Abstract
Children with autism spectrum disorder (ASD) have been shown to benefit from parent-implemented interventions (PIIs). This meta-analysis improved on prior reviews of PIIs by evaluating RCTs and multiple potential moderators, including indicators of research quality. Fifty-one effect sizes averaged moderately strong overall benefits of PIIs (g = 0.553), with studies having lower risk of research bias yielding lower estimates (g = 0.47). Parent and observer ratings yielded similar averaged estimates for positive behavior/social skills (g = 0.603), language/communication (g = 0.545), maladaptive behavior (g = 0.519), and to a lesser extent, adaptive behavior/life skills (g = 0.239). No other study, intervention, or participant characteristic moderated outcomes. PIIs with children with ASD tend to be effective across a variety of circumstances.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Parents and professionals can begin to recognize characteristics of autism spectrum disorder (ASD) in children as young as the first year of life (e.g., Tanner & Dounavi, 2020). To facilitate developmental outcomes in cognition, adaptive behaviors, and communication, researchers recommend early identification of and support for ASD (Koegel et al., 2014; Nahmias et al., 2019; Reichow, 2011; Sandbank et al., 2020; Warren et al., 2011). Clinical recommendations are often for intensive services (e.g., 25–40 h per week, one-to-one adult to child ratio, for a year or longer), which is difficult for many families to achieve. Obtaining intensive intervention for children with ASD can prove challenging for many parents due to costs, limitations of time, travel distance, access to appropriate services, long waitlists, and lack of insurance coverage (Buescher et al., 2014; Nevill et al., 2016; Symon, 2001). Recognizing the struggles and limitations faced by families with children with ASD, professionals increasingly evaluate alternatives to service delivery (Cidav et al., 2017; Hatcher & Page, 2020; Lee et al., 2018; Meadan et al., 2016), including interventions delivered by the parents (Pi et al., 2021).
Parent-implemented interventions (PIIs; also referred to as parent training or parent-mediated interventions) entail intensive professional training to inform and support parents to assist children with developmental disabilities (e.g., Akamoglu & Meadan, 2018). PIIs promote parent–child engagement and address behavior support, communication and social interaction, and daily living skills by increasing parent skills and knowledge through didactic instruction, role play, coaching/supervision, in-home practice assignments, handouts, and/or in-person or virtual home visits (e.g., Bearss et al., 2013; Kasari et al., 2014). Although PIIs can function as the primary intervention provided, such as when professional services are difficult to access, PIIs compliment professional programs by generalizing to daily routines and by expanding the frequency and scope of interventions provided (Bearss et al., 2015a; Dawson-Squibb et al., 2020). PIIs can also increase parents’ engagement and feelings of competence (Deb et al., 2020; Jhuo & Chu, 2022; Liu et al., 2020) and decrease parental stress and strain (Iadarola et al., 2018). Examples of PIIs include adapting the Early Start Denver Model (ESDM; Dawson et al., 2010; Jhuo & Chu, 2022; Rogers et al., 2012) and Project ImPACT (Ingersoll & Dvortcsak, 2019).
Prior reviews and meta-analyses have reported positive effects of PIIs on child behaviors and communication (Black & Therrien, 2018; Dyches et al., 2018; Nevill et al., 2016; Postorino et al., 2017). For example, Deb and colleagues (2020) found mild to moderate benefits of three specific PIIs across 15 of 17 papers reviewed. Summarizing 21 PIIs in Asia, Liu et al. (2020) reported strong benefits, averaging d = 0.76, across a variety of child outcomes. Nevertheless, the results vary across studies (e.g., Alquraini et al., 2018; Jocelyn et al., 1998; Matthews et al., 2018; Reitzel et al., 2013). Child outcomes appear to differ based on study and PII characteristics, with most research focused on a few manualized PIIs that meet evidence-based practice criteria (Dawson-Squibb et al., 2020; Steinbrenner et al., 2020), such as Stepping Stone/Triple P (Turner et al., 2010). Comparing outcomes across PIIs will help to clarify the effectiveness of specific programs and will also clarify the circumstances when PIIs are most and least effective (across child, parent, and study characteristics).
Many scholars indicate that conclusions about the effectiveness of PIIs require improved quality of research evidence, specifically randomized experimental designs (e.g., Beaudoin et al., 2014; Dawson-Squibb et al., 2020; Oono et al., 2013), but several methodological limitations have characterized prior meta-analytic reviews of child outcomes following PIIs. First, many prior reviews have included retrospective or quasi-experimental designs that are susceptible to research bias, particularly selection bias when motivated parents seek out the intervention condition of the study. Second, previous meta-analyses have not evaluated if the results differ as a function of plausible study bias from participant attrition without intent-to-treat data, baseline differences across groups, or failing to conceal participant allocation or group conditions. Third, reviews have not distinguished outcomes based on professional observations versus parent-reports, which can provide holistic/continuous evaluations not possible by trained observers but which can vary in terms of reliability across participants/conditions and which may bias study findings (Bennetts et al., 2016). In outcome research, parents in the intervention group can presume that researchers expect child improvement, such that parents may rate their child’s outcomes differently than an independent observer blind to study conditions. It is therefore necessary to compare parent ratings with evaluators’ ratings to obtain more objective conclusions regarding PIIs' effectiveness. Fourth, studies included in prior meta-analyses have combined results across different types of conditions: waitlist controls, emotional support for parents without instruction about how to intervene with their child, or professionally delivered services without parent involvement. These differences in study conditions should be evaluated. Fifth, many prior reviews have not evaluated reports of treatment fidelity, such that differences in outcomes may be attributable to variability of treatment implementation. Sixth, some prior meta-analyses have included limited sources due to restricted search terms, which procedure may fail to locate studies using synonymous but distinct terminology. Seventh, some prior reviews have included only published articles, which may exacerbate the effects of publication bias (Van Aert et al., 2019) to overrepresent findings supportive of PIIs.
To address these multiple limitations, we conducted a meta-analytic review of randomized controlled trials (RCTs) using comprehensive search terms and extensive coding of study characteristics to obtain data beyond that of prior meta-analyses. We limited our review to group evaluations of PIIs to align with the common practice in the field of providing training to multiple parents simultaneously. Although rigorous single-subject research clearly contributes to the literature, individual parent training may yield different results that deserve separate consideration. Moreover, the different effect size calculations and circumstances in single-subject research would merit separate review. In this meta-analysis specific to RCTs, we sought to address the following research questions:
-
(1)
To what extent do parent-implemented interventions facilitate behavioral and language improvements among children with ASD compared with professional treatment, treatment as usual, or waitlist conditions?
-
(2)
To what extent do study characteristics (e.g., type of control group, source of outcome data, type of child outcome), intervention characteristics (e.g., duration and number of sessions), and participant characteristics (e.g., age, gender) moderate the effectiveness of PIIs?
Method
Procedures aligned with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) Statement (Moher et al., 2009), except we do not report individual study risk of research bias. We report risk of bias summary statistics and performed analyses to investigate the possible impact of risk of bias on summary estimates of the effect (Shea et al., 2017). All review methods were established prior to conducting the review.
Manuscript Search
We used multiple strategies to locate RCTs evaluating interventions involving parents as interventionists for their children with ASD. We searched eight electronic databases for articles entered from 1990 until June 3, 2020: Academic Search Ultimate, CINAHL, ERIC, Embase, Medline, ProQuest Dissertations, PsychINFO, and Social Sciences Abstracts. To capture relevant studies, our searches used lists of synonymous search terms and keywords that we identified using database search tools (full search terms available online supplementary material). To reduce inadvertent omissions, we searched each electronic database twice.
Additionally, we identified the following meta-analyses on related topics and searched their references for studies that met our inclusion criteria: Black and Therrien (2018), Dyches et al. (2018), Ferguson et al. (2019), McConachie and Diggle (2007), Nevill et al. (2016), Parsons et al. (2017), Postorino et al. (2017), Oono et al. (2013), Ratliff-Black and Therrien (2020), Tachibana et al. (2017), Tarver et al. (2019), and Virues-Ortega et al. (2013). As a final step, we examined the reference lists of all studies that met our inclusion criteria. To systematize our search and screening procedures, all located studies were uploaded to Covidence Systematic Review software (SaaS Enterprise, 2014).
Inclusion Criteria and Screening
We sought RCTs involving children with ASD receiving a PII compared with professional treatment, treatment as usual, or waitlist controls on one or more of the following outcomes: expected behaviors/social skills, maladaptive behaviors, language/communication, and/or adaptive behaviors/life skills. We excluded case studies, qualitative research, quasi-experimental designs, single-subject designs, and studies that only compared different intensities/modes of the same program. Furthermore, we excluded studies in which the child participants had not been evaluated for ASD, the parents’ involvement in the intervention was unclear or consisted solely of passive reception of information, or the intervention groups delivered only medication, software/apps, music, or sleep/diet modifications. To reduce the likelihood of publication bias adversely impacting the results, we included both published (journal articles and book chapters) and unpublished studies (conference presentations, dissertations, and theses).
