Abstract
Background
Myeloid cell leukemia-1 (MCL-1) is a component of the Bcl-2 anti-apoptotic family that plays a key role in cell proliferation and differentiation. Despite tremendous improvements toward identification of the role of MCL-1 in leukemia progression, the functional significance and molecular mechanism behind the effect of MCL-1 overexpression on the proliferation of B-cell precursor acute lymphoblastic leukemia (BCP-ALL) has not been clarified. In addition, less well appreciated is the effect of MCL-1 inhibition on the potentiation of doxorubicin-induced apoptosis in BCP-ALL cell lines. In the present study, we aimed to shed light on the anti-cancer properties of S63845, a potent Mcl-1 inhibitor, in BCP-ALL cell lines either alone or in combination with a chemotherapeutic drug.
Methods and results
Mononuclear cells from patients with Pre-B ALL and BCP-ALL cell lines were treated with S63845 in presence or absence of doxorubicin, induction of apoptosis was evaluated using Annexin-V/PI staining kit. mRNA and protein expression levels were assessed by qRT-PCR and western blot analysis, respectively. Our results declared that inhibition of Mcl-1 impairs cell growth and induces apoptosis in pre-B ALL cells through activation of caspase-3 and up-regulation of a repertoire of pro-apoptotic Bcl-2 family. Additionally, S63845 acts synergically with doxorubicin to induce apoptosis in BCP-ALL cell lines.
Conclusions
Our data declared that MCL-1 inhibition alone or in combination with a chemotherapeutic agent is considered an appealing strategy for the induction of apoptosis in BCP-ALL cells.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In spite of astonishing progress in the cure rate of patients with acute lymphoblastic leukemia (ALL), resistance to chemotherapeutic drugs still remains a major concern in the management of ALL [1]. On the other hand, relapse occurs in 15 to 20% of children with ALL, and after relapse, the cure rate becomes lower [2]. Pieces of evidence have shown that complex molecular events result in ALL development [3]. Deregulated expression of genes involved in lymphoid development is a hallmark of acute lymphoblastic leukemia progression [4]. In addition, evasion of leukemic cells from apoptosis is essential for development and expansion of the malignant cells [5].
Apoptosis is a regulated programmed cell death that is essential for normal cell growth and hemostasis [6]. Impaired apoptosis may result in cancer development and resistance to chemotherapeutics [7]. The BCL-2 family members are the dominant regulator of both cell proliferation and apoptosis, the two processes that are dysregulated during oncogenesis [8, 9]. Interaction between three subsets of Bcl-2 family proteins determines whether the cells undergo apoptosis or proliferation. The Bcl-2 family comprises a pro-survival group such as BCL-2, BCL-xL, MCL-1, BCL-W, and BFL-1 and two pro-apoptotic groups consist of pore formers (BAX, BAK, and BOK) and the BH3-only apoptosis factors (BIM, BAD, BID, BIK, NOXA, PUMA, etc.) [10]. For the initiation of apoptosis, the BH3-only proteins bind to the Bcl-2 anti-apoptotic proteins and prevent them from inhibition of BAK and BAX activation. Activated BAK/BAX proteins initiate intrinsic apoptotic pathway through mitochondrial outer membrane permeabilization and caspase cascade activation [10, 11].
Myeloid cell leukemia-1 (MCL-1), a pro-survival member of the BCL-2 family, plays a pivotal role in maintaining cell survival through binding and seizing pro-apoptotic factors, such as BAK, BAX, or BCL-2 homology proteins BAD and BIM. MCL-1 gene amplifies in a variety of human cancers and it’s overexpression is associated with chemotherapeutic resistance and relapse in patients [12, 13]. The importance of MCl-1 is its crucial role in the development and continuous growth of leukemic cells in acute myeloid leukemia, multiple myeloma, lymphoma, breast cancer, non-small-cell lung carcinoma [12, 14,15,16]. It has been proved that acute lymphoblastic leukemia cell lines are dependent on MCL-1 expression and function [17]. Additionally, MCL-1 has been described as an essential factor for initiation and maintenance of Ph+ B-ALL [18]. Down-regulation of MCL-1 in BCR-ABL positive cells sensitizes the leukemic cells to tyrosine kinase inhibitors [18]. Up-regulated expression of MCL-1 is associated with ABT-737 resistance and downregulation of this anti-apoptotic factor resulted in increased cytotoxicity of ABT-737 in ALL derived cell lines [19].
MCL-1 can be placed at the top of the experimental studies not only for its role in leukemogenesis but also for its role in chemo-resistance in a variety of malignancies. Conditional gene knockdown exhibit an essential role for MCL-1 in tumorigenesis and survival of hematopoietic stem cells [10, 20]. Many academic laboratories and institutes have been developed the researches on Mcl-1 inhibitors [21]. S63845, a potent Mcl-1 inhibitor, interacts with the BH3-binding groove of MCL-1 and disrupts attachment of BAK and BAX to MCL-1, whereas it does not affect BCL-2 or BCL-XL interaction with pro-apoptotic proteins [10].
In the present study we sought to determine the effect of MCL-1 inhibitor, S63845, either alone or in combination with doxorubicin in BCP-ALL cell lines. Our results demonstrated that S63845 induces apoptosis through BAK/BAX activation and acts synergistically with doxorubicin to augment apoptosis compared to either agent alone in BCP-ALL cell.
Material and method
Chemicals and reagent
The reagents in the study were provided from the following manufacturers: S63845, MCL-1 inhibitor (Selleckchem, USA), trypan blue (T6146), MTT powder 3-(4, 5-dimethylthiazol-2-yl)-2, 5-diphenyltetrazolium bromide (M5655), western blotting required antibodies including caspase-3(9665 S), PARP (9542P), Mcl-1 (5453P), c-Myc (5605 T) and b-actin (8H10D10) were purchased from Cell Signaling Technology (Danvers, Massachusetts, USA). HRP conjugated secondary antibodies were purchased from Santa Cruz Biotechnology (SantaCruz, California, USA).
