Abstract
When health care management considers implementing a new technology such as a medical device, it is crucial to take workflow, clinical outcome, economy, and environmental impacts into consideration in the decision-making process. This study outlines the knowledge status of this complex challenge via a systematic literature review (SLR). The SLR found 133 of 1570 screened publications that covered relevant frameworks for choosing hospital equipment (i.e., related economics, life cycle assessment, waste generation and health issues). Yet, just five publications addressed choosing single-use vs. reuse of tubes or similar types of equipment by economic and environmental considerations through a systematic quantitative approach. The SLR reveals few publicly available peer-reviewed studies for the optimal sustainable choice of equipment. This study assesses environmental impacts of carbon dioxide (CO2) emissions as CO2-equivalents and resource consumption of a single-use double-lumen tube (DLT) combined with a reusable bronchoscope were compared to a single-use DLT with an integrated single-use camera. Camera DLTs exclude or minimize the need for a bronchoscope to verify correct tube placement during one-lung ventilation. The life cycle assessment shows that the materials and energy used and needed for personnel protective equipment and cleaning of the reusable bronchoscope contribute significantly to CO2-equivalent emissions. To ensure the sustainable choice of equipment this aspect must not be overlooked. Secondly, future reuse of plastic waste materials from the use can contribute significantly to better environmental performance.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
1 Introduction
Today’s agenda on sustainable development challenges many aspects of approaches in society. The United Nations Sustainable Development Goals (Nations, 2015a) aim to provide a framework for those challenges that require a collaborative and joint focus from governments, the private sector, civil society, and people. These challenges include various environmental impacts such as those from climate change. A major task is to tackle climate change and mitigate its consequences, partly by swiftly reducing emissions of carbon dioxide (CO2) and other greenhouse gases arising from our use of fossil fuels (Take urgent action to combat climate change & its impacts, 2015).
This must be pursued in parallel to other challenges. A key one is ensuring both responsible consumption and production given the increasing scarcity of resources. As case in point is the accelerating exploitation of known but limited reserves, e.g., rare earth metals in the production of electronics and other digital consumables (Nations, 2015b).
The consumption of various devices causes various environmental impacts originating from the use of natural resources, energy used in their production. The impacts arising from the use of devices may apply to different sectors, including the medical sector (Marshall et al., 2017). The consumption of scarce resources often occurs in the manufacturing of products for the economy, while CO2 emissions are usually associated with the fossil fuels used in the production, transport, and utilization of a given product (Climate Change 2014 Synthesis Report Summary for Policymakers, 2014).
Mounting concern for the environment has also entered the healthcare sector. Hence, there is a now pressing need to better understand how various choice of products or medical operation and service contribute to environmental impact and map their impacts, when comparing different ways to perform the same medical operation or service. Recent studies have compared greenhouse gas emissions, calculated as CO2-equivalent emissions, for reusable and single-use bronchoscopes (Sørensen & Grüttner, 2018), reusable and single-use ureteroscopes (Niall F. Davis et al., 2018a, 2018b), environmental impacts of single-use vs. reusable scissors (Ibbotson et al., 2013), and single-use vs. reusable anesthetic equipment McGain et al. (2017).
The introduction of single-use alternatives has stressed the need for robust comparisons of their potential environmental impacts (Campion et al., 2015). Discarding single-use devices intuitively causes concern among hospital staff, and people in general, who care about whether such a single-use is environmentally friendly (Marshall et al., 2017). Disposable products were initially intended for use in exceptional circumstances or conditions, to guarantee proper disinfection (e.g., during warfare, disasters, epidemics) (Tvede et al., 2012; Viana et al., 2016). Furthermore, concerns related to patient safety have led to the introduction of high-level disinfection (HLD) standards and procedures that have replaced simple sterilization. Specialized functions in hospitals can now clean and disinfect reusable devices (Gupta & Wang, 2009; McCahon & Whynes, 2015); (Perbet et al., 2017). Such developments have naturally led to the greater use of personal protective equipment (PPE) and specialized cleaning and disinfection equipment, which have increased their environmental burden and potentially their economic burden as well (McGain et al., 2017); (Larsen et al., 2019). Consequently, due to increasing labor costs, capital costs, repair costs, and energy requirements related to reprocessing reusable devices, single-use devices have become the preferred choice for numerous surgical cases within different hospital specialties (e.g., anesthesia, pulmonology, emergency care)(McGain et al., 2017); (Perbet et al., 2017);(Gupta & Wang, 2009); (Tvede et al., 2012); (McCahon & Whynes, 2015). Single-use devices are often preferred in cases where availability and sterility are key factors for an optimized workflow.
The relationship between a product’s life cycle (i.e., its design/production/use/end-of-life) and its environmental burdens comprise a complex challenge. Hence, the decisions made in its design stages, for example, combined with certain external parameters, like context of use or end-of-life, can jointly influence its overall environmental impact (Moultrie et al., 2015). Methods to understand and support development toward better solutions have therefore been focus of interest for a long time, hence, e.g., Life cycle Assessment, Eco-design, Life Cycle Costing, and Circular Economy developed.
Concepts like the circular economy aim to improve companies’ decision-making process and to reduce the negative environmental impacts of the products’ life cycle. The overall goal is to design products and implement company approaches and policies that accommodate sustainability. The Ellen Macarthur Foundation frames the circular economy this way: "Circular economy is based on the principles of designing out waste and pollution, keeping products and materials in use, and regenerating natural systems" (Foundation, 2017). However, all environmental aspects are not always evident using principles as highlighted in the circular economy concept. An approach to clarify and be aware of the pitfalls in a specific context is to make a life cycle assessment to support the decision making. A complete life cycle assessment determines whether reuse or single use perform the best on various environmental parameters.
(Haber & Fargnoli, 2021) have developed methods for addressing this challenge using product service system perspective in the medical sector.
The circular economy concept aims to link environmental performance to the design approach. (MacNeill et al., 2020) have studied the barriers to circularity in the medical device industry. They highlight perceptions regarding infection, behaviors of customers and manufacturers as well as regulatory structures to be barriers. Therefore, policy and market driven solutions are needed to transform the market.
Similarly, a disconnect between practice and reuse or recycling of medical waste is found by (Ordway et al., 2020), which confirms the balancing and management challenge.
However, various health economic aspects, including clinical outcomes, should also be very relevant to consider when assessing the relevant performance assessment dimensions in comparing single-use and reusable devices. Aspects of health economics seek to investigate all appropriate costs associated with using the device in question.
Reusable devices entail reprocessing costs—including disposable cleaning equipment, water and detergent consumption, and electricity usage, among others—ongoing repair and maintenance costs, capital investments, as well as labor costs. For single-use devices, the economic aspects include the device's price and the costs associated with discarding it after each procedure. The micro-costing method is often used to derived the most precise estimates of running costs, especially when assessing new medical devices (Xu et al., 2014).
Quantifying and balancing all perspectives are as mentioned previously an acknowledged challenge.
This study aims to determine the status, and knowledge of balancing and quantifying environmental, economic, and social aspects by a substantial literature search focused on the choice between single-use and reusable equipment in the medical sector, e.g., double-lumen tubes (DLTs) and similar medical equipment and their use.
Secondly, this study compares the specific choice of either using a single-use double-lumen tube (DLT) combined with a reusable bronchoscope were compared to a single-use DLT with an integrated single-use camera. This comparison is made on the environmental impacts of carbon dioxide (CO2) emissions as CO2-equivalents and resource consumption. This study also explores scenarios with different levels of reuse of the plastics in the tubes to understand the future perspective of the investigated example of choice.
Combining the literature research and the current example aims to illustrate the aspects of the challenge for decision makers who wishes to aim for sustainable management.
1.1 Materials and methods
1.1.1 Study design
This study focused on two outcomes. The first outcome was to perform a literature review to investigate the current state of knowledge regarding the environmental and economic aspects of single-use vs. reusable medical equipment. Additionally, the literature review sought to identify potential research gaps within this topic, so as to include these aspects in the later discussion.
The second outcome was a carbon footprint analysis of using a camera DLT compared with using a conventional DLT-and-reusable bronchoscope. The aim here is to illustrate and exemplify the challenges of identifying the right choice to make for a device. The potential impact of reusing the plastic and cardboard in the waste handling is also investigated.
The functional unit chosen was one-lung operated patients, for whom single-lung ventilation was achieved using lung separation with a DLT. Two different scenarios to achieve one-lung ventilation were investigated:
-
1.
Using a conventional DLT and a reusable bronchoscope to verify correct tube placement (i.e., the reference scenario)
-
2.
Using a camera DLT (ETView Medical Ltd./Ambu A/S, Ballerup, Denmark), thus precluding the need for a bronchoscope to verify correct tube placement (i.e., the intervention scenario).
1.2 Literature review
A systematic literature review (SLR) was conducted to provide the accumulated knowledge on choosing between single-use and reuse devices in health care. More specifically, the literature was reviewed to identify research gaps and existing knowledge of the environmental and economic aspects of single-use vs. reusable medical devices. An SLR has four stages: planning stage (purpose and protocol), selection stage (literature search and screening), extraction stage (quality appraisal and data extraction), and an execution stage (analysis and findings and writing the review).
In the planning stage, the SLR's purpose was to identify the main aspects and conclusions deemed valid for choosing between single-use and reuse devices in health care. Here, the authors also agreed on a standard protocol regarding the review procedure, in part by identifying relevant databases and keywords for the study.
Studies were identified through literature searches. The searches considered all studies published until December 2021 in the databases used. The search was conducted in the electronic databases PubMed, Embase, Ei Compendex, and Web of Science.
The search was conducted using the following medical subject headings (MeSH) and keywords:
-
((hospital[MeSH Terms]) OR (surgery[MeSH Terms]) OR (medical device[MeSH Terms]) OR (equipment[MeSH Terms])
-
AND ((reusable[MeSH Terms]) OR (conventional[MeSH Terms]) OR (single-use[MeSH Terms])) OR (disposable equipment[MeSH Terms]) OR (multi-use[MeSH Terms])) OR (equipment, disposable[MeSH Terms]) OR (non-disposable[MeSH Terms]) OR (disposal, biologic waste[MeSH Terms])
-
AND ((allocation, cost[MeSH Terms]) OR (analysis, cost[MeSH Terms]) OR (analyses, cost benefit[MeSH Terms]) OR (analyses, cost[MeSH Terms])) OR (cost effectiveness[MeSH Terms]) OR (health economics[MeSH Terms]) OR (economics[MeSH Terms]))OR (environment and public health[MeSH Terms]) OR (life cycle[MeSH Terms])
-
AND ((life cycle assessment[MeSH Terms]) OR (environmental impact[MeSH Terms]) OR (environmental impacts[MeSH Terms]) OR (ecodesign[MeSH Terms]) OR (sustainability, program[MeSH Terms]) OR (sustainabilities, program[MeSH Terms]) OR (decision making[MeSH Terms]) OR (decision making, organizational[MeSH Terms]) OR (carbon footprint[MeSH Terms])
-
AND English [lang].