The screening procedure included three stages: (a) Covidence removed duplicate studies retrieved from different databases, (b) at least two independent reviewers screened articles based on title and abstract, and (c) at least two independent reviewers read full-text articles that had appeared to meet inclusion criteria. Thus, all studies located were screened twice during the initial screening and again during full-text review by individuals unaware of others’ decisions. Data managed in Covidence software indicated 91.7% inter-rater agreement for the independent initial screening based on titles and abstracts (Cohen’s kappa = 0.51) and 92.5% inter-rater agreement for the independent screening based on full-text review (Cohen’s kappa = 0.81). The first and second authors made final decisions for unresolved discrepancies and merged different publications when they reported the same data.
Data Coding
Teams of two members each were trained for and conducted data coding. A codebook describing all study variables facilitated consistency across coders. Two independent teams coded each study, including (a) number of child participants and their gender and average age; (b) caregiver who delivered the intervention; (c) type and dosage of the intervention provided and reports of treatment fidelity; (d) comparison group type and measurement type, including parent rating or professional observation; (e) intervention effectiveness in improving parent intervention skills; (f) indicators of study bias, including baseline differences after randomization, participant attrition, intent-to-treat analyses, allocation concealment, blinding of interventionists to group conditions, and blinding of assessors to group conditions; and (g) effect size calculated using data provided in the manuscript. Data managed in Covidence software indicated moderate but acceptable reliability across the categorical variables coded (Cohen’s kappa = 0.43) and good reliability across the continuous variables coded (intra-class correlation coefficient = 0.85). When discrepancies occurred, coding teams met to resolve the disagreement by further investigation of the manuscript to reach a consensus.
Computation of Effect Size Estimates
Different statistical values (e.g., f-tests, means and standard deviations, and p-values) reported in studies were initially converted to the standard metric of Cohen’s d using the Meta-Analysis Calculator (Wilson, 2021). Since several studies had low numbers of participants, we converted all effect sizes to Hedge’s g values to reduce bias associated with differences in variance that can occur in small studies (Marfo & Okyere, 2019). Where analyses were reported as statistically significant with no statistic provided, the corresponding alpha level determined the g value (assuming two-tailed alpha = 0.05 unless noted otherwise). Effect size g = 0 was set for analyses that report non-significant results with no additional information. These procedures yielded conservative effect size estimates. The direction of all effect sizes was coded uniformly: positive values indicate improved child outcomes as a function of the intervention, and negative values indicate a deleterious effect relative to the comparison group.
When studies reported multiple measures of child functioning at both pre-test and post-test, we extracted every effect size that was conceptually aligned with the description of the intervention, and we coded for differences across types of outcomes (e.g., separating effect sizes based on evaluations of child language/communication scores from those based on child adaptive behavior scores). We avoided coding effect sizes based solely on broad screeners or comprehensive diagnostic batteries inappropriately used as outcome measures. To avoid violating the assumption of statistical independence we averaged multiple effect sizes within studies, weighted by standard error or the number of participants evaluated, such that our omnibus analysis included only one effect size per study.
Risk of Research Bias and Publication Bias
We sought to obtain high-quality research evidence by coding only studies in which participants had been randomized to treatment and control conditions, and we also evaluated the risk of bias of each article in terms of: researcher awareness of participant allocation, interventionist awareness of study conditions, outcome evaluations conducted by either parents, researchers, or observers unaware of the treatment/control group, participant baseline differences across groups, participant attrition, and intent-to-treat analyses.
The direction and statistical significance of the results impact the publication of studies, which can introduce publication bias (Van Aert et al., 2019). In a meta-analysis, publication bias can lead to overestimation of effect sizes and underestimation of false-positive results. We used multiple methods to evaluate possible publication bias: Egger’s regression test, Begg’s regression test, trim and fill analysis, and funnel plot analysis to detect distribution asymmetry.
Statistical Analyses
We used IBM® SPSS® Statistics (Version 27.0) and STATA (Version 17.0) to analyze the data. The pooled effect size was calculated using an inverse-variance weighted random effects model. To assess the heterogeneity of the pooled effect size, we obtained the I-square (I2), tau-square (τ2), and Cochran’s Q. We specified a priori that if the omnibus effect size was heterogenous, we would conduct random effects weighted moderator analyses consisting of subgroup analyses for categorical variables and meta-regression for continuous variables. Analyses were pre-specified and conducted as planned, except for the addition of a Galbraith plot which was included after the first round of journal review to depict effect size heterogeneity and evaluate potential outliers.
Results
Study Selection
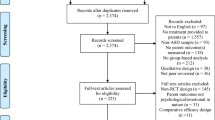
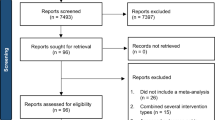
Our search strategies located 1939 non-duplicate studies which we reviewed for inclusion. After initial screening, 209 records remained for full-text review. A summary of the screening process and reasons for exclusion are reported in the PRISMA flow diagram (Fig. 1). Studies retained for coding included 3 unpublished and 51 published articles (54 total). However, three pairs of studies contained distinct but overlapping data (e.g., different measures reported in different articles with the same participants), so those studies were combined to yield one aggregate effect size each, for a total of 51 independent effect sizes.
Descriptive Characteristics of Participants and Interventions
The 51 extracted effect sizes involved a total of 2,895 child participants with an average age of 5.5 years and an average of 17% females and 83% males. A total of 43 records (84%) involved both mother and father, 6 (12%) involved only the mother, and 2 (4%) involved parents and other caregivers. Twelve studies targeted improvements in social skills and other pro-social behaviors, 8 targeted problem behaviors, 6 targeted language/communication, and 25 were mixed, with most of those mixed studies addressing both social/positive behaviors and language/communication.
Across interventions, parents received an average of 89.6 min and 13.3 sessions of training that typically occurred weekly (73%). Child outcomes were measured using direct observations by professionals in 20 (39%) studies, parent-completed standardized instruments in 15 (29%) studies, child-completed standardized instrument in 1 study (2%), with 14 studies (28%) using multiple measures (e.g., parent and observer ratings) and 1 (2%) not providing details regarding measurement source.
Baseline scores were equivalent between children in intervention and control groups (indicating that randomization resulted in balanced participants) in 38 studies (74.5%), with 3 (5.9%) having differences that favored the intervention group, 6 (11.8%) having group differences that favored the control group, and 4 (7.8%) not reporting. Only two records (4%) had all interventionists, observers, and data analysts who were “blind” or unaware of participant allocation, 23 (45%) involved blind observers for the outcome evaluations, 17 (33%) records did not provide enough information or stated that researchers were not blind, 7 (14%) reported that both the interventionists and the outcome observers were blind, 1 (2%) only kept the interventionists unaware, and 1 (2%) kept both the outcome observer and data analysts unaware. No information was provided for allocation concealment in 17 (33%) records; 29 (57%) indicated that researchers were not involved in the randomization process, and 5 (10%) declared that researchers conducted the randomization and were aware.
Studies differed in terms of improving parents’ self-reported abilities to intervene with the children. Twenty-one studies (57%) reported that parents in the intervention group gained statistically significantly more child intervention skills than those in the control group, but 8 (17%) reported no gains or worse performance than the control group, with 22 (43%) not reporting data regarding changes in parents’ intervention skills as a function of the intervention. Treatment fidelity was not measured or reported in 20 (39%) of the records; 18 (35%) reported that the PII was implemented as intended; 12 (23%) assessed fidelity but did not report if the intervention was implemented as intended; and 1 (2%) reported low treatment fidelity. The average overall participant attrition across studies was very low, averaging 2.89 participants (9.7%) in the experimental group and 2.34 participants (8.4%) in the control group.
Studies used different types of comparison groups, with only one study (2%) comparing PIIs to a specific intervention conducted by professionals without parent involvement, 17 (33%) using unspecified “treatment as usual” conducted by professionals, 7 (14%) involving parent support but not an active PII, and 26 (51%) using waitlist control groups. There were 35 (69%) outcomes based on data from intervention completers and 16 (31%) based on intent-to-treat analyses. A summary of the characteristics of the included studies appears in Table 1.
Omnibus Analysis
Analyses were conducted using Hedges’ g to minimize the likelihood of small study bias. Across all 51 effect sizes, the random effects weighted average was g = 0.55 (95% confidence interval g = 0.45 to 0.65, p < 0.0001; see Fig. 2).
