Abstract
Low health literacy and poor retention in care may contribute to HIV health disparities among African Americans, but causal pathways have not been examined. We utilized an adapted health literacy model to examine the role of health literacy on racial disparities in retention in care. Retention in care for 699 participants was assessed 24-months post survey and operationalized as 100% visit adherence versus less than 100% visit adherence. Most participants were African American (60%) and virally suppressed (93%). Results from a path analysis revealed that non-African American race was related to greater health literacy (p = .023) and to 100% visit adherence (p = .024). Greater health literacy was associated with 100% visit adherence (p = .008), which was in turn related to viral suppression (p < .001). Findings indicate that health literacy partially mediates the relationship between race and retention in care and are among the first to suggest these causal pathways.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
African Americans represent the greatest proportion of persons diagnosed, living with, and dying from HIV among all racial and ethnic groups [1, 2]. African Americans are also less likely than White and Hispanic/Latino persons living with HIV (PLWH) to attend regularly scheduled HIV appointments [3]. Poor retention in care is a significant predictor of antiretroviral treatment (ART) failure [4] and contributes to HIV morbidity and mortality among African Americans, including elevated HIV viral load [5,6,7], decreased CD4 count [8], development of AIDS-defining illnesses [5, 6, 9], and death [10]. Due to the significance of retention in care on HIV outcomes, understanding factors that contribute to poor retention in care may assist in improving HIV health disparities among African Americans.
Increasing evidence suggests a link between health literacy and retention in HIV care [11]. Health literacy is the ability to access, process, and use health information. Among African American adults, average health literacy is 20% lower than among White adults [12]. Lower health literacy may contribute to missed HIV appointments [13, 14], poor knowledge of HIV [15], and ART non-adherence [16, 17]. Low health literacy among African Americans combined with its negative effects on retention in care and HIV health outcomes suggests that health literacy may contribute to disparities in retention in care among African Americans.
Although health literacy is shaped by a variety of factors, this study focuses on the effects of socioeconomic status [18] and cognitive function [19]. Socioeconomic status encompasses a range of economic and social factors, such as education and income, and influences whether individuals seek out health information, where they will look, and how they will interpret health information [20]. Cognitive function is directly associated with health literacy among PLWH [21,22,23] and is influenced by HIV’s negative neurologic effects [24,25,26,27]. Health literacy is also associated with the patient-provider relationship and evidence suggests a direct effect of the patient-provider relationship on retention in care [28]. Poor health literacy minimizes effective communication between PLWH and their health care providers [29,30,31], which contributes to ART non-adherence [16, 32] and poor HIV health outcomes [33].
Preliminary evidence suggests causal pathways linking health literacy to health outcomes among disparate populations, but no studies have examined these pathways for retention in care among African Americans living with HIV. Among PLWH, health literacy mediates the relationship between gender and ART medication adherence [21], as well as between race and ART medication adherence [34, 35]. Due to disparities in retention in care and health literacy among African Americans and due to emerging causal pathways between health literacy and health outcomes, examining pathways linking health literacy and retention in care may identify potentially modifiable contributors associated with HIV health disparities.
For this study, we adapted Paasche-Orlow and Wolf’s health literacy model [36] to inform relationships among health literacy, retention in care, HIV clinical outcomes, and sociodemographic indicators of health literacy. Our model (Fig. 1) proposes that health literacy mediates the relationship between race and retention in care and that retention in care mediates the relationship between health literacy and HIV viral load. This model also proposes that socioeconomic status and cognitive function influence health literacy, which in turn influences the patient-provider relationship and HIV viral load. The purpose of this study is to test the proposed model in the role of health literacy on racial disparities in retention in care and HIV clinical outcomes.
Methods
This study is ancillary to an observational longitudinal study. The parent study recruited a purposive sample of participants from June 2012 to December 2015 from four outpatient HIV clinics in metro-Atlanta, Georgia. Methods for the parent study are described elsewhere [37]. The parent study collected several measures at baseline for 699 participants, including demographic information, health literacy, cognitive function, and patient-provider interactions. This ancillary study collected HIV viral load, socioeconomic status, and retention in care data from participant electronic medical records (EMR).
