Abstract
Metals play an important role in the development of diabetes mellitus (DM). The association of metals with diabetes among the Dong ethnicity in China remains poorly understood. The current study aimed to evaluate the association of single metal exposure and multi-metal co-exposure with DM risk. Urinary concentrations of arsenic, cadmium, chromium, copper, iron, lead, manganese, mercury, molybdenum, nickel, strontium, vanadium, and zinc were measured using inductively coupled plasma-mass spectrometry (ICP-MS) among 4479 Dong ethnic participants aged 30–79 years from the China Multi-Ethnic Cohort (CMEC) study. Based on tertiles, the metal exposure can be divided into three groups: low, middle, and high exposure. Multivariate logistic regression models and principal component analysis were performed to determine exposure to single-metal and multi-metal co-exposure in relation to DM. A decrease in risk of DM was associated with iron (OR = 0.78, 95% CI: 0.61–1.00 and 0.68, 0.53–0.88 for the middle and high vs. low) and strontium (OR = 0.87, 95% CI: 0.69–1.12 and 0.67, 0.51–0.86 for the middle and high vs. low), respectively. A principal component 3 (PC3) characterized by iron and strontium showed an inverse association with DM. A principal component 4 (PC4) characterized by manganese and lead positively associated with DM. Exposure to high concentrations of urinary iron and strontium may reduce the risk of diabetes mellitus. This study revealed an increase in the risk of diabetes mellitus by co-exposure to high concentrations of urinary manganese and lead.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Diabetes mellitus (DM) is a serious threat to the global economy and health. International Diabetes Federation estimated approximately 463 million people with diabetes in 2019 and projected this number to reach 700 million by 2045(Federation, 2019). Metals play a key role in the physiological and biochemical processes occurring in the body. However, excess or deficiency of metals, especially essential trace elements, leads to bodily dysfunction. With rapid economic development and urban industrialization, heavy metal pollution has emerged serious concern. Therefore, our intake of metals through the respiratory tract, food, and drinking water is increasing day by day.
Recently, several studies have shown that metals, including antimony (Sb), arsenic (As), barium (Ba), cadmium (Cd), cesium (Cs), chromium (Cr), copper (Cu), manganese (Mn), molybdenum (Mo), palladium (Pd), selenium (Se), strontium (Sr), vanadium (V), and zinc (Zn) are associated with type 2 diabetes mellitus (T2DM)(Chen et al., 2020; Li et al., 2017; Xiao et al., 2018). A case–control study in Norway indicates that metals, such as Cd, Cr, nickel (Ni), iron (Fe), silver (Ag), and Zn, are significantly associated with DM (Hansen et al., 2017). Another study suggested that Cr and Fe are negatively associated with fasting plasma glucose (FPG), and Se is positively associated with FPG in men (Ge et al., 2021). A prospective cohort study established direct and indirect effects of dietary Mn on DM and hemoglobin A1c (HbA1c) (Du S et al. 2018). Various toxic metals such as arsenic, cadmium, and lead are known to induce oxidative stress in a variety of tissues and cell types (Ercal et al., 2001). A study in the Pakistani population shows that serum levels of antioxidant biomarkers, such as glutathione (GSH) and malondialdehyde (MDA), decrease due to arsenic exposure (Saba et al., 2020). Mercury (Hg) exposure adversely affects pancreatic beta cell development and function (Schumacher & Abbott, 2017). Low-dose mercury-induced oxidative stress and PI3K activation lead to Akt signaling-related pancreatic β-cell dysfunction (Chen et al., 2006). A cross section shows that urinary Cd, Cr, Mo, V, and Zn show a positive correlation with oxidative stress (Domingo-Relloso et al., 2019), an essential causative factor for the development of diabetes(Brownlee, 2005). Besides, strontium appears to be involved in anti-oxidation (Barneo-Caragol et al., 2018; Yalin et al., 2012) and adipose metabolism(Saidak et al., 2012). And exposure to high iron and glucose concentrations results in cellular oxidative damage and may initiate insulin secretory dysfunction in pancreatic β-cells by modulation of the exocytotic machinery (Blesia et al., 2021).
