Abstract
Rotational Thromboelastometry (ROTEM) Delta has been described in several postpartum hemorrhage algorithms, but this device requires pipetting and careful mixing of reagents to initiate the clotting reaction. In contrast, thromboelastography (TEG 6s) and the Quantra devices operate utilizing an automated pre-mixed cartridge that only requires a blood sample to start the clot strength analysis. We compared the correlation between 3 point of care viscoelastic testing (POCVT) devices to laboratory Clauss fibrinogen and platelets, their inter-device correlation, and the total running time difference between Quantra and ROTEM. A high correlation was noted between the Clauss fibrinogen and the fibrinogen parameters from ROTEM (r = 0.76–0.84, P < 0.0001), TEG6s (r = 0.71, P < 0.0001) and Quantra (r = 0.72, P = 0.0001). A moderate correlation between laboratory platelets and the ROTEM (r = 0.54;0.45, P < 0.0001; P = 0.0013) and Quantra (r = 0.66, P = 0.0001) parameters was noted. The inter-device correlation showed to be high when comparing the fibrinogen parameters of TEG6s and Quantra to that of ROTEM (r = 0.88 and 0.74, P < 0.0001, respectively). In contrast, a moderate correlation was noted between the platelet parameters of Quantra and ROTEM (r = 0.51, p = 0.0036). The Quantra device resulted 20.9 min (95% CI -0.2 to 4.7, P = 0.07) faster than the ROTEM if the warming and pipetting of reagents of the latter were considered. All the POCVT devices demonstrated a high correlation to laboratory Clauss fibrinogen, making each beneficial for the early recognition and management of hypofibrinogenemia.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Postpartum hemorrhage (PPH) remains a predominant worldwide cause of maternal morbidity and mortality.[1] In cases of PPH, fibrinogen is the most rapid biomarker to decline, and hypofibrinogenemia is the most common coagulopathy.[2, 3] Low fibrinogen levels (< 2 g/L) have been shown to be a good predictor of severe hemorrhage.[4] Hence, there is a growing need to quickly monitor and report fibrinogen levels or a surrogate of it in cases of ongoing bleeding. Acting as the gold standard measurement, the Clauss fibrinogen level has a one-hour turnaround time, making it less than ideal for PPH management.[2, 5] It is for this reason that over the last decade, priority has been placed on prompt and efficient monitoring with subsequent replacement of this crucial factor as clinically indicated.[2, 6,7,8] In this respect, point of care viscoelastic testing (POCVT) devices, particularly the Rotational thromboelastometry (ROTEM) delta (TEM innovations GmbH, Munich, Germany), have demonstrated a high correlation to Clauss fibrinogen in the obstetric literature.[2, 5, 9,10,11].
Although not widely accepted, the use of POCVT guided algorithms for the management of PPH are supported by some institutions, task force groups, and several clinical guidelines.[2, 12,13,14] Proponents of its use cite the importance of real-time fibrinogen estimates in cases of PPH, whereas opposers argue that there is a lack of evidence for its use.[2, 6, 15] Despite the lack of consensus, some POCVT has adopted newer technology advancements resulting in fully automated and cartridge-based platforms. These technology adaptations may increase acceptability, as these new devices are smaller and are easier to calibrate and operate.
There are three leading platforms of POCVT currently available in the United States. Two of the available platforms provide cartridge-based technology approved by the Federal Drug Administration (FDA): the TEG6s (Haemonetics Corporation, Braintree, MA, USA) and Quantra QPlus system (HemoSonics, LLC, Charlottesville, VA), whereas the new ROTEM sigma (Wefen, Barcelona, Spain) has not received FDA approval in the United States. In comparison to previous POCVT platforms, these technological advancements capitalize on the use of pre-filled reagent wells, avoiding the need for pipetting, thus decreasing variability.[2, 5] The primary aim of this study was to compare the different platform output parameters against conventional laboratory tests, specifically platelet count and Clauss fibrinogen level. Our secondary aim was to compare the parameters provided by the Quantra and TEG6s against the Rotational thromboelastometry (ROTEM) delta, our current point of care viscoelastic testing (POCVT) interface. Lastly, we determine the difference in time related to processing, and obtaining results between the Quantra and the ROTEM.
