Summary
Signal transduction pathways, which regulate cell growth and survival, are up-regulated in many cancers and there is considerable interest in their pharmaceutical modulation for cancer treatment. However inhibitors of single pathway components induce feedback mechanisms that overcome the growth moderating effect of the inhibitor. Combination treatments have been proposed to provide a more complete pathway inhibition. Here the effect of dual treatment of cancer cells with a pan-Akt and a pan-mTOR inhibitor was explored. Breast (SKBr3 and MDA-MB-468) and colorectal (HCT8) cancer cells were treated with the pan-Akt inhibitor MK2206 and pan-mTOR inhibitor AZD8055. Cytotoxic effect of the two drugs were determined using the MTT assay and the Combination Index and isobolomic analysis used to determine the nature of the interaction of the two drugs. Flow cytometry and western blot were employed to demonstrate drug effects on cell cycle distribution and phosph-Aktser473 expression. Radiolabelled ([methyl-3H]) Choline uptake was measured in control and drug-treated cells to determine the modulatory effects of the drugs on choline incorporation. The two drugs acted synergistically to inhibit the growth rate of each cancer cell line. Flow cytometry demonstrated G0/G1 blockade with MK2206 and AZD8055 which was greater when cells were treated with both drugs. The incorporation of [methyl-3H] choline was found be decreased to a greater extent in cells treated with both drugs compared with cells treated with either drug alone. Conclusions Pan-mTOR and pan-Akt inhibition may be highly effective in cancer treatment and measuring changes in choline uptake could be useful in detecting efficacious drug combinations.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Cancer growth and development are frequently associated with upregulation of intracellular signalling pathways, including the PI3K/Akt/mTOR pathway, which drives cellular proliferation resulting in the uncontrolled cell growth that defines cancer [1]. The increased levels of activation of PI3K/Akt/mTOR can be the result [2] of activating mutations of genes coding for PI3K or Akt (also known as PKB (protein kinase B)), kinases that stimulate the pathway, or inactivating mutations in the gene for the inhibitory phosphatase, PTEN (phosphatase and tensin homolog).
In view of the central role of PI3K/Akt/mTOR in cancer cell proliferation in many tumour types there is much interest in oncology in the use of inhibitors targeting components of this pathway [3]. Although the use of such inhibitors has been shown to decrease cancer cell proliferation and survival, their efficacy as single-agents is poor [4] due to activation of feedback mechanisms [5, 6] so attenuating the clinical benefit from the drug. Consequently their use in combination treatments has been recommended [7] and it has been shown that drug combinations, including the dual use of Akt and mTOR inhibitors, are more efficacious than single drug regimens as they bring about a more complete pathway inhibition [8]. However drugs targeting the PI3K/Akt/mTOR pathway are associated with unpleasant and potentially dangerous side effects including nausea, diarrhoea and hyperglycaemia [9] which may be enhanced in drug combinations [8].
Therefore, early detection of the clinical benefit of multi-drug regimens is an important aspect of their utilisation. Positron emission tomography (PET) is a highly sensitive medical imaging technique that facilitates non-invasive measurement of metabolism. The most commonly used PET tracer is FDG (2-[18F] Fluor-2-deoxy-D-glucose) and many studies have demonstrated that changes in its tumour incorporation accompanies treatment response. However this is not always the case for drugs targeting the PI3K/Akt/mTOR pathway [10]. Choline uptake has been shown to be associated with proliferation rate [11] and [11C] choline-PET has been applied to response detection to treatments that target receptors upstream of signalling pathways [12]. Here we have demonstrated that treatment of breast cancer and colorectal cancer cells with a pan-mTOR inhibitor synergistically increases the growth-inhibitory action of the Akt-inhibitor MK2206 which corresponded with changes in the incorporation of radiolabelled choline.
Materials and methods
Materials
Breast cancer cells (MDA-MB 468 and SKBr3) and colon cancer cells (HCT8, HCT116 and SW620) were purchased from American Type Cell Culture Collection (ATCC). Unless stated otherwise all chemicals were purchased from Sigma-Aldrich chemical company. The inhibitors used in this study, MK2206 and AZD8055 targeting Akt and mTORC1 and 2 respectively, were obtained from Cambridge Biosciences (Cambridge, UK).
