Abstract
The study aims to investigate the impacts of hyperglycemia in the presence of fatty acids on early placentation processes that involves tube formation, cellular growth and proliferation, and metabolic activities of the first trimester trophoblast cells. Effects of maternal circulatory glucose levels that mimic physiological (5.5 mM), pre-diabetic (11 mM) and diabetic (≥25 mM) phenotypes on tube formation (as a measure of angiogenesis in vitro), cellular viability and proliferation, fatty acid uptake and expression of genes associated with invasion, angiogenesis and fatty acid metabolism were examined using HTR8/SVneo cells. Glucose (25 mM) induced tube formation, viability, and proliferation of the first trimester trophoblast cells, HTR8/SVneo. Tube formation was, however, disintegrated in the presence of high glucose (40 mM) which was partially protected by eicosapentaenoic acid, 20:5n-3 (EPA) and docosahexaenoic acid, 22:6n-3 in vitro. Glucose (25 mM)-mediated induction in tube formation was favored by increased cellular uptake of [14C]EPA (p < 0.05). Treatment of HTR8/SVneo cells with glucose (25 mM) significantly increased mRNA and protein level of matrix metalloproteinase-9 (MMP9) (p < 0.05). In addition, glucose (25 mM) stimulated the expression of fatty acid binding protein-4, FABP4, and plasma membrane fatty acid binding protein, FABPpm, in these cells (p < 0.05). Glucose-stimulated tube formation in a ‘concentration-dependent’ manner, and this may involve activation of several factors that include MMP9 and fatty acid uptake and metabolism.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Placenta of women with gestational diabetes mellitus (GDM) showed several changes that may be associated with impaired functioning, leading to bad perinatal outcome. With the onset of global epidemic of diabetes, it is imperative to measure effect of GDM on the feto-placental growth and development. Increased plasma levels of glucose associated with diabetes may affect placentation. The development of a placental vascular network is essential for the angiogenesis and growth of the developing fetus [1]. Hyperglycemia during pregnancy profoundly changes maternal and fetal milieu with higher levels of growth factors and free fatty acids [2]. Several factors are involved in angiogenic process, including vascular endothelial growth factor (VEGF), platelet-derived growth factor (PDGF), angiopoietin-like protein-4 (ANGPTL4), matrix metalloproteinase (MMP), FABP4, and others [3, 4]. Under hyperglycemia, vasculogenesis of the blood vessels in the yolk sac is disrupted, and the cellular structures in the vessels are altered [5, 6]. Direct effect of glucose on the first trimester trophoblast cells, HTR8/SVneo revealed lower activity of urokinase plasminogen activator and thus implicated reduced invasiveness of the trophoblast [7]. However, the combined effects of hyperglycemic factors such as glucose, free fatty acids on tube formation in the first trimester trophoblast cells are not known. Since fatty acids affect tube formation processes in these cells, the present study was aimed to examine the effects of fatty acids and glucose together, as both of these factors at higher levels can contribute in the pathogenesis of the GDM.
Placental uptake of long chain fatty acids (LCFAs) such as arachidonic acid, 20:4n-6 (AA), eicosapentaenoic acid, 20:5n-3 (EPA), and docosahexaenoic acid, 22:6n-3 (DHA) from the maternal circulation is indispensable for growth and brain development of the fetus [8]. Our previous data showed that these fatty acids favored energy-intensive tube formation process in the first trimester trophoblast cells [9–11]. Therefore, uptake of LCFAs (14C-LCFAs) by these cells was measured under hyperglycemic conditions. Although the physiological blood glucose level is ~5 mM, the precise glucose concentration at the fetal−maternal interface is not known [12].The placental glucose transport is, however, highly efficient and saturable at maternal circulatory concentration of ≥20 mM, which is well above the normal physiological range [13]. Since no information was available on the effect of excess maternal glucose level on the tube formation of the first trimester trophoblast cells, the study examined glucose levels at physiological (5.5 mM), pre-diabetic (11 mM), and diabetic (≥25 mM) on early placental development, using a first trimester trophoblast cell line, HTR8/SVneo.
In this paper, we report for the first time that glucose (25 mM) alters tube formation of the first trimester trophoblast cells, HTR8/SVneo and stimulates the expression of MMP9 with concomitant increases in the uptake of [14C]EPA. Moreover, glucose up-regulates the expression of the genes that encode fatty acid uptake and metabolism in these cells.