Patient sampling and mononuclear cell extraction
Bone marrow sample from patient with BCP-ALL was collected at diagnosis. Peripheral blood cells were collected from healthy donors. Samples were obtained after informed consents. Mononuclear cells in peripheral blood (PBMC) and bone marrow were isolated by density gradient centrifugation with lymphodex (Inno-Train Diagnostik, Kronberg, Germany) and cultured in RPMI1640 supplemented with 10% FBS and 2 mM l-glutamine, 100 units/ml penicillin, and 100 mg/ml streptomycin. Cells were treated with 200 nM doxorubicin either with or without S63845 (500 nM) for 24 h.
Cell culture
BCP-ALL cell lines including NALM-6 and SUP-B15 (obtained from Pasteur Institute, Tehran, Iran) were used in our experiment. NALM-6 cells were cultured in RPMI medium supplemented with 10% FBS. SUP-B15 (human Ph+ ALL cells) were maintained in Iscove’s Modified Dulbecco’s Medium (IMDM) with 20% FBS. Both culture mediums were contained 2 mM l-glutamine, 100 units/ml penicillin, and 100 mg/ml streptomycin. Cells were maintained in humidified 5% CO2 incubator at 37 °C under standard culture condition.
Trypan blue assay
Pre-B ALL-derived cell lines, NALM-6 and SUP-B15 cells were seeded at the density of 4 × 105 cells/ml (5 × 105 cells/ml for SUP-B15 cells) in a 24 well plate. Cells were treated either with S63845 alone or in combination with the doxorubicin for 24 and 48 h. Then, cells were mixed with trypan blue dye and incubated for 2 to 3 min at room temperature. The number of viable cells was counted with the Neubauer hemocytometer and represented as a percentage in figures [22].
Metabolic activity assay
The effect of S63845 in the presence or absence of doxorubicin on the metabolic activity of BCP-ALL cell lines was assessed using the MTT colorimetric method. Furthermore, to explore the synergic effect between the S63845 and doxorubicin, we used MTT assay. Briefly, NALM-6 and SUP-B15 cells were seeded in 96 well plates in a concentration of 20,000 cells/well and 40,000 cells/well, respectively. Cells were treated with various concentrations of S63845 with or without doxorubicin for 24 h. Following medium removal, MTT solution (5 mg/ml PBS) was added to the cells. After 4 h of incubation, the resulting formazan was solubilized with DMSO (100 µl). The absorbance of each well was measured at 570 nm in an ELISA reader.
Determination of combination index
To determine if the combination of S63845 and doxorubicin is synergistic, additive, or antagonistic, we assessed the value of the combination index (CI) using compucyn software. The CI values of <1, = 1, and >1 indicate synergism, additive, and antagonism effects of drugs, respectively [23].
Cell apoptosis assay
The cell lines were cultured in 12-well plates at a density of 5 × 105 cells/ml (6 × 105 cells/ml for SUP-B15) and treated with different concentrations of S63845 either in the presence or absence of doxorubicin for 24 h. After incubation, cells were harvested, washed with cold PBS, and stained by Annexin V-FITC apoptosis detection Kit II (BD Biosciences) according to the manufacturer´s instruction. Fluorescence was accessed using flow cytometry. Annexin-V-positive and PI-negative cells were categorized as early apoptotic cells, whereas cells positive for both Annexin-V and PI were presented as late apoptotic cells [23].
Measurement of caspase-3 enzymatic activity
To evaluate whether S63845 exerts its apoptotic effect by activation of caspase-3, the enzymatic activity of caspase-3 was assessed using the Caspase activity assay kit (Cell signaling). NALM-6 and SUP-B15 cells were cultured in a 96-well plate and treated with different concentrations of S63845 for 24 h. Then, cells were centrifuged at 500 g and washed with cold PBS. The cell lysis buffer was added to the cell plate and was left on ice for 10 min. Cell lysate solution was mixed with substrate solution and after incubation in 37 °C relative fluorescent units were assessed using an Elisa reader.
RNA extraction and quantitative real-time PCR
Cells treated with either S63845 or doxorubicin and total RNA were extracted using Tripure isolation reagent (Roche) according to the manufacturer’s protocol. One microgram of isolated RNA was utilized for cDNA preparation using Revert Aid First Strand cDNA Synthesis Kit (Thermo fisher). Quantitative reverse-transcription polymerase chain reaction (qRT-PCR) was performed using the synthesized cDNA and SYBER green mastermix (Amplicon) employing the Light Cycler 96 Realtime PCR system (Roche Diagnostics, Lewes, UK) [22]. cDNA was amplified in a 40 cycle PCR. The qRT-PCR reaction was performed with the following condition: 95 °C for 15 min, denaturation at 95 °C for 15 s, annealing and elongation at 60 °C for 60 s [22]. The fold induction or repression was determined relative to control cells and measured after adjustment with b-ACTIN. All samples were analyzed in a triplicate manner and the gene expression-related fold change was measured using comparative CT (2−∆∆CT). Primer sequences are available in Supplementary Table 1.
Protein extraction and western blot analysis
NALM-6 and SUP-B15 cells were treated with S63845 in the presence or absence of the doxorubicin for 24 h. Following incubation, cells were harvested, washed twice using cold PBS, and lysed by RIPA buffer (10 mM Tris-HCl, pH 7.4, 150 mM NaCl, 5 mM EDTA, 1% Triton X-100, 0.1% sodium dodecyl sulfate, and 0.5% sodium deoxycholate) containing protease and phosphatase inhibitor cocktails (Sigma-Aldrich) [24]. The suspension was centrifuged at 13,000 × g for 20 min at 4 °C and supernatant was collected. Protein concentrations were measured using the Bradford protein assay, and equivalent amounts of cellular protein (80 µg) were aliquoted and subjected to 10% SDS-PAGE. Afterward, gels were electroblotted onto nitrocellulose membranes (Hybond-ECL, Amersham Corp), The membranes were then blocked with 5% nonfat skim milk in Tris-buffered saline with 0.1% Tween-20 (TBST) for 1 h at room temperature. Then, membranes were incubated overnight at 4 °C with the specific primary antibodies. The day after, membranes were washed 3 times with TBS-T and were incubated with HRP-conjugated secondary antibodies. The protein signals were visualized with an ECL detection kit (Amersham ECL Advance Kit, GE Healthcare) [24].
