Abstract
Propofol is a widely used intravenous anesthetic. The aim of this study was to investigate the roles of nuclear factor erythroid-2-related factor 2 (Nrf2) and NADPH oxidase (NOX) in propofol protection in inflammatory conditions induced by lipopolysaccharide (LPS). Human alveolar epithelial cells (A549 cell line) were incubated with propofol (10, 25, and 50 μmol/L) for 1 h and then treated with LPS (100 ng/mL) for 24 h. Results indicated that propofol not only attenuated LPS-induced expression of iNOS, NOX, and COX2, but decreased the production of ROS, NO, and PGE2 as well. Propofol also increased the GSH levels and the mRNA and protein levels of Nrf2. Notably, Nrf2 siRNA and the inhibitors of COX-2 and NOX attenuated the inhibition of propofol on ROS production. In conclusion, propofol reduced LPS-induced ROS production via inhibition of inflammatory factors and enhancement of Nrf2-related antioxidant defense, providing its cytoprotective evidence under inflammatory conditions.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
INTRODUCTION
Septic shock is a life-threatening illness and multiple organ failure/dysfunction caused by infection with gram-negative bacteria [1]. Acute respiratory distress syndrome (ARDS), the most severe form of acute lung injury (ALI), is a common clinical syndrome in patients with sepsis or endotoxemia [2]. During sepsis, a heightened tissue level of superoxide anion and reactive oxygen species (ROS) result in oxidative stress. It mediates the reduced vasoconstriction, impairs bronchodilation, and causes endothelial dysfunction in endotoxemia [3]. In the cardiovascular system, the major sources of ROS generated are the NADPH oxidase (NOX) family of enzymes that produces ROS as their primary function [4, 5]. Among NOX family, the prototype NADPH oxidase is NOX2 and is also known as gp91phox.
Propofol (2,6-diisopropylphenol) is a widely used intravenous anesthetic agent. In addition to being the anesthetic drug of choice for induction and maintenance of anesthesia, it can also be used for sedative purposes in the intensive care unit (ICU). In high-risk patients, the opportunity for lung protection offered by the anti-oxidative property of propofol is absent in volatile anaesthetics [6, 7]. Propofol decreases oxidative stress-induced lipid peroxidation by scavenging free radicals and peroxynitrite and confers antioxidant activity [8]. In both in vivo and in vitro, the biosynthesis of iNOS and NO can be suppressed by propofol. It also can inhibit the generation of inflammatory mediators and decrease cytokine and chemokine production [9, 10]. However, the exact molecular mechanisms of propofol’s anti-inflammatory and anti-oxidant properties for lung protection remain unclear.
In addition to macrophages, a key defense agent, other cells in the lungs such as alveolar epithelial cells (AEC) have also played important roles against mycobacterial infection [11]. AEC, the lining cell of the pulmonary airways and alveoli, has a very rich number. A pathogen that encounters AEC has much greater chance than encountering a macrophage because of the location of these epithelial cells during the initial steps of infection. A number of chemokines, cytokines, and antimicrobial molecules can also be released by AEC upon infection [12]. Besides, the injury of the pulmonary alveolar–capillary membrane is the major pathophysiologic feature of ALI/ARDS [13]. In sepsis, the injury of pulmonary microvascular endothelial cell and barrier dysfunction can lead to neutrophils penetrating into the pulmonary interstitium and alveolar space and protein-rich edema fluid leakage [14]. Wang et al. have also reported that AEC attenuates PMEVC permeability under septic conditions [15]. Thus, AEC contributes to normal alveolar function, and its dysfunction often leads to poor outcomes of ALI/ARDS.