Cell culture and cytotoxicity assay
Cells were grown in Dulbecco’s Modified Eagle medium supplemented with 10% foetal bovine serum containing penicillin (100 units/ml) / streptomycin (10 μg/ml) in 75cm2 tissue culture flasks and incubated at 37 °C in a CO2 incubator (Thermo-Scientific UK) with a humidified atmosphere of 95% air; 5% CO2. When they reached confluency cells were detached with trypsin and after addition of medium the cells were counted in a haemocytometer (Improved Neubauer, Weber Scientific International UK) and cell suspensions of 30 × 103 cells/ ml prepared. Cell suspension (100 μl) was added to rows 2–10 (columns B to G) and 100ul of medium added to row H (background) of 96 well plate. The plates were then incubated at 37 °C for 24 h to allow cells to adhere. Medium (100 μl) was added to row B and H. To the remaining cells were added either MK2206 (0.04-20 μM) or AZD8055 (8-1000 nM) in increasing concentrations to rows C to G and the plate incubated for a further 72 h. The cytotoxic effect of each drug was assessed by the MTT (3-(4, 5-dimethylthiazol-2-yl)-2, 5- diphenyltetrazolium bromide) assay. Briefly medium was removed from the wells then replaced with medium containing 0.5 mg MTT/ml and the plates incubated in the incubator at 37 °C for 1-2 h depending on the time taken for the cells to appear dark purple. The medium was then removed and the purple aqueous-insoluble crystals that formed in the cells by reduction of MTT were solubilised by addition of 100 μl of DMSO. After a brief (10s) agitation the absorbance was measured in a multiwell platereader with the absorbance filter at 540 nm. The IC50 values of each drug were calculated using CompuSyn software (ComboSyn, Paramus, NJ) from the absorbance of drug-treated cells expressed as a percentage of absorbance of control (untreated) in well 2.
To determine the effect of combining MK2206 and AZD8055 on proliferation, cells were set up as for the dose curves but before adding the range of drug doses, cells were treated with a dose of the other drug that was known to appreciably (30–40%) decrease cell proliferation. The dose curves with and without combined treatment were then used to calculate the combination index as described by Chou and Talalay (Chou 2010) [13] using the following formula:
Suitable drug concentrations (Xa, Ya) are used such that their combined effect reduces cell viability to about 20–60% that of the control. Xb and Yb are the concentrations of each drug which when used alone produce the same level of growth inhibition as the combination. The data obtained from the dose curves in the presence and absence of the second drug were also subject to Isobolomic analysis.
Western blot analysis of Akt, p-Akt (Ser473), mTOR and p-mTOR (Ser2481) protein expression
MDA-MB 468 cells were treated with the MK2206, AZD8055 or the two drugs combined for 24 h and then washed with 5 ml ice cold PBS wash before harvesting by scraping with 150 μl of lysis buffer (PBS containing 1 mM DTT, a protease inhibitor cocktail, 10 mM sodium pyrophosphate and 1 mM sodium orthovanadate). Samples were kept frozen until they were lysed with a probe sonicator for 30 s. Protein concentration was determined using the bicinchonininic acid (BCA) assay. Lysates (25 μg protein/well) were resolved on 4%–12% acrylamide bis–tris gels (Invitrogen) and the proteins transferred to Immobilon-P polyvinylidene difluoride membranes (Millipore) at 30 V for 1.5 h using a wet transfer system (Invitrogen). Membranes were blocked for 1 h at room temperature in sea block PBS for the Akt antibody and 1% (w/v) BSA for the p-Akt antibody. Membranes were blotted with antibodies in PBST (PBS containing 0.1% Tween 20) at 4 °C overnight. Akt and p-Akt (1/667 dilution) and mTOR and p-mTOR (1/1000 dilution) were used. Membranes were washed four times in PBST prior to 1 h incubation with the appropriate anti-rabbit fluorescent secondary antibody in PBST in the dark. The secondary antibody used was IRdye680 donkey anti-rabbit secondary antibody (Licor) (1/10000 dilution). Blots were drained and wrapped in cling film to prevent drying and imaged using the Odyssey® CLx LI-CORE imaging system. Images were then analysed using the Odyssey Image Studio Lite (LI-CORE) software.
