Abstract
Osteoarthritis (OA) is the most prevalent joint disease predominantly characterized by inflammation which drives cartilage destruction. Mesenchymal stem cells-condition medium (MSC-CM) or the secretome is enriched with bioactive factors and possesses anti-inflammatory and regenerative effects. The present study aimed at evaluating the effects of combining MSC-conditioned medium with stigmasterol compared with the individual treatments in alleviating interleukin-1 beta (IL-1β)-induced inflammation in rat chondrocytes. Stigmasterol is a phytosterol exhibiting anti-inflammatory effects. IL-1β (10 ng/ml) was used to induce inflammation and mimic OA in-vitro in primary rat articular chondrocytes. The IL-1β-stimulated chondrocytes were treated with MSC-CM, stigmasterol, and a combination of MSC-CM and stigmasterol for 24 h. Cell viability was measured using MTT assay. Protein expression of inducible nitric oxide synthase (iNOS), interleukin-6 (IL-6), collagen II (COL2A1) and matrix metalloproteinase (MMP)-13 were evaluated by immunofluorescence. Gene expression levels of MMP-3, MMP-13 and A Disintegrin-like and Metalloproteinases with Thrombospondin Motifs (ADAMTS)-5 were measured using qRT-PCR. NF-κB signaling pathway was studied using western blotting. A significant reduction in the expression of iNOS, IL-6, MMP-3, MMP-13 and ADAMTS-5, and a significant increase in COL2A1 expression was observed in the rat chondrocytes across all the treatment groups. However, the combination treatment of MSC-CM and stigmasterol remarkably reversed the IL-1β-induced pro-inflammatory/pro-catabolic responses to near normal levels comparable to the control group. The combination treatment (MSC-CM + stigmasterol) elicited a superior anti-inflammatory/anti-catabolic effect by inhibiting the IL-1β-induced NF-κB activation evidenced by the negligible phosphorylation of p65 and IκBα subunits, thereby emphasizing the benefit of the combination therapy over the individual treatments.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Osteoarthritis (OA) is the common joint disorder primarily affecting the diarthrodial joints and advances into severe degenerative arthritis. OA forms the leading cause of disability and joint pain impacting the socio-economic status across the globe with a prevalence of 16% (Cui et al. 2020). With a multifactorial etiology including age, obesity, trauma, sports injuries and altered biomechanics, OA progresses as an irreversible, often heterogeneous disease commonly ending up with complete joint destruction (Chen et al. 2017). Inflammation triggered by mechanical trauma leading to initial cartilage breakdown has been identified to be a critical determinant in initiating and accelerating OA development (van der Kraan and van den Berg 2012). Evidence(s) suggest for a prominent role for IL-1β, a key early-stage pro-inflammatory cytokine, in exacerbating the pathogenesis of OA by activating key signaling pathways including the nuclear factor kappa-light-chain-enhancer of activated B cells (NF-κB), mitogen-activated protein kinases (MAPK), and transcription factors (Daheshia and Yao 2008). Consequently, this triggers a sequelae of intracellular events that culminate in the activation of cartilage-degrading proteinases (MMPs and ADAMTS), production of inflammatory molecules (iNOS), pro-inflammatory cytokines (IL-6), causing a decrease in the synthesis of cartilage extracellular matrix ultimately leading to cartilage degradation and joint damage (Jenei-Lanzl et al. 2019; Kobayashi et al. 2005). Till now there is no single therapeutic agent that has been deemed safe and effective for treating OA. Strategies aimed at targeting the IL-1β-induced catabolic metabolism and inflammatory responses have proven to offer immense promise(s) in curtailing OA progression (Ding et al. 2020).
In recent years, advances in regenerative medicine/stem cell research have led to promising stem cell-based therapies for cartilage repair in OA. Notably, mesenchymal stem cells (MSCs) have emerged as attractive candidates for application in laboratories and clinical studies for cartilage repair/regeneration in OA owning to their self-renewal, multipotent, anti-inflammatory and immunomodulatory functions (Jo et al. 2014; Lee et al. 2019a; Satué et al. 2019; Song et al. 2018; Xing et al. 2020). The MSCs are isolated from a variety of tissues such as bone marrow, adipose tissue, fetal liver, umbilical cord, muscle, endometrial polyps, dental tissue, synovial fluid, skin, foreskin, Wharton’s jelly, placenta, dental pulp, breast milk, gingiva, amnion and menstrual blood, and characterized as plastic adherent cells with fibroblastic morphology in culture (Kangari et al. 2020). MSCs have been demonstrated to offer their therapeutic potential towards regenerative medicine and tissue repair by their intrinsic potential to migrate and home into the damaged tissue, differentiate and integrate into the cells of the host tissue (Fan et al. 2020). However, in recent times, there is increasing evidence to suggest that the efficacy of many MSC-based therapies could be attributed to their paracrine secretion of a broad spectrum of lipids, proteins, nucleic acid, and biologically active trophic factors which include anti-apoptotic factors, growth factors, anti-inflammatory cytokines, chemokines and extracellular vesicles generally referred to as the secretome or the MSC-conditioned medium (MSC-CM) (Ahangar et al. 2020; Chen et al. 2008; Kim et al. 2008; Walter et al. 2010; Zhou et al. 2013). Regarding the composition, the secretome has been demonstrated to contain an array of growth/differentiation factors, including vascular endothelial growth factor (VEGF), platelet-derived growth factor (PDGF), epidermal growth factor, insulin-like growth factor I and II (IGF-I, IGF-II), hepatocyte growth factor (HGF), fibroblast growth factor 2/basic fibroblast growth factor (FGF-2/bFGF), keratinocyte growth factor/fibroblast growth factor-7 (KGF/FGF-7), platelet-derived endothelial cell growth factor, heparin-binding epidermal growth factor, neural growth factor (NGF), and brain-derived neurotrophic factor (BDNF), in addition to anti-inflammatory cytokines such as transforming growth factor- (TGF) β1 and interleukins (IL), including IL-6, IL-10, IL-27, IL-17, and IL-13 (El Moshy et al. 2020). The secretome/MSC-CM can modulate the injured tissue environment and orchestrate subsequent regenerative processes including cell migration, proliferation, differentiation, and matrix synthesis (González-González et al. 2020). Findings from a large number of experimental studies have also shown that MSC-derived secretome demonstrated similar therapeutic effects to those observed after transplantation of MSCs whilst circumventing the side effects of MSC-based therapy, such as unwanted differentiation of engrafted MSCs (Harrell et al. 2019). The MSC secretome offers distinctive biological and logistical advantages over the transplanted MSCs in tissue engineering/regenerative medicine including the ease of economical mass production from commercial cell lines under controlled laboratory conditions, better storage without toxic cryopreservative agents for longer periods without loss of potency, immediate availability for practical application and content evaluation similar to pharmaceutical agents (Vizoso et al. 2017). MSC-CM can also be manipulated, stored and characterized more easily than cells and sterilization is possible without loss of efficacy (Benavides-Castellanos et al. 2020). Accruing evidence(s) from several studies have also demonstrated the therapeutic effects of MSC-CM/secretome in treating many diseases (Sagaradze et al. 2019).