Effect sizes ranged from g = − 0.03 to 2.44, with small but statistically significant heterogeneity (I2 = 37.6%; τ2 = 0.05; Q = 86.4, p < 0.001). Three of 51 effect sizes fell outside the expected distribution in a Galbraith plot (Fig. 3), but that percentage (5.9%) approximated what would have been found by chance 95% of the time. Thus the data exhibited reasonable levels of variation around the mean, with 6 (12%) studies finding no effects of PIIs, 20 (39%) finding small to moderate effects, 12 (24%) finding moderate to large effects, and 13 (25%) finding large to very large effects. We evaluated possible moderating variables that may have accounted for differences in findings across studies.
Subgroup Analyses by Child Outcome
Within studies, authors evaluated different types of child outcomes. We categorized those outcomes into the following four groups: expected behaviors/social skills, maladaptive behaviors, adaptive behavior/life skills, and language/communication. We analyzed these data separately to ascertain the degree to which different kinds of outcomes were impacted by PIIs. Across 30 studies reporting child outcomes in terms of expected behavior/social skills, the random effects weighted average was g = 0.603 (95% CI 0.45 to 0.75, p < 0.001). These results were characterized by moderate and statistically significant heterogeneity (I2 = 46.6, 95% CI 18 to 65; Q = 54.3, p = 0.003). These results did not differ across parent versus observer ratings of child outcomes (Table 2).
Across 20 studies evaluating child outcomes in terms of maladaptive behavior, the random effects weighted average was g = 0.519 (95% CI 0.37 to 0.67, p < 0.001). These results were characterized by small but statistically significant heterogeneity (I2 = 37.1, 95% CI 0 to 63; Q = 30.2, p = 0.049). These results did not differ across parent versus observer ratings of child outcomes (Table 2).
Across six studies evaluating child outcomes in terms of adaptive behavior/life skills, the random effects weighted average was g = 0.239, with that value not reaching statistical significance (95% CI − 0.11 to 0.59, p > 0.05). These results were characterized by small and statistically non-significant heterogeneity (I2 = 31.5, 95% CI 0 to 72; Q = 7.3, p = 0.20). Averaged parent ratings of child outcomes tended to be lower than professional ratings (Table 2), but this difference was attributable to a single outlier with a value of g = − 0.795.
Across 19 studies evaluating child outcomes in terms of language/communication skills, the random effects weighted average was g = 0.545 (95% CI 0.34 to 0.75, p < 0.001). These results were characterized by moderate, statistically significant heterogeneity (I2 = 61.2, 95% CI 36 to 76; Q = 46.5, p < 0.001). Results did not differ across parent versus professional ratings of child outcomes (Table 2).
Evaluations of Publication Bias
We administered several tests to detect plausible publication bias. Both Egger’s regression test and Begg’s test did not reach statistical significance, suggesting the effect sizes were distributed normally. We also generated a contour-enhanced funnel plot to examine publication bias (see Fig. 4). In the plot, the data were only slightly asymmetrical, with most data evenly distributed around the mean. Subsequent trim-and-fill analyses did not identify any missing studies in the distribution. Therefore, publication bias did not appear to be a likely threat to the results of this meta-analysis.
Evaluations of Moderation by Participant, Intervention, and Study Characteristics
To evaluate whether effect size heterogeneity could be explained by other variables, we performed moderator analyses of participant, intervention, and study characteristics. Participant characteristics included the gender and mean age of child participants, as well as the identity of the caregiver performing the intervention (e.g., mother, father, both parents). Intervention characteristics included the type of intervention, intervention effectiveness in improving parents’ skills, treatment fidelity, and dosage (number of sessions, frequency, and duration). Study characteristics included year of publication and comparison group type (e.g., alternative intervention, wait list controls).
None of the variables evaluating participant, intervention, or study characteristics reached statistical significance in the random effects weighted meta-regressions and subgroup ANOVA analogues that we conducted. Thus, we found no indication of effect size moderation.
Evaluations of Risk of Study Bias
We had coded for five indicators of risk of study bias: allocation concealment, baseline differences across groups, masking of individuals involved in the interventions, participant attrition, and outcome data based on completers or intent-to-treat analyses. We observed no statistically significant differences in study effect sizes across these five variables when evaluated separately (p > 0.05). However, after combining indicators into one overall indicator of risk of research bias (e.g., Sterne et al., 2019), we observed a statistically significant random effects weighted correlation between study risk of bias and the corresponding effect size (r = 0.30, p = 0.02). The 29 studies with only one or two variables indicating risk of bias averaged g = 0.47 (95% CI 0.35 to 0.59, p < 0.001) while the 22 studies with three or more of the five variables indicating risk of bias averaged g = 0.68 (95% CI 0.51 to 0.84, p < 0.001). Thus, studies conducted with higher levels of research rigor yielded less robust child outcomes than studies failing to conduct or report aspects of RCT methodology.
Discussion
PII Effectiveness with Children with Autism Spectrum Disorder
The findings of this meta-analysis confirmed overall favorable effects of PIIs for children with ASD. Moderately strong improvements in child outcomes relative to control conditions were found (g = 0.55), even when restricting analyses to studies with lower risk of research bias (g = 0.47). The observed beneficial effects of PIIs were consistent with some prior meta-analyses and systematic reviews (Deb et al., 2020; Liu et al., 2020; Ratliff-Black & Therrien, 2020), but more favorable than data reported in others (Nevill et al., 2016; Oono et al., 2013; Tachibana et al., 2017).
The meta-analytic data indicated that PIIs helped children with ASD to improve in positive behaviors/social skills (Kent et al., 2019; Ona et al., 2019; Soares et al., 2020), maladaptive behaviors (Black & Therrien, 2018; Gerow et al., 2017; Postorino et al., 2017), and language/communication (Fuller et al., 2020; Sandbank et al., 2020; Wang et al., 2021; Yu et al., 2020). Although improvements were also made in adaptive behaviors/life skills (Rodgers et al., 2021), the averaged results tended to be much smaller (g = 0.24) than those obtained for the other outcome types, which ranged from g = 0.52 to 0.60. However, this difference may have occurred because all studies evaluating adaptive behavior/life skills had also addressed other aspects of child functioning; no interventions were exclusive to child adaptive behaviors/life skills.
Overall, PIIs enable parents to apply skills learned from professionals to real-life situations. PIIs likely benefit children with ASD more than comparison conditions because parents are continuously present with the child and can augment the effectiveness of any other intervention provided. Analyses were conducted to evaluate factors such as PII dosage that could have influenced PII outcomes.
Outcomes Across Participant, Intervention, and Study Characteristics
In this meta-analysis, we intentionally evaluated multiple participant, intervention, and study characteristics that could have moderated the effectiveness of PIIs with children with ASD. However, none of the variables we evaluated reached statistical significance. Results tended to be similar across a wide variety of circumstances.
In terms of study participants, PIIs tended to yield equivalent results irrespective of the average child age or the percentage of female participants. No differences were observed when the mother, father, or both implemented the intervention. It is also important to note that parents’ ratings of their own children yielded equivalent results to ratings by observers. This finding suggests that, on average, parent data do not necessarily bias research findings when parents remain aware of the research hypotheses. It also suggests that professional observations, necessarily limited in duration and scope, yield similar averaged estimates to the more continuous observations of parents.
Findings tended to be similar across intervention characteristics of dosage, fidelity, and changes in parents’ abilities to assist their children. These results were unexpected and raise questions about causality, since more intensive treatments conducted with fidelity that significantly improved parent skills should result in greater child gains. However, this finding is qualified by the fact that studies often did not report adequate information, with 43% not evaluating treatment fidelity, 39% not reporting parent changes in abilities to work with their children, and 19–39% not reporting details about intervention duration or frequency, with many only reporting the expected hours per week and only three studies logging parent intervention times. Future research needs to report intervention details.
Missing data also impacted our evaluations of risk of research bias. Studies often did not report allocation concealment (33%) or masking personnel involved in the interventions (33%), with 57% not reporting intent-to-treat analyses. Notably, studies that reported multiple procedures to reduce risk of research bias tended to yield outcomes of lower magnitude (g = 0.47) than studies reporting fewer procedures to reduce bias (g = 0.68). We therefore urge scholars to include risk of bias considerations when designing and reporting their studies.
Comparison with Previous Meta-Analyses and Systematic Reviews
Our meta-analysis included only RCTs yielded omnibus results that were very similar to the findings of prior meta-analyses that had included studies using quasi-experimental designs (e.g., Dyches et al., 2018). Notably, our review also yielded smaller inconsistency in findings across studies than prior reviews, which typically have reported higher variability (e.g., Beaudoin et al., 2014; Deb et al., 2020; Liu et al., 2020; Nevill et al., 2016; Parsons et al., 2017; Postorino et al., 2017; Ratliff-Black & Therrien, 2020; Tachibana et al., 2017; Tarver et al., 2019). Thus, restricting our focus to high quality research evidence (RCTs) apparently diminished sources of random error across studies and thus strengthened our confidence in the effectiveness of PIIs.
