Abstract
Purpose
To test whether some biometry measurements provided by the Lenstar LS900 compared well with the AL-Scan, Pentacam rotating Scheimpflug camera, Ultrasound Biomicroscopy (UBM) and Tomey EM-3000.
Methods
Two hundred and one patients having routine cataract surgery had standard preoperative assessment. In this clinical study, the axis length (AL) and lens thickness (LT) were taken by Lenstar LS900 and AL-Scan; anterior chamber depth (ACD) was taken by Lenstar LS900, A-Scan, Pentacam and UBM; central corneal thickness (CCT) was taken by Lenstar LS900, Pentacam and Tomey EM-3000. The results were compared using a Wilcoxon–Mann–Whitney U test and Pearson correlation calculations. Agreement was assessed through intraclass correlation coefficients and Bland–Altman plots.
Results
The highest correlation was found between Lenstar and AL-Scan for AL (r = 0.975; P < 0.001). For LT measurements, the correlation between these two devices was also good (r = 0.699; P < 0.001). Excellent correlations were showed between Lenstar and Pentacam or UBM for ACD (r = 0.948, 0.704, respectively, both P < 0.001), but not between Lenstar and AL-Scan (r = 0.453, P < 0.001). The correlations of CCT between Lenstar and Pentacam or Tomey EM-3000 were both excellent (r = 0.817, 0.882, respectively, both P < 0.001).
Conclusions
In phakic eyes of cataract patients, measurements of AL, LT, ACD and CCT from Lenstar LS900 yielded results that correlated very well with other clinical instruments.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Accurate and precise measurements of ocular biometric parameters are crucial for many clinical and research applications in ophthalmology. Interferometry and ultrasound are two currently used ocular biometry techniques for obtaining biometric data from patients’ eyes in clinic. Interferometry has been shown to be more precise and more reliable than ultrasound [1].
The Lenstar LS 900 (Haag-Streit, Bern, Switzerland) is a relatively new non-contact biometry device (a near-infrared optical low-coherence reflectometer) that can simultaneously provide axis length (AL), anterior chamber depth (ACD), central corneal thickness (CCT), lens thickness (LT), keratometry, retinal thickness, white-to-white distance (WTW) and eccentricity of the visual optical line [2]. The measurement of AL, LT, ACD and CCT has become a useful clinical and research technique in aphakic and phakic intraocular lens surgery. AL-Scan has been the common technique for a long time to measure ACD, LT and AL because of its cost-effectiveness and ease of use. Nevertheless, it has some shortcomings, such as the risk of infections and the need for topical anesthesia. As we all know, UBM can also measure ACD when obtaining the anterior segment image [3]. Tomey EM-3000, a non-contact specular microscopy device, not only can obtain endothelial parameters including endothelial cell count, maximum, minimum and average endothelial cell size, but also can measure CCT [4]. The Pentacam (Oculus, Wetzlar, Germany) uses a rotating Scheimpflug camera to image the anterior segment of the eye including the lens. The CCT and ACD measurements provided by the Pentacam have been reported to have excellent repeatability [5, 6].
When different ways of measuring the same variable are available, it is of interest to find out how well two different methods agree, as strong agreement implies that they can be used interchangeably. Previous studies have demonstrated excellent intra-operator repeatability, inter-operator reproducibility and accuracy of the Lenstar [7, 8]. Comparison of ocular biometric parameters including AL, LT, ACD and CCT between biometer Lenstar and the other common techniques of biometry has been made in multiple studies [9,10,11,12,13,14]. The purpose of this study was to prospectively evaluate agreement between AL, LT, ACD and CCT measurements derived from Lenstar and the other four biometers before cataract surgery.