Nuclear factor erythroid-2-related factor 2 (Nrf2), a Cap‘n’collar–basic region leucine zipper (CNC–bZIP) transcription factor, has an essential protective role in the lungs against oxidative airway diseases due to its control of the expression of antioxidant response element-regulated antioxidant and cytoprotective genes [16]. Under basal conditions, Nrf2 is bound to the actin cytoskeleton by the Keap1 (Kelch-associated protein 1) protein and sequestered in the cytoplasm to facilitate its proteasomal degradation. When oxidative stimuli occur, Nrf2 migrates into the nucleus because of the dissociation of Nrf2 and Keap1, then enhances expression of target gene, such as glutathione (GSH) [17]. In the lungs, the major sources of Nrf2 are airway epithelium, type II alveolar epithelial cells, and resident macrophages [18]. A common methodology for the experimental studies of endotoxemia is lipopolysaccharide (LPS) administration [19]. Currently, there have been no studies to investigate the direct pharmacologic effect of propofol on the activation of the Nrf2-related antioxidant pathway, and the mechanisms of cytoprotective effects of propofol have not been clearly understood; therefore, the objectives of the current study are to use the human lung epithelial cell line A549 to explore the relevance between propofol and Nrf2 activation, as well as the mechanism of its cytoprotective effects on LPS-induced inflammation and oxidative stress.
MATERIALS AND METHODS
Chemicals
Propofol (2,6-di-isopropylphenol), dimethyl sulfoxide (DMSO), 2',7'-dichlo-rodihydro-fluorescein diacetate (H2DCF-DA), Triton X-100, NS-398, DPI, mouse anti-inducible NO synthase (iNOS), anti-β-actin, and other chemicals were purchased from Sigma-Aldrich (St Louis, Mo). Lipofectamine 2000 reagent, Trizol, Dulbecco’s modified Eagle’s medium (DMEM), and all culture medium supplements were obtained from GIBCO/BRL Life Technologies (Grand Island, NY, USA). All materials for sodium dodecyl sulfate (SDS)-polyacrylamide gel electrophoresis were obtained from Bio-Rad (Hercules, CA, USA). Nrf2 siRNA, rabbit anti-Nrf2, goat anti-Lamin B, and all horseradish peroxidase-conjugated secondary antibodies were from Santa Cruz Biotechnology (Santa Cruz, CA, USA). Mouse anti-cyclooxygenase 2 (COX-2) was obtained from Abcam (Cambridge Science Park, Cambridge, UK). Commercial kit for GSH and PGE2 measurement were purchased from Enzo Life Sciences (Farmingdale, NY, USA) and Cayman Chemical (Ann Arbor, Mich.), respectively. Mouse anti-NOX2 was obtained from BD Bioscience (San Jose, CA, USA). Plasma membrane protein Extraction kit and NE-PER™ nuclear/cytoplasmic extraction kit were from BioVision (BioVision, CA, USA).
Cell Culture and Propofol Treatment
Human type II lung epithelial cell line A549 was purchased from American Type Culture Collection) and maintained DMEM supplemented with 10 % fetal bovine serum, 4 mM glutamine, 100 U/mL penicillin, 100 μg/mL streptomycin, and 0.25 mg/mL amphotericin B. Cells were cultured with complete medium at 37 °C in 100 % humidified atmosphere of 5 % CO2 in air. Propofol was prepared by dissolving freshly in DMSO. Cells were treated with propofol alone for 24 h or pretreated with propofol (10–50 μmol/L) for 1 h before LPS (100 ng/mL) was added for 24 h.
Nitrite Measurement
Nitric oxide (NO) release was indicated as nitrite generation, which was measured by the Griess reagent (1 % sulfanilamide and 0.1 % N-1-naphthylethylenediamide in 5 % phosphoric acid). Fifty microliters of medium from each group was incubated with Griess reagent at room temperature for 10 min in the dark and the absorbance measured at 540 nm (OD540). The concentration was calculated from a sodium nitrite standard reference curve.
Measurement of Prostaglandin E2 Production
Prostaglandin E2 (PGE2) production was detected with an enzyme-immunoassay kit from Cayman Chemical, following the manufacturer’s instructions. Medium from each group was collected and the absorbance was measured at 405 nm (OD405).
Determination of Glutathione (GSH) Level
After propofol treatment, A549 cells were collected by centrifugation, and the pellets were suspended and deproteinated in 5 % metaphosphoric acid by brief sonication. Then, the supernatants after centrifugation were collected for total glutathione measurement. Following this, the reaction mix and GSH reductase supplied was added. After incubation, the absorbance was measured at 405 nm for 20 min at 1-min intervals [20]. The total amount of GSH was determined by means of a calibration curve and normalized to the protein concentration. Protein concentration was quantified using a Bio-Rad protein assay kit.
