Abstract
Neurotrophic factors are well-known to be involved in the pathophysiology of depression and treatment of antidepressants. Brain-derived neurotrophic factor (BDNF), one of the most widely distributed and the most highly studied neurotrophic factors, has been demonstrated to play an important role in the pathophysiology of depression and the mechanism of antidepressants. According to the previous studies, we found that animal tissues were dissected for BDNF measurement mainly in daytime. Considering the circadian rhythm of BDNF expression, our present study evaluated the circadian variations in behaviors, serum corticosterone concentrations, hippocampal BDNF expression and neuronal cell proliferation in mice exposed to chronic mild stress (CMS), one of the most widely used depression-like animal models. Our results provided the first evidence that the difference of BDNF expression and neuronal cell proliferation between CMS and control mice underwent an oscillation related to the circadian variations (maximum at 20:00 h, minimum at 12:00 h or 16:00 h), while the difference of sucrose preference and first feeding latency was not affected by circadian rhythm. This oscillation difference was attributed to the relative constant BDNF expression and cell proliferation in CMS mice and the fluctuating BDNF expression and cell proliferation in control mice. CMS exposure might destroy the circadian rhythm of BDNF expression and cell proliferation in hippocampus of normal individual. Our present study suggests that animal decapitation at 20:00 h is the best time for BDNF-related measurement in CMS experiment, since the difference reaches the maximum.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Chronic mild stress (CMS), a depression-like animal model introduced by Katz and subsequently developed by Willner, is widely used for studying the pathophysiology of depression and the mechanism of antidepressants in lab (Katz et al. 1981; Willner et al. 1987). CMS mimics depression in a naturalistic way of socio-environmental stressors, involves the exposure of animals to a series of mild and unpredictable stressors during several weeks and results in a variety of behavioral, neurochemical, neuroendocrine, neuroimmune and neurotrophic alterations resembling some of the dysfunctions observed in depressed patients. Most abnormal effects of CMS can be reversed by antidepressant treatments, suggesting a strong predictive validity (Zhang et al. 2010).
Brain-derived neurotrophic factor (BDNF), which is present in high concentration in the hippocampus, plays an important role in the maintenance and survival of neurons and in synaptic plasticity. It promotes differentiation of neurons from stem cells, enhances neurite outgrowth and synaptogenesis, and prevents programmed cell death (Marosi and Mattson 2014). Clinical evidence suggests that regulation of BDNF expression and function in hippocampus could contribute to the pathophysiology and treatment of depression (Shirayama et al. 2002). Animal studies indicate that stress reduces BDNF expression or activity in the hippocampus and that this reduction can be prevented by treatment with antidepressant drugs (Yi et al. 2014). As a result, a growing number of studies evaluated the effects of CMS on the hippocampal BDNF levels.
Circadian rhythm, a powerful feature of the animal body, plays an important role in nervous regulation and reflects some degree of organization in the biological clock (Robillard et al. 2014). Time of day affects memory, executive function and attention in brain (Duncan and Northoff 2013). Evidence suggests that major depression has been linked to circadian rhythms alterations (Monteleone et al. 2011; Comai and Gobbi 2014). In addition, circadian rhythm controlled the BDNF expression in hippocampus in animals (Bova et al. 1998; Schaaf et al. 2000). However, according to the published reports, CMS animals were sacrificed mainly in the daytime especially at noon (Chandran et al. 2013; Liu et al. 2014). The circadian variations in BDNF levels of CMS animals remain unknown. Therefore, we hypothesized that the difference of BDNF levels between CMS animals and control animals displayed a circadian rhythm and thereby induced circadian changes in the cell proliferation. To investigate this, the hippocampal BDNF mRNA and protein levels were measured at different time points. In addition, we also measured the hippocampal cell proliferation at these time points.
Materials and methods
Animals
Male ICR mice (24 ± 2 g; 5 weeks old) were purchased from Shanghai Slac Animal Center, PR China. Eight animals were housed per cage (320 × 180 × 160 mm) with a normal 12-h/12-h light/dark schedule with the lights on at 07:00 a.m. (Circadian Time CT 0). The animals were allowed one week to acclimatize themselves to the housing conditions before the beginning of the experiments. Ambient temperature and relative humidity were maintained at 22 ± 2 °C and at 55 ± 5 %, respectively, and the animals were given standard chow and water ad libitum for the duration of the study. All procedures were approved by the Ethics Committee and performed in accordance with the published guidelines of the China Council on Animal Care (Regulations for the Administration of Affairs Concerning Experimental Animals, approved by the State Council on 31 October, 1988 and promulgated by Decree No. 2 of the State Science and Technology Commission on 14 November, 1988).
