Abstract
Vascular endothelial growth factor (VEGF)-D is a crucial mediator of angiogenesis. Following myocardial infarction (MI), cardiac VEGF-D and VEGF receptor (VEGFR)-3 are significantly upregulated. In addition to endothelial cells, myofibroblasts at the site of MI highly express VEGFR-3, implicating the involvement of VEGF-D in cardiac fibrogenesis that promotes repair and remodeling. The aim of the current study was to further explore the critical role of VEGF-D in fibrogenic response in myofibroblasts. Myofibroblast proliferation, migration, collagen synthesis, and degradation were investigated in cultured cardiac myofibroblasts subjected to VEGF-D with/without VEGFR antagonist or ERK inhibitor. Vehicle-treated cells served as controls. Myofibroblast proliferation and migration were detected by BrdU assay and Boyden Chamber method, respectively. Expression of type I collagen, metalloproteinase (MMP)-2/-9, tissue inhibitor of MMP (TIMP)-1/-2, and ERK phosphorylation were evaluated by Western blot analyses. Our results revealed that compared to controls, (1) VEGF-D significantly increased myofibroblast proliferation and migration; (2) VEGF-D significantly upregulated type I collagen synthesis in a dose- and time-dependent manner; (3) VEGFR antagonist abolished VEGF-D-induced myofibroblast proliferation and type I collagen release; (4) VEGF-D stimulated MMP-2/-9 and TIMP-1/-2 synthesis; (5) VEGF-D activated ERK phosphorylation; and (6) ERK inhibitor abolished VEGF-D-induced myofibroblast proliferation and type I collagen synthesis. Our in vitro studies have demonstrated that VEGF-D serves as a crucial profibrogenic mediator by stimulating myofibroblast growth, migration and collagen synthesis. Further studies are underway to determine the role of VEGF-D in fibrous tissue formation during cardiac repair following MI.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Following myocardial infarction (MI), scar formation is critical for cardiac repair that preserves the structural integrity of the heart and is essential to its recovery. Myofibroblasts play a central role in scar formation in the infarcted myocardium [1–3]. Myofibroblasts are phenotypically transformed fibroblasts, which are not present in the normal heart, but inevitably appear and accumulate in the infarcted myocardium. Myofibroblasts are highly active in collagen synthesis, which replaces the necrotic myocardium. Interstitial fibroblasts are the major source of myofibroblasts and differentiate into myofibroblasts under the stimulation of transforming growth factor (TGF)-β and mechanical stretch [3].
Local factors regulating cardiac repair/remodeling have drawn considerable attention. Numerous factors, including TGF-β [4, 5], fibroblast growth factor [6], placenta-derived growth factor [7], and connective tissue growth factor [8]. are well-recognized profibrogenic mediators in the injured heart, indicating that multiple pathways are involved in fibrous tissue formation during cardiac recovery processes.
Vascular endothelial growth factor (VEGF) is a sub-family of growth factors, which are important signaling proteins involved in both vasculogenesis and angiogenesis. The VEGF family consists of five distinct members in mammals. Our recent study revealed that the expression of VEGF-D and its specific receptors (VEGFR-3) is significantly upregulated in the infarcted myocardium, suggesting that VEGF-D plays a role in cardiac repair in an autocrine and/or paracrine manner [9]. VEGF-D is a key mediator of lymphangiogenesis and angiogenesis in the normal and pathological conditions. Our study further demonstrated that in addition to endothelial cells, VEGFR-3 is also highly expressed in myofibroblasts at the infarct site. These observations implicate that besides angio/lymphangiogenesis, VEGF-D is involved in fibrous tissue formation during cardiac repair. The aim of the current study was to further explore the hitherto unknown regulatory role of VEGF-D in fibrogenic response in myofibroblasts.
In the present in vitro study, the regulatory role of VEGF-D in the growth and activity of myofibroblasts was investigated. Cultured adult rat cardiac fibroblasts spontaneously differentiate into myofibroblasts in the first (P1) or second passage (P2) [10, 11]. Cardiac myofibroblasts reveal similar phenotypes in vitro and in vivo [10]. Using cultured myofibroblasts, we explored the role of VEGF-D in myofibroblast proliferation, migration, collagen synthesis, and degradation.