We explicitly sought to improve upon the methodology of prior reviews by conducting extensive literature searches and by evaluating possible indicators of study bias and effect size moderation. Our analyses of multiple indicators of research bias provide a major contribution to the field. We observed that many RCTs tended to be of low to moderate overall quality. All but two studies failed to report keeping researchers blind to participant allocation and isolated from the PII conditions/training. About 41% of studies did not report keeping researchers blind to outcome evaluations. Only 35% confirmed implementation fidelity. On a positive note, randomization tended to balance participants on baseline characteristics, as intended. A major strength of the PIIs evaluated in this meta-analysis was consistently low rates (< 10%) of participant attrition. Given high participant retention, intent-to-treat analyses should have yielded very similar outcomes to the results reported, but unfortunately only 31% of studies reported intent-to-treat analyses.
This meta-analysis also made a substantive contribution to the literature by evaluating differences in study outcomes when rated by either parents or researchers. Although parent-reported measures can be problematic for several reasons (Nevill et al., 2016; Oono et al., 2013; Wolstencroft et al., 2018), including expectancy and reporter bias (Tarver et al., 2019), the meta-analytic data suggest that such biases are not as systematic as anticipated. Parent observations have the advantages of being continuous across a broad range of circumstances, whereas professional observations are necessarily limited in duration and context. Researchers concerned about measurement bias may consider using multiple sources of data, including teacher-report measurements for child outcomes, which we rarely found in literature.
Our literature search was extensive and located studies from Japan, Korea, Thailand, Hong Kong, Taiwan, China, India, Pakistan, Iran, and Saudi Arabia. Unfortunately, many of those studies were excluded due to either not being RCTs or missing essential information (e.g., effect size data, active parent participation). Crucial information (e.g., frequency, duration, sessions, treatment fidelity) was missing in many studies, consistent with the findings and recommendations of Liu et al. (2020). Only nine studies from non-English speaking countries were included in our final analyses. Although we sought to improve on prior reviews, incomplete information hindered our ability to investigate how PIIs may work for non-Western populations with ASD. As Liu et al. (2020) emphasized, there is a need to increase research quality worldwide, particularly in developing nations.
Child gender was not a variable addressed in prior reviews. Across the studies we reviewed, females comprised an average of 16.8% of participants. When looking at individual studies' descriptive statistics, Kuravackel et al. (2018) was the only study with a high proportion of female participants with ASD (78.8%). Males with ASD were over-represented compared to females with ASD in the research we located, but consistent with the ratio of males to females with ASD. We could not find any interactions of the percentage of females with ASD with the effectiveness of PIIs. Similarly, we found no differences across child age, but the mean age of child participants was 5.5 years. Future research can consider intervention effectiveness among older children, as well as several other key considerations raised by this review.
Limitations and Directions for Future Research
Results of this meta-analysis should be interpreted in the context of several limitations. First, studies in this meta-analysis were almost always published, with only three (5.6%) being unpublished, even though we explicitly searched for unpublished studies. Although it stands to reason that scholars who conduct RCTs are more likely to persist to publication, it is also plausible that some RCTs with non-significant findings may not have been submitted for publication. We found no evidence of publication bias using standard meta-analytic methods, but it remains possible that unpublished data evaded our comprehensive search. Second, the literature search and subsequent coding required extensive time, with personal circumstances precluding updated coding after 2020. Third, the literature was characterized by a wide variety of interventions. It was therefore surprising that the child outcomes across different PIIs did not statistically differ, with a relatively small percentage of variability in outcomes across studies. Similarly, we do not know why intervention dosage was not predictive of child outcomes in this meta-analysis, except that effect size heterogeneity was small (with little variance to explain across studies). Fourth, we did not evaluate long-term outcomes because only a few studies included extended follow-up data. Future research needs to evaluate the effectiveness of PIIs over time (Deb et al., 2020; Liu et al., 2020; Parsons et al., 2017). Fifth, although we tried to include studies outside of North America, other world regions remained under-represented. Sixth, the studies did not adequately represent female children. Most of the RCTs consisted of predominantly male samples. Finally, we did not code for some potential moderators such as socioeconomic status, parent education level, parenting style, and marital status since those variables were inconsistently reported in the literature.
In addition to addressing the considerations just listed (e.g., long-term follow-up data and cultural differences), future research will need to consider ways to improve parent access to and utilization of PIIs. PIIs may be particularly useful for families unable to afford intensive ASD services or with limited access to nearby ASD services. Researchers can also examine how parent-implemented interventions impact the intersection of family functioning and child development (Stahmer & Pellecchia, 2015). Improved rigor and reporting of essential information remain high priorities. In particular, it is essential that researchers report the effectiveness of PIIs in improving parents’ abilities to facilitate child improvement, data which were reported only 57% of the time; researchers and future reviewers must evaluate this variable since evaluations of PIIs cannot assume that parents enact the skills taught them by professionals. Lastly, although RCTs provide strong research evidence, we invite other scholars to summarize rigorous single subject and multiple baseline designs that also contribute to our understanding of PII effectiveness. A synthesis of that important work will provide additional details about PIIs that cannot be provided in RCTs that average data across participants.
Conclusion
Data from 51 effect sizes extracted from RCTs involving 2895 children have demonstrated moderately strong benefits of PIIs compared with usual treatment and waitlist conditions. Child improvements were observed in positive behavior/social skills, maladaptive behaviors, and language/communication skills, with smaller gains in adaptive behavior/life skills. Different approaches to parent training and interventions yielded similar outcomes, whether a parent or professional provided the evaluations.
We restricted our analyses to RCTs, which reduced the likelihood of biases adversely impacting the results. Nevertheless, individual studies varied in terms of research quality. Scholars will benefit from considering the complexities of studying parent influence on children and should explicitly report attempts to reduce risk of research bias. When accounting for risk of research bias, the average estimate of PII effectiveness diminished slightly from g = 0.53 to g = 0.47, which remains a moderately strong improvement over treatment as usual and waitlist conditions.
A large body of data now supports services provided by parents and caregivers. Educational and human services and relevant public policy initiatives have an empirical basis for promoting PIIs, particularly when professional services cannot easily be accessed by all children in need of services.
References
*References marked with an asterisk indicate studies included in the meta-analysis
*Aldred, C., Green, J., & Adams, C. (2004). A new social communication intervention for children with autism: Pilot randomised controlled treatment study suggesting effectiveness. Journal of Child Psychology and Psychiatry, 45(8), 1420–1430. https://doi.org/10.1111/j.1469-7610.2004.00338.x
*Alquraini, T., Al-Odaib, A., Al-Dhalaan, H., Merza, H., & Mahoney, G. (2018). Feasibility of responsive teaching with mothers and young children with autism in Saudi Arabia. Journal of Early Intervention, 40(4), 304–316. https://doi.org/10.1177/1053815118789176
* Alvarado, C. R. (2017). The sensoriaffective interactional attunement scale: Development and preliminary validation of a measure geared toward interactional enhancement between primary caregivers and their young children with autism spectrum disorders. [Doctoral dissertation, Fielding Graduate University]. ProQuest Dissertations and Thesis Global.
Akamoglu, Y., & Meadan, H. (2018). Parent-implemented language and communication interventions for children with developmental delays and disabilities: A scoping review. Review Journal of Autism and Developmental Disorders, 5(3), 294–309.
*Amrollahi far, J., Hatami, H., & Ahadi, H. (2017). The effect of training play therapy to the mothers of autistic children to improve the verbal and nonverbal skills of their children. Novelty in Biomedicine, 5(1), 1–7.
