Abstract
Tumor blood vessels are a key target for cancer therapeutic management. Tumor cells secrete high levels of pro-angiogenic factors which contribute to the creation of an abnormal vascular network characterized by disorganized, immature and permeable blood vessels, resulting in poorly perfused tumors. The hypoxic microenvironment created by impaired tumor perfusion can promote the selection of more invasive and aggressive tumor cells and can also impede the tumor-killing action of immune cells. Furthermore, abnormal tumor perfusion also reduces the diffusion of chemotherapeutic drugs and radiotherapy efficiency. To fight against this defective phenotype, the normalization of the tumor vasculature has emerged as a new therapeutic strategy. Vascular normalization, by restoring proper tumor perfusion and oxygenation, could limit tumor cell invasiveness and improve the effectiveness of anticancer treatments. In this review, we investigate the mechanisms involved in tumor angiogenesis and describe strategies used to achieve vascular normalization.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
To support the high proliferative rate of cancer cells, tumors need to rapidly develop a new vascular network. However, tumor blood vessels are characterized by their immaturity, which impair their functionality [1]. The improper development of tumor blood vessels is caused in part by the abnormal levels of growth factors secreted by tumor and stromal cells, among which vascular endothelial growth factor (VEGF) plays a key role. Several other growth factors, including members of the angiopoietins, platelet-derived growth factor (PDGF-B) and transforming growth factor (TGF-β) families, have also been implicated in the formation of a defective vascular network in tumors [2]. The poor functionality of tumor blood vessels has profound consequences for the tumor microenvironment and can lead to hypoxia, decreased immune cell infiltration and activity, and increased risks of metastatic dissemination.
It has been suggested that anti-angiogenic therapies could correct the structural and functional flaws of tumor blood vessels, a process referred to as “vascular normalization” [3, 4]. The normalization of the tumor vasculature could restore proper blood vessel functions and may help in preventing cancer cells from acquiring an aggressive phenotype associated with a hypoxic microenvironment [5]. Furthermore, increased tumor perfusion would enhance the benefits of chemotherapeutic drugs and radiotherapy [6]. In this review, we highlight the hallmarks of tumor blood vessels and discuss potential signaling pathways that could be targeted to achieve vascular normalization.
Physiological blood vessels
Anatomy
Nutrients and oxygen supply and metabolic waste removal are ensured by an extensive vascular network. Blood vessels are organized in arteries, veins and capillaries with different morphological structures reflecting their functions in the body. The inner wall of blood vessels is composed of endothelial cells (ECs) forming a monolayer with a streamlined surface, interconnected by junctional molecules such as VE-cadherin and claudins. These ECs are bound to a basal membrane and surrounded by mural cells, which participate in maintaining the cohesion between EC themselves and the basal membrane, and in limiting hyperpermeability and vascular leakage. Furthermore, their contractile potential participates in the control of vessel diameter and blood pressure. Arteries are supported by multiple concentric layers of vascular smooth muscle cells to support the high-pressure system enabling transport of blood to capillaries. Veins, which are exposed to lower blood pressure, are surrounded by thinner smooth muscle cells layers. Blood vessels of smaller diameter (arterioles, venules and capillaries) are covered by specialized support cells called pericytes, which are involved in the maturation and stabilization of blood vessels, and play an essential role in EC differentiation and proliferation through direct contact and tight junctions.
Angiogenesis
In adults, blood vessels remain quiescent and rarely form new branches under physiological conditions. The vascular network develops during early embryogenesis through a combination of vasculogenesis and angiogenesis. While vasculogenesis refers to the de novo formation of new blood vessels from endothelial progenitors, angiogenesis refers to the formation of vessels from a preexisting vascular network. Vascular growth during development, tissue repair or in disease conditions involves the sprouting, migration and proliferation of ECs, which are regulated by multiple factors among which VEGF plays a critical role (Fig. 1a).
Stages of the angiogenic process. a Destabilization of blood vessels. Angiogenic signals, such as VEGF, promote pericyte detachment from the basement membrane and weaken the extracellular matrix by proteolytic degradation. b Tip and stalk cell selection. ECs display characteristic phenotypes after VEGF stimulation: migratory tips cell or proliferating stalk cells. c Guidance and lumen formation. Attractive and repulsive cues control the guidance of tip cell and vessel lumen is generated to initiate blood flow. d Maturation of blood vessels. PDGF-B and Ang1 signaling lead to pericyte recruitment, while junctional molecules such as VE-cadherin act to consolidate EC–EC adhesion
Endothelial tip/stalk cell concept
ECs stimulated with VEGF adopt a pro-migratory phenotype. These ECs, which are at the lead of growing capillaries, have been referred as tip cells [7] (Figure 1b). Tip cells are motile, invasive and extend numerous filopodia that can respond to growth factors, extracellular matrix and other attractive or repulsive cues. During physiological angiogenic growth, a fraction of ECs will switch to the tip cell phenotype and initiate sprouting, whereas following ECs (stalk cells) will proliferate and contribute to the maintenance of the structural and functional integrity of nascent vessels. The Notch pathway, critical for its roles in cell fate determination and differentiation, participates in the regulation of tip/stalk EC conversion. Expression of the Notch ligand Delta-like 4 (Dll4) has been shown to be upregulated by VEGF receptor 2 (VEGFR2) and neuropilin-1 (NRP1) signaling following VEGF stimulation [8]. Dll4 binds Notch1 in neighboring ECs, leading to the cleavage and release of the Notch1 intracellular domain (NICD) [9]. NCID acts as a transcriptional regulator and limits VEGF signaling through the modulation of the expression of numerous genes involved in cellular responses to VEGF [10]. Indeed, Notch activity has been shown to decrease Vegfr2, Vegfr3 and Nrp1 expression and to upregulate vegfr1 [11]. VEGFR1 has weak kinase activity with a strong affinity for VEGF and can act as a decoy receptor, competitively reducing VEGF binding to VEGFR2 and therefore regulating VEGF signaling in ECs [12]. The ability of an EC to become a tip cell appears dependent on VEGFR2 level expression, VEGF environment and the capacity to express Dll4 promptly or with a high level compared to their neighbors [11]. By contrast, JAGGED1 (JAG1) is a Notch receptor ligand strongly expressed in stalk cells. JAG1 antagonizes Dll4–Notch1 signaling and enhances differential Notch activity by competitively interfering with the ability of Dll4 expressed by stalk cells to activate Notch1 in tip cells. JAG1 therefore helps to maintain the phenotype differentiation by preventing Notch signaling in tip cells [13].
Nascent vasculature expansion
To guide sprout formation and vascular patterning, tip cells deploy numerous filopodia (Fig. 1c). These act as antennae that respond to pro-angiogenic signals, promote motility, help focal adhesions and detect the presence of other cells [14]. CDC42 is a small GTPase of the Rho family that is associated with Wiskott–Aldrich syndrome proteins (WASPs) and participates in the formation and maintenance of filopodia. The cellular extension depends on lamellipodia and cytoplasmic protrusions composed of actin polymerization and controlled by Rac-Arp2/3 complexes [15,16,17]. Interestingly, a recent study demonstrated that filopodia are not essential for the guided migration of endothelial tip cells [18]. These data suggest that attractive and repulsive cues, integrated without filopodia, are sufficient to prevent EC misguidance [18].
Tip cell guidance
Attractive and repulsive cues control tip cell guidance (Fig. 1c). In recent years, several axon guidance molecules belonging to the Slit/Robo, netrin/DCC/Unc5 and neuropilin/plexin/sema families have been shown to mediate vascular patterning. Blocking NRP1 function inhibits endothelial tip cell migration, suggesting cooperation between VEGFR2 and NRP1 in guided tip cell migration [19]. Guidance receptors expressed in the tip cell include Unc5B, which triggers tip cell filopodia repulsion on activation by netrin-1 [20]. Netrin-4 can also bind neogenin, which in turn recruits and activates Unc5B to mediate repulsion [19]. Roundabout 4 (Robo4) induces vessel repulsion after their activation by Slit [21]. It also counteracts the attractive signal of VEGF by impeding VEGFR2 activation and interacts with Unc5B to maintain vessel integrity by modulating VEGF signaling [22].
Lumen formation
During sprouting angiogenesis, new vessel branches need to generate a lumen to initiate blood flow (Figure 1c). ECs can use pinocytosis to internalize multiple vesicles of the plasma membrane that coalesce together to create an intracellular lumen. Contacts between ECs, extracellular matrix and adjacent cells facilitate the fusion of vacuoles and depend on signaling of integrins, particularly integrin α2β1 in collagen matrices, and integrins αvβ3 and α5β1 in fibrin matrices [23,24,25]. A recent study in the mouse dorsal aorta suggests that ECs modify their shape and junctions with their neighbor to create a lumen [26]. In this model, ECs negatively charge the glycoproteins specifically localized on the apical surface where the lumen will be generated. This specific polarity confers a repulsive signal to open up the lumen, supported by the redistribution of cell–cell adhesion to the periphery [26].
Maturation of newly formed blood vessels
New vessels must undergo maturation to become functional and stable (Fig. 1d). This implies the combined action of signaling pathways for the recruitment of mural cells such as pericytes and the consolidation of cell–cell adhesion. Basement membrane deposition is driven by tissue inhibitors of metalloproteinases (TIMPs) which counteract matrix metalloproteinases (MMPs) activity.
Pericyte recruitment
PDGF-B is a factor secreted by tip cells which plays a critical role in pericyte recruitment. PDGF-B is retained in close proximity to growing endothelial vessels by heparan sulfate proteoglycans, where it serves as an attractant for comigrating pericytes expressing the receptor-β (PDGFRβ) [27]. Angiopoietins (Ang) have also been shown to be required for vessel stabilization by perivascular cells. Ang1 is predominantly released by perivascular and mural cells and activates the Tie2 receptor present on ECs. Ang1-induced Tie2 phosphorylation leads to AKT activation, which promotes survival pathways in ECs, suppresses apoptotic pathways and deactivates the forkhead transcription factor (FOXO1) [28, 29]. Finally, the interaction between perivascular cells and ECs is stabilized through sphingosine-1-phosphate (S1P). S1P binds to G protein-coupled S1PRs (S1PR1-5) and mediates N-cadherin trafficking in order to strengthen adhesion between ECs and pericytes [30].
Strengthening of cell junctions
VE-cadherin is a transmembrane-adhesive protein which stabilizes EC–EC adhesion, thereby solidifying barrier properties and decreasing permeability and vascular leakage. The intracellular domain of VE-cadherin is attached to the cytoskeleton through beta-catenin, whereas the extracellular domain binds to another VE-cadherin molecule on neighboring ECs. Moreover, VE-cadherin dephosphorylates VEGFR2 through the recruitment of phosphatases and thereby contributes to the maintenance of blood vessel quiescence [31]. Multiple additional tight junction proteins, such as claudin-5, occludin and PECAM-1, also participate in the maintenance of cell–cell contacts by regulating the passage of solutes and ions and transducing intracellular signals [31, 32]. Tight junction proteins have intracellular partners, such as the well-characterized members of the ZO family, which are involved in signal transduction at cell–cell junctions [33].
