Abstract
Background
Regulatory T cells (Tregs) have an important role in the control of the immune responses. This study aimed to compare the frequency of peripheral blood (PB) CD4+ CD25+ FoxP3+ Treg cells and PB and duodenal expression levels of pro- and anti-inflammatory mediators in treated celiac disease (CD) patients and healthy controls.
Methods and results
Duodenal biopsy specimens and PB samples were collected from 60 treated CD patients and 60 controls. Flow cytometry analysis was conducted on peripheral blood mononuclear cell (PBMC) specimens and relative PB and duodenal mRNA expression levels of CD25, forkhead box P3 (Foxp3), interleukin (IL)-10 and granzyme B (GrzB) were evaluated using quantitative real-time PCR. The levels of serum IL-10 and IL-6 were tested with sandwich enzyme-linked immunosorbent assay kits. p values < 0.05 were considered significant. Flow cytometry analysis showed a significant decrease in the number of Tregs in CD patients’ PBMC specimens (p = 0.012). CD25 and Foxp3 PB mRNA expressions were also lower in CD patients without reaching the significance level (p > 0.05). IL-10 PB mRNA and protein expression did not differ between the groups (p > 0.05), and GrzB PB expression was significantly reduced in CD patients (p = 0.001). In duodenal specimens of CD patients, while significantly increased CD25, Foxp3 mRNA expression (p = 0.01 and 0.001, respectively) and decreased IL-10 mRNA expression (p = 0.02) were observed, GrzB mRNA expression did not differ between groups (p > 0.05). Moreover, a high serum level of IL-6 was observed in CD patients (p = 0.001).
Conclusions
Despite following the gluten free diet, there may still be residual inflammation in the intestine of CD patients. Accordingly, finding a therapeutic approach based on strengthening the function of Treg cells in CD might be helpful.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Celiac disease (CD), is a worldwide chronic small intestinal immune-mediated enteropathy triggered by exposure to dietary gluten as a result of the interplay between genetic, immunologic, and environmental factors [1,2,3,4]. Population‐based studies estimated that CD affects about 1% of the general population, although the majority of patients have not been diagnosed [5, 6]. Its prevalence has been reported to be increased over the last few decades, which can be due to the wide consumption of high gluten content cereals, and also increased knowledge about this disease [7, 8]. This enteropathy is considered a multi-system disorder, which is characterized by a combination of gastrointestinal and non-gastrointestinal symptoms and associated conditions [1].
It has been reported that both innate and adaptive immune responses are involved in CD pathogenesis [9, 10]. Actually, celiac disease occurs as a result of the change in the regulation of the mucosal immune responses to dietary gluten and breaks in patients’ intestinal homeostasis and tolerance toward harmless intestinal antigens such as gliadin [11, 12]. Tolerance toward innocuous antigens is induced by a number of different mechanisms including regulatory T cells (Tregs) activation, which has been shown to effectively suppress animal models of autoimmune diseases [13,14,15,16]. In mice, the loss of intestinal and peripheral tolerance to the food antigen has been reported as a result of the depletion of Treg cells [17]. A combination of different markers including CD4, forkhead box P3 (Foxp3), CD25, CD39, CD127, OX40 etc. are used to identify Treg cells [14, 16, 18, 19]. Moreover, CD4 (+) FoxP3 (+) CD25 (+) T cells are known as the major natural Treg cells population [14, 16, 18].
The transcription factor forkhead box P3 has been identified as an important regulator for the development, differentiation and function of Tregs [20,21,22]. However, according to Wang et al. study, Foxp3 can also be transiently upregulated in human activated CD4+T cells that did not acquire suppressive capacity and were hyporesponsive to TCR stimulation [23]. According to the previous reports, the expression of Foxp3 is required for maintaining homeostasis of T-cell-mediated immune responses and mutations in its gene are associated with a defective function of Tregs causing the fatal autoimmune disorder, named immune dysregulation polyendocrinopathy enteropathy X-linked syndrome (IPEX) syndrome [18, 21, 24, 25].
