. Cancer Cell 17(5):510–522. doi:10.1016/j.ccr.2010.03.017
Cheng HB, Yue W, Xie C, Zhang RY, Hu SS, Wang Z (2013) IDH1 mutation is associated with improved overall survival in patients with glioblastoma: a meta-analysis. Tumor Biol 34(6):3555–3559. doi:10.1007/s13277-013-0934-5
Kloosterhof NK, Bralten LB, Dubbink HJ, French PJ, van den Bent MJ (2011) Isocitrate dehydrogenase-1 mutations: a fundamentally new understanding of diffuse glioma? Lancet Oncol 12(1):83–91. doi:10.1016/S1470-2045(10)70053-X
Weller M, Felsberg J, Hartmann C, Berger H, Steinbach JP, Schramm J et al (2009) Molecular predictors of progression-free and overall survival in patients with newly diagnosed glioblastoma: a prospective translational study of the German glioma network. J Clin Oncol 27(34):5743–5750. doi:10.1200/jco.2009.23.0805
Beiko J, Suki D, Hess KR, Fox BD, Cheung V, Cabral M et al (2014) IDH1 mutant malignant astrocytomas are more amenable to surgical resection and have a survival benefit associated with maximal surgical resection. Neuro Oncology 16(1):81–91. doi:10.1093/neuonc/not159
Alvarez RH, Valero V, Hortobagyi GN (2010) Emerging targeted therapies for breast cancer. J Clin Oncol 28(20):3366–3379. doi:10.1200/jco.2009.25.4011
Perez EA, Romond EH, Suman VJ, Jeong JH, Sledge G, Geyer CE Jr et al (2014) Trastuzumab plus adjuvant chemotherapy for human epidermal growth factor receptor 2-positive breast cancer: planned joint analysis of overall survival from NSABP B-31 and NCCTG N9831. J Clin Oncol 32(33):3744–3752. doi:10.1200/jco.2014.55.5730
Sun Z, Wang Z, Liu X, Wang D (2015) New development of inhibitors targeting the PI3K/AKT/mTOR pathway in personalized treatment of non-small-cell lung cancer. Anticancer Drugs 26(1):1–14. doi:10.1097/cad.0000000000000172
Janne PA, Engelman JA, Johnson BE (2005) Epidermal growth factor receptor mutations in non-small-cell lung cancer: implications for treatment and tumor biology. J Clin Oncol 23(14):3227–3234. doi:10.1200/jco.2005.09.985
Prenen H, Tejpar S, Van Cutsem E (2010) New strategies for treatment of KRAS mutant metastatic colorectal cancer. Clin Cancer Res 16(11):2921–2926. doi:10.1158/1078-0432.ccr-09-2029
Beale S, Dickson R, Bagust A, Blundell M, Dundar Y, Boland A et al (2013) Vemurafenib for the treatment of locally advanced or metastatic BRAF V600 mutation-positive malignant melanoma: a NICE single technology appraisal. Pharmacoeconomics 31(12):1121–1129. doi:10.1007/s40273-013-0094-x
Liu F, Hon GC, Villa GR, Turner KM, Ikegami S, Yang H et al (2015) EGFR mutation promotes glioblastoma through epigenome and transcription factor network remodeling. Mol Cell 60(2):307–318. doi:10.1016/j.molcel.2015.09.002
Sampson JH, Heimberger AB, Archer GE, Aldape KD, Friedman AH, Friedman HS et al (2010) Immunologic escape after prolonged progression-free survival with epidermal growth factor receptor variant III peptide vaccination in patients with newly diagnosed glioblastoma. J Clin Oncol 28(31):4722–4729. doi:10.1200/jco.2010.28.6963
Peereboom DM, Shepard DR, Ahluwalia MS, Brewer CJ, Agarwal N, Stevens GH et al (2010) Phase II trial of erlotinib with temozolomide and radiation in patients with newly diagnosed glioblastoma multiforme. J Neurooncol 98(1):93–99. doi:10.1007/s11060-009-0067-2
Raizer JJ, Giglio P, Hu J, Groves M, Merrell R, Conrad C et al (2015) A phase II study of bevacizumab and erlotinib after radiation and temozolomide in MGMT unmethylated GBM patients. J Neurooncol. doi:10.1007/s11060-015-1958-z
van den Bent MJ, Brandes AA, Rampling R, Kouwenhoven MC, Kros JM, Carpentier AF et al (2009) Randomized phase II trial of erlotinib versus temozolomide or carmustine in recurrent glioblastoma: EORTC brain tumor group study 26034. J Clin Oncol 27(8):1268–1274. doi:10.1200/jco.2008.17.5984