1 Methods
This prospective observational study was approved by our institutional review board (IRB# 1,308,012,621). Verbal informed consent was considered sufficient as the study was deemed a quality assurance for testing the ability of Quantra or TEG6s to replace our current ROTEM device. We obtained the anonymized data from patients presenting for elective cesarean delivery during the months at which the Quantra (August 15 - Sept 1, 2020) and the TEG6s (June 1 - July 15, 2021) were trialed. POCVT and routine blood test results were available on the day of surgery and were entered into an anonymized spread sheet. Our study adhered to the applicable Enhancing the QUAlity and Transparency Of health Research (EQUATOR) guidelines.
2 Blood sampling and measurements
Blood samples from healthy pregnant women at their third trimester of pregnancy were obtained during their admission for scheduled cesarean delivery. The blood sample was obtained for patients with risk factors associated with PPH and for any patient we would have routinely ordered a ROTEM as part of our standard of care (e.g., patients scheduled for repeat cesarean delivery ≥ 3, history of PPH). Two samples were collected in 3 ml evacuated blood collection tubes containing 3.2% sodium citrate (blue top) at the time of intravenous cannulation. One of the samples was sent for Laboratory assays (e.g., Complete blood count and Clauss fibrinogen level) and analyzed, as per our standard of care. The second blood sample was simultaneously analyzed by ROTEM and the Quantra(R) plus or TEG6s. In the case of the Quantra plus, a physician independent from patient care noted the times at which a sample was processed (blood inserted into the cartridge or pipetting was started), and the time at which each device reported their corresponding parameters. In the case of ROTEM, we established the report of amplitude at 10 min as the end point as this the value we use for making clinical decisions.
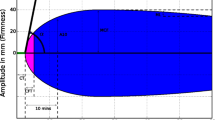
For the ROTEM device, we made sure that the liquid quality control was performed and passed weekly, and that the reagents were out for at least 15 min to bring them to room temperature, as recommended by the manufacturer. Each sample was run in accordance with the instructions provided by the manufacturer. The ROTEM parameters included the Amplitude at 10 min (A10) for the EXTrinsic ThromboElastoMetry (EXTEM) and FIBrinogen ThromboElastoMetry (FIBTEM) assays. Although not a reported parameter for the ROTEM, we calculated the platelet contribution to the clot stiffness utilizing the formula EXTEM A10-FIBTEM A10 = PLTEM, as previously described by Toffaletti et al.[16].
For the Quantra sample analysis, we assured that the device had passed its liquid control quality assurance test before running our samples. The Quantra QPlUS cartridge was used to perform our whole blood coagulation test. The cartridge was inserted into the machine, and the blue top sample was inverted and pushed into its designated chamber until the reaction was initiated. All procedures were performed according to the manufacturer’s guidelines. The analogous parameters to those of the ROTEM include clot stiffness (CS), fibrinogen (FCS) and platelet (PCS) contribution to clot stiffness. The POCVT ROTEM A10 run time (A10-RT) and Quantra run time (Q-RT) were defined as the time from mixing the reagents until obtaining the A10 in the case for the ROTEM, and time the sample was inserted in the cartridge until result. Total ROTEM A10 was defined as A10-RT plus the 15 min required for reagents to become room temperature as recommended by the manufacturer. [3]
Blood sample and parameters from the ROTEM were obtained as previously described (see ROTEM versus Quantra). As for the TEG6s, we assured that the device had passed the liquid control quality assurance test, and we introduced their cartridge into the system. A small amount of blood was then introduced into the loaded cartridge. All procedures were performed according to the manufacturer’s recommendations. The reported parameters for the TEG6s included: Citrated Rapid Teg Maximum Amplitude (CRT MA) and Citrated Functional Fibrinogen (CFF). The parameter for assessment of platelet contribution to clot stiffness was calculated as CRT MA – CFF = PLTEG, as described by Roberts et al.[2].
3 Statistical Analysis
Pearson correlation coefficients were used to estimate the linear associations between these variables. All hypothesis tests and confidence intervals are two-sided. We compared the mean times of the monitors using paired t-tests. A p-value of 0.05 was considered statistically significant. All analyses were conducted using the Stata (version 16.0) statistical package.
