Abstract
Immigrants, nearly half of whom prefer a language other than English (LOE), face structural barriers to healthcare. This subgroup is believed to be at increased risk for reduced access to quality healthcare, yet few studies have examined the health needs and utilization patterns of LOE-preferring patients who seek care in the Emergency Department (ED). Given that the ED is often an entry point to the health system, we sought to characterize the health patterns of this population in an urban ED setting. We conducted a retrospective chart review of the electronic medical records of 1,566 patients who utilized interpreter services in the ED or Urgent Care) at an urban safety net hospital. We found that LOE-preferring patients had high levels of chronic disease. We also found that the majority of these patients had not seen a primary care provider (PCP) within the study period. PCP visits were positively associated with ED utilization suggesting that those without a PCP are less likely to receive ED care. These findings point to a need for greater policy and community health solutions addressing the high burden of chronic disease and underutilization of healthcare for those with LOE preferences.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In 2021, there were over 20 million foreign-born individuals living in the United States (US) who prefer a language other than English (LOE), making up 6.6% of the country’s general population and nearly half of its immigrant population [1]. Immigration status is recognized as a social determinant of health that results in structural barriers to healthcare [2, 3]. For example, based on data from the 2021 American Community Survey, 23% of non-elderly legal immigrants and 46% of undocumented immigrants were without health insurance, compared to 8% of US-born and naturalized citizens [4]. Other healthcare related barriers include cost, navigation of complex systems, discrimination within the healthcare system, and fear of discovery [5, 6].
These barriers translate to health disparities and differences in healthcare utilization within immigrant populations. LOE-preferring individuals are less likely to have a regular Primary Care Provider (PCP) and have lower rates of healthcare utilization [7–9]. Immigration status has been associated with reduced preventative healthcare services, Emergency Department (ED) utilization, and healthcare spending [9, 10]. Factors associated with increased healthcare utilization include insurance, completion of high school, increased duration of residence in the US, and legal documentation status [9–11].
Studies suggest that newly arrived immigrants have a lower prevalence of most chronic diseases including diabetes, obesity, hypertension, and cardiovascular disease, as compared to their US-born peers [12,13,14,15]. However, the prevalence of chronic diseases among immigrants has been shown to increase with duration of residence in the US, with some studies suggesting that this occurs at rates higher than it does for their US-born peers [16,17,18]. Once diagnosed with chronic disease, immigrants are at higher risk for sub-optimal disease management [17, 19].
Recognizing structural barriers to routine care faced by LOE-preferring populations, and barriers to healthcare more generally, the ED can serve as a point of access for routine, urgent, and emergent needs, even potentially serving as a medical home for LOE-preferring populations [20]. Thus, the ED is an important and realistic setting to evaluate the healthcare patterns of LOE-preferring populations. In this study, we characterize the health status and healthcare utilization of individuals seeking emergency medical care who utilized language interpretive services (LIS) at an urban safety net hospital between 2019 and 2021.
Methods
Study Design
We conducted a single site retrospective chart review of patients with LOE preference who utilized LIS via a video remote interpreting (VRI) device in the ED or urgent care (UC) of a safety net hospital between January 1, 2019 and December 31, 2021. This study was evaluated and approved by the Emory University Institutional Review Board.
Setting
This study occurred at a large, Southeastern US urban academic Level I trauma and emergency care center. The hospital is a public safety-net hospital serving a largely uninsured/underinsured population with over 140,000 annual ED visits. Within the health system, there are seven neighborhood primary care clinics plus a primary care center at the main hospital site. The hospital serves two of the largest counties in the metro area, with one county being home to the largest number of resettled refugees in the state. Based on internal data from the hospital’s LIS Department, 13% of patients seeking care prefer a LOE with 7% speaking Spanish.
Population
The population of interest were patients with LOE preference with an ED or UC encounter at our study site between January 1, 2019 and December 31, 2021. In this study, utilization of LIS was used as a proxy for LOE preference.
Variables
Healthcare utilization variables collected included frequency of hospitalizations and ED, PCP, and subspecialty care encounters. Chronic diseases extracted included obesity (defined as having Body Mass Index [BMI] > 25), diabetes mellitus (type 1 and type 2 subclassifications), stroke, coronary artery disease or chronic heart failure, hypertension, cancer, substance use disorder, asthma, and chronic kidney disease. Patients were noted to have a chronic disease if they had a documented diagnosis in their most recent outpatient or ED encounter. Communicable diseases extracted included infection with Human Immunodeficiency Virus (HIV), hepatitis C (HCV), and COVID-19. BMI was abstracted directly from the chart or calculated.