Tumor vasculature
Features of tumor blood vessels
Compared to tissue blood vessels, the tumor vasculature demonstrates atypical morphological features. The tumor vascular network is characterized by dilated, tortuous and disorganized blood vessels. Vascular immaturity and lack of mural cells association lead to excessive permeability, poor perfusion and increased hypoxia. Moreover, tumors present a high degree of vascular heterogeneity, with hypervascular sites and other regions of low vessel density (Fig. 2a).
Characteristics and consequences of immature tumor blood vessels. a The vascular immaturity and lack of mural cells association lead to inadequate permeability, whereas the uncontrolled proliferation of cancer cells drives poor perfusion and increases hypoxia. b Vessel collapse, permeability and hypoperfused hypoxic areas lead to the exclusion of large tumor areas from exposure to administrated drugs and decrease efficiency of therapies
Blood vessels permeability
Perivascular cells, which are composed of pericytes and vascular smooth muscle cells, participate in blood flow regulation and contribute to limit vessel permeability. In tumors, the connection between perivascular cells with the basement membrane and ECs is impaired. The density of tumor-associated pericyte is not only low on vessels compared to normal tissue, but pericytes also display abnormal morphology [34, 35]. The involvement of PDGF-B in pericyte recruitment was studied in tumors transplanted into mice carrying a mutation in the pdgf-b gene, leading to C-terminal truncation of the PDGF-B retention motif in the endogenous PDGF-B protein (pdgf-b ret/ret) [36]. Immunohistochemical assessment of the tumor vasculature showed reduced pericyte coverage and decreased EC/pericyte association [36]. Increased EC proliferation, combined with defective pericyte coverage and function, contributes to vessel wall instability, leading to tumor hemorrhage. The high secretion level of VEGF by tumor cells can also suppress PDGFRβ signaling in vascular smooth muscle cells through the assembly of a receptor complex consisting of PDGFRβ and VEGFR2 [37].
Barrier integrity is also disrupted following the loss of VE-cadherin function. Tumor cells release proteolytic enzymes as MMPs, elastase or trypsin to promote VE-cadherin cleavage [31]. Tumor cells also secrete inflammatory factors that may affect blood vessel permeability [38]. Histamine stimulation on human umbilical vein cells (HUVECs) demonstrated that inflammatory processes increase EC permeability in association with a durable disruption of VE-cadherin [39]. Finally, VEGF can also increase vascular permeability through the modulation of the activity of several GTPases such as RhoA [40]. Thus, these studies provide evidence for a critical role for VE-cadherin in cancer-associated vascular permeability.
The vascular basement membrane is also a critical component of blood vessel integrity. Despite similar basal membrane coverage between tumor and normal blood vessels, confocal and electron microscopy distinguished structural alterations in RIP-Tag2 mice, MCa-IV breast carcinomas and Lewis lung carcinomas [41]. Layers of type IV collagen, CD31 and α-SMA appeared disjointed, indicative of a loose association of basement membrane, ECs and pericytes. Some broad segments extended away from the endothelium and into the tumor stroma. Finally, the perivascular basement membrane can also present profound structural abnormalities with irregular thickness and some perforations [41, 42]. All these factors can lead to vascular permeability, blood leakage and metastasis by facilitating entry of tumor cells into the bloodstream.
Inadequate perfusion
Uncontrolled cell growth is one of the main characteristic of tumors. The surrounding host tissue restricts tumor expansion and induces mechanical forces, which in turn compress or even collapse intratumoral vessels, suppressing blood flow [43]. In addition, compressive stress inhibits lymphatic network functionality and hinders the drainage of excessive interstitial fluid [43]. Vessel permeability further reduces perfusion by causing blood leakage in upstream vessels [35] and increases fluid flux from the vascular to the interstitial space [43]. Together, leakage of tumor blood vessels and unfunctional lymphatic networks elevate interstitial fluid pressure (IFP), which disorganizes vascular pressure and limits drug delivery [43]. Blood vessel compression by cellular growth limits perfusion, hence decreasing oxygen and nutrient supply, resulting in the formation of a hypoxic microenvironment that favors the selection of clones that can resist these harsh conditions [43]. Hypoxic tumor cells often show a more aggressive phenotype, activating oncogenes and undergoing an “epithelial to mesenchymal transition” (EMT), which heightens their metastatic potential [44]. Moreover, in cancer-associated fibroblasts and independently of hypoxia, mechanical compression downregulates miR-9 expression, which leads to VEGF expression [45]. Interestingly, the remaining uncompressed vessels often display excessive blood flow, which contributes to the increased IFP in tumors [46].
Molecular mechanisms involved in tumor blood vessel formation
Tumors cannot grow beyond 1–2 mm without a vascular supply. Due to an insufficient supply of nutrients and oxygen as well as poor clearance of metabolic waste, hypoxia and/or acidosis appears.
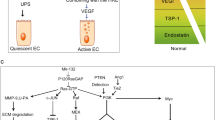
Hypoxia is a major driver of tumor angiogenesis. Under normoxia, prolyl hydroxylase domain protein 2 (PHD2) uses oxygen to hydrolyze hypoxia-inducible factors (HIF) transcription factors, which targets them for ubiquitination by the Von Hippel–Lindau (VHL) complex and leads to their degradation by the proteasome [47, 48]. Under hypoxic conditions, PHD2 becomes inactive, allowing HIF1 to escape degradation and to bind hypoxia response elements (HREs), a DNA sequence motif present in HIF target genes. Increased levels of HIF proteins lead to the transcription of genes involved in cellular adaptation against chronic or acute hypoxia such as angiogenesis, survival, cell proliferation and glucose metabolism [49]. Genes whose expression is regulated by HIF1 include VEGF, TGF-β, PDGF-B, plasminogen activator-1 (PAI-1), erythropoietin (EPO) and GLUT-1 [50]. HIF protein levels can also be increased in cancer cells due to activation of oncogenic pathways. Recently, it was demonstrated that the ERK signaling cascade can result in the increased rate of mRNA translation of HIF1 protein [51]. Furthermore, cAMP-dependant protein kinase A (PKA) which is deregulated in cancer, phosphorylates Thr(63) and Ser(692) on HIF1, enhancing HIF transcriptional activity and decreasing its degradation by the proteasome [52].
The angiogenic process and VEGF production may also be promoted by mutations, leading to increased expression of activated oncogenes or loss of tumor suppressor genes. VEGF can be upregulated by K-ras and H-ras, which will also downregulate Ang1 [53]. Other oncogenes, such as v-src, HER-2 and EGFR, have also been reported to increase VEGF levels [54]. Furthermore, PI3K/Akt signaling was demonstrated to be involved in VEGF expression, as it was shown that inhibition of PI3K signaling leads to decreased VEGF and MMPs expression, resulting in delayed tumor growth [55]. In melanocytes, the introduction of constitutively active MAPK leads to tumorigenesis, activation of the angiogenic switch and increased production of VEGF and MMPs [56]. The numerous oncogenes deregulations highlight the complexity of pathways involved in the regulation of tumor angiogenesis. Finally, in addition to molecular deregulations, conventional anticancer therapies may also aggravate vascular malformations of the tumor vascular network. For example, low-dose ionizing radiations drive the phosphorylation of several signaling proteins such as VEGFR2 and enhance EC migration [57].
Alternative neovascularization processes in tumors
Intussusceptive angiogenesis
Even though sprouting angiogenesis is the principal mean of new vessel formation, tumors exploit alternative mechanisms to acquire a vascular network (Fig. 3) [58]. Intussusceptive angiogenesis presents significant benefits over angiogenic sprouting. New vessels are generated faster and require fewer metabolic needs, as they do not depend on EC proliferation, membrane degradation and tissue invasion. Tumors use this strategy for rapid adaptations to a changing environment [59]. The intussusceptive process, also known as splitting angiogenesis, is characterized by the insertion of interstitial tissue pillars into the lumen of preexisting vessels that split them into two new functional vessels. The mechanisms of pillar formation [60] describe a four-step model in which (1) ECs form bridges inside the lumen and adhere to each other using collagen bundles, (2) proteolytic activity locally disrupts the basement membrane and the collagen bundle migrates into the lumen through the bridges of ECs, (3) the collagen bundle reaches the other side and connects the tissue, forming a nascent pillar, and (4) the new pillar becomes more mature and enlarges through the recruitment of fibroblasts, myofibroblasts and pericytes and the extracellular matrix deposition secreted by these cells. A large variety of tumors use intussusception to grow including human melanoma [61] or colon carcinoma [60].
Alternative means of tumor neovascularization. Sprouting angiogenesis: the growth of new capillary vessels is achieved through the sprouting of neovessels from existing ones. Intussusceptive angiogenesis: intussusceptive angiogenesis is driven by the insertion of interstitial tissue pillars into the lumen of preexisting vessels that split them in two new functional vessels. Vasculogenic mimicry and mosaic vessels: tumor cells can form vascular channel structures connected with normal blood vessels or can be part of the vessel wall, forming mosaic vessels. Vascular co-option: tumors grow by hijacking preexisting vessels in the peritumoral tissues. Endothelial precursors: circulating endothelial precursor cells are recruited by tumor vessels, integrate in the vessel wall and differentiate into ECs. Cancer stem cells can also play a similar role and integrate into the tumor vasculature
Vasculogenic mimicry
The term “vasculogenic mimicry” (VM) refers to tumor cells which behave as ECs. In 1999, this phenomenon was described for the first time by reporting patterned vessel-like channel structures in human melanomas in which red blood cells were detected [62]. Since then, VM has been reported in numerous malignant tumors types including carcinomas of the breast, ovaries, prostate, bladder and lungs, and in sarcomas and gliomas [63]. VM is characterized by tumor cells co-expressing endothelial and tumor markers and forming perfused channel structures. Indeed, in the context of VM, tumor cells express vascular markers such as VE-cadherin, which plays an important role in mimicry tube formation to maintain channel integrity by establishing cell–cell connection [63]. Moreover, tumor cells can be integrated in the walls of tumor-associated blood vessels, forming so-called mosaic vessels [64]. A physiological perfusion of blood in endothelial-lined mouse vessels interconnected with VM networks in human tumor xenografts was demonstrated using Doppler imaging [65]. The tumor cells lining the inner surface of the channels are directly exposed to blood flow. Thus, this can lead to the detachment of tumor cells lining these channel structures into the bloodstream. A recent clinical meta-analysis demonstrates that patients with VM in their tumor have poor clinical outcomes [66].
Vessel co-option
In well-vascularized tissues, cancer cells can grow without induction of newly formed vessel by hijacking the preexisting vessels in the surrounding normal tissues. In clear cell renal cell carcinoma, mature and well-differentiated vessels, commonly present in healthy tissues, are observed in the tumor margin, suggesting that blood vessels were recruited by the tumor for its benefit [67]. Cancer cells grow along existing vessels and integrate them during tumor expansion. Moreover, the adjacent tissue often exhibits an abnormal high density of large vessels which could be partly due to the increasing blood supply demands of the growing tumor. This process has been referred as “extratumoral angiogenesis” [67].
