Abstract
Therapeutic responses of most drugs are initiated by the rate and degree of binding to their receptors or targets. The law of mass action describes the rate of drug-receptor complex association (kon) and dissociation (koff) where the ratio koff/kon is the equilibrium dissociation constant (Kd). Drugs with slow reversible binding (SRB) often demonstrate delayed onset and prolonged pharmacodynamic effects. This report reviews evidence for drugs with SRB features, describes previous pharmacokinetic/pharmacodynamic (PK/PD) modeling efforts of several such drugs, provides a tutorial on the mathematics and properties of SRB models, demonstrates applications of SRB models to additional compounds, and compares PK/PD fittings of SRB with other mechanistic models. We identified and summarized 52 drugs with in vitro-confirmed SRB from a PubMed literature search. Simulations with a SRB model and observed PK/PD profiles showed delayed and prolonged responses and that increasing doses/kon or decreasing koff led to greater expected maximum effects and a longer duration of effects. Recession slopes for return of responses to baseline after single doses were nearly linear with an inflection point that approaches a limiting value at larger doses. The SRB model newly captured literature data for the antihypertensive effects of candesartan and antiallergic effects of noberastine. Their PD profiles could also be fitted with indirect response and biophase models with minimal differences. The applicability of SRB models is probably commonplace, but underappreciated, owing to the need for in vitro confirmation of binding kinetics and the similarity of PK/PD profiles to models with other mechanistic determinants.
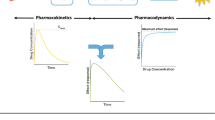
Graphical abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The pharmacological responses of most drugs are initiated by binding to its receptor or target. To translate the receptor binding into clinical outcomes, many factors need to be considered: drug concentrations at the target site, type of drug-receptor interaction, and receptor activation and transduction processes [1]. The term receptor or target here represents any biological entity that interacts with a drug, including enzymes, ion channels, carrier transporters, DNA, and structures in the nucleus producing ensuing biological responses. Most of the time, binding events occur rapidly so that the receptor-bound drug complex is in constant equilibrium with the free drug at the effect site. In this case, drug-receptor interaction is quantified by receptor affinity and IC50, Ki, or Kd values determined from affinity-based measurements can be used to provide insight into the drug potency, which is also known as the drug thermodynamic selectivity [2]. However, when drug-receptor interaction does not equilibrate instantly, binding kinetics should be considered in accounting for the time-dependent changes in receptor engagement. Various conditions can cause the lack of and variability in equilibration, such as limited accessibility of the receptor binding site, limited conformational flexibility of the receptor, and hydrogen bonds for drug-receptor interaction being shielded by surrounding hydrophobic regions [3]. Under these circumstances, drug efficacy is influenced by the association rate constant (kon), which primarily governes the time for drug to bind to the receptor, and the dissociation rate constant (koff), which mainly determines the duration of receptor occupancy. Thus, even for drugs with similar IC50 values for their targets, if their kon and koff values differ, they may still have different response profiles, which is known as kinetic selectivity [2].
For drugs with Slow Reversible Binding (SRB), the duration of drug action can be determined by the dissociation half-life (0.693/koff) or residence time (1/koff) in addition to its pharmacokinetics. Drug dissociation half-lives can vary from seconds to hours or even days. Long dissociation half-lives often result in prolonged drug action and maximized efficacy [4, 5]. For example, tiotropium is an inhaled long-acting muscarinic acetylcholine receptor antagonist in the management of chronic obstructive pulmonary disease [6]. In a radioligand binding study, tiotropium showed slow dissociation kinetics to human muscarinic receptors with a dissociation half-life of 7.7 h, which is longer than the older antimuscarinic ipratropium (0.17 h) [7]. The SRB of tiotropium explains its long duration of action of 24 h, compared to less than 6 h for ipratropium [7]. This allows less frequent administration and higher trough efficacy for tiotropium than ipratropium [8]. Compared to fast kinetic drugs, drugs with SRB may be more vulnerable to target-based toxicity. This can be evidenced with antipsychotic agents with different koff from D2 dopamine receptors. Typical antipsychotic agents, such as nemonapirde, spiperone, and haloperidol, have high affinities to D2 receptors with long dissociation half-lives (5.92 h, 3.33 h, and 0.67 h, respectively), and are often associated with severe extrapyramidal motor side effects and prolactin elevation [9]. Atypical antipsychotic agents such as clozapine and quetiapine, however, are free from these side effects and show less D2 receptor affinity with dissociation half-lives less than 0.5 min. This may be explained by the fact that when endogenous dopamine increases, drugs like clozapine can rapidly dissociate from the receptor to provide more access to the dopamine surge and thereby reduce the chance of extrapyramidal side effects and prolactin elevation [9]. Thus, drug binding kinetics, especially for those with slow dissociation, can shape the dose–response relationship by influencing the efficacy, duration of action, and safety [1, 10].
The concept of SRB was noticed by Fuseau and Sheiner in 1984, where nonequilibrium between the drug concentration at the effect site and receptor was considered as a violation of the assumption of an effect compartment model [11]. In 1996, Shimada et al. applied a SRB model to delineate the antihypertensive effects of eight calcium channel blockers [12]. These drugs exhibited long-lasting antihypertensive effects compared to their short plasma elimination half-lives. The delay between plasma concentrations and effects usually produced counterclockwise hysteresis. The delayed effects were captured by incorporating drug association and dissociation rates in the “ion-channel binding model” under the assumption that the pharmacological effect was directly proportional to the concentration of the drug-receptor complex. In addition to the model fitting, the estimated Kd values (ratio of koff /kon) were well correlated with those obtained from in vitro binding studies.
The implications of binding kinetics in drug discovery and lead optimization have been partly reviewed previously [2, 4, 5, 13, 14]. Copeland and Swinney both addressed the importance of obtaining these rate constants as they can provide additional insights on drug-target potency compared to traditional affinity parameters [5, 13]. Drugs with different dissociation half-lives were pointed out to demonstrate the relation of dissociation rate and drug efficacy [4, 5, 13]. Dahl et al. examined the combined effect of PK and binding kinetics on the duration of drug efficacy [14]. Most drugs have a longer elimination half-life than koff half-life.
This report reviews and evaluates PK/PD models of SRB. We provide a review of the literature on drugs with SRB. Since drugs with target-mediated drug disposition (TMDD) demonstrate much more complex PK/PD, they were not included in the current review. A basic SRB model is provided with mathematical derivations of key graphical properties and simulations with signature profiles to describe the effects of dose, kon, koff, Emax and elimination rate constant (kel) values on response patterns. Additional demonstrations of model applications to two drugs and their effects illustrate principles of data analysis. Finally, a comparison of the SRB with other basic mechanistic models is provided.
Theoretical
The SRB model (Fig. 1) is based on the classical receptor occupancy theory and the law of mass action [15] with the assumption that the effect of drug (∆E) is proportional and directly linked to the concentration of the drug-receptor complex (RC). In addition, the model assumes that the delay of response is due to the rate of drug binding to (kon) or dissociating from (koff) the receptors. The total number of receptors (Rt) is assumed to remain constant. The model also assumes that drug concentration at the target site (Ct) is proportional to the plasma drug concentration (Cp) and is in excess compared to receptor concentration.
Accordingly, the rate of change of RC is:
with an initial condition of
where Rt is the total receptor content, Ct is the free drug concentration at the target site, kon is a second-order association constant, and koff is a first-order dissociation constant. Free receptors (R) are equal to Rt–RC.
Since the pharmacological effect of drug is assumed to be proportional to the RC concentration, Ct is proportional to the plasma drug concentration (Cp), and the maximum effect (Emax) is obtained at RC = Rt. The relationship between drug effect and Cp can be defined as:
with an initial condition of
Thus drug effect as ∆E/Emax corresponds to receptor occupancy (RC/Rt). This assumes that the drug is a full agonist. If the mechanism is for a partial agonist or a system with spare receptors, there may exist a more complex proportionality.