Reardon DA, Desjardins A, Vredenburgh JJ, Gururangan S, Friedman AH, Herndon JE 2nd et al (2010) Phase 2 trial of erlotinib plus sirolimus in adults with recurrent glioblastoma. J Neurooncol 96(2):219–230. doi:10.1007/s11060-009-9950-0
Vivanco I, Robins HI, Rohle D, Campos C, Grommes C, Nghiemphu PL et al (2012) Differential sensitivity of glioma- versus lung cancer-specific EGFR mutations to EGFR kinase inhibitors. Cancer Discov 2(5):458–471. doi:10.1158/2159-8290.cd-11-0284
Ashby LS, Ryken TC (2006) Management of malignant glioma: steady progress with multimodal approaches. Neurosurg Focus 20(4):E3. doi:10.3171/foc.2006.20.4.3
Patel AP, Tirosh I, Trombetta JJ, Shalek AK, Gillespie SM, Wakimoto H et al (2014) Single-cell RNA-seq highlights intratumoral heterogeneity in primary glioblastoma. Science 344(6190):1396–1401. doi:10.1126/science.1254257
van Tellingen O, Yetkin-Arik B, de Gooijer M, Wesseling P, Wurdinger T, de Vries H (2015) Overcoming the blood–brain tumor barrier for effective glioblastoma treatment. Drug Resist Updates 19:1–12
Hendricks BK, Cohen-Gadol AA, Miller JC (2015) Novel delivery methods bypassing the blood-brain and blood-tumor barriers. Neurosurg Focus 38(3):E10. doi:10.3171/2015.1.FOCUS14767
Pitz MW, Desai A, Grossman SA, Blakeley JO (2011) Tissue concentration of systemically administered antineoplastic agents in human brain tumors. J Neurooncol 104(3):629–638. doi:10.1007/s11060-011-0564-y
Weidle UH, Niewohner J, Tiefenthaler G (2015) The blood-brain barrier challenge for the treatment of brain cancer, secondary brain metastases, and neurological diseases. Cancer Genom Proteom 12(4):167–177
Pardridge WM (2005) The blood-brain barrier: bottleneck in brain drug development. NeuroRx. 2(1):3–14. doi:10.1602/neurorx.2.1.3
Miller DS, Bauer B, Hartz AM (2008) Modulation of P-glycoprotein at the blood-brain barrier: opportunities to improve central nervous system pharmacotherapy. Pharmacol Rev 60(2):196–209. doi:10.1124/pr.107.07109
Mao H, Lebrun DG, Yang J, Zhu VF, Li M (2012) Deregulated signaling pathways in glioblastoma multiforme: molecular mechanisms and therapeutic targets. Cancer Invest 30(1):48–56. doi:10.3109/07357907.2011.630050
Sloan B, Scheinfeld NS (2008) Pazopanib, a VEGF receptor tyrosine kinase inhibitor for cancer therapy. Curr Opin Investig Drugs 9(12):1324–1335 (London, England: 2000)
Fellner S, Bauer B, Miller DS, Schaffrik M, Fankhanel M, Spruss T et al (2002) Transport of paclitaxel (Taxol) across the blood-brain barrier in vitro and in vivo. J Clin Investig 110(9):1309–1318. doi:10.1172/jci15451
Sardi I, Fantappie O, la Marca G, Giovannini MG, Iorio AL, da Ros M et al (2014) Delivery of doxorubicin across the blood brain barrier by ondansetron pretreatment: a study in vitro and in vivo. Cancer Lett. doi:10.1016/j.canlet.2014.07.018
Kraemer DF, Fortin D, Neuwelt EA (2002) Chemotherapeutic dose intensification for treatment of malignant brain tumors: recent developments and future directions. Curr Neurol Neurosci Rep 2(3):216–224
Neuwelt EA, Howieson J, Frenkel EP, Specht HD, Weigel R, Buchan CG et al (1986) Therapeutic efficacy of multiagent chemotherapy with drug delivery enhancement by blood-brain barrier modification in glioblastoma. Neurosurgery 19(4):573–582
Liu LB, Xue YX, Liu YH, Wang YB (2008) Bradykinin increases blood-tumor barrier permeability by down-regulating the expression levels of ZO-1, occludin, and claudin-5 and rearranging actin cytoskeleton. J Neurosci Res 86(5):1153–1168. doi:10.1002/jnr.21558
Ting CY, Fan CH, Liu HL, Huang CY, Hsieh HY, Yen TC et al (2012) Concurrent blood-brain barrier opening and local drug delivery using drug-carrying microbubbles and focused ultrasound for brain glioma treatment. Biomaterials 33(2):704–712. doi:10.1016/j.biomaterials.2011.09.096