CMS procedure
The procedure of CMS was performed as described previously (Yi et al. 2014). Briefly, the weekly stress regime consisted of food and water deprivation, exposure to an empty bottle, exposure to a soiled cage, light/dark succession every 2 h, space reduction, 45° cage tilt, overnight illumination, and predator sounds (Table 1). All stressors were applied individually and continuously both day and night. The control animals were housed in a separate room and had no contact with the stressed groups. To prevent habituation and ensure the unpredictability of the stressors, all of the stressors were randomly scheduled over a one-week period and were repeated throughout the five-week experiment. Body weights of all animals were measured every week.
Sucrose preference test (SPT)
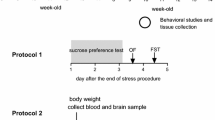
The SPT was conducted at the end of 5-week CMS exposure. Briefly, before the test, the mice were trained to adapt to sucrose solution (1 %, w/v): two bottles of sucrose solution were placed in each cage for 24 h, and then one bottle of sucrose solution was replaced with water for 24 h. After the adaptation, the mice were deprived of water and food for 24 h. The test was conducted at CT 1 (8:00 h), CT 5 (12:00 h), CT 9 (16:00 h), CT 13 (20:00 h), CT 17 (24:00 h) and CT 21 (4:00 h), in which the mice were housed in individual cages and had free access to two bottles containing sucrose solution and water, respectively. After 24 h, the volumes of the consumed sucrose solution and water were recorded.
Novelty-suppressed feeding test (NSFT)
The NSFT was conducted 24 h after the SPT. The NSFT was performed during an 8-min period as previously described (Yi et al. 2014). Briefly, the testing apparatus consisted of a plastic box (50 × 50 × 20 cm). Food was withheld from the mice for 24 h before the test. At the beginning of the test, a single pellet of food was placed on a white paper platform positioned at the center of the box. A mouse was placed in a corner of the maze and a stopwatch was immediately started. The scoring to measure the interest did not begin until the mouse reached for the food with its forepaws and began eating. The home-cage food consumption within 15 min was measured immediately following the test as a control value.
Serum and tissue sample collection
Twenty-four hours after completion of the NSFT, six mice per group were sacrificed by decapitation at different circadian time points CT 1 (8:00 h), CT 5 (12:00 h), CT 9 (16:00 h), CT 13 (20:00 h), CT 17 (24:00 h) and CT 21 (4:00 h), respectively. Blood was collected on ice and separated in a refrigerated centrifuge at 4 °C. Serum was stored at −20 °C until assays were performed. Whole brains were rapidly removed from mice and chilled in an ice-cold saline solution. Whole hippocampus was dissected on a cold plate and frozen in liquid nitrogen immediately. The tissue samples were stored at −80 °C until assay.
Serum corticosterone assay
Serum corticosterone levels were measured using an enzyme immunoassay kit (Enzo Life Sciences, USA).
Real-time RT-PCR
Total RNA was isolated from the hippocampus using Trizol reagent following the manufacturer’s instructions. Reverse transcription was performed using M-MLV reverse transcriptase for cDNA synthesis. Real-time PCR reactions were performed using a SYBR Premix Ex Taq Kit in ABI-7500 system. The BDNF (forward 5′-TTATTTCATACTTCGGTTGC-3′; reverse 5′-TGTCAGCCAGTGATGTCG-3′) and the internal control GAPDH (forward 5′-GGGTGTGAACCACGAGAAAT-3′; reverse 5′-GGAAGAATGGGAGTTGCTGT-3′) primers were used. The fluorescence signal was detected at the end of each cycle. Melting curve analysis was used to confirm the specificity of the products. The results were analyzed by the 2−ΔΔCT method. The results were normalized to the mRNA expression level of GAPDH in each sample.
