Abstract
Hydatid disease (HD) is a commonly occurring zoonotic disease caused by tapeworms of the genus Echinococcus. It is endemic in many parts of the world and can involve almost any organ of the body. Although HD of the liver and lungs is quite common, ovarian involvement is rare. We present a case of a 24-year-old female patient who was diagnosed with multifocal hydatidosis involving the liver and bilateral ovaries on imaging. Postoperative histopathology confirmed the hydatid disease in the liver and one ovary. However, the cystic lesion in the other ovary turned out to be a borderline serous cystadenoma. This case highlights the limitation of imaging in differentiating between simple hydatid cysts and serous cystadenomas of the ovaries. Another point we learnt is that even in the presence of multifocal hydatidosis in endemic regions, serous cystadenoma needs to be considered in imaging differential diagnosis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
HD is a parasitic infection caused by the tapeworm Echinococcus granulosus. The infection is commonly seen in underdeveloped cattle-raising countries of the world with poor veterinary control like the Mediterranean region, Middle East, Australia, Africa, and South America [1]. Dogs are the definitive host, while sheep and cattle are the intermediate hosts. Humans are infected by close contact with definitive hosts or by consumption of food or water contaminated with dog feces containing the eggs of the parasite.
Liver (75 %) and lungs (24 %) are the most common sites of involvement, although any organ of the body can be involved [2]. In the absence of previous surgery or cyst rupture, pelvic hydatidosis with involvement of the female genital tract is extremely rare [3]. Our case highlights the limitations of imaging in differentiating simple hydatid cysts from serous cystadenomas of the ovaries. Another point we learnt is that even in the presence of multifocal hydatidosis in endemic regions, a serous cystadenoma needs to be considered in imaging differential diagnosis. Concomitant involvement of the ovaries by a complex thick-walled hydatid cyst and a borderline ovarian serous cystadenoma is the uniqueness of our present case, which is very rarely reported in the English literature [4, 5].
Case report
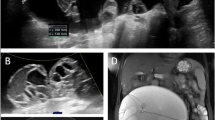
A 24-year-old female presented to the gynaecology outpatient department with complaint of pelvic discomfort persisting for 6 months. Physical examination was unremarkable except for mild pallor. The patient was advised to undergo trans-abdominal ultrasound, which revealed a complex cystic lesion with double wall, thick septations, echogenic debris, and internal floating membranes in segment 6 of the liver diagnosed as a hydatid cyst (Fig. 1a). There was a large thick-walled, multiloculated cystic lesion with thick septations in the right adnexa with non-visualization of the right ovary separately and a small thick-walled unilocular cyst seen in the left ovary (Fig. 1b, c). There was no evidence of calcifications, solid component, or papillary projections within the pelvic lesions. Chest radiograph showed bilateral clear lungs. CA-125 level was within normal limits. The serum echinococcus hemagglutination test was positive (1/2048), and enzyme-linked immunosorbent assay for echinococcal IgE was 52.1 Ku/L. Abdominal MRI was performed to delineate the extent of the lesion and to detect any additional lesions. A complex septated cystic lesion following the signal characteristics of fluid was noted in the liver. Both the outer wall and septa showed a low signal on both T1- and T2-weighted imaging (rim sign). In the pelvis, a large circumscribed cystic lesion with septations was seen in the right adnexa. The right ovary was not separately demarcated from the lesion. Another cystic lesion was seen in the left ovary (Fig. 2). The uterus appeared normal. An imaging diagnosis of multifocal hydatidosis involving the liver and bilateral ovaries was made.
a Transabdominal ultrasonography shows a well-defined complex septated cystic lesion with detached membrane and echogenic debris in the right lobe of the liver. b It shows a well-defined multiloculated cystic lesion giving rise to honeycombing appearance in the right adnexa. c Left ovarian unilocular cyst with a thick wall (white arrow). No evidence of wall calcification is seen in either of the pelvic lesions
The patient was started on albendazole therapy and surgical excision of the cysts was planned. The patient underwent an exploratory laparotomy under general anesthesia. It revealed a large 9 × 10-cm multilocular cystic lesion on the right side, which was confirmed on histopathology to be a hydatid cyst (Fig. 3). A 2 × 2-cm lesion in the left ovary was excised, and it turned out to be a borderline serous cystadenoma on histopathology (Fig. 4). No surgical procedure was done for the liver hydatid, which showed a marked reduction in size following the medical therapy. The patient was discharged on the 7th postoperative day with no significant postoperative complication noted.
Discussion
The liver and lungs are the most common sites of HD. Primary ovarian HD is extremely rare with very few cases reported in the literature [2, 6, 7]. Secondary ovarian HD is more common and is generally secondary to peritoneal spread of daughter cysts from ruptured liver HD. Clinical symptoms in pelvic HD are nonspecific and can range from entirely asymptomatic to vague pelvic pain, infertility, or urinary disturbances.
Pathologically, a hydatid cyst consists of three layers. Pericyst, the outermost layer, is made up of inflammatory host cells and is formed because of host immune response to the parasite. The middle layer, ectocyst or laminar membrane, is acellular and allows passage of nutrients. The innermost germinal layer is the germinative layer of the cyst. Larval embryos or scolices develop from outpouching of the germinal layer, called brood capsules. The cyst fluid is clear and antigenic. When released in the circulation, it may cause minor to severe allergic reactions [8, 9].
