Abstract
Annexin A10 (ANXA10) is a member of annexin A and has been reported to highly express in papillary thyroid carcinoma (PTC) tissues. Tumor susceptibility gene 101 (TSG101) also plays a role in PTC and is predicted to bind to ANXA10. This study intended to investigate whether ANXA10 could regulate PTC via binding to ANXA10. The expression of ANXA10 and TSG101 in normal thyroid follicular epithelial cell line and several PTC cell lines was analyzed using RT-qPCR and western blotting assays. Subsequently, PTC cell line BCPAP was silenced with ANXA10 followed by TSG101 overexpression or not, and then cell proliferation, apoptosis and mitogen-activated protein kinase (MAPK) signaling expression were assessed via MTT, colony formation, immunofluorescence staining, Tunel staining and western blotting assays. Besides, the interaction between ANXA10 and TSG101 was validated using Co-immunoprecipitation assay. ANXA10 and TSG101 expressions were up-regulated in PTC cell lines. ANXA10 silence inhibited proliferation, promoted apoptosis and inactivated MAPK/ extracellular regulated protein kinases (ERK) signaling pathway of BCPAP cells. Additionally, ANXA10 could bind to TSG101 and regulate its expression. However, the above effects of ANXA10 silence on BCPAP cells were all blocked by TSG101 overexpression. ANXA10 inhibited proliferation and promoted apoptosis of PTC cells via binding to TSG101, and these actions may depend on down-regulating MAPK/ERK pathway expression.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Thyroid cancer (TC) is one of the common malignant tumors in humans and the most common tumor in the endocrine system. In the past few decades, the incidence of TC has shown a significant upward trend worldwide (Seib and Sosa 2019). It is predicted that TC will become the fourth largest tumor in the United States in 2030 after breast cancer, prostate cancer, and lung cancer (Rahib et al. 2014). According to the different sources of tumor cells, TC is usually divided into four pathological types: papillary carcinoma, medullary carcinoma, follicular carcinoma and undifferentiated carcinoma. Among them, papillary thyroid carcinoma (PTC) is the most common pathological type, accounting for about 88% of all TC (Kitahara and Sosa 2016). Therefore, it is of great value to carry out relevant basic research to clarify the molecular mechanism of the occurrence and development of PTC.
Annexin A10 (ANXA10) is a new member of the annexin A (ANXA) family. ANXA is a subclass of the annexin, which is the largest type of Ca2+-regulated phospholipid binding protein in eukaryotic cells, and plays an important role in various cellular and physiological processes, including vesicle transport, exocytosis, endocytosis and calcium channel formation, thereby regulating cell differentiation and proliferation and other activities (Gerke et al. 2005; Gerke and Moss 2002). The abnormal expression and regulatory effect of ANXA10 in various cancers including lung cancer, serous epithelial ovarian cancer, bladder cancer, esophageal squamous cell carcinoma, cholangiocarcinoma and pancreatic cancer have been implicated and the role of ANXA10 in different cancers is also different (Hung et al. 2019; Kodaira et al. 2019; Munksgaard et al. 2011; Sun et al. 2019; Wang et al. 2019; Zhu et al. 2017). A recent study reported that among all ANXA members, ANXA10 has the highest expression in PTC. Compared with normal thyroid tissue, ANXA10 in PTC tissues was significantly up-regulated. Meanwhile, the expression of ANXA10 is related to the tumor size, differentiation and overall survival rate of patients with PTC (Liu et al. 2021). As a result, ANXA10 may be used as an independent prognostic biomarker to predict the poor prognosis of PTC. However, the effect and mechanism of ANXA10 on PTC cells have not been studied.
Tumor susceptibility gene 101 (TSG101) is a member of endosomal complexes required for transport-I (ESCRT-I) and plays an important role in cellular processes including endosomal transport, ubiquitination, promoting virus budding and maintaining cell survival (Kumar et al. 2016). A large number of studies have shown that the expression of TSG101 is significantly increased in many tumors, such as liver cancer, colorectal cancer, PTC, renal cell carcinoma and so on (Liu et al. 2002, 2019; Sai et al. 2015; Xu and Zheng 2019). Rue-Tsuan Li et al. (Liu et al. 2002) analyzed the expression of TSG101 gene in 20 cases of human PTC and determined the close association between the overexpression of TSG101 protein and human PTC. Notably, following searching the String website (https://www.string-db.org/cgi/network?taskId=btl6m3JYDIXW&sessionId=bYxCInv2T65G), we found that ANXA10 can bind to the TSG101 protein. Therefore, this study aimed to investigate whether ANXA10 can regulate PTC cells proliferation and apoptosis by interacting with TSG101.