Materials and methods
Materials
The HTR8/SVneo trophoblast cell line was kindly provided by Dr. CH Graham, Queen’s University, Canada. All the radiolabeled and unlabeled fatty acids were procured as described previously [9, 11]. Lactate dehydrogenase (LDH) assay kit was obtained from Roche Molecular Biochemical, Mannheim, Germany. Matrigel was procured from BD Biosciences (USA). Trypsin–EDTA solution, oleic acid, penicillin–streptomycin solution, RPMI 1640, d-glucose, other fine chemicals and solvents were obtained from Sigma-Aldrich Norway AS, Norway.
Cell culture
The HTR8/SVneo cells were cultured in RPMI-1640 medium as described before [9]. Normal RPMI 1640 media were enriched with glucose at the rate of 2 g/l which corresponds to ~11 mM of glucose (1 M glucose = 180 g/l). Glucose level in 100 % fetal bovine serum (FBS) was measured to be 4 mM [7]. Glucose was added externally to glucose-free RPMI with a final concentration of 5.5 (control), 11, 25, and 40 mM enriched with 5 % FCS.
Cytotoxicity of glucose and fatty acid on HTR8/SVneo cells
The cytotoxicity of glucose (5.5, 11, 25, and 40 mM) and fatty acid (100 μM) treatment on HTR8/SVneo cells was determined by measuring the enzyme LDH releases after incubating these cells for 24 h [10].
Cellular viability and proliferation assay
Cell viability and proliferation were performed as a measure of cellular growth and differentiation as described before [11]. Cells were incubated with different doses of glucose (5.5, 11, 25 mM). 3-(4,-dimethylthiazol-2-yl)-2,-diphenyl tetrazolium bromide (MTT) was used to detect viable proliferating cells. The absorbance was read at 560 nm.
Measurement of radiolabeled fatty acids (14C) uptake by HTR8/SVneo cells
The fatty acid uptake was carried out as described before [10]. The cells were pre-incubated with glucose (5.5, 11, and 25 mM) for 21 h followed by 3 h incubation with 14C fatty acids. The radioactivity was determined using a scintillation counter. Soluble protein content was measured by colorimetric estimation (at 562 nm) derived on the biuret reaction using bicinchoninic acid (Uptima). The data were derived from the standard (BSA) as microgram (µg) of the soluble protein. Fatty acid uptake was expressed as picomole (pmol) of fatty acid taken up per µg of cellular protein.
Quantitative estimation of gene expression by real-time PCR
HTR8/SVneo cells were incubated in presence of glucose (5.5, 11, and 25 mM) for 24 h. The cells were then lysed and total RNA was isolated as described previously [9, 11]. cDNAs were synthesized from RNA and analyzed using TaqMan Assays (Table 1) on ABI7900HT Real-Time PCR System.
Tube formation assay
Tube formation assay was performed in HTR8/SVneo cells as described before [9, 11]. The cells were seeded (7 × 104 cells/well/24 well plate) on matrigel (growth factor reduced) and glucose solution (5.5–40 mM) was added to the cells. The wells were captured after 16 h by an inverted microscope at 4× magnification (Nikon TS100F, Japan). Capillary tube length was quantified and expressed in pixel [9].
Western blot analysis of MMP9 expression
Cell lysates were prepared by adding 200 µl of radioimmuno-precipitation assay buffer (RIPA, Sigma Aldrich). The lysates were sonicated for 1 min in Vibra-Cell sonicator and centrifuged. The supernatants were estimated for protein levels with BCA protein assay (Pierce, USA), and 50 µg of proteins/lane were resolved by SDS-PAGE (12 %) prior to their transfer to polyvinylidene difluoride membranes (Immobilon-P, Millipore Corp.). After blocking with startingblock buffer (ThermoScientific), membranes were immunoblotted with antibodies against anti-MMP9 (1:500, bs-0397R, Bioss) and anti β-actin (1:1,000; ab-8227, Abcam) and incubated with HRP-conjugated goat anti-rabbit IgG (1:10,000; Sigma Aldrich). The blots were processed using enhanced chemiluminescence substrate (Cat-32134, Pierce, USA). Immunoblot signals were detected by Storm 860 phosphor imager and quantified by ImageQuant software (GE healthcare).