4 Results
4.1 Quantra versus Rotem
Thirty samples were analyzed for this comparison. The median (interquartile range) results for the ROTEM and Quantra results are summarized in Table 1. The median values for these two devices are markedly different due to the units utilized for measurement of millimeters (mm) for ROTEM and hectopascal (hPa) for Quantra. A summary of the Pearson correlation coefficients for inter-device and laboratory assays versus device comparisons are summarized in Fig. 1. A strong inter-device association between the clotting times of the ROTEM (INTEM CT) and the Quantra (CT) was noted (r = 0.70, P < 0.0001). When performing an inter-device comparison of the parameter related to fibrinogen for ROTEM (FIBTEM A10) and Quantra (FCS), a high correlation was noted between the devices (r = 0.74, P < 0.0001). The ROTEM and Quantra fibrinogen parameters demonstrated a high correlation to the measured Clauss fibrinogen levels (r = 0.84, P < 0.0001 and r = 0.72, P = 0.0001 for Fibtem A10 and FCS, respectively). A moderate correlation between PLTEM and PCS (r = 0.51, P = 0.0036) was noted. The correlation between the laboratory value of platelet count and PCS, PLTEM were r = 0.66, P = 0.0001 and r = 0.45, P = 0.0133, respectively. The mean (standard deviation) for the A10-RT, total ROTEM A10 time (A10-RT + 15 min), and Q-RT were 14.5 (6.40), 33.1 (6.48), and 12.2 (0.58), respectively. When excluding the 15 min recommended by the manufacturer to bringing the reagents to room temperature (A10 – RT) the difference between A10-RT and Q-RT was 2.3 min, 95% CI -0.2 to 4.7, P = 0.0656, and bordered on being statically different, while that of the total ROTEM A10 (A10-RT + 15 min) and Q-RT was significantly different at 20.9 min, 95% CI 18.4 to 23.4, P < 0.0001.
[A] Correlation between Clauss Fibrinogen level against the Fibrinogen thromboelastometry amplitude at 10 min FIBTEM A10. [B] Correlation between Clauss Fibrinogen level against the Quantra fibrinogen clot stiffness (FCS) parameter. [C] Inter- device correlation of FIBTEM and FCS. [D] Correlation between the platelet levels by laboratory assays against the calculated of platelet contribution, calculated by subtracting the Extrensic thromboelastometry at 10 min (EXTEM A10) minus the fibrinogen contribution (FIBTEM A10). [E] Correlation between the platelet laboratory assay against the platelet clot stiffness (PCS) derived from the Quantra device. [F] Correlation between the calculated platelet contribution (EXTEM – FIBTEM) against PCS. [G] Correlation between ROTEM Clotting time (CT) and Quantra CT
4.2 TEG6s versus Rotem
Forty-eight samples were analyzed for comparison. The median (interquartile range) results for the ROTEM and TEG6s results are summarized in Table 1. A summary of the Pearson correlation coefficients for inter-device, and laboratory assays versus device comparisons are summarized in Fig. 2. A moderate inter-device association between the clotting times of the ROTEM (INTEM CT) and the TEG6s (CK R) was noted (r = 0.40, P < 0.025). When performing an inter-device comparison of the parameter related to fibrinogen for ROTEM (FIBTEM A10) and TEG6s (FF MA) a high correlation was noted between the devices (r = 0.88, P < 0.0001). When comparing the fibrinogen parameters for ROTEM (FIBTEM A10) and TEG6s (CFF- MA) to the Clauss fibrinogen, a high correlation was noted between the devices and the laboratory assay with an r = 0.76, P < 0.0001 and r = 0.71, P < 0.0001, respectively. When comparing the laboratory values of platelets to the derived PLTEM and PLTEG, the correlation was noted to be modest and poor with an r = 0.54, P < 0.0001 and r = -0.20, P = 0.18, respectively. The average run time for this device was ~ 11 min (data not shown).