Materials and methods
Cell culture
The human normal thyroid follicular epithelial cell line Nthy-ori 3–1 was obtained from BeNa Chuanglian Biotechnology Research Institute (Beijing, China). Human PTC cell lines (BCPAP, TPC-1 and KTC-1) were obtained from Shanghai Institute of Biochemistry and Cell Biology (Shanghai, China). All cells were cultured in RPMI-1640 medium (Gibco; Thermo Fisher Scientific, Inc.) supplemented with 10% fetal bovine serum (FBS; Gibco) and 100 U/ml penicillin–streptomycin (Gibco), placed at 37 °C in a standard humidified incubator under a humid atmosphere of 5% CO2.
Cell transfection
To knockdown ANXA10 expression in BCPAP cells, short hairpin RNA (shRNA) targeting ANXA10 (shRNA-ANXA10-1 and shRNA-ANXA10-2) and corresponding negative control (shRNA-NC) were designed and synthesized by GenScript Biotech (Nanjing, China). To overexpress TSG101 in BCPAP cells, the TSG101 cDNA sequences were synthesized by GenScript Biotech and then inserted into the pcDNA3.1 vector (Invitrogen, USA). Empty pcDNA3.1 vector was used as the negative control. For transfection, BCPAP cells were seeded and grown in 6-well plates and plasmids were transfected using the Lipofectamine 2000 reagent (Invitrogen) according to the manufacturer’s instructions. At 48 h post-transfection, the cells were collected for next analysis.
MTT assay
Cell viability was measured using the MTT assay kit (Beyotime Institute of Biotechnology, China). Briefly, control or transfected BCPAP cells were seeded into 96-well plates at the density of 2 × 103/well. After being cultured under normal condition for 24, 48 and 72 h, cells were exposed to 10μL MTT solution for 4 h, followed by incubation with formazan lysis solution until the purple crystals were completely dissolved. Finally, the absorbance at 570 nm was measured using a spectrophotometer.
Colony formation
For the colony formation assays, the BCPAP cell suspension was resuspended in 1 mL RPMI-1640 medium and then plated into 24-well plates and incubated for 2 weeks. Then cells were fixed with methanol and stained with 0.5% crystal violet, colonies (> 50 cells) were counted under a Nikon Eclipse E600 microscope (Nikon Instruments, USA; magnification, × 100).
Real-time quantitative polymerasechain reaction (RT-qPCR)
Total RNA from cells was isolated with TRIzol reagent (Thermo Fisher Scientific, Inc.) according to the manufacturer’s instructions. Reverse transcription was performed using PrimeScript RT Reagent Kit (Takara, China) according to the manufacturer’s protocol. RT-qPCR was performed with SYBR Prime Script RT-PCR Kit (Takara) based on the manufacturer’s instructions. The levels of ANXA10 and TSG101 were calculated using the 2−ΔΔCt method after normalization to GAPDH. The expression levels were expressed as the fold change relative to the corresponding controls which were defined as 1.0. The primers used are as follows:
ANXA10, forward 5’-GGGGACCAGAGAGGAAGGAT-3’, and reverse 5’-TGCAGCATGGTTTTGTGCTC-3’;
TSG101, forward 5’-GCCAGCTCAAGAAAATGGTGT-3’, and reverse 5’-AGGCACAGGGATTGTTCCAG-3’;
GAPDH, forward 5’-CTGGGCTACACTGAGCACC-3’, and reverse 5’-AGTGGTCGTTGAGGGCAATG -3’.