Flow cytometry analysis of cell cycle distribution
Cells were seeded in 25cm2 flasks with 2 ml medium (1 × 106 cells) and incubated at 37 °C until treated with IC50 concentrations of each inhibitor or in combinations for 24 h, then trypsinized. After two PBS washes they were re-suspended in 300 μl PBS followed by fixation with 70% ice-cold ethanol during mixing on a vortex. The fixed cells were kept at −20 °C prior to flow cytometry analysis. For cell cycle analysis, fixed cells were adjusted to 5 × 105 cells/ml and washed 2 times with PBS supplemented with 1% bovine serum albumin (BSA). Then the cells were centrifuged at 1000 g for 5mins and suspended in 1 ml of staining buffer containing 50μg/ml propidium iodide, 50μg/ml ribonuclease A and 0.1% v/v triton-x-100 in PBS and incubated for 15 min at room temperature. The stained nuclei were kept at 4 °C and protected from light. Flow cytometry was performed using 488 nm laser light on a FACSCalibur flow cytometer (Becton Dickinson, UK) and CELLQuest software (Becton Dickinson, UK) equipped for fluorescence detection, forward, 90° angle light scatter and doublet discrimination. The data analysis was carried out with Flow-jo cell cycling software.
[Methyl-3H]-choline incorporation
For each experiment 12 flasks (25cm2) were seeded with 1 × 106 cells in 2 ml of medium and allowed to attach overnight at 37oC. Cells were then treated by addition of medium (6 flasks) or medium containing AZD8055 (6 flasks) and incubated overnight at 37 °C. To 3 untreated and 3 AZD8055-treated flasks of cells was added MK2206 and the flasks incubated for a further 24 h at 37 °C. Cells were then incubated with fresh medium containing [methyl-3H]-choline (37 kBq/ml) for 15 mins [14]. Then the cells were washed 5 times with phosphate buffer saline (PBS) and detached by treatment with trypsin (0.35 ml). After addition of medium (0.35 ml) to neutralise the trypsin half the cell suspension was added into 5 ml of Ultima Gold scintillation fluid (Perkin-Elmer UK) in a scintillation vial (Perkin-Elmer UK) and counted in the liquid scintillation counter (Packard Tricarb2300) for 10 mins per vial. The remaining cells were centrifuged and washed with 1 ml of PBS and the pellet dissolved in 0.1 ml of NaOH (1 M) overnight for determination of protein concentration after neutralization with 0.1 ml of HCl (1 M).
Protein assay
Protein assay was done by using the BCA protein assay kit (Sigma-Aldrich UK) with Bovine serum albumin (BSA) as a standard according to manufacturer’s protocol.
Statistical analysis
Statistical differences between means were determined using the data acquired from at least 3 independent experiments. Significance was set at p < 0.05. Statistical analysis for finding IC50 was performed using CompuSyn software (ComboSyn, Paramus, NJ). Combination index (CI) were calculated from fractions of dose-effect curves by Chou and Talalay [13] for drug interactions.
Results
Up-regulation of PI3K/Akt/mTOR is an important indicator for treatment with inhibitors of this pathway therefore an initial screen of phospho-Aktser473 and phosphor-mTORser2481 expression was carried out in 2 breast and 3 colorectal cancer cell lines. The western blots are shown in Fig. 1. SKBr3, MDA-MB-468 and HCT8 cells expressed p-Aktser473 at high levels. All lines expressed similar levels of p-mTORser2481 protein.