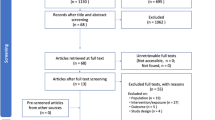
The literature search yielded in total 1611 records, of which 41 were duplicates, thus leaving 1570 records.
To limit the scope of inquiry eight subjects of interest were chosen (listed below). The records abstracts were screened accordingly to the subjects listed (i.e., economics, life cycle assessment, waste generation and health issues). The subjects cover various aspects of how to make sustainable choices when buying equipment.
The screening step resulted in a total of 133 records (Appendix 1) that constituted the dataset for our study.
In the extraction stage, both quality appraisal and data extraction from the dataset was carried out. The dataset was categorized into the eight subject areas of interest—listed above—to determine which of those subject areas were covered in each publication, and to what extent. The number of publications as a function of publication year was also investigated.
-
1.
Health economics
-
2.
Economics and life cycle assessment
-
3.
Life cycle assessment
-
4.
Economics and waste reduction
-
5.
Medical waste reduction
-
6.
Economics and environment
-
7.
Qualitative environmental and economic considerations
-
8.
Considerations related to the reuse or single-use devices
1.3 Goal and Scope of Life cycle assessment/carbon footprint
Life cycle assessment (LCA) is a well-known and established method to assess the environmental impacts from a device or service (ISO/TC207/SC5, 2016). The use of natural resources, such as energy, land, minerals and metals, and outputs in the form of products, by-products, emissions, and waste, are quantified for all steps in the device's life cycle. While LCAs have been carried out on many food products and production systems (Poore & Nemecek, 2018), the approach is now being used extensively in many other fields of research. Yet, the use of LCA is relatively new in the healthcare industry. A 'carbon footprint' is a subset of a full LCA, in which only the climate impact is investigated. Due to the increasing interest in this subject, the International Organization for Standardization (ISO) has issued a standard describing the principles and framework for the LCA and carbon footprint of products (ISO/TC207/SC5, 2016).
The reusable bronchoscope's cleaning and disinfection must be included to fairly compare the camera DLT with the conventional DLT and a reusable bronchoscope. This comparison was done using the LCA approach, which sometimes also referred to as the ‘cradle to grave approach’. This methodology to analyze environmental impacts is gaining popularity within the healthcare sector (Niall F. Davis et al., 2018a, 2018b); (Campion et al., 2015);(Viana et al., 2016). This study's LCA approach is comparable to the ISO 14040 standards and complies with the transparency criteria in that standard. Such an analysis covers the whole life cycle of the products, production of raw materials, manufacturing to the extent possible from the data available, the use phase, and disposal/recovery. The impacts not included in this analysis are water-related impacts and toxicity impacts. The former are not considered relevant in this analysis, though water use may be appropriate in other contexts, e.g., Australia (McGain et al., 2017). The toxicity impacts, however, may be substantial due to the phthalates in the devices. It is not possible to quantify the toxicity-related impacts because we lack information on their content of phthalates in the plastic materials. This aspect is, however, should be possible to quantify qualitatively.
Data on processing and material use impacts used for this study were pooled from Ecoinvent, using Simapro 9.0.0.5 (Sustainability, 2020). The background system chosen was a Danish context; that is, we used Danish heat and electricity production rates when waste is incinerated. Hospital waste is incinerated with 99% energy recovery in Denmark. These calculations were made using the International Reference Life Cycle Data System (ILCD). We should note that ILCD includes biogenic carbon.
1.3.1 Reference scenario
One-lung ventilation (OLV) is an essential technique for most traditional thoracic surgeries. It refers to the mechanical separation of the two lungs, wherein only one lung is ventilated while the other is deflated (Rapchuk et al., 2017); (Massot et al., 2015). The most common OLV method is intubation with a double-lumen tube (DLT). Situations requiring OLV procedures are often lobectomies, biopsies due to the suspicion of cancer, and lung resections. The annual number of OLV procedures in Denmark is approximately 2,100 procedures (Sundhedsdatastyrelsen, 2020). Reusable bronchoscopes are used to check and ensure the correct placement of the DLT to secure the non-ventilation of the lung to be operated on (Terjesen et al., 2017); (Koleva et al., 2013); (Communication, 2015); (Ofstead et al., 2017). Furthermore, it is the gold standard to check whether the tube placement is correct, by using a fiber-optic or video-enabled bronchoscope, or both, after the tube’s insertion. Also, it is crucial to recheck its placement after shifting the patient's position into the final lateral surgical position, since doing so could increase the risk of tube displacement (Atul et al., 2015). Therefore, to ensure the accurate placement of the tube, a new DLT with a camera in the tip can be used. When using the DLT with the inbuilt camera, there is no longer any need for a reusable bronchoscope. It has been shown that it is clinically faster and easier to use the DLT with a camera, and a cost-effectiveness analysis demonstrated a cost-saving aspect to it, because the reusable bronchoscopes are only used in 4% of the cases (Larsen et al., 2019).
The reference scenario investigates the single-use conventional DLTs used together with a reusable bronchoscope (Fig. 1). A flow diagram of the reference scenario processes is shown in Fig. 2.
Reusable bronchoscopes require cleaning that uses high-level disinfection (HLD) as well as drying after every use. This study’s evaluation of the impact from reprocessing reusable bronchoscopes is based on the procedure currently in use at the Odense University Hospital. The materials used for reprocessing is listed in Table 1.
-
After using the bronchoscope is manually brought to the cleaning room.
-
During the cleaning process the staff wear PPE (apron, gloves, etc.)
-
The bronchoscope is placed on a barrier.
-
The bronchoscope is soaked in a sink full of water, to which the cleaning detergent is added (Bordedex forte: 2 portions), and then manually cleaned with a brush and flushed with water.
-
The bronchoscope is then mounted in a special washer (automated endoscope reprocessor [AER]), one specially designed for endoscopes. The AER cleans the endoscopes and can house two endoscopes per cycle. The cleaning agents used are Aperlan A and Aperlan B. One cleaning cycle lasts 30 min.
-
After the manual cleaning, the table is cleaned using alcohol and napkins. All waste is put into a plastic waste bag and sent for incineration as part of the hospital waste.
-
After cleaning the bronchoscopes, each is placed inside a drying cabinet. It is left there to dry and stored overnight till its next use. One drying cabinet can hold eight endoscopes.
1.3.2 Intervention scenario
The intervention scenario investigated the single-use DLT with an integrated camera (VivaSight-DL, ETView Medical Ltd./Ambu A/S, Ballerup, Denmark). By having an integrated camera, the need for a bronchoscope to confirm correct tube placement is eliminated. It should be noted that a bronchoscope might still be required in certain cases (e.g., to check for a tumor mass further down in the lungs). The VivaSight tube is connected to a screen monitor (this monitor was not included in the assessment) (Fig. 3). A flow diagram of the processes and workflows for the intervention scenario using the VivaSight-DL is shown in Fig. 4 Table 2.
1.4 Other data
1.4.1 Energy use for washing drying and storing
Washing of scopes: Usually, the washer runs using 26 L of water, using 55 g of washing agent A and 55 g of washing agent B. Its maximum energy use is 11 kW when running a normal washing cycle of 30 min. Every 24 h the washer is running a cleaning cycle using 100 g of soap and 64 L of water. Based on the data mentioned, one washing cycle's energy use is estimated to be 0.65 kWh per washing cycling, in which two scopes are cleaned.
1.4.2 Drying Cabinet
Maximum energy use is 2.1 kW. The heating unit uses 1.5 kW; the compressor uses 300 W; UV light uses 15 W. The total energy use is based on the values listed and estimated at 43.2 kWh per day to keep eight scopes dry and stored safely.
1.4.3 Energy recovery
All waste is incinerated as hazardous waste in a Danish hazardous waste incineration plant. In the process, up to 99% of the energy is recovered as heat and electricity.
1.4.4 Disinfection before use
Tubes are presumed disinfected via cold sterilization with ethylene oxide.
1.4.5 Transport
The tubes are assumed to move 12,000 km, carried by a Euro 6 freight lorry. This transport includes going from production site to the consumer and is based on the tube’s production occurring in Europe. Table 3.
2 Results
2.1 Literature search
The literature search yielded a total of 133 relevant studies. Of these, 40 records reported comparing the environmental impact of single-use and reusable medical devices. However, only a limited number (n = 5) of these studies sought to compare DLTs or endoscopes. Only one out of 5 studies compared both environmental and health economics data. Figure 5 depicts 133 studies grouped into different categories, to provide an overview; the blue color shows the relevant investigations related to medical devices in general. The orange color presents those studies comparing single-use and reusable medical devices, while the last column are studies addressing the environmental or economic impact associated with single-use versus reusable DLTs or endoscopes. Only the five studies comparing DLTs or endoscopes were explored in more detail. Baseline characteristics for these studies are presented in Table 3. An overview of all articles found are listed in Appendix 1. It is also evident from Fig. 5 that mainly single subject areas are covered, e.g., health economics or life cycle assessment or waste.
Finding the optimal sustainable approach or sustainable choice of equipment will depend on the combination of several aspects (economic, health, and environmental impacts). Thirty studies focused only on financial aspects; 11 studies covered both economics and life cycle assessment approaches; 10 out of 29 studies were found that analyzed the equipment's environmental impacts using a systematic quantitative method equivalent to a life cycle assessment. This illustrates a profound research gap. Evidently, the topic of waste reduction has been studied, for which 37 records were found, of which 13 addressing both economics and waste reduction.
Figure 6 shows that in the last decade the number of publications investigating the topics of interest has increased over the preceding 27 years and especially the last 2 years. This trend illustrates the currently expanding focus on cost efficiency and the focus upon environmental aspects of using various medical devices. It illustrates the fact that the focus on these issues is relatively new in the healthcare industry and very pertinent.
As mentioned in the above introduction section, achieving sustainability requires the simultaneous consideration of economic and social aspects along with environmental impact. The SLR indicated that economic aspects have been researched, and waste generation optimization to similar extent, but few studies have inquired into a full life cycle assessment.
One analysis (McGain et al., 2017) revealed how the balance, as related to the global warming impact, between reuse and single-use choices of equipment depends on the background system (e.g., what sources supply the electricity used for washing and drying). Those authors also concluded that reuse in those assessed contexts resulted in a higher 10% CO2 impact and more than a doubling of water use.
A review paper (Drew et al., 2021) on Life cycle assessment of surgical and anesthetic care find that most data show that single-use devices tends to result in higher contributions to environment. They also find examples of the opposite conclusion.
Only five studies could be found that aimed to quantify environmental impacts in combination with equipment choice for single-use vs. reusable products like tubes and scopes. They are listed in Table 3. An additional paper is listed which reports on a health economic analysis of the tubes used in the illustrative example of our study.
The literature review clearly indicates a research gap regarding comparing, quantifying the environmental impact, and balancing the choice between single-use and reusable DLTs and endoscopes devices in the health care sector, from both a health economics and an environmental perspective. It has become clear that minimal evidence exists on the subject with respect to comparing economic and environmental aspects when evaluating new interventions.