When the effect reaches its peak, \(\frac{dE}{{dt}} =\) 0, the observed maximum effect (∆Em) can be expressed as:
where Cm is the plasma concentration when ∆Em is reached (Cm > 0). Since the equilibrium dissociation constant (Kd) = koff/kon, Eq. 5 can be rearranged as:
Therefore, at a high dose level, Cm is high, which leads to ∆Em closer to Emax. If Cm >> Kd, then ∆Em = Emax.
Pharmacodynamic parameter estimations
The following study design is advisable to fully illustrate a PK/PD model of SRB for PD parameter estimation: (1) drug is administered at two or more dose levels; (2) one of the doses should lead to Cmax much higher than Kd (around 10 times higher); (3) the baseline and/or placebo effects over time should be evident and constant.
Based on Eq. 6, the initial estimation of Emax can be obtained from the peak effect at the highest dose.
To obtain the initial estimation of kon, the initial slope (SI) from the effect versus time curve can be obtained. Since at the initial phase,
Using the concentration at the midpoint of the slope (Cmid), kon can be obtained as
Based on Eq. 5, an initial estimation of koff can be obtained from the ∆Em at a dose other than the highest dose, with Cm substituted by the maximum or initial plasma concentration (Cmax or C0):
Due to the non-linearity and time-dependency of the SRB model, the final parameters should be obtained based on fitting the PK/PD model equations using nonlinear least-squares regression analysis.
Methods
Data
Data from the literature were used in the present report. A literature search was performed in PubMed using the keywords “((slow binding kinetics) OR (slow dissociation)) AND (drug)”. In addition, references from published articles were traced. The mean values of PK/PD data from the publications were digitalized by WebPlotDigitizer (Version 4.5, https://automeris.io/WebPlotDigitizer). Thus, the estimated PK/PD parameters should be considered approximate.
Data analysis
The PK and PK/PD data were analyzed sequentially. The mean values of the plasma concentrations were first fitted to an appropriate PK model. The PK parameters were then fixed to obtain the plasma concentrations that drive the PD. The PD data were then fitted with the SRB model (Eqs. 3 and 4) to obtain kon, koff, and Emax. All data fitting and simulations were performed in NONMEM, version 7.4.1 (Sample model code is provided in Supplemental Materials). The proportional error model and the first-order conditional estimation method with interaction (FOCEI) were used. No interindividual variability was considered since mean values were used. The goodness-of-fit was assessed by the Akaike Information Criterion (AIC), residual error, precision (CV%) of the parameters, and visual check of the fitted curves.
Results
Literature review of drugs with slow binding kinetics
Literature search using PubMed resulted in 3443 articles (last accessed in April 2022). Although there is no clear demarcation between fast and slow binding kinetics, drugs with dissociation half-lives longer than 10 min (0.17 h) are considered SRB drugs in the current report and their in vitro binding kinetics, efficacy parameters, and plasma elimination half-lives are summarized in Table 1. These drugs have a variety of therapeutic indications with many of them from sartans, antihistamines, and antivirals. Several drugs demonstrated extremely long dissociation half-lives, such as darunavir (247 h) and dolutegravir (71 h), which explains their potent activities [16, 17]. Many slow binding drugs have long elimination half-lives, which was observed by Dahl et al. [14].
Sources of binding parameters
The drug dissociation rates for these drugs are generally determined by preincubation of radiolabeled drugs with receptors followed by measuring the time-course of the receptor binding under wash-out conditions [18]. The wash-out medium is usually supplied with an excess of unlabeled competitive ligands to replace the binding of radiolabeled drugs to the receptors. The koff can be obtained by fitting the percentage of receptor binding versus time (t) plot as:
Association rates of drugs can be directly measured by the time-course of binding of radiolabeled drugs to the receptors [19]. The percentage receptor binding versus time curve can be first fitted by:
to obtain the pseudo-first-order rate constant (kobs). Then kon can then be obtained based on:
where [D] is the radiolabeled drug concentration used for measuring receptor binding. The kon can also be determined in competitive association experiments, where only unlabeled drugs are required to co-incubate with competitive radiolabeled ligands using the Motulsky–Mahan model [20]. Several antihistamines, muscarinic receptor antagonists and antipsychotics were measured in this way [7, 21, 22]. Biosensor-based studies or surface plasmon resonance (SPR) technology has been applied to analyze the binding kinetics of antivirals, such as darunavir and atazanavir [16, 23]. It can measure the kon and koff and requires only a small amount of drug without radiolabeling. The drug affinity values (IC50/Ki) summarized in Table 1 are usually higher than Kd, suggesting the underprediction of drug affinity using IC50/Ki values for SRB drugs. Lastly, the value of kon can be determined from kon = koff/Kd, once the latter two have been assessed.
Previous SRB modeling
Although many drugs with SRB have been reported, only few studies applied SRB models to describe the PK/PD (Table 2). Besides the application by Shimada et al. [12], the SRB model was applied to describe the inotropic response of digoxin in rats [24]. The model well-captured the digoxin PD after bolus dose and in concentration—clamp experiments. The SRB model was applied in analyzing the anti-secretory effects of several gastric acid pump inhibitors in dogs and humans [25, 26]. One of these, H 335/25, showed rapid onset but delayed effects compared to its PK [25]. The delayed effects were captured by the SRB model and further compared with fittings using biophase and indirect response models. The SRB model was considered superior based on the Akaike Information Criterion. In addition, a SRB model was combined with a biophase model to describe the antinociceptive and respiratory depressant effects of buprenorphine in rats and humans [27,28,29,30]. In these studies, concentrations of buprenorphine at an effect site but not in plasma were assumed to form the drug-receptor complex to exert pharmacological effects.
Model simulations
To evaluate the expected properties of the SRB model, the response profiles for a theoretical drug with mono-exponential kinetics and a range of doses were simulated as shown in Fig. 2. The drug is assumed to have clearance (CL) = 20 L/h and volume of distribution (V) = 80 L after bolus intravenous (IV) doses of 0.1, 0.2, 0.5, 1, and 2 mg. The PD parameters of the drug were: baseline Ebl = 20, Emax = 10, kon = 0.125 L/µg·h, and koff = 0.125 /h. The observed effects E = Ebl−∆E were generated with no relative standard error.
Simulated PD effects (solid line) of a hypothetical drug with slow reversible binding following single bolus IV administration at doses of 0, 0.1, 0.2, 0.5, 1, and 2 mg. The corresponding PK profiles are shown as dashed lines. Values of CL = 20 L/h, V = 80 L, baseline Ebl = 20, Emax = 10, kon = 0.125 L/µg·h, and koff = 0.125 /h were used for simulations. The observed effect = Ebl − ∆E
As doses increased, the overall size of the response profile increased with a rapid initial decline, a plateau at the peak or nadir, and a return to baseline that was nearly linear and parallel at larger doses. The Em and SI increased with the time to reach Em (tEm) shifting to earlier times (at 5.1, 4.8, 3.9, 2.9, and 2 h from low to high doses). Thus, at higher dose levels, a lesser delay in onset of effects is expected.
The explicit formula for area between the baseline and effect curve (ABEC) is:
as shown by derivations in the Supplemental Materials.
Thus, ABEC is expected to increase in proportion to Emax, 1/kel, and the log of the dose at higher value This has similar determinants as the ABEC of direct and indirect response models [31, 32]. By substituting Cm with the initial concentration (C0) of 1.25, 2.5, 6.2, 12.5, and 25 µg/L from 5 doses in Eq. 6, the resulting effects were 4.67, 6.51, 8.38, 9.17, and 9.59, which were close to the Em of 2.57, 4.31, 7.02, 8.57, and 9.39. Thus, Em can be obtained based on Eq. 6 with either C0 or Cmax.
Response profiles were also generated for a dose of 0.5 mg with changes in kon (0.0125, 0.025, 0.125, 0.625, and 1.25 L/µg·h) or koff (0.0125, 0.025, 0.125, 0.625, and 1.25 /h) as demonstrated in Fig. 3. When kon increased, the Em and SI increased with tEm shifting to an earlier time. Decreasing koff led to increase in Em and a later tEm but without change in SI. The profiles for the SRB become particularly distinctive when koff is much smaller than kel producing, as expected, a prolonged duration of responses (also see Supplementary Fig. 2).