Western blotting
Total protein was extracted from cells using RIPA lysis buffer (Beyotime Institute of Biotechnology) and then quantified by BCA kit (Thermo Fisher Scientific, Inc.). Equal amount of proteins (20 μg per lane) were mixed with loading buffer, subjected to 10% SDS-PAGE and then transferred onto PVDF membranes. After being blocked with 5% non-fat milk and incubated with the corresponding primary antibodies at 4 °C overnight, the menbranes were incubated with the corresponding horseradish peroxidase (HRP)-conjugated secondary antibodies. Finally, the signals were detected using an enhanced chemiluminescence (ECL)-detection kit (Thermo Fisher Scientific, Inc.), followed by analysis with Tanon 5200 Chemiluminescent Imaging System (BioTanon, Shanghai, China). Primary antibodies used are antibodies against ANXA10 (cat. no. ab213656; 1:1,000), Bcl-2 (cat. no. ab32124; 1:1,000), Bax (cat. no. ab32503; 1:1,000), cleaved-caspase3 (cat. no. ab2302; 1:1,000), caspase3 (cat. no. ab32351; 1:5,000), cleaved-caspase9 (cat. no. ab2324; 1:1,000), caspase9 (cat. no. ab32539; 1:5,000), TSG101 (cat. no. ab125011; 1:5,000), phosphorylated (p)-extracellular regulated protein kinases (ERK; cat. no. ab201015; 1:1,000), ERK (cat. no. ab32537; 1:1000), p–c-Jun N-terminal kinase (JNK) (cat. no. ab76572; 1:5,000), JNK (cat. no. ab208035; 1:2,000), p-p38 (cat. no. ab178867; 1:1,000), p38 (cat. no. ab170099; 1:5,000) and GAPDH (cat. no. ab181602; 1:10,000), which were all purchased from Abcam. The secondary antibody was an HRP-conjugated goat anti-rabbit IgG (Abcam; cat. no. ab205718; 1:20,000). Protein expression levels were semi-quantified using Image-Pro Plus software version 6.0 (Roper Technologies, Inc.).
Immunofluorescence staining
BCPAP cells were fixed with 4% paraformaldehyde at 4˚C for 15 min and permeabilized with 0.2% Triton X-100 at 37˚C for 30 min. After being blocked with 10% Bovine Serum Albumin (Thermo Fisher Scientific, Inc.) for 30 min at room temperature, the cells were then incubated with primary antibodies against Ki67 (cat. no. ab15580; 1:500; Abcam) at 4˚C overnight. The following day, the cells were incubated with 100 μl/well working solution containing Alexa Fluor 488-conjugated goat anti-rabbit secondary antibodies (Abcam; cat. no. ab150081; 1:1,000) at room temperature for 1 h. DAPI was used for nuclear counterstaining. The stained slides were imaged using an inverted fluorescence microscope (magnification, × 200; Olympus Corporation).
Terminal-deoxynucleoitidyl Transferase Mediated Nick End Labeling (Tunel) staining
Cell apoptosis was assessed with the In Situ Cell Death Detection Fluorescein Kit (Roche, Germany). BCPAP cells on coverslips were immobilized using 4% paraformaldehyde for 1 h, then permeabilized using 0.1% citrate buffer (Sigma-Aldrich) with additional 0.1% Triton X-100 (Sigma-Aldrich). After being rinsed using PBS, cells were incubated for 1 h in TUNEL reaction solution. Coverslips were mounted to a slide and observed via an inverted fluorescence microscope (magnification, × 100; Olympus Corporation). DAPI was used for nuclear counterstaining.
Co-immunoprecipitation (Co-IP) assay
Total protein from BCPAP cells was isolated using RIPA lysis buffer (Beyotime Institute of Biotechnology) and then quantified by BCA kit (Thermo Fisher Scientific, Inc.). For immunoprecipitation, 500 μg protein was incubated with 1–2 μg of the specific antibodies against ANXA10 or TSG101 (same with the antibodies used in western blot; Abcam) overnight at 4 °C. Subsequently, 40 μL Protein A/G PLUS-Agarose beads (Invitrogen; Thermo Fisher Scientific, Inc.) was added, and incubated for a further 2 h at room temperature. Beads were then washed three times with the lysis buffer and collected by centrifugation at 12,000 × g for 2 min at 4 °C. Following the final wash, the supernatant was aspirated and discarded, then the precipitated proteins were eluted from the beads by re-suspending in 2 × SDS-PAGE loading buffer and boiling for 5 min. The products from immunoprecipitation were analyzed using western blotting.
Statistical analysis
All results were obtained from at least three independent experiments. The statistical analyses were performed using SPSS 16.0 (SPSS, Inc., USA) software. All results in the present study were analyzed by one-way ANOVA, followed by Tukey’s test. P < 0.05 was considered statistically significant.