Statistics and data analysis
All the values are presented as mean and standard errors of mean (SEM). Data were evaluated by one-way ANOVA followed by post-hoc Bonferroni test for the fatty acid groups. For glucose dose, the significance was calculated using Student’s t test. A p value of <0.05 was considered statistically significant.
Results
Effect of glucose on tube formation in the HTR8/SVneo cells
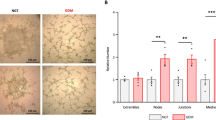
Dose-dependent effect of glucose (5.5–40 mM) on tube formation was measured in HTR8/SVneo cells (Fig. 1a). Number and length of tubes were increased dose-dependently up to 30 mM (2,800 ± 125 pixel) compared to 5.5 mM (500 ± 55 pixel) glucose. Tube formation was significantly increased at 20–35 mM compared to 5.5 mM glucose (Fig. 1b). Compared to 5.5 mM of glucose (control), tube formation was increased by 480 % (2,400 ± 110 pixel) and 530 % (2,650 ± 140 pixel) with 20 and 25 mM glucose (p < 0.05, Fig. 1a, b).
Effect of glucose on tube formation of the first trimester trophoblast cells, HTR8/SVneo. Serum starved cells (7 × 104 per well) were seeded to a pre-coated matrigel (8 mg/ml) wells. Cells were cultured in glucose-free media with different dosages of glucose as described in the methods. Total capillary tube length was quantified in pixel as described in “Materials and methods” section. Controls were cells received 5.5 mM glucose. Data are shown as mean ± SEM (n = 3). *p < 0.05 vs. control
Effect of glucose on viability and proliferation of the HTR8/SVneo cells
Since cellular viability and proliferation are often associated with tube formation, we investigated glucose effects on proliferation of these cells by incubating with different doses of glucose (5.5, 11, 25 mM). Glucose increased proliferation of the cells at 25 mM. Compared to 5.5 mM (control), proliferation was increased significantly over 30 % (mean OD 0.701 ± 0.04 vs. 0.929 ± 0.15, p < 0.01) with 25 mM glucose (Fig. 2).
Effect of glucose on viability and proliferation of HTR8/SVneo cells. Cell (2 × 103/well/96 plate) viability was measured by MTT assay as described in the method. The absorbance was read at 560 nm. Data represent mean ± SEM (n = 3). Percentage of changes in proliferation was calculated by considering 5.5 mM (control) as 100 % after normalized over basal values. **p value <0.01 versus control
Effects of fatty acids on glucose-mediated tube formation of the HTR8/SVneo cells
The cells were seeded with 40 mM glucose, and subsequently 50 μM of EPA or DHA or BSA (control) were added. High concentration of glucose (HG, 40 mM) significantly reduced tube formation by ~200 % (2,650 ± 135 vs. 1,300 ± 70 pixel, p < 0.05) of the HTR8/SVneo cells as compared to 25 mM glucose. BSA alone could not protect tube length as compared to fatty acids. EPA and DHA (50 μM) partially protected the high glucose (40 mM)-induced tubule disintegration by 65 % (EPA + HG: 2,770 ± 145 vs. BSA + HG: 1,680 ± 95 pixel) and 90 % (DHA + HG: 3,190 ± 175 vs. BSA + HG: 1,680 ± 95 pixel), respectively (p < 0.05, Fig. 3a, b).