Bearss, K., Burrell, T. L., Stewart, L., & Scahill, L. (2015a). Parent training in autism spectrum disorder: what’s in a name? Clinical Child and Family Psychology Review, 18(2), 170–182. https://doi.org/10.1007/s10567-015-0179-5
Bearss, K., Johnson, C., Handen, B., Smith, T., & Scahill, L. (2013). A pilot study of parent training in young children with autism spectrum disorders and disruptive behavior. Journal of Autism and Developmental Disorders, 43(4), 829–840. https://doi.org/10.1007/s10803-012-1624-7
*Bearss, K., Johnson, C., Smith, T., Lecavalier, L., Swiezy, N., Aman, M., McAdam, D. B., Butter, E., Stillitano, C., Minshawi, N., Sukhodolsky, D. G., Mruzek, D. W., Turner, K., Neal, T., Hallett, V., Mulick, J. A., Green, B., Handen, B., Deng, Y., … Scahill, L. (2015b). Effect of parent training vs parent education on behavioral problems in children with autism spectrum disorder. The Journal of the American Medical Association, 313(15), 1524–1533. https://doi.org/10.1001/jama.2015.3150
*Bearss, K., Johnson, C., Smith, T., Lecavalier, L., Swiezy, N., Aman, M., McAdam, D. B., Butter, E., Stillitano, C., Minshawi, N., Sukhodolsky, D. G., Mruzek, D. W., Turner, K., Neal, T., Hallett, V., Mulick, J. A., Green, B., Handen, B., Deng, Y., & Scahill, L. (2016). Baseline data incorrect. The Journal of the American Medical Association, 316(3), 350. https://doi.org/10.1001/jama.2016.9050
Beaudoin, A. J., Sébire, G., & Couture, M. (2014). Parent training interventions for toddlers with autism spectrum disorder. Autism Research and Treatment, 2014, 1–15. https://doi.org/10.1155/2014/839890
*Beaudoin, A. J., Sébire, G., & Couture, M. (2019). Parent-mediated intervention tends to improve parent-child engagement, and behavioral outcomes of toddlers with ASD-positive screening: A randomized crossover trial. Research in Autism Spectrum Disorders, 66, 1–12. https://doi.org/10.1016/j.rasd.2019.101416
Bennetts, S. K., Mensah, F. K., Westrupp, E. M., Hackworth, N. J., & Reilly, S. (2016). The agreement between parent-reported and directly measured child language and parenting behaviors. Frontiers in Psychology, 7, 1710.
Black, M. E., & Therrien, W. J. (2018). Parent training programs for school-age children with autism: A systematic review. Remedial and Special Education, 39(4), 243–256. https://doi.org/10.1177/0741932517730645
*Brian, J. A., Smith, I. M., Zwaigenbaum, L., & Bryson, S. E. (2017). Cross-site randomized control trial of the social ABCs caregiver-mediated intervention for toddlers with autism spectrum disorder. Autism Research, 10(10), 1700–1711. https://doi.org/10.1002/aur.1818
Buescher, A. V., Cidav, Z., Knapp, M., & Mandell, D. S. (2014). Costs of autism spectrum disorders in the United Kingdom and the United States. JAMA Pediatrics, 168(8), 721–728. https://doi.org/10.1001/jamapediatrics.2014.210
*Byford, S., Cary, M., Barrett, B., Aldred, C. R., Charman, T., Howlin, P., Hudry, K., Leadbitter, K., Le Couteur, A., McConachie, H., Pickles, A., Slonims, V., Temple, K. J., Green, J., the PACT Consortium. (2015). Cost-effectiveness analysis of a communication-focused therapy for pre-school children with autism: Results from a randomised controlled trial. BMC Psychiatry, 15(1), 1–13. https://doi.org/10.1186/s12888-015-0700-x
*Carter, A. S., Messinger, D. S., Stone, W. L., Celimli, S., Nahmias, A. S., & Yoder, P. (2011). A randomized controlled trial of Hanen’s ‘More Than Words’ in toddlers with early autism symptoms. Journal of Child Psychology and Psychiatry, 52(7), 741–752. https://doi.org/10.1111/j.1469-7610.2011.02395.x
*Casenhiser, D. M., Binns, A., McGill, F., Morderer, O., & Shanker, S. G. (2015). Measuring and supporting language function for children with autism: Evidence from a randomized control trial of a social-interaction-based therapy. Journal of Autism and Developmental Disorders, 45(3), 846–857. https://doi.org/10.1007/s10803-014-2242-3
*Casenhiser, D. M., Shanker, S. G., & Stieben, J. (2013). Learning through interaction in children with autism: Preliminary data from a social-communication-based intervention. Autism, 17(2), 220–241. https://doi.org/10.1177/1362361311422052
Cidav, Z., Munson, J., Estes, A., Dawson, G., Rogers, S., & Mandell, D. (2017). Cost offset associated with Early Start Denver Model for children with autism. Journal of the American Academy of Child & Adolescent Psychiatry, 56(9), 777–783. https://doi.org/10.1016/j.jaac.2017.06.007
* Clionsky, L. N. (2012). Child directed interaction training for young children with autism spectrum disorders: The impact on child language, social skills, adaptive skills, and problematic behaviors. [Doctoral dissertation, University of Florida]. ProQuest Dissertations and Thesis Global.
*Cook, J. M., Donovan, C. L., & Garnett, M. S. (2019). Parent-mediated cognitive behavioural therapy for young children with high-functioning autism spectrum disorder and anxiety: A randomized control trial. Early Child Development and Care, 189(1), 119–134. https://doi.org/10.1080/03004430.2017.1303684
Dawson, G., Rogers, S., Munson, J., Smith, M., Winter, J., Greenson, J., Donaldson, A., & Varley, J. (2010). Randomized, controlled trial of an intervention for toddlers with autism: The Early Start Denver Model. Pediatrics, 125(1), e17–e23. https://doi.org/10.1542/peds.2009-0958
Dawson-Squibb, J.-J., Davids, E. L., Harrison, A. J., Molony, M. A., & de Vries, P. J. (2020). Parent education and training for autism spectrum disorders: Scoping the evidence. Autism, 24(1), 7–25. https://doi.org/10.1177/1362361319841739
Deb, S., Retzer, A., Roy, M., Acharya, R., Limbu, B., & Roy, A. (2020). The effectiveness of parent training for children with autism spectrum disorder: A systematic review and meta-analyses. BMC Psychiatry. https://doi.org/10.1186/s12888-020-02973-7
*Dekker, V., Nauta, M. H., Timmerman, M. E., Mulde, E. J., van der Veen-Mulders, L., van den Hoofdakker, B. J., van Warners, S., Vet, L. J. J., Hoekstra, P. J., & de Bildt, A. (2019). Social skills group training in children with autism spectrum disorder: A randomized controlled trial. European Child & Adolescent Psychiatry, 28, 415–424. https://doi.org/10.1007/s00787-018-1205-1
Dyches, T. T., Smith, T. B., Korth, B. B., & Mandleco, B. (2018). Effects of parent-implemented interventions on outcomes for children with developmental disabilities: A meta-analysis. Perspectives on Early Childhood Psychology and Education, 3(1), 137–168.
Ferguson, J., Craig, E. A., & Dounavi, K. (2019). Telehealth as a model for providing behaviour analytic interventions to individuals with autism spectrum disorder: A systematic review. Journal of Autism and Developmental Disorders, 49(2), 582–616.
*Frankel, F., Myatt, R., Sugar, C., Whitham, C., Gorospe, C. M., & Laugeson, E. (2010). A randomized controlled study of parent-assisted children’s friendship training with children having autism spectrum disorders. Journal of Autism and Developmental Disorders, 40(7), 827–842. https://doi.org/10.1007/s10803-010-1016-9
Fuller, E. A., Oliver, K., Vejnoska, S. F., & Rogers, S. J. (2020). The effects of the Early Start Denver Model for children with autism spectrum disorder: A meta-analysis. Brain Sciences, 10(6), 1–17. https://doi.org/10.3390/brainsci10060368
Gerow, S., Hagan-Burke, S., Rispoli, M., Gregori, E., Mason, R., & Ninci, J. (2017). A systematic review of parent-implemented functional communication training for children with ASD. Behavior Modification, 42(3), 335–363. https://doi.org/10.1177/0145445517740872
*Ginn, N. C., Clionsky, L. N., Eyberg, S. M., Warner-Metzger, C., & Abner, J.-P. (2017). Child-directed interaction training for young children with autism spectrum disorders: Parent and child outcomes. Journal of Clinical Child & Adolescent Psychology, 46(1), 101–109. https://doi.org/10.1080/15374416.2015.1015135
*Green, J., Charman, T., McConachie, H., Aldred, C., Slonims, V., Howlin, P., Le Couteur, A., Leadbitter, K., Hudry, K., Byford, S., Barrett, B., Temple, K., Macdonald, W., Pickles, A., the PACT Consortium. (2010). Parent-mediated communication-focused treatment in children with autism (PACT): A randomised controlled trial. The Lancet, 375(9732), 2152–2160. https://doi.org/10.1016/s0140-6736(10)60587-9
*Handen, B. L., Aman, M. G., Arnold, L. E., Hyman, S. L., Tumuluru, R. V., Lecavalier, L., Corbett-Dick, P., Pan, X., Hollway, J. A., Buchan-Page, K. A., Silverman, L. B., Brown, N. V., Rice, R. R., Jr., Hellings, J., Mruzek, D. W., McAuliffe-Bellin, S., Hurt, E. A., Ryan, M. M., Levato, L., & Smith, T. (2015). Atomoxetine, parent training, and their combination in children with autism spectrum disorder and attention-deficit/hyperactivity disorder. Journal of the American Academy of Child & Adolescent Psychiatry, 54(11), 905–915. https://doi.org/10.1016/j.jaac.2015.08.013
*Handen, B. L., Johnson, C. R., Butter, E. M., Lecavalier, L., Scahill, L., Aman, M. G., McDougle, C. J., Arnold, L. E., Swiezy, N. B., Sukhodolsky, D. G., Mulick, J. A., White, S. W., Bearss, K., Hollway, J. A., Stigler, K. A., Dziura, J., Yu, S., Sacco, K., & Vitiello, B. (2013). Use of a direct observational measure in a trial of risperidone and parent training in children with pervasive developmental disorders. Journal of Developmental and Physical Disabilities, 25(3), 355–371. https://doi.org/10.1007/s10882-012-9316-y
*Hardan, A. Y., Gengoux, G. W., Berquist, K. L., Libove, R. A., Ardel, C. M., Phillips, J., Frazier, T. W., & Minjarez, M. B. (2015). A randomized controlled trial of pivotal response treatment group for parents of children with autism. Journal of Child Psychology and Psychiatry, 56(8), 884–892. https://doi.org/10.1111/jcpp.12354
Hatcher, A., & Page, J. (2020). Parent-implemented language intervention for teaching enhanced milieu teaching strategies to parents of low-socioeconomic status. Journal of Early Intervention, 42(2), 122–142. https://doi.org/10.1177/1053815119873085
*Ho, M.-H., & Lin, L.-Y. (2020). Efficacy of parent-training programs for preschool children with autism spectrum disorder: A randomized controlled trial. Research in Autism Spectrum Disorders, 71(101495), 1–10. https://doi.org/10.1016/j.rasd.2019.101495
*Iadarola, S., Levato, L., Harrison, B., Smith, T., Lecavalier, L., Johnson, C., Swiezy, N., Bearss, K., & Scahill, L. (2018). Teaching parents behavioral strategies for autism spectrum disorder: Effects on stress, strain, and competence. Journal of Autism and Developmental Disorders, 48, 1031–1040. https://doi.org/10.1007/s10803-017-3339-2
Ingersoll, B., & Dvortcsak, A. (2019). The project ImPACT manual for parents. Guilford.