Only one study compared the economic aspects and environmental aspects of reusable vs. single-use laryngoscopes (Sherman et al., 2018). Two studies did perform a full life cycle assessment comparing single-use ureteroscopes vs. reusable ureteroscopes and single-use bronchoscopes vs. reusable bronchoscopes. Lastly, only one study has compared the health economics aspects of VivaSight-DL to a DLT in combination with a reusable bronchoscope.
A previous study (Larsen et al., 2019) found that VivaSight-DL is more cost-effective than using DLTs that are combined with a reusable bronchoscope. One reason for this is that VivaSight-DL, with its integrated camera, significantly reduces the need for a reusable bronchoscope; hence, any reprocessing of the bronchoscope was eliminated. Reprocessing reusable endoscopes is time-consuming and consists of various mandatory reprocessing steps to minimize any risk of bacterial residues contaminating the endoscope and being transferred to another patient during a procedure. The reprocessing of endoscopes also requires substantial amounts of detergent, water, and disposable PPE, all of which is relevant for a transparent comparison with the amount of waste associated with a fully disposable endoscope or DLT.
A recent study (Sørensen & Grüttner, 2018) compared reusable bronchoscopes to single-use bronchoscopes, finding that the CO2 emissions were somewhat equivalent. In another study (N. F. Davis et al., 2018a, 2018b), the total carbon footprint of the single-use ureteroscope Lithovue™ (4.43 kg CO2 eq per case) was smaller than that for a reusable ureteroscope (4.47 kg CO2 eq per case).
2.2 Life cycle assessment and carbon footprint of DLTs.
The results are summarized in Fig. 7. Figure 7 shows the results for the categories chosen and the two tube systems are presented beside each other.
A general pattern is discernable, one that is related to energy consumption. The reusable scope, which requires washing after each use, seems to exert a considerable environmental burden. The single-use shows higher impacts related to resource consumption. It is related to the fact that for every time a tube is used there is use of materials, fossil as well as minerals. The single use tube includes a camera and a chip. The metals or minerals in the tube will be lost as waste. If a product includes rare resources, this could be a problematic loss of resources.
To better understand this pattern, the breakdown of the different contributors to the environmental impact is depicted in Fig. 8, since this enables their closer examination. Furthermore, the uncertainty and sensitivity of these results must be assessed. This study compares single-use DLTs with an integrated camera (VivaSight-DL) to single-use DLTs without a camera used in combination with a flexible, reusable bronchoscope. Figure 8 shows that the VivaSight-DL has a carbon footprint of 1.25 kg CO2 eq in the contextual framework assessed in this study. A comparable tube for single-use, combined with flexible reusable scope that undergoes cleaning and drying before reused, has a total carbon footprint of 2.1 kg CO2 eq under the current framework assessed.
Figure 8 shows that the amount of material (mainly plastic types) used to make the tubes is the main contributing factor followed by the incineration of their packaging and PET. Secondly, the material and energy use needed for the washing and handling during the cleaning of scopes slated for reuse have a significant, extra impact on their carbon footprint.
Figure 8 shows the breakdown of the carbon footprint in the systems including drying and storage. From those results, it is also evident that the energy used for drying and storing is significant but not the sole factor determining the overall totals.
To investigate the detail of reuse of packaging further, some more detailed scenarios have been made. According to (PlasticEurope, 2019), the proportion of plastics collected for recycling now averages 32.4% in EU member states. (Miljøstyrelsen, 2018) has estimated the actual recycling rate in DK to be 19%, even though more than 40% of plastic is collected. In the future, it may be possible to attain a higher recycling rate, especially if the products are designed with their recycling in mind, and waste collection systems are customized to better handle them (Moultrie et al., 2015). This is not the case today of hospital plastic waste, which is in Dansih context incinerated.
Figure 9 shows the effect of the carbon footprint of recycling between 100 and 25% of the plastics. The carbon footprint for the combined scenario can with full recycling get reduced to 0.6 kg CO2 eq. The single use scenario can get reduced to 0.3 kg CO2 eq. The reuse of plastics is especially challenging and presently still undergoing further development and refinement. Assuming 100% recycling of plastics is a very high level of recycling and not the case for most waste collection systems as of today. In the future, however, it may be a possible reachable target. Yet, some development within a design for reuse of materials and collection systems must be developed.
2.2.1 Sensitivity and Uncertainty
Based on the obtained dataset and specific scenarios evaluated here, our results uncovered a carbon footprint for single-use device that is comparable in size to that of the multiple-use device.
2.2.2 Data on the production and materials of tubes and scopes
It is evident from the breakdown of contributors that the amounts of plastic used in the various parts of the tubes play an important role. The durability of a product is also a function of the material quality and amounts used to make it. But the analysis indicates that the optimal use of this material is vital for the overall carbon footprint or other environmental impacts since the material used for either protective wear or equipment is a significant contributor (> 50%) to the product’s carbon footprint.
The amount of paper and cardboard used also significantly impacts the total carbon footprint of the scenarios examined. This effect, however, is mostly related to products’ disposal. The emissions generated from incineration augments the CO2 impact, whereas if the material is reused, it replaces production of new cardboard and thus reduces the CO2 impact.
2.2.3 Energy use and protective wear
The main uncertainty stems from uncertain empirical data for the energy use needed for one washing cycle and the storage of the devices in a ventilated cabinet. It was only possible to find technical data on the maximum energy use for the washing process and the storage cabinets. The energy used for this washing was assumed to be 0.65 kWh for one washing cycle carrying two scopes. The energy used for the storage of eight scopes was assumed to 43.2 kWh. The uncertainty due to unavailable data is significant. The effect of having 50%–90% less energy used for the washing reduces the contribution to 0.1 kg CO2 eq. Given the fraction of energy use contributing to the carbon footprint (= 0.2 kg CO2 eq), this will still favor the single-use tube if the recycling of paper, cardboard, and plastics are not enforced somehow.
It is also essential to note that a major contributor to the total carbon footprint is the use of protective wear and other materials for the washing and drying procedure, similar to the findings of (Sørensen & Grüttner, 2018). It follows that if it becomes possible to handle several scopes per set of protective wear, for instance, this should lead to a substantial reduction in the total carbon footprint for reusable equipment.
2.2.4 Recycling of paper, cardboard, and plastics
However, compared with model at hand, if paper, cardboard, and plastic can be fully reutilized, and the energy use for washing and storage is reduced by 50% (down to 20 kWh), both tube systems are almost on par in terms of their carbon footprint.
2.2.5 Transport
The model at hand presumed the products are produced in Europe and transported by truck. The environmental impact of other modes of transport, such as flying the same products to Europe from Asia, will introduce a significant difference. According to one study (Wernet, 2016), the CO2 eq emission for lorry transport (Euro 6) is 0,0923 kg CO2 eq per tkm and 1,17 kg CO2 eq per tkm for airfreight. That difference is at least tenfold greater, which surely would dominate a similar breakdown of results if the context used instead was airfreight transport.
3 Discussion
Single-use equipment is becoming more and more popular, chiefly due to the avoided risk of cross-contamination and patient-to-patient infections. Some evidence has been sought to address the health economics and environmental impact of implementing these new technologies, especially on large scale.
In the first part of this study a literature review was carried out to assess the status and gaps existed within this topic, especially when comparing single-use and reusable medical equipment, such as DLTs or endoscopes. We found five studies on environmental impact exist on those products as well as one resent review paper (Drew et al., 2021). Our literature search show there has been a significant increase in papers over the last 27 years on waste amounts and handling, health economics as well as the life cycle assessment of various aspects of health care. The topic on quantifying and comparing reuse and single use products combined with the economic aspects was covered in only five combined. The number of papers within the topic subjects in the literature search increased significantly in 2020 and 2021. This underlines the topic to be of increasing and significant interest as well relevant for more investigation.
In this study, we assessed a particular scenario, by comparing two different DLTs for OLV. Our findings nonetheless demonstrate a research gap regarding studies that investigate the environmental impact of single-use vs. reusable medical devices.
Our study did compare single-use DLTs with an integrated camera (VivaSight-DL) to single-use DLTs without a camera used in combination with a flexible, reusable bronchoscope. We found that VivaSight-DL has a carbon footprint of 1.25 kg CO2 eq in the contextual framework assessed in this study. A comparable tube for single-use, combined with flexible reusable scope that undergoes cleaning and drying before reused, has a total carbon footprint of 2.1 kg CO2 eq under the current framework assessed. And showed a significant potential to reduce the carbon footprint by increasing the recycling of packaging and plastics to between 0.6 kg CO2 eq and 0.3 kg CO2 eq depending on scenario.
The main uncertainties of our results are related to energy use for washing and drying, which significantly contribute to the carbon footprint. Such uncertainty admittedly makes it difficult to say, at this point, whether one solution is better than the other. The example at hand illustrates one of the important and critical points to be aware of when chosen between single-use and reuse equipment. The energy use for processing and the material uses as, e.g., for PPE is significant during reprocessing for reuse, this may become a significant contributor and change the balance between reuse or single-use to the benefit of single-use. The energy consumption in the current case, may be very uncertain in the current example and may change in the future energy system. The type of energy providers influences the carbon footprint. This is also mentioned by (McGain et al., 2020). However uncertain, the total contribution to carbon footprint is significant in this case. Focusing on the handling and process and, e.g., handle more than one or 2 items for reprocessing at the same time may reduce the influence of the mentioned aspects as, e.g., described in (Sørensen & Grüttner, 2018).
Another specific detail to be aware of in relation to environmental impact of using specific products is transport via air freight during production and distribution on the market. Air freight may influence the balance significantly. That type of carbon footprint impact will be distributed over times of uses and is therefore to the benefit of reused devices.
Nevertheless, the single-use tube does offer benefits with respect to toxicity effects because it does not contain phthalates. Using single-use tubes and equipment does generate more waste that reusable tubes. That is off course a benefit for applying the reusable framework. The handling of waste is space- and time-consuming (Lopes et al., 2019). The environmental impacts related to a device’s waste is, in some cases, possible to avoid if that waste is used for either heat and electricity production, or it is reused as illustrated in this study.
While the data presented in this study are informative for decision-makers and future environmental studies, there are several limitations that should be considered. One is that no data related to the content of phthalates was included. Secondly, significant uncertainties in the statistics used for electricity consumption prevented a firm overall conclusion for the comparison between a single-use product and reusable one.
Thirdly, no cost data was collected specifically for this study, since a previous cost-effectiveness analysis was already carried out comparing the same interventions described here, albeit only from a hospital perspective. Thus, no cost data were added to the environmental aspects of this study.
4 Conclusion
The aim of determining the status, and knowledge of balancing and quantifying environmental, economic, and social aspects in the context of medical devices was pursued. The key findings confirmed via the dearth of publicly published scientific studies addressing the process and procedure and facts involved for sustainably choosing medical equipment.
Further, the example used in this study for the particular devices of single use versus multiple use equipment demonstrated several key parameters to consider in making such choices.
The first key thing learned here is to consider the total material use product/products in question, or possible reuse. The material use must include all material, e.g., also material used for the processing of reuse itself. The current example shows significant contribution form PPE. This focus is of course eminent when considering waste materials and amounts.
Secondly, one should consider energy usage for the reprocessing impact when reusing products, since these may have an underappreciated but considerable impact on the total environmental impact of using a product. Therefore, a reusable device may not be the best choice once all other parameters are duly considered (economy and health).