Simulated PD profiles of drug with indicated kon or koff values following a single bolus IV dose of 0.5 mg. The PK and other parameters used for simulations were the same and held constant as those in Fig. 2. Note that the kel was assumed to be 0.25 1/h
The effects of Emax and kel on the PK/PD profiles for a dose of 0.5 mg were further evaluated. With increased Emax, the Em and SI increased with the tEm remaining constant (Supplementary Fig. 1). The recession slopes (Sfp) were directly proportional to Emax values. Decreasing kel (2.5, 1.25, 0.5, 0.05, and 0.025 /h) by changing CL to 200, 100, 20, 4, and 2 L/h resulted in an increased Em and a later tEm and without changes in SI values (Supplementary Fig. 2). The recession slopes increased with lower kel but decreased at higher kel values.
The pharmacodynamic profiles of the SRB model showed a single inflection point during the recession phase. The slope at the inflection point (Sfp) was derived and is fully determined by the kon, koff, kel, Emax, concentration at the inflection point (Cfp), and effect at the inflection point (∆Efp) (Supplementary Materials). However, it was found that Cfp approaches a limiting value as the dose becomes very large. This results in a limiting value for Sfp so that the recession slopes are parallel at larger doses (Supplementary Fig. 3). In addition, it can be noted that the occurrence of Cfp becomes closer to Kd in the effect curve when koff >> kel (Supplementary Fig. 4).
When koff becomes very large, the SRB model will behave like a simple direct effect model as drug-receptor binding essentially equilibrates instantly. The ratio of Sfp/koff is an upper bound for the difference between these two models (derivation provided in Supplementary Materials). Thus, after normalizing with the effect, the quotient \((S_{fp} /k_{off} )/\left( {E_{0} - E_{max} } \right) \) can serve as a metric to examine the convergence of a SRB to a direct effect model (Supplementary Fig. 5). When koff is larger than 4, corresponding to a dissociation half-life shorter than 10 min, \((S_{fp} /k_{off} )/\left( {E_{0} - E_{max} } \right) \) is close to zero, suggesting the convergence of the SRB to the direct effect model. Therefore, the SRB should be considered for drugs with a dissociation half-life longer than 10 min; otherwise, a simple direct effect model can be applied. A consequence of convergence of the SRB model to the simple direct model for large koff is that Cfp, ∆Efp, and Sfp are converging to the values reported for the latter model elsewhere [33]. Hence, Cfp becomes close to Kd, ∆Efp close to Emax/2 and Sfp close to kel·Emax/4.
Clinical PK/PD examples of SRB applications
Sartans
Sartans are orally active angiotensin II receptor type 1 (AT1) antagonists used for the treatment of hypertension and related diseases [34]. A number of sartans are frequently used in clinical therapy, including candesartan, olmesartan, telmisartan, valsartan, irbesartan, and losartan. Although they share a common binding site, their binding kinetics differ, which results in different binding potency and clinical effects. Losartan showed a surmountable antagonism phenomenon in an in vitro study, which is typical for fast-dissociating antagonists [35]. Most sartans, such as candesartan, olmesartan, telmisartan, valsartan, and irbesartan, produced partial depression of the maximal response in the in vitro study, which is known as insurmountable antagonism [19, 34, 36]. Such behaviors are largely due to their slow dissociation from AT1 receptors, especially for candesartan with a dissociation half-life of 3.25 h in the radioligand binding study [18]. Comparison of clinical studies showed that sartans with slow dissociation, such as valsartan, olmsartan and candesartan, had higher maximal effects on blood pressure than losaratan, which has a fast dissociation rate [5].
Candesartan cilexetil (TCV-116) is the esterified prodrug of candesartan and has been approved in many countries to treat hypertension [37]. Absorbed candesartan cilexetil is presumed to be completely metabolized to candesartan to exert pharmacological actions [38]. Delacrétaz et al. evaluated the inhibitory effect of candesartan on blood pressure after oral administration of candesartan cilexetil at 1, 2, 4, and 8 mg in healthy volunteers [39]. At 45 min before candesartan cilexetil or placebo administration, an IV bolus injection of angiotensin II at pre-established doses was given to increase the systolic blood pressure (SBP) by 31.1 mm Hg on average, which was considered as the baseline response. The plasma concentration of candesartan and change in SBP after drug intake were monitored. The plasma PK of candesartan following four oral doses were captured jointly by a one-compartment model with first-order absorption and elimination (Fig. 4). The PD of candesartan were assessed from the increase of SBP after angiotensin II challenge, which were back-calculated from the percent of baseline response in the published plot using the baseline response (BASL) of 31.1 mm Hg. The responses in the placebo group were described by a modified inverse Bateman function [40, 41]:
PK/PD profiles of candesartan on systolic blood pressure (SBP) after single oral administration of either candesartan cilexetil at the indicated doses or placebo in healthy volunteers. A one-compartment PK model with first-order absorption and elimination and SRB model as shown in Fig. 1 was applied. Symbols depict data calculated from Delacrétaz et al. [39], and lines are fitted responses. Parameters are presented in Table 3
where DREC is the amplitude of placebo effect and kep is the rate constant for the associated placebo effect.
The PD effects of candesartan were obtained by:
where ∆E was based on the operation of SRB model (Eqs. 3 and 4). The parameters for describing placebo effects were fixed during the model fitting of PD profiles of candesartan at four dose levels (Fig. 4). The PK and PD parameters after model fitting are listed in Table 3. The estimated kon = 0.0142 L/µg·h (12.9% CV) and Emax = 33 mm Hg (25.8% CV) demonstrated reasonable precision. The estimated koff was 0.277 1/h (62.5% CV), which translates to a dissociation half-life of around 2.5 h. This is close to the dissociation half-life of 3.25 h determined in the in vitro study [18].
H1-Antihistamines
H1-antihistamines are first-line treatments for allergic rhinoconjunctivitis and urticaria [42]. They target histamine, the major pathogenic mediator of allergic disorders, by binding to H1-receptors to reduce the constitutive activity of the receptor and block the binding of histamine to the receptor [43]. The first-generation antihistamines, such as chlorpheniramine, diphenhydramine, hydroxyzine, and ketotifen, demonstrated central nervous system (CNS) penetration that resulted in sedation and interference with the cognitive process [43]. The second-generation antihistamines overcome the CNS side effects with improved selectivity and tolerability. These include acrivastine, astemizole, cetirizine, ebastine, levocabastine, mizolastine, noberastine and terfenadine [44]. The in vitro receptor binding studies revealed the slow dissociation from the H1-receptor for several antihistamines, such as astemizole, cetirizine, fexofenadine, loratadine, levocetirizine, mequitazine, noberastine, and terfenadine [45, 46]. This may contribute to the delayed onset and prolonged pharmacological actions of antihistamines observed in clinical studies [43, 47].
Noberastine is a second-generation non-sedating antihistamine. The PK/PD profiles of noberastine at single oral doses of 10, 20, and 30 mg in healthy volunteers were published by Wood-Baker et al. [48]. The plasma concentrations of noberastine were fitted using a two-compartment model with zero-order absorption and first-order elimination (Fig. 5). The PD responses of noberatine were assessed by the wheal diameters caused by histamine skin prick testing. One hour before drug administration, the baseline skin prick testing was performed to get the baseline wheal diameter. After drug administration, wheal diameters at designated intervals remained at similar levels to baseline in the placebo group and were inhibited in the noberastine treatment groups. Thus, the observed wheal diameters were described by
PK/PD profiles of noberastine on histamine induced wheal diameter after single oral doses as indicated or placebo in healthy volunteers. A two-compartment PK model with zero-order absorption and first-order elimination and SRB model as shown in Fig. 1 was applied. Symbols depict the observed data from Wood-Baker et al. [48], and lines are fitted responses. Parameters are presented in Table 4
where BASL was the baseline level and ∆E was based on the operation of SRB model (Eqs. 3 and 4). The parameters after model fitting are listed in Table 4. The zero-absorption rate was fixed to 30 mg/h since the data points in the absorption phase are limited. The PD profiles at all dose levels were well captured by the SRB model with good precision (1.9 to 7.3% CV) (Fig. 5). The dissociation half-life calculated based on the estimated koff of 0.203 1/h was 3.41 h, which is close to the dissociation half-life of 2.75 h measured in an in vitro study [45].