BDNF ELISA
Brain samples were homogenized in lysis buffer containing 137 mM NaCl, 20 mM Tris–HCl (pH 8.0), 1 % Tergitol-type NP-40, 10 % glycerol, 1 mM phenylmethanesulfonyl fluoride, 10 μg/ml aprotinin, 1 μg/ml leupeptin, 0.5 mM sodium vanadate. The homogenate was centrifugated at 16,000×g for 30 min at 4 °C, and the supernatant was collected and stored at −80 °C until assay.
Protein levels of samples were measured using the Lowry Method. BDNF protein was measured using BDNF ELISA kit (Boster, P.R. China) according to the protocol of the manufacturer.
Brain extraction and immunohistochemistry
For analysis of hippocampal cell proliferation, four mice per group were injected with BrdU (50 mg/kg, twice per day for two successive days). At 24 h after the last BrdU injection, the mice were immediately anesthetized with chloral hydrate (0.35 g/kg) and then sacrificed by intracardial perfusion with heparinized 0.9 % saline followed by ice-cold 4 % paraformaldehyde at different circadian time points CT 1 (8:00 h), CT 7 (14:00 h), CT 13 (20:00 h) and CT 19 (2:00 h), respectively. The brains were removed and postfixed with 4 % paraformaldehyde overnight and incubated with 30 % sucrose solution in PBS at 4 °C for 2 days.
To determine the number of BrdU-incorporated cells in the hippocampus, six coronal sections (40 μm) were randomly selected throughout the hippocampus between 1.70 and 2.57 mm posterior to the bregma, as defined in the mouse brain atlas, and the sections were analyzed by immunohistochemistry. Free-floating brain sections were incubated for 15 min in 0.3 % H2O2 at room temperature to eliminate endogenous peroxidase. To detect BrdU-incorporated cells, the free-floating sections were rinsed extensively with PBS (0.05 M), and the sections were incubated for 30 min in HCl at 37 °C to denature the DNA. The sections were neutralized by incubating them for 10 min in borate buffer. Then, the anti-BrdU antibody was used as a primary antibody (1:5000) overnight at room temperature. Subsequently, the sections were intermittently rinsed with PBS and incubated with a biotinylated anti-rat IgG secondary antibody (1:200) followed by ABC complex (1:100) for 1 h at room temperature. BrdU-incorporated cells were visualized with 0.02 % 3,3’-diaminobenzidine tetrahydrochloride and 0.01 % hydrogen peroxide in 0.05 M PBS for approximately 3 min. The total number of BrdU-labelled cells per section was determined and added to obtain the total number of cells per animal.
Statistical analyses
All data are expressed as mean ± S.E.M. Data was analyzed using a two-way analysis of variance (ANOVA) followed by Bonferroni’s post-hoc test. A value of P < 0.05 was considered statistically significant for analysis.
Results
Body weight during the CMS procedure
As illustrated in Table 2, the body weight of animals between control and CMS did not have a significant difference at the beginning. A repeated ANOVA showed that during the 5-week experiment period, body weight during the whole experiment showed a continual increase [F (5,410) = 607.30, P < 0.01], and the CMS also reduced the body weight of animals [F (5,82) = 106.68, P < 0.01]. In a separate one-way ANOVA, the body weight of CMS mice was significantly lower than that of control mice from week 1 to week 5 [Week 1: F (1,83) = 6.72, P < 0.05; Week 2: F (1,83) = 78.30, P < 0.01; Week 3: F (1,83) = 82.62, P < 0.01; Week 4: F (1,83) = 99.82, P < 0.01; Week 5: F (1,83) = 120.53, P < 0.01; respectively].
The circadian variations in behaviors of CMS mice
The effects of CMS at different CT on sucrose preference were shown in Fig. 1. Two-way ANOVA indicated that only stress effect [F (1,108) = 33.71, P < 0.001] was significant on the sucrose preference. However, time effect [F (5,108) = 0.19, P > 0.05] and stress × time interaction [F (5,108) = 0.06, P > 0.05] did not reach a statistic significance. In addition, we did not detect any significant difference between any time points according to the post hoc test.
The effects of CMS at different CT on first feeding latency were shown in Fig. 2. Two-way ANOVA indicated that only stress effect [F (1,108) = 37.42, P < 0.001] was significant on the first feeding latency. However, time effect [F (5,108) = 0.61, P > 0.05] and stress × time interaction [F (5,108) = 0.04, P > 0.05] did not reach a statistic significance. In addition, a non-significant difference between any time points was shown according to the post hoc test.