Especially, this specific point of using either energy or significantly extra material when processing for reuse is where concept like circular economy may result in misinterpretation and therefore needs support from a life cycle assessment to quantify understanding exactly this point. This is a type of detail, where the circular economy concept, may result in a wrong priority and need support from, e.g., life cycle assessment.
The third key learning is when focusing on circular single-use products—where the materials are reused either via reprocessing of new types of products or back into the same type of product—is shown to be a possible way forward in terms of minimizing their overall environmental impact. Nevertheless, that is based on the ability to achieve the same quality or comparable quality of the reprocessed material.
Data availability statement
3All data generated or analyzed during this study are included in this published article.
Abbreviations
- CO2 :
-
Carbon dioxide
- DLT:
-
Double-lumen tube
- OLV:
-
One-lung ventilation
- PPE:
-
Personnel protective equipment
- SLR:
-
Systematic literature review
- CEA:
-
Cost-effectiveness analysis
- LCA:
-
Life cycle assessment
References
Agrawal, D., & Tang, Z. W. (2021). Sustainability of Single-Use Endoscopes. Techniques and Innovations in Gastrointestinal Endoscopy, 23(4), 353–362. https://doi.org/10.1016/j.tige.2021.06.001
Albert, M. G., & Rothkopf, D. M. (2015). Operating room waste reduction in plastic and hand surgery. Plastic Surgery, 23(4), 235–238.
Alkhamees, M. A. S., Alhamri, S., Ahmed, A., Yahya, G., Mohand, A., & Alothman, A. (2020). A prospective randomized cost analysis and comparison between reusable versus single-use cystoscopes procedure for removal of double J stent. European Urology Open Science, 19(Supplement 2), e1852. https://doi.org/10.1016/S2666-1683(20)33848-9
Alshemari, A., Breen, L., Quinn, G., & Sivarajah, U. (2020). Can we create a circular pharmaceutical supply chain (CPSC) to reduce medicines waste? Pharmacy, 8(4), 1–22. https://doi.org/10.3390/pharmacy8040221
Andrade, R. S., Podgaetz, E., Rueth, N. M., Majumder, K., Hall, E., Saric, C., & Thelen, L. (2014). Endobronchial Ultrasonography Versus Mediastinoscopy: A Single-Institution Cost Analysis and Waste Comparison. Annals of Thoracic Surgery, 98(3), 1003–1007. https://doi.org/10.1016/j.athoracsur.2014.04.104
Atul, P., Suresh, B., & Vandana, M. (2015). Lung isolation, one‑lung ventilation and hypoxaemia during lung isolation. 59, 606–617.
Baker, N., Bromley-Dulfano, R., Chan, J., Gupta, A., Herman, L., Jain, Navami, Taylor, A., Jonathan, Lu., Pannu, J., Patel, L., & Prunicki, M. (2020). COVID-19 Solutions Are Climate Solutions: Lessons From Reusable Gowns. Frontiers in Public Health. https://doi.org/10.3389/fpubh.2020.590275
Baxter, N. B., Yoon, A. P., & Chung, K. C. (2021). Variability in the Use of Disposable Surgical Supplies: A Surgeon Survey and Life Cycle Analysis. Journal of Hand Surgery, 46(12), 1071–1078. https://doi.org/10.1016/j.jhsa.2021.05.027
Bazin, J.-E., Koffel, C., & Dhonneur, G. (2017). Reusable versus single use fiberscope in the ICU: A medico-economical evaluation in the ICU. Annals of Intensive Care, 7(1), 91–91. https://doi.org/10.1186/s13613-016-0223-8
Belkin, N. L. (1993). Source reduction and the disposables vs. reusables debate. Regulatory analyst. Medical waste, 1(9), 6–11.
Bennett, N., Langley, R., & Reuter, G. (1998). The environmental impact of irradiation plants. Radiation Physics and Chemistry, 52(1–6), 515–517. https://doi.org/10.1016/s0969-806x(98)00040-1
Bhatter, P., Cypen, S. G., Carter, S. L., & Tao, J. P. (2021). Pharmaceutical and Supply Waste in Oculofacial Plastic Surgery at a Hospital-Based Outpatient Surgery Center. Ophthalmic Plastic and Reconstructive Surgery, 37(5), 435–438. https://doi.org/10.1097/iop.0000000000001891
Bhutta, M. F. (2021). Our over-reliance on single-use equipment in the operating theatre is misguided, irrational and harming our planet. Annals of the Royal College of Surgeons of England, 103(10), 709–712. https://doi.org/10.1308/rcsann.2021.0297
Blough, C. L., & Karsh, K. J. (2021). What’s Important: Operating Room Waste: Why We Should Care. Journal of Bone and Joint Surgery. American Volume, 103(9), 837–839. https://doi.org/10.2106/jbjs.20.01816
Bruning, L. M. (1992). Disposables v. reusables in or practice: Part II, Weighing costs, risks and wastes. Nursing management, 23(3), 72I-72K, 72N, 72P. https://doi.org/10.1097/00006247-199203000-00024
Campion, N., Thiel, C. L., Woods, N. C., Swanzy, L., Landis, A. E., & Bilec, M. M. (2015). Sustainable healthcare and environmental life-cycle impacts of disposable supplies: a focus on disposable custom packs. Journal of Cleaner Production, 94, 46–55. https://doi.org/10.1016/j.jclepro.2015.01.076
Carvalho, M., Lozano, M. A., & Serra, L. M. (2012). Multicriteria synthesis of trigeneration systems considering economic and environmental aspects. Applied Energy, 91(1), 245–254. https://doi.org/10.1016/j.apenergy.2011.09.029
Certosimo, F. J., Diefenderfer, K. E., & Mosur, M. A. (2003). Light output of disposable vs. nondisposable curing light tips following high-level disinfection. General dentistry, 51(2), 142–146.
Chang, D. F. (2020). Needless Waste and the Sustainability of Cataract Surgery. Ophthalmology, 127(12), 1600–1602. https://doi.org/10.1016/j.ophtha.2020.05.002
Chang, D. F., Thiel, C. L., Cleaning, O. I., & S. (2020). Survey of cataract surgeons’ and nurses’ attitudes toward operating room waste. Journal of Cataract and Refractive Surgery, 46(7), 933–940. https://doi.org/10.1097/j.jcrs.0000000000000267
Climate Change 2014 Synthesis Report Summary for Policymakers. (2014).
Chu, J., Ghenand, O., Collins, J., Byrne, J., Wentworth, A., Chai, P. R., Dadabhoy, F., Hur, C., & Traverso, G. (2021). Thinking green: Modelling respirator reuse strategies to reduce cost and waste. BMJ Open, 11(7), e048687. https://doi.org/10.1136/bmjopen-2021-048687
Chua, A. L. B., Amin, R., Zhang, J., Thiel, C. L., & Gross, J. S. (2021). The Environmental Impact of Interventional Radiology: An Evaluation of Greenhouse Gas Emissions from an Academic Interventional Radiology Practice. Journal of Vascular and Interventional Radiology, 32(6), 907-915.e903. https://doi.org/10.1016/j.jvir.2021.03.531
Chung, C.-Y., Peng, I. T., & Yeh, J.-C. (2020). Environmental Monitoring and Smart Garbage Sorting System Based on LoRa Wireless Transmission Technology.2nd IEEE Eurasia Conference on Biomedical Engineering, Healthcare and Sustainability 2020, ECBIOS 2020 2nd IEEE Eurasia Conference on Biomedical Engineering, Healthcare and Sustainability 2020, ECBIOS 2020, May 29, 2020 - May 31, 2020, Tainan, Taiwan.
Collins, T. A., Sparks, A. E., Walker, M. M., Kendall, L. V., Dobos, K. M., Bergdall, V. K., & Hickman-Davis, J. M. (2021). Reuse of Disposable Isolation Gowns in Rodent Facilities during a Pandemic. Journal of the American Association for Laboratory Animal Science, 60(4), 431–441. https://doi.org/10.30802/AALAS-JAALAS-20-000130
Communication, F. S. a. (2015). Safety Communications & Infections Associated with Reprocessed Flexible Bronchoscopes.
Cunningham, A. J., Krishnaswami, S., Schofield, C., & Kenron, D. (2020). Reducing Disposable Surgical Items: Decreasing Environmental Impact and Costs at a Children’s Hospital. Pediatrics, 146(1), 657–658.
Daschner, F. D., & Dettenkofer, M. (1997). Protecting the patient and the environment - New aspects and challenges in hospital infection control. Journal of Hospital Infection, 36(1), 7–15. https://doi.org/10.1016/s0195-6701(97)90086-4
Daughton, C. G., & Ruhoy, I. S. (2009). Environmental footprint of pharmaceuticals: The significance of factors beyond direct excretion to sewers. Environmental Toxicology and Chemistry, 28(12), 2495–2521. https://doi.org/10.1897/08-382.1
David, Y. (1985). The medical instrument life cycle strategy for clinical engineers. Engineering in Medicine & Biology, 4(2), 25–26.
Davis, N. F., McGrath, S., Quinlan, M., Jack, G., Lawrentschuk, N., & Bolton, D. M. (2018). Carbon Footprint in Flexible Ureteroscopy: A Comparative Study on the Environmental Impact of Reusable and Single-Use Ureteroscopes. Journal of Endourology, 32(3), 214–217. https://doi.org/10.1089/end.2018.0001
Davis, N. F., McGrath, S., Quinlan, M., Jack, G., Lawrentschuk, N., & Bolton, D. M. (2018b). Carbon Footprint in Flexible Ureteroscopy: A Comparative Study on the Environmental Impact of Reusable and Single-Use Ureteroscopes. Journal of Endourology, 32(3), 214–217. https://doi.org/10.1089/end.2018.0001
de Melo, S. W., Taylor, G. L., & Kao, J. Y. (2021). Packaging and Waste in the Endoscopy Suite. Techniques and Innovations in Gastrointestinal Endoscopy, 23(4), 371–375. https://doi.org/10.1016/j.tige.2021.07.004
Delavari, M. M., Perez-Cruz, A., & Stiharu, I. (2019). Biodegradable starch-based materials for wound dressing, monitoring, and healing.Proceedings of 30th International Conference on Adaptive Structures and Technologies, ICAST 2019 30th International Conference on Adaptive Structures and Technologies, ICAST 2019, October 7, 2019 - October 11, 2019, Montreal, QC, Canada.
Dettenkofer, M., Griesshammer, R., Scherrer, M., & Daschner, F. (1999). Life-Cycle Assessment of single-use versus reusable surgical drapes (cellulose/polyethylene mixed cotton system). Chirurg, 70(4), 485–491. https://doi.org/10.1007/s001040050677
Donahue, L. M., Hilton, S., Bell, S. G., Williams, B. C., & Keoleian, G. A. (2020). A Comparative Carbon Footprint Analysis of Disposable and Reusable Vaginal Specula. Obstetrical & Gynecological Survey, 75(6), 352–354.