Measures
Race and covariates known to be associated with the variables in the adapted health literacy model were collected via participant self-report at baseline. For this study, we categorized race as African American versus non-African American. Covariates included sex (born male/identify male; born female/identify female; born male/identify female; born female/identify male), marital status (never married/single; married, divorced/separated; widow/widower; living with partner/significant other; other), sexual orientation (homosexual, gay, or lesbian; heterosexual or straight; a man who has sex with men; bisexual; other; I choose not to answer), education (never attended school; grades 1 through 8; grades 9 through 11; grade 12 or GED; some college, associate’s degree or technical degree; bachelor’s degree; any post graduate studies), and age.
In accordance with previous research, we used insurance as a proxy for socioeconomic status (SES; [13, 38, 39]). We collected insurance data from the participant’s EMR that corresponded closest to the baseline interview date. We categorized participant SES as “not low SES” if using private or commercial insurance or self-pay; “low SES” if receiving Ryan White (income eligibility for Ryan White is less than 400% of the federal poverty level; [40]) “very low SES” if receiving Medicare or Medicaid services (income eligibility requirement for Medicaid in Georgia is less than 133% of the federal poverty level; [41]).
Cognitive Function was assessed using the Hopkins Verbal Learning Test Revised (HVLT-R; [42]) and Color Trails Test (CTT) 1 and 2 [43]. The HVLT-R uses verbal list learning tasks to measure verbal learning and memory [42]. CTT 1 and 2 measures attention and mental flexibility, a component of executive functioning [43]. For CTT 1 and 2, participants use a pencil to sequentially connect colored circles containing numbers and for CTT 2, participants must alternate between different colored circles in numeric order. For analysis, we created a continuous measure of cognitive function by averaging the baseline T-scores for HVLT-R, CTT 1, and CTT 2.
Health literacy was measured using the Short-Test of Functional Health Literacy (S-TOFHLA; [44]). S-TOFHLA includes prose passages and numeracy items to assess reading comprehension and numerical abilities, respectively. Health passages are from an upper gastrointestinal series, the patient’s rights and responsibilities section of the Medicaid application form, and a standard hospital informed consent form. The numeracy items are related to medication directions, blood glucose monitoring, and clinic appointments. The S-TOFHLA score is the cumulative percent correct for the prose passages and numeracy items. S-TOFHLA correlates well with other measures of health literacy [44].
The Attitudes Towards the HIV Health Care Provider Scale (ATHCP) [45] assessed patient attitudes toward the HIV health care provider. Participants score the 19-item scale using a 6-point Likert scale (1 = strongly disagree to 6 = strongly agree), with total scores ranging from 19 to 114. Higher total scores indicate more positive attitudes towards the HIV health care provider. The Cronbach’s alpha for participants in this study (α = 0.92) is consistent with previous research (α = 0.69; [45]).
Retention in care was defined as visit adherence [46], which is the percentage of kept HIV appointments out of all scheduled HIV appointments over a 24-month post baseline period. We extracted all outpatient appointments with an HIV primary care provider, including physicians and advanced care providers, who have prescribing authority. We excluded specialty HIV care visits, nursing visits, and laboratory visits. We collected the status of the appointment, such as completed, cancelled/missed, or no-show and used appointments with a completed status to represent kept HIV appointments. The total number of appointments with completed, cancelled/missed, or no-show status represented scheduled HIV appointments.
The health outcome of interest was HIV viral load. We obtained participant HIV viral load laboratory data from each participant’s EMR. We obtained a single HIV-1 RNA viral load value and laboratory collection date that was closest to the participant’s 24-month post baseline date. We categorized viral load as virally suppressed or non-suppressed based on the cut-point of 200 copies/mL, which corresponds to 2.3 log10. This definition is consistent with the Centers for Disease Control and Prevention’s criteria for viral suppression [47].
Statistical Analysis
Preliminary analyses of all study variables included descriptive statistics. We checked data for distributional assumptions and independence of observations using histograms and residual plots. Descriptive statistics of the visit adherence variable revealed a non-parametric distribution and the presence of two unique visit adherence groups—participants who attended 100% of their scheduled HIV appointments and participants who attended less than 100% of their scheduled HIV appointments. Due to the presence of these two unique groups, we conducted the analysis using a binary visit adherence outcome that compared PLWH with 100% visit adherence to PLWH with less than 100% visit adherence.