Determination of Reactive Oxygen Species (ROS) Production
The level of intracellular ROS production was determined by H2DCF-DA staining analyzed by flow cytometry [21]. After indicated treatments, A549 cells were loaded with 10 μM H2DCF-DA and incubated at 37 °C for 30 min. Cells were then detached and analyzed by a Coulter CyFlow® Cytometer (Partec, Germany) at excitation of 495 nm and emission of 520 nm.
Western Blot Analysis
Cells were lysed by lysis buffer and the supernatant collected after being centrifuged at 13,000×g for 30 min at 4 °C. Cell membranes and nuclear fraction were obtained by using a commercial kit according to the manufacturer’s instructions. Collected protein concentrations were determined by protein assay kit, and equal amounts of protein were used for SDS-polyacrylamide gel electrophoresis followed by PVDF membranes transference. Nonspecific binding was blocked with Tris-buffered saline and Tween 20 (50 mmol/L Tris–HCl, pH 7.6; 150 mmol/L NaCl; 0.1 % Tween 20) containing 5 % nonfat milk for 1 h at room temperature. The membranes were then each incubated with indicated primary antibodies overnight at 4 °C and then with appropriate dilutions of secondary antibodies for 1 h.
RNA Extraction and Quantitative of Messenger RNA
After indicated treatment, total RNA was isolated using Trizol reagent, and cDNA was synthesized using 1 μg of RNA and Reverse Transcription System kit (Promega, Madison, WI, USA) following the manufacturer’s guidance. Transcript levels were determined quantitatively using qPCR, which was performed on the ABI PRISM 7500 Sequence Detector System (Applied Biosystems, Foster City, CA, USA) using Power SYBR Green PCR Master Mix (Applied Biosystems). The respective primers used were as follows: Nrf2, 5′-GCGACGGAAAGAGTATGAC-3′ (forward) and 5′-GTTGGCAGATCCACTGG TTT-3′ (reverse); β-Actin, 5'-GCCAACACAGTGCTGTCT-3' (forward), 5'-AGGAGCAATGATCTTGATCTT-3' (reverse). The threshold cycle (Ct) was recorded as the mRNA level, and the amount of Nrf2 mRNA was normalized to the level of β-actin mRNA.
Transfection of Small Interfering RNA
The small interfering RNAs (siRNA) directed against human Nrf2 (Nrf2-siRNA) or nontargeting negative control siRNA (NC-siRNA) were purchased from Santa Cruz Biotechnology (Santa Cruz, CA, USA). A549 cells were transfected with 500 nM Nrf2-siRNA or NC-siRNA with Lipofectamine RNAi Max according to the manufacturer's protocol. After 48 h of transfection, cells were pretreated with propofol (50 μmol/L) for 1 h with or without LPS (100 ng/mL) treatment for 24 h.
Statistical Analysis
Data were expressed as means ± SEM. Analysis of variance was used to assess the statistical significance of the differences followed by Dunnett’s test for all paired comparisons. A value of p < 0.05 was considered statistically significant. Data were analyzed with the Statistical Package for Social Sciences (SPSS, Version 14.0, Chicago, IL, USA).
RESULTS
Propofol Attenuates LPS-Induced Inflammatory iNOS/NO and COX-2/PGE2 Pathways in A549 Cells
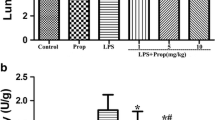
Because iNOS/NO and COX-2/PGE2 are important markers for inflammation resulting to lung injury, the anti-inflammatory effects of propofol were investigated in LPS-activated A549 lung epithelial cell. A549 cells were pretreated with propofol (10, 25, 50 μmol/L) for 1 h and further treated with LPS (100 ng/mL) for an additional 24 h. As shown in Fig. 1, LPS induced iNOS overexpression and markedly increased NO production in A549 cells. Pretreatment of propofol significantly decreased LPS-induced iNOS overexpression (Fig. 1a) and NO production (Fig. 1b). Similarly, propofol also attenuated LPS induced COX-2 overexpression (Fig. 1c) and PGE2 (Fig. 1d) production in A549 cells.