Vogelbaum MA, Aghi MK (2015) Convection-enhanced delivery for the treatment of glioblastoma. Neuro Oncology 17(Suppl 2):ii3–ii8. doi:10.1093/neuonc/nou354
Oberoi RK, Parrish KE, Sio TT, Mittapalli RK, Elmquist WF, Sarkaria JN (2015) Strategies to improve delivery of anticancer drugs across the blood-brain barrier to treat glioblastoma. Neuro Oncology. doi:10.1093/neuonc/nov164
Parrish KE, Pokorny J, Mittapalli RK, Bakken K, Sarkaria JN, Elmquist WF (2015) Efflux transporters at the blood-brain barrier limit delivery and efficacy of cyclin-dependent kinase 4/6 inhibitor palbociclib (PD-0332991) in an orthotopic brain tumor model. J Pharmacol Exp Ther 355(2):264–271. doi:10.1124/jpet.115.228213
Pardridge WM (2012) Drug transport across the blood-brain barrier. J Cereb Blood Flow Metab 32(11):1959–1972. doi:10.1038/jcbfm.2012.126
Peluffo H, Unzueta U, Negro-Demontel ML, Xu Z, Vaquez E, Ferrer-Miralles N et al (2015) BBB-targeting, protein-based nanomedicines for drug and nucleic acid delivery to the CNS. Biotechnol Adv 33(2):277–287. doi:10.1016/j.biotechadv.2015.02.004
Westphal M, Hilt DC, Bortey E, Delavault P, Olivares R, Warnke PC et al (2003) A phase 3 trial of local chemotherapy with biodegradable carmustine (BCNU) wafers (Gliadel wafers) in patients with primary malignant glioma. Neuro Oncology 5(2):79–88. doi:10.1215/s1522-8517-02-00023-6
Antonarakis ES, Heath EI, Smith DC, Rathkopf D, Blackford AL, Danila DC et al (2013) Repurposing itraconazole as a treatment for advanced prostate cancer: a noncomparative randomized phase II trial in men with metastatic castration-resistant prostate cancer. Oncologist 18(2):163–173. doi:10.1634/theoncologist.2012-314
Chong CR, Sullivan DJ Jr (2007) New uses for old drugs. Nature 448(7154):645–646. doi:10.1038/448645a
DiMasi JA, Hansen RW, Grabowski HG (2003) The price of innovation: new estimates of drug development costs. J Health Econ 22(2):151–185. doi:10.1016/S0167-6296(02)00126-1
Furtado CM, Marcondes MC, Sola-Penna M, de Souza ML, Zancan P (2012) Clotrimazole preferentially inhibits human breast cancer cell proliferation, viability and glycolysis. PLoS One 7(2):e30462. doi:10.1371/journal.pone.0030462
McDonald KL, Ha W, Sevim H (2014) MIF-CD74 guided therapeutic strategy for the upfront treatment of GBM patients with an unmethylated MGMT promoter. Neuro-Oncology 16(suppl 3):iii4–iii5. doi:10.1093/neuonc/nou206.15
Wurth R, Barbieri F, Florio T (2014) New molecules and old drugs as emerging approaches to selectively target human glioblastoma cancer stem cells. BioMed Res Int 2014:126586. doi:10.1155/2014/126586
Rosenfeld MR, Ye X, Supko JG, Desideri S, Grossman SA, Brem S et al (2014) A phase I/II trial of hydroxychloroquine in conjunction with radiation therapy and concurrent and adjuvant temozolomide in patients with newly diagnosed glioblastoma multiforme. Autophagy 10(8):1359–1368. doi:10.4161/auto.28984
Martuscello RT, Vedam-Mai V, McCarthy DJ, Schmoll ME, Jundi MA, Louviere CD et al (2015) A supplemented high-fat low-carbohydrate diet for the treatment of glioblastoma. Clin Cancer Res. doi:10.1158/1078-0432.ccr-15-0916
Snuderl M, Fazlollahi L, Le LP, Nitta M, Zhelyazkova BH, Davidson CJ et al (2011) Mosaic amplification of multiple receptor tyrosine kinase genes in glioblastoma. Cancer Cell 20(6):810–817. doi:10.1016/j.ccr.2011.11.005
Szerlip NJ, Pedraza A, Chakravarty D, Azim M, McGuire J, Fang Y et al (2012) Intratumoral heterogeneity of receptor tyrosine kinases EGFR and PDGFRA amplification in glioblastoma defines subpopulations with distinct growth factor response. Proc Natl Acad Sci USA 109(8):3041–3046. doi:10.1073/pnas.1114033109