Endothelial precursors
Multiple studies have been published in the last fifteen years describing the involvement of endothelial precursor cells (EPC) in tumor angiogenesis [68, 69]. According to this model, EPCs from the bone marrow can differentiate in situ and incorporate into growing vessels. EPCs can contribute to rapid neovascularization and provide a significant reservoir of cells that participate to the angiogenic process [70]. MMTV-PyMT transgenic mice, which develop mammary tumors that metastasize to the lung, were used to demonstrate EPC contribution to the dynamics of vessel assembly that turns micrometastases into lethal macrometastases [71]. Recent clinical investigation of the vasculature of human tumors suggests that 2–12% of ECs infiltrating the tumors were derived from the bone marrow [72]. However, their involvement and direct role as precursor cells remains a controversial topic [73]. Other studies have demonstrated that even though adult angioblasts can differentiate into EPC, their incorporation in the tumor vasculature is a rare or negligible event [74, 75]. Moreover, stimulation by VEGF does not seem to enhance this process [76]. Similar results were observed in other studies focusing on gliomas [77, 78]. Another source of progenitor cells can come from the tumor itself through cancer stem cells (CSCs). CSCs are cells that possess the capacity to self-renew and that produce all the cells that compound a heterogeneous tumor. Thereby, CSCs with their high degree of plasticity can express endothelial markers and participate in vasculogenic mimicry. In glioblastomas, a study showed that stem-like cells are able to form tumor vascular networks through endothelial differentiation [79]. Furthermore, other studies have reported that CSC can also differentiate into vascular smooth muscle cells and incorporate into vessels [80].
Consequences of immature tumor vessels
Immature blood vessels have a direct impact on tumor cells, but also impair anticancer treatment efficacy (Fig. 2b). Radiotherapy exposes cancer cells to ionizing radiation of high energy, leading to the generation of reactive oxygen species (ROS) in an aerobic microenvironment, which in turn induces lethal DNA damage leading to tumor cell death [81]. Radiation sensitivity of cancer cells is correlated with oxygen levels, and treatment efficacy is lowered in hypoxic conditions [82]. Chemotherapy will also be affected by tumor vessel immaturity, as vessel collapse, interruption of blood flow and hypoperfused hypoxic areas lead to the exclusion of large tumor areas from exposure to systemically administrated drugs. Chemotherapeutic drugs may not be able to reach some portions of the tumor in sufficient quantities, and their effectiveness is significantly reduced [43]. Furthermore, hypoxic cells tend to be quiescent, making chemotherapy drugs that target proliferating cells ineffective [83]. Several drugs routinely used for cancer treatment, such as doxorubicin or methotrexate, require oxygen for their tumor cell-killing activities [84,85,86]. As such, the activity of these agents will be significantly reduced in poorly perfused, hypoxic areas of tumors. Finally, in the tumor periphery, upstream vessel permeability and elevated interstitial fluid pressure can influence the delivery of therapeutics [46]. The blood fluid containing drugs leaks in the tumor periphery and does not reach the center of the tumor, which inhibits homogeneous distribution inside the tumor. This oozing fluid is involved in the transport of growth factors, fueling tumor progression, and reduces the retention time of small drugs [46].
One type of treatments that is particularly impaired by poor tumor perfusion is internal radiotherapy, which is a strategy used to target and specifically irradiate tumor cells through a specifically labeled vector [87] or antibody [88]. Injected intravenously, these agents require both a good distribution into the tumor and a supply of oxygen to mediate their activities. Their efficiency is dramatically decreased due to inappropriate perfusion of the tumor vasculature network resulting from (i) poor distribution of the agent and (ii) lack of oxygen required to potentiate the effects of ionizing radiation.
Immunotherapies, in which cells of the host immune system are primed to target and kill tumor cells, also show decreased therapeutic efficiency as a consequence of poor vessel perfusion [89]. Nonfunctional tumor blood vessels prevent immune cells from reaching the tumor. Although all immune cell types can infiltrate into the tumor parenchyma through functional tumor vessels, it has been shown that suppressive immune cell populations preferentially accumulate in tumors. This may be a consequence of the fact that tissue-resident macrophages are known to migrate to hypoxic and necrotic tumor areas where they switch to a tumor-associated macrophage (TAM) phenotype. Furthermore, regulatory T cells (Treg), which are immune-suppressive lymphoid cells, are also preferentially recruited into tumors via the expression of chemotactic factors, such as CCL-22 and CCL-28 in hypoxic areas of the tumor [90]. Finally, hypoxia and immunosuppressive factors in the tumor microenvironment can cause TAMs to switch to an immune-suppressive phenotype, impeding the recruitment and activation of effector lymphocytes [91, 92]. Thus, impaired tumor vessel functionality contributes to create an abnormal tumor microenvironment that leads to the preferential accumulation of immune suppressor cells and impairs immune cell functions in tumors, which constitute a major hurdle to successful immunotherapy treatments.
VEGF inhibitors and vascular normalization
VEGF signaling inhibitors
Since VEGF was discovered to be a critical regulator of blood vessel growth in the 1980s [93, 94], it has been suggested that this factor could be an important target to control tumor neovascularization. Bevacizumab is a humanized anti-VEGF-A monoclonal antibody approved by the US Food and Drug Administration (FDA) [95]. Additive or synergistic effects of bevacizumab with conventional chemotherapies or radiotherapies have been evaluated in a variety of tumor models and lines of therapies. In patients bearing gastric cancer, the combination of bevacizumab with chemotherapy has significantly improved the progression-free survival and overall response [96]. Similar results were observed in non-small cell lung cancer with the combination cisplatin/gemcitabine and bevacizumab [97] or in women bearing metastatic breast cancer with bevacizumab combined with paclitaxel [98]. In parallel to bevacizumab, inhibitors targeting VEGFRs, such as sunitinib or sorafenib, have been developed and are approved by the FDA for the treatment of metastatic renal cell carcinoma [99]. The successes and failures of VEGF blockade are thought to be highly dependent on tumor type [100]. Prostate and pancreatic cancers have been shown to be refractory to angiogenesis modulators, whereas some tumors such as renal cell carcinoma are more sensitive to VEGF inhibitors, in which anti-angiogenic drugs are often the first-line treatments to prevent metastatic spread [100]. Furthermore, recent studies show that chronic exposure of tumor cells to VEGF inhibitors increased expression of VEGF-A, VEGF-B, VEGF-C, PlGF, VEGFR-1 and VEGFR-1 phosphorylation, increased tumor cell migration and invasion, and metastatic potential in vivo [101]. Although anti-VEGF therapies were generally well tolerated, some serious toxicities exist. Venous thromboembolic complications as hypertension were among the most frequent adverse effects [102].
Vascular normalization theory
The concept of vascular normalization suggests that the improvements of chemotherapy and radiotherapy treatments in combination with VEGF signaling inhibitors are likely due to a maturation effect on blood vessels [3]. Tumor cells secrete abundant VEGF, which leads to the formation of immature vessels characterized by inadequate pericyte coverage [37]. Careful dosage of VEGF inhibitors can restore levels of angiogenic signals in tumors, leading to decreased permeability by tightening cell–cell junctions and by actively recruiting pericytes, resulting in increased tumor perfusion [103]. Indeed, VEGFR2 blockade leads to the recruitment of pericytes to blood vessels in part by activating Ang-1/Tie2 signaling [104]. Furthermore, inhibition of VEGF has been shown to increase PDGFRβ signaling and promote pericyte recruitment and maturation [37].
Another challenge in the use of VEGF inhibitors to obtain vascular normalization is achieving what has been referred to as a “window of opportunity,” which is the time frame and dosage of VEGF inhibitor administration required to observe normalization of tumor blood vessels [5]. The dosage of VEGF inhibitors required to obtain a normalization window is relatively narrow and depends on tumor type, schedule and VEGF signaling inhibitor used. The effect is typically short-lived (7–10 days) but could last from one to four months, depending on the drug used and the tumor type [105]. In the case of excessive neutralization of VEGF activity, seen with high doses or prolonged exposition, vascular normalization can soon be replaced by marked vascular regression leading to increased tumor hypoxia and favor the selection of invasive tumor cells, enhancing the risks of metastatic spread [106, 107]. As prolonged maintenance of vascular normalization would be required to enhance the therapeutic index of chemotherapy, radiotherapy and particularly immunotherapies, it becomes essential to develop strategies leading to efficient and long-term stabilization of tumor blood vessels [108].
Imaging and gene expression studies support the idea that restoration of proper vascular normalization is critical to alleviate hypoxia and increase the benefits of anticancer treatments [109]. Imaging of hypoxia, with specific radiotracer 18F-MISO developed for positron emission tomography (PET) or dynamic contrast-enhanced magnetic resonance imaging (DCE-MRI), is a noninvasive technique that could determine the functionality of tumor blood vessels after anti-angiogenic treatments and could help determine the ideal regimen required to achieve normalization [110, 111]. Moreover, tracers can also be used to monitor vascular normalization following treatments with VEGF inhibitors. A specific radioactive tracer (99 m)Tc-RGD, which binds the integrin αvβ3 expressed during active angiogenesis, has been shown to be helpful in monitoring vessel normalization after bevacizumab treatment and could help determine the ideal regimen required to improve radiotherapy efficiency [112].
Alternative targets for vascular normalization
In spite of the encouraging results of anti-VEGF therapies, some serious side effects can appear. First, risks of hemorrhage or venous thromboembolism are increased with conventional anti-angiogenic treatments [113, 114]. Secondly, severe vascular regression is associated with increased incidence of tumor metastasis [106]. Finally, the benefits of anti-VEGF are transitory and are followed by a resumption of tumor growth due to adaptive resistance or preexisting non-responsiveness [115]. For all these reasons, alternative targets to normalize tumor blood vessels would present great therapeutic benefits. Enhanced blood vessels maturation through improved pericyte coverage and restoration of cell junctions leading to increased tumor perfusion would limit tumor hypoxia and prevent the selection of tumor cells with a more invasive phenotype and improve the distribution and efficiency of anticancer treatments (Fig. 4).
Pericyte recruitment
Pericytes are an integral component of mature blood vessels, where they contribute to vascular quiescence and integrity [116], and tumor blood vessels frequently lack adequate pericyte coverage [117]. Increasing pericyte coverage has been proposed as a therapeutic option to achieve vascular normalization. Several signaling pathways could be exploited to modulate pericyte coverage.