Methods
This retrospective study was performed in accordance with the protocols of the Declaration of Helsinki and after the approval of the Clinical Research Ethics Committee at the affiliated hospital of Nantong University from January 2018 to August 2018. Informed consent form was obtained each of the participants prior to the enrollment. Eyes with previous ocular surgery and ocular diseases such as glaucoma, retinal disorder and corneal diseases were excluded. Measurements of ocular biometry were taken by experienced examiners. In this clinical study, AL and LT were obtained by Lenstar and AL-Scan (10 MHz, the classic A-mode ultrasonic technique, SW-1000, Tianjin Sower Electronic Technology Co., Ltd, China); ACD was taken by Lenstar (from tear film to anterior capsule of lens), AL-Scan (from corneal epithelium to anterior capsule of lens), Pentacam (from tear film to anterior capsule of lens) (Oculus, Wetzlar, Germany) and UBM (from corneal epithelium to anterior capsule of lens) (50 MHz, MD-300L, Tianjin Maida Electronic Technology Co., Ltd, China). CCT was taken by Lenstar, Pentacam and Tomey EM-3000 (Tomey, Nagoya, Japan). The results were compared using a Wilcoxon–Mann–Whitney U test and Pearson correlation calculations. The AL, LT, ACD and CCT were analyzed and compared between the two instruments. SPSS software version 19.0 (IBM) was used for descriptive statistical analysis using the mean, standard deviation, median and minimum/maximum values. Differences among the devices were tested with the Wilcoxon–Mann–Whitney U test. Bland–Altman graphs were plotted to show measurement differences against the mean values. Correlations were tested using the Pearson rank correlation coefficient, with P values less than 0.05 considered statistically significant.
Results
A total of 201 eyes of 201 patients were enrolled in this prospective, non-randomized, consecutive, mono-centric case series. The mean age was 66.7 ± 12.16 years (SD) (range 30–89). One hundred and three left eyes and 98 right eyes were measured in all patients (female 64%, male 36%).
Table 1 shows mean values, standard deviations, minimum and maximum AL measurements, LT, ACD and CCT from Lenstar, as well as other devices. On average, AL with the Lenstar showed higher values compared with the AL-Scan. The differences were statistically significant (P < 0.05).
Regarding measurements of LT, there were no any differences between Lenstar and AL-Scan. For ACD measurements, the Lenstar yielded higher mean values than Pentacam and UBM (P < 0.001; P < 0.001) and less mean values than AL-Scan (P < 0.001). The results are listed in Table 2.
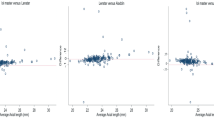
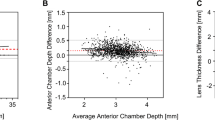
Figure 1a shows the differences in Bland–Altman graphs for AL between Lenstar and AL-Scan. Figure 1b shows the differences in Bland–Altman graphs for LT between Lenstar and AL-Scan. Figure 1c, d, f shows the ACD differences in Bland–Altman graphs for Lenstar, AL-Scan, UBM and Pentacam. Figure 1e, g shows the CCT differences in Bland–Altman graphs for Lenstar, AL-Scan, Tomey EM-3000 and Pentacam.
a Bland–Altman plot comparing AL, LT, CCT and ACD measured with the Lenstar and other 4 biometers (Pentacam, UBM, AL-Scan and Tomey EM-3000). a, b Lenstar showed no difference for AL and LT measurements compared with AL-Scan. c–e Bland–Altman plot comparing ACD measured with the Lenstar and other 3 biometers (Pentacam, UBM, AL-Scan). The Lenstar showed lower values for ACD measurements than AL-Scan and higher values than Pentacam and UBM. f, g Bland–Altman plot comparing CCT measured with Lenstar and 2 biometers (Pentacam and Tomey EM-3000). Lenstar yielded slightly lower values than Pentacam and slightly higher than Tomey EM-3000 (ACD = anterior chamber depth; AL = axial length; CCT = central corneal thickness; LT = lens thickness)
The correlations between Lenstar and the 4 devices for CCT, ACD, AL and LT are presented in Table 3. The correlation was very high between Lenstar and Pentacam or UBM for ACD (r = 0.948, 0.704, respectively), but not for AL-Scan (r = 0.453) and between Lenstar and Pentacam or Tomey EM-3000 for CCT (r = 0.817, 0.882, respectively). For LT measurements, the correlation between these two devices was also good (r = 0.699). The highest correlation was found between Lenstar and AL-Scan for AL (r = 0.975). These results are shown in Fig. 2.