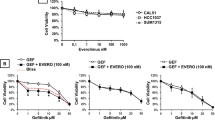
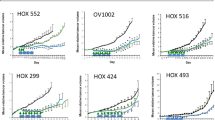
Figure 2 shows the effect of the pan-Akt inhibitor MK2206 and the pan-mTOR inhibitor AZD8055 on the growth rate of the breast cancer cell lines MDA-MB-468 and SKBr3 and the colorectal cell line HCT8. The IC50 doses of each drug are shown in Table 1. The effect of combining AZD8055 with a clinically relevant dose of MK2206 [3] that decreases cell growth by 30–40% (310 nM) is shown in Fig. 3. The combined effect of these drugs were then assessed using the combination index Table 2) and found to be synergistic. The results were confirmed using isobolomics using CompuSyn and the isobolograms displayed in Fig. 4.
Inhibition of proliferation of SKBr3 (empty squares), MDA-MB-468 (filled circles) and HCT8 (filled squares) cancer cells by treatment with increasing concentrations MK2206 (a) and AKD8055 (b) determined using the MTT assay. Results expressed as absorbance at 540 nm relative to cells in untreated wells (%)
Inhibition of proliferation of SKBr3 (a), MDA-MB-468 (b) and HCT8 (c) cancer cells by treatment with increasing concentrations AZD8055 alone (filled circles) and in the presence of an IC40 dose MK2206 (open circles) determined using the MTT assay. Results expressed as absorbance at 540 nm relative to cells in untreated wells (%)
To confirm that MK2206 and AZD8055 down-regulated pAktser473 [15, 16] the expression of p-Aktser473 and total Akt by MDA-MB-468 cells untreated and treated with MK2206 (310 nm), AZD8055 (31, 62 and 125 nM) or both drugs combined was determined. The results shown in Fig. 5 demonstrate that both drugs decrease the level of pAktser473 and that combining MK with AZD resulted in greater decreases in pAktser473 levels.
The effects of MK2206 and AZD8055 alone or in combination on cell cycle distribution was determined in SKBr3 and MDA-MB-468 cells and the results shown in Fig. 6. Each drug alone significantly (P < 0.05) increased the proportion of cells in G0/G1 and decreased the proportion in G2 in both cells lines. The two drugs together significantly (P < 0.05) increased the proportion of cells in G0/G1 and decreased the proportion of cells in G2 compared with either drug alone in both cell lines.
Treatment of SKBr3, MDA-MB-468 and HCT8 cells with AZD8055 and MK2206 significantly (p < 0.05) decreased choline incorporation compared with treatment with either MK2206 or AZD8055 alone (results shown in Fig. 7).
Discussion
Inhibition of intracellular signalling pathways is an attractive strategy for anticancer treatment. However due to feedback mechanisms and cross-talk cancer cells are able to minimise the proliferation-attenuating effects of signal pathway inhibiting drugs when administered as single agents. The PI3K/Akt/mTOR pathway is up-regulated in cancer due to several mechanism including activating mutations of PI3K and Akt, inactivating mutations of PTEN and over-expression of upstream receptors such as the tyrosine kinase human epithelial receptor family (HER). An initial screen of several cell lines confirmed high phospho-Aktser473 expression in SKBr3, MDA-MB-468 and to a lesser extent in HCT8 cells.
SKBr3 cells over-express HER-2 [10, 17] but are wild type for PI3K and PTEN, MDA-MB-468 cells harbour mutant PTEN [17] and HCT8 are mutant for PIK3CA [18]. MK2206 and AZD8055 synergistically inhibited proliferation of SKBr3, MDA-MB-468 and HCT8 cells. This would suggest that the underlying mechanism of PI3K/Akt/mTOR up-regulation is not necessarily a factor in the synergistic growth inhibitory effect of pan-Akt and pan-mTOR inhibitors.
Treatment of cancer cells with AZD8055 [19, 20] and MK2206 [21, 22] has been shown to cause accumulation of cells in G0/G1. Thus English et al. [19] found that response to treatment of uterine serous carcinoma cell lines, especially cells over-expressing HER2, with 1 μM or 5 μM AZD8055 was associated with G0/G1 cell cycle arrest in a concentration-dependent manner. Qian et al. 2016 [20] has reported that the pan-mTOR kinase inhibitors MTI-31 and AZD8055 induce G0/G1 cell cycle arrest corresponding with suppression of cyclin D1 and c-Myc in HER2+/PIK3CA mutant breast cancer cells. Similarly for the pan-Akt inhibitor, MK2206, studies [21, 22] have demonstrated that treatment with this drug induced G0/G1-phase arrest which was associated with a marked decrease in cyclin D1 levels in hepatocellular carcinoma HepG2 cells. In agreement with these studies we have found MK2206 and AZD8055 induced G0/G1 cell cycle arrest in breast cancer and colorectal cancer lines whilst the combination of MK2206 with AZD8055 exacerbated G0/G1 cell cycle arrest.