The alpha chain of the interleukin (IL)-2 receptor (IL-2 Rα/CD25) also plays a crucial role in Treg cells’ development and maintains their immunoregulatory functions [26, 27]. IL-2 by binding to the interleukin-2 receptor (IL-2R) and through signal transducer and activator of transcription 5 (STAT5) pathway upregulates Foxp3 expression and causes Treg cells differentiation in thymic precursors [28, 29]. Natural Tregs due to their chromatin inaccessibility of the IL-2 locus are dependent on other sources of IL-2 for survival and response to the T-cell growth factor IL-2 by expressing CD25 [20, 30, 31]. Moreover, Tregs’ high-level expression of CD25 is known as one of their suppressive mechanisms that leads to IL-2 deprivation-mediated metabolic disruption and apoptosis of effector T cells [32].
Treg cells also use other suppressive mechanisms including the secretion of inhibitory cytokines like IL-10 and the production of cytolytic factors such as granzyme B (GrzB) for modulating the inflammatory responses and controlling various types of immune responses [20, 33].
Currently, lifelong complete adherence to a gluten-free diet (GFD) has remained the mainstay of CD treatment that results in the normalization of the histological lesions and antibody levels [34]. However, strict GFD is difficult to maintain and re-exposure to gliadin results in the recurrence of acute disease and gliadin specific CD4+T cells activation [35,36,37,38]. In fact, the results of recent studies indicate the less effectiveness of GFD in treating CD and show that apparently well-controlled GFD-treated CD patients continue to have an intestinal injury and present gluten-induced acute symptoms [39]. Hence, finding a new treatment pathway for this disorder becomes an urgent need. Accordingly, emerging research has focused on evaluating the number and function of CD patients’ Treg cells. Since most celiac patients are on a gluten-free diet, we decided to evaluate the percentage of Tregs in peripheral blood (there are the same CD4+T cell clones in PB and intestine with the same phenotype that target gluten peptides [39]) from GFD-treated CD patients and evaluate the expression levels of pro- and anti-inflammatory mediators in patient’s peripheral blood as well as duodenal specimens.
Material and methods
Study subjects
Sixty CD patients under GFD treatment for at least 6 months [mean age 40 ± 12.24 years, male 25 (41.6%), female 35 (58.3%)] whose diagnosis was set based on clinical presentations and histological findings compatible with serological results (tTG IgA) were recruited from the outpatient clinic of Gastroenterology Department at the Taleghani Hospital (Tehran, Iran) during 2018–2020. Medical history from all subjects was revised by the gastroenterologist in charge of patient enrolment. The mean disease duration was 3.75 ± 3.2 years and patients were on a GFD for an average of 2.5 ± 0.9 years. Sixty gender and age- matched non-celiac subjects [mean age 38 ± 13.2 years, male 27 (45%), female 33 (55%)] with no family history of CD or other autoimmune diseases and food intolerance attending the endoscopy unit because of other gastrointestinal (GI) disorders, who had normal small intestinal biopsy specimens also considered as a control group. There was no significant difference between age (p = 0.715) and gender (p = 0.18) among CD patients and controls. Pregnant and lactating women, patients with any other autoimmune/gastrointestinal diseases, and who had a history of anti-inflammatory and prohibited drug intake were excluded from the study. The study was approved by the ethical committee of the Research Institute for Gastroenterology and Liver Diseases (RIGLD), Shahid Beheshti University of Medical Sciences, Tehran, Iran (IR.SBMU.MSP.REC.1397.564) and written informed consent was obtained from both patients and controls before enrollment.
Sampling
Distal duodenal biopsy specimens, as well as peripheral blood samples, were collected from patients and controls. All biopsy specimens were obtained using the single pass biopsy method that was performed for diagnostic or follow-up purposes and none were made only for the purpose of this study. Biopsy specimens were immediately submerged in cold RNA later solution and stored at 4 °C overnight and thereafter at − 20 °C until RNA purification.
Flow cytometry analysis
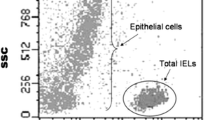
Peripheral blood mononuclear cells (PBMCs) of patients and controls were separated using Ficoll-Paque (GE Healthcare™) density gradient centrifugation. A regulatory T cell staining kit (eBioscience, San Diego, USA) was used according to the manufacturer’s instruction. Staining of surface molecules was performed using anti-CD4-FITC and anti-CD25-APC antibodies with a standard procedure and incubated at 4 °C for 15 min. Washing with flow cytometry staining buffer was carried out, and upon permeabilization, the cells were stained with anti-Foxp3-PE antibody and incubated at 4 °C for 30 min. All monoclonal antibodies (mAbs) were used at manufacturers’ recommended dilutions. At the end, the cells were washed, resuspended with flow cytometry staining buffer, and the frequency of CD4+ CD25+ Foxp3+ regulatory T cells was analyzed using BD flow cytometry (©FACSCalibur, BD Company, San Diego, CA, USA) and flowjo software (©FlowJo, LLC, Ashland, OR, USA). Indeed, CD4+ cells were gated (cells expressing CD4 at levels above those of the unstained cells) and assessed for surface expression of CD25 and Foxp3.