Comparison of SRB model with indirect response and biophase models
In addition to the SRB model, we fitted the PD data of candesartan and noberastine with indirect response model I and the biophase model. The data can be captured by all three models with their fitted curves close to each other (Figs. 6 and 7). The very similar predictions from the three models were also observed for describing the effects of the gastric acid pump inhibitor, H 335/25, by Äbelö et al. [25]. However, one of the noticeable differences between the three models is that the peak or nadir effect is reached earlier with increasing doses for the SRB model; indirect response models exhibit peak or nadir effects later with increasing doses; and biophase models produce the time to peak or nadir effects that are constant for all doses. The PD plots of candesartan and noberastine both demonstrated an earlier nadir at higher doses, suggesting that the SRB model may be more appropriate. In addition, the SRB model showed the lowest AIC with acceptable variability for the two drugs (Tables 5 and 6). The biophase model for candesartan showed the poorest precision of estimated parameters (CV > 71.6%). Therefore, the SRB model was superior to the other two models for the current PK/PD data for candesartan and noberastine. However, the differences between the three models are minimal. This may also result from the similar plasma elimination rates and dissociation rates for candesartan and noberastine, which will retain the return phase of the PD plots. Even when elimination rate is comparable or slower to the dissociation rate, the time to reach to peak or nadir effect are earlier at higher doses still hold true for SRB model. Thus, high quality data from a wide range of dose levels are required to differentiate the model type in performing fittings.
Model fittings for the effects of candesartan on systolic blood pressure in humans by the slow binding model (solid line), indirect response model I (broken line), and biophase model (dotted line). The data generated from Delacrétaz et al. [36] are shown as solid circles
Model fittings for the effects of noberastine on histamine induced wheal diameter in humans by the slow binding model (solid line), indirect response model I (broken line), and biophase model (dotted line). The observed data from Wood-Baker et al. [44] are shown as solid circles
It is interesting to note that the 50% effective drug concentration values (EC50, IC50 and Kd) are similar for each drug for the three models. This might be expected since it is the same PK profiles that are driving the same responses.
Discussion
The responses of many drugs with SRB can be described by a simple model based on the law of mass action and classical receptor occupancy theory. This model connects the drug PK and effects by considering the kinetics of receptor association and dissociation. Distinctive signature profiles are produced as compared to some other PD models.
The model of SRB demonstrated delayed onset and prolonged responses as the result of slow binding of the drug to the receptor. Increased doses lead to larger effects with peak or nadir effects shifting to earlier times. The onset slope is related to dose, kon and Emax while the recession slope exhibits more complex behavior and approaches to a limiting value determined by kel and Emax for higher doses. In addition, the SRB model will behave like simple direct effect model when koff becomes very large. Based on our simulations with kel of 0.25 1/h, the SRB model is generally considered for a drug with dissociation half-life longer than 10 min. However, it is difficult to define a clear cutoff value of koff or kon for SRB drugs based on these simulations as they cannot reflect the universe of possible combinations of the independent variables. Dahl et al. observed that the duration of effect will be most prolonged when koff is slower than kel [14], but most drugs have a faster koff as we also show in Table 1.
While ionotropic receptors might be most likely to produce SRB profiles, metabolotropic (G-protein mediated), kinase, and nuclear receptors might produce delayed responses owing to the signaling cascades that follow receptor binding. However, the drugs listed in Table 1 and 2 show interactions with diverse targets including receptors and protease and integrase enzymes.
Proper in vitro experimental conditions are essential to obtain accurate binding kinetic parameters for drugs with SRB. For measuring koff, the wash-out conditions are discerned by whether the fresh medium is used to replace the radiolabeled drug-containing medium and whether an excess amount of unlabeled competitive ligand is supplied [4]. The former condition may not substantially influence koff whereas the latter condition of adding unlabeled ligand can effectively prevent the rebinding of the dissociated drug to the receptor, a phenomenon pervasively found for drugs with slow dissociation that can further prolong the dissociation [4, 49]. In the in vitro dissociation study with candesartan, when unlabeled candesartan is supplied, the dissociation half-life of candesartan decreased from 11.6 h to around 2 h [50]. The acceleration in koff positively correlated with the amount of unlabeled ligand added in the medium, so the addition of an excess amount of unlabeled ligand (usually 100-fold) is required. Alternatively, diluting the radiolabeled drug-containing medium before adding unlabeled ligand to ensure the accuracy of measuring koff is needed [50]. The Kd is sometimes measured as a surrogate of binding kinetics and reflects the affinity of the drug to the receptor. However, Kd must be obtained at equilibrium condition, which may be difficult to achieve for drugs with long dissociation half-lives. Lack of equilibration may result in underpredicting the affinity, so a higher Kd value is obtained [51]. In a saturation binding assay of candesartan, increasing incubation times from 5 to 180 min resulted in decreased apparent Kd from 1 to 0.02 nM, suggesting a lack of equilibration with short incubation time [50]. Similarly, geldanamycin demonstrated a 40-fold decrease in Kd over 24 h incubation time [52]. The Kd of maraviroc obtained in the saturation binding study (0.86 nM) was also higher than the Kd calculated from the ratio of koff/kon (0.071 nM) [53]. Thus, for drugs with SRB, it is better to obtain Kd either from the kinetic parameters koff and kon or from saturation binding studies with sufficient incubation times (5-times the dissociation half-life) [51]. More advanced technology, such as resonance energy transfer (RET) based techniques with fluorescent or bioluminescent energy sources, enables high-throughput binding kinetic assays [54]. Surface plasmon resonance methodology provides a rigorous measurement of binding kinetics [16].
Several assumptions were made in our operation of the SRB model. The most important one is that the drug effect is assumed to be directly linked and proportional to the RC concentration. Under this condition, RC and Rt concentrations in the classical receptor occupancy theory can be replaced by drug effect and Emax. This is more of a simplified scenario as the true relationship between receptor occupancy and response may be of sigmoid shape and other transduction and homeostatic feedback mechanisms may be involved [1]. More complex models with binding kinetics have been reviewed [10]. Another assumption is that the plasma concentration is proportional to the drug concentration at the target site and is much greater than the receptor concentration. This allows the fraction of drug bound to the receptor to be negligible in relation to the free drug concentration; thus the plasma concentration can be used as a surrogate for free drug concentration and drug PK is not influenced by drug receptor binding. If the concentrations of drug and receptor are comparable, free drug concentrations change during receptor binding, which is a more complex situation known as slow tight-binding [55]. Under this condition, receptor binding may influence the drug PK, which can be described by the TMDD model [56]. This review does not consider drugs and proteins with TMDD properties as both the PK and PD become far more complicated.
The current report showed the application of the SRB model to the antihypertension effects of candesartan and antiallergic effects of noberastine. Their PD effects were well-captured by the SRB model. The dissociation half-lives of the two drugs from the model predictions were close to their in vitro dissociation half-lives [18, 45]. This suggests an opportunity for using the SRB model with in vitro binding kinetic parameters to predict drug responses. However, the predicted Kd for candesartan (19.5 ug/L) is higher than the in vitro measured Kd (5.7 ng/L) [18]. This may be attributed to the extensive plasma protein binding of candesartan (> 99% in humans) [37], which may lead to the true free drug concentrations for receptor binding being much lower than the total plasma concentration. Noberastine also showed an underpredicted Kd of 1.51 ug/L compared to its in vitro Ki of 47 ng/L [45]. Although no plasma protein binding information was found for noberastine, many secondary-generation antihistamines demonstrate high protein binding, which may contribute to in vitro/in vivo differences in affinity [57].
Besides the similarities in shapes and in fitting response profiles, the three basic PK/PD models (as well as direct effect models) share the properties of a ABEC that is proportional to log Dose at higher doses and recession slopes that are essentially linear, parallel for higher doses, and determined by the Emax (or equivalent) and terminal slope of the PK (kel) or biophase (keo) constant. Further, the SRB model can be interpreted as an indirect response model with a linear effect on kout when koff·Emax = kin, koff = kin, and Emax = Ro. This indicates the need for higher doses of drugs in order to discriminate between these models by fitting data. It can be noted that the SRB and biophase models only require fitting of 3 parameters, while full indirect response model models require 4 parameters.