Statistical analysis
All analyses were performed in a triplicate manner and data were expressed as mean standard deviation. Data were analyzed using a two-tailed student t-test. A p value of <0.05 was considered to be significant.
Results
S63845 induces an inhibitory effect on the growth and metabolic activity of BCP-ALL cell lines
In order to investigate the anti-proliferative effect of MCL-1 inhibitor, S63845, on BCP-ALL cell lines, we applied MTT assay and trypan blue method for evaluation of cell viability and drug cytotoxicity. To do so, NALM-6 and SUP-B15 cells were treated with increasing concentrations of S63845. After 24 and 48 h, cells were harvested for MTT analysis and trypan blue method. MTT assay showed that metabolic activity of pre-B ALL cell lines were reduced in a dose-dependent manner upon S63845 treatment (Fig. 1a, b) which was in agreement with trypan blue assay results (Supplementary Fig. 1a, b). However, our data showed that cell death induced by S63845 for 24 h was not significantly different with cell death after 48 h in both cell lines. Therefore, we used to treat cells for 24 h in our whole experiment. IC50 values of S63845 were determined by Compusyn software [25]. Estimated IC50 for NALM-6 and SUP-B15 cells were 2324 nM and 104.75 nM, respectively (Supplementary Fig. 1c, d). As depicted in the figures, NALM-6 and SUP-B15 cells responded differently to the various doses of S63845, so we treated our cells with different concentrations of S63845.
S63845 attenuates the viability of BCP ALL cell lines. Increasing concentrations of S63845 were used to treat a NALM-6 and b SUP-B15 cells for 24 and 48 h. Metabolic activity was assessed with colorimetric MTT assay. The results are presented as the mean SD of at least three independent experiments. (*P < 0.05, **P < 0.01, ***P < 0.001 compared to control untreated cells)
S63845 induces apoptosis through activation of the caspase 3 and pro-apoptotic BCL-2 family members in BCP-ALL cells
Having established the growth inhibitory effect of S63845 on NALM-6 and SUP-B15 cells, we sought to investigate whether the anti-proliferative role of S63845 on BCP-ALL cells is mediated through apoptosis induction. To do so, both cell lines were treated with increasing doses of S63845 for 24 h, and induction of apoptosis was assessed using FACS analysis of annexin-V/PI staining. Mcl-1 inhibition results in a considerable dose-dependent increase in annexin-V/PI double-positive cells in both BCP-ALL cell lines (Fig. 2a, b; and Supplementary Fig. 2a, b). To further investigating the effect of the MCL-1 inhibition on apoptosis mechanisms of BCP-ALL cells, mRNA expression of BAX, BAK, NOXA, BIM, BCL-2, BCL-xL, and MCL-1 were measured as the mitochondrial cell death effectors [26, 27]. With this aim, NALM-6 and SUP-B15 cells were treated with two concentrations of S63845 that induced significantly different apoptosis from each other in cells. After 24 h cells were harvested and mRNA expression of mentioned above genes was measured using qRT-PCR. S63845 treatment induced the dose-dependent elevation of BAX, BAK, NOXA, BIM but did not alter the expression levels of BCL-2 and BCL-xL in both cell lines (Fig. 2c, d). Notably, the mRNA expression level of MCL-1 was increased in cells treated with S63845. In addition, it was of great interest to evaluate whether cell death is mediated by caspase-3 activation. For this aim, apoptosis induction was evaluated by caspase-3 activity assay in NALM-6 and SUP-B15 cells following S63845 treatment for 24 h. The result disclosed that S63845-induced apoptosis is due to caspase-3 activation in both BCP-ALL cell lines (Supplementary Fig. 2c, d).
Effects of S63845 on induction of apoptosis in BCP-ALL cell lines. a NALM-6 cells were treated with different concentrations of S63845 (250, 500, and 750 nM) and b SUP-B15 cells were incubated with various doses of S63845 (40, 60, and 80 nM). After 24 h both cell lines were collected and subjected to Annexin-V/PI staining. c NALM-6 cells and d SUP-B15 cells were treated with indicated doses of S63845 for 24 h and then mRNA expression levels of BAX, BAK, BIM, NOXA, BCL-2, BCL-xL, and MCL-1 were measured using quantitative real-time PCR. Levels gene expression were normalized to ACTIN (n = 3, *P < 0.05, **P < 0.01, ***P < 0.0001, relative to control cells)
Doxorubicin-induced cell death is enhanced by Mcl-1 inhibition in BCP-ALL cell lines
Doxorubicin is a potent chemotherapeutic drug which routinely used in ALL treatment [28]. In our study, cytotoxicity of doxorubicin on BCP-ALL cells was first assessed by MTT assay to determine the viability of doxorubicin-treated cells. To evaluate the effect of doxorubicin on cells, NALM-6 and SUP-B15 cells were treated with 50, 100, 150, 200, 250, 300, 500 nM and SUP-B15 cells were treated with 5, 10, 20, 30, 40, 60, 70 nM of doxorubicin, respectively. The MTT results indicated that doxorubicin induces a dose-dependent inhibition of metabolic activity in both NALM-6 and SUP-B15 cells with an estimated IC50 of 533 nM and 38.5 nM, respectively, for 24 h (Supplementary Fig. 3a, b). Since doxorubicin can induce dose-dependent cardiomyopathy which limits the maximum dose uptake in clinic [29], it was intriguing to evaluate whether the inhibition of MCL-1 could reinforce the apoptotic effect of doxorubicin on BCP-ALL cells. To do so, NALM-6 and SUP-B15 cells were treated with two escalating doses of S63845 alone or in combination with doxorubicin for 24 h. MTT assay results indicated that cell metabolic activity decreased in cells treated with both doxorubicin and S63845 compared with either drug alone (Fig. 3a, b). To assess whether the interplay between these two agents caused a synergic or additive effect, the combination index (CI) was calculated using Compucyn software. As indicated in Fig. 3c and d, dose-effect and combination index curves demonstrated a synergic cytotoxic effect when doxorubicin was used in combination with S63845. Interestingly, the most effective doses with the least CI were selected for our experiment for both BCP-ALL cell lines (NALM-6 cells were treated with 500 nM S63845 in combination with 200 nM doxorubicin and SUP-B15 cells treated with 60 nM S63845 and 20 nM doxorubicin for 24 h).