Data Source
The medical record number (MRN) of patients was obtained from the hospital’s contracted LIS company. Hospital staff using the six dedicated ED VRI’s are required to record the patient’s MRN each time the VRI is used. After removing duplicates, we then conducted a chart review of the MRNs obtained using a standardized data extraction form which included patient demographics, insurance status, healthcare utilization, communicable and non-communicable/chronic diseases. This time-period was selected as the company had the most complete set of MRN data due to internal recording processes. Additionally, according to internal data, VRIs are the preferred source of interpretation services utilized at this hospital and were the main source of interpretation during the COVID-19 pandemic.
Statistical Analysis
Categorical variables were described using frequencies and percentages. Continuous variables were described using medians and interquartile ranges. The primary analyses focused on the relationships between patient characteristics and healthcare utilization patterns. For binary outcomes (e.g. subspecialty utilization), relationships were evaluated using binary logistic regressions and we present odds ratios (OR) and 95% confidence intervals (95% CI). For count-based outcomes (e.g. number of primary care visits), relationships were evaluated using negative binomial regressions and we present rate ratios (RR) and 95% CIs. Adjusted models were conducted using age, sex, comorbidities, BMI, inpatient class (emergency vs. inpatient), insurance status (insured vs. not insured), and area deprivation index [21]. Natural cubic splines were used to allow for non-linear effects of age, BMI, and ADI. Analyses were conducted using R (v. 4.3) [22].
Results
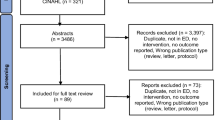
A total of 1,642 patients utilized VRI services during this time period. There is an ED-routine dialysis program at the study site with primarily Spanish speaking patients. Given their weekly ED encounters, these patients were excluded due to the unique nature of their utilization (n = 38). Additionally, 38 patients who utilized American Sign Language interpretation were excluded as the focus of this study was on spoken LIS. A total of 1,566 patients with a total of 3,234 ED encounters were ultimately included in this study.
Patient & Clinical Demographics
The majority of patients were Spanish-speaking (n = 1,328, 84.8%) with the next most common languages being Amharic (n = 30, 1.9%) and Vietnamese (n = 26, 1.7%) (Table 1). Approximately half of the participants in our sample were women (n = 788, 50.3%,) and the median age was 43 (IQR:34–53). Most patients had at least one chronic disease documented in their chart (n = 1,104, 68.8%) and nearly one third had two or more (n = 485, 30.2%). The three most common chronic diseases were obesity (n = 896, 57.2%), hypertension (n = 343, 21.9%), and diabetes mellitus (n = 283, 18.1%). With respect to communicable diseases, 1.6% (n = 25) of patients had HIV, 0.8% (n = 13) had HCV, and 13.3% (n = 208) had been diagnosed with COVID-19.
Healthcare Utilization
Most of the patients had never visited a primary care provider during the study period (n = 1,134, 69%). Patients who did have a PCP visit (n = 508, 38%) were more likely to utilize the ED compared to those who did not have a PCP visit with an average of 2.9 (CI = 2.62–3.23) visits compared to 1.6 (CI = 1.46–1.67) visits (Table 2). This was statistically significant with an adjusted rate ratio of 1.63 (CI = 1.41–1.88). Likewise, hospitalizations and ED visits were significantly higher for those with a PCP than for those without a PCP. Those with a PCP had an average of 0.76 hospitalizations (CI = 0.66–0.87) compared to 0.43 (CI = 0.38–0.49) for those without a PCP with an adjusted rate ratio of 1.53 (CI = 1.23–1.90). A total of 84.8% of patients with a PCP had seen a subspecialist, compared to 29.2% of those without a PCP with an odds ratio of 13.1 (CI = 9.6–18.0). ED visits were also positively predictive of subspecialty visits with an odds ratio of 1.38 (CI = 1.27–1.50).
Lastly, comorbidity was significantly and positively associated with ED and PCP visits (Table 3). Having ≥ 1, ≥ 2, and ≥ 3 comorbidities predicted ED visits with rate ratios of 2.99 (CI = 2.57–3.49), 2.43 (CI = 2.04–2.89), and 2.23 (CI = 1.75–2.85), respectively. The presence of ≥ 1, ≥ 2, and ≥ 3 comorbidities was predictive of PCP visits with rate ratios of 1.65 (CI = 1.44–1.89), 1.52 (CI = 1.29–1.80), and 1.73 (CI = 1.37–2.19) respectively.