Effect of LCFAs on glucose-induced tube formation in first trimester trophoblast cells, HTR8/SVneo. Tube formation was performed with 25 mM and 40 mM glucose-treated HTR8/SVneo cells in the presence or absence of EPA and DHA (50 μM) as described previously (a). Total capillary tube length was quantified in pixel as described in “Materials and methods” section (b). Controls were cells received BSA in place of fatty acids. Data are shown as mean ± SEM (n = 3). *p value <0.05 versus glucose (25 mM); **p value <0.05 versus (HG + BSA); ***p value <0.05 versus EPA; BSA bovine serum albumin, G glucose, HG high glucose
Effects of glucose on the uptake of LCFAs
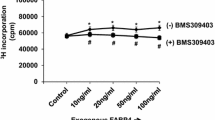
To investigate whether hyperglycemic condition affects uptake of LCFAs, [14C] fatty acid uptake by HTR8/SVneo cells was measured. Pre-incubation of HTR8/SVneo with glucose, stimulated the uptake of [14C]EPA by 26 % (46 ± 1.9 vs. 58 ± 3.0 pmol/µg protein: 5.5 vs. 25 mM, p < 0.05), while uptake of [14C]OA (48 ± 2.5 vs. 54 ± 2.9 pmol/µg protein: 5.5 vs. 25 mM), [14C]AA (114 ± 5.6 vs. 110 ± 5.7 pmol/µg protein) and [14C]DHA (29 ± 1.6 vs. 28 ± 1.3 pmol/µg protein) remained insignificant (Fig. 4). Uptake of [14C]EPA was increased dose-dependently when cells were pre-stimulated with glucose (5.5, 11 and 25 mM). [14C]EPA uptake was significantly increased by glucose (25 mM) compared with the uptake of other fatty acids (p < 0.05).
LCFA uptake of first trimester trophoblast cells, HTR8/SVneo in presence of glucose. [14C] Fatty acid uptake was measured in HTR8/SVneo cells after pre-incubation with glucose (5.5, 11 and 25 mM) with 100 µM LCFAs [oleic acid (OA), arachidonic acid (AA), eicosapentaenoic acid (EPA), and docosahexaenoic acid (DHA)] labeled with [14C]-FAs. Uptake of FAs was calculated as pmol of [14C]-FAs related to micrograms of protein per sample. The results are presented as percentage increase of [14C] fatty acid uptake over control (assigned as 100 %). Data are mean of three independent experiments performed in triplicates (n = 3) ± SEM. *p value <0.05 versus 5.5 mM glucose (control)
Effects of glucose on the mRNA expression of invasion and angiogenic factors
In order to understand the mechanism of glucose-induced tube formation, we measured the expression of invasion and angiogenesis growth factors, such as VEGFA, MMPs, and ANGPTL4. Among these, expression of MMP9 increased to 400 % (p < 0.05) when cells were treated with glucose (25 mM) compared to 5.5 mM glucose (control). The expression of MMP9 remained unaffected when the cells were challenged with 11 mM glucose. In contrast to MMP9, expression of VEGFA, MMP2, TIMP1, and TIMP2 remained insignificant (Fig. 5a). The expression of ANGPTL4 was decreased by 55 % at 25 mM glucose compared to 5.5 mM (p < 0.05) (Fig. 5b).
Effect of glucose on the mRNA expression of invasion and angiogenesis factors. Expression of mRNA was measured after the cells were pre-incubated with glucose (5.5, 11, 25 mM). The level of each mRNA expression was quantified after normalized with endogenous control, TBP, and calculated according to the ΔΔCt method. Percentage of changes in the level of mRNA expression was calculated based on control (glucose 5.5 mM) as 100 %. Results are mean of three independent experiments performed in triplicates (n = 3) ± SEM. *p value <0.05, where data are significantly different from 5.5 mM glucose (control)
Effect of glucose on MMP9 protein expression in HTR8/SVneo cells
In order to investigate the expression of MMP9 at protein level, HTR8/SVneo cells were pre-incubated with glucose (5.5, 11, and 25) for 24 h and harvested whole cell lysate for Western blotting. Figure 6a showed increased protein level for MMP9 with 25 mM glucose. Relative expression of MMP9 was increased significantly by ~60 % (mean density 0.28 ± 0.01 vs. 0.45 ± 0.02, p < 0.05) at 25 mM glucose as compared to 5.5 mM (Fig. 6b).
Effect of glucose on MMP9 expression in HTR8/SVneo cells. Cell lysates were prepared after treatment of HTR8/SVneo cells with glucose (5.5, 11, and 25). Western blot was performed for the expression of MMP9 as described in the methods. a MMP-9 protein signal and β-actin (internal control). The relative expression of MMP9 protein level was analyzed based on the density of the bands after normalized with β-actin (b). Values are mean of three independent experiments performed in duplicates (n = 3) ± SEM. *p value <0.05 versus 5.5 mM glucose (control)
Effects of glucose on the expression of fatty acid uptake and metabolic genes
Since pre-incubation of HTR8/Svneo cells with glucose (25 mM) stimulated fatty acid uptake, we, therefore, investigated the expression of genes related to fatty acid uptake, binding, and metabolic activities. Among these, expression of FABPpm, FABP4, and Cav1 was increased to 200, 152, and 166 %, respectively (p < 0.05) compared with those in controls (Fig. 7). However, expression of other intracellular fatty acid binding proteins such as FABP1, FABP3, FABP5 and fatty acid uptake and membrane transport proteins (FATP1-4,6, FAT, ACSL5, ADRP, DGAT1, LPIN1) remain unaffected (data not shown).