Progression of human mammary epithelial cells to a malignant phenotype is associated with altered membrane choline metabolism [23] due to changes in the expression of enzymes that control anabolic and catabolic reactions of choline metabolism resulting in increased levels of choline-containing precursors and breakdown products of membrane phospholipids [24]. Increased phosphocholine levels are frequently found in cancer tissue [25, 26] and studies have shown that the uptake and phosphorylation of radiolabelled choline by cancer cells correlates with proliferation rate [11]. Here choline uptake was decreased by breast cancer and colorectal cancer cells when treated with both MK2206 and AZD8055 but MK2206 alone only decreased choline uptake significantly in the breast cancer cell lines. Studies using 31P-NMR spectroscopy have demonstrated that inhibition of PI3K/AKT/mTOR signalling pathway by PI-103 reduced choline kinase activity, resulting in decreased in PCho in colon cancer cells [27]. Venkatesh et al. [28] has also demonstrated that treatment with the PI3K inhibitor LY294002 and mTOR inhibitor everolimus decreased phosphocholine levels associated with decreased in choline kinase activity in glioblastoma cell lines. However other studies have shown that phosphocholine content of cancer cells isn’t consistently altered by treatment with PI3K/Akt/mTOR inhibitors [29].
In summary treatment of tumour cells with pan-Akt and pan-mTOR synergistically inhibited the growth of cancer cells and was associated with arrest in G0/G1. Radiolabelled choline uptake was most strongly decreased by dual drug treatment and in combination with PET may be a useful non-invasive indicator of efficacious drug combinations.
References
Sanchez-Vega F, Mina M, Armenia J, Chatila WK, Luna A, La KC et al (2018) Oncogenic signaling pathways in the Cancer genome atlas. Cell 173:321–337. https://doi.org/10.1016/j.cell.2018.03.035
Millis SZ, Ikeda S, Reddy S, Gatalica Z, Kurzrock R (2016) Landscape of phosphatidylinositol-3-kinase pathway alterations across 19784 diverse solid tumors. JAMA Oncol 2:1565–1573. https://doi.org/10.1001/jamaoncol.2016.0891
Yap TA, Bjerke L, Clarke PA, Workman P (2015) Drugging PI3K in cancer: refining targets and therapeutic strategies. Curr Opin Pharmacol 23:98–107. https://doi.org/10.1016/j.coph.2015.05.016
Prêtre V, Wicki A (2018) Inhibition of Akt and other AGC kinases: a target for clinical cancer therapy? Semin Cancer Biol 48:70–77. https://doi.org/10.1016/j.semcancer.2017.04.011
Ewald F, Nörz D, Grottke A, Bach J, Herzberger C, Hofmann BT, Nashan B, Jücker M (2015) Vertical targeting of AKT and mTOR as well as dual targeting of AKT and MEK signaling is synergistic in hepatocellular carcinoma. J Cancer 6:1195–1205. https://doi.org/10.1007/s10637-014-0149-7
Feldman ME, Apsel B, Uotila A, Loewith R, Knight ZA, Ruggero D, Shokat KM (2009) Active-site inhibitors of mTOR target rapamycin-resistant outputs of mTORC1 and mTORC2. PLoS Biol 7:e38. https://doi.org/10.1371/journal.pbio.1000038
Jansen VM, Mayer IA, Arteaga CL (2016) Is there a future for AKT inhibitors in the treatment of cancer? Clin Cancer Res 22:2599–2601. https://doi.org/10.1158/1078-0432.CCR-16-0100