Results
ANXA10 is up-regulated in PTC cells, and knockdown of it inhibits proliferation and promotes apoptosis of PTC cells
First of all, the expression of ANXA10 in human normal thyroid follicular epithelial cell line Nthy-ori 3–1 and human PTC cell lines (BCPAP, TPC-1 and KTC-1) was evaluated by RT-qPCR and western blotting. As shown in Fig. 1A and B, ANXA10 exhibited significantly increased expression in PTC cell lines compared with Nthy-ori 3–1 cell line. At the same time, BCPAP possessed the highest expression of ANXA10, as a result, it was chosen for the subsequent experiments.
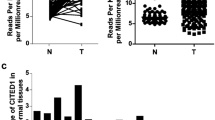
Expression of ANXA10 in PTC cell lines and effects of ANXA10 knockdown on PTC cells proliferation. A and B, the mRNA (A) and protein (B) expressions of ANXA10 in human normal thyroid follicular epithelial cell line Nthy-ori 3–1 and human PTC cell lines (BCPAP, TPC-1 and KTC-1). ***P < 0.001 vs. Nthy-ori 3–1 group. C and D, the mRNA (C) and protein (D) expressions of ANXA10 in control BCPAP cells or cells that transfected with indicated shRNAs. **P < 0.01 and ***P < 0.001 vs. Control group. E, the cell proliferation of control BCPAP cells or cells that transfected with indicated shRNAs at 24, 48 and 72 h post-culture. *P < 0.05 and ***P < 0.001 vs. Control group. F, representative images for colony formation assay in control BCPAP cells or cells that transfected with indicated shRNAs (magnification, × 100). G, representative images for immunofluorescence staining against Ki67 in control BCPAP cells or cells that transfected with indicated shRNAs (magnification, × 200). Ki67 was stained with green and DAPI was used for nuclear counterstaining (blue)
Then, ANXA10 was silenced in BCPAP cells using shRNAs to observe the alteration of cell proliferation and apoptosis. Figure 1C and D confirmed the knockdown efficiency of ANXA10 and sh-ANXA10-1 was selected for ANXA10 silence in next experiments owing to its better transfection efficiency. The cell viability was measured by MTT assay, the results showed that sh-ANXA10-1 resulted in a marked decrease in cell viability compared with the sh-NC group (Fig. 1E). Colony formation assay demonstrated that the ability of colony formation was also reduced by sh-ANXA10-1 (Fig. 1F). Consistently, BCPAP cells that transfected with sh-ANXA10-1 showed obvious lower expression of Ki67 than cells that transfected with sh-NC. These data indicated the inhibitory effect of ANXA10 knockdown on BCPAP cells proliferation.
Besides, Tunel staining was employed to assess cell apoptosis. As illustrated in Fig. 2A, ANXA10 silence caused a significant increase in ratio of cell apoptosis. Meanwhile, ANXA10 decreased Bcl-2 expression, but increased Bax, cleaved-caspase3/caspase3 and cleaved-caspase9/caspase9 expressions (Fig. 2B). These results suggested the promotive effect of ANXA10 silence on BCPAP cells apoptosis.
Effects of ANXA10 knockdown on PTC cells apoptosis. A, representative images for Tunel staining in control BCPAP cells or cells that transfected with indicated shRNAs (magnification, × 100). Apoptotic cells were stained with green and DAPI was used for nuclear counterstaining (blue). B, the protein expression of Bcl-2, Bax, cleaved-caspase3/caspase3 and cleaved-caspase9/caspase9 was detected by western blotting assay. ***P < 0.001 vs. Control group
TSG101 is up-regulated in PTC cells and can be regulated by ANXA10 via mutually binding
To determine whether ANXA10 exerted its effect on PTC via binding to TSG101, the expression of TSG101 in Nthy-ori 3–1 cell line and human PTC cell lines (BCPAP, TPC-1 and KTC-1) was also evaluated. It was demonstrated in Fig. 3A and B, both TSG101 mRNA and protein expressions were up-regulated in PTC cell lines. Thereafter, Co-IP assay verified the direct interaction between ANXA10 and TSG101 (Fig. 3C and D). Besides, the expression of TSG101 was down-regulated upon ANXA10 silence, indicating that ANXA10 could positively regulate TSG101 expression (Fig. 3E).