Nevertheless, limitations in clinical stratification of OA patients as well as the choice of available therapeutics have opened up newer avenues to look out for combination therapies which could offer a newer paradigm of treatment to realize better treatment outcomes. Several pre-clinical and clinical studies have documented credible evidence(s) for the synergistic effects of combination therapies resulting in enhanced treatment outcomes with better tolerability and less adverse side effects especially in the case of musculoskeletal disorders (Haleagrahara et al. 2018; Kaur et al. 2011; Lee et al. 2019b; Usha and Naidu 2004; Yu et al. 2018). Indeed the impetus obtained from our earlier study re-instates the efficacy of combination line of approach in OA management (Pragasam et al. 2021). Phytosterols or plant sterols are a group of naturally occurring plant compounds that have been shown to elicit immense health benefits across a wide range of disease conditions. Stigmasterol, also known as anti-stiffness factor, is the most common phytosterol found in several nuts, seeds, legumes, banana, cabbage, and medicinal herbs including Akebia quinata, Gypsophila oldhamiana, Emilia sonchifolia, Eucalyptus globules, Aralia cordata, Emilia sonchifolia, Theobroma cacao L (Yadav et al. 2018). In addition to its proven anti-osteoarthritic effects (Chen et al. 2012; Gabay et al. 2010), stigmasterol possesses anti-nociceptive (Walker et al. 2017), anti-tumor (Ghosh et al. 2011), anti-psychotic (Yadav et al. 2018), anti-oxidant (Panda et al. 2009), anti-inflammatory (García et al. 1999), anti-diabetic (Ramu et al. 2016), anti-allergic (Antwi et al. 2018), chemopreventive (Sofi et al. 2018) and neuroprotective effects (Haque et al. 2021). Very recently, we demonstrated that intra-articular transplantation of mesenchymal stem cells combined with stigmasterol resulted in better cartilage repair/regeneration compared to the individual treatments in a monosodium-iodoacetate induced rat model of OA (Pragasam et al. 2021). Considering the benefits of MSC-secretome in regenerative therapy, we anticipate that the MSC-derived secretome could represent a newer, cell-free MSC-based therapeutic approach for the attenuation of pro-inflammatory/catabolic responses in OA. Hence, in the present study, we aimed to assess the potential of combining rat bone marrow mesenchymal stem cells-derived conditioned medium (MSC-CM) with stigmasterol in ameliorating the IL-1β-induced inflammatory responses in rat primary chondrocytes. We hypothesize that combining MSC-CM with stigmasterol would elicit a superior anti-inflammatory/anti-catabolic effect compared to the individual treatments in-vitro.
Materials and methods
Animals
The animal study was approved by the Institutional Animal Ethical Committee, National Institute of Nutrition (NIN), Hyderabad (P29F/III-IAEC/NIN/12/2016/SSJ/WNIN(CG)-6F/WNIN-Gr-Ob-42F). Four-week-old female Wistar rats were obtained from the Animal Facility, NIN and were housed in standard polypropylene cages, maintained at 22 ± 1 °C with 12-h dark/light cycles, and humidity of 50–60%, and were fed standard laboratory rat chow prepared at our animal facility with free access to water. All the experiments were performed in accordance with the regulations and guidelines of the Committee for the Purpose of Control and Supervision of Experiments on Animals (CPCSEA).
Isolation of rat primary chondrocytes
Primary articular chondrocytes were isolated from four-week-old WNIN Wistar rats according to a previously published method (Oseni et al. 2013) with slight modifications (Pragasam and Venkatesan 2020). Briefly, the rats were euthanized by CO2 asphyxiation and the hind limbs were collected in sterile phosphate buffered saline (PBS, pH 7.4). The femur and tibia were separated from the hind limbs under sterile conditions. The cartilage at the ends of the femur and tibia were harvested using sterile scalpels, washed in sterile PBS, digested in 0.15% collagenase-II for 4 h at 37 ºC, 5% CO2, followed by the addition of culture medium (Dulbecco’s Modified Eagle Medium/Ham’s F12 (1:1) (DMEM/F12) supplemented with 10% fetal bovine serum (FBS), P/S (penicillin (100 IU/ml) and streptomycin (100 IU/ml)). The digested cell suspension was then centrifuged at 300xg for 10 min using a Sigma 3-18KS centrifuge. The cell pellet was washed twice in culture medium and seeded in a T25 culture flask at a density of 5 × 103 cells/cm2. The culture medium was changed every 2 days and upon reaching confluency, the cells were trypsinized using 0.25% trypin-EDTA and sub-cultured subsequently. The cells at passage 2 were used for all the further experiments.
Isolation of rat bone marrow mesenchymal stem cells (BM-MSCs)
Post euthanization by CO2 asphyxiation, the femur bones were harvested from four-week-old female WNIN Wistar rats under aseptic conditions in sterile PBS containing antibiotics. The BM-MSCs were isolated according to an earlier published protocol (Madhira et al. 2012). Briefly, the femurs were cut open at the metaphyseal ends and the bone marrow was flushed out using a 2-ml syringe containing DMEM/F12 containing 10% FBS and P/S. The flushed out bone marrow was adequately dispensed to get a uniform cell suspension which was washed thrice at 1800 rpm for 10 min. The resulting cell pellet was resuspended in the cell culture medium (DMEM/F12 containing 10% FBS and P/S) and seeded in T25 flasks at a seeding density of 5 × 103 cells/cm2. 48–72 h upon seeding, spindle-shaped adherent cells were observed and the non-adherent cells were removed during subsequent media change which was done every 2 days. The adherent cells formed a monolayer and upon reaching confluency, the cells were trypsinized using 0.25% trypsin–EDTA. The BM-MSCs at passage 3 to 5 were used for the subsequent experiments.
Characterization of rat BM-MSCs
BM-MSCs were characterized for their multi-lineage differentiation potential and phenotypic markers. The BM-MSCs were differentiated to chondrogenic, osteogenic and adipogenic lineages using commercially available kits (Gibco, Life Technologies, USA) as per the manufacturer’s instructions. For chondrogenic and osteogenic differentiation, BM-MSCs (P3) were grown in 35-mm culture dishes in DMEM/F12 containing 10% FBS and P/S. When the cells reached 80% confluency, the culture medium was replaced with the chondrogenic and osteogenic differentiation media (basal medium with supplement) for 14 days and 21 days, respectively, with the medium being changed every 2 days. At the end of 14 days, the BM-MSCs differentiating into the chondrogenic lineage were washed with PBS, fixed with 4% paraformaldehyde and stained with 1% Alcian Blue solution prepared in 0.1 N HCL for 30 min. The cells were rinsed with 0.1 N HCl, distilled water was added to neutralize the acidity, visualized under a light microscope and the images were captured. At the end of 21 days, the BM-MSCs differentiating into the osteogenic lineage were rinsed with PBS, fixed with 4% paraformaldehyde and stained with 2% Alizarin Red solution for 2–3 min. The cells were rinsed with distilled water, visualized under a light microscope and the images were captured. For adipogenic differentiation, monolayer cultures of BM-MSCs were grown in culture medium in 35-mm dishes until 80% confluency and replaced with adipogenic differentiation medium for 10 days with the medium being changed every 2 days. At the end of 10 days, the cells were rinsed with DPBS and fixed with 4% paraformaldehyde. The cells were rinsed with PBS and stained with Oil-Red-O stain, washed with PBS, visualized under a light microscope and images were captured. The BM-MSCs were also characterized for their expression of MSC specific markers CD29, CD73, CD90 and CD106 by immunofluorescence. Briefly, the BM-MSCs (P4) grown on coverslips in six-well culture dishes were fixed with 4% paraformaldehyde, washed with PBS, permeabilized with 50% chilled methanol, serum-blocked with 4% horse serum and incubated overnight at 4 ºC with primary antibodies specific to CD29 (1:100, BD Biosciences), CD73 (1:100, BD Biosciences), CD90 (1:100, BD Biosciences) and CD106 (1:100, BD Biosciences). The cells were washed with PBS, incubated with a fluorescent labeled (Cy3) secondary antibody (1:200 dilution) (Jackson’s Laboratories, USA) for 1 h at room temperature, washed with PBS and mounted using DAPI (Vectashield, Vector Laboratories, USA). All images were captured using Leica Advanced Fluorescence software in a Leica TCS SP5 Confocal Microscope (Mannheim, Germany).
Preparation of MSC-CM or secretome
MSC-CM was obtained from the cultured rat BM-MSCs as per the published method (Kay et al. 2017). Briefly, the BM-MSCs were seeded in T75 flasks at a density of 1.5 × 106 cells/flask in DMEM/F12 containing 10% FBS and P/S. Upon reaching 80–90% confluency, the cells were washed with PBS and added with serum free DMEM/F12 and maintained at 37 ℃, 5% CO2. The flasks were incubated for 48 h after which the medium was removed and centrifuged at 1500 rpm for 5 min at 4 ℃ to remove any cell debris. The resulting supernatant was termed the MSC-CM and used for the subsequent experiments.
Cell viability assay
The effect of stigmasterol on cell viability in the isolated rat primary chondrocytes was measured using the MTT assay. The chondrocytes were seeded at a density of 5 × 103 cells/well in a 96-well plate. After allowing the cells to adhere for 24 h, the cells were treated with different concentrations of stigmasterol (0–100 μM) in culture medium. After 24 h of the treatment, the media were removed, and the cells were incubated with MTT solution (5 mg/ml) for 4 h at 37 °C. The supernatant was removed and the formazan crystals were dissolved by adding DMSO to the wells. The absorbance was measured at 570 nm using a microplate reader (BioTek, US). The number of viable cells in the treatment groups was expressed as a percentage of the number in the control group. The chondrocytes without any stigmasterol treatment (0 μM) were considered as the control group.