Synergic effect of S63845 with doxorubicin in acute lymphoblastic leukemia cells. a NALM-6 and b SUP-B15 cells were treated with two different doses of S63845 and Dox. After 24 h cells were harvested and the metabolic activity of cells was evaluated by MTT assay. The combination index for NALM-6 (c) and SUP-B15 (d) cells was determined in accordance with the isobologram equation; (Dx)1 and (Dx)2 expressed the individual doses of Dox and S63845 required to inhibit a particular level of viability index, and (D)1 and (D)2 are the doses of Dox and S63845 that are essential to produce the same effect in combination, respectively. Points above and below the iso-effect line reflect antagonism and synergy, respectively
MCL-1 inhibitor intensifies doxorubicin-induced apoptosis in BCP-ALL cell lines through caspase activation and PARP cleavage
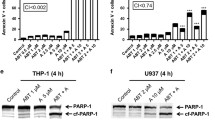
Having proved the synergic cytotoxic effect of S63845 in combination with doxorubicin on both BCP-ALL cell lines, it was of high interest to figure out if the induced cell death was due to the induction of caspase-mediated apoptosis. To this end, NALM-6 and SUP-B15 cells were treated with 500 nM and 60 nM of S63845 respectively with or without doxorubicin (200 nM and 20 nM for NALM-6 and SUP-B15, respectively). After 24 h cells were harvested and induction of apoptosis was assessed utilizing Annexin-V apoptosis detection kit by flowcytometry analysis. The rate of early apoptosis (Annexin V-positive cells) and late apoptosis (Annexin V/PI double-positive cells) was identified upon assorted treatment by doxorubicin and S63845 in both cell lines. As indicated in Fig. 4a, the total percentage of apoptotic cells (Annexin-V and Annexin-V/PI double-positive cells) exposing with both agents was increased by 46.3% compared to 19.2% with doxorubicin alone in NALM-6 cells. The apoptotic SUP-B15 cells were elevated by 41.6% in cells treated with a combination of both agents compared to 17.8% apoptosis in cells treated with doxorubicin alone (Fig. 4b). According to the flow cytometry results, it was tempting to verify the apoptotic events at the molecular level. For this purpose, we evaluated the cleavage of PARP and caspase-3 proteins through western blot analysis. Both cell lines were treated with mentioned above concentrations for 24 h and the total protein was subjected to western blot analysis. Combined treatment of NALM-6 and SUP-B15 cells with doxorubicin and S63845 results in significant activation and cleavage of PARP and caspase-3 compared with either agent alone (Fig. 4c).
S63845 potentiates doxorubicin-induced apoptosis through PARP activation. a NALM-6 cells were grown in a complete medium with 500 nM of S63845 in the presence or absence of 200 nM of Dox for 24 h. b SUP-B15 cells were incubated with S63845 (60 nM) with or without Dox (20 nM) for 24 h. Afterward, cells were assessed for Annexin-V/PI uptake by flow cytometry. The data shown are representative of at least three independent experiments. (*P < 0.05 compared to Dox treated cells). c BCP-ALL cell lines (NALM-6 and SUP-B15) were treated with indicated concentrations of S63845 with or without doxorubicin for 24 h. The total extracts were prepared and the same amounts of cell lysates (80 µg) were analyzed with western blotting
BAX/BCL-2 ratio was up-regulated through co-treatment of S63845 and doxorubicin in BCP-ALL cell lines
In order to investigate the effect of S63845 in combination with doxorubicin on BAX/BCL-2 ratio in BCP-ALL cells, NALM-6 and SUP-B15 cells were exposed to mentioned concentrations of S63845 and doxorubicin for 24 h. The mRNA expression levels of BAX and BCL-2 were examined using qRT-PCR. The data showed that BAX/BCL-2 mRNA expression ratio was significantly increased in NALM-6 (3.7-fold) and SUP-B15 cells (4.52-fold) compared with untreated control cells (Supplementary Fig. 4a, b). Strikingly, downregulation of BCL-2 in S63845-treated cells was not significant in comparison with untreated control cells, whereas in combination treatment it was down-regulated compared with cells treated with S63845 alone. However, BCL-2 expression was attenuated in cells treated with doxorubicin alone compared with cells in the combination group. All together, S63845 does not play a role in down-regulation of BCL-2 mRNA level but increases the mRNA level of BAX in both cell lines.