A biophase can be added to the SRB model either for greater mechanistic relevance or to further capture delays between drug concentrations and responses. This was done in investigating the antinociceptive and respiratory depressant effects of buprenorphine in rats and humans by Yassen et al. [27,28,29,30], where they showed that adding an effect compartment significantly improved the modeling performance. The biophase delay likely reflects the slow distribution of buprenorphine into or from the brain [29]. Thus, biophase equilibration and receptor binding can both contribute to the delayed and prolonged effects of slow binding drugs. Of course, other pharmacologic complexities may also apply such as turnover of targets, receptor desensitization, more complicated receptor binding kinetics, and nonlinear- or time-dependent transduction processes. When multiple steps are involved in the pharmacological response, such as for some corticosteroid actions, receptor-binding events with koff and kon can be included as an early step in a mRNA/protein/biomarker cascade [58]. In addition, free drug concentrations will often be the preferred substrate for many drugs and receptors. Further, when receptor mechanisms involve partial agonists, spare receptors, or nonlinear transduction the concepts from Black and Leff [59] should be invoked. In essence, our model is simply a basic starting point that can be expanded in many ways.
The SRB model has been introduced and used since 1990s but has been largely overlooked. One possible reason is that other PD models, like indirect response and biophase models, can produce similar profiles as SRB and produce similar Kd, EC50 or IC50 values. Many slow binding drugs also have long elimination half-lives, which may mask their SRB nature and produce similar profiles as direct effect models. Another reason is the limited availability of the kinetic binding parameters as additional in vitro experiments are required. However, the SRB model should clearly be part of the “toolbox” of pharmacometricians as it is intrinsically mathematically and graphically different from other PD models and might fit data better than with other models. The SRB model illustrated in the present study is a simplified version when binding kinetics are considered as the rate-limiting step for PD effects, but works quite well for many drugs.
Conclusions
The kinetics of SRB have significance in drug action and help shape the clinical outcomes and safety profiles of many drugs. For drugs with slow association or dissociation rates from targets, a simple SRB model can be used to describe delayed drug responses by incorporating drug binding kinetics. To apply the SRB model with better estimation, high quality data from a wide range of doses with rich sampling points and additional confirmation from in vitro experiments are required. However, if only based on drug PD responses, it may be difficult to discern the SRB from indirect response and biophase models. Thus, mechanistic studies are required to understand the rate-limiting step in affecting the drug responses and to ensure appropriate model selection and application.
References
Ploeger BA, van der Graaf PH, Danhof M (2009) Incorporating receptor theory in mechanism-based pharmacokinetic-pharmacodynamic (PK-PD) modeling. Drug Metab Pharmacokinet 24(1):3–15
Tonge PJ (2018) Drug–target kinetics in drug discovery. ACS Chem Neurosci 9(1):29–39
Pan AC, Borhani DW, Dror RO, Shaw DE (2013) Molecular determinants of drug–receptor binding kinetics. Drug Discov Today 18(13):667–673. https://doi.org/10.1016/j.drudis.2013.02.007
Vauquelin G, Charlton SJ (2010) Long-lasting target binding and rebinding as mechanisms to prolong in vivo drug action. Br J Pharmacol 161(3):488–508
Swinney DC (2008) Applications of binding kinetics to drug discovery. Pharmaceut Med 22(1):23–34. https://doi.org/10.1007/BF03256679
Price D, Sharma A, Cerasoli F (2009) Biochemical properties, pharmacokinetics and pharmacological response of tiotropium in chronic obstructive pulmonary disease patients. Expert Opin Drug Metab Toxicol 5(4):417–424
Dowling MR, Charlton SJ (2006) Quantifying the association and dissociation rates of unlabelled antagonists at the muscarinic M3 receptor. Br J Pharmacol 148(7):927–937. https://doi.org/10.1038/sj.bjp.0706819
van Noord JA, Smeets JJ, Custers FL, Korducki L, Cornelissen PJ (2002) Pharmacodynamic steady state of tiotropium in patients with chronic obstructive pulmonary disease. Eur Respir J 19(4):639–644. https://doi.org/10.1183/09031936.02.00238002
Kapur S, Seeman P (2000) Antipsychotic agents differ in how fast they come off the dopamine D2 receptors Implications for atypical antipsychotic action. J Psychiatry Neurosci 25(2):161–166
Daryaee F, Tonge PJ (2019) Pharmacokinetic–pharmacodynamic models that incorporate drug–target binding kinetics. Curr Opin Chem Biol 50:120–127
Fuseau E, Sheiner LB (1984) Simultaneous modeling of pharmacokinetics and pharmacodynamics with a nonparametric pharmacodynamic model. Clin Pharmacol Ther. https://doi.org/10.1038/clpt.1984.104
Shimada S, Nakajima Y, Yamamoto K, Sawada Y, Iga T (1996) Comparative pharmacodynamics of eight calcium channel blocking agents in Japanese essential hypertensive patients. Biol Pharm Bull 19(3):430–437
Copeland RA, Pompliano DL, Meek TD (2006) Drug–target residence time and its implications for lead optimization. Nat Rev Drug Discov 5(9):730–739
Dahl G, Akerud T (2013) Pharmacokinetics and the drug–target residence time concept. Drug Discov Today 18(15–16):697–707
Ariens EJ (1954) Affinity and intrinsic activity in the theory of competitive inhibition i Problems and theory. Arch Int Pharmacodyn Ther 99(1):32–49
Dierynck I, De Wit M, Gustin E, Keuleers I, Vandersmissen J, Hallenberger S, Hertogs K (2007) Binding kinetics of darunavir to human immunodeficiency virus type 1 protease explain the potent antiviral activity and high genetic barrier. J Virol 81(24):13845–13851. https://doi.org/10.1128/jvi.01184-07
Hightower KE, Wang R, DeAnda F, Johns BA, Weaver K, Shen Y, Tomberlin GH, Carter HL III, Broderick T, Sigethy S (2011) Dolutegravir (S/GSK1349572) exhibits significantly slower dissociation than raltegravir and elvitegravir from wild-type and integrase inhibitor-resistant HIV-1 integrase-DNA complexes. Antimicrob Agents Chemother 55(10):4552–4559
Fierens FL, Vanderheyden PM, Roggeman C, Vande Gucht P, De Backer JP, Vauquelin G (2002) Distinct binding properties of the AT(1) receptor antagonist [(3)H]candesartan to intact cells and membrane preparations. Biochem Pharmacol 63(7):1273–1279. https://doi.org/10.1016/s0006-2952(02)00859-6
Le MT, Pugsley MK, Vauquelin G, Van Liefde I (2007) Molecular characterisation of the interactions between olmesartan and telmisartan and the human angiotensin II AT1 receptor. Br J Pharmacol 151(7):952–962. https://doi.org/10.1038/sj.bjp.0707323
Motulsky HJ, Mahan L (1984) The kinetics of competitive radioligand binding predicted by the law of mass action. Mol Pharmacol 25(1):1–9