Angiopoietins
The angiopoietins and their receptor Tie2 (TEK) play a critical role in the formation and remodeling of blood vessels. Angiopoietin signaling has been shown to be involved in the control of microvascular permeability, vasodilation and vasoconstriction. Four angiopoietins have been identified so far: Ang1, Ang2, Ang3 and Ang4. Angiopoietins act by binding to Tie2, a tyrosine kinase receptor typically expressed on vascular endothelial cells and specific macrophage subsets [118], leading to receptor auto-phosphorylation and the activation of several intracellular signaling pathways leading to endothelial cell migration [119, 120], tube formation [121, 122], sprouting [120] and survival [123]. Ang1, which is produced by perivascular cells, promotes vessel maturation, while Ang2, which is produced by ECs and has been reported to possess antagonistic activity for the Tie2 receptor, is involved in the destabilization of EC/pericyte association [28]. However, other studies have also shown that Ang2 binding to Tie2 at high concentration can result in receptor activation with similar biological outcomes to Ang1 [122, 124]. Therefore, Ang2 may act as a context-dependent antagonist. Ang2 activity also appears to be dependent on VEGF levels; Ang2 will lead to pericyte detachment and vascular regression in the presence of low levels of VEGF, while it will enhance EC migration and angiogenesis in the presence of high levels of VEGF by weakening EC/pericyte interactions [125]. In the context of tumor angiogenesis, Ang2 inhibition has shown potential therapeutic benefits. The role of Ang2 on tumor angiogenesis has been demonstrated by grafting melanoma or Lewis lung carcinoma cancer cells into Ang2 knockout mice. In these models, absence of Ang2 led to decreased microvessel diameters and a more mature perivascular profile [126]. Several inhibitors targeting the angiopoietin/Tie signaling pathways have been developed and are being investigated in preclinical and clinical studies. The Ang2-blocking antibody MEDI3617 results in tumor angiogenesis reduction and an improvement of chemotherapy [127] as well as decreased lung metastasis and lymphangiogenesis in several preclinical models including colorectal, renal, hepatocellular, lung or ovarian carcinoma. Ang2 inhibition, using an antibody that promotes the internalization of Ang2-Tie2 receptor complexes without affecting Ang1-Tie2, was shown to reduce vascular leakage by enhancing the integrity of cell–cell junctions [128]. High Ang2 level compromised the benefit of VEGF signaling inhibition by altering vessel normalization [129]. Recent studies demonstrated that combined inhibition of VEGFR and Ang2 significantly improves survival in murine glioblastoma models by increasing normalization and reprogramming macrophages [129, 130]. AMG-386 (trebananib) is a peptide-Fc fusion protein (peptibody) that inhibits angiogenesis by interfering with the binding of Ang1 and Ang2 to the Tie2 receptor. In preclinical studies, trebananib exhibited anti-tumor activity against human epidermoid and colorectal tumor mice xenografts [131]. Trebananib combination with chemotherapy agents in adults with various solid tumors showed promising anti-tumor activity [132]. In a phase 3 study, trebananib has been tested on patients bearing recurrent epithelial ovarian cancer and significantly improved progression-free survival [133].
Tie2 is dephosphorylated and consequently inactivated by a specific EC-phosphatase: the vascular endothelial protein tyrosine phosphatase (VE-PTP). AKB-9778 is a selective VE-PTP inhibitor which induces Tie2 activation in ECs. AKB-9778 treatment delayed the early phase of breast cancer growth and decreased the size, number and progression of metastasis. In tumor vasculature, Tie2 activation increased pericyte coverage, vessel diameter, vasculature density, tumor perfusion and reduced blood vessel permeability [134]. Similarly, a recent study demonstrated that ABTAA, a specific antibody which simultaneously activates Tie2 and inhibits Ang2, normalized tumor blood vessels, reduced hypoxia and induced immune cell infiltration. ABTAA enhanced the delivery of cisplatin into Lewis lung carcinoma tumors and consequently the overall survival of mice [135].
Similarly, Ang1-upregulation was shown to lead to blood vessel stabilization [136]. Interestingly, dopamine has been shown to have an effect on tumor blood vessels by inducing Ang1 overexpression directly in pericytes and promoting the mobilization and recruitment of these cells [136]. Dopamine injections regulate the morphology and leakiness of tumor blood vessels, as well as decreasing hypoxia and increasing blood flow [136]. Simvastatin treatment, which induces Ang1/Tie2 expression, inhibited transendothelial migration of highly invasive prostate cancer cells, enhanced endothelial cell-barrier integrity via β-catenin stabilization, decreased VEGF expression and increased Ang1 expression [137].
PDGF-B
During angiogenesis, the PDGF-B/PDGFR axis closely mediates pericyte coverage in new blood vessels and several studies have evaluated the potential of this signaling pathway to modulate tumor angiogenesis. ECs, particularly tip cells, secrete high levels of PDGF-B, which exerts its cellular effects by binding to tyrosine kinase receptors (PDGFRα and PDGFRβ) expressed on perivascular cells, promoting pericyte recruitment [138]. A study demonstrated that anti-angiogenic resistance is due to active proliferation of mural cells and high PDGF-B expression [139]. These results initiated the idea that VEGF inhibition may be more efficient in combination with agents blocking PDGFRβ activity. SU6668 is a PDGFRβ kinase inhibitor that disrupts tumor vascularity by promoting pericyte detachment. Its combination with the VEGFR inhibitor SU5416 showed a synergistic effect on tumor size reduction [140, 141]. Moreover, SU5416 and SU6668 combination with radiotherapy enhanced local anti-tumor effects of irradiation [142]. PDGF-B inhibitors also include several antibodies, such as CR002 and IMC-2C5 or CDP860 which is a an engineered Fab’ fragment–polyethylene glycol conjugate that targets PDGFRβ and inhibits its activation [143,144,145]. The DNA aptamer AX102 sensitized tumor cells to chemotherapy by increasing the number of perfused tumor vessels [146, 147]. However, tumor cell death was not increased in primary tumors [148] and a recent study demonstrated that depleting the vessel of pericytes is no more efficient than monotherapy with anti-VEGF alone [149]. Moreover, loss of perivascular coverage induced increased vessel immaturity and enhanced metastases [6, 150]. An alternative strategy to achieve vascular normalization has been to promote PDGF/PDGFRβ signaling. PDGF-B contributes to the IFP regulation and participates in the regulation of vessel leakiness. PDGF-B overexpression in mouse models of colorectal and pancreatic cancer led to tumor growth inhibition by enhancing pericyte recruitment and decreasing EC proliferation [151]. In glioma models, PDGF-B expression increased after Wnt/β-catenin signaling activation, contributing to vascular quiescence and decreased vessel permeability [152]. PDGF-B overexpression also appears to be able to promote tumor growth and lymph node metastasis; however, used in association with chemotherapy, it can enhance drug delivery and hence improve the efficacy of administered therapeutics [153].
BMP signaling
Alk1 (activin receptor-like kinase 1) is a type I receptor expressed on ECs, which binds TGF-β (transforming growth factor-β) family members with a specific affinity for BMP9 (bone morphogenetic protein 9) and BMP10. During development, Alk1 is involved in the maturation and stabilization of the vascular network in part by stimulating pericyte recruitment [154]. BMP9 induces ID1 expression, which increases EC proliferation and migration [155, 156], but also promotes the expression of HEY1 and 2 which are ID1 antagonists and suppress its effects on angiogenesis [157]. BMP9 stimulation inhibits sprouting angiogenesis by cooperating with the notch pathway [158, 159], acts as an anti-angiogenic factor [160] and plays a role in vascular quiescence [161]. Alk1 inhibitors have been recently developed to modulate angiogenesis during tumor growth. Alk1-Fc is a recombinant protein composed of the extracellular domain of Alk1 receptor bound to the Fc part of a human antibody. It binds BMP9 with a high affinity and acts as a ligand trap to inhibit the activation of Alk1 signaling [162]. Alk1-Fc caused a reduction of ID1 expression in ECs, inhibited HUVEC cord formation and decreased angiogenesis in a chicken chorioallantoic membrane assay [163]. Moreover, in MCF7 breast cancer and B16 melanoma, the treatment with Alk1-Fc reduced tumor growth in both models. Dalantercept (Alk1-Fc) monotherapy was tested in a phase II study in patients bearing recurrent endometrial carcinoma [164]. However, no tumor response was observed, suggesting that the activity of Dalantercept is insufficient as a single agent and should be used as an adjuvant to a conventional therapy. Recently, dalantercept was combined with VEGFR tyrosine kinase inhibitors (sunitinib) in human RCC xenograft models [165]. This therapy association prevents tumor relapse and the resumption of tumor blood flow seen usually with monotherapy by sunitinib. The treatment combination leads to a downregulation of Notch signaling which affects Hey1/2 genes expression. Alk1 blocking antibodies have also been used for cancer treatment. PF-03446962 specifically binds Alk1 and neutralizes BMP9-induced signaling in HUVECs [166]. Smad1 phosphorylation and sprouting of ECs were inhibited without affecting VEGF signaling. Nonetheless, in phase 2 trial with patient bearing urothelial cancer, PF-03446962 showed no anti-tumor activity [167]. Interestingly, in most patients, VEGF levels increased after 2 months of treatment. In this study, the authors concluded that PF-03446962 will be not used without the association of anti-VEGF therapies. Given its role in vascular maturation and remodeling, agonists of Alk1 signaling may also be of future therapeutic interest to promote vascular normalization in cancer.
Junction enhancement
ECs are strongly connected through adherent junctions, of which VE-cadherin is a major component. VE-cadherin inhibition by specific antibodies increases vascular permeability and demonstrates their key role to control vascular barrier function [168].
Sac-1004 is a recent molecule developed to restore proper interstitial fluid pressure, prevent vascular leakage and improve perfusion. This compound strengthens the endothelial barrier through the cAMP/Rac/Cortactin pathway to form a cortical actin ring, which upregulates adherens junction such as VE-cadherin [169]. In a preclinical study using lung carcinoma or melanoma models, Sac-1004 reduced vascular leakage by increasing junctional integrity and perfusion in the tumor vasculature. Lung and node metastasis were decreased, as were H1F-1α tumor levels. Used in combination with cisplatin, chemotherapy efficiency was improved after vascular normalization by Sac-1004 [170]. Treatment of B16F0 melanoma tumors with Sac-1004 and sunitinib, an anti-angiogenic agent, significantly decreased tumor growth and increased tumor-bearing mice survival [171].
HIF-2α has a similar structure to HIF-1α but is only expressed in specific cells such as ECs and fibroblasts [172]. Mice with HIF-2α-deficient ECs developed high vessel permeability with aberrant EC structure. Tumor growth in such animals exhibited defective angiogenesis and increased hypoxic stress [173]. A study also indicates that HIF-2α is involved in VE-cadherin promoter activation in tumor cells independently of hypoxia [174]. Therefore, targeting HIF-2α could also strengthen cell–cell junctions [174].
Modulation of perfusion and hypoxia responses
Several studies have shown that radiation treatments or chemotherapeutic drugs can affect the tumor vasculature and may improve vascular perfusion. Recently, it has been demonstrated that fractionated radiation therapy substantially enhanced tumor perfusion after two weeks of treatment. It was associated with better tissue viability and decreased hypoxia, but with increased VEGF expression that was counteracted by sunitinib treatment [175]. Imatinib mesylate is a clinical drug approved for the treatment of gastrointestinal stromal tumors that can modify the tumor microenvironment such as tumor vessel density, normalization and perfusion [176]. Delivery of nanomedicines relies on the size of particles and blood vessels diameter, and after imatinib mesylate treatment, micelles around 23 nm had a significantly more effective penetration and homogeneous distribution in tumor tissues [176]. Chloroquine (CQ) is traditionally used as an autophagy blocker in anticancer treatment, but it can also affect tumor blood vessels [177]. CQ modifies the tumor microenvironment by improving perfusion and oxygenation, reducing hypoxia area, cancer cell dissemination and intravasation. CQ normalized vessels in part by increasing Notch1 signaling in ECs with nuclear accumulation and transcriptional activity of NICD [177].