Materials and methods
Myofibroblast culture
Cardiac fibroblasts were isolated from 8-week-old male Sprague–Dawley rats. Briefly, rats were anesthetized with isoflurane inhalation and the heart was excised, washed in PBS, and cut into 1-mm3 pieces. The myocardial tissue was digested at 37 °C in digestion medium containing a mixture of collagenase B (115 mg/100 ml; Worthington, Lakewood, NJ) and trypsin (50 mg/100 ml; Sigma, St. Louis, MO) for 10 min with constant shaking. Cells from the third through tenth digestions were pooled and pelleted down. The pellet was resuspended in 5 ml DMEM 10 % FBS, seeded into 60-mm dishes, and kept at 37 °C in CO2 incubator for a preplating period of 150 min. Unattached cells were discarded, and attached cells were washed and grown in the plating medium. Cultures were maintained at 37 °C in 95 % humidified air and 5 % CO2 atmosphere. Cells at P0 and P1 were allowed to remain in the culture for 24–48 h. Fibroblasts in culture spontaneously differentiated into myofibroblasts at P1 and P2 [10, 11]. Only myofibroblasts at P2 were used in the study.
This study was approved by the University of Tennessee Health Science Center Animal Care and Use Committee. The investigation conforms to the Guide for the Care and Use of Laboratory Animals published by the US National Institutes of Health.
Effect of VEGF-D on myofibroblast proliferation
Myofibroblast proliferation was assessed using bromodeoxyuridine (BrdU) cell proliferation assay kit (Cell Signaling, Danvers, MA) and was performed according to the manufacturer’s instructions. Myofibroblasts were seeded in 96-well plates. After being quiescent in serum-deprived medium for 24 h, cells were exposed to VEGF-D (200 ng/ml) for 20 h. BrdU (10 μM) was then added, and cells were further incubated for 4 h. At the end of the incubation, medium was withdrawn, 100 μl/well of fixing solution was added, and the plates were incubated at room temperature for 30 min. Afterwards, the solution was aspirated and the wells were rinsed three times with a washing solution and eventually dried on a paper towel. Anti-BrdU monoclonal antibodies were then added (100 μl/well), and the wells were incubated for 1 h at room temperature. Medium was removed and the wells were rinsed three times with a washing solution. Horseradish peroxidase-conjugated anti-mouse IgG was added, and the plate was incubated at room temperature for 30 min. After three washes, TMB substrate (100 μl) was added to each well, followed by 100 μl of stop solution for 30 min. The absorbance was read at 450 nm in a microplate reader [11, 12]. Eight different wells were counted for each group and the experiment was repeated three times to achieve statistically significant results.
Effect of VEGF-D on myofibroblast migration
Myofibroblast migration was detected with a modified Boyden’s chamber assay [13]. The cell culture inserts, which contain membranes with 8.0 μm pore size, were placed in a 24-well tissue culture plate (Millipore ECM508, Billerica, MA). Myofibroblasts were quiesced for 24 h, then trypsinized, resuspended in DMEM, and seeded into the upper chamber at 1 × 105 cells/well. The lower chamber contains DMEM with VEGF-D (200 ng/ml) as a chemoattractant. After incubation for 6 h at 37 °C, cells/media were removed from the top side of the insert by pipetting out the remaining cell suspension. The inserts were placed in clean wells containing 400 μl of cell stain for 20 min. The inserts were then rinsed in water, and cotton-tipped swabs were used to remove nonmigratory cells from the interior of the insert. The inserts were transferred to a clean well containing 200 μl of extraction buffer for 15 min. The dye mixture (100 μl) was transferred to a 96-well plate, and optical density was measured at 560 nm [11, 14]. Six different samples were tested from each group and the experiment was repeated three times.