Bosma R, Witt G, Vaas LAI, Josimovic I, Gribbon P, Vischer HF, Gul S, Leurs R (2017) The target residence time of antihistamines determines their antagonism of the G protein-coupled histamine H1 receptor. Front Pharmacol 8:667. https://doi.org/10.3389/fphar.2017.00667
Carboni L, Negri M, Michielin F, Bertani S, Fratte SD, Oliosi B, Cavanni P (2012) Slow dissociation of partial agonists from the D2 receptor is linked to reduced prolactin release. Int J Neuropsychopharmacol 15(5):645–656
Kati WM, Montgomery D, Carrick R, Gubareva L, Maring C, McDaniel K, Steffy K, Molla A, Hayden F, Kempf D, Kohlbrenner W (2002) In vitro characterization of A-315675, a highly potent inhibitor of A and B strain influenza virus neuraminidases and influenza virus replication. Antimicrob Agents Chemother 46(4):1014–1021. https://doi.org/10.1128/AAC.46.4.1014-1021.2002
Weiss M, Kang W (2004) Inotropic effect of digoxin in humans: mechanistic pharmacokinetic/pharmacodynamic model based on slow receptor binding. Pharm Res 21(2):231–236. https://doi.org/10.1023/b:pham.0000016236.36210.a6
Äbelö A, Gabrielsson J, Holstein B, Eriksson UG, Holmberg J, Karlsson MO (2001) Pharmacodynamic modelling of reversible gastric acid pump inhibition in dog and man. Eur J Pharm Sci 14(4):339–346
Abelö A, Andersson M, Holmberg AA, Karlsson MO (2006) Application of a combined effect compartment and binding model for gastric acid inhibition of AR-HO47108: a potassium competitive acid blocker, and its active metabolite AR-HO47116 in the dog. Eur J Pharm Sci 29(2):91–101. https://doi.org/10.1016/j.ejps.2006.05.014
Yassen A, Olofsen E, Dahan A, Danhof M (2005) Pharmacokinetic-pharmacodynamic modeling of the antinociceptive effect of buprenorphine and fentanyl in rats: role of receptor equilibration kinetics. J Pharmacol Exp Ther 313(3):1136–1149
Yassen A, Kan J, Olofsen E, Suidgeest E, Dahan A, Danhof M (2006) Mechanism-based pharmacokinetic-pharmacodynamic modeling of the respiratory-depressant effect of buprenorphine and fentanyl in rats. J Pharmacol Exp Ther 319(2):682. https://doi.org/10.1124/jpet.106.107953
Yassen A, Olofsen E, Romberg R, Sarton E, Danhof M, Dahan A (2006) Mechanism-based pharmacokinetic-pharmacodynamic modeling of the antinociceptive effect of buprenorphine in healthy volunteers. Anesthesiology 104(6):1232–1242. https://doi.org/10.1097/00000542-200606000-00019
Yassen A, Olofsen E, Romberg R, Sarton E, Teppema L, Danhof M, Dahan A (2007) Mechanism-based PK/PD modeling of the respiratory depressant effect of buprenorphine and fentanyl in healthy volunteers. Clin Pharmacol Ther 81(1):50–58. https://doi.org/10.1038/sj.clpt.6100025
Wagner J (1968) Kinetics of pharmacologic response I Proposed relationships between response and drug concentration in the intact animal and man. J Theor Biol 20(2):173–201
Krzyzanski W, Jusko WJ (1998) Integrated functions for four basic models of indirect pharmacodynamic response. J Pharm Sci 87(1):67–72
Krzyzanski W, Jusko WJ (1998) Characterization of pharmacodynamic recession slopes for direct and indirect response models. J Pharmacokinet Biopharm 26(4):409–436
Van Liefde I, Vauquelin G (2009) Sartan–AT1 receptor interactions: in vitro evidence for insurmountable antagonism and inverse agonism. Mol Cell Endocrinol 302(2):237–243
Vanderheyden PM, Fierens FL, De Backer J, Vauquelin G (2000) Reversible and syntopic interaction between angiotensin receptor antagonists on Chinese hamster ovary cells expressing human angiotensin II type 1 receptors. Biochem Pharmacol 59(8):927–935. https://doi.org/10.1016/s0006-2952(99)00403-7
Verheijen I, Fierens FL, Debacker JP, Vauquelin G, Vanderheyden PM (2000) Interaction between the partially insurmountable antagonist valsartan and human recombinant angiotensin II type 1 receptors. Fundam Clin Pharmacol 14(6):577–585. https://doi.org/10.1111/j.1472-8206.2000.tb00443.x
Gleiter CH, Mörike KE (2002) Clinical pharmacokinetics of candesartan. Clin Pharmacokinet 41(1):7–17
Shibouta Y, Inada Y, Ojima M, Wada T, Noda M, Sanada T, Kubo K, Kohara Y, Naka T, Nishikawa K (1993) Pharmacological profile of a highly potent and long-acting angiotensin II receptor antagonist, 2-ethoxy-1-[[2’-(1H-tetrazol-5-yl) biphenyl-4-yl] methyl]-1H-benzimidazole-7-carboxylic acid (CV-11974), and its prodrug,(+/-)-1-(cyclohexyloxycarbonyloxy)-ethyl 2-ethoxy-1-[[2’-(1H-tetrazol-5-yl) biphenyl-4-yl] methyl]-1H-benzimidazole-7-carboxylate (TCV-116). J Pharmacol Exp Ther 266(1):114–120
Delacrétaz E, Nussberger J, Biollaz J, Waeber B, Brunner HR (1995) Characterization of the angiotensin II receptor antagonist TCV-116 in healthy volunteers. Hypertension 25(1):14–21
Reddy VP, Kozielska M, Johnson M, Vermeulen A, de Greef R, Liu J, Groothuis GM, Danhof M, Proost JH (2011) Structural models describing placebo treatment effects in schizophrenia and other neuropsychiatric disorders. Clin Pharmacokinet 50(7):429–450
Bialer M (1980) A simple method for determining whether absorption and elimination rate constants are equal in the one-compartment open model with first-order processes. J Pharmacokinet Biopharm 8(1):111–113. https://doi.org/10.1007/BF01059453
Church MK (2016) Allergy histamine and antihistamines Handb Exp Pharmaco. Springer International Publishing, Cham
Cuvillo Bernal AD, Mullol I Miret J, Bartra Tomàs J, Dávila I, Jáuregui I, Montoro J, Sastre J, Valero A (2006) Comparative pharmacology of the H1 antihistamines. J Investig Allergol Clin Immunol 16:3–12
Desager J-P, Horsmans Y (1995) Pharmacokinetic-pharmacodynamic relationships of H1-antihistamines. Clin Pharmacokinet 28(5):419–432
Leysen JE, Gommeren W, Janssen PF, Janssen PA (1991) Comparative study of central and peripheral histamine-H1 receptor binding in vitro and ex vivo of non-sedating antihistamines and of noberastine, a new agent. Drug Dev Res 22(2):165–178
Gillard M, Van Der Perren C, Moguilevsky N, Massingham R, Chatelain P (2002) Binding characteristics of cetirizine and levocetirizine to human H(1) histamine receptors: contribution of Lys(191) and Thr(194). Mol Pharmacol 61(2):391–399. https://doi.org/10.1124/mol.61.2.391
Church MK, Gillard M, Sargentini-Maier ML, Poggesi I, Campbell A, Benedetti MS (2009) From pharmacokinetics to therapeutics. Drug Metab Rev 41(3):455–474
Wood-Baker R, Emanuel M, Hutchinson K, Howarth P (1993) The time course of action of three differing doses of noberastine, a novel H1-receptor antagonist, on histamine-induced skin wheals and the relationship to plasma drug concentrations in normal human volunteers. Br J Clin Pharmacol 35(2):166
Vauquelin G (2016) Effects of target binding kinetics on in vivo drug efficacy: koff, kon and rebinding. Br J Pharmacol 173(15):2319–2334
Fierens F, Vanderheyden PM, De Backer JP, Vauquelin G (1999) Binding of the antagonist [3H]candesartan to angiotensin II AT1 receptor-transfected [correction of tranfected] Chinese hamster ovary cells. Eur J Pharmacol 367(2–3):413–422. https://doi.org/10.1016/s0014-2999(98)00965-0