Quantitative real-time PCR (RT-qPCR)
Total ribonucleic acid (RNA) was isolated from fresh biopsy specimens and whole blood samples of all patients and controls using a YTA Total RNA Purification Mini kit for Blood/Cultured Cell/Tissue kit (Yekta Tajhiz Azma, Iran) according to the provided protocol. RNA concentration and quality were determined by an ND-1000 spectrophotometer (NanoDrop, Fisher Thermo, Wilmington, DE, USA). cDNA synthesis was performed using the 2 Step 2X RT-PCR Premix (Taq) kit (BioFact™, South Korea) according to the manufacturer’s instructions. Specific primer sequences were designed using gene runner software (V. 3.05). Quantitative RT-PCR was performed in technical duplicate via qPCR on the thermocycler Rotor Gene Q MDx (QIAGEN) with SYBR Green Master Mix (BioFact™, South Korea). Relative mRNA expression levels of CD25, Foxp3, as Treg cells specific markers, and IL-10 and GrzB, as their suppressive mediators, were evaluated and normalized to Beta-2-microglobulin (B2M) expression using the ΔΔCt method. The gene-specific primers sequences are shown in Table 1.
Enzyme-linked immunosorbent assay
Serum was obtained from fresh whole blood samples that were allowed to clot for 15 min and then centrifuged for 20 min at 2000 rpm, aliquoted and promptly stored at −80 °C until further assay. The levels of serum IL-10 (as Tregs developed anti-inflammatory cytokine) and IL-6 (as celiac disease pathogenesis related proinflammatory cytokine) were tested with sandwich enzyme-linked immunosorbent assay (ELISA) kits (Karmania Pars Gene, Iran). All samples were assayed in triplicate and all tests were performed according to the manufacturer’s protocols.
Statistical analysis
All the data were expressed as the mean ± standard deviation (SD). Two groups were compared by Student’s t-test. Results were analyzed using SPSS (version 24; Chicago, IL, USA) and GraphPad Prism 6.07 software. p values were considered significant at less than 0.05.
Results
Decreased frequencies of CD4 + CD25 + Foxp3 + Treg in PBMCs of CD patients
Flow cytometry was conducted to investigate the frequency of Tregs in PBMCs of CD patients and healthy controls. To identify Tregs, CD4+ lymphocytes were gated from a total cell population, and CD25+ and Foxp3+ populations were further gated. As shown in Fig. 1, the percentage of CD4+ CD25+ Foxp3+ Treg population was significantly decreased in treated CD patients (Mean ± SD: 0.29 ± 0.26) compared to healthy controls (Mean ± SD: 2.373 ± 1.44) (p = 0.012).
mRNA expression of CD25, Foxp3, GrzB and IL-10 in duodenal and PBMC specimens of CD patients
The data derived from the real-time PCR showed a significant increase in CD25 and Foxp3 mRNA expression in freshly isolated duodenal specimens of treated CD patients (Mean ± SD: 1.11 ± 1.25 and 2.32 ± 1.43, respectively) compared with healthy non-CD subjects (Mean ± SD: 0.62 ± 0.83 and 1.1 ± 1.12, respectively) (p = 0.01, 0.001, respectively) (Fig. 2). On the other hand, their expression was lower in CD patients’ PBMC specimens without reaching significant values (Mean ± SD: 0.71 ± 0.37 and 0.76 ± 0.28 vs. 0.88 ± 0.6 and 0.91 ± 0.41, respectively) (p > 0.05). Duodenal mRNA level of IL-10 was significantly decreased in CD patients (Mean ± SD: 0.25 ± 0.06) than controls (Mean ± SD: 0.8 ± 0.06) (p = 0.02), but its peripheral blood expression did not differ between the groups (Mean ± SD: 1.09 ± 0.33 vs. 0.99 ± 0.27) (p > 0.05). While no significant difference was observed in the expression levels of GrzB in CD patients’ and controls duodenal specimens (Mean ± SD: 1. 24 ± 0.69 vs. 1.11 ± 0.71) (p > 0.05) (p > 0.05), its peripheral blood expression was significantly lower in CD patients (Mean ± SD: 0.37 ± 0.22) relative to controls (Mean ± SD: 0.91 ± 0.25) (p = 0.001) (Fig. 2).