Time and dose effects of VEGF-D on type I collagen synthesis
Myofibroblasts were plated in 6-well plates and grown to subconfluence, then quiesced for 24 h in serum-deprived medium. Cells were then incubated with VEGF-D at the dose of 10, 50, and 200 ng/ml medium for 24 h or VEGF-D at the dose of 200 ng/ml for 6, 12, and 24 h. Type I collagen levels in the medium were assessed by Western blot. The medium was concentrated by centrifugation for 30 min in Amicon ultra centrifugal filters (Millipore, Billerica, MA). Proteins from cells and medium were loaded on gel, subjected to SDS-PAGE (10 % polyacrylamide gel), and transferred onto nitrocellulose membranes using a Bio-Rad Mini Trans Blot electrophoretic transfer unit. Membranes were blocked for non-specific protein with 5 % non-fat dry milk in TBS and probed overnight at 4 °C with primary antibodies against type I collagen (Millipore, Billerica, MA). Membranes were then washed three times (10 min per wash) with TBS with 0.05 % Tween 20 to remove unbound antibodies, and further incubated with appropriate HRP-conjugated secondary antibody (1:2000). Membranes were developed by a chemiluminescence reagent kit (Amersham Pharmacia Biotech, Piscataway, NJ) according to the manufacturer’s protocol. The amount of protein detected was assessed by means of quantitative densitometric analysis with a computer image analyzing system [11, 15]. Six different samples were tested in each group and the experiment was performed three times.
Impact of VEGF-D on MMP-2, MMP-9, TIMP-1 and TIMP-2 synthesis
Myofibroblasts were plated in 6-well plates and grown to subconfluence, then quiesced for 24 h in serum-deprived medium. Cells were incubated with or without VEGF-D at the dose of 200 ng/ml for 24 h. MMP-2, MMP-9, TIMP-1, and TIMP-2 protein levels in the medium were assessed by Western blot as described earlier [11, 16].
Effect of VEGFR-2/-3 inhibition on myofibroblast proliferation and type I collagen
Myofibroblasts were subjected to VEGFR-2 inhibitor (Ki8751, 1 µM) (R&D, Minneapolis, MN) [17], VEGFR-3 inhibitor (MAZ51 5 µM) (Sigma-Aldrich, St. Louis, MO) [18], or the combination of Ki8975 and MAZ51 at the above doses for 30 min before VEGF-D treatment (200 ng/ml). The medium was collected after 24 h. Myofibroblast proliferation and type I collagen production were then analyzed as described above.
Influence of VEGF-D on ERK activation
VEGF-D (200 ng/ml) was administered to the cells for 5, 15, 60, or 120 min. Cell lysate was collected in modified RIPA buffer. ERK phosphorylation was detected by Western blot using antibodies against ERK1/2 and phospho-ERK1/2 (Cell Signaling Technology, Danvers, MA).
Role of ERK inhibitor in myofibroblast proliferation and collagen synthesis
ERK inhibitor (U0126, 10 µM) [19] was administered to cells for 1 h, followed by VEGF-D treatment (200 ng/ml). After 24 h, myofibroblast proliferation and type I collagen release were then analyzed as described earlier.
Statistical analysis
Statistical analysis of cell proliferation, migration, and Western blot data among the groups was performed using Student t test or ANOVA. The values are expressed as mean ± SE and P < 0.05 considered significant. Multiple group comparisons among controls and each group were made by Scheffé’s F test.
Results
VEGF-D upregulates myofibroblast proliferation
Myofibroblasts are the most prevalent cell type in the infarcted myocardium and are the predominant effectors of fibrogenesis [20]. Myofibroblasts are primarily derived from fibroblasts under the stimulation of TGF-β and are characterized by increased expression of the specific contractile protein, α-SMA. After appearance, myofibroblasts rapidly proliferate and accumulate in the infarcted myocardium. In the current study, we examined the potential role of VEGF-D in myofibroblast proliferation. As demonstrated by BrdU proliferation assay, we found that VEGF-D treatment significantly increased myofibroblast proliferation compared to vehicle-treated control cells (Fig. 1a).
VEGF-D stimulates fibroblast migration
Cell migration is a central process in tissue repair. Myofibroblasts contain α-SMA, the contractile protein, which facilitates cell migration within the repairing tissue. Myofibroblast migration is stimulated by various factors, including TGF-β1 [21, 22], MMP [23], endothelin-1 [24], and VEGF-C [11]. In this study, we examined whether VEGF-D is involved in myofibroblast migration. Monitored by Boyden’s chamber assay, we observed significantly increased migration of VEGF-D-treated myofibroblasts compared to vehicle-treated cells (Fig. 1b).