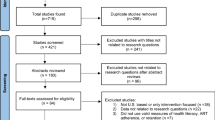
Due to low response rates for some categorical demographic covariates, we collapsed categories to have adequate cell sizes. These included sex/gender (identify male; identify female), marital status (single/never married; previously married; married/living with partner), sexual orientation (heterosexual; non-heterosexual), and education (less than high school; high school/GED; greater than high school). We removed participants who reported “other” for their marital status (n = 5), as we were unable to appropriately categorize these individuals into one of the marital status categories. Participants with no HIV appointments during the 24-month post-baseline follow-up period (n = 48) and participants missing HIV viral load data (n = 14) were dropped from the data set. We also assessed for outliers and removed 12 participants whose total number of scheduled HIV appointments were three standard deviations above the mean (mean = 12.75 ± 11.01). The participant sample size for this study is 699. After eliminating missing data and outliers, the final total sample size is 620 participants. Of these participants, 11 passed away at some point during the duration of the study; however, we included these participant’s data, as they completed baseline assessments and had scheduled HIV appointments during the study follow-up period. Examination of missing data identified data missing at random for cognitive function (1.24%), ATHCP (0.77%), insurance/SES (4.64%), and sex/gender (0.31%). We performed multiple imputation for variables with missing data in Mplus version 8.2 using the IMPUTE command, which utilizes a Bayesian estimator [48,49,50]. We used all study variables for imputation and created ten imputed data sets.
We performed path analysis in Mplus using theta parameterization and the imputed datasets to test the relationships hypothesized in the adapted health literacy model. Mplus performed the specified path analysis for each of the ten imputed data sets, pooling parameter estimates over the set of analyses and calculating standard errors using the average of the standard errors and between analysis parameter estimate variation [49, 50]. In the path analysis, we controlled for covariates that had a significant correlation (p < .05) with endogenous variables. The focus of the path analysis was on the statistical significance of the pathways and model goodness of fit. We assessed goodness of fit using chi squared (χ2), root mean squared residual (RMSR), standardized root mean squared residual (SRMR), Comparative Fit Index (CFI), and Tucker-Lewis Index (TLI). The RMSR and SRMR suggest relatively good model fit when they are less than 0.06 and 0.08, respectively, and the CFI and TLI suggest good model fit when they are greater than 0.95 [51]. We performed preliminary analyses using SAS Studio software, version 3.71, and conducted multiple imputation and path analysis in Mplus version 8.2.
Results
Descriptive statistics of all study variables for the non-imputed data set are detailed in Table 1. Most participants were African American (60.97%), while 32.18% identified White/non-Hispanic, 2.52% identified Hispanic/Latino, and 4.88% identified with another race (Asian, Native American/Alaska Native, Native Hawaiian/Other Pacific Islander, or biracial). Participants were predominately single/never married (56.94%), very low SES (45.08%), and had greater than high school education (58.87%). Most participants identified male (69.58%) and there were 16 transgender women in the female sex/gender category. The mean age of participants was 47.99 years (SD = 9.93) and on average participants were living with HIV for 15.55 years (SD = 8.54). Most participants were virally suppressed (92.58%) and attended less than 100% of their scheduled HIV appointments (62.10%). Overall, health literacy scores were high. On average, participants correctly answered 91.46% of reading comprehension and numeracy portions of the S-TOFHLA. African Americans exhibited significantly lower health literacy (88.89% ± 13.51) compared to non-African Americans (94.90% ± 8.37; p < .001).
Over the 24-month period, PLWH with 100% and less than 100% visit adherence had 8.35 ± 5.66 (range 1–33) and 14.02 ± 8.47 (range 1–43) scheduled HIV appointments, respectively. Participants with less than 100% visit adherence attended an average of 74.14% of their scheduled HIV appointments (range 0–98%) and African Americans comprised 64.81% of participants with less than 100% visit adherence.
Bivariate analyses showed multicollinearity between health literacy, education, and cognitive function. Health literacy was significantly correlated with education (r = 0.44, p < .0001) and cognitive function (r = 0.41, p < .0001), which collectively explained 31% of the variance in health literacy [F = (2, 609) = 139.51, p < .0001]. Due to concerns of multicollinearity, education was not included as a covariate in the path analysis, as it is a less robust measure compared to cognitive function. Additional bivariate correlations identified that sex/gender (r = − 0.14, p < .001), and sexual orientation (r = 0.16, p < .001) were significantly correlated with S-TOFHLA and that age was significantly correlated with viral load (r = 0.20, p < .001). No covariates were significantly correlated to visit adherence or ATHCP. Consequently, the path analysis controlled for the effect of sex and sexual orientation on S-TOFHLA and for the effect of age on viral load.