The c-Myc proto-oncogene expression was attenuated in the presence of both S63845 and doxorubicin in the BCP-ALL cell line
The Mcl-1 is a critical factor for survival of the c-Myc overexpressing lymphoma [30]. As regards the oncogenic characteristics of c-myc in malignancies through activation of hTERT, we decided to investigate the effect of S63845 on c-Myc expression in the presence or absence of doxorubicin. To this end, NALM-6 cells were treated with 500 nM of S63845 alone or in combination with 200 nM Doxorubicin and SUP-B15 cells were incubated with 60 nM S63845 in the presence or absence of 20 nM doxorubicin. After 24 h cells were harvested, and total cell lysate was subjected to western blot analysis. As indicated in Fig. 5, c-Myc protein expression was attenuated in combination treatment in comparison to each agent alone in both cell lines. For further confirmation, the mRNA expression of c-MYC and hTERT was evaluated with qRT-PCR. The mRNA expression of C-MYC and hTERT were reduced in combination treatment compared with each agent alone (Supplementary Fig. 5a, b). Additionally, mRNA and protein expression of MCL-1 was assessed by qRT-PCR and western blot. Intriguingly, treatment of BCP-ALL cell lines with S63845 results in higher Mcl-1 mRNA and protein expression levels compared with untreated cells (Supplementary Fig. 5). However, the high expression level of Mcl-1 in cells treated with S63845 was attenuated through doxorubicin exposure in combination treatment.
Down-regulation of c-Myc expression in presence of S63845 and doxorubicin in BCP-ALL cells. NALM-6 and SUP-B15 cells were treated with mentioned above doses of S63845 and doxorubicin for 24 h. Cell lysates were extracted and subjected to SDS-PAGE electrophoresis. Mcl-1 and c-Myc Protein expression levels were analyzed by western blotting. Equal sample loading was verified by β-actin. The quantitative values are presented below the western blot figure
Combined doxorubicin and Mcl-1 inhibition potentiate cell death in B Cell precursor acute lymphoblastic leukemia
To investigate the effect of the combination of S63845 and doxorubicin on apoptosis of B cell precursor acute lymphoblastic leukemia, mononuclear cells from bone marrow sample of patients with BCP-ALL and peripheral blood from healthy donor were isolated. Cells were treated with S63845 in present or absence of doxorubicin for 24 h. Apoptotic cells of each group were evaluated using flowcytometry. Our finding demonstrated that co-treatment of S63845 with doxorubicin resulted in significant cell death in BCP-ALL samples compared with healthy group samples (Supplementary Fig. 6).
Discussion
Human cancers have the capacity to commandeer a variety of mechanisms and cellular processes to improve the survival rate and attenuate the apoptosis of malignant cells. Mainly, cancer cells exhibit many characteristics to evade apoptosis [31]. There is growing evidence that one strategy is to overexpress the anti-apoptotic BCL-2 family member, MCL-1, in malignant cells [32]. MCL-1 overexpresses in various cancers and plays a crucial role in protecting cells from apoptosis [32]. Therefore, targeting and inhibiting the MCL-1 may be an attractive issue for finding an effective pharmacological approach for cancer treatment. In a study, Glaser et al., demonstrated that MCL-1 is crucial for sustained survival of acute myeloblastic leukemia cells but a large proportion of T-ALL cells can survive longer-term in absence of MCL-1 [15]. So, it demonstrates that the need for MCL-1 for constant survival of cells is highly specific to cell types. Therefore, we were encouraged to figure out the effect of MCL-1 inhibition on BCP-ALL cell lines either alone or in combination with DNA-damaging chemotherapeutic agent, doxorubicin. Our findings demonstrate that the abrogation of MCL-1 using S63845 alone resulted in reduced survival of BCP-ALL-derived cell lines, NALM-6, and SUP-B15. Furthermore, the anti-leukemic effect of S63845 was confirmed by indicating that MCL-1 inhibitor induces apoptosis through up-regulation of BCL-2 pro-apoptotic members such as BAK, BAX, BIM, and NOXA. In addition, our results demonstrated that S63845-induced cell death was linked with activation of caspase-3 and PARP cleavage in both BCP-ALL cell lines. Merino et al., reported that BAK/BAX are needed for the initiation of apoptosis by S63845 in breast cancer cells. They indicated that BAK/BAX knockdown impaired the S63845 cytotoxic effect on triple-negative breast cancer cells [33]. Merino et al., showed that S63845 disrupted MCL-1 complexes with NOXA, PUMA, BIM, and BID. However, down-regulation of BID and BIM induced a partial resistance to S63745 but, simultaneous targeting of BID, BIM, and PUMA significantly impaired S63845-induced cell death [33]. Our results demonstrated that pro-apoptotic BAX, BAK, and NOXA gene expression were up-regulated upon S63845 treatment in both BCP-ALL cell lines. However, our results demonstrated that the S63845 treatment did not affect BCL-xL and BCL-2 gene expression levels. Our findings are consistent with the results of the study conducted by Li et al., who showed that S63845 treatment had little effect on BCL-2 and BCL-XL expression in a panel of T-ALL cell lines [26]. In addition, our results demonstrated that MCL-1 mRNA and protein expression levels augmented in response to sole treatment with S63845 in both BCP-ALL cell lines. Li et al. did not report any correlation between MCL-1 protein levels and sensitivity to S63845 in these T-ALL cell lines. Furthermore, they expressed that, BCL-2 and BCL-XL levels could not predict response to S63845 treatment [26]. They declared that protein expression levels of Mcl-1 and Bcl-2 were compensatorily up-regulated after the S63845 treatment. Also, an experiment conducted by Andreeff et al., revealed that mRNA expression of BCL-2, BAX, and NOXA did not significantly modulate in presence of MCL-1 inhibitor in AML cell lines [34]. However, in our study, the expression level of BAX was significantly elevated in BCP-ALL cell lines. Powell et al., stated that S63845 binds and inhibits MCL-1 leading to free Noxa and Bim to inhibit other anti-apoptotic BCL-2 family members to initiate apoptosis [35]. So, it can be interpreted that, S63845 inhibits the function of Mcl-1, and up-regulation of MCL-1 mRNA and protein is a compensatory feedback response to maintain the leukemic cell survival. Our results demonstrated that treatment of BCP-ALL cells with S63845 initiates apoptosis through up-regulation of pro-apoptotic Bcl-2 members and cleavage and activation of caspase-3 and PARP that accounts for a hallmark of apoptosis. On the other hand, the adverse effects of chemotherapeutic agents or induction of secondary malignancies are undeniable side effects of non-specific chemotherapeutic [36]. Leading studies are concentrated on developing targeted therapy for the treatment of acute lymphoblastic leukemia [37]. Therefore, to realize whether the combination of the MCL-1 inhibitor with another common chemotherapeutic can enhance cancer cell elimination, we used S63845 in combination with doxorubicin in BCP-ALL derived cell lines, NALM-6, and SUP-B15. In the present study, we found that MCL-1 inhibitor, S63845 increased the susceptibility of NALM-6 and SUP-B15 cell lines to doxorubicin-induced apoptosis. Either S63845 or doxorubicin alone suppresses the growth of both BCP-ALL cell lines while their combination resulted in massive cell growth inhibition and apoptosis induction. Our results demonstrated that combination treatment of cells with both S63845 and doxorubicin causes caspase-dependent apoptosis and up-regulation of BAX mRNA levels in both BCP-ALL cell lines. Previous study claimed that, tumor cells driven by c-MYC overexpression are highly dependent on MCL-1 for their survival and S63845 induces a dose-dependent apoptosis in these group of malignancies [38]. Therefore, we analyzed the expression of c-Myc and its downstream target hTERT in our study. We figured out that mRNA and protein expression levels of c-Myc were down-regulated in combination treatment in comparison with either agent alone. However, co-treatment of cells with S63845 and doxorubicin did not exert tremendous effect on hTERT downregulation compared with either agent alone.