Dose and time response of VEGF-D in type I collagen synthesis
Collagen is the main structural protein in the extracellular space of the connective and fibrous tissue. Over 90 % of the collagen in the body is type I. The major role of myofibroblasts in repairing heart is to secrete collagen. Collagen synthesis is primarily regulated by cytokines and growth factors [25]. In the current study, we examined whether VEGF-D is involved in collagen synthesis. Collagen produced in cultured myofibroblasts is secreted into the culture medium. Our data revealed that VEGF-D treatment increased type I collagen levels in the medium in a dose- and time-dependent manner (Fig. 2a, b, respectively).
VEGF-D promotes MMP-2 and MMP-9 production
MMPs, large family of zinc-endopeptidases, are responsible for collagen degradation. MMP-2 and MMP-9 play a major role in collagen degradation in rodent, which are secreted by various types of cells, including myofibroblasts. By Western blot, we studied the effect of VEGF-D on MMP-2 and MMP-9 synthesis in cultured myofibroblasts. Our data showed that MMP-2 and MMP-9 were barely detectable in the medium of vehicle-treated cells. VEGF-D treatment, however, significantly elevated MMP-2 and MMP-9 levels in the medium (Fig. 3a, b, respectively).
VEGF-D promotes TIMP-1 and TIMP-2 synthesis
TIMPs are glycoprotein peptidases and involved in the inhibition of MMP activity [26]. TIMPs are secreted proteins that are released into the interstitial space in vivo and culture medium in vitro. Western blot analyses showed that untreated myofibroblasts produced extremely low levels of TIMP-1 and TIMP-2. VEGF-D treatment significantly upregulated TIMP-1 and TIMP-2 levels in the medium compared to the controls (Fig. 3c, d).
VEGFR inhibition abolishes VEGF-D-induced proliferation and collagen synthesis
The cellular actions of VEGF-D are mediated by their specific membrane-bound receptors, VEGFR-2 and VEGFR-3. Our study revealed that VEGFR-2 inhibitor (Ki8751) and VEGFR-3 inhibitor (MAZ51) co-treatment individually or in combination abolished VEGF-D-induced myofibroblast proliferation (Fig. 4a) and significantly attenuated type I collagen synthesis (Fig. 4b).
Effect of VEGFR inhibitors on myofibroblast growth and collagen synthesis. Co-treatment with VEGFR-2 inhibitor (Ki8759) and VEGFR-3 inhibitor (MAZ51) alone and their combination abolished VEGF-D-induced myofibroblast proliferation (a) and attenuated type I collagen synthesis (b). # p < 0.05 versus VEGF-D
VEGF-D activates ERK pathway
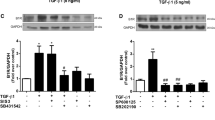
Once VEGF-D binds to its receptors, VEGFR-2 and VEGFR-3, it activates the downstream cascade of VEGF pathway, including ERK phosphorylation. Our data revealed that after VEGF-D treatment, phosphorylated ERK in myofibroblasts was significantly increased at 5 min, peaked at 15 min, and remained elevated at 60 and 120 min (Fig. 5).
ERK inhibitor attenuates VEGF-D-induced myofibroblast proliferation and collagen synthesis
Compared to VEGF-D-treated cells, co-treatment with ERK inhibitor (U0126) significantly attenuated VEGF-D-induced myofibroblast proliferation (Fig. 6a) and type I collagen release in the medium (Fig. 6b).
Discussion
Following MI, myofibroblasts are accumulated in the infarcted region of the myocardium and promote cardiac repair by forming scar tissue. We have recently reported that VEGF-D and VEGFR-3 are significantly increased at the infarct site, where cells expressing VEGFR-3 include myofibroblasts, implicating the potential autocrine/paracrine regulation of VEGF-D on cardiac fibrous tissue formation [9]. In the current study, we investigated the impact of VEGF-D on fibrogenic response in myofibroblasts.