Inhibition of propofol on LPS-induced iNOS expression (a), NO production (b), COX-2 expression (c), and PGE2 production (d) in A549 cells. A549 cells were pretreated with propofol (10, 25, and 50 μmol/L) for 1 h before LPS (100 ng/mL) addition for 24 h. Control: no treatment group. Vehicle: 0.1 % DMSO-treated group. Bars represent the mean ± SEM from at least three independent experiments. ### P < 0.001 versus control. *P < 0.05, **P < 0.01, ***P < 0.001 versus LPS group.
Propofol Attenuates LPS-Induced ROS Production and Increases GSH Levels in A549 Cells Treated With or Without LPS
ROS-mediated oxidative damage is a major mechanism to cause inflammation-related cellular damage. Therefore, we examined the effects of propofol on LPS-induced ROS production in A549 cell. As shown in Fig. 2a, LPS significantly increased ROS production, which was attenuated by propofol treatment. Moreover, GSH is a cytoprotective protein that protects against oxidative stress and inflammation. Results indicated that propofol significantly increased GSH level in LPS-treated A549 cells (Fig. 2b), and it also directly increased GSH levels of A549 cells without treatment with LPS (Fig.2c).
Propofol attenuates LPS-induced ROS production (a)and increases GSH level (b) in A549 cells treated with (b) or without (c) LPS. A549 cells were pretreated with propofol for 1 h before LPS (100 ng/mL) addition for 24 h or treated with propofol (10, 25, and 50 μmol/L) alone for 24 h. Control: no treatment group. Vehicle: 0.1 % DMSO-treated group. Bars represent the mean ± SEM from at least three independent experiments. ### P < 0.001 versus control. *P < 0.05, **P < 0.01, ***P < 0.001 versus LPS group.
Propofol Attenuates LPS-Induced NADPH Oxidase Activation and in A549 Cells
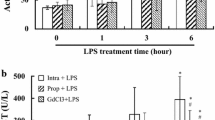
LPS-induced NADPH oxidase (NOX) activation is a major mechanism to cause oxidative stress- and inflammation-related cellular damage; therefore, we examined the effects of propofol on the activation of NOX2 on the cell membrane of A549 cell. Results indicated that LPS upregulated NOX2 expression on the cell membrane of A549 cell, and propofol treatment could attenuate LPS-induced NOX2 activation (Fig. 3a). Furthermore, NOX2 activation-induced ROS overproduction has been shown to be an important cause of oxidative stress-induced lung injury. To investigate the role of NOX2 in the antioxidant properties of propofol, a NOX inhibitor DPI was used. As shown in Fig. 3b, DPI pretreatment significantly attenuated the inhibitory effect of propofol on LPS-induced ROS production.
Propofol attenuates LPS-induced NOX2 expression (a) and DPI attenuates the inhibitory effect of propofol on LPS-induced ROS production (b). a A549 cells were pretreated with propofol (10, 25, and 50 μmol/L) for 1 h before addition of LPS (100 ng/mL) for 24 h. b Cells were treated with DPI (10 μmol/L, NOX inhibitor) for 1 h before propofol (50 μmol/L) treatment. And 1 h after propofol treatment, LPS was added for 24 h. Control: no treatment group. Bars represent the mean ± SEM from at least three independent experiments. ### P < 0.001 versus control group. *P < 0.05, **P < 0.01, ***P < 0.001 versus LPS group. ψ P < 0.05 versus LPS + propofol group.
Propofol Induces Nrf2 Activation
Next, we evaluated the effect of propofol on the activation of Nrf2 in the levels of mRNA and protein. Results indicated that propofol (10, 25, and 50 μmol/L) increased Nrf2 mRNA level in LPS-treated A549 cells and directly increased the level of Nrf2 mRNA at 50 μM (Fig. 4a). The protein expression of Nrf2 was also upregulated by propofol (Fig. 4b).
Propofol increases Nrf2 level in mRNA (a) and protein (b) level. A549 cells were pretreated with propofol (10, 25, and 50 μmol/L) for 1 h before addition of LPS (100 ng/mL) for 24 h or treated with propofol (50 μmol/L) alone for 24 h. Control: no treatment group. Vehicle: 0.1 % DMSO-treated group. ### P < 0.001 versus control. *P < 0.05, **P < 0.01 versus LPS group.