Findings from the path analysis are in Fig. 2 and include standardized beta coefficients, standard errors, and p values. Non-African American race was directly related to 100% visit adherence (p = .024), which was subsequently associated with viral suppression (p < .001). Additionally, Non-African Americans had greater health literacy (p = .023), which was in turn associated with 100% visit adherence (p = .008). Higher cognitive function (p < .001) and low and very low SES (p = .010) were also related to greater health literacy. Higher health literacy was related to more favorable attitudes towards the health care provider (p < .001). Attitudes towards the health care provider were not directly related to 100% visit adherence (p = .068). Health literacy and attitudes towards the health care provider were not directly related to viral suppression (p = .126 and p = .237, respectively). Age was a significant covariate of viral load (p < .001) and all other covariates were non-significant. Table 2 includes the indirect effects of health literacy and visit adherence. The model demonstrated good fit (χ2 = 16.624, p = .480; RMSEA = 0.002; SRMR = 0.042; CFI = 0.999; TLI = 1.003) and explains 21.3% of variance in health literacy, 38.0% of variance in viral load, 4.3% of variance in visit adherence, and 1.5% of the variance in attitudes towards the HIV health care provider.
Structural equation model of direct effects of patient and social-level factors on health literacy and retention in care (N = 620). Model controls for the effect of sex and sexual orientation on S-TOFHLA and the effect of age on viral load. Significant covariates include the effect of age on viral load (p < .001). Standardized beta coefficients are presented. Dashed and solid lines represent paths that are non-significant and significant, respectively. SE standard error, SES socioeconomic status, ATHCP attitudes towards the HIV health care provider. Coding for categorical variables are as follows: race is 0 = African American, 1 = Non-African American; visit adherence is 0 = < 100% visit adherence, 1 = 100% visit adherence; viral load is 0 = not suppressed, 1 = suppressed; SES/Insurance is 0 = not low SES, 1 = low SES, 2 = very low SES
Discussion
This study adapted a health literacy model by Paasche-Orlow and Wolf to examine the role of health literacy on racial disparities in retention in care and HIV clinical outcomes. This study evaluated the mediating effect of health literacy on the relationship between race and retention in care and the mediating effect of retention in care on the relationship between health literacy and HIV viral load. This study also tested the effect of socioeconomic status and cognitive function on health literacy, as well as the effect of patient-provider interactions on retention in care and viral load. The study sample included participants from the Southern United States who were predominately African American, male, and very low SES. Although most participants were virally suppressed (93%), nearly two-thirds of participants failed to attend all scheduled HIV appointments.
To our knowledge, this study is among the first to examine causal pathways linking health literacy to health outcomes among racially disparate PLWH. Our results suggest that health literacy partially explains the relationship between race and retention in care. Specifically, non-African Americans had greater health literacy and were more likely to attend 100% of scheduled HIV appointments. This finding supports previous research which found a relationship between health literacy and retention in care [13, 14]. Also, findings are similar to studies which found a mediating effect of health literacy between race and ART medication adherence [34, 35, 37]. Another study found that numeracy—a component of health literacy necessary to understand and use mathematical operations in daily life—drove the mediating effect of health literacy on race and ART adherence [34]. Consistency between findings from this study and findings from other studies on health literacy and ART adherence hold promise that health literacy is a contributing factor to health disparities in retention in care among African Americans living with HIV.
We also found that health literacy mediates the relationship between sociodemographic predictors of health literacy (cognitive function and socioeconomic status) and retention in care, as well as patient provider interactions. Results suggested that higher cognitive function was related to greater health literacy, which was then associated with 100% visit adherence and more favorable attitudes towards the HIV health care provider. Findings on the association between greater health literacy and more favorable patient attitudes towards the HIV health care provider is consistent with past research [28,29,30,31]. Additionally, findings support the established relationship between cognitive function and health literacy [19, 21,22,23, 52]. Research remains inconsistent on the relationship between neurocognitive impairment and retention in care [53, 54], of which discrepancies may be associated with the method of operationalizing retention in care, the retention in care observation period, or the cognitive function measures [53, 54].