Cytokine levels
Regulatory T cells are well known to suppress the effector activity of T cells. We then aimed to determine the production of IL-6 as a pro-inflammatory cytokine and IL-10 as Treg cells produced anti-inflammatory cytokine in serum samples of CD patients compared with these levels in non-CD controls using the ELISA method. According to our results, serum level of IL-6 was significantly higher in CD patients (Mean ± SD: 21.95 ± 8.25) compared with controls (Mean ± SD: 3 ± 1.16) (p = 0.001). Levels of serum IL-10 did not significantly differ between patients (Mean ± SD: 8.4 ± 2.96) and controls (Mean ± SD: 7.38 ± 3.71) (p > 0.05) (Fig. 3).
Discussion
In the present study, we evaluated the percentage of Tregs in peripheral blood of treated CD patients (who were on a GFD for more than 6 months) and investigated patients’ pro- and anti-inflammatory mediators’ expression relative to controls. Our results showed that CD4+ CD25+ Foxp3+ T cells were significantly decreased in the peripheral blood of treated CD patients (p = 0.012). Accordingly, the CD patient’s PB mRNA expression levels of CD25 and Foxp3 were lower than controls, though they did not reach statistical significance (p > 0.05). In this regard, Belhadj Hmida et al. reported a comparable percentage of peripheral blood Treg cells among treated CD patients and controls and observed resistance of intraepithelial lymphocytes to these cells’ suppressive effects [17]. Frisullo and colleagues also reported reduced peripheral blood level of CD4+ CD25+ Foxp3+ T cells in treated CD patients than in controls without reaching significant values [40]. Kumar et al. showed a reduced peripheral blood number of Foxp3+ T cells in treated CD patients than in controls [41]. The percentage of peripheral blood Treg cells in active CD patients has been described as increased, decreased or unchanged relative to controls [17, 18, 40,41,42,43]. It can be hypothesized that changes in these cells’ population might be transient in CD patients leading to different reports by researchers. Moreover, this is noteworthy that, Christophersen and colleagues evaluated the T cell response to gluten using tetramer-based techniques in HLA-DQ2.5+ individuals. According to their results, no gluten epitopes related Treg responses were observed in the majority of their study subjects. The exact reason why most susceptible individuals never develop CD despite gluten exposure is still unexplained, but based on this finding, Treg cells may not play a role in controlling the immune responses to gluten in healthy subjects. Therefore, defects in Tregs control are unlikely to result in celiac disease pathogenesis [44]. But it has been proven that the presence of Tregs in the inflamed area is necessary to modulate the immune reaction and suppress effector T cells [25]. In this regard, Belhadj Hmida et al. reported a significantly higher percentage of CD4+ CD25+ Foxp3+ lymphocytes in the lamina propria of GFD treated CD patients than controls [17]. Our results also showed increased duodenal expression of CD25 and Foxp3 in GFD treated CD patients compared to the control group (p = 0.01, 0.001, respectively). It can be assumed that despite following the diet, patients’ intestines may still have residual inflammation and Tregs accumulation in this area is to suppress tissue damage.
According to our results, PB mRNA and protein levels of IL-10 did not differ between two studied groups (p > 0.05), but the PB mRNA level of GrzB was significantly lower in patients than in the controls (p = 0.001). In duodenal samples of CD patients, GrzB mRNA expression did not show significant changes (p > 0.05), but IL-10 expression was significantly reduced relative to controls (p = 0.02). IL-6 serum level was also significantly increased in patients than in controls (p = 0.001). Cook et al. in their in vitro study, found the impaired polyclonal suppressive function of peripheral blood Foxp3 + Treg cells following oral gluten challenge of celiac patients who were on a GFD for ≥ 6 months [35]. As CD patients in our study have shown lower intestinal IL-10 and PB GZMB mRNA levels than controls, and due to their significantly higher protein levels of IL-6 as a proinflammatory cytokine, their re-exposure to small amounts of gliadin may lead to severe inflammation.