Several studies explored the relationship between single metals and diabetes, though their results differ (Ji et al., 2021; Soomro et al., 2019; Xiao et al., 2021). And the effects of multiple toxic metals on diabetes remain incompletely understood (Navas-Acien, 2019). These findings highlight the need to investigate the role of metal exposure in human risk of DM. China is a multi-ethnic country. In the past, research on the Chinese people mostly focused on the Han nationality. And the China Multi-Ethnic Cohort (CMEC) is a community population-based prospective observational study aiming to address the urgent need for understanding non-communicable diseases prevalence, risk factors, and associated conditions in resource-constrained settings for ethnic minorities in China. The Dong people in this study have a population of over one million and is the main ethnic minorities in Qiandongnan Prefecture, Guizhou Province. This population has fixed living habits and high genetic stability, and their data were more valuable than those of other floating population studies. Our objective was to evaluate the urinary exposure of trace elements (As, Cd, Cr, Cu, Fe, Hg, Mn, Mo, Ni, Pb, Sr, V, and Zn) in the Chinese Dong population and investigate the association of these trace elements with the risk of DM. We also aimed to evaluate how co-exposure to these trace elements may affect DM. The data from the CMEC study were used in the current study.
Method
Study population
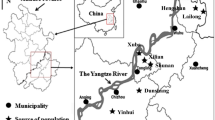
The CMEC study, which has been reconsidered, is a population-based survey from July 2018 to December 2018, involving 5,792 Dong ethnic participants aged 30–79 years in Guizhou Province of China (Zhao et al., 2020). In brief, the sampling method used in the survey was multistage stratified cluster sampling. In the first stage, the Qiandongnan Prefecture, China were selected as our study sites. In the second stage, two communities (Liping County and Kaili City) in the settlement were selected by the local Centres for Disease Control and Prevention (CDCs), taking into account migration status, local health conditions and, most importantly, ethnic structure. In the final stage, all participants who met our inclusion criteria were invited to participate in our studies in consideration of both sex ratio and age ratio. In total, 1,313 participants were excluded. Exclusion criteria were the following:
(a) Those fasting for < 8 h (n = 425), (b) Patients with existing or previous tumors (n = 21), (c). Those lacking physical examination data, such as height, weight, etc. (n = 35), (d). Those without blood biochemical examination data of FPG, HbA1c (n = 16), (e). Those with a history of organ removal (n = 126), and (f). Those without any urine samples (n = 690).
Therefore, a cross-sectional study on 4,479 Dong people within this cohort was undertaken to investigate the association between urinary metal concentrations and diabetes. All survey participants signed prior informed consent forms. This study was approved by the Sichuan University Medical Ethical Review Board (K2016038) and the Research Ethics Committee of The Affiliated Hospital of Guizhou Medical University (2018[094]).
Assessment of covariates
A tablet computer with a self-developed application was employed to collect the information on socio-demographic characteristics, lifestyle behaviors, and personal health and medical histories. The education levels of the participants were categorized as junior high school or below, senior high school or vocational school, or college or beyond. Current smokers were defined as smoking > 100 cigarettes so far (Zhao et al., 2020). Former smokers were defined as quitting smoking > 6 months a year (Zhao et al., 2020). The drinkers were defined as drinking alcohol every week for ≥ 1 year. The height and weight were measured by trained medical professionals in accordance with standard procedures. A tea drinker was defined as a person drinking tea every week for a year or more. Body mass index (BMI) is equal to weight (kg) divided by the square of height (m2).
Assessment of blood biochemical indicators
The blood samples, collected at the baseline after fasting > 8 h, were transported to Guizhou KingMed Diagnostics Group Co., Ltd via cold chain logistics for same-day testing. The levels of FPG, glycated hemoglobin (HbA1c), total cholesterol (TC), triglycerides (TG), high-density lipoprotein (HDL-C), and low-density lipoprotein (LDL-C) were determined using a fully automatic biochemical analyzer (HITACHI 7180, Tokyo, Japan).