Drew, J., Christie, S. D., Tyedmers, P., Smith-Forrester, J., & Rainham, D. (2021). Operating in a climate crisis: A state-of-the-science review of life cycle assessment within surgical and anesthetic care. Environmental Health Perspectives, 129(7), 076001. https://doi.org/10.1289/EHP8666
Eckelman, M., Mosher, M., Gonzalez, A., & Sherman, J. (2012). Comparative Life Cycle Assessment of Disposable and Reusable Laryngeal Mask Airways. Anesthesia and Analgesia, 114(5), 1067–1072. https://doi.org/10.1213/ANE.0b013e31824f6959
Esmizadeh, E., Chang, B. P., Jubinville, D., Ojogbo, E., Seto, C., Tzoganakis, C., & Mekonnen, T. H. (2021). Can Medical-Grade Gloves Provide Protection after Repeated Disinfection? ACS Applied Polymer Materials, 3(1), 445–454. https://doi.org/10.1021/acsapm.0c01202
Etim, M.-A., Academe, S., Emenike, PraiseGod, & Omole, David. (2021). Application of Multi-Criteria Decision Approach in the Assessment of Medical Waste Management Systems in Nigeria. Sustainability, 13(19), 10914. https://doi.org/10.3390/su131910914
Farrell, E., & Smyth, D. (2021). The environmental impact of personal protective equipment in a pre and post COVID era in the ENT clinic. European Archives of Oto-Rhino-Laryngology, 278(12), 5051–5058. https://doi.org/10.1007/s00405-021-06860-z
Feldman, L. A., & Hui, H. K. (1997). Compatibility of medical devices and materials with low-temperature hydrogen peroxide gas plasma. Medical Device and Diagnostic Industry, 19(12), 57–62.
Foundation, E. M. (2017). Circular Economy. Retrieved 19–09–2020 from https://www.ellenmacarthurfoundation.org/circular-economy/what-is-the-circular-economy
Gaberik, C., Mitchell, S., & Fayne, A. (2021). Saving lives and saving the planet: The readiness of irelands healthcare manufacturing sector for the circular economy.Smart Innovation, Systems and Technologies 7th KES International Conference on Sustainable Design and Manufacturing, KES-SDM 2020, September 9, 2020 - September 11, 2020, Split, Croatia.
Garay, O. U., Elorrio, E. G., Rodríguez, V., Spira, C., & Augustovski, & Pichon-Riviere, A. (2017). Single-Use Devices in Argentina: Cost Comparison Analysis of a “Re-Use” versus a “Single-Use” Policy for Trocars, Endocutters, Linear Cutters, and Harmonic Scalpels. Value in Health Regional Issues, 14, 89–95. https://doi.org/10.1016/j.vhri.2017.04.005
Ghodrat, M., & Samali, B. (2018). Thermodynamic analysis of incineration treatment of waste disposable syringes in an EAF steelmaking process. In Ziqi Sun, Cong Wang, Donna Post Guillen, Neale R. Neelameggham, Lei Zhang, John A. Howarter, Tao Wang, Elsa Olivetti, Mingming Zhang, Dirk Verhulst, Xiaofei Guan, Allie Anderson, Shadia Ikhmayies, York R. Smith, Amit Pandey, Sarma Pisupati, & Lu. Huimin (Eds.), Energy Technology 2018 (pp. 77–88). Cham: Springer International Publishing. https://doi.org/10.1007/978-3-319-72362-4_7
Gobbi, C. (2011). Challenges of the implementation of the WEEE Directive in the Danish context.Environmental Earth Sciences International Conference on Environment: Survival and Sustainability, February 19, 2007 - February 24, 2007, Nicosia, Cyprus.
Goel, H., Wemyss, T Alan, Harris, Tanya, Steinbach, In., Stancliffe, R., Cassels-Brown, A., Thomas, Peter B M., & Thiel, C. L. (2021). Improving productivity, costs and environmental impact in International Eye Health Services: using the ‘Eyefficiency’ cataract surgical services auditing tool to assess the value of cataract surgical services. BMJ Open Ophthalmology, 6(1), e000642. https://doi.org/10.1136/bmjophth-2020-000642
Grimmond, T. R., Bright, A., Cadman, J., Dixon, J., Ludditt, S., Robinson, C., & Topping, C. (2021). Before/after intervention study to determine impact on life-cycle carbon footprint of converting from single-use to reusable sharps containers in 40 UK NHS trusts. BMJ Open, 11(9) (no pagination), Article e046200. https://doi.org/10.1136/bmjopen-2020-046200
Gupta, D., & Wang, H. (2009). Cost-effectiveness analysis of flexible optical scopes for tracheal intubation: a descriptive comparative study of reusable and single-use scopes. Journal of Clinical Anesthesia, 632–635.
Haber, N., & Fargnoli, M. (2021). Sustainable Product-Service Systems Customization: A Case Study Research in the Medical Equipment Sector. Sustainability, 13. https://doi.org/10.3390/su13126624
Hazem, N., & Fahim, I. S. (2021). +The economic feasibility of converting agricultural waste to PLA using simventure.2021 3rd International Sustainability and Resilience Conference: Climate Change 3rd International Sustainability and Resilience Conference: Climate Change, ISRC 2021, November 15, 2021 - November 17, 2021, Virtual, Online, Bahrain.
Hemmes, M. (1991). Disposables or reusables? Try 4-step analysis. Health facilities management, 4(9), 37–38. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L21855598
Ho, G., & Copeland, R. (2020). Reducing use of polyethylene lined cups at Royal Belfast Hospital for Sick Children. Anaesthesia, 75(Supplement 2), 27. https://doi-org.proxy1-bib.sdu.dk/https://doi.org/10.1111/anae.14951
Hospodkova, P., & Vochyanova, A. (2019). The application of the total cost of ownership approach to medical equipmentcase study in the Czech Republic.IFMBE Proceedings World Congress on Medical Physics and Biomedical Engineering, WC 2018, June 3, 2018 - June 8, 2018, Prague, Czech republic.
Houngbo, P. T., Wilt, G. J. V. D., Medenou, D., Dakpanon, L. Y., Bunders, J., & Ruitenberg, J. (2008). Policy and management of medical devices for the public health care sector in Benin.IET Seminar Digest 5th IET International Seminar on Appropriate Healthcare Technologies for Developing Countries, AHT 2008, May 21, 2008 - May 22, 2008, London, United kingdom.
Hoyle, M. (2011). Accounting for the Drug Life Cycle and Future Drug Prices in Cost-Effectiveness Analysis. PharmacoEconomics, 29(1), 1–15. https://doi.org/10.2165/11584230-000000000-00000
Hsu, P.-F., Wu, C.-R., & Li, Y.-T. (2008). Selection of infectious medical waste disposal firms by using the analytic hierarchy process and sensitivity analysis. Waste Management, 28(8), 1386–1394. https://doi.org/10.1016/j.wasman.2007.05.016
Hughes, T., Pietropaolo, A., Tear, L., & Somani, B. K. (2021). Comparison of ureteric stent removal procedures using reusable and single-use disposable flexible cystoscopes following ureteroscopy and lasertripsy: A micro cost analysis. Journal of endourology, 35(SUPPL 1), A212. https://doi.org/10.1089/end.2021.35001.abstracts
Hunstiger, C. (1988). Life cycle of packaging materials in health care institutions. Tappi Journal, 71(12), 130–132.
Hunt, A. J., Dodson, J. R., Parker, H. L., Budarin, V. L., Matharu, A. S., & Clark, J. H. (2011). Industrial symbiosis and green chemistry: One's waste is another's resource!Technical Proceedings of the 2011 NSTI Nanotechnology Conference and Expo, NSTI-Nanotech 2011 Nanotechnology 2011: Electronics, Devices, Fabrication, MEMS, Fluidics and Computational - 2011 NSTI Nanotechnology Conference and Expo, NSTI-Nanotech 2011, June 13, 2011 - June 16, 2011, Boston, MA, United states.
Ibbotson, S., Dettmer, T., Kara, S., & Herrmann, C. (2013). Eco-efficiency of disposable and reusable surgical instruments - a sciccors case. International Journal of Life Cycle Assessment, 18, 1137–1148.
ISO/TC207/SC5. (2016). ISO 14040:2006, Environmental management — Life cycle assessment — Principles and framework. In. 13.020.10 Environmental management 13.020.60 Product life-cycles.
Iyer, V. G. (2018). Strategic Environmental Assessment (SEA) Process for Green Materials and Environmental Engineering Systems towards Sustainable Development-Business Excellence Achievements. In 2018 4th International Conference on Green Materials and Environmental Engineering. Destech Publicat, Inc. <Go to ISI>://WOS:000468579900025
Jordan, J. W. (1996). Waste and cost avoidance practices in New York City hospitals: five years of waste prevention, reuse and recycling and the impacts on the waste management infrastructure. In Proceedings of the Air Waste Management Association's Annual Meeting Exhibition Proceedings of the 1996 Air & Waste Management Association's 89th Annual Meeting & Exhibition, June 23, 1996 - June 28, 1996, Nashville, TN, USA.
Kane, G. M., Bakker, C. A., & Balkenende, A. R. (2018). Towards design strategies for circular medical products. Resources, Conservation and Recycling, 135, 38–47. https://doi.org/10.1016/j.resconrec.2017.07.030
Keyes, J. A., Bretz, J. F., & Moore, A. (1993). Development of a medical image capture, formatting, and display system in support of a medical diagnostic center. In Proceedings of SPIE - The International Society for Optical Engineering Medical Imaging 1993: Image Capture, Formatting, and Display, January 17, 1993 - January 22, 1993, Newport Beach, CA, USA.
Khan, M. R., & Ali, Z. (2014). Production of thermoelectric power from the infectious waste of hospitals of Lahore. InProceedings of the 2014 International Conference and Utility Exhibition on Green Energy for Sustainable Development, ICUE 2014 2014 International Conference and Utility Exhibition on Green Energy for Sustainable Development, ICUE 2014, March 19, 2014 - March 21, 2014, Pattaya, Thailand.
Kim, J. S., Dowdell, J., Cheung, Z. B., Arvind, V., Sun, L., Jandhyala, C., Ukogu, C., Ranson, W., Jacobs, S., McAnany, S., & Cho, S. K. W. (2018). The Seven-Year Cost-Effectiveness of Anterior Cervical Discectomy and Fusion Versus Cervical Disc Arthroplasty A Markov Analysis. Spine, 43(22), 1543–1551. https://doi.org/10.1097/brs.0000000000002665
Koch, F., & James, E. (1995). Single-use/multiple-use gowns and drapes: Criteria for decision making. Today’s OR Nurse, 17(2), 21–25.
Koleva, J., Peters, F., Van Der Mai, H., & Degener, J. (2013). Transmission of Infection by Flexible Gastrointestinal Endoscopy and Bronchoscopy.