[A] Correlatrion between Clauss Fibrinogen level and the Rotational thromboelastometry (ROTEM) parameter for measuring fibrinogen – FIBTEM. [B] Correlation between Clauss Fibrinogen level and the thromboelastography (TEG 6s) parameter for measuring fibrinogen -CFF at maximum amplitude (MA). [C] Inter- device correlation of the FIBTEM and CFF – MA. [D] Correlation between the platelet levels by laboratory assays against the calculated of platelet contribution, calculated by subtracting the Extrensic thromboelastometry at 10 min (EXTEM A10) minus the fibrinogen contribution (FIBTEM A10). [E] Correlation between the platelet levels by laboratory assays against the calculated of platelet contribution, calculated by subtracting the Citrated rapid maximum amplitude (CRT MA) minus the fibrinogen contribution (CFF MA). [F] Correlation between ROTEM clotting time (CT) and TEG6s (CT)
5 Discussion
The key finding in our study is that ROTEM, Quantra, and TEG6s demonstrated a strong correlation between the Clauss fibrinogen level and their relevant measures, FIBTEM A10 (r = 0.76–0.84), FCS (r = 0.72), and FF (r = 0.71). Our findings corroborate the findings from previous studies that have reported a correlation between fibrinogen level and FIBTEM, FCS, and FF of r = 0.59,[9] 0.78[5] and 0.68[2] respectively. Although not a linear correlation, most studies thus far have demonstrated that all three devices can be used for monitoring and estimating the trends in fibrinogen levels.[2, 9, 17] Indeed, Collins et al.,[10] demonstrated that a FIBTEM A5 < 10 (which corresponds to a fibrinogen < 2 g/L) clinically correlated with the trends of Clauss fibrinogen, and the FIBTEM could be used as an early biomarker to predict patients at risk for severe hemorrhage. All three devices have been shown to have clinically acceptable sensitivity and specificity, making them a safe and efficient way to provide close to real-time monitoring of fibrinogen levels and decide upon blood product transfusion management.[2, 3, 5] In recent years, several tertiary care centers have published their experience utilizing POCVT, demonstrating a reduction in blood product administration, transfusion-associated circulatory overload, and a trend towards fewer intensive care admissions, thus demonstrating that the correlation between these device parameters and Clauss fibrinogen is strong enough to improve maternal outcomes.[6, 8, 18].
One of the greatest advantages of POCVT, is their availability to provide results within 10–15 min, as opposed to laboratory alternatives that may take up to 60 min to result.[2, 10] The ROTEM delta, requires for the reagents to be at room temperature at the time of testing. This, according to the manufacturer instruction requires at least 15 min.[19] Besides, once the reagents are at room temperature, a trained physician or technician needs to carefully pipet the reagents to run the test. Our study demonstrated that the cartridge-based Quantra can provide results 18–23 min (20.9 min, 95% CI 18.4–23.4, P < 0.0001) faster than the ROTEM when warming of reagent is considered. The advantage of Quantra in terms of time disappears if the 15 min for bringing reagents to room temperature. Hence to produce similar results in terms of time outcomes all hemorrhage cases would need to be predicted by the clinician. The newer POCVT platforms, Quantra and TEG6s, have implemented the use of a fully automatic cartridge base technology that can be stored at room temperature. These implementations allow for shorter turnaround of results, and decreased end user variability. Our study results corroborate those of Idowu et al.,[20] who was able to demonstrate a statistically significant difference between the mean time needed to produce results for the Quantra (13 min) versus the non-cartridge base TEG 5000 (mean time of 57 min). Furthermore, when the time for transporting and processing the samples was taken into account, the total time to obtain results were 25 min versus 92 min for the Quantra and TEG 5000, respectively.[20] This comparison highlights that the handling of the blood sample and the location of the device may impact the time it takes for the results to be available to the team making clinical decisions.[2, 21, 22] To address this limitation, software has been developed to allow for remote real-time access as early as 5 min of starting the whole blood analysis.