Correlation between Lenstar and other 4 biometers as follows: a CCT; b ACD; c AL; d LT. a Blue squares describe correlation between Lenstar and Pentacam, and red rings denote correlation between Lenstar and Tomey EM-3000. b Black squares describe correlation between Lenstar and Pentacam, and red rings denote correlation between Lenstar and UBM, and green triangles show correlation between Lenstar and AL-Scan (ACD = anterior chamber depth; AL = axial length; CCT = central corneal thickness; LT = lens thick)
Discussion
In this study, we evaluated agreement between AL, LT, ACD and CCT measurements derived from Lenstar and the other four biometers in a clinical cohort of patients with age-related cataracts. The AL-Scan ultrasonic method was the most commonly used method that was regarded as the “gold standard” for the measurement of AL, LT and ACD for years. Although the optical biometry devices are more informative for ocular biometry compared with an AL-Scan contact ultrasound machine, the data about the reliability and interchangeability of the different measuring techniques are controversial [15].
A study compared Lenstar with AL-Scan in 234 eyes and reported that all of the measurements were correlated [16]. There is also a good agreement regarding ACD, AL and LT between Lenstar and A-Scan ultrasound in highly myopic subjects [17]. However, a research compared the CCT, AL, ACD and LT measured with Lenstar and AL-Scan in more than 500 children and found that there was agreement between instruments for CCT and ACD. There are the differences in AL and LT measured by Lenstar and ultrasound in a previous study. Therefore, it is suggested not to be used interchangeably [18]. However, the excellent correlations of AL and LT between Lenstar and AL-Scan were found. However, there was a weak correlation between two devices for ACD measurements in the present study (r = 0.453).
The average value of ACD in the eyes measured by UBM was found less than 3.0 mm. There was a significant difference between measured value by A-Scan and UBM [19]. There is a previous study to compare ACD between Lenstar and UBM [20]. In this present study, there is a good correlation between them. The difference between UBM and AL-Scan was significant, but the correlation was week (r = 0.294). In glaucoma patients, there was a statistically significant difference between the mean values of ACD, but not CCT when compared anterior segment measurements obtained using the Lenstar and Pentacam [12]. The ACD and CCT measurements obtained from the Lenstar and the Pentacam showed excellent correlation in cataract subjects and can be used interchangeably, and this is consistent with previous reports [1, 14, 21]. Mean values of CCT in cataract eyes measured by Lenstar and Tomey EM-3000 were 529.02 ± 32.17 mm and 526.81 ± 35.43 mm, respectively. There is no statistical significance between the two devices. There were some limitations in this study including a relatively small number of patients. We also did not compare the difference between Lenstar and other 4 devices for different AL in the patients.
In summary, there is a high correlation among the Lenstar and AL-Scan for AL and LT, Lenstar and Pentacam for ACD and CCT, Lenstar and UBM for ACD, Lenstar and Tomey EM-3000 for CCT.