Additionally, low and very low SES were related to higher health literacy, which led to an increased likelihood of 100% visit adherence. The relationship between socioeconomic status and health literacy is contrary to the body of research on socioeconomic disparities and health literacy, specifically among PLWH [12, 18, 55, 56]. The sample of PLWH for this study are predominately very low SES (i.e., on Medicaid or Medicare), virally suppressed, and have been living with HIV for nearly 16 years. Therefore, it is possible that among persons with very low SES, the number of years spent managing their HIV infection has a positive effect on their overall health literacy. Other explanations for the association between low SES and high health literacy include variations in methods of defining SES, such as monthly or annual income or financial situation. Further study is warranted on the relationship between health literacy, SES, and retention in care among PLWH.
Our results indicate that retention in care mediates the relationship between health literacy and HIV viral load. Particularly, increased health literacy is related to 100% visit adherence, which is subsequently related to viral suppression. The relationship between increased health literacy and 100% visit adherence supports Jones et al. [14] and Rebeiro et al. [13] who found that increased health literacy is associated with attending more than 75% of regularly scheduled HIV appointments and with a decreased number of missed HIV appointments, respectively. The effect of 100% visit adherence on viral suppression is also consistent with research indicating a direct relationship between retention in care and viral load [5, 6]. Results did not suggest a direct relationship between health literacy and viral suppression and the literature on this relationship remains inconsistent [33, 57].
Study Limitations
Findings from this study should be interpreted within its limitations. Due to differences in each clinic’s scheduling practices, appointments may have been misclassified as completed, missed, or no-show, categories which were used to calculate percent visit adherence. Percent visit adherence may also provide a biased estimate of retention in care, as participants with few scheduled appointments may have a disproportionately lower percent visit adherence if they miss a visit compared to persons with many scheduled appointments. Furthermore, this study used a conservative approach for a retention in care cut-off (100% vs. < 100% visit adherence), which may inaccurately represent individuals who are sufficiently retained in care to achieve viral suppression. Additionally, viral load and appointment data were collected from four HIV recruiting clinics in Metro-Atlanta and we were unable to gather data from clinics outside of these primary sites.
Study findings may not be generalizable to populations outside of Metro-Atlanta Georgia or the Southern United States. Although the sample of PLWH utilized in this study have similar demographics to PLWH in Georgia, the percentage of PLWH with viral suppression from this study (93%) is greater than the proportion of virally suppressed persons in Georgia (85%; [58]) and the United States (60%; [59]) This study also provides limited information on populations most affected by HIV, such as men who have sex with men, injection drug users, or transgender persons.
Our analyses were insufficiently powered to utilize a bootstrap approach. Our sample size minimized risk of model non-convergence and improper solutions and allowed for detection of a small effect size [60]. However, future studies would benefit from increasing study sample size and conducting the path analysis using a bootstrap approach. Future research utilizing this model would also benefit from including additional variables, such as transportation, proximity to the health care clinic, and patient-provider dynamics.
Implications for Future Research
Primary findings from this study show that health literacy mediates the relationship between race and retention in care, a new finding in this area, and that retention in care subsequently influences HIV viral load. Socioeconomic status and cognitive function directly influence health literacy, which then influences retention in care and patient-provider interactions. Health care providers may find it beneficial to assess health literacy and predictors of health literacy, particularly cognitive function and SES, in order to provide more targeted health care to meet the individual needs of PLWH. Future research should focus on developing interventions for retention in care that account for patient level differences in health literacy. In developing these interventions, it may be beneficial to understand additional modifiable factors that may influence health literacy and retention in care. Through addressing health literacy and its effects on HIV outcomes, these interventions should ultimately improve patient outcomes and reduce HIV morbidity and mortality among health disparate populations.
References
Centers for Disease Control and Prevention. HIV among African Americans. CDC Fact Sheet. 2018.
Centers for Disease Control and Prevention. Diagnoses of HIV infection in the United States and dependent areas, 2016. Nov 2016.
Centers for Disease Control and Prevention. HIV in the United States: the stages of care. Atlanta: Centers for Disease Control and Prevention; 2012.