Experimental approach
The chondrocytes were grown in six-well plates at a seeding density of 2 × 105 cells/well and cultured in DMEM/F12 containing 10% FBS and P/S until confluency. The study comprised of the following five groups: (1) chondrocytes maintained in DMEM/F12 medium for 24 h (Control), (2) chondrocytes treated with IL-1β (10 ng/ml) for 24 h (IL-1β), (3) chondrocytes treated with IL-1β (10 ng/ml) + MSC-CM for 24 h (IL-1β + CM), (4) chondrocytes treated with IL-1β (10 ng/ml) + 50 μM stigmasterol in plain medium for 24 h (IL-1β + S), (5) chondrocytes treated with IL-1β (10 ng/ml) + MSC-CM + 50 μM stigmasterol for 24 h (IL-1β + CM + S). The final volume across the different groups was kept constant at 2 ml. All the experiments were carried out under identical conditions and the experiment was designed according to a previous study by Huang et al. (2018) with the treatments given for 24 h.
Immunofluorescence
At the end of the experimental period (24 h), the chondrocytes grown on coverslips (all five groups) were washed with PBS and fixed with 4% paraformaldehyde. The cells were rinsed with PBS again and permeabilized with 50% chilled methanol, serum-blocked with 4% horse serum and incubated overnight at 4 °C with primary antibodies specific to collagen II alpha 1 (COL2A1) (1:25; Developmental Studies Hybridoma Bank, IA USA), inducible nitric oxide synthase (iNOS) (1:100, Abcam, MA, USA), Matrix metalloproteinase (MMP-13) (1:100; Abcam, MA, USA) and interleukin-6 (IL-6) (1:100, Invitrogen, MA, USA). The cells were washed with PBS, incubated with a Cy-3-labeled secondary antibody (1:200 dilution) (Jackson Laboratories, USA) for 1 h at room temperature, washed with PBS and mounted using DAPI (Vectashield, Vector Laboratories, USA). All images were captured using Leica Advanced Fluorescence software in a Leica TCS SP5 Confocal Microscope (Mannheim, Germany). The fluorescence intensities were calculated as relative fluorescent units (RFU) using the LAF software and represented as RFU per unit area. Values are represented as mean ± SD from three independent experiments performed in duplicate.
Quantitative real-time polymerase chain reaction (qRT-PCR) analysis
qRT-PCR analysis was carried out to quantify the gene expression levels of OA-specific markers: MMP-3, MMP-13 and ADAMTS-5 in the treated chondrocytes. Total RNA was isolated from the chondrocytes cultured in six-well plates using TRIzol reagent according to the manufacturer’s instructions. First-strand complementary DNA (cDNA) was synthesized from 1 μg of total RNA using the OneScript cDNA Synthesis kit (Applied Biological Materials, Canada). qRT-PCR was performed using a TB Green Premix Ex Taq II real-time PCR kit (Takara Bio, CA, USA) employing an Applied Biosystems StepOnePlus real-time PCR system (ThermoFisher Scientific, MA, USA). The level of target mRNA was normalized to the level of GAPDH and compared with control. Data were analyzed using the 2−ΔΔCT method. The primer sequences of the target genes used for the qRT-PCR were designed using the NCBI Primer-Blast tool and are listed as follows: MMP-3 (F): 5′- AATCCCCTGATGTCCTCGTGGTA-3′, (R): 5′- GGTCCTGAGAGATTTTCGCCAA-3′; MMP-13 (F): 5′-TCGCATTGTGAGAGTCATGCCAACA-3′, (R): 5′-TGTGGTT -CCAGCCACGCATAGTCA-3′; ADAMTS-5 (F): 5′-GGGGTCAGTGTTCTCGCTCTTG-3′, (R): 5′-GCCGTTAGGTGGGCAGGGTAT-3′.
Western Blot analysis
The total protein was extracted from the chondrocytes cultured in six-well plates using ice-cold radio immunoprecipitation assay (RIPA) lysis buffer containing protease inhibitors. The lysates were sonicated, kept on ice for 10 min followed by centrifugation at 12,000 rpm for 15 min at 4 °C. The protein concentration in the supernatants was measured using the bicinchoninic acid (BCA) protein assay kit (G-Biosciences, MO, USA). Equal amounts of protein (40 μg) were separated by sodium dodecylsulfate-polyacrylamide gel electrophoresis (SDS-PAGE) and transferred to a polyvinylidene difluoride membrane (Bio-Rad, USA). After blocking with 5% nonfat milk for 2 h, the membranes were incubated with the primary antibodies against NF-κB p65 (1:1000, Cell Signaling Technology), phospho-NF-κB p65 (1:1000, Cell Signaling Technology), IκBα (1:1000, Novus Biologicals), phospho-IκBα (1:1000, Novus Biologicals) and β-actin (1:1000, Cell Signaling Technology) overnight at 4 ℃ with gentle rocking. The membranes were washed with TBST and incubated with the corresponding horseradish peroxidase (HRP)-conjugated secondary antibodies (1:10,000, Southern Biotech) at room temperature for 1 h. After washing with TBST, the membranes were visualized with an enhanced chemiluminescence reagent (G-Biosciences, MO, USA) and the images were captured using an iBrightFL1500 Imaging System (ThermoFisher Scientific, USA).
Statistical analysis
The values given represent average of three independent experiments, carried out in duplicates. All data have been expressed as mean ± standard deviation (SD). Significant difference between the groups was measured using one-way analysis of variance (ANOVA) followed by Dunnett’s test using GraphPad Prism 8.0.2 software. p < 0.05 implied significance.
Results
Effect of stigmasterol on cell viability
The rat primary articular chondrocytes were isolated and cultured in DMEM/F12 containing 10% FBS and P/S. The cultured chondrocytes were identified by their typical polygonal shape when viewed under a bright field inverted microscope (Fig. 1A). The effect of stigmasterol on the cell viability/cytotoxicity of the cultured rat articular chondrocytes was evaluated by the MTT assay. The cells were treated with stigmasterol at varying concentrations ranging from 0 to 100 µM for 24 h. There was no significant cytotoxicity in the chondrocytes upon treatment with stigmasterol across all the tested concentrations (Fig. 1B). Stigmasterol at a concentration of 50 μM was used for all the further experiments of the study. This dosage was selected also considering a previous study by Gabay et al. (2010) Fig. 1.
Characterization of rat BM-MSCs
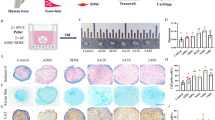
The cultured rat BM-MSCs were identified by their physical adherence to the plastic cell culture dish and their typical fibroblast-like spindle shaped morphology when viewed under the microscope (Fig. 2A). The ability of the isolated BM-MSCs to differentiate into the chondrogenic, osteogenic and adipogenic lineages was assessed using commercially available kits following the manufacturer’s instructions. The BM-MSCs were subjected to chondrogenic differentiation by maintaining the cells in chondrogenic differentiation medium for 14 days which was identified by the Alcian Blue staining for proteoglycans (Fig. 2B). The osteogenic differentiation potential of the BM-MSCs was carried out by maintaining the BM-MSCs in the osteogenic differentiation medium for 21 days and was confirmed by the Alizarin Red staining for calcium phosphate deposits (Fig. 2C). The adipogenic differentiation potential of the BM-MSCs was performed by maintaining the BM-MSCs in the adipogenic differentiation medium for 10 days and confirmed by the Oil-Red-O staining of the lipid droplets (Fig. 2D). The BM-MSCs (P4) grown on coverslips were paraformaldehyde fixed and processed for the expression of MSC-specific markers assessed by immunofluorescence. The BM-MSCs stained positive for the expression of MSC-specific markers CD29 (Fig. 2E), CD73 (Fig. 2F). CD90 (Fig. 2G) and CD106 (Fig. 2H) as confirmed by immunofluorescence using a Leica SP5 confocal laser scanning microscope using the LAS software Fig. 2.