The major limitation of the study is that our analysis of Tregs percentage is restricted to the peripheral blood samples and we did not evaluate their numbers in duodenal samples. Studies including active CD subjects and using Tregs in vitro suppressor activity assays are also needed to confirm the results of our study.
Conclusion
According to the last findings suggesting the less effectiveness of GFD in treating CD, evidence of pathogenic T cells remaining active during this regimen, observing reduced frequency of Tregs in GFD patients’ peripheral blood samples but reported increased Tregs frequency in their duodenal specimens, we speculate that, despite following the GFD, there may still be residual inflammation in the intestine. Accordingly, finding a therapeutic approach based on strengthening the function of Treg cells in celiac disease for reducing harmful immune responses in case of exposure to gluten becomes more important.
References
Vriezinga SL, Schweizer JJ, Koning F, Mearin ML (2015) Coeliac disease and gluten-related disorders in childhood. Nat Rev Gastroenterol Hepatol 12:527–536. https://doi.org/10.1038/nrgastro.2015.98
Bascuñán KA, Vespa MC, Araya M (2017) Celiac disease: understanding the gluten-free diet. Eur J Nutr 56:449–459. https://doi.org/10.1007/s00394-016-1238-5
Lebwohl B, Sanders DS, Green PHR (2018) Coeliac disease. Lancet 391:70–81. https://doi.org/10.1016/s0140-6736(17)31796-8
Rostami-Nejad M, Razzaghi Z, Esmaeili S, Rezaei-Tavirani S, Akbarzadeh Baghban A, Vafaee R (2020) Immunological reactions by T cell and regulation of crucial genes in treated celiac disease patients. Gastroenterol Hepatol Bed Bench 13:155–160
Bardella MT, Elli L, Velio P, Fredella C, Prampolini L, Cesana B (2007) Silent celiac disease is frequent in the siblings of newly diagnosed celiac patients. Digestion 75:182–187. https://doi.org/10.1159/000107979
Admou B, Essaadouni L, Krati K et al (2012) Atypical celiac disease: from recognizing to managing. Gastroenterol Res Pract 2012:637187–637187. https://doi.org/10.1155/2012/637187
Gujral N, Freeman HJ, Thomson ABR (2012) Celiac disease: prevalence, diagnosis, pathogenesis and treatment. World J Gastroenterol 18:6036–6059. https://doi.org/10.3748/wjg.v18.i42.6036
Caio G, Volta U, Sapone A et al (2019) Celiac disease: a comprehensive current review. BMC Med 17:142–142. https://doi.org/10.1186/s12916-019-1380-z
Meresse B, Ripoche J, Heyman M, Cerf-Bensussan N (2009) Celiac disease: from oral tolerance to intestinal inflammation, autoimmunity and lymphomagenesis. Mucosal Immunol 2:8–23. https://doi.org/10.1038/mi.2008.75
Asri N, Nazemalhosseini Mojarad E, Mirjalali H et al (2021) Toward finding the difference between untreated celiac disease and COVID-19 infected patients in terms of CD4, CD25 (IL-2 Rα), FOXP3 and IL-6 expressions as genes affecting immune homeostasis. BMC Gastroenterol 21:462–462. https://doi.org/10.1186/s12876-021-02056-1
Gianfrani C, Levings MK, Sartirana C et al (2006) Gliadin-specific type 1 regulatory T cells from the intestinal mucosa of treated celiac patients inhibit pathogenic T cells. J Immunol 177:4178–4186. https://doi.org/10.4049/jimmunol.177.6.4178
Torres MI, López Casado MA, Ríos A (2007) New aspects in celiac disease. World J Gastroenterol 13:1156–1161. https://doi.org/10.3748/wjg.v13.i8.1156
Pabst O, Mowat AM (2012) Oral tolerance to food protein. Mucosal Immunol 5:232–239. https://doi.org/10.1038/mi.2012.4
Schuster M, Plaza-Sirvent C, Visekruna A, Huehn J, Schmitz I (2019) Generation of Foxp3+CD25—regulatory T-cell precursors requires c-Rel and IκBNS. Front Immunol 10:1583. https://doi.org/10.3389/fimmu.2019.01583