Korambayil, S., Iyer, S., & Cross, K. (2020). A greener NHS: An overview of sustainable development practices in a rural district general hospital. British Journal of Surgery, 107(SUPPL 3), 15. https://doi.org/10.1002/bjs.11641
Kumar, P. A. (2021). Regulating Environmental Impact of Medical Devices in the United Kingdom-A Scoping Review. Prosthesis, 3(4), 370–387. https://doi.org/10.3390/prosthesis3040033
Kwakye, G., Pronovost, P. J., & Makary, M. A. (2010). Commentary: A Call to Go Green in Health Care by Reprocessing Medical Equipment. Academic Medicine, 85(3), 398–400. https://doi.org/10.1097/ACM.0b013e3181cd5a71
Larsen, S., Holm, J. H., Sauer, T. N., & Andersen, C. (2019). A Cost-effectiveness Analysis Comparing the VivaSight Double-lumen Tube to a Conventional. Pharmaco Economics.
Latta, M., Shaw, C., & Gale, J. (2021). The carbon footprint of cataract surgery in Wellington. New Zealand Medical Journal, 134(1541), 13–21.
Lee, J. Y., & Kim, K.-Y. (2019). Semantic and Association Rule Mining-based Knowledge Extension for Reusable Medical Equipment Random Forest Rules. Journal of Integrated Design and Process Science, 22(4), 55–81. https://doi.org/10.3233/JID180011
Leiden, A., Cerdas, F., Noriega, D., Beyerlein, J., & Herrmann, C. (2020). Life cycle assessment of a disposable and a reusable surgery instrument set for spinal fusion surgeries. Resources, Conservation and Recycling, 156, 104704. https://doi.org/10.1016/j.resconrec.2020.104704
Limani, F., Garley, D., Cocker, D., Patel, P., Patel, P., Gordon, S., Nyirenda, M., Sakala, S., Gadama, L. A., Dube, Q., Bodole, F., Mndolo, Kwazizira Samson, Mponda, K., & Freyne, B. (2021). Lessons learnt from the rapid implementation of reusable personal protective equipment for COVID-19 in Malawi. BMJ Global Health, 6(9), e006498. https://doi.org/10.1136/bmjgh-2021-006498
Lopes, C., Scavarda, A., de Carvalho, M., Vaccaro, G., & Korzenowski, A. (2019). Analysis of Sustainability in Hospital Laundry: The Social, Environmental, and Economic (Cost) Risks. Resources, 8(1), 37. https://doi.org/10.3390/resources8010037
MacNeill, A. J., Hopf, H., Khanuja, A., Alizamir, S., Bilec, M., Eckelman, M. J., Hernandez, L., McGain, F., Simonsen, K., Thiel, C., Young, S., Lagasse, R., & Sherman, J. D. (2020). Transforming The Medical Device Industry: Road Map To A Circular Economy. Health Affairs, 39(12), 2088–2097. https://doi.org/10.1377/hlthaff.2020.01118
Manns, B. J., Taub, K., Richardson, R. M. A., & Donaldson, C. (2002). To reuse or not to reuse? An economic evaluation of hemodialyzer reuse versus conventional single-use hemodialysis for chronic hemodialysis patients. International Journal of Technology Assessment in Health Care, 18(1), 81–93. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L34408531
Marshall, D. C., Dagaonkar, R. S., Yeow, C., Peters, A. T., Tan, S. K., Tai, D. Y. H., Gohs, S. K., Lim, A. Y. H., Ho, B., Lew, S. J. W., Abisheganaden, J., & Verma, A. (2017, April). Experience with the Use of Single-Use Disposable Bronchoscope in the ICU in a Tertiary Referral Center of Singapore. Journal of Bronchology & Interventional Pulmonolog, 136–143.
Massot, Julien, Dumand-Nizard, Virginie, Fischler, Marc, & Le Guen, Morgan. (2015). Evaluation of the Double-Lumen Tube Vivasight-DL (DLT-ETView): A Prospective Single-Center Study. Journal of Cardiothoracic and Vascular Anesthesia, 29(6), 1544–1549. https://doi.org/10.1053/j.jvca.2015.04.031
McCahon, R. A., & Whynes, D. K. (2015). Cost comparison of re-usable and single-use fibrescopes in a large English teaching hospital. Anaesthesia, 70(6), 699–706. https://doi.org/10.1111/anae.13011
McGain, F., McAlister, S., McGavin, A., & Story, D. (2010). The financial and environmental costs of reusable and single-use plastic anaesthetic drug trays. Anaesthesia and Intensive Care, 38(3), 538–544. <Go to ISI>://WOS:000277917400020
McGain, F., McAlister, S., McGavin, A., & Story, D. (2012). A life cycle assessment of reusable and single-use central venous catheter insertion kits. Anesthesia and Analgesia, 114(5), 1073–1080. https://doi.org/10.1213/ANE.0b013e31824e9b69
McGain, F., Muret, J., Lawson, C., & Sherman, J. D. (2020). Environmental sustainability in anaesthesia and critical care. British Journal of Anaesthesia, 125(5), 680–692. https://doi.org/10.1016/j.bja.2020.06.055
McGain, F., Story, D., Lim, T., & McAlister, S. (2017). Financial and environmental costs of reusable and single-use anaesthetic equipment. British Journal of Anaesthesia, 118(6), 862–869. https://doi.org/10.1093/bja/aex098
Miljøstyrelsen. (2018). Affaldsstatistik 2018 (978–87–7038–183–3). https://mst.dk/service/publikationer/publikationsarkiv/2020/maj/affaldsstatistik-2018/
Miniati, R., Dori, F., Cecconi, G., Gusinu, R., Niccolini, F., & Gentili, G. B. (2013). HTA decision support system for sustainable business continuity management in hospitals. The case of surgical activity at the University Hospital in Florence. Technology and Health Care, 21(1), 49–61. https://doi.org/10.3233/thc-120709
Monmousseau, F., Ramillon, J., Dubnitskiy-Robin, S., Faivre D'Arcier, B., Le Verger, M., Le Fol, T., Bruyere, F., Rusch, E., Brunet-Houdard, S., & Pradere, B. (2021). Relevance of adopting a hybrid strategy mixing single-use and reusable ureteroscopes for stones management: An economic study to support the best strategy. Journal of Clinical Medicine, 10(12) (no pagination), Article 2593. https://doi.org/10.3390/jcm10122593
Morton, H., & Baxter, I. (2021). Save money and the planet: Closing the audit loop on recycling and waste disposal in the operating department. Anaesthesia, 76(SUPPL 2), 68. https://doi.org/10.1111/anae.15336
Moultrie, J., Sutcliffe, L., & Maier, A. (2015). Exploratory study of the state of environmentally conscious design in the medical device industry. Journal of Cleaner Production, 108, 363–376. https://doi.org/10.1016/j.jclepro.2015.06.014
Murphy, L. (1993). Cost/benefit study of reusable and disposable OR draping materials. Journal of Healthcare Materiel Management, 11(3), 44–48.
Namburar, Sathvik, von Renteln, Daniel, Damianos, John, Bradish, Lisa, Barrett, Jeanne, Aguilera-Fish, Andres, Cushman-Roisin, Benoit, & Pohl, Heiko. (2021). Estimating the environmental impact of disposable endoscopic equipment and endoscopes. Gut, 71(7), 1326–1331. https://doi.org/10.1136/gutjnl-2021-324729
Nations, U. (2015b). Sustainable Dvelopment Goal 12 Ensure sustainable consumption and production patterns. https://www.un.org/sustainabledevelopment/sustainable-consumption-production/
Nations, U. (2015a). Sustainable Development Goals, 17 Goals to Transform our World. https://www.un.org/sustainabledevelopment/sustainable-development-goals/
Nieto, I., Murillo, S., Rojo, M., & Asai, M. (2008). Environmental protection and biosecurity program at the National Institute of Psychiatry Ramon de la Fuente. Salud Mental, 31(2), 111–117.
Niyongabo, E., Jang, Y. C., Kang, D., & Sung, K. (2019). Current treatment and disposal practices for medical wastes in Bujumbura. Burundi. Environmental Engineering Research, 24(2), 211–219. https://doi.org/10.4491/eer.2018.095
Oderda, M., Delarosette, J., Doizi, S., Estrade, V., Falcone, M., Grey, B., Knudsen, B., Olsburg, J., Rukin, N., & Gontero, P. (2020). The impact of single-use digital flexible cystoscope for double j removal on hospital costs and work organization in different health systems worldwide: A multicentric evaluation. Journal of Urology, 203(Supplement 4), e1046–e1047.
Ofstead, C., Quick, M., Eiland, J., & Adams, S. (2017). A glimpse at the true cost of reprocessing endoscopes: Results of a pilot project.
Ordway, A., Pitonyak, J. S., & Johnson, K. L. (2020). Durable medical equipment reuse and recycling: Uncovering hidden opportunities for reducing medical waste. Disability and Rehabilitation: Assistive Technology, 15(1), 21–28. https://doi.org/10.1080/17483107.2018.1508516
Ortsäter, G., Borgström, F., Soulard, S., & Miltenburger, C. (2019). A Budget Impact Model to Estimate the Environmental Impact of Adopting RESPIMAT® Re-usable in the Nordics and Benelux. Advances in Therapy, 36(12), 3435–3445. https://doi.org/10.1007/s12325-019-01114-1
Ouda, B. K., Saleh, N. S. K., & Mohamed, A. S. A. (2012). The effect of useful life and vendor performance on replacement decision of medical equipment.2012 Cairo International Biomedical Engineering Conference, CIBEC 2012 2012 Cairo International Biomedical Engineering Conference, CIBEC 2012, December 20, 2012 - December 22, 2012, Giza, Egypt.
Park, E. A., & LaMattina, K. C. (2020). Economic and Environmental Impact of Single-use Plastics at a Large Ophthalmology Outpatient Service. Journal of Glaucoma, 29(12), 1179–1183. https://doi.org/10.1097/ijg.0000000000001655
Parsons, M. S. (1998). The dilemma over reprocessing single-use medical devices. Journal of Healthcare Risk Management : The Journal of the American Society for Healthcare Risk Management, 18(4), 54–61. https://doi.org/10.1002/jhrm.5600180406
Pascual, C. D., & Subra-Paternault, P. (2015). Supercritical Fluid Nanotechnology: Advances and Applications in Composites and Hybrid Nanomaterials. Jenny Stanford Publishing. https://doi.org/10.1201/b19242
Perbet, S., Blanquet, M., Mourgues, C., Delmas, J., Bertran, S., Longères, Boïko-Alaux, V., Chennell, P., Bazin , J.-E., & Constantin, J.-M. (2017). Cost analysis of single-use (Ambu® aScope™) and reusable bronchoscopes in the ICU. Annals of Intensive Care.
Petre, M. A., & Malherbe, S. Environmentally sustainable perioperative medicine: simple strategies for anesthetic practice. Canadian Journal of Anesthesia-Journal Canadien D Anesthesie. https://doi.org/10.1007/s12630-020-01726-0
Pietropaolo, A., Hughes, T., Tear, L., & Somani, B. K. (2020). Comparison of ureteric stent removal procedures using reusable and single-use flexible cystoscopes following ureteroscopy and lasertripsy: A micro cost analysis. Central European Journal of Urology, 73(3), 342–348. https://doi.org/10.5173/ceju.2020.0159
PlasticEurope. (2019). Plastics - The Facts 2019. In (Vol. 2020): PlasticsEurope.