Characterization of rat bone-marrow mesenchymal stem cells (BM-MSCs). A Bright field micrograph of the rat BM-MSCs. B Alcian Blue Staining for chondrogenic differentiation of BM-MSCs. C Alizarin Red staining for osteogenic differentiation of BM-MSCs. D Oil-Red-O staining for adipogenic differentiation of BM-MSCs. E Immunofluorescence staining of BM-MSCs for the expression of CD29, F CD73, G CD90, and H CD106 by confocal microscopy
Effects of MSC-CM, stigmasterol, and combination of MSC-CM and stigmasterol on the expression of iNOS, IL-6, MMP-13 and COL2A1 in IL-1β stimulated rat chondrocytes by immunofluorescence
IL-β is the most critical pro-inflammatory cytokine implicated in OA pathogenesis which upregulates several inflammatory/catabolic mediators involved in cartilage degradation. The effects of MSC-CM and stigmasterol alone or in combination on the expression of key OA-related inflammatory markers such as iNOS (Fig. 3), IL-6 (Fig. 4) and MMP-13 (Fig. 5), and cartilage turnover marker COL2A1 (Fig. 6) in the rat chondrocytes upon were evaluated by immunofluorescence using confocal microscopy. The IL-1β stimulated chondrocytes showed a significant increase in the expression of iNOS, IL-6 and MMP-13 and a significant reduction in the expression of COL2A1 in the rat chondrocytes compared to the control. The IL-1β-stimulated chondrocytes treated with the MSC-CM (IL-1β + CM) or stigmasterol (IL-1β + S) alone resulted in a significant reduction in the expression of iNOS, IL-6 and MMP-13 and a significant increase in the expression of COL2A1 when compared to the IL-1β-treated groups. However, the combination treatment of MSC-CM and stigmasterol (IL-1β + CM + S) to IL-1β stimulated chondrocytes significantly reversed the levels of iNOS (Fig. 3), IL-6 (Fig. 4), MMP-13 (Fig. 5) and COL2A1 (Fig. 6) expression to near normal levels as comparable to the control group indicative of the beneficial effect of the combination therapy over the individual treatments Figs. 3, 4, 5 and 6.
A Immunofluorescence studies for iNOS expression in rat chondrocytes. MSC-CM, stigmasterol, and combination of MSC-CM and stigmasterol treatment reduced iNOS expression in IL-1β-stimulated rat chondrocytes. Combination of MSC-CM and stigmasterol treatment greatly reduced iNOS protein expression to near normal levels. B Quantitative fluorescence measurements for iNOS expression in the chondrocytes obtained from three independent experiments and values represented as mean ± SD. Significant differences between the groups defined as: **p < 0.01; ***p < 0.001 compared with control group; ##p < 0.01 compared with IL-1β group
A Immunofluorescence studies for IL-6 expression in rat chondrocytes. MSC-CM, stigmasterol, and combination of MSC-CM and stigmasterol treatment attenuated IL-6 expression in IL-1β stimulated rat chondrocytes. IL-6 protein expression was significantly reduced to near normal levels in chondrocytes treated with the combination of MSC-CM and stigmasterol. B Quantitative fluorescence measurements for IL-6 expression in the chondrocytes from three independent experiments and values represented as mean ± SD. Significant differences between the groups defined as: **p < 0.01; ***p < 0.001 compared with control group; ##p < 0.01 ###p < 0.001 compared with IL-1β group
A Immunofluorescence studies for MMP-13 expression in rat chondrocytes. MSC-CM, stigmasterol, and the combination of MSC-CM and stigmasterol treatment significantly attenuated MMP-13 expression in IL-1β-stimulated rat chondrocytes. MMP-13 expression was significantly reduced to near normal levels in chondrocytes treated with the combination of MSC-CM and stigmasterol. B Quantitative fluorescence measurements for MMP-13 expression in the chondrocytes from three independent experiments and values represented as mean ± SD. Significant differences between the groups defined as: **p < 0.01; ***p < 0.001 compared with control group; ###p < 0.001 compared with IL-1β group
A Immunofluorescence studies for COL2A1 expression in rat chondrocytes. MSC-CM, stigmasterol, and combination of MSC-CM and stigmasterol treatment significantly increased COL2A1 expression in IL-1β stimulated rat chondrocytes. The combination of MSC-CM and stigmasterol treatment significantly restored COL2A1 expression to near normal levels comparable to the control group. B Quantitative fluorescence measurements for COL2A1 expression in the chondrocytes from three independent experiments and values represented as mean ± SD. Significant differences between the groups defined as: **p < 0.01; ***p < 0.001 compared with control group; ###p < 0.001 compared with IL-1β group
Effects of MSC-CM, stigmasterol, and combination of MSC-CM and stigmasterol on mRNA expression levels of MMP-3, MMP-13 and ADAMTS-5 in IL-1β stimulated rat chondrocytes by qRT-PCR
The mRNA expression levels of MMP-3, MMP-13 and ADAMTS-5 genes in IL-β-stimulated rat chondrocytes treated with MSC-CM and/or stigmasterol were evaluated using qRT-PCR. As depicted in Fig. 7, IL-β stimulation in chondrocytes (IL-β group) resulted in a significant increase in the mRNA expression levels specific for MMP-3 (Fig. 7A), MMP-13 (Fig. 7B) and ADAMTS-5 (Fig. 7C). Treatments with either MSC-CM (IL-β + CM) or stigmasterol (IL-β + S) alone resulted in a significant reduction in the gene expression levels of MMP-3, MMP-13 and ADAMTS-5 compared to the IL-β group. Co-treatment of MSC-CM and stigmasterol (IL-1β + CM + S) also resulted in a significant reduction in the expression of MMP-3, MMP-13 and ADAMTS-5 genes when compared to the IL-β group. However, the combination therapy (IL-1β + CM + S) markedly reduced the gene expression of these OA-specific tissue degrading proteases to near normal levels as comparable to that of the control group underscoring the benefit of the combination therapy when compared to the individual treatments Fig. 7
Effects of MSC-CM, stigmasterol, and combination of MSC-CM and stigmasterol on the mRNA expression levels of A MMP-3, B MMP-13, and C ADAMTS-5 in IL-1β-stimulated chondrocytes. Values are expressed as mean ± SD with results obtained from three independent experiments performed in duplicate. Significant differences between the groups defined as: *p < 0.05 compared with control; #p < 0.05 compared with IL-1β group
Effects of MSC-CM, stigmasterol, and combination of MSC-CM and stigmasterol on the inhibition of IL-1β-mediated activation of NF-κB in rat chondrocytes by western blot analysis
IL-1β exerts its downstream catabolic/inflammatory effects chiefly mediated through the NF-κB signaling pathway. The effects of MSC-CM, stigmasterol, and the combination of MSC-CM and stigmasterol on the IL-1β-induced NF-κB activation in rat primary chondrocytes was evaluated using western blot analysis. As shown in Fig. 8, the results indicated that IL-1β treatment triggered NF-κB activation as seen by an increased expression of phosphorylated-p65 (Fig. 8B) and phosphorylated-IκBα (Fig. 8C). In the presence of MSC-CM (IL-1β + CM) or stigmasterol (IL-1β + S), the phosphorylation of both p65 (Fig. 8B) and IκBα (Fig. 8C) decreased significantly. Nonetheless, the results revealed that the inhibition of IL-1β-induced NF-κB activation was the greatest in combination therapy group (MSC-CM + stigmasterol) evidenced by the negligible levels of phosphorylation of both p65 and IκBα comparable to control levels. The effects of the treatments in inhibiting IL-1β-induced NF-κB activation was found to be as follows: (IL-1β + CM + S) > (IL-1β + CM) > (IL-1β + S) when compared to the IL-1β group Fig. 8.