Faria AMC, Weiner HL (2006) Oral tolerance: therapeutic implications for autoimmune diseases. Clin Dev Immunol 13:828392. https://doi.org/10.1080/17402520600876804
Coleman MM, Finlay CM, Moran B, Keane J, Dunne PJ, Mills KH (2012) The immunoregulatory role of CD4+ FoxP3+ CD25− regulatory T cells in lungs of mice infected with Bordetella pertussis. Immunol Med Microbiol 64:413–424. https://doi.org/10.1111/j.1574-695X.2011.00927.x
Hmida NB, Ben Ahmed M, Moussa A et al (2012) Impaired control of effector T cells by regulatory T cells: a clue to loss of oral tolerance and autoimmunity in celiac disease? Am J Gastroenterol 107:604–611. https://doi.org/10.1038/ajg.2011.397
Granzotto M, dal Bo S, Quaglia S et al (2009) Regulatory T-cell function is impaired in celiac disease. Dig Dis Sci 54:1513–1519. https://doi.org/10.1007/s10620-008-0501-x
Cook L, Munier CML, Seddiki N et al (2020) Circulating gluten-specific, but not CMV-specific, CD39(+) regulatory T cells have an oligoclonal TCR repertoire. Clin Transl Immunol 9:e1096–e1096. https://doi.org/10.1002/cti2.1096
Workman CJ, Szymczak-Workman AL, Collison LW, Pillai MR, Vignali DAA (2009) The development and function of regulatory T cells. Cell Mol Life Sci 66:2603–2622. https://doi.org/10.1007/s00018-009-0026-2
Li Z, Li D, Tsun A, Li B (2015) FOXP3+ regulatory T cells and their functional regulation. Cell Mol Immunol 12:558–565. https://doi.org/10.1038/cmi.2015.10
Zhao H, Liao X, Kang Y (2017) Tregs: where we are and what comes next? Front Immunol 8:1578. https://doi.org/10.3389/fimmu.2017.01578
Wang J, Ioan-Facsinay A, van der Voort EI, Huizinga TW, Toes RE (2007) Transient expression of FOXP3 in human activated nonregulatory CD4+ T cells. Eur J Immunol 37:129–138. https://doi.org/10.1002/eji.200636435
Lee W, Lee GR (2018) Transcriptional regulation and development of regulatory T cells. Exp Mol Med 50:e456–e456. https://doi.org/10.1038/emm.2017.313
Asri N, Rostami-Nejad M, Barzegar M et al (2020) Suppressive mechanisms induced by tregs in celiac disease. Iran Biomed J 24(3):140–147
Schmidt A, Oberle N, Krammer P (2012) Molecular mechanisms of treg-mediated T cell suppression. Front Immunol 3:51. https://doi.org/10.3389/fimmu.2012.00051
Jordan MA, Field J, Butzkueven H, Baxter AG (2014) Genetic predisposition, humans. In: Rose NR, Mackay IR (eds) The autoimmune diseases, 5th edn. Academic Press, Boston, pp 341–364
Kasper IR, Apostolidis SA, Sharabi A, Tsokos GC (2016) Empowering regulatory T cells in autoimmunity. Trends Mol Med 22:784–797. https://doi.org/10.1016/j.molmed.2016.07.003
Chinen T, Kannan AK, Levine AG et al (2016) An essential role for the IL-2 receptor in Treg cell function. Nat Immunol 17:1322–1333. https://doi.org/10.1038/ni.3540
Verbsky JW, Routes JR (2018) Recurrent fever, infections, immune disorders, and autoinflammatory diseases. In: Kliegman RM, Lye PS, Bordini BJ, Toth H, Basel D (eds) Nelson pediatric symptom-based diagnosis. Elsevier, Amsterdam, pp 746–773
Vella A, Cooper JD, Lowe CE et al (2005) Localization of a type 1 diabetes locus in the IL2RA/CD25 region by use of tag single-nucleotide polymorphisms. Am J Hum Genet 76:773–779. https://doi.org/10.1086/429843
Vignali DAA, Collison LW, Workman CJ (2008) How regulatory T cells work. Nat Rev Immunol 8:523–532. https://doi.org/10.1038/nri2343
Shevyrev D, Tereshchenko V (2020) Treg heterogeneity, function, and homeostasis. Front Immunol. https://doi.org/10.3389/fimmu.2019.03100
Penny HA, Baggus EMR, Rej A, Snowden JA, Sanders DS (2020) Non-Responsive coeliac disease: a comprehensive review from the NHS England national centre for refractory coeliac disease. Nutrients 12:216. https://doi.org/10.3390/nu12010216