Discussion
We sought to characterize the health status and healthcare utilization patterns of a sample of LOE-preferring patients seeking care in the ED of an urban safety net hospital. We found a high burden of chronic disease in our sample with 68.8% of patients having been diagnosed with at least one condition and nearly one third of patients demonstrating multimorbidity. The majority of patients had no visits to a PCP and PCP utilization was positively associated with ED utilization, subspecialty utilization, and hospitalizations.
Rates of chronic disease seen in our sample were notably higher than those seen in prior studies. Yun et al. identified that 50.1% of a newly resettled refugee population seen at a primary care clinic had at least one chronic disease (including behavioral health diagnoses) [23]. Our study differs in that we did not focus on a single arrival period or type of immigration status. We are unable to discern the legal status of our study population, but because our sample site was a safety net hospital, it is likely that our cohort includes individuals with a range of statuses. We did not extract mental health diagnoses given under-documentation of mental health diagnoses in medical charts [24]. Notably, the prevalence of chronic disease was still higher in our sample despite not including behavioral health diagnoses. The New Immigrant Survey (NIS), a national study of immigrant health status, demonstrated a chronic disease prevalence of 24.5% among their study population [16]. Importantly, the NIS is the only nationally representative study of chronic disease burden among immigrants in the United States. However, the sample only includes legal permanent residents and data is from 2003. This is relevant given the known association between duration of residence and immigration status with burden of chronic disease and healthcare access [2, 3]. The disparity may, at least in part, be attributable to differences in a survey of healthy individuals as compared to a study of those visiting the ED. However, the finding may also reflect changes in access to healthcare and chronic disease burden in the decades since 2003 and 2012, when Yun et al. was published. Notably, immigrants who gained insurance after the implementation of the Patient Protection and Affordable Care Act (ACA) were shown to have increased healthcare utilization, which may have contributed to increased diagnosis of chronic disease [11]. Despite the high prevalence of chronic diseases in our sample, most patients had no PCP visit during the study period, suggesting a low utilization of healthcare services overall.
The positive association between presence of a PCP and all studied domains of healthcare utilization is important, especially in the case of ED utilization. While it has often been hypothesized that PCP utilization leads to reductions in other forms of healthcare utilization, our findings join a body of literature in the general population that have found a positive association between primary care and ED utilization [25, 26]. There are several possible explanations for this finding. One explanation is that it may reflect comfort with and access to the healthcare system, with patients who receive any healthcare service at the hospital system being more likely to seek other types of care at the same location. Many of the barriers which prevent patients from accessing care in the ED may also prevent them from accessing primary care. For example, discussions of anti-immigrant policies have been associated with decreases or delays in immigrant utilization of both outpatient and ED services [27, 28]. Healthcare costs may also affect this relationship, with cost being a smaller barrier to accessing both primary and ED care for those who qualify for the health system’s financial assistance programming. Additionally, since we did not examine temporality of ED and PCP utilization it may be that ED access promotes PCP utilization, meaning that individuals are connected with primary care resources after visiting the ED. Lastly, our study was not equipped to examine the quality of primary care and its relationship with other types of healthcare utilization. Indeed, primary care factors such as extended hours of availability and status as a patient-centered medical home have been associated with reduced ED utilization [26, 29].
Taken together, our findings point to a potentially high-risk group of patients who may not have access to primary care nor utilize the ED with frequency. The relationship between primary care utilization and positive health outcomes is well-documented [30]. Thus, this pattern of low PCP utilization by LOE-preferring individuals could have negative short- and long-term health effects. These individuals may face a higher likelihood of undiagnosed or poorly managed chronic disease with limited access to any form of preventative or routine health screening.
All patients included in this study accessed the healthcare system through the ED at least once during the study period suggesting the role of the ED as a potential point of referral to primary and subspecialty care resources. Bilingual ED-based patient navigators have been demonstrated to be effective in connecting patients to primary and subspecialty care [31]. Given the associations between primary care access and prevention of costly morbidity and mortality from chronic disease, policies can seek to financially incentivize the implementation of health navigator programming [32, 33]. This model may also be expanded beyond the walls of the hospital to improve access for those who do not make it to the ED. Community health worker programming has been demonstrated to improve access to primary and subspecialty care, preventative screening, and chronic disease management for immigrants [31, 34].