A Western blot studies for the effects of MSC-CM, stigmasterol, and combination of MSC-CM and stigmasterol on the protein expression of p65, p-p65, IκBα and p-IκBα in IL-1β-stimulated chondrocytes. B Quantification analysis for the expression of p-p65. C Quantification analysis for the expression of p-IκBα. Values are expressed as mean ± SD with results obtained from three independent experiments performed in duplicate. Significant differences between the groups defined as *p < 0.05; **p < 0.01; ***p < 0.001 compared with control; ##p < 0.01; ###p < 0.001 compared with IL-1β group
Discussion
Chronic low-grade inflammation driven by pro-inflammatory mediators has been identified to have a pivotal role in propelling OA pathogenesis characterized by cartilage destruction, subchondral bone remodeling, pain, joint failure and deformity (Robinson et al. 2016). Apparently, therapeutic strategies targeting the inflammatory responses in OA could hold immense clinical value in treating OA (Conaghan et al. 2019; Pelletier et al. 2001; Philp et al. 2016). In the current study, we evaluated for the first time the beneficial effects of MSC-CM and stigmasterol alone and compared with a combination of MSC-CM with stigmasterol in negating the IL-1β-induced inflammatory responses in rat primary chondrocytes in-vitro.
Chondrocytes form the sole cellular components found in the cartilage tissue; they synthesize the extracellular matrix components and provide matrix turnover which are indispensable for maintaining the functional and structural integrity of the cartilage (Goldring and Marcu 2009). However, under OA, this dynamic balance between the cartilage matrix synthesis and degradation is disrupted by the induction of stress-induced inflammatory mediators. Notably, IL-1β exerts its detrimental effects on the chondrocytes by compromising the chondrocyte viability, inhibiting the anabolic processes critical to cartilage homeostasis including production of ECM components, impairing their fate of differentiation and dysregulating their functions to induce pro-inflammatory and pro-catabolic responses (Charlier et al. 2016). Hence IL-1β induction in chondrocytes has been employed as a conventional way to generate an OA model in-vitro (Li et al. 2019).
In our present study, we assessed the effects of IL-1β stimulation on the expression of inflammation-associated markers including iNOS, IL-6, and the cartilage turn-over markers COL2A1, MMP-3, MMP-13 and ADAMTS-5 in rat chondrocytes. The inducible nitric oxide synthase (iNOS) contributes to OA pathogenesis by increasing the production of nitric oxide which in turn inhibits the synthesis of collagen type II and proteoglycan (Sasaki et al. 1998). IL-6 is another key pro-inflammatory cytokine and a well-known player in amplifying OA by its inherent ability to work in synergy with IL-1β (Flannery et al. 2000) and through its role in transsignaling (Scheller et al. 2011). The cartilage matrix degrading enzymes including those that belong to the matrix metalloproteinase (MMP) family and the disintegrin and metalloproteinase with thrombospondin type-1 motifs (ADAMTS) family have been identified as potent diagnostic/therapeutic targets for early OA. Of the many MMPs involved in OA pathogenesis, MMP-13 has been identified as the central node in the cartilage degradation network in OA and is highly efficient in degrading collagen II, in addition to degrading proteoglycan, types IV and type IX collagen, osteonectin and perlecan in cartilage (Shiomi et al. 2010). MMP-3 also plays a crucial role in cartilage degradation capable of degrading a broad range of substrates including collagen types II, III, and IV, laminin, proteoglycans, and fibronectin, and also activates other MMPs including MMP-1, MMP-2, MMP-9 and MMP-13 (Tong et al. 2017). ADAMTS-5 is the primary aggrecanase responsible for aggrecan degradation in OA with evidence demonstrating for ADAMTS-5 knockout mice to exhibit significant resistance to cartilage erosion in a surgical model of OA (Glasson et al. 2005; Stanton et al. 2005). In our current study, we found that IL-1β stimulation significantly up-regulated the protein expression of iNOS, IL-6, MMP-13 with a concomitant down-regulated protein expression of COL2A1 in the rat chondrocytes. IL-1β treatment also significantly increased the gene expression levels of MMP-3 and ADAMTS-5 in the chondrocytes. These altered gene/protein expression levels of key OA-specific markers were significantly reversed by the MSC-CM/stigmasterol individual treatments. However, the combination therapy of MSC-CM and stigmasterol demonstrated a remarkably better anti-inflammatory and anti-catabolic effect by significantly restoring the levels of these OA-specific markers (iNOS, IL-6, COL2A1, MMP-3, MMP-13 and ADAMTS-5) to near normal levels comparable to that of the control group accentuating the benefits of the combination therapy over the individual treatments.
In OA, the overexpression of pro-inflammatory and catabolic factors in response to inflammatory stimuli is regulated by a set of pro-inflammatory signaling pathways. Chiefly, the transcription factor nuclear-factor kappa B (NF-κB)-mediated signaling is a critical and master regulator orchestrating the expression of various genes involved in inflammation, immune response, adhesion, tissue degradation and apoptosis implicated in OA pathophysiology (Choi et al. 2019). In chondrocytes, the IL-1β-mediated production of the downstream inflammatory/catabolic mediators such as the iNOS, IL-6 and MMPs is essentially regulated by the NF-κB pathway (Chow and Chin 2020) and hence strategies interfering with the activation of the NF-κB pathway hold immense potential in curtailing OA. Under normal conditions, the p65 subunit of NF-κB is sequestered into the cytoplasm and kept blocked by the IκBα proteins. However, during inflammation, NF-κB is activated where IκBα proteins are phosphorylated, followed by the subsequent phoshphorylation and translocation of the NF-κB p65 subunit into the nucleus, where it binds to the promoter regions of the DNA and activates the transcription of target genes (Liu et al. 2017). In our present study, western blot studies revealed that IL-1β stimulation resulted in NF-κB activation which was evidenced by a significant increase in phosphorylation of p65 and IκBα. Our results also indicated that the combination therapy (MSC-CM + stigmasterol) was the most effective in negating the IL-1β induced-NF-κB activation demonstrated by the negligible phosphorylation of p65 and IκBα which was comparable to that of the control group. These results reiterate the superiority of the combination therapy over the individual treatments in inhibiting iNOS, IL-6, MMP-3, MMP-13, ADAMTS-5 and improved collagen-II synthesis which could apparently be attributed to the upstream suppression of NF-κB activation.
Studies by Gabay et al. (2010) had demonstrated for the anti-inflammatory effect of stigmasterol in inhibiting key pro-inflammatory and matrix degradation mediators involved in OA-induced cartilage degradation, partly by inhibiting the NF-κB pathway. In similar lines, Simental-Mendía et al. (2020) had reported for an anti-inflammatory effect by MSC-CM treatment in an explant culture of IL-1β-stimulated human cartilage, and the MSC-CM also inhibited the gene expression of IL-1β, MMP-13, ADAMTS-5 and decreasing glycosaminoglycan release. Another recent study by Chen et al. (2019) had shown the ability of bone marrow derived MSC-CM to alleviate OA in a rodent model surgically induced with OA by maintaining the extracellular matrix homeostasis in cartilage tissue in-vivo. The findings from our current study using stigmasterol or MSC-CM treatments in IL-1β-stimuated rat chondrocytes are in line with the evidences from these earlier published reports. However, it is noteworthy that the anti-inflammatory/anti-catabolic effects exhibited by the combination therapy (MSC-CM and stigmasterol) clearly shows potent promise(s) as compared to the individual treatments, underscoring for possible synergistic effect augmented by the combination treatments.
Substantiating these findings, we had recently reported (Pragasam et al. 2021) in-vivo that intra-articularly transplanted MSCs in combination with stigmasterol facilitated for significant cartilage repair and regeneration in a monosodium-iodoacetate-induced rat model of OA. We attribute the beneficial effects to the paracrine, autocrine and immunomodulatory effects of MSCs in syngergy with the anti-inflammatory and antioxidant functions of stigmasterol. Several studies have demonstrated the distinctive advantages of employing MSC-CM/secretome in regenerative research/tissue engineering (Vizoso et al. 2017). The MSC-CM offers an optimal platform for therapy in retaining all the bioactive factors, can be freeze-dried, packaged, and transported whilst avoiding the operational and logistic challenges observed with stem cells, in addition to its ability as cell-free system to enhance the shelf life (Pawitan 2014). Furthermore, there is greater potential to further enhance the MSC-CM by identifying their components such as anti-inflammatory factors, extracellular vesicles (EV)/exosomes which could be purified and employed in isolation or in combination with complementing agents to maximize the therapeutic response. Several studies have also demonstrated the efficacy as well as safety of MSC-CM in treating a broad spectrum of diseases administered through various routes including topical (Joseph et al. 2020), intra-dermal (Cho et al. 2010), subcutaneous (Zhou et al. 2020), intra-venous, intra-peritoneal (Hashemi et al. 2020), intra-nasal (Kojima et al. 2020), intra-muscular (Shabbir et al. 2009), intra-articular delivery (Chen et al. 2019) with no reports of adverse events in either pre-clinical or clinical trials (Montero-Vilchez et al. 2021). Thus, the MSC-CM represents an attractive therapeutic option to be used alone/in combination with agents with complementing mechanisms of action in treating OA.