Sottoriva A, Spiteri I, Piccirillo SG, Touloumis A, Collins VP, Marioni JC et al (2013) Intratumor heterogeneity in human glioblastoma reflects cancer evolutionary dynamics. Proc Natl Acad Sci USA 110(10):4009–4014. doi:10.1073/pnas.1219747110
Yachida S, Jones S, Bozic I, Antal T, Leary R, Fu B et al (2010) Distant metastasis occurs late during the genetic evolution of pancreatic cancer. Nature 467(7319):1114–1117. doi:10.1038/nature09515
Shah SP, Morin RD, Khattra J, Prentice L, Pugh T, Burleigh A et al (2009) Mutational evolution in a lobular breast tumor profiled at single nucleotide resolution. Nature 461(7265):809–813. doi:10.1038/nature08489
Campbell PJ, Yachida S, Mudie LJ, Stephens PJ, Pleasance ED, Stebbings LA et al (2010) The patterns and dynamics of genomic instability in metastatic pancreatic cancer. Nature 467(7319):1109–1113. doi:10.1038/nature09460
Kim H, Zheng S, Amini SS, Virk SM, Mikkelsen T, Brat DJ et al (2015) Whole-genome and multisector exome sequencing of primary and post-treatment glioblastoma reveals patterns of tumor evolution. Genome Res 25(3):316–327. doi:10.1101/gr.180612.114
Rausch T, Jones DT, Zapatka M, Stutz AM, Zichner T, Weischenfeldt J et al (2012) Genome sequencing of pediatric medulloblastoma links catastrophic DNA rearrangements with TP53 mutations. Cell 148(1–2):59–71. doi:10.1016/j.cell.2011.12.013
Boisselier B, Gallego Perez-Larraya J, Rossetto M, Labussiere M, Ciccarino P, Marie Y et al (2012) Detection of IDH1 mutation in the plasma of patients with glioma. Neurology 79(16):1693–1698. doi:10.1212/WNL.0b013e31826e9b0a
Majchrzak-Celinska A, Paluszczak J, Kleszcz R, Magiera M, Barciszewska AM, Nowak S et al (2013) Detection of MGMT, RASSF1A, p15INK4B, and p14ARF promoter methylation in circulating tumor-derived DNA of central nervous system cancer patients. J Appl Genet 54(3):335–344. doi:10.1007/s13353-013-0149-x
Salkeni MA, Zarzour A, Ansay TY, McPherson CM, Warnick RE, Rixe O et al (2013) Detection of EGFRvIII mutant DNA in the peripheral blood of brain tumor patients. J Neurooncol 115(1):27–35. doi:10.1007/s11060-013-1209-0
Li A, Walling J, Kotliarov Y, Center A, Steed ME, Ahn SJ et al (2008) Genomic changes and gene expression profiles reveal that established glioma cell lines are poorly representative of primary human gliomas. Mol Cancer Res 6(1):21–30. doi:10.1158/1541-7786.mcr-07-0280
Lee J, Kotliarova S, Kotliarov Y, Li A, Su Q, Donin NM et al (2006) Tumor stem cells derived from glioblastomas cultured in bFGF and EGF more closely mirror the phenotype and genotype of primary tumors than do serum-cultured cell lines. Cancer Cell 9(5):391–403. doi:10.1016/j.ccr.2006.03.030
Pollard SM, Yoshikawa K, Clarke ID, Danovi D, Stricker S, Russell R et al (2009) Glioma stem cell lines expanded in adherent culture have tumor-specific phenotypes and are suitable for chemical and genetic screens. Cell Stem Cell 4(6):568–580. doi:10.1016/j.stem.2009.03.014
Quartararo CE, Reznik E, deCarvalho AC, Mikkelsen T, Stockwell BR (2015) High-throughput screening of patient-derived cultures reveals potential for precision medicine in glioblastoma. ACS Med Chem Lett 6(8):948–952. doi:10.1021/acsmedchemlett.5b00128
Malaney P, Nicosia SV, Dave V (2014) One mouse, one patient paradigm: new avatars of personalized cancer therapy. Cancer Lett 344(1):1–12. doi:10.1016/j.canlet.2013.10.010
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Jue, T.R., McDonald, K.L. The challenges associated with molecular targeted therapies for glioblastoma. J Neurooncol 127, 427–434 (2016). https://doi.org/10.1007/s11060-016-2080-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-016-2080-6