Nrf2 siRNA Attenuates the Inhibitory Effect of Propofol on LPS-Induced ROS Production
To examine the role of Nrf2 in anti-oxidative effects of propofol, siRNA was used to inhibit Nrf2 expression. The results indicated that Nrf2 expression was dramatically downregulated in A549 cells by Nrf2-siRNA (Fig. 5a). Then we added propofol into LPS-treated A549 cells with or without Nrf2-siRNA transfection. Results indicated Nrf2 siRNA significantly attenuated the inhibition of propofol on LPS-induced ROS production (Fig. 5b).
Propofol attenuates LPS-induced ROS production via Nrf2 regulation. Effects of Nrf2-siRNA in Nrf2 expression on A549 cells (a), and in ROS production on LPS-treated A549 cells with/without propofol (b). Cultures were transfected with control or Nrf2 siRNA for 48 h and then pretreated with propofol (50 μmol/L) for 1 h before addition of LPS (100 ng/mL) for 24 h or treated with propofol (50 μmol/L) alone for 24 h. Control: no treatment group. ### P < 0.001 versus control, ***P < 0.001 versus LPS group, ψψ P < 0.01 versus LPS + propofol group.
Role of COX-2 in the Inhibitory Effect of Propofol on LPS-Induced ROS Production
Because propofol had both anti-inflammatory and anti-oxidant effects, we further investigated the crosstalk between COX-2 and ROS production in propofol protection on LPS-treated A549 cells. The COX-2 inhibitor, NS-398, was used to block the activation of COX-2. For results indicated in the condition of blocking COX-2 activity, propofol showed less inhibition on LPS-induced ROS production (Fig. 6).
Propofol attenuates LPS-induced ROS production via COX-2 regulation. NS-398 (1 μmol/L, COX-2 inhibitor) attenuates the inhibitory effect of propofol on LPS-induced ROS production in A549 cells. Cells were treated with NS-398 for 1 h before propofol (50 μmol/L) treatment. And 1 h after propofol treatment, LPS was added for 24 h. Control: no treatment group. Bars represent the mean ± SEM from at least three independent experiments. ### P < 0.001 versus control group. ***P < 0.001 versus LPS group. ψψψ P < 0.001 versus LPS + propofol group.
DISCUSSION
ARDS, the most severe form of acute lung injury secondary to sepsis, is one of the causes of substantial morbidity and mortality in both adults and children [22, 23]. When patients suffer from gram-negative bacteria infection, the increasing production of NO, prostaglandins, and ROS lead to oxidative stress-induced acute and chronic pulmonary diseases [24]. Thus, anti-oxidative stress is one of the therapeutic strategies for the treatment of endotoxin-induced ALI/ARDS. Propofol has been shown to be a strong oxygen radical scavenger and could attenuate ALI in endotoxemia [7, 25, 26]. In this study, we examine the roles of Nrf2 and COX-2 in propofol protection against LPS-induced ROS production, supporting the anti-inflammatory and antioxidant effects of propofol using alveolar epithelial cells, which have been found to play important roles in the defense and pathogenesis of infection [11].
In the present study, propofol was shown to circumvent LPS-induced oxidative stress by inducing the cytoprotective gene, Nrf2, which increased the total GSH level and reduced cellular ROS levels in A549 cells. Results also indicated that propofol directly activated Nrf2 and increased GSH levels in A549 cells. The synthesis of GSH is considered to prevent oxidative stress-induced apoptosis [27]. In addition, based on our data, propofol itself could increase the level of Nrf2 expression directly. Besides, we found that Nrf2 knockdown by Nrf2-siRNA increased intracellular ROS production and attenuated anti-oxidative effect of propofol. Thus, we postulate that the mechanism whereby propofol protects LPS-treated A549 cells against oxidative stress, at least in part, is via upregulation of Nrf2 expression.