Conclusion
Taken together, the findings of our study clearly demonstrate the advantage of employing a combination therapy of MSC-CM and stigmasterol over the individual treatments in mitigating the IL-1β-induced inflammatory response in a rat chondrocyte model of OA in-vitro. The combination therapy significantly suppressed the IL-1β-induced iNOS, IL-6, MMP-3, MMP-13 and ADAMTS-5 expression chiefly by inhibiting the NF-κB signaling pathway. The leads obtained from our previous and current studies have shown promise for the possible application and evaluation of this combination therapy in clinical settings at least in OA patients presenting with early OA-like changes.
References
Ahangar P, Mills SJ, Cowin AJ (2020) Mesenchymal stem cell secretome as an emerging cell-free alternative for improving wound repair. Int J Mol Sci. https://doi.org/10.3390/ijms21197038
Antwi AO, Obiri DD, Osafo N, Essel LB, Forkuo AD, Atobiga C (2018) Stigmasterol alleviates cutaneous allergic responses in rodents. Biomed Res Int. https://doi.org/10.1155/2018/3984068
Benavides-Castellanos MP, Garzón-Orjuela N, Linero I (2020) Effectiveness of mesenchymal stem cell-conditioned medium in bone regeneration in animal and human models: a systematic review and meta-analysis. Cell Regener (london, England) 9:5. https://doi.org/10.1186/s13619-020-00047-3
Charlier E, Relic B, Deroyer C, Malaise O, Neuville S, Collée J, Malaise MG, De Seny D (2016) Insights on molecular mechanisms of chondrocytes death in osteoarthritis. Int J Mol Sci 17:2146. https://doi.org/10.3390/ijms17122146
Chen L, Tredget EE, Wu PY, Wu Y (2008) Paracrine factors of mesenchymal stem cells recruit macrophages and endothelial lineage cells and enhance wound healing. PLoS ONE 3:e1886. https://doi.org/10.1371/journal.pone.0001886
Chen D, Shen J, Zhao W, Wang T, Han L, Hamilton JL, Im HJ (2017) Osteoarthritis: toward a comprehensive understanding of pathological mechanism. Bone Res 5:16044. https://doi.org/10.1038/boneres.2016.44
Chen W, Sun Y, Gu X, Hao Y, Liu X, Lin J, Chen J, Chen S (2019) Conditioned medium of mesenchymal stem cells delays osteoarthritis progression in a rat model by protecting subchondral bone, maintaining matrix homeostasis, and enhancing autophagy. J Tissue Eng Regen Med 13:1618–1628. https://doi.org/10.1002/term.2916
Chen WP, Yu C, Hu PF, Bao JP, Tang JL, Wu JD (2012) Stigmasterol blocks cartilage degradation in rabbit model of osteoarthritis. Acta Biochimica Polonica https://doi.org/10.18388/abp.2012_2088
Cho JW, Kang MC (2010) TGF-β1-treated ADSCs-CM promotes expression of type I collagen and MMP-1, migration of human skin fibroblasts, and wound healing in vitro and in vivo. Int J Mol Sci 26:901–906. https://doi.org/10.3892/ijmm_00000540
Choi MC, Jo J, Park J, Kang HK, Park Y (2019) NF-κB signaling pathways in osteoarthritic cartilage destruction. Cells. https://doi.org/10.3390/cells8070734
Chow YY, Chin K-Y (2020) The role of inflammation in the pathogenesis of osteoarthritis. Mediat Inflamm 2020:8293921–8293921. https://doi.org/10.1155/2020/8293921
Conaghan PG, Cook AD, Hamilton JA, Tak PP (2019) Therapeutic options for targeting inflammatory osteoarthritis pain. Nat Rev Rheumatol 15:355–363. https://doi.org/10.1038/s41584-019-0221-y
Cui A, Li H, Wang D, Zhong J, Chen Y, Lu H (2020) Global, regional prevalence, incidence and risk factors of knee osteoarthritis in population-based studies. E Clin Med. https://doi.org/10.1016/j.eclinm.2020.100587
Daheshia M, Yao JQ (2008) The interleukin 1beta pathway in the pathogenesis of osteoarthritis. J Rheumatol 35:2306–2312. https://doi.org/10.3899/jrheum.080346
Ding S-L, Pang Z-Y, Chen X-M, Li Z, Liu X-X, Zhai Q-L, Huang J-M, Ruan Z-Y (2020) Urolithin a attenuates IL-1β-induced inflammatory responses and cartilage degradation via inhibiting the MAPK/NF-κB signaling pathways in rat articular chondrocytes. J Inflamm 17:13. https://doi.org/10.1186/s12950-020-00242-8
El Moshy S, Radwan IA, Rady D, Abbass MMS, El-Rashidy AA, Sadek KM, Dörfer CE, Fawzy El-Sayed KM (2020) Dental stem cell-derived secretome/conditioned medium: the future for regenerative therapeutic applications. Stem Cells Int 2020:7593402. https://doi.org/10.1155/2020/7593402
Fan XL, Zhang Y, Li X, Fu QL (2020) Mechanisms underlying the protective effects of mesenchymal stem cell-based therapy. Cell Mol Life Sci CMLS 77:2771–2794. https://doi.org/10.1007/s00018-020-03454-6
Flannery CR, Little CB, Hughes CE, Curtis CL, Caterson B, Jones SA (2000) IL-6 and its soluble receptor augment aggrecanase-mediated proteoglycan catabolism in articular cartilage. Matrix Biol J Int Soc Matrix Biol 19:549–553. https://doi.org/10.1016/S0945-053X(00)00111-6
Gabay O, Sanchez C, Salvat C, Chevy F, Breton M, Nourissat G, Wolf C, Jacques C, Berenbaum F (2010) Stigmasterol: a phytosterol with potential anti-osteoarthritic properties. Osteoarthr Cartil 18:106–116. https://doi.org/10.1016/j.joca.2009.08.019
García MD, Sáenz MT, Gómez MA, Fernández MA (1999) Topical antiinflammatory activity of phytosterols isolated from Eryngium foetidum on chronic and acute inflammation models. Phytother Res PTR 13:78–80. https://doi.org/10.1002/(SICI)1099-1573(199902)13:1%3c78::AID-PTR384%3e3.0.CO;2-F
Ghosh T, Maity TK, Singh J (2011) Evaluation of antitumor activity of stigmasterol, a constituent isolated from Bacopa monnieri Linn aerial parts against Ehrlich Ascites Carcinoma in mice. Orient Pharm Exp Med 11:41–49. https://doi.org/10.1007/s13596-011-0001-y
Glasson SS, Askew R, Sheppard B, Carito B, Blanchet T, Ma H-L, Flannery CR, Peluso D, Kanki K, Yang Z, Majumdar MK, Morris EA (2005) Deletion of active ADAMTS5 prevents cartilage degradation in a murine model of osteoarthritis. Nature 434:644–648. https://doi.org/10.1038/nature03369
Goldring MB, Marcu KB (2009) Cartilage homeostasis in health and rheumatic diseases. Arthr Res Ther 11:224. https://doi.org/10.1186/ar2592
González-González A, García-Sánchez D, Dotta M, Rodríguez-Rey JC, Pérez-Campo FM (2020) Mesenchymal stem cells secretome: The cornerstone of cell-free regenerative medicine. World J Stem Cells 12:1529–1552. https://doi.org/10.4252/wjsc.v12.i12.1529
Haleagrahara N, Hodgson K, Miranda-Hernandez S, Hughes S, Kulur AB, Ketheesan N (2018) Flavonoid quercetin–methotrexate combination inhibits inflammatory mediators and matrix metalloproteinase expression, providing protection to joints in collagen-induced arthritis. Inflammopharmacology 26:1219–1232. https://doi.org/10.1007/s10787-018-0464-2
Haque MN, Hannan MA, Dash R, Choi SM, Moon IS (2021) The potential LXRβ agonist stigmasterol protects against hypoxia/reoxygenation injury by modulating mitophagy in primary hippocampal neurons. Phytomedicine 81:153415. https://doi.org/10.1016/j.phymed.2020.153415