Effect of glucose on the expression of genes regulate fatty acid uptake and metabolism. Expression of mRNA was measured after the cells were pre-incubated with glucose (5.5, 11, 25 mM) for 24 h. Fold and percentage changes were expressed as described in Fig. 5. Data are mean of three independent experiments performed in triplicates (n = 3) ± SEM. *p value <0.05 versus 5.5 mM glucose (control)
Discussion
This paper reports for the first time that glucose (25 mM) activates the expression of pro-angiogenic factors such as MMP9, uptake of [14C]EPA, and expression of FABP4 in the first trimester trophoblast cells, HTR8/SVneo. All these positive modulatory factors of angiogenesis may be responsible for glucose-stimulated tube formation of these cells.
HTR8/SVneo tube-like formation reflects trophoblast migration and differentiation toward an invasive phenotype, a physiologic process that takes place during early human pregnancy [14]. This in vitro study raises the possibility that inappropriate glucose concentration might contribute to abnormal trophoblast migration and/or invasion, which are associated with major complications of pregnancy. Moreover, trophoblast invasion in vivo is controlled by angiogenic factors and accompanied by remodeling of extracellular matrix (ECM) by MMPs [15, 16]. MMP-2 and MMP-9 are the most important MMP enzymes produced by the cytotrophoblast during the first trimester of pregnancy, and their involvement in the success of extravillous trophoblast (EVT) functions, such as migration and invasion, has been well documented [17, 18]. Since MMP9 is a key molecule associated with cellular remodeling that involves trophoblast invasion and angiogenesis of the cells [19], therefore, selective activation of MMP9 over MMP2 without affecting MMP inhibitors could be the initial response under hyperglycemia in the trophoblast cells, HTR8/SVneo. This study also suggests that glucose regulates angiogenic factors that involved in EVT invasion and enzymes involved in the remodeling of the decidua by EVT during the first trimester of pregnancy, a crucial process for proper functioning of the maternal−fetal interface and trophoblast-mediated spiral artery remodeling of the decidua. Further, recent report suggests that altered MMP9 level could be the mediator in the development of insulin resistance and inflammation in pregnancies complicated with GDM [20]. In diabetes, placental morphology is altered since surface areas become enlarged due to hypervascularisation. Hyperglycemia induces thickening of the trophoblastic membrane with high amount of collagen deposition and increased surface area of the placenta that leads to alteration in the oxygen gradient across the placenta and creates local hypoxia in the maternal−placental−fetal axis. The resulting low oxygen level up-regulates expression of excess pro-angiogenic factors that leads to enhanced vascularization and endothelial cell proliferation and limited trophoblast invasion [19]. In the present study, higher expression of MMP9 and elevated tube formation in response to glucose challenge to the trophoblast cells could be the early response of the possible alteration of the trophoblast invasion, a key process that have been linked to the incidence of spontaneous abortion, pre-eclampsia, and intrauterine growth restriction associated with diabetes.
We demonstrated earlier that fatty acids stimulate tube formation by promoting the expression of angiogenic and invasive growth factors [9]. The LCFA, DHA stimulates maximum VEGF secretion in the first trimester trophoblast cells, HTR8/SVneo. It is not known if this attribute of DHA protects the first trimester trophoblast cells from the disintegration of the capillary tube formation induced by high amount of glucose (40 mM). Several biochemical pathways have been associated with hyperglycemia, including glucose-mediated increases in reactive oxygen species (ROS), diacylglycerol production, and the subsequent activation of the protein kinase C pathway flux through the polyol metabolic pathway, accumulation of advanced glycation end products and cytokine secretion [21]. DHA may protect one or more of these steps. Glucose- and fatty acid- mediated tube formation of the first trimester trophoblastic cells are not similar as fatty acid increased tube length threefold higher than glucose at their respective potent dose. VEGF and ANGPTL4 are the prominent angiogenic growth factors which are up-regulated by fatty acids in HTR8/SVneo cells [9]. Unlike fatty acids, glucose did not alter expression of VEGFA in these cells. VEGF-independent induction was evidenced with leptin- and CTGF-induced tube formation of the first trimester trophoblast cells [22, 23].