Conclusions
The results of the present study provide evidence for the first time that, Mcl-1 inhibitor, S63845 exerts a dose-dependent anti-proliferative effect on BCP-ALL cells and acts synergically with doxorubicin to induce caspase-dependent apoptosis. Therefore, targeting MCL-1 solely or in combination with chemotherapeutic drugs is considered a promising therapeutic strategy for BCP-ALL. However, further evaluations are requisite to explicate the exact mechanism of action of S63845 and its interaction with chemotherapeutic agents in BCP-ALL cells.
Abbreviations
- S:
-
S63845 (Mcl-1 inhibitor)
- Dox:
-
Doxorubicin
- qRT-PCR:
-
Quantitative-real time polymerase chain reaction
References
Aldoss IT, Marcucci G, Pullarkat V (2016) Treatment of acute lymphoblastic leukemia in adults: applying lessons learned in children. Oncology. https://doi.org/10.1007/s12032-009-9347-0
Hunger SP, Mullighan CG (2015) Acute lymphoblastic leukemia in children. New Engl J Med 373:1541–1552. https://doi.org/10.1056/NEJMra1400972
Schroeder MP, Bastian L, Eckert C, Gökbuget N, James AR, Tanchez JO, Schlee C, Isaakidis K, Häupl B, Baum K (2019) Integrated analysis of relapsed B-cell precursor Acute Lymphoblastic Leukemia identifies subtype-specific cytokine and metabolic signatures. Sci Rep 9:1–11. https://doi.org/10.1038/s41598-019-40786-1
Mullighan CG, the American Society of Hematology Education Program Book (2012) The molecular genetic makeup of acute lymphoblastic leukemia. Hematology 2010 2012:389–396. https://doi.org/10.1182/asheducation.V2012.1.389.3798360
Wong RS (2011) Apoptosis in cancer: from pathogenesis to treatment. J Exp Clin Cancer Res 30:87. https://doi.org/10.1186/1756-9966-30-87
Galluzzi L, Vitale I, Aaronson SA, Abrams JM, Adam D, Agostinis P, Alnemri ES, Altucci L, Amelio I, Andrews DW (2018) Molecular mechanisms of cell death: recommendations of the Nomenclature Committee on Cell Death 2018. Cell Death Differ 25:486–541. https://doi.org/10.1038/s41418-017-0012-4
Chen L, Zeng Y, Zhou S-F (2018) Role of apoptosis in cancer resistance to chemotherapy. Curr Underst Apoptosis Progr Cell Death. https://doi.org/10.5772/intechopen.80056
Youle RJ, Strasser A (2008) The BCL-2 protein family: opposing activities that mediate cell death. Nat Rev Mol Cell Biol 9:47–59. https://doi.org/10.1038/nrm2308
Akl H, Vervloessem T, Kiviluoto S, Bittremieux M, Parys JB, De Smedt H, Bultynck G (2014) A dual role for the anti-apoptotic Bcl-2 protein in cancer: mitochondria versus endoplasmic reticulum. Biochim Biophys Acta (BBA) Mol Cell Res 1843:2240–2252. https://doi.org/10.1016/j.bbamcr.2014.04.017
Kotschy A, Szlavik Z, Murray J, Davidson J, Maragno AL, Le Toumelin-Braizat G, Chanrion M, Kelly GL, Gong J-N, Moujalled DM (2016) The MCL1 inhibitor S63845 is tolerable and effective in diverse cancer models. Nature 538:477–482. https://doi.org/10.1038/nature19830
Heimer S, Knoll G, Schulze-Osthoff K, Ehrenschwender M (2019) Raptinal bypasses BAX, BAK, and BOK for mitochondrial outer membrane permeabilization and intrinsic apoptosis. Cell Death Dis 10:1–13. https://doi.org/10.1038/s41419-019-1790-z
Beroukhim R, Mermel CH, Porter D, Wei G, Raychaudhuri S, Donovan J, Barretina J, Boehm JS, Dobson J, Urashima M (2010) The landscape of somatic copy-number alteration across human cancers. Nature 463:899–905. https://doi.org/10.1038/nature08822
Wuilleme-Toumi S, Robillard N, Gomez P, Moreau P, Le Gouill S, Avet-Loiseau H, Harousseau J, Amiot M, Bataille R (2005) Mcl-1 is overexpressed in multiple myeloma and associated with relapse and shorter survival. Leukemia 19:1248–1252. https://doi.org/10.1038/sj.leu.2403784
Tron AE, Belmonte MA, Adam A, Aquila BM, Boise LH, Chiarparin E, Cidado J, Embrey KJ, Gangl E, Gibbons FD (2018) Discovery of Mcl-1-specific inhibitor AZD5991 and preclinical activity in multiple myeloma and acute myeloid leukemia. Nat Comm 9:1–14. https://doi.org/10.1038/s41467-018-07551-w
Glaser SP, Lee EF, Trounson E, Bouillet P, Wei A, Fairlie WD, Izon DJ, Zuber J, Rappaport AR, Herold MJ (2012) Anti-apoptotic Mcl-1 is essential for the development and sustained growth of acute myeloid leukemia. Gene Dev 26:120–125. https://doi.org/10.1101/gad.182980.111
Aichberger KJ, Mayerhofer M, Krauth M-T, Skvara H, Florian S, Sonneck K, Akgul C, Derdak S, Pickl WF, Wacheck V (2005) Identification of mcl-1 as a BCR/ABL-dependent target in chronic myeloid leukemia (CML): evidence for cooperative antileukemic effects of imatinib and mcl-1 antisense oligonucleotides. Blood 105:3303–3311. https://doi.org/10.1182/blood-2004-02-0749