Hypoxia leads to increased levels of PHD family activity, which in turn produces upregulation of HIF1-α and VEGF production. In preclinical studies, the direct injection of antisense HIF1-α vectors enhanced doxorubicin efficiency by suppressing hepatocellular carcinoma (HCC) angiogenesis [178]. Furthermore, the inactivation of HIF1-α by RNAi or Cre/loxP-mediated recombination modulated the chemosensitivity of carcinoma cells [179]. The combined knockdown of HIF-1α and IL-8 inhibits angiogenesis, tumor growth and increased survival rates of mice bearing HCC [180, 181]. Tumors implanted in Phd2 +/− heterozygous mice, expressing PHD2 at half normal levels, were more mature with tight EC junctions, reduced hypoxia and less leaky compared to tumors grafted in wild-type mice. These results suggest that PDH2 activation (and hence decreased hypoxia) drives tumor blood vessel normalization and immunostaining conjugated to RT-PCR confirmed that VE-cadherin was upregulated in tumors ECs in Phd2 +/− mice [48]. Interestingly, after VEGF stimulation in Phd2 +/− model, ECs showed reduced proliferation and displayed decreased motility and formation of lamellipodia compared to ECs in the wild-type model [48].
Conclusion and perspectives
Taken together, these observations highlight the complexity of pathways involved in tumor angiogenesis. Although initial preclinical studies showed that VEGF inhibition is able to prune tumor vessels and leads to tumor shrinkage, the results of bevacizumab monotherapy in patients with solid tumors were overwhelmingly disappointing. Furthermore, the increased incidence of metastasis in some patients led to the concept that vascular normalization, combined with chemotherapy or radiotherapy, might be a more efficient way to treat cancer patients. Indeed, anti-VEGF treatments have been able to improve the efficacy of systemic chemotherapy, suggesting that they augment the therapeutic index of chemotherapy. In addition, numerous pathways other than VEGF involved in vascular formation and maturation are currently being investigated. By modulating vascular responses in the tumor microenvironment, these therapies could restore a more normal tumor vasculature, capable of delivering cytotoxic drugs more efficiently into tumors and enhancing the effects of radiotherapy. Given the great heterogeneity in tumor vessels in tumor tissues, further studies of the mechanisms underlying the normalization process will be required before they can be effectively exploited in the clinic. In parallel with the development of strategies targeting different pathways of angiogenesis, future research directions would involve the identification of predictive biomarkers to identify patient group responders of non-responders. Personalized anti-angiogenic therapies could be offered to patients based on their potential response. Future challenges will involve the determination of the optimal duration and scheduling of vascular normalization agents, including how to develop effective therapies for metastatic, adjuvant and neoadjuvant cases and how to effectively combine different agents without significant developing toxicity. Close collaborations between basic researchers and clinicians in multiple disciplines will be of utmost importance to achieve this.
References
Carmeliet P, Jain RK (2011) Principles and mechanisms of vessel normalization for cancer and other angiogenic diseases. Nat Rev Drug Discov 10:417–427. doi:10.1038/nrd3455
Carmeliet P, Jain RK (2011) Molecular mechanisms and clinical applications of angiogenesis. Nature 473:298–307. doi:10.1038/nature10144
Jain RK (2001) Normalizing tumor vasculature with anti-angiogenic therapy: a new paradigm for combination therapy. Nat Med 7:987–989. doi:10.1038/nm0901-987
Jain RK (2005) Normalization of tumor vasculature: an emerging concept in antiangiogenic therapy. Science 307:58–62. doi:10.1126/science.1104819
Jain RK (2014) Antiangiogenesis strategies revisited: from starving tumors to alleviating hypoxia. Cancer Cell 26:605–622. doi:10.1016/j.ccell.2014.10.006
Goel S, Duda DG, Xu L et al (2011) Normalization of the vasculature for treatment of cancer and other diseases. Physiol Rev 91:1071–1121. doi:10.1152/physrev.00038.2010
Gerhardt H, Golding M, Fruttiger M et al (2003) VEGF guides angiogenic sprouting utilizing endothelial tip cell filopodia. J Cell Biol 161:1163–1177. doi:10.1083/jcb.200302047
Phng L-K, Gerhardt H (2009) Angiogenesis: a team effort coordinated by notch. Dev Cell 16:196–208. doi:10.1016/j.devcel.2009.01.015
Bray SJ (2016) Notch signalling in context. Nat Rev Mol Cell Biol. doi:10.1038/nrm.2016.94
Blanco R, Gerhardt H (2013) VEGF and Notch in Tip and Stalk Cell Selection. Cold Spring Harb Perspect Med. doi:10.1101/cshperspect.a006569
Jakobsson L, Franco CA, Bentley K et al (2010) Endothelial cells dynamically compete for the tip cell position during angiogenic sprouting. Nat Cell Biol 12:943–953. doi:10.1038/ncb2103
Ferrara N, Gerber H-P, LeCouter J (2003) The biology of VEGF and its receptors. Nat Med 9:669–676. doi:10.1038/nm0603-669
Benedito R, Roca C, Sörensen I et al (2009) The notch ligands Dll4 and Jagged1 have opposing effects on angiogenesis. Cell 137:1124–1135. doi:10.1016/j.cell.2009.03.025
Mattila PK, Lappalainen P (2008) Filopodia: molecular architecture and cellular functions. Nat Rev Mol Cell Biol 9:446–454. doi:10.1038/nrm2406
De Smet F, Segura I, De Bock K et al (2009) Mechanisms of vessel branching: filopodia on endothelial tip cells lead the way. Arterioscler Thromb Vasc Biol 29:639–649. doi:10.1161/ATVBAHA.109.185165
Lamalice L, Boeuf FL, Huot J (2007) Endothelial cell migration during angiogenesis. Circ Res 100:782–794. doi:10.1161/01.RES.0000259593.07661.1e
Ridley AJ (2015) Rho GTPase signalling in cell migration. Curr Opin Cell Biol 36:103–112. doi:10.1016/j.ceb.2015.08.005
Phng L-K, Stanchi F, Gerhardt H (2013) Filopodia are dispensable for endothelial tip cell guidance. Development 140:4031–4040. doi:10.1242/dev.097352
Larrivée B, Freitas C, Suchting S et al (2009) Guidance of vascular development: lessons from the nervous system. Circ Res 104:428–441. doi:10.1161/CIRCRESAHA.108.188144
Larrivée B, Freitas C, Trombe M et al (2007) Activation of the UNC5B receptor by Netrin-1 inhibits sprouting angiogenesis. Genes Dev 21:2433–2447. doi:10.1101/gad.437807
London NR, Smith MCP, Li DY (2009) Emerging mechanisms of vascular stabilization. J Thromb Haemost JTH 7(Suppl 1):57–60. doi:10.1111/j.1538-7836.2009.03421.x
Koch AW, Mathivet T, Larrivée B et al (2011) Robo4 maintains vessel integrity and inhibits angiogenesis by interacting with UNC5B. Dev Cell 20:33–46. doi:10.1016/j.devcel.2010.12.001
Davis GE, Bayless KJ (2003) An integrin and Rho GTPase-dependent pinocytic vacuole mechanism controls capillary lumen formation in collagen and fibrin matrices. Microcirc NY N 10:27–44. doi:10.1038/sj.mn.7800175
Davis GE, Koh W, Stratman AN (2007) Mechanisms controlling human endothelial lumen formation and tube assembly in three-dimensional extracellular matrices. Birth Defects Res Part C Embryo Today Rev 81:270–285. doi:10.1002/bdrc.20107
Sacharidou A, Stratman AN, Davis GE (2012) Molecular mechanisms controlling vascular lumen formation in three-dimensional extracellular matrices. Cells Tissues Organs 195:122–143. doi:10.1159/000331410
Strilić B, Kucera T, Eglinger J et al (2009) The molecular basis of vascular lumen formation in the developing mouse aorta. Dev Cell 17:505–515. doi:10.1016/j.devcel.2009.08.011
Andrae J, Gallini R, Betsholtz C (2008) Role of platelet-derived growth factors in physiology and medicine. Genes Dev 22:1276–1312. doi:10.1101/gad.1653708
Augustin HG, Koh GY, Thurston G, Alitalo K (2009) Control of vascular morphogenesis and homeostasis through the angiopoietin-Tie system. Nat Rev Mol Cell Biol 10:165–177. doi:10.1038/nrm2639
Huang H, Bhat A, Woodnutt G, Lappe R (2010) Targeting the ANGPT-TIE2 pathway in malignancy. Nat Rev Cancer 10:575–585. doi:10.1038/nrc2894
Lucke S, Levkau B (2010) Endothelial functions of sphingosine-1-phosphate. Cell Physiol Biochem Int J Exp Cell Physiol Biochem Pharmacol 26:87–96. doi:10.1159/000315109
Dejana E, Tournier-Lasserve E, Weinstein BM (2009) The control of vascular integrity by endothelial cell junctions: molecular basis and pathological implications. Dev Cell 16:209–221. doi:10.1016/j.devcel.2009.01.004
Privratsky JR, Newman PJ (2014) PECAM-1: regulator of endothelial junctional integrity. Cell Tissue Res 355:607–619. doi:10.1007/s00441-013-1779-3
Wallez Y, Huber P (2008) Endothelial adherens and tight junctions in vascular homeostasis, inflammation and angiogenesis. Biochim Biophys Acta BBA: Biomembr 1778:794–809. doi:10.1016/j.bbamem.2007.09.003
Bergers G, Song S (2005) The role of pericytes in blood-vessel formation and maintenance. Neuro-Oncol 7:452–464. doi:10.1215/S1152851705000232
Morikawa S, Baluk P, Kaidoh T et al (2002) Abnormalities in pericytes on blood vessels and endothelial sprouts in tumors. Am J Pathol 160:985–1000. doi:10.1016/S0002-9440(10)64920-6
Abramsson A, Lindblom P, Betsholtz C (2003) Endothelial and nonendothelial sources of PDGF-B regulate pericyte recruitment and influence vascular pattern formation in tumors. J Clin Invest 112:1142–1151. doi:10.1172/JCI200318549
Greenberg JI, Shields DJ, Barillas SG et al (2008) A role for VEGF as a negative regulator of pericyte function and vessel maturation. Nature 456:809–813. doi:10.1038/nature07424
Ribatti D, Crivellato E (2012) Mast cells, angiogenesis, and tumour growth. Biochim Biophys Acta 1822:2–8. doi:10.1016/j.bbadis.2010.11.010