Assessment of metals
The urine samples were stored at –20 °C before testing. Urinary metals/metalloids (As, Cd, Cr, Cu, Fe, Hg, Mn, Mo, Ni, Pb, Sr, V, and Zn) were measured by an inductively coupled plasma mass spectrometer (NexION 2000, PerkinElmer, Waltham, MA, USA). The standardized protocol, quality of control, and methods of accuracy evaluation have previously been described (Liu et al., 2021). The sample was placed at room temperature before dilution. Then, 1 mL original urine supernatant was diluted to 10 ml, with nitric acid (5%) (GR, Sinopharm Chemical Reagent Co., Ltd, Shanghai, China) and mixed well. Finally, the diluted sample was filtered through a 0.45 µm membrane and measured within 24 h. Internal standard solutions of Bi, Ge, In, 6Li, Sc, Tb, and Y at the concentration of 10 µg/L provided by PerkinElmer were used for internal online standardization, and the regression coefficient of the standard curve was not < 0.999. To check the accuracy, we used Seronorm™ Trace Elements Urine L-2 RUO (SERO, Billingstad, Norway). Percent recovery (i.e., amount of substance recovered on purification ÷ amount of substance originally taken) × 100) ranged from 82.92% – 115.71%. The limit of detection ranges from 0.0001- 0.1610 µg/L for the metals. The sample concentration below the limit of detection was expressed as half of the limit of quantification.
Diagnostic criteria
DM was defined as FPG ≥ 7.0 mmol/L or HbA1c ≥ 6.5% or self-reported history of DM (American Diabetes Association, 2018). Dyslipidemia was defined as TC ≥ 5.72 mmol/L or TG ≥ 1.70 mmol/L or LDL-C ≥ 3.40 mmol/L or HDL-C < 1.04 mmol/L or self-reported history of hyperlipidemia.
Statistical analysis
The continuous variables were expressed as median (interquartile range, IQR) because of skewed distribution; categorical variables were expressed as numbers (%). We evaluated the associations of 13 metals (As, Cd, Cr, Cu, Fe, Hg, Mn, Mo, Ni, Pb, Sr, V, and Zn) with diabetes through Logistic Regression models with adjustment for age, sex, education, smoking status, drinking status, tea consumption, BMI, dyslipidemia, and family history of diabetes. Principal component analysis (PCA) and weight quantile sum (WQS) regression were applied to investigate the effects of metal mixtures. The weights assigned to individual metals were estimated through PCA (weight range, 0–1 and the sum of all weights equal to 1) (Supplementary Fig. 1). WQS index was defined as under:
WQS index = As*0.11583 + Cd*0.08869 + Cr*0.11235 + Cu*0.04050 + Fe*0.08457 + Hg*0.01203 + Mn *0.04062 + Mo*0.08807 + Ni*0.07148 + Pb*0.06575 + Sr*0.10718 + V*0.08816 + Zn*0.08477.
Statistical analyses were performed with SPSS 25.0 (SPSS Inc, Chicago, IL) and EmpowerStats 2.0 (Inc. Boston, MA, USA). The inspection level was 0.05 (two-tailed).
Results
Demographic characteristics
Table 1 exhibits the baseline demographic characteristics of the participants in diabetic/non-diabetic groups. The total prevalence of diabetes was 9.5% (426/4479). The levels of FPG, HbA1c, TC, TG, LDL-C of the participants in the diabetic group were 3.13% –33.65% higher than those in the non-diabetic group (P < 0.05). No statistically significant differences were observed between diabetic and non-diabetic groups in education level and drinking status. Compared with non-diabetic participants, participants with diabetes had a higher percentage of men, older people, and tea drinkers. With respect to disease history, 300 (70.42%), 44 (10.33%) participants identified as dyslipidemia, and family history of diabetes in the diabetic group, respectively, whose ratio was higher than the non-diabetic group (P < 0.001).
Concentrations of urinary metals
Table 2 presents medians and interquartile ranges (IQRs) of metals in urine in the total population or by diabetes status. Only Hg and Ni were detected in < 80% of samples. Compared with the non-diabetes group, the concentrations of urinary Fe and Sr were about 11.84%/15.48% lower than those in the diabetes group, respectively (P < 0.05). Figure 1 depicts the correlations between metals. Most of the metals have a positive correlation, while only a few have a negative correlation (Mn-Cu, Pb-Cu, Mn-Fe, Mn-Ni, and Mn-V). The absolute value of the correlation coefficient ranged from 0.003–0.532. Moderately positive correlations were found for As-V, Cu-V, and Fe-Sr (P < 0.05).