Chia S, Gandhi S, Joy AA, Edwards S, Gorr D, Hopkins S, Kondejewski J, Ayoub JP, Califaretti N, Rayson D, Dent SF (2015) Novel agents and associated toxicities of inhibitors of the pi3k/Akt/mtor pathway for the treatment of breast cancer. Curr Oncol 22:33–48. https://doi.org/10.3747/co.22.2393
Yap TA, Yan L, Patnaik A, Fearen I, Olmos D, Papadopoulos K, Baird RD, Delgado L, Taylor A, Lupinacci L, Riisnaes R, Pope LL, Heaton SP, Thomas G, Garrett MD, Sullivan DM, de Bono JS, Tolcher AW (2011) First-in man clinical trial of the oral pan-AKT inhibitor MK-2206 in patients with advanced solid tumors. J Clin Oncol 29:4688–4695. https://doi.org/10.1200/JCO.2011.35.5263
Fleming IN, Andriu A, Smith TAD (2014) Early changes in [18F] FDG incorporation by breast cancer cells treated with trastuzumab in normoxic conditions: role of the Akt-pathway, glucose transport and HIF-1α. Breast Cancer Res Treat 144:241–248. https://doi.org/10.1007/s10549-014-2858-1
Al-saeedi F, Smith T, Welch A (2007) [Methyl-3H]-choline incorporation into MCF-7 cells: correlation with proliferation - choline kinase and phospholipase D assay. Anticancer Res 27:901–906
Kenny LM, Contractor KB, Hinz R, Stebbing J, Palmieri C, Jiang J, Shousha S, Al-Nahhas A, Coombes RC, Aboagye EO (2010) Reproducibility of [C-11]choline-positron emission tomography and effect of Trastuzumab. Clin Cancer Res 16:4236–4245. https://doi.org/10.1158/1078-0432.CCR-10-0468
Chou TC (2010) Drug combination studies and their synergy quantification using the Chou-Talalay method. Cancer Res 70:440–446. https://doi.org/10.1158/0008-5472.CAN-09-1947
Al-Saeedi F, Welch AE, Smith TAD (2005) [Methyl-H-3]Choline incorporation into MCF7 tumour cells: correlation with proliferation Eur. J Nucl Med Mol Imag 32:660–667. https://doi.org/10.1007/s00259-004-1707-6
Moestue SA, Dam CG, Gorad SS, Kristian A, Bofin A, Maelandsmo GM, Engebraten O, Gribbestad IS, Bjorkoy G (2013) Metabolic biomarkers for response to PI3K inhibition in basal-like breast cancer. Breast Cancer Res 15:R16. https://doi.org/10.1186/bcr3391
Chresta CM, Davies BR, Hickson I, Harding T, Cosulich S, Critchlow SE, Vincent JP, Ellston R, Jones D, Sini P, James D, Howard Z, Dudley P, Hughes G, Smith L, Maguire S, Hummersone M, Malagu K, Menear K, Jenkins R, Jacobsen M, Smith GCM, Guichard S, Pass M (2010) AZD8055 is a potent, selective, and orally bioavailable ATP-competitive mammalian target of rapamycin kinase inhibitor with in vitro and in vivo antitumor activity. Cancer Res 70:288–298. https://doi.org/10.1158/0008-5472.CAN-09-1751
She QB, Chandarlapaty S, Ye Q, Lobo J, Haskell KM, Leander KR, DeFeo-Jones D, Huber HE, Rosen N (2008) Breast tumor cells with PI3K mutation or HER2 amplification are selectively addicted to Akt signaling. PLoS One 3:e3065. https://doi.org/10.1371/journal.pone.0003065
Harada S, Yanagisawa M, Iwai T, Aida S, Kurasawa M, Yorozu K, Yamamoto K, Harada N (2013) Antitumor activities of bevacizumab for KRAS, BRAF, and PIK3CA mutated human colorectal cancer xenograft models. J Clin Oncol (S4):31, ab362. https://doi.org/10.1200/jco.2013.31.4_suppl.362
English DP, Roque DM, Carrara L, Lopez S, Bellone S, Cocco E, Bortolomai I, Schwartz PE, Rutherford T, Santin AD (2013) HER2/neu gene amplification determines the sensitivity of uterine serous carcinoma cell lines to AZD8055, a novel dual mTORC1/2 inhibitor. Gynaecological Oncol 131:753–758. https://doi.org/10.1016/j.ygyno.2013.08.033