On the other hand, there was no difference in the home-cage feed consumption conducted immediately following the NSFT (Data not shown), indicating that the effects were not due to a general increase in feeding.
The circadian variations in the serum corticosterone concentrations of CMS mice
The effects of CMS at different CT on the serum corticosterone concentrations are shown in Fig. 3. Two-way ANOVA revealed a significant stress effect [F (1,72) = 52.61, P < 0.001], a significant time effect [F (5, 72) = 3.85, P < 0.01] but not stress × time interaction [F (5, 72) = 0.38, P > 0.05] on the serum corticosterone concentrations. The minimum difference was observed at CT 17 (24:00 h), and the maximum difference was observed at CT 1 (8:00 h). Post hoc test showed that the serum corticosterone concentrations at CT 13 [P < 0.01] and CT 17 [P < 0.05] was significantly increased as compared with that at CT 1 in control animals.
The circadian variations in hippocampal BDNF expression of CMS mice
The effects of CMS at different CT on hippocampal BDNF mRNA expression were shown in Fig. 4. Two-way ANOVA revealed a significant stress effect [F (1,36) = 139.40, P < 0.001], a significant time effect [F (5,36) = 10.80, P < 0.001] and stress × time interaction [F (5,36) = 6.77, P < 0.001] on BDNF mRNA expression. The minimum difference was observed at CT 9 (16:00 h), and the maximum difference was observed at CT 13 (20:00 h). Post hoc test showed that the BDNF mRNA expression at CT 13 [P < 0.001] and CT 17 [P < 0.01] was significantly increased as compared with that at CT 9 in control animals. In addition, BDNF mRNA expression at CT 13 [P < 0.001] and CT 17 [P < 0.01] was significantly increased as compared with that at CT 5.
Two-way ANOVA revealed a significant stress effect [F (1,60) = 133.69, P < 0.001] and a significant time effect [F (5,60) = 3.65, P < 0.01] on the BDNF protein levels (Fig. 5). However, stress × time interaction [F (5,60) = 2.14, P = 0.073] did not reach a significant level. The minimum difference was observed at CT 5 (12:00 h), and the maximum difference was observed at CT 13 (20:00 h). Post hoc test showed that the BDNF protein levels at CT 13 [P < 0.01] was significantly increased as compared with that at CT 5 in control animals.
The circadian variations in hippocampal cell proliferation of CMS mice
The effects of CMS at different CT on hippocampal cell proliferation were shown in Fig. 6. Two-way ANOVA revealed a significant stress effect [F (1,36) = 243.03, P < 0.001], a significant time effect [F (5,36) = 27.70, P < 0.001] and stress × time interaction [F (5,36) = 10.00, P < 0.001] on cell proliferation. The minimum difference was observed at CT 9 (16:00 h), and the maximum difference was observed at CT 13 (20:00 h). Post hoc test showed that the cell proliferation at CT 13 [P < 0.001], CT 17 [P < 0.001] and CT 21 [P < 0.01] was significantly increased as compared with that at CT 9 in control animals. In addition, cell proliferation at CT 13 [P < 0.001], CT 17 [P < 0.001] and CT 21 [P < 0.001] was significantly increased as compared with that at CT 5.
Discussion
In the present study, we provide the first evidence that, the difference of BDNF expression and neuronal cell proliferation between CMS and control mice undergoes an oscillation related to the circadian variations. However, the difference of behaviors is not affected by circadian rhythm.
While comparing body weight from the beginning to the end of the stress procedure, we observed that the body weight of CMS mice was significantly lower than that of control mice from week 1 to week 5. This phenomenon was also found in other studies that CMS caused a reduction in body weight (Schweizer et al. 2009; Nollet et al. 2011). However, it should be noted that all the animals maintain a body weight gain during the five-week CMS procedure.
As a widely used model for researching and developing antidepressants (Willner 1997), the sucrose preference reduction, a measurement index of the CMS procedure, which reflects a state of anhedonia to produce a condition similar to human depression, can be restored by therapeutically effective drugs for the treatment of depression. The present results showed that a reduction of sucrose preference was induced by CMS procedure. However, no circadian variation in the difference of sucrose preference between CMS and control mice was observed. A similar study reported by Willner group also found that the difference of sucrose preference between CMS and control rats tended to be same between light phase and dark phase after 4 weeks’ CMS procedure (D’Aquila et al. 1997). In this case, our present study further supported their conclusion and demonstrated that the difference of sucrose preference was equal at any time point.