Guo M, Breslin JW, Wu MH et al (2008) VE-cadherin and beta-catenin binding dynamics during histamine-induced endothelial hyperpermeability. Am J Physiol Cell Physiol 294:C977–C984. doi:10.1152/ajpcell.90607.2007
Beckers CML, van Hinsbergh VWM, van Nieuw Amerongen GP (2010) Driving Rho GTPase activity in endothelial cells regulates barrier integrity. Thromb Haemost 103:40–55. doi:10.1160/TH09-06-0403
Baluk P, Morikawa S, Haskell A et al (2003) Abnormalities of basement membrane on blood vessels and endothelial sprouts in tumors. Am J Pathol 163:1801–1815. doi:10.1016/S0002-9440(10)63540-7
Inai T, Mancuso M, Hashizume H et al (2004) Inhibition of vascular endothelial growth factor (VEGF) signaling in cancer causes loss of endothelial fenestrations, regression of tumor vessels, and appearance of basement membrane ghosts. Am J Pathol 165:35–52. doi:10.1016/S0002-9440(10)63273-7
Jain RK, Martin JD, Stylianopoulos T (2014) The role of mechanical forces in tumor growth and therapy. Annu Rev Biomed Eng 16:321–346. doi:10.1146/annurev-bioeng-071813-105259
Reymond N, d’Água BB, Ridley AJ (2013) Crossing the endothelial barrier during metastasis. Nat Rev Cancer 13:858–870. doi:10.1038/nrc3628
Kim BG, Gao M-Q, Kang S et al (2017) Mechanical compression induces VEGFA overexpression in breast cancer via DNMT3A-dependent miR-9 downregulation. Cell Death Dis 8:e2646. doi:10.1038/cddis.2017.73
Heldin C-H, Rubin K, Pietras K, Östman A (2004) High interstitial fluid pressure—an obstacle in cancer therapy. Nat Rev Cancer 4:806–813. doi:10.1038/nrc1456
Giaccia AJ, Simon MC, Johnson R (2004) The biology of hypoxia: the role of oxygen sensing in development, normal function, and disease. Genes Dev 18:2183–2194. doi:10.1101/gad.1243304
Mazzone M, Dettori D, Leite de Oliveira R et al (2009) Heterozygous deficiency of PHD2 restores tumor oxygenation and inhibits metastasis via endothelial normalization. Cell 136:839–851. doi:10.1016/j.cell.2009.01.020
Marín-Hernández A, Gallardo-Pérez JC, Ralph SJ et al (2009) HIF-1alpha modulates energy metabolism in cancer cells by inducing over-expression of specific glycolytic isoforms. Mini Rev Med Chem 9:1084–1101
Darby IA, Hewitson TD (2016) Hypoxia in tissue repair and fibrosis. Cell Tissue Res 365:553–562. doi:10.1007/s00441-016-2461-3
Masoud GN, Li W (2015) HIF-1α pathway: role, regulation and intervention for cancer therapy. Acta Pharm Sin B 5:378–389. doi:10.1016/j.apsb.2015.05.007
Bullen JW, Tchernyshyov I, Holewinski RJ et al (2016) Protein kinase A-dependent phosphorylation stimulates the transcriptional activity of hypoxia-inducible factor 1. Sci Signal 9:ra56. doi:10.1126/scisignal.aaf0583
Larcher F, Franco M, Bolontrade M et al (2003) Modulation of the angiogenesis response through Ha-ras control, placenta growth factor, and angiopoietin expression in mouse skin carcinogenesis. Mol Carcinog 37:83–90. doi:10.1002/mc.10126
Rak J, Yu JL (2004) Oncogenes and tumor angiogenesis: the question of vascular “supply” and vascular “demand”. Semin Cancer Biol 14:93–104. doi:10.1016/j.semcancer.2003.09.014
Arbiser JL, Moses MA, Fernandez CA et al (1997) Oncogenic H-ras stimulates tumor angiogenesis by two distinct pathways. Proc Natl Acad Sci USA 94:861–866
Govindarajan B, Bai X, Cohen C et al (2003) Malignant transformation of melanocytes to melanoma by constitutive activation of mitogen-activated protein kinase kinase (MAPKK) signaling. J Biol Chem 278:9790–9795. doi:10.1074/jbc.M212929200
Sofia Vala I, Martins LR, Imaizumi N et al (2010) Low doses of ionizing radiation promote tumor growth and metastasis by enhancing angiogenesis. PLoS ONE 5:e11222. doi:10.1371/journal.pone.0011222
Hillen F, Griffioen AW (2007) Tumour vascularization: sprouting angiogenesis and beyond. Cancer Metastasis Rev 26:489–502. doi:10.1007/s10555-007-9094-7
Ribatti D, Djonov V (2012) Intussusceptive microvascular growth in tumors. Cancer Lett 316:126–131. doi:10.1016/j.canlet.2011.10.040
Paku S, Dezso K, Bugyik E et al (2011) A new mechanism for pillar formation during tumor-induced intussusceptive angiogenesis: inverse sprouting. Am J Pathol 179:1573–1585. doi:10.1016/j.ajpath.2011.05.033
Ribatti D, Nico B, Floris C et al (2005) Microvascular density, vascular endothelial growth factor immunoreactivity in tumor cells, vessel diameter and intussusceptive microvascular growth in primary melanoma. Oncol Rep 14:81–84
Maniotis AJ, Folberg R, Hess A et al (1999) Vascular channel formation by human melanoma cells in vivo and in vitro: vasculogenic mimicry. Am J Pathol 155:739–752. doi:10.1016/S0002-9440(10)65173-5
Paulis YWJ, Soetekouw PMMB, Verheul HMW et al (2010) Signalling pathways in vasculogenic mimicry. Biochim Biophys Acta 1806:18–28. doi:10.1016/j.bbcan.2010.01.001
Chang YS, di Tomaso E, McDonald DM et al (2000) Mosaic blood vessels in tumors: frequency of cancer cells in contact with flowing blood. Proc Natl Acad Sci USA 97:14608–14613. doi:10.1073/pnas.97.26.14608
Ruf W, Seftor EA, Petrovan RJ et al (2003) Differential role of tissue factor pathway inhibitors 1 and 2 in melanoma vasculogenic mimicry. Cancer Res 63:5381–5389
Yang JP, Liao YD, Mai DM et al (2016) Tumor vasculogenic mimicry predicts poor prognosis in cancer patients: a meta-analysis. Angiogenesis 19:191–200. doi:10.1007/s10456-016-9500-2
Qian C-N (2013) Hijacking the vasculature in ccRCC–co-option, remodelling and angiogenesis. Nat Rev Urol 10:300–304. doi:10.1038/nrurol.2013.26
Lyden D, Hattori K, Dias S et al (2001) Impaired recruitment of bone-marrow-derived endothelial and hematopoietic precursor cells blocks tumor angiogenesis and growth. Nat Med 7:1194–1201. doi:10.1038/nm1101-1194
Rafii S, Meeus S, Dias S et al (2002) Contribution of marrow-derived progenitors to vascular and cardiac regeneration. Semin Cell Dev Biol 13:61–67. doi:10.1006/scdb.2001.0285
Patenaude A, Parker J, Karsan A (2010) Involvement of endothelial progenitor cells in tumor vascularization. Microvasc Res 79:217–223. doi:10.1016/j.mvr.2010.01.007
Gao D, Nolan DJ, Mellick AS et al (2008) Endothelial progenitor cells control the angiogenic switch in mouse lung metastasis. Science 319:195–198. doi:10.1126/science.1150224
Peters BA, Diaz LA, Polyak K et al (2005) Contribution of bone marrow-derived endothelial cells to human tumor vasculature. Nat Med 11:261–262. doi:10.1038/nm1200
Larrivée B, Karsan A (2007) Involvement of marrow-derived endothelial cells in vascularization. Handb Exp Pharmacol. doi:10.1007/978-3-540-68976-8_5
Wickersheim A, Kerber M, de Miguel LS et al (2009) Endothelial progenitor cells do not contribute to tumor endothelium in primary and metastatic tumors. Int J Cancer 125:1771–1777. doi:10.1002/ijc.24605
Purhonen S, Palm J, Rossi D et al (2008) Bone marrow-derived circulating endothelial precursors do not contribute to vascular endothelium and are not needed for tumor growth. Proc Natl Acad Sci USA 105:6620–6625. doi:10.1073/pnas.0710516105
Larrivée B, Niessen K, Pollet I et al (2005) Minimal contribution of marrow-derived endothelial precursors to tumor vasculature. J Immunol Baltim Md 175:2890–2899
Machein MR, Renninger S, de Lima-Hahn E, Plate KH (2003) Minor contribution of bone marrow-derived endothelial progenitors to the vascularization of murine gliomas. Brain Pathol Zur Switz 13:582–597
Zentilin L, Tafuro S, Zacchigna S et al (2006) Bone marrow mononuclear cells are recruited to the sites of VEGF-induced neovascularization but are not incorporated into the newly formed vessels. Blood 107:3546–3554. doi:10.1182/blood-2005-08-3215
Ricci-Vitiani L, Pallini R, Biffoni M et al (2010) Tumour vascularization via endothelial differentiation of glioblastoma stem-like cells. Nature 468:824–828. doi:10.1038/nature09557
Kaur S, Bajwa P (2014) A “tête-à tête” between cancer stem cells and endothelial progenitor cells in tumor angiogenesis. Clin Trans Oncol 16:115–121. doi:10.1007/s12094-013-1103-4
Orth M, Lauber K, Niyazi M et al (2014) Current concepts in clinical radiation oncology. Radiat Environ Biophys 53:1–29. doi:10.1007/s00411-013-0497-2
Busk M, Horsman MR (2013) Relevance of hypoxia in radiation oncology: pathophysiology, tumor biology and implications for treatment. Q J Nucl Med Mol Imag 57:219–234
Cosse J-P, Michiels C (2008) Tumour hypoxia affects the responsiveness of cancer cells to chemotherapy and promotes cancer progression. Anticancer Agents Med Chem 8:790–797
Luk CK, Veinot-Drebot L, Tjan E, Tannock IF (1990) Effect of transient hypoxia on sensitivity to doxorubicin in human and murine cell lines. J Natl Cancer Inst 82:684–692
Young SD, Hill RP (1990) Effects of reoxygenation on cells from hypoxic regions of solid tumors: anticancer drug sensitivity and metastatic potential. J Natl Cancer Inst 82:371–380
Sanna K, Rofstad EK (1994) Hypoxia-induced resistance to doxorubicin and methotrexate in human melanoma cell lines in vitro. Int J Cancer 58:258–262
Viallard C, Chezal J-M, Mishellany F et al (2016) Targeting DNA repair by coDbait enhances melanoma targeted radionuclide therapy. Oncotarget 7:12927–12936. doi:10.18632/oncotarget.7340
Klein M, Lotem M, Peretz T et al (2013) Safety and efficacy of 188-rhenium-labeled antibody to melanin in patients with metastatic melanoma. J Skin Cancer 2013:828329. doi:10.1155/2013/828329
Huang Y, Goel S, Duda DG et al (2013) Vascular normalization as an emerging strategy to enhance cancer immunotherapy. Cancer Res 73:2943–2948. doi:10.1158/0008-5472.CAN-12-4354
Curiel TJ, Coukos G, Zou L et al (2004) Specific recruitment of regulatory T cells in ovarian carcinoma fosters immune privilege and predicts reduced survival. Nat Med 10:942–949. doi:10.1038/nm1093
Movahedi K, Laoui D, Gysemans C et al (2010) Different tumor microenvironments contain functionally distinct subsets of macrophages derived from Ly6C(high) monocytes. Cancer Res 70:5728–5739. doi:10.1158/0008-5472.CAN-09-4672