Association of urinary metals with diabetes
Urinary Fe and Sr concentrations were negatively associated with diabetes, while other urinary metals/metalloids showed no association with diabetes in Model 1 (Table 3). In the adjusted model (Model 2), the associations of urinary Fe and Sr with diabetes remained significant (P trend < 0.05), and the ORs (95% CI) (the high vs. low) were 0.68(0.53–0.88) and 0.67(0.51–0.86), respectively, consistent with model 1. Figure 2 shows the smooth fitting curve between the urinary Fe and Sr concentration and the prevalence of diabetes. As the concentrations of urinary Fe and Sr increase, the risk of diabetes decreases (P < 0.05).
The smooth fitting curve of Fe and Sr in urine and the prevalence of diabetes. Curve-adjusted sex, ages, BMI, education, smoking, drinking and tea consumption, dyslipidemia, and family history of diabetes. The red curve in the middle represents the estimated value, and the blue curves on both sides represent the 95% confidence intervals
Association of urinary metal mixture with diabetes
According to the scree plot and the criteria of eigenvalues of principal components > 1 (Supplementary Fig. 2), four principal components were selected, and the factor loading matrices of the four major PCAs are given in Supplementary Table 1. The three PC (PC 3) predominated by iron, nickel, and strontium, while the four PC (PC 4) were predominated by Mn and Pb. The PC 3 was negatively associated with diabetes and OR (95% CI) was 0.65(0.5–0.85). The PC 4 showed a positive association with diabetes and OR (95% CI) was 1.31(1.02–1.70). However, no association could be established between diabetes and the WQS index (Table 4).
Discussion
In the current study, we explored the association of various metals with the risk of DM and evaluated how co-exposure to these trace elements may affect DM. We document that lower levels of urinary Fe and Sr were associated with an increased risk of DM during single metal exposure. While multiple metals are exposed together, the harmful effects primarily result from Mn and Pb, followed by Cr, and the beneficial effects mainly come from Fe and Sr.
It is suggested that Fe may affect glucose metabolism by affecting lipid metabolism.(Mayneris Perxachs et al., 2020) Increased hepatic iron load promotes fat regeneration, increased gluconeogenesis, and increased free glucose levels (Altamura et al., 2021). A research discovered that increased hepatic iron load is accompanied by insulin resistance (IR) (Abbate et al., 2021). Compared with the control group, the serum Fe level was higher in the diabetic group (Skalnaya et al., 2017). High Fe concentration increases the risk of DM (Hansen et al., 2017). A population-based cohort study indicated that serum ferritin levels, which represents the most commonly used indicators of iron storage, are higher in patients with T2DM, compared with non-T2DM (Diaz-Lopez et al., 2020). A cohort study from China demonstrated that higher serum ferritin was associated with a higher risk of DM (Chen et al., 2018). One cohort study in Japan showed that dietary Fe intake is a high-risk factor for DM (Eshak et al., 2018). In the current study, higher urinary Fe concentration is accompanied by a lower risk of DM, and the relationship between iron concentration and diabetes risk was U-shaped (Fig. 2). An in vitro study reported that increased levels of intracellular iron activate the Akt signaling pathway and 5' AMP-activated protein kinase (AMPK) pathways result in decreased liver glucose production(Varghese et al., 2018). In contrast, insulin-induced painful activation of AKT is attenuated because of the decrease in IRS1/2 protein levels(Varghese et al., 2018). Maybe this can help explain the U-shaped relationship between urinary Fe concentration and DM risk. Our results illustrate that urine Fe is a protective factor for DM, contrary to other studies. The concentrations of urinary metals vary from region to region. Because the study populations and regions are different, results are inconsistent.
A case–control study demonstrated that plasma Sr is inversely related with TC, LDL-C, and MDA and that as the plasma SR concentration increases, the risk of diabetes decreases (Chen et al., 2020). Additionally, an animal study showed that Sr has anti-diabetic effects by regulating the expression of related genes, lowering blood glucose levels, thereby improving resistance to insulin, leptin, and adiponectin (Maehira et al., 2011). Urinary Sr is negatively associated with the risk of diabetes in the present study, consistent with the results of the previous case–control study. However, a study indicated that compared with the first quantile, the second quantile shows that urinary Sr has a positive correlation with diabetes risk, but as the urinary Sr concentration continues to rise, the correlation is not statistically significant (Feng et al., 2015). This finding contradicted our research results. In this study (Feng et al., 2015), the median urinary Sr concentration was approximately 123.3 µg/L, but in the current study, the median concentration of urinary SR was about 62.2 µg/L. The urinary Sr concentration of the two studies is quite different, which may lead to inconsistent conclusions.