Rastegar DA, Fingerhood MI, Jasinski DR. Highly active antiretroviral therapy outcomes in a primary care clinic. AIDS Care. 2003;15(2):231–7.
Giordano TP, Gifford AL, White AC Jr, Suarez-Almazor ME, Rabeneck L, Hartman C, et al. Retention in care: a challenge to survival with HIV infection. Clin Infect Dis. 2007;44(11):1493–9.
Crawford TN. Poor retention in care one-year after viral suppression: a significant predictor of viral rebound. AIDS Care. 2014;26(11):1393–9.
Mugavero MJ, Amico KR, Westfall AO, Crane HM, Zinski A, Willig JH, et al. Early retention in HIV care and viral load suppression: implications for a test and treat approach to HIV prevention. J Acquir Immune Defic Syndr. 2012;59(1):86–93.
Berg MB, Safren SA, Mimiaga MJ, Grasso C, Boswell S, Mayer KH. Nonadherence to medical appointments is associated with increased plasma HIV RNA and decreased CD4 cell counts in a community-based HIV primary care clinic. AIDS Care. 2005;17(7):902–7.
Park WB, Choe PG, Kim SH, Jo JH, Bang JH, Kim HB, et al. One-year adherence to clinic visits after highly active antiretroviral therapy: a predictor of clinical progress in HIV patients. J Intern Med. 2007;261(3):268–75.
Mugavero MJ, Westfall AO, Cole SR, Geng EH, Crane HM, Kitahata MM, et al. Beyond core indicators of retention in HIV care: missed clinic visits are independently associated with all-cause mortality. Clin Infect Dis. 2014;59(10):1471–9.
Mallinson RK, Relf MV, Dekker D, Dolan K, Darcy A, Ford A. Maintaining normalcy: a grounded theory of engaging in HIV-oriented primary medical care. ANS Adv Nurs Sci. 2005;28(3):265–77.
U.S. Department of Education. The health literacy of America’s adults: results from the 2003 national assessment of adult literacy. Washington, DC: National Center for Education Statistics, Institute of Education Sciences; 2006.
Rebeiro PF, McPherson TD, Goggins KM, Turner M, Bebawy SS, Rogers WB, et al. Health literacy and demographic disparities in HIV care continuum outcomes. AIDS Behav. 2018;22(8):2604–14.
Jones D, Cook R, Rodriguez A, Waldrop-Valverde D. Personal HIV knowledge, appointment adherence, and HIV outcomes. AIDS Behav. 2013;17(1):242–9.
Kalichman SC, Benotsch E, Suarez T, Catz S, Miller J, Rompa D. Health literacy and health-related knowledge among persons living with HIV/AIDS. Am J Prev Med. 2000;18(4):325–31.
Kalichman SC, Ramachandran B, Catz S. Adherence to combination antiretroviral therapies in HIV patients of low health literacy. J Gen Intern Med. 1999;14(5):267–73.
Miller LG, Liu H, Hays RD, Golin CE, Ye Z, Beck CK, et al. Knowledge of antiretroviral regimen dosing and adherence: a longitudinal study. Clin Infect Dis. 2003;36(4):514–8.
Mantwill S, Monestel-Umaña S, Schulz PJ. The relationship between health literacy and health disparities: a systematic review. PLoS ONE. 2015;10(12):e0145455.
Serper M, Patzer RE, Curtis LM, Smith SG, O’Conor R, Baker DW, et al. Health literacy, cognitive ability, and functional health status among older adults. Health Serv Res. 2014;49(4):1249–67.
Institute of Medicine of the National Academies. Health literacy: a prescription to end confusion. Washington, D.C.: The National Academies Press; 2004.
Waldrop-Valverde D, Jones DL, Gould F, Kumar M, Ownby RL. Neurocognition, health-related reading literacy, and numeracy in medication management for HIV infection. AIDS Patient Care STDS. 2010;24(8):477–84.
Waldrop-Valverde D, Jones DL, Weiss S, Kumar M, Metsch L. The effects of low literacy and cognitive impairment on medication adherence in HIV-positive injecting drug users. AIDS Care. 2008;20(10):1202–10.