Jhuo, R. A., & Chu, S. Y. (2022). A review of parent-implemented Early Start Denver Model for children with autism spectrum disorder. Children, 9(2), 285. https://doi.org/10.3390/children9020285
*Jocelyn, L. J., Casiro, O. G., Beattie, D., Bow, J., & Kneisz, J. (1998). Treatment of children with autism: A randomized controlled trial to evaluate a caregiver-based intervention program in community day-care centers. Journal of Developmental and Behavioral Pediatrics, 19(5), 326–334. https://doi.org/10.1097/00004703-199810000-00002
*Kasari, C., Gulsrud, A. C., Wong, C., Kwon, S., & Locke, J. (2010). Randomized controlled caregiver mediated joint engagement intervention for toddlers with autism. Journal of Autism and Developmental Disorders, 40(9), 1045–1056. https://doi.org/10.1007/s10803-010-0955-5
Kasari, C., Lawton, K., Shih, W., Barker, T. V., Landa, R., Lord, C., Orlich, F., King, B., Wetherby, A., & Senturk, D. (2014). Caregiver-mediated intervention for low-resourced preschoolers with autism: An RCT. Pediatrics, 134(1), e72–e79. https://doi.org/10.1542/peds.2013-3229
Kent, C., Cordier, R., Joosten, A., Wilkes-Gillan, S., Bundy, A., & Speyer, R. (2019). A systematic review and meta-analysis of interventions to improve play skills in children with autism spectrum disorder. Review Journal of Autism and Developmental Disorders, 7(1), 91–118. https://doi.org/10.1007/s40489-019-00181-y
Koegel, L. K., Koegel, R. L., Ashbaugh, K., & Bradshaw, J. (2014). The importance of early identification and intervention for children with or at risk for autism spectrum disorders. International Journal of Speech-Language Pathology, 16(1), 50–56. https://doi.org/10.3109/17549507.2013.861511
*Kuravackel, G. M., Ruble, L. A., Reese, R. J., Ables, A. P., Rodgers, A. D., & Toland, M. D. (2018). COMPASS for hope: Evaluating the effectiveness of a parent training and support program for children with ASD. Journal of Autism and Developmental Disorders, 48(2), 404–416. https://doi.org/10.1007/s10803-017-3333-8
Lee, L.-C., Stahmer, A. C., Wu, C.-C., Tsai, P.-C., & Chiang, C.-H. (2018). Home-based, parent-implemented intervention for underserved families in Taiwan. In M. Siller & L. Morgan (Eds.), Handbook of parent-implemented interventions for very young children with autism (pp. 385–391). Springer, Cham. https://doi.org/10.1007/978-3-319-90994-3_23
*Lehtonen, E., Muuvila, M. S., Helminen, T. M., Lauttia, J., Ahonen, S., Eriksson, K., & Kylliainen, A. (2020, June). Parent-led training for motivating eye contact in children with autism spectrum disorder: BOSCC outcome study [Poster presentation]. International Society for Autism Research, Virtual. Retrieved February 5, 2021, from https://insar.confex.com/insar/2020/meetingapp.cgi/Paper/34903
*Lindgren, S., Wacker, D., Schieltz, K., Suess, A., Pelzel, K., Kopelman, T., Lee, J., Romani, P., & O’Brien, M. (2020). A randomized controlled trial of functional communication training via telehealth for young children with autism spectrum disorder. Journal of Autism and Developmental Disorders, 50(12), 4449–4462. https://doi.org/10.1007/s10803-020-04451-1
Liu, Q., Hsieh, W.-Y., & Chen, G. (2020). A systematic review and meta-analysis of parent-mediated intervention for children and adolescents with autism spectrum disorder in mainland China, Hong Kong, and Taiwan. Autism, 24(8), 1960–1979. https://doi.org/10.1177/1362361320943380
*Mahoney, G., & Solomon, R. (2016). Mechanism of developmental change in the PLAY project home consultation program: Evidence from a randomized control trial. Journal of Autism and Developmental Disorders, 46(5), 1860–1871. https://doi.org/10.1007/s10803-016-2720-x
Moher, D., Liberati, A., Tetzlaff, J., Altman, D. G., PRISMA Group. (2009). Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. Annals of Internal Medicine, 151(4), 264–269. https://doi.org/10.7326/0003-4819-151-4-200908180-00135
Marfo, P., & Okyere, G. A. (2019). The accuracy of effect-size estimates under normals and contaminated normals in meta-analysis. Heliyon, 5(6), e01838.
*Matthews, N. L., Orr, B. C., Warriner, K., DeCarlo, M., Sorensen, M., Laflin, J., & Smith, C. J. (2018). Exploring the effectiveness of a peer-mediated model of the PEERS curriculum: A pilot randomized control trial. Journal of Autism and Developmental Disorders, 48(7), 2458–2475. https://doi.org/10.1007/s10803-018-3504-2
McConachie, H., & Diggle, T. (2007). Parent implemented early intervention for young children with autism spectrum disorder: A systematic review. Journal of Evaluation in Clinical Practice, 13(1), 120–129. https://doi.org/10.1111/j.1365-2753.2006.00674.x
*McDaniel, J., Yoder, P., Crandall, M., Millan, M. E., Ardel, C. M., Gengoux, G. W., & Hardan, A. Y. (2020). Effects of Pivotal Response Treatment on reciprocal vocal contingency in a randomized controlled trial of children with autism spectrum disorder. Autism, 24(6), 1566–1571. https://doi.org/10.1177/1362361320903138
Meadan, H., Snodgrass, M. R., Meyer, L. E., Fisher, K. W., Chung, M. Y., & Halle, J. W. (2016). Internet-based parent-implemented intervention for young children with autism. Journal of Early Intervention, 38(1), 3–23. https://doi.org/10.1177/1053815116630327
Nahmias, A. S., Pellecchia, M., Stahmer, A. C., & Mandell, D. S. (2019). Effectiveness of community-based early intervention for children with autism spectrum disorder: A meta-analysis. Journal of Child Psychology and Psychiatry, 60(11), 1200–1209. https://doi.org/10.1111/jcpp.13073
Nevill, R. E., Lecavalier, L., & Stratis, E. A. (2016). Meta-analysis of parent-mediated interventions for young children with autism spectrum disorder. Autism, 22(2), 84–98. https://doi.org/10.1177/1362361316677838
*Nowell, S. W., Watson, L. R., Boyd, B., & Klinger, L. G. (2019). Efficacy study of a social communication and self-regulation intervention for school-age children with autism spectrum disorder: A randomized controlled trial. Language, Speech, and Hearing Services in Schools, 50(3), 416–433. https://doi.org/10.1044/2019_lshss-18-0093
Ona, H. N., Larsen, K., Nordheim, L. V., & Brurberg, K. G. (2019). Effects of pivotal response treatment (PRT) for children with autism spectrum disorders (ASD): A systematic review. Review Journal of Autism and Developmental Disorders, 7(1), 78–90. https://doi.org/10.1007/s40489-019-00180-z
Oono, I. P., Honey, E. J., & McConachie, H. (2013). Parent-mediated early intervention for young children with autism spectrum disorders (ASD). Evidence-Based Child Health: A Cochrane Review Journal, 8(6), 2380–2479. https://doi.org/10.1002/ebch.1952
*Pajareya, K., & Nopmaneejumruslers, K. (2011). A pilot randomized controlled trial of DIR/Floortime™ parent training intervention for pre-school children with autistic spectrum disorders. Autism, 15(5), 563–577. https://doi.org/10.1177/1362361310386502
Parsons, D., Cordier, R., Vaz, S., & Lee, H. C. (2017). Parent-mediated intervention training delivered remotely for children with autism spectrum disorder living outside of urban areas: Systematic review. Journal of Medical Internet Research, 19(8), e198. https://doi.org/10.2196/jmir.6651
*Pashazadeh Azari, Z., Hosseini Hoseinzadeh, S. A., Rassafiani, M., Samadi, S. A., Hoseinzadeh, S., & Dunn, W. (2019). Contextual intervention adapted for autism spectrum disorder: An RCT of a parenting program with parents of children diagnosed with autism spectrum disorder (ASD). Iranian Journal Child Neurology, 13(4), 19–35.