Harrell CR, Fellabaum C, Jovicic N, Djonov V, Arsenijevic N, Volarevic V (2019) Molecular mechanisms responsible for therapeutic potential of mesenchymal stem cell-derived secretome. Cells. https://doi.org/10.3390/cells8050467
Hashemi SM, Hassan ZM, Hossein-Khannazer N, Pourfathollah AA, Soudi S (2020) Investigating the route of administration and efficacy of adipose tissue-derived mesenchymal stem cells and conditioned medium in type 1 diabetic mice. Inflammopharmacology 28:585–601. https://doi.org/10.1007/s10787-019-00661-x
Huang X, Xi Y, Pan Q, Mao Z, Zhang R, Ma X, You H (2018) Caffeic acid protects against IL-1β-induced inflammatory responses and cartilage degradation in articular chondrocytes. Biomed Pharmacother 107:433–439. https://doi.org/10.1016/j.biopha.2018.07.161
Jenei-Lanzl Z, Meurer A, Zaucke F (2019) Interleukin-1β signaling in osteoarthritis – chondrocytes in focus. Cell Signal 53:212–223. https://doi.org/10.1016/j.cellsig.2018.10.005
Jo CH, Lee YG, Shin WH, Kim H, Chai JW, Jeong EC, Kim JE, Shim H, Shin JS, Shin IS, Ra JC, Oh S, Yoon KS (2014) Intra-articular injection of mesenchymal stem cells for the treatment of osteoarthritis of the knee: a proof-of-concept clinical trial. Stem Cells (dayton, Ohio) 32:1254–1266. https://doi.org/10.1177/0363546517716641
Joseph A, Baiju I, Bhat IA, Pandey S, Bharti M, Verma M, Pratap Singh A, Ansari MM, Chandra V, Saikumar G, Amarpal, and G. Taru Sharma. (2020) Mesenchymal stem cell-conditioned media: A novel alternative of stem cell therapy for quality wound healing. J Cell Physiol 235:5555–5569. https://doi.org/10.1002/jcp.29486
Kangari P, Talaei-Khozani T, Razeghian-Jahromi I, Razmkhah M (2020) Mesenchymal stem cells: amazing remedies for bone and cartilage defects. Stem Cell Res Ther 11:492. https://doi.org/10.1186/s13287-020-02001-1
Kaur S, Bijjem KRV, Sharma PL (2011) Anti-inflammatory and antihyperalgesic effects of the combination of ibuprofen and hemin in adjuvant-induced arthritis in the Wistar rat. Inflammopharmacology 19:265. https://doi.org/10.1007/s10787-011-0090-8
Kay AG, Long G, Tyler G, Stefan A, Broadfoot SJ, Piccinini AM, Middleton J, Kehoe O (2017) Mesenchymal stem cell-conditioned medium reduces disease severity and immune responses in inflammatory arthritis. Sci Rep 7:18019. https://doi.org/10.1038/s41598-017-18144-w
Kim WS, Park BS, Kim HK, Park JS, Kim KJ, Choi JS, Chung SJ, Kim DD, Sung JH (2008) Evidence supporting antioxidant action of adipose-derived stem cells: protection of human dermal fibroblasts from oxidative stress. J Dermatol Sci 49:133–142. https://doi.org/10.1016/j.jdermsci.2007.08.004
Kobayashi M, Squires GR, Mousa A, Tanzer M, Zukor DJ, Antoniou J, Feige U, Poole AR (2005) Role of interleukin-1 and tumor necrosis factor α in matrix degradation of human osteoarthritic cartilage. Arthr Rheum 52:128–135. https://doi.org/10.1002/art.20776
Kojima K, Kawahata I, Izumi H, Yoshihara S-I, Oki K (2020) Intranasal administration of conditioned medium from cultured mesenchymal stem cells improves cognitive impairment in olfactory bulbectomized mice. Adv Alzheimer’s Dis 9:47. https://doi.org/10.4236/aad.2020.93004
Lee WS, Kim HJ, Kim KI, Kim GB, Jin W (2019a) Intra-articular injection of autologous adipose tissue-derived mesenchymal stem cells for the treatment of knee osteoarthritis: a phase IIb, randomized, placebo-controlled clinical trial. Stem Cells Transl Med 8:504–511. https://doi.org/10.1002/sctm.18-0122
Lee YS, Lee SY, Park SY, Lee SW, Hong KW, Kim CD (2019b) Cilostazol add-on therapy for celecoxib synergistically inhibits proinflammatory cytokines by activating IL-10 and SOCS3 in the synovial fibroblasts of patients with rheumatoid arthritis. Inflammopharmacology 27:1205–1216. https://doi.org/10.1007/s10787-019-00605-5
Li X, He P, Hou Y, Chen S, Xiao Z, Zhan J, Luo D, Gu M, Lin D (2019) Berberine inhibits the interleukin-1 beta-induced inflammatory response via MAPK downregulation in rat articular chondrocytes. Drug Dev Res 80:637–645. https://doi.org/10.1002/ddr.21541
Liu CC, Zhang Y, Dai BL, Ma YJ, Zhang Q, Wang Y, Yang H (2017) Chlorogenic acid prevents inflammatory responses in IL-1β-stimulated human SW-1353 chondrocytes, a model for osteoarthritis. Mol Med Rep 16:1369–1375. https://doi.org/10.3892/mmr.2017.6698
Madhira SL, Challa SS, Chalasani M, Nappanveethl G, Bhonde RR, Ajumeera R, Venkatesan V (2012) Promise(s) of mesenchymal stem cells as an in vitro model system to depict pre-diabetic/diabetic milieu in WNIN/GR-ob mutant rats. PLoS ONE 7:e48061. https://doi.org/10.1371/journal.pone.0048061
Montero-Vilchez T, Sierra-Sánchez Á, Sanchez-Diaz M, Quiñones-Vico MI, Sanabria-de-la-Torre R, Martinez-Lopez A, Arias-Santiago S (2021) Mesenchymal stromal cell-conditioned medium for skin diseases: a systematic review. Front Cell Develop Biol 9:1877. https://doi.org/10.3389/fcell.2021.654210
Oseni AO, Butler PE, Seifalian AM (2013) Optimization of chondrocyte isolation and characterization for large-scale cartilage tissue engineering. J Surg Res 181:41–48. https://doi.org/10.1016/j.joca.2013.03.018
Panda S, Jafri M, Kar A, Meheta BK (2009) Thyroid inhibitory, antiperoxidative and hypoglycemic effects of stigmasterol isolated from Butea monosperma. Fitoterapia 80:123–126. https://doi.org/10.1016/j.fitote.2008.12.002
Pawitan JA (2014) Prospect of Stem Cell Conditioned Medium in Regenerative Medicine. Biomed Res Int 2014:965849. https://doi.org/10.1155/2014/965849
Pelletier J-P, Martel-Pelletier J, Abramson SB (2001) Osteoarthritis, an inflammatory disease: Potential implication for the selection of new therapeutic targets. Arthr Rheum 44:1237–1247. https://doi.org/10.1002/1529-0131(200106)44:6%3c1237::AID-ART214%3e3.0.CO;2-F
Philp AM, Davis ET, Jones SW (2016) Developing anti-inflammatory therapeutics for patients with osteoarthritis. Rheumatology 56:869–881. https://doi.org/10.1093/rheumatology/kew278
Pragasam SSJ, Kotikalapudi N, Venkatesan V (2021) A novel therapeutic combination of mesenchymal stem cells and stigmasterol to attenuate osteoarthritis in rodent model system-a proof of concept study. Stem Cell Investig 8:5. https://doi.org/10.21037/sci-2020-048
Pragasam SSJ, Venkatesan V (2020) Metabolic syndrome predisposes to osteoarthritis: lessons from model system. Cartilage. https://doi.org/10.1177/1947603520980161
Ramu R, Shirahatti PS, Nayakavadi S, V. R, F. Zameer, B.L. Dhananjaya, and N. Prasad Mn. (2016) The effect of a plant extract enriched in stigmasterol and β-sitosterol on glycaemic status and glucose metabolism in alloxan-induced diabetic rats. Food Funct 7:3999–4011. https://doi.org/10.1039/C6FO00343E
Robinson WH, Lepus CM, Wang Q, Raghu H, Mao R, Lindstrom TM, Sokolove J (2016) Low-grade inflammation as a key mediator of the pathogenesis of osteoarthritis. Nat Rev Rheumatol 12:580–592. https://doi.org/10.1038/nrrheum.2016.136