Vance DE, Rubin LH, Valcour V, Waldrop-Valverde D, Maki PM. Aging and neurocognitive functioning in HIV-infected women: a review of the literature involving the women’s interagency HIV study. Curr HIV/AIDS Rep. 2016;13(6):399–411.
Grant I, Atkinson JH, Hesselink JR, Kennedy CJ, Richman DD, Spector SA, et al. Evidence for early central nervous system involvement in the acquired immunodeficiency syndrome (AIDS) and other human immunodeficiency virus (HIV) infections. Studies with neuropsychologic testing and magnetic resonance imaging. Ann Intern Med. 1987;107(6):828–36.
Martin EM, Robertson LC, Edelstein HE, Jagust WJ, Sorensen DJ, San Giovanni D, et al. Performance of patients with early HIV-1 infection on the Stroop Task. J Clin Exp Neuropsychol. 1992;14(5):857–68.
Peavy G, Jacobs D, Salmon DP, Butters N, Delis DC, Taylor M, et al. Verbal memory performance of patients with human immunodeficiency virus infection: evidence of subcortical dysfunction. The HNRC Group. J Clin Exp Neuropsychol. 1994;16(4):508–23.
Wilkie FL, Goodkin K, van Zuilen MH, Tyll MD, Lecusay R, Edwin T. Cognitive effects of HIV-1 infection. CNS Spectr. 2000;5(5):33–51.
Beach MC, Keruly J, Moore RD. Is the quality of the patient-provider relationship associated with better adherence and health outcomes for patients with HIV? J Gen Intern Med. 2006;21(6):661–5.
Kripalani S, Jacobson TA, Mugalla CI, Cawthon RC, Niesner KJ, Vaccarino V. Health literacy and the quality of physician-patient communication during hospitalization. J Hosp Med. 2010;5(5):269–75.
Katz MG, Jacobson TA, Veledar E, Kripalani S. Patient literacy and question-asking behavior during the medical encounter: a mixed-methods analysis. J Gen Intern Med. 2007;22(6):782–6.
Williams MV, Davis T, Parker RM, Weiss BD. The role of health literacy in patient-physician communication. Fam Med. 2002;34(5):383–9.
Baker DW, Parker RM, Williams MV, Pitkin K, Parikh NS, Coates W, et al. The health care experience of patients with low literacy. Arch Fam Med. 1996;5(6):329–34.
Kalichman SC, Rompa D. Functional health literacy is associated with health status and health-related knowledge in people living with HIV-AIDS. J Acquir Immune Defic Syndr. 2000;25(4):337–44.
Waldrop-Valverde D, Osborn CY, Rodriguez A, Rothman RL, Kumar M, Jones DL. Numeracy skills explain racial differences in HIV medication management. AIDS Behav. 2010;14(4):799–806.
Osborn CY, Paasche-Orlow MK, Davis TC, Wolf MS. Health literacy: an overlooked factor in understanding HIV health disparities. Am J Prev Med. 2007;33(5):374–8.
Paasche-Orlow MK, Wolf MS. The causal pathways linking health literacy to health outcomes. Am J Health Behav. 2007;31(1):S19–26.
Waldrop-Valverde D, Murden RJ, Guo Y, Holstad M, Ownby RL. Racial disparities in HIV antiretrovial medication management are mediated by health literacy. Health Lit Res Pract. 2018;2(4):205–13.
Chen SY, Moss WJ, Pipkin SS, McFarland W. A novel use of AIDS surveillance data to assess the impact of initial treatment regimen on survival. Int J STD AIDS. 2009;20(5):330–5.
Jain S, Schwarcz S, Katz M, Gulati R, McFarland W. Elevated risk of death for African Americans with AIDS, San Francisco, 1996-2002. J Health Care Poor Underserved. 2006;17(3):493–503.
Georgia Department of Public Health. Georgia Ryan White Part B, AIDS Drug Assistance Program (ADAP), and Health Insurance Continuation Program (HICP) Policies and Procedures 2017; 2017. p. 16.
Georgia Department of Community Health. Eligibility FAQs: Who is eligible for Medicaid? 2018. https://medicaid.georgia.gov/eligibility-faqs#field_related_links-431-0. Accessed 4 May 2019.
Brandt J, Benedict RHB. Hopkins verbal learning test—revised. Professional manual. Lutz: Psychological Assessment Resources, Inc.; 2001.