Corzo CA, Condamine T, Lu L et al (2010) HIF-1α regulates function and differentiation of myeloid-derived suppressor cells in the tumor microenvironment. J Exp Med 207:2439–2453. doi:10.1084/jem.20100587
Leung DW, Cachianes G, Kuang WJ et al (1989) Vascular endothelial growth factor is a secreted angiogenic mitogen. Science 246:1306–1309
Senger DR, Galli SJ, Dvorak AM et al (1983) Tumor cells secrete a vascular permeability factor that promotes accumulation of ascites fluid. Science 219:983–985
Crawford Y, Ferrara N (2009) VEGF inhibition: insights from preclinical and clinical studies. Cell Tissue Res 335:261–269. doi:10.1007/s00441-008-0675-8
Ohtsu A, Shah MA, Van Cutsem E et al (2011) Bevacizumab in combination with chemotherapy as first-line therapy in advanced gastric cancer: a randomized, double-blind, placebo-controlled phase III study. J Clin Oncol 29:3968–3976. doi:10.1200/JCO.2011.36.2236
Reck M, von Pawel J, Zatloukal P et al (2009) Phase III trial of cisplatin plus gemcitabine with either placebo or bevacizumab as first-line therapy for nonsquamous non-small-cell lung cancer: AVAil. J Clin Oncol 27:1227–1234. doi:10.1200/JCO.2007.14.5466
Miller K, Wang M, Gralow J et al (2007) Paclitaxel plus bevacizumab versus paclitaxel alone for metastatic breast cancer. N Engl J Med 357:2666–2676. doi:10.1056/NEJMoa072113
Escudier B, Eisen T, Stadler WM et al (2007) Sorafenib in advanced clear-cell renal-cell carcinoma. N Engl J Med 356:125–134. doi:10.1056/NEJMoa060655
Jayson GC, Kerbel R, Ellis LM, Harris AL (2016) Antiangiogenic therapy in oncology: current status and future directions. Lancet Lond Engl 388:518–529. doi:10.1016/S0140-6736(15)01088-0
Fan F, Samuel S, Gaur P et al (2011) Chronic exposure of colorectal cancer cells to bevacizumab promotes compensatory pathways that mediate tumour cell migration. Br J Cancer 104:1270–1277. doi:10.1038/bjc.2011.81
Widakowich C, de Castro G, de Azambuja E et al (2007) Review: side effects of approved molecular targeted therapies in solid cancers. Oncologist 12:1443–1455. doi:10.1634/theoncologist.12-12-1443
Tolaney SM, Boucher Y, Duda DG et al (2015) Role of vascular density and normalization in response to neoadjuvant bevacizumab and chemotherapy in breast cancer patients. Proc Natl Acad Sci USA 112:14325–14330. doi:10.1073/pnas.1518808112
Winkler F, Kozin SV, Tong RT et al (2004) Kinetics of vascular normalization by VEGFR2 blockade governs brain tumor response to radiation: role of oxygenation, angiopoietin-1, and matrix metalloproteinases. Cancer Cell 6:553–563. doi:10.1016/j.ccr.2004.10.011
Batchelor TT, Sorensen AG, di Tomaso E et al (2007) AZD2171, a pan-VEGF receptor tyrosine kinase inhibitor, normalizes tumor vasculature and alleviates edema in glioblastoma patients. Cancer Cell 11:83–95. doi:10.1016/j.ccr.2006.11.021
Graeber TG, Osmanian C, Jacks T et al (1996) Hypoxia-mediated selection of cells with diminished apoptotic potential in solid tumours. Nature 379:88–91. doi:10.1038/379088a0
Ebos JML, Kerbel RS (2011) Antiangiogenic therapy: impact on invasion, disease progression, and metastasis. Nat Rev Clin Oncol 8:210–221. doi:10.1038/nrclinonc.2011.21
Huang Y, Yuan J, Righi E et al (2012) Vascular normalizing doses of antiangiogenic treatment reprogram the immunosuppressive tumor microenvironment and enhance immunotherapy. Proc Natl Acad Sci USA 109:17561–17566. doi:10.1073/pnas.1215397109
Martin JD, Fukumura D, Duda DG et al (2016) Reengineering the tumor microenvironment to alleviate hypoxia and overcome cancer heterogeneity. Cold Spring Harb Perspect Med. doi:10.1101/cshperspect.a027094
Chen B-B, Lu Y-S, Lin C-H et al (2016) A pilot study to determine the timing and effect of bevacizumab on vascular normalization of metastatic brain tumors in breast cancer. BMC Cancer 16:466. doi:10.1186/s12885-016-2494-8
Lin A, Hahn SM (2012) Hypoxia imaging markers and applications for radiation treatment planning. Semin Nucl Med 42:343–352. doi:10.1053/j.semnuclmed.2012.04.002
Becker S, Bohn P, Bouyeure-Petit A-C et al (2015) Bevacizumab enhances efficiency of radiotherapy in a lung adenocarcinoma rodent model: role of αvβ3 imaging in determining optimal window. Nucl Med Biol 42:923–930. doi:10.1016/j.nucmedbio.2015.08.002
Hapani S, Sher A, Chu D, Wu S (2010) Increased risk of serious hemorrhage with bevacizumab in cancer patients: a meta-analysis. Oncology 79:27–38. doi:10.1159/000314980
Nalluri SR, Chu D, Keresztes R et al (2008) Risk of venous thromboembolism with the angiogenesis inhibitor bevacizumab in cancer patients: a meta-analysis. JAMA 300:2277–2285. doi:10.1001/jama.2008.656
Bergers G, Hanahan D (2008) Modes of resistance to anti-angiogenic therapy. Nat Rev Cancer 8:592–603. doi:10.1038/nrc2442
Xian X, Håkansson J, Ståhlberg A et al (2006) Pericytes limit tumor cell metastasis. J Clin Invest 116:642–651. doi:10.1172/JCI25705
García-Román J, Zentella-Dehesa A (2013) Vascular permeability changes involved in tumor metastasis. Cancer Lett 335:259–269. doi:10.1016/j.canlet.2013.03.005
Thomas M, Augustin HG (2009) The role of the Angiopoietins in vascular morphogenesis. Angiogenesis 12:125–137. doi:10.1007/s10456-009-9147-3
Witzenbichler B, Maisonpierre PC, Jones P et al (1998) Chemotactic properties of angiopoietin-1 and -2, ligands for the endothelial-specific receptor tyrosine kinase Tie2. J Biol Chem 273:18514–18521
Jones N, Master Z, Jones J et al (1999) Identification of Tek/Tie2 binding partners. Binding to a multifunctional docking site mediates cell survival and migration. J Biol Chem 274:30896–30905
Hayes AJ, Huang WQ, Mallah J et al (1999) Angiopoietin-1 and its receptor Tie-2 participate in the regulation of capillary-like tubule formation and survival of endothelial cells. Microvasc Res 58:224–237. doi:10.1006/mvre.1999.2179
Teichert-Kuliszewska K, Maisonpierre PC, Jones N et al (2001) Biological action of angiopoietin-2 in a fibrin matrix model of angiogenesis is associated with activation of Tie2. Cardiovasc Res 49:659–670
Kwak HJ, So JN, Lee SJ et al (1999) Angiopoietin-1 is an apoptosis survival factor for endothelial cells. FEBS Lett 448:249–253
Kim I, Kim JH, Moon SO et al (2000) Angiopoietin-2 at high concentration can enhance endothelial cell survival through the phosphatidylinositol 3′-kinase/Akt signal transduction pathway. Oncogene 19:4549–4552. doi:10.1038/sj.onc.1203800
Holash J, Wiegand SJ, Yancopoulos GD (1999) New model of tumor angiogenesis: dynamic balance between vessel regression and growth mediated by angiopoietins and VEGF. Oncogene 18:5356–5362. doi:10.1038/sj.onc.1203035
Nasarre P, Thomas M, Kruse K et al (2009) Host-derived angiopoietin-2 affects early stages of tumor development and vessel maturation but is dispensable for later stages of tumor growth. Cancer Res 69:1324–1333. doi:10.1158/0008-5472.CAN-08-3030
Leow CC, Coffman K, Inigo I et al (2012) MEDI3617, a human anti-angiopoietin 2 monoclonal antibody, inhibits angiogenesis and tumor growth in human tumor xenograft models. Int J Oncol 40:1321–1330. doi:10.3892/ijo.2012.1366
Holopainen T, Saharinen P, D’Amico G et al (2012) Effects of angiopoietin-2-blocking antibody on endothelial cell-cell junctions and lung metastasis. J Natl Cancer Inst 104:461–475. doi:10.1093/jnci/djs009
Peterson TE, Kirkpatrick ND, Huang Y et al (2016) Dual inhibition of Ang-2 and VEGF receptors normalizes tumor vasculature and prolongs survival in glioblastoma by altering macrophages. Proc Natl Acad Sci USA 113:4470–4475. doi:10.1073/pnas.1525349113
Kloepper J, Riedemann L, Amoozgar Z et al (2016) Ang-2/VEGF bispecific antibody reprograms macrophages and resident microglia to anti-tumor phenotype and prolongs glioblastoma survival. Proc Natl Acad Sci USA 113:4476–4481. doi:10.1073/pnas.1525360113
Coxon A, Bready J, Min H et al (2010) Context-dependent role of angiopoietin-1 inhibition in the suppression of angiogenesis and tumor growth: implications for AMG 386, an angiopoietin-1/2-neutralizing peptibody. Mol Cancer Ther 9:2641–2651. doi:10.1158/1535-7163.MCT-10-0213
Mita AC, Takimoto CH, Mita M et al (2010) Phase 1 study of AMG 386, a selective angiopoietin 1/2-neutralizing peptibody, in combination with chemotherapy in adults with advanced solid tumors. Clin Cancer Res 16:3044–3056. doi:10.1158/1078-0432.CCR-09-3368
Monk BJ, Poveda A, Vergote I et al (2016) Final results of a phase 3 study of trebananib plus weekly paclitaxel in recurrent ovarian cancer (TRINOVA-1): long-term survival, impact of ascites, and progression-free survival-2. Gynecol Oncol 143:27–34. doi:10.1016/j.ygyno.2016.07.112
Goel S, Gupta N, Walcott BP et al (2013) Effects of vascular-endothelial protein tyrosine phosphatase inhibition on breast cancer vasculature and metastatic progression. J Natl Cancer Inst 105:1188–1201. doi:10.1093/jnci/djt164
Park J-S, Kim I-K, Han S et al (2016) Normalization of tumor vessels by Tie2 activation and Ang2 inhibition enhances drug delivery and produces a favorable tumor microenvironment. Cancer Cell 30:953–967. doi:10.1016/j.ccell.2016.10.018
Chakroborty D, Sarkar C, Yu H et al (2011) Dopamine stabilizes tumor blood vessels by up-regulating angiopoietin 1 expression in pericytes and Kruppel-like factor-2 expression in tumor endothelial cells. Proc Natl Acad Sci USA 108:20730–20735. doi:10.1073/pnas.1108696108
Al-Husein B, Goc A, Somanath PR (2013) Suppression of interactions between prostate tumor cell integrin αvβ3 and endothelial ICAM-1 by simvastatin inhibits prostate cancer micrometastasis. J Cell Physiol 228:2139. doi:10.1002/jcp.24381
Heldin C-H (2013) Targeting the PDGF signaling pathway in tumor treatment. Cell Commun Signal CCS 11:97. doi:10.1186/1478-811X-11-97