The pathophysiology of ARDS is complex. Lung tissue cells, cells of inflammation, as well as apoptosis inhibitors and activators are involved in the mechanisms [28]. We were also interested in the crosstalk between the anti-oxidative and anti-inflammatory properties of propofol. In LPS/TLR4 signaling, ROS plays a key role for the activation of NF–κB and Akt [29]. Hsing et al. had demonstrated that propofol reduced endotoxic inflammation by inhibiting ROS-regulated Akt/IKKβ/NF–κB signaling in RAW 264.7 macrophages [30]. In this study, our results also showed that propofol attenuated LPS-induced inflammation by decreasing iNOS/NO and COX-2/PGE2 in A549 cells. Since the NADPH oxidase (NOX) was the major enzyme to produce ROS, we also measured the effect of propofol on NOX activation. Our data showed the propofol attenuated NOX2, the prototype NOX activation, and this result was consistent with the reduction of ROS. According to our results, propofol decreased LPS-induced ROS generation not only by inhibiting NOX-regulated ROS production, but also by inhibiting COX-regulated ROS production in A549 cells. Notably, the controversial effects of propofol on inflammatory responses have been demonstrated by Ko et al. who showed that propofol synergistically activates LPS-induced inflammatory responses in rat primary astrocytes and BV2 microglial cell lines [31]. Therefore, further studies to investigate these interesting and conflicting results of propofol on different cell types or organ system should be carried out.
In many human pathological conditions, the critical factor regulating cellular defense response is Nrf2. When cells are exposed to chemopreventive compounds or oxidative stress, Nrf2 migrates into the nucleus and several different types of genes, including those encoding endogenous antioxidants, phase II detoxifying enzymes, and transporters, are activated [16]. However, the other side of Nrf2 has been revealed in recent data. In many types of human cancer, Nrf2 over-expression offers cancer cells an advantage in survival and growth [32]. Garib et al. found that the migration of breast cancer cells was increased by propofol [33]. Another article reported that invasion and proliferation of gallbladder cancer cells induced by propofol were through the activation of Nrf2 [34]. However, the safety of using propofol in cancer patients is a contentious issue. Mammoto et al. demonstrated that propofol decreased the invasive ability of human cancer cells in clinically relevant concentrations [35]. A recent study [36] also reported that propofol suppressed invasion and migration of A549 cells by downregulating matrix metalopreteinase-2 and the p38 MAPK signaling pathway. Despite activation of Nrf2 increasing cancer activity, the net effect of propofol in cancer cells was interesting and still needs further investigation. So far, propofol is a widely used anesthetic for operations and ICU sedation, and is also a potential candidate for the treatment of sepsis-induced ALI/ARDS. However, using propofol in cancer patients should be cautioned, especially for long-term use in ICU sedation. Besides, due to the direct myocardial suppression effect, the cardiopulmonary interaction of propofol in septic patients should be more emphasized.
In conclusion, the present study demonstrated that propofol protects alveolar A549 cells against LPS through decreasing inflammatory factors and enhancing antioxidant defense. The multi-target mechanism of propofol on ROS production is by activation of Nrf2 and inhibition of NOX or COX2, suggesting that propofol might be a good intravenous anesthetic of choice when patients with ALI/ARDS require sedation and/or general anesthesia.
References
Riedemann, N.C., R.F. Guo, and P.A. Ward. 2003. Novel strategies for the treatment of sepsis. Nature Medicine 9: 517–24.
Brigham, K.L., and B. Meyrick. 1986. Endotoxin and lung injury. The American Review of Respiratory Disease 133: 913–27.
Callahan, L.A., D. Nethery, D. Stofan, A. DiMarco, and G. Supinski. 2001. Free radical-induced contractile protein dysfunction in endotoxin-induced sepsis. American Journal of Respiratory Cell and Molecular Biology 24: 210–7.
Lambeth, J.D. 2004. NOX enzymes and the biology of reactive oxygen. Nature Reviews Immunology 4: 181–9.
Touyz, R.M., A.M. Briones, M. Sedeek, D. Burger, and A.C. Montezano. 2011. NOX isoforms and reactive oxygen species in vascular health. Molecular Interventions 11: 27–35.
Allaouchiche, B., R. Debon, J. Goudable, D. Chassard, and F. Duflo. 2001. Oxidative stress status during exposure to propofol, sevoflurane and desflurane. Anesthesia & Analgesia 93: 981–5.