The interaction between ANXA10 and TSG101. A and B, the mRNA (A) and protein (B) expressions of TSG101 in human normal thyroid follicular epithelial cell line Nthy-ori 3–1 and human PTC cell lines (BCPAP, TPC-1 and KTC-1). ***P < 0.001 vs. Nthy-ori 3–1 group. C and D, the interaction between ANXA10 and TSG101 in BCPAP cells was determined by Co-IP assay. E, the protein expression of TSG101 in BCPAP cells before and after ANXA10 silence was tested by western blotting assay. ***P < 0.001 vs. Control group
TSG101 overexpression blocks the effect of ANXA10 silence on PTC cells proliferation and apoptosis
Subsequently, TSG101 was overexpressed in BCPAP cells using pcDNA3.1-TSG101 and Fig. 4A validated the successful up-regulation of TSG101 in BCPAP cells. As shown in Fig. 4B, the cell viability inhibited by ANXA10 knockdown was reversely enhanced by TSG101 overexpression. Similarly, the inhibited colony formation and Ki67 expression caused by ANXA10 silence were markedly recovered after TSG101 overexpression (Fig. 4C and D). Cell apoptosis of BCPAP cells that overexpressed with TSG101 in the presence of ANXA10 knockdown was also evaluated. Figure 5A illustrated that TSG101 overexpression resulted in a decrease in cell apoptosis ratio when compared with cells that transfected with empty vector pcDNA3.1 in the presence of ANXA10 knockdown (sh-ANXA10-1 + pcDNA3.1). Moreover, the protein expression of Bcl-2, Bax, cleaved-caspase3/caspase3 and cleaved-caspase9/caspase9 that altered by ANXA10 knockdown was remarkably recovered by TSG101 upregulation (Fig. 5B). The above data revealed that TSG101 inhibited the effect of ANXA10 overexpression on BCPAP cells proliferation and apoptosis.
TSG101 overexpression blocks the effect of ANXA10 silence on PTC cells proliferation. A, the protein expression of TSG101 in BCPAP cells before and after TSG101 overexpression was tested by western blotting assay. ***P < 0.001 vs. Control group. B, the cell proliferation of control BCPAP cells or cells that transfected with indicated plasmids at 24, 48 and 72 h post-culture was detected by MTT assay. **P < 0.01 and ***P < 0.001 vs. Control group. ##P < 0.01 and ###P < 0.001 vs. sh-NC group. C, representative images for colony formation assay in control BCPAP cells or cells that transfected with indicated plasmids (magnification, × 100). D, representative images for immunofluorescence staining against Ki67 in control BCPAP cells or cells that transfected with indicated plasmids (magnification, × 200). Ki67 was stained with green and DAPI was used for nuclear counterstaining (blue)
TSG101 overexpression blocks the effect of ANXA10 silence on PTC cells apoptosis. A, representative images for Tunel staining in control BCPAP cells or cells that transfected with indicated plasmids (magnification, × 100). Apoptotic cells were stained with green and DAPI was used for nuclear counterstaining (blue). B, the protein expression of Bcl-2, Bax, cleaved-caspase3/caspase3 and cleaved-caspase9/caspase9 was detected by western blotting assay. ***P < 0.001 vs. Control group. #P < 0.05 and ###P < 0.001 vs. sh-NC group
ANXA10 silence suppresses the activation of mitogen-activated protein kinase / (MAPK)/ERK signaling, but TSG101 overexpression blunts this effect
To uncover the underlying mechanism involved in the effects of ANXA10/TSG101 on PTC cells proliferation and apoptosis, the expression of MAPK signaling pathway was detected. As illustrated in Fig. 6, the expression of p-ERK/ERK was considerably decreased in cells that silenced with ANXA10 compared with sh-NC group, but was reversely increased after TSG101 overexpression when compared with cells that transfected with sh-ANXA10-1 + pcDNA3.1. Meanwhile, ANXA10 silence and TSG101 overexpression caused no significant effect on p-JNK/JNK and p-p38/p38 expression.