Furthermore, our work redemonstrates the structural barriers many individuals who prefer a LOE face in seeking healthcare. Policies addressing these barriers are critical to improving healthcare access for this population. For example, incentivizing interpreter utilization through insurance reimbursements may increase appropriate care for those preferring a LOE [8, 14]. Furthermore, state Medicaid expansion, removal of immigration status requirements for Medicaid, and/or provision of coverage for immigrants who are ineligible for Medicaid, including recent immigrants, those without documentation, and those seeking asylum or other forms of relief, may also lead to improvements in healthcare access [35, 36].
Lastly, the differences in our findings, the healthcare and immigration policy changes since 2003, and the known disparities in chronic disease prevalence by immigration status also suggest the need for a new nationally representative survey of immigrant health status, inclusive of immigrants from a diversity of backgrounds and statuses to best inform the aforementioned policy initiatives.
Limitations
We examined patients’ encounters within a singular, albeit large, healthcare system, therefore our data may exclude utilization of other hospital systems in the same metro area or exclude data for patients who are not based in the area long-term. Our study period also includes the COVID-19 pandemic, a time that had a decrease in healthcare utilization for non-COVID-19 related conditions [37]. Both factors may contribute to an underestimation of utilization.
Furthermore, patient encounters in which a phone or in-person interpreter was utilized would have been excluded from this study due to our sampling frame. Thus, not all LOE-preferring patients seen in the hospital’s ED were sampled. Finally, our analysis did not factor temporality of visits making causation difficult to infer with respect to healthcare-seeking behavior.
New Contribution to the Literature
This study is the first to examine the health status and healthcare utilization patterns of the LOE-preferring population seen at an urban ED. In summary, our findings suggest that patients with a LOE preference have relatively low utilization of routine care and ED care, despite a high burden of chronic disease. Without an established source of care, these patients are at risk for increased mortality and morbidity. The underestimation of chronic disease burden seen in the NIS compared to our sample speaks to the need for a new national survey of immigrant health status so that policies can be derived from more accurate updated data that is inclusive of immigrants of all backgrounds. Until then, increasing primary care access should be a priority of policies and community health efforts to create more equitable healthcare for all.
Abbreviations
- BMI:
-
Body mass index
- CI:
-
Confidence interval
- ED:
-
Emergency department
- OR:
-
Odds ratio
- PCP:
-
Primary care provider
- RR:
-
Rate ratio
References
Language. and Education, in Migration Data Hub. 2021, Migration Policy Institute.
Language. and Literacy. Healthy People 2030 [cited 2024 2/4/2024]; https://health.gov/healthypeople/priority-areas/social-determinants-health/literature-summaries/language-and-literacy.
Castañeda H, et al. Immigration as a social determinant of health. Annu Rev Public Health. 2015;36:375–92.
Key Facts on Health Coverage of Immigrants. 2023.
Omenka OI, Watson DP, Hendrie HC. Understanding the healthcare experiences and needs of African immigrants in the United States: a scoping review. BMC Public Health. 2020;20(1):27.
Khullar D, Chokshi DA. Challenges for immigrant health in the USA-the road to crisis. Lancet. 2019;393(10186):2168–74.
Jacobs DH, Tovar JM, Hung OL, et al. Behavioral Risk Factor and Preventive Health Care Practice Survey of Immigrants in the Emergency Department. 2002;9(6):599-608.https://doi.org/10.1111/j.1553-2712.2002.tb02297.x
Tarraf W, Vega W, González HM. Emergency Department Services Use Among Immigrant and Non-immigrant Groups in the United States. Journal of Immigrant and Minority Health. 2014;16(4):595-606.https://doi.org/10.1007/s10903-013-9802-z
Lebrun LA. Effects of length of stay and language proficiency on health care experiences among immigrants in Canada and the United States. Soc Sci Med. Apr 2012;74(7):1062-72.https://doi.org/10.1016/j.socscimed.2011.11.031
Mohanty SA, et al. Health Care expenditures of immigrants in the United States: a nationally Representative Analysis. Am J Public Health. 2005;95(8):1431–8.
Tarraf W, et al. Changes in Insurance Coverage and Healthcare Use among immigrants and US-Born adults following the Affordable Care Act. J Racial Ethnic Health Disparities. 2021;8(2):363–74.
Seo JY, et al. Disparities in Health Care utilization between Asian immigrant women and non-hispanic White women in the United States. J Womens Health (Larchmt). 2019;28(10):1368–77.
Pourat N, et al. Assessing health care services used by California’s undocumented immigrant population in 2010. Health Aff (Millwood). 2014;33(5):840–7.