Considering that depression displays high comorbidity with anxiety and cognitive disorders (Bessa et al. 2009), we tested the first feeding latency of mice, an indication of increased anxiety levels in NSFT. In parallel with the sucrose preference, although the prolonged first feeding latency was induced by CMS, the difference of first feeding latency between CMS and control mice remained unchanged. Thus, our present study indicates that the behaviors in CMS are not affected by circadian variations.
The CMS model causes not only behavioral dysfunctions, but also elicits neuroendocrine alterations in animals resembling several dysfunctions observed in depressed patients. Serum corticosterone is considered the main glucocorticoid involved in regulation of stress responses in rodents. Growing evidence suggests that CMS destroys the feedback of the hypothalamic–pituitary–adrenal axis, and shows a significant increase of corticosterone (Pan et al. 2010; Christiansen et al. 2012). We found that CMS mice maintained higher concentrations of serum corticosterone. In contrast, the serum corticosterone concentrations in control mice showed a circadian rhythm related oscillation. The maximum difference appeared in the light phase, while the minimum difference appeared in the dark phase. The difference change was consistent with previous studies (Ushijima et al. 2006; Toth et al. 2008).
Although clinical and experimental studies were providing some insights into the pathophysiological processes that may occur in depression, recent analyses indicated that approximately 30 % of depressive patients failed to respond satisfactorily to commercially available monoaminergic antidepressants (Papakostas et al. 2008). Therefore, besides the monoamine hypothesis of depression, neurotrophic hypothesis is proposed and accepted by most of researchers. One of the most widely distributed and the most highly studied neurotrophic factors is BDNF. The neurotrophic hypothesis has been tested using various strategies for over-expression or knockdown of BDNF (Duman and Li 2012). Although there are some limitations, the results are consistent with the hypothesis that down-regulation of BDNF contributes to depression and that up-regulation of BDNF plays a role in the actions of antidepressant treatment (Duman and Monteggia 2006). Moreover, since a delayed onset of antidepressant action is parallel with the delayed up-regulation of BDNF, BDNF may be used to monitor the onset of therapeutic action. Accordingly, there is an abundance of research that has examined the effects of CMS and antidepressants on BDNF expression (Hill et al. 2012).
Based on the previous published reports, we found that most of CMS animals were sacrificed and brain tissues were dissected in the daytime especially at noon (CT 5, 12:00 h). In this way, the BDNF levels were merely measured at CT 5 in these studies. In addition, the difference of BDNF levels between CMS and control animals did not reach a significance level in some reports. The non-significant difference finally resulted in a failure of antidepressant evaluation. Therefore, we hypothesized that the difference may be significant at other time points. In other words, it may be easy to obtain the difference of BDNF levels between CMS and control at other CT. Considering that a high significance of BDNF difference is benefit for the antidepressant evaluation, it is necessary to measure BDNF levels at different time points.
In contrast to the constant difference of behaviors between CMS and control mice, an oscillation of BDNF mRNA and protein levels during the 24-h period was observed in the hippocampus. The results indicated that the circadian rhythm of BDNF expression in control mice was statistically significant. However, CMS mice did not exhibit a significant oscillation of the BDNF levels. As a result, we found that the maximum difference of BDNF expression between CMS and control mice occurred at CT 13 (20:00 h); while the difference reached a minimum at CT 5 (12:00 h) or CT 9 (16:00 h).
It is well accepted that neuronal cell proliferation is regulated by BDNF (Hill et al. 2012). Knocking-out BDNF gene or blockade of BDNF receptor tyrosine receptor kinase B (TrkB) is reported to inhibit the cell proliferation in hippocampus. Thus, CMS decreases and antidepressant treatment increases the expression of BDNF, which in turn contributes to the regulation of cell proliferation (Duman and Li 2012). To understand whether circadian variations in BDNF affect the cell proliferation in a circadian rhythm way, we also assessed the hippocampal cell proliferation at different time points. Consistent with the circadian variations in BDNF expression, the difference of proliferation between CMS and control mice displays an oscillation during the day. Additionally, the change of control mice parallels the findings seen in a recent study (Bouchard-Cannon et al. 2013). The difference was also shown the maximum at CT 13 (20:00 h) and minimum at CT 9 (16:00 h). Similarly, this oscillation was attributed to the constant proliferation of CMS and various proliferation of control, which were mediated by distinguishing BDNF-TrkB signaling conduction regulation.