Although we found no association between Mn, Pb, Cr, and DM in single-metal-exposure analysis, PC4, dominated by Mn, Pb, and Cr, is positively associated with diabetes risk. Mn is an essential trace element. Mn is a component of manganese superoxidase (MnSOD) which protects mitochondrial DNA from glucose-induced oxidative damage to improve diabetic retinopathy (Sally A. Madsen-Bouterse and Kowluru 2010). An animal study reveals that Mn supplementation in normal mice can enhance the metalization and activity of MnSOD, and promote insulin secretion, thereby improving glucose tolerance (Lee et al., 2013). A cohort study in Japan found that high dietary manganese intake is associated with a reduced risk of T2DM in women (Eshak et al., 2021). Another study reported that high dietary manganese intake would reduce the risk of T2DM in women, mediated by interleukin-6 (IL-6) and high-sensitivity C-reactive protein (hs-CRP) (Jung Ho Gong 2020). Additionally, two cohort studies indicated the negative correlation between dietary manganese and glycosylated hemoglobin is statistically significant (Du S et al. 2018). However, a study revealed that blood Mn concentration has a J-shaped relationship with IR (Yang et al., 2020). And another cross-section study in China showed that blood Mn concentration has a U-shaped relationship with T2DM (Shan et al., 2016). The current study showed that as the urine Mn concentration increases, the risk of diabetes increases. A cross-section study revealed that diabetes patients have lower blood manganese and higher urine manganese compared with the control group (Kazi et al., 2008). This explains why our research shows that as the urinary Mn concentration increases, the risk of diabetes increases. A cohort study testified that higher Pb excretion is associated with a higher risk of DM (Wang et al., 2020). This is consistent with our findings. Pb can induce the occurrence and development of diabetes by promoting oxidative stress and altering intracellular signaling pathways, such as increasing resting intracellular Ca++. However, several studies approve that blood Pb has no association with DM, IR, beta-cell dysfunction, and FPG (Aziz et al., 2020; Feng et al., 2015; Moon, 2013). This may be because single metal exposure is inadequate to produce unhealthy outcomes, while multiple metal co-exposures increase health risks (Lv et al., 2021). The specific mechanism needs to be explored in future research.
This study has several strengths and limitations. First, we used the principal component analysis method to reduce the effect of collinearity between metals to a certain extent. Second, we used a generalized additive model to fit the dose–response relationship between metal concentration and diabetes risk. We also have some limitations. First, this study is a cross-sectional study that cannot directly explain the cause and effect. Second, this study did not involve eating habits that will affect the concentration of elements in the body. Although accurate measurement of dietary metals intake is challenging, it is interesting to explore the relationship between metals intake, plasma metals, urinary metals and diabetes. These will be explored in future research. Third, the diabetic patients in this study included newly-onset diabetic patients and those previously diagnosed with diabetes who may change their life behavior and dietary habits after the diagnosis of diabetes which may affect urine metal concentration.
Conclusion
The current study supports that co-exposure to multiple metals is associated with DM. The harmful effects are mainly from manganese and lead, and the protective effects are mainly from iron and strontium.
Data availability statement
The data that support the findings of this study are available on request from the corresponding author.