We observed a dose-dependent increase in the tube formation as well as cellular viability and proliferation of the HTR8/SVneo cells up to 25 mM of glucose. One could argue that 25 mM glucose is much higher than the physiological level (5.5 mM), however, several in vitro studies including HTR8/SVneo cells were reported using similar or higher glucose concentrations [24–27]. Considering the fact that in vitro cell culture routinely uses growth media containing glucose much higher than the physiological level (see “Cell culture” section), a dose of 25 mM of glucose may expose cells reasonably higher glucose concentration under in vitro conditions. While high level of glucose (50 mM) altered the angiogenic profiles of HTR8/SVneo cells [25], we, however, observed decreased tube formation beyond 40 mM glucose in these cells. Experimental conditions were different in terms of glucose dose and duration. In our study, HTR8/SVneo cells were pre-starved for 48 h prior (pre-requisite for tube formation) to glucose treatment that could favor instant glucose utilization by the cells to compensate the energy-intensive tube formation. Moreover, glucose treatment was restricted to 16 h (short term) as compared to 3–4 days (long term) in their study.
Glucose (25 mM) stimulated the uptake of [14C]EPA in these cells. EPA is the precursor of three series of prostaglandins and an inducer of tube formation in these cells [9], suggesting that glucose-induced tube formation could be facilitated by an increased [14C]EPA uptake. EPA increases glucose uptake in myotubes [28]. Increased uptake of [14C]EPA by glucose may be regulated by altered ANGPTL4 expression in these cells. ANGPTL4 is altered by high glucose in retinal epithelial cells [29]. Since ANGPTL4 inhibits fatty acid uptake by lowering plasma level of free fatty acid by inhibiting LPL activity, it is possible that this would augment the uptake of exogenously added free fatty acids in the cellular system [30]. The lower ANGPTL4 expression couples with increased fatty acid uptake ([14C]EPA) and expression of fatty acid metabolic genes might increase the availability of free fatty acids for cellular uptake and metabolism by these cells. Further work on ANGPLT4 secretion and fatty acid oxidation in the presence of glucose is required for definitive conclusions. Glucose (25 mM) stimulated expression of both intracellular (FABP4) and membrane-associated (FABPpm) fatty acid binding proteins. FABP4 is being increasingly established to be an intracellular mediator of angiogenesis [31, 32]. Increased expression of the FABPs may explain increased accumulation of fatty acids under high glucose levels. All these findings are crucial to understand the possible effects of hyperglycemia in the metabolism of first trimester trophoblast cells.
To our knowledge, this is the first report to demonstrate a selective activation of MMP9, a key invasive factor in the first trimester trophoblast cells, HTR8/SVneo when exposed to glucose (25 mM). Glucose (25 mM)-induced tube formation with concomitant increase in the uptake of [14C]EPA and expression of FABP4 may contribute to angiogenic and metabolic activities of these cells. DHA protects capillary tubular network disintegration of the HTR8/SVneo cells induced by high glucose more efficiently than EPA.
All of these aspects require further investigation possibly with primary trophoblast from the first trimester placenta.