ANXA10 silence suppresses the activation of MAPK/ERK signaling, but TSG101 overexpression blunts this effect. The protein expression of p-ERK/ERK, p-JNK/JNK and p-p38/p38 in control BCPAP cells or cells that transfected with indicated plasmids was detected by western blotting assay. ***P < 0.001 vs. Control group. ##P < 0.01 vs. sh-NC group
Discussion
TC is the most common malignant tumors of the head and neck, and PTC is the most common pathological type of TC, and the incidence is increasing year by year. In this study, we demonstrated the up-regulated expression of ANXA10 and TSG101 in PTC cells. Further studies revealed that ANXA10 silence inhibited proliferation and induced apoptosis of PTC cells, whereas TSG101 overexpression blocked these effects. Mechanically, ANXA10 knockdown suppressed the activation of MAPK/ERK signaling, but TSG101 overexpression re-activated this pathway.
ANXA is composed of 12 members, and the abnormal expression of ANXA members is observed in the occurrence and development of several types of cancer. For example, ANXA1 expression is up-regulated in pancreatic cancer, and the tumor growth and metastasis of mice that knockdown with ANXA1 are significantly reduced, indicating that ANXA1 played a key role in the progression of pancreatic cancer (Pessolano et al. 2018; Yi and Schnitzer 2009). However, the expressions of ANXA1 and ANXA7 are low in prostate cancer (Srivastava et al. 2001). Therefore, different ANXA may play different roles in diverse types of cancer. ANXA10 is a newly identified member of ANXA, thus the studies related to its role in cancers are relatively little. ANXA10 was obviously decreased in hepatocellular carcinoma (HCC) tissues and cells and inhibition of ubiquitination-mediated degradation of ANXA10 could suppressed the occurrence and development of HCC (Liu et al. 2020). ANXA10 exhibited the promoting role in progression of esophageal squamous cell carcinoma (ESCC) (Zang et al. 2019). Here, in accordance with a recent study (Liu et al. 2021), we showed the up-regulated expression of ANXA10 in PTC cell lines compared with human normal thyroid follicular epithelial cell line, indicating the possible role of ANXA10 in PTC. The uncontrolled cell proliferation and reduced cell apoptosis have been confirmed to contribute to the occurrence and progression of cancers (Evan and Vousden 2001). To investigate the specific effects of ANXA10, we knockdown it in PTC cell line BCPAP to observe the alteration of cell proliferation and apoptosis. We found that ANXA10 silence remarkably inhibited proliferation and promoted apoptosis of PTC cells, indicating that ANXA10 down-regulation could effectively inhibit PTC occurrence or progression.
TSG101 has been extensively implicated to play an oncogenic role in various cancers such as renal cell carcinoma, hepatocellular carcinoma, nasopharyngeal carcinoma and squamous cell/adenosquamous carcinomas (Chua et al. 2019; Liu et al. 2019, 2014; Xu and Zheng 2019). Consistent with a previous report (Liu et al. 2002), our results showed the up-regulated expression of TSG101 in PTC cell lines, strengthening the evidence that TSG101 plays a role in mediating tumorigenesis of human PTC. Importantly, we verified the direct interaction between ANXA10 and TSG101. Further results showed that ANXA10 silence down-regulated the expression of TSG101. Therefore, we speculated that ANXA10 knockdown may exerted its inhibitory effect on PTC tumorigenesis via binding to TSG101 and down-regulating TSG101 expression. In accordance with this hypothesis, results showed that TSG101 overexpression blocked all the effects of ANXA10 silence on PTC cells.
The MAPK signaling pathway consists of multiple sub-pathways including MAPK/ERK, MAPK/JNK and MAPK/p38. The abnormal regulation of the MAPK signaling pathway can lead to cancer (Sabio and Davis 2014). Studies have shown that the MAPK signaling pathway also plays a key regulatory role in the occurrence and development of TC, leading to the proliferation, growth, migration and survival of TC cancer cells, as well as tumor angiogenesis, invasion and metastasis (Xing 2013). Therefore, inhibiting the activation of MAPK signaling pathway may provide a new strategy for the treatment of TC.