References
Abbate, M., Montemayor, S., Mascaro, C. M., et al. (2021). Albuminuria is associated with hepatic iron load in patients with non-alcoholic fatty liver disease and metabolic syndrome. Journal of Clinical Medicine. https://doi.org/10.3390/jcm10143187
Altamura, S., Müdder, K., Schlotterer, A., et al. (2021). Iron aggravates hepatic insulin resistance in the absence of inflammation in a novel db/db mouse model with iron overload. Mol Metab., 51, 101235. https://doi.org/10.1016/j.molmet.2021.101235
American Diabetes Association. (2018). Classification and diagnosis of diabetes: standards of medical care in diabetes—2018. Diabetes Care, 1, S13–S27. https://doi.org/10.2337/dc18-S002
Aziz, F., Alhazmi, A., Aljameil, N., et al. (2020). Serum selenium and lead levels: a possible link with diabetes and associated proteinuria. Biological Trace Element Research, 193, 342–347. https://doi.org/10.1007/s12011-019-01721-7
Barneo-Caragol, C., Martinez-Morillo, E., Rodriguez-Gonzalez, S., et al. (2018). Strontium and oxidative stress in normal pregnancy. Journal of Trace Elements in Medicine and Biology, 45, 57–63. https://doi.org/10.1016/j.jtemb.2017.09.021
Blesia, V., Patel, V. B., Al-Obaidi, H., et al. (2021). Excessive iron induces oxidative stress promoting cellular perturbations and insulin secretory dysfunction in MIN6 beta cells. Cells-Basel., 10, 1141. https://doi.org/10.3390/cells10051141
Brownlee, M. (2005). The pathobiology of diabetic complications. Diabetes Metab, 25, 1615–1625.
Chen, L., Guo, Q., Wang, Q., et al. (2020). Association between plasma strontium, a bone-seeking element, and type 2 diabetes mellitus. Clinical Nutrition, 39, 2151–2157. https://doi.org/10.1016/j.clnu.2019.08.033
Chen, L., Li, Y., Zhang, F., et al. (2018). Elevated serum ferritin concentration is associated with incident type 2 diabetes mellitus in a Chinese population: A prospective cohort study. Diabetes Res Clin Pr., 139, 155–162. https://doi.org/10.1016/j.diabres.2018.03.001
Chen, Y. W., Huang, C. F., Tsai, K. S., et al. (2006). The role of phosphoinositide 3-Kinase/Akt signaling in low-dose mercury-induced mouse pancreatic β-cell dysfunction in vitro and in vivo. Diabetes, 55, 1614–1624. https://doi.org/10.2337/db06-0029
Diaz-Lopez, A., Iglesias-Vazquez, L., Palleja-Millan, M., et al. (2020). Association between iron status and incident type 2 diabetes: A population-based cohort study. Nutrients. https://doi.org/10.3390/nu12113249
Domingo-Relloso, A., Grau-Perez, M., Galan-Chilet, I., et al. (2019). Urinary metals and metal mixtures and oxidative stress biomarkers in an adult population from Spain: The Hortega Study. Environment International, 123, 171–180. https://doi.org/10.1016/j.envint.2018.11.055
Du, S., Wu, X., Han, T., et al. (2018). Dietary manganese and type 2 diabetes mellitus: Two prospective cohort studies in China. Diabetologia, 61, 1985–1995. https://doi.org/10.1007/s00125-018-4674-3
Ercal, N., Gurer-Orhan, H., & Aykin-Burns, N. (2001). Toxic metals and oxidative stress part I: Mechanisms involved in metal-induced oxidative damage. Current Topics in Medicinal Chemistry, 1, 529–539. https://doi.org/10.2174/1568026013394831
Eshak, E. S., Iso, H., Maruyama, K., et al. (2018). Associations between dietary intakes of iron, copper and zinc with risk of type 2 diabetes mellitus: A large population-based prospective cohort study. Clinical Nutrition, 37, 667–674. https://doi.org/10.1016/j.clnu.2017.02.010
Eshak, E. S., Muraki, I., Imano, H., et al. (2021). Manganese intake from foods and beverages is associated with a reduced risk of type 2 diabetes. Maturitas, 143, 127–131. https://doi.org/10.1016/j.maturitas.2020.10.009
Federation ID (2019) IDF DIABETES ATLAS
Feng, W., Cui, X., Liu, B., et al. (2015). Association of urinary metal profiles with altered glucose levels and diabetes risk: A population-based study in China. PLoS ONE, 10, e123742. https://doi.org/10.1371/journal.pone.0123742