Our results showed that the circadian variations in the hippocampal BDNF expression and cell proliferation could be observed in control mice but not in CMS mice, this observation strongly suggested that the CMS exposure might destroy the circadian rhythm of BDNF expression and cell proliferation in hippocampus of normal individual. This point was similar to a previous study which evaluated whether vitamin A deficiency affected circadian rhythmicity of retinoic acid nuclear receptors in the hippocampus (Navigatore-Fonzo et al. 2013). They found that vitamin A deficiency phase shifted the circadian rhythmicity of retinoic acid nuclear receptors expression, and abolished the circadian expression of a clock gene, PER1. In addition, previous study showed N-acetylserotonin, a TrkB agonist, activated BDNF-TrkB signaling in a circadian rhythm and displayed antidepressant-like effect (Jang et al. 2010). They found that TrkB receptor was activated higher at night and lower during the day. In addition, another previous study found TrkB is crucial in gating the circadian auditory clock to sound. Therefore, lack of BDNF expression after night noise resulted in the increased possibility of hearing loss. In contrast, TrkB agonist can recover brain activity after noise overexposure (Meltser et al. 2014). These results indicated that stress affected the circadian rhythm of BDNF expression, and the TrkB agonist can serve as a potential drug for the stress related disease. In this way, we speculated that antidepressant-like agents also induced BDNF-TrkB signaling in a circadian rhythm, and extensively normalized the signaling at night rather than in the daytime.
Furthermore, the most striking feature of our present study is the fact that we provide a best time point (CT 13, 20:00 h) for the BDNF measurement in the further research. First of all, due to the discrepancy (such as strains of animals, experimental conditions and stressed time) in the procedure of the CMS establishment, some studies did not obtain a result of BDNF reduction in animals exposed to CMS (Allaman et al. 2008; Fortunato et al. 2010). Therefore, if the animals were killed at the suggested CT 13, a significant reduction of BDNF expression in hippocampus might be observed. Additionally, several studies reported that some antidepressant agents improved the sucrose preference of animals in CMS (Hansson et al. 2011; Reus et al. 2012), however, the agents did not reverse the reduction of BDNF expression in hippocampus. Although it cannot be denied the fact that the antidepressant-like effect of some agents is mediated by a BDNF independent mechanism (Lindholm et al. 2012), at least we should consider another possibility that a longer treatment period or a higher dose is required for BDNF up-regulation. In such case, if we measured the BDNF expression at CT 13 instead of daytime, the antidepressant treatment duration might be shortened, or the dose might be lowered.
On the other hand, it should be noted that the neuronal nuclear antigen such as NeuN was not labeled in our present study, so that we cannot distinguish whether cell proliferation was occurring in neuronal precursors or in astroglia. This is one of the limitations of the present study.
Conclusion
These studies can be viewed as preliminary yet useful, demonstrating the potential circadian variations in BDNF in a widely used depression-like model. The relative constant BDNF expression in CMS and fluctuating BDNF expression in control contribute to the oscillation difference between CMS and control mice. The best time for BDNF and cell proliferation measurement in CMS study is CT 13 (20:00 h), since the difference reach the maximum. On the other hand, it should be noted that mice are nocturnal creature and therefore they remain active during the night. In this way, the unaffected behaviors by circadian rhythm may be attributed to this feature. More research will need to be further conducted in order to more fully understand what exact mechanism of the variations is and whether BDNF circadian variations are regulated by circadian gene.