Chu, C.H., D. David Liu, Y.H. Hsu, K.C. Lee, and H.I. Chen. 2007. Propofol exerts protective effects on the acute lung injury induced by endotoxin in rats. Pulmonary Pharmacology & Therapeutics 20: 503–12.
Hsing, C.H., W. Chou, J.J. Wang, H.W. Chen, and C.H. Yeh. 2011. Propofol increases bone morphogenetic protein-7 and decreases oxidative stress in sepsis-induced acute kidney injury. Nephrology Dialysis Transplantion 26: 1162–72.
Song, X.M., Y.L. Wang, J.G. Li, et al. 2009. Effects of propofol on pro-inflammatory cytokines and nuclear factor kappaB during polymicrobial sepsis in rats. Molecular Biology Reports 36: 2345–51.
Chiu, W.T., Y.L. Lin, C.W. Chou, and R.M. Chen. 2009. Propofol inhibits lipoteichoic acid-induced iNOS gene expression in macrophages possibly through downregulation of Toll-like receptor 2-mediated activation of Raf-MEK1/2-ERK1/2-IKK-NFkappaB. Chemico-Biological Interactions 181: 430–9.
Chuquimia, O.D., D.H. Petursdottir, M.J. Rahman, K. Hartl, and M. Singh. 2012. Fernandez C The role of alveolar epithelial cells in initiating and shaping pulmonary immune responses: communication between innate and adaptive immune systems. PloS One 7: e32125.
Lin, Y., M. Zhang, and P.F. Barnes. 1998. Chemokine production by a human alveolar epithelial cell line in response to Mycobacterium tuberculosis. Infection and Immunity 66: 1121–6.
Matthay, M.A., and R.L. Zemans. 2011. The acute respiratory distress syndrome: pathogenesis and treatment. Annual Review of Pathology: Mechanisms of Disease 6: 147–63.
Razavi, H.M., L. Wang, S. Weicker, et al. 2005. Pulmonary oxidant stress in murine sepsis is due to inflammatory cell nitric oxide. Critical Care Medicine 33: 1333–9.
Wang, L., R. Taneja, W. Wang, et al. 2013. Human alveolar epithelial cells attenuate pulmonary microvascular endothelial cell permeability under septic conditions. PloS One 8: e55311.
Kaspar, J.W., S.K. Niture, and A.K. Jaiswal. 2009. Nrf2:INrf2 (Keap1) signaling in oxidative stress. Free Radical Biology & Medicine 47: 1304–9.
Kensler, T.W., N. Wakabayashi, and S. Biswal. 2007. Cell survival responses to environmental stresses via the Keap1-Nrf2-ARE pathway. Annual Review of Pharmacology and Toxicology 47: 89–116.
Cho, H.Y., S.P. Reddy, A. Debiase, M. Yamamoto, and S.R. Kleeberger. 2005. Gene expression profiling of NRF2-mediated protection against oxidative injury. Free Radical Biology & Medicine 38: 325–43.
Redl, H., S. Bahrami, G. Schlag, and D.L. Traber. 1993. Clinical detection of LPS and animal models of endotoxemia. Immunobiology 187: 330–45.
Shih, Y.T., P.S. Chen, C.H. Wu, Y.T. Tseng, Y.C. Wu, and Y.C. Lo. 2010. Arecoline, a major alkaloid of the areca nut, causes neurotoxicity through enhancement of oxidative stress and suppression of the antioxidant protective system. Free Radical Biology & Medicine 49: 1471–9.
LeBel, C.P., H. Ischiropoulos, and S.C. Bondy. 1992. Evaluation of the probe 2',7'-dichlorofluorescin as an indicator of reactive oxygen species formation and oxidative stress. Chemical Research in Toxicology 5: 227–31.
Erickson, S.E., G.S. Martin, J.L. Davis, M.A. Matthay, and M.D. Eisner. 2009. Recent trends in acute lung injury mortality: 1996–2005. Critical Care Medicine 37: 1574–9.
Randolph, A.G. 2009. Management of acute lung injury and acute respiratory distress syndrome in children. Critical Care Medicine 37: 2448–54.