Hoare SRJ, Fleck BA, Williams JP, Grigoriadis DE (2020) The importance of target binding kinetics for measuring target binding affinity in drug discovery: a case study from a CRF(1) receptor antagonist program. Drug Discov Today 25(1):7–14. https://doi.org/10.1016/j.drudis.2019.09.011
Gooljarsingh LT, Fernandes C, Yan K, Zhang H, Grooms M, Johanson K, Sinnamon RH, Kirkpatrick RB, Kerrigan J, Lewis T (2006) A biochemical rationale for the anticancer effects of Hsp90 inhibitors: slow, tight binding inhibition by geldanamycin and its analogues. PNAS 103(20):7625–7630
Napier C, Sale H, Mosley M, Rickett G, Dorr P, Mansfield R, Holbrook M (2005) Molecular cloning and radioligand binding characterization of the chemokine receptor CCR5 from rhesus macaque and human. Biochem Pharmacol 71(1–2):163–172. https://doi.org/10.1016/j.bcp.2005.10.024
Hoare SR (2021) The problems of applying classical pharmacology analysis to modern in vitro drug discovery assays: slow binding kinetics and high target concentration. SLAS Discov 26(7):835–850
Morrison JF, Walsh CT (1988) The behavior and significance of slow-binding enzyme inhibitors. Adv Enzymol Relat Areas Mol Biol 61:201–301. https://doi.org/10.1002/9780470123072.ch5
Mager DE, Jusko WJ (2001) General pharmacokinetic model for drugs exhibiting target-mediated drug disposition. J Pharmacokinet Pharmacodyn 28(6):507–532. https://doi.org/10.1023/a:1014414520282
Slater JW, Zechnich AD, Haxby DG (1999) Second-generation antihistamines. Drugs 57(1):31–47
Ramakrishnan R, DuBois DC, Almon RR, Pyszczynski NA, Jusko WJ (2002) Fifth-generation model for corticosteroid pharmacodynamics: application to steady-state receptor down-regulation and enzyme induction patterns during seven-day continuous infusion of methylprednisolone in rats. J Pharmacokinet Pharmacodyn 29(1):1–24. https://doi.org/10.1023/a:1015765201129
Black JW, Leff P (1983) Operational models of pharmacological agonism. Proc R Soc Lond B Biol Sci 220(1219):141–162
Vanderheyden PM, Verheijen I, Fierens FL, Backer JP, Vauquelin G (2000) Binding characteristics of [(3)H]-irbesartan to human recombinant angiotensin type 1 receptors. J Renin Angiotensin Aldosterone Syst 1(2):159–165. https://doi.org/10.3317/jraas.2000.020
Israili Z (2000) Clinical pharmacokinetics of angiotensin II (AT1) receptor blockers in hypertension. J Hum Hypertens 14(1):S73–S86
Li X, Mo E, Chen L (2022) Pharmacokinetics and bioequivalence evaluation of 2 olmesartan medoxomil and amlodipine besylate fixed-dose combination tablets in healthy Chinese volunteers under fasting and fed conditions. Clin Pharmacol Drug Dev. https://doi.org/10.1002/cpdd.1086
Church DS, Church MK (2011) Pharmacology of antihistamines. World Allergy Organ J 4(3 Suppl):S22-27. https://doi.org/10.1097/WOX.0b013e3181f385d9
Anthes JC, Gilchrest H, Richard C, Eckel S, Hesk D, West RE Jr, Williams SM, Greenfeder S, Billah M, Kreutner W, Egan RE (2002) Biochemical characterization of desloratadine, a potent antagonist of the human histamine H(1) receptor. Eur J Pharmacol 449(3):229–237. https://doi.org/10.1016/s0014-2999(02)02049-6
Meier E, Narvekar A, Iyer GR, DuBiner HB, Vutikullird A, Wirta D, Sall K (2017) Pharmacokinetics and safety of olopatadine hydrochloride 0.77% in healthy subjects with asymptomatic eyes: data from 2 independent clinical studies. Clin Ophthalmol. https://doi.org/10.2147/OPTH.S126690
Kwon O-S, Kim H-J, Pyo H, Chung S-J, Chung YB (2005) Determination of mequitazine in human plasma by gas-chromatography/mass spectrometry with ion-trap detector and its pharmacokinetics after oral administration to volunteers. Arch Pharm Res 28(10):1190–1195
Moulton BC, Fryer AD (2011) Muscarinic receptor antagonists, from folklore to pharmacology; finding drugs that actually work in asthma and COPD. Br J Pharmacol 163(1):44–52
Horhota ST, van Noord JA, Verkleij CB, Bour LJ, Sharma A, Trunk M, Cornelissen PJ (2015) In vitro, pharmacokinetic, pharmacodynamic, and safety comparisons of single and combined administration of tiotropium and salmeterol in COPD patients using different dry powder inhalers. AAPS J 17(4):871–880
Abernethy DR (1992) Pharmacokinetics and pharmacodynamics of amlodipine. Cardiology 80:31–36
Gossas T, Vrang L, Henderson I, Sedig S, Sahlberg C, Lindström E, Danielson UH (2012) Aliskiren displays long-lasting interactions with human renin. Naunyn Schmiedebergs Arch Pharmacol 385(2):219–224
Luft FC, Weinberger MH (2008) Antihypertensive therapy with aliskiren. Kidney Int 73(6):679–683. https://doi.org/10.1038/sj.ki.5002732
Boas RA, Villiger JW (1985) Clinical actions of fentanyl and buprenorphine the significance of receptor binding. Br J Anaesth 57(2):192–196. https://doi.org/10.1093/bja/57.2.192
Elkader A, Sproule B (2005) Buprenorphine. Clin Pharmacokinet 44(7):661–680
Hale JJ, Mills SG, MacCoss M, Finke PE, Cascieri MA, Sadowski S, Ber E, Chicchi GG, Kurtz M, Metzger J, Eiermann G, Tsou NN, Tattersall FD, Rupniak NMJ, Williams AR, Rycroft W, Hargreaves R, MacIntyre DE (1998) Structural optimization affording 2-(R)-(1-(R)-3, 5-bis (trifluoromethyl) phenylethoxy)-3-(S)-(4-fluoro) phenyl-4-(3-oxo-1, 2, 4-triazol-5-yl) methylmorpholine, a potent, orally active, long-acting morpholine acetal human NK-1 receptor antagonist. J Med Chem 41(23):4607–4614. https://doi.org/10.1021/jm980299k
Majumdar AK, Howard L, Goldberg MR, Hickey L, Constanzer M, Rothenberg PL, Crumley TM, Panebianco D, Bradstreet TE, Bergman AJ (2006) Pharmacokinetics of aprepitant after single and multiple oral doses in healthy volunteers. J Clin Pharmacol 46(3):291–300
Rittweger M, Arastéh K (2007) Clinical pharmacokinetics of darunavir. Clin Pharmacokinet 46(9):739–756
Boffito M, Jackson A, Amara A, Back D, Khoo S, Higgs C, Seymour N, Gazzard B, Moyle G (2011) Pharmacokinetics of once-daily darunavir-ritonavir and atazanavir-ritonavir over 72 hours following drug cessation. Antimicrob Agents Chemother 55(9):4218–4223
Abel S, Back DJ, Vourvahis M (2009) Maraviroc: pharmacokinetics and drug interactions. Antivir Ther 14(5):607–618
Davies BE (2010) Pharmacokinetics of oseltamivir: an oral antiviral for the treatment and prophylaxis of influenza in diverse populations. J Antimicrob Chemother. https://doi.org/10.1093/jac/dkq015
Bardsley-Elliot A, Plosker GL (2000) Nelfinavir Drugs 59(3):581–620
Crommentuyn KM, Mulder JW, Mairuhu AT, van Gorp EC, Meenhorst PL, Huitema AD, Beijnen JH (2004) The plasma and intracellular steady-state pharmacokinetics of lopinavir/ritonavir in HIV-1-infected patients. Antivir Ther 9(5):779–785
Khaliq Y, Gallicano K, Venance S, Kravcik S, Cameron DW (2000) Effect of ketoconazole on ritonavir and saquinavir concentrations in plasma and cerebrospinal fluid from patients infected with human immunodeficiency virus. Clin Pharmacol Ther 68(6):637–646
Mehandru S, Markowitz M (2003) Tipranavir: a novel non-peptidic protease inhibitor for the treatment of HIV infection. Expert Opin Investig Drugs 12(11):1821–1828