A high index of suspicion is required to diagnose ovarian HD as the lesions can simulate cystadenomas, cystadenocarcinomas, endometriomas, or polycystic ovarian disease [2, 4, 5, 10, 11]. Pelvic HD is an important differential diagnosis that has to be considered, especially in endemic areas, in cases of cystic ovarian lesions on imaging [12]. The differentiation becomes more difficult when we encounter an unilocular cyst as seen in the left ovary in our case, especially in the absence of wall calcification or double wall sign [2].The presence of a cystic lesion with internal septation or a solid lesion with internal hypoechoic or cystic areas or atypical wall should raise the suspicion of a hydatid cyst in endemic regions [12]. The present case highlights the fact that even in the presence of multifocal hydatidosis, an unilocular cyst can be a cystadenoma.
The radiological appearance may vary according to the developmental stage of the parasite. In the initial stage (Type 1), the appearance can be completely anechoic on USG with or without septa or echogenic hydatid sand. In the later development stage (Type 2), detachment of the laminar membrane can give rise to a floating membrane appearance, while multiple peripherally arranged daughter cysts enclosed within a single capsule can lead to a spoke wheel or racemose appearance. The cyst wall can be seen as two echogenic lines separated by a thin hypoechoic zone, known as the “double wall sign”. Contrast enhanced CT or MR imaging leads to enhancement of the cyst wall and septations, an important differentiating feature from simple hepatic cysts. On MRI, the rim sign depicted as a low-intensity rim on T2-weighted imaging due to the fibrous nature of the pericyst is also a salient feature of hydatid cysts that helps to differentiate them from other types of cysts. The cyst can sometimes undergo complete calcification (Type 3) due to the death of the parasite. The cyst can also be complicated by rupture that can be contained, communicating, or direct. Contained ruptures are clinically silent. Communicating ruptures may lead to infection of the cyst or biliary communication. Direct ruptures into the peritoneal or pleural cavity can cause anaphylaxis or dissemination of the cyst [2, 8, 9].
The treatment of pelvic hydatid disease consists mainly of surgical excision of the lesion. Albendazole is given preoperatively to reduce the size. To avoid intraoperative rupture of the cyst, laparotomy is preferred over a laparoscopic procedure. In cases of ovarian HD, total cystectomy is the treatment of choice whenever possible [13]. However, because of the patient being in the reproductive age group in our case, left ovarian lesion excision was performed. In some cases of pelvic hydatid cyst, cyst extirpation and aspiration with saline or other agents has been reported. The overall prognosis of these cysts is good with reported recurrence of 7–14 % [9].
References
Beggs I. The radiology of hydatid disease. AJR Am J Roentgenol. 1985;145:639–48.
Polat P, Kantarci M, Alper F, et al. Hydatid disease from head to toe. Radiographics. 2003;23:475–94.
Georgakopoulos PA, Gogas CG, Sariyannis HG. Hydatid disease of the female genitalia. Obstet Gynecol. 1980;55:555–9.
Biswas B, Mondal P, Das T, et al. Rare coexisting primary hydatid cyst and mucinous cyst adenoma of right ovary. Indian J Clin Pract. 2013;24:469–71.
Gungor T, Altinkaya SO, Sirvan L, et al. Coexistence of borderline ovarian epithelial tumor, primary pelvic hydatid cyst, and lymphoepithelioma-like gastric carcinoma. Taiwan J Obstet Gynecol. 2011;50:201–4.
Hangval H, Habibi H, Moshref A, et al. Case report of an ovarian hydatid cyst. J Trop Med Hyg. 1979;82:34–5.
Amin MU, Mahmood R, Shafique M, et al. Pictorial review: imaging features of unusual patterns and complications of hydatid disease. J Radiol Case Rep. 2009;3:1–24.
Lewall DB. Hydatid disease: biology, pathology, imaging and classification. Clin Radiol. 1998;52:863–74.
Jha A, Ullah E, Gupta P, et al. Sonography of multifocal hydatidosis involving lung and liver in a female child. J Med Ultrason. 2013;40:471–4.
Pekindil G, Tenekeci N. Solid appearing pelvic hydatic cyst: transabdominal and transvaginal sonographic diagnosis. Ultrasound Obstet Gynecol. 1997;9:289–91.
Aysun A, Petek BK, Mehmet AY, et al. Huge solitary primary pelvic hydatid cyst presenting as an ovarian malignancy: case report. J Turkish German Gynecol Assoc. 2009;10:181–3.
Ranzini AC, Hale DC, Sonam MD, et al. Ultrasonographic diagnosis of pelvic echinococcosis: case report and review of the literature. J Ultrasound Med. 2002;21:207–10.
Hamamci EO, Besim H, Korkmaz A. Unusual locations of hydatid disease and surgical approach. ANZ J Surg. 2004;74:356–60.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical statement
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2008.
Informed consent
Informed consent was obtained from the patient for being included in this case report.
Conflict of interest
The authors declare that they have no conflict of interest.
About this article
Cite this article
Khalid, S., Jamal, F., Rafat, D. et al. Coexistent borderline serous cystadenoma with multifocal hydatidosis in a young female: lessons learnt. J Med Ultrasonics 43, 553–556 (2016). https://doi.org/10.1007/s10396-016-0727-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10396-016-0727-8