Firstly, we examined the role of VEGF-D in myofibroblast proliferation. VEGF-D is well known to stimulate vascular and lymphatic endothelial cell proliferation, thereby promoting angiogenesis and lymphangiogenesis in both normal and pathological conditions [27, 28]. However, the potential effect of VEGF-D on proliferation of other cell types remains uncertain. After appearance, myofibroblasts rapidly replicate and accumulate at the infarct site and release extracellular matrix. The current study revealed that VEGF-D stimulates cultured myofibroblast proliferation in a dose- and time-dependent manner, which is abolished by VEGFR inhibitor. This observation implicates that besides endothelial cells, VEGF-D also promotes myofibroblast proliferation. In addition to VEGF-D, TGF-β1 has been reported to stimulate myofibroblast differentiation and proliferation [29–31]. Our previous study further revealed that VEGF-C, another isoform of VEGF family, also promotes myofibroblast proliferation [11]. Taken together, myofibroblast growth appears to be regulated by multiple growth factors in the infarcted heart.
Secondly, we provided evidence for the potential role of VEGF-D in myofibroblast migration. Myofibroblasts are highly mobile and contractile. Myofibroblast migration plays a significant role in the tissue repair and remodeling process. Following MI, myofibroblasts first appear in the border zone, the region between noninfarcted and infarcted myocardium, and then migrate into the infarct site. Myofibroblast migration has been shown to be regulated by various cytokines, including PDGF, interstitial growth factor, endothelial growth factor, TGF-β1, and VEGF-C. [11, 32]. Therefore, a multitude of redundant synergistic mechanisms are involved in myofibroblast migration. The present study further indicates that VEGF-D also plays a stimulatory role in myofibroblast migration. In addition, VEGF-D is reported to stimulate endothelial cell migration and tumor cell motility, contributing to tumor metastasis [33]. These observations indicate that VEGF-D regulates various cellular actions in different cell types.
Thirdly, we investigated whether VEGF-D regulates the activity of myofibroblasts. The primary role of myofibroblasts is to synthesize collagen, the major component of fibrous tissue. Type I collagen is the main element of cardiac fibrous tissue. Synthesis of type I collagen is activated in the infarcted heart, which is co-localized with upregulated VEGF-D/VEGFR-3 [9]. Our current study has revealed that VEGF-D significantly upregulates type I collagen synthesis in cultured myofibroblasts in a dose- and time-dependent manner, which is abolished by VEGFR inhibitor. These observations implicate that VEGF-D serves as a fibrogenic mediator and promotes fibrous tissue formation in myofibroblasts. In addition to VEGF-D, we have reported that other VEGF isoforms, such as VEGF-C, also promote the production of extracellular matrix in myofibroblasts [11]. Therefore, besides angiogenesis, VEGF family also plays a key regulatory role in fibrous tissue formation, contributing to tissue repair and remodeling.
Collagen synthesis and degradation coexist simultaneously in the tissue and their equilibrium determines the collagen volume in tissue. Elevated collagen synthesis and/or suppressed collagen degradation lead to excessive accumulation of accumulated collagen in tissue undergoing remodeling. MMPs play a crucial role in collagen degradation. MMPs are a diverse family of enzymes capable of degrading various components of the extracellular matrix. Of these, MMP-2 and MMP-9 play a key role in the degradation of collagen in rats. MMP activity is regulated at multiple levels. All MMPs are secreted as proenzymes and require extracellular activation. MMPs are primarily produced by macrophages and fibroblast-like cells in the infarcted myocardium [26]. The current study reveals that VEGF-D significantly elevated MMP-2 and MMP-9 secretion in cultured myofibroblasts, implicating that VEGF-D increases MMP-2 and MMP-9 production in myofibroblasts.
Upon secretion into the interstitial space, MMP activity is controlled by TIMPs. TIMPs function as an important regulatory brake on MMP activity by inhibiting the active species, thereby suppressing MMP activity and collagen degradation [26]. Studies from this and other laboratories indicate that the expression of TIMP-1 and TIMP-2 is upregulated in the infarcted myocardium [26], where elevated VEGF-D/VEGFR-3 coincides with enhanced TIMP-1/-2 expression. The current study has revealed that VEGF-D treatment significantly upregulates TIMP-1 and TIMP-2 synthesis in cultured myofibroblasts, which in turn suppresses MMP activity and limits collagen degradation.