Pi, H. J., Kallapiran, K., Munivenkatappa, S., Kandasamy, P., Kirubakaran, R., Russell, P., & Eapen, V. (2021). Meta-Analysis of RCTs of technology-assisted parent-mediated interventions for children with ASD. Journal of Autism and Developmental Disorders. https://doi.org/10.1007/s10803-021-05206-2
Postorino, V., Sharp, W. G., McCracken, C. E., Bearss, K., Burrell, T. L., Evans, A. N., & Scahill, L. (2017). A systematic review and meta-analysis of parent training for disruptive behavior in children with autism spectrum disorder. Clinical Child and Family Psychology Review, 20(4), 391–402. https://doi.org/10.1007/s10567-017-0237-2
*Rahman, A., Divan, G., Hamdani, S. U., Vajaratkar, V., Taylor, C., Leadbitter, K., Aldred, C., Minhas, A., Cardozo, P., Emsley, R., Patel, V., & Green, J. (2016). Effectiveness of the parent-mediated intervention for children with autism spectrum disorder in south Asia in India and Pakistan (PASS): A randomised controlled trial. The Lancet Psychiatry, 3(2), 128–136. https://doi.org/10.1016/s2215-0366(15)00388-0
Ratliff-Black, M., & Therrien, W. (2020). Parent-mediated interventions for school-age children with ASD: A meta-analysis. Focus on Autism and Other Developmental Disabilities, 36(1), 3–13. https://doi.org/10.1177/1088357620956904
Reichow, B. (2011). Overview of meta-analyses on early intensive behavioral intervention for young children with autism spectrum disorders. Journal of Autism and Developmental Disorders, 42(4), 512–520. https://doi.org/10.1007/s10803-011-1218-9
*Reitzel, J., Summers, J., Lorv, B., Szatmari, P., Zwaigenbaum, L., Georgiades, S., & Duku, E. (2013). Pilot randomized controlled trial of a functional behavior skills training program for young children with autism spectrum disorder who have significant early learning skill impairments and their families. Research in Autism Spectrum Disorders, 7(11), 1418–1432. https://doi.org/10.1016/j.rasd.2013.07.025
*Roberts, J., Williams, K., Carter, M., Evans, D., Parmenter, T., Silove, N., Clark, T., & Warren, A. (2011). A randomised controlled trial of two early intervention programs for young children with autism: Centre-based with parent program and home-based. Research in Autism Spectrum Disorders, 5(4), 1553–1566. https://doi.org/10.1016/j.rasd.2011.03.001
Rodgers, M., Simmonds, M., Marshall, D., Hodgson, R., Stewart, L. A., Rai, D., Wright, K., Ben-Itzchak, E., Eikeseth, S., Eldevik, S., Kovshoff, H., Magiati, I., Osborne, L. A., Reed, P., Vivanti, G., Zachor, D., & Le Couteur, A. (2021). Intensive behavioural interventions based on applied behaviour analysis for young children with autism: An international collaborative individual participant data meta-analysis. Autism, 25(4), 1137–1153. https://doi.org/10.1177/1362361320985680
Rogers, S. J., Estes, A., Lord, C., Vismara, L., Winter, J., Fitzpatrick, A., Guo, M., & Dawson, G. (2012). Effects of a brief Early Start Denver Model (ESDM)–based parent intervention on toddlers at risk for autism spectrum disorders: A randomized controlled trial. Journal of the American Academy of Child & Adolescent Psychiatry, 51(10), 1052–1065. https://doi.org/10.1016/j.jaac.2012.08.003
SaaS Enterprise. (2014). Covidence Systematic Review Software [Online software]. Veritas Health Innovation. Retrieved July 15, 2022, https://www.covidence.org/
Sandbank, M., Bottema-Beutel, K., Crowley, S., Cassidy, M., Feldman, J. I., Canihuante, M., & Woynaroski, T. (2020). Intervention effects on language in children with autism: A project AIM meta-analysis. Journal of Speech, Language, and Hearing Research, 63(5), 1537–1560. https://doi.org/10.1044/2020_jslhr-19-00167
*Schertz, H. H., Odom, S. L., Baggett, K. M., & Sideris, J. H. (2013). Effects of joint attention mediated learning for toddlers with autism spectrum disorders: An initial randomized controlled study. Early Childhood Research Quarterly, 28(2), 249–258. https://doi.org/10.1016/j.ecresq.2012.06.006
*Schertz, H. H., Odom, S. L., Baggett, K. M., & Sideris, J. H. (2018). Mediating parent learning to promote social communication for toddlers with autism: Effects from a randomized controlled trial. Journal of Autism and Developmental Disorders, 48(3), 853–867. https://doi.org/10.1007/s10803-017-3386-8
*Scudder, A., Wong, C., Ober, N., Hoffman, M., Toscolani, J., & Handen, B. L. (2019). Parent–child interaction therapy (PCIT) in young children with autism spectrum disorder. Child & Family Behavior Therapy, 41(4), 201–220. https://doi.org/10.1080/07317107.2019.1659542
Shea, B. J., Reeves, B. C., Wells, G., Thuku, M., Hamel, C., Moran, J., Moher, D., Tugwell, P., Welch, V., Kristjansson, E., & Henry, D. A. (2017). AMSTAR 2: A critical appraisal tool for systematic reviews that include randomised or non-randomised studies of healthcare interventions, or both. British Medical Journal, 358, j4008. https://doi.org/10.1136/bmj.j4008
*Shire, S. Y., Gulsrud, A., & Kasari, C. (2016). Increasing responsive parent–child interactions and joint engagement: Comparing the influence of parent-mediated intervention and parent psychoeducation. Journal of Autism and Developmental Disorders, 46(5), 1737–1747. https://doi.org/10.1007/s10803-016-2702-z
*Shum, K.K.-M., Cho, W. K., Lam, L. M. O., Laugeson, E. A., Wong, W. S., & Law, L. S. K. (2019). Learning how to make friends for Chinese adolescents with autism spectrum disorder: A randomized controlled trial of the Hong Kong Chinese version of the PEERS® intervention. Journal of Autism and Developmental Disorders, 49(2), 527–541. https://doi.org/10.1007/s10803-018-3728-1
*Siller, M., Hutman, T., & Sigman, M. (2013). A parent-mediated intervention to increase responsive parental behaviors and child communication in children with ASD: A randomized clinical trial. Journal of Autism and Developmental Disorders, 43(3), 540–555. https://doi.org/10.1007/s10803-012-1584-y
Soares, E. E., Bausback, K., Beard, C. L., Higinbotham, M., Bunge, E. L., & Gengoux, G. W. (2020). Social skills training for autism spectrum disorder: A meta-analysis of in-person and technological interventions. Journal of Technology in Behavioral Science, 6(1), 166–180. https://doi.org/10.1007/s41347-020-00177-0
*Sofronoff, K., Attwood, T., Hinton, S., & Levin, I. (2007). A randomized controlled trial of a cognitive behavioural intervention for anger management in children diagnosed with Asperger syndrome. Journal of Autism and Developmental Disorders, 37, 1203–1214. https://doi.org/10.1007/s10803-006-0262-3
*Sofronoff, K., Leslie, A., & Brown, W. (2004). Parent management training and Asperger syndrome: A randomized controlled trial to evaluate a parent based intervention. Autism, 8(3), 301–317. https://doi.org/10.1177/1362361304045215
*Solomon, M., Ono, M., Timmer, S., & Goodlin-Jones, B. (2008). The effectiveness of parent–child interaction therapy for families of children on the autism spectrum. Journal of Autism and Developmental Disorders, 38(9), 1767–1776. https://doi.org/10.1007/s10803-008-0567-5
*Solomon, R., Van Egeren, L. A., Mahoney, G., Quon Huber, M. S., & Zimmerman, P. (2014). PLAY project home consultation intervention program for young children with autism spectrum disorders. Journal of Developmental & Behavioral Pediatrics, 35(8), 475–485. https://doi.org/10.1097/dbp.0000000000000096