References
Hill JA (2001) Maternal-embryonic cross-talk. Ann NY Acad Sci 943:17–25
Desoye G, Hauguel-de Mouzon S (2007) The human placenta in gestational diabetes mellitus: the insulin and cytokine network. Diabetes Care 30:S120–S126. doi:10.2337/dc07-s203
Torry DS, Torry RJ (1997) Angiogenesis and the expression of vascular endothelial growth factor in endometrium and placenta. Am J Reprod Immunol 37:21–29
Staun-Ram E, Shalev E (2005) Human trophoblast function during the implantation process. Reprod Biol Endocrinol 3:56. doi:10.1186/1477-7827-3-56
Pinter E, Haigh J, Nagy A, Madri JA (2001) Hyperglycemia-induced vasculopathy in the murine conceptus is mediated via reductions of VEGF-A expression and VEGF receptor activation. Am J Pathol 158:1199–1206. doi:10.1016/S0002-9440(10)64069-2
Yang P, Zhao Z, Reece EA (2008) Blockade of c-Jun N-terminal kinase activation abrogates hyperglycemia-induced yolk sac vasculopathy in vitro. Am J Obstet Gynecol 198:321.e1–321.e7. doi:10.1016/j.ajog.2007.09.010
Belkacemi L, Lash GE, Macdonald-Goodfellow SK, Caldwell JD, Graham CH (2005) Inhibition of human trophoblast invasiveness by high glucose concentrations. J Clin Endocrinol Metab 90:4846–4851. doi:10.1210/jc.2004-2242
Duttaroy AK (2009) Transport of fatty acids across the human placenta: a review. Prog Lipid Res 48:52–61. doi:10.1016/j.plipres.2008.11.001
Johnsen GM, Basak S, Weedon-Fekjaer MS, Staff AC, Duttaroy AK (2011) Docosahexaenoic acid stimulates tube formation in first trimester trophoblast cells, HTR8/SVneo. Placenta 32:626–632. doi:10.1016/j.placenta.2011.06.009
Basak S, Duttaroy AK (2013) Effects of fatty acids on angiogenic activity in the placental extravillious trophoblast cells. Prostaglandins Leukot Essent Fatty Acids 88:155–162. doi:10.1016/j.plefa.2012.10.001
Basak S, Duttaroy AK (2013) cis-9, trans-11 conjugated linoleic acid stimulates expression of angiopoietin like-4 in the placental extravillous trophoblast cells. Biochim Biophys Acta 1831:834–843. doi:10.1016/j.bbalip.2013.01.012
Jauniaux E, Hempstock J, Teng C, Battaglia FC, Burton GJ (2005) Polyol concentrations in the fluid compartments of the human conceptus during the first trimester of pregnancy: maintenance of redox potential in a low oxygen environment. J Clin Endocrinol Metab 90:1171–1175. doi:10.1210/jc.2004-1513
Desoye G, Gauster M, Wadsack C (2011) Placental transport in pregnancy pathologies. Am J Clin Nutr 94:1896S–1902S. doi:10.3945/ajcn.110.000851
Waddell JM, Evans J, Jabbour HN, Denison FC (2011) CTGF expression is up-regulated by PROK1 in early pregnancy and influences HTR-8/Svneo cell adhesion and network formation. Hum Reprod 26:67–75. doi:10.1093/humrep/deq294
Murray MJ, Lessey BA (1999) Embryo implantation and tumor metastasis: common pathways of invasion and angiogenesis. Semin Reprod Endocrinol 17:275–290. doi:10.1055/s-2007-1016235
Jovanović M, Stefanoska I, Radojčić L, Vićovac L (2010) Interleukin-8 (CXCL8) stimulates trophoblast cell migration and invasion by increasing levels of matrix metalloproteinase (MMP)2 and MMP9 and integrins α5 and β1. Reproduction 139:789–798. doi:10.1530/REP-09-0341
Lockwood CJ, Oner C, Uz YH, Kayisli UA, Huang SJ, Buchwalder LF, Murk W, Funai EF, Schatz F (2008) Matrix metalloproteinase 9 (MMP9) expression in preeclamptic decidua and MMP9 induction by tumor necrosis factor alpha and interleukin 1 beta in human first trimester decidual cells. Biol Reprod 78:1064–1072. doi:10.1095/biolreprod.107.063743
Monsonego-Ornan E, Kosonovsky J, Bar A, Roth L, Fraggi-Rankis V, Simsa S, Kohl A, Sela-Donenfeld D (2012) Matrix metalloproteinase 9/gelatinase B is required for neural crest cell migration. Dev Biol 364:162–177. doi:10.1016/j.ydbio.2012.01.028
Luo J, Qiao F, Yin X (2011) Hypoxia induces FGF2 production by vascular endothelial cells and alters MMP9 and TIMP1 expression in extravillous trophoblasts and their invasiveness in a cocultured model. J Reprod Dev 57:84–91