Bolomsky A, Vogler M, Köse MC, Heckman CA, Ehx G, Ludwig H, Caers J (2020) MCL-1 inhibitors, fast-lane development of a new class of anti-cancer agents. J Hematol Oncol 13:1–19. https://doi.org/10.1186/s13045-020-01007-9
Koss B, Morrison J, Perciavalle RM, Singh H, Rehg JE, Williams RT, Opferman JT (2013) Requirement for antiapoptotic MCL-1 in the survival of BCR-ABL B-lineage acute lymphoblastic leukemia. Blood 122:1587–1598. https://doi.org/10.1182/blood-2012-06-440230
Kang MH, Wan Z, Kang YH, Sposto R, Reynolds CP (2008) Mechanism of synergy of N-(4-hydroxyphenyl) retinamide and ABT-737 in acute lymphoblastic leukemia cell lines: Mcl-1 inactivation. J Natl Canc Inst 100:580–595. https://doi.org/10.1093/jnci/djn076
Wang H, Guo M, Wei H, Chen Y (2021) Targeting MCL-1 in cancer: current status and perspectives. J Hematol Oncol 14:1–18. https://doi.org/10.1186/s13045-021-01079-1
Fletcher S (2019) MCL-1 inhibitors–where are we now (2019)? Expert Opin Ther Pat 29:909–919. https://doi.org/10.1080/13543776.2019.1672661
Alikarami F, Safa M, Faranoush M, Hayat P, Kazemi A (2017) Inhibition of DNA-PK enhances chemosensitivity of B-cell precursor acute lymphoblastic leukemia cells to doxorubicin. Biomed Pharmacother 94:1077–1093. https://doi.org/10.1016/j.biopha.2017.08.022
Sheikh-Zeineddini N, Bashash D, Safaroghli‐Azar A, Riyahi N, Shabestari RM, Janzamin E, Safa M (2019) Suppression of c‐Myc using 10058‐F4 exerts caspase‐3‐dependent apoptosis and intensifies the antileukemic effect of vincristine in pre‐B acute lymphoblastic leukemia cells. J Cell Biochem 120:14004–14016. https://doi.org/10.1002/jcb.28675
Shabestari RM, Safa M, Alikarami F, Banan M, Kazemi A (2017) CREB knockdown inhibits growth and induces apoptosis in human pre-B acute lymphoblastic leukemia cells through inhibition of prosurvival signals. Biomed Pharmacother 87:274–279. https://doi.org/10.1016/j.biopha.2016.12.070
Chou T-C (2010) Drug combination studies and their synergy quantification using the Chou-Talalay method. Cancer Res 70:440–446. https://doi.org/10.1158/0008-5472.CAN-09-1947
Li Z, He S, Look AT (2019) The MCL1-specific inhibitor S63845 acts synergistically with venetoclax/ABT-199 to induce apoptosis in T-cell acute lymphoblastic leukemia cells. Leukemia 33:262–266. https://doi.org/10.1038/s41375-018-0201-2
Brenner D, Mak TW (2009) Mitochondrial cell death effectors. Curr Opin Cell Biol 21:871–877. https://doi.org/10.1016/j.ceb.2009.09.004
Bhutani M, Kumar L, Vora A, Bhardwaj N, Pathak AK, Singh R, Kochupillai V (2002) Randomized study comparing 4′-epi‐doxorubicin (Epirubicin) versus doxorubicin as a part of induction treatment in adult acute lymphoblastic leukemia. Am J Hematol 71:241–247. https://doi.org/10.1002/ajh.10211
Pugazhendhi A, Edison TNJI, Velmurugan BK, Jacob JA, Karuppusamy I (2018) Toxicity of Doxorubicin (Dox) to different experimental organ systems. Life Sci 200:26–30. https://doi.org/10.1016/j.lfs.2018.03.023
Grabow S, Kelly G, Delbridge A, Kelly P, Bouillet P, Adams J, Strasser A (2016) Critical B-lymphoid cell intrinsic role of endogenous MCL-1 in c-MYC-induced lymphomagenesis. Cell Death Dis 7:e2132–e2132. https://doi.org/10.1038/cddis.2016.43
Fernald K, Kurokawa M (2013) Evading apoptosis in cancer. Trends Cell Biol 23:620–633. https://doi.org/10.1016/j.tcb.2013.07.006
Quinn BA, Dash R, Azab B, Sarkar S, Das SK, Kumar S, Oyesanya RA, Dasgupta S, Dent P, Grant S (2011) Targeting Mcl-1 for the therapy of cancer. Expet Opin Investig Drugs 20:1397–1411. https://doi.org/10.1517/13543784.2011.609167
Merino D, Whittle JR, Vaillant F, Serrano A, Gong J-N, Giner G, Maragno AL, Chanrion M, Schneider E, Pal B (2017) Synergistic action of the MCL-1 inhibitor S63845 with current therapies in preclinical models of triple-negative and HER2-amplified breast cancer. Sci Transl Med 9:eaam7049. https://doi.org/10.1126/scitranslmed.aam7049
Pan R, Ruvolo VR, Wei J, Konopleva M, Reed JC, Pellecchia M, Andreeff M, Ruvolo PP (2015) Inhibition of Mcl-1 with the pan–Bcl-2 family inhibitor (–) BI97D6 overcomes ABT-737 resistance in acute myeloid leukemia. Blood 126:363–372. https://doi.org/10.1182/blood-2014-10-604975
Powell JA, Lewis AC, Pitson SM (2017) The MCL-1 inhibitor S63845: an exciting new addition to the armoury of anti-cancer agents. J Xiangya Med 2:1–4
Carr C, Ng J, Wigmore T (2008) The side effects of chemotherapeutic agents. Curr Anaesth Crit Care 19:70–79. https://doi.org/10.1016/j.cacc.2008.01.004