References
Allaman I, Papp M, Kraftsik R, Fiumelli H, Magistretti PJ, Martin JL (2008) Expression of brain-derived neurotrophic factor is not modulated by chronic mild stress in the rat hippocampus and amygdala. Pharmacol Rep 60:1001–1007
Bessa JM, Mesquita AR, Oliveira M, Pego JM, Cerqueira JJ, Palha JA, Almeida OF, Sousa N (2009) A trans-dimensional approach to the behavioral aspects of depression. Front Behav Neurosci 3:1
Bouchard-Cannon P, Mendoza-Viveros L, Yuen A, Kaern M, Cheng HY (2013) The circadian molecular clock regulates adult hippocampal neurogenesis by controlling the timing of cell-cycle entry and exit. Cell Rep 5:961–973
Bova R, Micheli MR, Qualadrucci P, Zucconi GG (1998) BDNF and trkB mRNAs oscillate in rat brain during the light–dark cycle. Brain Res Mol Brain Res 57:321–324
Chandran A, Iyo AH, Jernigan CS, Legutko B, Austin MC, Karolewicz B (2013) Reduced phosphorylation of the mTOR signaling pathway components in the amygdala of rats exposed to chronic stress. Prog Neuropsychopharmacol Biol Psychiatry 40:240–245
Christiansen S, Bouzinova EV, Palme R, Wiborg O (2012) Circadian activity of the hypothalamic-pituitary-adrenal axis is differentially affected in the rat chronic mild stress model of depression. Stress 15:647–657
Comai S, Gobbi G (2014) Unveiling the role of melatonin MT2 receptors in sleep, anxiety and other neuropsychiatric diseases: a novel target in psychopharmacology. J Psychiatry Neurosci 39:6–21
D’Aquila PS, Newton J, Willner P (1997) Diurnal variation in the effect of chronic mild stress on sucrose intake and preference. Physiol Behav 62:421–426
Duman RS, Li N (2012) A neurotrophic hypothesis of depression: role of synaptogenesis in the actions of NMDA receptor antagonists. Philos Trans R Soc Lond B Biol Sci 367:2475–2484
Duman RS, Monteggia LM (2006) A neurotrophic model for stress-related mood disorders. Biol Psychiatry 59:1116–1127
Duncan NW, Northoff G (2013) Overview of potential procedural and participant-related confounds for neuroimaging of the resting state. J Psychiatry Neurosci 38:84–96
Fortunato JJ, Reus GZ, Kirsch TR, Stringari RB, Fries GR, Kapczinski F, Hallak JE, Zuardi AW, Crippa JA, Quevedo J (2010) Effects of beta-carboline harmine on behavioral and physiological parameters observed in the chronic mild stress model: further evidence of antidepressant properties. Brain Res Bull 81:491–496
Hansson AC, Rimondini R, Heilig M, Mathe AA, Sommer WH (2011) Dissociation of antidepressant-like activity of escitalopram and nortriptyline on behaviour and hippocampal BDNF expression in female rats. J Psychopharmacol 25:1378–1387
Hill MN, Hellemans KG, Verma P, Gorzalka BB, Weinberg J (2012) Neurobiology of chronic mild stress: parallels to major depression. Neurosci Biobehav Rev 36:2085–2117
Jang SW, Liu X, Pradoldej S, Tosini G, Chang Q, Iuvone PM, Ye K (2010) N-acetylserotonin activates TrkB receptor in a circadian rhythm. Proc Natl Acad Sci U S A 107:3876–3881
Lindholm JS, Autio H, Vesa L, Antila H, Lindemann L, Hoener MC, Skolnick P, Rantamaki T, Castren E (2012) The antidepressant-like effects of glutamatergic drugs ketamine and AMPA receptor potentiator LY 451646 are preserved in bdnf(+)/(−) heterozygous null mice. Neuropharmacology 62:391–397
Liu D, Zhang Q, Gu J, Wang X, Xie K, Xian X, Wang J, Jiang H, Wang Z (2014) Resveratrol prevents impaired cognition induced by chronic unpredictable mild stress in rats. Prog Neuropsychopharmacol Biol Psychiatry 49:21–29
Marosi K, Mattson MP (2014) BDNF mediates adaptive brain and body responses to energetic challenges. Trends Endocrinol Metab 25:89–98
Meltser I, Cederroth CR, Basinou V, Savelyev S, Lundkvist GS, Canlon B (2014) TrkB-mediated protection against circadian sensitivity to noise trauma in the murine cochlea. Curr Biol 24:658–663
Monteleone P, Martiadis V, Maj M (2011) Circadian rhythms and treatment implications in depression. Prog Neuropsychopharmacol Biol Psychiatry 35:1569–1574