Flores MV, Strawbridge J, Ciaramella G, Corbau R (2009) HCV-NS3 inhibitors: determination of their kinetic parameters and mechanism. Biochim Biophys Acta 1794(10):1441–1448
Yamada I, Suzuki F, Kamiya N, Aoki K, Sakurai Y, Kano M, Matsui H, Kumada H (2012) Safety, pharmacokinetics and resistant variants of telaprevir alone for 12 weeks in hepatitis C virus genotype 1b infection. J Viral Hepat 19(2):e112–e119
Klibanov OM, Vickery SB, Olin JL, Smith LS, Williams SH (2012) Boceprevir: a novel NS 3/4 protease inhibitor for the treatment of hepatitis C. Pharmacotherapy 32(2):173–190
Cottrell ML, Hadzic T, Kashuba AD (2013) Clinical pharmacokinetic, pharmacodynamic and drug-interaction profile of the integrase inhibitor dolutegravir. Clin Pharmacokinet 52(11):981–994
Brainard DM, Wenning LA, Stone JA, Wagner JA, Iwamoto M (2011) Clinical pharmacology profile of raltegravir, an HIV-1 integrase strand transfer inhibitor. J Clin Pharmacol 51(10):1376–1402
Ramanathan S, Mathias AA, German P, Kearney BP (2011) Clinical pharmacokinetic and pharmacodynamic profile of the HIV integrase inhibitor elvitegravir. Clin Pharmacokinet 50(4):229–244
Wood ER, Truesdale AT, McDonald OB, Yuan D, Hassell A, Dickerson SH, Ellis B, Pennisi C, Horne E, Lackey K, Alligood KJ, Rusnak DW, Gilmer TM, Shewchuk L (2004) A unique structure for epidermal growth factor receptor bound to GW572016 (Lapatinib): Relationships among protein conformation, inhibitor off-rate, and receptor activity in tumor cells. Cancer Res 64(18):6652–6659. https://doi.org/10.1158/0008-5472.Can-04-1168
Spector NL, Robertson FC, Bacus S, Blackwell K, Smith DA, Glenn K, Cartee L, Harris J, Kimbrough CL, Gittelman M (2015) Lapatinib plasma and tumor concentrations and effects on HER receptor phosphorylation in tumor. PLoS ONE 10(11):e0142845
Lewandowicz A, Tyler PC, Evans GB, Furneaux RH, Schramm VL (2003) Achieving the ultimate physiological goal in transition state analogue inhibitors for purine nucleoside phosphorylase. J Biol Chem 278(34):31465–31468
Major PP, Agarwal RP, Kufe DW (1981) Clinical pharmacology of deoxycoformycin. Blood 58(1):91–96
Kim YB, Kopcho LM, Kirby MS, Hamann LG, Weigelt CA, Metzler WJ, Marcinkeviciene J (2006) Mechanism of Gly-Pro-pNA cleavage catalyzed by dipeptidyl peptidase-IV and its inhibition by saxagliptin (BMS-477118). Arch Biochem Biophys 445(1):9–18. https://doi.org/10.1016/j.abb.2005.11.010
Boulton DW (2017) Clinical pharmacokinetics and pharmacodynamics of saxagliptin, a dipeptidyl peptidase-4 inhibitor. Clin Pharmacokinet 56(1):11–24
Wang A, Dorso C, Kopcho L, Locke G, Langish R, Harstad E, Shipkova P, Marcinkeviciene J, Hamann L, Kirby MS (2012) Potency, selectivity and prolonged binding of saxagliptin to DPP4: Maintenance of DPP4 inhibition by saxagliptin in vitro and ex vivo when compared to a rapidly-dissociating DPP4 inhibitor. BMC Pharmacol 12(1):1–11
de Leon J, Diaz FJ, Wedlund P, Josiassen RC, Cooper TB, Simpson GM (2004) Haloperidol half-life after chronic dosing. J Clin Psychopharmacol 24(6):656–660
Lindström E, Levander S (2006) Sertindole: efficacy and safety in schizophrenia. Expert Opin Pharmacother 7(13):1825–1834
Yeung P-F, Hubbard J, Korchinski E, Midha K (1993) Pharmacokinetics of chlorpromazine and key metabolites. Eur J Clin Pharmacol 45(6):563–569
Winans E (2003) Aripiprazole. Am J Health Syst Pharm 60(23):2437–2445
Kohout TA, Xie Q, Reijmers S, Finn KJ, Guo Z, Zhu YF, Struthers RS (2007) Trapping of a nonpeptide ligand by the extracellular domains of the gonadotropin-releasing hormone receptor results in insurmountable antagonism. Mol Pharmacol 72(2):238–247. https://doi.org/10.1124/mol.107.035535
Suzuki H, Uemura H, Mizokami A, Hayashi N, Miyoshi Y, Nagamori S, Enomoto Y, Akaza H, Asato T, Kitagawa T (2019) Phase I trial of TAK-385 in hormone treatment-naïve Japanese patients with nonmetastatic prostate cancer. Cancer Med 8(13):5891–5902
Sullivan SK, Hoare SR, Fleck BA, Zhu YF, Heise CE, Struthers RS, Crowe PD (2006) Kinetics of nonpeptide antagonist binding to the human gonadotropin-releasing hormone receptor: implications for structure-activity relationships and insurmountable antagonism. Biochem Pharmacol 72(7):838–849. https://doi.org/10.1016/j.bcp.2006.07.011
Struthers RS, Chen T, Campbell B, Jimenez R, Pan H, Yen SS, Bozigian HP (2006) Suppression of serum luteinizing hormone in postmenopausal women by an orally administered nonpeptide antagonist of the gonadotropin-releasing hormone receptor (NBI-42902). J Clin Endocrinol Metab 91(10):3903–3907
Näbauer M, Erdmann E (1987) Reversal of toxic and non-toxic effects of digoxin by digoxin-specific fab fragments in isolated human ventricular myocardium. Klin Wochenschr 65(12):558–561
Noel F, Fagoo M, Godfraind T (1990) A comparison of the affinities of rat (Na++ K+)-ATPase isozymes for cardioactive steroids, role of lactone ring, sugar moiety and KCl concentration. Biochem Pharmacol 40(12):2611–2616
Iisalo E (1977) Clinical pharmacokinetics of digoxin. Clin Pharmacokinet 2(1):1–16
Sykes DA, Bradley ME, Riddy DM, Willard E, Reilly J, Miah A, Bauer C, Watson SJ, Sandham DA, Dubois G (2016) Fevipiprant (QAW039), a slowly dissociating CRTh2 antagonist with the potential for improved clinical efficacy. Mol Pharmacol 89(5):593–605
Erpenbeck VJ, Vets E, Gheyle L, Osuntokun W, Larbig M, Neelakantham S, Sandham D, Dubois G, Elbast W, Goldsmith P (2016) Pharmacokinetics, safety, and tolerability of fevipiprant (QAW039), a novel CRTh2 receptor antagonist: results from 2 randomized, phase 1, placebo-controlled studies in healthy volunteers. Clin Pharmacol Drug Dev 5(4):306–313
Day RO, Graham GG, Hicks M, McLachlan AJ, Stocker SL, Williams KM (2007) Clinical pharmacokinetics and pharmacodynamics of allopurinol and oxypurinol. Clin Pharmacokinet 46(8):623–644. https://doi.org/10.2165/00003088-200746080-00001
Lovmar M, Tenson T, Mn E (2004) Kinetics of macrolide action: the josamycin and erythromycin cases. J Biol Chem 279(51):53506–53515
Periti P, Mazzei T, Mini E, Novelli A (1989) Clinical pharmacokinetic properties of the macrolide antibiotics. Clin Pharmacokinet 16(4):193–214. https://doi.org/10.2165/00003088-198916040-00001
Acknowledgements
Supported by a Fellowship for TR from GlaxoSmithKline and by NIH Grant R35-GM131800 for WJJ.
Author information
Authors and Affiliations
Contributions
Contributed to the study conception and design TR, XZ, WJJ; Conducted literature review: TR, XZ; Performed data analysis: TR, XZ, NMJ, WK; Wrote or contributed to the writing of the manuscript: TR, XZ, WK, WJJ.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ren, T., Zhu, X., Jusko, N.M. et al. Pharmacodynamic model of slow reversible binding and its applications in pharmacokinetic/pharmacodynamic modeling: review and tutorial. J Pharmacokinet Pharmacodyn 49, 493–510 (2022). https://doi.org/10.1007/s10928-022-09822-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10928-022-09822-y