D’Elia LF, Satz P, Uchiyama CL, White T. Color trails test (CTT). Odessa: Psychological Assessment Resources, Inc.; 1994.
Baker DW, Williams MV, Parker RM, Gazmararian JA, Nurss J. Development of a brief test to measure functional health literacy. Patient Educ Couns. 1999;38(1):33–42.
Bodenlos JS, Grothe KB, Kendra K, Whitehead D, Copeland AL, Brantley PJ. Attitudes toward HIV health care providers scale: development and validation. AIDS Patient Care STDS. 2004;18(12):714–20.
Mugavero MJ, Westfall AO, Zinski A, Davila J, Drainoni ML, Gardner LI, et al. Measuring retention in HIV care: the elusive gold standard. J Acquir Immune Defic. 2012;61(5):574–80.
Centers for Disease Control and Prevention. HIV Treatment as Prevention. Atlanta, Georgia. 2018. https://www.cdc.gov/hiv/risk/art/index.html. Accessed 4 May 2019.
Rubin DB. Multiple imputation for nonresponse in surveys. Hoboken: Wiley; 1987.
Schafer JL. Analysis of incomplete multivariable data. Boca Raton: Chapman & Hall/CRC; 1997.
Muthén LK, Muthén BO. Mplus User’s Guide. 8th ed. Los Angeles, CA: Muthén & Muthén; 1998-2017.
Hu L-T, Bentler PM. Cutoff criteria for fit indexes in covariance structure analysis: conventional criteria versus new alternatives. Struct Equ Model. 1999;6(1):1–55.
Ownby RL, Acevedo A, Waldrop-Valverde D, Jacobs RJ, Caballero J. Abilities, skills and knowledge in measures of health literacy. Patient Educ Couns. 2014;95(2):211–7.
Jacks A, Arcy Wainwright D, Salazar L, Grimes R, York M, Strutt A, et al. Neurocognitive deficits increase risk of poor retention in care among older adults with newly diagnosed HIV infection. AIDS. 2015;29:1711–4.
Waldrop-Valverde D, Guo Y, Ownby RL, Rodriguez A, Jones DL. Risk and protective factors for retention in HIV care. AIDS Behav. 2014;18(8):1483–91.
Ayotte BJ, Allaire JC, Bosworth H. The associations of patient demographic characteristics and health information recall: the mediating role of health literacy. Aging Neuropsychol Cogn. 2009;16(4):419–32.
Rikard RV, Thompson MS, McKinney J, Beauchamp A. Examining health literacy disparities in the United States: a third look at the National Assessment of Adult Literacy (NAAL). BMC Public Health. 2016;16(1):975.
Kalichman SC, Rompa D, Cage M. Reliability and validity of self-reported CD4 lymphocyte count and viral load test results in people living with HIV/AIDS. Int J STD AIDS. 2000;11(9):579–85.
Georgia Department of Public Health. Georgia HIV care continuum update: persons living with HIV, and persons diagnosed with HIV, 2017. Atlanta: Georgia Department of Public Health; 2017.
Centers for Disease Control and Prevention. Selected national HIV prevention and care outcomes in the United States. Atlanta: Centers for Disease Control and Prevention; 2018.
Boomsma A, Hoogland JJ. The robustness of LISREL modeling revisited. In: Cudeck R, Du Toit S, Sorbom D, editors. Structural equation modeling: present and future. Lincolnwood: Scientific Software Internation, Inc.; 2001. p. 1–25.
Funding
This study was funded by the National Institute of Nursing Research and the National Institute of Mental Health of the National Institutes of Health under the following Award Numbers: F31 NR017580 (Principle Investigator [PI]: Ashley N. Anderson), R01 MH092284 (PI: Drenna Waldrop-Valverde), P30 NR014134 (PI: Drenna Waldrop-Valverde), T32NR012715 (PI: Sandra Dunbar). This work was also supported by the Center for AIDS Research at Emory University (P30AI050409).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of Emory University’s Institutional Review Board and with the Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Anderson, A.N., Haardörfer, R., Holstad, M.M. et al. A Path Analysis of Patient and Social-Level Factors on Health Literacy and Retention in Care Among African Americans Living with HIV. AIDS Behav 24, 1124–1132 (2020). https://doi.org/10.1007/s10461-019-02699-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10461-019-02699-y