Previously reported parameters for the recognition of hypofibrinogenemia (< 2 g/L) have been described as FIBTEM A5 (10 mm) or FIBTEM A10 (12 mm), CFF at 10 ≤ 17 and FCS < 1.9 hPa for ROTEM, TEG6s and Quantra, respectively.[2, 5, 16] When utilizing ROTEM, Collins et al.,[10] demonstrated that parturients with ongoing bleeding at study entry, and a FIBTEM A5 < 10 mm or fibrinogen level < 2 g/L had a 100% positive predictive value of requiring a blood product transfusion. For the TEG6s, a CFF at 10 ≤ 17 was noted to reflect a fibrinogen level of ≤ 2 g/L with a sensitivity of 0.74 and a specificity of 0.97.[2] For the Quantra device, although not in an obstetric population, an FCS < 1.9 was associated with fibrinogen level of ≤ 2 g/L with a sensitivity of 0.85 and a specificity of 0.76.[5]While it is well known that early fibrinogen deficiency develops during PPH, potential relationships between PPH and other clotting factors remains unclear. There is some evidence to suggest that PT and PTT remain unaffected in cases of severe hemorrhage and up to 5 L of blood loss.[4, 23] When enzymatic coagulation factor deficiency is present, the use of ROTEM-EXTEM CT, TEG6s CK-R and Quantra CT can guide the transfusion management, although with some limitations.[2, 9, 24, 25].
Platelets are the backbone of the coagulation cascade, and in addition to fibrin, gives clot the strength that is measured by POCVT as maximum amplitude (MA) [ROTEM and TEG] or clot stiffness (Quantra).[26, 27] Our study suggests that there was moderate correlation between laboratory platelet counts and Quanta, as well as with the calculated platelet contribution (PLTEM) for ROTEM. On the other hand, the correlation between the laboratory platelets and the calculated platelet contribution (PLTEG) for TEG6s was poor. The latter, contrasts with the moderate TEG6s and laboratory platelets correlation (r = 0.59) reported by Roberts et al. [2] This difference may be explained by the fact that Roberts et al.,[2] utilized the clot elasticity formula*, whereas we utilized the amplitude in mm as reported by the device. Solomon et al.,[28] has postulated that when utilizing amplitude instead of clot elasticity there is an inherent overestimation of the contribution of fibrinogen, which could have resulted in a lower calculated platelet contribution.
Clinically, the use of POCVT for the assessment of platelet transfusion triggers has been previously documented and known to have limitations. Some authors recommend considering platelet transfusion when the ROTEM results are consistent with any of the following: EXTEM A10 – FIBTEM A10 < 30, FIBTEM A10 > 10 mm and EXTEM A10 ≤ 40 mm, or EXTEM A5 < 47 when FIBTEM A5 > 12 mm. [9, 28, 29]. For the TEG 6s, Roberts et al.,[2] recommends considering platelet transfusion (equivalent of platelets < 75 × 109/L) when CRT- MA < 57 mm and CFF at 10 > 15 mm (positive and negative predicted value 80% and 99%, respecively). Although no robust obstetric literature at this moment exists for the guidance of platelet transfusions when utilizing Quantra, Naik et al.,[5] described a 100% negative predictive value for PCS < 11.2 Pa for platelets < 50 × 109/L, or PCS < 12.1 for 80 × 109/L. Hence although there is some guidance as to how to use these devices for assessing platelet contribution to the clot stiffness, some experts recommend the use of laboratory values to make decisions regarding the need for platelet transfusions.[30].
This study has limitations. Our sample size was small, secondary to the short duration trials for the TEG6s and ROTEM at our institution. All samples evaluated were considered “normal”, hence, we did not evaluate the correlation of these devices in active hemorrhaging cases. The variation in the correlation between ROTEM versus fibrinogen when comparing ROTEM to TEG6s and Quantra reflects that our sample size was small, smaller variations were to be expected had we had a larger sample. Ideally, when comparing these devices against the laboratory values one would like to have a large sample size that includes patients with and without coagulopathy to determine sensitivity and specificity of the parameters. Besides, we did not measure the TEG6s total running time as we did not have an independent physician annotating the time of results as was done for the Quantra trial. The clotting times from the devices were not compared to the laboratory PT/PTT, INR, as this is not part of our standard of care.
In conclusion, all three devices demonstrated a strong correlation to the Clauss fibrinogen assay, and increasingly, data suggests positive outcomes in the care of parturients with PPH when these devices are used. The use of cartridge-based technology may offer clinically significant faster results in cases of unexpected hemorrhage, as it does not require reagents to reach room temperature, or cumbersome pipetting. The Quantra device is the only one to provide information about the platelet contribution to the overall clot stiffness (PCS) without the need for additional calculation. Although several methods to calculate the platelet contribution to overall clot stiffness has been described (e.g., PLTEM, PLTEG), our study suggests that the use of POCVT for the guidance of platelet transfusion requires more research. Given the high correlation between the fibrinogen parameters and the Clauss fibrinogen, all three devices could be utilized for the management of postpartum hemorrhage, although multicenter randomized controlled trials are needed for validation of these results.