Poh, P., Dattani-Patel, R., & Ang, K. (2021). Stop the plastic tide. Anaesthesia, 76(SUPPL 6), 23. https://doi.org/10.1111/anae.15578
Poore, J., & Nemecek, T. (2018). Reducing food’s environmental impacts through producers and consumers. Science, 360, 987–992.
Power, N., Guillonneau, B., & Touijer, K. (2011). Carbon footprint of laparoscopy in the United States. European Urology, Supplements, 10(2), 303–303. https://doi.org/10.1016/S1569-9056(11)60954-8
Pryor, K. H. (2016). END OF LIFE DECISIONS FOR SEALED RADIOACTIVE SOURCES. Health Physics, 110(2), 168–174. https://doi.org/10.1097/hp.0000000000000398
Putri, C. A., Rezai, P., & Currie, Z. (2019). Cost analysis of disposable versus non-disposable instruments for oculoplastics minor operations. Investigative Ophthalmology and Visual Science, 60(9). http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L629939309
Putri, C. A., Rezai, P., Capel, J., & Currie, Z. (2021). Money, environment and eyelids. Eye (Basingstoke), 35(9), 2653–2654. https://doi.org/10.1038/s41433-020-01189-z
Rajaduraia, M., Chawlab, S., & Satheeshc, M. A. (2021). Economic impact and challenges in waste management. Journal of Pharmaceutical Sciences and Research, 13(3), 179–187.
Rapchuk, I., Kunju, S., & Faulke, D. (2017). Papers A six-month evaluation of the VivaSight TM video double-lumen endotracheal tube after introduction into thoracic anaesthetic practice at a single institution. Anaesth Intesive Care, 45(2), 189–196.
Rebehy, P., Lima, S. A. D., Novi, J. C., & Salgado, A. P. (2019). Reverse logistics systems in Brazil: Comparative study and interest of multistakeholders. Journal of Environmental Management. https://doi.org/10.1016/j.jenvman.2019.06.124
Renton, D., Denk, P., & Varban, O. (2018). Reprocessed single-use devices in laparoscopy: Assessment of cost, environmental impact, and patient safety. Surgical Endoscopy, 32(10), 4310–4313. https://doi.org/10.1007/s00464-018-6275-0
Reynier, T., Berahou, M., Albaladejo, P., & Beloeil, H. (2021). Moving towards green anaesthesia: Are patient safety and environmentally friendly practices compatible? A focus on single-use devices: Anaesthesia Critical Care & Pain Medicine. https://doi.org/10.1016/j.accpm.2021.100907
Rizan, C., & Bhutta, M. F. (2021). Environmental impact and life cycle financial cost of hybrid (reusable/single-use) instruments versus single-use equivalents in laparoscopic cholecystectomy. Surgical Endoscopy. https://doi.org/10.1007/s00464-021-08728-z
Rizan, C., Bhutta, M. F., Reed, M., & Lillywhite, R. (2021). The carbon footprint of waste streams in a UK hospital. Journal of Cleaner Production. https://doi.org/10.1016/j.jclepro.2020.125446
Rizan, C., Reed, M., & Bhutta, M. F. (2021b). Environmental impact of personal protective equipment distributed for use by health and social care services in England in the first six months of the COVID-19 pandemic. Journal of the Royal Society of Medicine, 114(5), 250–263. https://doi.org/10.1177/01410768211001583
Rizan, C., Steinbach, I., Nicholson, R., Lillywhite, R., Reed, M., & Bhutta, M. F. (2020). The Carbon Footprint of Surgical Operations A Systematic Review. Annals of Surgery, 272(6), 986–995. https://doi.org/10.1097/sla.0000000000003951
Romig, L. A., Hudak, D., & Barnard, J. (2005). Scrub or toss? Making the case for disposable laryngoscope blades. Emergency medical services, 34(3), 91–94,120. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L40671821
Rutala, W. A., & Weber, D. J. (2001). A review of single-use and reusable gowns and drapes in health care. Infection Control and Hospital Epidemiology, 22(4), 248–257. https://doi.org/10.1086/501895
Sanchez, S. A., Eckelman, M. J., & Sherman, J. D. (2020). Environmental and economic comparison of reusable and disposable blood pressure cuffs in multiple clinical settings. Resources, Conservation and Recycling. https://doi.org/10.1016/j.resconrec.2019.104643
Sarancha, V., Mirsic, L., Oreskovic, S., Sulyma, V., Kranjcec, B., & Vitale, K. (2021). Life Cycle Assessment and Management in Hospital Units Using Applicable and Robust Dual Group-Based Parameter Model.Smart Innovation, Systems and Technologies 4th International Conference on Information and Communication Technology for Intelligent Systems, ICTIS 2020, May 15, 2020 - May 16, 2020, Ahmedabad, India.
Scowen, P. (1994). Disposables versus reusables: the nappy debate continues. Professional care of mother and child, 4(4), 119–120. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L126255736
Shaw, M. A. (2003). Sustainability principles for product design.Design and Manufacture for Sustainable Development 2003 Design and Manufacture for Sustainable Development 2003, September 3, 2003 - September 4, 2003, Cambridge, United kingdom.
Sherman, J. D., Raibley, L. A., & Eckelman, M. J. (2018). Life Cycle Assessment and Costing Methods for Device Procurement: Comparing Reusable and Single-Use Disposable Laryngoscopes. Anesthesia and Analgesia, 127(2), 434–443. https://doi.org/10.1213/ane.0000000000002683
Sherman, J. D., Thiel, C., MacNeill, A., Eckelman, M. J., Dubrow, R., Hopf, H., Lagasse, R., Bialowitz, J., Costello, A., Forbes, M., Stancliffe, R., Anastas, P., Anderko, L., Baratz, M., Barna, S., Bhatnagar, U., Burnham, J., Cai, Y., Cassels-Brown, A., & Bilec, M. M. (2020). The Green Print: Advancement of Environmental Sustainability in Healthcare. Resources, Conservation and Recycling. https://doi.org/10.1016/j.resconrec.2020.104882
Shivakumar, N. S., Arora, M., & Mani, M. (2018). A Proposed Design of an Universal Electrochemical Reader Based on a Collated Medical Device Innovation Framework and Systems Thinking.Proceedings of the 4th International Conference on Biosignals, Images and Instrumentation, ICBSII 2018 4th International Conference on Biosignals, Images and Instrumentation, ICBSII 2018, March 22, 2018 - March 24, 2018, Chennai, India.
Sørensen, B. L., & Grüttner, H. (2018). Comparative Study on Environmental Impacts of Reusable and Single-Use Bronchoscopes. American Journal of Environmental Protection, 7(4). https://doi.org/10.11648/j.ajep.20180704.11
Stern, A., & Dickinson, E. (1994). Disposables vs. reusables. Throw and go vs. use and reuse. JEMS : a journal of emergency medical services, 19(11), 77–79,81.
Stutman, M. B. (2010). Using field measurements of air filter performance and HVAC fan energy measurements to select air filters with lowest life cycle cost.World Energy Engineering Congress, 2010Stutman, M. B. (2010). Using field measurements of air filter performance and HVAC fan energy measurements to select air filters with lowest life cycle cost.World Energy Engineering Congress 2010, WEEC 2010 World Energy Engineering Congress 2010, WEEC 2010, December 8, 2010 - December 10, 2010, Washington, DC, United states.
Stutman, M. (2012). Using field measurements of air filter performance and HVAC fan energy measurements to select air filters with lowest life cycle cost. Strategic Planning for Energy and the Environment, 32(1), 26–41. https://doi.org/10.1080/10485236.2012.10531826
Sundhedsdatastyrelsen. (2020). Landspatientregisteret. http://end2019.esundhed.dk/sundhedsregistre/LPR/Sider/LPR06A.aspx
Sustainability, P. (2020). SimaPro database manual. https://simapro.com/wp-content/uploads/2020/10/DatabaseManualMethods.pdf
Take urgent action to combat climate change and its impacts. (2015). https://www.un.org/sustainabledevelopment/climate-change-2/
Terjesen, C., Kolaleva, J., & Ehlers, L. (2017). Assessment of the Likely Cost Effectiveness of Single-Use Flexible Video Bronchoscopes. Pharmaco Economics, 133–141.
Thiel, C. L., Eckelman, M., Guido, R., Huddleston, M., Landis, A. E., Sherman, J., Shrake, S. O., Copley-Woods, N., & Bilec, M. M. (2015). Environmental impacts of surgical procedures: Life cycle assessment of hysterectomy in the United States. Environmental Science and Technology, 49(3), 1779–1786. https://doi.org/10.1021/es504719g
Thiel, C. L., Woods, N. C., & Bilec, M. M. (2018). Strategies to Reduce Greenhouse Gas Emissions from Laparoscopic Surgery. American Journal of Public Health, 108, S158–S164. https://doi.org/10.2105/ajph.2018.304397
Trindade, A. J., Copland, A., Bhatt, A., Bucobo, J. C., Chandrasekhara, V., Krishnan, K., Parsi, M. A., Kumta, N., Law, R., Pannala, R., Rahimi, E. F., Saumoy, M., Trikudanathan, G., Yang, J., & Lichtenstein, D. R. (2021). Single-use duodenoscopes and duodenoscopes with disposable end caps. Gastrointestinal Endoscopy, 93(5), 997–1005. https://doi.org/10.1016/j.gie.2020.12.033
Tudor, T. L., Noonan, C. L., & Jenkin, L. E. (2005). Healthcare waste management: A case study from the National Health Service in Cornwall. United Kingdom. Waste Manag, 25(6), 606–615. https://doi.org/10.1016/j.wasman.2004.10.004
Tvede, M. F., Kristensen, M. S., & Nyhus-Andreasen, M. (2012). A cost analysis of reusable and disposable flexible optical scopes for intubation. ACTA ANAESTHESIOLOGICA SCANDINAVICA, 577-584.
Unger, S. R., Campion, N., Bilec, M. M., & Landis, A. E. (2016). Evaluating quantifiable metrics for hospital green checklists. Journal of Cleaner Production, 127, 134–142. https://doi.org/10.1016/j.jclepro.2016.03.167
Unger, S., & Landis, A. (2016). Assessing the environmental, human health, and economic impacts of reprocessed medical devices in a Phoenix hospital’s supply chain. Journal of Cleaner Production, 112, 1995–2003. https://doi.org/10.1016/j.jclepro.2015.07.144
Urban, P., & Fernandez-Busquets, X. (2014). Nanomedicine Against Malaria. Current Medicinal Chemistry, 21(5), 605–629. https://doi.org/10.2174/09298673113206660292
van Straten, B., Ligtelijn, S., Droog, L., Putman, E., Dankelman, J., Weiland, N. H. S., & Horeman, T. (2021). A life cycle assessment of reprocessing face masks during the Covid-19 pandemic. Scientific Reports. https://doi.org/10.1038/s41598-021-97188-5
Viana, C., Vaccari, M., & Tudor, T. (2016). Recovering value from used medical instruments: A case study of laryngoscopes in England and Italy (pp. 1–9). Conservation and Recycling: Resources.