It is worth noting that ANXA10 can inhibit the proliferation of oral squamous cell carcinoma cells by inhibiting the MAPK signaling pathway (Shimizu et al. 2012). Furthermore, interference with the expression of TSG101 has been reported to inhibit the proliferation of breast cancer cells by preventing the activation of the MAPK/ERK signaling pathway (Zhang et al. 2011). Subsequently, we investigated the expression of MAPK/ERK, MAPK/JNK and MAPK/p38 in PTC cells in response to ANXA10 silence and TSG101 overexpression. We found that ANXA10 silence significantly inhibited the phosphorylation of ERK, but had no significant effect on p-JNK/JNK and p-p38/p38 expressions. In addition, TSG101 overexpression blunted the inhibitory effect of ANXA10 silence on MAPK/ERK activation. These results revealed that ANXA10 knockdown could inhibit MAPK/ERK signaling activation via down-regulating TSG101 expression. However, it could be observed that TSG101 overexpression didn’t canceled the effect of ANXA10 knockdown on PTC cells totally, suggesting the existence of other down-stream mediators or pathways involved in. Further studies are need to be performed to solve this problem. In addition, in vivo experiments using human samples or animal models will be carried out to further validate our findings.
Taken together, our study was the first to investigate the specific role of ANXA10 in PTC. The results indicated that ANXA10 was a novel potential oncogene in PTC, and its down-regulation could inhibit proliferation and promote apoptosis of PTC cells. TSG101 was a potential target of ANXA10, and MAPK/ERK signaling pathway mediated the function of ANXA10/TSG101 axis in PTC. This study implicated the potential application of ANXA10/TSG101 axis in the prognosis and treatment of PTC.
Data availability
The experimental data will be available on the request.
References
Chua HH, Kameyama T, Mayeda A, Yeh TH (2019) Cancer-specifically Re-Spliced TSG101 mRNA promotes invasion and metastasis of nasopharyngeal carcinoma. Int J Molec Sci 20. https://doi.org/10.3390/ijms20030773
Evan GI, Vousden KH (2001) Proliferation, cell cycle and apoptosis in cancer. Nature 411:342–348. https://doi.org/10.1038/35077213
Gerke V, Moss SE (2002) Annexins: from structure to function. Physiol Rev 82:331–371. https://doi.org/10.1152/physrev.00030.2001
Gerke V, Creutz CE, Moss SE (2005) Annexins: linking Ca2+ signalling to membrane dynamics. Nat Rev Mol Cell Biol 6:449–461. https://doi.org/10.1038/nrm1661
Hung MS et al. (2019) Cul4A modulates invasion and metastasis of lung cancer through regulation of ANXA10. Cancers 11. https://doi.org/10.3390/cancers11050618
Kitahara CM, Sosa JA (2016) The changing incidence of thyroid cancer. Nat Rev Endocrinol 12:646–653. https://doi.org/10.1038/nrendo.2016.110
Kodaira H et al (2019) ANXA10 induction by interaction with tumor-associated macrophages promotes the growth of esophageal squamous cell carcinoma. Pathol Int 69:135–147. https://doi.org/10.1111/pin.12771
Kumar B et al (2016) ESCRT-I protein Tsg101 plays a role in the post-macropinocytic trafficking and infection of endothelial cells by Kaposi’s sarcoma-associated herpesvirus. PLoS Pathog 12:e1005960. https://doi.org/10.1371/journal.ppat.1005960
Liu RT et al (2002) Overexpression of tumor susceptibility gene TSG101 in human papillary thyroid carcinomas. Oncogene 21:4830–4837. https://doi.org/10.1038/sj.onc.1205612
Liu Z et al (2014) TSG101 and PEG10 are prognostic markers in squamous cell/adenosquamous carcinomas and adenocarcinoma of the gallbladder. Oncol Lett 7:1128–1138. https://doi.org/10.3892/ol.2014.1886
Liu Z et al (2019) TSG101 promotes the proliferation, migration and invasion of hepatocellular carcinoma cells by regulating the PEG10. J Cell Mol Med 23:70–82. https://doi.org/10.1111/jcmm.13878
Liu X et al (2020) Upregulated lncRNA DLX6-AS1 underpins hepatocellular carcinoma progression via the miR-513c/Cul4A/ANXA10 axis. Cancer Gene Ther. https://doi.org/10.1038/s41417-020-00233-0