Lappas M (2014) NOD1 expression is increased in the adipose tissue of women with gestational diabetes. J Endocrinol 222:99–112. doi:10.1530/JOE-14-0179
Leach L, Taylor A, Sciota F (2009) Vascular dysfunction in the diabetic placenta: causes and consequences. J Anat 215:69–76. doi:10.1111/j.1469-7580.2009.01098.x
Das MK, Basak S, Ahmed MS, Attramadal H, Duttaroy AK (2014) Connective tissue growth factor induces tube formation and IL-8 production in first trimester human placental trophoblast cells. Eur J Obstet Gynecol Reprod Biol 181C:183–188. doi:10.1016/j.ejogrb.2014.07.045
Basak S, Duttaroy AK (2012) Leptin induces tube formation in first-trimester extravillous trophoblast cells. Eur J Obstet Gynecol Reprod Biol 164:24–29. doi:10.1016/j.ejogrb.2012.05.033
Fragiadaki M, Hill N, Hewitt R, Bou-Gharios G, Cook T, Tam FW, Domin J, Mason RM (2012) Hyperglycemia causes renal cell damage via CCN2-induced activation of the TrkA receptor: implications for diabetic nephropathy. Diabetes 61:2280–2288. doi:10.2337/db11-1138
Han CS, Thung SF, Nickless N, Lockwood CJ, Abrahams VM (2012) Excess glucose levels limit first trimester trophoblast migration and induce an anti-angiogenic profile. In: 32nd Annual meeting of the Society for Maternal-Fetal Medicine the pregnancy meeting 32nd Annual Scientific Meeting 206. 246:doi:10.1016/j.ajog.2011.10.264
Li C, Ren Y, Jia X, Liang P, Lou W, He L, Li M, Sun S, Wang H (2012) Twist overexpression promoted epithelial-to-mesenchymal transition of human peritoneal mesothelial cells under high glucose. Nephrol Dial Transplant 27:4119–4124. doi:10.1093/ndt/gfs049
Li W, Ma Q, Li J, Guo K, Liu H, Han L, Ma G (2011) Hyperglycemia enhances the invasive and migratory activity of pancreatic cancer cells via hydrogen peroxide. Oncol Rep 25:1279–1287. doi:10.3892/or.2011.1150
Figueras M, Olivan M, Busquets S, López-Soriano FJ, Argilés JM (2011) Effects of eicosapentaenoic acid (EPA) treatment on insulin sensitivity in an animal model of diabetes: improvement of the inflammatory status. Obesity (Silver Spring) 19:362–369. doi:10.1038/oby.2010.194
Yokouchi H, Eto K, Nishimura W, Takeda N, Kaburagi Y, Yamamoto S, Yasuda K (2013) Angiopoietin-like protein 4 (ANGPTL4) is induced by high glucose in retinal pigment epithelial cells and exhibits potent angiogenic activity on retinal endothelial cells. Acta Ophthalmol 91:e289–e297. doi:10.1111/aos.12097
Georgiadi A, Lichtenstein L, Degenhardt T, Boekschoten MV, van Bilsen M, Desvergne B, Müller M, Kersten S (2010) Induction of cardiac Angptl4 by dietary fatty acids is mediated by peroxisome proliferator-activated receptor beta/delta and protects against fatty acid-induced oxidative stress. Circ Res 106:1712–1721. doi:10.1161/CIRCRESAHA.110.217380
Basak S, Das MK, Duttaroy AK (2013) Fatty acid-induced angiogenesis in first trimester placental trophoblast cells: possible roles of cellular fatty acid-binding proteins. Life Sci 93:755–762. doi:10.1016/j.lfs.2013.09.024
Elmasri H, Ghelfi E, Yu C-w, Traphagen S, Cernadas M, Cao H, Shi G-P, Plutzky J, Sahin M, Hotamisligil G, Cataltepe S (2012) Endothelial cell-fatty acid binding protein 4 promotes angiogenesis: role of stem cell factor/c-kit pathway. Angiogenesis 15:457–468. doi:10.1007/s10456-012-9274-0
Acknowledgments
We are grateful to Aud Jørgensen for her technical assistance. This study was supported by grant from the Thune Holst Foundation.
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Basak, S., Das, M.K., Srinivas, V. et al. The interplay between glucose and fatty acids on tube formation and fatty acid uptake in the first trimester trophoblast cells, HTR8/SVneo. Mol Cell Biochem 401, 11–19 (2015). https://doi.org/10.1007/s11010-014-2287-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-014-2287-9