Navigatore-Fonzo LS, Golini RL, Ponce IT, Delgado SM, Plateo-Pignatari MG, Gimenez MS, Anzulovich AC (2013) Retinoic acid receptors move in time with the clock in the hippocampus. Effect of a vitamin-A-deficient diet. J Nutr Biochem 24:859–867
Nollet M, Gaillard P, Minier F, Tanti A, Belzung C, Leman S (2011) Activation of orexin neurons in dorsomedial/perifornical hypothalamus and antidepressant reversal in a rodent model of depression. Neuropharmacology 61:336–346
Pan Y, Wang FM, Qiang LQ, Zhang DM, Kong LD (2010) Icariin attenuates chronic mild stress-induced dysregulation of the LHPA stress circuit in rats. Psychoneuroendocrinology 35:272–283
Papakostas GI, Fava M, Thase ME (2008) Treatment of SSRI-resistant depression: a meta-analysis comparing within- versus across-class switches. Biol Psychiatry 63:699–704
Reus GZ, Abelaira HM, Stringari RB, Fries GR, Kapczinski F, Quevedo J (2012) Memantine treatment reverses anhedonia, normalizes corticosterone levels and increases BDNF levels in the prefrontal cortex induced by chronic mild stress in rats. Metab Brain Dis 27:175–182
Robillard R, Hermens DF, Naismith SL, White D, Rogers NL, Ip TK, Mullin SJ, Alvares GA, Guastella AJ, Smith KL, Rong Y, Whitwell B, Southan J, Glozier N, Scott EM, Hickie IB (2014) Ambulatory sleep-wake patterns and variability in young people with emerging mental disorders. J Psychiatry Neurosci 39:130247
Schaaf MJ, Duurland R, de Kloet ER, Vreugdenhil E (2000) Circadian variation in BDNF mRNA expression in the rat hippocampus. Brain Res Mol Brain Res 75:342–344
Schweizer MC, Henniger MS, Sillaber I (2009) Chronic mild stress (CMS) in mice: of anhedonia, 'anomalous anxiolysis' and activity. PLoS One 4:e4326
Shirayama Y, Chen AC, Nakagawa S, Russell DS, Duman RS (2002) Brain-derived neurotrophic factor produces antidepressant effects in behavioral models of depression. J Neurosci 22:3251–3261
Toth E, Gersner R, Wilf-Yarkoni A, Raizel H, Dar DE, Richter-Levin G, Levit O, Zangen A (2008) Age-dependent effects of chronic stress on brain plasticity and depressive behavior. J Neurochem 107:522–532
Ushijima K, Morikawa T, To H, Higuchi S, Ohdo S (2006) Chronobiological disturbances with hyperthermia and hypercortisolism induced by chronic mild stress in rats. Behav Brain Res 173:326–330
Willner P (1997) Validity, reliability and utility of the chronic mild stress model of depression: a 10-year review and evaluation. Psychopharmacology (Berl) 134:319–329
Willner P, Towell A, Sampson D, Sophokleous S, Muscat R (1987) Reduction of sucrose preference by chronic unpredictable mild stress, and its restoration by a tricyclic antidepressant. Psychopharmacology (Berl) 93:358–364
Yi LT, Li J, Liu BB, Luo L, Liu Q, Geng D (2014) BDNF-ERK-CREB signalling mediates the role of miR-132 in the regulation of the effects of oleanolic acid in male mice. J Psychiatry Neurosci 39:348–359
Zhang Y, Gu F, Chen J, Dong W (2010) Chronic antidepressant administration alleviates frontal and hippocampal BDNF deficits in CUMS rat. Brain Res 1366:141–148
Acknowledgments
The project was supported by grants from the National Natural Science Foundation of China (No. 81202940), the Science Research Foundation of ministry of Health & United Fujian Provincial Health and Education Project for Tacking the Key Research (WKJ-FJ-31), the Promotion Program for Young and Middle-aged Teacher in Science and Technology Research of Huaqiao University (ZQN-PY218), and the Outstanding Youth Scientific Research Training Program in Colleges and Universities of Fujian Province (JA14015).
Conflict of Interest
The authors declare that they have no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yi, LT., Luo, L., Wu, YJ. et al. Circadian variations in behaviors, BDNF and cell proliferation in depressive mice. Metab Brain Dis 30, 1495–1503 (2015). https://doi.org/10.1007/s11011-015-9710-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11011-015-9710-0