References
Owen MD, Cassidy AL, Weeks AD. Why are women still dying from obstetric hemorrhage? A narrative review of perspectives from high and low resource settings. Int J Obstet Anesth. 2021;46:102982.
Roberts TCD, Lloyd LD, Bell SF, Cohen L, James D, Ridgway A, et al. Utility of viscoelastography with TEG 6s to direct management of haemostasis during obstetric haemorrhage: a prospective observational study. Int J Obstet Anesth. 2021;47:103192.
Huissoud C, Carrabin N, Audibert F, Levrat A, Massignon D, Berland M, et al. Bedside assessment of fibrinogen level in postpartum haemorrhage by thrombelastometry. Bjog Int J Obstetrics Gynaecol. 2009;116:1097–102.
CHARBIT B, MANDELBROT L, BARON SAMAINE, HADDAOUI G. B, KEITA H, et al. The decrease of fibrinogen is an early predictor of the severity of postpartum hemorrhage. J Thromb Haemost. 2007;5:266 273.
Naik BI, Tanaka K, Sudhagoni RG, Viola F. Prediction of hypofibrinogenemia and thrombocytopenia at the point of care with the Quantra® QPlus® System. Thromb Res. 2021;197:88–93.
Bell SF, Collis RE, Pallmann P, Bailey C, James K, John M, et al. Reduction in massive postpartum haemorrhage and red blood cell transfusion during a national quality improvement project, Obstetric Bleeding Strategy for Wales, OBS Cymru: an observational study. Bmc Pregnancy Childb. 2021;21:377.
Bell SF, Collis RE, Bailey C, James K, John M, Kelly K, et al. The incidence, aetiology, and coagulation management of massive postpartum haemorrhage: a two-year national prospective cohort study. Int J Obstet Anesth. 2021;102983.
McNamara H, Kenyon C, Smith R, Mallaiah S, Barclay P. Four years’ experience of a ROTEM®-guided algorithm for treatment of coagulopathy in obstetric haemorrhage. Anaesthesia. 2019;74:984–91.
Collis RE, Kenyon C, Roberts TCD, McNamara H. When does obstetric coagulopathy occur and how do I manage it? Int J Obstet Anesth. 2021;46:102979.
Collins PW, Lilley G, Bruynseels D, Laurent DB-St, Cannings-John R, Precious E, et al. Fibrin-based clot formation as an early and rapid biomarker for progression of postpartum hemorrhage: a prospective study. Blood. 2014;124:1727–36.
Seto S, Itakura A, Okagaki R, Suzuki M, Ishihara O. An algorithm for the management of coagulopathy from postpartum hemorrhage, using fibrinogen concentrate as first-line therapy. Int J Obstet Anesth [Internet]. 2017;32:11 16. Available from: http://linkinghub.elsevier.com/retrieve/pii/S0959289X1630108X.
Collins P, Abdul-Kadir R, Thachil J, Coagulation TS. on W s HI in T and H and on DI. Management of coagulopathy associated with postpartum hemorrhage: guidance from the SSC of the ISTH. J Thromb Haemost. 2016;14:205–10.
Collins PW, Cannings-John R, Bruynseels D, Mallaiah S, Dick J, Elton C, et al. Viscoelastometric-guided early fibrinogen concentrate replacement during postpartum haemorrhage: OBS2, a double-blind randomized controlled trial. Brit J Anaesth. 2017;119:411–21.
Management AS of ATF on PB. Practice Guidelines for Perioperative Blood Management. Anesthesiology. 2015;122:241–75.
Amgalan A, Allen T, Othman M, Ahmadzia HK. Systematic review of viscoelastic testing (TEG/ROTEM) in obstetrics and recommendations from the women’s SSC of the ISTH. J Thromb Haemost. 2020;18:1813–38.
Toffaletti JG, Buckner KA. Use of Earlier-Reported Rotational Thromboelastometry Parameters to Evaluate Clotting Status, Fibrinogen, and Platelet Activities in Postpartum Hemorrhage Compared to Surgery and Intensive Care Patients. Anesth Analgesia. 2019;128:414–23.