Finally, we investigated the activation of downstream molecules of VEGF pathway. VEGF-D binds to VEGFR-2 and VEGFR-3 in the cell membrane, initiating the cascade of signals. Further downstream, phosphate signal activates ERK [34]. Phosphorylated ERK then regulates the transcription factors. Cardiac repair/remodeling involves extraordinary alteration in the phosphorylation of ERK, which is consistently elaborated at the infarct site [35]. Immunostaining of phosphorylated ERK is localized to fibrotic areas populated primarily by non-myocytes [35]. The current study unequivocally implicates that VEGF-D stimulates ERK phosphorylation in myofibroblasts and activates myofibroblast growth and activity. Furthermore, ERK inhibitor abolished VEGF-D-induced myofibroblast proliferation and type I collagen synthesis.
Taken together, our findings demonstrated that VEGF-D upregulates myofibroblast proliferation, migration, and collagen synthesis through activation of VEGF pathway. Further studies are underway to determine the specific regulatory roles of VEGF-D in fibrous tissue formation and cardiac remodeling following infarction.
References
Ma Y, de Castro Bras LE, Toba H, Iyer RP, Hall ME, Winniford MD, Lange RA, Tyagi SC, Lindsey ML (2014) Myofibroblasts and the extracellular matrix network in post-myocardial infarction cardiac remodeling. Pflugers Arch 466:1113–1127. doi:10.1007/s00424-014-1463-9
Sun Y, Weber KT (1996) Angiotensin converting enzyme and myofibroblasts during tissue repair in the rat heart. J Mol Cell Cardiol 28:851–858. doi:10.1006/jmcc.1996.0080
Small EM, Thatcher JE, Sutherland LB, Kinoshita H, Gerard RD, Richardson JA, Dimaio JM, Sadek H, Kuwahara K, Olson EN (2010) Myocardin-related transcription factor-a controls myofibroblast activation and fibrosis in response to myocardial infarction. Circ Res 107:294–304. doi:10.1161/CIRCRESAHA.110.223172
Lijnen PJ, Petrov VV, Fagard RH (2000) Induction of cardiac fibrosis by transforming growth factor-beta(1). Mol Genet Metab 71:418–435. doi:10.1006/mgme.2000.3032
Hao J, Ju H, Zhao S, Junaid A, Scammell-La Fleur T, Dixon IM (1999) Elevation of expression of Smads 2, 3, and 4, decorin and TGF-beta in the chronic phase of myocardial infarct scar healing. J Mol Cell Cardiol 31:667–678. doi:10.1006/jmcc.1998.0902
Virag JA, Rolle ML, Reece J, Hardouin S, Feigl EO, Murry CE (2007) Fibroblast growth factor-2 regulates myocardial infarct repair: effects on cell proliferation, scar contraction, and ventricular function. Am J Pathol 171:1431–1440. doi:10.2353/ajpath.2007.070003
Liu C, Zhao W, Meng W, Zhao T, Chen Y, Ahokas RA, Liu H, Sun Y (2014) Platelet-derived growth factor blockade on cardiac remodeling following infarction. Mol Cell Biochem 397:295–304. doi:10.1007/s11010-014-2197-x
Dean RG, Balding LC, Candido R, Burns WC, Cao Z, Twigg SM, Burrell LM (2005) Connective tissue growth factor and cardiac fibrosis after myocardial infarction. J Histochem Cytochem 53:1245–1256. doi:10.1369/jhc.4A6560.2005
Zhao T, Zhao W, Chen Y, Liu L, Ahokas RA, Sun Y (2013) Differential expression of vascular endothelial growth factor isoforms and receptor subtypes in the infarcted heart. Int J Cardiol 167:2638–2645. doi:10.1016/j.ijcard.2012.06.127