Stahmer, A. C., & Pellecchia, M. (2015). Moving towards a more ecologically valid model of parent-implemented interventions in autism. Autism, 19(3), 259–261. https://doi.org/10.1177/1362361314566739
Sterne, J. A., Savović, J., Page, M. J., Elbers, R. G., Blencowe, N. S., Boutron, I., & Higgins, J. P. (2019). RoB 2: A revised tool for assessing risk of bias in randomised trials. British Medical Journal, 366, l4898. https://doi.org/10.1136/bmj.l4898
Steinbrenner, J. R., Hume, K., Odom, S. L., Morin, K. L., Nowell, S. W., Tomaszewski, B., Szendrey, S., McIntyre, N. S., Yücesoy-Özkan, S., & Savage, M. N. (2020). Evidence-based practices for children, youth, and young adults with autism. The University of North Carolina at Chapel Hill, Frank Porter Graham Child Development Institute, National Clearinghouse on Autism Evidence and Practice Review Team. Retrieved July 15, 2022, from https://ncaep.fpg.unc.edu/sites/ncaep.fpg.unc.edu/files/imce/documents/EBP%20Report%202020.pdf
Symon, J. B. (2001). Parent education for autism: Issues in providing services at a distance. Journal of Positive Behavior Interventions, 3(3), 160–174. https://doi.org/10.1177/109830070100300304
Tachibana, Y., Miyazaki, C., Ota, E., Mori, R., Hwang, Y., Kobayashi, E., Terasaka, A., Tang, J., & Kamio, Y. (2017). A systematic review and meta-analysis of comprehensive interventions for pre-school children with autism spectrum disorder (ASD). PLoS ONE, 12(12), 1–28. https://doi.org/10.1371/journal.pone.0186502
Tanner, A., & Dounavi, K. (2020). The emergence of autism symptoms prior to 18 months of age: A systematic literature review. Journal of Autism and Developmental Disorders, 51(3), 973–993. https://doi.org/10.1007/s10803-020-04618-w
Tarver, J., Palmer, M., Webb, S., Scott, S., Slonims, V., Simonoff, E., & Charman, T. (2019). Child and parent outcomes following parent interventions for child emotional and behavioral problems in autism spectrum disorders: A systematic review and meta-analysis. Autism, 23(7), 1630–1644. https://doi.org/10.1177/1362361319830042
*Tellegen, C. L., & Sanders, M. R. (2014). A randomized controlled trial evaluating a brief parenting program with children with autism spectrum disorders. Journal of Consulting and Clinical Psychology, 82(6), 1193–1200. https://doi.org/10.1037/a0037246
*Tonge, B., Brereton, A., Kiomall, M., Mackinnon, A., & Rinehart, N. J. (2014). A randomised group comparison controlled trial of ‘preschoolers with autism’: A parent education and skills training intervention for young children with autistic disorder. Autism, 18(2), 166–177. https://doi.org/10.1177/1362361312458186
Turner, K. M., Markie-Dadds, C., & Sanders, M. R. (2010). Practitioner’s manual for primary care Triple P. Triple P International Proprietary Limited.
*Turner-Brown, L., Hume, K., Boyd, B. A., & Kainz, K. (2019). Preliminary efficacy of family implemented TEACCH for toddlers: Effects on parents and their toddlers with autism spectrum disorder. Journal of Autism and Developmental Disorders, 49(7), 2685–2698. https://doi.org/10.1007/s10803-016-2812-7
*Valeri, G., Casula, L., Menghini, D., Amendola, F. A., Napoli, E., Pasqualetti, P., & Vicari, S. (2019). Cooperative parent-mediated therapy for Italian preschool children with autism spectrum disorder: A randomized controlled trial. European Child & Adolescent Psychiatry, 29(7), 935–946. https://doi.org/10.1007/s00787-019-01395-5
Van Aert, R. C., Wicherts, J. M., & Van Assen, M. A. (2019). Publication bias examined in meta-analyses from psychology and medicine: A meta-meta-analysis. PLoS ONE, 14(4), 1–32. https://doi.org/10.1371/2Fjournal.pone.0215052
Virues-Ortega, J., Julio, F. M., & Pastor-Barriuso, R. (2013). The TEACCH program for children and adults with autism: A meta-analysis of intervention studies. Clinical Psychology Review, 33(8), 940–953. https://doi.org/10.1016/j.cpr.2013.07.005
Wang, Z., Loh, S. C., Tian, J., & Chen, Q. J. (2021). A meta-analysis of the effect of the Early Start Denver Model in children with autism spectrum disorder. International Journal of Developmental Disabilities. https://doi.org/10.1080/20473869.2020.1870419
Warren, Z., McPheeters, M. L., Sathe, N., Foss-Feig, J. H., Glasser, A., & Veenstra-VanderWeele, J. (2011). A systematic review of early intensive intervention for autism spectrum disorders. Pediatrics, 127, 1303–1311. https://doi.org/10.1542/peds.2011-0426
*Whittingham, K., Sofronoff, K., Sheffield, J., & Sanders, M. R. (2009). Stepping Stones Triple P: An RCT of a parenting program with parents of a child diagnosed with an autism spectrum disorder. Journal of Abnormal Child Psychology, 37(4), 469–480. https://doi.org/10.1007/s10802-008-9285-x
Wilson, D. B. (2021). Effect size calculator. Retrieved July 15, 2022 from https://www.campbellcollaboration.org/escalc/html/EffectSizeCalculator-Home.php.
Wolstencroft, J., Robinson, L., Srinivasan, R., Kerry, E., Mandy, W., & Skuse, D. (2018). A systematic review of group social skills interventions, and meta-analysis of outcomes, for children with high functioning ASD. Journal of Autism and Developmental Disorders, 48(7), 2293–2307. https://doi.org/10.1007/s10803-018-3485-1
*Wong, V. C. N., & Kwan, Q. K. (2010). Randomized controlled trial for early intervention for autism: A pilot study of the Autism 1-2-3 project. Journal of Autism and Developmental Disorders, 40(6), 677–688. https://doi.org/10.1007/s10803-009-0916-z
*Yoo, H.-J., Bahn, G., Cho, I.-H., Kim, E.-K., Kim, J.-H., Min, J.-W., Lee, W.-H., Seo, J.-S., Jun, S.-S., Bong, G., Cho, S., Shin, M.-S., Kim, B.-N., Kim, J.-W., Park, S., & Laugeson, E. A. (2014). A randomized controlled trial of the Korean version of the PEERS® parent-assisted social skills training program for teens with ASD. Autism Research, 7(1), 145–161. https://doi.org/10.1002/aur.1354
Yu, Q., Li, E., Li, L., & Liang, W. (2020). Efficacy of interventions based on applied behavior analysis for autism spectrum disorder: A meta-analysis. Psychiatry Investigation, 17(5), 432–443. https://doi.org/10.30773/pi.2019.0229
*Zand, D. H., Bultas, M. W., McMillin, S. E., Halloran, D., White, T., McNamara, D., & Pierce, K. J. (2018). A pilot of a brief positive parenting program on children newly diagnosed with autism spectrum disorder. Family Process, 57(4), 901–914. https://doi.org/10.1111/famp.12334
Funding
Financial support was received from the David O. McKay School of Education at Brigham Young University, Provo, Utah, USA.
Author information
Authors and Affiliations
Contributions
WMC, TS, TT: Conceptualization; WMC, MB, TS, DC: Data curation; WMC, MB, TS, DC: Data coding; WMC, TS: Formal analysis; TS: Funding acquisition; WMC, TS: Methodology; WMC: Project administration; WMC: Writing original draft; TS, TT: Supervision.
Corresponding authors
Ethics declarations
Conflict of interest
The authors affirm that there are no conflicts of interest or competing interests relevant to this manuscript.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Cheng, W.M., Smith, T.B., Butler, M. et al. Effects of Parent-Implemented Interventions on Outcomes of Children with Autism: A Meta-Analysis. J Autism Dev Disord 53, 4147–4163 (2023). https://doi.org/10.1007/s10803-022-05688-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10803-022-05688-8