DeAnda A, Levy G, Kinsky M, Sanjoto P, Garcia M, Avandsalehi KR, et al. Comparison of the Quantra QPlus System With Thromboelastography in Cardiac Surgery. J Cardiothor Vasc An. 2021;35:1030–6.
Snegovskikh D, Souza D, Walton Z, Dai F, Rachler R, Garay A, et al. Point-of-care viscoelastic testing improves the outcome of pregnancies complicated by severe postpartum hemorrhage. J Clin Anesth. 2018;44:50 56.
Huissoud C, Carrabin N, Benchaib M, Fontaine O, Levrat A, Massignon D, et al. Coagulation assessment by rotation thrombelastometry in normal pregnancy. Thromb Haemostasis. 2009;101:755–61.
Idowu O, Ifeanyi-Pillette I, Owusu‐Agyemang P, Holmes A, Kwater P, Jackson T, et al. The quantra hemostasis analyzer compared to thromboelastography (TEG) in the surgical oncologic population: A prospective observational trial. J Surg Oncol. 2021.
Waters JH, Bonnet MP. When and how should I transfuse during obstetric hemorrhage? Int J Obstet Anesth. 2021;46:102973.
Reale SC, Farber MK. Point-of-Care Coagulation Testing for Obstetric Hemorrhage: Time for a Theranostic Approach? Int J Obstet Anesth. 2019;38:1–3.
Lloyd L de, Bovington R, Kaye A, Collis RE, Rayment R, Sanders J, et al. Standard haemostatic tests following major obstetric haemorrhage. Int J Obstet Anesth. 2011;20:135–41.
Groves DS, Welsby IJ, Naik BI, Tanaka K, Hauck JN, Greenberg CS, et al. Multicenter Evaluation of the Quantra QPlus System in Adult Patients Undergoing Major Surgical Procedures. Anesth Analgesia. 2020;130:899–909.
Rigouzzo A, Louvet N, Favier R, Ore M-V, Piana F, Girault L, et al. Assessment of Coagulation by Thromboelastography During Ongoing Postpartum Hemorrhage: A Retrospective Cohort Analysis. Anesth Analgesia. 2020;130:416–25.
Inaba K, Rizoli S, Veigas PV, Callum J, Davenport R, Hess J, et al. 2014 Consensus conference on viscoelastic test–based transfusion guidelines for early trauma resuscitation. J Trauma Acute Care. 2015;78:1220–9.
Collins PW, Solomon C, Sutor K, Crispin D, Hochleitner G, Rizoli S, et al. Theoretical modelling of fibrinogen supplementation with therapeutic plasma, cryoprecipitate, or fibrinogen concentrate. Bja Br J Anaesth. 2014;113:585–95.
Solomon C, Ranucci M, Hochleitner G, Schöchl H, Schlimp CJ. Assessing the Methodology for Calculating Platelet Contribution to Clot Strength (Platelet Component) in Thromboelastometry and Thrombelastography. Anesth Analgesia. 2015;121:868–78.
Fiol AG, Fardelmann KL, McGuire PJ, Merriam AA, Miller A, Alian A. The Application of ROTEM in a Parturient With Antiphospholipid Syndrome in the Setting of Anticoagulation for Cesarean Delivery: A Case Report. Pract. 2020;14:e01182.
Butwick A, Lyell D, Goodnough L. How do I manage severe postpartum hemorrhage? Transfusion. 2020;60:897–907.
Author information
Authors and Affiliations
Contributions
This author contributed to the analysis of the data.
Corresponding author
Ethics declarations
Financial disclosure
None.
Conflict of interest
None.
Additional information
* A part of this work was presented at the 2021 American Society of Anesthesiologist.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Gonzalez-Fiol, A., Fardelmann, K.L., Yanez, D. et al. Comparison between the Rotational Thromboelastometry (ROTEM) Delta device against the Cartridge-based Thromboelastography 6s and Quantra in a healthy third trimester pregnant cohort. J Clin Monit Comput 37, 267–273 (2023). https://doi.org/10.1007/s10877-022-00888-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10877-022-00888-0