Santiago JJ, Dangerfield AL, Rattan SG, Bathe KL, Cunnington RH, Raizman JE, Bedosky KM, Freed DH, Kardami E, Dixon IM (2010) Cardiac fibroblast to myofibroblast differentiation in vivo and in vitro: expression of focal adhesion components in neonatal and adult rat ventricular myofibroblasts. Dev Dyn 239:1573–1584. doi:10.1002/dvdy.22280
Zhao T, Zhao W, Meng W, Liu C, Chen Y, Sun Y (2014) Vascular endothelial growth factor-C: its unrevealed role in fibrogenesis. Am J Physiol Heart Circ Physiol 306:H789–H796. doi:10.1152/ajpheart.00559.2013
Cohen S, Efraim AN, Levi-Schaffer F, Eliashar R (2011) The effect of hypoxia and cyclooxygenase inhibitors on nasal polyp derived fibroblasts. Am J Otolaryngol 32:564–573. doi:10.1016/j.amjoto.2010.11.010
Ferri N, Panariti F, Ricci C, Maiocchi G, Corsini A (2015) Aliskiren inhibits prorenin-induced human aortic smooth muscle cell migration. J Renin Angiotensin Aldosterone Syst 16:284–291. doi:10.1177/1470320314528364
Manso AM, Kang SM, Plotnikov SV, Thievessen I, Oh J, Beggs HE, Ross RS (2009) Cardiac fibroblasts require focal adhesion kinase for normal proliferation and migration. Am J Physiol Heart Circ Physiol 296:H627–H638. doi:10.1152/ajpheart.00444.2008
Iwasaki T, Mukasa K, Yoneda M, Ito S, Yamada Y, Mori Y, Fujisawa N, Fujisawa T, Wada K, Sekihara H, Nakajima A (2005) Marked attenuation of production of collagen type I from cardiac fibroblasts by dehydroepiandrosterone. Am J Physiol Endocrinol Metab 288:E1222–E1228. doi:10.1152/ajpendo.00370.2004
El Hajj EC, El Hajj MC, Voloshenyuk TG, Mouton AJ, Khoutorova E, Molina PE, Gilpin NW, Gardner JD (2014) Alcohol modulation of cardiac matrix metalloproteinases (MMPs) and tissue inhibitors of MMPs favors collagen accumulation. Alcohol Clin Exp Res 38:448–456. doi:10.1111/acer.12239
Kuo SW, Ke FC, Chang GD, Lee MT, Hwang JJ (2011) Potential role of follicle-stimulating hormone (FSH) and transforming growth factor (TGFbeta1) in the regulation of ovarian angiogenesis. J Cell Physiol 226:1608–1619. doi:10.1002/jcp.22491
Kazenwadel J, Secker GA, Betterman KL, Harvey NL (2012) In vitro assays using primary embryonic mouse lymphatic endothelial cells uncover key roles for FGFR1 signalling in lymphangiogenesis. PLoS One 7:e40497. doi:10.1371/journal.pone.0040497
Braun OO, Lu D, Aroonsakool N, Insel PA (2010) Uridine triphosphate (UTP) induces profibrotic responses in cardiac fibroblasts by activation of P2Y2 receptors. J Mol Cell Cardiol 49:362–369. doi:10.1016/j.yjmcc.2010.05.001
Peterson DJ, Ju H, Hao J, Panagia M, Chapman DC, Dixon IM (1999) Expression of Gi-2 alpha and Gs alpha in myofibroblasts localized to the infarct scar in heart failure due to myocardial infarction. Cardiovasc Res 41:575–585
Brenmoehl J, Miller SN, Hofmann C, Vogl D, Falk W, Scholmerich J, Rogler G (2009) Transforming growth factor-beta 1 induces intestinal myofibroblast differentiation and modulates their migration. World J Gastroenterol 15:1431–1442
Thannickal VJ, Lee DY, White ES, Cui Z, Larios JM, Chacon R, Horowitz JC, Day RM, Thomas PE (2003) Myofibroblast differentiation by transforming growth factor-beta1 is dependent on cell adhesion and integrin signaling via focal adhesion kinase. J Biol Chem 278:12384–12389. doi:10.1074/jbc.M208544200