Banerjee S, Li Y, Wang Z, Sarkar FH (2008) Multi-targeted therapy of cancer by genistein. Canc Lett 269:226–242. https://doi.org/10.1016/j.canlet.2008.03.052
Thijssen R, Alvarez-Diaz S, Grace C, Gao M-y, Segal DH, Xu Z, Strasser A, Huang DC (2020) Loss of RIPK3 does not impact MYC-driven lymphomagenesis or chemotherapeutic drug-induced killing of malignant lymphoma cells. Cell Death Differ 27:2531. https://doi.org/10.1038/s41418-020-0576-2
Acknowledgements
This study was derived from the thesis of E Ebrahimi and supported by a grant from Iran University of Medical Science.
Funding
This work was supported by the Grant No. 32662 from Iran University of Medical Sciences.
Author information
Authors and Affiliations
Contributions
MS conceived and designed the research. EEB and RMS conducted the experiment. MS and DB contributed reagent or analytical tools. MS, RMS and DB analyzed data. EEB and RMS wrote the manuscript. MS, DB and RMS revised the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
Elham Ebrahimi, Rima Manafi Shabestari, Davood Bashash, and Majid Safa declares that they have no conflict of interest.
Ethical approval
The procedure performed in present study involving human participants was in accordance with the ethical standards of the Medical Ethic Committee of Iran university of medical science and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all patients and healthy donors included in the study. All authors involved in this study are agree to publish the manuscript in your worthy journal.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
11033_2021_7021_MOESM1_ESM.tif
Supplementary Fig. 1 (a) NALM-6 and (b) SUP-B15 cells were treated with elevating concentrations of S63845 for 24 and 48 hr and cell viability was evaluated with trypan blue method. Dose-effect curve of diverse doses of S63845 in (c) NALM-6 and (d) SUP-B15 cells was measured using MTT assay and expressed using compusyn software. Supplementary material 1 (TIF 302.5 kb)
11033_2021_7021_MOESM2_ESM.tif
Supplementary Fig. 2 The apoptotic cell graphs for NALM-6 (a) and SUP-B15 cells (b) assessed by flowcytometery. Following the treatment of (c) NALM-6 and (d) SUP-B15 cells with mentioned doses of S63845 for 24 hr, caspase-3 activity assay was performed using a colorimetric caspase-3 kit (n=3, *P<0.05, **P<0.01, compared to control cells). Supplementary material 2 (TIF 395.6 kb)
11033_2021_7021_MOESM3_ESM.tif
Supplementary Fig. 3 (a) NALM-6 and (b) SUP-B15 cells were treated with diverse concentrations of doxorubicin and metabolic activity of cells was measured using MTT assay. The Dose-effect curve of different concentrations of Doxorubicin in was depicted using compusyn software. Supplementary material 3 (TIF 151.8 kb)
11033_2021_7021_MOESM4_ESM.tif
Supplementary Fig. 4 (a) NALM-6 cells were incubated with 500 nM concentrations of S63845 in the presence or absence of 200 nM doxorubicin for 24 hr. (b) SUP-B15 cells were cultured in medium containing 60 nM S63845 either with or without 20 nM doxorubicin for 24 hr. Total RNA was extracted and cDNA was prepared. BAX and BCL-2 mRNA expression levels were measured by quantitative reverse transcription polymerase chain reaction (qRT-PCR) and normalized to the expression of ACTIN (n=3, *P<0.05, **P<0.01 compared to Dox treated cells). Supplementary material 4 (TIF 181.2 kb)
11033_2021_7021_MOESM5_ESM.tif
Supplementary Fig. 5 (a) NALM-6 cells and (b) SUP-B15 cells were treated with indicated doses of MCL-1 S63845 and doxorubicin for 24 hr. Following extraction of total RNA and cDNA preparation, gene expression of C-MYC, hTERT, and MCL-1 was measured by qRT-PCR. All values were normalized to ACTIN. (n=3; *p<0.05, compared to cells treated with doxorubicin alone). Supplementary material 5 (TIF 296.1 kb)
11033_2021_7021_MOESM6_ESM.tif
Supplementary Fig. 6 Mononuclear cells from healthy donors (a) and patients with BCP-ALL (b) were treated with doxorubicin in present or absence of S63845 for 24hr. (*p<0.05, compared to cells treated with doxorubicin alone). Supplementary material 6 (TIF 1394.3 kb)
Rights and permissions
About this article
Cite this article
Ebrahimi, E., Shabestari, R.M., Bashash, D. et al. Synergistic apoptotic effect of Mcl-1 inhibition and doxorubicin on B-cell precursor acute lymphoblastic leukemia cells. Mol Biol Rep 49, 2025–2036 (2022). https://doi.org/10.1007/s11033-021-07021-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11033-021-07021-5