Ge, X., Yang, A., Huang, S., et al. (2021). Sex-specific associations of plasma metals and metal mixtures with glucose metabolism: An occupational population-based study in China. Science of the Total Environment, 760, 143906. https://doi.org/10.1016/j.scitotenv.2020.143906
Hansen, A. F., Simić, A., et al. (2017). Trace elements in early phase type 2 diabetes mellitus—A population-based study. The HUNT study in Norway. J Trace Elem Med Bio., 40, 46–53. https://doi.org/10.1016/j.jtemb.2016.12.008
Ji, J. H., Jin, M. H., Kang, J. H., et al. (2021). Relationship between heavy metal exposure and type 2 diabetes: A large-scale retrospective cohort study using occupational health examinations. British Medical Journal Open, 11, e39541. https://doi.org/10.1136/bmjopen-2020-039541
Jung, G. H. (2020). Dietary manganese, plasma markers of inflammation, and the development of type 2 diabetes in postmenopausalwomen: Findings from the women ’ s health initiative. Diabetes Care. https://doi.org/10.2337/dc20-1234
Kazi, T. G., Afridi, H. I., Kazi, N., et al. (2008). Copper, chromium, manganese, iron, nickel, and zinc levels in biological samples of diabetes mellitus patients. Biological Trace Element Research, 122, 1–18. https://doi.org/10.1007/s12011-007-8062-y
Lee, S. H., Jouihan, H. A., Cooksey, R. C., et al. (2013). Manganese supplementation protects against diet-induced diabetes in wild type mice by enhancing insulin secretion. Endocrinology, 154, 1029–1038. https://doi.org/10.1210/en.2012-1445
Li, X. T., Yu, P. F., Gao, Y., et al. (2017). Association between plasma metal levels and diabetes risk: A Case-control Study in China. Biomedical and Environmental Sciences, 30, 482–491. https://doi.org/10.3967/bes2017.064
Liu, Y., Zhang, C., Qin, Z., et al. (2021). Analysis of threshold effect of urinary heavy metal elements on the high prevalence of nephrolithiasis in men. Biological Trace Element Research. https://doi.org/10.1007/s12011-021-02740-z
Lv, Y., Xie, L., Dong, C., et al. (2021). Co-exposure of serum calcium, selenium and vanadium is nonlinearly associated with increased risk of type 2 diabetes mellitus in a Chinese population. Chemosphere, 263, 128021. https://doi.org/10.1016/j.chemosphere.2020.128021
Maehira, F., Ishimine, N., Miyagi, I., et al. (2011). Anti-diabetic effects including diabetic nephropathy of anti-osteoporotic trace minerals on diabetic mice. Nutrition, 27, 488–495. https://doi.org/10.1016/j.nut.2010.04.007
Mayneris Perxachs, J., Mousa, A., Naderpoor, N., et al. (2020). Plasma phospholipids with long-chain polyunsaturated fatty acids and dihydroceramides at the crossroads of iron stores and insulin resistance. Molecular Nutrition & Food Research, 64, 1901055. https://doi.org/10.1002/mnfr.201901055
Moon, S. S. (2013). Association of lead, mercury and cadmium with diabetes in the Korean population: The Korea National health and nutrition examination survey (KNHANES) 2009–2010. Diabetic Medicine, 30, e143–e148. https://doi.org/10.1111/dme.12103
Navas-Acien, C. K. A. (2019). Commentary: Environmental chemicals and diabetes: Which ones are we missing? International Journal of Epidemiology. https://doi.org/10.1093/ije/dyv004
Saba, S., Akash, M., Rehman, K., et al. (2020). Assessment of heavy metals by ICP-OES and their impact on insulin stimulating hormone and carbohydrate metabolizing enzymes. Clinical and Experimental Pharmacology and Physiology, 47, 1682–1691. https://doi.org/10.1111/1440-1681.13353
Saidak, Z., Haÿ, E., Marty, C., et al. (2012). Strontium ranelate rebalances bone marrow adipogenesis and osteoblastogenesis in senescent osteopenic mice through NFATc/Maf and Wnt signaling. Aging Cell, 11, 467–474. https://doi.org/10.1111/j.1474-9726.2012.00804.x
Madsen-Bouterse, S. A., & Kowluru, A. R. A. (2010). Oxidative damage of mitochondrial DNA in diabetes and its protection by manganese superoxide dismutase. NIH Public Access., 3, 313–321. https://doi.org/10.3109/10715760903494168
Schumacher, L., & Abbott, L. C. (2017). Effects of methyl mercury exposure on pancreatic beta cell development and function. Journal of Applied Toxicology, 37, 4–12. https://doi.org/10.1002/jat.3381