Wallace, J., Evans, V., Sanu, A., Howard, A., & Berry, S. (2021). Single use nasal endoscopes a review of the cost and organisational implications based on department size. British Journal of Surgery. https://doi.org/10.1093/bjs/znab259.558
Webb, S. R. (2002). Single-use disposable barrier reduces microbial concentrations on BP cuffs. Dialysis & Transplantation, 31(5), 337-+. <Go to ISI>://WOS:000175256700014
Wernet, G., Bauer, C., Steubing, B., Reinhard, J., Moreno-Ruiz, E., & Weidema, B. (2016). The ecoinvent database version 3 (part I): Overview and methodology. The International Journal of Life Cycle Assessment, 21, 1218–1123.
Whitaker, M. W. (1992). Health care: A leader or a follower? Reducing disposable waste. Hospital Materiel Management Quarterly, 14(1), 1–10.
Wu, S., & Cerceo, E. (2021). Sustainability Initiatives in the Operating Room. Joint Commission Journal on Quality and Patient Safety, 47(10), 663–672. https://doi.org/10.1016/j.jcjq.2021.06.010
Xu, X., Nardini, H. K. G., & Ruger, J. P. (2014). Micro-costing studies in the health and medical literature: Protocol for a systematic review. Systematic Reviews, 3(1), 47. https://doi.org/10.1186/2046-4053-3-47
Yang, J., Wang, B., Fan, C., & Wang, L. (2011). A new single-end mainstream CO2 capnograph. Computer Methods in Biomechanics and Biomedical Engineering, 14(12), 1033–1039. https://doi.org/10.1080/10255842.2010.504923
Zawierucha, J. P., Prystacki, T. R., Marcinkowski, W., & Malyszko, J. (2020). Medical waste management: How industry can help us protect the environment and money. Journal of the American Society of Nephrology, 31, 818.
Żebrowski, P., Zawierucha, J., Prystacki, T., Marcinkowski, W., & Małyszko, J. (2020). Medical waste management - how industry can help us to protect environment and money? Renal Failure, 42(1), 547–549. https://doi.org/10.1080/0886022x.2020.1774900
Acknowledgements
We thank AMBU A/S for making part of this work possible by contributing with data needed on products for the analysis as well as supported the project with 100.000 DKK.
Partial financial support was received from AMBU A/S, Ballerup, Denmark. They have supported the project with 100.000 DKK. AMBU A/S, Ballerup, Denmark, have provided data on content and amount of material in the products. Author Sara Larsen was employed by AMBU A/S, Ballerup, Denmark, during the genesis of this papers 1st draft.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Authors Birgitte Lilholt Sørensen and Claus Andersen do not have no financial interest to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendix 1. Publication records used in the systematic literature review – publications marked bold are included in Table 3
Appendix 1. Publication records used in the systematic literature review – publications marked bold are included in Table 3
Reference | Topics | Single-use vs. reuse |
|---|---|---|
(Agrawal & Tang, 2021) | Qualitative environmental & economic considerations | X |
(Albert & Rothkopf, 2015) | Economics & waste reduction | |
(Alkhamees et al., 2020) | Health economics | X |
(Alshemari et al., 2020) | Medical waste reduction | |
(Andrade et al., 2014) | Economics & waste reduction | |
(Baker et al., 2020) | Medical waste reduction | X |
(Baxter et al., 2021) | Life cycle assessment | |
(Bazin et al., 2017) | Health economics | X |
(Belkin, 1993) | Medical waste reduction | X |
(Bennett et al., 1998) | Life cycle assessment | |
(Bhatter et al., 2021) | Medical waste reduction | |
(Bhutta, 2021) | Life cycle assessment | X |
(Blough & Karsh, 2021) | Medical waste reduction | |
(Bruning, 1992) | Economics & waste reduction | X |
(Carvalho et al., 2012) | Economics & life cycle assessment | |
(Certosimo et al., 2003) | Health economics | |
(Chang et al., 2020) | Medical waste reduction | |
(Chang, 2020) | Medical waste reduction | |
(Chu et al., 2021) | Economics & waste reduction | |
(Chua et al., 2021) | Life cycle assessment | |
(Chung et al., 2020) | Medical waste reduction | |
(Collins et al., 2021) | Health economics | X |
(Cunningham et al., 2020) | Economics & waste reduction | |
(Daschner & Dettenkofer, 1997) | Medical waste reduction | |
(Daughton & Ruhoy, 2009) | Medical waste reduction | |
(David, 1985) | Life cycle assessment | |
(de Melo et al., 2021) | Medical waste reduction | X |
(Delavari et al., 2019) | Qualitative environmental & economic considerations | |
(Dettenkofer et al., 1999) | Life cycle assessment | |
(Domingo, 2015) | Qualitative environmental & economic considerations | |
(Donahue et al., 2020) | Life cycle assessment | X |
(Drew et al., 2021) | Life cycle assessment | |
(Eckelman et al., 2012) | Economics & life cycle assessment | X |
(Esmizadeh et al., 2021) | Qualitative environmental & economic considerations | X |
(Etim et al., 2021) | Medical waste reduction | |
(Farrell & Smyth, 2021) | Medical waste reduction | |
(Feldman & Hui, 1997) | Health economics | |
(Gaberik et al., 2021) | Qualitative environmental & economic considerations | |
(Garay et al., 2017) | Health economics | X |
(Ghodrat & Samali, 2018) | Economics & environment | |
(Gobbi, 2011) | Economics & waste reduction | |
(Goel et al., 2021) | Life cycle assessment | |
(Grimmond et al., 2021) | Life cycle assessment | X |
(Hazem & Fahim, 2021) | Economics & waste reduction | |
(Hemmes, 1991) | Health economics | X |
(Ho & Copeland, 2020) | Qualitative environmental & economic considerations | |
(Hospodkova & Vochyanova, 2019) | Health economics | |
(Houngbo et al., 2008) | Health economics | |
(Hoyle, 2011) | Health economics | |
(Hsu et al., 2008) | Health economics | |
(Hughes et al., 2021) | Health economics | X |
(Hunstiger, 1988) | Health economics | |
(Hunt et al., 2011) | Qualitative environmental & economic considerations | |
(Iyer, 2018) | Life cycle assessment | |
(Jordan, 1996) | Economics & waste reduction | |
(Kane et al., 2018) | Economics & environment | |
(Keyes et al., 1993) | Health economics | |
(Khan & Ali, 2014) | Medical waste reduction | |
(Kim et al., 2018) | Health economics | |
(Koch & James, 1995) | Health economics | X |
(Korambayil et al., 2020) | Economics & life cycle assessment | |
(Kumar, 2021) | Qualitative environmental & economic considerations | |
(Kwakye et al., 2010) | Economics & environment | X |
(Larsen et al., 2019) | Health economics | X |
(Latta et al., 2021) | Life cycle assessment | |
(Lee & Kim, 2019) | Health economics | X |
(Leiden et al., 2020) | Life cycle assessment | X |
(Limani et al., 2021) | Qualitative environmental & economic considerations | X |
(Lopes et al., 2019) | Economics & life cycle assessment | |
(MacNeill et al., 2020) | Qualitative environmental & economic considerations | |
(Manns et al., 2002) | Health economics | X |
(McGain et al., 2010) | Life cycle assessment | X |
(McGain et al., 2012) | Life cycle assessment | |
(McGain et al., 2017) | Economics & life cycle assessment | X |
(McGain et al., 2020) | Life cycle assessment | X |
(Miniati et al., 2013) | Health economics | |
(Monmousseau et al., 2021) | Health economics | |
(Morton & Baxter, 2021) | Medical waste reduction | |
(Moultrie et al., 2015) | Life cycle assessment | |
(Murphy, 1993) | Health economics | X |
(Namburar et al. 2021) | Medical waste reduction | |
Life cycle assessment | X | |
(Nieto et al., 2008) | Medical waste reduction | |
(Niyongabo et al., 2019) | Medical waste reduction | |
(Oderda et al., 2020) | Health economics | X |
(Ortsäter et al.,,2019) | Health economics | X |
(Ouda et al., 2012) | Economics & waste reduction | |
(Park & LaMattina, 2020) | Economics & waste reduction | |
(Parsons, 1998) | Health economics | X |
(Petre & Malherbe, 2020) | Economics & waste reduction | |
(Pietropaolo et al., 2020) | Health economics | X |
(Poh et al., 2021) | Medical waste reduction | |
(Power et al., 2011) | Life cycle assessment | |
(Pryor, 2016) | Medical waste reduction | |
(Putri et al., 2019) | Economics & environment | X |
(Putri et al., 2021) | Economics & environment | |
(Rajaduraia et al., 2021) | Economics & waste reduction | |
(Rebehy et al., 2019) | Medical waste reduction | |
(Renton et al., 2018) | Economics & life cycle assessment | |
(Reynier et al., 2021) | Economics & environment | |
(Rizan et al., 2020) | Life cycle assessment | |
Economics & life cycle assessment | X | |
(Rizan, Bhutta, et al., 2021) | Life cycle assessment | |
Life cycle assessment | ||
(Romig et al., 2005) | Health economics | X |
(Rutala & Weber, 2001) | Life cycle assessment | X |
(Sanchez et al., 2020) | Economics & life cycle assessment | X |
(Sarancha et al., 2021) | Life cycle assessment | |
(Scowen, 1994) | Qualitative environmental & economic considerations | X |
(Shaw, 2003) | Economics & environment | X |
(Sherman et al., 2018) | Economics & environment | X |
(Sherman et al., 2020) | Economics & environment | |
(Shivakumar et al., 2018) | Economics & environment | X |
(Sørensen & Grüttner, 2018) | Life cycle assessment | X |
(Stern & Dickinson, 1994) | Economics & environment | X |
(Stutman, 2010) | Economics & life cycle assessment | |
(Stutman, 2012) | Economics & life cycle assessment | |
(Thiel et al., 2015) | Life cycle assessment | |
(Thiel et al., 2018) | Life cycle assessment | |
(Trindade et al., 2021) | Qualitative environmental & economic considerations | X |
(Tudor et al., 2005) | Medical waste reduction | |
(Unger & Landis, 2016) | Life cycle assessment | |
(Unger et al., 2016) | Health economics | |
(Urban & Fernandez-Busquets, 2014) | Economics & environment | |
(van Straten et al., 2021) | Life cycle assessment | |
(Viana et al., 2016) | Medical waste reduction | |
(Wallace et al., 2021) | Health economics | X |
(Webb, 2002) | Health economics | |
(Whitaker, 1992) | Medical waste reduction | |
(Wu & Cerceo, 2021) | Qualitative environmental & economic considerations | |
(Yang et al., 2011) | Life cycle assessment | |
(Zawierucha et al., 2020) | Medical waste reduction | |
(Żebrowski et al., 2020) | Economics & waste reduction |
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Sørensen, B.L., Larsen, S. & Andersen, C. A review of environmental and economic aspects of medical devices, illustrated with a comparative study of double-lumen tubes used for one-lung ventilation. Environ Dev Sustain 25, 13219–13252 (2023). https://doi.org/10.1007/s10668-022-02611-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10668-022-02611-0