Folkerts, G., J. Kloek, R.B. Muijsers, and F.P. Nijkamp. 2001. Reactive nitrogen and oxygen species in airway inflammation. European Journal of Pharmacology 429: 251–62.
Votta-Velis, E.G., R.D. Minshall, D.J. Visintine, M. Castellon, and I.V. Balyasnikova. 2007. Propofol attenuates endotoxin-induced endothelial cell injury, angiotensin-converting enzyme shedding, and lung edema. Anesthesia & Analgesia 105: 1363–70. table of contents.
Yeh, C.H., W. Cho, E.C. So, et al. 2011. Propofol inhibits lipopolysaccharide-induced lung epithelial cell injury by reducing hypoxia-inducible factor-1alpha expression. British Journal of Anaesthesia 106: 590–9.
Zou, X., Z. Feng, Y. Li, et al. 2012. Stimulation of GSH synthesis to prevent oxidative stress-induced apoptosis by hydroxytyrosol in human retinal pigment epithelial cells: activation of Nrf2 and JNK-p62/SQSTM1 pathways. The Journal of Nutritional Biochemistry 23: 994–1006.
Galani, V., E. Tatsaki, M. Bai, et al. 2010. The role of apoptosis in the pathophysiology of acute respiratory distress syndrome (ARDS): an up-to-date cell-specific review. Pathology-Research and Practice 206: 145–50.
Asehnoune, K., D. Strassheim, S. Mitra, J.Y. Kim, and E. Abraham. 2004. Involvement of reactive oxygen species in Toll-like receptor 4-dependent activation of NF–kappa B. The Journal of Immunology 172: 2522–9.
Hsing, C.H., M.C. Lin, P.C. Choi, et al. 2011. Anesthetic propofol reduces endotoxic inflammation by inhibiting reactive oxygen species-regulated Akt/IKKbeta/NF–kappaB signaling. PloS One 6: e17598.
Ko, H.M., S.Y. Kim, S.H. Joo, et al. 2013. Synergistic activation of lipopolysaccharide-stimulated glial cells by propofol. Biochemical and Biophysical Research Communications 438: 420–6.
Mitsuishi, Y., H. Motohashi, and M. Yamamoto. 2012. The Keap1-Nrf2 system in cancers: stress response and anabolic metabolism. Frontiers in Oncology 2: 200.
Garib, V., K. Lang, B. Niggemann, K.S. Zanker, L. Brandt, and T. Dittmar. 2005. Propofol-induced calcium signalling and actin reorganization within breast carcinoma cells. Eur J Anaesthesiology 22: 609–15.
Zhang, L., N. Wang, S. Zhou, W. Ye, G. Jing, and M. Zhang. 2012. Propofol induces proliferation and invasion of gallbladder cancer cells through activation of Nrf2. Journal of Experimental & Clinical Cancer Research 31: 66.
Mammoto, T., M. Mukai, A. Mammoto, et al. 2002. Intravenous anesthetic, propofol inhibits invasion of cancer cells. Cancer Letters 184: 165–70.
Wu, K.C., S.T. Yang, T.C. Hsia, et al. 2012. Suppression of cell invasion and migration by propofol are involved in down-regulating matrix metalloproteinase-2 and p38 MAPK signaling in A549 human lung adenocarcinoma epithelial cells. Anticancer Research 32: 4833–42.
Acknowledgments
This study was supported by grants provided by Kaohsiung Medical University [grant number: M110022] and the National Science Council of Taiwan to Y.C.L. [grant number: NSC 102-2628-B-037-001-MY3].
Conflict of interest
None of the authors of this paper has a financial or personal relationship with other people or organizations that could inappropriately influence or bias the content of the paper. The authors report no potential conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hsu, HT., Tseng, YT., Hsu, YY. et al. Propofol Attenuates Lipopolysaccharide-Induced Reactive Oxygen Species Production Through Activation of Nrf2/GSH and Suppression of NADPH Oxidase in Human Alveolar Epithelial Cells. Inflammation 38, 415–423 (2015). https://doi.org/10.1007/s10753-014-0046-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-014-0046-4