Cook L, Munier CML, Seddiki N et al (2017) Circulating gluten-specific FOXP3(+)CD39(+) regulatory T cells have impaired suppressive function in patients with celiac disease. J Allergy Clin Immunol 140:1592-1603.e1598. https://doi.org/10.1016/j.jaci.2017.02.015
Tiittanen M, Westerholm-Ormio M, Verkasalo M, Savilahti E, Vaarala O (2008) Infiltration of forkhead box P3-expressing cells in small intestinal mucosa in coeliac disease but not in type 1 diabetes. Clin Exp Immunol 152:498–507. https://doi.org/10.1111/j.1365-2249.2008.03662.x
Mazzarella G (2015) Effector and suppressor T cells in celiac disease. World J Gastroenterol 21:7349–7356. https://doi.org/10.3748/wjg.v21.i24.7349
Bardella MT, Elli L, Ferretti F (2016) Non celiac gluten sensitivity. Curr Gastroenterol Rep 18:63. https://doi.org/10.1007/s11894-016-0536-7
Anderson RP (2022) Emergence of an adaptive immune paradigm to explain celiac disease: a perspective on new evidence and implications for future interventions and diagnosis. Expert Rev Clin Immunol 18:75–91. https://doi.org/10.1080/1744666x.2021.2006636
Frisullo G, Nociti V, Iorio R et al (2009) Increased CD4+CD25+Foxp3+ T cells in peripheral blood of celiac disease patients: correlation with dietary treatment. Hum Immunol 70:430–435. https://doi.org/10.1016/j.humimm.2009.04.006
Kumar S, Lal S, Bhatnagar A (2017) Regulatory T cell subsets in peripheral blood of celiac disease patients and TLR2 expression: correlation with oxidative stress. APMIS 125:888–901. https://doi.org/10.1111/apm.12735
Brazowski E, Cohen S, Yaron A, Filip I, Eisenthal A (2010) FOXP3 expression in duodenal mucosa in pediatric patients with celiac disease. Pathobiology 77:328–334. https://doi.org/10.1159/000322049
Vorobjova T, Uibo O, Heilman K et al (2009) Increased FOXP3 expression in small-bowel mucosa of children with coeliac disease and type I diabetes mellitus. Scand J Gastroenterol 44:422–430. https://doi.org/10.1080/00365520802624177
Christophersen A, Risnes LF, Bergseng E, Lundin KE, Sollid LM, Qiao SW (2016) Healthy HLA-DQ2.5+ subjects lack regulatory and memory T cells specific for immunodominant gluten epitopes of celiac disease. J Immunol 196:2819–2826. https://doi.org/10.4049/jimmunol.1501152
Acknowledgements
The authors would like to acknowledge the Gastroenterology and Liver Diseases Research Center of Shahid Beheshti University of Medical Sciences for their support and contribution to this study. The authors would also like to thanks Dr Robert P Anderson from Wesley Medical Research—The Wesley Hospital, Brisbane, Queensland, Australia for his critical review.
Funding
Research reported in this publication was supported by Elite Researcher Grant Committee under Award Number (983076) from the National Institute for Medical Research Development (NIMAD), Tehran, Iran and Gastroenterology and Liver Diseases Research Center of Shahid Beheshti University of Medical Sciences.
Author information
Authors and Affiliations
Contributions
Design of experiments by MRN and AN. Analysis of data by NA and EA. First draft of manuscript by NA, and subsequent drafting by MRN, MRZ and HAA. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interest to disclose.
Ethical approval
The study was approved by the ethical committee of the Research Institute for Gastroenterology and Liver Diseases (RIGLD), Shahid Beheshti University of Medical Sciences, Tehran, Iran (IR.SBMU.MSP.REC.1397.564).
Consent to participate
Not applicable.
Consent to publish
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Asri, N., Rostami-Nejad, M., Nikzamir, A. et al. Reduced frequency of circulating regulatory T cells and their related immunosuppressive mediators in treated celiac patients. Mol Biol Rep 49, 8527–8535 (2022). https://doi.org/10.1007/s11033-022-07674-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11033-022-07674-w