Fang J, Ayala C, Loustalot F. Association of birthplace and self-reported hypertension by racial/ethnic groups among US adults–National Health interview Survey, 2006–2010. J Hypertens. 2012;30(12):2285–92.
Fang J et al. Association of Birthplace and Coronary Heart Disease and Stroke among US adults: National Health Interview Survey, 2006 to 2014. J Am Heart Assoc, 2018. 7(7).
Jones RE, Tasnim L, Cunningham SA. The prevalence of Multimorbidity among Foreign-born adults in the United States. Volume 32. Ethnicity & Disease; 2022. pp. 213–22. 3.
Payton C, et al. Preventive care and management of chronic diseases in immigrant adults. Prim Care. 2021;48(1):83–97.
Monserud MA. Age trajectories of Physical Health among older adults of Mexican descent: implications of immigrant status, age at Immigration, and gender. J Aging Health. 2019;31(1):3–36.
Wieland ML, et al. Diabetes Care among Somali immigrants and refugees. J Community Health. 2012;37(3):680–4.
Antecol H, Bedard K. Unhealthy assimilation: why do immigrants converge to American health status levels? Demography. 2006;43(2):337–60.
Kind AJH, Buckingham WR. Making Neighborhood-Disadvantage Metrics Accessible - The Neighborhood Atlas. N Engl J Med. 2018;378(26):2456–8.
The R project for statistical computing.
Yun K, et al. High prevalence of chronic non-communicable conditions among adult refugees: implications for practice and policy. J Community Health. 2012;37(5):1110–8.
Kariotis TC, et al. Impact of Electronic Health Records on Information Practices in Mental Health Contexts: scoping review. J Med Internet Res. 2022;24(5):e30405.
Hinderaker K, Weinmann A. Association of patients’ perception of primary care provider listening with Emergency Department Use. PRiMER. 2020;4:7.
Maeng DD, Hao J, Bulger JB. Patterns of multiple Emergency Department visits: do Primary Care Physicians Matter? Perm J. 2017;21:16–063.
Jirmanus LZ, et al. Impact of United States 2017 Immigration Policy changes on missed appointments at two Massachusetts Safety-Net hospitals. J Immigr Minor Health. 2022;24(4):807–18.
Rodriguez RM, et al. Declared impact of the US President’s statements and campaign statements on latino populations’ perceptions of safety and emergency care access. PLoS ONE. 2019;14(10):e0222837.
DeVries A, et al. Impact of medical homes on quality, healthcare utilization, and costs. Am J Manag Care. 2012;18(9):534–44.
Starfield B, Shi L, Macinko J. Contribution of primary care to health systems and health. Milbank Q. 2005;83(3):457–502.
Shommu NS, et al. What is the scope of improving immigrant and ethnic minority healthcare using community navigators: a systematic scoping review. Int J Equity Health. 2016;15:6.
Gao J, et al. The Effect of Primary Care visits on total patient care cost: evidence from the Veterans Health Administration. J Prim Care Community Health. 2022;13:21501319221141792.
Basu S, et al. Association of Primary Care Physician Supply with Population Mortality in the United States, 2005–2015. JAMA Intern Med. 2019;179(4):506–14.
Knowles M, et al. Community Health Worker Integration with and Effectiveness in Health Care and Public Health in the United States. Annu Rev Public Health. 2023;44:363–81.
Ye W, Rodriguez JM. Highly vulnerable communities and the Affordable Care Act: Health insurance coverage effects, 2010–2018. Soc Sci Med. 2021;270:113670.
Rao P, Girosi F, Eibner C. Expanding Insurance Coverage to Undocumented immigrants in Connecticut. Rand Health Q. 2022;10(1):3.
Roy CM, et al. Assessing the indirect effects of COVID-19 on healthcare delivery, utilization and health outcomes: a scoping review. Eur J Public Health. 2021;31(3):634–40.
Acknowledgements
We would like to extend our thanks and appreciation to Dr. Claire Edelson and Kippie Lipham for their support with this project. The authors received no specific funding for this work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no financial disclosures or conflicts of interest.
Meetings & Grants
Selected for poster presentation at Southeastern Medical Scientist Symposium, November 18–19, 2023.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Bakdash, L., Chai, N., Olakunle, O.E. et al. Health Status and Healthcare Utilization Patterns of Emergency Department Patients Who Prefer a Language Other Than English. J Immigrant Minority Health (2024). https://doi.org/10.1007/s10903-024-01623-4
Accepted:
Published:
DOI: https://doi.org/10.1007/s10903-024-01623-4