Liu X, Yang M, Guo Y, Lu X (2021) Annexin A10 is a novel prognostic biomarker of papillary thyroid cancer. Ir J Med Sci 190:59–65. https://doi.org/10.1007/s11845-020-02263-x
Munksgaard PP et al (2011) Low ANXA10 expression is associated with disease aggressiveness in bladder cancer. Br J Cancer 105:1379–1387. https://doi.org/10.1038/bjc.2011.404
Pessolano E et al. (2018) Annexin A1 may induce pancreatic cancer progression as a key player of extracellular vesicles effects as evidenced in the in vitro MIA PaCa-2 model system. Int J Mol Sci 19. https://doi.org/10.3390/ijms19123878
Rahib L, Smith BD, Aizenberg R, Rosenzweig AB, Fleshman JM, Matrisian LM (2014) Projecting cancer incidence and deaths to 2030: the unexpected burden of thyroid, liver, and pancreas cancers in the United States. Can Res 74:2913–2921. https://doi.org/10.1158/0008-5472.can-14-0155
Sabio G, Davis RJ (2014) TNF and MAP kinase signalling pathways. Semin Immunol 26:237–245. https://doi.org/10.1016/j.smim.2014.02.009
Sai XB, Makiyama T, Sakane H, Horii Y, Hiraishi H, Shirataki H (2015) TSG101, a tumor susceptibility gene, bidirectionally modulates cell invasion through regulating MMP-9 mRNA expression. BMC Cancer 15:933. https://doi.org/10.1186/s12885-015-1942-1
Seib CD, Sosa JA (2019) Evolving understanding of the epidemiology of thyroid cancer. Endocrinol Metab Clin North Am 48:23–35. https://doi.org/10.1016/j.ecl.2018.10.002
Shimizu T et al (2012) Annexin A10 in human oral cancer: biomarker for tumoral growth via G1/S transition by targeting MAPK signaling pathways. PLoS ONE 7:e45510. https://doi.org/10.1371/journal.pone.0045510
Srivastava M et al (2001) ANX7, a candidate tumor suppressor gene for prostate cancer. Proc Natl Acad Sci USA 98:4575–4580. https://doi.org/10.1073/pnas.071055798
Sun R et al (2019) Annexin10 promotes extrahepatic cholangiocarcinoma metastasis by facilitating EMT via PLA2G4A/PGE2/STAT3 pathway. EBioMedicine 47:142–155. https://doi.org/10.1016/j.ebiom.2019.08.062
Wang J, Zhao S, Wang F, Wang J, Zhang Y (2019) Prognostic Significance of Increased Expression of Annexin A10 (ANXA10) in Serous Epithelial Ovarian Cancer. Med Sci Monit 25:5666–5673. https://doi.org/10.12659/msm.915911
Xing M (2013) Molecular pathogenesis and mechanisms of thyroid cancer. Nat Rev Cancer 13:184–199. https://doi.org/10.1038/nrc3431
Xu C, Zheng J (2019) siRNA against TSG101 reduces proliferation and induces G0/G1 arrest in renal cell carcinoma - involvement of c-myc, cyclin E1, and CDK2. Cell Mol Biol Lett 24:7. https://doi.org/10.1186/s11658-018-0124-y
Yi M, Schnitzer JE (2009) Impaired tumor growth, metastasis, angiogenesis and wound healing in annexin A1-null mice. Proc Natl Acad Sci USA 106:17886–17891. https://doi.org/10.1073/pnas.0901324106
Zang B, Zhao J, Chen C (2019) LncRNA PCAT-1 promoted ESCC progression via regulating ANXA10 expression by sponging miR-508-3p. Cancer Manag Res 11:10841–10849. https://doi.org/10.2147/cmar.s233983
Zhang Y et al (2011) Down-regulation of TSG101 by small interfering RNA inhibits the proliferation of breast cancer cells through the MAPK/ERK signal pathway. Histol Histopathol 26:87–94. https://doi.org/10.14670/hh-26.87
Zhu J, Wu J, Pei X, Tan Z, Shi J, Lubman DM (2017) Annexin A10 is a candidate marker associated with the progression of pancreatic precursor lesions to adenocarcinoma. PLoS ONE 12:e0175039. https://doi.org/10.1371/journal.pone.0175039
Funding
Young and Middle-aged Scientific Research Foundation of Wannan Medical College (WK2020F20).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare they have no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wei, T., Zhu, X. Knockdown of ANXA10 inhibits proliferation and promotes apoptosis of papillary thyroid carcinoma cells by down-regulating TSG101 thereby inactivating the MAPK/ERK signaling pathway. J Bioenerg Biomembr 53, 429–440 (2021). https://doi.org/10.1007/s10863-021-09902-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10863-021-09902-7