Sagaradze G, Grigorieva O, Nimiritsky P, Basalova N, Kalinina N, Akopyan Z, Efimenko A (2019) Conditioned medium from human mesenchymal stromal cells: towards the clinical translation. Int J Mol Sci 20:1656. https://doi.org/10.3390/ijms20071656
Sasaki K, Hattori T, Fujisawa T, Takahashi K, Inoue H, Takigawa M (1998) Nitric oxide mediates interleukin-1-induced gene expression of matrix metalloproteinases and basic fibroblast growth factor in cultured rabbit articular chondrocytes. J Biochem 123:431–439. https://doi.org/10.1210/endo.137.9.8756539
Satué M, Schüler C, Ginner N, Erben RG (2019) Intra-articularly injected mesenchymal stem cells promote cartilage regeneration, but do not permanently engraft in distant organs. Sci Rep 9:10153. https://doi.org/10.1038/s41598-019-46554-5
Scheller J, Chalaris A, Schmidt-Arras D, Rose-John S (2011) The pro- and anti-inflammatory properties of the cytokine interleukin-6. Biochem Biophys Acta 1813:878–888. https://doi.org/10.1016/j.bbamcr.2011.01.034
Shabbir A, Zisa D, Suzuki G, Lee T (2009) Heart failure therapy mediated by the trophic activities of bone marrow mesenchymal stem cells: A noninvasive therapeutic regimen. Ham H Physion Heart Circul Physiol 296:H1888-1897. https://doi.org/10.1152/ajpheart.00186.2009
Shiomi T, Lemaître V, D’Armiento J, Okada Y (2010) Matrix metalloproteinases, a disintegrin and metalloproteinases, and a disintegrin and metalloproteinases with thrombospondin motifs in non-neoplastic diseases. Pathol Int 60:477–496. https://doi.org/10.1111/j.1440-1827.2010.02547.x
Simental-Mendía M, Lozano-Sepúlveda SA, Pérez-Silos V, Fuentes-Mera L, Martínez-Rodríguez HG, Acosta-Olivo CA, Peña-Martínez VM, Vilchez-Cavazos F (2020) Anti-inflammatory and anti-catabolic effect of non-animal stabilized hyaluronic acid and mesenchymal stem cell-conditioned medium in an osteoarthritis coculture model. Mol Med Rep 21:2243–2250. https://doi.org/10.3892/mmr.2020.11004
Sofi MS, Sateesh MK, Bashir M, Ganie MA, Nabi S (2018) Chemopreventive and anti-breast cancer activity of compounds isolated from leaves of Abrus precatorius L. 3 Biotech 8:371. https://doi.org/10.1007/s13205-018-1395-8
Song Y, Du H, Dai C, Zhang L, Li S, Hunter DJ, Lu L, Bao C (2018) Human adipose-derived mesenchymal stem cells for osteoarthritis: a pilot study with long-term follow-up and repeated injections. Regen Med 13:295–307. https://doi.org/10.2217/rme-2017-0152
Stanton H, Rogerson FM, East CJ, Golub SB, Lawlor KE, Meeker CT, Little CB, Last K, Farmer PJ, Campbell IK, Fourie AM, Fosang AJ (2005) ADAMTS5 is the major aggrecanase in mouse cartilage in vivo and in vitro. Nature 434:648–652. https://doi.org/10.1038/nature03417
Tong Z, Liu Y, Chen B, Yan L, Hao D (2017) Association between MMP3 and TIMP3 polymorphisms and risk of osteoarthritis. Oncotarget 8: 83563–83569 https://doi.org/10.18632/oncotarget.18745
Usha PR, Naidu MUR (2004) Randomised, double-blind, parallel, placebo-controlled study of oral glucosamine, methylsulfonylmethane and their combination in osteoarthritis. Clin Drug Investig 24:353–363. https://doi.org/10.2165/00044011-200424060-00005
van der Kraan PM, van den Berg WB (2012) Chondrocyte hypertrophy and osteoarthritis: role in initiation and progression of cartilage degeneration? Osteoarthr Cartil 20:223–232. https://doi.org/10.1016/j.joca.2011.12.003
Vizoso FJ, Eiro N, Cid S, Schneider J, Perez-Fernandez R (2017) Mesenchymal stem cell secretome: toward cell-free therapeutic strategies in regenerative medicine. Int J Mol Sci 18:1852. https://doi.org/10.3390/ijms18091852
Walker CIB, Oliveira SM, Tonello R, Rossato MF, da Silva Brum E, Ferreira J, Trevisan G (2017) Anti-nociceptive effect of stigmasterol in mouse models of acute and chronic pain. Naunyn Schmiedebergs Arch Pharmacol 390:1163–1172. https://doi.org/10.1007/s00210-017-1416-x
Walter MN, Wright KT, Fuller HR, MacNeil S, Johnson WE (2010) Mesenchymal stem cell-conditioned medium accelerates skin wound healing: an in vitro study of fibroblast and keratinocyte scratch assays. Exp Cell Res 316:1271–1281. https://doi.org/10.1016/j.yexcr.2010.02.026
Xing D, Wu J, Wang B, Liu W, Liu W, Zhao Y, Wang L, Li JJ, Liu A, Zhou Q, Hao J, Lin J (2020) Intra-articular delivery of umbilical cord-derived mesenchymal stem cells temporarily retard the progression of osteoarthritis in a rat model. Int J Rheum Dis 23:778–787. https://doi.org/10.1111/1756-185X.13834
Yadav M, Parle M, Jindal DK, Dhingra S (2018) Protective effects of stigmasterol against ketamine-induced psychotic symptoms: Possible behavioral, biochemical and histopathological changes in mice. Pharmacol Rep 70:591–599. https://doi.org/10.1016/j.pharep.2018.01.001
Yu W, Xu P, Huang G, Liu L (2018) Clinical therapy of hyaluronic acid combined with platelet-rich plasma for the treatment of knee osteoarthritis. Exp Ther Med 16:2119–2125. https://doi.org/10.3892/etm.2018.6412
Zhou BR, Xu Y, Guo SL, Xu Y, Wang Y, Zhu F, Permatasari F, Wu D, Yin ZQ, Luo D (2013) The effect of conditioned media of adipose-derived stem cells on wound healing after ablative fractional carbon dioxide laser resurfacing. Biomed Res Int 2013:519126. https://doi.org/10.1155/2013/519126
Zhou H, Li X, Yin Y, He X-T, An Y, Tian B-M, Hong Y-L, Wu L-A, Chen F-M (2020) The proangiogenic effects of extracellular vesicles secreted by dental pulp stem cells derived from periodontally compromised teeth. Stem Cell Res Ther 11:110. https://doi.org/10.1186/s13287-020-01614-w
Acknowledgements
This study was supported by grants from Indian Council of Medical Research, New Delhi (Grant No. 3/1/3/PDF(14)/2016-HRD – Postdoctoral Research Fellowship Award to SJPS and Grant No. 35/5/2019-NANO/BMS). The authors also thank the Director, National Institute of Nutrition, Hyderabad and the Animal Facility, NIN for all the support extended for the conduct of the study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there is no conflict of interest.
Ethical approval
The animal studies were reviewed and approved by the Institutional Animal Ethical Committee, National Institute of Nutrition (NIN), Hyderabad (P29F/III-IAEC/NIN/12/2016/SSJ/WNIN(CG)-6F/WNIN-Gr-Ob-42F) and carried out in accordance with the regulations and guidelines of the Committee for the Purpose of Control and Supervision of Experiments on Animals (CPCSEA).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sampath, S.J.P., Rath, S.N., Kotikalapudi, N. et al. Beneficial effects of secretome derived from mesenchymal stem cells with stigmasterol to negate IL-1β-induced inflammation in-vitro using rat chondrocytes—OA management. Inflammopharmacol 29, 1701–1717 (2021). https://doi.org/10.1007/s10787-021-00874-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10787-021-00874-z