References
O’Donnell C, Hartwig A, Radhakrishnan H (2012) Comparison of central corneal thickness and anterior chamber depth measured using LenStar LS900, Pentacam, and Visante AS-OCT. Cornea 31(9):983–988
Huang J, Pesudovs K, Wen D et al (2011) Comparison of anterior segment measurements with rotating scheimpflug photography and partial coherence reflectometry. J Cataract Refract Surg 37(2):341–348
Shen L, Wang XN, Li DJ et al (2018) Comparison of swept source anterior segment optical coherence tomography and ultrasound biomicroscopy in measurement of anterior chamber depth and anterior chamber angle data in age-related cataract patients. Zhonghua Yan Ke Za Zhi 54(9):678–682
Gokcinar NB, Yumusak E, Ornek N et al (2019) Agreement and repeatability of central corneal thickness measurements by four different optical devices and an ultrasound pachymeter. Int Ophthalmol 39(7):1589–1598
Lackner B, Schmidinger G, Skorpik C (2005) Validity and repeatability of anterior chamber depth measurements with Pentacam and Orbscan. Optom Vis Sci 82(9):858–861
Ucakhan OO, Ozkan M, Kanpolat A (2006) Corneal thickness measurements in normal and keratoconic eyes: pentacam comprehensive eye scanner versus noncontact specular microscopy and ultrasound pachymetry. J Cataract Refract Surg 32(6):970–977
Cruysberg LP, Doors M, Verbakel F et al (2010) Evaluation of the Lenstar LS 900 non-contact biometer. Br J Ophthalmol 94(1):106–110
Tappeiner C, Rohrer K, Frueh BE et al (2010) Clinical comparison of biometry using the non-contact optical low coherence reflectometer (Lenstar LS 900) and contact ultrasound biometer (Tomey AL-3000) in cataract eyes. Br J Ophthalmol 94(5):666–667
Hashemi H, Heydarian S, Khabazkhoob M, et al (2021) Anterior chamber depth measurement using Pentacam and Biograph in children. Clin Exp Optom, pp 1–5
Arruda HA, Pereira JM, Neves A et al (2021) Lenstar LS 900 versus Pentacam-AXL: analysis of refractive outcomes and predicted refraction. Sci Rep 11(1):1449
Pereira JMM, Neves A, Alfaiate P et al (2018) Lenstar(R) LS 900 vs Pentacam(R)-AXL: comparative study of ocular biometric measurements and intraocular lens power calculation. Eur J Ophthalmol 28(6):645–651
Sen E, Inanc M, Elgin U, Yilmazbas P (2018) Comparison of anterior segment measurements with LenStar and Pentacam in patients with newly diagnosed glaucoma. Int Ophthalmol 38(1):171–174
Borrego-Sanz L, Saenz-Frances F, Bermudez-Vallecilla M et al (2014) Agreement between central corneal thickness measured using Pentacam, ultrasound pachymetry, specular microscopy and optic biometer Lenstar LS 900 and the influence of intraocular pressure. Ophthalmologica 231(4):226–235
Ucakhan OO, Akbel V, Biyikli Z, Kanpolat A (2013) Comparison of corneal curvature and anterior chamber depth measurements using the manual keratometer, Lenstar LS 900 and the Pentacam. Middle East Afr J Ophthalmol 20(3):201–206
Rose LT, Moshegov CN (2003) Comparison of the Zeiss IOLMaster and applanation A-scan ultrasound: biometry for intraocular lens calculation. Clin Exp Ophthalmol 31(2):121–124
Salouti R, Nowroozzadeh MH, Zamani M et al (2011) Comparison of the ultrasonographic method with 2 partial coherence interferometry methods for intraocular lens power calculation. Optometry 82(3):140–147
Shen P, Zheng Y, Ding X et al (2013) Biometric measurements in highly myopic eyes. J Cataract Refract Surg 39(2):180–187
Gursoy H, Sahin A, Basmak H et al (2011) Lenstar versus ultrasound for ocular biometry in a pediatric population. Optom Vis Sci 88(8):912–919
Xu T, Li YZ, Zhang S (2013) A comparison study of anterior chamber depth using a sonography and biomicroscopy in patient with cataract. Zhonghua Yan Ke Za Zhi 49(2):130–133
Dominguez-Vicent A, Perez-Vives C, Ferrer-Blasco T et al (2016) Device interchangeability on anterior chamber depth and white-to-white measurements: a thorough literature review. Int J Ophthalmol 9(7):1057–1065
Zhao J, Chen Z, Zhou Z et al (2013) Evaluation of the repeatability of the Lenstar and comparison with two other non-contact biometric devices in myopes. Clin Exp Optom 96(1):92–99
Acknowledgements
This study was supported by the National Natural Science Foundation of China (No. 81873676) and China Postdoctoral Science Foundation (2020M681686).
Funding
The authors have not disclosed any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zhang, J., Wang, Y. Agreement analysis of Lenstar with other four techniques of biometry before cataract surgery. Int Ophthalmol 42, 3541–3546 (2022). https://doi.org/10.1007/s10792-022-02352-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-022-02352-z