Shan, Z., Chen, S., Sun, T., et al. (2016). U-shaped association between plasma manganese levels and type 2 diabetes. Environ Health Persp., 124, 1876–1881. https://doi.org/10.1289/EHP176
Skalnaya, M. G., Skalny, A. V., & Tinkov, A. A. (2017). Serum copper, zinc, and iron levels, and markers of carbohydrate metabolism in postmenopausal women with prediabetes and type 2 diabetes mellitus. Journal of Trace Elements in Medicine and Biology, 43, 46–51. https://doi.org/10.1016/j.jtemb.2016.11.005
Soomro, M. H., Baiz, N., Huel, G., et al. (2019). Exposure to heavy metals during pregnancy related to gestational diabetes mellitus in diabetes-free mothers. Science of the Total Environment, 656, 870–876. https://doi.org/10.1016/j.scitotenv.2018.11.422
Varghese, J., James, J., Vaulont, S., et al. (2018). Increased intracellular iron in mouse primary hepatocytes in vitro causes activation of the Akt pathway but decreases its response to insulin. Biochimica et Biophysica Acta (BBA)- General Subjects, 1862, 1870–1882. https://doi.org/10.1016/j.bbagen.2018.05.022
Wang, X., Karvonen-Gutierrez, C. A., Herman, W. H., et al. (2020). Urinary metals and incident diabetes in midlife women: Study of women’s health across the nation (SWAN). BMJ Open Diabetes Research & Care., 8, e1233. https://doi.org/10.1136/bmjdrc-2020-001233
Xiao, L., Zhou, Y., Ma, J., et al. (2018). Oxidative DNA damage mediates the association between urinary metals and prevalence of type 2 diabetes mellitus in Chinese adults. Science of the Total Environment, 627, 1327–1333. https://doi.org/10.1016/j.scitotenv.2018.01.317
Xiao, L., Li, W., Zhu, C., et al. (2021). Cadmium exposure, fasting blood glucose changes, and type 2 diabetes mellitus: A longitudinal prospective study in China. Environmental Research, 192, 110259. https://doi.org/10.1016/j.envres.2020.110259
Yalin, S., Sagir, O., Comelekoglu, U., et al. (2012). Strontium ranelate treatment improves oxidative damage in osteoporotic rat model. Pharmacological Reports, 64, 396–402. https://doi.org/10.1016/s1734-1140(12)70780-6
Yang, J., Yang, A., Cheng, N., et al. (2020). Sex-specific associations of blood and urinary manganese levels with glucose levels, insulin resistance and kidney function in US adults: National health and nutrition examination survey 2011–2016. Chemosphere, 258, 126940. https://doi.org/10.1016/j.chemosphere.2020.126940
Zhao, X., Hong, F., Yin, J., et al. (2020). Cohort profile: The China Multi-Ethnic cohort (CMEC) study. International Journal of Epidemiology. https://doi.org/10.1093/ije/dyaa185
Acknowledgements
The authors gratefully acknowledge assistants from all persons involved in the project. And we are grateful to Prof. Xiaosong Li at Sichuan University for his leadership and fundamental contribution to the establishment of the CMEC. Prof. Li passed away in 2019 and will remain in our hearts forever.
Funding
This study was supported by the National Natural Science Foundation of China (No. 82173566) and the National Key R&D Program of China (NO. 2017YFC0907301).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation and data collection and analysis were performed by Qianyuan Yang, Yalan Liu, and Linyuan Zhang. The first draft of the manuscript was written by Qianyuan Yang, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethical approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Sichuan University Medical Ethical Review Board (K2016038) and the Research Ethics Committee of The Affiliated Hospital of Guizhou Medical University (2018[094]).
Consent to participate
Written informed consent was obtained from the participants.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yang, Q., Liu, Y., Liu, L. et al. Exposure to multiple metals and diabetes mellitus risk in dong ethnicity in China: from the China multi-ethnic cohort study. Environ Geochem Health 45, 2435–2445 (2023). https://doi.org/10.1007/s10653-022-01366-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10653-022-01366-x