Qian JC, Chen YQ, Meng T, Ma LP, Meng LF, Wang X, Yu T, Zask A, Shen JK, Yu K (2016) Molecular regulation of apoptotic machinery and lipid metabolism by mTORC1/mTORC2 dual inhibitors in preclinical models of HER2+/PIK3CAmut breast cancer. Oncotarget 7:67071–67086. https://doi.org/10.18632/oncotarget.11490
Jiao P, Zhou YS, Yang JX, Zhao YL, Liu QQ, Yuan C, Wang FZ (2013) MK-2206 induces cell cycle arrest and apoptosis in HepG2 cells and sensitizes TRAIL-mediated cell death. Mol Cell Biochem 382:217–224. https://doi.org/10.1007/s11010-013-1737-0
Wilson JM, Kunnimalaiyaan S, Gamblin TC, Kunnimalaiyaan M (2014) MK2206 inhibits hepatocellular carcinoma cellular proliferation via induction of apoptosis and cell cycle arrest. J Surg Res 191:280–285. https://doi.org/10.1016/j.jss.2014.05.083
Aboagye EO, Bhujwalla ZM (1999) Malignant transformation alters membrane choline phospholipid metabolism of human mammary epithelial cells. Cancer Res 59:80–84
Glunde K, Bhujwalla ZM (2011) Metabolic tumor imaging using magnetic resonance spectroscopy. Semin Oncol 38:26–41. https://doi.org/10.1053/j.seminoncol.2010.11.001
Smith TAD, Glaholm J, Leach MO, Machin L, Collins DJ, Payne GS, McCready VR (1991) A comparison of in vivo and in vitro P-31 NMR-spectra from human breast-tumours - variations in phospholipid-metabolism. Br J Cancer 63:514–516. https://doi.org/10.1038/bjc.1991.122
Leach MO, Verrill M, Glaholm J, Smith TAD, Collins DJ, Payne GS, Sharp J, Ronen SM, McCready VR, Powles TJ, Smith IE (1998) Measurements of human breast Cancer using magnetic resonance spectroscopy: a review of clinical measurement and a report of localized 31P measurements of response to treatment. NMR Biomed 11:314–340. https://doi.org/10.1002/(SICI)1099-1492(1998110)11:7<314::AID-NBM522>3.0.CO;2-Z
Al-Saffar NMS, Jackson LE, Raynaud FI, Clarke PA, de Molina AR, Lacal JC, Workman P, Leach MO (2010) The phosphoinositide 3-kinase inhibitor PI-103 downregulates choline kinase a leading to Phosphocholine and Total choline decrease detected by magnetic resonance spectroscopy. Cancer Res 70:5507–5517. https://doi.org/10.1158/0008-5472.CAN-09-4476
Venkatesh HS, Chaumeil MM, Ward CS, Haas-Kogan DA, James CD, Ronen SM (2012) Reduced phosphocholine and hyperpolarized lactate provide magnetic resonance biomarkers of PI3K/Akt/mTOR inhibition in glioblastoma. Neuro-Oncol 14:315–325. https://doi.org/10.1093/neuonc/nor209
Phyu SM, Tseng CC, Fleming IN, Smith TAD (2016) Probing the PI3K/Akt/mTor pathway using 31P-NMR spectroscopy: routes to glycogen synthase kinase 3. Sci Rep 6:36544. https://doi.org/10.1038/srep36544
Acknowledgements
The University of Aberdeen Development Trust is gratefully acknowledged.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
TADS declares that he has no conflict of interest. SMP declares that she has no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Phyu, S.M., Smith, T.A.D. Combination treatment of cancer cells with pan-Akt and pan-mTOR inhibitors: effects on cell cycle distribution, p-Akt expression level and radiolabelled-choline incorporation. Invest New Drugs 37, 424–430 (2019). https://doi.org/10.1007/s10637-018-0642-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10637-018-0642-5