Huang J, Soffer SZ, Kim ES et al (2004) Vascular remodeling marks tumors that recur during chronic suppression of angiogenesis. Mol Cancer Res MCR 2:36–42
Bergers G, Song S, Meyer-Morse N et al (2003) Benefits of targeting both pericytes and endothelial cells in the tumor vasculature with kinase inhibitors. J Clin Invest 111:1287–1295. doi:10.1172/JCI200317929
Erber R, Thurnher A, Katsen AD et al (2004) Combined inhibition of VEGF and PDGF signaling enforces tumor vessel regression by interfering with pericyte-mediated endothelial cell survival mechanisms. FASEB J 18:338–340. doi:10.1096/fj.03-0271fje
Timke C, Zieher H, Roth A et al (2008) Combination of vascular endothelial growth factor receptor/platelet-derived growth factor receptor inhibition markedly improves radiation tumor therapy. Clin Cancer Res 14:2210–2219. doi:10.1158/1078-0432.CCR-07-1893
Hawthorne T, Giot L, Blake L et al (2008) A phase I study of CR002, a fully-human monoclonal antibody against platelet-derived growth factor-D. Int J Clin Pharmacol Ther 46:236–244
Jayson GC, Parker GJM, Mullamitha S et al (2005) Blockade of platelet-derived growth factor receptor-beta by CDP860, a humanized, PEGylated di-Fab’, leads to fluid accumulation and is associated with increased tumor vascularized volume. J Clin Oncol 23:973–981. doi:10.1200/JCO.2005.01.032
Shen J, Vil MD, Prewett M et al (2009) Development of a fully human anti-PDGFRbeta antibody that suppresses growth of human tumor xenografts and enhances antitumor activity of an anti-VEGFR2 antibody. Neoplasia NY N 11:594–604
Falcon BL, Pietras K, Chou J et al (2011) Increased vascular delivery and efficacy of chemotherapy after inhibition of platelet-derived growth factor-B. Am J Pathol 178:2920. doi:10.1016/j.ajpath.2011.02.019
Lu C, Shahzad MMK, Moreno-Smith M et al (2010) Targeting pericytes with a PDGF-B aptamer in human ovarian carcinoma models. Cancer Biol Ther 9:176
Davis DW, Takamori R, Raut CP et al (2005) Pharmacodynamic analysis of target inhibition and endothelial cell death in tumors treated with the vascular endothelial growth factor receptor antagonists SU5416 or SU6668. Clin Cancer Res 11:678–689
Nisancioglu MH, Betsholtz C, Genové G (2010) The absence of pericytes does not increase the sensitivity of tumor vasculature to vascular endothelial growth factor-A blockade. Cancer Res 70:5109–5115. doi:10.1158/0008-5472.CAN-09-4245
Kim J, de Sampaio PC, Lundy DM et al (2016) Heterogeneous perivascular cell coverage affects breast cancer metastasis and response to chemotherapy. JCI Insight 1:e90733. doi:10.1172/jci.insight.90733
McCarty MF, Somcio RJ, Stoeltzing O et al (2007) Overexpression of PDGF-BB decreases colorectal and pancreatic cancer growth by increasing tumor pericyte content. J Clin Invest 117:2114. doi:10.1172/JCI31334
Reis M, Czupalla CJ, Ziegler N et al (2012) Endothelial Wnt/β-catenin signaling inhibits glioma angiogenesis and normalizes tumor blood vessels by inducing PDGF-B expression. J Exp Med 209:1611. doi:10.1084/jem.20111580
Liu J, Liao S, Huang Y et al (2011) PDGF-D improves drug delivery and efficacy via vascular normalization, but promotes lymphatic metastasis by activating CXCR4 in breast cancer. Clin Cancer Res 17:3638–3648. doi:10.1158/1078-0432.CCR-10-2456
Lamouille S, Mallet C, Feige J-J, Bailly S (2002) Activin receptor-like kinase 1 is implicated in the maturation phase of angiogenesis. Blood 100:4495–4501. doi:10.1182/blood.V100.13.4495
Suzuki Y, Ohga N, Morishita Y et al (2010) BMP-9 induces proliferation of multiple types of endothelial cells in vitro and in vivo. J Cell Sci 123:1684–1692. doi:10.1242/jcs.061556
Valdimarsdottir G, Goumans M-J, Rosendahl A et al (2002) Stimulation of Id1 expression by bone morphogenetic protein is sufficient and necessary for bone morphogenetic protein-induced activation of endothelial cells. Circulation 106:2263–2270
Itoh F, Itoh S, Goumans M-J et al (2004) Synergy and antagonism between Notch and BMP receptor signaling pathways in endothelial cells. EMBO J 23:541–551. doi:10.1038/sj.emboj.7600065
Larrivée B, Prahst C, Gordon E et al (2012) ALK1 signaling inhibits angiogenesis by cooperating with the Notch pathway. Dev Cell 22:489–500. doi:10.1016/j.devcel.2012.02.005
Rostama B, Turner JE, Seavey GT et al (2015) DLL4/Notch1 and BMP9 interdependent signaling induces human endothelial cell quiescence via P27KIP1 and thrombospondin-1. Arterioscler Thromb Vasc Biol 35:2626–2637. doi:10.1161/ATVBAHA.115.306541
Scharpfenecker M, van Dinther M, Liu Z et al (2007) BMP-9 signals via ALK1 and inhibits bFGF-induced endothelial cell proliferation and VEGF-stimulated angiogenesis. J Cell Sci 120:964–972. doi:10.1242/jcs.002949
David L, Mallet C, Keramidas M et al (2008) Bone morphogenetic protein-9 is a circulating vascular quiescence factor. Circ Res 102:914–922. doi:10.1161/CIRCRESAHA.107.165530
Gupta S, Gill D, Pal SK, Agarwal N (2015) Activin receptor inhibitors–dalantercept. Curr Oncol Rep 17:14. doi:10.1007/s11912-015-0441-5
Mitchell D, Pobre EG, Mulivor AW et al (2010) ALK1-Fc inhibits multiple mediators of angiogenesis and suppresses tumor growth. Mol Cancer Ther 9:379–388. doi:10.1158/1535-7163.MCT-09-0650
Makker V, Filiaci VL, Chen L-M et al (2015) Phase II evaluation of dalantercept, a soluble recombinant activin receptor-like kinase 1 (ALK1) receptor fusion protein, for the treatment of recurrent or persistent endometrial cancer: an NRG Oncology/Gynecologic Oncology Group Study 0229N. Gynecol Oncol 138:24–29. doi:10.1016/j.ygyno.2015.04.006
Wang X, Solban N, Khanna P et al (2016) Inhibition of ALK1 signaling with dalantercept combined with VEGFR TKI leads to tumor stasis in renal cell carcinoma. Oncotarget. doi:10.18632/oncotarget.9621
van Meeteren LA, Thorikay M, Bergqvist S et al (2012) Anti-human activin receptor-like kinase 1 (ALK1) antibody attenuates bone morphogenetic protein 9 (BMP9)-induced ALK1 signaling and interferes with endothelial cell sprouting. J Biol Chem 287:18551–18561. doi:10.1074/jbc.M111.338103
Necchi A, Giannatempo P, Mariani L et al (2014) PF-03446962, a fully-human monoclonal antibody against transforming growth-factor β (TGFβ) receptor ALK1, in pre-treated patients with urothelial cancer: an open label, single-group, phase 2 trial. Invest New Drugs 32:555–560. doi:10.1007/s10637-014-0074-9
Wilson CW, Ye W (2014) Regulation of vascular endothelial junction stability and remodeling through Rap1-Rasip1 signaling. Cell Adhes Migr 8:76–83
Maharjan S, Kim K, Agrawal V et al (2013) Sac-1004, a novel vascular leakage blocker, enhances endothelial barrier through the cAMP/Rac/cortactin pathway. Biochem Biophys Res Commun 435:420–427. doi:10.1016/j.bbrc.2013.04.104
Agrawal V, Maharjan S, Kim K et al (2014) Direct endothelial junction restoration results in significant tumor vascular normalization and metastasis inhibition in mice. Oncotarget 5:2761–2777
Lee K, Agrawal V, Kim K et al (2014) Combined effect of vascular-leakage-blocker Sac-1004 and antiangiogenic drug sunitinib on tumor angiogenesis. Biochem Biophys Res Commun 450:1320–1326. doi:10.1016/j.bbrc.2014.06.139
Loboda A, Jozkowicz A, Dulak J (2010) HIF-1 and HIF-2 transcription factors–similar but not identical. Mol Cells 29:435–442. doi:10.1007/s10059-010-0067-2
Skuli N, Liu L, Runge A et al (2009) Endothelial deletion of hypoxia-inducible factor-2alpha (HIF-2alpha) alters vascular function and tumor angiogenesis. Blood 114:469–477. doi:10.1182/blood-2008-12-193581
Le Bras A, Lionneton F, Mattot V et al (2007) HIF-2alpha specifically activates the VE-cadherin promoter independently of hypoxia and in synergy with Ets-1 through two essential ETS-binding sites. Oncogene 26:7480–7489. doi:10.1038/sj.onc.1210566
Kleibeuker EA, Fokas E, Allen PD et al (2016) Low dose angiostatic treatment counteracts radiotherapy-induced tumor perfusion and enhances the anti-tumor effect. Oncotarget. doi:10.18632/oncotarget.12814
Zhang B, Shi W, Jiang T et al (2016) Optimization of the tumor microenvironment and nanomedicine properties simultaneously to improve tumor therapy. Oncotarget 7:62607–62618. doi:10.18632/oncotarget.11546
Maes H, Kuchnio A, Peric A et al (2014) Tumor vessel normalization by chloroquine independent of autophagy. Cancer Cell 26:190–206. doi:10.1016/j.ccr.2014.06.025
Liu F, Wang P, Jiang X et al (2008) Antisense hypoxia-inducible factor 1alpha gene therapy enhances the therapeutic efficacy of doxorubicin to combat hepatocellular carcinoma. Cancer Sci 99:2055–2061. doi:10.1111/j.1349-7006.2008.00905.x
Daskalow K, Rohwer N, Raskopf E et al (2010) Role of hypoxia-inducible transcription factor 1alpha for progression and chemosensitivity of murine hepatocellular carcinoma. J Mol Med Berl Ger 88:817–827. doi:10.1007/s00109-010-0623-4
Choi SH, Shin HW, Park JY et al (2010) Effects of the knockdown of hypoxia inducible factor-1α expression by adenovirus-mediated shRNA on angiogenesis and tumor growth in hepatocellular carcinoma cell lines. Korean J Hepatol 16:280–287. doi:10.3350/kjhep.2010.16.3.280
Choi SH, Kwon O-J, Park JY et al (2014) Inhibition of tumour angiogenesis and growth by small hairpin HIF-1α and IL-8 in hepatocellular carcinoma. Liver Int 34:632–642. doi:10.1111/liv.12375
Acknowledgements
This work was supported from an operating grant of the Cancer Research Society of Canada and a New Investigator Award from the Heart and Stroke Foundation of Canada (B.L.).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Viallard, C., Larrivée, B. Tumor angiogenesis and vascular normalization: alternative therapeutic targets. Angiogenesis 20, 409–426 (2017). https://doi.org/10.1007/s10456-017-9562-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10456-017-9562-9