Sato M, Hirayama S, Lara-Guerra H, Anraku M, Waddell TK, Liu M, Keshavjee S (2009) MMP-dependent migration of extrapulmonary myofibroblast progenitors contributing to posttransplant airway fibrosis in the lung. Am J Transplant 9:1027–1036. doi:10.1111/j.1600-6143.2009.02605.x
Kernochan LE, Tran BN, Tangkijvanich P, Melton AC, Tam SP, Yee HF Jr (2002) Endothelin-1 stimulates human colonic myofibroblast contraction and migration. Gut 50:65–70
Amento EP, Ehsani N, Palmer H, Libby P (1991) Cytokines and growth factors positively and negatively regulate interstitial collagen gene expression in human vascular smooth muscle cells. Arterioscler Thromb 11:1223–1230
Lindsey ML, Zamilpa R (2012) Temporal and spatial expression of matrix metalloproteinases and tissue inhibitors of metalloproteinases following myocardial infarction. Cardiovasc Ther 30:31–41. doi:10.1111/j.1755-5922.2010.00207.x
Roy H, Bhardwaj S, Yla-Herttuala S (2006) Biology of vascular endothelial growth factors. FEBS Lett 580:2879–2887. doi:10.1016/j.febslet.2006.03.087
Tammela T, Enholm B, Alitalo K, Paavonen K (2005) The biology of vascular endothelial growth factors. Cardiovasc Res 65:550–563. doi:10.1016/j.cardiores.2004.12.002
Strutz F, Zeisberg M, Renziehausen A, Raschke B, Becker V, van Kooten C, Muller G (2001) TGF-beta 1 induces proliferation in human renal fibroblasts via induction of basic fibroblast growth factor (FGF-2). Kidney Int 59:579–592. doi:10.1046/j.1523-1755.2001.059002579.x
Clark RA, McCoy GA, Folkvord JM, McPherson JM (1997) TGF-beta 1 stimulates cultured human fibroblasts to proliferate and produce tissue-like fibroplasia: a fibronectin matrix-dependent event. J Cell Physiol 170:69–80. doi:10.1002/(SICI)1097-4652(199701)170:1<69:AID-JCP8>3.0.CO;2-J
Peng H, Carretero OA, Peterson EL, Rhaleb NE (2010) Ac-SDKP inhibits transforming growth factor-beta1-induced differentiation of human cardiac fibroblasts into myofibroblasts. Am J Physiol Heart Circ Physiol 298:H1357–H1364. doi:10.1152/ajpheart.00464.2009
Leeb SN, Vogl D, Falk W, Scholmerich J, Rogler G, Gelbmann CM (2002) Regulation of migration of human colonic myofibroblasts. Growth Factors 20:81–91
Yanagawa T, Shinozaki T, Watanabe H, Saito K, Raz A, Takagishi K (2012) Vascular endothelial growth factor-D is a key molecule that enhances lymphatic metastasis of soft tissue sarcomas. Exp Cell Res 318:800–808. doi:10.1016/j.yexcr.2012.01.024
Narasimhan P, Liu J, Song YS, Massengale JL, Chan PH (2009) VEGF Stimulates the ERK 1/2 signaling pathway and apoptosis in cerebral endothelial cells after ischemic conditions. Stroke 40:1467–1473. doi:10.1161/STROKEAHA.108.534644
Yeh CC, Li H, Malhotra D, Turcato S, Nicholas S, Tu R, Zhu BQ, Cha J, Swigart PM, Myagmar BE, Baker AJ, Simpson PC, Mann MJ (2010) Distinctive ERK and p38 signaling in remote and infarcted myocardium during post-MI remodeling in the mouse. J Cell Biochem 109:1185–1191. doi:10.1002/jcb.22498
Acknowledgments
This work was supported by NIH Heart, Blood, and Lung Institute (1RO1-HL096503, Yao Sun).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None declared.
Rights and permissions
About this article
Cite this article
Zhao, T., Zhao, W., Meng, W. et al. Vascular endothelial growth factor-D mediates fibrogenic response in myofibroblasts. Mol Cell Biochem 413, 127–135 (2016). https://doi.org/10.1007/s11010-015-2646-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-015-2646-1